Abstract
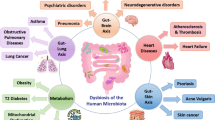
Microbes living in and on us have been recognized in the last decade as important part of ourselves and have been assigned a status of an organ with a wide range of functions—from metabolizing food to training our immune system. The intraindividual and interindividual variation of normal microbiota is vast and its composition is influenced by various external factors—most notable being diet, antibiotics and medication. External factors can cause a disturbance in microbiota frequently termed as dysbiosis which is often associated with a range of diseases—from inflammatory bowel disease and diabetes to obesity and cancer. Pioneering works in manipulating the microbiota for preventing and treating disease shows huge promise but also open a number of questions—from standardization and safety to personalization and reproducibility.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Notes
- 1.
Sender et al. (2016).
- 2.
Qin et al. (2010).
- 3.
Grice and Segre (2012).
- 4.
Turnbaugh et al. (2007).
- 5.
Arumugam et al. (2011).
- 6.
Knights et al. (2014).
- 7.
- 8.
DeGruttola et al. (2016).
- 9.
Aagaard et al. (2014).
- 10.
Dominguez-Bello et al. (2010).
- 11.
Lozupone et al. (2012).
- 12.
Koenig et al. (2011).
- 13.
De Filippo et al. (2010).
- 14.
Eckburg et al. (2005).
- 15.
Falony et al. (2016).
- 16.
David et al. (2014).
- 17.
Yatsunenko et al. (2012).
- 18.
Lin et al. (2013).
- 19.
Ou et al. (2013).
- 20.
Schnorr et al. (2014).
- 21.
Becattini et al. (2016).
- 22.
Jernberg et al. (2010).
- 23.
Risnes et al. (2011).
- 24.
Conlon and Bird (2015).
- 25.
Voreades et al. (2014).
- 26.
Morton et al. (2015).
- 27.
Martinez et al. (2015).
- 28.
Spor et al. (2011).
- 29.
Blekhman et al. (2015).
- 30.
Goodrich et al. (2016).
- 31.
Shanahan and Bernstein (2009).
- 32.
Marchesi et al. (2015).
- 33.
Hansen et al. (2012).
- 34.
Lupp et al. (2007).
- 35.
Turnbaugh et al. (2006).
- 36.
Ley et al. (2005).
- 37.
- 38.
Turnbaugh et al. (2008).
- 39.
Ridaura et al. (2013).
- 40.
Qin et al. (2012).
- 41.
Karlsson et al. (2013).
- 42.
Schulz et al. (2014).
- 43.
Sears and Pardoll (2011).
- 44.
Tjalsma et al. (2012).
- 45.
Warren et al. (2013).
- 46.
O’Keefe et al. (2015).
- 47.
Scott et al. (2015).
- 48.
Scott et al. (2014).
- 49.
Sokol et al. (2008).
- 50.
Sokol et al. (2009).
- 51.
Ramirez-Farias et al. (2009).
- 52.
Andrews and Tan (2012).
- 53.
Kruis et al. (2004).
- 54.
Hsiao et al. (2013).
- 55.
Engelbrektson et al. (2009).
- 56.
Zhang et al. (2015).
- 57.
Sanchez et al. (2014).
- 58.
Zhang et al. (2012).
- 59.
Borody et al. (2004).
- 60.
Drekonja et al. (2015).
- 61.
Choi and Cho (2016).
- 62.
- 63.
Brandt and Aroniadis (2013).
- 64.
Alang and Kelly (2015).
- 65.
Kazerouni et al. (2015).
- 66.
Li et al. (2016b).
- 67.
Kang et al. (2013).
- 68.
Li et al. (2016a).
