Abstract
Cancer immunotherapies, widely heralded as transformational for many adult cancer patients, are becoming viable options for selected subsets of pediatric cancer patients. Many therapies are currently being investigated, from immunomodulatory agents to adoptive cell therapy, bispecific T-cell engagers, oncolytic virotherapy, and checkpoint inhibition. One of the most exciting immunotherapies recently FDA approved is the use of CD19 chimeric antigen receptor T cells for pre-B-cell acute lymphoblastic leukemia. With this approval and others, immunotherapy for pediatric cancers is gaining traction. One of the caveats to many of these immunotherapies is the challenge of predictive biomarkers; determining which patients will respond to a given therapy is not yet possible. Much research is being focused on which biomarkers will be predictive and prognostic for these patients. Despite many benefits of immunotherapy, including less long-term side effects, some treatments are fraught with immediate side effects that range from mild to severe, although most are manageable. With few downsides and the potential for disease cures, immunotherapy in the pediatric population has the potential to move to the front-line of therapeutic options.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Immunotherapy is changing the treatment landscape for specific subsets of pediatric cancer patients. |
Several monoclonal antibodies are FDA approved for patients with hematologic malignancies but only one is FDA approved for patients with solid tumors; checkpoint inhibition therapy is FDA approved in very limited subsets of pediatric patients, such as those with melanoma, Hodgkin lymphoma, and biallelic mismatch repair deficiency. |
Chimeric antigen receptor T cell (CAR-T) therapy is FDA approved for some pediatric patients with leukemia but challenges remain in leveraging such technology for patients with solid tumors. |
Issues of importance are the investigation of combinations of immunotherapies, the identification of predictive biomarkers, and specific toxicities of immunotherapies in pediatric patients. |
1 Introduction
Pediatric patients are often faced with resistant or recurrent cancers that cannot be cured by chemotherapy, radiation, or surgery. Immunotherapies have become viable therapeutic options for many cancer patients. Some of these new pharmacologic medications are changing the landscape of treatment for pediatric cancers, while the utility of others is not yet known. Monoclonal antibodies (mAbs), checkpoint inhibitors, bispecific T-cell engagers (BiTEs), and chimeric antigen receptor T cells (CAR-Ts) have been FDA approved for use in children, whereas vaccines and oncolytic virotherapy are still being studied to determine their usefulness for pediatric cancer patients. Here we review the landscape of cancer immunotherapies including efficacy and toxicity for pediatric patients as well as emerging predictive biomarkers that might enable personalized approaches.
2 Cancer Immunotherapy/Tumor Microenvironment
Immunotherapy has been documented as a cancer therapy since the late 1800 s. In 1866, Wilhelm Busch in Germany observed tumor regression in a sarcoma patient after an erysipelas infection. In 1891, orthopedic surgeon Coley demonstrated remission in some patients with inoperable sarcomas by injecting streptococcus organisms and their toxins directly into the blood stream [1,2,3,4]. Much has been learned since then about the complexities of the immune system, the tumor microenvironment, and their interactions.
The immune system is a highly complex organization of cells and proteins that cooperate to eliminate infections while maintaining tolerance against self. Innate immunity includes nonspecific proteins like complement as well as cells responsible for the initial attack against a foreign pathogen, while the adaptive system requires further development to acquire more specific engagement of targets as well as memory of the foreign antigen [5].
The interplay between the patient’s immune system and cancer includes immune surveillance, immune cell infiltration, and tumor cytolysis. Immunosurvelliance, first described by Burnet and Thomas in 1957, occurs when a tumor becomes recognized in the body as ‘foreign’ [6]. Cancer cells release pathogen-associated molecular signals (PAMPs), damage-associated molecular signals (DAMPs), and ‘foreign’ antigens typically resulting from mutations in protein-coding genes, termed neoantigens [7]. These signals are detected by the immune system, leading to a coordinated attack by the innate and adaptive immune system to recognize these tumor-associated antigens. In response, cancers often counteract this immune response by downregulation of surface markers, downregulation of antigen presentation by class I molecules, and immunosuppression mediated by cytokines and small molecules expressed in the solid tumor microenvironment [8]. Over time, cancer cells can evolve to metastasize, express different neoantigens, or express further mechanisms of immunosuppression, thus escaping detection and eradication. These steps are the framework for the model of cancer ‘immunoediting’.
Immunoediting consists of three different phases: elimination, equilibrium, and escape [9]. Elimination involves the innate and adaptive cells identifying the neoantigens, forming tumor-reactive T cells, and destroying cancer cells. Some tumor cells survive the elimination phase and enter the equilibrium stage. During the equilibrium stage, the tumor is held dormant by the adaptive immune system. Finally, tumor cells evolve and evade the immune system, leading to the escape phase with subsequent cancer cell proliferation and/or T-cell exhaustion [9, 10]. The mechanisms behind the tumor cells evading the immune system are numerous and include loss of expression of tumor antigens and down-regulation of human leukocyte antigens (HLA) from tumor surfaces (so-called ‘edited’ tumor), recruitment of immunosuppressive regulatory T cells (Tregs), myeloid-derived suppressor cells (MDSC), or tumor-associated M2-like macrophages, upregulation of inhibitory receptors (i.e., cytotoxic T lymphocyte associated protein 4 [CTLA-4], Programmed death receptor 1 [PD-1]) on T cells, or upregulation of inhibitory ligands (PD-L1) on tumor and/or stromal cells [11,12,13] (Fig. 1). By targeting this tumor microenvironment, immunotherapies aim to counteract this escape phase and reinvigorate the patient’s immune system to recognize and eliminate cancer cells. As physicians, our ability to leverage this knowledge to develop cancer immunotherapies for children is largely in its infancy.
3 Immunostimulatory Agents
As a broad category, immunostimulatory agents enhance the elimination phase of the immunoediting paradigm (Fig. 2a).
One of the best studied examples of an immunomodulatory agent is liposomal muramyl tripeptide phosphatidylethanolamine (L-MTP-PE), which is a synthetic analog of a bacterial cell wall component that induces activation of the immune system, particularly macrophages [14,15,16]. Nucleotide-binding oligomerization domain-containing protein 2 (NOD2) detects L-MTP-PE, activating NF-κβ to stimulate the production of interleukin (IL)-1β, IL-6, and tissue necrosis factor (TNF)-α, which stimulate macrophages and monocytes [17,18,19]. Initially L-MTP-PE was studied in canine bone and soft tissue sarcomas and demonstrated a median overall survival (OS) of 222 days in the L-MTP-PE-treated group compared with 77 days in the control group [5]. In 1993, a cooperative group clinical trial INT0133 (http://www.clinicaltrials.gov, NCT00631631) analyzed whether, in addition to chemotherapy with methotrexate, doxorubicin, cisplatin, L-MTP-PE and/or ifosfamide would improve outcomes. The study enrolled 662 patients and found improvement of the 6-year OS from 70 to 78% (p = 0.03) with addition of L-MTP-PE; the hazard ratio was 0.71 (95% CI 0.52–0.96). Also, in a separate analysis of 91 patients with metastasis, there was no statistically significant survival difference between the groups (p = 0.27) [20,21,22,23]. These results have led to conflicting decisions about L-MTP-PE, with approval only in the UK, Turkey, Spain, Israel, and Mexico for patients aged 2–30 years with newly diagnosed non-metastatic osteosarcoma [22]. Despite the uncertainty of the utility of L-MTP-PE, further trials may include L-MTP-PE as recent studies have shown the density of tumor-associated macrophages to be associated with poor prognosis in osteosarcoma, with another study demonstrating optimization of L-MTP-PE after induction with interferon (IFN)-γ [24, 25].
Cytokines have also been tested as immunotherapies in pediatric cancers. The IFN family of molecules bind to IFN receptors with the type I IFNs, IFN-α and IFN-β, increasing antigen presentation to T cells. Type I IFNs have been approved for many adult cancers including IFN-α2a for stage II melanoma, hairy cell leukemia, chronic myeloid leukemia, and AIDS-related Kaposi’s sarcoma, and IFN-α2b for hairy cell leukemia, malignant melanoma, and AIDS-related Kaposi’s sarcoma. Numerous clinical trials have investigated both IFN-α2a and IFN-α2b. IFN-α2a was shown to be feasible in children with resected high-risk melanoma [26]. IFN-α has been investigated in osteosarcoma as monotherapy [27] and in combination with chemotherapy [28]. These studies showed IFN-α caused improvement in metastatic-free survival and sarcoma-free survival compared with surgery alone; however, no differences were found in disease-free survival compared with chemotherapy [27, 28]. EURAMOS-1 investigated the addition of PEGylated IFN-α-2b to standard chemotherapy compared with standard chemotherapy and found no statistical differences between the two groups (3-year event-free survival (EFS) 80 vs 77%, respectively) [29]. Thus, there is a continued need for more pediatric studies to determine the usefulness of IFN-α.
