Abstract
Infection is a serious complication of cardiac implantable electrical devices (CIED) leading to substantial morbidity and mortality with reported in-hospital mortality rates of 3.7–11.3%. The incidence of CIED infections (CIEDI) is increasing over time, outwaiting the increase in device implantation rate. The exact reasons for this phenomenon remains unclear. On one side it could derive from a shift in the implanted devices with a rising proportion of more complex systems. Although, it seems to be coupled to implantations in ‘higher-risk’ patients with comorbidities or conditions leading to immune compromise. The only treatment is complete removal of the entire CIED system. Given this background, it is highly warranted to identify valid risk factors for device infection as it may allow for preventive measures that may result in better infection control strategies for high-risk patients and which also can improve risk assessment in the management of device revisions. In this chapter we will describe all the known risk factors for CIEDI in the light of known pathophysiology. Later we will put these data in the perspective of CIEDI prophylaxis.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
3.1 Introduction
The incidence of infections related to cardiac implantable electrical devices (CIEDI) is increasing over time [1,2,3], partly related to an increasing numbers of cardiac implantable electronic device (CIED) implants due to widening indications and increasing numbers of generator replacements. While the proportion of more complex CIED systems implanted, such as implantable cardioverter defibrillator (ICD) and cardiac resynchronization therapy (CRT) devices [1, 4,5,6], is increasing, infections are increasing for all device types, particularly for CRT devices [2]. From 2000 to 2012, device-related infections increased from 1.45% to 3.41% (p < .001) [2]. The risk of infection for CRT devices was the highest, peaking in 2012 (adjusted odds ratio [OR] 2.43, p < .001) [2]. Although the exact reasons for increasing device-related infections remain unclear, it seems to be coupled to implantations in ‘higher-risk’ patients with comorbidities or conditions leading to immune compromise [1, 2].
Infection is a serious complication of CIED implantations leading to substantial morbidity and mortality with reported in-hospital mortality rates of 3.7–11.3% [1, 7,8,9,10].
Comorbidities associated with higher mortality during admissions for procedures related to device infection were stroke (OR, 3.19; p < .001), end-stage renal disease (OR, 2.91; p < .001), malnutrition (OR, 2.67; p < .001), cirrhosis (OR, 2.05; p = .001), organ transplantation (OR, 2.16; p < .001), congestive heart failure (OR, 2.00; p < .001), venous thromboembolism (OR, 1.68; P < .001), and chronic lung disease (OR, 1.43; P < .001) [2].
Device removal and systemic antibiotic therapy is the standard of care [11], which is based on randomized controlled trials including meta-analysis showing that antibiotic prophylaxis reduces the risk for CIED infectious complications [12, 13].
Given this background, it is highly warranted to identify valid risk factors for device infection as it may allow for preventive measures that may result in better infection control strategies for high-risk patients and which also can improve risk assessment in the management of device revisions.
3.2 Pathogenesis
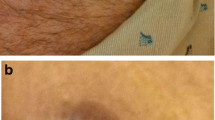
Device infections occur most commonly when leads and pulse generator are contaminated during implantation or later manipulation when crossing skin barrier. Contamination and subsequent bacterial colonization result in pocket infection which is the most common presentation of CIEDI [9, 14]. It commonly tracks along leads and can cause secondary bloodstream infection with progress to systemic infection and endocarditis. A less common mechanism is spread of bacteria from a distant infectious focus with secondary involvement of the CIED system by a bloodstream infection (Fig. 3.1).
Different pathogenetic mechanisms of CIED infection. (a) The infective process (in yellow) usually starts from the device pocket due to contamination, usually occurred during an intervention on the pocket (first implant, revision, generator replacement). Infection then spreads along the leads, reaching bloodstream. (b) An infection started elsewhere (from peripheral or central venous access in this example) and spreads through bloodstream; subsequently bacteria colonize the device leads (and lungs) as a metastatic infection
The pathogenesis of CIEDI consists of multiple factors, of which device-related factors are those associated with bacterial adherence to the generator or lead surfaces. Adherence is better on irregular and/or hydrophobic device surfaces. The propensity for bacterial adherence is higher for polyvinylchloride and silicone among the commonly used polymers than it is for polytetrafluoroethylene, while it is higher for polyethylene than polyurethane. Further bacterial adherence is higher for stainless steel than it is for titanium (Fig. 3.2).
