Abstract
Ionizing radiation administered for cancer treatment or from nuclear plant accidents are two common causes of radiation exposure. Ionizing radiation exposure generates reactive oxygen species and free radicals, which cause oxidative stress. We previously reported that taurine contributes to the recovery from radiation-induced injuries, suggesting its potential as a radioprotector and radiation mitigator. However, the effect of taurine on radiation-induced gastrointestinal syndrome remains poorly understood. The aim of this study was to examine the effect of taurine tissue depletion on radiation-induced gastrointestinal syndrome. Mouse models of radiation-induced gastrointestinal syndrome were established in TauT+/+ and TauT−/− mice by whole-body X-irradiation. We examined the 30-day survival rate, as well as the crypt-villus structure and proliferation of proliferating cell nuclear antigen (PCNA) + cells in the small intestine. The survival rate of TauT−/− mice was significantly lower than that of TauT+/+ mice. The villi in the small intestine of TauT−/− mice were significantly shorter than those in TauT+/+ mice. Additionally, there were significantly fewer PCNA+ cells in TauT−/− mice than in TauT+/+ mice. These data demonstrate that taurine is a key regulator of crypt stem cells and plays an important regulatory role in intestinal cell survival, proliferation, and fate. Therefore, taurine may reduce radiation-induced gastrointestinal syndrome.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Exposure to ionizing radiation generates reactive oxygen species (ROS) and free radicals, which, in turn, can cause oxidative stress in the irradiated cells. ROS attack, either directly or indirectly, virtually all cellular components, including DNA, proteins, and lipids. ROS can also impair cellular functions and enhance inflammatory responses (Li et al. 2018). Free radicals can cause double-stranded breaks (DSBs) and single-stranded breaks (SSBs) in DNA, promote apoptosis and modulate inflammatory processes (Duan et al. 2017; Smith et al. 2017). Radiation-induced injuries can easily induce DSBs and SSBs in organs such as the intestines, bone marrow, and skin. Radioprotective agents provide protection by removing free radicals and have been studied for a long time for their ability to reduce cell damage caused by free radicals in normal tissues (Weiss and Landauer 2009; Poggi et al. 2001).
Research on the radioprotective effect of taurine has been carried out since the 1960s (Sugahara et al. 1969), and the physiological roles of taurine include antioxidant activity and protection against ROS and free radical formation (Johnson et al. 2012). Thus, taurine appears to be an attractive candidate for use as a radioprotector and radiation mitigator. We previously reported that taurine can promote recovery from radiation-induced injuries (Yamashita et al. 2017). However, at present, the effect of taurine on radiation-induced injuries remains poorly understood.
Taurine is taken up by cells via the taurine transporter (TauT) (Kwon and Handler 1995). In TauT KO mice that lack the TauT gene, taurine levels are markedly decreased in several tissues. Compared to wild-type mice, taurine levels in TauT KO mice are decreased by 96–98%, in skeletal and cardiac muscle, and by 70–90% in the brain, kidney, and liver (Ito et al. 2010; Heller-Stilb et al. 2002). Taurine depletion is likely harmful because it blocks the recovery of physiological functions that depend on cellular growth, the immune system, and intestinal mucosa function.
Exposure to ionizing radiation causes injury to organs containing rapidly proliferating cells, resulting in acute radiation syndromes, such as hematopoietic syndrome and gastrointestinal syndrome (Suman et al. 2012). Gastrointestinal syndrome leads to death within 10–12 days after ionizing radiation exposure (Rosen et al. 2015). A loss of villus epithelial cells or crypt stem cells has been suggested as the potential cause of gastrointestinal syndrome (Qiu et al. 2008). Taurine has been reported to be essential for optimal proliferation, development, and maturation of brain cells. Furthermore, taurine increases neural stem/progenitor cell proliferation in the developing brain (Shivaraj et al. 2012). Thus, taurine might be involved in the proliferation of stem cells. Tissue depletion of taurine might be associated with the impairment of the proliferating ability of intestinal stem cells after X-irradiation. Therefore, it is of interest to investigate whether knockout of the taurine transporter in mice aggravates radiation-induced gastrointestinal syndrome. In this study, we evaluated the role of taurine on survival, the crypt-villus structure in the small intestine, and the proliferation of proliferating cell nuclear antigen (PCNA)+ cells in the small intestine using a taurine-deficient mouse model generated by knocking out the taurine transporter (Ito et al. 2008).
