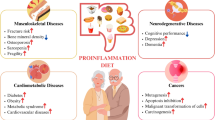
Abstract
Ageing, inflammation and diet represent three interrelated risk factors responsible for the development and worsening of a several diseases including cancer, cardiovascular diseases and metabolic disorders. Specifically, both ageing and diet are able to influence the inflammatory status of the organism through the so-called “inflamm-ageing” and “metaflammation” processes, creating a constant low-grade chronic and systemic inflammation responsible for several molecular alterations.
To establish how diet is able to promote inflammatory processes and consequently influence the development and progression of several diseases and pathophysiological conditions, including ageing and longevity, in recent years, a meter of the pro-inflammatory and anti-inflammatory power of foods, called “Dietary Inflammatory Index” (DII), has been developed.
This chapter discusses how the DII is a powerful instrument to accurately establish the relative risk of developing cardiovascular, metabolic and oncological diseases, taking into account not only the inflammatory power of foods but also the coadjuvant pathogenetic role of ageing in favouring the development of these pathologies. Furthermore, it is also emphasized how DII may influence longevity and healthy ageing.
The comprehensive analysis of the role of inflammation, diet, ageing and longevity and DII in several diseases proposed in this chapter can provide useful information to predict the risk of occurrence of specific diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
5.1 Introduction
Over the last century, several scientific findings in the epidemiological, biochemical, biological and molecular fields have allowed to identify numerous risk factors responsible for the development of various human diseases including metabolic disorders, cardiovascular diseases (CVDs), cancer and chronic degenerative diseases. Among these risk factors, a fundamental role is played by ageing, inflammation and diet, three interrelated risk factors able to modify the homeostasis of the organism leading to the onset of several age-related diseases [1, 2].
Ageing is a natural physiological process due to the loss of cell functions and tissue renewal caused by cell senescence and reduction in the number of stem cells and tissue plasticity, respectively [3, 4]. In the last decades, the increase in life expectancy has shown that ageing has led to an increase in the incidence rates of many diseases. Behind the increase in the incidence of age-related disorders, there is the loss of control mechanisms of different cellular processes including proliferation, apoptosis and senescence. In particular, ageing is characterized by the accumulation of genetic mutations mostly due to loss of DNA repair mechanisms, by the loss of telomeric sequences, by the inappropriate turnover of proteins, by epigenetic alterations (e.g. altered methylation patterns and de-regulation of microRNAs) and by mitochondrial dysfunction [5]. In addition, ageing is associated with alterations of inflammatory processes and oxidative stress that determine the increase in molecular changes [6]. In particular, the close relationship between inflammation and ageing has led the scientific community to define the inflammatory status present in the elderly with the term “inflamm-ageing” [7]. Inflamm-ageing is responsible for a constant low-grade chronic and systemic inflammation that deteriorates both cells and tissues, leading to the development of age-related pathologies including cancer, CVDs and type 2 diabetes (T2DM). All these pathologies share a common inflammatory background characterized by high levels of pro-inflammatory cytokines and mediators, such as interleukin (IL)-6 and C-reactive protein (CRP) [6].
With ageing, the metabolism of nutrients introduced with diet changes drastically. In particular, in recent decades, especially in the most developed countries, there has been a drastic increase in the number of overweight and obese people. The major increase was mainly observed in the sixth to seventh decades of life, as ageing predisposes to the accumulation of visceral fat and consequently to the increase in weight [8]. Through biochemical studies, it has been possible to establish that obesity is responsible for a mild but chronic inflammation, which represents a constant stress for the body [9].
An excess of macronutrients introduced through the diet determines an increased accumulation of body and circulating fatty acids harmful for the organism [10]. Consequently, obesity and the excess of circulating fatty acids lead to the stimulation of both macrophages and adipocytes with the triggering of different signal transduction pathways involved in the pro-inflammatory status [11]. Specifically, in obese subjects, there is an evident increase in pro-inflammatory cytokines and a reduction in adiponectin levels that lead to an increase in the production of reactive oxygen species (ROS) and a decrease in endothelial nitric oxide [11]. This chronic inflammatory status is called metaflammation, defined as “low-grade, chronic inflammation orchestrated by metabolic cells in response to excess nutrients and energy” [12, 13]. Metaflammation is not only the result of overweight and obesity, but it also depends on ageing [6]. Both metaflammation and inflamm-ageing are responsible for a bivalent cycle where the pro-inflammatory status induced by metaflammation and inflamm-ageing leads to cellular damage and senescence. On the other hand, senescent cells produce several growth factors, proteases, chemokines and pro-inflammatory cytokines that worsen the chronic inflammatory status, creating a vicious circle that, in the long period, determines the occurrence of different pathological conditions including age-related diseases [14]. In fact, the molecular pathways altered in both diet- and obesity-induced metaflammation and inflamm-ageing are signal transduction pathways whose alterations are associated with an increased risk of development of age-related diseases [15, 16].
In addition, both ageing and inflammation are sensitive to several environmental factors, among which diet represents the most powerful regulating determinant [17]. In particular, the diet, especially the individual foods that compose the diet, is able to change the body’s response to pro-inflammatory stimuli and to limit or change the ageing process [18].
For this purpose, in order to quantify the impact of specific food regimes on the inflammatory profile of the individual, a meter of the pro-inflammatory and anti-inflammatory power of foods, called “Dietary Inflammatory Index” (DII), has been developed [19].
Foods, through their inflammatory power, are able to modify cellular homeostasis and consequently different cellular processes including proliferation, apoptosis and senescence. There are numerous studies demonstrating how diet can play a fundamental role in ageing and anti-ageing, counteracting the formation of a pro-inflammatory cellular environment [20]. Indeed, whilst foods with a high inflammatory index lead to senescence and oxidative stress harmful to cells, it is true that foods with a low inflammatory index and functional foods can reduce oxidative stress thanks to antioxidants introduced with the diet, i.e. nutraceuticals (Chap. 11), which are very effective in counteracting both ageing and the onset of age-related diseases [21, 22].
