Abstract
Functional tricuspid regurgitation (FTR) is an important prognosticator in many cardiac diseases. Although surgical intervention has been being frequently applied, the success of current repair techniques is often uncertain and observation of residual or progressive FTR after tricuspid valve annuloplasty is not uncommon. Standard views obtained with two-dimensional transthoracic echocardiography, due to its inherent limitations, failed to evaluate geometric changes associated with FTR accurately. Transthoracic three-dimensional echocardiography (3DE) has revolutionized our approach for better understanding the 3D geometry of the tricuspid annulus both in normal subjects and in patients with FTR. The tricuspid annulus was found to be a non-planar structure with a distinct bimodal or saddle-shaped pattern like the mitral annulus, whereas, in patients with FTR, the annular area was larger and the annulus was flatter with markedly decreased annular height, which diminished the saddle shape. Potential contribution of right ventricular or right atrial geometric changes to the tricuspid annulus remodeling in FTR can also be evaluated using transthoracic 3DE data sets. 3DE, performed before and after the tricuspid annuloplasty, can provide an excellent opportunity to evaluate geometric changes associated with persistent or progressive FTR after the tricuspid annuloplasty. The current surgical approach can achieve tricuspid annulus size reduction at the expense of aggravation of leaflet tenting, which can explain suboptimal surgical results. 3DE color Doppler images can be adequately used for cross-sectional images of the vena contracta using multiplanar reconstruction images, which is useful to assess the severity of FTR. Thus, comprehensive and accurate evaluation of FTR is possible using 3DE and its impact to improve clinical outcome should be further tested.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Functional tricuspid regurgitation
- 3-Dimensional echocardiography
- Tricuspid annulus
- Leaflet tethering
- Pathophysiology
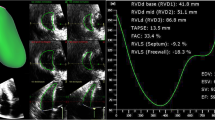
Functional tricuspid regurgitation (FTR) is frequently caused by increased right ventricular (RV) pressure overloading and associated with advanced stages of left-sided valve, myocardial, or pulmonary diseases [1], and development of FTR has been proved to be an independent factor associated with increased mortality and morbidity [2,3,4,5]. Thus, there has been an increasing tendency to repair the tricuspid valve (TV) to abolish or decrease FTR at the time of concomitant surgery for left-sided disease [6, 7]. However, the outcome of the current TV repair procedures is sometimes unpredictable and residual or progressive TR after TV annuloplasty is not uncommon [8,9,10]. Although it is generally believed that FTR results from a combination of tricuspid annular dilatation and valve apparatus deformation, the inherent limitations of conventional two-dimensional imaging techniques used to assess patients with FTR have limited our understanding of the pathophysiology of this valve disease. Three-dimensional echocardiography (3DE), by allowing an anatomically sound visualization of the TV from any perspective as well as the measurement of the geometry of its components and of the size and function of the right atrium and RV, can contribute to improve our understanding of the mechanisms leading to FTR in various cardiac conditions and thus providing better therapeutic options (Fig. 21.1).
Example of comprehensive assessment of the mechanism of functional tricuspid regurgitation. On the left, quantitative analysis of right ventricular volumes, shape and function. In the center, morphology of tricuspid leaflets and measurement of tricuspid annulus size and function. On the right, measurement of right atrial volumes and function
Geometric Changes of Tricuspid Valve Complex in Functional Tricuspid Regurgitation
3DE has revolutionized our approach to assess the TV apparatus in normal subjects and in patients with FTR [11,12,13]. Transthoracic 3DE can visualize all three TV leaflets simultaneously (Fig. 21.2) and full volume datasets of the TV can be used to perform quantitative analysis of the various components of the TV (see Chap. 18).
The tricuspid valve obtained from transthoracic 3DE and visualized from the right ventricular perspective in normal control (a, diastole) and a patient with functional tricuspid regurgitation (b, c). Septal (S), anterior (A) and posterior (P) leaflets are simultaneously visualized. The coaptation gap in functional tricuspid regurgitation can be easily observed by comparing leaflet position during diastole (b) and systole (c)
Pathophysiology of Functional Tricuspid Regurgitation
The pathophysiology of FTR involves several mechanisms that may contribute, to different extents, in different cardiac conditions [1, 12]: (1) dilation of the tricuspid annulus secondary to RV and/or right atrial dilation; (2) distortion of the spatial relationships among leaflets, chordae and papillary muscles leading to leaflet tethering and malcoaptation; (3) changes in TA geometry (dilated, more circular and flatter) and dynamics (reduced area shortening and excursion).
The association between tricuspid dilation and FTR has been well established [14,15,16,17,18]. Tricuspid annulus dilation and right/left atrial enlargement are early and sensitive indicators of FTR [15]. Right atrial enlargement occurs before RV dilation, which occurs late and is associated with more severe TR. Studies of patients with isolated TR (i.e. without left heart disease or pulmonary hypertension) associated with atrial fibrillation have shown a close correlation between tricuspid annulus area and right atrial volume (and lower correlation with RV end-systolic volume), and between annular area and TR severity [18]. Despite the mounting evidence of the role played by the right atrium in determining tricuspid annulus dilation, the size and the function of the right atrium are almost systematically neglected when discussing the pathophysiology and management of FTR [19].
On the other hand, it is also a common observation that not all patients with tricuspid annulus dilation have FTR and, with the same extent of tricuspid annulus dilation, different degrees of FTR may be observed. This may be related to differential TV leaflet remodeling. Afilalo et al. [20] demonstrated that, in patients with pulmonary hypertension, TV leaflets remodel by increasing their area and both the occurrence and severity of FTR are related to the extent of leaflet adaptation to increased tricuspid annulus area expressed as the ratio between TV leaflet area/closure area. Nonetheless, annular dilatation has recently been associated with outcomes [21]. In 213 patients with moderate or severe TR secondary to left-sided valve diseases, nonvalvular disease, or isolated primary TR, an enlarged tricuspid annulus was positively associated with cardiovascular outcomes (composite of hospitalization for worsening heart failure, stroke, and cardiovascular death) irrespective of subgroups according to type or severity of TR.
