Abstract
Small molecule-mediated bone regeneration is emerging as a promising strategy for replacing or enhancing the therapeutic protein-based growth factors. However, unknown non-specific toxicity of small molecules on non-target cells or organs due to the long-term exposure has been a concern. We previously demonstrated that the continuous treatment of osteoblast-like MC3T3-E1 cells with small molecule cyclic AMP analogue N6-benzoyladenosine-3′,5′-cyclic monophosphate (6-Bnz-cAMP) was capable of inducing in vitro osteogenesis via the protein kinase A (PKA) signaling pathway. In this study, we investigate the effect of short-term 6-Bnz-cAMP treatment, i.e., 1-day treatment, as compared to continuous treatment, on in vitro osteogenesis in osteoprogenitor cells. It is hypothesized that the proposed short-term 6-Bnz-cAMP treatment scheme would result in osteogenesis as in the case of continuous 6-Bnz-cAMP treatment. Our results showed that both short-term and continuous 6-Bnz-cAMP treatments elicited osteoblastic differentiation and mineralization of osteoblast-like MC3T3-E1 cells. Short-term treatment using small molecule 6-Bnz-cAMP can serve as a highly promising strategy for bone regeneration while mitigating potential non-specific side effect risks associated with small molecules.
Lay Summary
The goal of this work is to develop a simple, inexpensive, effective, and safe method to heal bone defect. We would like to treat the bone defects with a small molecule-based therapeutic agent in a short-term treatment so that undesirable side effects from the therapeutics would be significantly minimized. Our work may also result in novel bone graft materials that can potentially become a viable alternative to existing grafts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With the ever-growing need of better musculoskeletal regenerative therapies, small molecules are fast emerging as highly promising alternatives for conventional treatment options [1,2,3,4,5,6,7,8]. The magnitude and overwhelming impact of these musculoskeletal diseases on the US population and economy cannot be overemphasized. Over the years, grafting techniques have been on the front burner of musculoskeletal disorder treatment options [9,10,11,12]. Although these techniques are still very much in use, they are often plagued with donor morbidity and disease transmission, which has aroused genuine concern for patients and clinicians alike [13]. Ideally, regenerating a damaged, diseased, or lost musculoskeletal tissue is considered a better clinical strategy when compared to repairing the said tissue. Since regenerative engineering was put forward as a highly promising strategy for musculoskeletal tissue regeneration [14], a plethora of bioactive molecules and/or protein-based growth factors have been extensively investigated [2, 3].
Regenerative engineering systematically integrates advanced material sciences, stem cell technologies, physical forces, clinical translational science with advanced animal models, and developmental biology with bioactive factors towards the goal of regenerating complex musculoskeletal tissues or organ systems [15, 16]. Depending on the scaffolding system, the molecular processes of the myriad growth factors in platelet-rich plasma, pro-osteogenic chemokines, cytokines, and angiogenic factors leading to osteoblastic bone formation are well elucidated [17, 18]. In musculoskeletal applications, for example, bone morphogenetic proteins (BMPs) have proven very useful in bone regeneration. Thus, BMP-2 and BMP-7 have been approved by the FDA to be used clinically to promote fracture healing, spinal fusions, long bone non-unions, and periodontal and dental implants [5, 19,20,21].
Despite the promise of the current BMP-based therapeutics, the scores of limitations such as supraphysiological dosage, ectopic bone formation, immunogenicity, high cost, high dosage, and protein instability associated with the BMP therapeutics have led to the investigation of promising alternatives—osteogenic small molecules [5]. The size of these small molecules allows them to easily diffuse across the cellular membrane, thus activating intracellular signaling cascades that leads to gene transcription and osteogenic marker expressions (e.g., alkaline phosphatase, Runx2, osteocalcin, collagen, and osteopontin) [1, 22, 23]. Owing to their attractive intrinsic physical properties, small molecules hold great promise as the next generation of bone regenerative therapies. In the recent past, many novel small molecules with osteoinductive potential have been discovered via high-throughput chemical screens [24,25,26]. In addition, a number of small molecules have been reported to activate osteogenic-associated signaling pathways including BMP signaling, hedgehog (Hh) pathway, Wnt/beta-catenin pathway, cyclic AMP (cAMP) signaling pathways, rho-associated protein kinase (ROCK), and extracellular signal-regulated kinase (ERK) [1, 27, 22, 28,29,30,31,32]. Intriguingly, certain small molecules can activate or enhance the BMP-mediated signaling cascade in primary cells; efforts are underway to support, supplement, or replace therapeutic growth factors with these small molecules in order to lower the required therapeutic exogenous BMP dose or provide adequately effective alternatives [22, 33,34,35]. For instance, small molecule phenamil has been shown to induce BMP-mediated bone formation in mouse mesenchymal stem cells (MSCs) and pre-osteoblast MC3T3-E1 cells via the Smad signaling pathway. More specifically, phenamil acts cooperatively with BMPs to induce osteoblastic differentiation in MSCs and organ cultures [22, 36]. Recently, small molecule cAMP analogues have been demonstrated to enhance both angiogenesis and osteogenesis via cyclic AMP signaling pathways such as protein kinase A (PKA)/cAMP response element-binding protein (CREB) signaling cascade and exchange protein activating by cAMP (Epac) pathway [23]. It should be noted that the small molecule cAMP is a secondary messenger regulating diverse cellular processes such as cell adhesion and spreading, proliferation, apoptosis, differentiation, morphogenesis, osteogenesis, angiogenesis, and chondrogenesis [37,38,39].
