Abstract
Epithelial damage in the salivary gland (SG) resulting in irreversible dry mouth can be commonly induced by gamma radiation therapy. This radiation depletes the SG stem/progenitor cell niche slowing healing and natural gland regeneration. Biologists have been focused in understanding the development and differentiation of epithelial stem and progenitor cell niches during SG organogenesis. These organogenesis studies gave insights into novel cell-based therapies to recreate the three-dimensional (3D) salivary gland (SG) organ, recapitulate the SG native physiology, and restore saliva secretion. Such therapeutical strategies apply techniques that assemble, in a 3D organotypic culture, progenitor and stem cell lines to develop SG organ-like organoids or mini-transplants. Future studies will employ a combination of organoids, decellularized matrices, and smart biomaterials to create viable and functional SG transplants to repair the site of SG injury and reestablish saliva production.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Exocrine glands
- Salivary glands
- Radiotherapy
- Sjögren’s syndrome
- Hypofunction
- Dry mouth
- Xerostomia
- Regenerative medicine
- Tissue engineering
- Epithelial cell
- Progenitor cell
- Stem cell
- Three-dimensional cultures
- Bio-printing
Introduction
Salivary gland damage resulting in irreversible dry mouth (or xerostomia ) can be commonly induced by radiation therapy for head and neck cancers (HNC). Xerostomia is also usually observed in several systemic diseases, particularly autoimmune, such as graft-versus-host disease , Sjögren’s syndrome , granulomatous diseases, and uncontrolled diabetes among others [1].
Xerostomia is a major complication of radiation therapy (RT) , which can target more than 500,000 new cases of head and neck cancer that develop every year worldwide. Since saliva is required for food digestion, lubrication, and buffering effects and for protection against environmental hazards, xerostomia can cause various life-disturbing adverse effects, such as progressive caries, unbearable pain, oral fungal infections, speech deficits, taste loss, and swallowing impairment, which greatly impair patients’ oral and systemic health [2]. A multicenter randomized controlled trial by Nutting et al. [3] showed that the prevalence of xerostomia (grade 2 and above) can go up to approximately 40% in 12 months even after novel RT modalities are used (such as salivary gland-sparing or intensity-modulated radiation therapy). When the radiation field (during RT) lays on the salivary glands (SG), radiation injury is elicited on secretory epithelial cells , blood vessels, and adjacent nerves [4, 5]. Salivary glands consist of two types of secretory epithelial cells: 80% acinar and 20% ductal. Following RT , patients lose the majority of acinar cells with the surviving secretory cells being primarily ductal; consequently, RT will irreversibly impact salivary secretion and cause inflammatory damage and fibrosis on the long term. This radiation damage further depletes the SG stem/progenitor cell niche deterring healing and natural gland regeneration [4, 6,7,8]. Yet, no effective therapy has been devised to treat RT-induced xerostomia , and current treatment strategies are confined to the minimization of SG radiation damage or to the administration of artificial salivary substitutes and saliva secretion stimulators [2, 4].
Radiation-induced xerostomia can be an irreversible lifelong condition that will significantly affect the quality of life of cancer patients. Thus, novel and effective therapeutical strategies for SG hypofunction are required. Due to the depletion of the stem cell pool during RT damage, stem/progenitor cell therapies are vital to engender new SG secretory tissues and repair the damaged ones, for the restoration of salivary flow in xerostomia patients [9, 10].
Several biological therapies have been proposed in the last decade for SG regeneration at preclinical stages (the most relevant are summarized in Tables 9.1 and 9.2), which can involve the following biotechnology strategies :
-
1.
Implantation of SG stem/progenitor cells as salispheres into the irradiated gland to replace the functionally damaged cells [9, 24].
-
2.
Transplantation of adult stem cells (e.g., mesenchymal stem cells) with different differentiation cues in mono- or co-culture systems [25, 26].
-
3.
Tissue engineering techniques combining cells with or without environmental cues in 3D biomaterial constructs [21, 27].
-
4.
Epithelial cells can potentially be assembled as a 3D organotypic spheroid culture with capabilities to grow and mature into a secretory organ-like appearance (or organoid) [22].
