Abstract
Online and other forms of technology-assisted sex seeking are common among HIV positive men who have sex with men (MSM). Although many HIV positive MSM modify their sexual behaviors to reduce possible transmission after receiving an HIV positive diagnosis, some continue to engage in sexual risk. In this chapter, we describe the current state of research on technology use for sex seeking among HIV positive MSM, and technology-based interventions to address sexual risk taking among this population. The chapter opens with a brief history of research about online sex seeking, followed by a discussion of the methodological considerations in technology-based research. Next, online sex seeking and risks associated with this behavior are reviewed, with a focus on the psychological and social factors associated with online sexual encounters. We conclude with ways that technology has been used to provide prevention interventions to people living with HIV and consider areas for future directions.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- HIV positive
- Online
- Technology
- Sex seeking
- HIV transmission
- Positive prevention
- Chat rooms
- Serosorting
- Strategic positioning
- Barebacking
- Condomless sex
- HIV disclosure
- Global positioning system (GPS)
- Computer-based surveys
- Mental health
- Depression
- Substance use
Introduction
The resurgence of HIV among men who have sex with men (MSM) in the USA and Western Europe has been attributed to a number of factors, including increased rates of condomless anal sex (CAS) , higher rates of sexually transmitted infections (STIs) , reduced concern about the severity of HIV, and the lack of regular HIV testing (Stahlman et al., 2016; Sullivan et al., 2009; Wolitski, Vadiserri, Denning, & Levine, 2001). Moreover, with improved survival due to early diagnosis and more effective antiretroviral therapies, there are increasing numbers of people in need of treatment and with the potential to transmit HIV, which presents a continued public health challenge (Kilmarx & Mermin, 2012). Among MSM who are aware of their HIV diagnosis, Black MSM are the most likely to be virally unsuppressed (71.8%), followed by Latino MSM (63%) and White MSM (53.2%) (Hall, Holtgrave, Tang, & Rhodes, 2013). Although many HIV positive MSM modify their sexual behaviors to reduce possible transmission after receiving an HIV positive diagnosis, some continue to engage in sexual risk (Crepaz & Marks, 2002; Gorbach, Drumright, Daar, & Little, 2006; Kalichman, Rompa, & Cage, 2000; Scheer, Chu, Klausner, Katz, & Schwarcz, 2001; Schwarcz et al., 2007).
In addition to changing perceptions of the risks associated with CAS among MSM, the dramatic increase in the use of the Internet to facilitate partner seeking may partially explain increasing rates of HIV (Chiasson et al., 2006; Halkitis, Parsons, & Wilton, 2003; Hirshfield, Grov, Parsons, Anderson, & Chiasson, 2015; Hirshfield et al., 2015; McFarlane, Bull, & Reitmeijer, 2000; Pennise et al., 2015). In this chapter, we describe the current state of research on technology use for sex seeking among HIV positive MSM, and technology-based interventions to address sexual risk taking among this population. The chapter opens with a brief history of research about online sex seeking, followed by a discussion of the methodological considerations in technology-based research. Next, we review online sex seeking and the risks associated with this behavior, with a focus on the psychological and social factors associated with online sexual encounters. We conclude with considering ways that technology has been used to provide prevention interventions to people living with HIV (PLWH) and provide critical areas for future research.
Two points are needed to put the discussion that follows into greater context. First, while the focus of this chapter is on the relationship between technology use and the risk for HIV and other STIs—particularly among HIV positive MSM—the benefits of technology for many people should not be overlooked. The Internet offers unprecedented access to health and medical resources (Young, Holloway, Jaganath, Westmoreland, & Coates, 2014). Eighty-seven percent of the US adult population in 2014 went online (Pew Research Center, 2014a) and 80% of Internet users in 2010 (the most recent data available) have searched for health information (Pew Research Center, 2011). With roughly 1.2 million PLWH in the USA, studies show that many such persons are turning to the Internet for health-seeking purposes (Horvath, Carrico et al., 2013; Horvath, Michael Oakes et al., 2013). For example, an early study of how PLWH use the Internet showed that 46% of respondents searched online for information about antiretroviral therapy treatment (Kremer & Ironson, 2007). Therefore, this review should not be viewed as a one-sided depiction of the dangers of the Internet or other forms of technology.
Second, we and others (Lewis, Uhrig, Ayala, & Stryker, 2011; Weiss & Samenow, 2010) recognize that the use of the Internet in its traditional form (e.g., sitting at a desktop computer at home) to seek sex partners is now augmented by mobile- and global positioning system (GPS) -facilitated sex-seeking tools . However, research on these newer modes of technology-based sex-seeking tools is relatively recent (e.g., Goedel & Duncan, 2015, 2016; Hirshfield et al., 2012; Landovitz et al., 2012). Thus, we primarily focus on existing literature related to use of the Internet to meet sexual partners among HIV positive MSM and factors that may facilitate CAS with partners met online.
Early Research on Online Sex Seeking
Earliest reports of the association between HIV/STI risk and online sex seeking emerged at the beginning of this millennium. In the first study to receive widespread attention, McFarlane et al., (2000) reported that among a sample of 856 male and female clients receiving services at a Denver HIV clinic, persons who had sought sex partners online reported significantly more STIs , higher numbers of sex partners, higher rates of anal sex, more sex with men, and more partners known to be HIV positive than those who did not seek sex online. This early study demonstrated that a higher percentage of MSM went online to seek sex partners more than their heterosexual counterparts (59 vs. 32%), and that online sex seeking more often than offline sex seeking resulted in in-person sexual encounters (67 vs. 23%). A series of studies followed that demonstrated increased rates of actual or possible risk for HIV and other STIs among online sex-seeking persons, particularly among MSM (Bull, McFarlane, & King, 2001; Bull, McFarlane, & Reitmeijer, 2001; Rietmeijer, Bull, & McFarlane, 2001).
At the same time, several studies showed evidence directly linking online sex seeking with STI or HIV diagnoses. A syphilis outbreak among MSM in San Francisco was traced to users of a particular chat room to meet men for sex (Klausner, Wolf, Fischer-Ponce, Zolt, & Katz, 2000). In a second study, two cases of acute HIV infection were linked to sex with partners met in online chat rooms, prompting the call for physicians to discuss the risks of online sex seeking among their patients (Tashima, Alt, Harwell, Fiebich-Perez, & Flanigan, 2003). Taken together, these studies not only confirmed that risk for HIV and STIs is higher among persons who use the Internet for partner seeking, but that infections could be directly traced to online sex seeking.
Findings from these early studies were largely confirmed in a subsequent meta-analysis of online sex-seeking behavior among MSM, showing high rates of CAS among Internet-using MSM (Lewnard & Berrang-Ford, 2014). For these reasons, and the continued growth of the Internet to meet sexual partners among MSM (Rosser, West, & Weinmeyer 2008), interest remains high in how MSM use the Internet and other forms of technology (e.g., sex-seeking mobile applications) to facilitate partner selection and the possible risks inherent in such activities (Landovitz et al., 2012; Rendina, Jimenez, Grov, Ventuneac, & Parsons, 2014; Rosenberg, Khosropour, & Sullivan, 2012).
Methodological Considerations of Technology-Based Research
It is important to acknowledge the strengths and limitations of technology-based research and of studies on the association between technology use and risk behavior. A recognized strength of computer-based surveys is that they tend to elicit higher reporting of sexual risk and substance-using behaviors than mail, phone, and in-person surveys (Elford, Bolding, Davis, Sherr, & Hart, 2003; Link & Mokdad, 2005; Newman et al., 2002; Perlis, Des Jarlais, Friedman, Arasteh, & Turner, 2004). In addition, several large-scale studies comparing online to mail survey modes have found that online surveys have lower overall response rates but yield higher item response rates on both open- and close-ended questions, suggesting higher data quality (Bech & Kristensen, 2009; Denscombe, 2009; Kwak & Radler, 2002; Shin, Johnson, & Rao, 2012). These strengths and others (e.g., the potential to reach a wider segment of the target population; Pequegnat et al., 2007) are primary reasons why technology-based data collection is widely used in HIV-related research.
Limitations of technology-based research have been widely discussed (Chiasson et al., 2006; Pequegnat et al., 2007) and, therefore, interested readers are referred to these resources. We highlight two challenges that are particularly salient to the discussion below: generalizability and attrition. With respect to generalizability, it is common for studies examining the association between online sex seeking and risky sexual behavior among HIV positive MSM to recruit from online sex-seeking websites. Such websites facilitate identifying men with specific partner characteristics (e.g., men of a specific race or ethnicity), and may also facilitate locating sexual partners who seek particular sexual experiences (e.g., condomless sexual encounters). Thus, we suggest caution in extrapolating the results of these studies of online sex seeking and CAS among HIV positive MSM to the larger population of HIV positive MSM or those who do not use the Internet as a sex-seeking tool, as the recruitment source itself may attract high-risk HIV positive MSM (Mustanski, 2007).
A second identified challenge for online studies—particularly those that require multiple data collection points—is attrition. Online research studies tend to report higher attrition than offline research as there are fewer social constraints to retain participants in studies (Birnbaum, 2004). High attrition can threaten internal and external validity especially when attrition is associated with the main outcome variable (Johnson et al., 2008). Attrition is often associated with younger age and higher psychological distress (Johnson et al., 2008; Kalichman & Hunter, 1992; Orellana, Picciano, Roffman, Swanson, & Kalichman, 2006; Roffman, Klepsch, Wertz, Simpson, & Stephens, 1993; Vanable, Carey, Carey, & Maisto, 2002) and, depending on the study, reported as high as 85% (Bull, Lloyd, Rietmeijer, & McFarlane 2004) and as low as 13% (Horvath, Nygaard et al., 2012) in longitudinal online HIV prevention trials. However, attrition-related nonresponse alone does not mean that the data are inherently biased or invalid (Groves & Peytcheva, 2008). Recent advances in online retention protocols and technology are greatly improving online retention rates in HIV prevention trials, reporting similar rates to offline studies (Hirshfield et al., 2016; Khosropour, 2011; Rosser et al., 2010). These two limitations (generalizability and attrition) are important to recognize and should be considered when interpreting findings presented below.
Reasons for Seeking Sexual Partners Online
MSM were early adopters of technology and social media (Bolding, Davis, Sherr, Hart, & Elford, 2004; Wong, Gullo, & Stafford 2004), in part because the Internet holds a number of advantages in seeking sex partners over more traditional offline venues (Margolis et al., 2014). Ross and colleagues (2007) examined the responses of 1017 Latino MSM (5% of whom self-reported as HIV positive) to the question of whether they preferred to meet online or in person. The primary advantages that men reported for seeking sex partners online include the ability to seek partners anonymously, increased excitement with online sex seeking, ease and selection of sex partners, avoidance of interpersonal contact (i.e., being shy), the ability to get to know someone better, and the ability to present oneself positively, among others. In contrast, men in the study reported that advantages of meeting partners in person were to get a feel for the “real presence” of the person and to build a relationship.
The Internet and other forms of technology (e.g., global positioning system or GPS ) are efficient for sex-seeking purposes in that they can allow seekers to choose partners based on certain characteristics (e.g., HIV status), sexual preferences (e.g., a preference for condomless sex), or geography (e.g., same city, same block). These features may confer benefits or risks on users depending on the accuracy of information posted in these venues and whether such information informs subsequent sexual activity. Studies suggest that online partner seeking may facilitate seroadaptative practices to reduce HIV risk, such as serosorting (i.e., selecting a sexual partner based on an identical HIV status) or strategic positioning (i.e., assuming a sexual role based on the HIV status of the sexual partner). A meta-analysis of the sexual practices of HIV positive MSM in the US showed that the prevalence of CAS with seroconcordant partners (i.e., partners who were also HIV positive) was higher (30%) than with serodiscordant partners (16% for unknown HIV status and 13% for HIV negative partners; Crepaz et al., 2009). In a study of nearly 400 PLWH attending a medical clinic in Seattle, WA, approximately one-quarter reported that they decided not to have sex with a potential partner because the partner was HIV negative (Golden, Wood, Buskin, Fleming, & Harrington, 2007). In the same study, 31% of HIV positive men reported that a potential sex partner declined sex because of the HIV positive partner’s serostatus. In contrast, a study of Internet-using MSM in San Francisco found that while HIV negative men who went online to seek sex partners were at higher risk for having sex with a potentially serodiscordant partner, there was a trend toward seroconcordant partnerships among Internet-using HIV positive MSM (Berry, Raymond, Kellogg, & McFarland, 2008).
