Abstract
Background: Acquired resistance to antifungals is rising particularly among Candida species. Herbal ingredients have biological and pharmacological activities, which make them potential fungicidal agents. The present study investigated the effects of curcumin (CUR) and difluorinated curcumin (CDF) on Candida species.
Material and Method: CUR and CDF were examined against Candida isolates obtained from patients candidemia due to C. albicans (n = 13), C. dubliniensis (n = 2), C. parapsilosis (n = 2), and C. tropicalis (n = 1); and laboratory strains of C. albicans (TIMML 1292 and TIMML 183), C. krusei (TIMML 1321), C. parapsilosis (TIMML 2201), and C. tropicalis (TIMML 731) based on the M27-A3 guideline.
Results: At the concentrations of 1–512μg/mL, none of the CDF and CUR showed a significant minimum inhibitory concentration (MIC) range against Candida isolates. There was no significant difference between the effects of CUR and CDF against Candida species.
Conclusion: The CUR and CDF did not exert any inhibitory effect on the growth of Candida strains. Any possible effect on other yeast and filamentous fungi needs to be further investigated.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Nowadays, Candida species have become more frequent and common because of different factors such as the increase in the use of systemic antibiotics, chemotherapy, corticosteroids, etc. [1,2,3]. As reports show, in the United States, Candida species are the fourth leading cause of hospital-acquired bloodstream infections [4]. More than 90% of invasive candidiasis are caused by C. albicans, C. glabrata, C. parapsilosis, C. tropicalis, and C. krusei [1]. However, recently non-albicans Candida species have emerged as important opportunistic pathogens in humans [5]. The quick rise of multidrug-resistant Candida and the slow pace of novel antifungals development has become a serious concern [6]. Thus, various studies express more interest in natural products such as medicinal plants or essential oils, and testing for their antifungal activities [7, 8]. Recently, many studies have determined the efficiency of herbal extracts and their derivatives in treating bacterial and fungal infections [9, 10]. Often these medicinal plants have chemicals or metabolites that can be effective against human pathogens; nevertheless, their antimicrobial susceptibility should be tested on clinical isolates [7, 11]. However, there is not enough evidence about the in vitro activity of herbal plants against clinically significant Candida species. As a result, it is necessary to determine the antifungal susceptibility of these plants on common invasive Candida species. Curcumin (CUR) or diferuloylmethane is the main polyphenolic compound that can be found in the rhizome of Curcuma longa (turmeric) [12]. Turmeric is a well-known member of the Zingiberaceae family, which is used in South Asian traditional medicine to heal fresh wounds, and as a counterirritant for insect bites [13]. CUR has shown an acceptable safety plus numerous biological activities such as antioxidant, anti-inflammatory, antimutagenic, anti-tumor, antimicrobial, immunomodulatory, and anti-proliferative effects which can be effective against a wide variety of diseases [11, 14,15,16,17,18,19,20,21,22,23,24]. Owing to its relatively low bioavailability, several structural analogs of CUR have been developed. 3,4-difluorobenzylidene curcumin, or difluorinated curcumin (CDF), is one of the analogs that has been shown to have improved bioavailability and metabolic stability compared with CUR [25, 26]. Some reports show that CUR has an effective fungicidal activity against a limited number of fungi [27]. Nonetheless, there is not enough evidence about the antifungal effect of these compounds against various Candida species. The main focus of this study is to find out the impact of CUR and CDF against clinical isolates of Candida species obtained from patients with candidemia, along with Candida laboratory strains.
2 Materials and Methods
In this study, the antifungal effect of CUR and CDF was evaluated on 18 Candida clinical isolates collected from blood specimens of patients with candidemia (specialized pediatric Hospital, Mashhad, Iran), and 4 Candida laboratory strains. All of the clinical isolates were identified using the Vitek MS instrument (bioMérieux, Marcy-L’Etoile, France). The laboratory strains included C. albicans (TIMML 1292, and TIMML 183), C. krusei (TIMML 1321), C. parapsilosis (TIMML 2201), and C. tropicalis (TIMML 731). Moreover, the identified clinical isolates included C. albicans (n = 13), C. dubliniensis (n = 2), C. parapsilosis (n = 2), and C. tropicalis (n = 1). The antifungal susceptibility testing was performed according to the Clinical and Laboratory Standards Institute (CLSI) M27-A3 guidelines [28].
