Abstract
Background
Rupture of the Achilles tendon is a considerable cause of morbidity with reduced function following injury. Randomized studies have so far failed to show a difference in outcome between operative and nonoperative management of Achilles tendon rupture, provided that no re-rupture occurs. Percutaneous Achilles repair has been suggested to result in superior patient satisfaction compared with open repair in patients with an acute Achilles tendon rupture.
Aim and Objectives
To assess and evaluate the functional outcome after percutaneous repair in patients of the acute and closed Achilles tendon ruptures.
Materials and Methods
It was a prospective study conducted on patients diagnosed as having rupture of the Achilles tendon. A total of 25 patients with mean age of 44.4 (range 19–65) years were taken, who underwent percutaneous Achilles tendon repair.
Results
The number of patients who reported excellent or good scores (ATRS > 80) at 3, 6 and 12 months were 0%, 16% and 100%, respectively. The mean AOFAS hind foot score at 3-, 6- and 12-month follow-ups was 77.9 ± 4.3, 92.04 ± 2.4 and 96.16.32 ± 1.1, respectively. The number of patients who reported excellent or good scores (AOFAS > 74) at 3, 6 and 12 months were 76%, 100% and 100%, respectively. Most of the patients in our study showed no complications, and only 2 (8%) of patients had the features of sural nerve injury which was resolved in the subsequent follow-ups.
Conclusion
Percutaneous repair of the Achilles tendon is an effective procedure which gives excellent functional outcome with very few complications. The percutaneous technique gives an additional advantage of less operative time, no wound complications, less damage to the soft tissues, and improved cosmesis as compared to the open repair.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
The Achilles tendon is a thick band of tissue that attaches calf muscle to heel bone. It is the largest and longest tendon in the body and is built to handle a lot of stress. This thick band of tissue is very strong, which gives leg strength to walk, run and jump.
Achilles tendon rupture is an injury that affects the back of lower leg. An Achilles tendon rupture is a partial or full tear of the Achilles tendon. This sudden injury occurs when the tendon stretches to its breaking point. It mainly occurs in people playing recreational sports, but it can happen to anyone. It happens most frequently while playing sports. Tripping, falling or twisting ankle. Rupture usually occurs in the section of the tendon situated within 2.5 inches (about 6 cm) of the point where it attaches to the heel bone. This section might be prone to rupture because blood flow is poor, which also can impair its ability to heel. The vulnerability and morbidity caused by pathologies of the Achilles tendon was recognized by Hippocrates “The Achilles tendon if bruised or cut causes the most acute fever, induces choking deranges the mind and at length brings death.”
Treatment of a ruptured Achilles tendon often depends on patient age, activity level and the severity. In general, younger and more active people, particularly athletes tend to choose surgery. Open repair surgeries allow for direct confirmation of ruptured Achilles tendon and accurate suturing with tension, thereby reducing the frequency of recurrent ruptures. However, large incisions leading to potential infection, adhesion, and wound-related complications have been highlighted as the drawbacks of open repair surgery [1, 2]. While minimally invasive surgery has shown considerably reduced risk of superficial wound infection and a 3 times greater patient satisfaction rate [3, 4]. Percutaneous repair was described in 1977 by Ma and Griffith with no re-ruptures and only two minor complications. Since then, there have been mixed results in studies where some have shown higher re-rupture rates and sural nerve complications. These have led some authors to develop alternative methods of percutaneous repair [5,6,7,8]. Meanwhile numerous studies reported relatively favorable outcomes from conservative treatment. Although the proportion of favorable outcomes is increasing [1, 9], the possibilities of recurrent rupture and tendon elongation remain [10]. To overcome these limitations, less invasive techniques have been developed. Nonetheless, there have been reported issues of recurrent rupture and sural nerve injuries from these innovative techniques [2, 11,12,13,14]. The aim of this study is to assess the functional outcome in percutaneous Achilles tendon repair.
Materials and Methods
The present study was conducted in the Postgraduate Department of Orthopedics, Government Hospital for Bone and Joint Surgery, an associated Hospital of Government Medical College Srinagar from July 2019 to February 2021. It was a case series conducted on patients diagnosed as having rupture of the Achilles tendon and fulfilling the inclusion criteria for the study. Diagnosis was made via physical examination (presence of a palpable gap within the tendon, the loss of the normal resting tone of the ankle and lack of tendon continuity on performing a calf squeeze test [15].), and ultrasonography (Fig. 1). A total of 25 patients with mean age of 44.4 (range 19–65) years were taken, who underwent percutaneous Achilles tendon repair.