While the normal endothelial lining of the heart is resistant to bacterial adhesion, bacteria (especially gram-positive species) are able to adhere to abnormal or damaged endothelium using surface adhesins, which are specialized proteins that mediate attachment to extracellular host matrix proteins. Bacterial adhesion gives rise to colonization eventually leading to formation of a mature vegetation [15]. Many of the microorganisms associated with CIEDI produce biofilms allowing bacterial populations to be encased within an extracellular polysaccharide slime-like matrix, which once established protects bacteria from host immune defences and inhibits antimicrobial efficacy [16]. Biofilm-forming capacity is an important determinant of virulence in the development of staphylococcal device-related infections [17].
Most infections are caused by bacteria from the normal skin flora of the patient. Gram-positive species are most frequent and Staphylococcus species remain the most common pathogens causing nearly 70% of CIEDI. Coagulase-negative species (37.6%) were more common than Staphylococcus aureus (30.8%) of these, while, altogether, methicillin-resistant staphylococci were isolated in 33.8% of CIEDI (49.4% of all staphylococcal infections) according to a large study of over 800 consecutive patients with confirmed CIEDI [18]. Gram-negative pathogens were identified in 8.9% of cases and 13.2% were with negative cultures. Other microbes including streptococci, enterococci, anaerobes, fungi, and mycobacteria species are rare [9, 19].
Of pocket infections, 40% of early and over 50% of late infections were related to coagulase-negative staphylococci while most endovascular infections were related to Staphylococcus aureus. The distribution of pathogens as reported from this series is shown in Table 3.1 [18]. (For additional readings on microbiology and culturing please see Chap. 2.)
3.3 Risk Factors for CIEDI
Risk stratification for device infection is important as it increases awareness and may allow for preventive measures. While some risk factors are modifiable, such as avoiding temporary pacing and delaying implantation in case of fever, some are not, such as the presence of diabetes. Although many risk factors cannot be modified, most of them can be specifically targeted for optimized therapy.
Risk factors are by tradition classified as patient-related, procedure-related, device-related factors and as environmental and organizational. Risk factors reported to contribute to the development of CIEDI include patient factors (comorbidities, medications, self-care, microbiome), procedural and device factors (pre-procedural preparations, type of device—surgery, contamination, complications, operator, and antimicrobial use), environmental and organizational factors (patient safety culture, facility barriers, quality of environmental cleaning), and microbial factors.
Most studies that have attempted to identify risk factors for CIEDI are retrospective or based on small cohort investigations and many are limited by including only few variables. There are, however, few systematic analyses of large databases and meta-analysis of available evidence on risk factors for CIEDI listed in Table 3.2.
In a large meta-analysis with data from 60 studies and over 200,000 patients, pooled to identify risk factors for CIEDI, the average device infection rate was 1–1.3% [20]. The risk factors identified in this meta-analysis are summarized in Table 3.3. Another study used an administrative claims database for privately insured and Medicare Advantage enrollees and collected data from 40,837 patients with de novo ICD or cardiac resynchronization therapy defibrillators (CRT-D) implanted from January 1, 2003, to June 30, 2015 [21]. Patients were followed for a mean 2.3 ± 2.1 years until they had the procedure or their last active date in the database. Of 20,580 device procedures, 771 (1.9%) had device-related complications [21]. The 5-year rate of freedom from an infectious complication requiring an intervention was 97.1% and 96.1% for patients with an ICD and a CRT-D, respectively. Acute infections (defined as occurring in the first 90 days after implantation) were recorded in 0.9% of patients. Another recent large study used data from 4,144,683 device-related procedures in the National Inpatient Sample database in the United States and reported 85,203 (2.06%) device-related infections (Table 3.2) [2]. The risk factors identified in these database studies are also summarized in Table 3.3. One study including patients from the Taiwan National Health Insurance Database reported that old age and high-volume centres (>200 per year) were protectors against CIEDI. The study included 40,608 patients and the risk factors identified are listed in Table 3.3.
