Abstract
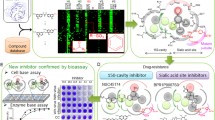
Depending on the strain, influenza A virus causes animal, zoonotic, pandemic, or seasonal influenza with varying degrees of severity. Two surface glycoprotein spikes, hemagglutinin (HA) and neuraminidase (NA), are the most important influenza A virus antigens. NA plays an important role in the propagation of influenza virus by removing terminal sialic acid from sialyl decoy receptors and thereby facilitating the release of viruses from traps such as in mucus and on infected cells. Some NA inhibitors have become widely used drugs for treatment of influenza. However, attempts to develop effective and safe NA inhibitors that can be used for treatment of anti-NA drugs-resistant influenza viruses have continued. In this chapter, we describe the following updates on influenza A NA inhibitor development: (i) N-acetylneuraminic acid (Neu5Ac)-based derivatives, (ii) covalent NA inhibitors, (iii) sulfo-sialic acid analogs, (iv) N-acetyl-6-sulfo-β-d-glucosaminide-based inhibitors, (v) inhibitors targeting the 150-loop of group 1 NAs, (vi) conjugation inhibitors, (vii) acylhydrazone derivatives, (viii) monoclonal antibodies, (ix) PVP-I, and (x) natural products. Finally, we provide future perspectives on the next-generation anti-NA drugs.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
ICTV Website (2021) Virus taxonomy: 2020 release. https://talk.ictvonline.org/ictv-reports/ictv_9th_report/negative-sense-rna-viruses-2011/w/negrna_viruses/209/orthomyxoviridae
Tong S, Zhu X, Li Y et al (2013) New world bats harbor diverse influenza A viruses. PLoS Pathog 9:e1003657
Sriwilaijaroen N, Suzuki Y (2020) Host receptors of influenza viruses and coronaviruses-molecular mechanisms of recognition. Vaccines (Basel) 8:587
WHO Website (2021) Influenza – estimating burden of disease. https://www.euro.who.int/en/health-topics/communicable-diseases/influenza/seasonal-influenza/burden-of-influenza
Wang K, Lei Z, Zhao L et al (2020) Design, synthesis and biological evaluation of oseltamivir derivatives containing pyridyl group as potent inhibitors of neuraminidase for influenza A. Eur J Med Chem 185:111841
de Vries E, Du W, Guo H et al (2020) Influenza A virus hemagglutinin-neuraminidase-receptor balance: preserving virus motility. Trends Microbiol 28:57–67
Kiefel MJ, von Itzstein M (1999) Influenza virus sialidase: a target for drug discovery. Prog Med Chem 36:1–28
von Itzstein M, Wu WY, Kok GB et al (1993) Rational design of potent sialidase-based inhibitors of influenza virus replication. Nature 363:418–423
Kim CU, Lew W, Williams MA et al (1997) Influenza neuraminidase inhibitors possessing a novel hydrophobic interaction in the enzyme active site: design, synthesis, and structural analysis of carbocyclic sialic acid analogues with potent anti-influenza activity. J Am Chem Soc 119:681–690
Babu YS, Chand P, Bantia S et al (2000) BCX-1812 (RWJ-270201): discovery of a novel, highly potent, orally active, and selective influenza neuraminidase inhibitor through structure-based drug design. J Med Chem 43:3482–3486
Yamashita M, Tomozawa T, Kakuta M et al (2009) CS-8958, a prodrug of the new neuraminidase inhibitor R-125489, shows long-acting anti-influenza virus activity. Antimicrob Agents Chemother 53:186–192
Shidmoossavee FS, Watson JN, Bennet AJ (2013) Chemical insight into the emergence of influenza virus strains that are resistant to Relenza. J Am Chem Soc 135:13254–13257
Moscona A (2005) Oseltamivir resistance-disabling our influenza defenses. N Engl J Med 353:2633–2636
Hurt AC, Holien JK, Parker M et al (2009) Zanamivir-resistant influenza viruses with a novel neuraminidase mutation. J Virol 83:10366–10373
Nitsch-Osuch A, Brydak LB (2014) Influenza viruses resistant to neuraminidase inhibitors. Acta Biochim Pol 61:505–508
