Abstract
Helminth parasites infect billions of people, primarily in the poorest countries, where they are a major cause of morbidity. Despite extensive organismal diversity within the helminth parasite grouping, these pathogens are united in inducing type 2 immune responses. Type 2 immunity, in which innate cells such as basophils, eosinophils, mast cells, and type 2 innate lymphoid cells are engaged, and adaptive immune responses that include T helper 2 (Th2) cells, T follicular helper (Tfh) cells, and B cells, are essential for resistance to, or survival with, helminth infections. The core cytokines made during these responses are IL-4 and IL-13, and through their effects on other cells such as macrophages and goblet cells, they together or separately orchestrate effector functions that mediate parasite expulsion or killing, as well as the healing of tissue damage caused by the parasites. Detrimental side effects of type 2 immunity, such as tissue fibrosis, develop during chronic helminth infections but are rarely fatal since hosts and parasites have evolved mechanisms to regulate these processes to favor survival of both parties.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Helminth parasites are multicellular pathogens from two distinct phyla—the Platyhelminthes (flatworms) and Nematoda (roundworms). As a group they infect billions of people, largely in the poorest parts of the world where infection transmission is supported by underdeveloped sanitation and poor vector control [1]. While helminth infections have relatively low fatality rates they are increasingly recognized to be the cause of severe morbidity, and as such have recently gained heightened recognition as important but neglected tropical diseases [2, 3].
Despite enormous organismal heterogeneity and life cycle complexity amongst parasitic helminths, these pathogens are united immunologically by the fact that they nearly always induce pronounced Th2 immune responses. The origins of our understanding of this fact date to the observations that elevated IgE levels and eosinophilia are strong indications of helminth infections (see [4–6]). In the 1980s it became clear that the expression of IL-4 and IL-5, cytokines that control immunoglobulin isotype class switching to IgE in B cells, and increased eosinophil release from the bone marrow and survival in the periphery, are linked and characteristic of a subset of CD4+T cells defined as T helper type 2 cells (Th2 cells) [7]. From this finding, it was a relatively straightforward step to the realization that the dominant response to helminth parasites was likely to be Th2 in nature [8]. Helminth infections are often chronic, and sometimes associated with the development of severe pathology, and early work linked Th2 response development during infection with the parasitic flatworm Schistosoma mansoni to the onset of disease [9, 10], so there was initially some debate as to whether Th2 responses serve any protective function in the context of helminthic disease [11]. However, it quickly became clear that Th2 cells regulate a spectrum of protective responses that allow animals to eradicate, or live with, helminth parasites [12–15].
The “Th2 Response”: Innate and Adaptive Components
Put most simply, Th2 cells are MHC class II restricted CD4 T cells which make physiologically relevant levels of IL-4, IL-5, and/or IL-13. In humans and mice, the IL-4 allele is in a clustered locus with IL-5 and IL-13 and although each allele can be expressed independently, all three are often coordinately regulated, such that production of these “Th2 cytokines” is considered to be a mark of a Th2 response [16, 17]. In detail, the situation is more complex and the production of IL-4, IL-5, and IL-13 is often accompanied by the expression of additional genes, such as Il9, Il10, and Areg, that add to the overall Th2 signature (e.g. [18, 19]). While IL-4 is not strictly necessary for the development of Th2 cells, it is strongly supportive of the expansion and establishment of Th2 cell responses [20]. Th cells were named based on their perceived role in helping B cells to make antibody, and the production of IgG1 and IgE by B cells requires T cell help including the provision of IL-4, and increased amounts of specific and non-specific antibodies in these classes typify helminth infections [21]. It is now clear that a subset of Th cells, T follicular helper (Tfh) cells, which differ from naïve or effector cells in being specialized to enter B cell follicles and germinal centers, is specialized for helping B cells [22]. In helminth infections these cells share with Th2 cells the ability to make IL-4 (thus accounting for their ability to induce class switching to IgG1 and IgE production) but additionally produce IL-21 [23–25], a cytokine that is critical for plasma cell differentiation.
Helminth infection-induced immune responses in which Th2 cells are prominent are best considered “type 2” responses, since they are usually characterized by the additional participation of a range of cells of the innate immune system, including eosinophils, basophils, mast cells, and type 2 innate lymphoid cells (ILC2s), all of which have the potential to produce one or more of the canonical Th2 cytokines [26–30].
The Protective Roles of Type 2 Responses During Helminth Infection
Immunity to helminth infections is manifested in at least three ways (Fig. 1): (1) The resolution of a primary infection; (2) Resistance to reinfection; and (3) Protection of vital functions during chronic, immunologically unresolvable infection. Specific examples of these types of immunity will be discussed below. Functionally, protective responses in each of these categories are largely mediated by the direct or indirect effect of type 2 cytokines on other cells, which assume effector functions under their influence. The primary effector cells of immunity to helminth infections are B cells (the antibody products of which can work in conjunction with other cell types), macrophages, granulocytes, epithelial cells, and muscle cells.
Immunity to helminth infections is manifested in at least three ways. (a) The resolution of a primary infection. Some intestinal nematodes are killed as a result of the effects of IL-4/IL-13 produced by innate type 2 cells and Th2 cells on intestinal epithelial cells, including goblet cells, and on associated musculature. (b) Following drug treatment of some helminth infections, hosts are resistant to reinfection. Immunity may be mediated by cytokines from Th2 cells and cooperating innate system cells, through mechanisms similar to those that mediate resolution of primary infection, but enhanced by faster kinetics associated with the secondary immune response. Immunity is additionally more potent in some cases because of antibody that has developed as a result of initial infection and clearance, and because of the rapid recruitment of cells such M2 macrophages to the immune reaction that targets incoming larval parasites and prevents their establishment. (c) Protection of vital functions during chronic, immunologically unresolvable infection. In these settings, the immune response promotes tissue repair and sequesters parasites and any toxic molecules that they may make (indicated by the lightning symbol). In these settings, excessive tissue damage is prevented by immune system intrinsic regulatory mechanisms and immunomodulatory molecules released by the parasites themselves
Resolution of Primary Infection
The resolution of primary infection is perhaps the exception rather than the rule since many parasitic helminths cause chronic infection—indeed, chronicity is often considered a hallmark of helminth infection. Nevertheless, various intestinal nematodes, including the whipworm Trichuris muris and the hookworm Nippostrongylus brasiliensis, are immunologically expelled by murine hosts shortly after adult worms establish in the intestine and initiate egg production (Fig. 1a). These protective responses are often heavily dependent on the early production of IL-13 and/or IL-4, and the ability of these cytokines to stimulate intestinal smooth muscle contraction [31, 32], altered intestinal epithelial cell function leading to increased luminal fluid flow [33, 34], increased epithelial cell turnover [35], and goblet cell expression of effector RELMβ, which inhibits parasite feeding and chemotaxis [36, 37], and Muc5ac, which is directly detrimental to T. muris and N. brasiliensis, as well as to another intestinal nematode Trichinella spiralis [38] (Fig. 2). Together these effects lead to worm expulsion. These processes can be stimulated by IL-4/IL-13 made by innate type 2 cells, or by Th2 cells and therefore additionally play essential roles in the spectrum of protective responses from those that begin to work during early primary infection to those recalled in immune animals upon re-exposure to infection. Interestingly, the ability of innate type 2 cells to participate in resolution of primary infection, as discussed below, is dependent on the presence of CD4+ T cells (discussed in [28, 39]). Thus there is an intimate reciprocal link between innate and adaptive immunity during the development of responses that will lead to expulsion of primary infections and resistance to secondary infection.