2 Methods
2.1 Animals
TauTKO (TauT−/−) mice and their wild-type (TauT+/+) littermates were obtained by breeding heterozygous (Tau+/−) males and females. Female, 6-week-old TauTKO mice and WT littermates were handled according to the Guidelines for the Regulation of Animals, from the Animal Ethics Committee of Suzuka University of Medical Science (Suzuka, Mie-ken, Japan). The animals were maintained under controlled conditions at 22 ± 3 °C with 65 ± 5% relative humidity and a 12 h light/dark cycle (light from 08:00 to 20:00).
2.2 X-Irradiation of Mice
Mice were placed in well-ventilated boxes (five mice in each box) and irradiated with 5 Gy of whole-body irradiation at a dose rate of 0.331 Gy/min at 200 kV and 9 mA (Phillips MG226, Tokyo, Japan). The beam was filtered through a 0.2 mm copper and 1 mm aluminum board. After irradiation, the mice were returned to their cages and maintained on food and water ad libitum.
2.3 Survival Studies
Two groups of 10 mice each were used in the survival experiments. Mice were exposed to whole-body X-irradiation (5 Gy/mouse) and then monitored continuously for a period of 30 days for survival and apparent behavioral deficits.
2.4 Immunohistochemical Studies
TauTKO (TauT−/−) mice and wild-type (TauT+/+) mice exposed to 5 Gy of radiation were killed on day 3 (n = 3 per group) for immunochemical analysis of the small intestine. After sacrifice, the small intestines were removed, fixed with 3.7% paraformaldehyde overnight, and then embedded in paraffin. Then, 7 μm thick paraffin sections were stained with hematoxylin and eosin (H&E). Rabbit taurine-specific antibodies were prepared as described previously (Ma et al. 1994). A PCNA antibody (bs-2007R) was obtained from Bioss Inc. (Woburn, MA, USA). PCNA antibody immunoreactivity in intestinal sections from the mice was observed using the peroxidase anti-peroxidase (PAP) method. Briefly, paraffin sections (6 μm thick) were incubated with rabbit anti-PCNA polyclonal antibody (2 μg/ml) overnight at room temperature. Then, the sections were incubated with a goat antibody against rabbit IgG (1:200) for 2 h, followed by peroxidase anti-peroxidase complex (1:200) for 2 h. The sections were incubated for 10 min at RT with 3, 3′-diaminobenzidine tetrahydrochloride as a chromogen that had been freshly prepared as a 20 mg solution in 100 ml of PBS containing 0.01% H2O2. Images of the developed tissue sections were captured using an optical microscope (Olympus, Tokyo, Japan).
2.5 Statistical Analysis
Means were compared using the t-test for two-group comparisons. Survival was assessed by the Kaplan Meier method. Data are expressed as the means ± SEM. For all tests, significance was set at P < 0.05.
3 Results
3.1 Tissue Depletion of Taurine Decreased the Survival Rate of Mice After X-Irradiation
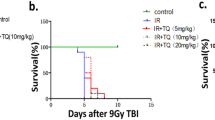
Exposure to high-dose radiation affects the gastrointestinal system. To investigate whether tissue depletion of taurine aggravates radiation-induced gastrointestinal syndrome, the 30-day survival of TauT+/+ and TauT−/− mice following 5 Gy of whole-body X-ray irradiation was analyzed (Fig. 1). The survival rate of mice in the TauT−/− group was significantly lower than that of the TauT+/+ group. Moreover, the bodyweight of mice in the TauT−/− group was reduced rapidly. These results suggested that the intestinal epithelium of TauT−/− mice was more sensitive to radiation, causing lethal gastrointestinal syndrome.