More in detail, a diet characterized by foods with a high DII is responsible for the production of several cytokines able to negatively stimulate epithelial cells for the production of ROS and to induce the activation of the signalling pathway responsible for the decision of the cell fate [23, 24]. Moreover, a diet with a high DII triggers the production of multiple secreted inflammatory cytokines, their cognate receptors and positive-feedback loops with corresponding transcription factors as key mediators of cell senescence [25]. All these molecular alterations result in the accumulation of DNA damages that, in turn, induce the activation of the NF-κB signalling pathway, resulting in the cell cycle arrest and the induction of a senescent phenotype [25, 26].
In the following paragraphs, it is emphasized how the DII has allowed to accurately establish the relative risk of developing cardiovascular, metabolic and oncological diseases, taking into consideration not only the inflammatory power of food but also the pathogenetic role of ageing in favouring the development of these pathologies. It is also be analysed how dietary habits affect ageing and longevity processes of individuals and how the DII can be used as a tool to measure the anti-ageing potential of diet.
5.2 The Dietary Inflammatory Index
The DII is a literature-derived tool developed to have a comprehensive evaluation of the inflammatory potential of diet [19]. The DII has been validated in a variety of longitudinal and cross-sectional studies using various inflammatory markers including CRP, IL-6 and tumour necrosis factor-α [19, 27, 28].
Briefly, DII is based on a literature review of the association between dietary habits and inflammatory biomarkers, which identified and scored 45 foods or nutrients derived from usual diets [19, 29]. An inflammatory effect score was available for each food parameter, ranked according to inflammatory potential in anti-inflammatory (negative scores) and pro-inflammatory (positive scores) food parameters. Table 5.1 reports some examples of anti- and pro-inflammatory foods and nutrients included in the DII calculation, as originally reported by Shivappa and colleagues [19]. A person’s usual intake of each food parameter is weighted according to its inflammatory effect score and then summed to produce the overall DII. DII score increases with increasing inflammatory potential of diet, with negative values indicating anti-inflammatory diets and positive ones indicating pro-inflammatory diets.
Although originally developed to identify the inflammatory potential of diet [9, 29], the DII has the additional property to indicate a general nutritional quality of diet. Indeed, several studies reported a positive association between anti-inflammatory diets and adequate intake of nutrients. Results from the Whitehall II cohort study, a cohort study of men and women originally employed by the British civil service in London-based offices, showed that people taking anti-inflammatory diets reported higher intake of fibres, proteins and polyunsaturated fatty acids and lower intake of carbohydrates, fats and fatty acids than people with pro-inflammatory diets [30]. Similarly, in the ORISCAV-LUX cohort, a cross-sectional study on the prevalence of cardiovascular risk factors among the adult population of Luxembourg, aged 18–69 years, people taking anti-inflammatory diets reported higher intake of vitamins and minerals than those taking pro-inflammatory diets [31]. Further, an association between DII and other indicators of healthy diets has been reported [30, 32]. In particular, anti-inflammatory scores have been consistently reported in people who follow a Mediterranean Diet, whose beneficial effects on healthy ageing and longevity are discussed in Chap. 10 [33,34,35].
Bearing in mind this second DII property, it is of great interest to understand how DII varies across age groups, with a particular focus on the elderly. Figure 5.1 shows DII scores for Italian men and women enrolled in population-based studies [35].
Both genders reported anti-inflammatory diets (i.e. negative DII scores), even if DII score in men were consistently lower than that in women. The score starts increasing from the age of 55 to 59 years, with a similar trend in both men and women. Although some differences emerged across geographic areas, the rising trend with age in the elderly was consistent [35]. The increase in the inflammatory potential of diet with age could have relevant health implication: in addition to its impact on several clinical outcomes, it could indicate a general worsening of diet in the elderly. An adequate nutritional status is important to prevent frailty in this vulnerable population, thereby the DII score could be a useful tool to identify people with inadequate diet who could benefit from nutritional intervention [36].
A pro-inflammatory status has been associated with several conditions that could affect the quality of life in the elderly, including depression and osteoporosis. In the next paragraphs, we focus on the role of DII in metabolic disorders, CVDs and cancer, as well as in healthy ageing and longevity.
5.3 DII and Metabolic Disorders
The metabolic syndrome is a complex disorder defined as a cluster of at least three risk factors among abdominal obesity, glucose intolerance, high blood pressure, high triglyceride levels and low high-density lipoprotein cholesterol levels [37]. Current evidence on the association between DII and metabolic syndrome is summarized in Table 5.2.
All studies but one were conducted in middle-aged individuals, reporting inconsistent results [44]. Two cohort studies reported a mild positive association, with an increased risk of metabolic syndrome in people with pro-inflammatory diets, whereas the SUN Project (“Seguimiento Universidad de Navarra” [University of Navarra Follow-up] Project is a dynamic prospective cohort study, conducted in Spain with university graduates since December 1999) found no association [44,45,46]. However, the younger age of patients in the SUN Project could have limited the capability to detect the effect of dietary indexes on the incidence of chronic diseases that are strongly related to age. Evidence from case–control studies generally indicates the lack of any association between DII and metabolic syndrome. Only one Korean case–control study found a significant association in both women (RR = 1.67; 95% CI: 1.15–2.44) and men (RR = 1.40; 95% CI: 1.06–1.85) [47]. Further, a cross-sectional study in overweight and sedentary individuals indicates a positive association between a metabolic syndrome score and pro-inflammatory diets [48].
