Abstract
Introduction
Prostaglandin D synthase (PGDS) is responsible for the biosynthesis of PGD and J series, which have been shown to exhibit anti-inflammatory and anticatabolic effects. Two isoforms have been identified: hematopoietic- and lipocalin-type PGDS (H-PGDS and L-PGDS, respectively). The aims of this study were to investigate the expressions of H-PGDS and L-PGDS in cartilage from healthy donors and from patients with osteoarthritis (OA) and to characterize their regulation by interleukin-1-beta (IL-1β) in cultured OA chondrocytes.
Methods
The expressions of H-PGDS and L-PGDS mRNA and protein in cartilage were analyzed by real-time reverse transcriptase-polymerase chain reaction (RT-PCR) and immunohistochemistry, respectively. Chondrocytes were stimulated with IL-1β, and the expression of L-PGDS was evaluated by real-time RT-PCR and Western blotting. The roles of de novo protein synthesis and of the signalling pathways mitogen-activated protein kinases (MAPKs), nuclear factor-kappa-B (NF-κB), and Notch were evaluated using specific pharmacological inhibitors.
Results
L-PGDS and H-PGDS mRNAs were present in both healthy and OA cartilage, with higher levels of L-PGDS than H-PGDS (> 20-fold). The levels of L-PGDS mRNA and protein were increased in OA compared with healthy cartilage. Treatment of chondrocytes with IL-1β upregulated L-PGDS mRNA and protein expressions as well as PGD2 production in a dose- and time-dependent manner. The upregulation of L-PGDS by IL-1β was blocked by the translational inhibitor cycloheximide, indicating that this effect is indirect, requiring de novo protein synthesis. Specific inhibitors of the MAPK p38 (SB 203580) and c-jun N-terminal kinase (JNK) (SP600125) and of the NF-κB (SN-50) and Notch (DAPT) signalling pathways suppressed IL-1β-induced upregulation of L-PGDS expression. In contrast, an inhibitor of the extracellular signal-regulated kinase (ERK/MAPK) (PD98059) demonstrated no significant influence. We also found that PGD2 prevented IL-1β-induced upregulation of L-PGDS expression.
Conclusions
This is the first report demonstrating increased levels of L-PGDS in OA cartilage. IL-1β may be responsible for this upregulation through activation of the JNK and p38 MAPK and NF-κB signalling pathways. These data suggest that L-PGDS might have an important role in the pathophysiology of OA.
Similar content being viewed by others
Introduction
Osteoarthritis (OA) is the most common joint disorder and is a leading cause of disability throughout the world [1]. It can cause pain, stiffness, swelling, and loss of function in the joints. Pathologically, OA is characterized by progressive degeneration of articular cartilage, synovial inflammation, and subchondral bone remodeling. These processes are thought to be largely mediated through excess production of proinflammatory and catabolic mediators. Among these mediators, interleukin-1-beta (IL-1β) has been demonstrated to be predominantly involved in the initiation and progression of the disease [2–4]. One mechanism through which IL-1β exerts its effects is by inducing connective tissue cells, including chondrocytes, to produce matrix metalloproteinases (MMPs), aggrecanases, reactive oxygen species, and prostaglandins (PGs) [2].
The biosynthesis of PGs involves multiple enzymatically regulated reactions. The process is initiated through the release of arachidonic acid (AA) from the cell membrane by phospholipases. Subsequently, AA is converted to an intermediate substrate PGH2 by the actions of cyclooxygenase (COX). Two distinct isoforms have been identified: COX-1 is constitutively expressed, whereas COX-2 is induced by various stimuli such as proinflammatory cytokines and growth factors [5]. Once formed by COX-1 or COX-2, the unstable PGH2 intermediate is metabolized by specific PG synthase enzymes to generate the classical bioactive PGs, including PGE2, PGD2, PGF2α, PGI2, and thromboxane [6].
There is a growing body of evidence suggesting that PGD2 may have protective effects in OA and possibly other chronic articular diseases. For instance, treatment with PGD2 enhances the expression of the cartilage-specific matrix components collagen type II and aggrecan [7] and prevents chondrocyte apoptosis [8]. In addition, we have recently shown that PGD2 inhibits the induction of MMP-1 and MMP-13, which play an important role in cartilage damage [9]. Thus, PGD2 can mediate its chondroprotective effects not only through chondrogenesis enhancement, but also through inhibition of catabolic events. PGD2 was also shown to exhibit anti-inflammatory properties. Indeed, increased levels of PGD2 are observed during the resolution phase of inflammation and the inflammation is exacerbated by COX inhibitors [10, 11]. The anti-inflammatory role of PGD2 is supported by studies using PGD2 synthase-deficient and transgenic mice. The knockout animals show impaired resolution of inflammation, and transgenic animals have little detectable inflammation [12]. In addition, retroviral delivery of PGD2 synthase suppresses inflammatory responses in a murine air-pouch model of monosodium urate monohydrate crystal-induced inflammation [13]. Some effects of PGD2 can be mediated by its dehydration end product, 15d-PGJ2 (15-deoxy-delta12,14-PGJ2), which has been shown to exhibit potent anti-inflammatory and anticatabolic properties [14]. PGD2 exerts its effects principally by binding and activating two plasma membrane receptors, the D prostanoid receptor (DP) 1 [15] and chemoattractant-receptor-like molecule expressed on Th2 cells (CRTH2), also known as DP2 [16]. The effects of the PGD2 metabolite 15d-PGJ2 are mediated through mechanisms independent of and dependent on nuclear peroxisome proliferator-activated receptor-gamma (PPARγ) [14, 17, 18].
The biosynthesis of PGD2 from its precursor PGH2 is catalyzed by two PGD synthases (PGDSs): one is gluthatione-independent, the lipocaline-type PGDS (L-PGDS), and the other is glutathione-requiring, the hematopoietic PGDS (H-PGDS) [19]. L-PGDS (also called β-trace) is expressed abundantly in the central nervous system [20, 21], the heart [22], the retina [23], and the genital organs [24]. H-PGDS is expressed mainly in mast cells [25], megakaryocytes [26], and T-helper 2 lymphocytes [27]. So far, little is known about the expression and regulation of L-PGDS and H-PGDS in cartilage. To better understand the role of PGD2 in the joint, we investigated the expressions of H-PGDS and L-PGDS in healthy and OA cartilage. Moreover, we explored the effect of IL-1β, a key cytokine in the pathogenesis of OA, on L-PGDS expression in cultured chondrocytes.
Materials and methods
Reagents
Recombinant human IL-1β was obtained from Genzyme (Cambridge, MA, USA). Cycloheximide (CHX) was purchased from Sigma-Aldrich Canada (Oakville, ON, Canada). SB203580, SP600125, PD98059, SN-50, and N-[N-(3,5-diflurophenylacetate)-L-alanyl]-(S)-phenylglycine t-butyl ester (DAPT) were from Calbiochem (now part of EMD Biosciences, Inc., San Diego, CA, USA). PGD2 was from Cayman Chemical Company (Ann Arbor, MI, USA). Dulbecco's modified Eagle's medium (DMEM), penicillin and streptomycin, foetal calf serum (FCS), and TRIzol® reagent were from Invitrogen (Burlington, ON, Canada). All other chemicals were purchased from either Bio-Rad Laboratories (Mississauga, ON, Canada) or Sigma-Aldrich Canada.