Cyclic AMP is increasingly attracting attention in the field as a potential musculoskeletal regenerative therapeutic agent because several studies have demonstrated that several cAMP small molecule analogues can modulate osteogenesis in vitro and in vivo [27] [40]. Cyclic AMP analogues, such as 8-bromoadenosine-3′,5′-cyclic monophosphate (8-Br-cAMP), have recently been investigated as novel bone-inducing biofactors, promoting osteogenesis and angiogenesis in osteoprogenitor MC3T3-E1 cells [37]. It has been demonstrated that a novel protein kinase A (PKA)-specific cAMP analogue, N6-benzoyladenosine-3′,5′-cyclic monophosphate (6-Bnz-cAMP) (Fig. 1), was able to induce osteoblastic differentiation and matrix mineralization in osteoblast-like MC3T3-E1 cell culture [40]. Because of their small molecular size, these osteogenic small molecules are often accompanied by non-specific effects as they are able to diffuse to neighboring tissues where they are not needed [1]. Researchers have actively investigated various targeted drug delivery strategies such as encapsulation of small molecules in microspheres, nanofibers-based scaffolds, or nanoparticles to ensure a controlled and sustained drug release in the targeted tissue whereas others have tried to mitigate the potential toxicities or unwanted physiological responses by modifying the drug dosing and treatment frequency [7, 8]. Previously, we aimed to work to minimize side effects associated with the small molecule phenamil by reducing the frequency of administration (e.g., less than 24-h treatment) as well as loading it into a biodegradable poly(lactide-co-glycolide acid) (PLGA) polymeric microsphere-based scaffold to evaluate its bioactivity [41, 42]. In this study, we adopt the similar drug treatment strategy to investigate the effect of short-term 6-Bnz-cAMP treatment, i.e., 1-day treatment, as compared to continuous treatment on in vitro osteogenesis. We hypothesized that short-term 6-Bnz-cAMP treatment would result in osteogenesis as in the case of continuous 6-Bnz-cAMP treatment. Our results revealed that both short-term and continuous 6-Bnz-cAMP treatments elicit osteoblastic differentiation and mineralization of osteoblast-like MC3T3-E1 cells, and that hence the short treatment plan can serve as a highly promising strategy to mitigate any potential risks associated with small molecules.
Chemical structure of N6-benzoyladenosine-3′,5′-cyclic monophosphate (6-Bnz-cAMP), sodium salt. Various studies indicate that 6-Bnz-cAMP interacts with PKA by binding to site 2 on the regulatory subunit. Due to its lipophilic nature, this small molecule compound can easily travel across cell membranes in various cells
Materials and Methods
Reagents
The specific chemicals and supplies necessary for this study included N6-benzoyladenosine-3′,5′-cyclic monophosphate (6-Bnz-cAMP) (Alexis Biochemicals, San Diego, CA), recombinant BMP-2 (R&D Systems, Minneapolis, MN), mouse Collagen Type 1 (Col1A1) ELISA kit (mybiosource.com, San Diego, CA), mouse osteocalcin ELISA kit (AlfaAesar, Tewksbury, MA), anti-osteopontin antibody (AKm2A1) and Protein A/G agarose beads (Santa Cruz Biotechnology, Inc., Dallas, TX), mouse IgG and rabbit IgG antibodies labeled with horseradish peroxidase (HRP) (KPL, Gaithersburg, MD), and chemiluminescent substrate and X-ray films (Thermo Scientific, Rockford, IL).
Cell Culture
The effects of 6-Bnz-cAMP on differentiation and mineralization of osteoprogenitor MC3T3-E1 (sublcone 4) cell cultures (American Type Culture Collection, Manassas, VA) (passage 21 to 30) were examined in this study. Tissue culture flasks and alpha minimal essential medium (Invitrogen, Carlsbad, CA), supplemented with 10% fetal bovine serum (FBS) and 1% of pen/strep antibiotic (100 U/ml penicillin G and 100 mg/ml streptomycin), were used to maintain the cells. Rat adipose-derived stem cells (rADSCs) were a gift from Dr. Laurencin’s lab at UConn Health. These cells were grown in DMEM medium (Invitrogen, Carlsbad, CA) supplemented with 10% FBS and 1% pen/strep, and incubated at 37 °C with 5% carbon dioxide and 85% relative humidity. MC3T3-E1 cells were cultured in regular growth medium with or without 100 μM of 6-Bnz-cAMP in order to assess the osteogenic effects of this small molecule. Positive controls for osteoblastic differentiation used in this study included cells cultured in a mineralization-promoting medium (alpha minimal essential medium supplemented with 10% FBS, 1% pen/strep, 3 mM β-glycerophosphate, and 10 μg/ml ascorbic acid, 0.1 nM dexamethasone), as well as cells cultured in regular media supplemented with 50 ng/ml BMP-2. To clarify which media were being used in the experimental studies in each figure, the term “Control or no treatment” refers to regular growth medium. “1D” indicates regular or mineralization growth medium supplemented with 6-Bnz-cAMP and administered just for 1 day (24 h) only, after which the cells were washed once with 1xPBS and switched to unsupplemented regular or mineralization growth medium for the remainder of the culture period. “CT” denotes regular or mineralization growth medium supplemented with 6-Bnz-cAMP and administered continuously—introduced into the media at every fresh media change. Media were changed every 3–4 days during the culture period after the first day’s media change. “Osteo” refers to mineralization medium, and “BMP” refers to regular or mineralization growth medium supplemented with recombinant BMP-2 and administered continuously [40].
Cell Proliferation and Viability Assay
A colorimetric cell proliferation assay kit (MTS) was used to study cell proliferation (Promega, Madison, WI), according to the manufacturer’s instructions. Cells were collected at different time points as indicated in the Fig. 7a and b for the proliferation assays. Briefly, 5 × 104 cells per ml of regular growth medium, with or without 100 μM of 6-Bnz-cAMP, were seeded in the wells of a 24-well tissue culture plate. Note that no mineralization media were used in this experiment. At the experimental time points, media were removed and cells were washed with phosphate-buffered saline (PBS). For the cell viability studies, each of the well plates were trypsinized at the end of each time point and the cell suspension was stained with trypan blue before live/dead cells were counted using a hemocytometer.