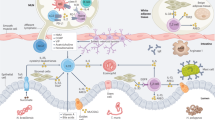
Innate and adaptive type 2 immunity is tightly integrated. Innate responses to helminth parasites can be initiated by epithelial cell damage, leading to the production of the alarmins IL-25, IL-33, and TSLP. IL-25 and IL-33 can activate ILC2s to make IL-13 (but not IL-4), which has marked effects on epithelial cell (EC), goblet cell (GC), and muscle cell biology that together can promote the expulsion of intestinal parasites. IL-13 also alternatively activates macrophages, which can then proliferate and begin making mediators that lead to parasite damage, but which also promote tissue healing and regulate Th2 cell responses to prevent overt immunopathology. TSLP made by epithelial cells can promote basophil hematopoiesis and activation, and by inhibiting IL-12 production by DCs promotes the induction of Th2 cell responses. Many helminths also produce molecules that limit the ability of DCs to make IL-12. T-cell response initiation involves the extensive proliferation of T cells that are specific for the target antigens and the emergence of Th2 cells that make IL-13 and IL-4, and of Tfh cells that make IL-4 and IL-21 and are specialized to help IgG1 and IgE B-cell responses. Th2 cells can move into sites of infection where the cytokines that they make perpetuate effects on epithelial cells, muscle cells, and macrophages initiated by ILC2s. T cells also sustain ILC2 populations. Eosinophils are not depicted in this figure. However, these cells participate in type 2 immunity due to the strong production of IL-5 by ILC2s and Th2 cells. Mast cells are also absent from the figure, but would be expected to participate in type 2 responses. Mediators in red have been shown to have detrimental effects on helminth parasites. PC plasma cell. Areg amphiregulin, a cytokine made by Th2 cells and ILC2s that promotes epithelial cell turnover
Innate type 2 cells are present in naïve mice, poised to produce Th2 cytokines upon appropriate stimulation, and are mobilized within hours/days during the early stage of the response to helminth parasites. Because of the kinetics of the innate type 2 response, which occurs at a time when the adaptive Th2 response is at its very earliest stage of development, there has been a focus on whether the cells that make up this response are able to mediate innate protective responses against helminths and/or to help promote Th2 cell responses, by perhaps secreting IL-4 and/or IL-13. Of special current interest in this regard are ILC2s (Fig. 2). Discovered only recently, these cells are derived from lymphoid progenitors, but do not express markers of other immune cell lineages, or clonotypic antigen receptors [40–42]. ILC2s produce IL-5 and IL-13, exist throughout the body and play important homeostatic roles (e.g. [43]). However, ILC2s can become activated and increase in numbers in response to helminth infection, a response that is mediated by IL-25 and IL-33 [28, 40–42]. These cytokines are released by epithelial cells (and possibly other cells such as mast cells and macrophages) in response to necrotic damage or other signals (e.g. Trefoil Factor 2 [44]), and through their effects on ILC2s acts as “alarmins” to initiate innate responses [28] (Fig. 2). Conceptually, this mode of action fits well with the idea of intestinal or skin epithelial surfaces being broached by invading or migrating helminth larvae. Indeed, ILC2s are engaged rapidly following infection with N. brasiliensis [42, 45], and stimulated by IL-25 released by intestinal epithelial cells [46]. In the absence of IL-25, or IL-25R, mice have fewer ILC2s and exhibit delayed parasite expulsion kinetics [41, 45]. However, injection of IL-25 into infected WT mice or transfer of activated WT ILC2s into infected IL-25R-deficient infected mice is sufficient to mediate rapid expulsion through an IL-13-dependent mechanism [41, 45]. Interestingly, in mice lacking the IL-33R (T1/TS2), or in which T1/TS2 is blocked, expansion of the ILC2 population following infection with N. brasiliensis fails to occur, and the mice are unable to rapidly clear the parasite [41, 44], indicating that despite their similar roles in promoting ILC2 activation, IL-33 and IL-25 must each have essential non-redundant functions in immunity, although what these are is currently unclear. IL-33 has also been shown to play a role in immunity to the nematode parasite to T. spiralis [47], and to be able to induce immunity to T. muris [48].
Multi-potent projenitor type 2 cells (MMPtype 2), IL-25-dependent but T1/ST2-negative and IL-33-independent cells associated with type 2 immunity but distinct from ILC2s, have been implicated in resistance to T. muris [49, 50]. As their name suggests, these cells have the potential to differentiate into other cell types, including basophils, monocytes, mast cells, and macrophages, and are thought to promote the expression of Th2 immunity in part through extramedullary hematopoiesis to produce cell types that contribute to protection.
Basophils, circulating cells that enter tissues from the blood, are also activated early following helminth infection during which they can rapidly accumulate in affected tissues and enter reactive lymphoid organs [51]. Based on the outcome of depletion by antibodies directed at the FcεR, basophils were implicated as antigen-presenting cells responsible for activating naïve CD4+ T cells during the development of Th2 responses following infection with helminths [52]. However, the more recent use of engineered mice in which basophils are deleted with high specificity has shown that these cells are dispensable for polarized Th2 responses elicited by N. brasiliensis or S. mansoni [53]. Nevertheless, IL-4 and IL-13 from these cells contribute to the expulsion of primary N. brasiliensis infection [54]. Basophils also play an important role in the clearance of primary T. muris infection [55]. Immunity to this parasite is dependent on TSLP, another alarmin made by epithelial cells. In contrast to the situation in WT mice, peripheral basophil numbers along with Th2 responses and associated downstream effector functions (discussed below) fail to develop in infected Tslpr −/− mice, and adult parasites persist as a chronic infection. However, transfer of WT basophils into infected Tslpr −/− mice is able to partially restore the spectrum of type 2 immune responses and resulting worm expulsion [55]. This study revealed that TSLP can selectively promote basophil hematopoiesis and the emergence of a population of basophils that differs transcriptionally from basophils elicited by IL-3 (Fig. 2). TSLP has other important functions in Th2 immunity, as discussed further below.
Mast cells are found throughout the body, especially adjacent to epithelia. Mastocytosis is a common feature of helminth infections [56], and mast cells have been implicated in resistance to the nematodes T. spiralis [57] and Strongyloides spp. [58, 59]. There is recent evidence that mast cell-deficient mice have diminished Th2 responses and are more susceptible to primary infection with T. muris and to the trichostrongyle nematode H. polygyrus (once known as Nematospiroides dubius, and more recently referred to as H. polygyrus bakeri) [60], due to a failure of ILC2 activation resulting from a deficit in IL-25, IL-33, and TSLP production by epithelial cells. Thus mast cells may play an important role in initiating type 2 immunity by provoking the production of alarmins, although the mechanism underlying this response is unclear at present.
Resistance to Reinfection
The second important role for type 2 responses in helminth infection is in adaptive immunity to reinfection. This is well illustrated by infection with H. polygyrus. Primary infection in mice with this intestinal nematode can be chronic even when the host mounts a type 2 response, but in these cases chemotherapy leaves the cured host immunologically resistant to secondary infection [61] (Fig. 1b).
There is a long-standing recognition that, while IL-4 and IL-13 made by memory Th2 cells may contribute heavily to resistance to secondary H. polygyrus infection by directly modulating epithelial cell, muscle cell, and macrophage responses [62], antibody is also playing a crucial role in adaptive immunity in this system [21]. Thus μMT mice and JhD mice, which lack B cells, and AID mice, which have B cells but are unable to secrete antibodies, are unable to resist secondary infection with H. polygyrus, despite developing what for the most part appear to be normal Th2 responses [63–65]. Moreover, IgG1 antibody from animals immune to H. polygyrus is able to passively confer immunity to naïve animals [63, 65, 66], and mice deficient in IL-21 fail to develop IgG1 secreting plasma cells and subsequently are unable to resist reinfection following drug cure [67]. Antibodies are also recognized to be important for protection against primary infection with T. spiralis, or H. polygyrus following maternal transfer in milk from immune mothers to offspring [68, 69].