Spinner et al. [14] demonstrated that both annular dilation and papillary muscle displacement contribute to FTR. Significant FTR occurs with only 40% dilation of tricuspid annulus area (compared to a 75% annulus area dilation needed to create functional mitral regurgitation). TA dilation caused the displacement of the anterior and posterior leaflets from the central coaptation line, with a progressive reduction of the leaflet coaptation surface until a gap occurred. In this experimental study, the minimum coaptation length to prevent regurgitation was 5 mm. The anterior leaflet was found to be the most affected by tricuspid annulus dilation. The investigators demonstrated also that isolated papillary muscle displacement (i.e. without tricuspid annulus dilation) can cause FTR, and identified the septal as the most affected leaflet by papillary displacement. Of course, the concomitant presence of tricuspid annulus dilation and papillary muscle displacement produced the largest FTR.
The importance of RV geometry in the generation of tricuspid malcoaptation is supported by a number of other studies. Fukuda et al. [22] were one of the first to attribute changes in right-sided cavity size, RV sphericity and left ventricular function to tethering of the TV leaflets and consequent TR. These changes in ventricular geometry and function did not affect annular area. Topilsky et al. [23] studied patients with idiopathic FTR and compared them to patients with pulmonary hypertension with TR. Patients with idiopathic FTR had the largest basal RV diameter and annular area and lowest valvular/annular coverage ratio but normal valve tenting height and a conical RV shape. FTR associated with pulmonary hypertension had mild annular enlargement but excessive valve tenting height and an elliptical/spherical RV shape. Valvular changes were linked to specific RV changes: the largest basal dilatation, and normal length (RV conical deformation) in idiopathic functional TR versus longest RV with elliptical/spherical deformation (i.e. dilatation of the mid-ventricle) in pulmonary hypertension TR. Song et al. [24] reported that RV inlet dimension were the main determinants of TV geometry and severity of FTR. In particular, septal-lateral RV inlet dimension was the main determinant of the extent of TV leaflet tethering and septal-lateral tricuspid annulus diameter, whereas antero-posterior annulus diameter was determined by antero-posterior RV inlet dimension.
Accordingly, we can hypothesize two different pathophysiological models of FTR development in different cardiac conditions: a first model, where the starting mechanism is TA dilation, typical of patients with significantly dilated right atrium and normal or mildly dilated RV (e.g. chronic atrial fibrillation) [17, 18, 25]; and a second model, where the starting mechanism is the remodeling of the RV with the displacement of the papillary muscles and the tenting of TV leaflets, typical of patients with pulmonary hypertension, dilated RV and normal or mildly dilated right atrium [26, 27]. Once initiated, the RV and right atrium remodeling secondary to the volume overload may easily produce a further dilation of the tricuspid annulus, which aggravates the FTR starting a vicious circle in which FTR begets more FTR and both tricuspid annulus dilation and leaflet tethering coexist in the same patient.
Evaluation of Tricuspid Valve Apparatus
Evaluation of patients with FTR who are considered either for surgery or transcatheter procedures should include tricuspid annulus size, mode of leaflet coaptation, as well as the extent of leaflet tethering in addition to the severity of regurgitation [28].
Tricuspid Annulus
Current guidelines [29, 30] recommend two-dimensional echocardiography to size the tricuspid annulus. A cut-off value of 40 mm (or 21 mm/m2 of body surface area) for the tricuspid annulus diameter obtained from an apical 4-chamber view, in diastole, has been selected to indicate the need of concomitant procedures on the TV when the patient needs surgery for left-sided heart valve diseases. However, two-dimensional echocardiography has several limitations in sizing the tricuspid annulus diameter.
Using a single linear dimension to size the tricuspid annulus is based on the assumptions that the tricuspid annulus is a flat structure, its shape is circular and the measured dimension is the actual diameter of the circle. In patients with severe FTR, the tricuspid annulus is more planar [31, 32]. However, in patients with mild or moderate FTR in whom surgical annuloplasty may be considered based solely on this measurement, it is a complex three-dimensional (3D) non-planar structure (See Fig. 18.4 in Chap. 18). Moreover, both the shape and the spatial orientation of the tricuspid annulus are quite variable [33]. Dreyfus et al. [33] found that, although tricuspid annulus shape was generally oval (mean eccentricity index = 1.35), there were large inter-individual differences from circular (eccentricity index = 1.07) to severely oval (eccentricity index 2.04) tricuspid annulus. Taking the vertical axis at the level of interventricular septum as the reference, the long axis of the tricuspid annulus can be positioned at a variable angle between 5° and 140° with a bimodal distribution with the most frequent orientations located at 40° and 140° [33]. Finally, the conventional apical 4-chamber view obtained with two-dimensional echocardiography does not have any anatomical landmark to allow a proper and reproducible orientation of the view [34]. Comparisons between the tricuspid annulus diameter obtained with two-dimensional echocardiography in apical 4-chamber view and anatomically oriented tricuspid annulus long-axis from 3DE showed an underestimation of 4–9 mm of the former, with wide limits of agreement (7 mm), reflecting also the variability of the differences related to the different shapes and orientations of the tricuspid annulus [33, 35]. Accordingly, 3DE, which allows acquisition of anatomically oriented tricuspid annulus measurements independent of assumptions about its shape and orientation, should be the first line imaging to size it. Tricuspid annulus measurements by 3DE are more accurate than those obtained by two-dimensional echocardiography, when compared with cardiac magnetic resonance [36], and the correlation between tricuspid annulus diameter obtained by two-dimensional echocardiography and severity of FTR is poor [35, 37]. In patients with insufficient acoustic window and in sinus rhythm, both 320-slices multislice computed tomography [38,39,40] and cardiac magnetic resonance [36, 41] can be used to measure the size of tricuspid annulus.