Stem and Progenitor Cells
The first proof of concept study on autologous transplantation of SG cells to functionally rescue salivary hypofunction used in vitro floating spheroid-like cultures of mouse SG progenitor cells, named salispheres [9]. In vitro salisphere cultures have been shown to enrich for SG stem/progenitor cell populations that include KIT (C-KIT, CD117), Sca-1, and Mushashi-1 (Table 9.1) [9]. KIT-expressing (KIT+) progenitors are also found in other epithelial organs beside the SG, such as the prostate gland and lungs, where KIT+ progenitors have remarkable regeneration capabilities [28, 29]. In a salisphere study in mice, 100–300 KIT+ donor-derived cells isolated from the salisphere cultures were sufficient to form both new acini and saliva-transporting ductal structures, restoring the morphology and function of irradiated SG (Table 9.1) [9].
Regrettably, human major SG biopsies hold a very limited number of KIT+ progenitor cells [17]. Also, due to the heterogeneity of the KIT+ cell population, further studies have included co-expression of other putative salivary stem cell markers, such as CD24 (HSA) and CD49f (Itga6) [11]. KIT+ cells co-expressing CD24 and CD49f showed an enhanced functional recovery compared to a heterogeneous KIT+ population, which indicates that this subpopulation of KIT+ cells is enriched for SG stem/progenitor cells (Table 9.1) [11]. It is yet to be determined whether human KIT+/CD24+/CD49f+ cells have similar stem−/progenitor-like functions. Nevertheless, recently, SG sphere-derived single cells expressing high CD24 and CD29 markers (CD24hi/CD29hi) could be expanded ex vivo by fourfold after seven passages [12], though karyotypic changes (chromosome doubling) were noticed after passage 3. The same research group placed the same spheres in a 3D matrix mixture with Matrigel and collagen, and spheres differentiated in vitro into organoids with ductal/lobular structures. Upon in vivo transplantation of differentiated spheres into an irradiated mouse model, salivary flow was restored to ~46% (of pre-irradiated levels). Interestingly, undifferentiated spheres also partially restored the salivary flow, which denotes these cells may be secreting microenvironment cues that are stimulating the repair of the remaining gland [12]. Despite the abnormal chromosome number, tumor formation was not observed within 4 months (120 days) post-RT. Though, long-term follow-up studies are necessary to confirm tissues are tumor-free. Furthermore, enrichment of C-KIT+ cells within the CD24hi/CD29hi and the CD24+/CD49f+ subpopulations showed similar salivary flow outcomes [12]. The formation of acini and ductal-containing organoids from single cells is an important achievement for the field. However, this salisphere model cannot be translated into humans as it is yet to be demonstrated whether similar salispheres can be obtained from human SG biopsies and in particularly from elderly patients. Salisphere formation is in fact problematic in SG of old age mice [17].
To overcome the above limitations of salisphere-based cultures , our laboratory tested novel 3D spheroid bio-printing cell assembly systems incorporating human dental pulp stem cells expressing KIT+ with high expansion capabilities and binding/tagging them with magnetic nanoparticles [30,31,32,33,34,35,36]. Interestingly, KIT is clearly expressed in neural crest progenitors found in the dental pulp of human permanent teeth [37, 38]. These progenitors are termed human dental pulp stem cells, and our research group is enriching them to move SG cell-based therapies from mice to clinically relevant human SG organoids.
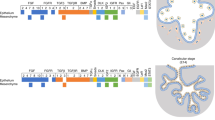
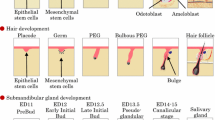
Consequently, methodologies for cryopreservation and biobanking of these progenitors have been established. Neumann and others [39] have developed a stem cell biobanking setup where salivary gland integrin α6β1+ cells have been cryopreserved in the long term without affecting their functional and genetic stability, serving as a future therapy in cancer patients. Furthermore, it is crucial to understand how progenitors proliferate and expand particularly during organogenesis. Several researcher groups have demonstrated that KIT and fibroblast growth factor receptor 2b (FGFR2b) signaling are essential for progenitor survival and expansion in the fetal submandibular gland, lung, pancreas, tooth, and skin [40,41,42].