Regarding sexual negotiation with partners met online versus offline, it also appears that MSM report different reasons for not using condoms. In an analysis of written responses of the reasons for not using condoms with online and offline partners, MSM (9% self-reported HIV positive) who had CAS with online partners were more likely to cite an individual preference for sex without condoms (often referring to greater physical pleasure) and mutually agreeing to forgo condoms prior to the sexual encounter compared to reasons for CAS with their offline partners (Ostergren, Rosser, & Horvath, 2010). In the same study, CAS with offline partners was more likely attributed to contextual (e.g., alcohol and drugs) and relationship (e.g., in a monogamous relationship) factors.
Finally, in a study of condomless sex and the Internet, a high percentage of MSM (all of whom were familiar with the term “barebacking ” and 20% of whom were HIV positive) agreed with the following statements: “Barebackers can find others like them to communicate with on [the] Internet” (75.7%); “[The] Internet makes it easy to find other men who bareback” (73.4%); and “Because [the] Internet is anonymous, gay men are more likely to use it to look for other barebackers” (70.0%) (Halkitis et al., 2003). Although these studies were not exclusively restricted to PLWH, the results demonstrate the complex relationships between the technological features afforded by the Internet, individual preferences for partner selection, sexual negotiation, and sexual practices. Whether or not the Internet and other technology-based venues for sex seeking heightens or reduces sexual risk depends on the personal characteristics of individuals who use these technologies (e.g., individual level of risk taking or risk aversion), the social norms about HIV disclosure and risk taking on the particular venue (i.e., whether the site caters to persons seeking condomless sex or not) appears to translate into tangible sexual practices when partners meet offline . The dynamic interplay between these factors often results in findings from research studies that do not consistently align with each other, and call for continued efforts to understand these associations as the relationship between the individual and technologies change over time.
Online Sex Seeking and Risk Behavior
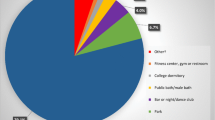
The Internet is a common venue for MSM to seek sex partners (Lewnard & Berrang-Ford, 2014). A meta-analysis of online sex-seeking and sexual risk showed that approximately 40% of MSM had used the Internet to seek sex partners (Liau et al., 2006). In a separate study of 1683 MSM (11% self-reporting as HIV positive) who completed an online survey, results showed that the majority (82%) had sex with someone they met online, and 66% stated that they had more sex once they started meeting partners online (Chiasson et al., 2007). A study in which MSM were intercepted at gay community events in Los Angeles and New York showed that over half (53.5%) of MSM (12.5% of whom self-reported as HIV positive) reported meeting sex partners online in the past 3 months, compared to 55% who met sex partners at the bar and 40% who met sex partners at bathhouses (Grov, Parsons, & Bimbi, 2007).
In general, online studies of MSM find that men who meet men on the Internet report a greater number of sex partners (Benotsch, Kalichman, & Cage, 2002; Horvath, Rosser, & Remafedi, 2008; Margolis et al., 2014; McFarlane, Bull, & Rietmeijer, 2000; Rosser, Miner et al., 2009; Rosser, Oakes et al., 2009; Rosser et al., 2008; Taylor et al., 2004), having sex with casual partners (Horvath et al., 2008; Kim, Kent, McFarland, & Klausner, 2001; Rosser, Miner et al., 2009; Rosser, Oakes et al., 2009; Rosser et al., 2008; Taylor et al., 2004; Tikkanen & Ross, 2003), and higher rates of CAS (Benotsch et al., 2002; for a recent review see Lewnard & Berrang-Ford, 2014). However, some studies did not find a higher reporting of CAS among men who met sex partners online versus offline (Chiasson et al., 2007). A possible explanation for these contradictory findings is a difference in study measures to assess CAS. Studies that use the frequency of CAS in a given time period as the main outcome show that men who meet sex partners on the Internet appear to be at higher risk because of the heightened availability of sex partners found through online venues . However, when CAS is calculated as a proportion of sex partners met either online or offline, several studies have shown less risk behavior with online partners (Horvath et al., 2008; Mustanski, 2007). Therefore, in addition to the methodological considerations of technology-based research described earlier, close attention to issues of measurement is needed to understand the complexity of findings regarding sexual risk.
HIV positive gay men and other MSM appear to utilize the Internet more often and have greater levels of CAS with online partners, than MSM who have not been diagnosed with HIV (Lewnard & Berrang-Ford, 2014). The meta-analysis by Liau and his colleagues (Liau et al., 2006) showed that nearly one-half of HIV positive MSM went online seeking sex partners , compared to 41% of MSM who had not been diagnosed with HIV. The odds of CAS with sex partners met online was 1.68 times higher than for sex partners not met online, and this was particularly true for HIV positive MSM. The results of another study suggested that differences in risk behavior by venue are magnified among very highly sexually active MSM. In a study of 50 MSM who reported nine or more sex partners in the past 90 days, HIV positive men were more likely than HIV negative men to use the Internet to meet men for sex (95 vs. 68%), and were more likely to report CAS with online partners than HIV negative men (63 vs. 20%) (Grov, Golub, & Parsons, 2010). Online sex seeking is high among samples of HIV positive youth . In a recent qualitative study of 68 HIV positive (68% of the sample) and HIV negative youth (ages 18–24), 71% of HIV positive participants spent 5 or more hours on dating applications (or apps) a day (Camacho-Gonzalez et al., 2016).
Studies that focus on serodiscordant CAS (i.e., HIV positive persons reporting CAS with a HIV negative or HIV status unknown partner) as the outcome also reveal concerning rates of risk behavior among a substantial minority of HIV positive MSM. For example, the prevalence of serodiscordant CAS among samples of HIV positive MSM recruited online ranged from 23 to 51% (Chiasson, Hirshfield, Humberstone, DiFilippi et al., 2005; Chiasson, Hirshfield, Humberstone, Remien et al., 2005; Chiasson et al., 2007; Grov, Hirshfield, Remien, Humberstone, & Chiasson, 2011; Hirshfield, Remien, Humberstone et al., 2004a). These results are comparable to those in a community-based venue study in New York and California in which 47% of HIV positive men with non-main partners reported serodiscordant CAS in the previous 3 months (Parsons et al., 2005). The findings of these and other studies (Halkitis & Parsons, 2003; Halkitis et al., 2003) are reflected in a recent meta-analysis (Lewnard & Berrang-Ford, 2014) of the sexual behavior among MSM with online and offline partners across 11 studies. Findings showed that online partner seeking was associated with higher odds of CAS, seroconcordant CAS, and seroconcordant CAS with strategic positioning compared to offline partner seeking, with higher effect sizes noted among HIV positive compared to HIV negative groups across these outcomes. Therefore, there is a clear need to target HIV positive MSM who seek online partners with effective interventions.
Online sex seeking may be driven by a number of factors that are particularly salient to MSM living with HIV, including HIV disclosure , personal beliefs about responsibility to reduce the risk for transmission to sex partners, and mental health and substance use issues. Each of these is discussed in more detail below.
Contextual Issues Affecting Online Sex Seeking and HIV Transmission
HIV Disclosure Online and Offline. Disclosure of HIV status has been identified as a critical—although an imperfect (Horvath, Oakes, & Rosser, 2008)—component of sexual negotiation for MSM that has been cited in empirical studies (Carballo-Dieguez, Miner, Dolezal, Rosser, & Jacoby, 2006; Klitzman et al., 2007; Rietmeijer, Bull, McFarlane, Patnaik, & Douglas, 2002) and by the CDC (Centers for Disease Control and Prevention, 2003). Belief among PLWH that HIV positive individuals should disclose their status to sex partners has been associated with more frequent disclosure to sex partners (Duru et al., 2006). HIV positive men who do not disclose their serostatus and engage in condomless sex may be more likely to report using drugs before sex and less likely to know their partner’s serostatus (Marks & Crepaz, 2001).
A study by Rosser and colleagues showed that approximately equal proportions of HIV positive MSM disclosed their HIV status to none (30%), some (31%), or all (39%) of their secondary sexual partners (Rosser, Horvath et al., 2008). The same study found that higher disclosure was associated with having fewer sex partners, being extremely out as a gay or bisexual man, more years of living with HIV, knowledge of CD4 count, having a detectable viral load, and White race. Biomedical advances in HIV prevention (i.e., treatment as prevention; Cohen et al., 2011) suggest that disclosure may include sharing one’s health status in addition to HIV status. Evidence that effective HIV treatment greatly reduces the likelihood of HIV transmission among those who are virally suppressed—especially for early ART initiators (i.e., those who begin treatment immediately after receiving an HIV diagnosis, regardless of CD4 count)—provides strong support for the disclosure of whether antiretroviral therapy is being taken and current viral load status (Cohen et al., 2016). In a study of 304 HIV negative and 22 HIV positive MSM recruited online, CAS was reported in 75% of sexual encounters in which viral load was not discussed compared to 56% of sexual encounters in which viral load was discussed (Horvath, Smolenski, Iantaff et al., 2012).
Many reasons exist for why PLWH may not disclose their HIV status to potential sex partners, such as fear of a stigmatizing response with each new disclosure (Berger, Ferrans, & Lashley, 2001). To complicate matters, disclosure to sexual partners and its relationship to sexual risk can vary by partner type and venue (Grov, 2011; Grov et al., 2011; Simoni & Pantalone, 2004). Some studies show that men may be more likely to disclose to sex partners met online (Carballo-Dieguez et al., 2006; Chiasson et al., 2007). HIV status disclosure may be facilitated online through synchronous discussions in Internet chat rooms or mobile GPS apps and by disclosing HIV status through online profiles. In November 2016, Grindr, a popular GPS smartphone app used by MSM to meet other men, added two optional fields to user profiles to assist in the HIV disclosure process: HIV status (HIV positive; HIV positive, Undetectable; HIV negative; HIV negative, On PrEP [pre-exposure prophylaxis]) and last HIV test date (Corbett, 2016).
Studies show mixed results regarding the use of online profiles as an HIV status disclosure tool. A study of whether MSM report their HIV status on their online profiles showed that 72% of MSM who had never tested for HIV and 75% of HIV negative men reported that they were HIV negative in all of their online profiles (Horvath et al., 2008). In contrast, the same study found that 16.8% of HIV positive MSM reported their status as HIV negative in all of their online profiles, while only 25% reported their status as HIV positive in all of their online profiles. Nodin and colleagues examined 199 online sex-seeking profiles of MSM on six of the most popular websites for men seeking condomless sex in New York City (Nodin, Valera, Ventuneac, Maynard, & Carballo-Diéguez, 2011). Profiles indicating that the user was HIV positive were more likely to contain full body pictures (50 vs. 22%), face pictures (77 vs. 51%), and multiple pictures (89 vs. 67%). Together, these results suggest that HIV positive MSM may be less likely to accurately disclose their HIV status in online profiles; however, among those that do, HIV positive MSM may be more inclined to reveal other physical attributes of themselves than HIV negative or serostatus unknown men. Revealing these attributes may be a way that some HIV positive MSM manage stigma surrounding their HIV status by projecting to potential sex partners that they have desirable characteristics rather than solely being identified with their HIV status.
Personal Responsibility to Reduce Risk for Transmission . Most HIV positive men feel a personal responsibility to protect their sex partners, via disclosure and/or condom use (O'Leary & Wolitski, 2009). Some PLWH, however, report having lower feelings of personal responsibility to not transmit HIV, which they may justify by minimizing potential consequences (Bandura, 1999, 2002) and based on unconfirmed assumptions about a sex partner’s serostatus (Parsons et al., 2006). Studies using quantitative measures of personal responsibility among HIV positive MSM show that higher personal responsibility ratings are correlated with less sexual transmission risk behavior (Parsons, Halkitis, Wolitski, & Gomez, 2003; Wolitski, Flores, O'Leary, Bimbi, & Gomez, 2007).
Personal responsibility appears to vary by venue in which HIV positive MSM meet their sex partners. One study showed that HIV positive MSM had highest levels of personal responsibility to protect their sexual partners from HIV or other STIs when they met those partners through friends or family (O’Leary, Horvath, & Rosser, 2012). Personal responsibility was next highest for partners met at a bar, followed by the Internet and finally for sex partners met in public sex venues. Among the 98 men who reported meeting sex partners in multiple venues, those who reported inconsistent responsibility beliefs across venues where sex partners were met or had lower personality beliefs across all venues reported higher risk behavior than those who reported consistently very high personal responsibility beliefs across venues. Collectively, these studies demonstrate that personal responsibility beliefs may be critical targets for prevention, and that addressing beliefs by venue may be important since responsibility beliefs appear to differ with partners met online and offline.