However, the current guidelines use a thresholds of ≥40 mm (or 21 mm/m2 of body surface) obtained by two-dimensional echocardiography in the 4-chamber apical view in “diastole” without defining whether that measurement is taken in early, late or end-diastole. Tricuspid annulus area may change by 30% during the cardiac cycle [42, 43] and, within the diastolic time interval, the tricuspid annulus changes significantly [42,43,44] (Fig. 21.3). Current recommendations comes from a single study that identified a cut-off value of the stretched diameter of the tricuspid annulus ≥70 mm, measured intraoperatively, as an indication to perform concomitant tricuspid annuloplasty in patients undergoing mitral valve surgery independent on the severity of FTR [6]. Although this paper is consistently cited as support for the echocardiographically-measured tricuspid annulus end-diastolic 4-chamber diameter criteria of ≥40 mm [28, 29, 45], there is no echocardiographic data about the tricuspid annulus size in the original paper [6]. Moreover, it is unclear how a 40 mm diameter measured by two-dimensional echocardiography, in the beating heart, from the mid-septal to the mid-anterior (or mid-posterior) annulus could correspond to a 70 mm maximal diameter between the anteroseptal and anteroposterior commissure measured in the arrested heart. Finally, in healthy subjects the tricuspid annulus diameter is correlated to subject age, gender, right atrial and RV volume [46], and, in patients with FTR, tricuspid annulus diameter is also influenced by RV loading conditions. Using a 40 mm cutoff for diastolic tricuspid annulus diameter in 4-chamber view, 20% of healthy subjects would be classified as having “dilated” tricuspid annulus [46].
Time course of tricuspid annulus area change during the cardiac cycle [43]. ED end-diastole, ES end-systole, LD late diastole. Modified from Addetia K, Muraru D, Veronesi F, et al. 3-Dimensional Echocardiographic Analysis of the Tricuspid Annulus Provides New Insights Into Tricuspid Valve Geometry and Dynamics. JACC Cardiovasc Imaging. 2019;12:401–412
Since, 3DE is highly feasible and both the TV and the right heart are often better imaged by transthoracic than by transesophageal approach [11], we need dedicated software packages to measure the various components of the TV apparatus (Fig. 21.4). Then, outcome studies using 3DE to obtain anatomically sound measures, will be needed to identify the threshold of the tricuspid annulus dilation (taking into account patient age, gender, right heart chamber size and loading conditions) which can indicate the need of concomitant tricuspid annuloplasty at the time of left heart surgery.
Results of the 3D reconstruction of the tricuspid annulus geometry in a normal subject (left) and in a patient with functional tricuspid regurgitation (right) using a custom-made software package [43]. Normal tricuspid annulus is a non-planar structure with two high points (oriented superiorly toward the right atrium) and a bimodal or saddle-shaped pattern like the mitral annulus. In patients with functional tricuspid regurgitation, the tricuspid annulus is characterized by increased annular area and decreased annular height diminishing the saddle shape
Tricuspid Valve Leaflet Coaptation
The extent and mode of leaflet coaptation is another important determinant of the presence and severity of FTR [28]. A coaptation of the body of the leaflet (body-to-body coaptation) guarantees TV sealing and absence of FTR. Normal coaptation of the TV leaflets takes place either at the TA level or more apically, just below it, with a 5–10 mm of the leaflets’ body surfaces in contact during systole. When the coaptation surface decreases due to tricuspid annulus dilation and/or leaflets’ tethering, the coaptation takes place on the free edges of the leaflets and FTR occurs. Current recommendations [47] suggest measuring the distance between the leaflet coaptation point and the annular plane (tethering distance) and the area between the closed leaflet and the annular plane (tenting area) to estimate the extent of leaflet tethering (Fig. 21.5). When the tethering distance is >8 mm and the tenting area is >1.6 cm2, the extent of TV leaflet tethering is considered pathologic [10, 28]. However, these measurements obtained with two-dimensional echocardiography are based on the assumptions that tethering of the TV leaflets is symmetric and that the apical 4-chamber view allows the visualization of the highest coaptation point. Both conditions are unlikely to occur in patients with FTR and, not surprisingly, it has been reported that the tenting volume is a better predictor of FTR severity and of the occurrence of residual FTR after tricuspid annuloplasty [48] (Fig. 21.6).
Two-dimensional echocardiography assessment of the extent of the tethering of tricuspid valve leaflets in functional tricuspid regurgitation. Compared to normal control (left), in patients with functional tricuspid regurgitation (right), the annulus is dilated (double arrow white dashed line), the coaptation depth (double arrow yellow line) is more apically displaced and the tenting area (blue triangle) is larger. RA right atrium, RV right ventricle
Visualization and measurement of the tenting volume (V, green beutels) using three-dimensional echocardiography in two patients with similar dilatation of the tricuspid annulus (L). Upper panels, patient with dilatation of the right ventricle and tethering of the tricuspid leaflets. Lower panels, patient with dilatation of the right atrium, normal right ventricle and minimal tenting of tricuspid leaflets. From the left: two-dimensional echocardiography, apical 4-chamber view; transthoracic three-dimensional echocardiography, longitudinal cut-plane showing the right atrium (RA) and the right ventricle (RV); transthoracic three-dimensional color Doppler acquisition showing the extent of the tricuspid regurgitation jet; three-dimensional echocardiography, transversal cut-plane showing an “en face” view of the tricuspid valve from the ventricular perspective. A tenting area, RA right atrium, RV right ventricle
Evaluation of Tricuspid Regurgitation Severity
Because of the complexity for TR evaluation with invasive methods, echocardiography has always played a central role for TR assessment. The parameters used for this purpose range from qualitative to quantitative, and both of them are recommended by current American and European Guidelines [47, 49]. Among them, the measurement of the diameter of the vena contracta of the regurgitant jet and the calculation of the tricuspid effective regurgitation orifice area by the proximal isovelocity surface area (PISA) method are the most widely used, even if the final grading of the severity of TR should be further supported by other parameters.
The use of traditional quantitative parameters to assess the severity of TR is based on geometrical assumptions about the shape of the tricuspid regurgitant orifice and extrapolation of concepts learned from studying the mitral valve [50]. As the TV has unique features, being highly dynamic, with a complex coaptation among its three leaflets which determines complex geometric configurations of the regurgitant orifice, there is an urgent need for these parameters to be questioned [51, 52].
