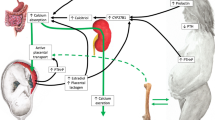
Abstract
Vitamin D and calcium are essential micronutrients for reproductive success. Vitamin D deficiency during pregnancy is associated with increased risk of pregnancy complications including pre-eclampsia and preterm birth (PTB). However, inconsistencies in the literature reflect uncertainties regarding the true biological importance of vitamin D but may be explained by maternal calcium intakes. We aimed to determine whether low dietary consumption of calcium along with vitamin D deficiency had an additive effect on adverse pregnancy outcome by investigating placental morphogenesis and foetal growth in a mouse model. Female mice were randomly assigned to one of four diets: control-fed (+Ca+VD), reduced vitamin D only (+Ca−VD), reduced calcium only (−Ca+VD) and reduced calcium and vitamin D (−Ca−VD), and sacrificed at gestational day (GD) 18.5. Maternal serum 25-hydroxyvitamin D (25(OH)D3) levels were lower in each reduced diet group when compared with levels in +Ca+VD-fed mice. While the pregnancy rate did not differ between groups, in the −Ca−VD-fed group, 55% (5 out of 9 pregnant of known gestational age) gave birth preterm (<GD18.5). Of the −Ca−VD animals that gave birth at GD18.5, mean foetal weight increased by 8% when compared with +Ca+VD (P < 0.05) which was associated with increased placental efficiency (P = 0.05) as a result of changes to the placental labyrinth microstructure. In conclusion, we observed an interactive effect of low calcium and vitamin D intake that may impact offspring phenotype and preterm birth rate supporting the hypothesis that both calcium and vitamin D status are important for a successful pregnancy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pregnancy complications such as pre-eclampsia (PE), foetal growth restriction (FGR) and spontaneous preterm birth (PTB) predict lifelong morbidity and mortality to both mother and infant [1]. The underlying pathophysiology is often associated with placental dysfunction as the placenta is the interface between the foetal and maternal circulations [2]. A number of factors have been identified as necessary to support adequate placental development and function including micronutrients such as vitamin D [3, 4]. Indeed, vitamin D has the ability to regulate placental physiology and there have been a number of mechanistic studies on vitamin D’s actions in the placenta during pregnancy using mouse models [5,6,7,8]. However, classically, vitamin D’s actions have been in maintaining calcium homeostasis and bone mineralisation and the role of calcium in these models has largely been ignored.
The body obtains vitamin D from two sources: diet and UV-B-mediated conversion of 7-dehydrocholesterol in the skin epidermis [9]. From the diet, vitamin D can be obtained in two isoforms: vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol), which differ only in their side-chain structures. D2 is sourced from plants while D3 can be obtained from foods such as fatty fish, some mushroom species and fortified foods [10]. Calcium on the other hand is exclusively obtained through diet. Supplementation for both micronutrients has been recommended for pregnant women as high-dose calcium supplementation and high-dose vitamin D supplementation have been shown to reduce the risk of hypertensive disorders of pregnancy [11]. This is supported by evidence that shows that severe vitamin D deficiency in pregnancy is associated with pregnancy disorders including PE, FGR and PTB [12,13,14].
Vitamin D’s actions in pregnancy, beyond regulating calcium metabolism, include stimulation of the innate immune system, reduction of inflammation and induction of antimicrobial proteins such as cathelicidin [15]. Furthermore, by the third trimester, serum levels of the active vitamin D metabolite 1,25(OH)2D increase as much as twofold when compared with non-pregnant or post-partum highlighting the importance of adequate vitamin D in pregnancy [16,17,18]. This increase is largely driven by placental expression of a number of key genes within the vitamin D metabolic pathway including CYP27B1, which encodes 1α-hydroxylase enzyme [18], and repression of CYP24A1, which encodes 24-hydroxylase which inactivates 1,25(OH)2D [19]. The increase in 1,25(OH)2D is not exclusively caused by the placenta as renal production has also been shown to be influential, as well as hormones such as oestradiol, placental lactogen and prolactin which have stimulatory effects on 1,25(OH)2D production and increase themselves during pregnancy [20].
In mice, dietary vitamin D restriction during pregnancy results in elevated maternal blood pressure, changes to placental morphology and function, increased foetal weight and aberrant foetal neurodevelopment [6, 8, 21]. Less is known about the effects of calcium deficiency in pregnancy, but increased blood pressure in the offspring from mothers fed a low-calcium diet during pregnancy have been reported [22]. In that study, there did appear to be no effect on fertility or foetal growth. Furthermore, the effects of combined vitamin D and calcium deficiency on placental morphogenesis and how this contributes to adverse pregnancy outcomes are largely unknown. We have previously published using the vitamin D receptor (Vdr) knockout mouse model that maternal vitamin D status has a greater role in determining pregnancy outcome than ablated expression of Vdr in the placenta or foetus [7]. Thus, we aimed to investigate the effects of dietary vitamin D and calcium deficiencies on pregnancy and placental development and, in particular, ascertain whether a diet deficient in both calcium and vitamin D has an additive effect compared with a reduction in the diet of just one or the other on adverse pregnancy outcome.