Memoli MJ, Hrabal RJ, Hassantoufighi A et al (2010) Rapid selection of oseltamivir- and peramivir-resistant pandemic H1N1 virus during therapy in 2 immunocompromised hosts. Clin Infect Dis 50:1252–1255
L’Huillier AG, Abed Y, Petty TJ et al (2015) E119D neuraminidase mutation conferring pan-resistance to neuraminidase inhibitors in an A(H1N1)pdm09 isolate from a stem-cell transplant recipient. J Infect Dis 212:1726–1734
Matrosovich MN, Klenk HD, Kawaoka Y (2006) Receptor specificity, host-range, and pathogenicity of influenza viruses. In: Kawaoka Y (ed) Influenza virology: current topics. Caister Academic Press, Wymondham, pp 95–137
Sriwilaijaroen N, Suzuki Y (2020) Sialoglycovirology of lectins: sialyl glycan binding of enveloped and non-enveloped viruses. Methods Mol Biol 2132:483–545
McAuley JL, Corcilius L, Tan HX et al (2017) The cell surface mucin MUC1 limits the severity of influenza A virus infection. Mucosal Immunol 10:1581–1593
Matrosovich MN, Matrosovich TY, Gray T et al (2004) Neuraminidase is important for the initiation of influenza virus infection in human airway epithelium. J Virol 78:12665–12667
Ohuchi M, Asaoka N, Sakai T et al (2006) Roles of neuraminidase in the initial stage of influenza virus infection. Microbes Infect 8:1287–1293
McAuley JL, Gilbertson BP, Trifkovic S et al (2019) Influenza virus neuraminidase structure and functions. Front Microbiol 10:39
Yagi H, Watanabe S, Suzuki T et al (2012) Comparative analyses of N-glycosylation profiles of influenza A viruses grown in different host cells. Open Glycosci 5:2–12
Palese P, Compans RW (1976) Inhibition of influenza virus replication in tissue culture by 2-deoxy-2,3-dehydro-N-trifluoroacetylneuraminic acid (FANA): mechanism of action. J Gen Virol 33:159–163
Xu R, Zhu X, McBride R et al (2012) Functional balance of the hemagglutinin and neuraminidase activities accompanies the emergence of the 2009 H1N1 influenza pandemic. J Virol 86:9221–9232
Du W, Wolfert MA, Peeters B et al (2020) Mutation of the second sialic acid-binding site of influenza A virus neuraminidase drives compensatory mutations in hemagglutinin. PLoS Pathog 16:e1008816
da Silva DV, Nordholm J, Madjo U et al (2013) Assembly of subtype 1 influenza neuraminidase is driven by both the transmembrane and head domains. J Biol Chem 288:644–653
Wang M, Qi J, Liu Y et al (2011) Influenza A virus N5 neuraminidase has an extended 150-cavity. J Virol 85:8431–8435
Sun X, Li Q, Wu Y et al (2014) Structure of influenza virus N7: the last piece of the neuraminidase “jigsaw” puzzle. J Virol 88:9197–9207
Du W, Dai M, Li Z et al (2018) Substrate binding by the second sialic acid-binding site of influenza A virus N1 neuraminidase contributes to enzymatic activity. J Virol 92:e01243–18
Durrant JD, Kochanek SE, Casalino L et al (2020) Mesoscale all-atom influenza virus simulations suggest new substrate binding mechanism. ACS Cent Sci 6:189–196
Taylor NR, von Itzstein M (1994) Molecular modeling studies on ligand binding to sialidase from influenza virus and the mechanism of catalysis. J Med Chem 37:616–624
Vavricka CJ, Liu Y, Kiyota H et al (2013) Influenza neuraminidase operates via a nucleophilic mechanism and can be targeted by covalent inhibitors. Nat Commun 4:1491
Russell RJ, Haire LF, Stevens DJ et al (2006) The structure of H5N1 avian influenza neuraminidase suggests new opportunities for drug design. Nature 443:45–49
Amaro RE, Swift RV, Votapka L et al (2011) Mechanism of 150-cavity formation in influenza neuraminidase. Nat Commun 2:388
Edmond JD, Johnston RG, Kidd D et al (1966) The inhibition of neuraminidase and antiviral action. Br J Pharmacol Chemother 27:415–426
Meindl P, Tuppy H (1969) 2-Deoxy-2,3-dehydrosialic acids. I. Synthesis and properties of 2-deoxy-2,3-dehydro-N-acylneuraminic acids and their methyl esters. Monatsh Chem 100:1295–1306
