Abstract
The serotonin 2B receptor (5-HT2BR) is the most recent addition to the 5-HT2R family. During the last decade, a growing number of studies have shown that the central 5-HT2BR participates in the control of serotonin (5-HT) and dopamine (DA) neuron activity and have underlined its potential for new therapeutic strategies for several neuropsychiatric disorders such as drug addiction, depression and schizophrenia. After reviewing the major advances in the identification and characterization of this receptor within the central nervous system, this chapter focuses on its functional role in the control of ascending DA pathway activity and on the mechanisms underlying this interaction, by covering electrophysiological, neurochemical and behavioral data mainly from in vivo studies in rats. Afterwards, the therapeutic relevance of 5-HT2BR antagonists for treating DA-dependent neuropsychiatric disorders is discussed by focusing on schizophrenia.
This study was supported by grants from the Institut National de la Santé et de la Recherche Médicale (INSERM) and Bordeaux University.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Serotonin 2B receptor
- Serotonin
- Dopamine
- Intracerebral microdialysis
- Rat
- Nucleus accumbens
- Medial prefrontal cortex
- Dorsal raphe nucleus
- Schizophrenia
1 Introduction
The serotonin 2B receptor (5-HT2BR) is the most recent addition to the 5-HT2R family, which also comprises the 5-HT2AR and the 5-HT2CR subtypes [1]. Formerly called 5-HT2FR, the 5-HT2BR belongs to the seven transmembrane spanning receptor superfamily commonly referred to as G-protein-coupled receptors . It was first cloned and characterized in the rat stomach fundus [2, 3], then in mice [4] and in humans [5,6,7]. It has been shown to be present in various peripheral tissues in both rodents and humans, where it participates in the regulation of several physiological functions such as the gastrointestinal, the vascular, the pulmonary, the cardiac and the immune ones, for review, see [8]. In 1997, a few years after its cloning, the 5-HT2BR was shown to be localized also in the mammalian brain. Immunohistochemistry studies assessing 5-HT2BR protein expression in the rat brain demonstrated its presence in the frontal cortex (FC), the cerebellum, the lateral septum, the dorsal hypothalamus and the medial amygdala [9]. Subsequent investigations showed that 5-HT2BR mRNA is expressed in additional rat brain regions such as the dorsal raphe nucleus (DRN), the locus coeruleus, the cerebellum, the habenula, the hippocampus and the hypothalamic paraventricular nucleus [10]. In humans, 5-HT2BR mRNA was detected in the whole brain, and in particular in the cerebellum, the occipital cortex and the FC [5, 11]. Recent studies in mice have provided information about the cellular localization of 5-HT2BRs within the central nervous system (CNS), this issue remaining relatively unexplored in rats [8]. Thus, 5-HT2BRs have been shown to be expressed in primary astrocyte cultures from the neocortex [12], in 5-HT transporter-expressing primary neurons from embryonic raphe nuclei [13], in 5-HT neurons of raphe nuclei [14], in post-natal microglia [15], and in a subpopulation of ventral tegmental area (VTA) DA neurons innervating the nucleus accumbens (NAc) shell subregion [16].
With respect to the peripheral 5-HT2BR, its functional role within the CNS has received much less attention until recently. Indeed, the first studies assessing the role of the central 5-HT2BR on dopamine (DA) ascending pathway activity reported that the 5-HT2BR agonist BW 723C86 and the 5-HT2BR antagonist SB 204741 had no effect on DA neuron firing or on basal DA outflow in the FC, the NAc and the striatum [17, 18]. These negative findings, along with the risk of agonist-induced side effects related to heart-valve pathogenesis [19, 20], probably led to the discontinued use of 5-HT2BR compounds in drug research and development when studying the central 5-HT system, and, in particular, the 5-HT/DA interaction within the CNS. Indeed, it was not until 2008 that the pivotal article by Maroteaux and co-workers showed that the central 5-HT2BR participates in both the neurochemical and behavioral effect of 3,4-methylendioxymethamphetamine (MDMA) in mice [21]. They showed that selective pharmacological blockade with RS 127445 or genetic ablation of the 5-HT2BR reverses MDMA-increased DA outflow in the NAc and 5-HT outflow in the NAc and the VTA, as well as MDMA-induced hyperlocomotion [21]. Subsequently, over the last decade and thanks to the development and availability of potent and high affinity 5-HT2BR antagonists such as LY 266097 and RS 127445 [8, 22, 23], a growing number of studies have confirmed the key role of the central 5-HT2BR in the control of DA and 5-HT neuron activity, and have highlighted its potential as a new pharmacological target for treating several neuropsychiatric disorders such as schizophrenia, depression and drug addiction [8, 14, 16, 24,25,26,27,28,29,30].