Mental Health Depression is common in men with, or at risk for, HIV (Dew et al., 1997). Rates of depression among MSM participating in research studies are higher than that of the general population (Rabkin, McElhiney, & Ferrando, 2004). Several nationally representative US surveys have found that 1–3% of men report same-sex partners or self-identify as gay or bisexual; among these men, past-year major depression ranged from 10 to 31%, compared to men who report sex with women, with past year ranges from 5 to 10% (Cochran & Mays, 2000; Cochran, Sullivan, & Mays, 2003; Gilman et al., 2001). In a US-based household probability sample of MSM (Mills et al., 2004), 17% screened positive for depression and 12% for distress (subthreshold for depression). Characteristics associated with depression included not having a domestic partner and not identifying as gay/homosexual. In another study of young MSM (Kipke et al., 2007), 21% screened positive for depression and 18% for distress, with 12% of men from the sample reporting no access to care when ill or in need of health advice. Using the two-item Patient Health Questionnaire (PHQ-2), 18% screened positive for current depressives symptoms in an online study among MSM from the USA and Canada (Hirshfield et al., 2008); characteristics associated with a positive screen included having low education, being HIV positive, not having a main same-sex partner, being married to a woman, and not reporting recent sex. Another online study among US MSM found a 17% prevalence of current depressive symptoms, which were associated with a recent STI diagnosis (Downing, Chiasson, & Hirshfield, 2016).
Many individuals with depressed mood report decreased sexual interest and activity (Casper et al., 1985; Kennedy, Dickens, Eisfeld, & Bagby, 1999; Mathew & Weinman, 1982). However, in a study of mood and sexual interest among 662 MSM, a minority (16%) of men reported increased sexual interest when depressed and nearly one-quarter reported heightened sexual interest when anxious (Bancroft, Janssen, Strong, & Vukadinovic, 2003). The relationship between mood, sexual interest, and sexual behavior is complex among PLWH. In a study of the relationship between negative affective states (e.g., depression-dejection, tension-anxiety, confusion-bewilderment) and risk behavior among 155 sexually active HIV positive men, negative affective states were associated with CAS with male partners, but not female partners (Marks, Bingman, & Duval, 1998). Other studies have confirmed an increase in sexual risk behavior among HIV positive MSM with high levels of depressive symptoms (Beck, McNally, & Petrak, 2003; Kelly et al., 1993; Parsons et al., 2003). HIV positive men who experience depression may feel disconnected from others and may consequently be less likely to enact risk-reduction strategies with sexual partners (Poppen, Reisen, Zea, Bianchi, & Echeverry, 2004).
Findings on the association between Internet use and depression are not uniform. Some studies show that Internet use is associated with high depressive symptomatology (Kraut et al., 1998), while other studies have found that online activities in which people interact with one another (e-mail, chat rooms) was associated with lower levels of loneliness and depression (Morgan & Cotten, 2003; Shaw & Gant, 2002). Kalichman and colleagues examined levels of depressive symptoms among HIV positive men who seek sex partners online compared to those who only seek sex partners offline (Kalichman, Cherry, Cain, Pope, & Kalichman, 2005). Unadjusted models showed that depression scores were higher among men who sought sex partners online compared to men who did not (Centers for Epidemiologic Studies Depression Scale [CES-D] = 17.5 vs. 13.2). However, CES-D scores were not significantly associated with online sex seeking in the multivariate model. In sum, there is modest evidence that online sex seeking is associated with depression , although this relationship may be attenuated by other factors (e.g., levels of social support or adaptive coping). Persons who report high levels of depressive symptoms and are either at risk for HIV or are currently living with HIV should be assessed for partner-seeking behaviors to address possible depression-related risk activity in need of intervention.
Drug Use Drug use has been consistently linked to HIV transmission risk , particularly among MSM (Carey et al., 2009; Harawa et al., 2008). Certain drugs such as poppers (nitrite inhalants), ecstasy (MDMA), and crystal methamphetamine may be used specifically to enhance sexual experiences (Lewis & Ross, 1995). Ecstasy, crystal methamphetamine, gamma hydroxybutyrate (G or GHB), cocaine, and other substances have been associated with increased sexual risk behaviors, including CAS and group sex with anonymous, HIV negative or unknown status partners (Beck & Rosenbaum, 1994; Carey et al., 2009; Chiasson, Hirshfield, Humberstone, DiFilippi et al., 2005; Chiasson, Hirshfield, Humberstone, Remien et al., 2005; Chiasson, Shuchat Shaw, Humberstone, Hirshfield, & Hartel, 2009; Chiasson et al., 2006; Frosch, Shoptaw, Huber, Rawson, & Ling, 1996; Hirshfield, Grov et al., 2015; Hirshfield, Schrimshaw et al., 2015; Hirshfield, Remien, & Chiasson, 2006; Hirshfield, Remien, Humberstone et al., 2004a; Phillips, Grov, & Mustanski, 2015; Hirshfield, Remien, Walavalkar et al., 2004b; Semple, Zians, Strathdee, & Patterson, 2008; Thiede et al., 2008; Topp, Hando, & Dillon, 1999; Yu, Wall, Chiasson, & Hirshfield, 2015).
Substance use and its relationship to high-risk sexual behavior among MSM is of particular concern, as drugs and alcohol may help men to avoid feelings of anxiety associated with same-sex behavior and self-awareness of HIV (Mckirnan, Ostrow, & Hope, 1996; McKirnan, Vanable, Ostrow, & Hope, 2001). Impaired judgment due to drug use may lead to condomless sex , increasing the risk of HIV/STI transmission (Colfax & Guzman, 2006; Halkitis, Parsons, & Stirratt, 2001). Polydrug use and frequent drug use have been associated with HIV seropositivity or unknown HIV serostatus (Greenwood et al., 2001). For these reasons, it is not surprising that a high proportion (70%) of MSM who report engaging in CAS attribute increasing acceptance and practice of “barebacking ” to the use of club drugs, including methamphetamines, ecstasy, and GHB (Halkitis et al., 2003).
High levels of substance use have been shown among MSM who seek sex partners online. In a study of MSM recruited at a gay pride event in Atlanta, Georgia, those who reported meeting sex partners via the Internet (n = 201) were more likely to report using methamphetamines and in the previous 6 months than men who did not meet sex partners online (10 vs. 5%) (Benotsch et al., 2002). Another study showed that MSM (of which one-sixth were HIV positive) who reported online sex seeking were significantly more likely to report ecstasy use during sex (Mettey, Crosby, DiClemente, & Holtgrave, 2003). Moreover, among men diagnosed with early stage syphilis infection, online sex seeking was associated with non-intravenous drug use after controlling for other factors (Taylor et al., 2004).
Recent HIV seroconversion is significantly associated with drug use during sex (Carey et al., 2009) and substance use is high among HIV positive MSM recruited both online and offline. One study showed that a high proportion of HIV positive White MSM reported recent stimulant (30%), methamphetamine (27%), and amyl nitrite (46%) use, while crack and cocaine use were high among Black MSM (38%) (Hatfield et al., 2009). In a study of MSM recruited to participate in an online survey, HIV positive men were significantly more likely to use two or more drugs before or during sex than their HIV negative or HIV status unknown counterparts (Hirshfield, Remien, Humberstone et al., 2004a). Other studies have similarly found associations between drug use and seroconversion (Plankey et al., 2007), particularly among MSM who use methamphetamine (Colfax, Shoptaw, Colfax, & Shoptaw, 2005; Hirshfield, Remien, Walavalkar et al., 2004b; Mimiaga et al., 2008).
Locating sex partners who may want to use drugs to enhance their sexual experiences may be facilitated by online profile options. Horvath and colleagues found that 12.5% of HIV positive MSM reported that all or some of their online profiles reported a preference for drug use during sex (“Party and Play”), compared to 6.9% of profiles of men who have only tested HIV negative and 4.5% of profiles of men who have never been tested for HIV (Horvath et al., 2008). Thus, although drug use may not necessarily be more common among HIV positive MSM who use the Internet to seek sex partners, the Internet may facilitate locating sex partners who wish to use drugs to enhance the sexual experience.
Overall, there is a consistent association between drug use, online sex seeking, and HIV risk. Addressing drug use as a risk factor for HIV and other STIs remains an important avenue to address high HIV/STI rates among MSM. However, as noted in a review of treatment outcome studies of HIV positive MSM who abuse methamphetamines (Rajasingham et al., 2012), effective interventions to reduce rates of drug use among this group remain sparse. Thus, greater emphasis should be placed on developing novel and culturally tailored interventions to address drug use among HIV-infected MSM to improve their own health outcomes and reduce risk for HIV transmission to sexual partners (Horvath, Carrico et al., 2013; Horvath, Michael Oakes et al., 2013).
Internet Use Among MSM of Color and Sexual Risk Taking
Although Black and Latino MSM are at a significant increased risk for HIV, few HIV risk reduction interventions—and even fewer that use technology—have been designed to target these groups (Young et al., 2014). The lack of technology-based interventions focusing on gay and MSM of color at risk or infected with HIV may stem in part from the belief that communities of color have not adopted technology as widely as White MSM or other non-minority groups. However, the US population online now has similar proportions of White (85%), Black (81%), and Latino/a adults (83%) (Pew Research Center, 2014a; Smith, 2010b). Black (90%) and English-speaking Latino/a (92%) adults are as or more likely to own a mobile phone than Whites (90%; Pew Research Center, 2014b), and are also more likely to use their mobile devices to send text messages, use social networking sites, watch videos, and e-mail (Smith, 2010a).
Although most studies examining Internet use and sexual risk taking do not exclusively focus on MSM of color, there are several notable exceptions. A series of published studies from the MINTS trial led by Rosser and a team of investigators focused on Internet use and sexual risk among Latino MSM (Carballo-Dieguez et al., 2006; Ross, Rosser, & Stanton, 2004; Ross, Rosser, Stanton, & Konstan, 2004; Rosser, Miner et al., 2009; Rosser, Oakes et al., 2009). In one of those studies, sexual negotiation and serostatus disclosure were more likely to occur with online than offline sexual partners among both HIV positive and HIV negative MSM; however, HIV positive participants were less likely to disclose their status than HIV negative MSM (Carballo-Dieguez et al., 2006). The same study showed that HIV positive Latino MSM reported lower intentions to use condoms than HIV negative Latino MSM, citing greater pleasure with condomless intercourse. In another study by this research team, Latino MSM—5% who self-identified as HIV positive (as reported in Rosser, Miner et al., 2009; Rosser, Oakes et al., 2009)—who reported a high preference for using the Internet to facilitate face-to-face interactions also reported relatively low levels of HIV status disclosure and discussions about safer sex with prospective partners and reported high rates of receptive oral and anal sex during Internet-mediated sexual liaisons (Ross, Rosser, & Stanton, 2004).
A study of online sex seeking among Black MSM (18% of who were living with HIV) showed that 20% reported meeting a sexual partner in the past 12 months (White, Mimiaga, Reisner, & Mayer, 2012). Findings also showed that Black MSM who met partners online reported more male sex partners and higher rates of condomless sex than Black MSM who did not report meeting sex partners online. Online sex seeking was significantly associated with condomless sex in multivariate models. In a second online study of serodisclosure in partnerships among men of varying races and ethnicities, HIV positive Black men were 60% less likely than White men to discuss their serostatus with sexual partnerships (Winter, Sullivan, Khosropour, & Rosenberg, 2012). In the same study, discussion of serostatus were more likely to occur with CAS partners than among non-CAS partner for HIV negative and HIV positive White MSM and HIV negative Latino and Black MSM; however, serostatus discussions were less likely among CAS partners than non-CAS partners for HIV positive Black and Latino MSM.
Low rates of serostatus disclosure among Internet-recruited Black and Latino HIV positive MSM has been attributed to both minority stress and high rates of homophobia experienced by these groups (Mays, Cochran, & Zamudio, 2004; Radcliffe et al., 2010; Stein et al., 1998; Winter et al., 2012). Thus, calls for interventions that address stigma and experiences of minority stress have been made (Winter et al., 2012), with a need to promote serostatus disclosure as normative behavior prior to sexual activity. Such intervention may benefit from addressing issues of sexual stereotyping in online partner selection that may increase possible risk behavior. Sexual stereotyping was investigated in a study by Wilson and colleagues that showed that online sex-seeking MSM of varying races and ethnicities used race-based sexual stereotypes that both directly and indirectly affected sexual partnering choices (Wilson et al., 2009). For example, Black MSM reported feeling a deeper connection with sexual partners who were Black, and feeling objectified by White sexual partners. The study by Wilson and colleagues shows the complex ways that MSM may be using the Internet to locate sex partners based on a variety of existing racial and ethnic stereotypes, which may be facilitated by online profiles (providing visual cues indicating race and ethnicity) or technology-mediated discussions (via supporting sexual stereotypes through conversational cues).