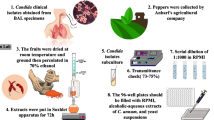
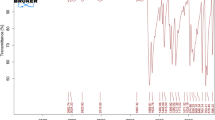
Curcuminoids were obtained from Sami Labs Ltd. (C3 Complex®, Bangalore, India). Synthesis of CDF was performed on the basis of a previously published method [29]. In brief, the mixture of curcumin (1 mmol) and piperidine (0.05 mmol) was added to difluorobenzaldehyde (1 mmol) in methanol. The reaction mixture was stirred for 48 h under N2 stream at room temperature. Synthesis of CDF was confirmed by the validation of its chemical structure using nuclear magnetic resonance spectroscopy.
Briefly, all isolates were sub-cultured on sabouraud dextrose agar (SDA, Sigma, Germany) and incubated at 35 °C for two days. To prepare inoculum suspensions, yeasts were dissolved in a sterile saline solution. The transmittance rate of these yeast suspensions was set to 75–77% at a wavelength of 530 nm using a spectrophotometer. Subsequently, suspensions were diluted 1:1000 in RPMI 1640 medium to reach the final concentration of 1–3 × 103 CFU/ml. Moreover, 3-N-morpholinepropanesulfonic acid (MOPS) (Bio basic, Canada) was used as a buffer for RPMI 1640 medium. First, all of the 96-well plates were filled with 0.1 ml of RPMI 1640 medium; then, the indicated concentrations of CUR and CDF (previously dissolved in dimethyl sulfoxide (DMSO) 1%) along with the fungal suspensions were added to them, and then incubated at 35 °C for two days. The final concentrations of CUR and CDF were 1–512 (1, 2, 4, 8, 16, 32, 64, 128, 256, and 512) μg/ml. Eventually, the minimum inhibitory concentration (MIC) ranges were evaluated visually as the lowest concentration of CUR or CDF, which inhibited at least 80% of the fungal growth, in comparison to positive control well.
3 Results
Based on the results, neither CUR nor CDF could inhibit the fungal growth compared to the control. Therefore, CUR and CDF could not exert a significant MIC range on clinical isolates and laboratory strains of Candida. Moreover, there was no significant difference between CUR and CDF against Candida species. On the other hand, Candida clinical isolates did not show a different susceptibility compared with laboratory strains.
Table 1 summarizes information about the efficacy of CUR and CDF as antifungal agents used in this study.
4 Discussion
The development of new resistance mechanisms against antifungal agents, especially azoles, in Candida species is a critical issue for public health worldwide [30]. Azole resistance among Candida species can happen owing to cellular changes induced by stress responses or upregulation of drug transporters [31]. Moreover, some Candida species such as C. glabrata and C. auris are described to be multidrug-resistant [32]. This study aimed to evaluate the antifungal activity of CUR and CDF against the clinical isolates and laboratory strains of Candida. In general, none of these compounds showed admissible antifungal activity against the tested isolates. Though some studies found the formulation of curcumin and its analogs can be developed against fungal pathogens like Candida species [27, 33]. Various studies show that some natural products can have antifungal activities. Thus, they are valuable as the potential source to develop novel antifungal agents [10, 34]. In traditional medicine, some plants or herbal extracts are described to be effective in preventing or curing infectious diseases [35]. This, mainly the aromatic compounds and secondary metabolites, as a line of defense, can act against microbial invasions [11]. Polyphenols are a great example of such products, can be found in a wide variety of edible plants [9]. Turmeric is a well-known medicinal plant that comes from the Zingiberaceae family [36]. The most active component of turmeric is a lipophilic polyphenol called curcumin [37]. Many factors, such as geographical conditions, can impact the growth and nutrition composition of turmeric. Therefore, 100 grams of turmeric powder may contain around two to five grams of curcumin [27, 38]. Some researches show that this polyphenolic substance has antioxidant, antimicrobial, and anti-inflammatory activities; therefore, it is useful against bacterial and fungal pathogens [39,40,41,42]. Nonetheless, it can decrease the adhesion and biofilm growth of some fungi and bacteria, leading to less severe symptoms in patients [43, 44]. Studies suggest that curcumin can directly affect cell wall permeability by inhibiting or activating pathways such as MAP-kinase and calcineurin-mediated signaling pathways, which play an influential role in the maintenance of cell wall integrity [45]. Moreover, some studies show that curcumin can decrease the amount of aflatoxin B1 produced by Aspergillus flavus too [46].