The present chapter provides an overview of the role of the 5-HT2BR in the control of ascending DA pathway activity, covering neurochemical, electrophysiological and behavioral data mainly obtained from in vivo studies in the rat. After discussing the role of 5-HT2BRs in controlling the release of DA in the medial prefrontal cortex (mPFC), the NAc and the striatum, we describe recent neurochemical and molecular findings providing the anatomo-functional basis underlying the effects of 5-HT2BR antagonists on the activity of the mesocorticolimbic DA system. Finally, we present some behavioral data adding functional evidence for the therapeutic potential of 5-HT2BR antagonists in the treatment of schizophrenia.
2 The Central 5-HT2BR and DA Ascending Pathways
2.1 Regulation of DA Neuron Activity: In Vivo Neurochemical and Electrophysiological Data
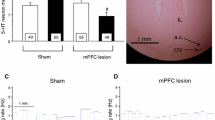
Compelling in vivo biochemical and electrophysiological data demonstrate that, unlike 5-HT2BR agonists [8, 17, 18, 24], 5-HT2BR antagonists modulate DA ascending pathway activity in a differential manner. Thus, both the 5-HT2BR antagonists RS 127445 and LY 266097 increase and decrease DA outflow in the mPFC and the shell subregion of the NAc, respectively, but do not modify DA outflow in the striatum or in the core subregion of the NAc [24,25,26]. In line with these results, electrophysiological findings have shown that selective blockade of 5-HT2BRs has no effect at the level of the substantia nigra pars compacta but decreases the firing rate of DA neurons in the VTA, presumably those projecting to the shell subregion of the NAc [26]. Based on these findings which provide additional support for the insensitivity of the nigrostriatal DA pathway to 5-HT2BR modulation, it is tempting to hypothesize that 5-HT2BR antagonism reduces accumbal DA outflow via an inhibitory modulation of mesoaccumbal DA neuronal firing. Nevertheless, as discussed elsewhere [26], in keeping with the cellular heterogeneity of the VTA [31,32,33,34], further studies are needed to identify DA neurons projecting to the NAc or to the mPFC. Altogether, these findings demonstrate that 5-HT2BRs independently control the activity of the three ascending DA pathways by specifically providing tonic excitatory and inhibitory controls on NAc and mPFC DA outflow , respectively, and no effect in the striatum (Fig. 19.1).
Differential control exerted by central serotonin 2B receptors (5-HT2BRs) on the activity of ascending dopamine (DA) pathways. They exert a tonic inhibitory control on DA outflow in the medial prefrontal cortex (mPFC), a tonic excitatory control on DA outflow in the nucleus accumbens (NAc), but have no effect at the level of the striatum (Str), for details see [26]
This conclusion contrasts with that offered by the first studies assessing the effect of this receptor on DA neuron activity and reporting that 5-HT2BR blockade has no effect on DA ascending pathway activity [17, 18]. As discussed elsewhere [8], the use of high doses of non-selective 5-HT2B compounds as well as some methodological drawbacks could be responsible for the discrepancies observed.
During recent years, much attention has been devoted to identifying the mechanisms and the anatomo-functional basis underlying the modulatory control exerted by 5-HT2BRs on the mesocorticolimbic DA system. Interestingly, it has been demonstrated that the opposite effect of 5-HT2BR antagonists on mPFC and NAc shell DA outflow involves a functional interplay between 5-HT2BRs and 5-HT1ARs located in the DRN and in the mPFC, respectively (Fig. 19.2). By increasing cortical 5-HT outflow, intra-DRN 5-HT2BR blockade triggers the stimulation of 5-HT1ARs located on mPFC GABAergic interneurons [35], thereby leading to the activation of pyramidal glutamatergic neurons [36] which drive opposite changes of mPFC and NAc DA outflow through direct or indirect interactions with VTA DA neurons [27, 37]. The involvement of these polysynaptic cortical-subcortical pathways is supported by the finding that the opposite change of mPFC and NAc DA outflow induced by the intra-DRN administration of RS 127445 is suppressed by the intra-mPFC perfusion of the selective 5-HT1AR antagonist WAY 100635 [27]. These results provide the first evidence for a functional role of a specific 5-HT2BR population in the regulatory control of DA neuron activity, and show that the DRN is a key brain region driving the 5-HT2BR-DA system interaction.