HIV Positive Perspectives on Technology-Based HIV Resources
Technology-based intervention approaches may benefit from research examining the perspectives of PLWH about technology-supported HIV-related resources. In a mixed method study of gay men, heterosexual women and men, and transgender women who were recently (<1 year) diagnosed with HIV, participants were asked about their perceptions of HIV-related websites (Courtenay-Quirk et al., 2010). The most appealing aspects of highly rated websites included websites that: provided relevant information on topics that were important to participants’ health and well-being, were easy to navigate, were perceived as trustworthy, and represented a diversity of perspectives that represented a broad spectrum of PLWH. Participants in this study reported greatest interest in online resources that addressed HIV treatment issues, strategies for coping with depression and fear about living with HIV, and ways to learn how others have coped with HIV.
A study of technology use among PLWH in the USA demonstrated the widespread use of social networking websites and mobile phones among this population (Horvath, Danilenko et al., 2012; Horvath, Nygaard et al., 2012). When asked to describe their ideal social networking health website for PLWH, participants overall described it as one that would facilitate social interactions between people, contain relevant HIV-related information, and address privacy issues. In a more recent study, HIV positive MSM attending focus groups were asked about features and functions of mobile applications (apps) they believed keep them engaged with the apps on their smartphones (Horvath, Alemu, Danh, Baker, & Carrico, 2016). Consistent with theories of technology acceptance (Venkatesh & Bala, 2008), men in the study reported that the apps they used most often and for long periods of time were useful, easy to use, engaging (i.e., fun, visually engaging), credible, secure, and ones that they had control over (e.g., could easily change notifications or other features). Taken together, the results of these studies draw attention to two important points. First, that technology use is common among some PLWH, and therefore technology-based environments may be important venues to deliver interventions. Second, providing intervention in a technology-based environment will require considerations of both the advantages that such mediums provide (e.g., the ability to connect with other PLWH) as well as the potential concerns that PLWH have regarding technology (e.g., privacy concerns).
Technology-Based HIV Prevention Strategies: Promising Evidence and Clear Gaps
Meta-analyses of the efficacy of computer technology-based HIV prevention interventions showed a statistically significant impact of these interventions on sexual health knowledge, safer sex self-efficacy, safer-sex intentions, and condom use, suggesting that technology-based HIV prevention interventions have similar or higher efficacy than more traditional, face-to-face interventions (Bailey et al., 2012; Noar, Black, & Pierce, 2009). Technology-based HIV prevention approaches include computer and Internet-based, mobile app, chat room , text messaging, and social media interventions (for reviews see Noar & Willoughby, 2012; Simoni, Kutner, & Horvath, 2015; Sullivan, Jones, Kishore, & Stephenson, 2015). However, relatively few face-to-face interventions have been developed and evaluated for HIV positive MSM. For example, out of the nearly 100 evidence-based interventions for best practices for HIV prevention compiled by the CDC, only 15 target HIV positive persons; of those, 13 are delivered face to face (Centers for Disease Control and Prevention, 2016). With few notable exceptions (see below), most existing online or other technology-delivered HIV prevention interventions that have been rigorously tested do not specifically target PLWH (Bailey et al., 2010). Published randomized control trials (RCTs ) of online HIV behavioral interventions targeting HIV negative MSM have shown reductions in one or more HIV risk behaviors (Bull, Pratte, Whitesell, Rietmeijer, & McFarlane, 2008; Carpenter, Stoner, Mikko, Dhanak, & Parsons, 2009; Hirshfield et al., 2012; Lelutiu-Weinberger et al., 2015; Mustanski, Garofalo, Monahan, Gratzer, & Andrews, 2013; Rosser et al., 2010), increases in HIV testing (Bauermeister et al., 2015; Blas et al., 2010), or short-term increases in knowledge, self-efficacy, and outcome expectancies (Bowen, Horvath, & Williams, 2007). However, other trials reported no changes in behavior (Bull, Lloyd, Rietmeijer, & McFarlane, 2004; Lau, Lau, Cheung, & Tsui, 2008).
In addition to Internet-based studies, reaching and engaging MSM of color for HIV prevention through mobile technology has also shown promise (Young et al., 2014). Preliminary data show that text messaging is an acceptable and viable method for reaching young Black men with prevention messages (Wright, Fortune, Juzang, & Bull, 2011) and that a sufficient proportion of this population can be retained in a text message intervention over at least 3 months (77%, although retention at 6 months was 65%; Fortune, Wright, Juzang, & Bull, 2010). Approaches that leverage commonly used social media platforms, such as Facebook, to deliver peer-delivered HIV information have been shown to be associated with a higher likelihood of getting tested for HIV and discussions of sexual behaviors online among mostly Black and Latino MSM (Huang, Marlin, Young, Medline, & Klausner, 2016; Young et al., 2014). These results indicate that technology-based approaches to HIV prevention intervention are promising, however, there continues to be a gap in extending these approaches to address the needs of PLWH (Noar & Willoughby, 2012). These gaps may be addressed through closer coordination of efforts between researchers and community-based organizations to develop and test technology-delivered interventions to address risk reduction strategies among PLWH, and through the prioritization of funding mechanisms by federal and state agencies to support technology-based approaches to prevention among high-risk PLWH.
Despite the dearth of research in this area, a few notable technology-based interventions have emerged that may address the prevention and healthcare needs of PLWH. These include interventions to teach HIV positive persons Internet information consumer skills (Kalichman et al., 2006); online, texting, and pager interventions to assist people living with HIV manage their health and adherence to antiretroviral medication (Gamage et al., 2011; Harris et al., 2010; Horvath, Carrico et al., 2013; Horvath, Oakes et al., 2013; Lester et al., 2010; for a review see Amico, 2015); and an Internet-based intervention to reduce HIV-related stigma (Adam et al., 2011). Thus, most technology-based interventions focus on helping PLWH to manage their HIV illness, rather than on reducing sexual risk.
There are recent efforts to include HIV positive MSM in technology-based sexual risk reduction interventions that also include HIV negative or unknown serostatus MSM. For example, although not exclusively targeted to PLWH, Hightow-Weidman and colleagues recently developed and reported the feasibility and acceptability of an online intervention to reduce sexual risk among young Black MSM, of whom 42% reported living with HIV (Hightow-Weidman et al., 2012). As described by the authors: “Key interactive features of the site include live chats with an HIV expert, interactive quizzes of varying levels of difficulty, personalized health and ‘hook-up/sex’ journals, and decision support tools for assessing and modifying risk behaviors (p. 911).” At the conclusion of the pilot study (50 men, half of whom were randomized to the intervention and the other half to control), high levels of 1- (90%) and 3-month (78%) follow-up assessment retention were attained, and intervention assigned participants reported high satisfaction and interest in the website and low levels of frustration with website features. Another technology-delivered online RCT study compared the effect of two videos and a HIV prevention webpage to a control condition to lower sexual risk taking among MSM, 25% of whom were either HIV positive or did not know their serostatus (Hirshfield et al., 2012). At follow-up, HIV positive men who received the videos reported significantly lower CAS and serodiscordant CAS compared to those in the control condition. Both the study by Hightow-Weidman et al., (2012), and a new online video RCT for sub-optimally adherent HIV positive MSM (Hirshfield et al., 2016), are currently being tested in large-scale efficacy trials. In sum, studies that recruit HIV positive MSM in addition to men of other serostatus show evidence that technology-delivered interventions may reduce sexual risk, and should be explored in future research.
Several technology-facilitated interventions that focus exclusively on PLWH have been published, with encouraging findings. HIV positive MSM were asked to complete a computerized sexual risk assessment prior to their next HIV medical appointment (Chen et al., 2008). The results of the assessment were given to the provider to prompt discussions about sexual risk with their patients. Positive ratings were given by the majority of providers (79%) and patients (84%) regarding the quality of prevention services during the appointment, and providers reported feeling more confident in communicating prevention strategies with their patients. However, no information was collected on whether men reduced their sexual risk behavior as a result of the intervention. In a similar study (Bachmann et al., 2013), a printed hand-out from a computer-based assessment of HIV positive MSM’s intention to change in one of three risk behaviors (condom use, reduction in sex partners, and HIV disclosure) were given to providers during the healthcare encounter to guide discussion about sexual risk reduction. In this single-condition trial, reductions in CAS with seroconcordant and serodiscordant sex partners and in the number of male sex partners in the prior 6 months were shown at post-intervention follow-up. The “Positive Choice: Interactive Video Doctor intervention” (Gilbert et al., 2008) is administered to PLWH while they wait for their healthcare appointment. PLWH complete a computerized risk assessment, which is followed by a virtual doctor delivering tailored risk reduction messages. A printout of these messages was available to patients and provided to their healthcare provider to guide discussion about risk reduction. Among 471 PLWH randomized to intervention or control arm, 51% were MSM and most were Black or Hispanic/Latino. Significant reductions in CAS and condomless vaginal intercourse were shown at 3- and 6-month assessment time points compared to the control condition, as well as fewer casual sex partners at the 6-month follow-up assessment. Finally, “CARE+” is an individually delivered, computer-based counseling intervention with the goal of improving medication adherence and reducing sexual risk behavior among 239 PLWH (Kurth et al., 2014). Nearly three-quarters of the sample identified as a gay, bisexual or other MSM, and just over half were white. Compared to the control group, those receiving the CARE+ intervention demonstrated greater reductions in sexual risk (i.e., CAS or condom use with errors) at the 6- and 9-month assessment time points, as well as improved self-reported ART adherence.
Conclusions and Recommendations
Addressing the sexual, physical, and mental health needs of people living with HIV has received increasing attention in recent years, recognizing that reducing risk for transmission among persons already infected with the virus can have a larger impact on overall rates of HIV than focusing efforts on low or moderate risk uninfected individuals (Lasry, Sansom, Hicks, & Uzunangelov, 2012). Despite evidence that technology-mediated HIV risk reduction approaches are efficacious (Bailey et al., 2012), limited prevention interventions have been developed and rigorously tested exclusively for HIV positive populations (Horvath, Carrico et al., 2013; Horvath, Oakes et al., 2013).
Three conclusions are reached from this review of technology use, risk associated with online sex seeking, and current technology-based interventions for persons living with HIV. First, technology use is widespread among HIV positive populations who (much like other people living with chronic health conditions) are using technology as a resource to inform their medical care and connect with others who are living with HIV. Their experiences with, and beliefs about, technology provide invaluable information about best practices for designing interventions with a focus on HIV positive persons. However, people living with HIV are not a single homogenous group; rather, HIV status intersects with one or more identities (sexual orientation; gender; age; race and ethnicity; geographic residency) that will impact needs, preferences, and response to interventions. Therefore, inclusion of the target population in the development and testing of technology-based intervention approaches for PLWH is critical to design and implement effective interventions. This may take the form of community-based participatory research (Cashman et al., 2008; Rhodes et al., 2007), establishing a community advisory board, or conducting formative research prior to intervention development.
Second, even considering substantial methodological limitations of current studies of HIV risk behavior among HIV positive samples, studies consistently demonstrate high rates of HIV risk behavior among PLWH, particularly MSM. This may be in large part the result of broader social and cultural factors that influence PLWH at an individual level. Developing interventions that can reach and engage at-risk PLWH in their routine contexts and in a cost-effective manner are advantages of technology-based prevention approaches, and should be further developed. This review suggests that technology-mediated approaches targeting at-risk HIV positive persons may be enhanced by addressing issues of stigma, HIV status disclosure, personal responsibility, mental health problems, and substance use factors associated with increased risk for transmission. These complex issues may have more credibility and acceptability if they are rolled into interventions that also address the medical and social support needs of persons living with HIV.
Third, substantially more financial resources and institutional support are needed to develop and rigorously evaluate technology-based risk reduction approaches for PLWH, particularly those that target Black and Latino MSM, and to address critical questions that remain about these approaches (Noar, 2011; Sullivan et al., 2015). MSM of color are greatly underrepresented in intervention efforts, in contrast to the overrepresentation of MSM of color living with HIV (Wolitski et al., 2001). Failing to provide such support will result in a notable missed opportunity to improve the physical and mental well-being of PLWH through technology-based communication channels, as well as to reduce overall high rates of HIV infection among these populations (Simoni et al., 2015).
Numerous reviews of technology-based interventions note the vast opportunities that these approaches open for the HIV prevention field to address core needs of groups most affected and infected with HIV (Bailey et al., 2010; Chiasson et al., 2006; Noar & Willoughby, 2012; Sullivan et al., 2015). Despite this promise and evidence that PLWH are appropriate targets for intervention, we have collectively failed to take full advantage of technology-based approaches to HIV intervention. Despite the challenges that remain ahead, the time is right to invest in this future.