Moreover, other putative markers that can be used to isolate SG stem/progenitor cells include K5 (Cytokeratin 5), CD29 (Itga1), CD133 (Prom1), Sca1, CD44, CD34, CD90 (Thy1), CD105, CD9, and CD81, but only few populations were proven to actively restore damaged glands [9, 11, 43,44,45]. Yet, the KIT+ cell population still appears to have the highest stem−/progenitor-like potential in mice. Analysis of regenerated SGs after transplantation of enriched KIT+ progenitor cells shows restoration of tissue homeostasis following irradiation whereby upon an increase in cytokeratin markers of epithelial ductal cells (K7, K8, K14, and K18) and in stem cell markers (KIT, CD133, CD24, and CD49f) induces normalization of vasculature and reduces fibrosis [9, 11]. Other populations of epithelial progenitor/stem cells have been found to be required for glandular branching in the developing mouse model, which are positive for K5+ [43, 46]. These K5+ progenitor cells are from neural crest and may have the potential for SG regeneration by supporting gland innervation [47].
A major obstacle in stem/progenitor cell therapies is the limited lifespan of the cells obtained from in vitro cultivation systems , hence needing to be used within a short time window. Thus, other cell culture systems and cell sources are necessary for the regeneration of salivary glands as well as systems to enrich sufficient numbers of autologous SG progenitor cells. Cell culture systems have been recently established on human minor salivary gland epithelial cells (phmSG) to achieve the maintenance of these cells in an acinar-like phenotype after optimizing growth conditions [48]. These phmSG cells displayed progenitor cell markers (K5 and Nanog) as well as acinar-specific markers such as α-amylase, cystatin C, TMEM16A, and NKCC1. After beta-adrenergic receptor stimulation, phmSG cultures exhibited calcium ion mobilization and formed an epithelial monolayer with transepithelial electrical resistance (TER) and polarization.
This study raises the question on whether the limited available number of human minor SG cells can generate enough saliva to ameliorate the irreversible hyposalivation found in several patients (post-RT, Sjögren’s, etc.). Major SG transplants (i.e., from the parotid gland) may be a more feasible option to accomplish higher salivary secretion rates [17], but they are not always available. To generate a reasonable salivary flow, larger in vitro salivary tissues are needed and, consequently, new cell sources capable of generating high cell numbers (in short-term passaging) and a matrix-rich environment [12]. Adult stem cell sources can potentially offer predictable high expansion rates, and due to their heterogeneity, they can be combined into organotypic cultures to generate larger organoids capable of restoring the salivary flow.
Adult Stem Cells
Recently, intraglandular bone marrow-derived (BM) transplants using either mesenchymal stem cells (MSC) or BM bioactive lysates have been shown to induce paracrine pro-survival effects on remaining SG tissues and to potentially induce site-specific multi-lineage transdifferentiation toward a more functional SG tissue architecture [25, 26]. For example, intraglandular transplantation of BM-MSC improves saliva production, reduces apoptosis, and increases microvessel density in irradiated mice, and transdifferentiation into acinar cells was observed [26]. Highly homogenous bone marrow clonal MSC (BM-cMSC) have recently shown potential to regenerate the SMG, although currently, the regenerative mechanisms are not well understood [25]. Earlier studies in mice have shown that granulocyte colony-stimulating factor-mobilized BM-derived cells can partially regenerate and also functionally restore an irradiated SG [49]. In addition, an in vitro study using BM stem cells (BMSCs) that are co-cultured with neonatal rat parotid acinar cells using a double chamber system showed an increase in the induction of acinar-specific α-amylase expression in BMSCs [50]. This observation indicates that BMSCs can transdifferentiate into acinar-like cells. Yet, transdifferentiation of BMSCs into acinar-like cells was found to occur only in 50% of the cells after co-culturing for 2 weeks. Further studies are still needed to test the secretory function of these acinar-like cells from bone marrow sources. Transdifferentiated BMSCs have not convincingly showed a proper secretory function in vivo.
