Abstract
Inflammatory breast cancer (IBC) is the most lethal variant of locally advanced breast cancer and carries with it a very low survival rate of 40 % at 5 years. IBC does not present as a lump but rather mimics characteristics of an inflammation that first appears as swelling of the breast, with edema, redness, and common lymph node involvement. The physical changes in the breast are associated with the presence of nests of aggregated tumor cells, defined as tumor emboli that are encircled by lymphatic vessels, effectively blocking lymphatic drainage. Little is understood about IBC, in part due to the lack of preclinical models that recapitulate its distinct characteristics. This chapter provides an overview of our studies that have profiled all available preclinical models of IBC, including two new models recently developed, to elucidate the molecular underpinnings of this lethal variant of breast cancer. Our studies demonstrate that IBC is enriched for cells that express CD44+ and CD133+ and have aldehyde dehydrogenase-1 (ALDH1) activity, supporting a cancer stem cell/tumor initiating phenotype, associated with a very high metastatic potential to multiple distant organ sites. IBC has a distinct gene signature including E-cadherin expression with associated loss of expression of ZEB1, a transcriptional repressor of E-cadherin. IBC is also characterized by loss of expression of genes within the transforming growth factor-beta (TGFβ) signaling pathway, which is permissive for cohesive invasion by IBC tumor emboli. Taken together, these studies suggest that IBC is a very distinct variant of breast cancer characterized by epithelial plasticity, enrichment of a stem cell phenotype, and cohesive invasion as an adaptive survival mechanism, consistent with the definition of IBC as the most metastatic variant of breast cancer.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
14.1 Introduction
Inflammatory breast cancer (IBC) is the most lethal form of locally advanced breast cancer (reviewed in [1]). Although primary IBC is less commonly diagnosed than other types of breast cancer, accounting for an estimated 2–5 % of all breast cancers in the United States and an estimated 13 % worldwide, IBC is responsible for a disproportionate number of breast cancer-related deaths (7 %) that occur each year worldwide [2, 3].
A clinical diagnosis of IBC is based on the combination of the physical appearance of the affected breast, a careful medical history, physical examination, and pathological findings from a skin biopsy and/or needle or core biopsy to confirm the diagnosis of carcinoma [4]. IBC does not occur as a lump but rather is characterized by a very rapid onset of changes in the skin overlying the involved breast that include edema, redness, and swelling in over one half to two thirds of the breast and that may also include a wrinkled, orange peel appearance of the skin, defined as “peau d’orange” [1, 5, 6]. The changes in the skin of the involved breast of IBC patients are the first clinical signs of IBC and are due to the presence of tumor emboli lodged within dermal lymphatic vessels, which is one of the classical histopathological findings in IBC [7–9]. While their presence is not a requirement for a diagnosis of IBC, approximately 75 % of IBC patients have tumor emboli, and they serve as one of most distinctive characteristics of IBC.
Research to elucidate the molecular mechanisms that underlie the rapid metastasis exhibited by IBC has been hampered by the relatively rarity of the disease and an associated lack of preclinical models that recapitulate the human disease. This chapter describes the characteristics of all of the available preclinical models of IBC, including two new models that we have developed using cells derived from IBC patients that we have designated as FC-IBC01 and FC-IBC02. We describe the use of these preclinical IBC models to validate the cancer stem cell phenotype that is a characteristic of IBC. This chapter also describes gene profiling studies that have elucidated genomic signatures of IBC which provide insight into the molecular basis for the aggressive metastasis that characterize this lethal variant of breast cancer.
14.2 Characteristics of Preclinical Models of IBC
As with non-IBC breast cancers, IBC tumors can be categorized into intrinsic subtypes including luminal A, luminal B, ErbB2/Her-2+, and triple-negative breast cancers which lack ER/PR and ERBB2/Her-2. Although IBC tumors can be of any subtype, the predominant molecular subtypes are either triple-negative or ERBB2+ tumors [10–13], which is also reflected in the preclinical models of IBC.
There are currently seven preclinical models of IBC, which include SUM149, SUM190, KPL-4, MDA-IBC-3, Mary-X, and two newly developed models, FC-IBC01 and FC-IBC02. Of these preclinical models, four of these are classified as triple negative based on their lack of expression of ER, PR, and the ErBB2/Her-2 oncogene. The triple-negative IBC models include the most well-characterized IBC cell line, SUM149, as well as Mary-X, FC-IBC01, and FC-IBC02. The remaining IBC models, SUM190, MDA-IBC-3, and KPL-4 cell lines, all express the Her-2 oncogene. The prevalence of triple negative and Her-2+ in preclinical IBC models mirrors the prevalence of these subtypes in the tumors of IBC patients. The heat map of the levels of expression of genes used to subtype breast cancers, including estrogen receptor (ER), progesterone receptor (PR), and the Her-2/ERBB2 oncogene, in preclinical models of IBC is shown in Fig. 14.1.