Parasite-specific antibodies have also been shown to be capable of conferring protection against a broad spectrum of other helminth infections following experimental passive transfer, even in cases where there is not demonstrable role for antibody in naturally acquired immunity (reviewed in [21]). However, some of these findings have been difficult to reproduce, a problem that may be ultimately due to differences in antibody titer between different experiments. This would be consistent with the fact that there is a correlation between the efficacy of immune serum in passive immunization and the number of times the donor animals have been infected/boosted [21, 61], since titer would be expected to rise with each boost. In a real world setting, the role of immunologic boosting due to the death of existing parasites and reinfection has been postulated in human immunity to infection against schistosomes [70, 71]; in this infection, resistance can develop following drug treatment, and is correlated with the amount of IgE antibody against key parasite antigens [72].
Antibodies exert protective roles through a variety of mechanisms that vary depending on the infection and life stage targeted. For example, in the intestine, antibodies promote the entrapment of T. spiralis worms in mucus, leading to expulsion [73], whereas in tissues antibody can mediate FcR-dependent cytotoxic effects by neutrophils and eosinophils, as illustrated in the case of immunity to the nematode Strongyloides stercoralis [74]. In H. polygyrus infection, antibodies associated with FcR on basophils allow the antigen-specific production of IL-4/IL-13 during challenge infection [75], leading to the induction of protective intestinal responses linked to the activation of epithelial cells, goblet cells, and muscle cells (Fig. 2), which together promote expulsion of worms from the gut [15]. Moreover, basophils can mediate protection against secondary infection with N. brasiliensis independently of Th2 cells [76].
In addition to antibody, macrophages also play a crucial role in immunity to H. polygyrus. These cells exist throughout the body as resident components of most tissues. These cells are embryonically derived, seeded into tissues in utero, and maintained by in situ proliferation [77, 78]. It is well established that during inflammation, additional macrophages of hematopoietic origin can develop from monocytes recruited from the bone marrow [77]. Macrophages play crucial roles in immunity and can adopt different activation states depending on context. Interferon-γ in combination with TLR agonists promotes M1 (or classical) activation, whereas IL-4 and IL-13 promote M2 (or alternative) activation by the IL-4Rα [79, 80]. From the host defense standpoint, M1 macrophages are inflammatory. In contrast, M2 macrophages are pro-angiogenic and pro-fibrotic, and make a range of molecules that serve to modulate inflammation, promote tissue repair, and regulate adaptive immunity [80, 81] (Fig. 2). Recent work has revealed that increases in macrophage numbers at sites of infection with helminth parasites can additionally, or exclusively, be driven by IL-4-stimulated proliferation of local macrophages [82] (Fig. 2), a finding that has spurred significant re-examination of the origin of these cells in different inflammatory settings.
M1 macrophages can kill growing schistosomes, and may be important for immunity to these pathogens in certain experimental vaccination settings where deliberately induced Th1 responses are protective [83]. However, M2 macrophages dominate during naturally developing type 2 responses during helminth infection, and play a significant protective role in some instances, such as H. polygyrus infection. In this case, ingested infectious larvae invade the intestinal wall before emerging into the intestinal lumen to grow into adult parasites. Whilst in their tissue invasive life stages, the parasites become foci of granulomatous inflammation, which by definition involves macrophages. Global deletion of macrophages during this period of a challenge infection in infected and cured mice effectively ablates protective immunity [62]. Immunity in this setting is sensitive to inhibition of arginase1, which is strongly expressed by M2 macrophages, and it appears as though larvae are being killed through a mechanism that induces metabolic stress [62]. M2 macrophages also play a role in inducing the IL-4/IL-13-dependent smooth muscle contractions that lead to the expulsion of N. brasiliensis worms [31].
Recently, M2 macrophages were shown to be capable of cooperating with neutrophils to kill S. stercoralis larvae in vivo [84]. While not restricted to roles in type 2 immunity, neutrophils do participate in inflammation associated with helminth infections [15], playing a role in the promotion of type 2 immune responses during N. brasiliensis infection, for example [85]. However, they can assume pathologic roles in settings where type 2 immunity is less robust and Th17 responses emerge. This has been well documented in mouse strains which are genetically susceptible to developing acutely lethal disease when infected with S. mansoni, and in strains which normally develop chronic infection with this parasite, but which have been immunized prior to infection with schistosome egg antigens in complete Freund’s adjuvant [86, 87].
The Protection of Vital Functions During Chronic Infection
The third role for protective type 2 responses is to allow host survival during chronic infection (Fig. 1c). This is the case during infection with the parasitic flatworm S. mansoni. Despite mounting a strong type 2 response during infection with this parasite, the host is unable to clear infection, which consequently is chronic. Nevertheless, loss of function of IL-4 in this system leads to severe morbidity and death associated with excessive inflammation in the absence of any increase in infectious burden [14]. During infection with this organism, eggs produced by the parasites (living in the portal vasculature) can become trapped in the sinusoids of the liver where they act as foci for CD4+ T-cell-dependent granulomatous inflammation, a process that serves a critical host-protective role by participating in the sequestration of parasite eggs and the toxins that they secrete [88]. In the absence of IL-4 or IL-4Rα, schistosomiasis is acutely lethal [14, 89, 90], and this phenotype is recapitulated in mice that lack IL-4Rα expression on macrophages [89]; this indicates that the protective effects of IL-4 are mediated by macrophages and therefore, presumably, that M2 activation is critical. A failure to heal damage caused by the transit of parasite eggs into the gut lumen appears to be at least partially responsible for increased morbidity and mortality in the absence of M2 macrophages, although the emergence of M1 macrophages and associated inflammation also appears to play a contributing role [89]. A role for M2 macrophages in controlling acute tissue damage has also been noted in mice infected with the N. brasiliensis. Following transcutaneous infection, larval N. brasiliensis migrate through the lungs prior to entering the digestive system and maturing as adult worms in the intestine. In wild-type mice, pulmonary migration is associated with rapidly developing hemorrhage, inflammation, and reduced lung function, that resolves coincidently with the appearance of M2 macrophages at the site, but fails to resolve and rather is lethal in mice that lack IL-4Rα or are depleted of macrophages [91].
M2 macrophages also play an important role in regulating the intensity of the immune response to the benefit of the host. Several IL-4-induced genes are implicated in this process. For example, in S. mansoni infection, Relmα negatively regulates CD4+ T-cell responses and in so doing prevents the development of severe type 2-associated immunopathology [92, 93] and Arginase1 produced by macrophages suppresses Th2 cell cytokine production and associated downstream inflammation and fibrosis [94, 95]. Moreover, following exposure to the filarial nematode Brugia malayi, M2 macrophages develop the ability to potently suppress the proliferation of other cells through a cell contact-dependent mechanism that is presumably distinct from those mediated by Arginase1 or Relmα [96].
In the steady state, eosinophils have a clear role in adipose metabolic homeostasis [97]. During infections with helminths they increase in number and accumulate at tissue sites of invasion and inflammation. However, it has been difficult to assign eosinophils a defining role in either immunity or immunopathology commensurate with the magnitude at which they are involved in the response, and there remains a sense that the primary role of these cells during infection is yet to be discovered. Nevertheless, eosinophils have been shown to be capable of killing helminth larvae of various types [98], and can, along with M2 macrophages, make mediators such as Relmα, that regulate the intensity of type 2 inflammation [92].
The Modulation of Th2 Responses and Associated Inflammation During Chronic Helminth Infection: Everyone Benefits?
During chronic helminth infections caused by schistosomes and by filarial nematodes, Th2 responses peak during early stages of infection and then decline despite the fact that parasites, and therefore parasite antigens, persist [99–102] (Fig. 3). This process is reminiscent of the development of CD8+ T-cell exhaustion during chronic viral infection [103]. It has been argued that loss of Th2 cell function over time in helminth infections reflects the development of adaptive immunologic tolerance to parasite antigens [104], resulting from persistent antigenic stimulation [105], and/or extrinsic processes in which hyporesponsiveness is imposed by other cells such as M2 macrophages (discussed above, and [106]) or regulatory T (and B) cells (discussed by Maizels in “Regulatory T Cell Control of Type 2 Inflammation”, and [107, 108]) (Fig. 3). The regulatory cytokines TGFβ and IL-10 have been implicated in this process [109], and IL-10 serves the additional function of suppressing residual Th1 responses that can occur in certain helminth infections, and therefore further polarizes the adaptive response in the Th2 direction [110, 111] (Fig. 3).