The basic geometrical assumptions in using the diameter of the vena contracta of the regurgitant jet are that the proximal part of the jet has a circular cross section and that the two-dimensional echocardiography view used to measure its diameter is passing though the actual diameter of the cross-sectional area of the vena contracta. Both of them are unlikely to occur in clinical practice where the regurgitant orifice assumes complex and unpredictable shapes (Fig. 21.7).
Variable geometry of the tricuspid regurgitation orifice in different patients with functional tricuspid regurgitation. Upper panels, transthoracic three-dimensional color Doppler echocardiography. The data set has been cut transversally to show the regurgitant orifice from the ventricular perspective. Lower panels, the data sets have been sliced to allow the planimetry of the area of the vena contracta. The yellow dashed line shows the position of the apical 4-chamber view to allow to appreciate the lack of relationship between the vena contracta diameter and its actual shape and area
In addition to the fluidodynamic considerations about the TR jet [53], accurate calculations of the effective regurgitant orifice area using the PISA method are based on the following assumptions: (1) the regurgitant orifice is circular; (2) the regurgitant orifice is flat; (3) the PISA is a hemisphere and its area can be calculated by measuring the radius of the hemisphere. However, the regurgitant orifice is unlikely to be circular in FTR (Fig. 21.7). The regurgitant orifice is not flat, since a variable degree of tenting of the TV leaflets occurs according to the main mechanism determining the regurgitation (i.e. tricuspid annulus dilation and/or papillary muscle displacement) [14]. Finally, due to the variable shape of the regurgitant orifice of the TV, the large regurgitant orifice and relatively low velocity of regurgitant flow (when compared to mitral regurgitation) the hemispheric geometry of the PISA is unlikely to occur in real patients (Fig. 21.8).
Transthoracic three-dimensional color Doppler echocardiography obtained from a patient with functional tricuspid regurgitation. Three-dimensional reconstruction of the proximal isovelocity surface (green beutel shown by the white arrow in the magnified image) showing that its actual shape is quite far from that of a hemisphere
Interestingly, the partition values to define mild, moderate or severe the TR for the diameter of the vena contracta (<0.3 cm, 0.31–0.69 cm, and ≥0.7 cm, respectively) and the effective regurgitant orifice area (<0.2 cm2, 0.2–0.39 cm2, ≥0.4 cm2, respectively) are similar to those identified to grade mitral regurgitation severity, despite the anatomical differences between the two valves and the different hemodynamic environment in which they operate.
The diameter of the vena contracta of the TR jet was validated by Tribouilloy et al. [50] in 71 patients with various degrees of TR. They measured it from a single 4-chamber apical view and used the effective regurgitant orifice area by PISA and hepatic venous flow as reference, both parameters having suboptimal accuracy and a number of limitation in patients with TR [49]. They found that a vena contracta diameter >6.5 mm identified severe TR with 88.5% sensitivity and 93.3% specificity. However, they tested the accuracy of the parameter on the same study population from which the parameter was derived and no other study has ever tested this cut-off value on any different population.
The effective orifice area calculated by means of the PISA method (used as the reference for the vena contracta diameter by Tribouilloy et al. [50]) was “validated” by Rivera et al. [54] in 45 patients using the Doppler 2DE volumetric method as reference. Notably, the Doppler 2DE volumetric method has shown to significantly overestimate the regurgitant volume and to have limited reproducibility in patients with mitral regurgitation [55], in whom the geometry of the annulus is more predictable than in TR, and there is no evidence for the partition values used to grade TR severity. They just adopted them in analogy with the mitral valve. However, it is unlikely that the same amount of regurgitation may have the same hemodynamic impact on a “pressure pump” (i.e. the left ventricle) and on a “flow pump” (i.e. the RV). Conversely, it is likely that the RV can handle larger regurgitant volumes than its left counterpart. Indeed, the need for a new TR grading scheme has recently been advocated [56]. However, the proposed partition values for “massive” and “torrential” TR were based “…on the ranges of values for the current grades of mild or moderate”, with no outcome evidence supporting these cut-off values. Alternatively, we should consider the hypothesis that to be “clinically severe” (in terms of patient’s morbidity and mortality) TR requires a larger regurgitant volume than mitral regurgitation.
Moreover, even if both the diameter of the vena contracta and the effective regurgitant orifice area were accurate estimates of TR severity in the frame they are calculated, it remains the problem of the actual hemodynamic and clinical significance of a static measure (in one frame) of a rapidly changing phenomenon throughout the cardiac systole like the TR. In patients with FTR, regurgitant flow is not constant (Fig. 21.9), but it varies continuously throughout systole, therefore a measurement taken in a single frame does not seem to be the ideal parameter to assess FTR severity.
Time course of tricuspid effective regurgitant orifice area during cardiac systole obtained from three-dimensional reconstruction of the proximal isovelocity surface area. Effective regurgitant orifice area is larger in proto- and end-systole and smaller in mid-systole when the contraction of the right ventricle pushes leaflets towards the annulus
Furthermore, both the regurgitant orifice area and the regurgitant volume across the TV are influenced by the respiratory cycle (Fig. 21.10) and loading conditions. Compared to expiration, during inspiration, TR presents a decrease in driving forces while the size of the regurgitant orifice increases by 69% [57]. During inspiration, as venous return to the right side of the heart increases, the RV and right atrium expand their width to accommodate a higher volume, without significantly changing their longitudinal dimensions. The increase in width of the right atrium and RV result in an increase of tricuspid annulus size. Moreover, the horizontal displacement of the papillary muscles [38] and the anatomical particularities of the TV (with the insertion of chordae tendineae to multiple papillary muscles and the RV free wall) determine an increase in leaflet coaptation height and tenting area. Consequently, tricuspid regurgitant orifice area increases (Fig. 21.10), ultimately resulting in an average increase in 20% of regurgitant volume during inspiration [57]. Currently, it remains to be determined which is the best moment to quantitate TR: during inspiration, during expiration, during halted respiration or, maybe, integrating the regurgitant volume over time throughout the respiratory cycle.
