Abstract
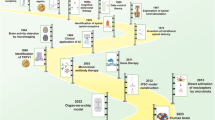
After the publication of the First Edition of this book in the series of Methods in Molecular Medicine (volume 99 in the series) in 2004, pain research continues its rapid acceleration until 2009, during which it experienced a plateau of growth that likely resulted from the economic downturn started in 2008 (Fig. 1.1). This rapid growth in pain research could be the driving force for an impressive 66% increase in new randomized, double-blind, placebo-control trials for neuropathic pain medications in the past 5 years compared with the last four decades. Unfortunately, little improvement in pain medications has been obtained [1] due to primarily our limited understanding of mechanisms mediating different pain states, especially that for chronic pain. It is highly possible that the growth in pain research will continue for decades to come due to three main reasons. First, there is an urgent need for more efficacious and safer pain medications that are necessary for better and individualized pain management. The increase in life expectancy of the general population and patients due to improvements in quality of health care and medicine is likely to increase the demand for better pain medications for improving the quality of daily life of those living with pain. It is estimated that the continuous increase in percentage of patients suffering from chronic pain (pain conditions lasting more than 6 months) arranges from 11 to 47% between 40 and 75 years of age [2], which will inevitably and continually increase the demand for better pain medications. Second, the cost of pain conditions to our society is high, estimated $55 billion per year in loss of productivity from full-time workers alone [3], so better pain management can significantly help economic growth and stability. Third, the swift advancement in technologies and our better understanding of sensory circuitries and pain pathways serves as a driving force for timely drug discovery research and development at an unprecedented pace to meet the demand for better pain medications.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Finnerup, N. B., Sindrup, S. H., and Jensen, T. S. (2010) The evidence for pharmacological treatment of neuropathic pain. Pain 150, 573–81.
Kopf, A. (2010) Pain in Old Age and Dementia, in Guide to Pain Management in Low-Resource Settings (Kopf, A., and Patel, N. B., Eds.), pp 269–75, International Association for the Study of Pain, Seattle.
Katz, N. (2002) The impact of pain management on quality of life. J Pain Symptom Manage 24, S38–47.
Neely, G. G., Hess, A., Costigan, M., Keene, A. C., Goulas, S., Langeslag, M., Griffin, R. S., Belfer, I., Dai, F., Smith, S. B., Diatchenko, L., Gupta, V., Xia, C. P., Amann, S., Kreitz, S., Heindl-Erdmann, C., Wolz, S., Ly, C. V., Arora, S., Sarangi, R., Dan, D., Novatchkova, M., Rosenzweig, M., Gibson, D. G., Truong, D., Schramek, D., Zoranovic, T., Cronin, S. J., Angjeli, B., Brune, K., Dietzl, G., Maixner, W., Meixner, A., Thomas, W., Pospisilik, J. A., Alenius, M., Kress, M., Subramaniam, S., Garrity, P. A., Bellen, H. J., Woolf, C. J., and Penninger, J. M. (2010) A genome-wide Drosophila screen for heat nociception identifies alpha2delta3 as an evolutionarily conserved pain gene. Cell 143, 628–38.
Kim, H., Ramsay, E., Lee, H., Wahl, S., and Dionne, R. A. (2009) Genome-wide association study of acute post-surgical pain in humans. Pharmacogenomics 10, 171–9.
Fukuda, K., Hayashida, M., Ide, S., Saita, N., Kokita, Y., Kasai, S., Nishizawa, D., Ogai, Y., Hasegawa, J., Nagashima, M., Tagami, M., Komatsu, H., Sora, I., Koga, H., Kaneko, Y., and Ikeda, K. (2009) Association between OPRM1 gene polymorphisms and fentanyl sensitivity in patients undergoing painful cosmetic surgery. Pain 147, 194–201.
Lotsch, J., Klepstad, P., Doehring, A., and Dale, O. (2010) A GTP cyclohydrolase 1 genetic variant delays cancer pain. Pain 148, 103–6.
Costigan, M., Belfer, I., Griffin, R. S., Dai, F., Barrett, L. B., Coppola, G., Wu, T., Kiselycznyk, C., Poddar, M., Lu, Y., Diatchenko, L., Smith, S., Cobos, E. J., Zaykin, D., Allchorne, A., Shen, P. H., Nikolajsen, L., Karppinen, J., Mannikko, M., Kelempisioti, A., Goldman, D., Maixner, W., Geschwind, D. H., Max, M. B., Seltzer, Z., and Woolf, C. J. (2010) Multiple chronic pain states are associated with a common amino acid-changing allele in KCNS1. Brain 133, 2519–27.