IL-2 is an immunotherapy cytokine that activates T-cell proliferation and facilitates maintenance of natural killer (NK) cells [30]. In the pediatric population, IL-2 is most noted for its success in high-risk neuroblastoma when combined with an anti-GD2 monoclonal antibody and granulocyte-macrophage colony-stimulating factor (GM-CSF). Unfortunately, many other studies utilizing IL-2 have shown no antitumor effects [31, 32]. Schwinger et al. investigated high-dose IL-2 in patients with heavily pre-treated solid tumors after resection of primary and/or metastatic lesions in an attempt to maintain remission. Whether or not IL-2 played any role in the five (neuroblastoma, n = 3; osteosarcoma, n = 2) out of twelve patients who did not experience relapse is unknown [33]. However, all patients experienced significant toxicities and another high-dose IL-2 trial reported 1–2% treatment-related deaths [5]. Due to significant adverse events, it is unlikely that high-dose IL-2 will be used alone but it may be useful in lower doses to augment other immunotherapies.
4 Antibody and Antibody-Like Therapy
Antibody therapy has been used in many pediatric cancer types and has shown much promise. mAbs are engineered to attach to a specific tumor surface antigen with subsequent engagement and activation of NK cells and macrophages via Fc-receptor binding. Once activated, these cells release cytotoxic granules to kill the tumor cell in a process called antibody-dependent cellular cytotoxicity (ADCC). One of the advantages of monoclonal antibody therapy is they are tumor-specific instead of patient-specific, thus can be easily stored in clinics and hospitals without the need for local manufacturing expertise. BiTEs are based on mAb technology, but unlike mAbs, these synthetic molecules connect and activate T cells with the tumor-specific antigen. They consist of two single-chain variable fragments connected by a flexible linker. One side binds to the CD3 receptor of the T cell while the other side binds to the tumor antigen. This results in the activation of T cells and subsequent cytolysis of the tumor [34, 35] (Fig. 2b).
4.1 Monoclonal Antibody (mAb) Therapy for Pediatric Hematologic Malignancies
Rituximab, a CD20 targeting mAb, was the first mAb approved for clinical use in 1997 for adults. Its use is now approved for non-Hodgkin lymphoma (NHL) and chronic lymphocytic leukemia. In the pediatric NHL population, the addition of rituximab to standard chemotherapy increased the 1-year EFS from 81.5 to 94.2%, thus proving its value in pediatric NHL [36]. In 2011, brentuximab vedotin, an anti-CD30 mAb drug conjugate (ADC), was approved by the FDA for relapsed or refractory Hodgkin lymphoma (HL) and anaplastic large-cell lymphoma. A higher overall response rate was seen in patients with relapsed/refractory HL who received brentuximab vedotin compared with vinorelbine (76 vs 50%, respectively) [37]. Currently there is a phase III Children’s Oncology Group (COG) study combining brentuximab vedotin with gemcitabine for relapsed HL (NCT01780662).
In 2000, the FDA approved an anti-CD33 ADC, gemtuzumab ozogamicin, for acute myelogeous leukemia (AML) in adults. The drug was discontinued in 2010 due to concerns for hepatic veno-occlusive disease and a lack of statistically significant clinical benefit in an adult phase III trial [38]. Anti-CD33 mAb interest was renewed with promising data in pediatric AML, but now is primarily utilized as BiTE therapy [39]. Lastly, anti-CD22 mAbs have been utilized in adult and pediatric B-cell acute lymphoblastic leukemia (ALL) with success [40,41,42].
BiTE therapy has shown much promise in the treatment of pediatric hematologic malignancies. The CD19/anti-CD3 BiTE, blinatumomab, was FDA approved in 2017 for the treatment of relapsed or refractory B-cell ALL in the pediatric population after being approved in 2014 for adult patients. OS, remission rates, and EFS were significantly longer or higher in the blinatumomab group compared with standard chemotherapy [43, 44]. Most recently, the FDA has approved blinatumomab for the treatment of minimal residual disease positive B-cell ALL patients.
4.2 mAb Therapy for Pediatric Solid Tumors
The most notable mAb for pediatric solid tumors is the anti-GD2 mAb dinutuximab, which is FDA approved for neuroblastoma. The pivotal study was performed by COG, which found an improved 2-year EFS of 64% compared with 44% with retinoic acid alone when given in combination with IL-2 and granulocyte monocyte colony stimulating factor [45]. Currently, dinutuximab is being used in high-risk neuroblastoma in combination with chemotherapy and radiation therapy [35]. A humanized 14.18 GD2 disialoganglioside mAb conjugated to IL-2 has also shown activity in a COG phase II trial in pediatric relapsed/refractory neuroblastoma [46]. Another anti-GD2 mAb is also being investigated, a humanized GD2 antibody, Hu3F8, in high risk neuroblastoma and other GD2-positive pediatric cancers (NCT01419834).
Antibodies directed to other pediatric solid tumor targets have had less success. A phase II COG study of trastuzumab, a human epidermal growth factor receptor 2 (HER2) mAb, failed to show efficacy in osteosarcoma [47]. Another phase II COG study utilizing cixutumumab, an insulin-like growth factor 1 (IGF-1) mAb, combined with standard chemotherapy in pediatric solid tumors, showed no objective responses [48, 49]. Because GD2 is also expressed in other cancers besides neuroblastoma [50], there are numerous trials investigating anti-GD2 mAbs alone or in combination with other immunotherapies in solid tumors expressing GD2 (NCT02100930, NCT01857934, NCT01419834, NCT02502786, NCT01662804). BiTEs for pediatric solid tumors are only beginning to be explored, an example of which is a phase I study utilizing anti-GD2 BiTE in neuroblastoma and osteosarcoma (NCT02173093).
5 Adoptive Therapy
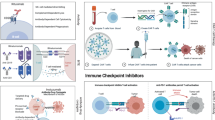
Adoptive cell therapies comprise a variety of strategies that use a patient’s cytolytic immune cells manipulated ex vivo and re-introduced to elicit an anti-tumor response [7]. There are numerous strategies that are being used in many different cancer types, including CAR-T therapy, NK cell, and tumor-infiltrating lymphocytes (TIL) therapy (Fig. 3b).
Immunotherapies for pediatric cancers. a Oncolytic virotherapy. b Adoptive therapy. c Checkpoint inhibition. See Fig. 1 for definition of cell types. CAR-T chimeric antigen receptor T cells, CTLA-4 cytotoxic T lymphocyte associated protein 4, DAMPs damage-associated molecular signals, LAG-3 Lymphocyte activation gene 3, MHC major histocompatibility complex, PAMPs pathogen-associated molecular signals, PD-L1 Programmed death ligand 1, PD-1 Programmed death receptor 1, TIM-3 T-cell immunoglobulin and mucin domain containing 3
5.1 Chimeric Antigen Receptor T Cell (CAR-T) Therapy in Pediatric Hematologic Malignancies
Tumors have the ability to evade the immune system by decreasing expression of their HLA molecules and/or tumor antigens. A therapeutic option to overcome this challenge includes CAR-Ts that are engineered to engage a specific antigen without the need of HLA presentation of tumor neoantigens. A chimeric antigen receptor is composed of an extracellular domain with an antigen-binding domain derived from a monoclonal antibody specific for a tumor surface antigen, a spacer domain, a transmembrane domain, and an intracellular signal-transducing chain of the T-cell receptor [51, 52]. The process includes harvesting autologous T cells from the patient, ex vivo expansion with proliferative cytokines, transduction of cells with an engineered T-cell receptor, and reinfusion of selected T cell into the patient [34].
The most exciting and impressive immunotherapy results have come from the CD19 CAR-T therapy for pre-B-cell ALL. Adult studies first showed profound reduction in tumor burden in a majority of patients with chemoresistant B-cell ALL [53, 54]. Soon after, pediatric studies confirmed efficacy in childhood B-cell ALL [55, 56]. In the first phase I trial, two children with refractory, heavily pretreated B-cell ALL achieved complete remissions; however, one relapsed with CD19-negative disease [57]. The full study from Children’s Hospital of Philadelphia included 25 children, with the majority being post-allogeneic stem-cell transplant, who received CD19 CAR-T therapy with a complete response in 90% of the patients [56]. From these studies, CD19 CAR-T therapy (Kymriah) was FDA approved in 2017 [35]. As illustrated by patients who experienced relapse due to antigen escape, more CAR-T therapy targets are needed for hematologic malignancies. A novel CD-22 CAR-T has been developed and shown promising preclinical data in pediatric CD19+ and CD19− B-cell ALL [58, 59]. Other CAR-T targets being investigated in the laboratory setting include CD30 [60], thymic stromal lymphopoietin receptor [61], and CD123 [62].