Specimen selection and chondrocyte culture
Healthy cartilage and synovial fluids were obtained at necropsy, within 12 hours of death, from donors with no history of arthritic diseases (n = 13, mean ± standard deviation [SD] age of 64 ± 17 years). To ensure that only healthy tissue was used, cartilage specimens were thoroughly examined both macroscopically and microscopically. OA cartilage and synovial fluids were obtained from patients undergoing total knee replacement (n = 32, mean ± SD age of 67 ± 16 years). All OA patients were diagnosed on criteria developed by the American College of Rheumatology Diagnostic Subcommittee for OA [28]. At the time of surgery, the patients had symptomatic disease requiring medical treatment in the form of nonsteroidal anti-inflammatory drugs or selective COX-2 inhibitors. Patients who had received intra-articular injections of steroids were excluded. The Clinical Research Ethics Committee of Notre-Dame Hospital (Montreal, QC, Canada) approved the study protocol and the informed consent form.
Chondrocytes were released from cartilage by sequential enzymatic digestion as previously described [29]. Briefly, this consisted of 2 mg/mL pronase for 1 hour followed by 1 mg/mL collagenase for 6 hours (type IV; Sigma-Aldrich Canada) at 37°C in DMEM and antibiotics (100 U/mL penicillin and 100 μg/mL streptomycin). The digested tissue was briefly centrifuged and the pellet was washed. The isolated chondrocytes were seeded at high density in tissue culture flasks and cultured in DMEM supplemented with 10% heat-inactivated FCS. At confluence, the chondrocytes were detached, seeded at high density, and allowed to grow in DMEM, supplemented as above. The culture medium was changed every second day, and 24 hours before the experiment, the cells were incubated in fresh medium containing 0.5% FCS. Only first-passaged chondrocytes were used.
RNA extraction and reverse transcriptase-polymerase chain reaction
Total RNA from homogenized cartilage or stimulated chondrocytes was isolated using the TRIzol® reagent (Invitrogen) in accordance with the manufacturer's instructions. To remove contaminating DNA, isolated RNA was treated with RNase-free DNase I (Ambion, Inc., Austin, TX, USA). The RNA was quantitated using the RiboGreen RNA quantitation kit (Molecular Probes, Inc., now part of Invitrogen Corporation, Carlsbad, CA, USA), dissolved in diethylpyrocarbonate (DEPC)-treated H2O, and stored at -80°C until use. One microgram of total RNA was reverse-transcribed using Moloney murine leukemia virus reverse transcriptase (RT) (Fermentas, Burlington, ON, Canada), as detailed in the manufacturer's guidelines. One fiftieth of the RT reaction was analyzed by real-time quantitative polymerase chain reaction (PCR) as described below. The following primers were used: L-PGDS [GeneBank: NM000954], sense 5'-AACCAGTGTGAGACCCGAAC-3', antisense 5'-AGGCGGTGAATTTCTCCTTT-3'; H-PGDS [GeneBank: NM014485], sense 5'-CCCCATTTTGGAAGTTGATG-3', antisense 5'-TGAGGCGCATTATACGTGAG-3; and glyceraldehyde-3-phosphate dehydrogenase (GAPDH) [GeneBank: NM002046], sense 5'-CAGAACATCATCCCTGCCTCT-3', antisense 5'-GCTTGACAAAGTGGTCGTTGAG-3'.
Quantitative PCR analysis was performed in a total volume of 50 μL containing template DNA, 200 nM of sense and antisense primers, 25 μL of SYBR® Green master mix (Qiagen, Mississauga, ON, Canada), and uracil-N-glycosylase (UNG) (0.5 units; Epicentre Biotechnologies, Madison, WI, USA). After incubation at 50°C for 2 minutes (UNG reaction) and at 95°C for 10 minutes (UNG inactivation and activation of the AmpliTaq Gold enzyme; Qiagen), the mixtures were subjected to 40 amplification cycles (15 seconds at 95°C for denaturation and 1 minute for annealing and extension at 60°C). Incorporation of SYBR® Green dye into PCR products was monitored in real time using a GeneAmp 5700 Sequence detection system (Applied Biosystems, Foster City, CA, USA), allowing the determination of the threshold cycle (CT) at which exponential amplification of PCR products begins. After PCR, dissociation curves were generated with one peak, indicating the specificity of the amplification. A CT value was obtained from each amplification curve using the software provided by the manufacturer (Applied Biosystems).
Relative amounts of mRNA in healthy and OA cartilage were determined using the standard curve method. Serial dilutions of internal standards (plasmids containing cDNA of target genes) were included in each PCR run, and standard curves for the target gene and for GAPDH were generated by linear regression using log (CT) versus log (cDNA relative dilution). The CT values were then converted to number of molecules. Relative mRNA expression in cultured chondrocytes was determined using the ΔΔCT method, as detailed in the guidelines of the manufacturer (Applied Biosystems). A ΔCT value was first calculated by subtracting the CT value for the housekeeping gene GAPDH from the CT value for each sample. A ΔΔCT value was then calculated by subtracting the ΔCT value of the control (unstimulated cells) from the ΔCT value of each treatment. Fold changes compared with the control were then determined by raising 2 to the -ΔΔCT power. Each PCR generated only the expected specific amplicon as shown by the melting-temperature profiles of the final product and by gel electrophoresis of test PCRs. Each PCR was performed in triplicate on two separate occasions for each independent experiment.
Immunohistochemistry
Cartilage specimens were processed for immunohistochemistry as previously described [29]. The specimens were fixed in 4% paraformaldehyde and embedded in paraffin. Sections (5 μm) of paraffin-embedded specimens were deparaffinized in toluene and were dehydrated in a graded series of ethanol. The specimens were then preincubated with chondroitinase ABC (0.25 U/mL in phosphate-buffered saline [PBS] pH 8.0) for 60 minutes at 37°C, followed by a 30-minute incubation with Triton X-100 (0.3%) at room temperature. Slides were then washed in PBS followed by 2% hydrogen peroxide/methanol for 15 minutes. They were further incubated for 60 minutes with 2% healthy serum (Vector Laboratories, Burlingame, CA, USA) and overlaid with primary antibody for 18 hours at 4°C in a humidified chamber. The antibody was a rabbit polyclonal anti-human L-PGDS (United States Biological Inc., Swampscott, MA, USA), used at 10 μg/mL. Each slide was washed three times in PBS pH 7.4 and stained using the avidin-biotin complex method (Vectastain ABC kit; Vector Laboratories). The colour was developed with 3,3'-diaminobenzidine (DAB) (Vector Laboratories) containing hydrogen peroxide. The slides were counterstained with eosin. The specificity of staining was evaluated by using antibody that had been preadsorbed (1 hour at 37°C) with a 20-fold molar excess of recombinant human L-PGDS (Cayman Chemical Company) and by substituting the primary antibody with nonimmune rabbit IgG (Chemicon International, Temecula, CA, USA), used at the same concentration as the primary antibody. The evaluation of positive-staining chondrocytes was performed using our previously published method [29]. For each specimen, six microscopic fields were examined under × 40 magnification. The total number of chondrocytes and the number of chondrocytes staining positive were evaluated, and the results were expressed as the percentage of chondrocytes staining positive (cell score).
