Abstract
Background: Carnitine-acylcarnitine translocase (CACT) deficiency is a rare autosomal recessive disease in the mitochondrial transport of long-chain fatty acids. Despite early diagnosis and treatment, the disease still has a high mortality rate.
Methods: Clinical symptoms, long-term follow-up, and biochemical and molecular results of four cases are described and compared with the reviewed literature data of 55 cases.
Results: Two cases with neonatal onset, carrying in homozygosity the novel variant sequences p.Gly20Asp (c.59G>A) and p.Arg179Gly (c.536A>G), died during an intercurrent infectious process in the first year of life despite adequate dietetic treatment (frequent feeding, high-carbohydrate/low-fat diet, MCT, carnitine). The other two cases, one with infantile onset and the other diagnosed in the newborn period after a previous affected sibling, show excellent development at 4 and 16 years of age under treatment. The review shows that the most frequent presenting symptoms of CACT deficiency are hypoketotic hypoglycemia, hyperammonemia, hepatomegaly, cardiomyopathy and/or arrhythmia, and respiratory distress. The onset of symptoms is predominantly neonatal in 82% and infantile in 18%. The mortality rate is high (65%), most in the first year of life due to myocardiopathy or sudden death. Outcomes seem to correlate better with the absence of cardiac disease and with a higher long-chain fatty acid oxidation rate in cultured fibroblasts than with residual enzyme activity.
Conclusion: Diagnosis before the occurrence of clinical symptoms by tandem MS–MS and very early therapeutic intervention together with good dietary compliance could lead to a better prognosis, especially in milder clinical cases.
Competing interests: None declared
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Carnitine-acylcarnitine translocase (CACT) belongs to the family of SLC25 mitochondrial carriers and catalyzes both unidirectional transport of carnitine and carnitine/acylcarnitine exchange in the inner mitochondrial membrane, allowing the import of long-chain fatty acids into the mitochondria where they are oxidized by the β-oxidation pathway (Palmieri 2008). The mitochondrial oxidation of fatty acids is an important source of energy for humans during prolonged fasting and long-term exercise in the skeletal and cardiac muscles.
CACT is present in the mitochondria of all tissues, particularly in the heart, liver, and skeletal muscle. The CACT protein is encoded by the SLC25A20 (solute carrier family 25, member 20) gene which has been mapped to chromosome 3p21.31 and consists of nine exons (Huizing et al. 1997). CACT is the key component of the carnitine cycle which consists of four steps: uptake of carnitine across the plasma membrane by the organic cation carnitine transporter OCTN2, transfer of acyl groups from acyl CoA to carnitine through CPTI in the outer mitochondrial membrane, CACT-mediated transport of acylcarnitines across the inner mitochondrial membrane, and transfer of acyl groups from acylcarnitines to coenzyme A inside the mitochondria through CPTII. Since CACT-mediated transport is an essential step in the long-chain fatty acid β-oxidation pathway, CACT deficiency results in the unavailability of long-chain fatty acids for mitochondrial β-oxidation and ketogenesis.
CACT deficiency (OMIM 212138), first recognized in 1992 (Stanley et al. 1992), is an autosomal recessive disorder presenting in the neonatal period or early infancy with heart problems (cardiac arrhythmia, cardiomyopathy, heart block), muscle weakness, seizures, abnormal liver function, and severe episodes of hypoglycemia and hyperammonemia triggered by fasting or infections. It is one of the more uncommon defects among the fatty acid oxidation disorders; so far, only 55 cases have been reported.
The management of patients consists of fasting prevention with frequent meals, high-carbohydrate intake especially during illness or fever, supplementation of lipids as medium-chain triglycerides (MCT) and essential polyunsaturated fatty acids, and administration of carnitine (Spiekerkoetter et al. 2009).
Here, we report four cases from Spanish pediatric hospitals, two of them with severe neonatal presentation and a fatal outcome, each carrying novel mutations in homozygosity and the remaining two with a good clinical evolution. We have reviewed the clinical, biochemical, and/or molecular data of 55 previously reported cases to better understand the natural history of the disease, focusing on long-term outcome. Despite the improvement in early diagnosis and management in the last decade, CACT deficiency still has a high mortality rate (Spiekerkoetter et al. 2009; Baruteau et al. 2013).