Effect of TauT knockout on the survival rates of mice after exposure to whole-body X-ray irradiation (5 Gy/mouse). Kaplan Meier survival curve of TauT+/+ and TauT−/− mice after X-ray irradiation. Female mice (n = 10 mice per group) were treated with 5 Gy of whole-body X-ray irradiation and monitored continuously for 30 days to determine the survival rates. Data are expressed as the percentage of surviving mice. The survival rate of the TauT−/− group was significantly lower than that of the TauT+/+ group
3.2 Tissue Depletion of Taurine Aggravates Radiation-Induced Gastrointestinal Syndrome
Radiation-induced gastrointestinal syndrome is primarily caused by the death of epithelial stem cells in the crypts of the small intestine (Ghosh et al. 2012). In this study, the blood feces of mice in the TauT−/− group was observed. Therefore, H&E staining was performed to assess the damage in the small intestine after X-irradiation (Fig. 2a). The villi in the small intestines of both TauT+/+ and TauT−/− mice 3 days after irradiation were shorter than those in normal nonirradiated mice. Moreover, the villi in the small intestine of TauT−/− mice were significantly shorter than those of TauT+/+ mice. Mice in the TauT−/− group exhibited significant, severe villous epithelial atrophy and a loss of normal crypt architecture (Fig. 2b).
Histological analysis of intestinal injury in mice after 5 Gy of whole-body X-ray irradiation. (a) Representative intestinal sections (top panel) stained with H&E (200×) at 3 days postirradiation. Scale bar = 100 μm. The villi in the small intestine of mice in the TauT+/+ and TauT−/− groups were shorter than those in the normal, nonirradiated small intestine of control mice. (b) Compared to Tau+/+ mice, TauT−/− mice showed significant villous epithelial atrophy (p < 0.001). Data are shown as means ± SE
3.3 Tissue Depletion of Taurine Decrease the Number of Proliferating Cells in Crypts After X-Irradiation
Intestinal stem cells are indispensable for intestinal regeneration following radiation exposure. Staining for PCNA was performed to assess the proliferation ability of intestinal stem cells after X-irradiation (Fig. 3a). The results showed that the numbers of PCNA+ cells in TauT+/+ mice and TauT−/− mice were lower than the numbers in normal nonirradiated mice. Moreover, the numbers of PCNA+ cells in the TauT−/− group were significantly lower than those in the TauT+/+ group. These data show that the loss of TauT and taurine in TauT−/− mouse resulted in reducing the number of epithelial proliferating cells in the villi.
Histological analysis of the proliferation ability of intestinal stem cells in mice after 5 Gy of whole-body X-ray irradiation. (a) Representative immunohistochemical images of PCNA stained sections of the small intestine (200×). (b) At 3 days postirradiation, the numbers of PCNA+ cells in TauT−/− mice were significantly lower than those in TauT+/+ mice (p < 0.001). Data are shown as means ± SE
4 Discussion
The mechanisms underlying radiation-induced cell damage are complex and varied and mainly include ROS, DNA damage, inflammation, and oxidative stress. ROS destroy large molecules in cells, such as DNA, proteins, and lipids, leading to cell necrosis and apoptosis (Chen et al. 2012). Radiation exposure can injure hematopoietic and gastrointestinal systems, depending on the dose of radiation received (Suman et al. 2012). The morphological changes that occur in the intestinal mucosa after high-dose radiation exposure have been well documented (Driák et al. 2008; Labéjof et al. 2002). However, the molecular events that regulate the radiosensitivity of the intestinal epithelial cells and radiation-induced gastrointestinal syndrome are not fully understood (Li et al. 2015).
Taurine (2-aminoethanesulfonic acid) is a major intracellular amino acid with several important functions, including antioxidant and anti-inflammatory activities (Oliveira et al. 2010; Ma et al. 2010; Kato et al. 2015). Taurine is taken up by cells via taurine transporter. Therefore, loss of the taurine transporter can aggravate radiation-induced gastrointestinal syndrome. We previously reported the critical role of taurine by showing that increasing the expression of taurine transporter had a mitigating effect on radiation exposure (Yamashita et al. 2019). Here, we explored the effect of taurine on radiation-induced intestinal injury to determine whether tissue depletion of taurine aggravates radiation-induced gastrointestinal syndrome. To this end, we established mouse models of radiation-induced gastrointestinal syndrome in TauT+/+ and TauT−/− mice by exposure to whole-body X-irradiation. The survival rate of the TauT−/− mice was significantly lower than that of the TauT+/+ mice. These results suggested that the intestinal epithelium in TauT−/− mice was more sensitive to radiation, causing lethal gastrointestinal syndrome. This result is most likely due to incomplete recovery from intestinal injury and the death of epithelial stem cells in the crypts. Therefore, we examined the crypt-villus structure of the small intestine and the proliferation of PCNA+ cells in the small intestine.