Western blot analysis
Chondrocytes were lysed in ice-cold lysis buffer (50 mM Tris-HCl, pH 7.4, 150 mM NaCl, 2 mM EDTA [ethylenediaminetetraacetic acid], 1 mM PMSF [phenylmethylsulphonyl fluoride], 10 μg/mL each of aprotinin, leupeptin, and pepstatin, 1% NP-40, 1 mM Na3VO4, and 1 mM NaF). Lysates were sonicated on ice and centrifuged at 12,000 revolutions per minute for 15 minutes. The protein concentration of the supernatant was determined using the bicinchoninic acid method (Pierce, Rockford, IL, USA). Twenty micrograms of total cell lysate was subjected to SDS-PAGE and electrotransferred to a nitrocellulose membrane (Bio-Rad Laboratories). After blocking in 20 mM Tris-HCl pH 7.5 containing 150 mM NaCl, 0.1% Tween 20, and 5% (wt/vol) nonfat dry milk, blots were incubated overnight at 4°C with the primary antibody and washed with a Tris buffer (Tris-buffered saline pH 7.5 with 0.1% Tween 20). The blots were then incubated with horseradish peroxidase-conjugated secondary antibody (Pierce), washed again, incubated with SuperSignal Ultra Chemiluminescent reagent (Pierce), and, finally, exposed to Kodak X-Omat film (Eastman Kodak Company, Rochester, NY, USA). Bands on the films were scanned using the imaging system Chemilmager 4000 (Alpha Innotech Corporation, San Leandro, CA, USA), and the intensity of the L-PGDS bands was normalized by dividing them by the intensity of the β-actin band of the corresponding sample.
11β-PGF2α and PGD2assays
The levels of 11β-PGF2α in hyaluronidase-treated synovial fluids and of PGD2 in chondrocyte supernatants were determined using competitive enzyme immunoassays from Cayman Chemical Company. Assays were performed according to the manufacturer's recommendation.
Statistical analysis
Data are expressed as the mean ± standard error of the mean (SEM). Statistical significance was assessed by the two-tailed Student t test. P values of less than 0.05 were considered significant.
Results
Expressions of L-PGDS and H-PGDS in healthy and osteoarthritis cartilage
We first analyzed the levels of L-PGDS and H-PGDS mRNAs in healthy and OA cartilage using real-time quantitative RT-PCR. As shown in Figure 1, cartilage predominantly expresses L-PGDS mRNA, and its levels of expression were approximately threefold higher in OA cartilage compared with healthy cartilage. In contrast to L-PGDS, there was no statistically significant difference in the levels of H-PGDS mRNA between OA and healthy cartilage (Figure 1). In preliminary experiments, we showed that the amplification efficiencies of tested genes and GAPDH were similar. The efficiencies for the amplification of each gene and the reference were approximately equal, ranging between 1.95 and 2.
Lipocalin-type prostaglandin D synthase (L-PGDS) and hematopoietic-type PGDS (H-PGDS) mRNA levels in healthy and osteoarthritis (OA) human cartilage. RNA was extracted from healthy (n = 9) and OA (n = 9) cartilage, reverse-transcribed into cDNA, and processed for real-time polymerase chain reaction. The threshold cycle values were converted to the number of molecules, as described in Materials and methods. Data are expressed as copies of the gene's mRNA detected per 10,000 GAPDH copies. *P < 0.05 versus healthy samples. GAPDH, glyceraldehyde-3-phosphate dehydrogenase.
Next, we used immunohistohemistry to analyze the localization and the expression level of L-PGDS and H-PGDS proteins in healthy and OA cartilage. As shown in Figures 2a and 2b, the immunostaining for L-PGDS was located in the superficial and upper intermediate layers of cartilage. Statistical evaluation for the cell score revealed a clear and significant increase in the number of chondrocytes staining positive for L-PGDS in OA cartilage (43% ± 6%, mean ± SEM) compared with healthy cartilage (20% ± 4%, mean ± SEM). The specificity of the staining was confirmed using antibody that had been preadsorbed (1 hour at 37°C) with a 20-fold molar excess of the recombinant protein (Figure 2c) or nonimmune control IgG (data not shown). Using several commercially available antibodies directed against human H-PGDS, we were unable to detect H-PGDS protein expression in OA or healthy cartilage. Together, these data indicate that the expression level of L-PGDS is increased in OA cartilage.
Expression of lipocalin-type prostaglandin D synthase (L-PGDS) protein in healthy and osteoarthritis (OA) cartilage. Representative immunostaining of human healthy (a) and OA (b) cartilage for L-PGDS protein. (c) OA specimens treated with anti-L-PGDS antibody that was preadsorbed with a 20-fold molar excess of recombinant human L-PGDS (control for staining specificity). (d) Percentage of chondrocytes expressing L-PGDS in healthy and OA cartilage. Results are expressed as the mean ± standard error of the mean of nine healthy and nine OA specimens. *P < 0.05 versus healthy cartilage.
To assess the level of PGD2 in synovial fluids from OA and healthy donors, we quantified its major stable metabolite, 11β-PGF2α. We measured this metabolite because PGD2 is unstable in vivo [30] and quantification of PGD2 in synovial fluid can be unreliable. We found a higher level of 11β-PGF2α in OA synovial fluid when compared with healthy synovial fluid (Figure 3), indicating that the production of PGD2 is higher in OA synovial fluids. Together, these data indicate increased expression and activity of L-PGDS in OA tissues.
Synovial levels of the prostaglandin D 2 (PGD 2 ) metabolite 11β-PGF 2 α. 11β-PGF2α levels were measured in synovial fluids from healthy subjects and patients with osteoarthritis (OA). The results are expressed as picograms per milligram of proteins and are the mean ± standard error of the mean of 7 healthy subjects and 11 OA patients. *P < 0.05 versus healthy subjects.
Interleukin-1-beta induces L-PGDS expression in chondrocytes
IL-1β plays a major role in the cartilage physiology and in the pathogenesis of OA [2]; therefore, we examined its effects on the expression of L-PGDS in cultured OA chondrocytes. Cells were treated with IL-1β (100 pg/mL) for different time periods, and the levels of L-PGDS mRNA were quantified using real-time RT-PCR. IL-1β-induced changes in gene expression were evaluated as fold over control (untreated cells) after normalization to the internal control gene, GAPDH. As shown in Figure 4a, treatment with IL-1β (100 pg/mL) enhanced L-PGDS mRNA expression in a time-dependent manner. L-PGDS mRNA expression started to gradually increase 24 hours post-stimulation with IL-1β and remained elevated until 72 hours. The induction of L-PGDS mRNA by IL-1β was also dose-dependent. A significant increase at concentrations as low as 10 pg/mL was observed and the maximal effect was reached at 100 pg/mL (Figure 4b). To determine whether changes in mRNA levels were paralleled by changes in L-PGDS protein levels, we performed Western blot analysis. Consistent with its effects on L-PGDS mRNA, treatment with IL-1β led to a dose- and time-dependent increase in the L-PGDS protein expression (Figure 4c, d). To establish whether the IL-1β-induced increase in L-PGDS expression corresponded with an increase in PGDS activity, we measured PGD2 levels in conditioned media. As shown in Figures 4e and 4f, the increased expression of L-PGDS protein was accompanied by a time- and dose-dependent increase in PGD2 production.
