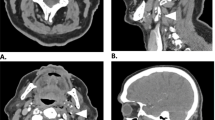
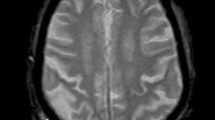
Abstract
Different modalities of instrumental neuromonitoring techniques of the risk of cerebral ischemia during carotid endarterectomy (CEA) are described. To assess the rate of ischemic complications, and provide possible solutions to decrease risk factors for carotid clamping (temporary interruption of blood flow through carotid artery during its reconstruction), the selective indwelling shunt and the use of correct intraoperative biomarkers of cerebral ischemia are especially critical. The transcranial Doppler ultrasound (TDUS) examination, cerebral oximetry (CO), and electroencephalography (EEG, evoked potentials) techniques with detailed analyses of principles, methodology, and ischemia thresholds are compared with currently available data. These monitoring modalities during awaked carotid endarterectomy in 148 patients with carotid clamping are evaluated, and potential benefits and limitations are considered for recommendations of the optimal multimodal neuromonitoring strategy based on more sensitive and specific instrumental biomarkers of cerebral ischemia.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Powers WJ, Derdeyn CP, Biller J, Coffey CS, Hoh BL, Jauch EC, Johnston KC, Johnston SC, Khalessi AA, Kidwell CS, Meschia JF, Ovbiagele B, Yavagal DR, American Heart Association Stroke C (2015) 2015 American Heart Association/American Stroke Association Focused Update of the 2013 guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 46(10):3020–3035. https://doi.org/10.1161/STR.0000000000000074
MRC European Carotid Surgery Trial (ECST) (1998) Randomised trial of endarterectomy for recently symptomatic carotid stenosis: final results of the MRC European Carotid Surgery Trial (ECST). Lancet 351(9113):1379–1387
Abbott AL, Paraskevas KI, Kakkos SK, Golledge J, Eckstein HH, Diaz-Sandoval LJ, Cao L, Fu Q, Wijeratne T, Leung TW, Montero-Baker M, Lee BC, Pircher S, Bosch M, Dennekamp M, Ringleb P (2015) Systematic review of guidelines for the management of asymptomatic and symptomatic carotid stenosis. Stroke 46(11):3288–3301. https://doi.org/10.1161/STROKEAHA.115.003390
North American Symptomatic Carotid Endarterectomy Trial C, Barnett HJM, Taylor DW, Haynes RB, Sackett DL, Peerless SJ, Ferguson GG, Fox AJ, Rankin RN, Hachinski VC, Wiebers DO, Eliasziw M (1991) Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. N Engl J Med 325(7):445–453. https://doi.org/10.1056/NEJM199108153250701
Eckstein HH (2018) European Society for Vascular Surgery guidelines on the management of atherosclerotic carotid and vertebral artery disease. Eur J Vasc Endovasc Surg 55(1):1–2. https://doi.org/10.1016/j.ejvs.2017.06.026
Guay J, Kopp S (2013) Cerebral monitors versus regional anesthesia to detect cerebral ischemia in patients undergoing carotid endarterectomy: a meta-analysis. Can J Anaesth 60(3):266–279. https://doi.org/10.1007/s12630-012-9876-4
Hajibandeh S, Hajibandeh S, Antoniou SA, Torella F, Antoniou GA (2018) Meta-analysis and trial sequential analysis of local vs. general anaesthesia for carotid endarterectomy. Anaesthesia 73(10):1280–1289. https://doi.org/10.1111/anae.14320
Jones DW, Brott TG, Schermerhorn ML (2018) Trials and frontiers in carotid endarterectomy and stenting. Stroke 49(7):1776–1783. https://doi.org/10.1161/STROKEAHA.117.019496