3.3.1 Patient-Related Risk Factors
Of the patient-related risk factors for infection, end-stage renal disease and history of a previous device infection (Table 3.3) was associated with the highest risk emphasizing the importance of carefully evaluating whether CIED therapy is really indicated in these patients (Table 3.3). Even though only few studies were available to be pooled for host-related factors in a meta-analyses after exclusion of retrospective studies, diabetes mellitus, NYHA class ≥2, and pre-procedural fever remained significant predictors of infection [20]. Other strong patient-related risk factors as reported from a large database of procedures for device-related infections were haematoma (OR, 2.44; p < .001), malnutrition (OR, 2.66; p < .001), venous thromboembolism (OR, 2.37; p < .001), and organ transplantation (OR, 2.37; P < .001) as listed in Table 3.3 [2]. Even though most of the comorbidities are not modifiable per se, many of them can be subject to optimized treatment interventions, such as optimizing heart failure and diabetes, which in itself may lower the risk for device-related infections. Peri-implantation device infections were reported to be more likely in patients with atrial fibrillation, diabetes mellitus, renal disease, and CRT-D device, while those appearing as chronic infections were more likely in patients aged <65 years at implantation, male sex, diabetes mellitus, renal disease, and heart failure [21]. The strongest risk factors for CIEDI in the more recent years are conditions that compromise the patient’s immune status, including diabetes, end-stage renal disease, rheumatologic diseases (which often necessitate steroid use), and malnutrition [2]. Long-term steroid therapy suppressing immunity and delaying wound healing has been associated with device-related infections and is likely the reason why patients with chronic obstructive pulmonary disease and rheumatologic diseases, who are often on steroid therapy, have higher risk of infection, as also seen in our analysis [2, 20, 24]. Age and gender were not associated with increased risk in the meta-analysis [20] (Fig. 3.3).
Conditions with high risk of CIEDI. Results of the multivariable analysis with procedures for device-related infections from 2000 to 2006 vs. 2007 to 2012 recorded in the National Inpatient Sample (NIS) US database (Reproduced from Joy et al. [2] with permission)
3.3.2 Procedure-Related Factors
Procedure-related factors with the highest predictors of CIED infection included lack of antibiotic prophylaxis with a 70% relative risk reduction in infection [20].
The use of routine antibiotic prophylaxis at CIED implantations is largely based on a meta-analysis of randomized trials showing significantly reduced risk for pacemaker (PM)-related infections by antibiotics on short term after implant [12], later confirmed on long term by a large prospective study [5]. Other strong predictors for device infections were post-operative haematoma associated with an eightfold increased risk [20] with similar risk for all types of devices [2]. This observation was further confirmed by the randomized BRUISE-CONTROL INFECTION study, which demonstrated a strong association between clinically significant haematoma and subsequent device infection (hazard ratio for infection 7.7; 95% CI, 2.9–20.5; p < 0.0001) with as many as 11% risk of developing infection over 1-year follow-up [25]. Given this knowledge, special attention should be given on adequate haemostasis, particularly in patients with increased risk for perioperative bleeding.
Another clinically significant predictor for infection was reintervention for lead dislodgement with a sixfold and generator change with roughly a twofold risk for infection, which may be related to activation of pre-existing bacterial colonization or reduced penetration of antibiotics into the encapsulated generator pocket [20], also confirmed by others [6, 22]. This knowledge is of particular importance in the present era of frequent generator or lead recommendations and recalls and a decision to replace a device should therefore be made on a risk versus benefit ratio weighting the risk for death due to device failure, the rate of device failure, and the risk for procedure-related death.
In a recent prospective registry study CIEDI occurring after initial implantation (178 patients) had a higher Charlson comorbidity score, were more likely to have had a solid organ transplant (2.8% vs. 0%, p = 0.011), and be on immunosuppressive medications (10.1% vs. 4.3%, p = 0.03) than those occurring after reoperation (254 patients) [24]. They were also more likely to present with metastatic foci of infection (16.9% vs. 8.7%, p = 0.016) and sepsis (30.9% vs. 19.3%, p = 0.006). Pocket infections occurred more likely after a reoperation (70.1% vs. 48.9%, p < 0.001) and with coagulase-negative staphylococci as the most frequently isolated organism (p = 0.029). No differences were seen in age, sex, or device type. There were no differences in in-hospital (7.9% vs. 5.2%, p = 0.31) or 6-month mortality (21.9% vs. 14.0%, p = 0.056). Device-related infections after initial implant thus occur earlier, more aggressively, and are often due to Staphylococcus aureus, while those after reoperation have more indolent manifestations and are due to coagulase-negative staphylococci [24].