Inclusion criteria:
-
Acute tendon ruptures (duration less than 3 weeks)
-
Closed tendon ruptures.
-
Tendon ruptures occurring within 2–8 cm from the insertion site.
-
Tendon gap less than 2 cm.
-
Compliant patients.
-
All sexes
Exclusion criteria:
-
Chronic tendon ruptures (duration greater than 3 weeks)
-
Open tendon ruptures.
-
Re-rupture after previous repair.
-
Non-compliant patients.
Surgical Technique
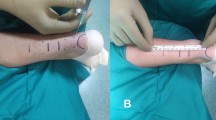
The patients were operated under spinal or regional anesthesia. and all inductions of anesthesia were performed using ultrasound-guided peripheral nerve block (femoral nerve, sciatic nerve, and posterior femoral cutaneous nerve block). The patient was put in prone position with tourniquet before the induction of anesthesia. Injured foot was put in about 25 degrees of plantar flexion. Starting distally first a suture on long straight or semi-curved needle is passed through the tendon followed by a diagonal cross-suture and thread was then led longitudinally, subcutaneously and extratendinously. The next cross through the tendon was done proximally and both thread ends were led extratendinously back through the second and third holes distally and pulled symmetrically back until both ends of the torn Achilles tendon are completely approximated and the defect is no longer palpable. After approximating the torn Achilles tendon ends, the lateral end of the thread was passed medially, the final simultaneous tightening of both ends of thread is done and suture is tied. Hence, the procedure was started and finished medially and distally and the knots were buried subcutaneously in the widened 2nd medial stab incision. This procedure leaves only 8 small stab incisions visible and these incisions were closed with fine silk sutures (Fig. 2). Antiseptic dressing is applied. Foot and ankle were fixed in gravity equinus position using a short leg cast.
A distally semi-curved needle passed through the tendon. B Diagonal cross-suture. C Longitudinally, subcutaneously and extratendinously thread pass. D Proximal cross through tendon. E Distally back of both thread ends through the second and third holes. F No palpable defect. G Medially pass of the lateral end of the thread. H Suture is tied. I Buried knots subcutaneously
Follow-Up
The passive range of motion of the ankle started 3 weeks post-operatively, but partial weight-bearing started after 4 weeks and full weight-bearing by 6 weeks. At 6 weeks post-operatively, patients were advised for straight leg raises, hip and knee exercises. Between 8 and 12 weeks post-operatively, the patients were given transition from cast to shoes with heel lift. Full weight-bearing with heel lift as tolerated was advised for ankle and foot range of motion exercises. After 12 weeks, the patients were allowed to perform jogging and single heel raise motions. Continuity of the tendon was confirmed at 3, 6, and 12 months post-operatively using ultrasonography. In addition, bilateral ankle angles were compared in the neutral position with the patient in the prone position and knee joint bent at 90 to check for potential recurrent rupture or elongation of Achilles tendon. The functional outcomes were assessed using AOFAS (American Orthopaedic Foot and Ankle Society) hindfoot score (1994) and ATRS (Achilles Tendon Total Rupture Score) (2007) (Tables 1, 2).
Results
In our study, 25 patients with Achilles tendon rupture were treated with percutaneous Achilles repair. Mean age of patients was 44.4 years (range 19–65 years). Mean operative time was 23.6(range 15–30) minutes and mean hospital stay was 2.36 (range 2–3) days. The median ATRS results at 3, 6 and 12 month follow-up was 66.16 ± 2.9, 77.84 ± 2.2 and 89.32 ± 2.2, respectively. The number of patients who reported excellent or good scores (ATRS > 80) at 3, 6 and 12 months were 0%, 16% and 100%, respectively. The mean AOFAS hind foot score at 3-, 6- and 12-month follow-ups was 77.9 ± 4.3, 92.04 ± 2.4 and 96.16.32 ± 1.1, respectively. The number of patients who reported excellent or good scores (AOFAS > 74) at 3, 6 and 12 months were 76%, 100% and 100%, respectively. Most of the patients in our study had no complications, and only 2 (8%) of patients had the features of sural nerve injury which was resolved in the subsequent follow-ups (Tables 3, 4).
Discussion
Achilles tendon rupture incidence is increasing and is attributed to increasing recreational sport activities [16, 17]. More than 75% cases are related to sport and athletic activities [16, 18]. In our study, sport activity (38.50%) is the most common mode of injury and occupational injuries (30%) have a significant percentage. Mean age of our study was 44.4 which is comparable to the study done by Carmont et al. 2013 [19] where mean age was 45.5. The majority of the patients in our study were males. The likely cause of more male sex involvement in our study was more involvement of males in heavy occupational and sports-related activities. The male to female ratio in our study was 2.6:1, which is comparable to the study done by Maffulli et al. 2020 [20] where male to female ratio was 2.5:1. Yong Li et al. 2021 [21] did a comparative study in which the mean operative time of the percutaneous group was 23.1 min comparable to our study. The mean operative time in our study was 23.6 min with a range from 15 to 30 min.