Radiation exposure inflicted severe damage to the villi in the small intestine. This evidence proved that failure to absorb nutrients can affect the metabolic function after X-irradiation. Depletion of taurine transporter in the small intestine, and the resulting taurine depletion, reduced the number of proliferating cells in the crypts. Taurine deficiency can aggravate the damage in intestinal epithelium in TauT−/− mouse, and taurine deficiency can also enhance the irradiation damage in intestinal epithelium. The severe pathological damage was observed in TauT−/− mouse intestine after X-irradiation, while PCNA+ cells were reduced, which proves taurine can also affect regeneration after irradiation damage. Exposure to ionizing radiation induces apoptotic cells, which are associated with a loss of villus epithelial cells and crypt stem cells. Yang (2017) reported that taurine reduced the percentage of apoptotic spermatocyte-derived GC-2 cells after exposure to ionizing radiation. Taurine also significantly suppressed UVB-induced apoptosis in lens epithelial cells (Dayang and Dongbo 2017). Thus, the protective effect of taurine against organ damage may stem from its ability to suppress oxidative stress and apoptotic responses (Nagai et al. 2016).
Taurine prevents arsenic-induced oxidative stress and apoptotic damage by inhibiting JNK signaling pathways (Ghosh et al. 2009; Das et al. 2010). Jun N-terminal kinase (JNK) is one of the three main members of the mitogen-activated protein kinase (MAPK) superfamily (Gururajan et al. 2005). JNK is activated in response to certain stresses, such as γ radiation, UV-C, and arsenic, and stress-induced activation of JNK leads to cell death through activation of the mitochondrial apoptotic pathway (Chen et al. 1996).
It was reported that taurine deficiency reduces life span by promoting mitochondrial-dependent and ER stress-mediated apoptosis (Jong et al. 2017). Taurine depletion causes cardiomyocyte atrophy, mitochondrial and myofiber damage, and cardiac dysfunction (Ito et al. 2008). Schaffer et al. (2009) reported that taurine may inhibit the production of ROS by regulating mitochondrial function. Thus, taurine might contribute to the recovery from radiation-induced gastrointestinal syndrome by regulating mitochondria, and JNK signaling pathways.
The results observed in the TauT−/− mice suggest that taurine plays a role in protecting against radiation-induced gastrointestinal syndrome. Taurine modulates the kinetics of crypt cell proliferation, reduces radiation-induced DNA damage, and promotes crypt regeneration.
Our data demonstrate that taurine transporter and taurine are important factors in the radiation response of normal tissue.
5 Conclusion
This study showed that tissue depletion of taurine aggravates radiation-induced gastrointestinal syndrome in mice. The results observed in the radiation-exposed TauT−/− mice indicate that taurine and taurine transporter are important factors in the radiation response of normal tissue. Taurine modulates crypt cell proliferation kinetics, reduces radiation-induced villus structural damage, and promotes crypt regeneration. Our data demonstrate that taurine is a key regulator of crypt stem cells that has important roles in intestinal cell proliferation and survival.