Heat map of IBC breast cancer cell lines showing the expression of ER, PR, Her-2, and EGFR (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi:10.4172/2161-0681.1000119)
Using an expanded database of IBC patient tumors, recent studies reported that IBC patients with luminal A subtype (ER+/PR+/Her-2−) have shorter, distant-metastases-free survival intervals compared with their non-luminal IBC counterparts [10]. This is in direct contrast to observations in non-IBC breast cancers, in which patients with luminal A tumors have improved survival compared to all other subtypes of breast cancer [14]. The preclinical models of IBC are either triple negative or Her-2 amplified, which is reflective of the most prevalent subtypes of this variant of breast cancer. The observation that the worst prognosis is associated with those with a luminal A subtype of IBC underscores the need for further development of preclinical models of IBC, which will be critical to define the molecular basis for the observation of this differential lower overall survival of patients with luminal A subtype IBC.
14.2.1 Characteristics of Triple-Negative Preclinical Models of IBC
The Mary-X IBC model is a stable transplantable xenograft model developed by Dr. Sanford H. Barsky from the primary tumor of an IBC patient with triple-negative basal-like breast cancer [15–17]. Prior to 2011, Mary-X was the only preclinical model of IBC that recapitulated the formation of tumor emboli and encircling lymphatic vessels that commonly occurs in IBC patients. Mary-X grows as xenografts that appear red and highly vascularized (Fig. 14.2a). Examination of tumor tissues isolated from mice bearing Mary-X reveals the presence of multiple tumor emboli within the dermis (Fig. 14.2b, inset, and c), and metastasis readily occurs, primarily in lung (Fig. 14.2d). Mary-X tumors and tumor emboli that invade into the dermal layer of the skin (Fig. 14.2e, f) and metastatic lesions in lung (Fig. 14.2g–i) have very robust expression of the surface glycoprotein, E-cadherin. Mary-X tumor cells can only be optimally propagated as 3-dimensional tumor spheroids (Fig. 14.2j, k) and have not been successfully maintained as 2-dimensional adherent cultures on plastic. Mary-X tumor spheroids retain expression of E-cadherin (Fig. 14.2l). Our gene profiling studies identified only a ten gene difference between Mary-X tumor emboli isolated by laser capture microdissection, and Mary-X tumor spheroids [18], suggesting that the Mary-X tumor spheroids provide a convenient in vitro model with which to study characteristics of tumor emboli as well as a method to determine the ability of therapeutic agents to target tumor spheroids as surrogates of tumor emboli.
Histological characteristics of Mary-X preclinical model of IBC. (a) Mary-X tumor xenograft grows as large tumor with visible vascularization. (b) Light micrograph of H&E-stained tumor tissue isolated from Mary-X. Insets show the presence of tumor emboli in the dermis. (c) Higher magnification of Mary-X tumor tissue which contains numerous tumor emboli within the dermal Fig. 14.2 (continued) layer of the skin. (d) Mary-X tumor cells form lung metastasis visible as tumor emboli. (e) Tumor tissue isolated from Mary-X has robust expression of E-cadherin protein present in tumor emboli in the dermis (f) and in the lungs (g–i). (j) and (k) Mary-X tumor cells isolated from tumor xenografts spontaneously form 3-dimensional tumor spheroids when placed into low-adherence culture conditions. (l) Tumor spheroids in culture retain robust expression of E-cadherin (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi:10.4172/2161-0681.1000119)
In addition to the Mary-X preclinical model of IBC, we have developed two new models of IBC, designated as FC-IBC01 and FC-IBC02, derived from tumor cells isolated following thoracentesis of IBC patients who had developed metastatic pleural effusions [19, 20]. As was observed with Mary-X cells, FC-IBC01 and FC-IBC02 cells spontaneously form 3-dimensional tumor spheroids in vitro and are optimally propagated for short periods of time in low-adherence culture. When FC-IBC01 and FC-IBC02 tumor cells are injected into immunocompromised mice, tumors develop within 2–3 weeks, with the formation of IBC tumor emboli that invade into the skin and rapid metastasis to multiple sites [19, 20]. Mary-X, FC-IBC01, and FC-IBC02 tumor cells form tumor emboli that express E-cadherin protein (green fluorescence) that are encircled by lymphatic vessels that express podoplanin, used as a selective marker of lymphatic endothelium (red fluorescence) (Fig. 14.3a–c, respectively). Topro-3 was used as a marker of nuclear DNA (blue fluorescence).
(a)–(c) Triple-color immunofluorescence and fluorescence microscopy identified tumor emboli in tissues isolated from xenografts of Mary-X (a), FC-IBC01 (b), and FC-IBC02 (c) that express E-cadherin protein (green fluorescence) that are encircled by lymphatic vessels that selectively express podoplanin (red fluorescence). Topro-3 was used to identify nuclear DNA, shown as blue fluorescence (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi:10.4172/2161-0681.1000119)
The SUM149 cell line was developed in the laboratory of Dr. Stephe Ethier and colleagues [21, 22], and has been used for the vast majority of IBC studies. SUM149 cells were developed from a patient with invasive ductal carcinoma prior to receiving chemotherapy. As shown in Fig. 14.1, SUM149 cells are classified as triple-negative subtype based on the lack of ER, PR, and the Her-2 oncogene. Note that all of the triple-negative IBC cell lines, including SUM149, express EGFR. SUM149 cells do not form tumor emboli when grown as xenografts in immunocompromised mice in vivo; however, these cells do rapidly form primary tumors as well as commonly form metastatic lesions at multiple sites, including bone (Fig. 14.4a, b), lung (Fig. 14.4c), lymph nodes, liver, and soft tissues when injected via the intracardiac injection route into immunocompromised mice.