Liu ZJ, Fu WG, Guo ZY, Shen LG, Shi ZY, Li JH (2012) Updated systematic review and meta-analysis of randomized clinical trials comparing carotid artery stenting and carotid endarterectomy in the treatment of carotid stenosis. Ann Vasc Surg 26(4):576–590. https://doi.org/10.1016/j.avsg.2011.09.009
Noiphithak R, Liengudom A (2017) Recent update on carotid endarterectomy versus carotid artery stenting. Cerebrovasc Dis 43(1–2):68–75. https://doi.org/10.1159/000453282
Benes V, Bradac O (2018) Carotid endarterectomy and carotid artery stenting in the light of ICSS and CREST studies. Acta Neurochir Suppl 129:95–99. https://doi.org/10.1007/978-3-319-73739-3_14
Heo SH, Bushnell CD (2017) Factors influencing decision making for carotid endarterectomy versus stenting in the very elderly. Front Neurol 8:220. https://doi.org/10.3389/fneur.2017.00220
De Haro J, Michel I, Bleda S, Canibano C, Acin F (2017) Carotid stenting in patients with high risk versus standard risk for open carotid endarterectomy (REAL-1 trial). Am J Cardiol 120(2):322–326. https://doi.org/10.1016/j.amjcard.2017.04.023
Aburahma AF, Mousa AY, Stone PA (2011) Shunting during carotid endarterectomy. J Vasc Surg 54(5):1502–1510. https://doi.org/10.1016/j.jvs.2011.06.020
Khattar NK, Friedlander RM, Chaer RA, Avgerinos ED, Kretz ES, Balzer JR, Crammond DJ, Habeych MH, Thirumala PD (2016) Perioperative stroke after carotid endarterectomy: etiology and implications. Acta Neurochir 158(12):2377–2383. https://doi.org/10.1007/s00701-016-2966-2
Thirumala PD, Thiagarajan K, Gedela S, Crammond DJ, Balzer JR (2016) Diagnostic accuracy of EEG changes during carotid endarterectomy in predicting perioperative strokes. J Clin Neurosci 25:1–9. https://doi.org/10.1016/j.jocn.2015.08.014
Li J, Shalabi A, Ji F, Meng L (2016) Monitoring cerebral ischemia during carotid endarterectomy and stenting. J Biomed Res 31. https://doi.org/10.7555/JBR.31.20150171
Lareyre F, Raffort J, Weill C, Marse C, Suissa L, Chikande J, Hassen-Khodja R, Jean-Baptiste E (2017) Patterns of acute ischemic strokes after carotid endarterectomy and therapeutic implications. Vasc Endovasc Surg 51(7):485–490. https://doi.org/10.1177/1538574417723482
Chongruksut W, Vaniyapong T, Rerkasem K (2014) Routine or selective carotid artery shunting for carotid endarterectomy (and different methods of monitoring in selective shunting). Cochrane Database Syst Rev 6:CD000190. https://doi.org/10.1002/14651858.CD000190.pub3
Perini P, Bonifati DM, Tasselli S, Sogaro F (2017) Routine shunting during carotid endarterectomy in patients with acute watershed stroke. Vasc Endovasc Surg 51(5):288–294. https://doi.org/10.1177/1538574417708130
Baram A, Majeed G, Subhi Abdel-Majeed A (2018) Carotid endarterectomy: neither shunting nor patching technique. Asian Cardiovasc Thorac Ann 26(6):446–450. https://doi.org/10.1177/0218492318788777
Ben Ahmed S, Daniel G, Benezit M, Ribal JP, Rosset E (2017) Eversion carotid endarterectomy without shunt: concerning 1385 consecutive cases. J Cardiovasc Surg 58(4):543–550. https://doi.org/10.23736/S0021-9509.16.08495-0
Bendok BR, Naidech AM, Walker MT (2012) Hemorrhagic and ischemic stroke: medical, imaging, surgical and interventional approaches. Thieme Medical Publishers, Noida
Lee J, Lee S, Kim SW, Chang JW (2018) Selective shunting based on dual monitoring with electroencephalography and stump pressure for carotid endarterectomy. Vasc Spec Int 34(3):72–76. https://doi.org/10.5758/vsi.2018.34.3.72
Loftus CM (2006) Carotid endarterectomy: principles and technique. Taylor & Francis, Abingdon