Interestingly, studies using human adipose-derived mesenchymal stem cells (hAdMSCs) via systemic administration exhibit improved salivary flow rates 4 months after radiation therapy [51]. hAdMSC-transplanted SGs showed lesser tissue fibrosis and epithelial acinar apoptosis and higher secretory mucin and amylase levels. At 4 weeks, a large number of infused hAdMSCs were detected in vivo and were found to have differentiated, whereas in vitro, only low number of co-cultured hAdMSCs (13–18%) were found to transdifferentiate into salivary epithelial-like cells [51]. More recently, soluble signals from feeder layers of hair follicle-derived MSC (that were mitotically inactive) coupled with laminin-111 substrates supported the formation of clusters of mouse submandibular gland cells with multiple lumens [23]. This was a successful attempt to improve the differentiation and organization of SG cells, though its clinical applicability is yet to be demonstrated.
Nonetheless, three-dimensional (3D) tissue/organ constructs are still required to integrate multiple BM-derived tissues and cell lines in biomaterial constructs or extracellular matrices (ECM) under specific growth factor conditions in order to generate whole SG organ-like structures or organoids.
Three-Dimensional Tissue Engineering Strategies
A recent advancement in SG regenerative medicine showed that a bioengineered gland made from embryonic epithelium and mesenchyme can be transplanted into an adult mouse to produce a whole functional SG [13]. This bioengineered SG was composed of a variety of progenitor and stem cells, including cell from epithelial, mesenchymal, endothelial, and neuronal origins. More interestingly, the SG reconnected with the existing ductal system and possessed functional activity. The new SG was able to secrete saliva, protect the oral cavity from bacteria, and restore swallowing functions.
Thus, future research may translate these bioengineering strategies to animal models with salivary glands that have more structurally and functionally similarities to the human SG. Further studies may also focus on the usage of stem cells or adult salivary progenitors with high expansion capabilities in 3D scaffolds in order to form a bioengineered construct that grows into a functional gland in the adult microenvironment.
Salivary gland tissue engineering requires three essential components: (1) the stem/progenitor cells that retain epithelial progenitor biomarkers typical of the native salivary gland (SG ), (2) the extracellular matrix (ECM) proteins that can orchestrate the differentiation of progenitor cells into functional structures, and (3) a biocompatible and biodegradable three-dimensional (3D) scaffold that can hold these components together to recreate the microenvironment found in the native SG [27].
Since dynamic cell-ECM interactions are essential in processes such as epithelial ductal formation/branching , a recent strategy has been to engineer scaffolds that structurally and functionally resemble native ECM architecture . Three-dimensional (3D) collagen matrices have been used for homing salisphere stem/progenitor cells which form epithelial ductal structures with mucin-positive acini, indicating their capability to differentiate in response to the ECM environment [12]. Various biomaterials such as collagen type I, Matrigel, and other animal-derived products have been showing promising results in the differentiation and organization of human SG cells [12, 14, 15]; nevertheless, these biomaterials are not human-compatible. Thus, tissue engineering-based research is gearing toward the creation of xeno-free biomaterials, which can eventually be transplanted into humans.
Recently, researchers have started to utilize the soft hyaluronic acid (HA) hydrogels , which are human-compatible, as biocompatible substrates for SG tissue engineering [52]. When encapsulated in HA hydrogels, human SG cells can grow into organized spheroid structures that merge and proliferate to form larger acini-like structures with a central lumen and are maintained for long term in these gels in vitro [52]. These in vitro 3D acini-like structures also secrete α-amylase, express β-adrenergic and muscarinic receptors that activate protein transport, and induce calcium oscillations upon treatment with cholinergic stimulants. Furthermore, these 3D spheroids continue to secrete α-amylase when hydrogels were implanted in vivo in an athymic rat model [22]. However, these latter 3D structures have reversed polarity suggesting that further environmental cues from the ECM and the myoepithelial cells may be needed to reverse inside-out acini and correct the polarity.
Culture of salivary gland progenitor cells on human perlecan domain IV peptide has been shown to support the formation of 3D acini-like salivary units that express α-amylase [18]. It will be useful to incorporate the perlecan IV domain peptide into biomaterial scaffolds to mediate differentiation and correct polarity and directional secretion of the 3D salivary gland cell cultures in the future.
