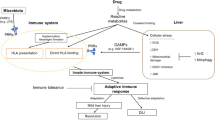
Abstract
Numerous publications contributed to the expanding knowledge base about drug-induced liver injury (DILI) in 2015. New findings from the US Drug Induced Liver Injury Network (DILIN) in their most recently updated registry include a 1- to 3-week delay in the appearance of acute DILI from short-course antibiotics such as cefazolin. They corroborated the finding that acute DILI in patients with underlying liver disease was far more severe and potentially fatal than in patients without liver disease. The only drug that seemed to have an increased risk of hepatotoxicity in these patients was azithromycin. While nearly one in six patients with acute DILI had persistently elevated liver tests at 6 months, and results for 75 % of these patients continued to be abnormal at 12 months, most of these “chronic” injury cases were relatively minor and the result of cholestatic hepatotoxins. Newly described DILI agents include tolvaptan, as well as some new direct-acting antiviral protease inhibitors for chronic hepatitis C. The latter have been associated with serious acute hepatitis, hyperbilirubinemia, and decompensation. Herbal hepatotoxicity continues to be increasingly reported, although applying causality assessment to these cases can, in fact, be more challenging than with prescription drugs. As important as cases with DILI, the class of PCSK9 inhibitors used to lower low-density lipoprotein (LDL) cholesterol have not been associated with significant liver injury, in contrast with other lipid-lowering agents. With respect to pharmacologic DILI risk factors, new data show that drugs metabolized by cytochrome P450 enzymes had a nearly four times higher likelihood of causing DILI. Interestingly, high lipophilicity, which was previously felt to be a risk factor for DILI, was not found to be associated, although more study is needed to confirm this observation. While human leukocyte antigen (HLA) genotypes have been linked to several specific agents, the role of such testing in the general population remains undefined due to the currently low positive and negative predictive values of the available tests. New DILI biomarkers, specifically microRNA-122 and keratin-18, among others, appear to have the necessary predictive value to determine the prognosis and outcome of patients with paracetamol (acetaminophen [AAP])-induced acute liver failure (ALF), and may be of great benefit in deciding who requires N-acetylcysteine (NAC), and for what duration. Treatment options for other forms of DILI remain limited; no firm conclusions can currently be drawn for the use of NAC in non-AAP ALF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The US Drug-Induced Liver Injury Network (DILIN) remains an important resource for analyzing DILI and continues to provide new information about idiosyncratic liver injury in an increasing number of agents as well as subpopulations and clinical scenarios. |
Herbal and dietary supplements have been gaining popularity in westernized nations but also represent an increasing proportion of DILI cases seen in the USA and abroad. |
The field of DILI pharmacogenomics continues to expand; however, its utility in identifying patients at the highest risk of developing acute DILI is currently limited by relatively low positive and negative predictive values. |
The efforts of regional and global consortia to identify better means of diagnosing and predicting hepatotoxicity are poised to improve the hepatic safety of current and future drugs. |
1 Introduction
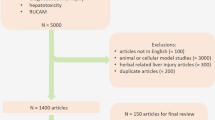
The literature dealing with drug-induced liver injury (DILI) continues to expand at a rapid pace [1]. A query of PubMed using the search terms DILI or hepatotoxicity yielded over 1500 publications from January to December 2015. These included several reviews as well as numerous case series of DILI caused by new agents or established agents and an increasing number of papers describing liver injury caused by herbal and dietary supplements (HDS) and weight loss supplements.
New and updated DILI registries and information on the epidemiology and outcomes of DILI were also among important new information published this year. Advances in the field of pharmacogenomics and the use of new biomarkers in the diagnostic and prognostic evaluation of DILI rounded out the progress being made. However, as stated by Senior [2], “Many issues [in DILI] still remain to be resolved.” This review highlights the most relevant reports and studies addressing many of these unresolved topics in the expanding knowledge base about DILI.
Without a specific DILI biomarker [3], drug-induced hepatotoxicity generally remains a “diagnosis of exclusion” [4]. Given the large number of agents described as causing liver injury (>670 in the LiverTox database [5], and >1000 when chemical agents are included [6]), and the ever-expanding number of potentially confounding causes, our ability to confidently assign causality to a particular drug, chemical, or herbal agent alone has in fact become increasingly complex [1, 7, 8]. As a case in point, hepatitis E virus (HEV) has been found retrospectively to have been the cause of a number of instances of what was initially felt to be acute DILI [9, 10]. But such serologic testing can be inaccurate [11], leading to the fact that no FDA-approved HEV tests are currently available [12]. Similarly, being able to distinguish between drug injury in a patient with underlying liver disease or hepatobiliary malignancy is often extremely difficult [13].
In a critical re-analysis of the 671 drugs currently listed in the LiverTox database, Björnsson and Hoofnagle [5] found that nearly half (n = 318; 47 %), when subjected to a stringent causality assessment, lacked convincing evidence of hepatotoxicity as they had no existing published case reports. For now, the opinions offered by experienced hepatologists and others working in the field of DILI remain the most “accurate” and efficient means of assessing cases in the clinic and during clinical trials with old and new agents [7]. While a specific diagnostic biochemical or other biomarker is destined to supplant such “expert opinion” in the future, learning how to assess suspected DILI or HDS-related cases with the data at hand remains an ongoing challenge.
1.1 Methods
We conducted a MEDLINE/PubMed search of the terms “drug-induced liver injury”, “DILI”, and “hepatotoxicity” and reviewed the recent literature to identify articles of potential interest. We attempted to look at all articles published during 2015, including some we became aware of by 31 December 2015 that were initially available only online, to ensure a complete database. We felt these particular “ahead of print” reports were valuable additions for inclusion in this review. As we have done in prior reviews [14], we selected publications dealing primarily with human DILI that we felt had the greatest impact on the field of drug-induced hepatotoxicity during the past year. Priority in our selection process was given to reports of hepatotoxins from randomized controlled clinical trials, high-quality research publications dealing with the epidemiology and risk factors of DILI, as well as sufficiently adjudicated case series. We tended to exclude individual case reports or abstracts and review articles where the extent of the causality assessment from source materials could not be easily ascertained. In some instances, we cited older studies to place the newer information into proper context. Given the large number of publications reviewed and space limitations, not all DILI articles were selected for comment. Given that opinions can vary between clinicians as to which articles are essential for inclusion, papers that are not cited here should not be construed as lacking relevance or importance to the field.
2 Epidemiology
Several new and updated case series of DILI appeared in 2015, bringing the total number of global registries and series to nearly one dozen [1, 15]. Those we chose to include here provided significantly new information.
2.1 Drug-Induced Liver Injury (DILI) in the USA
Chalasani et al. [16] updated the 10-year data from the ongoing US Drug-Induced Liver Injury Network (DILIN). The first 1257 patients enrolled in the study have been analyzed, and 899 of these subjects were considered to have either definite, highly likely, or probable DILI. Cases of acetaminophen-related liver injury are not part of the DILIN registry, but instances of idiosyncratic liver injury from all other classes, as well as HDS are being prospectively collected in this ongoing National Institutes of Health (NIH)-funded effort. To date, about 10 % of patients overall have either died (6.2 %) or required liver transplantation (4 %), which confirms the clinical observations of the late Hyman Zimmerman, from which the term “Hy’s Law” was derived [1, 17]. Several new subgroup analyses were performed by the DILIN investigators. Among these was an analysis of patients suspected of having acute DILI in the setting of chronic liver disease (CLD). Of this group, 10 % (n = 89) of the group had pre-existing liver disease (mostly non-alcoholic fatty liver disease or chronic hepatitis C virus [HCV]), and DILI outcomes appeared to be more severe in these individuals than in those without underling liver disease (mortality rates 16 vs. 5.2 %; p < 0.001). However, the causes of DILI did not differ significantly from the cohort without CLD, with one exception: azithromycin was associated with a statistically significant higher risk of causing DILI in those with CLD (6.7 vs. 1.5 %). These data confirm the long-held observation of Zimmerman that most drugs can be taken safely by patients with CLD, but if acute DILI develops, the outcome may be more severe.
The DILIN investigators also examined patients with latency periods at the extremes of what is usually considered typical for DILI. Among 41 cases with an ultrashort latency of ≤7 days, they found that most of these cases were caused by antimicrobial agents (71 %). Likewise, the two most common causes for the 60 DILI cases with a prolonged latency over 365 days were nitrofurantoin (25 %) and minocycline (17 %). Interestingly, there were no differences in outcomes comparing DILI with short or long latency periods. Nine (1 %) patients had concomitant severe skin reactions associated with liver injury. The agents implicated were lamotrigine, azithromycin, carbamazepine, moxifloxacin, cephalexin, diclofenac, and nitrofurantoin. Four of these patients died, consistent with a high mortality for the associated hypersensitivity reaction.
Nearly one in six (16.6 %) patients with acute DILI had persistent elevations in liver-associated biochemistries at 6 months. In a follow-up DILIN study, three-quarters of patients with abnormalities at 6 months continued to have elevations at 12 months, suggesting that chronic injury was developing [18]. Most of these causes of chronic DILI were associated with cholestatic hepatotoxins, which have been previously described as leading to chronic DILI, including instances of vanishing bile duct and other syndromes [19]. We discuss additional data on the prognosis and individual classes of agents causing DILI as analyzed by the DILIN investigators in a number of the following sections.