SDS-Polyacrylamide Gel Electrophoresis and Western Blotting
SDS-polyacrylamide gel electrophoresis (SDS-PAGE) and western blotting were performed as previously described [43]. Osteogenic protein markers such as osteopontin (OPN) were analyzed by SDS-PAGE and western blot. Protein samples were first resolved by SDS-PAGE on a 4–15% Mini-PROTEAN® TGX™ Precast Protein Gel (Bio-Rad, Hercules, CA). The separated protein was then transferred electrophoretically onto polyvinylidene difluoride membranes. Membranes were blocked with a 10% skim milk solution, and then the respective antibodies were used to probe the membranes for the proteins of interest, to be visualized by a chemiluminescent detection kit (Thermo Scientific, Rockford, IL).
Immunoprecipitation
The cell culture media after 21-day incubation were collected in microcentrifuge tubes. The extracellullar protein osteopontin (OPN), collected by extracting samples of culture media, was isolated by incubating with anti-osteopontin antibody (Santa Cruz Biotech, Dallas, TX). The antibody-bound proteins were precipitated by incubating with Protein A/G agarose beads (Santa Cruz Biotech, Dallas, TX) for another 2 h at 4 °C. Immunocomplexes were then washed four times with PBS. The beads were then resuspended in 2× Laemmli SDS sample buffer (Bio-Rad, Hercules, CA) for SDS-PAGE and western blot analysis [40].
Alkaline Phosphatase Activity
Alkaline Phosphatase (ALP) activities were measured using an ALP assay kit and its established protocol (Bio-Rad, Hercules, CA). Note that mineralization medium was not used in this experiment. Briefly, at days 4, 7, and 14, media were removed and cells were washed four times with PBS and then lysed with radioimmunoprecipitation assay (RIPA) lysis buffer (Sigma, Saint Louis, MI). Cell lysates were collected and mixed with ALP substrate solution which was added to the cell lysates and incubated for 1–2 h at 37 °C. ALP activity was assessed using a spectrophotometric plate reader at 405 nm to quantify the color change produced by the assay reagent. The absorbance values were normalized to bicinchoninic acid (BCA) protein, quantified by a similar colorimetric assay (Thermo Scientific, Rockford, IL) that was read at 562 nm.
Matrix Mineralization Assay
The osteoblast-like MC3T3-E1 cells were cultured in mineralization medium and supplied with 6-Bnz-cAMP (100 μM), according to the continuous, 1 day, and control treatment protocols. The mineralization media were replaced every 3–4 days during the culture period. To qualitatively assess calcified matrix mineralization, media were removed at day 21, and cells were rinsed three times with calcium-free PBS. Any precipitated calcium from mineralized matrix was fixed with 70% ethanol for 1 h at 4 °C. The extracted calcium was first stained with alizarin red (Sigma, Saint Louis, MI), washed five times, and dissolved in cetyl pyridinium chloride (CPC) (Sigma, Saint Louis, MI) which turned the red color reaction product into purple. The absorbance was finally read at with a plate reader at 562 nm.
Real-Time Reverse Transcription PCR Analysis
MC3T3-E1 cells were plated in 6-well culture plates. At 90% confluence, the cells were then treated with corresponding conditioned media according to the treatment group paradigms without the use of mineralization medium for 7 days. Quantitative reverse transcription polymerase chain reaction (qRT-PCR) was used to quantify different osteogenic markers: osteocalcin (Bglap), alkaline phosphatase (Alpl), collagen 1A1 (col1a1), Runt-related transcription factor 2 (Runx2), and osteopontin (Spp1) gene expressions. Total RNA was isolated using the RNeasy Mini System (Qiagen, Hilden, Germany). One microgram of total RNA was used as a template for synthesis of complementary DNA (cDNA). A light cycler instrument (Bio-Rad iCycler iQ system, Hercules, CA) along with SuperMix Premix (Bio-Rad, Hercules, CA) and Taqman Gene Expression Assays (Applied Biosystems, Guilford, CT) was used for this real-time PCR analysis. The comparative CT method (ΔΔCt) was employed to normalize the gene expressions to the quantity of housekeeping gene Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) [37].
Enzyme-Linked Immunosorbent Assay
Mouse osteocalcin enzyme-linked immunosorbent assay (ELISA) kit (AlfaAesar, Tewksbury, MA) was used to quantify secreted col1A1 and osteocalcin protein levels in the cell culture media respectively according to the manufacturer’s instructions. Samples were obtained from cultures using the three media treatment groups, without mineralization media. The assay product solution called for the use of a microplate reader (Biotek Synergy™ HT, Winooski, VT) at a wavelength of 450 nm. The absorbance was used to determine protein concentrations, based on a standard curve using the protein standards provided by the manufacturer.
Non-target Cell Side Effects
A colorimetric assay employing 3-(4,5-dimethylthiazol-2-yl)-5-(3-carboxymethoxyphenyl)-2-(4-sulfophenyl)-2H-tetrazolium, internal salt (MTS) (Promega, Madison, WI) was used to assess the proliferation of adipose-derived stem cells (ADSCs) when exposed to the different treatment paradigms of 6-Bnz-cAMP in normal growth medium. Hindrance of proliferation in ADSCs, as a non-target cell type, could reveal potential undesirable side effects associated with the use of 6-Bnz-cAMP. The experimental cells were exposed to the MTS reagent-containing media for 50 min at the end of each time point (3, 7, and 14 days), and the media were analyzed according to the manufacturer’s protocol.
Statistical Analysis
Replicates were averaged and the average values were used for group comparisons. One-way ANOVA (GraphPad Prism) was applied followed by post hoc comparisons via two-sample independent t tests. Due to small sample sizes, the t test results were not adjusted for multiple testing in favor of the control of type II error. A p value smaller than 0.05 was considered statistically significant. All the statistical analyses were performed in Microsoft Excel.