Meindl P, Bodo G, Palese P et al (1974) Inhibition of neuraminidase activity by derivatives of 2-deoxy-2,3-dehydro-N-acetylneuraminic acid. Virology 58:457–463
Palese P, Schulman JL, Bodo G et al (1974) Inhibition of influenza and parainfluenza virus replication in tissue culture by 2-deoxy-2,3-dehydro-N-trifluoroacetylneuraminic acid (FANA). Virology 59:490–498
Colman PM, Varghese JN, Laver WG (1983) Structure of the catalytic and antigenic sites in influenza virus neuraminidase. Nature 303:41–44
Varghese JN, Smith PW, Sollis SL et al (1998) Drug design against a shifting target: a structural basis for resistance to inhibitors in a variant of influenza virus neuraminidase. Structure 6:735–746
Varghese JN, McKimm-Breschkin JL, Caldwell JB et al (1992) The structure of the complex between influenza virus neuraminidase and sialic acid, the viral receptor. Proteins 14:327–332
Sriwilaijaroen N, Magesh S, Imamura A et al (2016) A novel potent and highly specific inhibitor against influenza viral N1-N9 neuraminidases: insight into neuraminidase-inhibitor interactions. J Med Chem 59:4563–4577
PHE Website (2019) PHE guidance on use of antiviral agents for the treatment and prophylaxis of seasonal influenza. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/833572/PHE_guidance_antivirals_influenza_201920.pdf
von Itzstein M (2007) The war against influenza: discovery and development of sialidase inhibitors. Nat Rev Drug Discov 6:967–974
Cass LM, Efthymiopoulos C, Bye A (1999) Pharmacokinetics of zanamivir after intravenous, oral, inhaled or intranasal administration to healthy volunteers. Clin Pharmacokinet 36(Suppl 1):1–11
Lew W, Chen X, Kim CU (2000) Discovery and development of GS 4104 (oseltamivir): an orally active influenza neuraminidase inhibitor. Curr Med Chem 7:663–672
Wu Y, Qin G, Gao F et al (2013) Induced opening of influenza virus neuraminidase N2 150-loop suggests an important role in inhibitor binding. Sci Rep 3:1551
Chand P, Kotian PL, Dehghani A et al (2001) Systematic structure-based design and stereoselective synthesis of novel multisubstituted cyclopentane derivatives with potent antiinfluenza activity. J Med Chem 44:4379–4392
Barroso L, Treanor J, Gubareva L et al (2005) Efficacy and tolerability of the oral neuraminidase inhibitor peramivir in experimental human influenza: randomized, controlled trials for prophylaxis and treatment. Antivir Ther 10:901–910
Alame MM, Massaad E, Zaraket H (2016) Peramivir: a novel intravenous neuraminidase inhibitor for treatment of acute influenza infections. Front Microbiol 7:450
PDR Website (2021) Peramivir – drug summary. https://www.pdr.net/drug-summary/Rapivab-peramivir-3660
Ison MG (2013) Clinical use of approved influenza antivirals: therapy and prophylaxis. Influenza Other Respir Viruses 7:7–13
Watanabe A, Chang SC, Kim MJ et al (2010) Long-acting neuraminidase inhibitor laninamivir octanoate versus oseltamivir for treatment of influenza: a double-blind, randomized, noninferiority clinical trial. Clin Infect Dis 51:1167–1175
Koyama K, Nakai D, Takahashi M et al (2013) Pharmacokinetic mechanism involved in the prolonged high retention of laninamivir in mouse respiratory tissues after intranasal administration of its prodrug laninamivir octanoate. Drug Metab Dispos 41:180–187
Magesh S, Sriwilaijaroen N, Moriya S et al (2011) Evaluation of a set of C9 N-acyl Neu5Ac2en mimetics as viral sialidase selective inhibitors. Int J Med Chem 2011:539245
Wu Y, Gao F, Qi J et al (2016) Resistance to mutant group 2 influenza virus neuraminidases of an oseltamivir-zanamivir hybrid inhibitor. J Virol 90:10693–10700
Kerry PS, Mohan S, Russell RJ et al (2013) Structural basis for a class of nanomolar influenza A neuraminidase inhibitors. Sci Rep 3:2871