Goldberg et al. [20] performed a retrospective cohort study on the incidence of acute liver failure (ALF) using data from adult members of the Kaiser Permanente Northern California (KPNC) healthcare system for the years 2004–2010. Among the more than 5 million KPNC members, 669 met diagnostic criteria indicating potential ALF. A total of 62 (9.3 %) of these patients were categorized as having definite or possible ALF, and 32 (51.6 %) of these patients had a drug-induced etiology. Acetaminophen was implicated in 18 (56.3 %) events, HDS in six (18.8 %) events, antimicrobials in two (6.3 %) events, and miscellaneous medications in six (18.8 %) events. One patient (5.6 %) with acetaminophen-induced ALF died compared with three patients (21.4 %) with non-acetaminophen-induced ALF. Overall, six patients (18.8 %) underwent liver transplantation and 22 patients (68.8 %) were discharged without transplantation. These numbers are quite similar to those reported by the ALFSG (US Acute Liver Failure Study Group) [21]. Of the 2000 patients with ALF, 45.8 % were due to acetaminophen and 11 % to other drugs. The remaining etiologies were indeterminate (12.3 %), hepatitis A (1.8 %) and B (7.1 %), and all others (22 %). Additionally, the US ALFSG described cases of idiosyncratic drug-induced ALF during a 10-year period. A total of 133 patients were found to have DILI-induced ALF. The most common agents were antimicrobials (46 %). Transplant-free survival was poor, at 27.1 %; however, with successful transplantation in 42.1 %, overall survival was 66.2 % [22].
Kulkarni et al. [23] investigated cases of pediatric ALF in the USA between 2008 and 2013 using the Pediatric Health Information System database. Data were collected for children admitted with ALF in 16 US pediatric liver transplant centers. The etiology could not be determined for more than half of the patients (52.5 % of 583) who met selection criteria for pediatric ALF. Acetaminophen toxicity was the most common identifiable etiology at 18.7 %. Mortality was lower than previously reported, with 95.4 % surviving overall, and 73.2 % surviving without a liver transplant. Acute respiratory failure (odds ratio [OR] 3.4), acute kidney injury (OR 3.6), and cerebral edema (OR 3.6) were independently associated with an increased mortality.
2.2 DILI in China
Hao et al. [24] are among the latest investigators to describe the etiology, clinical features, and prognosis of liver injury associated with DILI in China. The most prevalent agents among 140 patients with DILI were Chinese traditional medications (62.1 %) followed by antipyretic analgesic drugs (10 %) and antibiotics (5 %). The male to female ratio in the study cohort was 1:1.69, and half of the patients were aged between 40 and 60 years. The percentages with hepatocellular injury, cholestatic injury, and mixed injury were 51.4, 30.7, and 17.9 %, respectively. The median age of patients with cholestatic liver injury was 55.6 years, which was older than patients with hepatocellular (47.1 years) or mixed injury type (49.9 years); this finding is consistent with DILI in Western registries [25].
Zhu et al. [26] investigated DILI in a pediatric population. They performed a retrospective analysis on 69 children who were hospitalized with DILI between January 2009 and December 2011. Antibiotics were the most common Western medicines to cause DILI, at 26.1 %. The major implicated herbal causes were Ephedra sinica and Polygonum multiflorum. Compared with injuries caused by Western medicines, children whose liver injury was caused by Chinese herbal medicines showed a higher level of total bilirubin (1.4 vs. 16.6 mg/dl) and a longer prothrombin time (11.8 vs. 17.3 s), suggesting more severe hepatic impairment.
2.3 DILI in Germany
Douros et al. [27] conducted a case–control study to determine the hepatotoxic risk of a wide range of drugs in 51 Berlin hospitals. Between 2002 and 2011, a total of 198 patients developed acute idiopathic hepatitis. Drug exposure was obtained in what was termed by the authors as a “face-to-face” interview, implying that an adequate history was obtained to assess causality by applying the updated Council for International Organizations of Medical Sciences (CIOMS) scale. Their study corroborated the hepatotoxic risks seen for a number of drugs, including phenprocoumon, amiodarone, clozapine, and flupirtine. Increased risks were also found for substances including angiotensin II receptor blockers, atypical antipsychotics, and biperiden, a drug not previously reported to be hepatotoxic.
2.4 DILI in Latin America
A new branch of the Spanish DILI registry was established in Latin America (SpanishLatin DILI registry) in 2012 [15]. Among the first 200 DILI cases that have been collected to date, the patient demographics and drugs responsible appear quite similar to those in the larger Spanish registry. Anti-infectives constituted 24 % of the cases, musculoskeletal treatments were seen in 18 %, and HDS were found in 10 %. Liver-related death or the need for transplantation was reported in 5 % of these patients.
2.5 Incidence of DILI in Patients with Elevated Alanine Transaminase
Galvin et al. [28] performed a single-center retrospective analysis of patients with an alanine transaminase (ALT) level >1000 UI/L. A total of 182 patients were identified over a 2-year period in Dublin, Ireland. Ischemic liver injury was the most common etiology (61 %), followed by DILI (15.9 %), and acute viral hepatitis (12.1 %). The next most common causes were undetermined (5 %) and acute choledocholithiasis (4.4 %). Acetaminophen (AAP) toxicity accounted for almost half of the DILI cases (13 of 29). Other causes of DILI included anti-tuberculosis (anti-TB) drugs (6 of 29) and other antibiotics (4 of 29). These findings are consistent with the fact that acute idiosyncratic DILI (including ALF) generally does not present with aminotransferase values in this high range, and reminds the clinician that other etiologies are much more likely to be responsible [1].
3 Newly Reported Risk factors for DILI
Numerous factors affect susceptibility to DILI, including genetic, pharmacologic, and extrinsic factors. Several of these variables that have been recently linked to or corroborated as being associated with DILI are discussed in the following section.
3.1 Cytochrome P450 Metabolism
Previous observations have shown that drugs extensively metabolized by the liver have a higher likelihood of causing DILI [29, 30]. As cytochrome P450 (CYP) enzymes are primarily involved in hepatic metabolism, Yu et al. [31] investigated the association of DILI with drugs that are CYP substrates, inhibitors, or inducers. They collected data on 254 orally administered drugs contained in the Liver Toxicity Knowledge Base Benchmark Dataset and found that drugs metabolized by CYP enzymes were four times as likely to cause DILI as drugs not metabolized by P450 enzymes. Specifically, drugs metabolized by CYP1A2, CYP2C8/CYP2C9, and CYP3A5 were closely associated with an increased risk of DILI. Drugs given in a high daily dose (>100 mg) were nearly five times as likely to cause DILI as lower daily doses. In contrast with the recently reported “rule of two”, where high daily dosage and high lipophilicity were strongly associated with each other as conveying an increased risk of DILI [32], Yu et al. [31] did not find lipophilicity to be a significant factor. Whether or not their findings will be corroborated by other investigators remains to be determined.
3.2 DILI Pharmacogenomics
Pharmacogenomic risk factors for DILI continue to be identified [33–35]. However, their clinical utility for use as a pre-prescription screening tool with potential hepatotoxins remains unclear [36, 37]. Aithal [37] emphasized that, because DILI is a rare condition, the positive predictive value of existing HLA screening tests is relatively low, even when dealing with HLA alleles associated with a high incidence of DILI (such as flucloxacillin and amoxicillin–clavulanate). Perhaps the best use of such HLA screening at present is to rule out DILI, given the high negative predictive values seen with various drugs. As a case in point, whereas 34 % of all patients being considered for lumiracoxib would be excluded from therapy if they harbor the HLA-DQA1*0102 allele, only 5.6 % of HLA carriers would actually be expected to develop DILI [37]. To date, the only instance in which a drug is not being prescribed based on HLA testing remains abacavir, because of the very high likelihood of developing a severe hypersensitivity reaction, which can include DILI, in individuals harboring HLA-B*5701 [38].
Although the focus of many DILI-related studies in the current literature has been on HLA risk associations, a recent report by Overby et al. [36] demonstrated that common variants outside of HLA testing may also contribute to DILI susceptibility. They studied the heritability of DILI using genome-wide association studies, looking at single-nucleotide polymorphisms related to chromosome 6 as well as genome wide. They found that for flucloxacillin-associated DILI, almost all of the heritability could be attributed to chromosome 6, whereas for patients with amoxicillin–clavulanate-induced DILI, chromosome 6 only explained part of the heritability. Their findings suggest that contributions from additional common heritable variants have yet to be discovered, and that further genome-wide complex trait analysis might serve as a valuable method for future DILI-related study designs [36]. Table 1 lists a number of other pharmacogenomic associations for DILI that have recently been described.
4 Newly/Recently Described Hepatotoxins
The past year saw a few new drugs added to the growing list of well-documented hepatotoxins.