5.2 CAR-T Therapy in Pediatric Solid Tumors
Pediatric patients with solid tumors have experienced less efficacy of CAR-T therapy compared with those with hematologic malignancies; however, some promising results are emerging. In a phase I study using GD2 CAR-T cells in refractory neuroblastoma, 27% with active disease eventually achieved complete response with two patients achieving durable remission of > 60 months [63]. HER2 CAR-T cells have also been utilized in some solid tumors; however, during a phase I trial, an adult patient died unexpectedly from immune-mediated toxicity [64]. Concerns were raised that the HER2 CAR-T cell recognized low levels of HER2 on the lung and heart, a theory that has largely been debunked [64]. Recently, a phase I/II trial of a HER2 CAR-T in osteosarcoma (NCT00924287) showed no dose-limiting toxicities, suggesting safety in pediatric patients, and some patients experienced stable disease [65]. In patients with glioblastoma, CAR-Ts are under study against interleukin-13 receptor alpha (IL-13Rα) and epidermal growth factor receptor variant III, which are not expressed on normal CNS cells [66, 67]. Other preclinical models of solid tumors utilizing CAR-T directed against IL11-R-α and HER2, or CAR-T against IGF1-R and tyrosine-kinase-like orphan receptor 1 showed suppressed tumor growth and prolonged animal survival [34, 68].
5.3 NK Cell-Based Therapy
NK cells are lymphocytes in the innate immune system that are unlike T and B cells in that they can recognize a target without engaging specific antigens. Utilizing NK cells for the destruction of tumor cells was first performed by Kiessling et al. in mice with leukemia and has now been verified in preclinical and clinical trials [69]. AML patients have experienced the most success, with these studies confirming that haploidentical NK cells could be expanded in vivo and induce remissions [70, 71]. A pilot study of ten children with AML utilized haploidentical donor NK cells combined with IL-2 and showed remission in all patients 2 years after the treatment [72].There are a few clinical trials ongoing utilizing NK cell therapy for pediatric hematologic malignancies (NCT02763475, NCT03068819).
In the adult population, there have been some successes in patients with solid tumors utilizing NK cell therapy [73, 74]. In a pilot study of pediatric patients with refractory solid tumors, haploidentical stem cell transplant led to 50% survival at 14 months with haploidentical NK cell infusion resulting in complete and partial responses [75]. In another study, a pediatric patient with rhabdomyosarcoma experienced resolution of lung metastases following NK cell therapy [76]. There are also numerous ongoing clinical trials for pediatric solid tumors utilizing NK cell therapy (NCT01807468, NCT03420963, NCT02573896, NCT02650648, NCT02100891).
6 Oncolytic Virotherapy
Oncolytic viruses that are engineered to selectively infect and destroy cancer cells are being tested in preclinical and clinical trials for pediatric cancer. Oncolytic viral infection not only directly kills tumor cells, but also releases PAMPs and DAMPs resulting from so-called ‘immunogenic cell death,’ leading to adaptive immune responses [77] (Fig. 3a). Numerous studies have shown that intratumoral injection of talimogene laherparepvec (Imlygic or T-VEC), a herpes simplex virus type 1-derived oncolytic virus expressing GM-CSF, has caused benefit on both injected and non-injected lesions (abscopal effect) in preclinical and clinical trials [78, 79], leading to FDA approval in adult patients with melanoma.
Preclinical data have shown the benefit of oncolytic virotherapy in numerous pediatric tumor models [80,81,82,83]. In a phase I dose escalation study, a genetically modified herpes simplex virus designed to only replicate in cancer cells was utilized intratumorally in nine pediatric patients with relapsed/refractory, non-CNS solid tumors. This study suggested that intratumoral virotherapy was safe in the pediatric population, but no objective responses were seen [84]. A COG phase I study of reovirus in children with relapsed or refractory extracranial solid tumors demonstrated safety but there were no responses seen in any of the patients [85, 86]. Finally, another phase I trial in children using a modified vaccinia virus in patients with extracranial solid tumors showed safety, but again no responses were seen [87]. It should be noted that doses were not escalated to a maximum tolerated dose, suggesting that higher doses may be needed. In addition, their lack of toxicities suggest they can likely be safely combined with other cancer therapeutics including other immunotherapies, a strategy that has been successful in animal models [88,89,90]. Currently, there are three ongoing studies of oncolytic viruses in pediatric brain tumor patients using attenuated versions of herpes simplex type 1 (NCT02457845), polio virus (NCT03043391), and measles virus (NCT02962167).
7 Checkpoint Inhibitors
The anti-tumor effect of immunotherapies is not only dependent on the quantity of the immune cells present, but also the quality and function of these cells. Past endeavors have been focused on “pushing the gas pedal” by supplying the tumor microenvironment with a higher number of immune cells. Recently, researchers have recognized the importance of “taking the foot off the brake” by reducing the immunosuppressive tumor microenvironment to enhance antitumor immunity [91]. Most prominently, studies have shown that immunogenic tumors can escape immune surveillance by dampening the immune response via checkpoint ligands [92]. There have been many successes in the adult population using T-cell checkpoint inhibition, including metastatic melanoma [93], non-small-cell lung cancer (NSCLC) [94], HL [95], bladder cancer [96], and head and neck cancer [97].
CTLA-4 is an immune checkpoint that functions to prevent autoimmunity in Tregs and memory T cells [5, 98, 99]. CTLA-4 expressed on the surface of T cells binds to CD80/86 on dendritic cells (DCs), leading to deactivation of the T cell [93, 100,101,102,103]. CTLA-4 signaling is utilized by some tumor types to evade T-cell antitumor immunity [104]. Blockade of CTLA-4 signaling is FDA approved for adult and pediatric melanoma, but preclinical data also suggest other solid tumors have high expression of CTLA-4 as well [105,106,107]. A recent phase I study (NCT01445379) of pediatric patients with melanoma and other solid tumors treated with CTLA-4 blockade revealed increased cytotoxic T lymphocyte activation without increased infiltration of Tregs; however, there were no observable antitumor responses [108].
PD-1 is expressed on chronically activated T cells, B cells, DCs, and macrophages. PD-1 signaling limits the inflammatory immune response to prevent autoimmunity [109, 110]. PD-1 interacts with PD-L1 expressed on numerous cancer types and PD-L2 expressed on macrophages and DCs [5, 111, 112]. There have been a number of studies detailing the expression of PD-L1 and PD-1 on numerous pediatric cancer subtypes. Most of these studies show conflicting data on expression levels with Majzner et al. finding only 9% of 451 pediatric tumors demonstrating > 1% expression while Geoerger et al. showed 33% of patients had expression [113,114,115,116,117,118]. In the first phase I study of a PD-1 antibody in children, the Sarcoma Alliance for Research through Collaboration investigated single therapy PD-1 antibody in advanced soft tissue and bone sarcomas. Side effects were similar to the adult studies, but there were no antitumor effects noted in any tumor types except undifferentiated pleomorphic sarcoma (40% with objective response) [119]. Confirming these results, the KEYNOTE-051 study demonstrated tolerance of PD-1 therapy at adult doses, but no objective responses [118]. In March 2017, the FDA approved the anti-PD1 antibody, pembrolizumab, for the treatment of both adults and children with refractory classic HL or those who relapsed after three or more prior treatments. The KEYNOTE-087 trial included 210 adult patients with classical HL and demonstrated an overall response rate of 69% with complete remission of 22% and partial remission rate of 47% in the pembrolizumab group [120]. Efficacy in the pediatric population was extrapolated from the results in adults with safety demonstrated in the aforementioned KEYNOTE-051 study [121]. With the exception of HL, for which anti-PD1 therapy is FDA approved, single therapy checkpoint inhibition has been disappointing in pediatric clinical trials.
Lymphocyte activation gene 3 (LAG-3) and T-cell immunoglobulin and mucin domain containing 3 (TIM-3) are two immune checkpoint proteins that have gained recent interest in cancer therapy. LAG-3 is expressed on activated T cells and binds to major histocompatibility complex II (MHC II), which then causes CD8+ T-cell exhaustion and CD4+ T-cell down-regulation; this results in tumor evasion from the antitumor immune response [122, 123]. TIM-3 is expressed on activated T helper cells and TILs, which causes T-cell inhibition or apoptosis when TIM-3 binds galectin 9 or other unknown ligands [124]. Preclinical data of patients with colon carcinoma treated with PD-1/TIM-3 dual inhibition demonstrated reactivation of TILs and increased numbers of tumor regressions [125]. LAG-3 inhibition is currently in clinical trials for adult solid tumors and hematologic cancers (NCT01968109, NCT02061761) but has not yet progressed to pediatric trials.
One of the hypotheses to explain the differences in response rates between certain adult cancers compared with pediatric cancers is the mutational load or lack thereof. Checkpoint inhibitors permit stimulation of T-cell-mediated antitumor responses to neoantigens presented by tumor cells via the MHC [35] (Fig. 3c). Thus, the higher the number of neoantigens, the higher the probability of successful therapy with checkpoint inhibitors. A high mutational load in the tumor leads to more neoantigens and a more immunogenic tumor [126, 127]. The success of checkpoint inhibitors in the treatment of melanoma and NSCLC appears to be due to the high mutational load of both of these cancer types [96, 128,129,130,131,132]. In contrast, pediatric cancers in general do not have high rates of mutations [133]. The one exception involves pediatric patients with biallelic mismatch repair deficiency (bMMRD). This diagnosis leads to numerous childhood cancers and it is associated with a high mutational rate, even higher than adult cancers [134]. The FDA has approved the PD-1 antibody pembrolizumab for the treatment of mismatch repair deficiency tumors in patients 12 years and older.