Putative neuronal circuits involved in the opposite effect of serotonin 2B receptor (5-HT2BR) antagonists on dopamine (DA) outflow in the medial prefrontal cortex (mPFC) and the nucleus accumbens (NAc). In the dorsal raphe nucleus (DRN), in addition to the autoinhibitory control exerted by somatodendritic 5-HT1A autoreceptors, 5-HT neurons are regulated by a local negative-feedback circuit involving GABA interneurons. The 5-HT2BR is expressed on these GABA interneurons, together with other post-synaptic 5-HTRs (5-HT1AR, 5-HT2AR and 5-HT2CR), and provides a tonic inhibitory control on 5-HT cells innervating the mPFC via GABAARs. The 5-HT1AR is expressed in the mPFC by GABA interneurons and pyramidal glutamatergic (Glu) neurons innervating the ventral tegmental area (VTA). In the VTA, Glu afferencies arising from mPFC Glu neurons provide a direct excitatory and GABA-mediated inhibitory control on the mesocortical and mesoaccumbal DA ascending pathways, respectively. Thus, by reducing GABA inhibitory tone, blockade of DRN 5-HT2BRs leads to increased activity of 5-HT neurons and consequently to increased 5-HT outflow in the DRN and the mPFC. Increased mPFC 5-HT outflow could trigger the stimulation of 5-HT1ARs expressed by local GABA interneurons. Subsequent disinhibition of mPFC Glu neurons innervating the VTA could respectively stimulate and inhibit the activity of the mesocortical and the mesoaccumbal DA pathways, thereby leading to increased and decreased DA outflow in the mPFC and the NAc, respectively, for details see [26, 27, 38]
Subsequent investigations exploring the mechanisms underlying the facilitatory effect of 5-HT2BR antagonists on DRN 5-HT neurons innervating the mPFC demonstrated that 5-HT2BRs, in the rat DRN exert a GABA-mediated tonic inhibitory control on 5-HT neurons [38], (Fig. 19.2). This conclusion is supported by several compelling findings. First, it has been shown that intra-DRN perfusion of the GABAAR antagonist bicuculline prevents the increase in DRN and mPFC 5-HT outflow induced by intra-DRN administration of RS 127445 [38]. These results confirm and extend previous observations that peripheral administration of RS 127445 increases the firing rate of DRN 5-HT neurons and 5-HT outflow in the mPFC [27]. Second, the increase in DRN 5-HT outflow induced by the local administration of the selective 5-HT reuptake inhibitor citalopram is potentiated by the intra-DRN administration of RS 127445 only in the absence of bicuculline perfusion into the DRN [38]. Third, in agreement with the above-mentioned in vivo neurochemical findings, in vitro experiments coupling immunohistochemistry to reverse transcription-polymerase chain reaction revealed the presence of 5-HT2BR mRNA on DRN GABAergic interneurons [38].While confirming the DRN as the main site of action of 5-HT2BR antagonists, these results provide the first evidence for the location of the 5-HT2BR in a specific cell population in the rat brain, and demonstrate its role in controlling the local negative-feedback loop regulating DRN 5-HT neuron activity via GABA interneurons (see Fig. 19.2), [38,39,40,41]. Of note, among the different 5-HTRs located on DRN GABA interneurons (5-HT2AR, 5-HT2CR and 5-HT1AR) and participating in the local control of 5-HT neurons [39,40,41], the 5-HT2BR is the only one providing a tonic control on 5-HT neurons [38]. From a functional point of view, these findings provide additional information on the mechanisms subsuming the effect of 5-HT2BR antagonists on the mesocorticolimbic DA system, which has been shown to result from their ability to increase the activity of DRN 5-HT neurons projecting to the mPFC [27]. However, these data contrast with recent findings in mice showing that 5-HT2BRs are located on 5-HT neurons and exert a direct positive control on 5-HT neuron activity [42]. As discussed elsewhere [8, 38], these discrepant findings may result from species related anatomo-functional differences, so additional comparative studies between rats and mice are required to identify possible differences in the brain cellular distribution of the 5-HT2BR.