4.1 Tolvaptan
Tolvaptan is a V2 receptor antagonist approved for short-term use for the treatment of hyponatremia and is being investigated for long-term use to slow the progression of autosomal dominant polycystic kidney disease (ADPKD). Watkins et al. [44] performed an analysis of the clinical trial data for ADPKD and reported that hepatic injury (defined as ALT >3× the upper limit of normal [ULN]) was more commonly observed in tolvaptan recipients (4.4 %) than in placebo recipients (1 %), including the findings of three cases that met Hy’s Law criteria. The apparent clinical signature of DILI based on cases adjudicated as probably related to tolvaptan included a latency period of 3–18 months of daily use, a hepatocellular injury pattern, and reversibility of the injury after drug discontinuation over a median duration of 46 days in all subjects. There were no instances of ALF in the clinical trial subjects, although the potential for ALF exists and was estimated to occur in 1 in 4000 patients, based on these data. Liver biopsies obtained in four subjects did not reveal any pathognomonic histologic features of the injury. The cause is considered idiosyncratic, although several individuals who were re-challenged with tolvaptan after ALT values normalized re-developed rapid ALT elevations, suggesting an immunoallergic mechanism may be present in some individuals. It is not thought that the presence of hepatic cysts contributed to the risk of injury. Monitoring of ALT was deemed warranted for patients receiving long-term tolvaptan treatment.
4.2 Novel Oral Anticoagulants
4.2.1 Direct Factor Xa Inhibitors
In modern treatment of thromboembolic disease, current medical practice has been moving away from traditional anticoagulation with warfarin, as the use of novel oral anticoagulants (NOACs) has been gaining in popularity. Russmann et al. [45] reported 14 cases of liver injury attributed to rivaroxaban, two of which were confirmed with liver biopsy. As a result, other investigators have recently evaluated the data on the hepatotoxicity of NOACs. Liakoni et al. [46] found the frequency ranged between 0.1 and 1 %, with some case reports describing potentially life-threatening toxicity. Rivaroxaban was noted to have been associated with more hepatic adverse events than apixaban or dabigatran. Raschi et al. [47] assessed the FDA Adverse Event Reporting System (FAERS) for post-marketing reports of liver injury with rivaroxaban and dabigatran and found that DILI represented 3.7 and 1.7 % of all adverse event reports for these two agents, respectively. While clinical information is often limited in disproportionality analyses within FAERS, a hepatotoxicity signal did arise with rivaroxaban, but not with dabigatran (or with warfarin as a comparator). As a result, while these authors call for additional studies comparing the potential risk of DILI between rivaroxaban and other agents, given the rarity of severe hepatotoxicity, we note there is no need for routine liver enzyme monitoring according to the prescribing information for any of these agents. An interesting case report by Anastasia et al. [48] described a patient with suspected rivaroxaban-associated DILI that rapidly resolved after discontinuation, in whom apixaban was then safely prescribed as an alternative factor Xa inhibitor. This implies that cross reactivity may not be present and that the mechanism of injury is likely unrelated to its mechanism of action as an anticoagulant.
4.2.2 Low Molecular-Weight Heparins
Enoxaparin and other low molecular-weight heparins are rare causes of DILI. Hahn et al. [49] reviewed the FAERS database and the published literature and found that self-limited, reversible, asymptomatic elevations of ALT >3× ULN have been reported in 4–13 % of patients receiving enoxaparin in clinical trials, with fewer than a dozen cases published in the literature. These investigators noted even fewer cases have appeared describing other members of this class (one case of dalteparin and no cases to date attributed to tinzaparin). While the FAERS database lists liver injury in 4 % of more than 8300 enoxaparin-associated adverse events collected between January 2000 and September 2014, all of the serious outcomes (hospitalization, death, etc.) were attributed to non-hepatic AEs, such as bleeding and thrombocytopenia [49].
4.3 Hepatitis C Direct-Acting Antivirals
While several new oral antiviral drugs have received FDA approval for the treatment of chronic HCV, reports have emerged suggesting a possible association with serious acute hepatitis and decompensation in patients receiving protease inhibitors, especially those with advanced cirrhosis [50]. Many of these reports involved simeprevir, a second-generation protease inhibitor used in combination with other HCV agents. Okajima et al. [51] described possible simeprevir hepatitis in a 56-year-old male Japanese patient who had relapsed after several prior treatment regimens, including telaprevir that resulted in a skin rash and had to be discontinued. Simeprevir was then added to pegylated interferon and ribavirin, which had already been taken for 60 months. After 6 weeks, despite having a rapid virological response, the patient developed elevated ALT without a rash and he required hospital admission and stoppage of all three antivirals. A liver biopsy was read as consistent with DILI. The patient’s serum aminotransferases rapidly decreased following discontinuation of treatment, and this positive de-challenge response suggested that a drug was responsible for the event. Simeprevir was considered the most likely cause based on the temporal relationship. Igawa et al. [52] also reported a case of suspected simeprevir-induced liver injury in a 65-year-old male that occurred on day 49 of treatment despite the patient achieving a virological response. The patient’s ALT peaked at 700 IU/l, and a subsequent liver biopsy on day 60 demonstrated a pattern consistent with acute hepatitis. Following discontinuation of treatment, the liver injury improved significantly within a few weeks. Both of these cases suggested acute DILI rather than hepatic decompensation.
In contrast, Stine et al. [53] reported hepatic decompensation with hyperbilirubinemia that developed in two patients with advanced HCV cirrhosis treated with simeprevir-containing regimens under a compassionate use protocol. One patient developed marked increases in aspartate transaminase (AST)/ALT, with bilirubin rising from 6.6 to 28 mg/dl by week 4, and a Model for End-stage Liver Disease (MELD) score rising from 17 to 36. He required a liver transplant 4 weeks later despite the HCV having cleared and the aminotransferases having normalized. A Roussel Uclaf Causality Assessment Method (RUCAM) score of 7 suggested a probable relationship with the antivirals. The second individual had a baseline MELD score of 20 and a marked rise in bilirubin, from 9.5 to 25 mg/dl by week 2 of therapy, with only modest elevations in AST and ALT. During the 10 weeks of simeprevir–sofosbuvir (SIM-SOF) therapy, he also received a course of treatment with trimethoprim–sulfamethoxazole for a soft tissue infection (during week 7), but had no sign of a hypersensitivity reaction. When the SIM-SOF regimen was stopped, his bilirubin trended downwards and his MELD declined back to 21 in what was considered a positive de-challenge response with a RUCAM score in the possible range. On the basis of these cases, the transplant service felt that using simeprevir or other protease inhibitors needed to be carefully considered for patients with advanced cirrhosis going forward, because of the apparent hepatic decompensation.
Another protease inhibitor, asunaprevir, has also been reported to be hepatotoxic. Fujii et al. [54] reported on a 57-year-old man with pegylated interferon (PEG-IFN) and ribavirin-resistant HCV who developed liver injury and jaundice accompanied by fever and eosinophilia with an asunaprevir-containing regimen. Although the patient’s fever resolved after discontinuation of treatment, his liver injury persisted, suggesting a longer-lasting hypersensitivity reaction. Asunaprevir has not been approved in the USA because of the risk of hepatotoxicity and the fact that ALT monitoring would be required with its use. A unique drug-induced immunoallergic hepatitis during combination therapy with daclatasvir and asunaprevir was reported in Japan [55].
Both Viekira Pak (Abbvie; North Chicago, IL, USA) (ombitasvir, paritaprevir/ritonavir, dasabuvir) and Technivie (Abbvie; North Chicago, IL, USA) (ombitasvir plus paritaprevir/ritonavir) have recently received FDA warnings about hepatotoxicity that contraindicates the use of these products in patients with advanced cirrhosis. FDA warnings on Viekira Pak and Technivie are likely related to its protease inhibitor component, paritaprevir [56]. The latest direct antiviral regimen (DAA) regimen for chronic hepatitis C, Zepatier™ (Merck; Kenilworth, NJ, USA) (elbasvir and grazoprevir), produced ALT elevations >5× ULN in about 1 % of clinical trial patients (in both patients with and without cirrhosis) [57] and its labelling requires ALT testing during the first few weeks of treatment [58]. We are unaware of any hepatotoxity attributed to the other components of Viekira Pak or Technivie. Similarly, no hepatic injury has been reported with sofosbuvir, ledipasvir, or daclatasvir.
4.4 Biologics
Eculizumab (Soliris [Alexion; Cheshire, CT, USA]) is a humanized anti-C5 antibody approved for the treatment of atypical hemolytic uremic syndrome (HUS) and paroxysmal nocturnal hemoglobinemia (PNH) in both pediatric and adult populations. Hayes et al. [59] report the first instances of possible DILI with this agent in their review of the clinical and biochemical data from a single center where 11 children were treated with eculizumab for atypical HUS (aHUS). Elevated aminotransferases were observed in seven children with liver injury. One patient developed tender hepatomegaly and liver enzyme elevation 20× ULN. Patients were re-challenged with eculizumab, resulting in recurrent liver injury and subsequent discontinuation of treatment. While the authors suggested that liver enzymes should be monitored in all patients receiving eculizumab treatment for aHUS, this recommendation was likely made out of an abundance of caution on their part, as the prescribing information does not call for such testing as part of the broader Risk Evaluation and Mitigation Strategy (REMS) aimed specifically to prevent meningococcal infection in these patients.
A variety of toxicities, including DILI, has been reported with several other biologic agents, including anti-tumor necrosis factor (TNF)-α therapies. Ghabril et al. [60] analyzed the US DILIN series and identified six patients in their registry, along with 28 cases reported in the literature, considered as having probable or higher causality scores. Most instances were associated with infliximab (n = 26), with a few reports relating to etanercept (n = 4) and adalimumab (n = 4). The median latency period was 13 weeks, with a broad range of onset from 2 to 104 weeks. Two-thirds (22 of 33) of patients who underwent testing had antinuclear or anti-smooth muscle antibodies, and nearly all of those undergoing liver biopsy had histologic features of autoimmune hepatitis (15 of 17). Of 34 patients, 33 improved after the drug was withdrawn, with 12 individuals receiving corticosteroids. One patient with underlying cirrhosis required a liver transplant after the acute-on-chronic injury.