References
Aagaard K, Ma J, Antony KM, Ganu R, Petrosino J, Versalovic J (2014) The placenta harbors a unique microbiome. Sci Transl Med 6(237):237ra65. https://doi.org/10.1126/scitranslmed.3008599
Alang N, Kelly CR (2015) Weight gain after fecal microbiota transplantation. Open Forum Infect Dis 2(1):ofv004. https://doi.org/10.1093/ofid/ofv004
Andrews JM, Tan M (2012) Probiotics in luminal gastroenterology: the current state of play. Intern Med J 42(12):1287–1291. https://doi.org/10.1111/imj.12015
Arumugam M, Raes J, Pelletier E, Le Paslier D, Yamada T, Mende DR et al (2011) Enterotypes of the human gut microbiome. Nature 473(7346):174–180. https://doi.org/10.1038/nature09944
Bakken JS, Borody T, Brandt LJ, Brill JV, Demarco DC, Franzos MA et al (2011) Treating Clostridium difficile infection with fecal microbiota transplantation. Clin Gastroenterol Hepatol 9(12):1044–1049. https://doi.org/10.1016/j.cgh.2011.08.014
Becattini S, Taur Y, Pamer EG (2016) Antibiotic-induced changes in the intestinal microbiota and disease. Trends Mol Med 22(6):458–478. https://doi.org/10.1016/j.molmed.2016.04.003
Bien J, Palagani V, Bozko P (2013) The intestinal microbiota dysbiosis and Clostridium difficile infection: is there a relationship with inflammatory bowel disease? Ther Adv Gastroenterol 6(1):53–68. https://doi.org/10.1177/1756283X12454590
Blekhman R, Goodrich JK, Huang K, Sun Q, Bukowski R, Bell JT et al (2015) Host genetic variation impacts microbiome composition across human body sites. Genome Biol 16(1):191. https://doi.org/10.1186/s13059-015-0759-1
Borody TJ, Warren EF, Leis SM, Surace R, Ashman O, Siarakas S (2004) Bacteriotherapy using fecal flora: toying with human motions. J Clin Gastroenterol 38(6):475–483
Brandt LJ, Aroniadis OC (2013) An overview of fecal microbiota transplantation: techniques, indications, and outcomes. Gastrointest Endosc 78(2):240–249. https://doi.org/10.1016/j.gie.2013.03.1329
Choi HH, Cho Y-S (2016) Fecal microbiota transplantation: current applications, effectiveness, and future perspectives. Clin Endosc 49(3):257–265. https://doi.org/10.5946/ce.2015.117
Conlon MA, Bird AR (2015) The impact of diet and lifestyle on gut microbiota and human health. Nutrients 7(1):17–44. https://doi.org/10.3390/nu7010017
David LA, Maurice CF, Carmody RN, Gootenberg DB, Button JE, Wolfe BE et al (2014) Diet rapidly and reproducibly alters the human gut microbiome. Nature 505(7484):559–563. https://doi.org/10.1038/nature12820
De Filippo C, Cavalieri D, Di Paola M, Ramazzotti M, Poullet JB, Massart S et al (2010) Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. Proc Natl Acad Sci U S A 107(33):14691–14696. https://doi.org/10.1073/pnas.1005963107
DeGruttola AK, Low D, Mizoguchi A, Mizoguchi E (2016) Current understanding of dysbiosis in disease in human and animal models. Inflamm Bowel Dis 22(5):1137–1150. https://doi.org/10.1097/MIB.0000000000000750
Dominguez-Bello MG, Costello EK, Contreras M, Magris M, Hidalgo G, Fierer N, Knight R (2010) Delivery mode shapes the acquisition and structure of the initial microbiota across multiple body habitats in newborns. Proc Natl Acad Sci U S A 107(26):11971–11975. https://doi.org/10.1073/pnas.1002601107
Drekonja D, Reich J, Gezahegn S, Greer N, Shaukat A, MacDonald R, Rutks I, Wilt TJ (2015) Fecal Microbiota Transplantation for Clostridium difficile Infection: A Systematic Review. Ann Intern Med 162(9):630–638. https://doi.org/10.7326/M14-2693
Duncan SH, Lobley GE, Holtrop G, Ince J, Johnstone AM, Louis P, Flint HJ (2008) Human colonic microbiota associated with diet, obesity and weight loss. Int J Obes (Lond) 32(11):1720–1724. https://doi.org/10.1038/ijo.2008.155
Eckburg PB, Bik EM, Bernstein CN, Purdom E, Dethlefsen L, Sargent M et al (2005) Diversity of the human intestinal microbial flora. Science (New York, NY) 308(5728):1635–1638. https://doi.org/10.1126/science.1110591
