Abstract
Surgical techniques for treating early onset scoliosis have evolved over the last 60 years. Distraction-based techniques have become the standard of care when treating spinal deformity in young patients. These techniques allow for continued chest and spine development and reduce the risk of thoracic insufficiency syndrome. However, these patients have a high rate of complications due to their small stature and amount of growth remaining. The use of traditional growing rods (TGR) is a common distraction-based technique where lengthening of the instrumentation is done in the operating room until sufficient growth has been achieved. Magnetically controlled growing rod (MCGR) constructs were developed to have the advantage of being lengthened in the office thus avoiding the risks associated with multiple surgical procedures. When magnetic and traditional growing rod constructs have been compared, the outcomes were similar except the initial cost of MCGR was greater and the number of planned surgical procedures with TGR was less. Some of the early enthusiasm for MCGR has been tempered by follow-up results and similar rates of unplanned trips to the operating room. Therefore, the use of TGR remains a viable primary or revision surgical option for patients unable to undergo placement of MCGR.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Early onset scoliosis
- Spine growth
- Traditional growing rods
- Dual growing rods
- Magnetically controlled growing rods
-
Dual traditional growing rods have superior results to single rod constructs.
-
Outcomes with TGR have been similar to those obtained with MCGR.
-
Unplanned re-operation rates are similar between TGR and MCGR.
-
TGR can be used for revision surgery after failed MCGR lengthening.
-
TGR may be a better option for obese patients, hyperkyphotic patients, or patients too small for a magnetic actuator.
-
Patients who require frequent magnetic resonance imaging (MRI) of the chest or abdomen may be better candidates for TGR due to image artifact scatter produced by the MCGR actuator.
1 Background
Patients with early onset scoliosis (EOS) represent a challenge for any pediatric spinal surgeon due to their often severe deformities, small stature, and years of remaining growth. Historically, the goals of pediatric spinal deformity surgery have been to attain a three-dimensional deformity correction that is well balanced. Achieving this with an all posterior fusion in young children can result in a crankshaft phenomenon secondary to the remaining growth of the anterior spine [1, 2]. Additionally, spinal fusions performed at a young age whether approached from posterior, anterior, or both decrease chest and spinal growth and lead to diminished pulmonary function [3]. As the understanding of spinal and chest wall growth has evolved, so too have implant designs and surgical techniques.
Surgical options for EOS fall into three categories: distraction based, compression based, or guided growth [4]. Paul Harrington [5] is credited with describing the first fusionless instrumentation for the growing spine. He placed a single distraction rod on the concave side of the deformity with subperiosteal dissection using hooks as anchor points. This technique was modified by Moe et al. [6] to create a distraction-based approach with limited dissection at the anchor sites and submuscular passage of the distraction rod. They performed lengthening if there was greater than 10° loss of correction of the major curve. However, the complication rate with both of these early techniques approached 50% [6].
Over the last 30 years, distraction-based techniques continued to evolve as did the understanding of the growing spine. Due to a high rate of instrumentation-related complications with early single rod constructs, the use of modern distraction-based growing rod techniques developed. A single traditional growing rod (TGR) technique can be utilized in cases where the patients are small, the skin tenuous, or the rod may be too prominent over the convexity of the curve. However, dual rod fixation is our preferred technique whenever possible. The modern distraction-based technique using dual TGR was popularized by Akbarnia et al. in 2005 [7]. In their initial series of 23 patients, they showed maintained curve correction as well as spinal growth in patients with EOS of various etiologies [7]. However, the complication rate with this technique has been shown to range from 48% to 58% [7, 8]. The use of TGR has been mainly used in EOS patients with idiopathic, neuromuscular, and syndromic etiologies. Elsebai et al. [9] showed that TGR was also effective for treating EOS patients with congenital deformity. When the uses of single and dual TGR were compared there was improved deformity correction and less catastrophic implant related complications with dual TGR [10]. However, due to higher implant density and prominence with dual TGR there is a higher wound complication rate associated with their use [8, 10, 11].
TGR techniques were widely adopted until recently when magnetically controlled growing rods (MCGR) were developed [12, 13]. Direct comparisons between TGR and MCGR have shown similar results with regard to maintained curve correction and continued chest and spine growth [14, 15]. The main differences between the two are the higher upfront cost for the MCGR implants and greater surgical burden with TGR. The initial cost associated with MCGR is substantially greater than TGR but becomes more cost effective after 4–6 years by avoiding the need for repeat trips to the operating room for lengthening procedures with TGR [16,17,18,19]. Even with the use of MCGR there remains a high rate of unplanned return to the operating room for implant related complications and failed lengthening of the implant [20,21,22,23]. Studies of explanted first generation magnetic rods have shown metallosis and reduced ability to lengthen over time [24,25,26]. With these findings, the utility of MCGR implants as the “magic bullet” to treat all EOS deformities has been called into question. Therefore, even with expanded use of MCGR both single and dual TGR techniques remain viable options as primary or revision surgical approaches to EOS of various etiologies (neuromuscular, congenital, idiopathic, and syndromic). The purpose of this chapter is to outline the indications as well as techniques for both single and dual TGR.