Materials and Methods
Animals
Three-week-old C57Bl/6J female mice (Laboratory Animal Services, University of Adelaide) were fed one of four diets: control (+Ca+VD: 1% Ca, 1000 IU/kg diet vitamin D3, n = 15), vitamin D deficient (+Ca−VD: 1% Ca, 0 IU/kg vitamin D3, n = 15), calcium deficient (−Ca+VD: 0.1% Ca, 1000 IU/kg vitamin D3, n = 14) or calcium and vitamin D deficient (−Ca−VD: 0.1% Ca, 0 IU/kg vitamin D3, n = 14) based on AIN93G [23] from Specialty Feeds (Australia; see SF1). All diet compositions contained the same 16.1 MJ/kg digestible energy. Mice were fed their assigned diet for 10 weeks until mating and then through to sacrifice at gestational day (GD) 18.5. Animals were housed and maintained at Laboratory Animal Services, University of Adelaide, on a 12-h:12-h light-dark cycle. Both food and water were provided ad libitum. At mating, females were placed with a male C57Bl6J fed standard chow (Specialty Feeds) and the presence of a vaginal copulatory plug the following morning designating GD0.5. At sacrifice, maternal serum was collected along with organs including the spleen and kidneys. For the animals in which pregnancy was maintained, the reproductive tract was excised and foetuses and placentas weighed and either fixed for histology or snap frozen in liquid nitrogen for further analyses. This work was dual approved by the University of Adelaide Animal Ethics Committee, the Institute of Medical and Veterinary Sciences and the Central Northern Adelaide Health Service Animal Ethics Committee (Ethics #M-2010-069A) and the SA Pathology/CALHNS Animal Ethics Committee (#86.10) with animal work complying with the Australian Code for Practice for the Care and Use of Animals.
Biochemical Analysis of Calcium and Vitamin D
At GD18.5 serum from the first forty mice sacrificed (n = 10 per diet) were analysed for vitamin D, calcium and phosphorus levels. Whole blood was collected at post-mortem by sub-orbital bleed and serum was obtained by incubation on ice for 1 h to allow clotting and then stored at − 80 °C. Vitamin D3 was measured using a radioimmunoassay kit for 25(OH)D3 (Immuno Diagnostic Systems) following standard manufacturer’s protocol. Total calcium, inorganic phosphorus and albumin were measured using specific detection kits (Calcium reagent: Arsenazo III; Inorganic phosphorus reagent: 2-amino-6-mercapto-7-methylpurine riboside; Albumin reagent: Bromocresol Green method; Fisher Diagnostics, ThermoFisher). Calcium levels were corrected for serum albumin using the standard formula [24] [corrected Ca (mmol/L) = measured total Ca (mmol/L) + 0.02 × (40 − serum albumin (g/L))]. This formula uses the average human albumin level of 40 g/L, which is reported to be similar in C57Bl6 mice [25].
Placental Morphometry
Placental and foetal tissue were collected and the number of total, viable and resorbing implantation sites recorded as previously described [26, 27]. From each pregnant female, two placentas per litter were fixed in 4% (w/v) paraformaldehyde with 2.5% (w/v) polyvinylpyrrolidone in 70 mM phosphate buffer. Five-micrometre-thick, mid-sagittal full-faced sections were stained by Masson’s Trichrome in order to characterise the labyrinth and junctional zone areas of the placenta. Placenta sections were also labelled using immunohistochemistry (IHC) in order to characterise the labyrinthine densities of foetal capillaries, maternal blood space and trophoblast as previously described [7, 26, 27]. Briefly, sections were double immunolabelled with mouse anti-vimentin (Vim3B4, Dako; diluted 1 in 10) and mouse anti-cytokeratin (AE1/AE3, Merk Millipore; diluted 1 in 100) with the aid of a Mouse on Mouse IHC Kit (Abcam) to eliminate non-specific staining. All sections were photographed with a NanoZoomer Digital Pathology scanner (Model C9600 v1.2, Hamamatsu Photonics K.K.) and analysed with NDP Scan software (v2.2, Hamamatsu Photonics K.K.). Analysis occurred by randomly choosing a starting field and systematically choosing 10 adjacent fields 500-μm apart and counting with an isotropic L-36 Merz grid. Error rate was calculated by counting one placenta 5 times and was less than 5%.
RNA Extraction and qPCR Analysis of Gene Expression in the Placentas, and Maternal Spleens and Kidneys
RNA from maternal kidney, spleen and bisected placentas was extracted with TRIzol (Invitrogen, Life Technologies) as per manufacturer’s instructions. Briefly, tissue was homogenised in TRIzol by Powerlyser (MoBio) with ceramic beads (CK14, Geneworks). Rigorous DNase treatment was performed using a TURBO DNase kit (Ambion, Life Technologies). RNA integrity was assessed by Experion (BioRad) and RNA with an RQI of > 4 determined acceptable for real-time PCR. Five hundred nanograms of DNase treated RNA was reverse transcribed using iScript cDNA synthesis kit (BioRad) as per the manufacturer’s instructions. Expression of genes associated with vitamin D metabolism was analysed in both kidney and placenta tissue by TaqMan® Gene Expression Assays (Applied Biosystems, Life Technologies). These were Cyp2r1 (Mm00616774_g1), Cyp27b1 (Mm01165918_g1), Cyp24a1 (Mm00487244_m1) and Vdr (Mm00437297_m1). Reference genes were Gusb (Mm06003537_s1), Hmbs (Mm01143545_m1), Gapdh (Mm99999915_g1) and Hprt1 (Mm00446968_m1). Real-time quantitative PCR was set up using a QIAgility (QIAGEN) liquid handling robot and run on a CFX-384 Real-Time PCR machine (BioRad). Ten-microlitre PCR reactions were run containing 5 μL TaqMan® Gene Expression Master Mix (Applied Biosystems, Life Technologies), 0.5 μL TaqMan® Gene Expression Assay, with 2 μL of