Case Reports
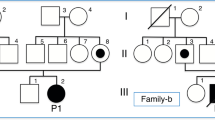
P1, a male born to unrelated parents of sub-Saharan African origin, after normal gestation and delivery (BW 3,050 g), presented at 12 h of life with symptomatic hypoglycemia and hypothermia. Hypotonia, hepatomegaly, biventricular hypertrophic myocardiopathy, hyperammonemia (312 μmol/L), cholestasis and hepatic steatosis (Table 1), increased alpha-fetoprotein (18,000 μg/L; normal value <10), and tubular dysfunction with glucosuria and proteinuria were noted. Plasma amino acids and coagulation studies were normal. Plasma acylcarnitine (ACC) profile showed marked hypocarnitinemia and high C12–C18 species, especially C16 and C18:1. GC-MS analysis of urine organic acids showed increased medium-chain dicarboxylic aciduria. CPT II activity in fibroblasts was normal. Mutation analysis of SLC25A20 gene revealed homozygosity for a novel mutation, c.59G>A (p.Gly20Asp). Both parents were carriers of the mutation. Feeding was initiated with a medium-chain fatty acid-enriched formula (Monogen©) (90% as MCT and 10% as LCT), carnitine (30 mg/kg/day), and sunflower oil (4 mL/day). Due to persistent free hypocarnitinemia (8.5 μmol/L), carnitine was increased to 100 mg/kg/day that normalized the levels. At 100 days due to acute metabolic decompensation. ECG and EcoCG showed no worsening of the myocardiopathy. Between 5 and 8 months of age, the diet was diversified (fruits, vegetables, meat, and cereals) and supplemented with docosahexaenoic acid (DHA) and soybean oil. The patient died at home at 8 months of age, coinciding with febrile process. Postmortem examination showed pneumonia, myocardiopathy, and hepatic steatosis.
P2, a female born after normal gestation and delivery (BW 3,100 g) to unrelated Spanish parents, presented with transient tachypnea of the newborn and cutaneous candidiasis in the newborn period. She was asymptomatic until 8 months of age when she was admitted to the hospital after a catarrhal process with duration of 48 h and fever. She presented with generalized tonic–clonic convulsions, hypotonia, irritability, somnolence, hepatosplenomegaly, metabolic acidosis, hypoglycemia, liver dysfunction, high CK (Table 1) and a severe neurological alteration (Glasgow index 10). The cardiologic study was normal. Ophthalmologic examination revealed salt-and-pepper retinopathy. Liver biopsy showed hepatic steatosis. The process slowly reverted after supportive measures with i.v. carnitine administration (150 mg/kg/day) and feeding with a high-carbohydrate, low-fat diet and Monogen©. Plasma ACC profile showed marked hypocarnitinemia and an increase in C14–C18:1. CPT II activity in fibroblasts was normal. The patient was compound heterozygote for two previously described mutations, c.160_163del4ins4 (p.Gly54_Thr55delinsTrpAla) on the maternal allele and c.532C>T (p.Arg178Term) on the paternal allele. She continues to be treated with a special diet with 30% fat (20% as MCT and 10% as LCT, linoleic acid 3.5%, and linolenic acid 1%), multivitamins, oral carnitine 30 mg/kg/day (persisting deficient plasma free carnitine levels (below 10 μmol/L), and avoidance of fasting. Now, at 4 years of age, she is asymptomatic with normal psychomotor and growth development (weight 25th percentile, height 90th percentile, BMI 10–25th percentile).
P3 was the fifth child born to unrelated Moroccan parents after a normal gestation and delivery (BW 3,475 g). Two sisters experienced sudden death at 24 and 48 h of life. No studies were performed for the first sister. Postmortem studies in the second sister did not reveal significant abnormalities. At 33 h of life, the proband showed hypoketotic hypoglycemia, lactic acidosis, and hyperammonemia (400 μmol/L) (Table 1). Administration of glucose, carnitine, phenylbutyrate, and carbamylglutamate decreased the ammonia levels. The patient was transferred to a neonatal intensive care unit in a referral hospital. The plasma acylcarnitine profile showed marked hypocarnitinemia and increased C12–C18 species, especially C16 and C18:1, and a slight increase in urinary excretion of suberic acid. Sequencing of CPTII and SLC25A20 genes identified homozygosis for a new SLC25A20 mutation, c.536A>G (p.Asp179Gly). Both parents were carriers of the mutation. The child was fed orally every 3 h during the day and by a nocturnal continuous nasogastric tube, with a normocaloric, low-fat diet, with medium-chain fatty acid-enriched formula (Monogen©), supplemented with carnitine 30 mg/kg/day. At 2 months of age, his weight was 6.4 kg (p25), length 65 cm (p75), and head circumference 42.5 cm (p50). Psychomotor development and cardiologic study were normal. Due to marked hypocarnitinemia (C0 7.96 μmol/L) and a deficiency of PUFAS in the plasma and erythrocytes, carnitine was increased to 80 mg/kg/day and a supplement of DHA (63 mg/day) was added. At 3 months of age, nocturnal enteral feeding was changed to two separate meals, at midnight and 4 a.m., as the parents requested. Between 5 and 9 months, the patient presented with several infections in which an emergency protocol was used. This protocol consisted of i.v. infusion of glucose at a rate of 10 mg/kg/min in order to prevent lipolysis. By that time, a failure to thrive was observed. At 9 months of age, the child was admitted to hospital with cardiac arrest coinciding with respiratory syncytial virus pneumonia, from which he recovered after resuscitation. A port-a-cath catheter was installed at that moment for easy access in case of emergency. Despite this, he died of severe gastroenteritis in a Moroccan hospital at 12 months of age.