2 Indications for Traditional Growing Rods
The indications for surgical intervention in EOS are similar whether using TGR or MCGR implants. MCGR background and surgical techniques are covered in greater detail in Chap. 44. Growth-friendly implants should be considered for EOS patients younger than 10 years old (9 years of age or less) with significant remaining chest and spine growth and who meet indications for surgical intervention. In our practice, we discuss surgery when there is evidence of progression of the major curve beyond 50°, stiffening of the curve, and consideration for remaining growth. Early surgical intervention is considered in patients with who have had progressive deformity despite active nonoperative treatment such as bracing or casting. We typically utilize a dual TGR construct unless the patient’s size or deformity only allows for use of a single rod. We consider dual TGR as a primary surgical technique in patients with obesity, small stature, severe kyphotic deformities, difficulty with frequency of MCGR follow-up, or patients requiring frequent magnetic resonance imaging. Conversion to either a single or dual TGR also remains a viable revision option for patients who have failed MCGR.
2.1 Obesity
Childhood obesity presents a risk for implant failure in patients with EOS. Patients with Prader–Willi syndrome are at a particular risk for this because the syndrome is characterized by excessive weight gain, hypotonia, and progressive scoliosis at an early age. Treating the spinal deformity in this patient population can be challenging due to their body habitus. Casting or bracing may not be as effective at improving or holding spinal alignment due to increased adipose tissue. In any pediatric patient with EOS and obesity the depth of their soft tissues is important to consider when determining how to proceed once the indications for surgical intervention are met. Obesity may lead to treatment failure for MCGR if the external magnet is unable to penetrate the soft tissue envelope. Patients with Prader–Willi syndrome have increased risk of rapid weight gain and can go from an average body mass index (BMI) to an elevated BMI in a short period of time (Fig. 38.1). In these patients either the initial use of TGR or conversion from MCGR after they have failed to lengthen will allow for continued distraction-based lengthening of the growing spine (Fig. 38.2).
A 3-year-old male with Prader–Willi syndrome whose proximal thoracic and main thoracic curves progressed from 36° and 32° to 53° and 49°. He initially underwent MCGR placement at 3 years of age after curve progression despite elongation derotation flexion casting (a). At age 6 years, MCGR failed to lengthen on two subsequent clinic lengthening. His posterior soft tissue depth to the rod had increased from 30 mm to 50 mm (b)
Patient in Fig. 38.1 who was a 6-year-old male with Prader–Willi syndrome and converted to TGR from MCGR. At the time of MCGR removal, the rod appeared to be functioning contributing to the hypothesis that the increased soft tissue contributed to failed MCGR [TG1]. After revision to TGR, his curve magnitude remains unchanged
2.2 Small Stature
In patients with EOS, their small stature and severe progressive scoliosis often prompt the need for surgical invention prior to skeletal maturity. When considering surgical options the prominence of the implants in these patients must be taken into consideration. For MCGR the smallest actuator is 70 mm in length and can be quite bulky if not placed into an area with adequate soft tissue coverage. This actuator segment cannot be contoured to the patient and some small stature patients may not be able to accommodate the actuator without an increased risk of wound complications and hardware prominence. In these patients the use of either a single or dual TGR may be a more versatile option due to the ability to better contour the rod and optimize placement of the rod connector. A recent study evaluating the use of TGR in the MCGR era found that TGR patients on average had an 8 cm shorter spinal length (192 mm vs. 273 mm) compared to those that had an initial MCGR inserted [27]. Reducing the size of the implant or actuator can reduce the risk of hardware prominence and potential wound complications. However, in very small patients the use of TGR in a spine-to-spine fashion may also not be feasible due to their anatomy. In these cases, hybrid techniques using proximal rib fixation with distal spine or pelvic anchors may be a better option for distraction-based lengthening.