Results
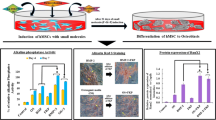
Figure 1 presents the chemical structure of the 6-Bnz-cAMP molecule. The molecule differs from the natural cyclic AMP molecule in that a lipophilic benzoyl group replaces a hydrogen of the position 6 amino group of the nucleobase, providing greater lipophilicity and cell membrane permeability. Due to the fact that ALP activity is an early-stage marker of osteoblastic differentiation, the osteogenic potential of the various 6-Bnz-cAMP treatment plans (1-day vs continuous treatment) was determined with a commercial ALP activity assay kit. ALP is an enzyme produced by osteoblasts that is involved in the mineralization of bone. It is generally considered as a routine marker to evaluate osteoblastic differentiation and its increased expression and/or activity is associated with the progressive differentiation of osteoblasts. Measurements of ALP activities at 14-day time points demonstrated that the 1-day 6-Bnz-cAMP administration is significantly higher than the untreated negative control group (Fig. 2c). The observed elevated ALP activity indicated that both 1-day and continuous 6-Bnz-cAMP treatments were able to induce osteoblastic differentiation of osteoblast-like MC3T3-E1 cells.
Effect of various 6-Bnz-cAMP treatment plans on osteoblastic differentiation of osteoblast-like MC3T3-E1-E1 cells. 4 days (a), 7 days (b), and 14 days (c) alkaline phosphatase (ALP) assay of 1-day vs continuous treatment of 6-Bnz-cAMP were determined using a commercial ALP activity substrate assay kit. The ALP absorbance values were normalized to cellular protein. To facilitate the comparison of the various experimental groups, the normalized ALP absorbance values of the negative control group was set to one relative unit. Error bars represent means ± SD (n = 4). NT negative control (untreated basal media), 1D 1 day treatment group, CT continuous treatment group, OST osteogenic media (positive control 1), BMP 2 bone morphogenic protein 2 (positive control 2). Individual groups labeled with “*” are statistically significantly higher than negative control (NT) (p < 0.05)
Although the ALP enzyme is a marker usually employed to estimate osteogenic levels during the bone maturation process [44], matrix mineralization or calcification is considered a definitive hallmark or in vitro endpoint that reflects advanced cell differentiation and maturation in osteogenic cell culture studies [42, 45, 46]. Data in Fig. 3a indicated that there was statistically significantly higher calcification formed in 1-day 6-Bnz-cAMP and continuous 6-Bnz-cAMP treatment groups when compared to untreated cells cultured in regular media. It indicated that both 1-day and continuous 6-Bnz-cAMP treatments induced matrix mineralization, and this was consistent with our previous study [40]. Similar to the hydroxyapatite (i.e., calcium phosphate) found in bone, teeth, and hard tissue, it is worth noting that the observed deposited mineral in vitro is also in the form of calcium phosphate (Fig. 3b) [47, 48].
Effect of various 6-Bnz-cAMP treatment plans on matrix mineralization of osteoblast-like MC3T3-E1 cells. Matrix mineralization was assessed after 21 days of culturing MC3T3-E1 cells in untreated regular basal media (NT), untreated osteogenic media (Osteo), osteogenic media supplemented with 1-day and continuous 6-Bnz-cAMP treatments and positive BMP 2 treatment group. The qualitative assay was carried out using alizarin red solution as shown in panel b whereas the quantitative assay was analyzed via the colorimetric assay of the total calcium deposited in the matrix using cetyl pyridinium chloride (CPC) (b). *Individual group is statistically significantly higher than negative control (NT) (p < 0.05)
In an attempt to evaluate the expression levels of other relevant osteoblast-specific marker genes (alkaline phosphatase (Alpl), osteocalcin (Bglap), collagen 1A1 (col1a1), Runt-related transcription factor 2 (Runx2), and osteopontin (Spp1)), we conducted a real-time RT-PCR assay on the cells. The data represented in Fig. 4 show higher expression of all the gene markers in 1-day 6-Bnz-cAMP treatment as compared to the negative control, though the strongly positive control BMP-2 exhibited greater expression levels for many of the genes. The early osteoblast marker Runx2 [49], the late osteoblast developing markers Bglap and Col1A1 [50], and the extracellular matrix protein Spp1 are all important osteogenic markers during osteogenesis [51,52,53], despite the fact that some of these markers are considered late-stage markers, for instance, Bglap, Spp1, and Col1A1 were already significantly upregulated on day 7 for both BMP-treated cells and the 1-day treatment group. Taken together, the upregulation of these osteogenic gene markers in 1-day 6-Bnz-cAMP treatment suggests that the 1-day administration of the drug was still effective for osteogenesis even after 7 days.
Gene expression profiling of osteoblast-specific marker genes by quantitative RT-PCR. The osteoblast-specific gene markers were assayed after 7 days of cell seeding employing the qRT-PCR. Alkaline phosphatase (Alpl), osteocalcin (Bglap), collagen 1A1 (col1a1), RunX2, and osteopontin (Spp1) were all upregulated in the 1D and BMP2 treatment groups. *, #Individual group statistically significantly higher than the negative control (p < 0.05)
We performed an immunoprecipitation assay to evaluate the presence of the late osteoblast-associated marker, osteopontin (OPN). As a secretory highly phosphorylated glycoprotein matrix with prominent cell attachment properties, OPN can be isolated using immunoprecipitation techniques after which western blot is be performed on the immunoprecipate [40, 54, 55]. The cells were cultured in either drug-supplemented osteogenic media or not; hence, osteogenic media was considered as the negative control in this case whereas BMP-2 served as the positive control. Figure 5 shows that both 1-day 6-Bnz-cAMP and BMP-2 treatments caused OPN upregulation as compared to the negative control.