diluted cDNA. Cycling conditions were 95 °C for 10 min, 40 cycles of 95 °C for 15 s and 60 °C for 1 min. Additionally, in kidneys from control-fed and double-deficient dams, expression of 64 genes related to blood pressure control was analysed using the PrimePCR™ Pre-eclampsia Tier 1 M384 plates (cat. # 10039501, BioRad) (n = 5 +Ca+VD, n = 5 −Ca−VD no PTB and n = 4 −Ca−VD PTB). Immune function was also analysed in these mice by measuring maternal spleen gene expression of 84 genes using the PrimePCR™ Immune Tier 1 M384 plates (cat. # 10029798, BioRad) (n = 6 +Ca+VD, n = 3 −Ca−VD no PTB and n = 5 −Ca−VD PTB). Briefly, 1 μg of RNA was reverse transcribed using the iScript Advanced cDNA Synthesis Kit for RT-QPCR (BioRad) as per manufacturer’s instructions. Real-time quantitative PCR was set up using a QIAgility (QIAGEN) liquid handling robot and run using the iTaq Universal SYBR Supermix (BioRad) with cycling as per manufacturer’s instructions (30-s denaturation at 95 °C, with 40 cycles of 95 °C for 5 s and 60 °C for 15 s) on a CFX-384 Real-Time PCR machine (BioRad). Reference gene suitability was analysed by GeNorm (qBasePlus v2, Biogazelle). For kidney qPCR analysis of vitamin D metabolism genes, a combination of Hmbs and Hprt1 was optimal (M = 0.22, V < 0.1), whereas for placentas, Gapdh and Hmbs were optimal (M = 0.31, V < 0.1). For PCR array plates, kidney was normalised to Hmbs and Hprt1 and for spleen Tbp and Gapdh.
Statistics
All statistical analyses were performed in R (v3.1.1) [28] using Dunn’s test with Benjamini-Hochberg post hoc analysis unless otherwise specified. Foetal, placental and maternal organ weights were corrected for viable litter size using the lme function in the nlme package to generate predicted values based on an average litter size of 7.2. Exact p values were then calculated based on the predicted results. For spleen and kidney gene expression analyses, differential expression between the diet groups was determined using a Mann-Whitney U test and multiple testing corrected by adjusting the p value using the Benjamini-Hochberg method. Results are reported as median ± interquartile range unless otherwise stated and not separated by foetal sex.
Results
Effects of Diets on Serum 25OHD3 and Calcium
Serum calcium and 25OHD3 were measured in samples collected at post-mortem in order to determine the impact the diets had on 25OHD3 or calcium levels in maternal serum. Regardless of whether the animals were pregnant or not, serum 25OHD3 was higher in the control-fed animals compared with all other diets (Fig. 1a). Serum calcium on the other hand did not differ between the diets nor did serum calcium corrected for serum albumin (Fig. 1b and c). Food consumption during the 10-week dietary conditioning period did not differ between the diets indicating that the differences in serum 25OHD3 was not due to anorexia (mean (SD): +Ca+VD = 2.81 (0.08) vs. +Ca−VD = 2.87 (0.21) vs. −Ca+VD = 2.83 (0.10) vs. −Ca−VD = 2.79 (0.02) g/mouse/day, P > 0.05). Focusing on only those animals pregnant at post-mortems, there was no difference in circulating 25OHD3, calcium or corrected calcium (Fig. 1d–f).
Serum measures of 25-hydroxy vitamin D3 (25(OH)D3), calcium and calcium corrected for serum albumin in non-pregnant (black/grey squares) and pregnant (red dots) mice at GD18.5. Compared with control-fed (+Ca+VD) animals, serum 25(OH)D was reduced in the mice fed a reduced vitamin D only diet (+Ca−VD), reduced calcium only diet (−Ca+VD) and reduced vitamin D and calcium diet (−Ca−VD) (a). There was no difference in serum calcium between the animals fed different diets (b) nor after correcting for serum albumin (c). Analysis of only pregnant animals showed no difference in serum measures of 25(OH)D (d), calcium (e) or calcium corrected for albumin (f) in any of the diet groups. Data are median and interquartile range (n = 10 +Ca+VD and −Ca+VD, 9 +Ca−VD and 8 −Ca−VD). Statistical significance was determined using Dunn’s test and Benjamini-Hochberg multiple test adjustment
Effects of Calcium and Vitamin D on Pregnancy Outcome
Global pregnancy rate at GD18.5 was 62% (36 out of 58 mice) and did not differ between diet groups (n (%): +Ca+VD = 11 (73) vs. +Ca−VD = 7 (47) vs. −Ca+VD = 8 (57) vs. −Ca−VD = 10 (71), P = 0.394). However, 55% (5 out of 9 pregnant of known gestational age) of the mice fed the −Ca−VD diet gave birth preterm (ranging from GD15.5-GD18.5). This was only observed in the mice fed this diet. There was no difference in the number of viable foetuses or resorptions per litter between the dietary groups (mean (SD): +Ca+VD = 6.0 (3.5) vs. +Ca−VD = 6.6 (2.0) vs. −Ca+VD = 6.3 (2.4) vs. −Ca−VD = 6.1 (2.9) viable foetuses, P > 0.05 and +Ca+VD = 0.9 (1.4) vs. +Ca−VD = 1.0 (0.8) vs. −Ca+VD = 1.3 (1.1) vs. −Ca−VD = 0.6 (0.9) resorptions, P > 0.05). There was also no difference in maternal carcass weight (maternal weight minus foetus and placenta weight) between the dietary groups (mean (SD): +Ca+VD = 25.1 (0.60) vs. +Ca−VD = 26.35 (0.74) vs. −Ca+VD = 25.9 (0.60) vs. −Ca−VD = 25.9 (0.60) g, P > 0.05). Compared with the control-fed animals, foetal weight was 8% higher in the double-deficient mice (Fig. 2a; P = 0.023). Placental weight on the other hand did not differ between the −Ca−VD mice and the control mice (Fig. 2b) resulting in an increased foetal-placental weight ratio indicating greater placental efficiency in those animals that did not give birth preterm (Fig. 2c). Placental efficiency was also higher in the double-deficient animals compared with the +Ca−VD and the −Ca+VD animals (Fig. 2c).