2.3 Severe Kyphotic Deformity
Similar to patients with small stature, those with severe kyphotic deformities may not be able to tolerate placement of MCGR due to the lack of a straight segment of spine available to accommodate the 70 mm or 90 mm actuator. Additionally, the lack of ability to contour the rods to match or correct some of the patient’s sagittal plane deformity places them at additional risk for developing proximal anchor failure or proximal junctional kyphosis as greater kyphotic forces are created with posterior lengthening of the straight actuator. In these patients, TGR can be a more versatile option due to the ability to customize the implants to match the patient’s sagittal plane deformity and reduce the risk of proximal anchor failure and soft tissue necrosis (Fig. 38.3). In a recent series of 25 patients who had MCGR available, surgeons chose to use TGR in 11 because of concern for the patients’ sagittal profile [27].
2.4 Patient Compliance with MCGR
The interval for lengthening MCGR is frequently much shorter than what is typically used with TGR. In families who are unable to comply with postoperative commitment of more frequent lengthening with MCGR due to travel from a distance or socioeconomic factors, then alternative treatment options such as TGR or guided spinal growth may be a better option due to the reduced frequency of follow-up needed for treatment success.
2.5 Frequent Magnetic Resonance Imaging
Patients who require frequent magnetic resonance imaging (MRI) of the chest or abdomen may be better candidates for TGR. MCGR are considered to be MRI-conditional implants by the manufacturer and they recommend scanning with a magnetic field strength of 1.5 Tesla and a maximum spatial field gradient of 3000 gauss/cm (30 T/m) to limit increase in temperature greater than 3.7 °C [28]. Woon et al. [29] found that MCGR are safe for MRI and found no inadvertent lengthening or collapse. Cadaveric and in vivo studies have found little risk of thermal injury or failure of the MCGR implant to lengthen after MRI [29, 30]. However, both studies found the MCGR implant generates significant artifact making images of the thoracic and lumbar spine less interpretable [29, 30]. According to the manufacturer: “the image artifact caused by the MAGEC® system extends beyond the imaging field of view when imaged with a gradient-echo pulse sequence in a 1.5 T MRI system. However, imaging in locations approximately 20cm away from the actuator of the MAGEC System may produce images in which anatomical features may be discerned” [28].
The use of TGR in patients with ongoing medical care that requires frequent MRI comes with the same risk of implant heating and artifact generation. For these reasons, the use of TGR can be considered in these patients with the use of titanium rods to reduce the MRI artifact [31].
2.6 Failed MCGR
The use of TGR can also be considered as a revision technique for failed MCGR. The most common complications seen with MCGR are failure to lengthen, proximal anchor failure, and rod fracture [20]. In cases where the rod has failed to lengthen, the conversion to a TGR construct is an option for revision surgery in patients with significant growth remaining (Fig. 38.4). If the proximal anchor sites remain intact, a TGR construct can be created using the cephalad portion of the MCGR rods left in place by cutting just above the taper of the actuator avoiding disruption of the fragile proximal soft tissue envelope (see Fig. 38.4).
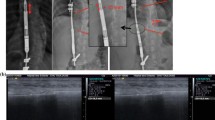
An example of conversion from MCGR to TGR for failure of rods to lengthen for the patient in Fig. 38.1. (a) MCGR rods had failed to lengthen over two consecutive in-office lengthening procedure without obvious hardware failure. (b) MCGR rod was cut just proximal to the actuator connected to in-line connector. (c) Distal anchor site with new rod and in-line connector in place for distraction
3 Conclusion
Over the last 15 years, the use of single and dual TGR has declined as pediatric spinal surgeons have shifted to using MCGR as the primary distraction-based method for treating EOS. However, understanding the indications and surgical techniques for both single and dual TGR remains an important adjunct for pediatric spinal surgeons. This technique has been proven to be an effective primary distraction-based approach to treating EOS. Additionally, the use of TGR can be used as a revision technique if other growth-friendly techniques have failed. When compared with MCGR, the results for curve correction and increased thoracic height are the same or better with TGR [14, 15].
Despite advances in technology and techniques, the complication rate with TGR remains high due to the inherent challenges of this patient population. As long-term results have returned on the use of MCGR, some of the early enthusiasm for this technique to significantly reduce the number of complications has been tempered due to a similar rate of hardware complications and unplanned return to the operating room [20,21,22]. One of the proposed benefits to children with EOS undergoing MCGR is reduced physical and psychologic stress from the limited number of the surgical procedures with MCGR compared to TGR. However, several authors have shown that the reduced burden of surgery with MCGR has not translated into improved patient reported outcome scores or reduced psychologic stress [32,33,34].
In conclusion, TGR remains a steadfast option in treating patients with EOS. As techniques and technology continue to evolve, there remains a patient population who can benefit from TGR as opposed to MCGR. It is pertinent for EOS spinal surgeons to understand the indications and contraindications for both devices and techniques.