Identification of sites of metastasis in SUM149, SUM190, and MDA-IBC-3 preclinical xenograft models of IBC. (a) and (b) Luciferase-based images of the presence of metastatic lesions detected at 21–60 days following injection of SUM149 cells (5 × 106) tagged with a luciferase bioluminescent tag into mammary fat pads of NOD. Cg-Prkdcscid Il2rgtm1Wjl/SzJ mice, identifying multiple sites of metastasis of SUM149 to scapula, humerus, tibia, and pelvis. (c) Images of the presence of lung metastasis following injection of SUM149, SUM190, MDA-IBC-3, and MDA-MB-231 cells that were tagged with a luciferase bioluminescent tag, detected by bioluminescent signal in cells within isolated lungs (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi: 10.4172/2161-0681.1000119)
14.2.2 Characteristics of Her-2 Expressing Preclinical Models of IBC
The SUM190 IBC cell line was also developed from a patient with invasive ductal carcinoma prior to receiving chemotherapy [21], has amplified Her-2 [21, 22], and proliferates at a much slower rate compared with SUM149 cells, with a doubling time of ~42 h. However, when SUM190 cells are cultured under low-adherence conditions which supports formation of tumor spheroids and then injected into immunocompromised mice, SUM190 produces primary tumors as well as metastatic lesions, primarily to the lung but this occurs less frequently (Fig. 14.4c).
KPL-4 is an additional IBC cell line derived from tumor cells isolated from pleural effusion of a patient with inflammatory skin metastasis [22]. KPL-4 cells have 15-fold amplification of Her-2. When grown as xenografts, KPL-4 cells induced cachexia, which is associated with production of interleukin-6 (IL-6) [23–25], leading to the use of this model to examine the effects of therapeutic agents that block IL-6 production [23–25]. More recently, the KPL-4 model has been used to demonstrate the benefit of combining trastuzumab (Herceptin®; Genentech, South San Francisco, CA) with fluoropyrimidines or a taxane in circumstances where trastuzumab resistance has developed [26, 27]. Due to the very high passage number of KPL-4, this cell line is less commonly used in studies to identify the molecular basis of IBC.
MDA-IBC-3 cells were developed from an IBC patient with pleural effusion by serial transplantation [28]. MDA-IBC-3 cells express Her-2, and although they have a very slow doubling time (~76 h) when cultured as adherent cultures on plastic substrates, they readily form tumor spheroids when placed in low-adherence conditions and grow as xenografts when injected into immunocompromised mice. In our hands, MDA-IBC-3 cells form primary tumors but very rarely form metastatic lung tumors (Fig. 14.4c); however, they do not form tumor emboli when grown as xenografts.
14.3 IBC Is Enriched for Cells with a Cancer Stem Cell Phenotype
Studies using the Mary-X preclinical model of IBC made the initial seminal observation that 3-dimensional tumor spheroids derived from Mary-X tumor tissue have characteristics in common with embryonal blastocysts including expression of transcription factors OCT-4, NANOG, and SOX-2, which are all associated with stem cell self-renewal and embryonic pluripotency, as well as addiction to NOTCH3 [29]. Mary-X spheroids were also shown to express markers of cancer stem cells characterized by the presence of CD44+/CD24−/low and the presence of cells positive for aldehyde dehydrogenase-1 activity (ALDH1) and that express CD133. Additional evidence offered in support of IBC being enriched for cells with a cancer stem cell phenotype came from the demonstration that Mary-X tumor cells expressed genes within stem cell signaling pathways such as NOTCH3 and as few as 100 Mary-X tumor cells could recapitulate the IBC phenotype of tumor emboli formation within the skin. This study also reported that the stem cell phenotype exhibited by Mary-X was also exhibited by the lymphovascular emboli of human IBC cases regardless of the molecular subtype of the tumor, which was the first indication that IBC may be a tumor type enriched for cells with a stem cell phenotype [29]. Following these studies in the Mary-X preclinical model of IBC, Charafe-Jauffret et al. demonstrated that IBC is enriched for cells with a cancer stem cell phenotype based on detection of ALDH1 positive cells [30], which supports the clinical observation that IBC is a disease characterized by resistance to chemotherapy, early disease recurrence, metastasis, and poor clinical outcomes [31]. Our studies were the first to describe the bipotency of IBC tumor cells and also illustrated the self-renewal potential of these IBC tumor cells [32]. The results of our analysis of preclinical models of IBC revealed the presence of cancer stem cell marker CD44, which is expressed primarily by the triple-negative IBC models (Fig. 14.5a, b) and expression of CD133 by Mary-X and FC-IBC02 models of IBC (Fig. 14.5c) [32, 33]. These studies demonstrate that the triple-negative models of IBC are highly enriched for cells with a cancer stem cell phenotype compared to the Her-2+ models of IBC. We are currently using these preclinical models of IBC to define the effectiveness of agents that may target cancer stem cells, with the goal of moving the best candidates into clinical trials.