Effect of interleukin-1-beta (IL-1β) on lipocalin-type prostaglandin D synthase (L-PGDS) expression in osteoarthritis chondrocytes. Chondrocytes were treated with 100 pg/mL IL-1β for the indicated time periods or with increasing concentrations of IL-1β for 48 hours. (a, b) Total RNA was isolated and reverse-transcribed into cDNA, and L-PGDS and GAPDH mRNAs were quantified using real-time polymerase chain reaction. All experiments were performed in triplicate, and negative controls without template RNA were included in each experiment. Results are expressed as fold changes, considering 1 as the value of untreated cells, and represent the mean ± standard error of the mean (SEM) of four independent experiments. *P < 0.05 compared with unstimulated cells. (c, d) Cell lysates were prepared and analyzed for L-PGDS and β-actin proteins by Western blotting. Representative Western blots are shown in the upper panels. In the lower panels, the bands were scanned, and the L-PGDS band intensity values were normalized to the corresponding β-actin band intensity value. Data are expressed as fold induction, considering 1 as the value of unstimulated cells, and represent the mean ± SEM of four independent experiments. *P < 0.05 compared with unstimulated cells. (e, f) Conditioned media was collected and analyzed for prostaglandin D2 (PGD2) content. Results are expressed as the mean ± SEM of four independent experiments. *P < 0.05 compared with unstimulated cells. GAPDH, glyceraldehyde-3-phosphate dehydrogenase.
The upregulation of L-PGDS mRNA expression in chondrocytes requires de novoprotein synthesis
The lag period required for IL-1β to induce L-PGDS mRNA in chondrocytes contrasts with those required for other IL-1β-inducible genes, the expression of which starts as early as 2 to 6 hours and reaches a maximum at 8 to 18 hours. This suggests that de novo protein synthesis is required for IL-1β-induced L-PGDS expression. To evaluate this possibility, we examined the impact of the protein synthesis inhibitor CHX. Chondrocytes were stimulated with IL-1β in the absence or presence of CHX, and the levels of L-PGDS mRNA were analyzed by real-time PCR. As shown in Figure 5, treatment with CHX prevented IL-1β-mediated upregulation of L-PGDS mRNA expression. This suggests that, to upregulate L-PGDS expression in chondrocytes, IL-1β must induce the synthesis of one or more proteins.
The interleukin-1-beta (IL-1β)-induced upregulation of lipocalin-type prostaglandin D synthase (L-PGDS) mRNA expression requires de novo protein synthesis. Chondrocytes were incubated with cycloheximide (CHX) (10 μg/mL) for 30 minutes prior to stimulation with 100 pg/mL IL-1β for 48 hours. Total RNA was isolated and reverse-transcribed into cDNA, and L-PGDS mRNA was quantified using real-time polymerase chain reaction. Results are expressed as fold changes, considering 1 as the value of untreated cells, and represent the mean ± standard error of the mean of four independent experiments. *P < 0.05 compared with cells treated with IL-1β alone.
JNK and p38 MAPKs and NF-κB pathways contribute to interleukin-1-beta-induced upregulation of L-PGDS
IL-1β exerts its effects acting through activation of the mitogen-activated protein kinase (MAPK) (extracellular signal-regulated kinase [ERK], c-jun N-terminal kinase [JNK], and p38) and nuclear factor-kappa-B (NF-κB) signalling cascades [31–35]. To evaluate the potential contribution of these pathways in IL-1β-induced L-PGDS expression, we used specific pharmacological inhibitors. Chondrocytes were pretreated for 30 minutes with selective inhibitors for the above pathways and then stimulated or not with IL-1β for 48 hours. As shown in Figure 6a, pretreatment with the p38 MAPK inhibitor SB203580 (1 μM), the JNK MAPK inhibitor SP600125 (10 μM), or the NF-κB inhibitor SN-50 (1 μM) suppressed IL-1β-induced upregulation of L-PGDS expression. In contrast, pretreatment with the p42/44 MAPK inhibitor PD98059 (10 μM) had no effect on IL-1β-induced upregulation of L-PGDS. The concentration of the MAPK and NF-κB inhibitors used for these experiments had no significant effect on cell viability as indicated by the results of the MTT (3- [4,5-dimethylthiazol-2-yl]-2,5-diphenyltetrazolium bromide) assay (data not shown). These results suggest that the activation of JNK and p38 MAPK as well as NF-κB is essential to the induction of L-PGDS by IL-1β in chondrocytes.
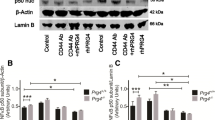
Effect of mitogen-activated protein kinase, nuclear factor-kappa-B, and Notch inhibitors on interleukin-1-beta (IL-1β)-induced upregulation of lipocalin-type prostaglandin D synthase (L-PGDS) expression. Osteoarthritis chondrocytes were pretreated with SB203580 (1 μM), SP600125 (10 μM), PD98059 (10 μM), or SN-50 (1 μM) for 30 minutes (a) or with increasing concentrations (1, 5, and 10 mM) of DAPT for 48 hours (b) prior to stimulation with IL-1β (100 pg/mL). After 48 hours, cell lysates were prepared and analyzed for L-PGDS and β-actin protein expression by Western blotting. Representative Western blots are shown in the upper panels. In the lower panels, the bands were scanned, and the L-PGDS band intensity values were normalized to the corresponding β-actin band intensity value. Data are expressed as fold induction, considering 1 as the value of unstimulated cells, and represent the mean ± standard error of the mean of four independent experiments. *P < 0.05 compared with cells treated with IL-1β alone. DAPT, N-[N-(3,5-diflurophenylacetate)-L-alanyl]-(S)-phenylglycine t-butyl ester.
The Notch signalling pathway regulates diverse cellular processes, including proliferation, differentiation, and apoptosis [36], and was reported to contribute to the regulation of L-PGDS expression [37]. To determine whether this pathway participates in IL-1β-induced L-PGDS expression in human chondrocytes, we assessed the effect of DAPT. DAPT is a γ-secretase inhibitor, which blocks cleavage of the intracellular domain of all Notch proteins, and is widely used to evaluate the effect of Notch inhibition [36]. As shown in Figure 6b, pretreatment with DAPT dose-dependently prevented IL-1β-induced L-PGDS protein expression, indicating the involvement of Notch signalling in this process. Notch inhibition was confirmed by transcriptional inhibition of its direct target gene, Hes1 (data not shown).
PGD2downregulated L-PGDS expression
To further characterize the regulation of L-PGDS expression in cartilage, we examined the effect of PGD2, the end product of L-PGDS. Chondrocytes were stimulated with IL-1β in the absence or presence of increasing concentrations of PGD2 for 48 hours, and the expression of L-PGDS was evaluated by Western blotting. As shown in Figure 7, treatment with PGD2 dose-dependently reduced IL-1β-induced L-PGDS expression.
Effect of prostaglandin D 2 (PGD 2 ) on interleukin-1-beta (IL-1β)-induced upregulation of lipocalin-type prostaglandin D synthase (L-PGDS) expression. Osteoarthritis chondrocytes were pretreated with increasing concentrations of PGD2 for 30 minutes prior to stimulation with IL-1β (100 pg/mL). After 48 hours, cell lysates were prepared and analyzed for L-PGDS and β-actin protein expression by Western blotting. A representative Western blot is shown in the upper panel. In the lower panel, the bands were scanned, and the L-PGDS band intensity values were normalized to the corresponding β-actin band intensity value. Data are expressed as fold induction, considering 1 as the value of unstimulated cells, and represent the mean ± standard error of the mean of four independent experiments. *P < 0.05 compared with cells stimulated with IL-1β alone.