Other research groups have used poly(lactic)-co-glycolic acid (PLGA) , an FDA-approved constituent in implantable dental and orthopedic devices, as a synthetic material to show that it can support the attachment, proliferation, and survival of salivary gland epithelial cells [19]. The same group further shows that nanofiber PLGA scaffolds can support development and morphogenesis of intact fetal SMG organ cultures and promote natural self-organization of dissociated SMG cells into branched SG-like structures [53]. However, adult SG cells grown on flat polymeric substrates fail to form a complex 3D branching structure and are unable to assemble tight junctions that are needed for unidirectional flow of saliva. To overcome this, recent studies generated lithographically based micropatterning curved “craters” that mimic the physical structure of the basement membrane, which have increased both the surface area and allowed apicobasal polarization and differentiation of salivary gland epithelial cells [20]. An increase in aquaporin-5, a water channel protein marking acinar differentiation, was also detected in SG cells cultured on higher curvature scaffolds. Further studies with PLGA nanofibers coupled with laminin-111 and chitosan showed that laminin-111 promotes the formation of mature epithelial tight junctions and apicobasal polarization, and on the other hand, the chitosan antagonizes this phenomenon [22].
Taken together, current cell-based therapies and tissue engineering studies have provided a promising outlook to regenerate SG and restore the saliva secretory function. However, in order to test these techniques in humans, several hurdles need to be surpassed. To overcome these hurdles, further research steps should include: (1) the elimination of xenogeneic elements from transplants for feasible human use to comply with good manufacturing practices, (2) a thorough assessment of histocompatibility barriers, (3) an evaluation of long-term transplant survival and saliva secretion in larger animal models with a better SG human resemblance (i.e., pigs), and (4) an assessment of tumor sensitivity to bioengineered transplants in SG cancer models. Recent studies indicate that the above research steps are currently being pondered [18, 22, 54, 55].
Novel 3D Bio-printed Magnetic Nanotechnologies for SG Regeneration
Biomedical researchers have been moving toward cell culture technologies in 3D to better recapitulate native cellular environments and ultimately develop organotypic cultures [18, 22]. Novel bio-printing nanotechnologies have been recently developed using magnetic patterning or levitation in which cells bind with a magnetic nanoparticle assembly overnight to render them magnetic (Fig. 9.1) [30,31,32,33,34,35,36]. This nanoparticle assembly includes gold, iron oxide, and poly-l-lysine, which can easily tag via electrostatic interaction different cell types at the plasma membrane level. When resuspended in medium, a mild external magnetic field can concentrate and magnetically bio-print cells at the bottom of a cell-repellent plate , where they assemble to form larger 3D spheroids or organoids (Fig. 9.1). The resulting dense cultures can synthesize ECM and can be analyzed similarly to other 2D/3D culture systems, using assays/techniques such as cytotoxicity assays , immunohistochemical analysis , Western blotting, and other biochemical assays [56]. These 3D bio-printed systems have been recently found to recapitulate the native ECM from several tissues such as fat, lung, aortic valve, blood vessels, and breast and glioblastoma tumors [30,31,32,33,34,35,36]. Further, our research group has showed that these magnetic bio-printing systems can develop SG epithelial organoids with innervation, secretory function upon cholinergic stimulation, and epithelial polarity [57]. The apicobasal polarity in epithelial cells is essential to overcome the challenges related to the directionality of salivary flow. These SG-like organoids will provide a better understanding of human SG physiology in vitro and in vivo, in homeostatic and disease states, although these organoids still lack a robust vascular network [57]. The use of natural ECM can be a plausible alternative that can be accomplished by decellularizing organs with detergents followed by reseeding primary SG cells onto the ECM core [27, 58]. A decellularized SG can be further tested in combination with 3D bio-printed SG epithelial organoids.
The in vitro biofabrication of human SG-like transplants or organoids is crucial to:
-
1.
Generate scaled-up xeno-free biocompatible 3D structures that provide the native architecture with environmental cues to support cell growth [30, 31, 56], differentiation, and biointegration in the remaining tissues (after damage) to restore homeostasis and functionality [57, 58].
-
2.