Nissenbaum, J., Devor, M., Seltzer, Z., Gebauer, M., Michaelis, M., Tal, M., Dorfman, R., Abitbul-Yarkoni, M., Lu, Y., Elahipanah, T., delCanho, S., Minert, A., Fried, K., Persson, A. K., Shpigler, H., Shabo, E., Yakir, B., Pisante, A., and Darvasi, A. (2010) Susceptibility to chronic pain following nerve injury is genetically affected by CACNG2. Genome Res 20, 1180–90.
Treister, R., Pud, D., Ebstein, R. P., Laiba, E., Gershon, E., Haddad, M., and Eisenberg, E. (2009) Associations between polymorphisms in dopamine neurotransmitter pathway genes and pain response in healthy humans. Pain 147, 187–93.
Estevez, M., and Gardner, K. L. (2004) Update on the genetics of migraine. Hum Genet 114, 225–35.
Luo, Z. D., and Figueroa, K. W. (2008) Multilevel genomic approach in pain research: basic science and clinical implications. Rev. Analg. 10, 45–58.
Wang, H., Sun, H., Della Penna, K., Benz, R. J., Xu, J., Gerhold, D. L., Holder, D. J., and Koblan, K. S. (2002) Chronic neuropathic pain is accompanied by global changes in gene expression and shares pathobiology with neurodegenerative diseases. Neuroscience 114, 529–46.
Kim, D. S., Figueroa, K. W., Li, K. W., Boroujerdi, A., Yolo, T., and David Luo, Z. (2009) Profiling of dynamically changed gene expression in dorsal root ganglia post peripheral nerve injury and a critical role of injury-induced glial fibrillary acidic protein in maintenance of pain behaviors (corrected]. Pain 143, 114–22.
Costigan, M., Befort, K., Karchewski, L., Griffin, R. S., D’Urso, D., Allchorne, A., Sitarski, J., Mannion, J. W., Pratt, R. E., and Woolf, C. J. (2002) Replicate high-density rat genome oligonucleotide microarrays reveal hundreds of regulated genes in the dorsal root ganglion after peripheral nerve injury. BMC Neurosci 3, 16. Print 2002 Oct 25.
Bauer, C. S., Nieto-Rostro, M., Rahman, W., Tran-Van-Minh, A., Ferron, L., Douglas, L., Kadurin, I., Sri Ranjan, Y., Fernandez-Alacid, L., Millar, N. S., Dickenson, A. H., Lujan, R., and Dolphin, A. C. (2009) The increased trafficking of the calcium channel subunit alpha2delta-1 to presynaptic terminals in neuropathic pain is inhibited by the alpha2delta ligand pregabalin. J Neurosci 29, 4076–88.
Boroujerdi, A., Kim, H. K., Lyu, Y. S., Kim, D. S., Figueroa, K. W., Chung, J. M., and Luo, Z. D. (2008) Injury discharges regulate calcium channel alpha-2-delta-1 subunit upregulation in the dorsal horn that contributes to initiation of neuropathic pain. Pain 139, 358–66.
Boroujerdi, A., Zeng, J., Sharp, K., Kim, D., Steward, O., and Luo, Z. D. (2011) Calcium channel alpha-2-delta-1 protein upregulation in dorsal spinal cord mediates spinal cord injury induced neuropathic pain states. Pain 152 , 649–55.
Li, C. Y., Song, Y. H., Higuera, E. S., and Luo, Z. D. (2004) Spinal dorsal horn calcium channel alpha2delta-1 subunit upregulation contributes to peripheral nerve injury-induced tactile allodynia. J Neurosci 24, 8494–9.
Luo, Z. D., Calcutt, N. A., Higuera, E. S., Valder, C. R., Song, Y. H., Svensson, C. I., and Myers, R. R. (2002) Injury type-specific calcium channel alpha 2 delta-1 subunit up-regulation in rat neuropathic pain models correlates with antiallodynic effects of gabapentin. J Pharmacol Exp Ther 303, 1199–205.
Luo, Z. D., Chaplan, S. R., Higuera, E. S., Sorkin, L. S., Stauderman, K. A., Williams, M. E., and Yaksh, T. L. (2001) Upregulation of dorsal root ganglion (alpha)2(delta) calcium channel subunit and its correlation with allodynia in spinal nerve-injured rats. J. Neurosci. 21, 1868–75.
Newton, R. A., Bingham, S., Case, P. C., Sanger, G. J., and Lawson, S. N. (2001) Dorsal root ganglion neurons show increased expression of the calcium channel alpha2delta-1 subunit following partial sciatic nerve injury. Brain Res Mol Brain Res 95, 1–8.
Valder, C. R., Liu, J. J., Song, Y. H., and Luo, Z. D. (2003) Coupling gene chip analyses and rat genetic variances in identifying potential target genes that may contribute to neuropathic allodynia development. J Neurochem 87, 560–73.