2.2 5-HT2BR Antagonists: Behavioral Data and Therapeutic Potential for the Treatment of Schizophrenia
Altogether, the neurochemical findings discussed above indicate that 5-HT2BR antagonists may provide a useful pharmacological tool for treating neuropsychiatric disorders requiring the independent control of ascending DA pathways. In this context, schizophrenia is an emblematic mental illness that could benefit from 5-HT2BR antagonist treatment. It is characterized by three main groups of symptoms: positive (i.e. hallucinations, delusions), negative (i.e. social interaction deficits, blunted affect) and cognitive (i.e. working and reference memory deficits, executive function impairments, decreased vigilance) [43,44,45]. This multimodal symptomatology is classically related to an imbalance in central DA neurotransmission: positive symptoms are thought to result from DA hyperfunction in the NAc, whereas negative and cognitive symptoms might involve DA hypofunction in the FC [45, 46]. The pharmacological treatment of schizophrenia is based on the use of DA-D2 receptor antagonists classified as typical and atypical antipsychotic drugs (APDs) [43]. Although effective in controlling positive symptoms, typical APD such as haloperidol and chlorpromazine are responsible for the occurrence of extrapyramidal side effects (EPS) due to altered striatal DA activity [43, 47]. On the other hand, atypical APDs, of which clozapine is the prototype, display a wider therapeutic spectrum covering positive, negative and cognitive symptoms with a limited propensity to induce EPS [43, 44].
Thus, given their unique DAergic profile of effects, 5-HT2BR antagonists should be able to improve all the symptoms of schizophrenia without inducing EPS by restoring normal DA function. This hypothesis has been demonstrated by recent studies in rats assessing their effectiveness in different DA-dependent behavioral models classically used to predict the ability of APDs to alleviate positive [hyperlocomotion induced by the non-competitive N-methyl-D-aspartate receptor antagonist phencyclidine (PCP)] and cognitive [PCP-induced deficit in novel object recognition (NOR) test] symptoms of schizophrenia, as well as their propensity to induce EPS (catalepsy test), [45]. These behavioral tests are known to be related to increased, reduced and altered DA function in the NAc, the mPFC and the striatum, respectively [47,48,49]. Thus, in line with their differential effects on DA outflow in these brain regions, the 5-HT2BR antagonists RS 127445 and LY 266097 have been shown to reduce the hyperlocomotion induced by PCP [26]. This result is consistent with previous findings showing that 5-HT2BR blockade reduces amphetamine-induced hyperlocomotion [24], another behavioral model used to investigate the potential of APDs to restore normal accumbal DA function [45]. Furthermore, both 5-HT2BR antagonists were able to reverse PCP-induced NOR deficit to a similar extent as clozapine [26]. Finally, unlike haloperidol, neither RS 127445 nor LY 266097 produced a cataleptic state [26].
These findings providing additional support for the therapeutic relevance of 5-HT2BR antagonists for treating schizophrenia suggest that these compounds could represent a new class of atypical APDs, given their ideal profile of effects expected to alleviate cognitive and positive symptoms, without eliciting EPS [8, 26]. However, as discussed elsewhere [8, 26], this proposal has to be confirmed, so additional investigations are required to profile the acute or chronic effects of 5-HT2BR antagonists in a palette of other experimental conditions predictive of therapeutic efficacy or side effects [45, 50]. Their involvement in metabolism, body mass and diabetic disorders, commonly referred to as “metabolic syndrome” [43, 45], as well as their ability to alleviate the negative symptoms of schizophrenia deserve dedicated studies.
In addition to the therapeutic potential of 5-HT2BR antagonists per se, 5-HT2BRs could contribute to the therapeutic benefit of atypical APDs, many of which (clozapine, amisulpride, asenapine, aripiprazole, cariprazine) display antagonist properties at the 5-HT2BR [51,52,53,54,55] and the DA-D2R, together with partial agonist properties towards the 5-HT1AR [45, 56]. This hypothesis is supported by the ability of 5-HT2BR blockade to potentiate and decrease haloperidol-induced DA outflow in the mPFC and the NAc, respectively [24, 26], together with the functional role of 5-HT1AR stimulation in the 5-HT2BR-mediated control of DA outflow [27].
Importantly, these conclusions pointing to the potential of 5-HT2BR antagonists for treating schizophrenia diverge from those offered by studies in mice showing that genetic ablation of 5-HT2BRs generate an antipsychotic-sensitive schizophrenic-like phenotype [29]. As discussed elsewhere [8, 26], in keeping with the role of 5-HT2BRs in brain maturation [15], developmental neural adaptations triggered by the permanent suppression of this receptor as well as species-related anatomo-functional differences may account for these divergences. Nonetheless, although additional investigations are warranted to clarify this issue, these findings support the role of 5-HT2BRs in the neurobiology and/or improved treatment of schizophrenia.