Wiske C, Arhuidese I, Malas M, Patterson R (2018) Comparing the efficacy of shunting approaches and cerebral monitoring during carotid endarterectomy using a national database. J Vasc Surg 68(2):416–425. https://doi.org/10.1016/j.jvs.2017.11.077
Bennett KM, Scarborough JE, Cox MW, Shortell CK (2015) The impact of intraoperative shunting on early neurologic outcomes after carotid endarterectomy. J Vasc Surg 61(1):96–102. https://doi.org/10.1016/j.jvs.2014.06.105
Loftus CM (2015) Tips, tricks, subtleties, and superiority of carotid artery surgery. World Neurosurg 83(5):758–761. https://doi.org/10.1016/j.wneu.2013.07.091
Antoniou GA, Kuhan G, Sfyroeras GS, Georgiadis GS, Antoniou SA, Murray D, Serracino-Inglott F (2013) Contralateral occlusion of the internal carotid artery increases the risk of patients undergoing carotid endarterectomy. J Vasc Surg 57(4):1134–1145. https://doi.org/10.1016/j.jvs.2012.12.028
Banga PV, Varga A, Csobay-Novak C, Kolossvary M, Szanto E, Oderich GS, Entz L, Sotonyi P (2018) Incomplete circle of Willis is associated with a higher incidence of neurologic events during carotid eversion endarterectomy without shunting. J Vasc Surg. https://doi.org/10.1016/j.jvs.2018.03.429
Pennekamp CW, Immink RV, den Ruijter HM, Kappelle LJ, Bots ML, Buhre WF, Moll FL, de Borst GJ (2013) Near-infrared spectroscopy to indicate selective shunt use during carotid endarterectomy. Eur J Vasc Endovasc Surgery 46(4):397–403. https://doi.org/10.1016/j.ejvs.2013.07.007
Udesh R, Natarajan P, Thiagarajan K, Wechsler LR, Crammond DJ, Balzer JR, Thirumala PD (2017) Transcranial doppler monitoring in carotid endarterectomy: a systematic review and meta-analysis. J Ultrasound Med 36(3):621–630. https://doi.org/10.7863/ultra.16.02077
Wang BH, Leung A, Lownie SP (2016) Circle of Willis collateral during temporary internal carotid artery occlusion II: observations from computed tomography angiography. Can J Neurol Sci 43(4):538–542. https://doi.org/10.1017/cjn.2016.10
Kim GE, Cho YP, Lim SM (2002) The anatomy of the circle of Willis as a predictive factor for intra-operative cerebral ischemia (shunt need) during carotid endarterectomy. Neurol Res 24(3):237–240. https://doi.org/10.1179/016164102101199846
Jaffer U, Normahani P, Harrop-Griffiths W, Standfield NJ (2015) Pre-operative methods to predict need for shunting during carotid endarterectomy. Int J Surg 23(Pt A):5–11. https://doi.org/10.1016/j.ijsu.2015.09.007
Sef D, Skopljanac-Macina A, Milosevic M, Skrtic A, Vidjak V (2018) Cerebral neuromonitoring during carotid endarterectomy and impact of contralateral internal carotid occlusion. J Stroke Cerebrovasc Dis 27(5):1395–1402. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.12.030
Spence JD (2017) Transcranial Doppler monitoring for microemboli: a marker of a high-risk carotid plaque. Semin Vasc Surg 30(1):62–66. https://doi.org/10.1053/j.semvascsurg.2017.04.011
D’Andrea A, Conte M, Scarafile R, Riegler L, Cocchia R, Pezzullo E, Cavallaro M, Carbone A, Natale F, Russo MG, Gregorio G, Calabro R (2016) Transcranial Doppler ultrasound: physical principles and principal applications in neurocritical care unit. J Cardiovasc Echogr 26(2):28–41. https://doi.org/10.4103/2211-4122.183746
Shahidi S, Owen-Falkenberg A, Gottschalksen B (2017) Clinical validation of 40-mmHg carotid stump pressure for patients undergoing carotid endarterectomy under general anesthesia. J Cardiovasc Surg 58(3):431–438. https://doi.org/10.23736/S0021-9509.16.08173-8