Flow cytometric detection of cancer stem cell surface markers. (a, b) Flow cytometric detection of CD44/CD24 expressed by (a) SUM149, Mary-X, FC-IBC01, and FC-IBC02 cells and (b) SUM190 and MDA-IBC-3 cells. (c) Flow cytometric detection of CD133 expression by Mary-X and FC-IBC02 cells (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi: 10.4172/2161-0681.1000119)
The expression of cancer stem cell markers coincides with the metastatic capabilities of the preclinical models of IBC. Each of the seven preclinical IBC cell systems grows as orthotopic tumors when implanted into the mammary fat pad and grows as xenografts when injected into the hind flank, with robust tumor emboli formation in the dermal lymphatics by Mary-X, FC-IBC01, and FC-IBC02 (Fig. 14.3) [33], which we did not observe in the other preclinical IBC cell systems. Additionally, we have found that all of the preclinical models of IBC form metastatic lesions at multiple sites (Fig. 14.4a–c).
14.4 Gene Signatures of IBC
As we have described above, the primary pathological hallmark of IBC is the presence of tumor emboli, which are multicellular aggregates of cells that invade into the dermal lymphatics and retain an epithelial phenotype, characterized by expression of E-cadherin (Figs. 14.2 and 14.3) [7–9, 15, 18, 33, 34]. With the goal of identifying other genes that may be associated with E-cadherin, we evaluated expression of genes involved in cell–cell aggregation and the adherens junctions. Based on whole unbiased transcriptional analysis of preclinical models of IBC, we validated the expression of CDH1, which encodes for E-cadherin with the exception of KPL-4 cells. We found that E-cadherin expression coincided with the expression by IBC tumor models of a cassette of genes including gamma (γ) catenin/JUP, p120/delta (δ) catenin, and DSC2 (Fig. 14.6a). Collectively, these genes regulate the tight homotypic aggregation of tumor cells, forming adherens junctions [35, 36], such as occurs in the cell aggregates that comprise IBC tumor emboli [33, 34]. Figure 14.6b shows the Western blot results of studies evaluating the presence of E-cadherin, DSC2, γ-catenin/JUP, and p120/δ catenin proteins in all of the preclinical models of IBC.
Analysis of genes and proteins associated with cell–cell aggregation in preclinical models of IBC. (a) Heat map showing expression of genes involved in cell–cell aggregation in preclinical models of IBC. (b) Western blot analysis of proteins involved in cell–cell aggregation in preclinical models of IBC (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi: 10.4172/2161-0681.1000119)
The observation that E-cadherin is retained in IBC cells is, at first glance, paradoxical to the current hypothesis that invasion and metastasis occurs with the loss of E-cadherin, as part of the process of the epithelial-mesenchymal transition (EMT) [37, 38]. The loss of E-cadherin during EMT favors a mesenchymal motile phenotype that is associated with acquisition of characteristics of cancer stem cells regulated by transcription factors such as TWIST1 [39]. In contrast, previous studies in models of IBC using dominant negative molecular approaches or neutralizing antibodies demonstrated that inhibiting the function of E-cadherin effectively blocked the invasion and survival of IBC tumor cells in vitro [15] and diminished the integrity of tumor emboli in vivo [15, 40]. Although E-cadherin has been demonstrated to be necessary for survival of IBC tumor cells, little is known about the transcriptional program that supports the retention of E-cadherin while exhibiting a program of accelerated metastasis.
We performed gene profiling to evaluate the genes associated with the process of EMT that were expressed by preclinical models of IBC (Fig. 14.7a). We found that the expression of CDH1, which encodes for E-cadherin, was accompanied by a loss of the zinc finger E-box binding homeobox gene, ZEB1, a transcriptional repressor of CDH1 (Fig. 14.6a), which we validated by Western blot analysis (Fig. 14.7b). In contrast, the preclinical models of IBC expressed transcription factors SNAI1 and SNAI2 and TWIST1 (Fig. 14.7a) that are known to be involved in maintenance of a stem cell phenotype [33]. To validate the loss of ZEB1 in IBC, we used laser capture microdissection techniques to specifically isolate IBC patient tumor emboli from six samples of IBC core biopsies and four samples taken from skin punch biopsies and also performed laser capture microdissection of tumor emboli taken from the Mary-X preclinical model of IBC. These studies demonstrated the loss of ZEB1 in tumor emboli and in primary tumor biopsy tissues, which was mirrored by the loss of ZEB1 in IBC cell lines (Fig. 14.6c, Table 14.1).