Discussion
This is the first report to demonstrate the presence of L-PGDS in human cartilage and to show that its levels are elevated in OA cartilage compared with healthy cartilage. The proinflammatory cytokine IL-1β upregulated, whereas PGD2 downregulated, the expression of L-PGDS in cultured chondrocytes. These findings suggest that L-PGDS may be implicated in the pathogenesis of OA.
In healthy cartilage, L-PGDS immunostaining was located in only a few cells in the superficial and middle zones. By contrast, in OA cartilage, the cell score was significantly higher, particularly in cartilage areas showing significant damage (fibrillation). Given the anti-inflammatory and anticatabolic roles of PGD2, it is reasonable to speculate that the upregulation of L-PGDS may act as a sort of chondroprotective mechanism. Increased expression of L-PGDS was described in other diseases such as atherosclerosis [22], multiple sclerosis [38], diabetes [39] essential hypertension [40], and Tay-Sachs and Sandhoff diseases [41]. Thus, L-PGDS expression is upregulated in many pathologies.
The enhanced expression of L-PGDS in the superficial and middle zones of cartilage could potentially be due to the increased level of the proinflammatory cytokine IL-1β in these zones. Indeed, IL-1β, which plays pivotal roles in the initiation and progression of OA, has been shown to accumulate in these zones [42–46]. To prove this hypothesis, we performed cell culture experiments. Our results revealed that exposure to IL-1β led to a time- and concentration-dependent upregulation of L-PGDS expression and PGD2 production. The upregulation of L-PGDS expression by IL-1β was blocked by CHX, suggesting that this effect of IL-1β requires de novo protein synthesis and would be consistent with an indirect stimulatory mechanism.
The delayed induction of L-PGDS by IL-1β in chondrocytes is consistent with the recently reported anti-inflammatory and anticatabolic properties of PGD2. Indeed, the production of PGD2 is markedly elevated during the resolution of inflammation in carrageenan-induced pleurisy in rats, and exogenous PGD2 significantly reduces neutrophil levels in the inflammatory exudates [10, 11]. Enhanced production of PGD2 was also described during the resolution phase of the wound-healing process [47]. Cipollone and colleagues [48] examined the expression of L-PGDS in atherosclerotic arteries and found lower expression of L-PGDS and higher expression of microsomal prostaglandin E synthase-1 (mPGES-1) in symptomatic plaques and found higher expression of L-PGDS and lower expression of mPGES-1 in asymptomatic ones. This suggests that the balance between PGD2 and PGE2 contributes to the pathology of atherosclerosis and that a shift toward PGD2 synthesis may have an anti-inflammatory role. This is supported by the observation that increased biosynthesis of PGD2 is associated with reduced production of PGE2 in several in vitro studies [49, 50]. Recently, two separate studies demonstrated anti-inflammatory properties of PGD2 in an air-pouch model of inflammation induced by monosodium urate monohydrate crystals [13, 51]. Moreover, H-PGDS knockout mice fail to resolve a delayed-type hypersensitivity reaction [12]. In addition to its anti-inflammatory effects, PGD2 was shown to induce the expression of collagen type II and aggrecan [7], to prevent apoptosis [8], and to inhibit the induction of MMP-1 and MMP-13 [52] in chondrocytes. Together, these data and those from the present study favour the hypothesis that the upregulation of L-PGDS expression in chondrocytes may be part of a negative feedback control of inflammatory and catabolic responses activated by IL-1β in the joint.
The production of PGD2 by chondrocytes is of particular interest since PGD2 is readily converted to 15d-PGJ2, a potent antiarthritic agent [14]. 15dPGJ2 downregulates the expression of a number of inflammatory and catabolic mediators involved in the pathogenesis of OA, including IL-1β, tumour necrosis factor-alpha, inducible nitric-oxide synthase, and MMPs [14]. Moreover, many in vivo studies support a protective effect of 15d-PGJ2 and other PPARγ ligands in experimental animal models of OA [53, 54]. Thus, the increased expression of L-PGDS can lead to the production of a PPARγ ligand in the joint. In contrast to classical PGs, which induce their effects through binding to cell surface G protein-coupled receptors, 15d-PGJ2 induces most of its effects through the nuclear receptor PPARγ. We have previously shown that PPARγ expression is reduced in OA cartilage and that IL-1β downregulates its expression in chondrocytes [29], which may interfere with the protective effect of the PGD2 metabolite 15d-PGJ2. Therefore, the increased expression of L-PGDS observed in our study may represent a compensatory mechanism to counter the reduced expression of PPARγ in OA and to limit local inflammatory and catabolic responses. Also, it should be noted that 15d-PGJ2 can induce many of its effects independently of PPARγ [14, 17, 18]. In addition, PGD2 can directly exert protective effects in OA before being metabolized into 15d-PGJ2. Indeed, we have recently demonstrated that human chondrocytes express functional DP1 and CRTH-2 and that PGD2 downregulates MMP-1 and MMP-13 expressions through activation of the DP1 pathway [9].
To elucidate the mechanisms by which IL-1β upregulates L-PGDS expression, we evaluated the roles played by downstream signalling cascades using specific pharmacological inhibitors. We found that JNK and p38 MAPK inhibitors blocked IL-1β-induced L-PGDS upregulation, whereas an inhibitor of the ERK MAPK was without effect. We also found that NF-κB blockade caused a significant decrease in IL-1β-induced upregulation of L-PGDS protein expression. These findings support the hypothesis that the JNK and p38 MAPKs as well as the NF-κB pathways are involved in the upregulation of L-PGDS expression by IL-1β. Our results are concordant with previous reports that implicate activation of MAPKs (JNK and p38) and NF-κB in the upregulation of L-PGDS in leptomeningel cells [55], endothelial cells [56], and macrophages [57]. The activation of JNK and p38 MAPK and of NF-κB pathways in chondrocytes has been shown to cause activation of their downstream transcription factors, including activation protein-1 (AP-1) and NF-κB [31–35]. Interestingly, the promoter region of the human L-PGDS contains binding sites for NF-κB and AP-1 [55, 56]. Therefore, one could speculate that upregulation of L-PGDS expression by IL-1β could be mediated by AP-1 and NF-κB. Our results also demonstrate that the Notch signalling pathway positively contributes to IL-1β-induced L-PGDS expression in chondrocytes because DAPT, a Notch signalling inhibitor, blocked this process. These findings contrast with previous data showing that the Notch pathway downregulates L-PGDS expression in the brain-derived TE671 cells [37]. The reasons for these discrepancies are presently unclear but are most likely due to cell-type differences or to differences in experimental conditions.
We also found that PGD2 inhibits IL-1β-induced L-PGDS expression. These results suggest that PGD2 may exert a negative feedback mechanism to downregulate L-PGDS expression and activity. Given that the levels of L-PGDS are elevated in OA cartilage and that IL-1β upregulated its expression in chondrocytes, it is possible that the IL-1β effect prevails over that of PGD2 in vivo during advanced stages of the disease. Indeed, the OA cartilage specimens used in this study were from donors with long-established OA. Further studies are clearly warranted to determine the expression profile of L-PGDS over the course of OA in animal models of the disease.
The concentrations of PGD2 used to suppress IL-1β-induced L-PGDS expression are likely to be much higher than those produced in synovial fluids. However, it should be noted that, like other eicosanoids, PGD2 functions as an autocrine and paracrine molecule and can readily reach pharmacological levels in the microenvironment of cells that produce it.
