Abstract
Pilon fractures can have extensive bone loss including the plafond of the ankle joint. Intercalary bone transport to arthrodesis can salvage the extremity as an alternative to below-knee amputation.
The clinical photographs are the copyright property of James Hutson, MD. Their use is granted to Springer Reference for print and electronic publication without restriction. James Hutson, MD
Access provided by Autonomous University of Puebla. Download reference work entry PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Brief Clinical History
A motorcycle rider had his leg crushed between a car bumper and his bike frame. The patient was advised to consider amputation as reconstruction. The posterior tibial nerve function was intact and the anterior tibial artery was intact across the zone of injury. The patient was a nonsmoker and capable of participating in long-term reconstruction.
2 Preoperative Clinical Photos and Radiographs
(a) Anterior-posterior X-ray after debridement and placement of 13.5 cm spacer. The leg is stabilized with half pin distraction external fixator. The spacer was manufactured with 4.8 g of tobramycin, 2 g of vancomycin, and 40 g of bone cement. (b) Lateral X-ray. The foot is aligned in plantar neutral position. The antibiotic spacer is aligned by 0.0062 Steinman pin. The dome of the talus has to be drilled with a small-diameter drill bit to place the Steinman pin
3 Preoperative Problem List
-
1.
Loss of 13.5 cm of distal tibia including plafond
-
2.
Loss of soft tissue medial distal tibia requiring free flap
-
3.
Loss of posterior tibial artery with the foot surviving on anterior tibial artery and peroneal collateral arterioles
-
4.
Maintenance of plantar neutral position of the foot and alignment/flexibility of the toes during long reconstruction
4 Treatment Strategy
After multiple aggressive debridements, the reconstruction tunnel is commenced by placing the antibiotic spacer 26 mm in diameter. The extremity is maintained in good alignment with the half pin external fixator. The fixator is designed to give access to the plastic surgeons for the anastomosis of the flap. In this case an end-to-end hookup with the posterior tibial artery was accomplished. The flap was allowed to mature for 3 months before the bone reconstruction commenced. The flap is the most technical stage of the reconstruction. In sequential reconstruction, the soft tissues are resuscitated and healthy before starting the reconstruction of the tibia. The 3-month delay also creates a stable reconstruction tunnel with reactive membrane (Masquelet technique ) that will not collapse as the tibia is transported distally to arthrodesis under the flap. After transport of more than 1–2 months, the end of the transport will have developed a stable neocortex bone cap that requires docking site revision and squaring of the tibia shaft and dome of the talus to the bleeding bone.
5 Basic Principles
-
1.
The Ilizarov fixator proximal fixation block consists of a 5/8 ring connected to a full ring with 3 cm hexagonal sockets (an alternative is a 2/3 spatial open ring).
-
2.
The mid-tibia has a single-ring fixation block with three divergent 6 mm titanium hydroxyapatite pins.
-
3.
The distal fixation block is a single or double foot ring with opposed olive wires in the calcaneus and opposed olive wires in the talus. Small feet have a single ring with the talar wire on post. Large feet have two foot rings separated by 3 cm hexagonal sockets with the talar wires based on the proximal ring.
-
4.
There is enough distance between the mid-tibia ring distal half pin and the end of the tibia shaft to allow it to pass the tibia under the flap. Two-level corticotomy forces new bone creation at a mid-tibia location; this bone is of poor quality. Better long-term results are obtained using a single metaphyseal corticotomy creating massive 35 mm thick new tubular bone.
6 Images During Treatment
(See Figs. 4, 5, 6, 7, and 8).