8 Combination Therapies
Despite the promising developments in immunotherapy for adult oncology, fewer successes have been achieved in the pediatric setting [135, 136]. This result may in part be due to the significantly lower mutational load in pediatric cancers, which limits the number of neoantigens for immunotherapies to target. Preclinical data also demonstrate that tumors can quickly develop resistance to immunotherapy if treatment is limited to a single approach [112, 137, 138]. Therefore, combinations of multiple immunotherapeutics may be required to overcome these challenges in pediatric cancer immunotherapy.
While both PD-1 and CTLA-4 act as immune checkpoint proteins, they function on different stages of the immune response. PD-1 signaling primarily regulates CTL proliferation while CTLA-4 has a unique role inhibiting memory T-cell activity [78, 91]. Thus, combination therapy may enhance the response. PD-1/CTLA-4 signaling blockade combination therapy against adult metastatic melanoma resulted in 30% of patients experiencing a > 80% decrease in tumor volume [139, 140]. Combination therapy in preclinical metastatic osteosarcoma models resulted in 50% of treated mice experiencing complete protection from metastasis and T-cell memory against tumor rechallenge [138]. Currently, there is an ongoing trial testing PD-1/CTLA-4 signaling blockade combination therapy against recurrent/refractory pediatric cancers (NCT02304458) [34].
Another approach to improving immune checkpoint inhibition therapy is to increase the infiltration of TILs. Metastatic lesions of osteosarcoma have also been shown to have higher TIL infiltration in addition to higher PD-L1 expression compared with primary tumors, suggesting that metastatic osteosarcoma patients would benefit from TIL activation combined with PD-1 inhibition therapies [112, 141,142,143]. Other pediatric cancers can also overcome their poor immunogenic potential by combining immune checkpoint inhibition with TIL-activating therapies like chemotherapy, cancer vaccines, or T-cell-based therapy [144, 145]. Chemotherapy agents that induce immunogenic cell death [92] and therefore might potentiate immunotherapies include taxanes, cyclophosphamide, and platinum analogs [100, 146]. Nivolumab and platinum-based chemotherapy for advanced NSCLC showed 2-year OS of 62% [147]. Currently, there is a trial of nivolumab with cyclophosphamide in recurrent pediatric cancers (NCT02813135).
Cancer vaccines work by stimulating T cells with tumor neoantigens, thus leading to a greater anti-tumor response [148,149,150,151]. Cancer vaccines alone have been shown to activate antigen-specific T cells; however, these T cells eventually become dampened by the suppressive tumor microenvironment [91]. These T cells have been shown to have an increased expression of PD-1, thus suggesting a role for PD-1 blockade [150, 151]. Preclinical murine models of prostate, neuroblastoma, and pancreatic cancers have demonstrated increased immunogenicity by increasing TILs with subsequent greater anti-tumor effect when combining CLTA-4 blockade with cancer vaccines [152,153,154]. Metastatic melanoma and osteosarcoma models in particular are vulnerable to cancer vaccine and immune checkpoint combination therapy [155].
Lastly, immune checkpoint inhibition can enhance T-cell therapies such as CAR-T and BiTE therapies, which like other TILs are prone to exhaustion [156,157,158]. PD-1 expression can be increased by Treg infiltration, immunosuppressive cytokine signaling, loss of neoantigen expression, and genomic instability; ultimately this results in T-cell therapy exhaustion and tumor recurrence [156, 159,160,161,162,163]. Preclinical studies on hepatocellular and prostate cancers found that PD-1 blockade could lead to increased anti-tumor responses and T-cell proliferation [157, 158]. There are ongoing clinical trials combining immune checkpoint inhibition, cancer vaccine, and T-cell therapy (NCT02070406 and NCT02775292).
9 Challenges: Limited Biomarkers
A critical challenge that must be overcome is the identification of biomarker(s) to identify patients who would benefit from immunotherapy. Ideally, we should identify prognostic biomarkers, so that patients can be placed in appropriate individualized risk-stratified treatment groups, and predictive biomarkers, so that response can be monitored. In melanoma and NSCLC, there has been an association with high PD-L1 expression and poor prognosis [164]. There are many reports suggesting the PD-L1 expression is correlated with response to PD-1 antibody in adult patients [164,165,166,167,168]; however, there are others that have found some patients will respond without elevated levels of PD-L1 [140, 169,170,171]. Other studies have also shown that PD-L1 expression is heterogeneous within a tumor and also amongst metastatic lesions [112, 172]. Preliminary results demonstrated that patients whose NSCLC tumors express PD-L1 and IFNγ have better outcomes compared with those expressing only PD-L1, but there are not yet data in other cancer types [92].
Another potential biomarker is the ‘hot versus cold’ tumor delineation, in which hot tumors have abundant T cells whereas cold tumors lack such infiltrative cells. TILs have been associated with better patient survival in numerous cancer types [173,174,175,176,177,178,179,180,181]. One study showed that increasing the amount of TILs increased the response to PD-L1 therapy and demonstrated that PD-L1+ tumors with low levels of TILs were unresponsive to PD-L1 therapy [182]. Unfortunately, these observations have just been associations and have not been validated as true biomarkers.
A biomarker that has shown a positive correlation with response is the mutational burden of the tumor [94, 130, 167, 183, 184]. Somatic mutations lead to higher rate of neoantigens, which alert the immune system to the tumor as something foreign. One study found that patients with tumors of mismatch repair deficiency (MMRD) showed a response rate of 40% with the PD-L1 inhibitor pembrolizumab compared with a response rate of 0% in those tumors without MMRD [132]. In the pediatric population, bMMRDs have been found to have mutations of > 250 per megabase and show response to checkpoint inhibition [134]. A high frequency of nonsynonymous mutational burden, tumor antigens, and mutations in DNA repair pathways were strongly associated with therapeutic benefit after CLTA-4 and PD-1 blockade. Two studies suggest a mutational threshold of approximately 100 mutations per exome would be needed to show clinical response to checkpoint inhibition [128, 132]; however, this number has not been validated.
Besides biomarkers, it is critical that adequate immunotherapy targets are identified as well for CAR-T, mAb, and BiTE therapies. An immunotherapy target must be highly expressed on the tumor tissue and poorly expressed on normal tissue to provide a sufficient therapeutic window [185]. Optimal targets are exceedingly rare, as most targets expressed on tumors are also expressed on vital normal human tissues. It is also necessary that the target is presented on the surface of the cell for mAb therapy and CAR-T. Of the 75 National Cancer Institute consensus high value targets, two-thirds are internal antigens [7]. Efforts are underway to identify and validate adequate targets for selection.
10 Challenges: Toxicity
In general, immunotherapies are thought to exhibit fewer long-term toxicities than chemotherapy and radiation, a significant appeal in pediatrics. The immunomodulatory agents, cytokines and L-MTP-PE, are generally well tolerated. There are potentials for chills, fever, headaches, myalgias, and fatigue, especially during the first infusion. For L-MTP-PE, the reaction to the medicine will decrease in intensity with subsequent doses [22].
mAbs are also well tolerated. Acute infusion reactions are fairly common, but easily managed with antipyretics, antihistamines, and/or corticosteroids. mAbs will deplete the body of all cells that express its directed target, even if they are normal. For example, rituximab will cause B-cell depletion and humoral immunosuppression. Depending on the target, this could lead to higher risk for certain infections [186].
In adoptive T-cell transfer, toxicity poses a serious concern. Due to T-cell therapy using targets that are expressed on normal tissues, there is the potential that these normal tissues (even if expression is low) will be targeted and destroyed. The results of this attack can be life threatening. Thus, there are limitations on the choice of certain targets that can be used [187, 188]. Another toxicity associated with adoptive T-cell therapy is cytokine release, which can also be severe and fatal. Cytokine release syndrome occurs when an overwhelming amount of immune cells are activated leading to large amounts of inflammatory cytokines being released through the body, resulting in organ dysfunction and death [189].
With checkpoint inhibition, adverse drug events (ADEs) were mild to moderate and affected 70% (any Common Terminology Criteria for Adverse Events [CTCAE] grade) of patients treated with ipilimumab [105, 190]. In the pediatric population, incidence of grade 3–4 ADE was 27% with most common being pancreatitis, pneumonitis, colitis, and hepatitis when treated with ipilimumab [147]. The toxicity profile of PD-1/PD-L1 blockade was less severe than ipilimumab with grade 3–4 ADE incidence of 7–14% [191]. Toxicity of anti-PD1 is immune related, including pneumonitis, colitis, hepatitis, hypophysitis, thyroiditis, and dermatitis [105, 108, 192,193,194,195]. Most of these side effects responded to early and aggressive high-dose steroids with minimal long-term effects [193]. Interestingly, ADEs were associated with tumor responses and favorable outcomes, likely due to the fact that these patients have a more active immune system [105, 108, 192,193,194]. Another interesting phenomenon that has been seen with checkpoint inhibition and oncolytic virotherapy is so-called psuedoprogression, which occurs when the tumor lesion increases in size during therapy as part of the antitumor immune response. This phenomenon has led to a modified response assessment to allow for this immune-related response [196].