Conclusion
Our study has demonstrated for the first time that L-PGDS is upregulated in OA cartilage. The proinflammatory cytokine IL-1β may be responsible for this upregulation via a mechanism that seems to involve the activation of the JNK and p38 MAPK and NF-κB signalling pathways. These results suggest that the increased expression of L-PGDS may play a protective role against articular inflammation and cartilage damage.
Abbreviations
- 15d-PGJ2:
-
15-deoxy-delta12,14-PGJ2
- AA:
-
arachidonic acid
- AP-1:
-
activation protein-1
- CHX:
-
cycloheximide
- COX:
-
cyclooxygenase
- CRTH2:
-
chemoattractant-receptor-like molecule expressed on Th2 cells
- CT:
-
threshold cycle
- DAPT:
-
N-[N-(3,5-diflurophenylacetate)-L-alanyl]-(S)-phenylglycine t-butyl ester
- DMEM:
-
Dulbecco's modified Eagle's medium
- DP:
-
D prostanoid receptor
- ERK:
-
extracellular signal-regulated kinase
- FCS:
-
foetal calf serum
- GAPDH:
-
glyceraldehyde-3-phosphate dehydrogenase
- H-PGDS:
-
hematopoietic-type prostaglandin D synthase
- IL-1β:
-
interleukin-1-beta
- JNK:
-
c-jun N-terminal kinase
- L-PGDS:
-
lipocalin-type prostaglandin D synthase
- MAPK:
-
mitogen-activated protein kinase
- MMP:
-
matrix metalloproteinase
- mPGES-1:
-
microsomal prostaglandin E synthase-1
- NF-κB:
-
nuclear factor-kappa-B
- OA:
-
osteoarthritis
- PBS:
-
phosphate-buffered saline
- PCR:
-
polymerase chain reaction
- PG:
-
prostaglandin
- PGDS:
-
prostaglandin D synthase
- PPARγ:
-
peroxisome proliferator-activated receptor-gamma
- RT:
-
reverse transcriptase
- RT-PCR:
-
reverse transcriptase-polymerase chain reaction
- SD:
-
standard deviation
- SEM:
-
standard error of the mean
- UNG:
-
uracil-N-glycosylase.
References
Lawrence RC, Helmick CG, Arnett FC, Deyo RA, Felson DT, Giannini EH, Heyse SP, Hirsch R, Hochberg MC, Hunder GG, Liang MH, Pillemer SR, Steen VD, Wolfe F: Estimates of the prevalence of arthritis and selected musculoskeletal disorders in the United States. Arthritis Rheum. 1998, 41: 778-799. 10.1002/1529-0131(199805)41:5<778::AID-ART4>3.0.CO;2-V.
Goldring MB: The role of cytokines as inflammatory mediators in osteoarthritis: lessons from animal models. Connect Tissue Res. 1999, 40: 1-11. 10.3109/03008209909005273.
Pelletier JP, Martel-Pelletier J, Abramson SB: Osteoarthritis, an inflammatory disease: potential implication for the selection of new therapeutic targets. Arthritis Rheum. 2001, 44: 1237-1247. 10.1002/1529-0131(200106)44:6<1237::AID-ART214>3.0.CO;2-F.
Goldring MB, Berenbaum F: The regulation of chondrocyte function by proinflammatory mediators: prostaglandins and nitric oxide. Clin Orthop Relat Res. 2004, S37-46. 10.1097/01.blo.0000144484.69656.e4.
Smith WL, Langenbach R: Why there are two cyclooxygenase isozymes. J Clin Invest. 2001, 107: 1491-1495. 10.1172/JCI13271.
Martel-Pelletier J, Pelletier JP, Fahmi H: Cyclooxygenase-2 and prostaglandins in articular tissues. Semin Arthritis Rheum. 2003, 33: 155-167. 10.1016/S0049-0172(03)00134-3.
Jakob M, Demarteau O, Suetterlin R, Heberer M, Martin I: Chondrogenesis of expanded adult human articular chondrocytes is enhanced by specific prostaglandins. Rheumatology (Oxford). 2004, 43: 852-857. 10.1093/rheumatology/keh197.
Relic B, Benoit V, Franchimont N, Ribbens C, Kaiser MJ, Gillet P, Merville MP, Bours V, Malaise MG: 15-deoxy-delta12,14-prostaglandin J2 inhibits Bay 11–7085-induced sustained extracellular signal-regulated kinase phosphorylation and apoptosis in human articular chondrocytes and synovial fibroblasts. J Biol Chem. 2004, 279: 22399-22403. 10.1074/jbc.M314118200.
Zayed N, Afif H, Chabane N, Mfuna-Endam L, Benderdour M, Martel-Pelletier J, Pelletier JP, Motiani RK, Trebak M, Duval N, Fahmi H: Inhibition of interleukin-1beta-induced matrix metalloproteinases 1 and 13 production in human osteoarthritic chondrocytes by prostaglandin D(2). Arthritis Rheum. 2008, 58: 3530-3540. 10.1002/art.23958.
Gilroy DW, Colville-Nash PR, Willis D, Chivers J, Paul-Clark MJ, Willoughby DA: Inducible cyclooxygenase may have anti-inflammatory properties. Nat Med. 1999, 5: 698-701. 10.1038/9550.
Ianaro A, Ialenti A, Maffia P, Pisano B, Di Rosa M: Role of cyclopentenone prostaglandins in rat carrageenin pleurisy. FEBS Lett. 2001, 508: 61-66. 10.1016/S0014-5793(01)03035-6.
Trivedi SG, Newson J, Rajakariar R, Jacques TS, Hannon R, Kanaoka Y, Eguchi N, Colville-Nash P, Gilroy DW: Essential role for hematopoietic prostaglandin D2 synthase in the control of delayed type hypersensitivity. Proc Natl Acad Sci USA. 2006, 103: 5179-5184. 10.1073/pnas.0507175103.
Murakami Y, Akahoshi T, Hayashi I, Endo H, Hashimoto A, Kono S, Kondo H, Kawai S, Inoue M, Kitasato H: Inhibition of monosodium urate monohydrate crystal-induced acute inflammation by retrovirally transfected prostaglandin D synthase. Arthritis Rheum. 2003, 48: 2931-2941. 10.1002/art.11271.
Fahmi H, Pelletier JP, Martel-Pelletier J: PPARgamma ligands as modulators of inflammatory and catabolic responses on arthritis. An overview. J Rheumatol. 2002, 29: 3-14.
Hirata M, Kakizuka A, Aizawa M, Ushikubi F, Narumiya S: Molecular characterization of a mouse prostaglandin D receptor and functional expression of the cloned gene. Proc Natl Acad Sci USA. 1994, 91: 11192-11196. 10.1073/pnas.91.23.11192.
Hirai H, Tanaka K, Yoshie O, Ogawa K, Kenmotsu K, Takamori Y, Ichimasa M, Sugamura K, Nakamura M, Takano S, Nagata K: Prostaglandin D2 selectively induces chemotaxis in T helper type 2 cells, eosinophils, and basophils via seven-transmembrane receptor CRTH2. J Exp Med. 2001, 193: 255-261. 10.1084/jem.193.2.255.
Boyault S, Bianchi A, Moulin D, Morin S, Francois M, Netter P, Terlain B, Bordji K: 15-Deoxy-delta(12,14)-prostaglandin J(2) inhibits IL-1beta-induced IKK enzymatic activity and IkappaBalpha degradation in rat chondrocytes through a PPARgamma-independent pathway. FEBS Lett. 2004, 572: 33-40. 10.1016/j.febslet.2004.06.090.