Hata K, Koseki K, Yamaguchi K et al (2008) Limited inhibitory effects of oseltamivir and zanamivir on human sialidases. Antimicrob Agents Chemother 52:3484–3491
Li Z, Meng Y, Xu S et al (2017) Discovery of acylguanidine oseltamivir carboxylate derivatives as potent neuraminidase inhibitors. Bioorg Med Chem 25:2772–2781
Watts AG, Damager I, Amaya ML et al (2003) Trypanosoma cruzi trans-sialidase operates through a covalent sialyl-enzyme intermediate: tyrosine is the catalytic nucleophile. J Am Chem Soc 125:7532–7533
Newstead SL, Potter JA, Wilson JC et al (2008) The structure of Clostridium perfringens NanI sialidase and its catalytic intermediates. J Biol Chem 283:9080–9088
Kim JH, Resende R, Wennekes T et al (2013) Mechanism-based covalent neuraminidase inhibitors with broad-spectrum influenza antiviral activity. Science 340:71–75
Dirr L, El-Deeb IM, Guillon P et al (2015) The catalytic mechanism of human parainfluenza virus type 3 haemagglutinin-neuraminidase revealed. Angew Chem Int Ed Engl 54:2936–2940
Vavricka CJ, Muto C, Hasunuma T et al (2017) Synthesis of sulfo-sialic acid analogues: potent neuraminidase inhibitors in regards to anomeric functionality. Sci Rep 7:8239
Hadhazi A, Pascolutti M, Bailly B et al (2017) A sialosyl sulfonate as a potent inhibitor of influenza virus replication. Org Biomol Chem 15:5249–5253
Hadhazi A, Li L, Bailly B et al (2018) A sulfonozanamivir analogue has potent anti-influenza virus activity. ChemMedChem 13:785–789
Sasaki K, Nishida Y, Kambara M et al (2004) Design of N-acetyl-6-sulfo-b-D-glucosaminide-based inhibitors of influenza virus sialidase. Bioorg Med Chem 12:1367–1375
Rudrawar S, Dyason JC, Rameix-Welti MA et al (2010) Novel sialic acid derivatives lock open the 150-loop of an influenza A virus group-1 sialidase. Nat Commun 1:113
Rudrawar S, Kerry PS, Rameix-Welti MA et al (2012) Synthesis and evaluation of novel 3-C-alkylated-Neu5Ac2en derivatives as probes of influenza virus sialidase 150-loop flexibility. Org Biomol Chem 10:8628–8639
Hsu KC, Hung HC, HuangFu WC et al (2017) Identification of neuraminidase inhibitors against dual H274Y/I222R mutant strains. Sci Rep 7:12336
Jia R, Zhang J, Ai W et al (2019) Design, synthesis and biological evaluation of “Multi-Site”-binding influenza virus neuraminidase inhibitors. Eur J Med Chem 178:64–80
Jia R, Zhang J, Bertagnin C et al (2021) Discovery of highly potent and selective influenza virus neuraminidase inhibitors targeting 150-cavity. Eur J Med Chem 212:113097
Ai W, Zhang J, Zalloum WA et al (2020) Discovery of novel “dual-site” binding oseltamivir derivatives as potent influenza virus neuraminidase inhibitors. Eur J Med Chem 191:112147
Wang HX, Zeng MS, Ye Y et al (2021) Antiviral activity of puerarin as potent inhibitor of influenza virus neuraminidase. Phytother Res 35:324–336
Fu L, Bi Y, Wu Y et al (2016) Structure-based tetravalent zanamivir with potent inhibitory activity against drug-resistant influenza viruses. J Med Chem 59:6303–6312
Liu X, Zhang B, Wang Y et al (2020) A universal dual mechanism immunotherapy for the treatment of influenza virus infections. Nat Commun 11:5597
Sriwilaijaroen N, Suzuki Y (2014) Molecular basis of a pandemic of avian-type influenza virus. Methods Mol Biol 1200:447–480
Yu Y, Qin HJ, Shi XX et al (2020) Thiosialoside-decorated polymers use a two-step mechanism to inhibit both early and late stages of influenza virus infection. Eur J Med Chem 199:112357
Li M, Cheng LP, Pang W et al (2020) Design, synthesis, and biological evaluation of novel acylhydrazone derivatives as potent neuraminidase inhibitors. ACS Med Chem Lett 11:1745–1750
Chen YQ, Lan LY, Huang M et al (2019) Hemagglutinin stalk-reactive antibodies interfere with influenza virus neuraminidase activity by steric hindrance. J Virol 93:e01526-18