Reproductive outcome, measured at GD18.5 in animals fed calcium and/or vitamin D-deficient diets. Foetal weight at GD18.5 was higher in the animals fed a reduced calcium and vitamin D (−Ca−VD) diet when compared with control fed (+Ca+VD) and reduced vitamin D only (+Ca−VD) diet (a). Placental weight was higher in the animals fed a reduced calcium only (−Ca+VD) diet when compared with control fed (b). Increased placental efficiency, as determined by the foetal-placental weight ratio was found in the −Ca−VD animals when compared with all other diet groups (c). Data are median and interquartile range (n = 7 +Ca+VD, −Ca+VD and +Ca−VD and 4 −Ca−VD). Statistical significance was determined using Dunn’s test and Benjamini-Hochberg multiple test adjustment based on an average litter size of 7.2
Effects of Diets on Aspects of Vitamin D Metabolite Gene Expression in the Placenta and Kidneys
In order to elucidate the effect of the different diets on vitamin D metabolism, several vitamin D metabolite genes were measured in placenta and maternal kidney at GD18.5. Placental expression of Cyp24a1, which encodes the protein responsible for degrading the active vitamin D metabolite, was 2.6-fold higher in tissue collected from the −Ca+VD-fed animals when compared with the control-fed animals (Fig. 3a; P = 0.027). Expression of Cyp24a1 was also marginally higher in the placentas from the double-deficient animals when compared with control-fed animals (P = 0.066) and indicated potentially reduced bioavailability of active vitamin D in the placentas of the animals fed a calcium-deficient diet. However, there was no difference in placental expression of Vdr, Cyp27b1 and Cyp2r1 between any of the diet groups (data not shown). In contrast, kidney expression of Cyp27b1 was higher in the −Ca+VD and the −Ca−VD-fed animals compared with the control-fed animals (Fig. 3b; P = 0.008 and P = 0.018, respectively). This included a 3.2-fold increased expression in the kidneys of the double-deficient animals that gave birth preterm (P = 0.006). Vdr was also differentially expressed in the kidneys between the different diets (Fig. 3c) while Cyp2r1 and Cyp24a1 did not change (data not shown).
Placental and maternal kidney gene expression of vitamin D metabolite genes in pregnant animals at GD18.5. Placental expression of Cyp24a1 was higher in animals fed the reduced calcium only (−Ca+VD) diet and marginally higher in the reduced calcium and vitamin D-fed (−Ca−VD) mice when compared with control-fed (+Ca+VD) animals (a). Kidney expression of Cyp27b1 was higher in the animals on the reduced calcium diets as well as in animals fed the reduced calcium and vitamin D diets that gave birth preterm (−Ca−VDPTB) when compared with control-fed animals (b). Differential expression of the Vdr gene in kidney tissue was observed between the different diet groups including in animals fed a reduced vitamin D only (+Ca−VD) diet (c). Data are median and interquartile range (n = 7 +Ca+VD, −Ca+VD and +Ca−VD, 4 −Ca−VD and 5 −Ca−VDPTB). Statistical significance was determined using Mann-Whitney U test and Benjamini-Hochberg multiple test adjustment
Effects of Calcium and Vitamin D on Placental Morphometry
Placental efficiency was greater in the mice fed the double-deficient diet that did not deliver preterm. Therefore, we examined placental morphology at GD18.5 in order to elucidate whether changes to the placental microstructure may contribute to an increase in foetal growth in these dams. Compared with control-fed mice, the junctional zone area or region of the placenta containing the glycogen and hormone producing cells was 24% greater in the double-deficient animals (Fig. 4a; P = 0.051). In contrast, the labyrinth zone area or region, where nutrient and waste transfer between maternal and foetal circulations occurs, was not different in the placentas from any of the diet groups (Fig. 4b). This resulted in a decrease in the placental labyrinth zone area to junctional zone area ratio in the animals fed the double-deficient diet compared with the control-fed mice (Fig. 4c; P = 0.013) and implied a disproportionate shift in the placental architecture. Further analysis using immunohistochemistry to quantify the three main compartments of the labyrinth zone, maternal blood space (MBS: maternal circulation), the foetal capillaries (FC: foetal circulation) and the trophoblasts which coordinate nutrient and waste exchange and act as a barrier between the FC and MBS, revealed a 27% increase in the volume density of the MBS within the placentas from the double-deficient animals when compared with the placentas from the control-fed animal (Fig. 4d; P = 0.010). A 44% increase in MBS volume density was also observed in the placentas from the calcium-deficient only diet animals when compared with the control fed (Fig. 4d; P = 0.009). No changes in the proportion of FC or trophoblasts were observed in the placentas between any of the diet groups (Fig. 4e and f). However, trophoblast barrier thickness was reduced in the placentas from the calcium-deficient only animals and a marginal decrease in trophoblast barrier thickness was observed in the placentas from the double-deficient animals when compared with the control-fed animals (Fig. 4g; P = 0.047 and P = 0.062). Altogether, this suggested that nutrient exchange within the labyrinth zone is less impeded and supports an increased placental efficiency and increased foetal growth in the animals fed the calcium-deficient diets.