The modulation of Th2 responses and associated inflammation during chronic helminth infection. Th2 cell responsiveness declines during chronic antigen despite the persistence of parasites. Immunomodulation does not reflect the loss of Th2 cells, but rather their regulation by M2 macrophages, Treg and Breg cells, cytokines, inhibitory receptor ligation, and parasite-derived molecules
Downregulation of Th2 responses during chronic infection is generally thought of as being advantageous in settings where the immune response is incapable of clearing the infection and Th2 cells are causing immunopathology. This is the case in schistosomiasis, where despite the fact that the type 2 response plays a vital tissue-protective role there is a risk that the inflammatory and wound healing components of this type of immunity can themselves become pathological. Specifically, ongoing schistosome egg deposition and focused production of the pro-fibrotic cytokine IL-13 (which is linked to protective IL-4 production) in the liver can lead to severe fibrosis with portal hypertension [112]. In the absence of appropriate regulatory mechanisms, these processes can become overwhelmingly damaging (e.g. [94]).
Antibody can also play a protective role during helminth infection by regulating inflammation [21]. This is apparent in chronic S. mansoni infection in B-cell-deficient mice, in which immunopathology is exaggerated, leading to greater morbidity and mortality than is the case in infected wild-type mice [113]. Mechanistically, immunoregulation by antibody is likely to reflect the binding of IgG1-containing immune complexes to macrophages [114], with resultant anti-inflammatory effects, since in other systems macrophages that interact with immune complexes assume marked regulatory roles [115, 116], by producing IL-10 and TGF-β1, two cytokines which play important roles in regulating inflammation during schistosomiasis [117]. More broadly, the roles of B cells and antibody in survival during chronic schistosomiasis may reflect a mechanism analogous to that mediated by intravenous immunoglobulin therapy (IVIG), which is used successfully in humans for the treatment of autoimmune diseases [118]. Recent work has shown that the canonical type 2 cytokine IL-4 induces the increased expression of FcγRIIB on monocytes in humans and mice, and that mice which lack IL-4 or FcγRIIB are not protected against inflammation by IVIG [119].
In some cases, Th2 response downregulation favors parasite persistence. For example, reversal of hyporesponsiveness by blockade of the inhibitory receptor PD-1 expressed by Th2 cells during chronic infection with the filarial worm Litomosoides sigmodontis infection allows the expression of effective antiparasite immune responses [120]. The realization that type 2 immunity is often tightly regulated during helminth infections, and that these processes can favor parasite survival, led to the realization that parasites are able to produce molecules that strongly influence the immune response [121] (Fig. 3). The characterization of these molecules, and the possibility that they might be developed for therapeutic use in conditions where immune responses (particularly type 2 responses) are pathogenic, such as allergy and asthma, is a subject of considerable current interest (discussed by Loukas in “Developments in the Design of Anti-helminth Vaccines,” and [122]). The fact that many inflammatory conditions are alleviated by helminth infection attests to the promise of this approach [123].
How Do Helminth Antigens Promote Type 2 Responses?
One of the greatest advances in our understanding of the how type 2 immunity develops following exposure to helminth parasites has come from recent work on the “alarmins,” IL-25, IL-33 and TSLP, cytokines made by damaged or activated epithelial cells that trigger innate immune responses and help orchestrate complementary adaptive immune responses (Fig. 2). IL-25 and IL-33 have been discussed above. The third alarmin, TSLP, has at least 2 known functions in type 2 immunity. The first is to suppress IL-12 production, thereby favoring the induction of Th2 responses [124]. TSLP is critical for type 2 response development during infection with T. muris [55, 124] but not during infection with H. polygyrus, N. brasiliensis [125] or S. mansoni [126], which may reflect differences in the inherent abilities of these parasites to suppress the production of IL-12 by DCs [125]. The second function of TSLP is to promote basophil hematopoiesis that is independent of IL-3, the cytokine conventionally associated with basophilia [55]. Wild-type basophils induced by TSLP, which are functionally distinct from IL-3-elicited basophils, are capable of restoring immunity to T. muris in otherwise susceptible Tslpr−/− mice [55].
The fact that IL-4 is essential for Th2 cell differentiation in vitro led to much speculation that an innate source of IL-4 would be critical for Th2 cell development in vivo, and consistent with this there have been many reports that type 2 innate cells are key players in Th2 cell activation. However, early observations showed that DCs exposed to helminth antigens preferentially induce Th2 cell differentiation, suggesting that despite the ability of many other cell types to contribute to type 2 immunity, direct contact of parasite products with these APCs is sufficient for Th2 polarization [127, 128]. The subsequent establishment of the primary importance of DCs in Th2 response development during helminth infections [129, 130], and the molecular identification of helminth products such as nematode chitin [131], and S. mansoni Omega 1, that possess Th2 adjuvanticity and are, at least in the case of the latter, able to drive Th2 cell development through effects on DCs [132, 133], has led to considerable interest in specific pathways activated in DCs that condition them to preferentially induce Th2 responses [29]. A major focus of this work has been on the identification of lectins that recognize and permit the uptake of helminth glycoproteins [134, 135], with mannose receptor being implicated as playing a major role in this process [136]. A detailed discussion of the role of distinct dendritic cell subtypes in Th2 immune response induction can be found elsewhere in this volume in the chapter “Dendritic Cells and Type 2 Inflammation” by Lambrecht.
Summary
The response to helminth infections involves the engagement of innate type 2 cells that in the steady state play important roles in metabolic homeostasis and sterile wound healing, and the overlapping initiation of adaptive immune responses in which Th2 cells, in an antigen-specific manner, make many of the same cytokines that are made by the innate type 2 cells. The type 2 cytokines IL-4 and IL-13 made during these innate and adaptive responses activate a variety of other cell types, notably including macrophages, that play crucial roles in parasite expulsion, or in establishing an environment in which infected hosts can survive in the face of ongoing tissue damage associated with worm persistence. A key feature of the adaptive response is the emergence of B cells making helminth-specific antibodies that can interact with other cell types, or act directly, to provide protection against further infection. During chronic infection with helminths, regulatory mechanisms develop, in part stimulated by immunomodulatory parasite products, that promote host and (directly or indirectly) parasite survival and have beneficial effects that can ameliorate unrelated inflammatory conditions. Rapid advancements in our understanding of type 2 immunity raise the possibility of the rationale development of new immunologic approaches for preventing or treating helminth infections, and developing approaches to minimize the effects of the inflammatory diseases that emerge in areas where helminth parasite transmission is prevented.
References
Hotez P, Ottesen E, Fenwick A, Molyneux D. The neglected tropical diseases: the ancient afflictions of stigma and poverty and the prospects for their control and elimination. Adv Exp Med Biol. 2006;582:23–33.
Olds GR. Deworming the world. Trans Am Clin Climatol Assoc. 2013;124:265–74. Epub 2013/07/23.
Hotez PJ, Brindley PJ, Bethony JM, King CH, Pearce EJ, Jacobson J. Helminth infections: the great neglected tropical diseases. J Clin Invest. 2008;118(4):1311–21.
Ogilvie BM. Reagin-like antibodies in animals immune to helminth parasites. Nature. 1964;204:91–2. Epub 1964/10/03.
Jarrett EE. Helminth infection and the biosynthesis of IgE antibodies. Trans R Soc Trop Med Hyg. 1972;66(4):546. Epub 1972/01/01.
Vaughn J. The function of the eosinophile leukocyte. Blood. 1953;8(1):1–15. Epub 1953/01/01.
Mosmann TR, Coffman RL. TH1 and TH2 cells: different patterns of lymphokine secretion lead to different functional properties. Annu Rev Immunol. 1989;7:145–73.