References
Adam, B. D., Murray, J., Ross, S., Oliver, J., Lincoln, S. G., & Rynard, V. (2011). ivstigma.com, an innovative web-supported stigma reduction intervention for gay and bisexual men. Health Education Research, 26(5), 795–807.
Amico, K. R. (2015). Evidence for technology interventions to promote ART adherence in adult populations: A review of the literature 2012–2015. Current HIV/AIDS Reports, 1–10. doi:10.1007/s11904-015-0286-4
Bachmann, L. H., Grimley, D. M., Gao, H., Aban, I., Chen, H., Raper, J. L., … Hook, E. W. (2013). Impact of a computer-assisted, provider-delivered intervention on sexual risk behaviors in HIV-positive men who have sex with men (MSM) in a primary care setting. AIDS Education and Prevention, 25(2), 87–101. doi:10.1521/aeap.2013.25.2.87
Bailey, J. V., Murray, E., Rait, G., Mercer, C. H., Morris, R. W., Peacock, R., … Nazareth, I. (2010). Interactive computer-based interventions for sexual health promotion. Cochrane Database of Systematic Reviews, 9, CD006483.
Bailey, J. V., Murray, E., Rait, G., Mercer, C. H., Morris, R. W., Peacock, R., … Nazareth, I. (2012). Computer-based interventions for sexual health promotion: Systematic review and meta-analyses. International Journal of STD & AIDS, 23(6), 408–413.
Bancroft, J., Janssen, E., Strong, D., & Vukadinovic, Z. (2003). The relation between mood and sexuality in gay men. Archives of Sexual Behavior, 32(3), 231–242.
Bandura, A. (1999). Moral disengagement in the perpetration of inhumanities. Personality and Social Psychology Review, 3, 193–209.
Bandura, A. (2002). Selective moral disengagement in the exercise of moral agency. Journal of Moral Education, 31, 101–119.
Bauermeister, J. A., Pingel, E. S., Jadwin-Cakmak, L., Harper, G. W., Horvath, K., Weiss, G., & Dittus, P. (2015). Acceptability and preliminary efficacy of a tailored online HIV/STI testing intervention for young men who have sex with men: The get connected! Program. AIDS and Behavior. doi:10.1007/s10461-015-1009-y
Bech, M., & Kristensen, M. B. (2009). Differential response rates in postal and web-based surveys among older respondents. Survey Research Methods, 3, 1–6.
Beck, A., McNally, I., & Petrak, J. (2003). Psychosocial predictors of HIV/STI risk behaviours in a sample of homosexual men. Sexually Transmitted Infections, 79(2), 142–146.
Beck, J., & Rosenbaum, M. (1994). Pursuit of ecstasy: The MDMA experience. New York: State University of New York Press.
Benotsch, E., Kalichman, S., & Cage, M. (2002). Men who have met sex partners via the internet: Prevalence, predictors, and implications for HIV prevention. Archives of Sexual Behavior, 31(2), 177–183.
Berger, B. E., Ferrans, C. E., & Lashley, F. R. (2001). Measuring stigma in people with HIV: Psychometric assessment of the HIV stigma scale. Research in Nursing & Health, 24(6), 518–529.
Berry, M., Raymond, H. F., Kellogg, T., & McFarland, W. (2008). The internet, HIV serosorting and transmission risk among men who have sex with men, San Francisco. AIDS, 22(6), 787–789.
Birnbaum, M. (2004). Human research and data collection via the internet. Annual Review of Psychology, 55, 803–832.
Blas, M. M., Alva, I. E., Carcamo, C. P., Cabello, R., Goodreau, S. M., Kimball, A. M., & Kurth, A. E. (2010). Effect of an online video-based intervention to increase HIV testing in men who have sex with men in Peru. PLoS One, 5(5), e10448.
Bolding, G., Davis, M., Sherr, L., Hart, G., & Elford, J. (2004). Use of gay internet sites and views about online health promotion among men who have sex with men. AIDS Care, 16, 993–1001.
Bowen, A. M., Horvath, K., & Williams, M. L. (2007). A randomized control trial of internet-delivered HIV prevention targeting rural MSM. Health Education Research, 22(1), 120–127.
Bull, S., Lloyd, L., Rietmeijer, C., & McFarlane, M. (2004). Recruitment and retention of an online sample for an HIV prevention intervention targeting men who have sex with men: The smart sex quest project. AIDS Care, 16(8), 931–943.
Bull, S., McFarlane, M., & King, D. (2001). Barriers to STD/HIV prevention on the internet. Health Education Research, 16(6), 661–670.
Bull, S., Pratte, K., Whitesell, N., Rietmeijer, C., & McFarlane, M. (2008). Effects of an internet-based intervention for HIV prevention: The Youthnet Trials. AIDS and Behavior, 13(3), 474–487.
Bull, S. S., McFarlane, M., & Reitmeijer, C. (2001). HIV and sexually transmitted infection risk behaviors among men seeking sex with men on-line. American Journal of Public Health, 91(6), 988–999.
Camacho-Gonzalez, A. F., Wallins, A., Toledo, L., Murray, A., Gaul, Z., Sutton, M. Y., … Chakraborty, R. (2016). Risk factors for HIV transmission and barriers to HIV disclosure: Metropolitan Atlanta youth perspectives. AIDS Patient Care and STDs, 30(1), 18–24. doi:10.1089/apc.2015.0163
Carballo-Dieguez, A., Miner, M., Dolezal, C., Rosser, B. R., & Jacoby, S. (2006). Sexual negotiation, HIV-status disclosure, and sexual risk behavior among Latino men who use the internet to seek sex with other men. Archives of Sexual Behavior, 35(4), 473–481.
Carey, J. W., Mejia, R., Bingham, T., Ciesielski, C., Gelaude, D., Herbst, J. H., … Stall, R. (2009). Drug use, high-risk sex behaviors, and increased risk for recent HIV infection among men who have sex with men in Chicago and Los Angeles. AIDS and Behavior, 13(6), 1084–1096.
Carpenter, K. M., Stoner, S. A., Mikko, A. N., Dhanak, L. P., & Parsons, J. T. (2009). Efficacy of a web-based intervention to reduce sexual risk in men who have sex with men. AIDS and Behavior. doi:10.1007/s10461-009-9578-2
Cashman, S. B., Adeky, S., Allen, A. J., 3rd, Corburn, J., Israel, B. A., Montano, J., … Eng, E. (2008). The power and the promise: Working with communities to analyze data, interpret findings, and get to outcomes. American Journal of Public Health, 98(8), 1407–1417. doi:10.2105/ajph.2007.113571
Casper, R. C., Redmond, D. E., Jr., Katz, M. M., Schaffer, C. B., Davis, J. M., & Koslow, S. H. (1985). Somatic symptoms in primary affective disorder. Presence and relationship to the classification of depression. Archives of General Psychiatry, 42(11), 1098–1104.
Centers for Disease Control and Prevention. (2003). Advancing HIV prevention: New strategies for a changing epidemic--United States, 2003. Morbidity and Mortality Weekly Report, 52(15), 329–332.
Centers for Disease Control and Prevention. (2016). Compendium of evidence-based interventions and best practices for HIV prevention. Retrieved from https://www.cdc.gov/hiv/research/interventionresearch/compendium/rr/index.html.
Chen, H. T., Grimley, D. M., Waithaka, Y., Aban, I. B., Hu, J., & Bachmann, L. H. (2008). A process evaluation of the implementation of a computer-based, health provider-delivered HIV-prevention intervention for HIV-positive men who have sex with men in the primary care setting. AIDS Care, 20(1), 51–60.
Chiasson, M., Hirshfield, S., Humberstone, M., DiFilippi, J., Koblin, B., & Remien, R. (2005). Increased high risk sexual behavior after September 11 in men who have sex with men: An internet survey. Archives of Sexual Behavior, 34(5), 527–535. doi:10.1007/s10508-005-6278-5
Chiasson, M., Hirshfield, S., Humberstone, M., Remien, R., Wolitski, R., & Wong, T. (2005). A comparison of on-line and off-line risk among men who have sex with men. Conference on Retroviruses and Opportunistic Infections.
Chiasson, M., Parsons, J., Tesoriero, J., Carballo-Dieguez, A., Hirshfield, S., & Remien, R. (2006). HIV behavioral research online. Journal of Urban Health, 83(1), 73–85.
Chiasson, M., Shuchat Shaw, F., Humberstone, M., Hirshfield, S., & Hartel, D. (2009). Increased HIV disclosure three months after an online video intervention for men who have sex with men (MSM). AIDS Care, 21, 1081–1089.
Chiasson, M. A., Hirshfield, S., Remien, R. H., Humberstone, M., Wong, T., & Wolitski, R. J. (2007). A comparison of on-line and off-line sexual risk in men who have sex with men: An event-based on-line survey. Journal of Acquired Immune Deficiency Syndromes, 44(2), 235–243.
Cochran, S., & Mays, V. (2000). Relation between psychiatric syndromes and behaviorally defined sexual orientation in a sample of the US population. American Journal of Epidemiology, 151, 516–523.
Cochran, S., Sullivan, J., & Mays, V. (2003). Prevalence of mental disorders, psychological distress, and mental health services use among lesbian, gay, and bisexual adults in the United States. Journal of Consulting and Clinical Psychology, 71(1), 53–61.
Cohen, M. S., Chen, Y. Q., McCauley, M., Gamble, T., Hosseinipour, M. C., Kumarasamy, N., … Fleming, T. R. (2011). Prevention of HIV-1 infection with early antiretroviral therapy. New England Journal of Medicine, 365(6), 493–505.
Cohen, M. S., Chen, Y. Q., McCauley, M., Gamble, T., Hosseinipour, M. C., Kumarasamy, N., … Godbole, S. V. (2016). Antiretroviral therapy for the prevention of HIV-1 transmission. New England Journal of Medicine, 375(9), 830–839.
Colfax, G., & Guzman, R. (2006). Club drugs and HIV infection: A review. Clinical Infectious Diseases, 42(10), 1463–1469.
Colfax, G., Shoptaw, S., Colfax, G., & Shoptaw, S. (2005). The methamphetamine epidemic: Implications for HIV prevention and treatment. [Review]. Current HIV/AIDS Reports, 2(4), 194–199.
Corbett, T. (2016). New to Grindr profiles: HIV status and last test date fields. Retrieved from http://www.grindr.com/blog/new-grindr-profiles-hiv-status-last-test-date/.
Courtenay-Quirk, C., Horvath, K. J., Ding, H., Fisher, H., McFarlane, M., Kachur, R., … Harwood, E. (2010). Perceptions of HIV-related websites among persons recently diagnosed with HIV. AIDS Patient Care and STDs, 24(2), 105–115.
Crepaz, N., & Marks, G. (2002). Towards an understanding of sexual risk behavior in people living with HIV: A review of social, psychological, and medical findings. AIDS, 16(2), 135–149.
Crepaz, N., Marks, G., Liau, A., Mullins, M. M., Aupont, L. W., Marshall, K. J., … Wolitski, R. J. (2009). Prevalence of unprotected anal intercourse among HIV-diagnosed MSM in the United States: A meta-analysis. AIDS, 23(13), 1617–1629.
Denscombe, M. (2009). Item non-response rates: Acomparison of online and paper questionnaires. International Journal of Social Research Methodology, 12, 281–291.
Dew, M., Becker, J., Sanchez, J., Caldararo, R., Lopez, O., Wess, J., … Banks, G. (1997). Prevalence and predictors of depressive, anxiety and substance use disorders in HIV-infected and uninfected men: A longitudinal evaluation. Psychological Medicine, 27, 395–409.
Downing, M., Chiasson, M. A., & Hirshfield, S. (2016). Recent anxiety symptoms and drug use associated with STI diagnosis among an online U.S. sample of men who have sex with men. Journal of Health Psychology, 21(12), 2799–2812.
Duru, O. K., Collins, R. L., Ciccarone, D. H., Morton, S. C., Stall, R., Beckman, R., … Kanouse, D. E. (2006). Correlates of sex without serostatus disclosure among a national probability sample of HIV patients. AIDS and Behavior, 10(5), 495–507.
Elford, J., Bolding, G., Davis, M., Sherr, L., & Hart, G. (2003). Web-based behavioural surveillance among men who have sex with men: A comparison of online and offline samples in London, UK. Paper presented at the STD/HIV prevention and the Internet 2003, Washington, DC.