Effects of dietary calcium and/or vitamin D restriction on placental morphology and microstructure. An increase in the mid-sagittal cross-sectional area of the junctional zone was observed in the placentas from animals fed a reduced calcium and vitamin D (−Ca−VD) diet when compared with placentas from control-fed (+Ca+VD) animals (a). There was no difference in the mid-sagittal cross-sectional area of the placental labyrinth zone between any of the diet groups (b). Labyrinth zone (LZ) to junctional zone (JZ) area ratio was reduced in the placentas from the −Ca−VD animals compared with control-fed and reduced calcium only (−Ca+VD) animals (c). Maternal blood space (MBS) volume density within the placental labyrinth zone was greater in the tissue collected from the −Ca+VD and −Ca−VD animals compared with control-fed animals (d) although there was no difference in the volume density of the foetal capillaries (e) or trophoblasts (f). Trophoblast barrier thickness (BT) was also reduced in the placental labyrinth of tissue collected from animals on a reduced calcium diet but not from those on a reduced vitamin D only (+Ca−VD) diet when compared with control fed (g). Data are median and interquartile range (n = 7 +Ca+VD, −Ca+VD and +Ca−VD and 4 −Ca−VD). Statistical significance was determined using Dunn’s test and Benjamini-Hochberg multiple test adjustment based on an average litter size of 7.2
Effects of Calcium and Vitamin D on Immunological Parameters
Given that half of the mice fed the double-deficient diet delivered preterm, we sought to investigate the role of the immune system as vitamin D has been shown to influence immunological function (reviewed in [29]). Spleen weight as a percentage of carcass weight (maternal weight at GD18.5 minus foetal and placental weight) was between 2.4- and 3.4-fold higher in the mice that were fed the −Ca−VD diet that gave birth preterm compared with all other diet groups (Fig. 5a) indicating a clear involvement of the immune system likely driven by the delivery and labour. To further investigate this, we performed qPCR gene expression analyses of 84 genes involved in immune function in the spleen of double-deficient and control-fed animals. There were only two differentially expressed genes: Mapk3 and Il15 in the spleens of the −Ca−VD animals that did not give birth preterm when compared with control-fed animals (Fig. 6a and b). In the −Ca−VD animals that did give birth preterm, these two genes, along with 52 other genes, were downregulated when compared with the control-fed animals; 37 of these were also downregulated when compared with the −Ca−VD-fed animals that did not give birth preterm (Supplementary Table 1). Most of the genes that were downregulated including Mapk3 and IL15 feature in the toll-like receptor signalling pathway indicating a downregulation of pro-inflammatory effects and T cell stimulation most likely caused by parturition.
Spleen and kidney weight at GD18.5 in animals fed reduced calcium and/or vitamin D diets. Spleen weight as a percentage of carcass weight (maternal weight minus foetus and placenta weights) was higher in the mice fed a reduced calcium and vitamin D diet that delivered preterm (−Ca−VD PTB) when compared with all other diet groups (a). Kidney weight as a percentage of carcass weight was marginally higher in the −Ca−VD PTB animals when compared with control fed (+Ca+VD) and reduced calcium and vitamin D diet group that did not give birth preterm (−Ca−VD) (b). Data are median and interquartile range (n = 7 +Ca+VD, −Ca+VD and +Ca−VD, 4 −Ca−VD and 5 −Ca−VD PTB). Statistical significance was determined using Dunn’s test and Benjamini-Hochberg multiple test adjustment based on an average litter size of 7.2. +Ca−VD: reduced vitamin D only diet; −Ca+VD: reduced calcium only diet
Expression of genes relating to immune function in the spleens of mice at GD18.5. Spleen expression of Mapk3 was higher in the animals that were fed a reduced calcium and vitamin D diet that did not give birth preterm (−Ca−VD) compared with control-fed (+Ca+VD) and those fed a reduced calcium and vitamin D diet that did give birth preterm (−Ca−VD PTB) (a). Mapk3 expression was also lower in the −Ca−VD PTB animals when compared with control-fed animals. Expression of Il15 in the spleen was lowest in the animals fed a reduced calcium and vitamin D diet that delivered preterm and highest in the control-fed animals (b). Data are median and interquartile range (n = 6 +Ca+VD, 3 −Ca−VD and 5 −Ca−VD PTB). Statistical significance was determined using Dunn’s test and Benjamini-Hochberg multiple test adjustment
Effects of Calcium and Vitamin D on Renal Gene Expression
Adequate placental blood flow is critical in maintaining foetal growth and maternal cardiovascular adaptations to pregnancy are necessary to maintain appropriate perfusion of the placenta [30]. We therefore sought to analyse the expression of 61 genes related to blood pressure control in kidney tissue from −Ca−VD animals and control-fed animals. Total kidney weight as a percentage of carcass weight was moderately higher in the −Ca−VD animals that gave birth preterm when compared with both the control- and −Ca−VD-fed animals that did not give birth preterm (Fig. 5b). In the kidneys of the animals that were fed a reduced calcium and vitamin D diet that did not give birth preterm, there was a 42% reduction in the expression of Nfkbia (P = 0.008) and a 29% increase in the expression of Aldh3a2 (P = 0.032) when compared with control-fed animals (Supplementary Table 2). There were 5 genes found to be differentially expressed in kidneys of the −Ca−VD−fed animals that gave birth preterm when compared with control fed including Cbx7 and Gnai3 and 3 genes differentially expressed in the kidneys of the animals that were fed a reduced calcium and vitamin D diet that did and did not give birth preterm (Supplementary Table 2).