Rodrigues et al. [61] performed a retrospective analysis of medical records from a single center and described seven cases of autoimmune-like hepatitis involving infliximab, and one case involving adalimumab. All eight patients responded well to corticosteroid treatment, with liver biochemistries normalizing 2 months after discontinuation. Only two individuals required long-term steroid treatment for ongoing injury. In a similar study, Shelton et al. [62] performed a retrospective analysis of 1753 inflammatory bowel disease (IBD) patients initiating anti-TNFα therapy, 102 (6 %) of whom developed new-onset ALT elevations. While over half of these cases were attributed to non-DILI causes, six patients who underwent liver biopsy had findings consistent with autoimmune hepatitis that was considered drug related. The majority of patients saw their liver function tests normalize after discontinuation of anti-TNFα therapy.
French et al. [63] remind us that our understanding of the frequency of the injury and the precise mechanism of drug-induced autoimmune hepatitis (DI-AIH) from anti-TNFα agents remains incomplete. They suggest that specific pharmacological properties of the agents implicated as well as host genetics may be significant risk factors, and such knowledge may offer future clues as to how best to manage the hepatotoxicity.
Ipilimumab is a monoclonal antibody that targets cytotoxic T lymphocytes antigen 4 (CTLA-4), a co-stimulatory and inhibitory receptor on T cells, ultimately blunting the adaptive immune response to malignant T cells. It is used as treatment for patients with advanced melanoma and, while highly effective, upregulation of T cells can cause deleterious effects on normal cells. As a result, ipilimumab is known to cause a number of immune-related adverse events (irAEs), including hepatitis and colitis [64]. Immune-related hepatitis typically occurs 3–9 weeks after the start of ipilimumab therapy, and usually resolves after about 2 weeks when following protocol-specific guidelines. Cheng et al. [65] described three males with ipilimumab-induced hepatitis, each patient showing improvement of symptoms and ALT elevations following a high-dose pulsed steroid regimen (intravenous prednisolone 1 gm daily for 3–5 days). Recommendations published by this group to guide clinicians in managing irAEs include supportive measures and discontinuation of ipilimumab until resolution for mild to moderate hepatitis. Severe immune-related hepatitis (AST or ALT levels >8× ULN, or bilirubin levels >5× ULN, or severe diarrhea) can be treated with parenteral steroids (e.g., methylprednisolone 1–2 mg/kg/day) with a slow steroid taper over at least 1 month. Mycophenolate mofetil has been suggested as a second-line immunosuppressive agent in patients for whom systemic steroid treatment fails. However, the optimal management of ipilimumab-related hepatitis in the absence of autoimmune markers that is unresponsive to steroids has not been clearly defined [65].
5 New Reports of Established Hepatotoxins
5.1 Paracetamol (Acetaminophen, N-Acetyl-Para-Amino-Phenol [AAP])
AAP remains the leading cause of ALF in the USA and other Western nations, outnumbering other drug causes by a factor of three- to fourfold. Serper et al. [66] analyzed 666 cases of AAP-related liver failure using the ALFSG database from 1998 to 2012. The majority of these patients (56.6 %) overdosed using a combination of AAP with opioids compared with 30.3 % who overdosed with AAP alone. On presentation, 58 % in the AAP–opioid group had advanced encephalopathy compared with 43 % with AAP alone (p = 0.001).
King et al. [67] focused on the labeling practices for commonly prescribed AAP-containing analgesics, including oxycodone and hydrocodone combinations. AAP was found fully spelled out on only 6.9 % of 245 drug labels, with various abbreviations used in more than 90 % of cases [67]. Moreover, most of the study participants were not able to appropriately identify AAP as an active ingredient in their prescription. The authors remarked that, because of such ambiguity, many opportunities were missed to clearly convey important hepatotoxicity risk information on prescription bottles. They correctly point out that the lack of such information may actually contribute to the burden of AAP-induced liver injury.
Treatment with N-acetylcysteine (NAC) continues to serve as the mainstay for AAP toxicity worldwide. The threshold for treatment is based on the serum AAP levels measured between 4 and 24 h following acute ingestion, which are plotted on the Rumack–Matthew nomogram. While various treatment lines exist, there is no worldwide consensus on which serum AAP level is optimal to begin treatment with NAC. In the USA, Hong Kong, Australia, and New Zealand, the 150-treatment line is preferred, i.e., NAC treatment is initiated if the serum AAP concentration is plotted at or above a singular treatment line beginning at 150 mg/l at 4 h following ingestion. Chan et al. [68] evaluated the failure rate of the 150-treatment line and assessed the impact of lowering the treatment threshold. In this case series, the authors gathered data from the Hong Kong Poison Control Information Centre, including all patients with acute AAP toxicity documented from January 2011 through December 2013 and evaluated the timing of serum AAP concentrations and their relationship to different treatment lines. A total of 893 cases were identified, with 187 (20.9 %) patients with serum AAP concentrations above the 150-treatment line; 112 (12.5 %) between the 100- and 150-treatment line, and 594 (66.5 %) below the 100-treatment line. Of these patients, only 25 (2.8 %) sustained significant hepatotoxicity, two of whom were between the 100- and 150-treatment lines and two of whom were below the 100-treatment line. The authors calculated the failure rate of the 150-treatment line to be only 0.45 %, and that decreasing the treatment threshold to the 100-treatment line would possibly decrease the failure rate to 0.22 %. However, this would require 37 additional patients to be treated annually, at a cost of 189,131 Hong Kong dollars. Additionally, 112 patients would need to be treated to prevent one significant liver injury; a relatively high number needed to treat (NNT) that will require further analysis to determine its cost effectiveness.
In patients with AAP toxicity, elevation of serum aminotransferases AST and ALT indicate liver-specific injury, as they tend to initially increase at similar rates, followed by reduction of AST more rapidly than ALT because of the shorter half-life of the former (17 vs. 47 h). A retrospective study by McGovern et al. [69] investigated whether the AST to ALT ratio could potentially indicate that a patient has passed the time of peak AST concentration. The authors compared various thresholds of the AST to ALT ratio by increments of ten to determine the optimal value that would reliably indicate that these biochemical parameters were resolving. They found an AST to ALT ratio of ≤0.4 was 99 % sensitive in predicting recovery of patients with AAP toxicity who were treated with NAC. Such findings could prove useful in assisting with clinical decision making as to when to discontinue NAC treatment.
5.1.1 Primary Prevention of AAP Hepatotoxicity
Restricting the availability of AAP in the EU as well as in the USA has had an important impact in reducing the incidence of ALF. Hawton et al. [70] compared the number of deaths from AAP poisoning before and after legislation was passed that restricted AAP pack sizes to as little as 12–16 g. They found an estimated average reduction of 17 deaths per quarter, representing a 43 % reduction, as well as a 61 % reduction in registrations for liver transplantation for AAP-induced hepatotoxicity. Overall, this legislation was thought to have prevented 765 deaths over the past 11 years.
5.1.2 Liver Transplantation for Acute Liver Failure Due to AAP
A large multi-country study of ALF leading to registration for liver transplantation (ALFT) was reported by Gulmez et al. [71]. A total of 600 ALFT cases were identified in 52 of 57 eligible transplant centers in France, Greece, Ireland, Italy, the Netherlands, Portugal, and the UK between 2005 and 2007. Of the 600 cases, 114 were from overdose, and 111 (97.3 %) of these were from AAP. Most overdoses were intentional (63 %). The highest proportion of these patients was in Ireland (52 %), followed by the UK (28 %), France (18 %), the Netherlands (8 %), and Italy (1 %). No overdose ALFTs were identified in Greece, highlighting the widely differing rates of AAP overdoses in Europe.
5.1.3 Predictive AAP Biomarkers
A number of serum biomarkers, including microRNA (miR)-122, keratin (K)-18, and high-mobility group box-1 (HMGB-1) have been implicated in the mechanism of DILI in human subjects [72–75]. In particular, those most related to mitochondrial damage have been shown to have a positive predictive value in determining the outcome of AAP toxicity [76–78]. Such biomarkers may also be instrumental in determining the need for liver transplantation as well as for the identification of novel therapeutic agents. A study investigating AAP toxicity in healthy volunteers compared with patients receiving treatment for combined HIV and TB in Ethiopia, examined the value of biomarkers K18:M65 and miR-122 [79]. The investigators found these particular biomarkers had higher sensitivity and specificity in predicting DILI than traditional serum ALT and AST. However, Senior [80] reminds us that despite these findings, serum biomarkers have thus far failed to produce evidence of what actually caused the liver injury. He suggests the best method to assess causality remains traditional medical reasoning, as DILI essentially remains a diagnosis of exclusion. By focusing on our understanding of the underlying mechanisms of DILI, the investigation of biomarkers associated with hepatotoxicity is expected to garner added insight into predicting DILI in the future.
