Abstract
The medial sural vessels represent a reliable alternative as a vascular recipient site if needed in the knee region. Their location and anatomical characteristics are already well known to most reconstructive surgeons, as this is the source pedicle for the work-horse medial head of the gastrocnemius muscle. Found at the level of the knee joint, this may be a superior option to use instead of the middle third of the popliteal vessels, as end-to-end microanastomoses are possible, the added length of its pedicle may avoid the need for vein grafts, and the capability to reach a more superficial location will physically assist the performance of the microsurgery. Several approaches are possible depending on the location of the defect requiring coverage, and whether the patient must be in a prone, supine, or lateral decubitus position. Finally, the surgeon should be reassured that due to the existence of sufficient collaterals, viability and function of the medial gastrocnemius muscle will not be altered.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Soft tissue wounds about the knee have traditionally most simply been covered using either head of the gastrocnemius muscle as a local flap [1] or today some form of perforator flap such as an island medial sural artery perforator flap [2]. However, for larger defects or if the former are unavailable, a microsurgical tissue transfer becomes the next best option. The conundrum then becomes the selection of an appropriate recipient site that may or may not itself be readily available. Possible choices, of course, encompass the major lower limb vessels including the superficial femoral, popliteal, or anterior or posterior tibial arteries or nearby branches such as the superior lateral or medial genicular, inferior lateral or medial genicular, descending genicular, or even reversed flow via the descending branch of the lateral circumflex femoral [3,4,5,6,7,8]. The actual selection oftentimes is determined by what is exposed following a surgical extirpation, trauma, or essential debridement or what is closest, what is easiest to dissect, or what has not been previously violated.
Another option is the well-known medial sural vessels that supply the medial head of the gastrocnemius muscle [MG], as were originally used as early as 1984 to extend that muscle as a local free flap using vein grafts, with these vessels being both the donor and recipient vessels [9, 10]! This became a more general recipient site via a posterior approach [1987] [11], followed then by a medial approach [1994] [12] that was similar to that used by macrovascular surgeons. Regardless of the approach, since most injuries in the lower limb occur in the anterior region, the gastrocnemius muscles usually have protected these vessels so they remain outside the zone of injury. Additional attributes are the provision of a vascular extension of the popliteal vessels to potentially augment flap reach in lieu of vein grafts, provide a more superficial exposure to facilitate end-to-end microanastomoses, and avoidance of any potential injury to a major lower limb source vessel [12]. Although the MG muscle is stated to be a type I muscle according to the schema of Nahai and Mathes implying it has only a solitary source pedicle [13], sacrifice of these vessels when used as a vascular recipient site does not alter the muscle’s viability nor function [14, 15], due to other sufficient vascular collaterals as Tsetsonis et al. [16] have proven do exist.
Applied Anatomy
The middle portion of the popliteal artery lies in a diamond-shaped space behind the knee bound superiorly by the medial hamstring [semimembranosus and semitendinosus] and biceps femoris muscles and inferiorly by the medial and lateral heads of the gastrocnemius muscles themselves. Just under the deep fascia in the popliteal space will be found the lesser saphenous vein and medial sural cutaneous nerve, well known as the anatomic landmark separating the heads of the gastrocnemius muscle [17]. The popliteal artery will be found more medial and anterior to the popliteal vein and tibial nerve in this region. The medial sural artery originates from the popliteal artery
at the level of the femoral condyles and then travels posteriorly to enter the undersurface of the medial head of the gastrocnemius at the level of the fibular head, which corresponds to the knee joint (Fig. 40.1) [10, 12, 18]. Be wary that sometimes a median [sic. superficial] sural artery that has a variable caliber may be found here as well, coursing with the medial sural cutaneous nerve [12]!
The caliber of the medial sural artery at its popliteal origin in cadaver studies is reported to vary from 1.4 mm [14, 18, 19] to 2.5 ± 0.8 mm [20] and its venae comitantes from 1.4 mm [14] to 5 mm [19]. The extramuscular length of this pedicle also is variable, from as short as 2.6 cm [18] to 5 cm or even more [14, 20]. Numerous other venous branches will be found nearby including the lesser saphenous vein itself that in turn could also suffice as a means for venous egress if the medial sural venae comitantes were too diminutive.