One-day 6-Bnz-cAMP administration showed an enhanced osteopontin level in pre-osteoblast MC3T3-E1 cells. Immunoprecipitation followed by western blot analysis of osteoblast-like MC3T3-E1 cells treated with the various treatment groups and cultured for 21 days revealed that obvious osteopontin protein levels were observed in the BMP-2 and 1-day (1D) treatment groups whereas no detectable osteopontin was observed in the non-treated (NT) group. The HC and LC bands are the heavy chain and light chain fractions, respectively, of the antibody molecules used in the immunoprecipitation procedure
Osteocalcin (OCN), a hydroxyapatite-binding protein expressed mainly during bone formation phase, has been implicated in organizing extracellular matrix and osteoid mineralization owing to the three vitamin K-dependent gamma-carboxyglutamic acid residues that confer the calcium-binding properties [56]. Its ability to interact with other cell surface receptor proteins at the carboxy-terminus renders them active in coordinating the extracellular matrix [56,57,58]. The OCN proteins were detected and quantified using ELISA. Figure 6 demonstrates that both 1-day and continuous 6-Bnz-cAMP treatments were able to induce OCN extracellular protein productions but only the BMP treatment group had statistically significant higher OCN as compared to the no treatment group.
Taken together, coupled to the elevated ALP and matrix mineralization observed, various osteoblast-associated gene expressions from the RT-PCR, increased OPN secretion from the immunoprecipitation assay have all clearly demonstrated that short-term treatment of 6-Bnz-cAMP could significantly enhance osteogenic protein expressions and ultimately results in matrix mineralization of osteoblast-like MC3T3-E1 cells.
In an attempt to determine the toxicity of a single-dose treatment versus continuous treatment, trypan blue live/dead cell assay and MTS biochemical assay were used to measure the cell viability and proliferation, respectively. The results in Fig. 7a indicated that there was no apparent difference in the percent viabilities of all the experimental groups assayed in osteoblast-like MC3T3-E1 cells. The percent viability of the seeded cells in all the groups at the end of 21 days was greater than 95%, which suggests that all the groups still had a substantial numbers of viable cells at that time. Furthermore, to show the proliferation effect of 6-Bnz-cAMP on non-target cells like tissue-derived stem cells like adipose-derived stem cells (ADSC), the cell proliferation data for treated rat ADSCs in Fig. 7b show that there is no statistically significant difference in proliferation on the day 3 and 7 time points between treatment groups. On day 14, there were significant differences between the continuous treatment group and the 1-day treatment group, and between the continuous treatment group and the no treatment group. There were no apparent reductions in cell proliferation at day 14 compared to day 3.
a Cell viability study. There were no significant differences in the percentage MC3T3-E1 cell viabilities of all the groups. b MTS assay on rADSCs to evaluate proliferation and potential toxicity of 6-Bnz-cAMP treatment for a non-target cell type. Statistical analysis within each time point reveals significant differences between treatment groups only on day 14. ***, ###p < 0.001
Discussion
Our goal was to study the in vitro osteogenesis of the small molecule drug 6-Bnz-cAMP using short-term administration, in an effort to reduce the treatment costs and potential toxicity and side effects of the small molecule drug. Drug toxicity is arguably a major contributor of the high cost of drug development and design especially when it is recognized at late-stage clinical trials or post marketing [59, 60]. It is thought to account for the attrition of approximately one third of the administered drugs [60]. Immune hypersensitivity, bio-activation, covalent modification, mechanism-based (on-target) toxicity, and off-target toxicities are a few known causes of drug toxicities among others [60]. Given that small molecule drugs like 6-Bnz-cAMP can easily diffuse to other nearby non-target tissues due to their small size, it is imperative to devise a strategy that retains the therapeutic effect of 6-Bnz-cAMP while mitigating the risk of toxicity. Related to this work, our research group previously demonstrated that the continuous treatment of pre-osteoblast MC3T3-E1 cells with 6-Bnz-cAMP successfully induced in vitro osteogenesis [40]. Despite its osteogenic potential, there could be concern regarding non-specific effects that are linked to these small molecule drugs. In an attempt to minimize side effects and other non-specific toxicities associated with small molecule drugs via reduction of administration frequency, we demonstrated in this study that 1-day 6-Bnz-cAMP treatment (24 h) sufficiently stimulated in vitro osteogenesis in osteoblast-like MC3T3-E1 cells as evident by the elevated various osteogenic markers. In short, the treatment of osteoblast-like MC3T3-E1 cells with 6-Bnz-cAMP for as short as a single day resulted in enhanced alkaline phosphatase (ALP) activity as well as matrix mineralization, indicating in vitro osteoblastic differentiation.
Furthermore, the differentiation of osteoblast-like MC3T3-E1 cells observed in this study may be partially due to the increased integrin-dependent cell adhesion induced by 6-Bnz-cAMP [43, 61]. Given that several integrin subunits have been reported to elicit various signaling that activates distinct downstream signal transduction [62,63,64], we believe that integrin-dependent cell adhesion could be playing a significant role in osteoblast function. Our group has earlier shown that 6-Bnz-cAMP, while mediated by integrin subunits, successfully enhances osteoblast cell adhesion, suggesting that cell adhesion is dominated by the PKA-mediated signal pathway [43]. Cell adhesion is an important process that influences biological processes such as cell morphology, proliferation, differentiation, specialization, and, ultimately, bone formation [61]. It is interesting to note that cell adhesion is the initiating step to any cell activity as these cells will undergo apoptosis if they are not attached to a surface properly [61, 65, 66].