Fortune, T., Wright, E., Juzang, I., & Bull, S. (2010). Recruitment, enrollment and retention of young black men for HIV prevention research: Experiences from the 411 for safe text project. Contemporary Clinical Trials, 31(2), 151–156.
Frosch, D., Shoptaw, S., Huber, A., Rawson, R. A., & Ling, W. (1996). Sexual HIV risk and gay and bisexual methamphetamine abusers. Journal of Substance Abuse Treatment, 13, 483–386.
Gamage, D. G., Sidat, M., Read, T., Cummings, R., Bradshaw, C. S., Howley, K., … Fairley, C. K. (2011). Evaluation of health map: A patient-centred web-based service for supporting HIV-infected patients. Sexual Health, 8(2), 194–198.
Gilbert, P., Ciccarone, D., Gansky, S. A., Bangsberg, D. R., Clanon, K., McPhee, S. J., … Gerbert, B. (2008). Interactive “video doctor” counseling reduces drug and sexual risk behaviors among HIV-positive patients in diverse outpatient settings. PLoS One, 3(4), e1988. doi:10.1371/journal.pone.0001988
Gilman, S., Cochran, S., Mays, V., Hughes, M., Ostrow, D., & Kessler, R. (2001). Risk of psychiatric disorders among individuals reporting same-sex sexual partners in the National Comorbidity Survey. American Journal of Public Health, 91(6), 933–939.
Goedel, W. C., & Duncan, D. T. (2015). Geosocial-Networking app usage patterns of gay, bisexual, and other men who have sex with men: Survey among users of Grindr, a mobile dating app. JMIR Public Health and Surveillance, 1(1), e4. doi:10.2196/publichealth.4353
Goedel, W. C., & Duncan, D. T. (2016). Contextual factors in geosocial-networking smartphone application use and engagement in condomless anal intercourse among gay, bisexual, and other men who have sex with men who use Grindr. Sexual Health. doi:10.1071/sh16008
Golden, M. R., Wood, R. W., Buskin, S. E., Fleming, M., & Harrington, R. D. (2007). Ongoing risk behavior among persons with HIV in medical care. AIDS and Behavior, 11(5), 726–735.
Gorbach, P. M., Drumright, L. N., Daar, E. S., & Little, S. J. (2006). Transmission behaviors of recently HIV-infected men who have sex with men. Journal of Acquired Immune Deficiency Syndromes, 42(1), 80–85.
Greenwood, G., White, E., Page-Shafer, K., Bein, E., Osmond, D., Paul, J., & Stall, R. (2001). Correlates of heavy substance use among young gay and bisexual men: The San Francisco Young Men's Health Study. Drug and Alcohol Dependence, 61(2), 105–112.
Grov, C. (2011). HIV risk and substance use in men who have sex with men surveyed in bathhouses, bars/clubs, and on Craigslist.org: Venue of recruitment matters. AIDS and Behavior, 16(4), 807–817.
Grov, C., Golub, S. A., & Parsons, J. T. (2010). HIV status differences in venues where highly sexually active gay and bisexual men meet sex partners: Results from a pilot study. AIDS Education and Prevention, 22(6), 496–508.
Grov, C., Hirshfield, S., Remien, R. H., Humberstone, M., & Chiasson, M. A. (2011). Exploring the venue's role in risky sexual behavior among gay and bisexual men: An event-level analysis from a National Online Survey in the U.S. Archives of Sexual Behavior, 42(2), 291–302.
Grov, C., Parsons, J. T., & Bimbi, D. S. (2007). Sexual risk behavior and venues for meeting sex partners: An intercept survey of gay and bisexual men in LA and NYC. AIDS and Behavior, 11(6), 915–926.
Groves, R. M., & Peytcheva, E. (2008). The impact of nonresponse rates on nonresponse bias. Public Opinion Quarterly, 72(2), 167–189.
Halkitis, P., Parsons, J., & Stirratt, M. (2001). A double epidemic: Crystal methamphetamine drug use in relation to HIV transmission among gay men. Journal of Homosexuality, 41(2), 17–35.
Halkitis, P., Parsons, J., & Wilton, L. (2003). Barebacking among gay and bisexual men in New York City: Explanations for the emergence of intentional unsafe behavior. Archives of Sexual Behavior, 32(4), 351–357.
Halkitis, P. N., & Parsons, J. T. (2003). Intentional unsafe sex (barebacking) among HIV-positive gay men who seek sexual partners on the Internet. AIDS Care, 15(3), 367–378.
Hall, H. I., Holtgrave, D. R., Tang, T., & Rhodes, P. (2013). HIV transmission in the United States: considerations of viral load, risk behavior, and health disparities. AIDS and Behavior, 17(5), 1632–1636. doi:10.1007/s10461-013-0426-z
Harawa, N. T., Williams, J. K., Ramamurthi, H. C., Manago, C., Avina, S., & Jones, M. (2008). Sexual behavior, sexual identity, and substance abuse among low-income bisexual and non-gay-identifying African American men who have sex with men. Archives of Sexual Behavior, 37(5), 748–762. doi:10.1007/s10508-008-9361-x
Harris, L. T., Lehavot, K., Huh, D., Yard, S., Andrasik, M. P., Dunbar, P. J., & Simoni, J. M. (2010). Two-way text messaging for health behavior change among human immunodeficiency virus-positive individuals. Telemedicine Journal and E-Health, 16(10), 1024–1029.
Hatfield, L. A., Horvath, K. J., Jacoby, S. M., Simon Rosser, B. R., Hatfield, L. A., Horvath, K. J., & Jacoby, S. M. (2009). Comparison of substance use and risky sexual behavior among a diverse sample of urban, HIV-positive men who have sex with men. Journal of Addictive Diseases, 28(3), 208–218.
Hightow-Weidman, L. B., Pike, E., Fowler, B., Matthews, D. M., Kibe, J., McCoy, R., & Adimora, A. A. (2012). HealthMpowerment.org: Feasibility and acceptability of delivering an internet intervention to young black men who have sex with men. AIDS Care, 24(7), 910–920.
Hirshfield, S., Chiasson, M. A., Joseph, H., Scheinmann, R., Johnson, W. D., Remien, R. H., … Margolis, A. D. (2012). An online randomized controlled trial evaluating HIV prevention digital media interventions for men who have sex with men. PLoS One, 7(10), e46252.
Hirshfield, S., Downing, M. J., Parsons, J. T., Grov, C., Gordon, R. J., Houang, S. T., … Chiasson, M. A. (2016). Developing a video-based randomized controlled trial for HIV-positive gay, bisexual and other men who have sex with men. JMIR Research Protocols, 5(2), e125.
Hirshfield, S., Grov, C., Parsons, J., Anderson, I., & Chiasson, M. A. (2015). Social media use and HIV transmission risk behavior among ethnically diverse HIV-positive men who have sex with men: Results of an online study in three U.S. States. Archives of Sexual Behavior, 44(7), 1969–1978.
Hirshfield, S., Remien, R., & Chiasson, M. (2006). Crystal methamphetamine use among men who have sex with men: Results from two National Online Studies. Journal of Gay and Lesbian Psychotherapy, 10, 85–93.
Hirshfield, S., Remien, R., Humberstone, M., Walavalkar, I., & Chiasson, M. (2004a). Substance use and high-risk sex among men who have sex with men: A national online study in the USA. AIDS Care, 16(8), 1036–1047.
Hirshfield, S., Remien, R. H., Walavalkar, I., & Chiasson, M. A. (2004b). Crystal methamphetamine use predicts incident STD infection among men who have sex with men recruited online: A nested case-control study. Journal of Medical Internet Research, 6, e41.
Hirshfield, S., Schrimshaw, E. W., Stall, R., Margolis, A. D., Downing, M. J., & Chiasson, M. A. (2015). Drug use, sexual risk, and syndemic production among MSM who engage in group sex encounters. American Journal of Public Health, e1–e10.
Hirshfield, S., Wolitski, R. J., Chiasson, M. A., Remien, R. H., Humberstone, M., & Wong, T. (2008). Screening for depressive symptoms in an online sample of men who have sex with men. AIDS Care, 20, 904–910.
Horvath, K. J., Carrico, A. W., Simoni, J., Boyer, E., Amico, K. R., & Petroll, A. E. (2013). Engagement in HIV medical care and technology use among stimulant-using and nonstimulant-using men who have sex with men. AIDS Research & Treatment, 2013, 121352. doi:10.1155/2013/121352
Horvath, K. J., Danilenko, G., Williams, M., Simoni, J., Amico, K. R., Oakes, J. M., & Simon Rosser, B. R. (2012). Technology use and reasons to participate in social networking health websites among people living with HIV in the US. AIDS and Behavior, 16(4), 900–910.
Horvath, K. J., Nygaard, K., Danilenko, G., Goknur, S., Michael Oakes, J., & Simon Rosser, B. (2012). Strategies to retain participants in a longterm HIV prevention randomized controlled trial: Lessons from the MINTS-II study. AIDS and Behavior, 16(2), 469–479.
Horvath, K. J., Alemu, D., Danh, T., Baker, J. V., & Carrico, A. W. (2016). Creating effective mobile phone apps to optimize antiretroviral therapy adherence: Perspectives from stimulant-using HIV-positive men who have sex with men. JMIR Mhealth Uhealth, 4(2), e48. doi:10.2196/mhealth.5287
Horvath, K. J., Michael Oakes, J., Simon Rosser, B. R., Danilenko, G., Vezina, H., Rivet Amico, K., … Simoni, J. (2013). Feasibility, acceptability and preliminary efficacy of an online peer-to-peer social support ART adherence intervention. AIDS and Behavior, 17(6), 2031–2044.
Horvath, K. J., Oakes, J. M., & Rosser, B. R. S. (2008). Sexual negotiation and HIV serodisclosure among men who have sex with men with their online and offline partners. Journal of Urban Health, 85(5), 744–758.
Horvath, K. J., Rosser, B., & Remafedi, G. (2008). Sexual risk taking among young internet-using men who have sex with men. American Journal of Public Health, 98(6), 1059–1067.
Horvath, K. J., Smolenski, D., Iantaffi, A., Grey, J. A., & Rosser, B. R. (2012). Discussions of viral load in negotiating sexual episodes with primary and casual partners among men who have sex with men. AIDS Care, 24(8), 1052–1055.
Huang, E., Marlin, R. W., Young, S. D., Medline, A., & Klausner, J. D. (2016). Using Grindr, a smartphone social-networking application, to increase HIV self-testing among black and Latino men who have sex with men in Los Angeles, 2014. AIDS Education and Prevention, 28(4), 341–350. doi:10.1521/aeap.2016.28.4.341
Johnson, M. O., Dilworth, S. E., Neilands, T. B., Chesney, M. A., Rotheram-Borus, M. J., Remien, R. H., … Morin, S. F. (2008). Predictors of attrition among high risk HIV-infected participants enrolled in a multi-site prevention trial. AIDS and Behavior, 12(6), 974–977.
Kalichman, S. C., Cherry, C., Cain, D., Pope, H., & Kalichman, M. (2005). Psychosocial and behavioral correlates of seeking sex partners on the internet among HIV-positive men. Annals of Behavioral Medicine, 30(3), 243–250.
Kalichman, S. C., Cherry, C., Cain, D., Pope, H., Kalichman, M., Eaton, L., … Benotsch, E. G. (2006). Internet-based health information consumer skills intervention for people living with HIV/AIDS. Journal of Consulting and Clinical Psychology, 74(3), 545–554.
Kalichman, S. C., & Hunter, T. L. (1992). The disclosure of celebrity HIV infection: Its effects on public attitudes. American Journal of Public Health, 82(10), 1374–1376.
Kalichman, S. C., Rompa, D., & Cage, M. (2000). Sexually transmitted infections among HIV seropositive men and women. Sexually Transmitted Infections, 76(5), 350–354.
Kelly, J. A., Murphy, D. A., Bahr, G. R., Koob, J. J., Morgan, M. G., Kalichman, S. C., … St Lawrence, J. S. (1993). Factors associated with severity of depression and high-risk sexual behavior among persons diagnosed with human immunodeficiency virus (HIV) infection. Health Psychology, 12(3), 215–219.
Kennedy, S., Dickens, S., Eisfeld, B., & Bagby, R. (1999). Sexual dysfunction before antidepressant therapy in major depression. Journal of Affective Disorders, 56, 201–208.
Khosropour, C. M. (2011). Retention and HIV testing of MSM enrolled in a 12-month online study. Paper presented at the Sex Tech Conference, San Francisco, CA. Retrieved from http://www.slideshare.net/isisinc/retension-and-hivtestingkhosropour.