Wang, X. M., Wu, T. X., Hamza, M., Ramsay, E. S., Wahl, S. M., and Dionne, R. A. (2007) Rofecoxib modulates multiple gene expression pathways in a clinical model of acute inflammatory pain. Pain 128, 136–47.
Wang, X. M., Hamza, M., Gordon, S. M., Wahl, S. M., and Dionne, R. A. (2008) COX inhibitors downregulate PDE4D expression in a clinical model of inflammatory pain. Clin Pharmacol Ther 84, 39–42.
Wang, X. M., Hamza, M., Wu, T. X., and Dionne, R. A. (2009) Upregulation of IL-6, IL-8 and CCL2 gene expression after acute inflammation: Correlation to clinical pain. Pain 142, 275–83.
Kim, H., Clark, D., and Dionne, R. A. (2009) Genetic contributions to clinical pain and analgesia: avoiding pitfalls in genetic research. J Pain 10, 663–93.
Espina, V., Woodhouse, E. C., Wulfkuhle, J., Asmussen, H. D., Petricoin, E. F., 3rd, and Liotta, L. A. (2004) Protein microarray detection strategies: focus on direct detection technologies. J Immunol Methods 290, 121–33.
Sandoz, G., Thummler, S., Duprat, F., Feliciangeli, S., Vinh, J., Escoubas, P., Guy, N., Lazdunski, M., and Lesage, F. (2006) AKAP150, a switch to convert mechano-, pH- and arachidonic acid-sensitive TREK K(+) channels into open leak channels. Embo J 25, 5864–72.
Sung, H. J., Kim, Y. S., Kim, I. S., Jang, S. W., Kim, Y. R., Na, D. S., Han, K. H., Hwang, B. G., Park, D. S., and Ko, J. (2004) Proteomic analysis of differential protein expression in neuropathic pain and electroacupuncture treatment models. Proteomics 4, 2805–13.
Kunz, S., Tegeder, I., Coste, O., Marian, C., Pfenninger, A., Corvey, C., Karas, M., Geisslinger, G., and Niederberger, E. (2005) Comparative proteomic analysis of the rat spinal cord in inflammatory and neuropathic pain models. Neurosci Lett 381, 289–93.
Park, S., and Lee, J. (2009) Proteomic analysis to identify early molecular targets of pregabalin in C6 glial cells. Cell Biol Int 34, 27–33.
Riedl, M. S., Braun, P. D., Kitto, K. F., Roiko, S. A., Anderson, L. B., Honda, C. N., Fairbanks, C. A., and Vulchanova, L. (2009) Proteomic analysis uncovers novel actions of the neurosecretory protein VGF in nociceptive processing. J Neurosci 29, 13377–88.
Singh, O. V., Yaster, M., Xu, J. T., Guan, Y., Guan, X., Dharmarajan, A. M., Raja, S. N., Zeitlin, P. L., and Tao, Y. X. (2009) Proteome of synaptosome-associated proteins in spinal cord dorsal horn after peripheral nerve injury. Proteomics 9, 1241–53.
Wu, L. J., Ko, S. W., and Zhuo, M. (2007) Kainate receptors and pain: from dorsal root ganglion to the anterior cingulate cortex. Curr Pharm Des 13, 1597–605.
Xu, H., Wu, L. J., Wang, H., Zhang, X., Vadakkan, K. I., Kim, S. S., Steenland, H. W., and Zhuo, M. (2008) Presynaptic and postsynaptic amplifications of neuropathic pain in the anterior cingulate cortex. J Neurosci 28, 7445–53.
Li, X. Y., Ko, H. G., Chen, T., Descalzi, G., Koga, K., Wang, H., Kim, S. S., Shang, Y., Kwak, C., Park, S. W., Shim, J., Lee, K., Collingridge, G. L., Kaang, B. K., and Zhuo, M. (2010) Alleviating neuropathic pain hypersensitivity by inhibiting PKMzeta in the anterior cingulate cortex. Science 330, 1400–4.
Qu, X. X., Cai, J., Li, M. J., Chi, Y. N., Liao, F. F., Liu, F. Y., Wan, Y., Han, J. S., and Xing, G. G. (2009) Role of the spinal cord NR2B-containing NMDA receptors in the development of neuropathic pain. Exp Neurol 215, 298–307.
Sunesen, M., and Jacobsen, R. B. (2011) Study of TRP Channels by Automated Patch Clamp Systems. Adv Exp Med Biol 704, 107–23.
Perret, D. M., Kim, D.-S., Li, K.-W., Sinavsky, K., Newcomb, R. L., Miller, J. M., and Luo, Z. D. (2011) Application of Pulsed Radiofrequency Currents to Rat Dorsal Root Ganglia Modulates Nerve Injury-Induced Tactile Allodynia. Anesthesia & Analgesia 113, 610–6.