Procedure duration was also associated with multifold risk (Table 3.3), but when only studies with adequate definition were pooled, all listed procedure factors except for procedure duration were still associated with higher infection rates [20].
Temporary pacing is associated with a twofold increased risk for device infections, which may be related to deviations in managing sterility in urgent situations. Indication for temporary transvenous pacing should therefore be carefully considering alternatives such as backup transthoracic pacing or infusion of rate-accelerating drugs (Table 3.3). Inexperienced operator, in particular thoracic surgeon, is associated with an almost threefold risk for CIEDI (Table 3.3) [26].
3.3.3 Device-Related Risk Factors
Device-related factors with the highest risk for infection were abdominal pocket with a fourfold risk and CRT device with an eightfold risk (Table 3.3). Although abdominal pocket was the only remaining significant risk factor after pooling only prospective studies (Table 3.3) [20], several other studies have confirmed that CRT is a major risk factor for device-related infections [2, 21, 27,28,29].
The infection risk after pacemaker implant, 0.5–1% within the first 6–12 months [4,5,6], is reported to be higher, 1.7%, with ICDs [19, 22]; even higher in CRT recipients, 9.5% over 2 years [14]; and highest with CRT-D [29]. In a recent analysis of ICD Registry data from 2006 to 2009 matched to Medicare claims data; however, the infection rate was 1.4%, 1.5%, and 2.0% for single, dual, and biventricular ICDs, respectively (P < 0.001) [22]. A greater risk of infection with increasing number of device lead implants has also been reported by others [27, 28]. Other factors that may explain the increased risk of infection for CRT devices are more advanced procedures, reoperation for upgrade to biventricular device, and higher comorbidity burden of CRT patients. Chronic kidney disease and rheumatologic diseases were more common in CRT recipients with device infections than among other device types [2]. In a multivariable regression analysis for independent risk factors for CIEDI, CRT devices and single-chamber pacemakers had higher risk than ICDs [2]. Infections in CRT devices and single-chamber pacemakers carried a higher mortality rate, which may be related to greater severity of cardiovascular disease in CRT recipients.
3.3.4 Environmental/Organizational Risk Factors
High-volume centre was shown to decrease the infection rate if more than 200 procedures were performed annually (Table 3.3) [23].
Nasal carriers of Staphylococcus aureus are at increased risk for healthcare-associated infections with this organism [30]. Rapid identification of S. aureus nasal carriers by means of a real-time polymerase-chain-reaction (PCR) assay, followed by treatment with nasal ointment and chlorhexidine soap, reduced the risk of hospital-associated S. aureus infection to 3.4% in the mupirocin-chlorhexidine group, as compared with 7.7% in the placebo group (relative risk of infection, 0.42; 95% CI, 0.23 to 0.75) [31]. There are no reports on risk factors for device-related infections depending on minimum standards for the environment for CIED procedures such as operating room standards for sterile procedures.
3.4 Conclusions
Comparison of the comorbidities associated with greater risk for device-related infections suggests that currently the strongest risk factors are disease states that compromise the patient’s immune status including diabetes, end-stage renal disease, rheumatologic diseases, and malnutrition [2]. The greater rise in device-related infections for CRT recipients may reflect a combination of more complex procedures performed in patients with higher comorbidity burden, which is unmodifiable in the short term. Efforts should therefore be made to target risk factors that are modifiable in order to modify and reduce the risk for device-related infections and further to optimize treatment of any comorbidity that imposes increased risk for infection. Examples of risk stratification and modification are delineated in Table 3.4.
References
Greenspon AJ, Patel JD, Lau E, Ochoa JA, Frisch DR, Ho RT, et al. 16-year trends in the infection burden for pacemakers and implantable cardioverter-defibrillators in the United States: 1993 to 2008. J Am Coll Cardiol. 2011;58(10):1001–6.