11 Conclusion
Although the ultimate contribution of immunotherapies to the outcome of pediatric cancer patients is uncertain, the landscape of therapy in the near future is likely to be quite different from traditional surgery, radiation, and chemotherapy. A variety of immunotherapies hold significant promise for children with cancer, both in terms of improving survival outcomes and reducing late effects. As we continue to increase our understanding of cancer cells, the immune system, and the tumor microenvironment, we are likely to devise novel ways in which to decrease immunosuppressive factors, interrupt pathways used for immune evasion, and identify useful biomarkers for treatment stratification and monitoring. We are optimistic that the incorporation of immunotherapies into treatment regimens will enable increased patient survival and quality of life for children with cancer.
References
Coley WB II. Contribution to the knowledge of sarcoma. Ann Surg. 1891;14(3):199–220.
McCarthy EF. The toxins of William B. Coley and the treatment of bone and soft-tissue sarcomas. Iowa Orthop J. 2006;26:154–8.
Coley WB. The treatment of malignant tumors by repeated inoculations of erysipelas. With a report of ten original cases. 1893. Clin Orthop Relat Res. 1991;262:3–11.
Nauts HC, Fowler GA, Bogatko FH. A review of the influence of bacterial infection and of bacterial products (Coley’s toxins) on malignant tumors in man; a critical analysis of 30 inoperable cases treated by Coley’s mixed toxins, in which diagnosis was confirmed by microscopic examination selected for special study. Acta Med Scand Suppl. 1953;276:1–103.
Uehara T, et al. Immunotherapy for bone and soft tissue sarcomas. Biomed Res Int. 2015;2015:820813.
Burnet M. Cancer: a biological approach. III. Viruses associated with neoplastic conditions. IV. Practical applications. Br Med J. 1957;1(5023):841–7.
Roberts SS, Chou AJ, Cheung NK. Immunotherapy of childhood sarcomas. Front Oncol. 2015;5:181.
Zitvogel L, et al. The anticancer immune response: indispensable for therapeutic success? J Clin Invest. 2008;118(6):1991–2001.
Schreiber RD, Old LJ, Smyth MJ. Cancer immunoediting: integrating immunity’s roles in cancer suppression and promotion. Science. 2011;331(6024):1565–70.
Peggs KS, Quezada SA, Allison JP. Cell intrinsic mechanisms of T-cell inhibition and application to cancer therapy. Immunol Rev. 2008;224:141–65.
Najjar YG, et al. Myeloid-derived suppressor cell subset accumulation in renal cell carcinoma parenchyma is associated with intratumoral expression of IL1beta, IL8, CXCL5, and Mip-1alpha. Clin Cancer Res. 2017;23(9):2346–55.
Laoui D, et al. Functional relationship between tumor-associated macrophages and macrophage colony-stimulating factor as contributors to cancer progression. Front Immunol. 2014;5:489.
Nishikawa H, Sakaguchi S. Regulatory T cells in cancer immunotherapy. Curr Opin Immunol. 2014;27:1–7.
Mori K, Ando K, Heymann D. Liposomal muramyl tripeptide phosphatidyl ethanolamine: a safe and effective agent against osteosarcoma pulmonary metastases. Expert Rev Anticancer Ther. 2008;8(2):151–9.
Ando K, et al. Mifamurtide for the treatment of nonmetastatic osteosarcoma. Expert Opin Pharmacother. 2011;12(2):285–92.
Meyers PA. Muramyl tripeptide (mifamurtide) for the treatment of osteosarcoma. Expert Rev Anticancer Ther. 2009;9(8):1035–49.
Geddes K, Magalhaes JG, Girardin SE. Unleashing the therapeutic potential of NOD-like receptors. Nat Rev Drug Discov. 2009;8(6):465–79.
Frampton JE. Mifamurtide: a review of its use in the treatment of osteosarcoma. Paediatr Drugs. 2010;12(3):141–53.
Steidl C, et al. Tumor-associated macrophages and survival in classic Hodgkin’s lymphoma. N Engl J Med. 2010;362(10):875–85.
Anderson PM, et al. Mifamurtide in metastatic and recurrent osteosarcoma: a patient access study with pharmacokinetic, pharmacodynamic, and safety assessments. Pediatr Blood Cancer. 2014;61(2):238–44.
Chou AJ, et al. Addition of muramyl tripeptide to chemotherapy for patients with newly diagnosed metastatic osteosarcoma: a report from the Children’s Oncology Group. Cancer. 2009;115(22):5339–48.
Kager L, Potschger U, Bielack S. Review of mifamurtide in the treatment of patients with osteosarcoma. Ther Clin Risk Manag. 2010;6:279–86.
Meyers PA, et al. Osteosarcoma: the addition of muramyl tripeptide to chemotherapy improves overall survival—a report from the Children’s Oncology Group. J Clin Oncol. 2008;26(4):633–8.
Buddingh EP, et al. Tumor-infiltrating macrophages are associated with metastasis suppression in high-grade osteosarcoma: a rationale for treatment with macrophage activating agents. Clin Cancer Res. 2011;17(8):2110–9.
Pahl JH, et al. Macrophages inhibit human osteosarcoma cell growth after activation with the bacterial cell wall derivative liposomal muramyl tripeptide in combination with interferon-gamma. J Exp Clin Cancer Res. 2014;33:27.
Navid F, et al. Feasibility of pegylated interferon in children and young adults with resected high-risk melanoma. Pediatr Blood Cancer. 2016;63(7):1207–13.
Muller CR, et al. Interferon-alpha as the only adjuvant treatment in high-grade osteosarcoma: long term results of the Karolinska Hospital series. Acta Oncol. 2005;44(5):475–80.
Winkler K, et al. Neoadjuvant chemotherapy for osteogenic sarcoma: results of a Cooperative German/Austrian study. J Clin Oncol. 1984;2(6):617–24.
Bielack SS, et al. Methotrexate, Doxorubicin, and cisplatin (MAP) plus maintenance pegylated interferon alfa-2b versus MAP alone in patients with resectable high-grade osteosarcoma and good histologic response to preoperative MAP: first results of the EURAMOS-1 good response randomized controlled trial. J Clin Oncol. 2015;33(20):2279–87.
Shaw JP, et al. Identification of a putative regulator of early T cell activation genes. Science. 1988;241(4862):202–5.
Bauer M, et al. A phase II trial of human recombinant interleukin-2 administered as a 4-day continuous infusion for children with refractory neuroblastoma, non-Hodgkin’s lymphoma, sarcoma, renal cell carcinoma, and malignant melanoma. A Childrens Cancer Group study. Cancer. 1995;75(12):2959–65.
Kalwak K, et al. Immunologic effects of intermediate-dose IL-2 i.v. after autologous hematopoietic cell transplantation in pediatric solid tumors. J Interferon Cytokine Res. 2003;23(4):173–81.
Schwinger W, et al. Feasibility of high-dose interleukin-2 in heavily pretreated pediatric cancer patients. Ann Oncol. 2005;16(7):1199–206.
Lettieri CK, et al. Progress and opportunities for immune therapeutics in osteosarcoma. Immunotherapy. 2016;8(10):1233–44.
Majzner RG, Heitzeneder S, Mackall CL. Harnessing the immunotherapy revolution for the treatment of childhood cancers. Cancer Cell. 2017;31(4):476–85.
Minard-Colin V, et al. Results of the randomized intergroup trial inter-B-NHL Ritux 2010 for children and adolescents with high risk B-cell non Hodgkin’s lymphoma and mature acute leukemia: evaluation of rituximab efficacy in addition to standard LMB chemotherapy regimen. J Clin Oncol. 2016;34(15_suppl):10507.
Younes A, et al. Results of a pivotal phase II study of brentuximab vedotin for patients with relapsed or refractory Hodgkin’s lymphoma. J Clin Oncol. 2012;30(18):2183–9.
Loke J, et al. Mylotarg has potent anti-leukaemic effect: a systematic review and meta-analysis of anti-CD33 antibody treatment in acute myeloid leukaemia. Ann Hematol. 2015;94(3):361–73.
Laing AA, et al. Unlocking the potential of anti-CD33 therapy in adult and childhood acute myeloid leukemia. Exp Hematol. 2017;54:40–50.
Kantarjian H, et al. Inotuzumab ozogamicin, an anti-CD22-calecheamicin conjugate, for refractory and relapsed acute lymphocytic leukaemia: a phase 2 study. Lancet Oncol. 2012;13(4):403–11.
Kantarjian HM, et al. Inotuzumab ozogamicin versus standard therapy for acute lymphoblastic leukemia. N Engl J Med. 2016;375(8):740–53.
Kantarjian HM, Vandendries E, Advani AS. Inotuzumab ozogamicin for acute lymphoblastic leukemia. N Engl J Med. 2016;375(21):2100–1.
Kantarjian H, et al. Blinatumomab versus chemotherapy for advanced acute lymphoblastic leukemia. N Engl J Med. 2017;376(9):836–47.
von Stackelberg A, et al. Phase I/phase II study of blinatumomab in pediatric patients with relapsed/refractory acute lymphoblastic leukemia. J Clin Oncol. 2016;34(36):4381–9.