6-Bnz-cAMP is a target-specific cAMP analogue which exclusively activates PKA signaling, and its mechanism of action is via PKA 1 activation which in turn phosphorylates and elicits other downstream signal cascades such as CREB [67]. Continuous activation of these downstream signals might result in additional unwanted physiological effects on the cells. Thus, this can be circumvented by reducing drug administration dose or reducing the frequency of administration, as this will in turn lower the frequency of activating many downstream signaling cascades. In addition, researchers have developed various drug delivery systems that can deliver these signaling molecules locally to their target sites with appropriate control release kinetics [7, 8, 68, 69]. Overall, it was shown that 1-day treatment of 6-Bnz-cAMP is adequate to induce differentiation of osteoblast-like MC3T3-E1 cells. The result of the viability in Fig. 7 did not show any obvious difference in MC3T3-E1 cells but these signaling molecules may present significant toxicities in other cells and tissues [70]. The results of the rADSC proliferation study, shown in Fig. 7b, indicate that 1-day treatment did not cause an apparent significant decrease in proliferation over the three time points, compared to the non-treatment control group. This would suggest that 1-day treatment for effective bone repair can be used without causing significant negative effects on this particular non-target cell type such as rADSC. It is interesting to note that continuous 6-Bnz-cAMP treatment can cause significantly increased proliferation of rADSC at day 14 (Fig. 7b). The continuous 6-Bnz-cAMP treatment may cause the unwanted side effect of increasing ADSC proliferation. Thus, additional tests of this treatment paradigm on non-target tissue types are needed in order to more thoroughly elucidate the mechanisms and scope of non-specific effects and to verify and expand the understanding of these preliminary results regarding the behavior of treated rADSCs.
Due to the fact that a considerable number of patients have suffered from undesirable side effects of their drug treatments instead of the actual ailment, it is advisable to administer these small molecules only when they are ultimately needed and cannot be avoided. Future experiments are required to investigate the detailed molecular mechanisms underlying the osteogenic effects from 1-day treatment of 6-Bnz-cAMP and to examine the osteoconductivity, dosages, and best treatment regimens of 6-Bnz-cAMP in preclinical and clinical studies. The short-term 6-Bnz-cAMP administration resulted in an osteogenic differentiation response. Our short-term drug treatment studies could serve as a drug discovery model for other osteoinductive small molecules for bone repair and regeneration. Our short-term exposure of small molecule 6-Bnz-cAMP study (previously phenamil and 8-Br-cAMP) may represent an emerging treatment strategy (i.e., short-term drug treatment) for the management of skeletal disorders with lower treatment costs and toxicity.
References
Lo KW-H, Ashe KM, Kan HM, Laurencin CT. The role of small molecules in the musculoskeletal regeneration. Regen Med. 2012;7:1–15.
Lo KW, Jiang T, Gagnon KA, Nelson C, Laurencin CT. Small-molecule based musculoskeletal regenerative engineering. Trends Biotechnol. 2014;32:74–81.
Laurencin CT, Ashe KM, Henry N, Kan HM, Lo KW. Delivery of small molecules for bone regenerative engineering: preclinical studies and potential clinical applications. Drug Discov Today. 2014;19:794–800.
Lo KW, Ulery BD, Deng M, Ashe KM, Laurencin CT. Current Patents on Osteoinductive Molecules for Bone Tissue Engineering. Recent Patents on Biomedical Engineering. 2011;4:153–67.
Lo KW-H, Ulery BD, Ashe KM, Laurencin CT. Studies of bone morphogenetic protein based surgical repair. Adv Drug Deliv Rev. 2012;64:1277–91. https://doi.org/10.1016/j.addr.2012.1003.1014.
Awale G, Wong E, Rajpura K, Lo KW. Engineered bone tissue with naturally-derived small molecules. Curr Pharm Des. 2017;23:3585–94. https://doi.org/10.2174/1381612823666170516145800.
Carbone EJ, Jiang T, Nelson C, Henry N, Lo KW. Small molecule delivery through nanofibrous scaffolds for musculoskeletal regenerative engineering. Nanomedicine. 2014;10:1691–9.
Carbone EJ, Rajpura K, Allen BN, Cheng E, Ulery BD, Lo KW. Osteotropic nanoscale drug delivery systems based on small molecule bone-targeting moieties. Nanomedicine. 2017;13:37–47.
Laurencin C, Khan Y, El-Amin SF. Bone graft substitutes. Expert Rev Med Devices. 2006;3:49–57.
Hartigan BJ, Makowiec RL. Use of bone graft substitutes and bioactive materials in treatment of distal radius fractures. Hand Clin. 2009;23:241–6.
Finkemeier CG. Bone-grafting and bone-graft substitutes. J Bone Joint Surg Am. 2002;84-A:454–64.
De Long WG Jr, Einhorn TA, Koval K, McKee M, Smith W, Sanders R, et al. Bone grafts and bone graft substitutes in orthopaedic trauma surgery. A critical analysis. J Bone Joint Surg Am. 2007;89:649–58.
Rogers GF, Greene AK. Autogenous bone graft: basic science and clinical implications. J Craniofac Surg. 2012;23:323–7.
Laurencin CT, Khan Y. Regenerative engineering. Sci Transl Med. 2012;4:160ed169.
Laurencin CT, Nair LS. Regenerative engineering: approaches to limb regeneration and other grand challenges. Regen Eng Transl Med. 2015;1:1–3.
Laurencin CT, Nair LS. The Quest toward limb regeneration: a regenerative engineering approach. Regen Biomater. 2016;3:123–5.
Cui Q, Dighe AS, Irvine JN Jr. Combined angiogenic and osteogenic factor delivery for bone regenerative engineering. Curr Pharm Des. 2013;19:3374–83.
Segar CE, Ogle ME, Botchwey EA. Regulation of angiogenesis and bone regeneration with natural and synthetic small molecules. Curr Pharm Des. 2013;19:3403–19.
Bessa PC, Casal M, Reis RL. Bone morphogenetic proteins in tissue engineering: the road from laboratory to clinic, part II (BMP delivery). J Tissue Eng Regen Med. 2008;2:81–96.
Bessa PC, Casal M, Reis RL. Bone morphogenetic proteins in tissue engineering: the road from the laboratory to the clinic, part I (basic concepts). J Tissue Eng Regen Med. 2008;2:1–13.