P4 has already been described (Iacobazzi et al. 2004a). She is reported here in order to provide updated information regarding her clinical status. In brief, she is a female born after normal gestation and delivery (BW 3,300 g) to unrelated Spanish parents. Her sibling had died at 5 days of life after developing renal failure, hepatosplenomegaly, episodes of ventricular fibrillation and hyperCKemia. Necropsy revealed lipid deposits in different tissues. No further biochemical study was performed. So, this subsequent pregnancy was monitored, and glucose infusion was started soon after birth. The newborn was normal and healthy. Urine organic acid analysis showed mild dicarboxylic aciduria and normal levels of plasma C10:1n-6 and C14:1n-9 fatty acids. However, plasma free carnitine was very low (5.7 μmol/L; normal value 36 ± 7 μmol/L) with elevated long-chain acylcarnitines (15.9 μmol/L; normal value 1.1 ± 0.35 μmol/L). CACT enzyme activity in fibroblasts was reduced (6.8% of control). The patient was compound heterozygous for c.160_163del4ins4 (p. Gly54_Thr55delinsTrpAla) and c.532C>T (p.Arg178Term). Mutations were confirmed in the parents. A low-fat/high-carbohydrate diet with frequent feedings, MCT supplementation, and carnitine (100 mg/kg/day) was started. At 2 years of age, the dose was increased to 150 mg/kg/day, and plasma free carnitine was 19.34 μmol/L. She has never had an episode of metabolic decompensation. She had menarche at 11.5 years of age. Now, at 16 years of age, she is completely asymptomatic with normal psychomotor and growth development (weight and height 97th percentile) and excellent school performance.
Results and Discussion
Thirty-one articles describing clinical reports of CACT deficiency were found by searching the PubMed database (Al Aqeel et al. 2003; Al-Sannaa and Cheriyan 2010; Brivet et al. 1996; Chalmers et al. 1997; Costa et al. 1999; Costa et al. 2003; Fearing et al. 2011; Fukushima et al. 2013; Galron et al. 2004; Geven et al. 2007; Huizing et al. 1997, 1998; Iacobazzi et al. 2004a; Iacobazzi et al. 2004b; Korman et al. 2006; Lee et al. 2007; Lopriore et al. 2001; Morris et al. 1998; Niezen-Koning et al. 1995; Nuoffer et al. 2000; Ogawa et al. 2000; Ogier de Baulny et al. 1995; Olpin et al. 1997; Pande et al. 1993; Parini et al. 1999; Pierre et al. 2007; Roschinger et al. 2000; Rubio-Gozalbo et al. 2003; Rubio-Gozalbo et al. 2004; Stanley et al. 1992; Wang et al. 2011; Yang et al. 2001). Data from the literature were compiled, compared with the cases reported here, and discussed.
Clinical and Laboratory Presenting Findings
The literature group consisted of 55 patients from 53 families (Table 2). Consanguinity was reported in 58% and death of siblings, before the diagnosis of the proband, in 60% of cases.
The onset of clinical symptoms was in the first days of life in 28 out of 34 cases, 24 of them in the first week, and only in 6 out of 34 cases symptoms appeared later than 1 month of age. The most frequent initial symptoms reported were hepatomegaly (34%), arrhythmia and/or bradycardia (32%), and respiratory distress (30%). Hypoketotic hypoglycemia (68%) and hyperammonemia (54%) were the most frequent laboratory findings. The suggested mechanism leading to hyperammonemia is urea cycle dysfunction due to defective N-acetyl-glutamate synthesis secondary to an insufficient supply of mitochondrial acetyl CoA and enzymatic inhibition of CPS1 (Brivet 2004; Haberle 2013).