Braz, J. M., Nassar, M. A., Wood, J. N., and Basbaum, A. I. (2005) Parallel “pain” pathways arise from subpopulations of primary afferent nociceptor. Neuron 47, 787–93.
Braz, J. M., and Basbaum, A. I. (2009) Triggering genetically-expressed transneuronal tracers by peripheral axotomy reveals convergent and segregated sensory neuron-spinal cord connectivity. Neuroscience 163, 1220–32.
Neumann, S., Braz, J. M., Skinner, K., Llewellyn-Smith, I. J., and Basbaum, A. I. (2008) Innocuous, not noxious, input activates PKCgamma interneurons of the spinal dorsal horn via myelinated afferent fibers. J Neurosci 28, 7936–44.
Braz, J. M., and Basbaum, A. I. (2008) Genetically expressed transneuronal tracer reveals direct and indirect serotonergic descending control circuits. J Comp Neurol 507, 1990–2003.
Li, C. Y., Zhang, X. L., Matthews, E. A., Li, K. W., Kurwa, A., Boroujerdi, A., Gross, J., Gold, M. S., Dickenson, A. H., Feng, G., and Luo, Z. D. (2006) Calcium channel alpha2delta1 subunit mediates spinal hyperexcitability in pain modulation. Pain 125, 20–34.
Schorscher-Petcu, A., Sotocinal, S., Ciura, S., Dupre, A., Ritchie, J., Sorge, R. E., Crawley, J. N., Hu, S. B., Nishimori, K., Young, L. J., Tribollet, E., Quirion, R., and Mogil, J. S. (2010) Oxytocin-induced analgesia and scratching are mediated by the vasopressin-1A receptor in the mouse. J Neurosci 30, 8274–84.
Sowa, N. A., Taylor-Blake, B., and Zylka, M. J. (2010) Ecto-5′-nucleotidase (CD73) inhibits nociception by hydrolyzing AMP to adenosine in nociceptive circuits. J Neurosci 30, 2235–44.
Diaz, J. L., Zamanillo, D., Corbera, J., Baeyens, J. M., Maldonado, R., Pericas, M. A., Vela, J. M., and Torrens, A. (2009) Selective sigma-1 (sigma1) receptor antagonists: emerging target for the treatment of neuropathic pain. Cent Nerv Syst Agents Med Chem 9, 172–83.
Jones, R. C., 3rd, Xu, L., and Gebhart, G. F. (2005) The mechanosensitivity of mouse colon afferent fibers and their sensitization by inflammatory mediators require transient receptor potential vanilloid 1 and acid-sensing ion channel 3. J Neurosci 25, 10981–9.
Yuan, F. L., Chen, F. H., Lu, W. G., and Li, X. (2009) Acid-sensing ion channels 3: a potential therapeutic target for pain treatment in arthritis. Mol Biol Rep 37, 3233–8.
Vardanyan, A., Wang, R., Vanderah, T. W., Ossipov, M. H., Lai, J., Porreca, F., and King, T. (2009) TRPV1 receptor in expression of opioid-induced hyperalgesia. J Pain 10, 243–52.
Wang, Z. Y., Wang, P., Merriam, F. V., and Bjorling, D. E. (2008) Lack of TRPV1 inhibits cystitis-induced increased mechanical sensitivity in mice. Pain 139, 158–67.
Kim, H. Y., Kim, K., Li, H. Y., Chung, G., Park, C. K., Kim, J. S., Jung, S. J., Lee, M. K., Ahn, D. K., Hwang, S. J., Kang, Y., Binshtok, A. M., Bean, B. P., Woolf, C. J., and Oh, S. B. (2010) Selectively targeting pain in the trigeminal system. Pain 150, 29–40.
Fioravanti, B., De Felice, M., Stucky, C. L., Medler, K. A., Luo, M. C., Gardell, L. R., Ibrahim, M., Malan, T. P., Jr., Yamamura, H. I., Ossipov, M. H., King, T., Lai, J., Porreca, F., and Vanderah, T. W. (2008) Constitutive activity at the cannabinoid CB1 receptor is required for behavioral response to noxious chemical stimulation of TRPV1: antinociceptive actions of CB1 inverse agonists. J Neurosci 28, 11593–602.
Acknowledgments
Supported in part by grants from the National Institutes of Health (DE019298, NS064341) (Z.D. Luo).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2012 Springer Science+Business Media, LLC
About this protocol
Cite this protocol
Luo, Z.D. (2012). Advancements in Pain Research. In: Luo, Z. (eds) Pain Research. Methods in Molecular Biology, vol 851. Humana Press. https://doi.org/10.1007/978-1-61779-561-9_1
Download citation
DOI: https://doi.org/10.1007/978-1-61779-561-9_1
Published:
Publisher Name: Humana Press
Print ISBN: 978-1-61779-560-2
Online ISBN: 978-1-61779-561-9
eBook Packages: Springer Protocols