Coffman RL, Seymour BW, Hudak S, Jackson J, Rennick D. Antibody to interleukin-5 inhibits helminth-induced eosinophilia in mice. Science. 1989;245(4915):308–10. Epub 1989/07/21.
Grzych JM, Pearce E, Cheever A, Caulada ZA, Caspar P, Heiny S, et al. Egg deposition is the major stimulus for the production of Th2 cytokines in murine schistosomiasis mansoni. J Immunol. 1991;146(4):1322–7.
Pearce EJ, Caspar P, Grzych JM, Lewis FA, Sher A. Downregulation of Th1 cytokine production accompanies induction of Th2 responses by a parasitic helminth, Schistosoma mansoni. J Exp Med. 1991;173(1):159–66.
Finkelman FD, Pearce EJ, Urban Jr JF, Sher A. Regulation and biological function of helminth-induced cytokine responses. Immunol Today. 1991;12(3):A62–6. Epub 1991/03/11.
Urban Jr JF, Katona IM, Paul WE, Finkelman FD. Interleukin 4 is important in protective immunity to a gastrointestinal nematode infection in mice. Proc Natl Acad Sci U S A. 1991;88(13):5513–7.
Grencis RK, Hultner L, Else KJ. Host protective immunity to Trichinella spiralis in mice: activation of Th cell subsets and lymphokine secretion in mice expressing different response phenotypes. Immunology. 1991;74(2):329–32. Epub 1991/10/01.
Brunet LR, Finkelman FD, Cheever AW, Kopf MA, Pearce EJ. IL-4 protects against TNF-alpha-mediated cachexia and death during acute schistosomiasis. J Immunol. 1997;159(2):777–85.
Anthony RM, Rutitzky LI, Urban Jr JF, Stadecker MJ, Gause WC. Protective immune mechanisms in helminth infection. Nat Rev Immunol. 2007;7(12):975–87.
Kelly BL, Locksley RM. Coordinate regulation of the IL-4, IL-13, and IL-5 cytokine cluster in Th2 clones revealed by allelic expression patterns. J Immunol. 2000;165(6):2982–6. Epub 2000/09/07.
Ansel KM, Lee DU, Rao A. An epigenetic view of helper T cell differentiation. Nat Immunol. 2003;4(7):616–23.
Kopf M, Le Gros G, Bachmann M, Lamers MC, Bluethmann H, Kohler G. Disruption of the murine IL-4 gene blocks Th2 cytokine responses. Nature. 1993;362(6417):245–8. Epub 1993/03/18.
Zaiss DM, Yang L, Shah PR, Kobie JJ, Urban JF, Mosmann TR. Amphiregulin, a TH2 cytokine enhancing resistance to nematodes. Science. 2006;314(5806):1746. Epub 2006/12/16.
Paul WE. What determines Th2 differentiation, in vitro and in vivo? Immunol Cell Biol. 2010;88(3):236–9. Epub 2010/02/17.
Harris N, Gause WC. To B or not to B: B cells and the Th2-type immune response to helminths. Trends Immunol. 2011;32(2):80–8. Epub 2010/12/17.
Crotty S. Follicular helper CD4 T cells (TFH). Annu Rev Immunol. 2011;29:621–63. Epub 2011/02/15.
Glatman Zaretsky A, Taylor JJ, King IL, Marshall FA, Mohrs M, Pearce EJ. T follicular helper cells differentiate from Th2 cells in response to helminth antigens. J Exp Med. 2009;206(5):991–9. Epub 2009/04/22.
King IL, Mohrs M. IL-4-producing CD4+ T cells in reactive lymph nodes during helminth infection are T follicular helper cells. J Exp Med. 2009;206(5):1001–7. Epub 2009/04/22.
Reinhardt RL, Liang HE, Locksley RM. Cytokine-secreting follicular T cells shape the antibody repertoire. Nat Immunol. 2009;10(4):385–93. Epub 2009/03/03.
Mohrs M, Shinkai K, Mohrs K, Locksley RM. Analysis of type 2 immunity in vivo with a bicistronic IL-4 reporter. Immunity. 2001;15(2):303–11.
Voehringer D, Shinkai K, Locksley RM. Type 2 immunity reflects orchestrated recruitment of cells committed to IL-4 production. Immunity. 2004;20(3):267–77.
Hwang YY, McKenzie AN. Innate lymphoid cells in immunity and disease. Adv Exp Med Biol. 2013;785:9–26. Epub 2013/03/05.
Pulendran B, Artis D. New paradigms in type 2 immunity. Science. 2012;337(6093):431–5. Epub 2012/07/28.
Voehringer D. Protective and pathological roles of mast cells and basophils. Nat Rev Immunol. 2013;13(5):362–75. Epub 2013/04/06.
Zhao A, Urban Jr JF, Anthony RM, Sun R, Stiltz J, van Rooijen N, et al. Th2 cytokine-induced alterations in intestinal smooth muscle function depend on alternatively activated macrophages. Gastroenterology. 2008;135(1):217–25. e1. Epub 2008/05/13.
Horsnell WG, Vira A, Kirstein F, Mearns H, Hoving JC, Cutler AJ, et al. IL-4Ralpha-responsive smooth muscle cells contribute to initiation of TH2 immunity and pulmonary pathology in Nippostrongylus brasiliensis infections. Mucosal Immunol. 2011;4(1):83–92. Epub 2010/08/26.
Shea-Donohue T, Sullivan C, Finkelman FD, Madden KB, Morris SC, Goldhill J, et al. The role of IL-4 in Heligmosomoides polygyrus-induced alterations in murine intestinal epithelial cell function. J Immunol. 2001;167(4):2234–9. Epub 2001/08/08.
Su CW, Cao Y, Kaplan J, Zhang M, Li W, Conroy M, et al. Duodenal helminth infection alters barrier function of the colonic epithelium via adaptive immune activation. Infect Immun. 2011;79(6):2285–94. Epub 2011/03/30.
Cliffe LJ, Humphreys NE, Lane TE, Potten CS, Booth C, Grencis RK. Accelerated intestinal epithelial cell turnover: a new mechanism of parasite expulsion. Science. 2005;308(5727):1463–5. Epub 2005/06/04.
Artis D, Wang ML, Keilbaugh SA, He W, Brenes M, Swain GP, et al. RELMbeta/FIZZ2 is a goblet cell-specific immune-effector molecule in the gastrointestinal tract. Proc Natl Acad Sci U S A. 2004;101(37):13596–600. Epub 2004/09/02.
Herbert DR, Yang JQ, Hogan SP, Groschwitz K, Khodoun M, Munitz A, et al. Intestinal epithelial cell secretion of RELM-beta protects against gastrointestinal worm infection. J Exp Med. 2009;206(13):2947–57. Epub 2009/12/10.
Hasnain SZ, Evans CM, Roy M, Gallagher AL, Kindrachuk KN, Barron L, et al. Muc5ac: a critical component mediating the rejection of enteric nematodes. J Exp Med. 2011;208(5):893–900. Epub 2011/04/20.
Klementowicz JE, Travis MA, Grencis RK. Trichuris muris: a model of gastrointestinal parasite infection. Semin Immunopathol. 2012;34(6):815–28. Epub 2012/10/12.
Moro K, Yamada T, Tanabe M, Takeuchi T, Ikawa T, Kawamoto H, et al. Innate production of T(H)2 cytokines by adipose tissue-associated c-Kit(+)Sca-1(+) lymphoid cells. Nature. 2010;463(7280):540–4. Epub 2009/12/22.
Neill DR, Wong SH, Bellosi A, Flynn RJ, Daly M, Langford TK, et al. Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity. Nature. 2010;464(7293):1367–70. Epub 2010/03/05.
Price AE, Liang HE, Sullivan BM, Reinhardt RL, Eisley CJ, Erle DJ, et al. Systemically dispersed innate IL-13-expressing cells in type 2 immunity. Proc Natl Acad Sci U S A. 2010;107(25):11489–94. Epub 2010/06/11.