However, there are limited data about the antifungal activity of curcumin as a natural compound against human fungal pathogens. Besides, there is limited evidence about the biological and pharmacological effects of difluorinated curcumin, as an analog for curcumin, and its antifungal properties. Altogether, most of the studies on curcumin centered on the effect of this compound against Aspergillus and Candida species [9, 39]. In 2015, Zhang et al. conducted an in vitro study about the inhibitory effects of curcumin against non-C. albicans species, and concluded that curcumin effectively prevents the biofilm formation and hyphal extension of Candida spp. [47]. In another study, Tsao et al. evaluated the effects of curcumin combined with amphotericin B or fluconazole against Candida isolates, and showed that curcumin, at concentrations of 32 to 128μg/ml, can increase the antifungal potential in treating Candidiasis [48]. In 2015, Carmello et al. investigated the effects of photodynamic therapy mediated by curcumin, which achieved the increase of reactive oxygen species (ROS) and the DNA damage of C. albicans. Moreover, a study by Kumar et al. confirmed that curcumin can damage the cell wall of C. albicans [43]. In 2020, Zarrinfar et al. studied on the effects of curcuminoids and difluorinated curcumin against dermatophyte isolates such as Trichophyton tonsurans, T. interdigitale, T. mentagrophtes, Microsporum canis, etc., and concluded that this natural compound and its analog could be effective in preventing and treating dermatophytosis [49]. Interestingly, other researchers described curcumin and its analogs as effective antifungal agents against the genera of Alternaria, Aspergillus, and Penicillium too. Thus, it can be helpful to analyze the effect of these analogs against clinical isolates. However, there are limited data about the possible antifungal effects of difluorinated curcumin on Candida species [27]. In the current study, the effect of these compounds was not significant and acceptable against the clinical isolates and laboratory strains of Candida. These findings contradict the results obtained by other studies, which therefore requires further investigation using different designs and tested strains to explore the possible reasons underlying discrepant findings.
5 Conclusion
The results of the present study showed that neither CUR nor CDF had any significant inhibitory effect against both clinical isolates and laboratory strains of Candida. Thus, further investigations are required to find out whether these compounds have any other effects on Candida spp. or other fungal pathogens.
References
Kauffman, C. A., Pappas, P. G., Sobel, J. D., & Dismukes, W. E. (2011). Essentials of clinical mycology. New York: Springer.
Esmailzadeh, A., Zarrinfar, H., Fata, A., & Sen, T. (2018). High prevalence of candiduria due to non-albicans Candida species among diabetic patients: A matter of concern? Journal of Clinical Laboratory Analysis, 32(4), e22343.
Zarrinfar, H., Kaboli, S., Dolatabadi, S., & Mohammadi, R. (2016). Rapid detection of Candida species in bronchoalveolar lavage fluid from patients with pulmonary symptoms. Brazilian Journal of Microbiology, 47(1), 172–176.
Odds, F. (1988). Ecology of Candida and Epidemiology of Candidadosis. Candida and Candidosis, 2nd edn. 68–92.
Arastehfar, A., Daneshnia, F., Najafzadeh, M. J., Hagen, F., Mahmoudi, S., Salehi, M., et al. (2020). Evaluation of molecular epidemiology, clinical characteristics, antifungal susceptibility profiles, and molecular mechanisms of antifungal resistance of Iranian Candida parapsilosis species complex blood isolates. Frontiers in Cellular and Infection Microbiology, 10, 206.