Discussion
It has been known for some time that calcium and vitamin D are integral in supporting a healthy pregnancy. However, this study is one of the first to show that a diet deficient in both results in preterm delivery and that adequate consumption of both micronutrients is integral in supporting appropriate foetal growth. Underlying this relationship is the contribution of the placenta in which structure and function appear to be altered in dams fed a double-deficient diet and hence contributes valuable knowledge about the shared importance of calcium and vitamin D in pregnancy.
Although fertility is reduced in Vdr knockout mice and rescued by calcium [31], there was no evidence of reduced fertility in our model of reduced dietary vitamin D and calcium intake. This is consistent with findings from other studies that have examined dietary vitamin D restriction [8, 21] and may be due to the relatively mild phenotype induced by the vitamin D-deficient diets, as pregnant mice had mild 25(OH)D3 deficiency (range 14–26 nmol/L). However, over 50% of the mice fed the double-deficient diet gave birth preterm which if translated to women has important implications for human health. Maternal vitamin D deficiency has been associated with increasing the risk of PTB in some human populations [32,33,34,35,36] and could be related to low calcium intakes. However, not all of the mice fed the double-deficient diet delivered preterm and, in these mice, foetal weight near term was higher and placental efficiency increased highlighting the multifaceted nature of how vitamin D and calcium support pregnancy.
Increased foetal weight due to vitamin D deficiency has previously been observed with no associated increase in placental weight [8], a surrogate for increased placental efficiency. Placental efficiency has previously been reported to increase due to mild insults, such as moderate alteration of nutrients [37]. Within this model, although the diet compositions were extremely deficient in vitamin D and/or calcium, this did not translate to severely low levels in the circulation. For serum calcium, this is not unsurprising as circulating calcium is tightly controlled and never radically changed due to the strength of the feedback mechanisms. However, a modest reduction in serum 25OHD3 was seen in the deficient animals compared with the control-fed counterparts. Furthermore, changes to the labyrinth zone microstructure within the placentas from the mice fed the double-deficient diet are consistent with enhanced nutrient transfer. Increased MBS volume density represents a greater area in which maternal blood can flow and potentially increased placental perfusion in conjunction with increased maternal blood pressure. Furthermore, along with reduced thickness of the trophoblast layer which lies between the MBS and FC, these results suggest an increased opportunity for nutrient exchange and hence increased foetal growth. Increased placental efficiency is observed in rodent models of undernutrition, particularly during the foetal growth spurt between GD15-16 [37]. This may be due to morphological adaptations of the placenta or changes in the expression of nutrient transporter systems and is highly dependent on placental size [38]. Additionally, foetal derived factors may signal to the placenta nutrient insufficiencies and alter placental nutrient delivery [39]. Thus, in this model, it is possible that the placentas and/or foetuses from those on the double-deficient diets responded to the nutrient deprivation to either increase placental efficiency and possibly nutrient transport resulting in prolonging pregnancy to term or delivery preterm. This hypothesis requires further investigation including measuring maternal blood pressure changes throughout pregnancy as placental perfusion is strongly associated with maternal blood pressure.
Given that maternal cardiovascular adaptations to pregnancy and placental function are closely inter-related, we analysed 61 genes relating to blood pressure control in kidney tissue in order to elucidate whether aberrant blood pressure control may mediate pregnancy outcome in the mice fed the double-deficient diet. Vitamin D-deficient diets in mice result in increased blood pressure [8] and human epidemiological studies have shown increased blood pressure in those suffering from vitamin D deficiency [40, 41]. Furthermore, calcium influx into vascular smooth muscle cells augments vascular tone and blood pressure [42]. In terms of vitamin D, it plays a supportive role in regulating blood pressure through the renin-angiotensin system (RAS) which functions to increase blood pressure through the production of the potent vasoconstrictor angiotensin II [43]. We did not find evidence to suggest that the animals fed the −Ca−VD diets had alterations to the expression of components of this system or that there were significant changes in renal expression of key genes relating to blood pressure regulation. However, RAS actions are mediated by enzyme activity and receptor sensitivity such that gene expression may not reflect blood pressure changes and thus does not rule out the possibility for there to be changes to maternal blood pressure worth further investigation.
Another possible contributor to why reproductive outcome in the mice fed a double-deficient diet was altered is in the regulation of the immune system. Analysis of gene expression in the spleen of the animals that delivered preterm indicated a downregulation of the toll-like receptor signalling pathway and includes Mapk3 and IL15. This is surprising as preterm birth is often considered a result of increased inflammation [44]. During pregnancy, aspects of the adaptive immune system are suppressed in order to maintain the semi-allogeneic foetus [45]. However, this is not the case for the innate immune system, which is stimulated in order to reduce susceptibility of the foetus and mother to infection (reviewed in [46]). A decrease in the expression of genes relating to the toll-like receptor signalling pathway would indicate a downregulation of innate immune responses in the mice that delivered preterm. This may be a direct result of parturition in these animals or indicate that the reduced dietary calcium and vitamin D intake has resulted in augmented innate immunity in pregnancy and as a consequence, increased the chances of preterm delivery. Further investigations are required but this does provide the basis for increased examination of the role of calcium and vitamin D in immune regulation and the consequences on gestation length.