Analysis of EMT-associated genes and proteins in preclinical models of IBC. (a) Heat map showing expression of genes involved in EMT in preclinical models of IBC. (b) Western blot analysis of ZEB1 and vimentin proteins in preclinical models of IBC compared with non-IBC breast tumor cell lines. (c) Gene expression of ZEB1 in IBC tumor cells, non-IBC tumor cells, and tissue from primary tumor biopsy obtained from six IBC patients isolated by laser capture microdissection and in tissues isolated from tumor emboli isolated from skin punch biopsies of four IBC patients isolated by laser capture microdissection (This figure was originally published in J Clin Exp Pathol. 2012;2:119. doi: 10.4172/2161-0681.1000119)
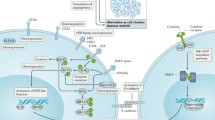
Pathway map of genes within the TGFβ signaling pathway in preclinical models of IBC, with upregulated genes shown in red and downregulated genes shown in green (This figure was originally published in J Clin Exp Pathol 2:119. doi: 10.4172/2161-0681.1000119)
Taken together, the gene signature and phenotypic characteristics that we have defined suggest that IBC exhibits characteristics of epithelial plasticity, where the tumor cells retain an epithelial phenotype through E-cadherin expression, while simultaneously expressing markers consistent with cells with a cancer stem cell phenotype and the associated expression of the transcription factors TWIST1, SNAI1, and SNAI2. The triple-negative IBC cells also express VIM, which encodes for vimentin, usually associated with the process of EMT.
While the process of EMT has become an accepted dogma, there is currently a controversy about how necessary this process is to invasion and metastasis, with very few examples of EMT identified in human tumor specimens. Recent studies suggest that EMT is not required for metastatic spread, but more often the cells express cancer stem cell markers regulated by transcription factors while maintaining an epithelial phenotype [41]. These observations are consistent with our result demonstrating simultaneous robust expression of E-cadherin and other genes associated with tight homotypic aggregation while maintaining a stem cell phenotype associated with the expression of transcription factors that is involved in maintenance of the stem cell characteristics [33, 34].
14.5 IBC Characterized by Loss of TGFβ Signaling in IBC
One of the growth factors known to induce the process of EMT is transforming growth factor-beta (TGFβ) [42]. Recent studies demonstrated that TGFβ is a key factor in the reversible regulation of motility by single cells, which in its absence, allows cells to revert to a process that has been defined as “cohesive invasion” [43]. Our gene profiling studies demonstrated that, in addition to retention of E-cadherin, preclinical models of IBC have a loss of expression of genes involved in TGFβ signaling (Fig. 14.7, Table 14.2), which is consistent with our collaborative studies reporting similar changes in IBC patient tumor tissues [10]. Since IBC tumor cells are characterized by formation of highly motile aggregates of tumor cells that migrate and invade into the dermis as a collective unit, it is perhaps not surprising that IBC is characterized by a loss of genes within the TGFβ signaling pathway and gain of genes such as SMAD6 and RUNX3 (Table 14.2), which suppress the process of EMT induced by TGFβ. The simultaneous retention of an epithelial phenotype with a lack of TGFβ signaling activation in IBC may be the molecular basis for the ability of aggregates of tumor cells to migrate into lymphatic vessels, as we have demonstrated occurs in the Mary-X, FC-IBC01, and FC-IBC02 preclinical models of IBC [19, 20, 33] and as has been demonstrated in IBC patient skin punch biopsy tissues [1, 7–9].
Interestingly, the same study reporting the loss of TGFβ signaling as permissive for cohesive invasion demonstrated that tumor cells exhibiting collective invasion due to a lack of TGFβ signaling invaded into lymphatic vessels but were incapable of hematogenous metastasis [43]. This is the pattern of metastatic spread exhibited in IBC, which favors lymphatic dissemination leading to locoregional recurrence prior to the occurrence of systemic metastasis. Collectively, the results of our gene profiling studies are consistent with observations that IBC tumor emboli primarily invade into dermal lymphatic vessels, providing a route of metastasis to local lymph nodes, which is the pattern of disease progression that is commonly observed in IBC patients. Our studies suggest that IBC tumor cells display plasticity in their gene signature that allows them to retain the epithelial phenotype, while modulating specific signaling pathways that program them to a specific lymphatic route of metastasis. Based on the high degree of plasticity exhibited in IBC tumor cells, it may be that they are capable of expressing genes within different signaling pathways, depending upon whether they display a propensity for a lymphatic or blood-borne route of metastasis.
While loss of E-cadherin has been associated with the phenotypic program of EMT characterized by increased motility and invasion similar to that of fibroblasts [37, 38], the ability to revert from a mesenchymal phenotype back to an epithelial phenotype is now believed to be necessary for colonization to form distant metastasis. Using the triple-negative breast cancer cell line MDA-MB-231, one study demonstrated that the microenvironment of the lung induced reexpression of E-cadherin associated with what was defined as mesenchymal-to-epithelial reverting transition (MErT) [44]. This phenotypic change of the MDA-MB-231 cells, which usually have a mesenchymal cell phenotype, was associated with altered cell behavior and was critical to their survival at the sites of metastasis. A recent review pointed out that there are a number of tumor types including IBC, ovarian carcinoma, and glioblastoma, which all exhibit an accelerated program of metastasis and are characterized by retention of E-cadherin and exhibiting cohesive invasion. These studies suggested that the role of E-cadherin in metastasis may be currently unappreciated [45].