Yu AL, et al. Anti-GD2 antibody with GM-CSF, interleukin-2, and isotretinoin for neuroblastoma. N Engl J Med. 2010;363(14):1324–34.
Shusterman S, et al. Antitumor activity of hu14.18-IL2 in patients with relapsed/refractory neuroblastoma: a Children’s Oncology Group (COG) phase II study. J Clin Oncol. 2010;28(33):4969–75.
Ebb D, et al. Phase II trial of trastuzumab in combination with cytotoxic chemotherapy for treatment of metastatic osteosarcoma with human epidermal growth factor receptor 2 overexpression: a report from the children’s oncology group. J Clin Oncol. 2012;30(20):2545–51.
Weigel B, et al. Phase 2 trial of cixutumumab in children, adolescents, and young adults with refractory solid tumors: a report from the Children’s Oncology Group. Pediatr Blood Cancer. 2014;61(3):452–6.
Malempati S, et al. Phase I/II trial and pharmacokinetic study of cixutumumab in pediatric patients with refractory solid tumors and Ewing sarcoma: a report from the Children’s Oncology Group. J Clin Oncol. 2012;30(3):256–62.
Heiner JP, et al. Localization of GD2-specific monoclonal antibody 3F8 in human osteosarcoma. Cancer Res. 1987;47(20):5377–81.
Wolfl M, et al. Expression of MHC class I, MHC class II, and cancer germline antigens in neuroblastoma. Cancer Immunol Immunother. 2005;54(4):400–6.
Garcia-Lora A, Algarra I, Garrido F. MHC class I antigens, immune surveillance, and tumor immune escape. J Cell Physiol. 2003;195(3):346–55.
Porter DL, et al. Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N Engl J Med. 2011;365(8):725–33.
Brentjens RJ, et al. Safety and persistence of adoptively transferred autologous CD19-targeted T cells in patients with relapsed or chemotherapy refractory B-cell leukemias. Blood. 2011;118(18):4817–28.
Lee DW, et al. T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet. 2015;385(9967):517–28.
Maude SL, et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N Engl J Med. 2014;371(16):1507–17.
Grupp SA, et al. Chimeric antigen receptor-modified T cells for acute lymphoid leukemia. N Engl J Med. 2013;368(16):1509–18.
Haso W, et al. Anti-CD22-chimeric antigen receptors targeting B-cell precursor acute lymphoblastic leukemia. Blood. 2013;121(7):1165–74.
Wayne AS, et al. Phase 1 study of the anti-CD22 immunotoxin moxetumomab pasudotox for childhood acute lymphoblastic leukemia. Blood. 2017;130(14):1620–7.
Di Stasi A, et al. T lymphocytes coexpressing CCR4 and a chimeric antigen receptor targeting CD30 have improved homing and antitumor activity in a Hodgkin tumor model. Blood. 2009;113(25):6392–402.
Qin H, et al. Eradication of B-ALL using chimeric antigen receptor-expressing T cells targeting the TSLPR oncoprotein. Blood. 2015;126(5):629–39.
Ruella M, et al. Dual CD19 and CD123 targeting prevents antigen-loss relapses after CD19-directed immunotherapies. J Clin Invest. 2016;126(10):3814–26.
Louis CU, et al. Antitumor activity and long-term fate of chimeric antigen receptor-positive T cells in patients with neuroblastoma. Blood. 2011;118(23):6050–6.
Morgan RA, et al. Case report of a serious adverse event following the administration of T cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol Ther. 2010;18(4):843–51.
Ahmed N, et al. Human epidermal growth factor receptor 2 (HER2) -specific chimeric antigen receptor-modified T cells for the immunotherapy of HER2-positive sarcoma. J Clin Oncol. 2015;33(15):1688–96.
Kahlon KS, et al. Specific recognition and killing of glioblastoma multiforme by interleukin 13-zetakine redirected cytolytic T cells. Cancer Res. 2004;64(24):9160–6.
Morgan RA, et al. Recognition of glioma stem cells by genetically modified T cells targeting EGFRvIII and development of adoptive cell therapy for glioma. Hum Gene Ther. 2012;23(10):1043–53.
Huang X, et al. IGF1R- and ROR1-specific CAR T cells as a potential therapy for high risk sarcomas. PLoS One. 2015;10(7):e0133152.
Kiessling R, et al. “Natural” killer cells in the mouse. II. Cytotoxic cells with specificity for mouse Moloney leukemia cells. Characteristics of the killer cell. Eur J Immunol. 1975;5(2):117–21.
Rosenberg SA, et al. A progress report on the treatment of 157 patients with advanced cancer using lymphokine-activated killer cells and interleukin-2 or high-dose interleukin-2 alone. N Engl J Med. 1987;316(15):889–97.
Miller JS, et al. Successful adoptive transfer and in vivo expansion of human haploidentical NK cells in patients with cancer. Blood. 2005;105(8):3051–7.
Rubnitz JE, et al. NKAML: a pilot study to determine the safety and feasibility of haploidentical natural killer cell transplantation in childhood acute myeloid leukemia. J Clin Oncol. 2010;28(6):955–9.
Geller MA, et al. A phase II study of allogeneic natural killer cell therapy to treat patients with recurrent ovarian and breast cancer. Cytotherapy. 2011;13(1):98–107.
Iliopoulou EG, et al. A phase I trial of adoptive transfer of allogeneic natural killer cells in patients with advanced non-small cell lung cancer. Cancer Immunol Immunother. 2010;59(12):1781–9.
Perez-Martinez A, et al. Natural killer cells can exert a graft-vs-tumor effect in haploidentical stem cell transplantation for pediatric solid tumors. Exp Hematol. 2012;40(11):882.e1–891.e1.
Perez-Martinez A, et al. KIR-HLA receptor-ligand mismatch associated with a graft-versus-tumor effect in haploidentical stem cell transplantation for pediatric metastatic solid tumors. Pediatr Blood Cancer. 2009;53(1):120–4.
Yin J, Markert JM, Leavenworth JW. Modulation of the intratumoral immune landscape by oncolytic herpes simplex virus virotherapy. Front Oncol. 2017;7:136.
Kyi C, Postow MA. Immune checkpoint inhibitor combinations in solid tumors: opportunities and challenges. Immunotherapy. 2016;8(7):821–37.
Andtbacka RH, et al. Talimogene laherparepvec improves durable response rate in patients with advanced melanoma. J Clin Oncol. 2015;33(25):2780–8.
Wang PY, et al. Neuroblastomas vary widely in their sensitivities to herpes simplex virotherapy unrelated to virus receptors and susceptibility. Gene Ther. 2016;23(2):135–43.
Morton CL, et al. Initial testing of the replication competent Seneca Valley virus (NTX-010) by the pediatric preclinical testing program. Pediatr Blood Cancer. 2010;55(2):295–303.
Hingorani P, et al. Systemic administration of reovirus (Reolysin) inhibits growth of human sarcoma xenografts. Cancer. 2011;117(8):1764–74.
Lun X, et al. Double-deleted vaccinia virus in virotherapy for refractory and metastatic pediatric solid tumors. Mol Oncol. 2013;7(5):944–54.
Streby KA, et al. Intratumoral injection of HSV1716, an oncolytic herpes virus, is safe and shows evidence of immune response and viral replication in young cancer patients. Clin Cancer Res. 2017;23(14):3566–74.
Comins C, et al. REO-10: a phase I study of intravenous reovirus and docetaxel in patients with advanced cancer. Clin Cancer Res. 2010;16(22):5564–72.
Vidal L, et al. A phase I study of intravenous oncolytic reovirus type 3 Dearing in patients with advanced cancer. Clin Cancer Res. 2008;14(21):7127–37.
Cripe TP, et al. Phase 1 study of intratumoral Pexa-Vec (JX-594), an oncolytic and immunotherapeutic vaccinia virus, in pediatric cancer patients. Mol Ther. 2015;23(3):602–8.
Chen CY, et al. Cooperation of oncolytic herpes virotherapy and PD-1 blockade in murine rhabdomyosarcoma models. Sci Rep. 2017;7(1):2396.
Hutzen B, et al. TGF-beta inhibition improves oncolytic herpes viroimmunotherapy in murine models of rhabdomyosarcoma. Mol Ther Oncolytics. 2017;7:17–26.
Meyers DE, et al. Current immunotherapeutic strategies to enhance oncolytic virotherapy. Front Oncol. 2017;7:114.
Morse MA, Lyerly HK. Checkpoint blockade in combination with cancer vaccines. Vaccine. 2015;33(51):7377–85.
Wagner LM, Adams VR. Targeting the PD-1 pathway in pediatric solid tumors and brain tumors. Onco Targets Ther. 2017;10:2097–106.
Postow MA, Callahan MK, Wolchok JD. Immune checkpoint blockade in cancer therapy. J Clin Oncol. 2015;33(17):1974–82.
Brahmer J, et al. Nivolumab versus docetaxel in advanced squamous-cell non-small-cell lung cancer. N Engl J Med. 2015;373(2):123–35.