Fisher, M. C., Hawkins, N. J., Sanglard, D., & Gurr, S. J. (2018). Worldwide emergence of resistance to antifungal drugs challenges human health and food security. Science, 360(6390), 739–742.
Katiraee, F., Eidi, S., Bahonar, A., Zarrinfar, H., & Khosravi, A. (2008). Comparision of MICs of some Iranian herbal essences against azole resistance and azole susceptible of Candida Albicans. Journal of Medicinal Plants, 3(27), 37–44.
Kazemi, M., Akbari, A., Zarrinfar, H., Soleimanpour, S., Sabouri, Z., Khatami, M., et al. (2020). Evaluation of antifungal and photocatalytic activities of gelatin-stabilized selenium oxide nanoparticles. Journal of Inorganic and Organometallic Polymers and Materials, 30:3036–3044.
Gupta, S. C., Patchva, S., Koh, W., & Aggarwal, B. B. (2012). Discovery of curcumin, a component of golden spice, and its miraculous biological activities. Clinical and Experimental Pharmacology and Physiology, 39(3), 283–299.
Pulido-Moran, M., Moreno-Fernandez, J., Ramirez-Tortosa, C., & Ramirez-Tortosa, M. (2016). Curcumin and health. Molecules, 21(3), 264.
Mahmood, K., Zia, K. M., Zuber, M., Salman, M., & Anjum, M. N. (2015). Recent developments in curcumin and curcumin based polymeric materials for biomedical applications: A review. International Journal of Biological Macromolecules, 81: 81877–81890.
Nelson, K. M., Dahlin, J. L., Bisson, J., Graham, J., Pauli, G. F., & Walters, M. A. (2017). The essential medicinal chemistry of curcumin: Miniperspective. Journal of Medicinal Chemistry, 60(5), 1620–1637.
E Wright, L., B Frye, J., Gorti, B., N Timmermann, B., & L Funk, J. (2013). Bioactivity of turmeric-derived curcuminoids and related metabolites in breast cancer. Current Pharmaceutical Design, 19(34), 6218–6225.
Mahady, G., Pendland, S., Yun, G., & Lu, Z. (2002). Turmeric (Curcuma longa) and curcumin inhibit the growth of Helicobacter pylori, a group 1 carcinogen. Anticancer Research, 22(6C), 4179–4181.
Vera-Ramirez, L., Pérez-Lopez, P., Varela-Lopez, A., Ramirez-Tortosa, M., Battino, M., & Quiles, J. L. (2013). Curcumin and liver disease. BioFactors, 39(1), 88–100.
Wayne, P. (2008). Clinical and Laboratory Standards Institute (CLSI): Reference method for broth dilution antifungal susceptibility testing of filamentous fungi. Carol Stream: Allured Publishing Corporation.
Ghandadi, M., & Sahebkar, A. (2017). Curcumin: An effective inhibitor of interleukin-6. Current Pharmaceutical Design, 23(6), 921–931.
Hassanzadeh, S., Read, M. I., Bland, A. R., Majeed, M., Jamialahmadi, T., & Sahebkar, A. (2020). Curcumin: An inflammasome silencer. Pharmacological Research, 159.
Iranshahi, M., Sahebkar, A., Hosseini, S.T., Takasaki, M., Konoshima, T., Tokuda, H. (2010) Cancer chemopreventive activity of diversin from Ferula diversivittata in vitro and in vivo. Phytomedicine, 17(3–4), 269–273.
Mollazadeh, H., Cicero, A. F. G., Blesso, C. N., Pirro, M., Majeed, M., & Sahebkar, A. (2019). Immune modulation by curcumin: The role of interleukin-10. Critical Reviews in Food Science and Nutrition, 59(1), 89–101.
Momtazi, A. A., Derosa, G., Maffioli, P., Banach, M., & Sahebkar, A. (2016). Role of microRNAs in the therapeutic effects of curcumin in non-cancer diseases. Molecular Diagnosis and Therapy, 20(4), 335–345.