Surgical Site Exposure
Just like the factors determining the selection of an appropriate recipient site around the knee, the approach to the medial sural vessels will depend on the location of the defect, any preexisting scars or open wounds that will facilitate their exposure, and the position of the patient on the operating table.
The Medial Approach
This is similar to that used by the macrovascular surgeon who has planned access to the middle third of the popliteal artery for whatever purpose. Either a supine or an ipsilateral decubitus position is possible, with the knee flexed and thigh externally rotated. A curvilinear incision is first made starting medially from the adductor tubercle of the femur to the medial condyle of the tibia (Fig. 40.2) [18]. The greater saphenous vein is retracted posteriorly and then the deep fascia divided between the sartorius muscle and the pes anserinus, which often consists of a common tendon of the gracilis, sartorius, and semitendinosus muscles. At the level of the knee joint, the saphenous nerve emerges between the sartorius and gracilis muscles and should be kept with the greater saphenous vein that it accompanies [18]. The sartorius muscle is retracted anteriorly, while the pes anserinus is usually divided and the medial head of the gastrocnemius detached from its origin from the medial condyle of the femur. The popliteal artery will then be exposed and followed distally behind the medial gastrocnemius muscle. As the latter is turned down, the medial sural neurovascular pedicle should become obvious as it proceeds medially and posteriorly from the popliteal artery to enter the muscle hilum. The medial sural artery and venae comitantes are carefully separated, while the motor nerve is protected. These extramuscular vessels can then be divided where their caliber and pedicle length are most suitable to match the requirements of the given free flap. If the medial sural vein is inadequate, numerous other veins will be found in the vicinity including the lesser saphenous vein that may be more satisfactory to complete the microvascular tissue transfer (Fig. 40.3).
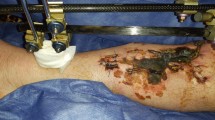
(a) Anteromedial proximal right leg wound with exposed tibia. Medial gastrocnemius muscle also exposed [arrow] that simplified the medial approach to the medial sural recipient vessels on its undersurface, (b) latissimus dorsi muscle free flap used to provide bone coverage, (c) ultimate result following skin grafting
The Posterior Approach
Godina actually preferred the posterior approach to all blood vessels in the lower extremity whether the patient was in a prone or contralateral decubitus position [21]. For access to the middle third of the popliteal artery, an oblique or midline incision may be adequate [11, 14], but wider exposure is possible with a transverse line marked in the popliteal fossa just above the head of the fibula, which would correspond to the level of the knee joint [21]. This should curve medially upward along the medial hamstring tendons and then laterally downward toward the lateral head of the gastrocnemius (Fig. 40.4) [18]. Skin flaps are retracted in a suprafascial plane, with the deep fascia then incised in the midline. The medial sural cutaneous nerve and lesser saphenous vein found separating the heads of the gastrocnemius should be preserved. Following the lesser saphenous vein will lead to the popliteal vein. The popliteal artery will be found anterior and medial to the vein. That should be followed distally, with complete exposure possible by retraction of the heads of the gastrocnemius muscle. The medial sural neurovascular pedicle will be seen on the undersurface of the medial head extending to the muscle hilum. These extramuscular vessels can then be divided where their caliber and pedicle length are most suitable to match that of the chosen free flap (Fig. 40.5). Through the same posterior approach, the lateral sural vessels may be followed distal to the popliteal artery to visualize underneath the lateral head. The potential of these vessels as recipient should be evaluated based on their length and caliber characteristics. In this region, if the vena comitantes of sural vessels are inadequate, numerous other more satisfactory veins will be found in the vicinity including the lesser saphenous vein that has already been encountered (Video 40.1).