Establish methodologies to generate SG-like organoids for scale-up production. These methodologies may need in vitro co-culture systems to integrate in a 3D architecture the cellular complexity of all human SG compartments, such as the acinar and ductal epithelia, myoepithelia, and the networks of parasympathetic nerves and lumenized ducts and vessels [55].
-
3.
Lastly, test new surgical techniques in vivo with ex vivo bio-printed SG transplants/organoids to promptly repair SG damage particularly after RT.
Conclusion
Organotypic 3D bioengineered culture systems are on the rise in regenerative medicine . These novel systems are essential to recapitulate the different cellular components of the SG and create an artificial gland for restoration of secretory function. Researchers have used floating salisphere culture systems combined or not with biomaterial 3D constructs to mimic native environments. Nevertheless, these models provided limited cellular expansion, poor acinar epithelial polarization, and skewed directionality of salivary flow. Bio-printing strategies in 3D using human cells are an avenue that has revealed promising outcomes in several types of tissue including exocrine glands [35, 57].
References
von Bultzingslowen I, Sollecito TP, Fox PC et al (2007) Salivary dysfunction associated with systemic diseases: systematic review and clinical management recommendations. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103(Suppl 57):e51–e15
Wijers OB, Levendag PC, Braaksma MM et al (2002) Patients with head and neck cancer cured by radiation therapy: a survey of the dry mouth syndrome in long-term survivors. Head Neck 24(8):737–747
Nutting CM, Morden JP, Harrington KJ et al (2011) Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol 12(2):127–136
Vissink A, Mitchell JB, Baum BJ et al (2010) Clinical management of salivary gland hypofunction and xerostomia in head-and-neck cancer patients: successes and barriers. Int J Radiat Oncol Biol Phys 78(4):983–991
Grundmann O, Mitchell GC, Limesand KH (2009) Sensitivity of salivary glands to radiation: from animal models to therapies. J Dent Res 88(10):894–903
Baum BJ (1993) Principles of saliva secretion. Ann N Y Acad Sci 694:17–23
Baum BJ, Zheng C, Alevizos I et al (2010) Development of a gene transfer-based treatment for radiation-induced salivary hypofunction. Oral Oncol 46(1):4–8
Lombaert IM, Hoffman MP (2013) Stem cells in salivary gland development and regeneration. In: Huang GT-J, Thesleff I (eds) Stem cells in craniofacial development and regeneration, vol 1. Wiley, Hoboken, pp 271–284
Lombaert IM, Brunsting JF, Wierenga PK et al (2008) Rescue of salivary gland function after stem cell transplantation in irradiated glands. PLoS One 3(4):e2063
Coppes RP, Stokman MA (2011) Stem cells and the repair of radiation-induced salivary gland damage. Oral Dis 17(2):143–153
Nanduri LS, Lombaert IM, van der Zwaag M et al (2013) Salisphere derived c-kit+ cell transplantation restores tissue homeostasis in irradiated salivary gland. Radiother Oncol 108(3):458–463
Nanduri LS, Baanstra M, Faber H et al (2014) Purification and ex vivo expansion of fully functional salivary gland stem cells. Stem Cell Reports 3(6):957–964
Ogawa M, Oshima M, Imamura A et al (2013) Functional salivary gland regeneration by transplantation of a bioengineered organ germ. Nat Commun 4:2498
Maria OM, Maria O, Liu Y et al (2011) Matrigel improves functional properties of human submandibular salivary gland cell line. Int J Biochem Cell Biol 43(4):622–631
Maria OM, Zeitouni A, Gologan O et al (2011) Matrigel improves functional properties of primary human salivary gland cells. Tissue Eng Part A 17(9–10):1229–1238
Lim JY, Yi T, Lee S et al (2015) Establishment and characterization of mesenchymal stem cell-like clonal stem cells from mouse salivary glands. Tissue Eng Part C Methods 21(5):447–457
