Abstract
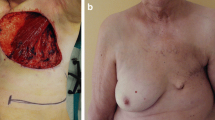
Greater clarity is needed in the surgical management of breast sarcoma. Breast sarcoma should not be managed according to breast carcinoma algorithms, and should mandate the involvement of a tertiary sarcoma center experienced in the management of such cases. This case centers around the management of a patient with primary breast angiosarcoma, initially treated in a non-sarcoma center with mastectomy and latissimus dorsi (LD) flap reconstruction, but with incomplete surgical margins. The patient’s further management was discussed through the National Scottish Sarcoma Network MDT, and surgical care transferred to the specialist sarcoma unit in Glasgow. A radical extended neo-mastectomy was performed on the right side, and reconstruction with an anterolateral thigh (ALT) flap at 1 week, once definitive pathology confirmed clear margins. Treatment goals are aimed at primary clearance of sarcoma, with angiosarcoma showing a clear survival benefit with a negative margin excision, with positive margins having a 6-month mean survival versus negative margin 42 months. Subsequent metastasis to the contralateral breast was later treated with paclitaxel followed by radical mastectomy and lateral thigh perforator (LTP) flap. The supporting rationale, current evidence, data from the West of Scotland breast sarcoma audit, and recent Scottish Sarcoma Network guidelines on breast sarcoma are discussed in the context of this case.
Similar content being viewed by others
References
Barrow BJ, Janjan NA, Gutman H, Benjamin RS, Allen P, Romsdahl MM, Ross MI, Pollock RE. Role of radiotherapy in sarcoma of the breast – a retrospective review of the M.D. Anderson experience. Radiother Oncol. 1999;52(2):173–8.
Chen Z, Zhang P, Xu Y, et al. Surgical stress and cancer progression: the twisted tango. Mol Cancer. 2019;18(1):132. https://doi.org/10.1186/s12943-019-1058-3.
Fong Y, Coit DG, Woodruff JM, Brennan MF. Lymph node metastasis from soft tissue sarcoma in adults. Analysis of data from a prospective database of 1772 sarcoma patients. Ann Surg. 1993;217(1):72–7.
Huang JY, Wang YY, Lo S, et al. Visfatin mediates malignant behaviors through adipose-derived stem cells intermediary in breast cancer. Cancers. 2019;12(1):29. https://doi.org/10.3390/cancers12010029.
Jallali N, James S, Searle A, et al. Surgical management of radiation-induced angiosarcoma after breast conservation therapy. Am J Surg. 2012;203(2):156–61. https://doi.org/10.1016/j.amjsurg.2010.12.011.
Lo S, Foster N, Campbell L, et al. A need for clarity on surgical management of breast sarcoma: Scottish sarcoma network guidelines and regional audit. J Plast Reconstr Aesthet Surg. 2021;74(6):1180–92. https://doi.org/10.1016/j.bjps.2020.10.072.
Panigrahy D, Gartung A, Yang J, et al. Preoperative stimulation of resolution and inflammation blockade eradicates micrometastases. J Clin Invest. 2019;129(7):2964–79. https://doi.org/10.1172/JCI127282.
Pencavel T, Allan CP, Thomas JM, Hayes AJ. Treatment for breast sarcoma: a large, single-Centre series. Eur J Surg Oncol. 2011;37(8):703–8. https://doi.org/10.1016/j.ejso.2011.04.006.
Seinen JM, Styring E, Verstappen V, et al. Radiation-associated angiosarcoma after breast cancer: high recurrence rate and poor survival despite surgical treatment with R0 resection. Ann Surg Oncol. 2012;19(8):2700–6. https://doi.org/10.1245/s10434-012-2310-x.
Wang YY, Hung AC, Lo S, Yuan SF. Adipocytokines visfatin and resistin in breast cancer: clinical relevance, biological mechanisms, and therapeutic potential. Cancer Lett. 2021;498:229–39. https://doi.org/10.1016/j.canlet.2020.10.045.
Zelek L, Llombart-Cussac A, Terrier P, et al. Prognostic factors in primary breast sarcomas: a series of patients with long-term follow-up. J Clin Oncol. 2003;21(13):2583–8.
Author information
Authors and Affiliations
Section Editor information
Rights and permissions
Copyright information
© 2022 Springer Nature Switzerland AG
About this entry
Cite this entry
Lo, S.J. (2022). Breast Sarcoma Case: ALT and LTP Flaps in the Management of Bilateral Asynchronous Breast Angiosarcoma. In: Clinical Scenarios in Reconstructive Microsurgery. Springer, Cham. https://doi.org/10.1007/978-3-319-94191-2_85-1
Download citation
DOI: https://doi.org/10.1007/978-3-319-94191-2_85-1
Received:
Accepted:
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-94191-2
Online ISBN: 978-3-319-94191-2
eBook Packages: Springer Reference MedicineReference Module Medicine