Wide exposure using the posterior approach to the medial sural vessels follows a transverse line in the popliteal fossa corresponding to the knee joint, which curves upward medially along the course of the medial hamstring muscles, then downward laterally toward the lateral head of the gastrocnemius muscle
(a) Wound dehiscence involving chronic atrophic scar of popliteal space in below-knee amputation stump, (b) posterior approach to the medial sural artery [a.] and vein [v.] seen in vessel loops. Incidental exposure of lateral gastrocnemius muscle [LG] verified level of dissection in this scarred region, (c) profunda artery perforator free flap chosen to resurface the defect using medial sural vessels recipient site [microgrid] with flap artery anastomosed in end-to-end fashion to medial sural artery [a.] and vein coupled to medial sural vein [v.] as seen in enlarged view, (d) early successful flap revascularization
The Intramuscular Perforator Approach
Another possibility with the patient in a supine or ipsilateral decubitus position requires first the identification using available imaging modalities of a musculocutaneous perforator in the medial calf [22], identical to that when harvesting a medial sural artery perforator flap [23]. This is easiest with the knee flexed and hip externally rotated. If a thigh tourniquet is used, exsanguination should not be done to insure that all veins remain filled and obvious. A subfascial longitudinal exploratory incision is first made to confirm the exact location of the perforator (Fig. 40.6). Just as with any perforator flap, the usual tedious intramuscular dissection of the perforator back to its origin from a medial sural branch requires careful control of side branches to maintain hemostasis (Fig. 40.7). This dissection is completed when the medial sural vein and artery are of sufficient caliber to match that of the flap as apropos and can actually be continued back to their origin from the popliteal vessels if necessary [24]. If the vein is inadequate, a nearby subcutaneous branch or the greater saphenous vein itself may be sought.
Dissection of medial sural musculocutaneous perforator [p] through medial gastrocnemius muscle [MG] will lead to a branch of the medial sural vessels [MS, here encircled in vessel loop] that can be further dissected toward the vascular hilum until the desired caliber is reached to serve as a recipient site
Discussion
The medial sural vessels represent alternative if a recipient vascular site is needed around the knee [11, 12]. Unlike some other branches of the major vessels of the thigh, these will always be present and always of reasonable caliber. An end-to-end microanastomosis can always be done with good exposure, as these vessels can be brought up somewhat from the depths of the popliteal space. In addition, this will also avoid using an end-to-side anastomosis to the popliteal vessels, which could be technically challenging.
The medial approach to the popliteal fossa probably is the simplest for finding the extramuscular course of the medial sural vessels [12] and best if the patient must be in a supine position to allow access to the more common anterior lower leg injures requiring simultaneous debridement or flap insetting. Postoperative external pressures on microanastomosis here will be better avoided, particularly when compared to the posterior approach. That, of course, would be imperative if a prone position were mandatory [11]. The newest option is the intramuscular perforator approach to the medial sural vessels which would be just like raising the pedicle of any perforator flap. That in itself requires a more difficult microsurgical dissection [25] than the other approaches. Rarely, the purported medial sural musculocutaneous perforator chosen with this approach may turn out to be a median [superficial] sural perforator that might have insufficient dimensions even with more proximal dissection [26]. In addition, access to the cornucopia of vein options as found with either the medial or posterior approach would not be readily available. However, the detachment of muscles or tendons or even injury to the tibial nerve will be avoided with maximum function preservation. As time marches on, the new generation of supermicrosurgeons may even use the perforator alone for a perforator-to-perforator microanastomosis!
References
McCraw JB, Fishman JH, Sharzer LA. The versatile gastrocnemius myocutaneous flap. Plast Reconstr Surg. 1978;62:15–23.
Hallock GG. The medial sural (medial gastrocnemius) perforator local flap. Ann Plast Surg. 2004;53:501–5.
Chien WH, Chen IC, Tan TS, Tang YW. Salvage of knee joint tumor prosthesis using turnover reverse-flow descending branch of lateral circumflex femoral artery as recipient vessel for the free ALT flap: a case report. J Reconstr Microsurg. 2007;23:505–9.
Kim JS, Lee HS, Jang PY, Choi TH, Lee KS, Kim NG. Use of the descending branch of lateral circumflex femoral artery as a recipient pedicle for coverage of a knee defect with free flap: anatomical and clinical study. Microsurgery. 2010;30:32–6.
Gao SH, Feng SM, Chen C, Jiao C, Sun LQ, Zhang WL. A new recipient artery for reconstruction of soft-tissue defects in the lower limb with a free anterolateral thigh flap: the reversed descending branch of the lateral femoral circumflex artery. Plast Reconstr Surg. 2012;130:1059–65.
Yuen JC, Zhou AT. Free flap coverage for knee salvage. Ann Plast Surg. 1996;37:158–66.
Park S, Eom JS. Selection of the recipient vessel in the free flap around the knee: the superior medial genicular vessels and the descending genicular vessels. Plast Reconstr Surg. 2001;105:1177–82.
Fang T, Zhang EW, Lineaweaver WC, Zhang F. Recipient vessels in the free flap reconstruction around the knee. Ann Plast Surg. 2013;71:429–33.