3 Conclusions and Perspectives
In conclusion, this chapter provides an updated overview of the important advances in the understanding of the physiological role of the central 5-HT2BR in the control of DA ascending pathways and the anatomo-functional basis underlying this interaction. Specifically, the findings reported herein identify the DRN as a major site of action for the 5-HT2BR-dependent control of DA and 5-HT neuron activity. First, the differential control exerted by 5-HT2BR antagonists on the mesocorticolimbic DA system takes place in the DRN and involves complex polysynaptic cortico-subcortical pathways driven by a functional interplay between DRN 5-HT2BRs and mPFC 5-HT1ARs [27]. Second, in the DRN, 5-HT2BRs are located on GABA interneurons and exert a tonic inhibitory control on 5-HT neurons projecting to the mPFC by participating in the control of the local negative-feedback loop regulating 5-HT neuron activity [38].
From a clinical point of view and in keeping with their unique profile of effects on DA network, the data reported here highlight the therapeutic potential of 5-HT2BR antagonists for the treatment of schizophrenia, a major neuropsychiatric disorder whose optimal treatment requires the independent control of ascending DA pathways [8, 44, 45].
Additional experiments are warranted to obtain a deeper insight into the pathophysiological role of the 5-HT2BR in the mammalian brain, and to verify the extent to which the contrasting findings observed between rats and mice are related to anatomo-physiological differences between species and/or to brain development-related factors. In addition, further investigations in a larger palette of experimental conditions including long-term treatments are mandatory to confirm the therapeutic potential of 5-HT2BR antagonists for treating schizophrenia [8, 45]. In this context, investigations in advanced genetic models such as conditional 5-HT2BR knock-out animals should be pursued. Finally, these data reported in this chapter provide additional knowledge about the regulation of ascending DA pathways by the central 5-HT system, and highlight the legitimacy of 5-HT2BRs as key modulators of the activity of the central DA network.
Abbreviations
- 5-HT:
-
Serotonin
- 5-HT2BR:
-
5-HT2B receptor
- APD:
-
Antipsychotic drug
- CNS:
-
Central nervous system
- DA:
-
Dopamine
- DRN:
-
Dorsal raphe nucleus
- EPS:
-
Extrapyramidal side effects
- FC:
-
Frontal cortex
- MDMA:
-
3,4-methylendioxymethamphetamine
- mPFC:
-
Medial prefrontal cortex
- NAc:
-
Nucleus accumbens
- NOR:
-
Novel object recognition
- PCP:
-
Phencyclidine
- VTA:
-
Ventral tegmental area
References
Hannon J, Hoyer D (2008) Molecular biology of 5-HT receptors. Behav Brain Res 195:198–213
Foguet M, Hoyer D, Pardo LA, Parekh A, Kluxen FW, Kalkman HO, Stuhmer W, Lubbertet H (1992) Cloning and functional characterization of the rat stomach fundus serotonin receptor. EMBO J 11:3481–3487
Kursar JD, Nelson DL, Wainscott DB, Cohen ML, Baez M (1992) Molecular cloning, functional expression, and pharmacological characterization of a novel serotonin receptor (5-hydroxytryptamine2F) from rat stomach fundus. Mol Pharmacol 42:549–557
Loric S, Launay JM, Colas JF, Maroteaux L (1992) New mouse 5-HT2-like receptor Expression in brain, heart and intestine. FEBS Lett 312:203–207
Bonhaus DW, Bach C, DeSouza A, Salazar FH, Matsuoka BD, Zuppan P, Chan HW, Eglenet RM (1995) The pharmacology and distribution of human 5-hydroxytryptamine2B (5-HT2B) receptor gene products: comparison with 5-HT2A and 5-HT2C receptors. Br J Pharmacol 115:622–628
Kursar JD, Nelson DL, Wainscott DB, Baez M (1994) Molecular cloning, functional expression, and mRNA tissue distribution of the human 5-hydroxytryptamine2B receptor. Mol Pharmacol 46:227–234