Molofsky AB, Nussbaum JC, Liang HE, Van Dyken SJ, Cheng LE, Mohapatra A, et al. Innate lymphoid type 2 cells sustain visceral adipose tissue eosinophils and alternatively activated macrophages. J Exp Med. 2013;210(3):535–49. Epub 2013/02/20.
Wills-Karp M, Rani R, Dienger K, Lewkowich I, Fox JG, Perkins C, et al. Trefoil factor 2 rapidly induces interleukin 33 to promote type 2 immunity during allergic asthma and hookworm infection. J Exp Med. 2012;209(3):607–22. Epub 2012/02/15.
Fallon PG, Ballantyne SJ, Mangan NE, Barlow JL, Dasvarma A, Hewett DR, et al. Identification of an interleukin (IL)-25-dependent cell population that provides IL-4, IL-5, and IL-13 at the onset of helminth expulsion. J Exp Med. 2006;203(4):1105–16.
Zhao A, Urban Jr JF, Sun R, Stiltz J, Morimoto M, Notari L, et al. Critical role of IL-25 in nematode infection-induced alterations in intestinal function. J Immunol. 2010;185(11):6921–9. Epub 2010/10/27.
Scalfone LK, Nel HJ, Gagliardo LF, Cameron JL, Al-Shokri S, Leifer CA, et al. Participation of MyD88 and interleukin-33 as innate drivers of Th2 immunity to Trichinella spiralis. Infect Immun. 2013;81(4):1354–63. Epub 2013/02/14.
Humphreys NE, Xu D, Hepworth MR, Liew FY, Grencis RK. IL-33, a potent inducer of adaptive immunity to intestinal nematodes. J Immunol. 2008;180(4):2443–9. Epub 2008/02/06.
Saenz SA, Siracusa MC, Perrigoue JG, Spencer SP, Urban Jr JF, Tocker JE, et al. IL25 elicits a multipotent progenitor cell population that promotes T(H)2 cytokine responses. Nature. 2010;464(7293):1362–6. Epub 2010/03/05.
Saenz SA, Siracusa MC, Monticelli LA, Ziegler CG, Kim BS, Brestoff JR, et al. IL-25 simultaneously elicits distinct populations of innate lymphoid cells and multipotent progenitor type 2 (MPPtype2) cells. J Exp Med. 2013;210(9):1823–37. Epub 2013/08/21.
Min B, Prout M, Hu-Li J, Zhu J, Jankovic D, Morgan ES, et al. Basophils produce IL-4 and accumulate in tissues after infection with a Th2-inducing parasite. J Exp Med. 2004;200(4):507–17.
Perrigoue JG, Saenz SA, Siracusa MC, Allenspach EJ, Taylor BC, Giacomin PR, et al. MHC class II-dependent basophil-CD4+ T cell interactions promote T(H)2 cytokine-dependent immunity. Nat Immunol. 2009;10(7):697–705. Epub 2009/05/26.
Sullivan BM, Liang HE, Bando JK, Wu D, Cheng LE, McKerrow JK, Allen CD, Locksley RM. Genetic analysis of basophil function in vivo. Nat Immunol. 2011;12(6):527–35.
Sullivan BM, Liang HE, Bando JK, Wu D, Cheng LE, McKerrow JK, et al. Genetic analysis of basophil function in vivo. Nat Immunol. 2011;12(6):527–35. Epub 2011/05/10.
Siracusa MC, Saenz SA, Hill DA, Kim BS, Headley MB, Doering TA, et al. TSLP promotes interleukin-3-independent basophil haematopoiesis and type 2 inflammation. Nature. 2011;477(7363):229–33. Epub 2011/08/16.
Pennock JL, Grencis RK. The mast cell and gut nematodes: damage and defence. Chem Immunol Allergy. 2006;90:128–40. Epub 2005/10/08.
Grencis RK, Else KJ, Huntley JF, Nishikawa SI. The in vivo role of stem cell factor (c-kit ligand) on mastocytosis and host protective immunity to the intestinal nematode Trichinella spiralis in mice. Parasite Immunol. 1993;15(1):55–9. Epub 1993/01/01.
Lantz CS, Boesiger J, Song CH, Mach N, Kobayashi T, Mulligan RC, et al. Role for interleukin-3 in mast-cell and basophil development and in immunity to parasites. Nature. 1998;392(6671):90–3. Epub 1998/03/24.
Watanabe K, Kishihara K, Hamano S, Koga M, Nomoto K, Tada I. Strongyloides ratti: implication of mast cell-mediated expulsion through FcepsilonRI-independent mechanisms. Parasite. 2009;16(3):209–14. Epub 2009/10/21.
Hepworth MR, Danilowicz-Luebert E, Rausch S, Metz M, Klotz C, Maurer M, et al. Mast cells orchestrate type 2 immunity to helminths through regulation of tissue-derived cytokines. Proc Natl Acad Sci U S A. 2012;109(17):6644–9. Epub 2012/04/12.
Reynolds LA, Filbey KJ, Maizels RM. Immunity to the model intestinal helminth parasite Heligmosomoides polygyrus. Semin Immunopathol. 2012;34(6):829–46. Epub 2012/10/12.
Anthony RM, Urban Jr JF, Alem F, Hamed HA, Rozo CT, Boucher JL, et al. Memory T(H)2 cells induce alternatively activated macrophages to mediate protection against nematode parasites. Nat Med. 2006;12(8):955–60.
McCoy KD, Stoel M, Stettler R, Merky P, Fink K, Senn BM, et al. Polyclonal and specific antibodies mediate protective immunity against enteric helminth infection. Cell Host Microbe. 2008;4(4):362–73. Epub 2008/10/16.
Wojciechowski W, Harris DP, Sprague F, Mousseau B, Makris M, Kusser K, et al. Cytokine-producing effector B cells regulate type 2 immunity to H. polygyrus. Immunity. 2009;30(3):421–33. Epub 2009/03/03.
Liu Q, Kreider T, Bowdridge S, Liu Z, Song Y, Gaydo AG, et al. B cells have distinct roles in host protection against different nematode parasites. J Immunol. 2010;184(9):5213–23. Epub 2010/04/02.
Brindley PJ, Dobson C. Specificity of passive serum protection against Nippostrongylus brasiliensis and Nematospiroides dubius in mice. Aust J Exp Biol Med Sci. 1983;61(Pt 1):37–45. Epub 1983/02/01.
King IL, Mohrs K, Mohrs M. A nonredundant role for IL-21 receptor signaling in plasma cell differentiation and protective type 2 immunity against gastrointestinal helminth infection. J Immunol. 2010;185(10):6138–45. Epub 2010/10/12.
Appleton JA, McGregor DD. Rapid expulsion of Trichinella spiralis in suckling rats. Science. 1984;226(4670):70–2. Epub 1984/10/05.
Harris NL, Spoerri I, Schopfer JF, Nembrini C, Merky P, Massacand J, et al. Mechanisms of neonatal mucosal antibody protection. J Immunol. 2006;177(9):6256–62. Epub 2006/10/24.
Woolhouse ME, Hagan P. Seeking the ghost of worms past. Nat Med. 1999;5(11):1225–7.
Pinot de Moira A, Jones FM, Wilson S, Tukahebwa E, Fitzsimmons CM, Mwatha JK, et al. Effects of treatment on IgE responses against parasite allergen-like proteins and immunity to reinfection in childhood schistosome and hookworm coinfections. Infect Immun. 2013;81(1):23–32. Epub 2012/10/17.
Webster M, Fulford AJ, Braun G, Ouma JH, Kariuki HC, Havercroft JC, et al. Human immunoglobulin E responses to a recombinant 22.6-kilodalton antigen from Schistosoma mansoni adult worms are associated with low intensities of reinfection after treatment. Infect Immun. 1996;64(10):4042–6. Epub 1996/10/01.