Joy PS, Kumar G, Poole JE, London B, Olshansky B. Cardiac implantable electronic device infections: who is at greatest risk? Heart Rhythm. 2017;14(6):839–45.
VOIGT A, SHALABY A, SABA S. Continued rise in rates of cardiovascular implantable electronic device infections in the United States: temporal trends and causative insights. Pacing Clin Electrophysiol. 2010;33(4):414–9.
Johansen JB, Jørgensen OD, Møller M, Arnsbo P, Mortensen PT, Nielsen JC. Infection after pacemaker implantation: infection rates and risk factors associated with infection in a population-based cohort study of 46299 consecutive patients. Eur Heart J. 2011;32(8):991–8.
Klug D, Balde M, Pavin D, Hidden-Lucet F, Clementy J, Sadoul N, et al. Risk factors related to infections of implanted pacemakers and cardioverter-defibrillators. Results of a Large Prospective Study. 2007;116(12):1349–55.
Kirkfeldt RE, Johansen JB, Nohr EA, Jørgensen OD, Nielsen JC. Complications after cardiac implantable electronic device implantations: an analysis of a complete, nationwide cohort in Denmark. Eur Heart J. 2014;35(18):1186–94.
Le KY, Sohai LMR, Friedman PA, Uslan DZ, Cha SS, Hayes DL, et al. Clinical predictors of cardiovascular implantable electronic device-related infective endocarditis. Pacing Clin Electrophysiol. 2011;34(4):450–9.
Sohail MR, Henrikson CA, Braid-Forbes M, Forbes KF, Lerner DJ. Mortality and cost associated with cardiovascular implantable electronic device infections. Arch Intern Med. 2011;171(20):1821–8.
Tarakji KG, Chan EJ, Cantillon DJ, Doonan AL, Hu T, Schmitt S, et al. Cardiac implantable electronic device infections: presentation, management, and patient outcomes. Heart Rhythm. 2010;7(8):1043–7.
Habib A, Le KY, Baddour LM, Friedman PA, Hayes DL, Lohse CM, et al. Predictors of mortality in patients with cardiovascular implantable electronic device infections. Am J Cardiol. 2013;111(6):874–9.
Bongiorni MG, Marinskis G, Lip GYH, Svendsen JH, Dobreanu D, Blomström-Lundqvist C, et al. How European centres diagnose, treat, and prevent CIED infections: results of an European heart rhythm association survey. EP Europace. 2012;14(11):1666–9.
Da Costa A, Kirkorian G, Cucherat M, Delahaye F, Chevalier P, Cerisier A, et al. Antibiotic prophylaxis for permanent pacemaker implantation. A Meta-Analysis. 1998;97(18):1796–801.
de Oliveira JC, Martinelli M, Nishioka SADO, Varejão T, Uipe D, Pedrosa AAA, et al. Efficacy of antibiotic prophylaxis before the implantation of pacemakers and Cardioverter-defibrillators. Results of a large, prospective, randomized, double-blinded, placebo-controlled trial. Circ Arrhythm Electrophysiol. 2009;2(1):29–34.
Palmisano P, Accogli M, Zaccaria M, Luzzi G, Nacci F, Anaclerio M, et al. Rate, causes, and impact on patient outcome of implantable device complications requiring surgical revision: large population survey from two centres in Italy. EP Europace. 2013;15(4):531–40.
Werdan K, Dietz S, Löffler B, Niemann S, Bushnaq H, Silber R-E, et al. Mechanisms of infective endocarditis: pathogen–host interaction and risk states. Nat Rev Cardiol. 2013;11:35.
Elgharably H, Hussain ST, Shrestha NK, Blackstone EH, Pettersson GB. Current hypotheses in cardiac surgery: biofilm in infective endocarditis. Semin Thorac Cardiovasc Surg. 2016;28(1):56–9.
Chung PY, Toh YS. Anti-biofilm agents: recent breakthrough against multi-drug resistant Staphylococcus aureus. Patho Dis. 2014;70(3):231–9.