Hyperglycaemia plays an important role in the definition of metabolic syndrome, and it has relevant implication on individual health. Generally, pro-inflammatory diets are associated with hyperglycaemia [45,46,47, 49, 50]. In particular, in the Mexico City Diabetes Mellitus Survey, a cross-sectional probabilistic population-based survey, individuals in the highest quintile of DII have a threefold higher risk of type 2 diabetes mellitus (95% CI: 1.39–6.58) than people in the lowest DII quintile [51]; this association was much stronger among people aged ≥55 years (OR = 9.8; 95% CI: 3.8–25.5) than among younger individuals. This result is in agreement with a previous case–control study in Iran, which reported an elevated risk of prediabetes (OR = 18.9; 95% CI: 7.0–50.8) in people taking pro-inflammatory diets [52]. In addition to the possible enhancement of insulin resistance in pro-inflammatory diets, elevated DII scores could identify diets rich in foods such as refined cereals, soft drinks, and red and processed meat associated with the onset of T2DM [51].
5.4 DII and Cardiovascular Diseases
The association between DII and CVDs has been investigated in several longitudinal studies on unselected populations (Table 5.3), generally reporting a moderate association. People taking pro-inflammatory diets reported an increased risk of CVD onset ranging from 3 to 103% compared with those taking anti-inflammatory diets. A similar risk was found for CVD mortality, with excess risk among people taking pro-inflammatory diets, ranging from 9 to 102%.
A few studies were conducted in the elderly. Only one study was specifically focused on women aged 70 years or older (mean age: 75 years) who were originally enrolled in the Calcium Intake Fracture Outcome Study [40]. Although this trial failed to demonstrate an effect of calcium supplementation on carotid atherosclerosis, it provided important information of dietary habits and CVD risk. In particular, pro-inflammatory diets were associated with increased mortality for atherosclerotic vascular disease (HR = 2.02; 95% CI: 1.30–3.13), ischaemic heart disease (HR = 2.51; 95% CI: 1.37–4.62) and possibly with cerebrovascular disease (HR = 1.76; 95% confidence interval 0.92–3.40). Three other studies enrolled participants with a mean age above 60 years. The PREDIMED Study, a Spanish long-term nutritional intervention study aimed at assessing the efficacy of the Mediterranean Diet in the primary prevention of cardiovascular disease, was a randomized trial enrolling men aged 55–80 years and women aged 60–80 years [39]. After a 5-year follow-up, a significant increase in CVD risk of 73% was observed in people following pro-inflammatory diets. This effect was consistent across dietary intervention arms. Two longitudinal studies investigated CVD mortality in women. In the Iowa Women’s Health Study designed to examine the effect of host, dietary and lifestyle factors on the incidence of cancer among postmenopausal women, a moderate association emerged between CVD mortality and DII score after adjustment for potential confounders [38]. Conversely, in the participants in the population-based Swedish Mammography Cohort, the association between DII and CVD mortality was no longer significant after adjustment for overweight/obesity, tobacco smoking and alcohol drinking [53].
Studies on different cardiovascular endpoints showed a consistent result. A recent meta-analysis of case–control and cohort studies revealed an increased risk of myocardial infarction in people with pro-inflammatory diets compared with those with anti-inflammatory diets (RR = 1.43; 95% CI: 1.09–1.89) [41]. Although not significant, the relative risks in people with elevated DII were still indicative of an excess risk for ischaemic/coronary heart disease (RR = 1.18; 95% CI: 0.89–1.58) and stroke (RR = 1.10; 95% CI: 0.60–2.00).
In summary, pro-inflammatory diets are associated with CVD incidence and mortality in both adults and the elderly. Therefore, the promotion of anti-inflammatory diets rich in vegetable, fish and cereals consumption may help to reduce CVD incidence, improving healthy ageing.
5.5 DII and Cancer
Several studies have shown that besides the well-known genetic and molecular alterations responsible for neoplastic transformation, also microenvironmental perturbations of the inflammatory status may lead to the accumulation of genetic damages responsible for malignant transformation of cells and to tumour progression [42, 43, 54]. A pro-inflammatory microenvironment, characterized by high concentrations of several pro-inflammatory cytokines and other mediators, is associated with an increased risk of tumour onset due to the inflammation-induced cellular stress and damages [55, 56].
However, alongside diet, the regulation of the cancer-related inflammatory status depends on other factors including ageing and the alteration of the organism redox state [18, 57]. Therefore, it is clear how all these factors may contribute to the formation of a more predisposing pro-inflammatory microenvironment and consequently to the development of cancer.
To date, there is a well-established axis among inflammation, diet, ageing and the increased risk of cancer, although the molecular basis of this multifactorial interaction has not yet been fully elucidated [58].
In the context of the diet-related pathogenesis of cancer, both quantitative and qualitative characteristics of nutrients play key roles in the development of a pro-inflammatory carcinogenic environment [59, 60]. Diet positively and negatively influences the incidence, natural progression and therapeutic response of several cancer types through the modulation of chronic inflammation [61, 62]. In particular, epidemiological studies demonstrate that certain types of cancers are more sensitive to disequilibria in food composition, especially when this imbalance characterizes obese people [63]. To date, among the most common malignancies associated with obesity or unhealthy dietary habits, more than 13 different types of cancers including cancer of the gallbladder, kidney cancer, liver cancer, breast cancer, ovarian cancer and thyroid cancer have been recognized [64].
In addition to overweight and obesity, specific foods and nutrients are now considered as probable or certain carcinogens for humans. The latest foods included in the International Agency for Research on Cancer list as probable and certain carcinogens for humans are the red and processed meats, respectively [65]. In developed countries, the diet is generally rich in red meat, high-fat foods, refined grains and complex carbohydrates that promote a pro-inflammatory status [66].