Tan TW, Garcia-Toca M, Marcaccio EJ Jr, Carney WI Jr, Machan JT, Slaiby JM (2009) Predictors of shunt during carotid endarterectomy with routine electroencephalography monitoring. J Vasc Surg 49(6):1374–1378. https://doi.org/10.1016/j.jvs.2009.02.206
Yun WS (2017) Cerebral monitoring during carotid endarterectomy by transcranial Doppler ultrasonography. Ann Surg Treat Res 92(2):105–109. https://doi.org/10.4174/astr.2017.92.2.105
Arnold M, Sturzenegger M, Schaffler L, Seiler RW (1997) Continuous intraoperative monitoring of middle cerebral artery blood flow velocities and electroencephalography during carotid endarterectomy. A comparison of the two methods to detect cerebral ischemia. Stroke 28(7):1345–1350
Radak D, Sotirovic V, Obradovic M, Isenovic ER (2014) Practical use of near-infrared spectroscopy in carotid surgery. Angiology 65(9):769–772. https://doi.org/10.1177/0003319713508642
Huibers A, Calvet D, Kennedy F, Czuriga-Kovacs KR, Featherstone RL, Moll FL, Brown MM, Richards T, de Borst GJ (2015) Mechanism of procedural stroke following carotid endarterectomy or carotid artery stenting within the international carotid stenting study (ICSS) randomised trial. Eur J Vasc Endovasc Surg 50(3):281–288. https://doi.org/10.1016/j.ejvs.2015.05.017
Pedrini L, Magnoni F, Sensi L, Pisano E, Ballestrazzi MS, Cirelli MR, Pilato A (2012) Is near-infrared spectroscopy a reliable method to evaluate clamping ischemia during carotid surgery? Stroke Res Treat 2012:156975. https://doi.org/10.1155/2012/156975
Pennekamp CW, Bots ML, Kappelle LJ, Moll FL, de Borst GJ (2009) The value of near-infrared spectroscopy measured cerebral oximetry during carotid endarterectomy in perioperative stroke prevention. A review. Eur J Vasc Endovasc Surg 38(5):539–545. https://doi.org/10.1016/j.ejvs.2009.07.008
Samra SK, Dy EA, Welch K, Dorje P, Zelenock GB, Stanley JC (2000) Evaluation of a cerebral oximeter as a monitor of cerebral ischemia during carotid endarterectomy. Anesthesiology 93(4):964–970
Nwachuku EL, Balzer JR, Yabes JG, Habeych ME, Crammond DJ, Thirumala PD (2015) Diagnostic value of somatosensory evoked potential changes during carotid endarterectomy: a systematic review and meta-analysis. JAMA Neurol 72(1):73–80. https://doi.org/10.1001/jamaneurol.2014.3071
Thirumala PD, Natarajan P, Thiagarajan K, Crammond DJ, Habeych ME, Chaer RA, Avgerinos ED, Friedlander R, Balzer JR (2016) Diagnostic accuracy of somatosensory evoked potential and electroencephalography during carotid endarterectomy. Neurol Res 38(8):698–705. https://doi.org/10.1080/01616412.2016.1200707
Ito K, Sasaki M, Kobayashi M, Ogasawara K, Nishihara T, Takahashi T, Natori T, Uwano I, Yamashita F, Kudo K (2014) Noninvasive evaluation of collateral blood flow through circle of Willis in cervical carotid stenosis using selective magnetic resonance angiography. J Stroke Cerebrovasc Dis 23(5):1019–1023. https://doi.org/10.1016/j.jstrokecerebrovasdis.2013.08.018
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Lukshin, V.A., Usachev, D.Y., Shmigelsky, A.V., Shulgina, A.A., Ogurtsova, A.A. (2020). Preoperative and Intraoperative Markers of Cerebral Ischemia. In: Peplow, P.V., Martinez, B., Dambinova, S.A. (eds) Stroke Biomarkers. Neuromethods, vol 147. Humana, New York, NY. https://doi.org/10.1007/978-1-4939-9682-7_17
Download citation
DOI: https://doi.org/10.1007/978-1-4939-9682-7_17
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-4939-9681-0
Online ISBN: 978-1-4939-9682-7
eBook Packages: Springer Protocols