Hussein AA, Baghdy Y, Wazni OM, Brunner MP, Kabbach G, Shao M, et al. Microbiology of cardiac implantable electronic device infections. JACC Clin Electrophysiol. 2016;2(4):498–505.
Uslan DZ, Sohail MR, St. Sauver JL, et al. Permanent pacemaker and implantable cardioverter defibrillator infection: a population-based study. Arch Intern Med. 2007;167(7):669–75.
Polyzos KA, Konstantelias AA, Falagas ME. Risk factors for cardiac implantable electronic device infection: a systematic review and meta-analysis. EP Europace. 2015;17(5):767–77.
Koneru JN, Jones PW, Hammill EF, Wold N, Ellenbogen KA. Risk factors and temporal trends of complications associated with Transvenous implantable cardiac defibrillator leads. J Am Heart Assoc. 2018;7(10)
Prutkin JM, Reynolds MR, Bao H, Curtis JP, Al-Khatib SM, Aggarwal S, et al. Rates of and factors associated with infection in 200 909 Medicare implantable Cardioverter-defibrillator implants. Results From the National Cardiovascular Data Registry. 2014;130(13):1037–43.
Lin Y-S, Hung S-P, Chen P-R, Yang C-H, Wo H-T, Chang P-C, et al. Risk factors influencing complications of cardiac implantable electronic device implantation: infection, pneumothorax and heart perforation: a Nationwide population-based cohort study. Medicine. 2014;93(27):e213.
Harper MW, Uslan DZ, Greenspon AJ, Baddour LM, Carrillo RG, Danik SB, et al. Clinical presentation of CIED infection following initial implant versus reoperation for generator change or lead addition. Open Heart. 2018;5(1):e000681.
Essebag V, Verma A, Healey JS, Krahn AD, Kalfon E, Coutu B, et al. Clinically significant pocket hematoma increases long-term risk of device infection: bruise Control infection study. J Am Coll Cardiol. 2016;67(11):1300–8.
Al-Khatib SM, Greiner MA, Peterson ED, Hernandez AF, Schulman KA, Curtis LH. Patient and implanting physician factors associated with mortality and complications following implantable Cardioverter-defibrillator implantation, 2002–2005: Al-Khatib — patient and physician factors and ICD outcomes. Circ Arrhythm Electrophysiol. 2008;1(4):240–9.
Nery PB, Fernandes R, Nair GM, Sumner GL, Ribas CS, Menon SMD, et al. Device-related infection among patients with pacemakers and implantable defibrillators: incidence, risk factors, and consequences. J Cardiovasc Electrophysiol. 2010;21(7):786–90.
Mittal S, Shaw RE, Michel K, Palekar R, Arshad A, Musat D, et al. Cardiac implantable electronic device infections: incidence, risk factors, and the effect of the AigisRx antibacterial envelope. Heart Rhythm. 2014;11(4):595–601.
Romeyer-Bouchard C, Da Costa A, Dauphinot V, Messier M, Bisch L, Samuel B, et al. Prevalence and risk factors related to infections of cardiac resynchronization therapy devices†. Eur Heart J. 2010;31(2):203–10.
Muñoz P, Hortal J, Giannella M, Barrio JM, Rodríguez-Créixems M, Pérez MJ, et al. Nasal carriage of <em>S. aureus</em> increases the risk of surgical site infection after major heart surgery. J Hosp Infect. 2008;68(1):25–31.
Bode LGM, Kluytmans JAJW, Wertheim HFL, Bogaers D, Vandenbroucke-Grauls CMJE, Roosendaal R, et al. Preventing surgical-site infections in nasal carriers of Staphylococcus aureus. N Engl J Med. 2010;362(1):9–17.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Blomstrom-Lundqvist, C. (2020). The Risk Factors for Cardiac Device Infections: Patient, Physician, Device, and Procedure. In: Diemberger, I., Boriani, G. (eds) Infections of Cardiac Implantable Devices. Springer, Cham. https://doi.org/10.1007/978-3-030-46255-0_3
Download citation
DOI: https://doi.org/10.1007/978-3-030-46255-0_3
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-46254-3
Online ISBN: 978-3-030-46255-0
eBook Packages: MedicineMedicine (R0)