En-face view of the tricuspid regurgitant orifice from the ventricular perspective obtained during quiet respiration by real-time transthoracic three-dimensional echocardiography showing the wide variation of the size of the regurgitant orifice from expiration (left) to inspiration (right) in a patient with functional tricuspid regurgitation. ATL anterior tricuspid leaflet, LV left ventricle, PTL posterior tricuspid leaflet, RVOT right ventricular outflow tract, STL septal tricuspid leaflet
Finally, assessment of TR is further complicated by the fact that the right heart is more sensitive to both preload and afterload than its left counterpart. Within physiological limits, RV contractility can increase with increasing end diastolic volume, using the Frank Starling mechanism, translating in increased RV longitudinal function which can be measured using conventional two-dimensional echocardiography measurements [58]. Therefore, an increase in preload during inspiration will also increase RV contractility. However, in patients with severe TR, because of the increase of TR during inspiration, right atrial pressure also increases, approximating RV systolic pressure. Consequently, TR peak velocity measured by Doppler echocardiography decreases as well, and this decrease of peak velocity can variably affect effective orifice area calculations. An inspiratory decrease of TR peak velocity by 0.6 m/s or more has high specificity (94%), and negative predictive value (92%) for severe TR [59]. RV preload is also affected by treatment. Effective diuretic treatment at the time of the echocardiography study may dramatically decrease the estimate of TR severity.
The role of RV afterload as a mechanism contributing to FTR is also worth noting. The high prevalence of FTR in patients with pulmonary hypertension has been documented. However, the cause-effect relationship between pulmonary pressure and FTR is not that clear. Mutlak et al. [60] studied in a large cohort of patients divided in three groups according to pulmonary artery systolic pressure (<50 mmHg, 50–70 mmHg, >70 mmHg). Despite the fact that pulmonary systolic pressure (per 10 mmHg increase) was independently associated with significant TR (Odds Ratio = 2.26), not all patients with pulmonary hypertension had significant FTR. Sixty-five percent of patients with pulmonary systolic pressure between 50 and 70 mmHg, and 45% of those with pulmonary systolic pressure higher than 70 mmHg had only mild TR [60]. Extent of right atrial and RV remodeling was strongly associated with severe TR (Odds Ratio = 6.34 and 7.02, respectively) independent on pulmonary systolic pressure. In addition, this data supports the concept that even if RV afterload is related to FTR, this relationship is modulated by various other factors that affect the size of the TA or the extent of leaflet tethering.
Novel Echocardiographic Techniques to Assess Patients with Functional Tricuspid Regurgitation
3DE planimetry of the area of the vena contracta has been proposed as a method to overcome the problems related to the irregular shape of the regurgitant orifice in patients with FTR. This method solves the issues related to the irregular contour of the regurgitant orifice (Fig. 21.11). However, the regurgitant orifice is a curvilinear surface and, using a planimetry on a tomographic plane to measure it, will include the errors due to the fact that, on the atrial side, part of the jet is not yet contracted, whereas, on the ventricular side, part of the jet is not contracted anymore. Moreover, the size of the vena contracta is heavily dependent on color Doppler gain setting and does not overcome the fact that it is a static measure obtained in a single frame. In addition, a validated cut-off for the diagnosis of severe TR using 3DE planimetry of the vena contracta is still lacking. Velayudhan et al. [51] showed that a planimetered regurgitant orifice area >75 mm2 was associated with severe TR, defined as a TR regurgitant jet larger than 10 cm2 or a TR jet area/right atrial area ratio >34%. This cut-off was selected because of its high sensitivity and negative predictive value of 95%. Chen et al. [52] studied the role of 3DE planimetry of the vena contract to assess TR severity. In their study, both 3DE and 2DE acquisitions were performed during breath-holding. Influence of cardiac rhythm was also controlled by excluding patients with atrial fibrillation with more than 20% variation in R-R cycle length. They found a cut-off of 36 mm2 to have a sensitivity of 89% and a specificity of 84% for predicting severe TR [52] defined using a multiparameteric approach as indicated by ASE [49] and EACVI [47] guidelines. Another study in which 3DE planimetry of the area of the vena contracta has been explored identified a cut-off of >37 mm2 for moderate TR (sensitivity 100%, specificity 69%), and >57 mm2 for severe TR (sensitivity 100%, specificity 64%) defined using the effective regurgitant orifice area calculated with conventional PISA method [61]. Lacking an accepted reference method to quantitate FTR, the reported studies used different definitions of severe FTR and, as expected, found different cut-offs of 3DE vena contracta area to define severe FTR.
Multislice display of a transthoracic 3DE color-Doppler data set of the regurgitant jet in a patient with functional tricuspid regurgitation. By slicing the proximal part of the jet with orientation of the cut planes perpendicular to the direction of the jet, the smaller cross-sectional area of the jet (vena contracta) can be identified and planimetered (see text for details). A area, C perimeter
Another proposed method to assess the severity of TR using 3DE is to try to reconstruct the actual 3D volume of the PISA and to measure it independent of any geometric assumptions (Fig. 21.8). This technique is based on real-time (single-beat) 3DE acquisition of color Doppler data set using a vendor-specific equipment and, since it is supposed to allow a frame-by-frame measurement of the PISA volume, it can be applied to patients in atrial fibrillation. However, flow velocity measurements by color Doppler (as with any Doppler technique) are angle-dependent and, due to this angle-dependency, color Doppler displays only the vector velocity component (towards or away from the probe) and not the actual flow velocity. Therefore, color Doppler cannot show the “isovelocity surface” but only the “iso-Doppler surface” which cannot be a hemisphere and significantly underestimate the size of the proximal isovelocity surface [62, 63]. Thus, the 3DE PISA does not make any geometrical assumption about the shape of the iso-Doppler shell, but it assumes that color Doppler is angle independent. Moreover, only the peak velocity of TR jet is included in the formula for the calculation of the regurgitant orifice area. Therefore, the method cannot allow an actual measurement of frame-by-frame effective regurgitant orifice area change.