Panahi, Y., Ahmadi, Y., Teymouri, M., Johnston, T. P., & Sahebkar, A. (2018). Curcumin as a potential candidate for treating hyperlipidemia: A review of cellular and metabolic mechanisms. Journal of Cellular Physiology, 233(1), 141–152.
Panahi, Y., Khalili, N., Sahebi, E., Namazi, S., Simental-Mendía, L.E., Majeed, M., Sahebkar, A. (2018) Effects of Curcuminoids Plus Piperine on Glycemic, Hepatic and Inflammatory Biomarkers in Patients with Type 2 Diabetes Mellitus: A Randomized Double-Blind Placebo-Controlled Trial. Drug Research, 68(7), 403–409.
Teymouri, M., Pirro, M., Johnston, T. P., & Sahebkar, A. (2017). Curcumin as a multifaceted compound against human papilloma virus infection and cervical cancers: A review of chemistry, cellular, molecular, and preclinical features. BioFactors, 43(3), 331–346.
Padhye, S., Banerjee, S., Chavan, D., Pandye, S., Swamy, K. V., Ali, S., et al. (2009). Fluorocurcumins as cyclooxygenase-2 inhibitor: Molecular docking, pharmacokinetics and tissue distribution in mice. Pharmaceutical Research, 26(11), 2438–2445.
Momtazi, A.A., Sahebkar, A. (2016) Difluorinated Curcumin: A Promising Curcumin Analogue with Improved Anti-Tumor Activity and Pharmacokinetic Profile. Curr Pharm Des, 22(28):4386–4397.
Martins, C., Da Silva, D., Neres, A., Magalhaes, T., Watanabe, G., Modolo, L., et al. (2009). Curcumin as a promising antifungal of clinical interest. Journal of Antimicrobial Chemotherapy, 63(2), 337–339.
Cowen, L. E., Sanglard, D., Howard, S. J., Rogers, P. D., & Perlin, D. S. (2015). Mechanisms of antifungal drug resistance. Cold Spring Harbor Perspectives in Medicine, 5(7), a019752.
Qiu, X., Du, Y., Lou, B., Zuo, Y., Shao, W., Huo, Y., et al. (2010). Synthesis and identification of new 4-arylidene curcumin analogues as potential anticancer agents targeting nuclear factor-kappaB signaling pathway. Journal of Medicinal Chemistry, 53(23), 8260–8273.
Sardari, A., Zarrinfar, H., & Mohammadi, R. (2019). Detection of ERG11 point mutations in Iranian fluconazole-resistant Candida albicans isolates. Current Medical Mycology, 5(1), 7.
Kuttan, R., Bhanumathy, P., Nirmala, K., & George, M. (1985). Potential anticancer activity of turmeric (Curcuma longa). Cancer Letters, 29(2), 197–202.
Prasad, C. S., Shukla, R., Kumar, A., & Dubey, N. (2010). In vitro and in vivo antifungal activity of essential oils of Cymbopogon martini and Chenopodium ambrosioides and their synergism against dermatophytes. Mycoses, 53(2), 123–129.
Katiraee, F., Helan, J. A., Emami, S. J., Hamidian, G., & Babaei, E. (2016). An investigation of the inhibitory effects of dendrosomal nanocurcumin on Candida albicans and systemic candidiasis in BALB/c mice. Current Medical Mycology, 2(1), 7.
Alalwan, H., Rajendran, R., Lappin, D. F., Combet, E., Shahzad, M., Robertson, D., et al. (2017). The anti-adhesive effect of curcumin on Candida albicans biofilms on denture materials. Frontiers in Microbiology, 8659.
Jurenka, J. S. (2009). Anti-inflammatory properties of curcumin, a major constituent of Curcuma longa: A review of preclinical and clinical research. Alternative Medicine Review, 14(2):141–53.
Hayakawa, H., Kobayashi, T., Minaniya, Y., Ito, K., Miyazaki, A., Fukuda, T., et al. (2011). Development of a molecular marker to identify a candidate line of turmeric (Curcuma longa L.) with a high curcumin content. American Journal of Plant Sciences, 2(01), 15.