The present study shows that the treatment of acute Achilles tendon repair with a percutaneous repair technique delivers good clinical results combined with very low re-rupture and surgical complication rates. The clinical scores were very good in the present study. Since Ma and Griffith [22] have reported percutaneous repair as an eclectic treatment of open repair surgery and conservative treatment, multiple studies have compared this innovative technique with open repair surgery, and there are ongoing studies on different minimally invasive surgery techniques, which are improved versions of these operative techniques. Several previous studies have mentioned that percutaneous repair decreases the prevalence of skin complications and provides a similarly exceptional level of clinical and functional outcomes [23]. Yang et al. [24] suggested that percutaneous repair is better than open repair in operative time, infection, and AOFAS scores.
In our study, mean AOFAS Hindfoot Score improved from 77.9 at 3 months to 96.16 at final follow-up which is near about equivalent to the study by Andrej Cretnik et al. 2005 [2] where mean AOFAS Hindfoot score at 12-month follow-up was 96.1. The mean ATRS Score improved from 66.16 at 3 months to 89.32 at final follow-up equivalent o he study by Carmont et al. 2013 [19] where it was 89 at 12-month follow-up.
However, the sural nerve has varying anatomical pathways, and thus, percutaneous repair will always expose the patient to the risk of sural nerve injury [25]. The possibility of sural nerve injury during percutaneous repair was approximately 15% [14, 26]. In our study, we had complications like sural nerve injury in 2 (8%) of patients, which is likely less as demonstrated in previous studies. To minimize the risk of sural nerve injury, Webb and Bannister [8] described a technique of percutaneous repair using posterior incisions.
The main finding of the present investigation is that patients reported marked limitation of function by 3 months, little limitation of function by 6 months, and a near excellent/good outcome at 6–12 months following surgery. The success of this treatment method is similar in younger and older patients, and the timing of surgery within a week of injury does not appear to influence the results. This method of percutaneous repair of the Achilles tendon rupture is a reliable and reproducible method of restoring good function, with minimal limitation or complications.
Conclusion
Percutaneous repair of the Achilles tendon is an effective procedure which gives excellent functional outcome with very few complications. The percutaneous technique gives an additional advantage of less operative time, no wound complications, less damage to the soft tissues, and improved cosmesis as compared to the open repair. The disadvantages are that it is technically demanding, long learning curve and inherent risk of injury to the Sural nerve due to its blind nature.
References
Khan, R. J., Fick, D., Keogh, A., et al. (2005). Treatment of acute Achilles tendon ruptures: A meta-analysis of randomized, controlled trials. Journal of Bone and Joint Surgery American, 87(10), 2202–2210.
Yang, B., Liu, Y., Kan, S., et al. (2017). Outcomes and complications of percutaneous versus open repair of acute Achilles tendon rupture: A meta-analysis. International Journal of Surgery, 40, 178–186.
Khan, R. J., Fick, D., Keogh, A., Crawford, J., Brammar, T., & Parker, M. (2005). Treatment of acute Achilles tendon ruptures. A meta-analysis of randomized controlled trials. J Journal of Bone and Joint Surgery American, 87, 2202–2210.
McMahon, S. E., Smith, T. O., & Hing, C. B. (2011). A meta-analysis of randomized controlled studies comparing conventional to mini-invasive approaches for repair of Achilles tendon rupture. Foot and Ankle Surgery, 17, 211–217.
Buchgrabber, A., & Passier, H. H. (1997). Percutaneous repair of Achilles Tendon rupture. Immobilization versus functional postoperative treatment. Clinical Orthopaedics and Related Research, 341, 113–122.
Delponte, P., Potier, L., de Poulpiquet, P., & Buisson, P. (1992). Treatment of subcutaneous ruptures of the Achilles tendon by percutaneous tenorraphy. Revue de Chirurgie Orthopedique et Reparatrice, 78, 404–407.
Gorschewsky, O., Vogel, U., Schweizer, A., & van Lear, B. (1999). Percutaneous tenodesis of the Achilles tendon. A nevy surgical method for treatment of acute Achilles tendon rupture through percutaneous tenodesis. Injury, 30(5), 315–321.
Webb, J. W., & Bannister, G. C. (1999). Percutaneous repair of the ruptured tendo Achilles. The Journal of Bone and Joint Surgery British, 81-B(5), 877–880.