Stutchfield et al. [81] described the prognostic significance of serum levels of macrophage colony-stimulating factor (CSF1) in patients with acute liver injury from AAP, as well as in patients who underwent partial hepatectomy. These authors found increased serum levels of CSF1 in patients who underwent hepatic surgery, directly in proportion to the extent of liver resected. Additionally, low serum levels of CSF1 were associated with increased mortality in AAP-induced ALF, suggesting its utility as another prognostic biomarker.
5.2 Antimicrobials
5.2.1 Anti-Tuberculosis Agents
Isoniazid is a leading cause of hepatotoxicity and ALF [82]. Most recommendations for identifying DILI in isoniazid-treated patients rely on monitoring of self-reported hepatitis-related symptoms rather than formal ALT testing. In a study from the US DILI Network, Hayashi et al. [83] found that isoniazid was the second most frequently reported hepatotoxic agent in the DILIN registry, and cases are likely under-reported. Importantly, these investigators found a significant delay in the time to discontinuing isoniazid after the development of hepatitis-related symptoms. Over 50 % of patients who developed symptoms that met criteria that would otherwise call for the drug to be stopped immediately (i.e., nausea, abdominal pain, jaundice, or unexplained fatigue) were found to have continued taking isoniazid for more than 7 days, and 24 patients (40 %) continued taking isoniazid for more than 14 days after meeting such symptomatic criteria. Not surprisingly, the outcome for these patients was more severe than for individuals who promptly stopped taking isoniazid, with 9 of 13 patients who continued taking isoniazid for more than 7 days listed as having died or needing a liver transplant. Their results call into question the utility of relying solely on self-reported symptoms for a drug with such a significant hepatotoxic potential.
5.2.2 Antibiotics
The updated US DILIN database has yielded new information of several antibiotics and antibiotic classes causing DILI. Martinez et al. [84] defined the clinical and histological features as well as the outcome of azithromycin-induced liver injury based on 18 patients in the current DILIN registry. The injury was mostly hepatocellular in nature, and occurred within 1–3 weeks of exposure. Although outcomes were typically favorable, azithromycin was been found to cause chronic injury as well as associated cutaneous reactions, and in some cases resulted in liver transplantation or even death. In a similar study, Alqahtani et al. [85] characterized the hepatotoxicity associated with cefazolin exposure. The authors found 19 cases of DILI caused by cefazolin, and noted that even one dose of cefazolin could cause hepatotoxicity, typically preceded by a latency period of 1–3 weeks after exposure. Most injury was moderate to severe but self-limited in nature. The finding of a short course of antibiotic therapy with delayed onset of DILI is similar to that described for amoxicillin–clavulanate, where injury can be delayed for up to 6–7 weeks [86].
In contrast to the antibiotics frequently implicated in DILI (such as azithromycin or amoxicillin–clavulanate), fluoroquinolone-induced liver injury appears relatively rare. Orman et al. [87] found 12 cases in the DILIN registry and noted that fluoroquinolone liver injury was typically rapid in onset and often had immunological features suggestive of a hypersensitivity reaction. Patterns of injury included hepatocellular injury (predominantly increased levels of alanine aminotransferase), cholestatic injury (predominantly increased levels of alkaline phosphatase), and mixed. Additionally, both acute and chronic liver failure occurred.
5.2.3 Drug-Induced Autoimmune Hepatitis
Several reports of drug-induced autoimmune-like hepatitis (DI-AIH) have recently appeared, adding to the growing list of drugs that are associated with this form of hepatotoxicity (see Sect. 4.4 above). Yeong et al. [88] published a retrospective study in 82 patients with autoimmune hepatitis, 11 of which were felt to be drug induced (13.4 %). The likely causes included nitrofurantoin, statins, herbals, and diclofenac. The authors reported that DI-AIH was more likely to occur in patients aged >60 years and took longer to relapse after immunosuppression was discontinued than idiopathic AIH. Björnsson et al. [89] found a similar outcome to cases of DI-AIH in the Mayo Clinic series.
Cyproterone acetate (CPA) is an anti-androgenic drug used in the treatment of prostate cancer that has been associated with DILI. Bessone et al. [90] examined 22 patients with CPA-associated hepatotoxicity, with most (91 %) presenting with jaundice and hepatocellular injury. Elevated international normalized ratio (INR) >1.5 was observed in 66 % of patients, five of whom developed ascites and four of whom had encephalopathy. Liver biopsy results showed a mixed pathology, with one patient displaying liver injury pattern suggestive of AIH. After CPA was discontinued, 19 patients recovered; however, three required corticosteroid treatment, two of whom had elevated antinuclear antibody (ANA) titers, suggesting an autoimmune mechanism.
5.3 Miscellaneous Causes of DILI
5.3.1 Antidepressants
Antidepressants comprise multiple chemical classes and, as recently noted by Friedrich et al. [91], the identification of hepatic injury associated with these agents is highly dependent on the frequency of liver enzyme testing. In their review of more than 184,000 in-patient admissions between 1993 and 2011 at 80 German-speaking psychiatric hospitals in Austria, Germany, and Switzerland, the overall risk of DILI was very low (0.03 % for selective serotonin reuptake inhibitors [SSRIs] and 0.14 % for tricyclic antidepressants). The most commonly implicated agents were mianserin (a tetracyclic compound available outside of the USA), clomipramine, and agomelatine. These investigators suggest that drug warnings (e.g., in the form of Dear Doctor letters) may have the greatest impact in performing surveillance testing among psychiatrists, as seemed to be the case with agomelatine [92].
5.3.2 Methylprednisolone
Although methylprednisolone is frequently used to treat drug-induced autoimmune-like hepatitis and DILI associated with hypersensitivity reactions [61, 65, 88, 89], Davidov et al. [93] remind us that high-dose treatment of disorders such as multiple sclerosis (MS) can be associated with acute hepatic injury. They describe a 23-year-old woman with MS who developed an episode of acute hepatocellular jaundice following a 3-day course of intravenous methylprednisolone 1 gm daily. Her ALT at that time peaked at 2287 U/l, with total bilirubin 6.3 mg/dl, and a positive smooth muscle antibody was found. Liver tests normalized after 3 months; 6 months later, she received the same 3-day high-dose intravenous regimen of methylprednisolone 1 gm/day and again had an ALT peak above 2000 U/l with bilirubin 6.85 mg/dl. Viral serology was negative, and a liver biopsy showed changes of centrizonal drop-out, congestion, and chronic inflammation with lymphocytes, eosinophils, and a few plasma cells, along with acidophilic bodies consistent with DILI. A RUCAM assessment score of 9 for methylprednisolone indicated a high probability that the drug was responsible. As with the first episode, her liver tests again normalized within 3 months. These researchers also performed a review of the literature and found an additional 24 cases implicating high-dose methylprednisolone as the cause of acute DILI. Most patients were female, with a median age of 45 years, and many had associated Grave’s ophthalmopathy. The onset of injury ranged between several days and weeks, and several patients also had a positive re-challenge response. Peak ALT values were often above 1000–2000 U/l. Also, as seen in the index case, autoantibodies were present in one-third of patients, suggesting that the course of high-dose steroid therapy might have paradoxically triggered an acute autoimmune-like hepatitis. Alternatively, a previously quiescent AIH might have become clinically apparent after the steroids were withdrawn, although it resolved without any further immunosuppression.
Caster et al. [94] confirmed the association by analyzing the more than 8 million safety reports in the World Health Organization (WHO) global database (VigiBase). They found 26 cases of hepatotoxicity related to high-dose methylprednisolone (1 gm daily for 3 days; most often for a relapse of MS) (3.6 % of 723 high-dose reports) and 22 cases from low-dose treatment (500 mg/day for 5 days; most frequently for asthma) (0.9 % of 2583 reports). Many cases were confirmed through a positive re challenge, although the evidence to implicate high-dose regimens was generally stronger than for patients receiving low-dose treatment. Clearly, such cases give us pause to consider methylprednisolone as a potential cause of acute DILI, and not always a benign therapy.
6 Herbals and Dietary Supplements Causing Liver Injury
With Eastern medicine showing an increased popularity in the USA and other Westernized nations in recent years, reports of HDS-induced liver injury continue to appear [95–99]. In the updated US DILIN series as reported by Navarro et al. [100], 16 % of all DILI cases were related to HDS, second only to antimicrobials as an etiologic class. These investigators found that HDS had increased from 7 to 20 % between 2004 and 2013. Interestingly, they found that HDS products intended for bodybuilding were an important cause of prolonged jaundice in young men, although there were no reported cases of liver transplant or deaths with these specific agents. In contrast, those HDS products not intended for body building were found to cause more severe hepatocellular injury, with a significantly higher rate of unfavorable outcomes (13 vs. 3 %), including liver transplant and death compared with non-HDS-induced liver injury [100].
The proportion of DILI cases related to HDS is even higher in Asia. For example, Lee et al. [101] published a systematic review specifically to identify and categorize cases of HDS-induced liver injury in Korea. After reviewing six databases, 31 reports and 97 cases of HDS-induced liver injury were discovered, with the majority of cases demonstrating a hepatocellular-type hepatotoxicity. The most common species of herbs causing liver injury in this population were Polygoni multiflori and Dictamnus dasycarpus.