Ansell SM, et al. PD-1 blockade with nivolumab in relapsed or refractory Hodgkin’s lymphoma. N Engl J Med. 2015;372(4):311–9.
Powles T. Immune checkpoint inhibitors for urologic cancer: the tip of the iceberg? Eur Urol. 2015;68(2):280–2.
Topalian SL, Drake CG, Pardoll DM. Immune checkpoint blockade: a common denominator approach to cancer therapy. Cancer Cell. 2015;27(4):450–61.
Pedicord VA, et al. Single dose of anti-CTLA-4 enhances CD8 + T-cell memory formation, function, and maintenance. Proc Natl Acad Sci USA. 2011;108(1):266–71.
Jain N, et al. Dual function of CTLA-4 in regulatory T cells and conventional T cells to prevent multiorgan autoimmunity. Proc Natl Acad Sci USA. 2010;107(4):1524–8.
Callahan MK, Postow MA, Wolchok JD. CTLA-4 and PD-1 pathway blockade: combinations in the clinic. Front Oncol. 2014;4:385.
Linsley PS, Ledbetter JA. The role of the CD28 receptor during T cell responses to antigen. Annu Rev Immunol. 1993;11:191–212.
June CH, et al. The B7 and CD28 receptor families. Immunol Today. 1994;15(7):321–31.
Thompson CB, et al. CD28 activation pathway regulates the production of multiple T-cell-derived lymphokines/cytokines. Proc Natl Acad Sci USA. 1989;86(4):1333–7.
Leach DR, Krummel MF, Allison JP. Enhancement of antitumor immunity by CTLA-4 blockade. Science. 1996;271(5256):1734–6.
Wolchok JD, et al. Ipilimumab monotherapy in patients with pretreated advanced melanoma: a randomised, double-blind, multicentre, phase 2, dose-ranging study. Lancet Oncol. 2010;11(2):155–64.
Hingorani P, et al. Increased CTLA-4(+) T cells and an increased ratio of monocytes with loss of class II (CD14(+) HLA-DR(lo/neg)) found in aggressive pediatric sarcoma patients. J Immunother Cancer. 2015;3:35.
Contardi E, et al. CTLA-4 is constitutively expressed on tumor cells and can trigger apoptosis upon ligand interaction. Int J Cancer. 2005;117(4):538–50.
Merchant MS, et al. Phase I clinical trial of ipilimumab in pediatric patients with advanced solid tumors. Clin Cancer Res. 2016;22(6):1364–70.
Pauken KE, Wherry EJ. Overcoming T cell exhaustion in infection and cancer. Trends Immunol. 2015;36(4):265–76.
Staron MM, et al. The transcription factor FoxO1 sustains expression of the inhibitory receptor PD-1 and survival of antiviral CD8(+) T cells during chronic infection. Immunity. 2014;41(5):802–14.
Heymann MF, Brown HK, Heymann D. Drugs in early clinical development for the treatment of osteosarcoma. Expert Opin Investig Drugs. 2016;25(11):1265–80.
Lussier DM, et al. Enhanced T-cell immunity to osteosarcoma through antibody blockade of PD-1/PD-L1 interactions. J Immunother. 2015;38(3):96–106.
Paydas S, et al. Clinical and prognostic significance of PD-1 and PD-L1 expression in sarcomas. Med Oncol. 2016;33(8):93.
Kim C, et al. Prognostic implications of PD-L1 expression in patients with soft tissue sarcoma. BMC Cancer. 2016;16:434.
Inaguma S, et al. Comprehensive immunohistochemical study of programmed cell death ligand 1 (PD-L1): analysis in 5536 cases revealed consistent expression in trophoblastic tumors. Am J Surg Pathol. 2016;40(8):1133–42.
van Erp AEM, et al. Expression and clinical association of programmed cell death-1, programmed death-ligand-1 and CD8(+) lymphocytes in primary sarcomas is subtype dependent. Oncotarget. 2017;8(41):71371–84.
Majzner RG, et al. Assessment of programmed death-ligand 1 expression and tumor-associated immune cells in pediatric cancer tissues. Cancer. 2017;123(19):3807–15.
Geoerger B, et al. Phase 1/2 KEYNOTE-051 study of pembrolizumab (pembro) in pediatric patients (pts) with advanced melanoma or a PD-L1 + advanced, relapsed, or refractory solid tumor or lymphoma. J Clin Oncol. 2017;35(15_suppl):10525.
Tawbi HA, et al. Pembrolizumab in advanced soft-tissue sarcoma and bone sarcoma (SARC028): a multicentre, two-cohort, single-arm, open-label, phase 2 trial. Lancet Oncol. 2017;18(11):1493–501.
Chen R, et al. Phase II study of the efficacy and safety of pembrolizumab for relapsed/refractory classic hodgkin lymphoma. J Clin Oncol. 2017;35(19):2125–32.
Pembrolizumab (KEYTRUDA) for classical Hodgkin lymphoma. 2017 3/15/2017 [cited 2018 April 30]. https://www.fda.gov/Drugs/InformationOnDrugs/ApprovedDrugs/ucm546893.htm. Accessed 30 Apr 2018.
Huard B, et al. T cell major histocompatibility complex class II molecules down-regulate CD4+ T cell clone responses following LAG-3 binding. Eur J Immunol. 1996;26(5):1180–6.
Sierro S, Romero P, Speiser DE. The CD4-like molecule LAG-3, biology and therapeutic applications. Expert Opin Ther Targets. 2011;15(1):91–101.
Sanchez-Fueyo A, et al. Tim-3 inhibits T helper type 1-mediated auto- and alloimmune responses and promotes immunological tolerance. Nat Immunol. 2003;4(11):1093–101.
Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012;12(4):252–64.
Champiat S, et al. Exomics and immunogenics: bridging mutational load and immune checkpoints efficacy. Oncoimmunology. 2014;3(1):e27817.
Kansara M, et al. Translational biology of osteosarcoma. Nat Rev Cancer. 2014;14(11):722–35.
Snyder A, et al. Genetic basis for clinical response to CTLA-4 blockade in melanoma. N Engl J Med. 2014;371(23):2189–99.
Snyder A, Wolchok JD, Chan TA. Genetic basis for clinical response to CTLA-4 blockade. N Engl J Med. 2015;372(8):783.
Rizvi NA, et al. Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science. 2015;348(6230):124–8.
Herbst RS, et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature. 2014;515(7528):563–7.
Le DT, et al. PD-1 blockade in tumors with mismatch-repair deficiency. N Engl J Med. 2015;372(26):2509–20.
Lawrence MS, et al. Mutational heterogeneity in cancer and the search for new cancer-associated genes. Nature. 2013;499(7457):214–8.
Shlien A, et al. Combined hereditary and somatic mutations of replication error repair genes result in rapid onset of ultra-hypermutated cancers. Nat Genet. 2015;47(3):257–62.
Huang MA, Krishnadas DK, Lucas KG. Cellular and antibody based approaches for pediatric cancer immunotherapy. J Immunol Res. 2015;2015:675269.
Capitini CM, et al. Immunotherapy in pediatric malignancies: current status and future perspectives. Future Oncol. 2014;10(9):1659–78.
Korkolopoulou P, et al. Loss of antigen-presenting molecules (MHC class I and TAP-1) in lung cancer. Br J Cancer. 1996;73(2):148–53.
Lussier DM, et al. Combination immunotherapy with alpha-CTLA-4 and alpha-PD-L1 antibody blockade prevents immune escape and leads to complete control of metastatic osteosarcoma. J Immunother Cancer. 2015;3:21.
Wolchok JD, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369(2):122–33.
Larkin J, et al. Combined nivolumab and ipilimumab or monotherapy in untreated melanoma. N Engl J Med. 2015;373(1):23–34.
Sundara YT, et al. Increased PD-L1 and T-cell infiltration in the presence of HLA class I expression in metastatic high-grade osteosarcoma: a rationale for T-cell-based immunotherapy. Cancer Immunol Immunother. 2017;66(1):119–28.
Koirala P, et al. Immune infiltration and PD-L1 expression in the tumor microenvironment are prognostic in osteosarcoma. Sci Rep. 2016;6:30093.
Aoki T, et al. Low frequency of programmed death ligand 1 expression in pediatric cancers. Pediatr Blood Cancer. 2016;63(8):1461–4.
De Henau O, et al. Overcoming resistance to checkpoint blockade therapy by targeting PI3Kgamma in myeloid cells. Nature. 2016;539(7629):443–7.
Swart M, Verbrugge I, Beltman JB. Combination approaches with immune-checkpoint blockade in cancer therapy. Front Oncol. 2016;6:233.
D’Angelo SP, et al. Sarcoma immunotherapy: past approaches and future directions. Sarcoma. 2014;2014:391967.
Park JA, Cheung NV. Limitations and opportunities for immune checkpoint inhibitors in pediatric malignancies. Cancer Treat Rev. 2017;58:22–33.
Sheikh NA, et al. Sipuleucel-T immune parameters correlate with survival: an analysis of the randomized phase 3 clinical trials in men with castration-resistant prostate cancer. Cancer Immunol Immunother. 2013;62(1):137–47.