Carlisle MS, McGregor DD, Appleton JA. The role of mucus in antibody-mediated rapid expulsion of Trichinella spiralis in suckling rats. Immunology. 1990;70(1):126–32. Epub 1990/05/01.
Bonne-Annee S, Hess JA, Abraham D. Innate and adaptive immunity to the nematode Strongyloides stercoralis in a mouse model. Immunol Res. 2011;51(2-3):205–14. Epub 2011/11/22.
Khodoun MV, Orekhova T, Potter C, Morris S, Finkelman FD. Basophils initiate IL-4 production during a memory T-dependent response. J Exp Med. 2004;200(7):857–70. Epub 2004/10/07.
Ohnmacht C, Voehringer D. Basophils protect against reinfection with hookworms independently of mast cells and memory Th2 cells. J Immunol. 2010;184(1):344–50. Epub 2009/12/04.
Geissmann F, Manz MG, Jung S, Sieweke MH, Merad M, Ley K. Development of monocytes, macrophages, and dendritic cells. Science. 2010;327(5966):656–61. Epub 2010/02/06.
Schulz C, Gomez Perdiguero E, Chorro L, Szabo-Rogers H, Cagnard N, Kierdorf K, et al. A lineage of myeloid cells independent of Myb and hematopoietic stem cells. Science. 2012;336(6077):86–90. Epub 2012/03/24.
Gordon S. Alternative activation of macrophages. Nat Rev Immunol. 2003;3(1):23–35. Epub 2003/01/04.
Wynn TA, Chawla A, Pollard JW. Macrophage biology in development, homeostasis and disease. Nature. 2013;496(7446):445–55. Epub 2013/04/27.
Gause WC, Wynn TA, Allen JE. Type 2 immunity and wound healing: evolutionary refinement of adaptive immunity by helminths. Nat Rev Immunol. 2013;13(8):607–14. Epub 2013/07/06.
Jenkins SJ, Ruckerl D, Cook PC, Jones LH, Finkelman FD, van Rooijen N, et al. Local macrophage proliferation, rather than recruitment from the blood, is a signature of TH2 inflammation. Science. 2011;332(6035):1284–8. Epub 2011/05/14.
James SL, Boros DL. Immune effector role of macrophages in experimental schistosomiasis mansoni. Immunol Ser. 1994;60:461–73. Epub 1994/01/01.
Bonne-Annee S, Kerepesi LA, Hess JA, O’Connell AE, Lok JB, Nolan TJ, et al. Human and mouse macrophages collaborate with neutrophils to kill larval Strongyloides stercoralis. Infect Immun. 2013;81(9):3346–55. Epub 2013/06/27.
Pesce JT, Liu Z, Hamed H, Alem F, Whitmire J, Lin H, et al. Neutrophils clear bacteria associated with parasitic nematodes augmenting the development of an effective Th2-type response. J Immunol. 2008;180(1):464–74. Epub 2007/12/22.
Rutitzky LI, Stadecker MJ. CD4 T cells producing pro-inflammatory interleukin-17 mediate high pathology in schistosomiasis. Mem Inst Oswaldo Cruz. 2006;101 Suppl 1:327–30. Epub 2007/02/20.
Smith PM, Shainheit MG, Bazzone LE, Rutitzky LI, Poltorak A, Stadecker MJ. Genetic control of severe egg-induced immunopathology and IL-17 production in murine schistosomiasis. J Immunol. 2009;183(5):3317–23. Epub 2009/08/14.
Pearce EJ, MacDonald AS. The immunobiology of schistosomiasis. Nat Rev Immunol. 2002;2(7):499–511.
Herbert DR, Holscher C, Mohrs M, Arendse B, Schwegmann A, Radwanska M, et al. Alternative macrophage activation is essential for survival during schistosomiasis and downmodulates T helper 1 responses and immunopathology. Immunity. 2004;20(5):623–35.
Fallon PG, Richardson EJ, McKenzie GJ, McKenzie AN. Schistosome infection of transgenic mice defines distinct and contrasting pathogenic roles for IL-4 and IL-13: IL-13 is a profibrotic agent. J Immunol. 2000;164(5):2585–91.
Chen F, Liu Z, Wu W, Rozo C, Bowdridge S, Millman A, et al. An essential role for TH2-type responses in limiting acute tissue damage during experimental helminth infection. Nat Med. 2012;18(2):260–6. Epub 2012/01/17.
Nair MG, Du Y, Perrigoue JG, Zaph C, Taylor JJ, Goldschmidt M, et al. Alternatively activated macrophage-derived RELM-{alpha} is a negative regulator of type 2 inflammation in the lung. J Exp Med. 2009;206(4):937–52. Epub 2009/04/08.
Pesce JT, Ramalingam TR, Wilson MS, Mentink-Kane MM, Thompson RW, Cheever AW, et al. Retnla (relmalpha/fizz1) suppresses helminth-induced Th2-type immunity. PLoS Pathog. 2009;5(4), e1000393. Epub 2009/04/22.
Pesce JT, Ramalingam TR, Mentink-Kane MM, Wilson MS, El Kasmi KC, Smith AM, et al. Arginase-1-expressing macrophages suppress Th2 cytokine-driven inflammation and fibrosis. PLoS Pathog. 2009;5(4), e1000371. Epub 2009/04/11.
Herbert DR, Orekov T, Roloson A, Ilies M, Perkins C, O’Brien W, et al. Arginase I suppresses IL-12/IL-23p40-driven intestinal inflammation during acute schistosomiasis. J Immunol. 2010;184(11):6438–46. Epub 2010/05/21.
Loke P, MacDonald AS, Robb A, Maizels RM, Allen JE. Alternatively activated macrophages induced by nematode infection inhibit proliferation via cell-to-cell contact. Eur J Immunol. 2000;30(9):2669–78.
Wu D, Molofsky AB, Liang HE, Ricardo-Gonzalez RR, Jouihan HA, Bando JK, et al. Eosinophils sustain adipose alternatively activated macrophages associated with glucose homeostasis. Science. 2011;332(6026):243–7. Epub 2011/03/26.
O’Connell AE, Hess JA, Santiago GA, Nolan TJ, Lok JB, Lee JJ, et al. Major basic protein from eosinophils and myeloperoxidase from neutrophils are required for protective immunity to Strongyloides stercoralis in mice. Infect Immun. 2011;79(7):2770–8. Epub 2011/04/13.
Domingo EO, Warren KS. Endogenous desensitization: changing host granulomatous response to schistosome eggs at different stages of infection with schistosoma mansoni. Am J Pathol. 1968;52(2):369–79.
Babu S, Blauvelt CP, Kumaraswami V, Nutman TB. Regulatory networks induced by live parasites impair both Th1 and Th2 pathways in patent lymphatic filariasis: implications for parasite persistence. J Immunol. 2006;176(5):3248–56.
Grogan JL, Kremsner PG, Deelder AM, Yazdanbakhsh M. Antigen-specific proliferation and interferon-gamma and interleukin-5 production are down-regulated during Schistosoma haematobium infection. J Infect Dis. 1998;177(5):1433–7. Epub 1998/05/21.
Sartono E, Kruize YC, Kurniawan A, Maizels RM, Yazdanbakhsh M. Depression of antigen-specific interleukin-5 and interferon-gamma responses in human lymphatic filariasis as a function of clinical status and age. J Infect Dis. 1997;175(5):1276–80. Epub 1997/05/01.
Wherry EJ. T cell exhaustion. Nat Immunol. 2011;12(6):492–9. Epub 2011/07/09.
Maizels RM, Lawrence RA. Immunological tolerance: the key feature in human filariasis? Parasitol Today. 1991;7(10):271–6. Epub 1991/01/01.
Taylor JJ, Krawczyk CM, Mohrs M, Pearce EJ. Th2 cell hyporesponsiveness during chronic murine schistosomiasis is cell intrinsic and linked to GRAIL expression. J Clin Invest. 2009;119(4):1019–28. Epub 2009/03/05.