Engelbrektson A, Korzenik JR, Pittler A, Sanders ME, Klaenhammer TR, Leyer G, Kitts CL (2009) Probiotics to minimize the disruption of faecal microbiota in healthy subjects undergoing antibiotic therapy. J Med Microbiol 58(Pt 5):663–670. https://doi.org/10.1099/jmm.0.47615-0
Falony G, Joossens M, Vieira-Silva S, Wang J, Darzi Y, Faust K et al (2016) Population-level analysis of gut microbiome variation. Science (New York, NY) 352(6285):560–564. https://doi.org/10.1126/science.aad3503
Goodrich JK, Davenport ER, Waters JL, Clark AG, Ley RE (2016) Cross-species comparisons of host genetic associations with the microbiome. Science (New York, NY) 352(6285):532–535. https://doi.org/10.1126/science.aad9379
Grice EA, Segre JA (2012) The human microbiome: our second genome. Annu Rev Genomics Hum Genet 13:151–170. https://doi.org/10.1146/annurev-genom-090711-163814
Hansen R, Russell RK, Reiff C, Louis P, McIntosh F, Berry SH et al (2012) Microbiota of de-novo pediatric IBD: increased Faecalibacterium prausnitzii and reduced bacterial diversity in Crohn’s but not in ulcerative colitis. Am J Gastroenterol 107(12):1913–1922. https://doi.org/10.1038/ajg.2012.335
Hsiao EY, McBride SW, Hsien S, Sharon G, Hyde ER, McCue T et al (2013) Microbiota modulate behavioral and physiological abnormalities associated with neurodevelopmental disorders. Cell 155(7):1451–1463. https://doi.org/10.1016/j.cell.2013.11.024
Jernberg C, Lofmark S, Edlund C, Jansson JK (2010) Long-term impacts of antibiotic exposure on the human intestinal microbiota. Microbiology (Reading, England) 156(Pt 11):3216–3223. https://doi.org/10.1099/mic.0.040618-0
Kang MJ, Kim HG, Kim JS, Oh DG, Um YJ, Seo CS et al (2013) The effect of gut microbiota on drug metabolism. Expert Opin Drug Metab Toxicol 9(10):1295–1308. https://doi.org/10.1517/17425255.2013.807798
Karlsson FH, Tremaroli V, Nookaew I, Bergstrom G, Behre CJ, Fagerberg B et al (2013) Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature 498(7452):99–103. https://doi.org/10.1038/nature12198
Kazerouni A, Burgess J, Burns LJ, Wein LM (2015) Optimal screening and donor management in a public stool bank. Microbiome 3:75. https://doi.org/10.1186/s40168-015-0140-3
Knights D, Lassen KG, Xavier RJ (2013) Advances in inflammatory bowel disease pathogenesis: linking host genetics and the microbiome. Gut 62(10):1505–1510. https://doi.org/10.1136/gutjnl-2012-303954
Knights D, Ward TL, McKinlay CE, Miller H, Gonzalez A, McDonald D, Knight R (2014) Rethinking “enterotypes”. Cell Host Microbe 16(4):433–437. https://doi.org/10.1016/j.chom.2014.09.013
Koenig JE, Spor A, Scalfone N, Fricker AD, Stombaugh J, Knight R et al (2011) Succession of microbial consortia in the developing infant gut microbiome. Proc Natl Acad Sci U S A 108(Suppl 1):4578–4585. https://doi.org/10.1073/pnas.1000081107
Kruis W, Fric P, Pokrotnieks J, Lukas M, Fixa B, Kascak M et al (2004) Maintaining remission of ulcerative colitis with the probiotic Escherichia coli Nissle 1917 is as effective as with standard mesalazine. Gut 53(11):1617–1623. https://doi.org/10.1136/gut.2003.037747
Ley RE, Backhed F, Turnbaugh P, Lozupone CA, Knight RD, Gordon JI (2005) Obesity alters gut microbial ecology. Proc Natl Acad Sci U S A 102(31):11070–11075. https://doi.org/10.1073/pnas.0504978102
Ley RE, Turnbaugh PJ, Klein S, Gordon JI (2006) Microbial ecology: human gut microbes associated with obesity. Nature 444(7122):1022–1023. https://doi.org/10.1038/4441022a
Li H, He J, Jia W (2016a) The influence of gut microbiota on drug metabolism and toxicity. Expert Opin Drug Metab Toxicol 12(1):31–40. https://doi.org/10.1517/17425255.2016.1121234
Li SS, Zhu A, Benes V, Costea PI, Hercog R, Hildebrand F et al (2016b) Durable coexistence of donor and recipient strains after fecal microbiota transplantation. Science (New York, NY) 352(6285):586–589. https://doi.org/10.1126/science.aad8852