Xiong FF, Liu XY, Gao FX et al (2020) Protective efficacy of anti-neuraminidase monoclonal antibodies against H7N9 influenza virus infection. Emerg Microbes Infect 9:78–87
Stadlbauer D, Zhu X, McMahon M et al (2019) Broadly protective human antibodies that target the active site of influenza virus neuraminidase. Science 366:499–504
Sriwilaijaroen N, Wilairat P, Hiramatsu H et al (2009) Mechanisms of the action of povidone-iodine against human and avian influenza A viruses: its effects on hemagglutination and sialidase activities. Virol J 6:124
Gottardi W (1999) Iodine and disinfection: theoretical study on mode of action, efficiency, stability, and analytical aspects in the aqueous system. Arch Pharm (Weinheim) 332:151–157
Ito H, Ito T, Hikida M et al (2006) Outbreak of highly pathogenic avian influenza in Japan and anti-influenza virus activity of povidone-iodine products. Dermatology 212(Suppl 1):115–118
Priyanka S, Gupta E, Neha M et al (2020) Chapter 16: Shikimic acid as intermediary model for the production of drugs effective against influenza virus. In: Egbuna C, Kumar S, Ifemeje JC, Ezzat SM, Kaliyaperumal S (eds) Phytochemicals as lead compounds for new drug discovery. Elsevier, pp 245–256
Sriwilaijaroen N, Kadowaki A, Onishi Y et al (2011) Mumefural and related HMF derivatives from Japanese apricot fruit juice concentrate show multiple inhibitory effects on pandemic influenza A (H1N1) virus. Food Chem 127:1–9
Sriwilaijaroen N, Fukumoto S, Kumagai K et al (2012) Antiviral effects of Psidium guajava Linn. (guava) tea on the growth of clinical isolated H1N1 viruses: its role in viral hemagglutination and neuraminidase inhibition. Antivir Res 94:139–146
Song JM, Lee KH, Seong BL (2005) Antiviral effect of catechins in green tea on influenza virus. Antivir Res 68:66–74
Kim YS, Li W, Kim JH et al (2020) Anti-influenza activity of an ethyl acetate fraction of a Rhus verniciflua ethanol extract by neuraminidase inhibition. Oxidative Med Cell Longev 2020:8824934
de Freitas CS, Rocha MEN, Sacramento CQ et al (2020) Agathisflavone, a biflavonoid from Anacardium occidentale L., inhibits influenza virus neuraminidase. Curr Top Med Chem 20:111–120
Luo S, Guo L, Sheng C et al (2020) Rapid identification and isolation of neuraminidase inhibitors from mockstrawberry (Duchesnea indica Andr.) based on ligand fishing combined with HR-ESI-Q-TOF-MS. Acta Pharm Sin B 10:1846–1855
Li P, Du R, Chen Z et al (2021) Punicalagin is a neuraminidase inhibitor of influenza viruses. J Med Virol 93:3465–3472
Li P, Du R, Wang Y et al (2020) Identification of chebulinic acid and chebulagic acid as novel influenza viral neuraminidase inhibitors. Front Microbiol 11:182
Grienke U, Schmidtke M, Kirchmair J et al (2010) Antiviral potential and molecular insight into neuraminidase inhibiting diarylheptanoids from Alpinia katsumadai. J Med Chem 53:778–786
Lai Y, Yan Y, Liao S et al (2020) 3D-quantitative structure-activity relationship and antiviral effects of curcumin derivatives as potent inhibitors of influenza H1N1 neuraminidase. Arch Pharm Res 43:489–502
Hahm HS, Toroitich EK, Borne AL et al (2020) Global targeting of functional tyrosines using sulfur-triazole exchange chemistry. Nat Chem Biol 16:150–159
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Sriwilaijaroen, N., Vavricka, C.J., Kiyota, H., Suzuki, Y. (2022). Influenza A Virus Neuraminidase Inhibitors. In: Suzuki, Y. (eds) Glycovirology. Methods in Molecular Biology, vol 2556. Humana, New York, NY. https://doi.org/10.1007/978-1-0716-2635-1_21
Download citation
DOI: https://doi.org/10.1007/978-1-0716-2635-1_21
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-2634-4
Online ISBN: 978-1-0716-2635-1
eBook Packages: Springer Protocols