Taylor MD, Harris A, Nair MG, Maizels RM, Allen JE. F4/80+ alternatively activated macrophages control CD4+ T cell hyporesponsiveness at sites peripheral to filarial infection. J Immunol. 2006;176(11):6918–27.
Maizels RM, Smith KA. Regulatory T cells in infection. Adv Immunol. 2011;112:73–136. Epub 2011/11/29.
Hussaarts L, van der Vlugt LE, Yazdanbakhsh M, Smits HH. Regulatory B-cell induction by helminths: implications for allergic disease. J Allergy Clin Immunol. 2011;128(4):733–9. Epub 2011/06/21.
Herbert DR, Orekov T, Perkins C, Finkelman FD. IL-10 and TGF-beta redundantly protect against severe liver injury and mortality during acute schistosomiasis. J Immunol. 2008;181(10):7214–20. Epub 2008/11/05.
Sher A, Fiorentino D, Caspar P, Pearce E, Mosmann T. Production of IL-10 by CD4+ T lymphocytes correlates with down-regulation of Th1 cytokine synthesis in helminth infection. J Immunol. 1991;147(8):2713–6.
Mahanty S, Nutman TB. Immunoregulation in human lymphatic filariasis: the role of interleukin 10. Parasite Immunol. 1995;17(8):385–92. Epub 1995/08/01.
Wynn TA, Ramalingam TR. Mechanisms of fibrosis: therapeutic translation for fibrotic disease. Nat Med. 2012;18(7):1028–40. Epub 2012/07/10.
Jankovic D, Cheever AW, Kullberg MC, Wynn TA, Yap G, Caspar P, et al. CD4+ T cell-mediated granulomatous pathology in schistosomiasis is downregulated by a B cell-dependent mechanism requiring Fc receptor signaling. J Exp Med. 1998;187(4):619–29.
Fairfax KC, Amiel E, King IL, Freitas TC, Mohrs M, Pearce EJ. IL-10R blockade during chronic schistosomiasis mansoni results in the loss of B cells from the liver and the development of severe pulmonary disease. PLoS Pathog. 2012;8(1), e1002490. Epub 2012/02/01.
Mosser DM, Edwards JP. Exploring the full spectrum of macrophage activation. Nat Rev Immunol. 2008;8(12):958–69. Epub 2008/11/26.
Fleming BD, Mosser DM. Regulatory macrophages: setting the threshold for therapy. Eur J Immunol. 2011;41(9):2498–502. Epub 2011/09/29.
Herbert DR, Orekov T, Perkins C, Rothenberg ME, Finkelman FD. IL-4R alpha expression by bone marrow-derived cells is necessary and sufficient for host protection against acute schistosomiasis. J Immunol. 2008;180(7):4948–55. Epub 2008/03/21.
Nimmerjahn F, Ravetch JV. Antibody-mediated modulation of immune responses. Immunol Rev. 2010;236:265–75. Epub 2010/07/20.
Anthony RM, Kobayashi T, Wermeling F, Ravetch JV. Intravenous gammaglobulin suppresses inflammation through a novel T(H)2 pathway. Nature. 2011;475(7354):110–3. Epub 2011/06/21.
van der Werf N, Redpath SA, Azuma M, Yagita H, Taylor MD. Th2 cell-intrinsic hypo-responsiveness determines susceptibility to helminth infection. PLoS Pathog. 2013;9(3), e1003215. Epub 2013/03/22.
Maizels RM, Balic A, Gomez-Escobar N, Nair M, Taylor MD, Allen JE. Helminth parasites—masters of regulation. Immunol Rev. 2004;201:89–116.
McSorley HJ, Hewitson JP, Maizels RM. Immunomodulation by helminth parasites: defining mechanisms and mediators. Int J Parasitol. 2013;43(3-4):301–10. Epub 2013/01/08.
Elliott DE, Weinstock JV. Helminth-host immunological interactions: prevention and control of immune-mediated diseases. Ann N Y Acad Sci. 2012;1247:83–96. Epub 2012/01/14.
Taylor BC, Zaph C, Troy AE, Du Y, Guild KJ, Comeau MR, et al. TSLP regulates intestinal immunity and inflammation in mouse models of helminth infection and colitis. J Exp Med. 2009;206(3):655–67. Epub 2009/03/11.
Massacand JC, Stettler RC, Meier R, Humphreys NE, Grencis RK, Marsland BJ, et al. Helminth products bypass the need for TSLP in Th2 immune responses by directly modulating dendritic cell function. Proc Natl Acad Sci U S A. 2009;106(33):13968–73. Epub 2009/08/12.
Ramalingam TR, Pesce JT, Mentink-Kane MM, Madala S, Cheever AW, Comeau MR, et al. Regulation of helminth-induced Th2 responses by thymic stromal lymphopoietin. J Immunol. 2009;182(10):6452–9. Epub 2009/05/06.
Whelan M, Harnett MM, Houston KM, Patel V, Harnett W, Rigley KP. A filarial nematode-secreted product signals dendritic cells to acquire a phenotype that drives development of Th2 cells. J Immunol. 2000;164(12):6453–60.
MacDonald AS, Straw AD, Bauman B, Pearce EJ. CD8- dendritic cell activation status plays an integral role in influencing Th2 response development. J Immunol. 2001;167(4):1982–8.
Phythian-Adams AT, Cook PC, Lundie RJ, Jones LH, Smith KA, Barr TA, et al. CD11c depletion severely disrupts Th2 induction and development in vivo. J Exp Med. 2010;207(10):2089–96. Epub 2010/09/08.
Smith KA, Harcus Y, Garbi N, Hammerling GJ, MacDonald AS, Maizels RM. Type 2 innate immunity in helminth infection is induced redundantly and acts autonomously following CD11c(+) cell depletion. Infect Immun. 2012;80(10):3481–9. Epub 2012/08/02.
Reese TA, Liang HE, Tager AM, Luster AD, Van Rooijen N, Voehringer D, et al. Chitin induces accumulation in tissue of innate immune cells associated with allergy. Nature. 2007;447(7140):92–6. Epub 2007/04/24.
Steinfelder S, Andersen JF, Cannons JL, Feng CG, Joshi M, Dwyer D, et al. The major component in schistosome eggs responsible for conditioning dendritic cells for Th2 polarization is a T2 ribonuclease (omega-1). J Exp Med. 2009;206(8):1681–90. Epub 2009/07/29.
Everts B, Perona-Wright G, Smits HH, Hokke CH, van der Ham AJ, Fitzsimmons CM, et al. Omega-1, a glycoprotein secreted by Schistosoma mansoni eggs, drives Th2 responses. J Exp Med. 2009;206(8):1673–80. Epub 2009/07/29.
van Die I, Cummings RD. Glycans modulate immune responses in helminth infections and allergy. Chem Immunol Allergy. 2006;90:91–112. Epub 2005/10/08.
Tundup S, Srivastava L, Harn Jr DA. Polarization of host immune responses by helminth-expressed glycans. Ann N Y Acad Sci. 2012;1253:E1–13. Epub 2012/09/15.
Everts B, Hussaarts L, Driessen NN, Meevissen MH, Schramm G, van der Ham AJ, et al. Schistosome-derived omega-1 drives Th2 polarization by suppressing protein synthesis following internalization by the mannose receptor. J Exp Med. 2012;209(10):1753–67. Epub 2012/09/12.
Acknowledgements
The author’s research is written by grants from the NIH (AI32573, AI082548, and CA164062).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this chapter
Cite this chapter
Pearce, E.J. (2016). Th2 Cell Responses in Immunity and Inflammation Following Helminth Infection. In: Gause, W., Artis, D. (eds) The Th2 Type Immune Response in Health and Disease. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-2911-5_4
Download citation
DOI: https://doi.org/10.1007/978-1-4939-2911-5_4
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-2910-8
Online ISBN: 978-1-4939-2911-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)