Feng J, van der Zwaag M, Stokman MA et al (2009) Isolation and characterization of human salivary gland cells for stem cell transplantation to reduce radiation-induced hyposalivation. Radiother Oncol 92(3):466–471
Pradhan S, Zhang C, Jia X et al (2009) Perlecan domain IV peptide stimulates salivary gland cell assembly in vitro. Tissue Eng Part A 15(11):3309–3320
Jean-Gilles R, Soscia D, Sequeira S et al (2010) Novel modeling approach to generate a polymeric nanofiber scaffold for salivary gland cells. J Nanotechnol Eng Med 1(3):31008
Soscia DA, Sequeira SJ, Schramm RA et al (2013) Salivary gland cell differentiation and organization on micropatterned PLGA nanofiber craters. Biomaterials 34(28):6773–6784
Cantara SI, Soscia DA, Sequeira SJ et al (2012) Selective functionalization of nanofiber scaffolds to regulate salivary gland epithelial cell proliferation and polarity. Biomaterials 33(33):8372–8382
Pradhan-Bhatt S, Harrington DA, Duncan RL et al (2013) Implantable three-dimensional salivary spheroid assemblies demonstrate fluid and protein secretory responses to neurotransmitters. Tissue Eng Part A 19(13–14):1610–1620
Maruyama CL, Leigh NJ, Nelson JW et al (2015) Stem cell-soluble signals enhance multilumen formation in SMG cell clusters. J Dent Res 94(11):1610–1617
Sugito T, Kagami H, Hata K et al (2004) Transplantation of cultured salivary gland cells into an atrophic salivary gland. Cell Transplant 13(6):691–699
Lim JY, Yi T, Choi JS et al (2013) Intraglandular transplantation of bone marrow-derived clonal mesenchymal stem cells for amelioration of post-irradiation salivary gland damage. Oral Oncol 49(2):136–143
Tran SD, Liu Y, Xia D et al (2013) Paracrine effects of bone marrow soup restore organ function, regeneration, and repair in salivary glands damaged by irradiation. PLoS One 8(4):e61632
Aframian DJ, Palmon A (2008) Current status of the development of an artificial salivary gland. Tissue Eng Part B Rev 14(2):187–198
Leong KG, Wang BE, Johnson L et al (2008) Generation of a prostate from a single adult stem cell. Nature 456(7223):804–808
Kajstura J, Rota M, Hall SR et al (2011) Evidence for human lung stem cells. N Engl J Med 364(19):1795–1806
Haisler WL, Timm DM, Gage JA et al (2013) Three-dimensional cell culturing by magnetic levitation. Nat Protoc 8(10):1940–1949
Souza GR, Molina JR, Raphael RM et al (2010) Three-dimensional tissue culture based on magnetic cell levitation. Nat Nanotechnol 5(4):291–296
Lee JS, Morrisett JD, Tung CH (2012) Detection of hydroxyapatite in calcified cardiovascular tissues. Atherosclerosis 224(2):340–347
Daquinag AC, Souza GR, Kolonin MG (2013) Adipose tissue engineering in three-dimensional levitation tissue culture system based on magnetic nanoparticles. Tissue Eng Part C Methods 19(5):336–344
Tseng H, Gage JA, Raphael RM et al (2013) Assembly of a three-dimensional multitype bronchiole coculture model using magnetic levitation. Tissue Eng Part C Methods 19(9):665–675
Jaganathan H, Gage J, Leonard F et al (2014) Three-dimensional in vitro co-culture model of breast tumor using magnetic levitation. Sci Rep 4:6468
Tseng H, Balaoing LR, Grigoryan B et al (2014) A three-dimensional co-culture model of the aortic valve using magnetic levitation. Acta Biomater 10(1):173–182
Pisciotta A, Carnevale G, Meloni S et al (2015) Human dental pulp stem cells (hDPSCs): isolation, enrichment and comparative differentiation of two sub-populations. BMC Dev Biol 15:14
Karamzadeh R, Eslaminejad MB, Aflatoonian R (2012) Isolation, characterization and comparative differentiation of human dental pulp stem cells derived from permanent teeth by using two different methods. J Vis Exp 69:pii: 4372
Neumann Y, David R, Stiubea-Cohen R et al (2012) Long-term cryopreservation model of rat salivary gland stem cells for future therapy in irradiated head and neck cancer patients. Tissue Eng Part C Methods 18(9):710–718