References
Dubousset J, Herring JA, Shufflebarger H. The crankshaft phenomenon. J Pediatr Orthop. 1989;9(5):541–50.
Sanders JO, Herring JA, Browne RH. Posterior arthrodesis and instrumentation in the immature (Risser-grade-0) spine in idiopathic scoliosis. J Bone Joint Surg Am. 1995;77(1):39–45.
Karol LA, Johnston C, Mladenov K, Schochet P, Walters P, Browne RH. Pulmonary function following early thoracic fusion in non-neuromuscular scoliosis. J Bone Joint Surg Am. 2008;90(6):1272–81.
Skaggs DL, Akbarnia BA, Flynn JM, Myung KS, Sponseller PD, Vitale MG, et al. A classification of growth friendly spine implants. J Pediatr Orthop. 2014;34(3):260–74.
Harrington PR. Treatment of scoliosis. Correction and internal fixation by spine instrumentation. J Bone Joint Surg Am. 1962;44-A:591–610.
Moe JH, Kharrat K, Winter RB, Cummine JL. Harrington instrumentation without fusion plus external orthotic support for the treatment of difficult curvature problems in young children. Clin Orthop Relat Res. 1984;185:35–45.
Akbarnia BA, Marks DS, Boachie-Adjei O, Thompson AG, Asher MA. Dual growing rod technique for the treatment of progressive early-onset scoliosis: a multicenter study. Spine. 2005;30(17 Suppl):S46–57.
Bess S, Akbarnia BA, Thompson GH, Sponseller PD, Shah SA, Sebaie HE, et al. Complications of growing-rod treatment for early-onset scoliosis: analysis of one hundred and forty patients. J Bone Joint Surg Am. 2010;92(15):2533–43.
Elsebai HB, Yazici M, Thompson GH, Means JB, Skaggs DL, Crawford AH, et al. Safety and efficacy of growing rod technique for pediatric congenital spinal deformities. J Pediatr Ortho. 2011;31(1):1–5.
Elsebai HB, Yazici M, Thompson GH, Emans JB, Skaggs DL, Crawford AH, et al. Comparison of single and dual growing rod techniques followed through definitive surgery: a preliminary study. Spine. 2005;30(18):2039–44.
Xu G, Fu X, Tian P, Ma J, Ma X. Comparison of single and dual growing rods in the treatment of early onset scoliosis: a meta-analysis. J Orthop Surg Res. 2016;11(1):80.
Akbarnia BA, Cheung K, Noordeen H, Elsebaie H, Yazici M, Dannawi Z, et al. Next generation of growth-sparing techniques: preliminary clinical results of a magnetically controlled growing rod in 14 patients with early-onset scoliosis. Spine. 2013;38(8):665–70.
Hosseini P, Pawelek J, Mundis GM, Yaszay B, Ferguson J, Helenius I, et al. Magnetically controlled growing rods for early-onset scoliosis: a multicenter study of 23 cases with minimum 2 years follow-up. Spine. 2016;41(18):1456–62.
Erdoğan S, Polat B, Atıcı Y, Özyalvaç ON, Öztürk C. Comparison of the effects of magnetically controlled growing rod and traditional growing rod techniques on the sagittal plane in the treatment of early-onset scoliosis. J Korean Neurosurg Soc. 2019;62(5):577–85.
Akbarnia BA, Pawelek JB, Cheung KM, Demirkiran GH, Elsebaie H, Emans JE, et al. Traditional growing rods versus magnetically controlled growing rods for the surgical treatment of early-onset scoliosis: a case-matched 2-year study. Spine Deform. 2014;2(6):493–7.
Oetgen ME, McNulty EM, Matthew AL. Cost-effectiveness of magnetically controlled growing rods: who really benefits? Spine Deform. 2019;7(3):501–4.
Luhmann SJ, McAughey EM, Ackerman SJ, Bumpass DB, McCarthy RE. Cost analysis of a growth guidance system compared with traditional and magnetically controlled growing rods for early-onset scoliosis: a US-based integrated health care delivery system perspective. Clinicoecon Outcomes Res. 2018;10:179–87.
Wong C, Cheung J, Cheung P, Lam C, Cheung K. Traditional growing rod versus magnetically controlled growing rod for treatment of early onset scoliosis: cost analysis from implantation till skeletal maturity. J Orthop Surg. 2017;25(2):2309499017705022.
Polly DW, Ackerman SJ, Schneider K, Pawelek JB, Akbarnia BA. Cost analysis of magnetically controlled growing rods compared with traditional growing rods for early-onset scoliosis in the US: an integrated health care delivery system perspective. Clinicoecon Outcomes Res. 2016;8:457–65.