In conclusion, this study describes the effects of reduced dietary vitamin D and calcium intakes on placental development and foetal growth, as well as aspects of the maternal immune system and blood pressure regulation. The work implicates potential physiological responses by which inadequate vitamin D and calcium intake from before during pregnancy may impact offspring phenotype and result in preterm birth. Our findings emphasise the need to examine the contribution of both calcium and vitamin D in pregnancy and thus assist in better understanding the importance of vitamin D metabolism in pregnancy. Perhaps the disparate published findings on the association of vitamin D deficiency with PTB and other pregnancy complications may be due to differences in the calcium status of women in the different study populations.
References
Roberts CT. IFPA award in placentology lecture: complicated interactions between genes and the environment in placentation, pregnancy outcome and long term health. Placenta. 2010;31(Suppl):S47–53.
Cross JC. Formation of the placenta and extraembryonic membranes. Ann N Y Acad Sci. 1998;857:23–32.
Evans KN, Bulmer JN, Kilby MD, Hewison M. Vitamin D and placental-decidual function. J Soc Gynecol Investig. 2004;11(5):263–71.
Wagner CL, Hollis BW. The implications of vitamin D status during pregnancy on mother and her developing child. Front Endocrinol (Lausanne). 2018;9:500.
Shahbazi M, Jeddi-Tehrani M, Zareie M, Salek-Moghaddam A, Akhondi MM, Bahmanpoor M, et al. Expression profiling of vitamin D receptor in placenta, decidua and ovary of pregnant mice. Placenta. 2011;32(9):657–64.
Tesic D, Hawes JE, Zosky GR, Wyrwoll CS. Vitamin D deficiency in BALB/c mouse pregnancy increases placental transfer of glucocorticoids. Endocrinology. 2015;156(10):3673–9.
Wilson RL, Buckberry S, Spronk F, Laurence JA, Leemaqz S, O’Leary S, et al. Vitamin D receptor gene ablation in the conceptus has limited effects on placental morphology, function and pregnancy outcome. PLoS One. 2015;10(6):e0131287.
Liu NQ, Ouyang Y, Bulut Y, Lagishetty V, Chan SY, Hollis BW, et al. Dietary vitamin D restriction in pregnant female mice is associated with maternal hypertension and altered placental and fetal development. Endocrinology. 2013;154(7):2270–80.
Lehmann B. The vitamin D3 pathway in human skin and its role for regulation of biological processes. Photochem Photobiol. 2005;81(6):1246–51.
Holick MF. Vitamin D: a D-Lightful health perspective. Nutr Rev. 2008;66(10 Suppl 2):S182–94.
Hollis BW, Wagner CL. Vitamin D and pregnancy: skeletal effects, nonskeletal effects, and birth outcomes. Calcif Tissue Int. 2013;92(2):128–39.
Lerchbaum E, Obermayer-Pietsch B. Vitamin D and fertility: a systematic review. European journal of endocrinology / European Federation of Endocrine Societies. 2012;166(5):765–78.
Aghajafari F, Nagulesapillai T, Ronksley PE, Tough SC, O’Beirne M, Rabi DM. Association between maternal serum 25-hydroxyvitamin D level and pregnancy and neonatal outcomes: systematic review and meta-analysis of observational studies. BMJ (Clinical research ed). 2013;346:f1169.
Wei SQ, Qi HP, Luo ZC, Fraser WD. Maternal vitamin D status and adverse pregnancy outcomes: a systematic review and meta-analysis. The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2013;26(9):889–99.
Liu NQ, Hewison M. Vitamin D, the placenta and pregnancy. Arch Biochem Biophys. 2012;523(1):37–47.
Kumar R, Cohen WR, Silva P, Epstein FH. Elevated 1,25-dihydroxyvitamin D plasma levels in normal human pregnancy and lactation. J Clin Invest. 1979;63(2):342–4.
Hollis BW, Johnson D, Hulsey TC, Ebeling M, Wagner CL. Vitamin D supplementation during pregnancy: double-blind, randomized clinical trial of safety and effectiveness. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. 2011;26(10):2341–57.
Weisman Y, Harell A, Edelstein S, David M, Spirer Z, Golander A. 1 alpha, 25-dihydroxyvitamin D3 and 24,25-dihydroxyvitamin D3 in vitro synthesis by human decidua and placenta. Nature. 1979;281(5729):317–9.
Novakovic B, Sibson M, Ng HK, Manuelpillai U, Rakyan V, Down T, et al. Placenta-specific methylation of the vitamin D 24-hydroxylase gene: implications for feedback autoregulation of active vitamin D levels at the fetomaternal interface. J Biol Chem. 2009;284(22):14838–48.
Kovacs CS. Maternal mineral and bone metabolism during pregnancy, lactation, and post-weaning recovery. Physiol Rev. 2016;96(2):449–547.
Hawes JE, Tesic D, Whitehouse AJ, Zosky GR, Smith JT, Wyrwoll CS. Maternal vitamin D deficiency alters fetal brain development in the BALB/c mouse. Behav Brain Res. 2015;286:192–200.
Bergel E, Belizan JM. A deficient maternal calcium intake during pregnancy increases blood pressure of the offspring in adult rats. BJOG. 2002;109(5):540–5.
Reeves PG, Nielsen FH, Fahey GC Jr. AIN-93 purified diets for laboratory rodents: final report of the American Institute of Nutrition ad hoc writing committee on the reformulation of the AIN-76A rodent diet. J Nutr. 1993;123(11):1939–51.
Goldstein DA. Serum Calcium. In: Walker HK, Hall WD, Hurst JW, editors. Clinical methods: the history, physical and laboratory examinations. Boston: Butterworths; 1990. p. 677–9.