Schmuck K, Ullmer C, Engels P, Lübbert H (1994) Cloning and functional characterization of the human 5-HT2B serotonin receptor. FEBS Lett 342:85–90
Devroye C, Cathala A, Piazza PV, Spampinato U (2018) The central serotonin2B receptor as a new pharmacological target for the treatment of dopamine-related neuropsychiatric disorders: rationale and current status of research. Pharmacol Ther 181:143–155
Duxon MS, Flanigan TP, Reavley AC, Baxter GS, Blackburn TP, Fone KC (1997) Evidence for expression of the 5-hydroxytryptamine-2B receptor protein in the rat central nervous system. Neuroscience 76:323–329
Bonaventure P, Guo H, Tian B, Liu X, Bittner A, Roland B, Salunga R, Ma XJ, Kamme F, Meurers B, Bakker M, Jurzak M, Leysen JE, Erlander MG (2002) Nuclei and subnuclei gene expression profiling in mammalian brain. Brain Res 943:38–47
Bevilacqua L, Doly S, Kaprio J, Yuan Q, Tikkanen R, Paunio T, Zhou Z, Wedenoja J, Maroteaux L, Diaz S, Belmer A, Hodgkinson CA, Dell’Osso L, Suvisaari J, Coccaro E, Rose RJ, Peltonen L, Virkkunen M, Goldman D (2010) A population-specific HTR2B stop codon predisposes to severe impulsivity. Nature 468:1061–1066
Li B, Zhang S, Zhang H, Nu W, Cai L, Hertz L, Penget L (2008) Fluoxetine-mediated 5-HT2B receptor stimulation in astrocytes causes EGF receptor transactivation and ERK phosphorylation. Psychopharmacology 201:443–458
Launay JM, Schneider B, Loric S, Da Prada M, Kellermann O (2006) Serotonin transport and serotonin transporter-mediated antidepressant recognition are controlled by 5-HT2B receptor signaling in serotonergic neuronal cells. FASEB J 20:1843–1854
Diaz SL, Doly S, Narboux-Nême N, Fernández S, Mazot P, Banas SM, Boutourlinsky K, Moutkine I, Belmer A, Roumier A, Maroteaux L (2012) 5-HT(2B) receptors are required for serotonin-selective antidepressant actions. Mol Psychiatry 17:154–163
Kolodziejczak M, Béchade C, Gervasi N, Irinopoulou T, Banas SM, Cordier C, Rebsam A, Roumier A, Maroteaux L (2015) Serotonin modulates developmental microglia via 5-HT2B receptors: potential implication during synaptic refinement of retinogeniculate projections. ACS Chem Neurosci 6:1219–1230
Doly S, Quentin E, Eddine R, Tolu S, Fernandez SP, Bertran-Gonzalez J, Valjent E, Belmer A, Viñals X, Callebert J, Faure P, Meye FJ, Hervé D, Robledo P, Mameli M, Launay JM, Maldonado R, Maroteaux L (2017) Serotonin 2B receptors in mesoaccumbens dopamine pathway regulate cocaine responses. J Neurosci 37:10372–10388
Di Matteo V, Di Giovanni G, Di Mascio M, Esposito E (2000) Biochemical and electrophysiological evidence that RO 60-0175 inhibits mesolimbic dopaminergic function through serotonin(2C) receptors. Brain Res 865:85–90
Gobert A, Rivet JM, Lejeune F, Newman-Tancredi A, Adhumeau-Auclair A, Nicolas JP, Cistarelli L, Melon C, Millan MJ (2000) Serotonin(2C) receptors tonically suppress the activity of mesocortical dopaminergic and adrenergic, but not serotonergic, pathways: a combined dialysis and electrophysiological analysis in the rat. Synapse 36:205–221
Elangbam CS (2010) Drug-induced valvulopathy: an update. Toxicol Pathol 38:837–848
McCorvy JD, Roth BL (2015) Structure and function of serotonin G protein-coupled receptors. Pharmacol Ther 150:129–142
Doly S, Valjent E, Setola V, Callebert J, Herve D, Launay JM, Maroteaux L (2008) Serotonin 5-HT2B receptors are required for 3,4-methylenedioxymethamphetamine-induced hyperlocomotion and 5-HT release in vivo and in vitro. J Neurosci 28:2933–2940
Audia JE, Evrard DA, Murdoch GR, Droste JJ, Nissen JS, Schenck KW, Fludzinski P, Lucaites VL, Nelson DL, Cohen ML (1996) Potent, selective tetrahydro-beta-carboline antagonists of the serotonin 2B (5-HT2B) contractile receptor in the rat stomach fundus. J Med Chem 39:2773–2780