Bianchi A, Moulin D, Sebillaud S, Koufany M, Galteau MM, Netter P, Terlain B, Jouzeau JY: Contrasting effects of peroxisome-proliferator-activated receptor (PPAR)gamma agonists on membrane-associated prostaglandin E2 synthase-1 in IL-1beta-stimulated rat chondrocytes: evidence for PPARgamma-independent inhibition by 15-deoxy-Delta12,14prostaglandin J2. Arthritis Res Ther. 2005, 7: R1325-1337. 10.1186/ar1830.
Urade Y, Eguchi N: Lipocalin-type and hematopoietic prostaglandin D synthases as a novel example of functional convergence. Prostaglandins Other Lipid Mediat. 2002, 68–69: 375-382. 10.1016/S0090-6980(02)00042-4.
Blodorn B, Mader M, Urade Y, Hayaishi O, Felgenhauer K, Bruck W: Choroid plexus: the major site of mRNA expression for the beta-trace protein (prostaglandin D synthase) in human brain. Neurosci Lett. 1996, 209: 117-120. 10.1016/0304-3940(96)12614-8.
Urade Y, Fujimoto N, Hayaishi O: Purification and characterization of rat brain prostaglandin D synthetase. J Biol Chem. 1985, 260: 12410-12415.
Eguchi Y, Eguchi N, Oda H, Seiki K, Kijima Y, Matsu-ura Y, Urade Y, Hayaishi O: Expression of lipocalin-type prostaglandin D synthase (beta-trace) in human heart and its accumulation in the coronary circulation of angina patients. Proc Natl Acad Sci USA. 1997, 94: 14689-14694. 10.1073/pnas.94.26.14689.
Beuckmann CT, Gordon WC, Kanaoka Y, Eguchi N, Marcheselli VL, Gerashchenko DY, Urade Y, Hayaishi O, Bazan NG: Lipocalin-type prostaglandin D synthase (beta-trace) is located in pigment epithelial cells of rat retina and accumulates within interphotoreceptor matrix. J Neurosci. 1996, 16: 6119-6124.
Gerena RL, Irikura D, Eguchi N, Urade Y, Killian GJ: Immunocytochemical localization of lipocalin-type prostaglandin D synthase in the bull testis and epididymis and on ejaculated sperm. Biol Reprod. 2000, 62: 547-556. 10.1095/biolreprod62.3.547.
Urade Y, Ujihara M, Horiguchi Y, Igarashi M, Nagata A, Ikai K, Hayaishi O: Mast cells contain spleen-type prostaglandin D synthetase. J Biol Chem. 1990, 265: 371-375.
Fujimori K, Kanaoka Y, Sakaguchi Y, Urade Y: Transcriptional activation of the human hematopoietic prostaglandin D synthase gene in megakaryoblastic cells. Roles of the oct-1 element in the 5'-flanking region and the AP-2 element in the untranslated exon 1. J Biol Chem. 2000, 275: 40511-40516. 10.1074/jbc.M007688200.
Tanaka K, Ogawa K, Sugamura K, Nakamura M, Takano S, Nagata K: Cutting edge: differential production of prostaglandin D2 by human helper T cell subsets. J Immunol. 2000, 164: 2277-2280.
Altman RD: Criteria for the classification of osteoarthritis of the knee and hip. Scand J Rheumatol Suppl. 1987, 65: 31-39. 10.3109/03009748709102175.
Afif H, Benderdour M, Mfuna-Endam L, Martel-Pelletier J, Pelletier JP, Duval N, Fahmi H: Peroxisome proliferator-activated receptor gamma1 expression is diminished in human osteoarthritic cartilage and is downregulated by interleukin-1beta in articular chondrocytes. Arthritis Res Ther. 2007, 9: R31-10.1186/ar2151.
O'Sullivan S, Mueller MJ, Dahlen SE, Kumlin M: Analyses of prostaglandin D2 metabolites in urine: comparison between enzyme immunoassay and negative ion chemical ionisation gas chromatography-mass spectrometry. Prostaglandins Other Lipid Mediat. 1999, 57: 149-165. 10.1016/S0090-6980(98)00076-8.
Geng Y, Valbracht J, Lotz M: Selective activation of the mitogen-activated protein kinase subgroups c-Jun NH2 terminal kinase and p38 by IL-1 and TNF in human articular chondrocytes. J Clin Invest. 1996, 98: 2425-2430. 10.1172/JCI119056.
Ding GJ, Fischer PA, Boltz RC, Schmidt JA, Colaianne JJ, Gough A, Rubin RA, Miller DK: Characterization and quantitation of NF-kappaB nuclear translocation induced by interleukin-1 and tumor necrosis factor-alpha. Development and use of a high capacity fluorescence cytometric system. J Biol Chem. 1998, 273: 28897-28905. 10.1074/jbc.273.44.28897.
Mengshol JA, Vincenti MP, Coon CI, Barchowsky A, Brinckerhoff CE: Interleukin-1 induction of collagenase 3 (matrix metalloproteinase 13) gene expression in chondrocytes requires p38, c-Jun N-terminal kinase, and nuclear factor kappaB: differential regulation of collagenase 1 and collagenase 3. Arthritis Rheum. 2000, 43: 801-811. 10.1002/1529-0131(200004)43:4<801::AID-ANR10>3.0.CO;2-4.
Mendes AF, Caramona MM, Carvalho AP, Lopes MC: Role of mitogen-activated protein kinases and tyrosine kinases on IL-1-Induced NF-kappaB activation and iNOS expression in bovine articular chondrocytes. Nitric Oxide. 2002, 6: 35-44. 10.1006/niox.2001.0378.
Fan Z, Bau B, Yang H, Aigner T: IL-1beta induction of IL-6 and LIF in normal articular human chondrocytes involves the ERK, p38 and NFkappaB signaling pathways. Cytokine. 2004, 28: 17-24. 10.1016/j.cyto.2004.06.003.
Fiuza UM, Arias AM: Cell and molecular biology of Notch. J Endocrinol. 2007, 194: 459-474. 10.1677/JOE-07-0242.
Fujimori K, Kadoyama K, Urade Y: Protein kinase C activates human lipocalin-type prostaglandin D synthase gene expression through de-repression of notch-HES signaling and enhancement of AP-2 beta function in brain-derived TE671 cells. J Biol Chem. 2005, 280: 18452-18461. 10.1074/jbc.M411755200.
Kagitani-Shimono K, Mohri I, Oda H, Ozono K, Suzuki K, Urade Y, Taniike M: Lipocalin-type prostaglandin D synthase (beta-trace) is upregulated in the alphaB-crystallin-positive oligodendrocytes and astrocytes in the chronic multiple sclerosis. Neuropathol Appl Neurobiol. 2006, 32: 64-73. 10.1111/j.1365-2990.2005.00690.x.
Hirawa N, Uehara Y, Ikeda T, Gomi T, Hamano K, Totsuka Y, Yamakado M, Takagi M, Eguchi N, Oda H, Seiki K, Nakajima H, Urade Y: Urinary prostaglandin D synthase (beta-trace) excretion increases in the early stage of diabetes mellitus. Nephron. 2001, 87: 321-327. 10.1159/000045937.