Quimby FW, Luong RH. Clinical chemistry of the laboratory mouse. In: Fox JG, Barthold SW, Davisson MT, Newcomer CE, Quimby FW, Smith AL, eds. The mouse in biomedical research. Vol 3. 2nd ed. MA, USA: Elsevier; 2007:181.
Roberts CT, White CA, Wiemer NG, Ramsay A, Robertson SA. Altered placental development in interleukin-10 null mutant mice. Placenta. 2003;24(Suppl A):S94–9.
Wilson RL, Leemaqz SY, Goh Z, McAninch D, Jankovic-Karasoulos T, Leghi GE, et al. Zinc is a critical regulator of placental morphogenesis and maternal hemodynamics during pregnancy in mice. Sci Rep. 2017;7(1):15137.
R: A Language and Environment for Statistical Computing [computer program]. Vienna, Austria: R Foundation for Statistical Computing; 2011.
Prietl B, Treiber G, Pieber TR, Amrein K. Vitamin D and immune function. Nutrients. 2013;5(7):2502–21.
Reynolds LP, Caton JS, Redmer DA, Grazul-Bilska AT, Vonnahme KA, Borowicz PP, et al. Evidence for altered placental blood flow and vascularity in compromised pregnancies. J Physiol. 2006;572(Pt 1):51–8.
Johnson LE, DeLuca HF. Vitamin D receptor null mutant mice fed high levels of calcium are fertile. J Nutr. 2001;131(6):1787–91.
Baker AM, Haeri S, Camargo CA Jr, Stuebe AM, Boggess KA. A nested case-control study of first-trimester maternal vitamin D status and risk for spontaneous preterm birth. Am J Perinatol. 2011;28(9):667–72.
Shand AW, Nassar N, Von Dadelszen P, Innis SM, Green TJ. Maternal vitamin D status in pregnancy and adverse pregnancy outcomes in a group at high risk for pre-eclampsia. BJOG. 2010;117(13):1593–8.
Dunlop AL, Taylor RN, Tangpricha V, Fortunato S, Menon R. Maternal micronutrient status and preterm versus term birth for black and white US women. Reprod Sci. 2012;19(9):939–48.
Fernandez-Alonso AM, Dionis-Sanchez EC, Chedraui P, et al. First-trimester maternal serum 25-hydroxyvitamin D(3) status and pregnancy outcome. Int J Gynaecol Obstet. 2012;116(1):6–9.
Perez-Ferre N, Torrejon MJ, Fuentes M, Fernandez MD, Ramos A, Bordiu E, et al. Association of low serum 25-hydroxyvitamin D levels in pregnancy with glucose homeostasis and obstetric and newborn outcomes. Endocr Pract. 2012;18(5):676–84.
Fowden AL, Sferruzzi-Perri AN, Coan PM, Constancia M, Burton GJ. Placental efficiency and adaptation: endocrine regulation. J Physiol. 2009;587(Pt 14):3459–72.
Coan PM, Vaughan OR, Sekita Y, Finn SL, Burton GJ, Constancia M, et al. Adaptations in placental phenotype support fetal growth during undernutrition of pregnant mice. J Physiol. 2010;588(Pt 3):527–38.
Constancia M, Angiolini E, Sandovici I, et al. Adaptation of nutrient supply to fetal demand in the mouse involves interaction between the Igf2 gene and placental transporter systems. Proc Natl Acad Sci U S A. 2005;102(52):19219–24.
Anderson JL, May HT, Horne BD, Bair TL, Hall NL, Carlquist JF, et al. Relation of vitamin D deficiency to cardiovascular risk factors, disease status, and incident events in a general healthcare population. Am J Cardiol. 2010;106(7):963–8.
Forman JP, Giovannucci E, Holmes MD, Bischoff-Ferrari HA, Tworoger SS, Willett WC, et al. Plasma 25-hydroxyvitamin D levels and risk of incident hypertension. Hypertension. 2007;49(5):1063–9.
Dora KA, Doyle MP, Duling BR. Elevation of intracellular calcium in smooth muscle causes endothelial cell generation of NO in arterioles. Proc Natl Acad Sci U S A. 1997;94(12):6529–34.
Vallotton M. The renin-angiotensin system. Trends Pharmacol Sci. 1987;8(2):69–74.
Romero R, Dey SK, Fisher SJ. Preterm labor: one syndrome, many causes. Science (New York, NY). 2014;345(6198):760–5.
Mor G, Cardenas I. The immune system in pregnancy: a unique complexity. Am J Reprod Immunol. 2010;63(6):425–33.
Sacks G, Sargent I, Redman C. An innate view of human pregnancy. Immunol Today. 1999;20(3):114–8.
Acknowledgements
We thank Rebecca Sawyer for conducting the serum assays, Gary Heinemann and Dylan McCullough for assistance with animal and laboratory work.
Funding
This work was funded by a grant from the National Health and Medical Research Council of Australia (NHMRC) awarded to CTR and PHA (GNT1020754). CTR was supported by a NHMRC Senior Research Fellowship (GNT1020749) and currently supported by the Lloyd Cox Professorial Research Fellowship, University of Adelaide. PHA is supported by a NHMRC Career Development Award (GNT1051858). RLW and JAL were recipients of Australian Postgraduate Awards.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
ESM 1
(DOCX 32 kb)
Rights and permissions
About this article
Cite this article
Wilson, R.L., Phillips, J.A., Bianco-Miotto, T. et al. Reduced Dietary Calcium and Vitamin D Results in Preterm Birth and Altered Placental Morphogenesis in Mice During Pregnancy. Reprod. Sci. 27, 1330–1339 (2020). https://doi.org/10.1007/s43032-019-00116-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-019-00116-2