Although in the Western Countries there is the highest percentage of overweight and obese people, in some areas, especially in those facing the Mediterranean Sea, healthy food styles are widespread, first of all being the Mediterranean diet, characterized by the consumption of high quantities of fruit, vegetables and olive oil [67]. The Mediterranean diet plays a protective role against various human diseases thanks to the various beneficial nutrients of which it is constituted [68]. One of the more important features of the Mediterranean diet is to have a low inflammatory index and antioxidant effects [33, 69]. Hence, the adoption of Mediterranean diet and healthy dietary habits may reduce the risk of cancer development and together the detrimental effects of ageing [70, 71].
Thanks to the use of the DII as a parameter for measuring the inflammatory potential of foods, several studies have been conducted to evaluate the role of pro-inflammatory diets on cancer risk. A recent meta-analysis summarized the current evidence based on case–control and cohort study [72]. Overall, a positive association between pro-inflammatory diets and overall cancer risk was found, with a RR = 1.58 (95% CI: 1.45–1.72) for the highest versus the lowest DII category. This overall risk estimate should be considered with caution, since it strongly depends on the cancer sites included in the original studies. Although a direct association emerged for all cancer sites, the risk magnitude was heterogeneous. Indeed, the pooled relative risks were 2.74 for oesophageal cancer, 1.57 for ovarian cancer, 1.45 for prostate cancer, 1.43 for colorectal cancer, 1.33 for breast cancer and 1.32 for renal cancer. The association was not significant for lung cancer (RR = 1.27; 95% CI: 0.93–1.72). Subgroup analysis by gender and ethnic group did not substantially modify study findings. A dose–response analysis generally showed a rising risk of cancer with increase DII score [72].
Considering that both DII score (Fig. 5.1) and overall cancer risk increase with age, it is compelling to understand whether their association changes according to age [73]. Using data from a series of case–control studies in Italy, Accardi et al. estimated the association between DII score and several cancer sites according to age groups [35]. The changes in DII scores according to age were similar in cancer cases and in cancer-free controls, so that the association between DII and relative risk for pro-inflammatory diets versus anti-inflammatory diets remained stable across age groups for all considered cancers. Indeed, the relative risk could be considered a magnifier of the baseline risk. Given the higher cancer incidence in the elderly, the impact of DII on absolute cancer risk was much higher among them than among middle-aged people [73]. Therefore, dietary intervention to improve healthy, anti-inflammatory diets in the elderly could help in reducing the cancer burden in this population.
Besides these epidemiological data, several animal models of cancer have also shown that the quantity of nutrients and the fasting and feeding cycles play an important role in cancer through their effects towards the immune system and the tumour microenvironment [60].
All these data suggest that dietary interventions may contribute to the regulation of both chronic low-grade metaflammation and inflamm-ageing. Therefore, diet is considered to play a key role not only in the pathogenesis and development of tumours but also as a possible therapeutic approach. This is based on the administration of specific foods or active natural compounds extracted from plants or microorganisms, i.e. nutraceuticals and probiotics, with proven antitumour activity or able to enhance the efficacy of the several pharmaceutical cancer treatments [74,75,76,77]. Finally, to date, diet is also considered a fundamental element in anticancer prevention strategies that promotes the adoption of healthy dietary lifestyles [68].
5.6 DII and Longevity
Several aspects may have an impact on healthy ageing, including good physical, cognitive and mental functioning. Therefore, conditions and lifestyle factors impacting on overall survival and on the incidence of chronic diseases and functional disabilities may be relevant.
Presently, very few studies have investigated the association between DII and healthy ageing using a multidimensional approach. Using data from the SU.VI.MAX, i.e. French Supplémentation en Vitamines et Minéraux Antioxydants study, the authors have prospectively evaluated the health status of almost 2800 participants (mean age at enrolment: 52 years) after a mean follow-up of 13.3 years [17]. Healthy ageing during follow-up was defined considering overall perceived health; physical and cognitive functioning; incidence of major chronic diseases; limitation in daily activities; depression and health-related limitations in social life. People having a pro-inflammatory diet at baseline had 15% lower probability to have healthy ageing than people with anti-inflammatory diets. Similarly, the Tsurugaya Project, a Japanese prospective study on community-dwelling older individuals aged 70 years or older (mean age: 75 years), evaluated the incidence of functional disabilities using a composite outcome. In this study, elevated DII was associated with a 25% increase in risk of developing disabilities during a maximum follow-up of 12 years [78].
Further, a Korean study on community-dwelling individuals aged 70–85 years investigated DII in relation to frailty [47]. A frailty index was calculated basing on five criteria: weight loss, exhaustion, low physical activity, low walking speed and low handgrip strength. A higher mean DII score was reported among frail individuals than among non-frail ones, with a 68% increase in the risk of frailty (95% CI: 1.25–2.17) among elderly with pro-inflammatory diets in comparison with anti-inflammatory diets. A similar association was found in a previous analysis of the Osteoarthritis Initiative [79]. In this study, frailty was defined according to the presence of at least two out of three of the following conditions: (1) weight loss ≥5%; (2) inability to carry out chair stand and (3) poor strength. During an 8-year follow-up, the incidence of frailty was higher in people taking pro-inflammatory diets than in those taking anti-inflammatory diets (HR = 1.37; 95% CI: 1.01–1.89).
Dietary habits may affect longevity through the modification of telomere length, which is considered a proxy of biological cell ageing [80] (Chap. 8). Chronic inflammation is a mechanism involved in telomere shortening; therefore, anti-inflammatory diets may contribute in slowing down biological ageing [81].