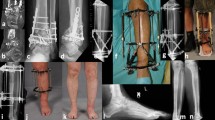
(a) AP X-ray of Ilizarov fixator following application. The use of threaded rods and square nuts to motor the mid ring is chosen to create a light and narrow frame. (b) Lateral X-ray. Observe the divergent pin spread of the AP half pins. The distance from the half pin to the end of the shaft is adequate to nose under the flap in the reconstruction tunnel. (c and d) Clinical photographs of the Ilizarov external fixator. There is a proximal and distal “dummy” ring to stiffen the frame for this long transport. This frame has a double-ring foot fixation block with the talus wires tensioned on the proximal ring. (e) Schematic drawing of the transport technique
(a and b) During the initial resuscitation, the leg was shortened. After docking, the frame is revised to a bifocal proximal lengthening and distal compression frame. This allows regaining equal length for the patient. Distraction clickers are used in the proximal frame to continue the lengthening. The fibula will require an osteotomy to free the transport for lengthening. The schematic drawing illustrates the process
7 Technical Pearls
-
1.
Docking site revision is essential to gain rapid union.
-
2.
Always mix a high concentration of the antibiotic in the spacer. Always use a 0.0062 Steinman pin to fixate the spacer between the bones of the defect. The spacer is removed by elevating the tail of the flap working between the flap muscle and underlying tissue. Split the spacer into smaller fragments to facilitate removal.
-
3.
Encourage physical therapy participation and active weight bearing during the transport.
-
4.
If the leg is shortened during the initial debridement stage, do not attempt to lengthen the leg acutely when applying the Ilizarov frame. Reconstruct the bone defect and then convert to bifocal lengthening configuration.
8 Outcome Clinical Photos and Radiographs
(See Fig. 9).
(a) AP X-ray of the reconstructed tibia. There is a massive tubular transport that will mature over many years gaining strength. Distally the tibia has a secondary Masquelet bone expansion from the effects of the spacer tunnel. (b) Lateral X-ray of the reconstructed tibia. Broken half pin from proximal ring block. (c) Lateral ankle X-ray illustrating mature arthrodesis of the tibia shaft to the dome of the talus. (d) Reconstructed extremity. Occasional pain with heavy activity. Limited hindfoot motion. Mobile forefoot. Uses well-cushioned walking shoes. The patient works full time as salesman. Married with several children
9 Avoiding and Managing Problems
-
1.
Treat pin and wire inflammation with early antibiotics. Some patient may need to be on long-term Septra DS during treatment.
-
2.
Have an open-door policy for patient care. If the patient has a problem, he/she can come to the office anytime or to the emergency room during off-hours.
-
3.
Use meticulous technique in aligning the frame during application. The tibia must be orthogonal in the frame and the distal bone segment aligned accurately.
11 See Also in Vol. 1
Case 7: Cable Bone Transport for Segmental Bone Loss Secondary to Grade IIIB Open Tibial Fracture
References and Suggested Reading
Hutson JJ (2008) Salvage of pilon fracture nonunion and infection with circular tensioned wire fixation. Foot Ankle Clin N Am 13:29–68
Hutson JJ (2013) Chapter 32, Tibial pilon fractures: tensioned wire circular fixation. In: Wiss DA (ed) Master techniques in orthopedic surgery fractures, 3rd edn. Lippincott Williams and Wilkins, New York, pp 635–672
Hutson JJ, Dayicioglu D, Oltjen JC, Pantaki Z, Armstrong M (2010) Treatment of Gustilo grade IIIB tibial fractures with application of antibiotic spacer, flap and sequential Ilizarov distraction osteogenesis. Ann Plast Surg 64:541–552
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this entry
Cite this entry
Hutson, J.J. (2015). Case 31: GIII B Open Pilon Fracture. Spacer, Flap, and 13.5 Centimeter Bone Transport to Ankle Arthrodesis (Delayed Arthrodesis Secondary to Large Bone Loss Including Ankle Plafond). In: Rozbruch, S., Hamdy, R. (eds) Limb Lengthening and Reconstruction Surgery Case Atlas. Springer, Cham. https://doi.org/10.1007/978-3-319-18026-7_180
Download citation
DOI: https://doi.org/10.1007/978-3-319-18026-7_180
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-18025-0
Online ISBN: 978-3-319-18026-7
eBook Packages: MedicineReference Module Medicine