Walter S, et al. Multipeptide immune response to cancer vaccine IMA901 after single-dose cyclophosphamide associates with longer patient survival. Nat Med. 2012;18(8):1254–61.
Fu J, et al. Preclinical evidence that PD1 blockade cooperates with cancer vaccine TEGVAX to elicit regression of established tumors. Cancer Res. 2014;74(15):4042–52.
Soares KC, et al. PD-1/PD-L1 blockade together with vaccine therapy facilitates effector T-cell infiltration into pancreatic tumors. J Immunother. 2015;38(1):1–11.
Hurwitz AA, et al. CTLA-4 blockade synergizes with tumor-derived granulocyte-macrophage colony-stimulating factor for treatment of an experimental mammary carcinoma. Proc Natl Acad Sci USA. 1998;95(17):10067–71.
Hurwitz AA, et al. Combination immunotherapy of primary prostate cancer in a transgenic mouse model using CTLA-4 blockade. Cancer Res. 2000;60(9):2444–8.
Williams EL, et al. Immunomodulatory monoclonal antibodies combined with peptide vaccination provide potent immunotherapy in an aggressive murine neuroblastoma model. Clin Cancer Res. 2013;19(13):3545–55.
Sierro SR, et al. Combination of lentivector immunization and low-dose chemotherapy or PD-1/PD-L1 blocking primes self-reactive T cells and induces anti-tumor immunity. Eur J Immunol. 2011;41(8):2217–28.
Sun C, Dotti G, Savoldo B. Utilizing cell-based therapeutics to overcome immune evasion in hematologic malignancies. Blood. 2016;127(26):3350–9.
Morales-Kastresana A, et al. Combined immunostimulatory monoclonal antibodies extend survival in an aggressive transgenic hepatocellular carcinoma mouse model. Clin Cancer Res. 2013;19(22):6151–62.
Slovin SF, et al. Ipilimumab alone or in combination with radiotherapy in metastatic castration-resistant prostate cancer: results from an open-label, multicenter phase I/II study. Ann Oncol. 2013;24(7):1813–21.
Zhao X, et al. Silencing of B7-H3 increases gemcitabine sensitivity by promoting apoptosis in pancreatic carcinoma. Oncol Lett. 2013;5(3):805–12.
Zhu X, et al. Severe cerebral edema following nivolumab treatment for pediatric glioblastoma: case report. J Neurosurg Pediatr. 2017;19(2):249–53.
Zitvogel L, Kepp O, Kroemer G. Immune parameters affecting the efficacy of chemotherapeutic regimens. Nat Rev Clin Oncol. 2011;8(3):151–60.
Zinselmeyer BH, et al. PD-1 promotes immune exhaustion by inducing antiviral T cell motility paralysis. J Exp Med. 2013;210(4):757–74.
Krupka C, et al. Blockade of the PD-1/PD-L1 axis augments lysis of AML cells by the CD33/CD3 BiTE antibody construct AMG 330: reversing a T-cell-induced immune escape mechanism. Leukemia. 2016;30(2):484–91.
Gibney GT, Weiner LM, Atkins MB. Predictive biomarkers for checkpoint inhibitor-based immunotherapy. Lancet Oncol. 2016;17(12):e542–51.
Topalian SL, et al. Mechanism-driven biomarkers to guide immune checkpoint blockade in cancer therapy. Nat Rev Cancer. 2016;16(5):275–87.
Patel SP, Kurzrock R. PD-L1 Expression as a Predictive Biomarker in Cancer Immunotherapy. Mol Cancer Ther. 2015;14(4):847–56.
Reck M, et al. Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer. N Engl J Med. 2016;375(19):1823–33.
Maleki Vareki S, Garrigos C, Duran I. Biomarkers of response to PD-1/PD-L1 inhibition. Crit Rev Oncol Hematol. 2017;116:116–24.
Antonia SJ, et al. Nivolumab alone and nivolumab plus ipilimumab in recurrent small-cell lung cancer (CheckMate 032): a multicentre, open-label, phase 1/2 trial. Lancet Oncol. 2016;17(7):883–95.
Postow MA, et al. Nivolumab and ipilimumab versus ipilimumab in untreated melanoma. N Engl J Med. 2015;372(21):2006–17.
Festino L, et al. Cancer treatment with anti-PD-1/PD-L1 agents: is PD-L1 expression a biomarker for patient selection? Drugs. 2016;76(9):925–45.
Callea M, et al. Differential expression of PD-L1 between primary and metastatic sites in clear-cell renal cell carcinoma. Cancer Immunol Res. 2015;3(10):1158–64.
Adams S, et al. Tumor infiltrating lymphocytes (TILs) improve prognosis in patients with triple negative breast cancer (TNBC). Oncoimmunology. 2015;4(9):e985930.
Mina M, et al. Tumor-infiltrating T lymphocytes improve clinical outcome of therapy-resistant neuroblastoma. Oncoimmunology. 2015;4(9):e1019981.
Vassilakopoulou M, et al. Evaluation of PD-L1 expression and associated tumor-infiltrating lymphocytes in laryngeal squamous cell carcinoma. Clin Cancer Res. 2016;22(3):704–13.
Berghuis D, et al. Pro-inflammatory chemokine-chemokine receptor interactions within the Ewing sarcoma microenvironment determine CD8(+) T-lymphocyte infiltration and affect tumour progression. J Pathol. 2011;223(3):347–57.
Kim JR, et al. Tumor infiltrating PD1-positive lymphocytes and the expression of PD-L1 predict poor prognosis of soft tissue sarcomas. PLoS One. 2013;8(12):e82870.
Fujii H, et al. CD8(+) tumor-infiltrating lymphocytes at primary sites as a possible prognostic factor of cutaneous angiosarcoma. Int J Cancer. 2014;134(10):2393–402.
Schatton T, et al. Tumor-infiltrating lymphocytes and their significance in melanoma prognosis. Methods Mol Biol. 2014;1102:287–324.
Stanton SE, Disis ML. Clinical significance of tumor-infiltrating lymphocytes in breast cancer. J Immunother Cancer. 2016;4:59.
Dieu-Nosjean MC, et al. Long-term survival for patients with non-small-cell lung cancer with intratumoral lymphoid structures. J Clin Oncol. 2008;26(27):4410–7.
Tang H, et al. Facilitating T cell infiltration in tumor microenvironment overcomes resistance to PD-L1 blockade. Cancer Cell. 2016;29(3):285–96.
Borghaei H, et al. Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer. N Engl J Med. 2015;373(17):1627–39.
Robert C, et al. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med. 2011;364(26):2517–26.
Cheever MA, et al. The prioritization of cancer antigens: a national cancer institute pilot project for the acceleration of translational research. Clin Cancer Res. 2009;15(17):5323–37.
Wayne AS, Capitini CM, Mackall CL. Immunotherapy of childhood cancer: from biologic understanding to clinical application. Curr Opin Pediatr. 2010;22(1):2–11.
Morgan RA, et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science. 2006;314(5796):126–9.
Corrigan-Curay J, et al. T-cell immunotherapy: looking forward. Mol Ther. 2014;22(9):1564–74.
Topp MS, et al. Safety and activity of blinatumomab for adult patients with relapsed or refractory B-precursor acute lymphoblastic leukaemia: a multicentre, single-arm, phase 2 study. Lancet Oncol. 2015;16(1):57–66.
Hodi FS, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363(8):711–23.
Abdel-Rahman O, et al. Treatment-related death in cancer patients treated with immune checkpoint inhibitors: a systematic review and meta-analysis. Clin Oncol (R Coll Radiol). 2017;29(4):218–30.
Attia P, et al. Autoimmunity correlates with tumor regression in patients with metastatic melanoma treated with anti-cytotoxic T-lymphocyte antigen-4. J Clin Oncol. 2005;23(25):6043–53.
Yang JC, et al. Ipilimumab (anti-CTLA4 antibody) causes regression of metastatic renal cell cancer associated with enteritis and hypophysitis. J Immunother. 2007;30(8):825–30.
Fecher LA, et al. Ipilimumab and its toxicities: a multidisciplinary approach. Oncologist. 2013;18(6):733–43.
Abdel-Wahab N, Shah M, Suarez-Almazor ME. Adverse events associated with immune checkpoint blockade in patients with cancer: a systematic review of case reports. PLoS One. 2016;11(7):e0160221.
Nishino M. Immune-related response evaluations during immune-checkpoint inhibitor therapy: establishing a “common language” for the new arena of cancer treatment. J Immunother Cancer. 2016;4:30.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No external funding was used in the preparation of this manuscript.
Conflict of interest
Mary Frances Wedekind, Nick Denton, Chun-Yu Chen, and Timothy Cripe declare that they have no conflicts of interest that might be relevant to the contents of this manuscript.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Wedekind, M.F., Denton, N.L., Chen, CY. et al. Pediatric Cancer Immunotherapy: Opportunities and Challenges. Pediatr Drugs 20, 395–408 (2018). https://doi.org/10.1007/s40272-018-0297-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40272-018-0297-x