Thakar C, Kieser DC, Mardare M, Haleem S, Fairbank J, Nnadi C. Systematic review of the complications associated with magnetically controlled growing rods for the treatment of early onset scoliosis. Eur Spine J. 2018;27:2062–71.
Choi E, Yaszay B, Mundis G, Hosseini P, Pawelek J, Alanay A, et al. Implant complications after magnetically controlled growing rods for early onset scoliosis: a multicenter retrospective review. J Pediatr Orthop. 2017;37(8):e588–92.
Kwan K, Alanay A, Yazici M, Demirkiran GH, Helenius I, Nnadi C, et al. Unplanned reoperations in magnetically controlled growing rod surgery for early onset scoliosis with a minimum of two-year follow-up. Spine. 2017;42(24):E1410–4.
Cheung J, Yiu K, Kwan K, Cheung K. Mean 6-year follow-up of magnetically controlled growing rod patients with early onset scoliosis: a glimpse of what happens to graduates. Neurosurgery. 2019;84(5):1112–23.
Rushton PRP, Smith SL, Forbes L, Bowey AJ, Gibson MJ, Joyce TJ. Force testing of explanted magnetically controlled growing rods. Spine. 2019;44(4):233–9.
Joyce TJ, Smith SL, Rushton PRP, Bowey AJ, Gibson MJ. Analysis of explanted magnetically controlled growing rods from seven UK spinal centers. Spine (Phila Pa 1976). 2018;43(1):E16–22.
Rushton PRP, Smith SL, Kandemir G, Forbes L, Fender D, Bowey AJ, et al. Spinal lengthening with magnetically controlled growing rods: data from the largest series of explanted devices. Spine (Phila Pa 1976). 2020;45(3):170–6.
Varley ES, Yaszay B, Pawelek JB, Mundis GM, Oetgen ME, Sturm PF, et al. The role of traditional growing rods in the era of magnetically-controlled growing rods for the treatment of early-onset scoliosis. SRS Meeting Abstract 2018.
MAGEC® MRI Compatibility [Internet]. Nuvasive. 2016 [cited 2020 Apr 28]. Available from: https://www.nuvasive.com/wp-content/uploads/2017/11/MAGEC-MR-Conditional-Clearance-Notice-Updated-11-2017.pdf.
Poon S, Chen YH, Wendolowski SF, Graver A, Nixon R, Amaral T, et al. Cadaveric study of the safety and device functionality of magnetically controlled growing rods after exposure to magnetic resonance imaging. Spine Deform. 2018;6(3):290–8.
Woon RP, Andras LM, Noordeen H, Morris S, Hutchinson J, Shah SA, et al. Surgeon survey shows no adverse events with MRI in patients with Magnetically Controlled Growing Rods (MCGRs). Spine Deform. 2018;6(3):299–302.
Ahmad FU, Sidani C, Fourzali R, Wang MY. Postoperative magnetic resonance imaging artifact with cobalt-chromium versus titanium spinal instrumentation. J Neurosurg Spine. 2013;19(5):629–36.
Aslan C, Olgun ZD, Ayik G, Karaokur R, Ozusta S, Demirkiran GH, et al. Does decreased surgical stress really improve the psychosocial health of early-onset scoliosis patients?: a comparison of traditional growing rods and magnetically-controlled growing rods patients reveals disappointing results. Spine. 2019;44(11):E656–63.
Bauer JM, Yorgova P, Neiss G, Rogers K, Sturm PF, et al. Early onset scoliosis: is there an improvement in quality of life with conversion from traditional growing rods to magnetically controlled growing rods? J Pediatr Orthop. 2019;39(4):e284–8.
Doany ME, Olgun ZD, Kinikli GI, Bekmez S, Kocyigit A, Demirkiran GH, et al. Health-related quality of life in early-onset scoliosis patients treated surgically: EOSQ scores in traditional growing rod versus magnetically controlled growing rods. Spine. 2018;43(2):148–53.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Koehler, R., Murphy, J.S., Fletcher, N.D., Yaszay, B. (2022). Indications for Traditional Growing Rods in the Era of Magnetically Controlled Growing Rods. In: Akbarnia, B.A., Thompson, G.H., Yazici, M., El-Hawary, R. (eds) The Growing Spine. Springer, Cham. https://doi.org/10.1007/978-3-030-84393-9_38
Download citation
DOI: https://doi.org/10.1007/978-3-030-84393-9_38
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-84392-2
Online ISBN: 978-3-030-84393-9
eBook Packages: MedicineMedicine (R0)