Hirawa N, Uehara Y, Yamakado M, Toya Y, Gomi T, Ikeda T, Eguchi Y, Takagi M, Oda H, Seiki K, Urade Y, Umemura S: Lipocalin-type prostaglandin d synthase in essential hypertension. Hypertension. 2002, 39: 449-454. 10.1161/hy0202.102835.
Mohri I, Taniike M, Okazaki I, Kagitani-Shimono K, Aritake K, Kanekiyo T, Yagi T, Takikita S, Kim HS, Urade Y, Suzuki K: Lipocalin-type prostaglandin D synthase is up-regulated in oligodendrocytes in lysosomal storage diseases and binds gangliosides. J Neurochem. 2006, 97: 641-651. 10.1111/j.1471-4159.2006.03753.x.
Pelletier JP, Lascau-Coman V, Jovanovic D, Fernandes JC, Manning P, Connor JR, Currie MG, Martel-Pelletier J: Selective inhibition of inducible nitric oxide synthase in experimental osteoarthritis is associated with reduction in tissue levels of catabolic factors. J Rheumatol. 1999, 26: 2002-2014.
Tetlow LC, Adlam DJ, Woolley DE: Matrix metalloproteinase and proinflammatory cytokine production by chondrocytes of human osteoarthritic cartilage: associations with degenerative changes. Arthritis Rheum. 2001, 44: 585-594. 10.1002/1529-0131(200103)44:3<585::AID-ANR107>3.0.CO;2-C.
Towle CA, Hung HH, Bonassar LJ, Treadwell BV, Mangham DC: Detection of interleukin-1 in the cartilage of patients with osteoarthritis: a possible autocrine/paracrine role in pathogenesis. Osteoarthritis Cartilage. 1997, 5: 293-300. 10.1016/S1063-4584(97)80008-8.
Melchiorri C, Meliconi R, Frizziero L, Silvestri T, Pulsatelli L, Mazzetti I, Borzi RM, Uguccioni M, Facchini A: Enhanced and coordinated in vivo expression of inflammatory cytokines and nitric oxide synthase by chondrocytes from patients with osteoarthritis. Arthritis Rheum. 1998, 41: 2165-2174. 10.1002/1529-0131(199812)41:12<2165::AID-ART11>3.0.CO;2-O.
Moos V, Fickert S, Muller B, Weber U, Sieper J: Immunohistological analysis of cytokine expression in human osteoarthritic and healthy cartilage. J Rheumatol. 1999, 26: 870-879.
Kapoor M, Kojima F, Yang L, Crofford LJ: Sequential induction of pro- and anti-inflammatory prostaglandins and peroxisome proliferators-activated receptor-gamma during normal wound healing: a time course study. Prostaglandins Leukot Essent Fatty Acids. 2007, 76: 103-112. 10.1016/j.plefa.2006.11.006.
Cipollone F, Fazia M, Iezzi A, Ciabattoni G, Pini B, Cuccurullo C, Ucchino S, Spigonardo F, De Luca M, Prontera C, Chiarelli F, Cuccurullo F, Mezzetti A: Balance between PGD synthase and PGE synthase is a major determinant of atherosclerotic plaque instability in humans. Arterioscler Thromb Vasc Biol. 2004, 24: 1259-1265. 10.1161/01.ATV.0000133192.39901.be.
Fournier T, Fadok V, Henson PM: Tumor necrosis factor-alpha inversely regulates prostaglandin D2 and prostaglandin E2 production in murine macrophages. Synergistic action of cyclic AMP on cyclooxygenase-2 expression and prostaglandin E2 synthesis. J Biol Chem. 1997, 272: 31065-31072. 10.1074/jbc.272.49.31065.
Matsumoto H, Naraba H, Murakami M, Kudo I, Yamaki K, Ueno A, Oh-ishi S: Concordant induction of prostaglandin E2 synthase with cyclooxygenase-2 leads to preferred production of prostaglandin E2 over thromboxane and prostaglandin D2 in lipopolysaccharide-stimulated rat peritoneal macrophages. Biochem Biophys Res Commun. 1997, 230: 110-114. 10.1006/bbrc.1996.5894.
Jung SM, Schumacher HR, Kim H, Kim M, Lee SH, Pessler F: Reduction of urate crystal-induced inflammation by root extracts from traditional oriental medicinal plants: elevation of prostaglandin D2 levels. Arthritis Res Ther. 2007, 9: R64-10.1186/ar2222.
Stewart MD, Li J, Wong J: Relationship between histone H3 lysine 9 methylation, transcription repression, and heterochromatin protein 1 recruitment. Mol Cell Biol. 2005, 25: 2525-2538. 10.1128/MCB.25.7.2525-2538.2005.
Kobayashi T, Notoya K, Naito T, Unno S, Nakamura A, Martel-Pelletier J, Pelletier JP: Pioglitazone, a peroxisome proliferator-activated receptor gamma agonist, reduces the progression of experimental osteoarthritis in guinea pigs. Arthritis Rheum. 2005, 52: 479-487. 10.1002/art.20792.
Boileau C, Martel-Pelletier J, Fahmi H, Mineau F, Boily M, Pelletier JP: The peroxisome proliferator-activated receptor gamma agonist pioglitazone reduces the development of cartilage lesions in an experimental dog model of osteoarthritis: in vivo protective effects mediated through the inhibition of key signaling and catabolic pathways. Arthritis Rheum. 2007, 56: 2288-2298. 10.1002/art.22726.
Fujimori K, Fujitani Y, Kadoyama K, Kumanogoh H, Ishikawa K, Urade Y: Regulation of lipocalin-type prostaglandin D synthase gene expression by Hes-1 through E-box and interleukin-1 beta via two NF-kappa B elements in rat leptomeningeal cells. J Biol Chem. 2003, 278: 6018-6026. 10.1074/jbc.M208288200.
Miyagi M, Miwa Y, Takahashi-Yanaga F, Morimoto S, Sasaguri T: Activator protein-1 mediates shear stress-induced prostaglandin d synthase gene expression in vascular endothelial cells. Arterioscler Thromb Vasc Biol. 2005, 25: 970-975. 10.1161/01.ATV.0000159702.68591.0d.
Joo M, Kwon M, Sadikot RT, Kingsley PJ, Marnett LJ, Blackwell TS, Peebles RS, Urade Y, Christman JW: Induction and function of lipocalin prostaglandin D synthase in host immunity. J Immunol. 2007, 179: 2565-2575.
Acknowledgements
This work was supported by the Canadian Institutes of Health Research (CIHR) (grant MOP-84282) and the Fonds de la Recherche du Centre de Recherche du Centre Hospitalier de l'Université de Montréal (CHUM). HF is a Research Scholar of the Fonds de Recherche en Santé du Québec (FRSQ).
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
NZ conceived the study and designed and carried out cell and real-time RT-PCR experiments and some immunohistochemistry experiments. NC contributed to the study design and carried out immunoassays and some cell experiments. XL carried out some cell experiments and data analysis. MB participated in the study design and data analysis. JM-P, J-PP, and ND helped to obtain tissues and participated in the study design and some immunohistochemistry experiments. HF conceived, designed, and coordinated the study, carried out some cell experiments, and drafted the manuscript. All authors read and approved the final manuscript.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Zayed, N., Li, X., Chabane, N. et al. Increased expression of lipocalin-type prostaglandin D2synthase in osteoarthritic cartilage. Arthritis Res Ther 10, R146 (2008). https://doi.org/10.1186/ar2581
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1186/ar2581