Jeon OH, Elisseeff J. Orthopedic tissue regeneration: cells, scaffolds, and small molecules. Drug Deliv Transl Res. 2017;6:105–20.
Park KW, Waki H, Kim WK, Davies BS, Young SG, Parhami F, et al. The small molecule phenamil induces osteoblast differentiation and mineralization. Mol Cell Biol. 2009;29:3905–14.
Ifegwu OC, Awale G, Rajpura K, Lo KW, Laurencin CT. Harnessing cAMP signaling in musculoskeletal regenerative engineering. Drug Discov Today. 2017;22:1027–44.
Alves H, Dechering K, Van Blitterswijk C, De Boer J. High-throughput assay for the identification of compounds regulating osteogenic differentiation of human mesenchymal stromal cells. PLoS One. 2011;6:e26678.
Brey DM, Motlekar NA, Diamond SL, Mauck RL, Garino JP, Burdick JA. High-throughput screening of a small molecule library for promoters and inhibitors of mesenchymal stem cell osteogenic differentiation. Biotechnol Bioeng. 2011;108:163–74.
Han CY, Wang Y, Yu L, Powers D, Xiong X, Yu V, et al. Small molecules with potent osteogenic-inducing activity in osteoblast cells. Bioorg Med Chem Lett. 2009;19:1442–5.
Doorn J, Leusink M, Groen N, van de Peppel J, van Leeuwen JP, van Blitterswijk CA, et al. Diverse effects of cyclic AMP variants on osteogenic and adipogenic differentiation of human mesenchymal stromal cells. Tissue Eng A. 2012;18:1431–42.
Sefcik LS, Petrie Aronin CE, Botchwey EA. Engineering vascularized tissues using natural and synthetic small molecules. Organogenesis. 2008;4:215–27.
Siddappa R, Martens A, Doorn J, Leusink A, Olivo C, Licht R, et al. cAMP/PKA pathway activation in human mesenchymal stem cells in vitro results in robust bone formation in vivo. Proc Natl Acad Sci U S A. 2008;105:7281–6.
Nohria A, Prsic A, Liu PY, Okamoto R, Creager MA, Selwyn A, et al. Statins inhibit Rho kinase activity in patients with atherosclerosis. Atherosclerosis. 2009;205:517–21.
Woo SM, Lim HS, Jeong KY, Kim SM, Kim WJ, Jung JY. Vitamin D promotes odontogenic differentiation of human dental pulp cells via ERK activation. Mol Cells. 2015;38:604–9.
Tintut Y, Parhami F, Bostrom K, Jackson SM, Demer LL. cAMP stimulates osteoblast-like differentiation of calcifying vascular cells. Potential signaling pathway for vascular calcification. J Biol Chem. 1998;273:7547–53.
Wong E, Sangadala S, Boden SD, Yoshioka K, Hutton WC, Oliver C, et al. A novel low-molecular-weight compound enhances ectopic bone formation and fracture repair. J Bone Joint Surg Am. 2011;95:454–61.
Fan J, Guo M, Im CS, Pi-Anfruns J, Cui ZK, Kim S, et al. Enhanced mandibular bone repair by combined treatment of bone morphogenetic protein 2 and small-molecule phenamil. Tissue Eng A. 2017;23:195–207.
Fan J, Im CS, Cui ZK, Guo M, Bezouglaia O, Fartash A, et al. Delivery of phenamil enhances BMP-2-induced osteogenic differentiation of adipose-derived stem cells and bone formation in calvarial defects. Tissue Eng A. 2015;21:2053–65.
Lo KW, Ulery BD, Kan HM, Ashe KM, Laurencin CT. Evaluating the feasibility of utilizing the small molecule phenamil as a novel biofactor for bone regenerative engineering. J Tissue Eng Regen Med. 2014;8:728–36.
Lo KW, Kan HM, Gagnon KA, Laurencin CT. One-day treatment of small molecule 8-bromo-cyclic AMP analogue induces cell-based VEGF production for in vitro angiogenesis and osteoblastic differentiation. J Tissue Eng Regen Med. 2016;10:867–75.
Beavo JA, Brunton LL. Cyclic nucleotide research—still expanding after half a century. Nat Rev Mol Cell Biol. 2002;3:710–8.
Ho WC, Greene RM, Shanfeld J, Davidovitch Z. Cyclic nucleotides during chondrogenesis: concentration and distribution in vivo and in vitro. J Exp Zool. 1982;224:321–30.
Lo KW-H, Kan HM, Ashe KM, Laurencin CT. The small molecule PKA-selective cyclic AMP analogue as an inducer of osteoblast-like cells differentiation and mineralization. J Tissue Eng Regen Med. 2012;6:40–8.
Lo KW-H, Ulery BD, Ashe KM, Kan HM, Laurencin CT. Evaluating the feasibility of utilizing small molecule phenamil as a novel biofactor factor for bone regenerative engineering. J Tissue Eng Regen Med. 2014;8:728–36.
Lo KW, Kan HM, Laurencin CT. Short-term administration of small molecule phenamil induced a protracted osteogenic effect on osteoblast-like MC3T3-E1 cells. J Tissue Eng Regen Med. 2016;10:518–26.
Lo KWH, Ashe KM, Kan HM, Lee DA, Laurencin CT. Activation of cyclic AMP/protein kinase A signaling pathway enhances osteoblast cell adhesion on biomaterials for regenerative engineering. J Orthop Res. 2011;29:602–8.
Baek D, Villen J, Shin C, Camargo FD, Gygi SP, Bartel DP. The impact of microRNAs on protein output. Nature. 2008;455:64–71.
Quarles LD, Yohay DA, Lever LW, Caton R, Wenstrup RJ. Distinct proliferative and differentiated stages of murine MC3T3-E1 cells in culture: an in vitro model of osteoblast development. J Bone Miner Res. 1992;7:683–92.