Our four cases were born to unrelated parents of North African or Spanish origin. Two cases (P3–P4) had previous siblings that died in the newborn period due to sudden death or multiorgan failure. Cases P1–P3 presented in the first hours of life with severe hypoglycemia. Although the onset of symptoms began later, at 8 months in P2, she had severe multisystem involvement. P4 never presented symptoms and has been treated since the newborn period due a previous affected sibling. Hepatopathy was present in cases P1–P2, and myocardiopathy only in P1.
Biochemical Findings
In the literature, patients were identified by high levels of plasma long-chain acylcarnitines (C16:0, C18:0, C18:1, and C18:2) and hypocarnitinemia, although this profile is indistinguishable from CPT II deficiency. C6–C10 dicarboxylic aciduria might also be present during decompensation episodes. Our cases (P1–P2–P3) were also identified by deficient plasma carnitine levels and increased C16 and C18:1 acylcarnitines. P4 was diagnosed after a previous affected sibling with a severe hypocarnitinemia and increased long-chain acylcarnitines.
The abnormal blood acylcarnitine profile can be detected by tandem mass spectrometry (MS–MS), allowing the early recognition of this severe disease in the neonatal period. To the best of our knowledge, until now, only two cases have been identified by positive expanded newborn screening (NBS) (Wang et al. 2011; Chien et al. 2013). No clinical data, only the genotype, are available from the first case (Wang et al. 2011). The second case was already symptomatic at the time of diagnosis through NBS (he presented with hyperammonemia and hypoglycemia after birth), and no further data about long-term outcome have been described (Chien et al. 2013).
To confirm the CACT defect, CACT activity was performed in fibroblasts from 31 out of 55 cases. Cases with residual CACT activity (<5%) seem to have a worse outcome than those with>5% activity (Table 3). Oxidation rates of [3H]myristate, [3H]palmitate, and/or [3H]oleate in cultured fibroblasts have also been determined in a few cases in the literature (Table 3). It seems that the surviving cases had a significantly higher oxidation rate of myristate, palmitate, and/or oleate than the deceased cases (p < 0.002).
In our cohort, CACT activity was only determined in P4 (residual activity 6.8% of control). In the remaining three cases, CPTII deficiency was first ruled out by enzyme determination in fibroblasts or by gene sequencing; the final diagnosis was achieved by SLC25A20 gene analysis.
Mutational Findings
A total of 39 mutations have been reported so far in the SLC25A20 gene which seem to be pan-ethnic (Wang et al. 2011; Indiveri et al. 2011); (HGMD Professional Release 2013.4 www.biobase-international.com). Functional characterization has been performed in very few of them. Mutations are summarized in Table 4, including the two novel changes described in the present study. The most frequently found were the splicing mutation c.199-10T>G in patients from East Asia (Japan, China, Vietnam), and the missense mutation c.713A>G (p.Gln238Arg) in patients of Arab origin, both associated in homozygosity to a severe clinical phenotype. Meaningful phenotype–genotype correlations were limited because of the fact that many mutations were private. Nevertheless clinical phenotype could be elicited from the homozygous and functionally hemizygous patients (Table 4).
We have identified two new homozygous missense mutations, c.59G>A (p.Gly20Asp) in P1 and c.536A>G (p.Asp179Gly) in P3, both of them with a severe clinical phenotype. Both residues of the CACT protein, glycine at position 20, and arginine at position 179 are evolutionarily conserved from frog to human. Both changes were predicted to be damaging by the algorithms Polyphen (http://genetics.bwh.harvard.edu/pph/) and SIFT (http://sift.jcvi.org/). P2 and P4, two unrelated Spanish cases, both of them with a milder clinical phenotype, presented the same genotype (p.Gly54_Thr55delinsTrpAla/p.Arg178Term). The mutation p.Gly54_Thr55delinsTrpAla has been identified so far in homozygosity in one other Spanish patient with a severe clinical phenotype (Iacobazzi et al. 2004a) and in heterozygosis with c.804delG (p.Phe269Serfs*) in one Cape Indian patient with a late onset of symptoms (Wang et al. 2011; Fearing et al. 2011). The mutation p.Arg178Term has been previously reported in patients of Turkish and North African origin (Rubio-Gozalbo et al. 2003; Costa et al. 2003; Iacobazzi et al. 2004a).