Finally, the 3DE PISA method has never been tested against any independent reference method to grade TR. De Agustin et al. [64] tested it against the effective regurgitant tricuspid orifice area calculated with 2DE and Doppler echocardiography volumetric method, and the 3DE planimetry of the vena contracta. Despite the known limitations of the volumetric method [55], the Authors found a very close correlation (r = 0.97) among the effective tricuspid regurgitant areas measured with the three echocardiographic methods [64], even higher than the correlations found during the in vitro testing of the 3DE PISA method (r = 0.91) [65].
Indeed, effective regurgitant orifice area may be a suboptimal parameter to estimate the severity of FTR. For the same effective regurgitant orifice area, the regurgitant volume can be quite different with different pressure gradients and we have discussed how the gradient between the RV and the right atrium can change throughout cardiac systole in patients with TR. Between a TR with an end-systolic effective regurgitant orifice area of 0.4 cm2 and a TR with a holosystolic effective regurgitant orifice area of 0.3 cm2—which would be more severe? The key parameter that best accounts for the volume overload on the right heart chambers is most likely the regurgitant volume, and not the single-frame regurgitant orifice area measurement.
Recently, a new software package has been released allowing to measure the regurgitant volume by tracking color flow during the whole cardiac cycle using real-time 3DE color flow acquisitions. Acquiring data sets of 3DE color flow at the level of the tricuspid and the pulmonary valves over 5–10 cardiac cycles and averaging the results allows the actual measurement of the TR volume independent on geometric assumptions about regurgitant orifice and/or proximal isovelocity surface shape, and taking into account intra-beat and respiratory variations of TR. Further studies about the feasibility and accuracy of these measurements are needed.
Conclusion
FTR is characterized by geometric changes of TV apparatus including leaflets and tricuspid annulus with associated RV and right atrial enlargement. Comprehensive evaluation of geometric changes of anatomical structures potentially involved in the pathophysiology of FTR can be possible using transthoracic 3DE. Moreover, 3D color Doppler imaging may help to overcome the limitations of conventional two-dimensional and Doppler echocardiography in the assessment of TR severity. Thus, transthoracic 3DE, including 3DE color Doppler imaging, should be the recommended technique for routine clinical practice for patients with FTR. Further investigations are necessary to evaluate whether certain measurements obtained from 3DE data set can affect the clinical outcomes in these patients.
References
Badano LP, Muraru D, Enriquez-Sarano M. Assessment of functional tricuspid regurgitation. Eur Heart J. 2013;34(25):1875–85.
Nath J, Foster E, Heidenreich PA. Impact of tricuspid regurgitation on long-term survival. J Am Coll Cardiol. 2004;43:405–9.
Calafiore AM, Gallina S, Iaco AL, et al. Mitral valve surgery for functional mitral regurgitation: should moderate-or-more tricuspid regurgitation be treated? a propensity score analysis. Ann Thorac Surg. 2009;87:698–703.
Varadarajan P, Pai RG. Prognostic implications of tricuspid regurgitation in patients with severe aortic regurgitation: results from a cohort of 756 patients. Interact Cardiovasc Thorac Surg. 2012;14:580–4.
Mascherbauer J, Kammerlander AA, Marzluf BA, Graf A, Kocher A, Bonderman D. Prognostic impact of tricuspid regurgitation in patients undergoing aortic valve surgery for aortic stenosis. PLoS One. 2015;10:e0136024.
Dreyfus GD, Corbi PJ, Chan KM, Bahrami T. Secondary tricuspid regurgitation or dilatation: which should be the criteria for surgical repair? Ann Thorac Surg. 2005;79:127–32.
McCarthy PM, Sales VL. Evolving indications for tricuspid valve surgery. Curr Treat Options Cardiovasc Med. 2010;12:587–97.
Bernal JM, Gutierrez-Morlote J, Llorca J, San Jose JM, Morales D, Revuelta JM. Tricuspid valve repair: an old disease, a modern experience. Ann Thorac Surg. 2004;78:2069–74.
McCarthy PM, Bhudia SK, Rajeswaran J, et al. Tricuspid valve repair:durability and risk factors for failure. J Thorac Cardiovasc Surg. 2004;127:674–85.
Fukuda S, Song JM, Gillinov AM, et al. Tricuspid valve tethering predicts residual tricuspid regurgitation after tricuspid annuloplasty. Circulation. 2005;111:975–9.
Muraru D, Hahn RT, Soliman IA, Faletra F, Basso C, Badano LP. Three-dimensional echocardiography in imaging the tricuspid valve. JACC Cardiovasc Imaging. 2019;12:500–15.
Muraru D, Surkova E, Badano LP. Revisit of functional tricuspid regurgitation; current trends in the diagnosis and management. Korean Circ J. 2016;46:443–55.
Badano LP, Agricola E, Perez de Isla L, Gianfagna P, Zamorano JL. Evaluation of the tricuspid valve morphology and function by transthoracic real-time three-dimensional echocardiography. Eur J Echocardiogr. 2009;10:477–84.
Spinner EM, Shannon P, Buice D, et al. In vitro characterization of the mechanisms responsible for functional tricuspid regurgitation. Circulation. 2011;124:920–9.
Nemoto N, Lesser JR, Pedersen WR, et al. Pathogenic structural heart changes in early tricuspid regurgitation. J Thorac Cardiovasc Surg. 2015;150:323–30.
Mutlak D, Lessick J, Reisner SA, Aronson D, Dabbah S, Agmon Y. Echocardiography-based spectrum of severe tricuspid regurgitation: the frequency of apparently idiopathic tricuspid regurgitation. J Am Soc Echocardiogr. 2007;20:405–8.
Najib MQ, Vinales KL, Vittala SS, Challa S, Lee HR, Chaliki HP. Predictors for the development of severe tricuspid regurgitation with anatomically normal valve in patients with atrial fibrillation. Echocardiography. 2012;29:140–6.
Utsunomiya H, Itabashi Y, Mihara H, et al. Functional tricuspid regurgitation caused by chronic atrial fibrillation: a real-time 3-dimensional transesophageal echocardiography study. Circ Cardiovasc Imaging. 2017;10(1). pii: e004897.