Hoemann CD, El-Gabalawy H, McKee MD. In vitro osteogenesis assays: influence of the primary cell source on alkaline phosphatase activity and mineralization. Pathol Biol (Paris). 2009;57:318–23.
Landis WJ. Mineral characterization in calcifying tissues: atomic, molecular and macromolecular perspectives. Connect Tissue Res. 1996;34:239–46.
Dean DD, Schwartz Z, Bonewald L, Muniz OE, Morales S, Gomez R, et al. Matrix vesicles produced by osteoblast-like cells in culture become significantly enriched in proteoglycan-degrading metalloproteinases after addition of beta-glycerophosphate and ascorbic acid. Calcif Tissue Int. 1994;54:399–408.
Jikko A, Harris SE, Chen D, Mendrick DL, Damsky CH. Collagen integrin receptors regulate early osteoblast differentiation induced by BMP-2. J Bone Miner Res. 1999;14:1075–83.
Aubin JE. Bone stem cells. J Cell Biochem Suppl. 1998;30-31:73–82.
Cheng SL, Shao JS, Charlton-Kachigian N, Loewy AP, Towler DA. MSX2 promotes osteogenesis and suppresses adipogenic differentiation of multipotent mesenchymal progenitors. J Biol Chem. 2003;278:45969–77.
Kulterer B, Friedl G, Jandrositz A, Sanchez-Cabo F, Prokesch A, Paar C, et al. Gene expression profiling of human mesenchymal stem cells derived from bone marrow during expansion and osteoblast differentiation. BMC Genomics. 2007;8:70.
Lee DJ, Tseng HC, Wong SW, Wang Z, Deng M, Ko CC. Dopaminergic effects on in vitro osteogenesis. Bone Res. 2015;3:15020.
Widaa A, Claro T, Foster TJ, O’Brien FJ, Kerrigan SW. Staphylococcus aureus protein A plays a critical role in mediating bone destruction and bone loss in osteomyelitis. PLoS One. 2012;7:e40586.
Standal T, Borset M, Sundan A. Role of osteopontin in adhesion, migration, cell survival and bone remodeling. Exp Oncol. 2004;26:179–84.
Seibel MJ. Biochemical markers of bone turnover: part I: biochemistry and variability. Clin Biochem Rev. 2005;26:97–122.
Delmas PD, Malaval L, Arlot ME, Meunier PJ. Serum bone Gla-protein compared to bone histomorphometry in endocrine diseases. Bone. 1985;6:339–41.
Liu SH, Yang RS, Al-Shaikh R, Lane JM. Collagen in tendon, ligament, and bone healing. A current review. Clin Orthop Relat Res. 1995;318:265–78.
Wang YX, Yan SX. Biomedical imaging in the safety evaluation of new drugs. Lab Anim. 2008;42:433–41.
Guengerich FP. Mechanisms of drug toxicity and relevance to pharmaceutical development. Drug Metab Pharmacokinet. 2011;26:3–14.
Marquis ME, Lord E, Bergeron E, Drevelle O, Park H, Cabana F, et al. Bone cells-biomaterials interactions. Front Biosci. 2009;14:1023–67.
Gronowicz G, McCarthy MB. Response of human osteoblasts to implant materials: integrin-mediated adhesion. J Orthop Res. 1996;14:878–87.
Garcia AJ. Get a grip: integrins in cell-biomaterial interactions. Biomaterials. 2005;26:7525–9.
Enserink JM, Price LS, Methi T, Mahic M, Sonnenberg A, Bos JL, et al. The cAMP-Epac-Rap1 pathway regulates cell spreading and cell adhesion to laminin-5 through the alpha3beta1 integrin but not the alpha6beta4 integrin. J Biol Chem. 2004;279:44889–96.
Ribeiro VP, Almeida LR, Martins AR, Pashkuleva I, Marques AP, Ribeiro AS, et al. Modulating cell adhesion to polybutylene succinate biotextile constructs for tissue engineering applications. J Tissue Eng Regen Med. 2016;11:2853–63.
Rosales C, O’Brien V, Kornberg L, Juliano R. Signal transduction by cell adhesion receptors. Biochim Biophys Acta. 1995;1242:77–98.
Poppe H, Rybalkin SD, Rehmann H, Hinds TR, Tang XB, Christensen AE, et al. Cyclic nucleotide analogs as probes of signaling pathways. Nat Methods. 2008;5:277–8.
Carbone EJ, Rajpura K, Jiang T, Kan HM, Yu X, Lo KW-H. Osteotropic nanoscale drug delivery system via a single aspartic acid as the bone-targeting moiety. J Nanosci Nanotechnol. 2017;17:1747–52.
Rooney GE, Knight AM, Madigan NN, Gross L, Chen B, Giraldo CV, et al. Sustained delivery of dibutyryl cyclic adenosine monophosphate to the transected spinal cord via oligo [(polyethylene glycol) fumarate] hydrogels. Tissue Eng A. 2011;17:1287–302.
Siddappa R, Doorn J, Liu J, Langerwerf E, Arends R, van Blitterswijk C, et al. Timing, rather than the concentration of cyclic AMP, correlates to osteogenic differentiation of human mesenchymal stem cells. J Tissue Eng Regen Med. 2010;4:356–65.
Acknowledgements
We wish to thank Dr. Cato T. Laurencin, the Director of the Institute for Regenerative Engineering (IRE), for his leadership.
Funding
This work was supported by the Project Fund from the Connecticut Institute for Clinical and Translational Science (CICATS) to Dr. Kevin Lo.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ifegwu, O.C., Awale, G., Kan, H.M. et al. Bone Regenerative Engineering Using a Protein Kinase A-Specific Cyclic AMP Analogue Administered for Short Term. Regen. Eng. Transl. Med. 4, 206–215 (2018). https://doi.org/10.1007/s40883-018-0063-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40883-018-0063-1