Long-Term Prognosis
In the literature, information about the survival rate was provided for 43 out of 55 cases (Table 2). The mortality rate was high (65%), with most deaths in the first year of life. In a French retrospective multicenter study of fatty acid oxidation (FAO) patients, lethality was even higher (92%) (Baruteau et al. 2013). Reported causes of death were myocardiopathy, intercurrent infectious processes, or sudden death, as occurred in P1 and P3. About 80% of the surviving reported patients were less than 12 years of age. Very few of the surviving patients presented with a milder clinical phenotype (normal physical development with no evidence of cardiac disease or myopathy) and showed homozygosity for private mutations (Morris et al. 1998; Iacobazzi et al. 2004a; Parini et al. 1999; Ijlst et al. 2001). Outcomes seem to correlate better with the absence of cardiac disease and a higher long-chain fatty acid oxidation rate in cultured fibroblasts than with residual enzyme activity. Cases P2 and P4 are at present in good clinical condition at 4 and 16 years of age; to the best of our knowledge, P4 is the oldest surviving case of CACT deficiency.
Dietary Treatment and Monitoring
The dietary treatment basically consists of frequent meals, avoiding fasting, restricting fat, and increasing carbohydrates. MCT supplementation is a critical component in the management of these patients. There is no consensus on fasting, changing from every 3 h in neonates to 8–10 h in infancy (Spiekerkoetter et al. 2009). Fat intake should be 30% or less of the total caloric value, with 20% as low C10 MCT that do not need the carnitine system to enter mitochondria and 10% as LCT (Iacobazzi et al. 2004b; Spiekerkoetter et al. 2009; Parini et al. 1999). Low C10 MCT is recommended due to the evidence that C10 fats require CACT for oxidation (Rubio-Gozalbo et al. 2004). Some cases with long-chain FAO disorders (LCHAD, VLCAD, CPT1, CPT2, and CACT) have been treated with triheptanoin, a fatty acid with seven carbon acids, with good results, especially with respect to myocardiopathy and hypoglycemia (Roe and Mochel 2006). The essential fatty acids linoleic acid (3–4%) and linolenic acid (0.5–1%) should be provided, in a ratio from 5:1 to 10:1, with walnut, canola, linseed, sunflower, wheat germ, or soy oil; this has been used with our patients (Spiekerkoetter et al. 2009). Our cases P1 and P3 required supplements of DHA to normalize plasma levels.
Emergency treatment of CACT deficiency in case of vomiting, diarrhea, fever, or other triggers of catabolism should include oral glucose solutions, glucose polymers or increased intake of carbohydrates, as well as maintaining the MCT and carnitine treatment. If the patient does not improve, 10% i.v. glucose (7–12 mg/kg/min), with insulin if required and MCT dripped enterally or in several doses, should be administered (Spiekerkoetter and Duran 2014). In the case of hyperammonemia, N-carbamylglutamate that replaces the CPS1 activator N-acetylglutamate can be used, as we did in P3 with a good response. A central line catheter for easy access in case of an emergency must be assessed in each case.
There is no consensus regarding the use of carnitine administration in CACT. Some authors do not recommend it because an accumulation of long-chain acylcarnitines may be toxic for cardiac rhythm (Rubio-Gozalbo et al. 2004). However, other authors recommend its use, even with high doses of carnitine in decompensation episodes, in order to restore the mitochondrial pool of coenzyme A (Brivet 2004). In all of our four cases, carnitine was administered (30–150 mg/kg/day) in order to maintain free carnitine in the low-normal level.
Other therapeutic possibilities for milder phenotypes with some residual CACT activity may be the administration of statins and fibrates that have been shown to enhance transcription of the human CACT gene via the peroxisome proliferator response element site, both separately and synergistically (Iacobazzi et al. 2009). This approach has already been used successfully in other FAO defects such as CPTII or VLCAD (Djouadi et al. 2003; Gobin-Limballe et al. 2007; Bonnefont et al. 2009).
Evidence-based guidelines for the treatment and monitoring of this specific disease are lacking. Only recommendations based on the experience of experts on clinical and biochemical monitoring of patients with FAO disorders have been published (Spiekerkoetter et al. 2009; Lund et al. 2010). Follow-up studies have to be performed in metabolic centers. Clinical evaluation, normalization of transaminases and creatine kinase, low-normal plasma free carnitine levels, and decreased long-chain acylcarnitines are considered ideal markers of treatment. Dietary compliance should be evaluated in each checkup. On the other hand, the liposoluble vitamins and polyunsaturated fatty acid (PUFAS) plasma levels should be monitored regularly along with annual cardiologic and ophthalmologic control. However, the best monitoring of treatment is the clinical evaluation. P2 always maintains deficient plasma free carnitine levels (<10 μmol/L), high-normal levels of C16 and C18:1 acylcarnitines, and mild dicarboxylic aciduria. P4 also had deficient plasma free carnitine levels up to 7 years of age and thereafter low-normal levels (15–20 μmol/L). Plasma long-chain acylcarnitines have always been increased in this patient.