Soroceanu, A., Sidhwa, F., Aarabi, S., et al. (2012). Surgical versus nonsurgical treatment of acute Achilles tendon rupture. Journal of Bone and Joint Surgery. American Volume, 94, 2136–2143.
Jacobs, D., Martens, M., Van Audekercke, R., et al. (1978). Comparison of conservative and operative treatment of Achilles tendon rupture. American Journal of Sports Medicine, 6(3), 107–111.
Kim, J.-H., Gwak, H.-C., Lee, C.-R., et al. (2017). A comparative study of surgical treatment result in the ruptured Achilles tendon: Minimal incision percutaneous repair and open repair. Journal of the Korean Orthopaedic Association, 52(3), 249–256.
Sutherland, A., & Maffulli, N. (1999). A modified technique of percutaneous repair of ruptured Achilles tendon. Orthopaedics and Traumatology, 7(4), 288–295.
Assal, M., Jung, M., Stern, R., et al. (2002). Limited open repair of Achilles tendon ruptures: A technique with a new instrument and findings of a prospective multicenter study. Journal of Bone and Joint Surgery. American Volume, 84(2), 161–170.
Wilkins, R., & Bisson, L. J. (2012). Operative versus nonoperative management of acute Achilles tendon ruptures: A quantitative systematic review of randomized controlled trials. American Journal of Sports Medicine, 40(9), 2154–2160.
Maffulli, N. (1998). The clinical diagnosis of subcutaneous tear of the Achilles tendon. A prospective study in 174 patients. The American Journal of Sports Medicine., 26, 266–270.
Leppilahti, J., Puranen, J., & Orava, S. (1996). Incidence of Achilles tendon rupture. Acta Orthopaedica Scandinavica, 67(3), 277–279.
Houshian, S., Tscherning, T., & Riegels-Nielsen, P. (1998). The epidemiology of Achilles tendon rupture in a Danish county. Injury, 29(9), 651–654.
Jozsa, L., Kvist, M., Balint, B. J., et al. (1989). The role of recreational sport activity in Achilles tendon rupture. A clinical, pathoanatomical, and sociological study of 292 cases. The American Journal of Sports Medicine, 17, 338–343.
Carmont, M. R., Silbernagel, K. G., Edge, A., Mei-Dan, O., Karlsson, J., & Maffulli, N. (2013). Functional outcome of percutaneous Achilles repair: Improvements in Achilles Tendon Total Rupture Score during the first year. Orthopaedic Journal of Sports Medicine, 1(1), 2325967113494584.
Maffulli, N., D’Addona, A., Maffulli, G. D., Gougoulias, N., & Oliva, F. (2020). Delayed (14–30 days) percutaneous repair of Achilles tendon ruptures offers equally good results as compared with acute repair. The American Journal of Sports Medicine. https://doi.org/10.1177/0363546520908592
Li, Y., Jiang, Q., Chen, H., Xin, H., He, Q., & Ruan, D. (2021). Comparison of mini-open repair system and percutaneous repair for acute Achilles tendon rupture. BMC Musculoskeletal Disorders, 22, 914.
Ma, G. W., & Griffith, T. G. (1977). Percutaneous repair of acute closed ruptured Achilles tendon: A new technique. Clinical Orthopaedics and Related Research, 128, 247–255.
Sutherland, A., & Maffulli, N. (1999). A modified technique of percutaneous repair of ruptured Achilles tendon. Orthopaedics & Traumatology, 7(4), 288–295.
Cretnik, A., Kosanovic, M., & Smrkolj, V. (2005). Percutaneous versus open repair of the ruptured Achilles tendon: A comparative study. American Journal of Sports Medicine, 33(9), 1369–1379.
Porter, K., Karia, P., Szarko, M., et al. (2014). An anatomical and cadaveric study examining the risk of sural nerve injury in percutaneous Achilles tendon repair using the Achillon device. Foot and Ankle Surgery, 20(2), 90–93.
Klein, W., Lang, D., & Saleh, M. (1991). The use of the Ma-Griffith technique for percutaneous repair of fresh ruptured tendo Achillis. Chirurgia Degli Organi di Movimento, 76(3), 223–228.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Ethical Approval
Manuscript read and approved by all the authors.
Informed consent
Informed consent was obtained from all the participant individuals included in the study after ethical approval by ethics committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bashir, A., Parry, M.A. & Bhat, A.A. Functional Outcome in Percutaneous Achilles Tendon Repair. JOIO 57, 917–922 (2023). https://doi.org/10.1007/s43465-023-00852-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-023-00852-3