Kilmarx, P. H., & Mermin, J. (2012). Prevention with people with HIV in the United States: The nexus of HIV prevention and treatment. Journal of Acquired Immune Deficiency Syndromes, 60(3), 219–220.
Kim, A., Kent, C., McFarland, W., & Klausner, J. (2001). Cruising on the Internet highway. Journal of Acquired Immune Deficiency Syndrome, 28(1), 89–93.
Kipke, M., Kubicek, K., Weiss, G., Wong, C., Lopez, D., Iverson, E., & Ford, W. (2007). The health and health behaviors of young men who have sex with men. Journal of Adolescent Health, 40, 342–350.
Klausner, J., Wolf, W., Fischer-Ponce, L., Zolt, I., & Katz, M. (2000). Tracing a syphilis outbreak through cyberspace. [see comment]. JAMA, 284(4), 447–449.
Klitzman, R., Exner, T., Correale, J., Kirshenbaum, S. B., Remien, R., Ehrhardt, A. A., … Charlebois, E. (2007). It's not just what you say: Relationships of HIV dislosure and risk reduction among MSM in the post-HAART era. AIDS Care, 19(6), 749–756.
Kraut, R., Patterson, M., Lundmark, V., Kiesler, S., Mukopadhyay, T., & Scherlis, W. (1998). Internet paradox. A social technology that reduces social involvement and psychological well-being? American Psychologist, 53(9), 1017–1031.
Kremer, H., & Ironson, G. (2007). People living with HIV: Sources of information on antiretroviral treatment and preferences for involvement in treatment decision-making. European Journal of Medical Research, 12(1), 34–42.
Kurth, A. E., Spielberg, F., Cleland, C. M., Lambdin, B., Bangsberg, D. R., Frick, P. A., … Holmes, K. K. (2014). Computerized counseling reduces HIV-1 viral load and sexual transmission risk: Findings from a randomized controlled trial. Journal of Acquired Immune Deficiency Syndromes: JAIDS, 65(5), 611–620. doi:10.1097/qai.0000000000000100
Kwak, N., & Radler, B. (2002). A comparison between mail and web surveys: Response pattern, respondent profile, and data quality. Journal of Official Statistics, 18(2), 257–273.
Landovitz, R. J., Tseng, C. H., Weissman, M., Haymer, M., Mendenhall, B., Rogers, K., … Shoptaw, S. (2012). Epidemiology, sexual risk behavior, and HIV prevention practices of men who have sex with men using GRINDR in Los Angeles, California. Journal of Urban Health, 90(4), 729–739.
Lasry, A., Sansom, S. L., Hicks, K. A., & Uzunangelov, V. (2012). Allocating HIV prevention funds in the United States: Recommendations from an optimization model. PLoS One, 7(6), e37545.
Lau, J. T., Lau, M., Cheung, A., & Tsui, H. Y. (2008). A randomized controlled study to evaluate the efficacy of an Internet-based intervention in reducing HIV risk behaviors among men who have sex with men in Hong Kong. AIDS Care, 20(7), 820–828.
Lelutiu-Weinberger, C., Pachankis, J. E., Gamarel, K. E., Surace, A., Golub, S. A., & Parsons, J. T. (2015). Feasibility, acceptability, and preliminary efficacy of a live-chat social media intervention to reduce HIV risk among young men who have sex with men. AIDS and Behavior, 19(7), 1214–1227. doi:10.1007/s10461-014-0911-z
Lester, R. T., Ritvo, P., Mills, E. J., Kariri, A., Karanja, S., Chung, M. H., … Plummer, F. A. (2010). Effects of a mobile phone short message service on antiretroviral treatment adherence in Kenya (WelTel Kenya1): A randomised trial. The Lancet, 376(9755), 1838–1845.
Lewis, L., & Ross, M. (1995). A select body: The gay dance party subculture and the HIV/AIDS pandemic. New York: Cassell.
Lewis, M. A., Uhrig, J. D., Ayala, G., & Stryker, J. (2011). Reaching men who have sex with men for HIV prevention messaging with new media: Recommendations from an expert consultation. Annals of the Forum for Collaborative HIV Research, 13(3), 11–18.
Lewnard, J. A., & Berrang-Ford, L. (2014). Internet-based partner selection and risk for unprotected anal intercourse in sexual encounters among men who have sex with men: A meta-analysis of observational studies. Sexually Transmitted Infections, 90, 290–296.
Liau, A., Millett, G., & Marks, G. (2006). Meta-analytic examination of online sex-seeking and sexual risk behavior among men who have sex with men. Sexually Transmitted Diseases, 33(9), 576–584.
Link, M. W., & Mokdad, A. H. (2005). Alternative modes for health surveillance surveys: An experiment with web, mail, and telephone. Epidemiology, 16(5), 701–704.
Margolis, A. D., Joseph, H., Hirshfield, S., Chiasson, M. A., Belcher, L., & Purcell, D. W. (2014). Anal intercourse without condoms among HIV-positive men who have sex with men recruited from a sexual networking web site, United States. Sexually Transmitted Diseases, 41, 749–755.
Marks, G., Bingman, C. R., & Duval, T. S. (1998). Negative affect and unsafe sex in HIV-positive men. AIDS and Behavior, 2(2), 89–99.
Marks, G., & Crepaz, N. (2001). HIV-positive men's sexual practices in the context of self-disclosure of HIV status. Journal of Acquired Immune Deficiency Syndromes, 27(1), 79–85.
Mathew, R. J., & Weinman, M. L. (1982). Sexual dysfunctions in depression. Archives of Sexual Behavior, 11(4), 323–328.
Mays, V. M., Cochran, S. D., & Zamudio, A. (2004). HIV prevention research: Are we meeting the needs of African American men who have sex with men? Journal of Black Psychology, 30(1), 78–105.
McFarlane, M., Bull, S., & Rietmeijer, C. (2000). The Internet as a newly emerging risk environment for sexually transmitted diseases. JAMA, 284(4), 443–446.
McFarlane, M., Bull, S. S., & Reitmeijer, C. A. (2000). The Internet as a newly emerging risk environment for sexually transmitted diseases. Journal of the American Medical Association, 284(4), 443–446.
Mckirnan, D., Ostrow, D., & Hope, B. (1996). Sex, drugs and escape: A psychological model of HIV-risk sexual behaviours. AIDS Care, 8(6), 655–659.
McKirnan, D., Vanable, P., Ostrow, D., & Hope, B. (2001). Expectancies of sexual “escape” and sexual risk among drug and alcohol-involved gay and bisexual men. Journal of Substance Abuse, 13(1–2), 137–154.
Mettey, A., Crosby, R., DiClemente, R., & Holtgrave, D. (2003). Associations between Internet sex seeking and STI associated risk behaviours among men who have sex with men. Sexually Transmitted Infections, 79(6), 466–468.
Mills, T., Paul, J., Stall, R., Pollack, L., Canchola, J., Chang, Y., … Catania, J. (2004). Distress and depression in men who have sex with men: The urban Men's health study. American Journal of Psychiatry, 161, 278–285.
Mimiaga, M. J., Fair, A. D., Mayer, K. H., Koenen, K., Gortmaker, S., Tetu, A. M., … Safren, S. A. (2008). Experiences and sexual behaviors of HIV-infected MSM who acquired HIV in the context of crystal methamphetamine use. AIDS Education and Prevention, 20(1), 30–41.
Morgan, C., & Cotten, S. (2003). The relationship between Internet activities and depressive symptoms in a sample of college freshmen. Cyberpsychology & Behavior, 6(2), 133–142.
Mustanski, B., Garofalo, R., Monahan, C., Gratzer, B., & Andrews, R. (2013). Feasibility, acceptability, and preliminary efficacy of an online HIV prevention program for diverse young men who have sex with men: The keep it up! Intervention. AIDS and Behavior, 17(9), 2999–3012. doi:10.1007/s10461-013-0507-z
Mustanski, B. S. (2007). Are sexual partners met online associated with HIV/STI risk behaviours? Retrospective and daily diary data in conflict. AIDS Care, 19(6), 822–827.
Newman, J., Des Jarlais, D., Turner, C., Gribble, J., Cooley, P., & Paone, D. (2002). The differential effects of face-to-face and computer interview modes. American Journal of Public Health, 92, 294–297.
Noar, S. M. (2011). Computer technology-based interventions in HIV prevention: State of the evidence and future directions for research. AIDS Care, 23(5), 525–533.
Noar, S. M., Black, H. G., & Pierce, L. B. (2009). Efficacy of computer technology-based HIV prevention interventions: A meta-analysis. AIDS, 23(1), 107–115.
Noar, S. M., & Willoughby, J. F. (2012). eHealth interventions for HIV prevention. AIDS Care, 24(8), 945–952.
Nodin, N., Valera, P., Ventuneac, A., Maynard, E., & Carballo-Diéguez, A. (2011). The Internet profiles of men who have sex with men within bareback websites. Culture, Health & Sexuality, 13(9), 1015–1029.
O’Leary, A., Horvath, K., & Simon Rosser, B. R. (2012). Associations between partner-venue specific personal responsibility beliefs and transmission risk behavior by HIV-positive men who have sex with men (MSM). AIDS and Behavior, 1–7.
O'Leary, A., & Wolitski, R. J. (2009). Moral agency and the sexual transmission of HIV. Psychological Bulletin, 135(3), 478–494.
Orellana, E. R., Picciano, J. F., Roffman, R. A., Swanson, F., & Kalichman, S. C. (2006). Correlates of nonparticipation in an HIV prevention program for MSM. AIDS Education and Prevention, 18(4), 348–361.
Ostergren, J. E., Rosser, B. R. S., & Horvath, K. J. (2010). Reasons for non-use of condoms among men who have sex with men: A comparison of receptive and insertive role in sex and online and offline meeting venue. Culture, Health & Sexuality, 13(2), 123–140.
Parsons, J. T., Halkitis, P. N., Wolitski, R. J., & Gomez, C. A. (2003). Correlates of sexual risk behaviors among HIV-positive men who have sex with men. AIDS Education and Prevention, 15(5), 383–400.
Parsons, J. T., Schrimshaw, E. W., Wolitski, R. J., Halkitis, P. N., Purcell, D. W., Hoff, C. C., & Gomez, C. A. (2005). Sexual harm reduction practices of HIV-seropositive gay and bisexual men: Serosorting, strategic positioning, and withdrawal before ejaculation. AIDS, 19(Suppl 1), S13–S25.
Parsons, J. T., Severino, J., Nanin, J., Punzalan, J. C., von Sternberg, K., Missildine, W., & Frost, D. (2006). Positive, negative, unknown: Assumptions of HIV status among HIV-positive men who have sex with men. AIDS Education and Prevention, 18(2), 139–149.
Pennise, M., Inscho, R., Herpin, K., Owens, J., Jr., Bedard, B. A., Weimer, A. C., & Kennedy, B. S. (2015). Using smartphone apps in STD interviews to find sexual partners. Public Health Reports, 130, 245–252.
Pequegnat, W., Rosser, B. R., Bowen, A. M., Bull, S. S., Diclemente, R. J., Bockting, W. O., … Zimmerman, R. (2007). Conducting Internet-based HIV/STD prevention survey research: Considerations in design and evaluation. AIDS and Behavior, 11(4), 505–521.
Perlis, T. E., Des Jarlais, D., Friedman, S., Arasteh, K., & Turner, C. (2004). Audio-computerized self-interviewing versus face-to-face interviewing for research data collection at drug abuse treatment programs. Addiction, 99, 885–896.
Pew Research Center. (2011). Health topics: 80% of Internet users look for health information online. Retrieved December 9, 2016 from http://www.pewinternet.org/files/old-media//Files/Reports/2011/PIP_Health_Topics.pdf.
Pew Research Center. (2014a). Internet user demographics. Retrieved from http://www.pewinternet.org/data-trend/internet-use/latest-stats/.
Pew Research Center. (2014b). Cell phone and smartphone ownership demographics. Retrieved from http://www.pewinternet.org/data-trend/mobile/cell-phone-and-smartphone-ownership-demographics/.
Phillips, G., Grov, C., & Mustanski, B. (2015). Engagement in group sex among geosocial networking mobile application-using men who have sex with men. Sexual Health, 12(6), 495–500.
Plankey, M. W., Ostrow, D. G., Stall, R., Cox, C., Li, X., Peck, J. A., … Jacobson, L. P. (2007). The relationship between methamphetamine and popper use and risk of HIV seroconversion in the multicenter AIDS cohort study. Journal of Acquired Immune Deficiency Syndromes: JAIDS, 45(1), 85–92.