Final Considerations
CACT deficiency is a very rare FAO disorder; no more than 60 patients have been reported worldwide in the last two decades. Although significant progress in early recognition has been made according to clinical symptoms in the neonatal period, even with expanded newborn screening, i.e., detecting C16 and C18:1 acylcarnitines in dried blood spots, the disease still has a high mortality rate in the first year of life. Prognosis seems to be better in presymptomatic individuals identified after a previous affected sibling like P4 or by NBS. It also depends on good compliance with the diet as well as urgent adequate medical intervention in metabolic decompensation episodes. Sometimes, gastrostomy or a feeding tube has to be prescribed to ensure that the energy requirements are met. In cases with frequent decompensations, a port-a-cath catheter should be installed for easy access in case of emergency.
There are few data in the literature about the long-term prognosis of milder clinical cases. The excellent outcome of P4, now 16 years old, who has never presented with metabolic decompensation and shows good compliance with the diet, supports the importance of very early therapeutic intervention.
References
Al Aqeel AI, Rashid MS, Ruiter JP, Ijlst L, Wanders RJ (2003) A novel molecular defect of the carnitine acylcarnitine translocase gene in a Saudi patient. Clin Genet 64:163–165
Al-Sannaa NA, Cheriyan GM (2010) Carnitine-acylcarnitine translocase deficiency. Clinical course of three Saudi children with a severe phenotype. Saudi Med J 31:931–934
Baruteau J, Sachs P, Broue P et al (2013) Clinical and biological features at diagnosis in mitochondrial fatty acid beta-oxidation defects: a French pediatric study from 187 patients. Complementary data. J Inherit Metab Dis 37:137–139
Bonnefont JP, Bastin J, Behin A, Djouadi F (2009) Bezafibrate for an inborn mitochondrial beta-oxidation defect. N Engl J Med 360:838–840
Brivet M (2004) Carnitine-acylcarnitine translocase deficiency. Orphanet Encyclopedia 1–5
Brivet M, Slama A, Millington DS et al (1996) Retrospective diagnosis of carnitine-acylcarnitine translocase deficiency by acylcarnitine analysis in the proband Guthrie card and enzymatic studies in the parents. J Inherit Metab Dis 19:181–184
Chalmers RA, Stanley CA, English N, Wigglesworth JS (1997) Mitochondrial carnitine-acylcarnitine translocase deficiency presenting as sudden neonatal death. J Pediatr 131:220–225
Chien YH, Lee NC, Chao MC et al (2013) Fatty Acid oxidation disorders in a chinese population in taiwan. JIMD Rep 11:165–172
Costa C, Costa JM, Nuoffer JM et al (1999) Identification of the molecular defect in a severe case of carnitine-acylcarnitine carrier deficiency. J Inherit Metab Dis 22:267–270
Costa C, Costa JM, Slama A et al (2003) Mutational spectrum and DNA-based prenatal diagnosis in carnitine-acylcarnitine translocase deficiency. Mol Genet Metab 78:68–73
Djouadi F, Bonnefont JP, Thuillier L et al (2003) Correction of fatty acid oxidation in carnitine palmitoyl transferase 2-deficient cultured skin fibroblasts by bezafibrate. Pediatr Res 54:446–451
Fearing MK, Israel EJ, Sahai I, Rapalino O, Lisovsky M (2011) Case records of the Massachusetts General Hospital. Case 12–2011. A 9-month-old boy with acute liver failure. N Engl J Med 364:1545–1556
Fukushima T, Kaneoka H, Yasuno T et al (2013) Three novel mutations in the carnitine-acylcarnitine translocase (CACT) gene in patients with CACT deficiency and in healthy individuals. J Hum Genet 58:788–793
Galron D, Birk OS, Kazanovitz A, Moses SW, Hershkovitz E (2004) Carnitine-acylcarnitine translocase deficiency: identification of a novel molecular defect in a Bedouin patient. J Inherit Metab Dis 27:267–273
Geven WB, Niezen-Koning KE, Timmer A, van Loon AJ, Wanders RJ, van Spronsen FJ (2007) Pre-eclampsia in a woman whose child suffered from lethal carnitine-acylcarnitine translocase deficiency. BJOG 114:1028–1030
Gobin-Limballe S, Djouadi F, Aubey F et al (2007) Genetic basis for correction of very-long-chain acyl-coenzyme A dehydrogenase deficiency by bezafibrate in patient fibroblasts: toward a genotype-based therapy. Am J Hum Genet 81:1133–1143