The ability to diagnose HDS-related hepatotoxicity can be as difficult or more difficult than non-HDS-induced liver injury given the multiple components and concerns about adulterants and other contaminants in products that are often not closely regulated [97, 98, 102]. Teschke et al. [99, 103] noted that, while approximately 60 distinct commonly used herbs and herbal supplements, and more than 100 different herbs or herbal mixtures are used in Traditional Chinese Medicine that are reported to cause hepatotoxicity, most of these agents lack conclusive proof of hepatotoxicity. These investigators have been tireless in their efforts to demonstrate that many (if not most) reports of herbal hepatotoxicity do not stand up to intensive scrutiny where causality assessment is concerned. This includes agents such as kava kava, black cohosh, and greater celandine, among others [99]. The latest example of their causality re-assessment is the diet and muscle-building supplement, OxyElite Pro (USPLabs; Dallas, TX, USA). The toxicity of this compound made headlines when several cases were reported from a single hospital in Hawaii [104] as well as other locations [105]. Teschke et al. [106, 107] have raised significant concerns that alternative etiologies are more likely. The exhaustive causality assessment they performed concerning one of the cases serves as a model on which other cases of possible DILI or HDS-induced liver injury can and should be based. Their findings that call into question the accuracy of several other case series implicating a number of HDS formulations also have major implications for regulatory bodies that oversee the manufacturing and sale of HDS formulations and are responsible for issuing safety alerts, calls for re-formulating certain products, and/or the product’s removal from the market [1, 14, 103]. Indeed, in the case of OxyElite Pro, laboratory analysis of the product did not identify any specific hepatotoxins or mechanism of liver injury, raising questions as to whether or not the original formulation containing 1,3-dimethylamylamine, or the reformulation containing aegeline, were causative of the hepatotoxicity [108, 109]. The US DILIN has also weighed in on the importance of being able to exclude alternative etiologies when attempting to diagnose HDS-related hepatotoxicity [102, 110]. In one investigation, green tea extract was found to be present in >40 % of HDS compounds that failed to list this potentially hepatotoxic component in their list of ingredients [90]. Clearly, it can be argued that causality assessment for both suspected HDS as well as DILI will require ongoing refinements, not the least of which is ensuring that a minimal number of elements are available to conduct a meaningful analysis [8, 110].
7 DILI Outcomes and Prognosis
7.1 Long-Term Survival from Acute Liver Failure
Fontana et al. [111] published 2-year clinical outcomes among initial survivors and liver transplant recipients who were alive 3 weeks after enrollment in the US ALFSG between 1998 and 2010. The results show that 2-year survival was slightly higher in the 262 liver transplant recipients (92.4 %) than in the 306 spontaneous survivors of AAP toxicity (89.5 %) and the 200 non-AAP spontaneous survivors (77.5 %). The causes of death were similar across all groups, but the time to death, not surprisingly, was significantly longer in the liver transplant recipients (p < 0.0001). Of note, independent predictors of mortality in the AAP group included a high serum phosphate (median value of 2.75 mg/dl for those that died vs. 2.20 in survivors) and older age (median age of patients who died was 42 years vs. 35 in long-term survivors). In the non-AAP group, predictors of mortality included older patient age (median age of 50 years in patients who died vs. 42 in survivors), and days from jaundice to ALF onset. In the liver transplant group, predictors of mortality were older age (median age of 45.5 years in patients who died vs. 38 in survivors), days from jaundice to ALF onset, and coma grade (60 % of patients with grade 3 or 4 encephalopathy died compared with 36 %). The authors concluded that the survival of patients with non-AAP DI-ALF is significantly lower, possibly related to pre-existing medical conditions. In addition, spontaneous survivors of AAP overdose experience higher degrees of morbidity during follow-up from ongoing psychiatric and substance abuse issues.
7.2 Risk of Chronic DILI
The US DILIN reported on the risk of chronic DILI emerging from acute liver injury. Fontana et al. [112] compared liver biochemistry abnormalities persisting at 6 months with those at 12 months. Persistent injury was defined as ALT or AST >1.5× ULN or an alkaline phosphatase >ULN. They found that only 25 % of patients with abnormalities at 6 months had resolution of the biochemical injury by 12 months. Those with chronic elevations at 12 months were more likely to have a cholestatic injury pattern at the onset of liver injury (54 vs. 20 %) compared with those whose injury resolved. “Persisters” tended to be older (52.6 vs. 43.7 years) and had worse SF-36 physical summary scores than “resolvers”. A total of 17 patients with suspected chronic DILI underwent liver biopsy at a median of 387 days after injury onset: nine had chronic cholestasis, three had steatohepatitis, and three had a form of chronic non-specific hepatitis. A total of 12 patients had biopsies that could be compared with their initial biopsy, in whom chronic injury was frequently apparent (Table 2). These patients will be followed for at least another 12 months to determine the true incidence of persistent/chronic DILI, although the true clinical significance of just minor biochemical abnormalities may be in the eye of the beholder. Interestingly, the DILIN observation that chronic injury occurred predominantly from cholestatic hepatotoxins is similar to that reported by Aithal and Day [113] more than 15 years ago. It should be noted that the proportion of “chronic” cases reported in other series has been lower [114, 115].
7.3 Hy’s Law Cases
Robles-Diaz et al. [116] attempted to optimize the definition of Hy’s Law and develop a model for predicting ALF in DILI. Data were obtained from the Spanish DILI registry for 771 patients with DILI. Of these patients, 32 developed ALF. Hepatocellular injury, female sex, high levels of total bilirubin, and high AST-to-ALT ratio were independent risk factors for ALF. Three methods of using Hy’s Law were used to predict which patients would develop ALF. All three methods included a total serum bilirubin >2× ULN and either ALT >3× ULN, a ratio (R) value (ALT × ULN/alkaline phosphatase × ULN) >5, or a new ratio (nR) value (AST or ALT, whichever produced the highest × ULN/alkaline phosphatase × ULN) of ≥5. The level of ALT and the nR model each identified patients who developed ALF with 90 % sensitivity. The R-value criteria alone identified them with 83 % sensitivity. The authors concluded that when applied to DILI recognition, the nR criteria for Hy’s Law provides the best balance of sensitivity and specificity in predicting the ultimate development of ALF.
Lo Re et al. [117] investigated other potential markers for identifying patients at risk of developing DILI-induced ALF. In this study, 15,353 KPNC members were diagnosed with DILI from 2004 to 2010; 30 of these cases resulted in ALF. Logistic regression was used to develop prognostic models for ALF based on laboratory results measured at DILI diagnosis. Hy’s Law identified patients who developed ALF with a specificity of 92 % and negative predictive value of 99 %, but a low level of sensitivity at 68 % and positive predictive value of only 2 %. A model was developed comprising data on platelet count and total bilirubin level that enabled the calculation of a risk score called the Drug-Induced Liver Toxicity ALF Score (DrITox ALF score). The calculation is as follows: DrIL Tox ALF score = −0.00691292 × platelet count (per 109/l) + 0.19091500 × total bilirubin (per 1.0 mg/dl). A cut-off score of −1.08141 or greater identified patients at high risk for ALF with a sensitivity of 91 % and specificity of 76 %.
7.4 Model for End-stage Liver Disease (MELD) Score as a Predictor of Short-Term Outcome
Jeong et al. [118] investigated the predictive value of the MELD score in DILI. In this study, patients diagnosed with DILI between January 2010 and December 2012 at the Asan Medical Center in Seoul, Korea, were retrospectively analyzed. The main outcomes analyzed were liver transplantation or death within 30 days of the initial hospital visit. Of 213 patients diagnosed with DILI, 13.1 % had these poor outcomes. The most common etiologic agents were herbal folk remedies (69 %). Multivariate analysis showed that the MELD score and hemoglobin were independent predictors of poor outcome within 30 days.
8 DILI Miscellany
8.1 Intestinal Microbiota and AAP-Induced Hepatotoxicity
Variations in the intestinal microbiome are thought to influence AAP metabolism [119]. In this study, conventionally housed (CH) and germ-free (GF) mice were given large doses of AAP. It was found that the GF mice had milder evidence of ALF and reduced bilirubin levels and creatinine, although there were no significant differences in the extent of hepatocellular injury (ALT levels or percentage necrosis). The role of the intestinal microbiome in other aspects of DILI seems poised for significant future avenues of research.
8.2 Liver Injury in Drug reaction with eosinophilia and systemic symptoms (DRESS)
Drug reaction with eosinophilia and systemic symptoms (DRESS) is a syndrome with manifestations in multiple organ systems, with liver injury being the most common. Lin et al. [120] investigated the types of liver injury and factors associated with DRESS. This retrospective study from Taiwan compiled data between December 2000 and March 2013; 72 cases of DRESS were included in the study. Among these, 62 (86.1 %) involved liver injury, six of which (9.7 %) occurred before skin presentation. The liver injury patterns were as follows: 23 (37.1 %) cholestatic type, 17 (27.4 %) mixed type, and 12 (19.4 %) hepatocellular type. Patients with hepatocellular-type injuries were younger (median age 31.4 years) and patients with liver enzyme elevations more than 10× ULN were more likely to have fever and took longer to recover. These findings are similar to those of Avancini et al. [121], who found that, in 60 patients with a diagnostic suspicion of DRESS, hepatic involvement (85.1 %), fever (96.2 %), and maculopapular exanthema (85.1 %) were the most common clinical features.