Bonhaus DW, Flippin LA, Greenhouse RJ, Jaime S, Rocha C, Dawson M, Van Natta K, Chang LK, Pulido-Rios T, Webber A, Leung E, Eglen RM, Martin GR (1999) RS-127445: a selective, high affinity, orally bioavailable 5-HT2B receptor antagonist. Br J Pharmacol 127:1075–1082
Auclair AL, Cathala A, Sarrazin F, Depoortère R, Piazza PV, Newman-Tancredi A, Spampinato U (2010) The central serotonin 2B receptor: a new pharmacological target to modulate the mesoaccumbens dopaminergic pathway activity. J Neurochem 114:1323–1332
Devroye C, Cathala A, Di Marco B, Caraci F, Drago F, Piazza PV, Spampinato U (2015) Central serotonin(2B) receptor blockade inhibits cocaine-induced hyperlocomotion independently of changes of subcortical dopamine outflow. Neuropharmacology 97:329–337
Devroye C, Cathala A, Haddjeri N, Rovera R, Vallée M, Drago F, Piazza PV, Spampinato U (2016) Differential control of dopamine ascending pathways by serotonin2B receptor antagonists: New opportunities for the treatment of schizophrenia. Neuropharmacology 109:59–68
Devroye C, Haddjeri N, Cathala A, Rovera R, Drago F, Piazza PV, Artigas F, Spampinato U (2017) Opposite control of mesocortical and mesoaccumbal dopamine pathways by serotonin2B receptor blockade: Involvement of medial prefrontal cortex serotonin1A receptors. Neuropharmacology 119:91–99
Doly S, Bertran-Gonzalez J, Callebert J, Bruneau A, Banas SM, Belmer A, Boutourlinsky K, Hervé D, Launay JM, Maroteaux L (2009) Role of serotonin via 5-HT2B receptors in the reinforcing effects of MDMA in mice. PLoS ONE 4:e7952
Pitychoutis PM, Belmer A, Moutkine I, Adrien J, Maroteaux L (2015) Mice lacking the serotonin Htr2B receptor gene present an antipsychotic-sensitive schizophrenic-like phenotype. Neuropsychopharmacology 40:2764–2773
Maroteaux L, Ayme-Dietrich E, Aubertin-Kirch G, Banas S, Quentin E, Lawson R, Monassier L (2017) New therapeutic opportunities for 5-HT2 receptor ligands. Pharmacol Ther 170:14–36
Beier KT, Steinberg EE, DeLoach KE, Xie S, Miyamichi K, Schwarz L, Gao XJ, Kremer EJ, Malenka RC, Luo L (2015) Circuit architecture of VTA dopamine neurons revealed by systematic input-output mapping. Cell 162:622–634
Carr DB, Sesack SR (2000) Projections from the rat prefrontal cortex to the ventral tegmental area: target specificity in the synaptic associations with mesoaccumbens and mesocortical neurons. J Neurosci 20:3864–3873
Ikemoto S (2007) Dopamine reward circuitry: two projection systems from the ventral midbrain to the nucleus accumbens-olfactory tubercle complex. Brain Res Rev 56:27–78
Lammel S, Lim BK, Malenka RC (2014) Reward and aversion in a heterogeneous midbrain dopamine system. Neuropharmacology 76:351–359
Santana N, Bortolozzi A, Serrats J, Mengod G, Artigas F (2004) Expression of serotonin1A and serotonin2A receptors in pyramidal and GABAergic neurons of the rat prefrontal cortex. Cereb Cortex 14:1100–1109
Lladó-Pelfort L, Santana N, Ghisi V, Artigas F, Celada P (2012) 5-HT1A receptor agonists enhance pyramidal cell firing in prefrontal cortex through a preferential action on GABA interneurons. Cereb Cortex 22:1487–1497
Sesack SR, Carr DB, Omelchenko N, Pinto A (2003) Anatomical substrates for glutamate-dopamine interactions: evidence for specificity of connections and extrasynaptic actions. Ann N Y Acad Sci 1003:36–52
Cathala A, Devroye C, Drutel G, Revest JM, Artigas F, Spampinato U (2019) Serotonin2B receptors in the rat dorsal raphe nucleus exert a GABA-mediated tonic inhibitory control on serotonin neurons. Exp Neurol 311:57–66
Liu R, Jolas T, Aghajanian G (2000) Serotonin 5-HT(2) receptors activate local GABA inhibitory inputs to serotonergic neurons of the dorsal raphe nucleus. Brain Res 873:34–45