Poppen, P., Reisen, C., Zea, M., Bianchi, F., & Echeverry, J. (2004). Predictors of unprotected anal intercourse among HIV-positive Latino gay and bisexual men. AIDS and Behavior, 8(4), 379–389.
Rabkin, J., McElhiney, M., & Ferrando, S. (2004). Mood and substance use disorders in older adults with HIV/AIDS: Methodological issues and preliminary evidence. AIDS, 18(Suppl 1), S43–S48.
Radcliffe, J., Doty, N., Hawkins, L. A., Gaskins, C. S., Beidas, R., & Rudy, B. J. (2010). Stigma and sexual health risk in HIV-positive African American young men who have sex with men. AIDS Patient Care and STDs, 24(8), 493–499.
Rajasingham, R., Mimiaga, M. J., White, J. M., Pinkston, M. M., Baden, R. P., & Mitty, J. A. (2012). A systematic review of behavioral and treatment outcome studies among HIV-infected men who have sex with men who abuse crystal methamphetamine. AIDS Patient Care and STDs, 26(1), 36–52.
Rendina, H. J., Jimenez, R. H., Grov, C., Ventuneac, A., & Parsons, J. T. (2014). Patterns of lifetime and recent HIV testing among men who have sex with men in New York City who use Grindr. AIDS and Behavior, 18(1), 41–49. doi:10.1007/s10461-013-0573-2
Rhodes, S. D., Hergenrather, K. C., Duncan, J., Ramsey, B., Yee, L. J., & Wilkin, A. M. (2007). Using community-based participatory research to develop a chat room-based HIV prevention intervention for gay men. Progress in Community Health Partnerships, 1(2), 175–184.
Rietmeijer, C., Bull, S., McFarlane, M., Patnaik, J., & Douglas, J., Jr. (2002). Risks and benefits of the Internet for populations at risk for sexually transmitted infections (STIs). Sexually Transmitted Diseases, 30, 15–19.
Rietmeijer, C. A., Bull, S. S., & McFarlane, M. (2001). Sex and the Internet. AIDS, 15, 1433–1434.
Roffman, R. A., Klepsch, R., Wertz, J. S., Simpson, E. E., & Stephens, R. S. (1993). Predictors of attrition from an outpatient marijuana-dependence counseling program. Addictive Behaviors, 18(5), 553–566.
Rosenberg, E. S., Khosropour, C. M., & Sullivan, P. S. (2012). High prevalence of sexual concurrency and concurrent unprotected anal intercourse across racial/ethnic groups among a national, Web-based study of men who have sex with men in the United States. Sexually Transmitted Diseases, 39(10), 741–746.
Ross, M. W., Rosser, B. R., & Stanton, J. (2004). Beliefs about cybersex and Internet-mediated sex of Latino men who have Internet sex with men: Relationships with sexual practices in cybersex and in real life. AIDS Care, 16(8), 1002–1011.
Ross, M. W., Rosser, B. R., Stanton, J., & Konstan, J. (2004). Characteristics of Latino men who have sex with men on the Internet who complete and drop out of an Internet-based sexual behavior survey. AIDS Education and Prevention, 16(6), 526–537.
Ross, M. W., Rosser, B. R. S., McCurdy, S., & Feldman, J. (2007). The advantages and limitations of seeking sex online: A comparison of reasons given for online and offline sexual liaisons by men who have sex with men. Journal of Sex Research, 44(1), 59–71.
Rosser, B., Miner, M. H., Bockting, W. O., Ross, M. W., Konstan, J., Gurak, L., … Coleman, E. (2009). HIV risk and the Internet: Results of the Men's INTernet Sex (MINTS) Study. AIDS and Behavior, 13(4), 746–756.
Rosser, B., Oakes, J., Horvath, K., Konstan, J., Danilenko, G., & Peterson, J. (2009). HIV sexual risk behavior by men who use the Internet to seek sex with men: Results of the Men’s INTernet Sex Study-II (MINTS-II). AIDS and Behavior, 13(3), 488–498.
Rosser, B. R., Oakes, J. M., Konstan, J., Hooper, S., Horvath, K. J., Danilenko, G. P., … Smolenski, D. J. (2010). Reducing HIV risk behavior of men who have sex with men through persuasive computing: Results of the Men's INTernet Study-II. AIDS, 24(13), 2099–2107.
Rosser, B. R. S., Horvath, K. J., Hatfield, L. A., Peterson, J. L., Jacoby, S., Stately, A., & the Positive Connections. (2008). Predictors of HIV disclosure to secondary partners and sexual risk behavior among a high-risk sample of HIV-positive MSM: Results from six epicenters in the US. AIDS Care, 20(8), 925–930.
Rosser, B. R. S., West, W., & Weinmeyer, R. (2008). Are gay communities dying or just in transition? Results from an international consultation examining possible structural change in gay communities. AIDS Care, 20(5), 588–595.
Scheer, S., Chu, P., Klausner, J., Katz, M., & Schwarcz, S. (2001). Effect of highly active antiretroviral therapy on diagnoses of sexually transmitted diseases in people with AIDS. Lancet, 357(9254), 432–435.
Schwarcz, S., Scheer, S., McFarland, W., Katz, M., Valleroy, L., Chen, S., & Catania, J. (2007). Prevalence of HIV infection and predictors of high-transmission sexual risk behaviors among men who have sex with men. American Journal of Public Health, 97(6), 1067–1075.
Semple, S. J., Zians, J., Strathdee, S. A., & Patterson, T. L. (2008). Sexual marathons and methamphetamine use among HIV-positive men who have sex with men. Archives of Sexual Behavior, 38(4), 583–590.
Shaw, L., & Gant, L. (2002). In defense of the Internet: The relationship between Internet communication and depression, loneliness, self-esteem, and perceived social support. Cyberpsychology & Behavior, 5(2), 157–171.
Shin, E., Johnson, T. P., & Rao, K. (2012). Survey mode effects on data quality: Comparison of web and mail modes in a U.S. National Panel Survey. Social Science Computer Review, 30(2), 212–228.
Simoni, J. M., Kutner, B. A., & Horvath, K. J. (2015). Opportunities and challenges of digital technology for HIV treatment and prevention. Current HIV/AIDS Reports, 1–4. doi:10.1007/s11904-015-0289-1
Simoni, J. M., & Pantalone, D. W. (2004). Secrets and safety in the age of AIDS: Does HIV disclosure lead to safer sex? Topics in HIV Medicine, 12(4), 109–118.
Smith, A. (2010a). Mobile Access 2010. Pew Internet & American Life Project. Retrieved November 8, 2011 from http://www.Pewinternet.Org/reports/2010/mobile-access-2010/part-2.Aspx – footnote3
Smith, A. (2010b). Technology trends among people of color. Pew Internet & American life project. Retrieved November 8, 2011 from http://www.pewinternet.org/Commentary/2010/September/Technology-Trends-Among-People-of-Color.aspx.
Stahlman, S., Lyons, C., Sullivan, P. S., Mayer, K. H., Hosein, S., Beyrer, C., & Baral, S. D. (2016). HIV incidence among gay men and other men who have sex with men in 2020: Where is the epidemic heading? Sexual Health. doi:10.1071/sh16070
Stein, M. D., Freedberg, K. A., Sullivan, L. M., Savetsky, J., Levenson, S. M., Hingson, R., & Samet, J. H. (1998). Sexual ethics. Disclosure of HIV-positive status to partners. Archives of Internal Medicine, 158(3), 253–257.
Sullivan, P. S., Hamouda, O., Delpech, V., Geduld, J. E., Prejean, J., Semaille, C., … Fenton, K. A. (2009). Reemergence of the HIV epidemic among men who have sex with men in North America, Western Europe, and Australia, 1996–2005. Annals of Epidemiology, 19(6), 423–431.
Sullivan, P. S., Jones, J., Kishore, N., & Stephenson, R. (2015). The roles of Technology in Primary HIV prevention for men who have sex with men. Current HIV/AIDS Reports, 12(4), 481–488. doi:10.1007/s11904-015-0293-5
Tashima, K., Alt, E., Harwell, J., Fiebich-Perez, D., & Flanigan, T. (2003). Internet sex-seeking leads to acute HIV infection: A report of two cases. International Journal of STD & AIDS, 14(4), 285–286.
Taylor, M., Aynalem, G., Smith, L., Bemis, C., Kenney, K., & Kerndt, P. (2004). Correlates of Internet use to meet sex partners among men who have sex with men diagnosed with early syphilis in Los Angeles County. Sexually Transmitted Diseases, 31, 552–556.
Thiede, H., Jenkins, R. A., Carey, J. W., Hutcheson, R., Thomas, K. K., Stall, R. D., … Golden, M. R. (2008). Determinants of recent HIV infection among Seattle-area men who have sex with men. American Journal of Public Health, 99(Suppl 1), S157–S164.
Tikkanen, R., & Ross, M. (2003). Technological tearoom trade: Characteristics of Swedish men visiting gay Internet chat rooms. AIDS Education and Prevention, 15(2), 122–132.
Topp, L., Hando, J., & Dillon, P. (1999). Sexual behaviour of ectasy users in Sydney, Australia. Culture, Health, & Sexuality, 1, 147–159.
Vanable, P. A., Carey, M. P., Carey, K. B., & Maisto, S. A. (2002). Predictors of participation and attrition in a health promotion study involving psychiatric outpatients. Journal of Consulting and Clinical Psychology, 70(2), 362–368.
Venkatesh, V., & Bala, H. (2008). Technology acceptance model 3 and a research agenda on interventions. Decision Sciences, 39(2), 273–315. doi:10.1111/j.1540-5915.2008.00192.x
Weiss, R., & Samenow, C. P. (2010). Smart phones, social networking, sexting and problematic sexual behaviors—A call for research. Sexual Addiction & Compulsivity, 17(4), 241–246.
White, J. M., Mimiaga, M. J., Reisner, S. L., & Mayer, K. H. (2012). HIV sexual risk behavior among black men who meet other men on the Internet for sex. Journal of Urban Health, 90(3), 464–481.
Wilson, P. A., Valera, P., Ventuneac, A., Balan, I., Rowe, M., & Carballo-Dieguez, A. (2009). Race-based sexual stereotyping and sexual partnering among men who use the Internet to identify other men for bareback sex. Journal of Sex Research, 46(5), 399–413.
Winter, A. K., Sullivan, P. S., Khosropour, C. M., & Rosenberg, E. S. (2012). Discussion of HIV status by Serostatus and partnership sexual risk among Internet-using MSM in the United States. Journal of Acquired Immune Deficiency Syndromes: JAIDS, 60(5), 525–529.
Wolitski, R., Vadiserri, R., Denning, P., & Levine, W. (2001). Are we headed for a resurgence of the HIV epidemic among men who have sex with men? American Journal of Public Health, 91(6), 883–888.
Wolitski, R. J., Flores, S. A., O'Leary, A., Bimbi, D. S., & Gomez, C. A. (2007). Beliefs about personal and partner responsibility among HIV-seropositive men who have sex with men: Measurement and association with transmission risk behavior. AIDS and Behavior, 11(5), 676–686.
Wong, N., Gullo, K., & Stafford, J. (2004). Gays lead non-gays in cell phone use, cable TV and HDTV viewership. Technology use and preferences of gay and non-gay consumers [News story]. Retrieved from http://www.prnewswire.com/.
Wright, E., Fortune, T., Juzang, I., & Bull, S. (2011). Text messaging for HIV prevention with young black men: Formative research and campaign development. AIDS Care, 23(5), 534–541.
Young, S. D., Holloway, I., Jaganath, D., Westmoreland, D., & Coates, T. (2014). Project HOPE: Online social network changes in an HIV prevention randomized controlled trial for African American and Latino men who have sex with men. American Journal of Public Health, 104, 1707–1712.
Yu, G., Wall, M. W., Chiasson, M. A., & Hirshfield, S. (2015). Complex drug use patterns and associated HIV transmission risk behaviors in an Internet sample of US men who have sex with men. Archives of Sexual Behavior, 44(2), 421–428.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer Science+Business Media LLC
About this chapter
Cite this chapter
Horvath, K.J., Hirshfield, S. (2017). “Poz” in the Age of Technology: Technology, Sex, and Interventions to Reduce Risk for HIV Positive Men Who Have Sex with Men. In: Wilton, L. (eds) Understanding Prevention for HIV Positive Gay Men. Springer, New York, NY. https://doi.org/10.1007/978-1-4419-0203-0_16
Download citation
DOI: https://doi.org/10.1007/978-1-4419-0203-0_16
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4419-0202-3
Online ISBN: 978-1-4419-0203-0
eBook Packages: MedicineMedicine (R0)