Abbreviations
- PCNA:
-
Proliferating cell nuclear antigen
- ROS:
-
Reactive oxygen species
- TauT:
-
Taurine transporter
References
Chen YR, Wang X, Templeton D, Davis RJ, Tan TH (1996) The role of c-Jun N-terminal kinase (JNK) in apoptosis induced by ultraviolet C and gamma radiation. Duration of JNK activation may determine cell death and proliferation. J Biol Chem 271(50):31929–31936
Chen X, Guo C, Kong J (2012) Oxidative stress in neurodegenerative diseases. Neural Regen Res 7(5):376–385
Das J, Ghosh J, Manna P, Sil PC (2010) Protective role of taurine against arsenic-induced mitochondria-dependent hepatic apoptosis via the inhibition of PKCdelta-JNK pathway. PLoS One 5(9):e12602
Dayang W, Dongbo P (2017) Taurine protects lens epithelial cells against ultraviolet B-induced apoptosis. Curr Eye Res 42(10):1407–1411
Driák D, Osterreicher J, Vávrová J, Reháková Z, Vilasová Z (2008) Morphological changes of rat jejunum after whole body gamma-irradiation and their impact in biodosimetry. Physiol Res 57:475–479
Duan Y, Yao X, Zhu J, Li Y, Zhang J, Zhou X, Qiao Y, Yang M, Li X (2017) Effects of yak-activated protein on hematopoiesis and related cytokines in radiation-induced injury in mice. Exp Ther Med 14(6):5297–5304
Ghosh J, Das J, Manna P, Sil PC (2009) Taurine prevents arsenic-induced cardiac oxidative stress and apoptotic damage: role of NF-kappa B, p38 and JNK MAPK pathway. Toxicol Appl Pharmacol 240(1):73–87
Ghosh SP, Kulkarni S, Perkins MW, Hieber K, Pessu RL, Gambles K, Maniar M, Kao TC, Seed TM, Kumar KS (2012) Amelioration of radiation-induced hematopoietic and gastrointestinal damage by Ex-RAD(R) in mice. J Radiat Res 53(4):526–536
Gururajan M, Chui R, Karuppannan AK, Ke J, Jennings CD, Bondada S (2005) c-Jun N-terminal kinase (JNK) is required for survival and proliferation of B-lymphoma cells. Blood 106(4):1382–1391
Heller-Stilb B, van Roeyen C, Rascher K, Hartwig HG, Huth A, Seeliger MW, Warskulat U, Häussinger D (2002) Disruption of the taurine transporter gene (taut) leads to retinal degeneration in mice. FASEB J 16(2):231–233
Ito T, Kimura Y, Uozumi Y, Takai M, Muraoka S, Matsuda T, Ueki K, Yoshiyama M, Ikawa M, Okabe M, Schaffer SW, Fujio Y, Azuma J (2008) Taurine depletion caused by knocking out the taurine transporter gene leads to cardiomyopathy with cardiac atrophy. J Mol Cell Cardiol 44(5):927–937
Ito T, Oishi S, Takai M, Kimura Y, Uozumi Y, Fujio Y, Schaffer SW, Azuma J (2010) Cardiac and skeletal muscle abnormality in taurine transporter-knockout mice. J Biomed Sci 17:S20
Johnson CH, Patterson AD, Krausz KW, Kalinich JF, Tyburski JB, Kang DW, Luecke H, Gonzalez FJ, Blakely WF, Idle JR (2012) Radiation metabolomics. 5. Identification of urinary biomarkers of ionizing radiation exposure in nonhuman primates by mass spectrometry-based metabolomics. Radiat Res 178:328–340
Jong CJ, Ito T, Prentice H, Wu JY, Schaffer SW (2017) Role of mitochondria and endoplasmic reticulum in taurine-deficiency-mediated apoptosis. Nutrients 9(8):795
Kato T, Okita S, Wang S, Tsunekawa M, Ma N (2015) The effects of taurine administration against inflammation in heavily exercised skeletal muscle of rats. Adv Exp Med Biol 803:773–784
Kwon HM, Handler JS (1995) Cell volume regulated transporters of compatible osmolytes. Curr Opin Cell Biol 7:465–471
Labéjof LP, Galle P, Mangabeira PA, de Oliveira AH, Severo MI (2002) Histological changes in rat duodenum mucosa after whole-body gamma irradiation. Cell Mol Biol 48:537–545
Li M, Gu Y, Ma YC, Shang ZF, Wang C, Liu FJ, Cao JP, Wan HJ, Zhang XG (2015) Krüppel-Like Factor 5 promotes epithelial proliferation and DNA damage repair in the intestine of irradiated mice. Int J Biol Sci 11:1458–1468