Lombaert IM, Abrams SR, Li L et al (2013) Combined kit and Fgfr2b signaling regulates epithelial progenitor expansion during organogenesis. Stem Cell Reports 1(6):604–619
Petiot A, Conti FJ, Grose R et al (2003) A crucial role for Fgfr2-IIIb signalling in epidermal development and hair follicle patterning. Development 130(22):5493–5501
De Moerlooze L, Spencer-Dene B, Revest JM et al (2000) An important role for the IIIb isoform of fibroblast growth factor receptor 2 (Fgfr2) in mesenchymal-epithelial signalling during mouse organogenesis. Development 127(3):483–492
Knox SM, Lombaert IM, Haddox CL et al (2013) Parasympathetic innervation improves epithelial organ regeneration. Nat Commun 4:1494
Pradhan-Bhatt S, Harrington DA, Duncan RL et al (2014) A novel in vivo model for evaluating functional restoration of a tissue-engineered salivary gland. Laryngoscope 124(2):456–461
Rotter N, Oder J, Schlenke P et al (2008) Isolation and characterization of adult stem cells from human salivary glands. Stem Cells Dev 17(3):509–518
Knox SM, Lombaert IM, Reed X et al (2010) Parasympathetic innervation maintains epithelial progenitor cells during salivary organogenesis. Science 329(5999):1645–1647
Ferreira JN, Hoffman MP (2013) Interactions between developing nerves and salivary glands. Organ 9(3):199–205
Jang SI, Ong HL, Gallo A et al (2015) Establishment of functional acinar-like cultures from human salivary glands. J Dent Res 94(2):304–311
Lombaert IM, Wierenga PK, Kok T et al (2006) Mobilization of bone marrow stem cells by granulocyte colony-stimulating factor ameliorates radiation-induced damage to salivary glands. Clin Cancer Res 12(6):1804–1812
Lin CY, Lee BS, Liao CC et al (2007) Transdifferentiation of bone marrow stem cells into acinar cells using a double chamber system. J Formos Med Assoc 106(1):1–7
Lim JY, Ra JC, Shin IS et al (2013) Systemic transplantation of human adipose tissue-derived mesenchymal stem cells for the regeneration of irradiation-induced salivary gland damage. PLoS One 8(8):e71167
Pradhan S, Liu C, Zhang C et al (2010) Lumen formation in three-dimensional cultures of salivary acinar cells. Otolaryng Head Neck 142(2):191–195
Sequeira SJ, Soscia DA, Oztan B et al (2012) The regulation of focal adhesion complex formation and salivary gland epithelial cell organization by nanofibrous plga scaffolds. Biomaterials 33(11):3175–3186
Vissink A, van Luijk P, Langendijk JA et al (2015) Current ideas to reduce or salvage radiation damage to salivary glands. Oral Dis 21(1):1–10
van Luijk P, Pringle S, Deasy JO et al (2015) Sparing the region of the salivary gland containing stem cells preserves saliva production after radiotherapy for head and neck cancer. Sci Transl Med 7(305):305ra147
Tseng H, Gage JA, Shen T et al (2015) A spheroid toxicity assay using magnetic 3D bioprinting and real-time mobile device-based imaging. Sci Rep 5:13987
Adine C, Ng KK, Rungarunlert S, Souza GR, Ferreira JN (2018) Engineering innervated secretory epithelial organoids by magnetic three-dimensional bioprinting for stimulating epithelial growth in salivary glands. Biomaterials 180:52–66
Gao Z, Wu T, Xu J et al (2014) Generation of bioartificial salivary gland using whole-organ Decellularized bioscaffold. Cells Tissues Organs 200(3–4):171–180
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Urkasemsin, G., Ferreira, J.N. (2019). Unveiling Stem Cell Heterogeneity Toward the Development of Salivary Gland Regenerative Strategies. In: Birbrair, A. (eds) Stem Cells Heterogeneity - Novel Concepts. Advances in Experimental Medicine and Biology, vol 1123. Springer, Cham. https://doi.org/10.1007/978-3-030-11096-3_9
Download citation
DOI: https://doi.org/10.1007/978-3-030-11096-3_9
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-11095-6
Online ISBN: 978-3-030-11096-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)