Hossain, M. A., & Ishimine, Y. (2005). Growth, yield and quality of turmeric (Curcuma longa L.) cultivated on dark-red soil, gray soil and red soil in Okinawa, Japan. Plant Production Science, 8(4), 482–486.
Kocaadam, B., & Şanlier, N. (2017). Curcumin, an active component of turmeric (Curcuma longa), and its effects on health. Critical Reviews in Food Science and Nutrition, 57(13), 2889–2895.
Prasad, S., Gupta, S. C., Tyagi, A. K., & Aggarwal, B. B. (2014). Curcumin, a component of golden spice: from bedside to bench and back. Biotechnology Advances, 32(6), 1053–1064.
Shehzad, A., Rehman, G., & Lee, Y. S. (2013). Curcumin in inflammatory diseases. BioFactors, 39(1), 69–77.
Shahzad, M., Millhouse, E., Culshaw, S., Edwards, C. A., Ramage, G., & Combet, E. (2015). Selected dietary (poly) phenols inhibit periodontal pathogen growth and biofilm formation. Food & Function, 6(3), 719–729.
Shahzad, M., Sherry, L., Rajendran, R., Edwards, C. A., Combet, E., & Ramage, G. (2014). Utilising polyphenols for the clinical management of Candida albicans biofilms. International Journal of Antimicrobial Agents, 44(3), 269–273.
Kumar, A., Dhamgaye, S., Maurya, I. K., Singh, A., Sharma, M., & Prasad, R. (2014). Curcumin targets cell wall integrity via calcineurin-mediated signaling in Candida albicans. Antimicrobial Agents and Chemotherapy, 58(1), 167–175.
Temba, B. A., Fletcher, M. T., Fox, G. P., Harvey, J., Okoth, S. A., & Sultanbawa, Y. (2019). Curcumin-based photosensitization inactivates Aspergillus flavus and reduces aflatoxin B1 in maize kernels. Food Microbiology, 82: 8282–8288.
Cheraghipour, K., Ezatpour, B., Masoori, L., Marzban, A., Sepahvand, A., Rouzbahani, A. K., et al. (2020). Anti-candida activity of curcumin: A review. Current Drug Discovery Technologies, 1600–1600.
Tsao, S.-M., & Yin, M.-C. (2000). Enhanced inhibitory effect from interaction of curcumin with amphotericin B or fluconazole against Candida species. Journal of Food and Drug Analysis, 8(3):208–212.
Carmello, J. C., Pavarina, A. C., Oliveira, R., & Johansson, B. (2015). Genotoxic effect of photodynamic therapy mediated by curcumin on Candida albicans. FEMS Yeast Research, 15(4), fov018.
Mustafa, Y. F., Bashir, M. K., & Oglah, M. K. (2020). Original and innovative advances in the synthetic schemes of coumarin-based derivatives: A review. Systematic Reviews in Pharmacy, 11(6), 598–612.
Zarrinfar, H., Behnam, M., Hatamipour, M., & Sahebkar, A. (2021). Antifungal Activities of Curcuminoids and Difluorinated Curcumin Against Clinical Dermatophyte Isolates Adv Exp Med Biol. 1308:101–107.
Acknowledgments
We appreciate the staff of Medical Mycology and Parasitology Laboratory in Ghaem Hospital, Mashhad University of Medical Sciences.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding authors
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Azari, B., Zahmatkesh Moghadam, S., Zarrinfar, H., Tasbandi, A., Jamialahmadi, T., Sahebkar, A. (2021). Antifungal Activity of Curcuminoids and Difluorinated Curcumin Against Clinical Isolates of Candida Species. In: Sahebkar, A., Sathyapalan, T. (eds) Natural Products and Human Diseases. Advances in Experimental Medicine and Biology(), vol 1328. Springer, Cham. https://doi.org/10.1007/978-3-030-73234-9_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-73234-9_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-73233-2
Online ISBN: 978-3-030-73234-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)