Thus, the apparent dichotomy of the gene signatures of IBC that includes expression of transcription factors involved in maintenance of a stem cell phenotype while retaining an epithelial phenotype may be explained by the extreme plasticity exhibited by IBC tumor cells as one of their adaptive mechanisms for survival and accelerated rates of metastasis to multiple sites. We have identified the lack of ZEB1 expression and the loss of genes involved in the TGFβ signaling pathway that induce EMT, with expression of genes that suppress TGFβ−mediated EMT to be characteristic of all of the preclinical models of IBC. Additionally, the lack of ZEB1 expression, a known transcriptional repressor of E-cadherin, may be the molecular basis for the retention of robust E-cadherin expression in IBC, which we have previously demonstrated to be associated with the presence of microRNA 200c, which regulates E-cadherin expression [34]. Additionally, our gene profiling studies also demonstrated that preclinical models of IBC express a specific repertoire of transcription factors, including Snail and TWIST1, that allows maintenance of a cancer stem cell phenotype, which may confer a survival advantage in the face of chemotherapy and radiation as well as conferring a tumor initiating capability [33, 34].
14.6 Conclusions
Taken together, the simultaneous expression of genes in IBC that support an epithelial phenotype with suppression of expression of genes associated with a mesenchymal phenotype such as ZEB1 and TGFβ allows IBC tumor emboli to migrate as aggregates of cells into lymphatic vessels, providing a conduit for IBC tumor emboli to rapidly colonize regional lymph nodes. This program of simultaneous gain and loss of specific gene programs may be the basis for the metastatic phenotype exhibited in IBC patient, which is recapitulated in preclinical models of IBC, especially those that are triple negative and can be accurately characterized by a high degree of epithelial plasticity.
Collectively, our studies are among the first to identify that retention of E-cadherin expression in preclinical models of IBC was associated with the suppression of genes within the TGFβ signaling pathway and lack of or low expression of the ZEB1 transcription factor that are both known to be involved in the process of EMT (Fig. 14.8). These results are among the first to shed light on molecular mechanisms underlying the retention of E-cadherin observed in IBC patient tumors and on a signaling pathway that supports the retention of an epithelial phenotype, in the face of enrichment of cells with a cancer stem cell phenotype and a program of accelerated metastasis that is consistent with the disease in a patient with an IBC diagnosis. The observations for the suppression of expression of genes within the TGFβ signaling pathway are consistent with results of gene profiling of IBC patient tumors [11]. Collectively, these data provide first-time evidence that IBC is characterized by a signature of epithelial plasticity with enrichment for cancer stem cells, similar to the observations made in collaborative studies in IBC patient tumors.
References
Robertson FM, Bondy M, Yang W, Yamauchi H, Wiggins S, Kamrudin S, Krishnamurthy S, Le-Petross H, Bidaut L, Player AN, Barsky SH, Woodward WA, Buchholz T, Lucci A, Ueno N, Cristofanilli M. Inflammatory breast cancer: the disease, the biology, the treatment. CA Cancer J Clin. 2010;60(6):351–75.
Hance KW, Anderson WF, Devesa SS, Young HA, Levine PH. Trends in inflammatory breast carcinoma incidence and survival: the surveillance, epidemiology, and end results program at the National Cancer Institute. J Natl Cancer Inst. 2005;97:966–75.
Levine PH, Veneroso C. The epidemiology of inflammatory breast cancer. Semin Oncol. 2008;35:11–6.
Dawood S, Merajver SD, Viens P, Vermeulen PB, Swain SM, Buchholz TA, Dirix LY, Levine PH, Lucci A, Krishnamurthy S, Robertson FM, Woodward WA, Yang WT, Ueno NT, Cristofanilli M. International expert panel on inflammatory breast cancer: consensus statement for standardized diagnosis and treatment. Ann Oncol. 2011;22(3):515–23.
Cristofanilli M, Valero V, Buzdar AU, Kau SW, et al. Inflammatory breast cancer (IBC) and patterns of recurrence: understanding the biology of a unique disease. Cancer. 2007;110(7):1436–44.
Singletary SE, Cristofanilli M. Defining the clinical diagnosis of inflammatory breast cancer. Semin Oncol. 2008;35(1):7–10.
Kleer CG, van Golen KL, Braun T, Merajver SD. Persistent E-cadherin expression in inflammatory breast cancer. Mod Pathol. 2001;14:458–64. 561–574.
Vermeulen PB, van Golen KL, Dirix LY. Angiogenesis, lymphangiogenesis, growth pattern, and tumor emboli in inflammatory breast cancer: a review of the current knowledge. Cancer. 2010;116(11 Suppl):2748–54.
Kleer CG, van Golen KL, Merajver SD. Molecular biology of breast cancer metastasis. Inflammatory breast cancer: clinical syndrome and molecular determinants. Breast Cancer Res. 2000;2:423–9.