Devarbhavi et al. [122] also described DILI associated with Stevens–Johnson Syndrome/toxic epidermal necrolysis (SJS/TEN). The patient cohort was obtained from a registry of DILI patients from a single center in India. Among 748 consecutive patients with DILI from 1997 to March 2015, a total of 36 (4.8 %) had associated features of SJS/TEN. The mean age was 32 years. Children and HIV patients constituted 25 % (n = 9) and 22 % (n = 8), respectively. Antiepileptic agents, sulfonamides, and antiretroviral drugs accounted for the majority of cases. Overall mortality was 36 % (n = 13) and increased to 45.5 % in the presence of jaundice. Mortality was lower in children (11 %; n = 1) and HIV patients (12.5 %; n = 1).
A recent study from Korea investigated the incidence of hepatic injury in patients with drug-induced hypersensitivity syndromes (DIHS) [123]. Among 136 patients with DIHS, which manifested as DRESS, SJS/TEN, and other forms of rash, 45 % had hepatic involvement. Liver injury was defined as ALT/AST greater than the ULN for the laboratory, and “significant” liver disease was defined as AST/ALT greater than twice the ULN. The offending agents included antibiotics (46 %), non-steroidal anti-inflammatory drugs (NSAIDS) (18 %), antiretrovirals (10 %), and allopurinol (9 %). Overall mortality was 5 %, and steroids were not found to alter outcomes of recovery.
8.3 Liver Biopsy
Although there is no pathognomonic finding on liver biopsy in patients with DILI [1], Foureau et al. [124] investigated inflammatory infiltrates in the liver that may improve our understanding of the underlying pathogenesis of DILI. Their study aimed to enumerate and characterize leukocytes infiltrating liver tissue in patients with acute DILI (n = 32) versus non-DILI causes of acute liver injury (n = 25). All biopsies showed numerous CD8 (+) T cells and macrophages. Their results found that DILI cases had significantly fewer B lymphocytes than AIH and viral hepatitis, as well as significantly fewer natural killer cells than viral hepatitis.
8.4 Risk of Underlying Viral Hepatitis and DILI
Nooredinvand et al. [125] assessed the prevalence of chronic hepatitis B virus (HBV) and HCV infection and their association with DILI in patients undergoing anti-TB therapy. This study included 429 patients with newly diagnosed TB who were due to commence anti-TB therapy. Of these patients, 270 (62.9 %) had active TB and 159 (37.1 %) had a latent infection. A total of 61 patients (14.2 %) had isolated hepatitis B core antibody (anti-HBc) positivity, 11 (2.6 %) were also HBV surface antigen (HBsAg)-positive and seven (1.6 %) were HCV-antibody positive. In contrast to other studies, no association was found between DILI and the presence of serological markers of HBV or HCV as three patients (5.3 %) with serological markers of HBV and HCV infection had DILI compared with 25 patients (9.5 %) without these viral markers.
8.5 Absence of DILI Seen With Some New Drug Classes
Perhaps as important as reports of newly described hepatotoxins tend to be, the absence of DILI seen with new drug classes is of equal clinical relevance. So it is noteworthy that, in contrast to statins and lomitapide, which are associated with varying degrees of liver injury and other potential toxicities in their role as cholesterol-lowering agents [126, 127], the newly approved proprotein convertase subtilisin kexin type 9 (PCSK9) inhibitors appear to be relatively free of any significant hepatotoxic potential. PCSK9 is secreted by hepatocytes and leads to degradation of the low-density lipoprotein receptor (LDLR) at the cell surface, thereby reducing LDL uptake and leading to increased LDL cholesterol plasma concentrations [128]. Inhibition of PCSK9 has become a novel target for LDL-lowering therapies, and several anti-PCSK9 monoclonal antibodies have proven to be effective and safe, especially for patients with severe homozygous and heterozygous familial hypercholesterolemia [129–133]. Two agents, evolocumab and alirocumab are approved, and bococizumab is under study. Liver biochemical abnormalities have been largely unaffected in clinical trials, with small elevations in aminotransferases being essentially no different than those seen with placebo or other comparators. As a result, labeling does not mention any requirement for routine liver enzyme monitoring, unlike lomitapide, or what was necessary for years with statins until recently.
8.6 DILI Consortia
The global efforts being undertaken to better understand the epidemiology, pathophysiology, and risk factors of DILI have recently been well-summarized by Andrade et al. [15]. The various national and multi-national DILI registries described, and international research consortia (including the Safe-T [134], International Serious Adverse Event Consortium [ISEAC]) [135] and the DILI-sim initiative [136]), are all aimed at improving the hepatic safety of current and future drugs and HDS products in development through discoveries in pharmacogenomics, structural alerts, and other related fields of study. The interested reader is encouraged to review these specific sources for additional information.
9 Treatment and Prevention of DILI
Apart from NAC treatment for ALF from AAP, treatment options for idiosyncratic DILI or HDS liver injury due to specific agents remains limited, and often anecdotal [1]. Early discontinuation of the suspected drug remains the most important action to be taken, along with supportive care [4]. Corticosteroids have been used in cases of DI-AIH that fail to resolve after the drug is stopped, and in cases of DILI associated with hypersensitivity reactions, including those with serious skin injury as mentioned in Sect. 8.2 above. These and additional potential therapies have recently been reviewed in detail [137]. The following paragraphs describe the potential use of NAC for non-AAP DILI, along with the potential role for cytoprotective agents and liver assist devices.
9.1 NAC for Non-AAP Acute Liver Failure
Early studies by the US ALFSG demonstrated transplant-free survival was significantly improved (40 vs. 27 %; p = 0.043) for non-AAP ALF patients with early coma stages I–II treated with intravenous NAC compared with placebo [138]. In contrast, NAC was not shown to be of benefit in adults with more advanced coma grades (III–IV), nor was any benefit in overall survival seen [138]. In the pediatric US ALFSG, children with non-AAP ALF were also shown not to benefit from NAC in non-AAP ALF [139]. Chughlay et al. [140] reported that the current evidence, based on the published literature, does not allow for any firm conclusions to be drawn one way or the other for its use in non-AAP DILI. Nevertheless, it is likely that NAC will continue to be used as a potential therapy and as a bridge to liver transplant in the setting of acute non-AAP DILI and ALF in patients outside of clinical trials, pending the results of any future studies.
9.2 Use of Cytoprotective Agents
Silibinin is the major active constituent of silymarin, a standardized extract of milk thistle seeds. Gu et al. [141] conducted a prospective, multicenter, randomized study investigating 568 patients undergoing primary treatment of pulmonary TB. The control group received conventional 2HRZE/4HR therapy (i.e., 2 months of isoniazid, rifampin, pyrazinamide, and ethambutol followed by 4 months of rifampin and isoniazid), while the experimental group received the same conventional therapy along with silibinin capsules administered orally three times daily for 8 weeks. Their statistical analysis showed no significant difference in incidence of liver injury between the two groups at each treatment period (2, 4, and 8 weeks). However, there was a statistically significant reduction in the incidence of nausea and anorexia symptoms in the silibinin group. Furthermore, after 8 weeks of treatment, a higher percentage of sputum AFB cultures were negative in the silibinin group (98.30 %) compared with the control group (92.98 %). The authors concluded that silibinin may reduce the incidence of anti-TB drug discontinuation rates, as well as improve patient compliance and outcomes of anti-TB treatment in a general population.
Luangchosiri et al. [142] also investigated the use of silymarin in preventing DILI due to anti-TB drug in a double-blind placebo-controlled trial of 55 patients. Overall, 1 of 27 (3.7 %) and 9 of 28 (32.1 %) patients developed DILI in the silymarin and placebo groups, respectively. According to these investigators, the beneficial hepato-protective mechanism of silymarin might be explained by its ability to restore superoxide dismutase.
9.3 Liver Assist Devices
The use of liver assist devices for acute liver failure remains investigational in the USA, but it is more widely utilized abroad [143]. Molecular Adsorbent Recirculating System treatment (MARS) is one such device based on the principle of albumin dialysis. It has been used in patients with ALF with varying degrees of success [143–145]. Lee et al. [146] studied the use of a novel liver-dialysis device in experimental AAP toxicity. Its use resulted in a 67 % reduction in the risk of death in AAP-induced ALF in pigs. The authors reported no adverse clinic effects from the device in this animal study and concluded that the results support additional clinical trials of the liver-dialysis device in patients with ALF.
10 Conclusions
2015 represented another year in which the knowledge base for DILI expanded in several directions. The US DILIN is now a decade old and continues to provide new information about idiosyncratic liver injury due to an increasing number of agents and in several important subgroups. Their results have corroborated many of the clinical observations of the past, including validating Hy’s Law, demonstrating the worsening prognosis of acute DILI that develops in patients with underlying liver disease, and showing that chronic injury develops in a substantial proportion of acute DILI cases. The causes of DI-ALF as seen in the Kaiser Permanente Health System in California largely reflect the findings in the more broadly based US ALFSG, with AAP being the most commonly implicated agent. An increasing percentage of DILI cases due to HDS has been seen in the USA and abroad, although the validity of some case reports and case series has been called into question. Since the diagnosis of DILI and HDS-induced liver injury is still largely one of exclusion, the challenges to causality raised by Teschke and others serve as a reminder that readers are often asked to accept the limited information in some published case reports at face value, when, in fact, delving deeper into a particular case history or having more complete serologic testing might change the causality entirely. Such diagnostic skepticism further serves to emphasize the need for a validated DILI biomarker that will take what is sometimes akin to guesswork out of current and future causality assessment.