Prihadi EA, Delgado V, Hahn RT, Leipsic J, Min JK, Bax JJ. Imaging needs in novel transcatheter tricuspid valve interventions. JACC Cardiovasc Imaging. 2018;11:736–54.
Afilalo J, Grapsa J, Nihoyannopoulos P, et al. Leaflet area as a determinant of tricuspid regurgitation severity in patients with pulmonary hypertension. Circ Cardiovasc Imaging. 2015;8(5). pii: e002714.
Kim H, Kim IC, Yoon HJ, et al. Prognostic usefulness of tricuspid annular diameter for cardiovascular events in patients with tricuspid regurgitation of moderate to severe degree. Am J Cardiol. 2018;121:1343–50.
Fukuda S, Gillinov AM, Song JM, et al. Echocardiographic insights into atrial and ventricular mechanisms of functional tricuspid regurgitation. Am Heart J. 2006;152:1208–14.
Topilsky Y, Khanna A, Le Tourneau T, et al. Clinical context and mechanism of functional tricuspid regurgitation in patients with and without pulmonary hypertension. Circ Cardiovasc Imaging. 2012;5:314–23.
Song JM, Jang MK, Kim YJ, Kim DH, Kang DH, Song JK. Right ventricular remodeling determines tricuspid valve geometry and the severity of functional tricuspid regurgitation: a real-time 3-dimensional echocardiography study. Korean Circ J. 2010;40:448–53.
Rogers JH, Bolling SF. The tricuspid valve: current perspective and evolving management of tricuspid regurgitation. Circulation. 2009;119:2718–25.
Sukmawan R, Watanabe N, Ogasawara Y, et al. Geometric changes of tricuspid valve tenting in tricuspid regurgitation secondary to pulmonary hypertension quantified by novel system with transthoracic real-time 3-dimensional echocardiography. J Am Soc Echocardiogr. 2007;20:470–6.
Park YH, Song JM, Lee EY, Kim YJ, Kang DH, Song JK. Geometric and hemodynamic determinants of functional tricuspid regurgitation: a real-time three-dimensional echocardiography study. Int J Cardiol. 2008;124:160–5.
Dreyfus GD, Martin RP, Chan KM, Dulguerov F, Alexandrescu C. Functional tricuspid regurgitation: a need to revise our understanding. J Am Coll Cardiol. 2015;65:2331–6.
Nishimura RA, Otto CM, Bonow RO, et al. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63:e57–185.
Baumgartner H, Falk V, Bax JJ, et al. 2017 ESC/EACTS guidelines for the management of valvular heart diseases. Eur Heart J. 2017;38(36):2739–91.
Ton-Nu TT, Levine RA, Handschumacher MD, et al. Geometric determinants of functional tricuspid regurgitation:insights from 3-dimensional echocardiography. Circulation. 2006;114:143–9.
Fukuda S, Saracino G, Matsumura Y, et al. Three-dimensional geometry of the tricuspid annulus in healthy subjects and in patients with functional tricuspid regurgitation: a real-time, 3-dimensional echocardiographic study. Circulation. 2006;114:I492–8.
Dreyfus J, Durand-Viel G, Raffoul R, et al. Comparison of 2-dimensional, 3-dimensional, and surgical measurements of the tricuspid annulus size: clinical implications. Circ Cardiovasc Imaging. 2015;8:e003241.
Stankovic I, Daraban AM, Jasaityte R, Neskovic AN, Claus P, Voigt JU. Incremental value of the en face view of the tricuspid valve by two-dimensional and three-dimensional echocardiography for accurate identification of tricuspid valve leaflets. J Am Soc Echocardiogr. 2014;27:376–84.
Anwar AM, Geleijnse ML, Ten Cate FJ, Meijboom FJ. Assessment of tricuspid valve annulus size, shape and function using real-time three-dimensional echocardiography. Interact Cardiovasc Thorac Surg. 2006;5:683–7.
Anwar AM, Soliman OI, Nemes A, van Geuns RJ, Geleijnse ML, Ten Cate FJ. Value of assessment of tricuspid annulus: real-time three-dimensional echocardiography and magnetic resonance imaging. Int J Cardiovasc Imaging. 2007;23:701–5.
Spinner EM, Lerakis S, Higginson J, et al. Correlates of tricuspid regurgitation as determined by 3D echocardiography: pulmonary arterial pressure, ventricle geometry, annular dilatation, and papillary muscle displacement. Circ Cardiovasc Imaging. 2012;5:43–50.
van Rosendael PJ, Joyce E, Katsanos S, et al. Tricuspid valve remodelling in functional tricuspid regurgitation: multidetector row computed tomography insights. Eur Heart J Cardiovasc Imaging. 2016;17:96–105.
Takaoka H, Funabashi N, Kataoka A, et al. Utilities of 320-slice computed-tomography for evaluation of tricuspid valve annular diameter before tricuspid-valve-plasty compared with the direct-measurement of tricuspid valve annular diameter during open heart-surgery. Int J Cardiol. 2013;168:2889–93.
Kabasawa M, Kohno H, Ishizaka T, et al. Assessment of functional tricuspid regurgitation using 320-detector-row multislice computed tomography: risk factor analysis for recurrent regurgitation after tricuspid annuloplasty. J Thorac Cardiovasc Surg. 2014;147:312–20.
Maffessanti F, Gripari P, Pontone G, et al. Three-dimensional dynamic assessment of tricuspid and mitral annuli using cardiovascular magnetic resonance. Eur Heart J Cardiovasc Imaging. 2013;14:986–95.
Tei C, Pilgrim JP, Shah PM, Ormiston JA, Wong M. The tricuspid valve annulus: study of size and motion in normal subjects and in patients with tricuspid regurgitation. Circulation. 1982;66:665–71.
Addetia K, Muraru D, Veronesi F, et al. 3-Dimensional Echocardiographic Analysis of the Tricuspid Annulus Provides New Insights Into Tricuspid Valve Geometry and Dynamics. JACC Cardiovasc Imaging. 2017;10. pii: S1936-878X(17)30902-6.