Serrats J, Mengod G, Cortés R (2005) Expression of serotonin 5-HT2C receptors in GABAergic cells of the anterior raphe nuclei. J Chem Neuroanat 29:83–91
Sharp T, Boothman L, Raley J, Quérée P (2007) Important messages in the ‘post’: recent discoveries in 5-HT neurone feedback control. Trends Pharmacol Sci 28:629–636
Belmer A, Quentin E, Diaz SL, Guiard BP, Fernandez SP, Doly S, Banas SM, Pitychoutis PM, Moutkine I, Muzerelle A, Tchenio A, Roumier A, Mameli M, Maroteaux L (2018) Positive regulation of raphe serotonin neurons by serotonin 2B receptors. Neuropsychopharmacology 43:1623–1632
Meltzer HY (2013) Update on typical and atypical antipsychotic drugs. Annu Rev Med 64:393–406
Meltzer HY (2017) New trends in the treatment of schizophrenia. CNS Neurol Disord Drug Targets 16:900–906
Newman-Tancredi A, Kleven MS (2011) Comparative pharmacology of antipsychotics possessing combined dopamine D2 and serotonin 5-HT1A receptor properties. Psychopharmacology 216:451–473
Svensson TH (2000) Dysfunctional brain dopamine systems induced by psychotomimetic NMDA-receptor antagonists and the effects of antipsychotic drugs. Brain Res Rev 31:320–329
Schapira AH, Bezard E, Brotchie J, Calon F, Collingridge GL, Ferger B, Hengerer B, Hirsch E, Jenner P, Le Novère N, Obeso JA, Schwarzschild MA, Spampinato U, Davidai G (2006) Novel pharmacological targets for the treatment of Parkinson’s disease. Nat Rev Drug Discov 5:845–854
Neill JC, Barnes S, Cook S, Grayson B, Idris NF, McLean SL, Snigdha S, Rajagopal L, Harte MK (2010) Animal models of cognitive dysfunction and negative symptoms of schizophrenia: focus on NMDA receptor antagonism. Pharmacol Ther 128:419–432
Steinpreis RE, Salamone JD (1993) The role of nucleus accumbens dopamine in the neurochemical and behavioral effects of phencyclidine: a microdialysis and behavioral study. Brain Res 612:263–270
Porsolt RD, Moser PC, Castagné V (2010) Behavioral indices in antipsychotic drug discovery. J Pharmacol Exp Ther 333:632–638
Abbas AI, Hedlund PB, Huang XP, Tran TB, Meltzer HY, Roth BL (2009) Amisulpride is a potent 5-HT7 antagonist: relevance for antidepressant actions in vivo. Psychopharmacology 205:119–128
De Deurwaerdère P (2016) Cariprazine: new dopamine biased agonist for neuropsychiatric disorders. Drugs Today 52:97–110
Kiss B, Horváth A, Némethy Z, Schmidt E, Laszlovszky I, Bugovics G, Fazekas K, Hornok K, Orosz S, Gyertyán I, Agai-Csongor E, Domány G, Tihanyi K, Adham N, Szombathelyi Z (2010) Cariprazine (RGH-188), a dopamine D(3) receptor-preferring, D(3)/D(2) dopamine receptor antagonist-partial agonist antipsychotic candidate: in vitro and neurochemical profile. J Pharmacol Exp Ther 333:328–340
Shahid M, Walker GB, Zorn SH, Wong EH (2009) Asenapine: a novel psychopharmacologic agent with a unique human receptor signature. J Psychopharmacol 23:65–73
Shapiro DA, Renock S, Arrington E, Chiodo LA, Liu LX, Sibley DR, Roth BL, Mailman R (2003) Aripiprazole, a novel atypical antipsychotic drug with a unique and robust pharmacology. Neuropsychopharmacology 28:1400–1411
Meltzer HY, Massey BW (2011) The role of serotonin receptors in the action of atypical antipsychotic drugs. Curr Opin Pharmacol 11:59–67
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Cathala, A., Spampinato, U. (2021). Serotonin 2B Receptor Interactions with Dopamine Network: Implications for Therapeutics in Schizophrenia. In: Maroteaux, L., Monassier, L. (eds) 5-HT2B Receptors. The Receptors, vol 35. Springer, Cham. https://doi.org/10.1007/978-3-030-55920-5_19
Download citation
DOI: https://doi.org/10.1007/978-3-030-55920-5_19
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-55919-9
Online ISBN: 978-3-030-55920-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)