The association between leukocyte telomere length and inflammatory potential of diet was first investigated in the PREDIMED-NAVARRA, that is, in a subset of participants from the PREDIMED study recruited at NAVARRA centre [82]. The authors assessed the dietary inflammatory potential in 520 patients at high risk for CVD who underwent a nutritional intervention based on the Mediterranean diet. At study enrolment, the DII score was inversely associated with leukocyte telomere length at baseline, with an 80% higher risk of shorter telomere (95% CI: 1.03–3.17) in pro-inflammatory than in anti-inflammatory diets. More interestingly, pro-inflammatory diets were also inversely associated with telomere shortening rate after 5 years of follow-up: participants who had the greatest increase in DII had almost a twofold higher risk (OR = 1.94; 95% CI: 1.10–3.43) to have the highest telomere shortening rate.
These results should be considered with caution; although consistent with a beneficial effect of anti-inflammatory diets in slowing down telomere shortening, potential selection bias may limit their validity. Indeed, the PREDIMED-NAVARRA study was based on a population with several comorbidities (i.e., diabetes, overweight/obesity, hypertension and current smoking), which may confound the reported association between DII and telomere length. Although no interaction was found, there was a tendency for individuals with overweight/obesity or hypertension to have shorter telomeres [82].
A subsequent analysis of data from the NHANES study, a programme designed to assess the health and nutritional status of children and adults in the United States, confirmed an inverse association between DII and telomere length, with shorter leukocyte telomeres in people with the most pro-inflammatory DII scores [83]. This analysis was conducted on a probabilistic sample of US general population of over 7000 individuals aged 18 years or older. Conversely, no such association was found in middle-aged Asklepios population, i.e. a community situated on both sides of the busy motorway from Brussels to Ghent, with divergent effects in men and women [84].
People adherent to Mediterranean diet reported anti-inflammatory scores [34, 35]; therefore, an indirect support to the association between pro-inflammatory diets and telomere shortening may derive from study on Mediterranean diet. Although presently scarce, the current evidence confirms an inverse association between telomere length and adherence to the Mediterranean diet [85]. This association was not evident for any single Mediterranean diet food, suggesting that the dietary Mediterranean pattern, rather than single foods or nutrients, may be responsible for the beneficial effect on telomere shortening. An Italian study on Caucasian elderly reported a similar association between adherence to Mediterranean diet and telomere length in people over 70 years of age [86].
Finally, in two large prospective Spanish cohorts, the SUN [87] and PREDIMED studies [39], a high inflammatory diet, as measured by the DII, was associated with higher all-cause mortality. A diet rich in vegetables, fruits, fish, nuts and legumes and low in meats, dairy and baked goods, that is, a higher anti-inflammatory DII, is therefore likely to reduce many potential causes of premature death, potentially favouring the attainment of longevity [88].
5.7 Conclusion
The complexity of the ageing and longevity phenomena and their regulatory elements is progressively being revealed thanks to the multidisciplinary studies carried out in recent years in this field. The predominant role of inflammation in these physiological processes has made possible to understand how the accurate regulation of the inflammatory status is responsible for the development of different pathological processes, shifting the interest of researchers on the factors able to change inflammatory status. As described in this chapter, several studies have shown that diet is one of the most effective regulators of inflammatory processes by identifying specific pro-inflammatory and anti-inflammatory dietary habits associated with different pathologies or their treatment. An important turning point in the study of diet-associated diseases was the definition of the DII, which allows to quantify the pro- or anti-inflammatory power of a specific food. After the introduction of the DII, it is possible to identify dietary regimens associated with an increased risk of metabolic disorders, CVDs and cancer and reciprocally healthy ageing and longevity. It is becoming clear that the comprehensive study of inflammation, diet, ageing and longevity and the understanding of the relationships between these four elements can provide useful information to predict the risk of occurrence of specific diseases. This will be helpful to develop a new preventive and therapeutic approach based on the modulation of diet, thereby enhancing the possibility to achieve healthy ageing and longevity.
References
Leon BM, Maddox TM. Diabetes and cardiovascular disease: epidemiology, biological mechanisms, treatment recommendations and future research. World J Diabetes. 2015;6(13):1246–58.
Koene RJ, Prizment AE, Blaes A, Konety SH. Shared risk factors in cardiovascular disease and cancer. Circulation. 2016;133(11):1104–14.
Rose MR, Flatt T, Graves JL, Greer LF, Martinez DE, Matos M, et al. What is aging? Front Genet. 2012;3:134.
Ahmed AS, Sheng MH, Wasnik S, Baylink DJ, Lau KW. Effect of aging on stem cells. World J Exp Med. 2017;7(1):1–10.
López-Otín C, Blasco MA, Partridge L, Serrano M, Kroemer G. The hallmarks of aging. Cell. 2013;153(6):1194–217.
Leonardi GC, Accardi G, Monastero R, Nicoletti F, Libra M. Ageing: from inflammation to cancer. Immun Ageing. 2018;15:1.
Accardi G, Caruso C. Immune-inflammatory responses in the elderly: an update. Immun Ageing. 2018;15:11.
Hunter GR, Gower BA, Kane BL. Age related shift in visceral fat. Int J Body Compos Res. 2010;8(3):103–8.
Deng T, Lyon CJ, Bergin S, Caligiuri MA, Hsueh WA. Obesity, inflammation, and cancer. Annu Rev Pathol. 2016;11:421–49.
Suiter C, Singha SK, Khalili R, Shariat-Madar Z. Free fatty acids: circulating contributors of metabolic syndrome. Cardiovasc Hematol Agents Med Chem. 2018;16(1):20–34.
Ellulu MS, Patimah I, Khaza’ai H, Rahmat A, Abed Y. Obesity and inflammation: the linking mechanism and the complications. Arch Med Sci. 2017;13(4):851–63.