Keller A, Allen R, Shaw W. The medial gastrocnemius muscle flap: a local free flap. Plast Reconstr Surg. 1984;73:974–6.
Salibian AH, Rogers FR, Lamb RC. Microvascular gastrocnemius muscle transfer to the distal leg using saphenous vein grafts. Plast Reconstr Surg. 1984;73:302–7.
Johnson PE, Harris GD, Nagle DJ, Lewis VL. The sural artery and vein as recipient vessels in free flap reconstruction about the knee. J Reconstr Microsurg. 1987;3:233–41.
Hallock GG. The medial approach to the sural vessels to facilitate microanastomosis about the knee. Ann Plast Surg. 1994;32:388–93.
Mathes SJ, Najai F. Classification of the vascular anatomy of muscles: experimental and clinical correlation. Plast Reconstr Surg. 1981;67:177–87.
Beumer JD, Karoo R, Caplash Y, Semmler JG, Taylor J. The medial sural artery as recipient vessel and the impact on the medial gastrocnemius. Ann Plast Surg. 2011;67:382–6.
Ghosh MM. The gastrocnemius vessels as recipient vessels for lower limb free-tissue transfer. Plast Reconstr Surg. 2003;112:936–7.
Tsetsonis CH, Kaxira OS, Laoulakos DH, Spiliopoulou CA, Koutselinis AS. The arterial communications between the gastrocnemius muscle heads: a fresh cadaveric study and clinical implications. Plast Reconstr Surg. 2000;105:94–8.
Arnold PG, Mixter RC. Making the Most of the gastrocnemius muscles. Plast Reconstr Surg. 1983;72:38–48.
Strauch B, Yu HL. Atlas of microvascular surgery. New York: Thieme Medical Publishers; 1993. p. 244–85.
Cavadas PC, Sanz-Giménez-Rico JR, Gutierrez-de la Cámara A, Navarro-Monzonίs A, Soler-Nomdedeu S, Martίnez-Soriano. The medial sural artery perforator free flap. Plast Reconstr Surg. 2001;108:1609–15.
Dusseldorp JR, Pham QJ, Ngo W, Gianoutsos M, Moradi P. Vascular anatomy of the medial sural artery perforator flap: a new classification system of intra-muscular branching patterns. J Plast Reconstr Aesthet Surg. 2014;67:1267–75.
Godina M, Arnez ZM, Lister GD. Preferential use of the posterior approach to blood vessels of the lower leg in microvascular surgery. Plast Reconstr Surg. 1991;88:287–91.
Kosutic D, Pejkovic B, Anderhuber F, Vadnjal-Donlagic S, Zic R, Gulic R, Krajnc I, Solman L, Kocbek L. Complete mapping of lateral and medial sural artery perforators: anatomical study with Duplex-Doppler ultrasound correlation. J Plast Reconstr Aesth Surg. 2012;65:1530–6.
Daar DA, Abdou SA, Cohen JM, Wilson SC, Levine JP. Is the medial sural artery perforator flap a new workhorse flap? A systematic review and meta-analysis. Plast Reconstr Surg. 2019;143:393e–403e.
Smith ML, Molina BJ, Dayan E, Kim JN, Kagen A, Dayan JH. Use of distal medial sural vessels as recipient vessels in free tissue transfer. J Recon Microsurg. 2017;33:59–62.
Georgescu AV, Matei I, Ardelean F, Capota I. Microsurgical non-microvascular flaps in forearm and hand reconstruction. Microsurgery. 2007;27:384–94.
Hallock GG. Anatomic basis of the gastrocnemius perforator-based flap. Ann Plast Surg. 2001;47:517–22.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Electronic Supplementary Material
Cadaver dissection demonstrating exposure of the medial sural and lateral sural vessels through posterior approach (MP4 486378 kb)
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Hallock, G.G., Gurunian, R. (2021). Medial Sural Vessels. In: Gurunian, R., Djohan, R. (eds) Recipient Vessels in Reconstructive Microsurgery. Springer, Cham. https://doi.org/10.1007/978-3-030-75389-4_40
Download citation
DOI: https://doi.org/10.1007/978-3-030-75389-4_40
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-75388-7
Online ISBN: 978-3-030-75389-4
eBook Packages: MedicineMedicine (R0)