Van Laere SJ, Ueno NT, Finetti P, Vermeulen PB, Lucci A, et al. An integrated analysis of three distinct IBC/nIBC Affymetrix gene expression data sets further unveils the molecular biology of IBC. Cancer Res. 2011;71 Suppl 24:33s.
Iwamoto T, Bianchini G, Qi Y, Cristofanilli M, Lucci A, et al. Different gene expressions are associated with the different molecular subtypes of inflammatory breast cancer. Breast Cancer Res Treat. 2011;125(3):785–95.
Van Laere SJ, Van der Auwera I, Van den Eynden GG, Trinh X, Van Hummelen P, et al. Confirmation of the distinct molecular phenotype of inflammatory breast cancer compared to non-inflammatory breast cancer using Affymetrix based genome-wide gene expression analysis. J Clin Oncol. 2007;25(18S):21055.
Van Laere SJ, Ueno NT, Finetti P, Vermeulen PB, Lucci A, et al. An integrated analysis of three distinct IBC/non-IBC affymetrix gene expression data sets to study the transcriptional heterogeneity both between IBC and non-IBC and within IBC. J Clin Oncol. 2011;29:10571.
Voduc KD, Cheang MC, Tyldesley S, Gelmon K, Nielsen TO, Kennecke H. Breast cancer subtypes and the risk of local and regional relapse. J Clin Oncol. 2012;28(10):1684–91.
Tomlinson JS, Alpaugh ML, Barsky SH. An intact overexpressed E-cadherin/alpha, beta-catenin axis characterizes the lymphovascular emboli of inflammatory breast carcinoma. Cancer Res. 2001;61(13):5231–41.
Alpaugh ML, Tomlinson JS, Shao ZM, Barsky SH. A novel human xenograft model of inflammatory breast cancer. Cancer Res. 1999;59(20):5079–84.
Mahooti S, Porter K, Alpaugh ML, Ye Y, Xiao Y, et al. Breast carcinomatous tumoral emboli can result from encircling lymphovasculogenesis rather than lymphovascular invasion. Oncotarget. 2010;1(2):131–47.
Ye Y, Tian H, Lange AR, Yearsley K, Robertson FM, Barsky SH. The genesis and unique properties of the lymphovascular tumor embolus are because of calpain-regulated proteolysis of E-cadherin. Oncogene. 2012;32:1702–13. doi:10.1038/onc.2012.180.
Chu K, Mu Z, Alpaugh RK, Fernandez S, Freiter EM, et al. Development and comparative characterization of metastasis in newly developed pre-clinical models of inflammatory breast cancer. Cancer Res. 2011;71(24 Suppl):439s.
Fernandez SV, Robertson FM, Pei J, Aburto-Chumpitaz L, Mu Z, Chu K, Alpaugh RK, Huang Y, Cao Y, Ye Z, Cai KQ, Boley KM, Klein-Szanto AJ, Devarajan K, Addya S, Cristofanilli M. Inflammatory breast cancer (IBC): Clues for targeted therapies. Breast Cancer Res Treat. 2013;140(1):23–33. doi:10.1007/s10549-013-2600-4.
Forozan F, Veldman R, Ammerman CA, Parsa NZ, Kallioniemi A, et al. Molecular cytogenetic analysis of 11 new breast cancer cell lines. Br J Cancer. 1999;81(8):1328–34.
Ignatoski KM, Ethier SP. Constitutive activation of pp125fak in newly isolated human breast cancer cell lines. Breast Cancer Res Treat. 1999;54(2):173–82.
Kurebayashi J, Otsuki T, Tang CK, Kurosumi M, Yamamoto S, et al. Isolation and characterization of a new human breast cancer cell line, KPL-4, expressing the Erb B family receptors and interleukin-6. Br J Cancer. 1999;79(5–6):707–17.
Kurebayashi J, Yamamoto S, Otsuki T, Sonoo H. Medroxyprogesterone acetate inhibits interleukin 6 secretion from KPL-4 human breast cancer cells both in vitro and in vivo: a possible mechanism of the anticachectic effect. Br J Cancer. 1999;79(3–4):631–6.
Kurebayashi J. Regulation of interleukin-6 secretion from breast cancer cells and its clinical implications. Breast Cancer. 2000;7(2):124–9.
Fujimoto-Ouchi K, Sekiguchi F, Tanaka Y. Antitumor activity of combinations of anti-HER-2 antibody trastuzumab and oral fluoropyrimidines capecitabine/5′-dFUrd in human breast cancer models. Cancer Chemother Pharmacol. 2002;49(3):211–6.
Fujimoto-Ouchi K, Sekiguchi F, Yamamoto K, Shirane M, Yamashita Y, Mori K. Preclinical study of prolonged administration of trastuzumab as combination therapy after disease progression during trastuzumab monotherapy. Cancer Chemother Pharmacol. 2010;66(2):269–76.
Klopp AH, Lacerda L, Gupta A, Debeb BG, Solley T, et al. Mesenchymal stem cells promote mammosphere formation and decrease E-cadherin in normal and malignant breast cells. PLoS One. 2010;5(8):e12180.