Forsythe LK, Wallace JM, Livingstone MB. Obesity and inflammation: the effects of weight loss. Nutr Res Rev. 2008;21(2):117–33.
Gregor MF, Hotamisligil GS. Inflammatory mechanisms in obesity. Annu Rev Immunol. 2011;29:415–45.
Xia S, Zhang X, Zheng S, Khanabdali R, Kalionis B, Wu J, et al. An update on inflamm-aging: mechanisms, prevention, and treatment. J Immunol Res. 2016;2016:8426874.
Frasca D, Blomberg BB, Paganelli R. Aging, obesity, and inflammatory age-related diseases. Front Immunol. 2017;8:1745.
Bottazzi B, Riboli E, Mantovani A. Aging, inflammation and cancer. Semin Immunol. 2018;40:74–82.
Assmann KE, Adjibade M, Shivappa N, Hébert JR, Wirth MD, Touvier M, et al. The inflammatory potential of diet at midlife is associated with later healthy aging in French adults. J Nutr. 2018;148(3):437–44.
Minihane AM, Vinoy S, Russell WR, Baka A, Roche HM, Tuohy KM, et al. Low-grade inflammation, diet composition and health: current research evidence and its translation. Br J Nutr. 2015;114(7):999–1012.
Shivappa N, Steck SE, Hurley TG, Hussey JR, Hebert JR. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17(8):1689–96.
Cătană CS, Atanasov AG, Berindan-Neagoe I. Natural products with anti-aging potential: affected targets and molecular mechanisms. Biotechnol Adv. 2018;36(6):1649–56.
Muñoz A, Costa M. Nutritionally mediated oxidative stress and inflammation. Oxid Med Cell Longev. 2013;2013:610950.
Tan BL, Norhaizan ME, Liew WP. Nutrients and oxidative stress: friend or foe? Oxid Med Cell Longev. 2018;2018:9719584.
Zhang X, Li J, Sejas DP, Pang Q. The ATM/p53/p21 pathway influences cell fate decision between apoptosis and senescence in reoxygenated hematopoietic progenitor cells. J Biol Chem. 2005;280(20):19635–40.
Sasaki M, Ikeda H, Sato Y, Nakanuma Y. Proinflammatory cytokine-induced cellular senescence of biliary epithelial cells is mediated via oxidative stress and activation of ATM pathway: a culture study. Free Radic Res. 2008;42(7):625–32.
Bartek J, Hodny Z, Lukas J. Cytokine loops driving senescence. Nat Cell Biol. 2008;10(8):887–9.
Soria-Valles C, López-Soto A, Osorio FG, López-Otín C. Immune and inflammatory responses to DNA damage in cancer and aging. Mech Ageing Dev. 2017;165(Pt A):10–6.
Shivappa N, Hebert JR, Rietzschel ER, De Buyzere ML, Langlois M, Debruyne E, et al. Associations between dietary inflammatory index and inflammatory markers in the Asklepios study. Br J Nutr. 2015;113(4):665–71.
Tabung FK, Steck SE, Zhang J, Ma Y, Liese AD, Agalliu I, et al. Construct validation of the dietary inflammatory index among postmenopausal women. Ann Epidemiol. 2015;25(6):398–405.
Shivappa N, Hebert JR, Marcos A, Diaz LE, Gomez S, Nova E, et al. Association between dietary inflammatory index and inflammatory markers in the HELENA study. Mol Nutr Food Res. 2017;61(6):1600707.
Shivappa N, Hebert JR, Kivimaki M, Akbaraly T. Alternate healthy eating index 2010, dietary inflammatory index and risk of mortality: results from the Whitehall II cohort study and meta-analysis of previous dietary inflammatory index and mortality studies. Br J Nutr. 2017;118(3):210–21.
Alkerwi A, Vernier C, Crichton GE, Sauvageot N, Shivappa N, Hébert JR. Cross-comparison of diet quality indices for predicting chronic disease risk: findings from the observation of cardiovascular risk factors in Luxembourg (ORISCAV-LUX) study. Br J Nutr. 2015;113(2):259–69.
Wirth MD, Hébert JR, Shivappa N, Hand GA, Hurley TG, Drenowatz C, et al. Anti-inflammatory dietary inflammatory index scores are associated with healthier scores on other dietary indices. Nutr Res. 2016;36(3):214–9.
Billingsley HE, Carbone S. The antioxidant potential of the Mediterranean diet in patients at high cardiovascular risk: an in-depth review of the PREDIMED. Nutr Diabetes. 2018;8(1):13.
Hodge AM, Bassett JK, Dugué PA, Shivappa N, Hébert JR, Milne RL, et al. Dietary inflammatory index or Mediterranean diet score as risk factors for total and cardiovascular mortality. Nutr Metab Cardiovasc Dis. 2018;28(5):461–9.
Accardi G, Shivappa N, Di Maso M, Hébert JR, Fratino L, Montella M, et al. Dietary inflammatory index and cancer risk in elderly: a pooled-analysis of Italian case-control studies. Nutrition. 2019;63–64:205–10.
Hernández Morante JJ, Martínez CG, Morillas-Ruiz JM. Dietary factors associated with frailty in old adults: a review of nutritional interventions to prevent frailty development. Nutrients. 2019;11(1):E102.
Kassi E, Pervanidou P, Kaltsas G, Chrousos G. Metabolic syndrome: definition and controversies. BMC Med. 2011;9:48.
Shivappa N, Blair CK, Prizment AE, Jacobs DR Jr, Steck SE, Hébert JR. Association between inflammatory potential of diet and mortality in the Iowa Women’s health study. Eur J Nutr. 2016;55(4):1491–502.