Haberle J (2013) Clinical and biochemical aspects of primary and secondary hyperammonemic disorders. Arch Biochem Biophys 536:101–108
Hsu BY, Iacobazzi V, Wang Z, Harvie H, Chalmers RA, Saudubray JM, Palmieri F, Ganguly A, Stanley CA (2001) Aberrant mRNA splicing associated with coding region mutations in children with carnitine-acylcarnitine translocase deficiency. Mol Genet Metab 74:248–255
Huizing M, Iacobazzi V, Ijlst L et al (1997) Cloning of the human carnitine-acylcarnitine carrier cDNA and identification of the molecular defect in a patient. Am J Hum Genet 61:1239–1245
Huizing M, Wendel U, Ruitenbeek W et al (1998) Carnitine-acylcarnitine carrier deficiency: identification of the molecular defect in a patient. J Inherit Metab Dis 21:262–267
Iacobazzi V, Invernizzi F, Baratta S et al (2004a) Molecular and functional analysis of SLC25A20 mutations causing carnitine-acylcarnitine translocase deficiency. Hum Mutat 24:312–320
Iacobazzi V, Pasquali M, Singh R et al (2004b) Response to therapy in carnitine/acylcarnitine translocase (CACT) deficiency due to a novel missense mutation. Am J Med Genet A 126A:150–155
Iacobazzi V, Convertini P, Infantino V, Scarcia P, Todisco S, Palmieri F (2009) Statins, fibrates and retinoic acid upregulate mitochondrial acylcarnitine carrier gene expression. Biochem Biophys Res Commun 388:643–647
Ijlst L, van Roermund CW, Iacobazzi V, Oostheim W, Ruiter JP, Williams JC, Palmieri F, Wanders RJ (2001) Functional analysis of mutant human carnitine acylcarnitine translocases in yeast. Biochem Biophys Res Commun 280:700–706
Indiveri C, Iacobazzi V, Tonazzi A et al (2011) The mitochondrial carnitine/acylcarnitine carrier: function, structure and physiopathology. Mol Aspects Med 32:223–233
Korman SH, Pitt JJ, Boneh A et al (2006) A novel SLC25A20 splicing mutation in patients of different ethnic origin with neonatally lethal carnitine-acylcarnitine translocase (CACT) deficiency. Mol Genet Metab 89:332–338
Lee RS, Lam CW, Lai CK et al (2007) Carnitine-acylcarnitine translocase deficiency in three neonates presenting with rapid deterioration and cardiac arrest. Hong Kong Med J 13:66–68
Lopriore E, Gemke RJ, Verhoeven NM et al (2001) Carnitine-acylcarnitine translocase deficiency: phenotype, residual enzyme activity and outcome. Eur J Pediatr 160:101–104
Lund AM, Skovby F, Vestergaard H, Christensen M, Christensen E (2010) Clinical and biochemical monitoring of patients with fatty acid oxidation disorders. J Inherit Metab Dis 33:495–500
Morris AA, Olpin SE, Brivet M, Turnbull DM, Jones RA, Leonard JV (1998) A patient with carnitine-acylcarnitine translocase deficiency with a mild phenotype. J Pediatr 132:514–516
Niezen-Koning KE, van Spronsen FJ, Ijlst L et al (1995) A patient with lethal cardiomyopathy and a carnitine-acylcarnitine translocase deficiency. J Inherit Metab Dis 18:230–232
Nuoffer JM, de Lonlay P, Costa C et al (2000) Familial neonatal SIDS revealing carnitine-acylcarnitine translocase deficiency. Eur J Pediatr 159:82–85
Ogawa A, Yamamoto S, Kanazawa M, Takayanagi M, Hasegawa S, Kohno Y (2000) Identification of two novel mutations of the carnitine/acylcarnitine translocase (CACT) gene in a patient with CACT deficiency. J Hum Genet 45:52–55
Ogier de Baulny H, Slama A, Touati G, Turnbull DM, Pourfarzam M, Brivet M (1995) Neonatal hyperammonemia caused by a defect of carnitine-acylcarnitine translocase. J Pediatr 127:723–728
Olpin SE, Bonham JR, Downing M et al (1997) Carnitine-acylcarnitine translocase deficiency–a mild phenotype. J Inherit Metab Dis 20:714–715
Palmieri F (2008) Diseases caused by defects of mitochondrial carriers: a review. Biochim Biophys Acta 1777:564–578
Pande SV, Brivet M, Slama A, Demaugre F, Aufrant C, Saudubray JM (1993) Carnitine-acylcarnitine translocase deficiency with severe hypoglycemia and auriculo ventricular block. Translocase assay in permeabilized fibroblasts. J Clin Invest 91:1247–1252
Parini R, Invernizzi F, Menni F et al (1999) Medium-chain triglyceride loading test in carnitine-acylcarnitine translocase deficiency: insights on treatment. J Inherit Metab Dis 22:733–739