Xiao Y, Ye Y, Yearsley K, Jones S, Barsky SH. The lymphovascular embolus of inflammatory breast cancer expresses a stem cell-like phenotype. Am J Pathol. 2008;173(2):561–74.
Charafe-Jauffret E, Ginestier C, Iovino F, Tarpin C, Diebel M, Esterni B, Houvenaeghel G, Extra JM, Bertucci F, Jacquemier J, Xerri L, Dontu G, Stassi G, Xiao Y, Barsky SH, Birnbaum D, Viens P, Wicha MS. Aldehyde dehydrogenase 1-positive cancer stem cells mediate metastasis and poor clinical outcome in inflammatory breast cancer. Clin Cancer Res. 2010;16(1):45–55.
Van Laere S, Limame R, Van Marck EA, Vermeulen PB, Dirix LY. Is there a role for mammary stem cells in inflammatory breast carcinoma? a review of evidence from cell line, animal model, and human tissue sample experiments. Cancer. 2010;116(11 Suppl):2794–805.
Robertson FM, Ogasawara MA, Ye Z, Chu K, Pickei R, Debeb BG, Woodward WA, Hittelman WN, Cristofanilli M, Barsky SH. Imaging and analysis of 3D tumor spheroids enriched for a cancer stem cell phenotype. J Biomol Screen. 2010;15(7):820–9.
Robertson, FM, Chu, K, Fernandez, S, Mu, Z, Zhang, X, Liu, H, Boley, KM, Alpaugh, RK, Ye, Z, Wright, MC, Luo, A, Moraes, R, Wu, H, Zook, M, Barsky, SH and Cristofanilli, M. Genomic profiling of pre-clinical models of inflammatory breast cancer identifies a signature of mesenchymal-epithelial plasticity and suppression of TGF beta signaling. J Clin Exp Pathol 2(5), 2012. http://dx.doi.org/10.4172/2161-0681.1000119.
Robertson FM, Chu K, Circo R, Wulfkuhle J, Krishanmurthy S. Genomic and proteomic pathway reveals signatures of mesenchymal epithelial plasticity in inflammatory breast cancer. In: Done SJ, editor. Breast cancer: recent advances in biology, imaging and therapeutics. New York: Intech; 2011. ISBN 978-953-307-0730-7.
David JM, Rajasekaran AK. Dishonorable discharge: the oncogenic role of cleaved E-cadherin fragments. Cancer Res. 2012;72(12):2917–23. ©2112 AACR.
Harris TJ, Tepass U. Adherens junctions: from molecules to morphogenesis. Nat Rev Mol Cell Biol. 2010;11(7):502–14. Review.
Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial-mesenchymal transitions in development and disease. Cell. 2009;139(5):871–90.
Kalluri R, Weinberg RA. The basics of epithelial-mesenchymal transition. J Clin Invest. 2009;119:1420–8.
Mani SA, Guo W, Liao MJ, Eaton EN, Ayyanan A, et al. The epithelial-mesenchymal transition generates cells with properties of stem cells. Cell. 2008;133(4):704–15.
Dong HM, Liu G, Hou YF, Wu J, Lu JS, et al. Dominant negative E-cadherin inhibits the invasiveness of inflammatory breast cancer cells in vitro. J Cancer Res Clin Oncol. 2007;133(2):83–92.
Chui MH. Insights into cancer metastasis from a clinicopathologic perspective: epithelial mesenchymal transition is not a necessary step. Int J Cancer. 2013;132(7):1487–95. doi:10.1002/ijc.27745.
Fuxe J, Karlsson MC. TGF-β-induced epithelial-mesenchymal transition: a link between cancer and inflammation. Semin Cancer Biol. 2012;22:455–61.
Giampieri S, Manning C, Hooper S, Jones L, Hill CS, Sahai E. Localized and reversible TGFbeta signalling switches breast cancer cells from cohesive to single cell motility. Nat Cell Biol. 2009;11(11):1287–96.
Chao YL, Shepard CR, Wells A. Breast carcinoma cells re-express E-cadherin during mesenchymal to epithelial reverting transition. Mol Cancer. 2010;9:179.
Rodriguez FJ, Lewis-Tuffin LJ, Anastasiadis PZ. E-cadherin’s dark side: possible role in tumor progression. Biochim Biophys Acta. 2012;1826(1):23–31.
Acknowledgements
This project was supported by the KG081287 American Airlines-Susan G. Komen for the Cure Organization (FMR, MC).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media New York
About this chapter
Cite this chapter
Robertson, F.M., Chu, K., Fernandez, S.V., Ye, Z., Barsky, S.H., Cristofanilli, M. (2013). Gene Signatures of Inflammatory Breast Cancer: Epithelial Plasticity and a Cancer Stem Cell Phenotype. In: Schatten, H. (eds) Cell and Molecular Biology of Breast Cancer. Humana Press, Totowa, NJ. https://doi.org/10.1007/978-1-62703-634-4_14
Download citation
DOI: https://doi.org/10.1007/978-1-62703-634-4_14
Published:
Publisher Name: Humana Press, Totowa, NJ
Print ISBN: 978-1-62703-633-7
Online ISBN: 978-1-62703-634-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)