Lin A, Bik EM, Costello EK, Dethlefsen L, Haque R, Relman DA, Singh U (2013) Distinct distal gut microbiome diversity and composition in healthy children from Bangladesh and the United States. PLoS One 8(1):e53838. https://doi.org/10.1371/journal.pone.0053838
Lozupone CA, Stombaugh JI, Gordon JI, Jansson JK, Knight R (2012) Diversity, stability and resilience of the human gut microbiota. Nature 489(7415):220–230. https://doi.org/10.1038/nature11550
Lupp C, Robertson ML, Wickham ME, Sekirov I, Champion OL, Gaynor EC, Finlay BB (2007) Host-mediated inflammation disrupts the intestinal microbiota and promotes the overgrowth of Enterobacteriaceae. Cell Host Microbe 2(3):204
Marchesi JR, Adams DH, Fava F, Hermes GDA, Hirschfield GM, Hold G et al (2015) The gut microbiota and host health: a new clinical frontier. Gut 65(2):330–339. https://doi.org/10.1136/gutjnl-2015-309990
Martinez I, Stegen JC, Maldonado-Gomez MX, Eren AM, Siba PM, Greenhill AR, Walter J (2015) The gut microbiota of rural papua new guineans: composition, diversity patterns, and ecological processes. Cell Rep 11(4):527–538. https://doi.org/10.1016/j.celrep.2015.03.049
Morton ER, Lynch J, Froment A, Lafosse S, Heyer E, Przeworski M et al (2015) Variation in Rural African Gut microbiota is strongly correlated with colonization by Entamoeba and subsistence. PLoS Genet 11(11):e1005658. https://doi.org/10.1371/journal.pgen.1005658
O’Keefe SJ, Li JV, Lahti L, Ou J, Carbonero F, Mohammed K, Posma JM, Kinross J, Wahl E, Ruder E, Vipperla K, Naidoo V, Mtshali L, Tims S, Puylaert PG, DeLany J, Krasinskas A, Benefiel AC, Kaseb HO, Newton K, Nicholson JK, de Vos WM, Gaskins HR, Zoetendal EG (2015) Fat, fibre and cancer risk in African Americans and rural Africans. Nat Commun 6:6342. https://doi.org/10.1038/ncomms7342
Ou J, Carbonero F, Zoetendal EG, DeLany JP, Wang M, Newton K et al (2013) Diet, microbiota, and microbial metabolites in colon cancer risk in rural Africans and African Americans. Am J Clin Nutr 98(1):111–120. https://doi.org/10.3945/ajcn.112.056689
Qin J, Li R, Raes J, Arumugam M, Burgdorf KS, Manichanh C et al (2010) A human gut microbial gene catalogue established by metagenomic sequencing. Nature 464(7285):59–65. https://doi.org/10.1038/nature08821
Qin J, Li Y, Cai Z, Li S, Zhu J, Zhang F et al (2012) A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature 490(7418):55–60. https://doi.org/10.1038/nature11450
Ramirez-Farias C, Slezak K, Fuller Z, Duncan A, Holtrop G, Louis P (2009) Effect of inulin on the human gut microbiota: stimulation of Bifidobacterium adolescentis and Faecalibacterium prausnitzii. Br J Nutr 101(4):541–550. https://doi.org/10.1017/S0007114508019880
Ridaura VK, Faith JJ, Rey FE, Cheng J, Duncan AE, Kau AL et al (2013) Gut microbiota from twins discordant for obesity modulate metabolism in mice. Science 341(6150):1241214. https://doi.org/10.1126/science.1241214
Risnes KR, Belanger K, Murk W, Bracken MB (2011) Antibiotic exposure by 6 months and asthma and allergy at 6 years: Findings in a cohort of 1,401 US children. Am J Epidemiol 173(3):310–318. https://doi.org/10.1093/aje/kwq400
Sanchez M, Darimont C, Drapeau V, Emady-Azar S, Lepage M, Rezzonico E et al (2014) Effect of Lactobacillus rhamnosus CGMCC1.3724 supplementation on weight loss and maintenance in obese men and women. Br J Nutr 111(8):1507–1519. https://doi.org/10.1017/S0007114513003875
Schnorr SL, Candela M, Rampelli S, Centanni M, Consolandi C, Basaglia G et al (2014) Gut microbiome of the Hadza hunter-gatherers. Nat Commun 5:3654. https://doi.org/10.1038/ncomms4654
Schulz MD, Atay C, Heringer J, Romrig FK, Schwitalla S, Aydin B et al (2014) High-fat-diet-mediated dysbiosis promotes intestinal carcinogenesis independently of obesity. Nature 514(7523):508–512. https://doi.org/10.1038/nature13398
Scott KP, Martin JC, Duncan SH, Flint HJ (2014) Prebiotic stimulation of human colonic butyrate-producing bacteria and bifidobacteria, in vitro. FEMS Microbiol Ecol 87(1):30–40. https://doi.org/10.1111/1574-6941.12186