Garcia-Arellano A, Ramallal R, Ruiz-Canela M, Salas-Salvadó J, Corella D, Shivappa N, et al. Dietary inflammatory index and incidence of cardiovascular disease in the PREDIMED study. Nutrients. 2015;7(6):4124–38.
Bondonno NP, Lewis JR, Blekkenhorst LC, Shivappa N, Woodman RJ, Bondonno CP, et al. Dietary inflammatory index in relation to sub-clinical atherosclerosis and atherosclerotic vascular disease mortality in older women. Br J Nutr. 2017;117(11):1577–86.
Shivappa N, Godos J, Hébert JR, Wirth MD, Piuri G, Speciani AF, et al. Dietary inflammatory index and cardiovascular risk and mortality—a meta-analysis. Nutrients. 2018;10(2):E200.
Kawanishi S, Ohnishi S, Ma N, Hiraku Y, Murata M. Crosstalk between DNA damage and inflammation in the multiple steps of carcinogenesis. Int J Mol Sci. 2017;18(8):E1808.
Sui X, Lei L, Chen L, Xie T, Li X. Inflammatory microenvironment in the initiation and progression of bladder cancer. Oncotarget. 2017;8(54):93279–94.
Pimenta AM, Toledo E, Rodriguez-Diez MC, Gea A, Lopez-Iracheta R, Shivappa N, et al. Dietary indexes, food patterns and incidence of metabolic syndrome in a Mediterranean cohort: the SUN project. Clin Nutr. 2015;34(3):508–14.
Neufcourt L, Assmann KE, Fezeu LK, Touvier M, Graffouillère L, Shivappa N, et al. Prospective association between the dietary inflammatory index and metabolic syndrome: findings from the SU.VI.MAX study. Nutr Metab Cardiovasc Dis. 2015;25(11):988–96.
Mazidi M, Shivappa N, Wirth MD, Hebert JR, Mikhailidis DP, Kengne AP, et al. Dietary inflammatory index and cardiometabolic risk in US adults. Atherosclerosis. 2018;276:23–7.
Kim HY, Lee J, Kim J. Association between dietary inflammatory index and metabolic syndrome in the general Korean population. Nutrients. 2018;10(5):E648.
Camargo-Ramos CM, Correa-Bautista JE, Correa-Rodríguez M, Ramírez-Vélez R. Dietary inflammatory index and cardiometabolic risk parameters in overweight and sedentary subjects. Int J Environ Res Public Health. 2017;14(10):E1104.
Ren Z, Zhao A, Wang Y, Meng L, Szeto IMY, Li T, et al. Association between dietary inflammatory index, C-reactive protein and metabolic syndrome: a cross-sectional study. Nutrients. 2018;10(7):E831.
Sokol A, Wirth MD, Manczuk M, Shivappa N, Zatonska K, Hurley TG, et al. Association between the dietary inflammatory index, waist-to-hip ratio and metabolic syndrome. Nutr Res. 2016;36(11):1298–303.
Denova-Gutiérrez E, Muñoz-Aguirre P, Shivappa N, Hébert JR, Tolentino-Mayo L, Batis C, et al. Dietary inflammatory index and type 2 diabetes mellitus in adults: the diabetes mellitus survey of Mexico City. Nutrients. 2018;10(4):382.
Vahid F, Shivappa N, Karamati M, Naeini AJ, Hébert JR, Davoodi SH. Association between dietary inflammatory index (DII) and risk of prediabetes: a case-control study. Appl Physiol Nutr Metab. 2017;42(4):399–402.
Shivappa N, Harris H, Wolk A, Héberty JR. Association between inflammatory potential of diet and mortality among women in the Swedish mammography cohort. Eur J Nutr. 2016;55(5):1891–900.
Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008;454(7203):436–44. https://doi.org/10.1038/nature07205.
Multhoff G, Molls M, Radons J. Chronic inflammation in cancer development. Front Immunol. 2011;2:98.
Landskron G, De la Fuente M, Thuwajit P, Thuwajit C, Hermoso MA. Chronic inflammation and cytokines in the tumor microenvironment. J Immunol Res. 2014;2014:149185.
Zinger A, Cho WC, Ben-Yehuda A. Cancer and aging—the inflammatory connection. Aging Dis. 2017;8(5):611–27.
Sapienza C, Issa JP. Diet, nutrition, and cancer epigenetics. Annu Rev Nutr. 2016;36:665–81.
Mierke CT. The fundamental role of mechanical properties in the progression of cancer disease and inflammation. Rep Prog Phys. 2014;77(7):076602.
Zitvogel L, Pietrocola F, Kroemer G. Nutrition, inflammation and cancer. Nat Immunol. 2017;18(8):843–50.
Thomas F, Rome S, Mery F, Dawson E, Montagne J, Biro PA, et al. Changes in diet associated with cancer: an evolutionary perspective. Evol Appl. 2017;10(7):651–7.
Soldati L, Di Renzo L, Jirillo E, Ascierto PA, Marincola FM, De Lorenzo A. The influence of diet on anti-cancer immune responsiveness. J Transl Med. 2018;16(1):75.
Mazzarella L. Why does obesity promote cancer? Epidemiology, biology, and open questions. Ecancermedicalscience. 2015;9:554.
Hooper L, Anderson AS, Birch J, Forster AS, Rosenberg G, Bauld L, et al. Public awareness and healthcare professional advice for obesity as a risk factor for cancer in the UK: a cross-sectional survey. J Public Health. 2018;40(4):797–805.
IARC Working Group on the Evaluation of Carcinogenic Risk to Humans. Red meat and processed meat. Lyon: International Agency for Research on Cancer; 2018.