Pierre G, Macdonald A, Gray G, Hendriksz C, Preece MA, Chakrapani A (2007) Prospective treatment in carnitine-acylcarnitine translocase deficiency. J Inherit Metab Dis 30:815
Roe CR, Mochel F (2006) Anaplerotic diet therapy in inherited metabolic disease: therapeutic potential. J Inherit Metab Dis 29:332–340
Roschinger W, Muntau AC, Duran M et al (2000) Carnitine-acylcarnitine translocase deficiency: metabolic consequences of an impaired mitochondrial carnitine cycle. Clin Chim Acta 298:55–68
Rubio-Gozalbo ME, Vos P, Forget PP et al (2003) Carnitine-acylcarnitine translocase deficiency: case report and review of the literature. Acta Paediatr 92:501–504
Rubio-Gozalbo ME, Bakker JA, Waterham HR, Wanders RJ (2004) Carnitine-acylcarnitine translocase deficiency, clinical, biochemical and genetic aspects. Mol Aspects Med 25:521–532
Spiekerkoetter U, Duran M (2014) Mitochondrial fatty acid oxidation defects. In: Blau N, Duran M, Gibson KM, Dionisi-Visi C (eds) Physician’s guide to the diagnosis, treatment, and follow-up of inherited metabolic diseases. Springer-Verlag, Berlin/Heidelberg, pp 247–264
Spiekerkoetter U, Lindner M, Santer R et al (2009) Treatment recommendations in long-chain fatty acid oxidation defects: consensus from a workshop. J Inherit Metab Dis 32:498–505
Stanley CA, Hale DE, Berry GT, Deleeuw S, Boxer J, Bonnefont JP (1992) Brief report: a deficiency of carnitine-acylcarnitine translocase in the inner mitochondrial membrane. N Engl J Med 327:19–23
Wang GL, Wang J, Douglas G et al (2011) Expanded molecular features of carnitine acyl-carnitine translocase (CACT) deficiency by comprehensive molecular analysis. Mol Genet Metab 103:349–357
Yang BZ, Mallory JM, Roe DS et al (2001) Carnitine/acylcarnitine translocase deficiency (neonatal phenotype): successful prenatal and postmortem diagnosis associated with a novel mutation in a single family. Mol Genet Metab 73:64–70
Acknowledgments
The authors would like to thank the families for giving their consent. We are grateful to Dr. Nerea Gorria from Hospital General Yagüe in Burgos for supplying the first clinical data from case 3. We gratefully acknowledge the funding by Mitolab (S2010/BMD-2402) DGUI Comunidad de Madrid.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Additional information
Communicated by: Gregory Enns
Appendices
Take-Home Message
Long-term clinical outcome in carnitine-acylcarnitine translocase deficiency seems to be better in those cases with a very early therapeutic intervention and a good dietary compliance with diet.
Compliance with Ethics Guidelines
Conflict of Interest
I Vitoria, E Martín-Hernández, L Peña-Quintana, M Bueno, P Quijada-Fraile, J Dalmau, S Molina-Marrero, B Pérez, and B Merinero declare that they have no conflict of interest.
Informed Consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Details of the Contributions of Individual Authors
IV: clinical data of case 1, conception and design, drafting, and coordination of the manuscript
EM-H: clinical data of case 3, analysis of the data, and critical reading of the manuscript
LP-Q: clinical data of case 2, analysis of the data, and critical reading of the manuscript
MB: clinical care of case 4 and critical reading of the manuscript
PQF: critical reading of the manuscript
JD: clinical data of case 1 and critical reading of the manuscript
SM-M: clinical data of case 2 and critical reading of the manuscript
BP: molecular genetic analysis and interpretation of cases 1, 2, and 3
BM: biochemical diagnosis and interpretation of cases 1, 2, and 3, conception and design, and drafting of the manuscript
Rights and permissions
Copyright information
© 2014 SSIEM and Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Vitoria, I. et al. (2014). Carnitine-Acylcarnitine Translocase Deficiency: Experience with Four Cases in Spain and Review of the Literature. In: Zschocke, J., Baumgartner, M., Morava, E., Patterson, M., Rahman, S., Peters, V. (eds) JIMD Reports, Volume 20. JIMD Reports, vol 20. Springer, Berlin, Heidelberg. https://doi.org/10.1007/8904_2014_382
Download citation
DOI: https://doi.org/10.1007/8904_2014_382
Received:
Revised:
Accepted:
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-46699-5
Online ISBN: 978-3-662-46700-8
eBook Packages: MedicineMedicine (R0)