Scott KP, Antoine J-M, Midtvedt T, van Hemert S (2015) Manipulating the gut microbiota to maintain health and treat disease. Microb Ecol Health Dis 26:25877
Sears CL, Pardoll DM (2011) Perspective: alpha-bugs, their microbial partners, and the link to colon cancer. J Infect Dis 203(3):306–311. https://doi.org/10.1093/jinfdis/jiq061
Sender R, Fuchs S, Milo R (2016) Revised estimates for the number of human and bacteria cells in the body. PLoS Biol 14(8):e1002533. https://doi.org/10.1371/journal.pbio.1002533
Shanahan F, Bernstein CN (2009) The evolving epidemiology of inflammatory bowel disease. Curr Opin Gastroenterol 25(4):301–305. https://doi.org/10.1097/MOG.0b013e32832b12ef
Sokol H, Pigneur B, Watterlot L, Lakhdari O, Bermudez-Humaran LG, Gratadoux J-J et al (2008) Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proc Natl Acad Sci U S A 105(43):16731–16736. https://doi.org/10.1073/pnas.0804812105
Sokol H, Seksik P, Furet JP, Firmesse O, Nion-Larmurier I, Beaugerie L et al (2009) Low counts of Faecalibacterium prausnitzii in colitis microbiota. Inflamm Bowel Dis 15(8):1183–1189. https://doi.org/10.1002/ibd.20903
Spor A, Koren O, Ley R (2011) Unravelling the effects of the environment and host genotype on the gut microbiome. Nat Rev Microbiol 9(4):279–290. https://doi.org/10.1038/nrmicro2540
Surawicz CM, Brandt LJ, Binion DG, Ananthakrishnan AN, Curry SR, Gilligan PH et al (2013) Guidelines for diagnosis, treatment, and prevention of clostridium difficile infections. Am J Gastroenterol 108(4):478–498; quiz 499. https://doi.org/10.1038/ajg.2013.4
Tjalsma H, Boleij A, Marchesi JR, Dutilh BE (2012) A bacterial driver-passenger model for colorectal cancer: beyond the usual suspects. Nat Rev Microbiol. https://doi.org/10.1038/nrmicro2819
Turnbaugh PJ, Ley RE, Mahowald MA, Magrini V, Mardis ER, Gordon JI (2006) An obesity-associated gut microbiome with increased capacity for energy harvest. Nature 444(7122):1027–1031. https://doi.org/10.1038/nature05414
Turnbaugh PJ, Ley RE, Hamady M, Fraser-Liggett CM, Knight R, Gordon JI (2007) The human microbiome project. Nature 449(7164):804–810. https://doi.org/10.1038/nature06244
Turnbaugh PJ, Backhed F, Fulton L, Gordon JI (2008) Diet-induced obesity is linked to marked but reversible alterations in the mouse distal gut microbiome. Cell Host Microbe 3(4):213–223. https://doi.org/10.1016/j.chom.2008.02.015
Voreades N, Kozil A, Weir TL (2014) Diet and the development of the human intestinal microbiome. Front Microbiol 5:494. https://doi.org/10.3389/fmicb.2014.00494
Warren RL, Freeman DJ, Pleasance S, Watson P, Moore RA, Cochrane K et al (2013) Co-occurrence of anaerobic bacteria in colorectal carcinomas. Microbiome 1(1):16. https://doi.org/10.1186/2049-2618-1-16
Yatsunenko T, Rey FE, Manary MJ, Trehan I, Dominguez-Bello MG, Contreras M et al (2012) Human gut microbiome viewed across age and geography. Nature 486(7402):222–227. https://doi.org/10.1038/nature11053
Zhang F, Luo W, Shi Y, Fan Z, Ji G (2012) Should we standardize the 1,700-year-old fecal microbiota transplantation? Am J Gastroenterol. https://doi.org/10.1038/ajg.2012.251
Zhang Q, Wu Y, Fei X (2015) Effect of probiotics on body weight and body-mass index: a systematic review and meta-analysis of randomized, controlled trials. Int J Food Sci Nutr 67(5):571–580. https://doi.org/10.1080/09637486.2016.1181156
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Zucko, J., Starcevic, A., Diminic, J., Oros, D. (2019). Microbiota: Novel Gateway Towards Personalised Medicine. In: Bodiroga-Vukobrat, N., Rukavina, D., Pavelić, K., Sander, G.G. (eds) Personalized Medicine in Healthcare Systems. Europeanization and Globalization, vol 5. Springer, Cham. https://doi.org/10.1007/978-3-030-16465-2_9
Download citation
DOI: https://doi.org/10.1007/978-3-030-16465-2_9
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-16464-5
Online ISBN: 978-3-030-16465-2
eBook Packages: Law and CriminologyLaw and Criminology (R0)