Smidowicz A, Regula J. Effect of nutritional status and dietary patterns on human serum C-reactive protein and interleukin-6 concentrations. Adv Nutr. 2015;6(6):738–47.
Vasto S, Buscemi S, Barera A, Di Carlo M, Accardi G, Caruso C. Mediterranean diet and healthy ageing: a Sicilian perspective. Gerontology. 2014;60(6):508–18.
Romagnolo DF, Selmin OI. Mediterranean diet and prevention of chronic diseases. Nutr Today. 2017;52(5):208–22.
Casas R, Sacanella E, Estruch R. The immune protective effect of the Mediterranean diet against chronic low-grade inflammatory diseases. Endocr Metab Immune Disord Drug Targets. 2014;14(4):245–54.
Martucci M, Ostan R, Biondi F, Bellavista E, Fabbri C, Bertarelli C, et al. Mediterranean diet and inflammaging within the hormesis paradigm. Nutr Rev. 2017;75(6):442–55.
Schwingshackl L, Schwedhelm C, Galbete C, Hoffmann G. Adherence to Mediterranean diet and risk of cancer: an updated systematic review and meta-analysis. Nutrients. 2017;9(10):E1063.
Li D, Hao X, Li J, Wu Z, Chen S, Lin J, et al. Dose-response relation between inflammatory index and human cancer risk: evidence from 44 epidemiological studies involving 1,082,092 participants. Am J Clin Nutr. 2018;107(3):371–88.
Bray F, Colombet M, Mery L, Piñeros M, Znaor A, Zanetti R and Ferlay J. editors. Cancer incidence in five continents, Vol. XI (electronic version). Lyon: International Agency for Research on Cancer; 2017. http://ci5.iarc.fr. Accessed 14 Jan 2019.
Banna GL, Torino F, Marletta F, Santagati M, Salemi R, Cannarozzo E, et al. Lactobacillus rhamnosus GG: an overview to explore the rationale of its use in cancer. Front Pharmacol. 2017;8:603.
Hamzehzadeh L, Atkin SL, Majeed M, Butler AE, Sahebkar A. The versatile role of curcumin in cancer prevention and treatment: a focus on PI3K/AKT pathway. J Cell Physiol. 2018;233(10):6530–7.
Vivarelli S, Salemi R, Candido S, Falzone L, Santagati M, Stefani S, et al. Gut microbiota and cancer: from pathogenesis to therapy. Cancers (Basel). 2019;11(1). pii: E38.
Falzone L, Salomone S, Libra M. Evolution of cancer pharmacological treatments at the turn of the third millennium. Front Pharmacol. 2018;9:1300.
Tomata Y, Shivappa N, Zhang S, Nurrika D, Tanji F, Sugawara Y, et al. Dietary inflammatory index and disability-free survival in community-dwelling older adults. Nutrients. 2018;10(12):E1896.
Shivappa N, Stubbs B, Hébert JR, Cesari M, Schofield P, Soysal P, et al. The relationship between the dietary inflammatory index and incident frailty: a longitudinal cohort study. J Am Med Dir Assoc. 2018;19(1):77–82.
Müezzinler A, Zaineddin AK, Brenner H. A systematic review of leukocyte telomere length and age in adults. Ageing Res Rev. 2013;12(2):509–19.
Wong JY, De Vivo I, Lin X, Fang SC, Christiani DC. The relationship between inflammatory biomarkers and telomere length in an occupational prospective cohort study. PLoS One. 2014;9(1):e87348.
García-Calzón S, Zalba G, Ruiz-Canela M, Shivappa N, Hébert JR, Martínez JA, et al. Dietary inflammatory index and telomere length in subjects with a high cardiovascular disease risk from the PREDIMED-NAVARRA study: cross-sectional and longitudinal analyses over 5 y. Am J Clin Nutr. 2015;102(4):897–904.
Shivappa N, Wirth MD, Hurley TG, Hébert JR. Association between the dietary inflammatory index (DII) and telomere length and C-reactive protein from the National Health and Nutrition Examination Survey-1999-2002. Mol Nutr Food Res. 2017;61(4):1600630.
De Meyer T, Bekaert S, De Buyzere ML, De Bacquer DD, Langlois MR, Shivappa N, et al. Leukocyte telomere length and diet in the apparently healthy, middle-aged Asklepios population. Sci Rep. 2018;8(1):6540.
Freitas-Simoes TM, Ros E, Sala-Vila A. Nutrients, foods, dietary patterns and telomere length: update of epidemiological studies and randomized trials. Metabolism. 2016;65(4):406–15.
Boccardi V, Esposito A, Rizzo MR, Marfella R, Barbieri M, Paolisso G. Mediterranean diet, telomere maintenance and health status among elderly. PLoS One. 2013;8(4):e62781.
Ramallal R, Toledo E, Martínez-González MA, Hernández-Hernández A, García-Arellano A, et al. Dietary inflammatory index and incidence of cardiovascular disease in the SUN cohort. PLoS One. 2015;10(9):e0135221.
Garcia-Arellano A, Martínez-González MA, Ramallal R, Salas-Salvadó J, Hébert JR, Corella D, eSUN and PREDIMED Study Investigators. Dietary inflammatory index and all-causemortality in large cohorts: the SUN and PREDIMED studies. Clin Nutr. 2019;38(3):1221–31.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Falzone, L., Libra, M., Polesel, J. (2019). Dietary Inflammatory Index in Ageing and Longevity. In: Caruso, C. (eds) Centenarians. Springer, Cham. https://doi.org/10.1007/978-3-030-20762-5_5
Download citation
DOI: https://doi.org/10.1007/978-3-030-20762-5_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-20761-8
Online ISBN: 978-3-030-20762-5
eBook Packages: MedicineMedicine (R0)