Miglioranza MH, Mihaila S, Muraru D, Cucchini U, Iliceto S, Badano LP. Variability of tricuspid annulus diameter measurement in healthy volunteers. JACC Cardiovasc Imaging. 2015;8:864–6.
Joint Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology (ESC); European Association for Cardio-Thoracic Surgery (EACTS), Vahanian A, Alfieri O, Andreotti F, Antunes MJ, Barón-Esquivias G, Baumgartner H, et al. Guidelines on the management of valvular heart disease (version 2012). Eur Heart J. 2012;33:2451–96.
Miglioranza MH, Mihaila S, Muraru D, Cucchini U, Iliceto S, Badano LP. Dynamic changes in tricuspid annular diameter measurement in relation to the echocardiographic view and timing during the cardiac cycle. J Am Soc Echocardiogr. 2015;28:226–35.
Lancellotti P, Moura L, Pierard LA, et al. European Association of Echocardiography recommendations for the assessment of valvular regurgitation. Part 2: mitral and tricuspid regurgitation (native valve disease). Eur J Echocardiogr. 2010;11:307–32.
Min SY, Song JM, Kim JH, et al. Geometric changes after tricuspid annuloplasty and predictors of residual tricuspid regurgitation: a real-time three-dimensional echocardiography study. Eur Heart J. 2010;31:2871–80.
Zoghbi WA, Adams D, Bonow RO, et al. Recommendations for noninvasive evaluation of native valvular regurgitation: a report from the American Society of Echocardiography Developed in Collaboration with the Society for Cardiovascular Magnetic Resonance. J Am Soc Echocardiogr. 2017;30:303–71.
Tribouilloy C, Enriquez-Sarano M, Bailey K, Tajik A, Seward J. Quantification of tricuspid regurgitation by measuring the width of the vena contracta with Doppler color flow imaging: a clinical study. J Am Coll Cardiol. 2000;36:472–8.
Velayudhan DE, Brown TM, Nanda NC, et al. Quantification of tricuspid regurgitation by live three-dimensional transthoracic echocardiographic measurements of vena contracta area. Echocardiography. 2006;23:793–800.
Chen TE, Kwon SH, Enriquez-Sarano M, Wong BF, Mankad SV. Three-dimensional color Doppler echocardiographic quantification of tricuspid regurgitation orifice area: comparison with conventional two-dimensional measures. J Am Soc Echocardiogr. 2013;26:1143–52.
Hahn RT, Thomas JD, Khalique OK, Cavalcante JL, Praz F, Zoghbi WA. Imaging assessment of tricuspid regurgitation severity. JACC Cardiovasc Imaging. 2019;12:469–90.
Rivera JM, Vandervoort PM, Mele D, et al. Quantification of tricuspid regurgitation by means of the proximal flow convergence method: a clinical study. Am Heart J. 1994;127:1354–62.
Cawley PJ, Hamilton-Craig C, Owens DS, et al. Prospective comparison of valve regurgitation quantitation by cardiac magnetic resonance imaging and transthoracic echocardiography. Circ Cardiovasc Imaging. 2013;6:48–57.
Hahn RT, Zamorano JL. The need for a new tricuspid regurgitation grading scheme. Eur Heart J Cardiovasc Imaging. 2017;18:1342–3.
Topilsky Y, Tribouilloy C, Michelena HI, Pislaru S, Mahoney DW, Enriquez-Sarano M. Pathophysiology of tricuspid regurgitation. Quantitative Doppler echocardiographic assessment of respiratory dependence. Circulation. 2010;122:1505–13.
Haddad F, Hunt SA, Rosenthal DN, Murphy DJ. Right ventricular function in cardiovascular disease, part I: anatomy, physiology, aging, and functional assessment of the right ventricle. Circulation. 2008;117:1436–48.
Mutlak D, Carasso S, Lessick J, Aronson D, Reisner SA, Agmon Y. Excessive respiratory variation in tricuspid regurgitation systolic velocities in patients with severe tricuspid regurgitation. Eur Heart J Cardiovasc Imaging. 2013;14:957–62.
Mutlak D, Aronson D, Lessick J, Reisner SA, Dabbah S, Agmon Y. Functional tricuspid regurgitation in patients with pulmonary hypetension: is pulmonary artery pressure the only determinant of regurgitation severity? Chest. 2009;135:115–21.
Song JM, Jang MK, Choi YS, et al. The vena contracta in functional tricuspid regurgitation: a real-time three-dimensional color Doppler echocardiography study. J Am Soc Echocardiogr. 2011;24:663–70.
Francis DP, Willson K, Ceri Davies L, Florea VG, Coats AJ, Gibson DG. True shape and area of proximal isovelocity surface area (PISA) when flow convergence is hemispherical in valvular regurgitation. Int J Cardiol. 2000;73:237–42.
Moraldo M, Cecaro F, Shun-Shin M, et al. Evidence-based recommendations for PISA measurements in mitral regurgitation: systematic review, clinical and in-vitro study. Int J Cardiol. 2013;168:1220–8.
de Agustin JA, Viliani D, Vieira C, et al. Proximal isovelocity surface area by single-beat three-dimensional color Doppler echocardiography applied for tricuspid regurgitation quantification. J Am Soc Echocardiogr. 2013;26:1063–72.
Thavendiranathan P, Liu S, Datta S, et al. Quantification of chronic functional mitral regurgitation by automated 3-dimensional peak and integrated proximal isovelocity surface area and stroke volume techniques using real-time 3-dimensional volume color Doppler echocardiography: in vitro and clinical validation. Circ Cardiovasc Imaging. 2013;6:125–33.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Song, JK., Muraru, D., Guta, AC., Badano, L.P. (2019). Functional Tricuspid Regurgitation. In: Badano, L., Lang, R., Muraru, D. (eds) Textbook of Three-Dimensional Echocardiography. Springer, Cham. https://doi.org/10.1007/978-3-030-14032-8_21
Download citation
DOI: https://doi.org/10.1007/978-3-030-14032-8_21
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-14030-4
Online ISBN: 978-3-030-14032-8
eBook Packages: MedicineMedicine (R0)