Li Y, Kong S, Yang F, Xu W (2018) Protective effects of 2-amino-5,6-dihydro-4H-1,3-thiazine and its derivative against radiation-induced hematopoietic and intestinal injury in mice. Int J Mol Sci 19(5):E1530
Ma N, Aoki E, Semba R (1994) An immunohistochemical study of aspartate, glutamate, and taurine in rat kidney. J Histochem Cytochem 42:621–626
Ma N, Sasoh M, Kawanishi S, Sugiura H, Piao F (2010) Protection effect of taurine on nitrosative stress in the mice brain with chronic exposure to arsenic. J Biomed Sci 17:S7
Nagai K, Fukuno S, Oda A, Konishi H (2016) Protective effects of taurine on doxorubicin-induced acute hepatotoxicity through suppression of oxidative stress and apoptotic responses. Anti-Cancer Drugs 27(1):17–23
Oliveira MW, Minotto JB, de Oliveira MR, Zanotto-Filho A, Behr GA, Rocha RF, Moreira JC, Klamt F (2010) Scavenging and antioxidant potential of physiological taurine concentrations against different reactive oxygen/nitrogen species. Pharmacol Rep 62:185–193
Poggi MM, Coleman CN, Mitchell JB (2001) Sensitizers and protectors of radiation and chemotherapy. Curr Probl Cancer 25:334–411
Qiu W, Carson-Walter EB, Liu H, Epperly M, Greenberger JS, Zambetti GP, Zhang L, Yu J (2008) PUMA regulates intestinal progenitor cell radiosensitivity and gastrointestinal syndrome. Cell Stem Cell 2(6):576–583
Rosen EM, Day R, Singh VK (2015) New approaches to radiation protection. Front Oncol 4:381
Schaffer SW, Azuma J, Mozaffari M (2009) Role of antioxidant activity of taurine in diabetes. Can J Physiol Pharmacol 87(2):91–99
Shivaraj MC, Marcy G, Low G, Ryu JR, Zhao X, Rosales FJ, Goh EL (2012) Taurine induces proliferation of neural stem cells and synapse development in the developing mouse brain. PLoS One 7(8):e42935
Smith TA, Kirkpatrick DR, Smith S, Smith TK, Pearson T, Kailasam A, Herrmann KZ, Schubert J, Agrawal DK (2017) Radioprotective agents to prevent cellular damage due to ionizing radiation. J Transl Med 15(1):232
Sugahara T, Nagata H, Tanaka T (1969) Experimental studies on radiation protection by taurine. Nihon Igaku Hoshasen Gakkai Zasshi 29:156–161
Suman S, Maniar M, Fornace AJ Jr, Datta K (2012) Administration of ON 01210.Na after exposure to ionizing radiation protects bone marrow cells by attenuating DNA damage response. Radiat Oncol 7:6
Weiss JF, Landauer MR (2009) History and development of radiation-protective agents. Int J Radiat Biol 85:539–573
Yamashita T, Kato T, Tunekawa M, Gu Y, Wang S, Ma N (2017) Effect of radiation on the expression of taurine transporter in the intestine of mouse. Adv Exp Med Biol 975:729–740
Yamashita T, Kato T, Isogai T, Gu Y, Ma N (2019) Protective effects of taurine on the radiation exposure induced cellular damages in the mouse intestine. Adv Exp Med Biol 1155:443–450
Yang W, Huang J, Xiao B, Liu Y, Zhu Y, Wang F, Sun S (2017) Taurine protects mouse spermatocytes from ionizing radiation-induced damage through activation of Nrf2/HO-1 signaling. Cell Physiol Biochem 44(4):1629–1639
Acknowledgments
We thank Rina Funaki and Aoi Mashimo for the handling of the animals of this work. This work was supported by JSPS KAKENHI Grant Number JP 20K08120.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Yamashita, T., Kato, T., Isogai, T., Gu, Y., Ito, T., Ma, N. (2022). Taurine Deficiency in Tissues Aggravates Radiation-Induced Gastrointestinal Syndrome. In: Schaffer, S.W., El Idrissi, A., Murakami, S. (eds) Taurine 12. Advances in Experimental Medicine and Biology, vol 1370. Springer, Cham. https://doi.org/10.1007/978-3-030-93337-1_10
Download citation
DOI: https://doi.org/10.1007/978-3-030-93337-1_10
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-93336-4
Online ISBN: 978-3-030-93337-1
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)