A few new agents were added to the list of hepatotoxins in the past year, notably tolvaptan, a vasopressin V2 receptor antagonist, when used long term for the treatment of autosomal dominant adult polycystic kidney disease. Of interest, short-term use of the drug in patients with hyponatremia from SIADH (syndrome of inappropriate antidiuretic hormone), heart failure, and cirrhosis was not associated with any hepatotoxicity. Despite its efficacy in this setting, tolvaptan carries a contraindication for its use in any patient with liver disease, which effectively prevents a potentially useful agent from being used in a large segment of the hyponatremic population. In contrast to the hepatic injury seen with statins and microsomal triglyceride transfer protein MTP inhibitors (e.g., lomitapide) for the treatment of hyperlipidemia, clinical trial results with the novel LDL-lowering PCSK9 inhibitors have not demonstrated any significant hepatotoxic risk, eliminating an important safety concern in this essential therapeutic area.
The field of pharmacogenomics continues to expand, although the ultimate goal of identifying patients who are at the highest risk of developing acute DILI is currently constrained by the relatively low positive and negative predictive values of the existing discoveries. Similarly, biomarker discovery to diagnose DILI and predict outcomes and prognosis seems most advanced for cases of AAP overdose, but has lagged somewhat behind for causes of idiosyncratic DILI. Clearly, however, the future is bright for improving our understanding of the mechanisms of DILI and for the development of novel prevention and treatment strategies.
References
Lewis JH. The art and science of diagnosing and managing drug-induced liver injury in 2015 and beyond. Clin Gastroenterol Hepatol. 2015;13(12):2173–89.e8. doi:10.1016/j.cgh.2015.06.017.
Senior JR. Evolution of the Food and Drug Administration approach to liver safety assessment for new drugs: current status and challenges. Drug Saf. 2014;37(Suppl 1):S9–17. doi:10.1007/s40264-014-0182-7.
Weiler S, Merz M, Kullak-Ublick GA. Drug-induced liver injury: the dawn of biomarkers? F1000Prime Rep. 2015;7:34. doi:10.12703/P7-34.
Chalasani NP, Hayashi PH, Bonkovsky HL, Navarro VJ, Lee WM, Fontana RJ, Practice Parameters Committee of the American College of Gastroenterology. ACG Clinical Guideline: the diagnosis and management of idiosyncratic drug-induced liver injury. Am J Gastroenterol. 2014;109(7):950–66. doi:10.1038/ajg.2014.131 (quiz 967).
Björnsson ES, Hoofnagle JH. Categorization of drugs implicated in causing liver injury: Critical assessment based on published case reports. Hepatology. 2016;63(2):590–603. doi:10.1002/hep.28323 (Epub 2015 Dec 21).
Zimmerman HJ. Hepatotoxicity: the adverse effects of drugs and other chemicals on the liver. Lippincott Williams & Wilkins; 1999.
Lewis JH. Causality assessment: which is best—expert opinion or RUCAM? Clin Liver Dis. 2014;4:4–8. doi:10.1002/cld.365.
Hayashi PH. Drug-induced liver injury network causality assessment: criteria and experience in the United States. Int J Mol Sci. 2016;17(2). doi:10.3390/ijms17020201.
Davern TJ, Chalasani N, Fontana RJ, Hayashi PH, Protiva P, Kleiner DE, Drug-Induced Liver Injury Network (DILIN), et al. Acute hepatitis E infection accounts for some cases of suspected drug-induced liver injury. Gastroenterology. 2011;141(5):1665–72.e1–9. doi:10.1053/j.gastro.2011.07.051.
Dalton HR, Fellows HJ, Stableforth W, Joseph M, Thurairajah PH, Warshow U, et al. The role of hepatitis E virus testing in drug-induced liver injury. Aliment Pharmacol Ther. 2007;26(10):1429–35.
Pérez-Gracia MT, García M, Suay B, Mateos-Lindemann ML. Current Knowledge on Hepatitis E. J Clin Transl Hepatol. 2015;3(2):117–26. doi:10.14218/JCTH.2015.00009.
Centers for Disease Control and Prevention. Hepatitis E FAQs for Health Professionals. http://www.cdc.gov/hepatitis/hev/hevfaq.htm. Accessed 27 Feb 2016.
Kullak-Ublick GA, Merz M, Griffel L, Kaplowitz N, Watkins PB. Liver safety assessment in special populations (hepatitis B, C, and oncology trials). Drug Saf. 2014;37(Suppl 1):S57–62. doi:10.1007/s40264-014-0186-3.
Chalhoub WM, Sliman KD, Arumuganathan M, Lewis JH. Drug-induced liver injury: what was new in 2013? Expert Opin Drug Metab Toxicol. 2014;10(7):959–80. doi:10.1517/17425255.2014.909408.
Andrade RJ, Ortega-Alonso A, Lucena MI. Drug-Induced Liver Injury Clinical Consortia: a global research response for a worldwide health challenge. Expert Opin Drug Metab Toxicol. 2016:1–5. PubMed PMID: 26820043 [Epub ahead of print].
Chalasani N, Bonkovsky HL, Fontana R, Lee W, Stolz A, Talwalkar J, United States Drug Induced Liver Injury Network, et al. Features and outcomes of 899 patients with drug-induced liver injury: the DILIN Prospective Study. Gastroenterology. 2015;148(7):1340–52.e7. doi:10.1053/j.gastro.2015.03.006.
Reuben A. Hy’s law. Hepatology. 2004;39(2):574–8.
Fontana RJ, Hayashi PH, Gu J, Reddy KR, Barnhart H, Watkins PB, DILIN Network, et al. Idiosyncratic drug-induced liver injury is associated with substantial morbidity and mortality within 6 months from onset. Gastroenterology. 2014;147(1):96–108.e4. doi:10.1053/j.gastro.2014.03.045.
Levine C, Trivedi A, Thung SN, Perumalswami PV. Severe ductopenia and cholestasis from levofloxacin drug-induced liver injury: a case report and review. Semin Liver Dis. 2014;34(2):246–51. doi:10.1055/s-0034-1375964.
Goldberg DS, Forde KA, Carbonari DM, Lewis JD, Leidl KB, Reddy KR, et al. Population-representative incidence of drug-induced acute liver failure based on an analysis of an integrated health care system. Gastroenterology. 2015;148(7):1353–61.e3. doi:10.1053/j.gastro.2015.02.050.
Lee WM. Drug-induced acute liver failure. Clin Liver Dis. 2013;17(4):575–86, viii. doi:10.1016/j.cld.2013.07.001.
Reuben A, Koch DG, Lee WM, Acute Liver Failure Study Group. Drug-induced acute liver failure: results of a U.S. multicenter, prospective study. Hepatology. 2010;52(6):2065–76. doi:10.1002/hep.23937.
Kulkarni S, Perez C, Pichardo C, Castillo L, Gagnon M, Beck-Sague C, et al. Use of Pediatric Health Information System database to study the trends in the incidence, management, etiology, and outcomes due to pediatric acute liver failure in the United States from 2008 to 2013. Pediatr Transplant. 2015;19(8):888–95. doi:10.1111/petr.12596.
Hao K, Yu Y, He C, Wang M, Wang S, Li X. RUCAM scale-based diagnosis, clinical features and prognosis of 140 cases of drug-induced liver injury. Zhonghua Gan Zang Bing Za Zhi. 2014;22(12):938–41. doi:10.3760/cma.j.issn.1007-3418.2014.12.012.
Fontana RJ, Watkins PB, Bonkovsky HL, Chalasani N, Davern T, Serrano J, DILIN Study Group, et al. Drug-Induced Liver Injury Network (DILIN) prospective study: rationale, design and conduct. Drug Saf. 2009;32(1):55–68. doi:10.2165/00002018-200932010-00005.
Zhu Y, Li YG, Wang JB, Liu SH, Wang LF, Zhao YL, et al. Causes, features, and outcomes of drug-induced liver injury in 69 children from China. Gut Liver. 2015;9(4):525–33. doi:10.5009/gnl14184.
Douros A, Bronder E, Andersohn F, Klimpel A, Thomae M, Sarganas G, et al. Drug-induced liver injury: results from the hospital-based Berlin Case-Control Surveillance Study. Br J Clin Pharmacol. 2015;79(6):988–99. doi:10.1111/bcp.12565.
Galvin Z, McDonough A, Ryan J, Stewart S. Blood alanine aminotransferase levels >1,000 IU/l—causes and outcomes. Clin Med (Lond). 2015;15(3):244–7. doi:10.7861/clinmedicine.15-3-244.
Lammert C, Bjornsson E, Niklasson A, Chalasani N. Oral medications with significant hepatic metabolism at higher risk for hepatic adverse events. Hepatology. 2010;51(2):615–20. doi:10.1002/hep.23317.
Chen M, Suzuki A, Borlak J, Andrade RJ, Lucena MI. Drug-induced liver injury: Interactions between drug properties and host factors. J Hepatol. 2015;63(2):503–14. doi:10.1016/j.jhep.2015.04.016.
Yu K, Geng X, Chen M, Zhang J, Wang B, Ilic K, Tong W. High daily dose and being a substrate of cytochrome P450 enzymes are two important predictors of drug-induced liver injury. Drug Metab Dispos. 2014;42(4):744–50. doi:10.1124/dmd.113.056267.
Chen M, Borlak J, Tong W. High lipophilicity and high daily dose of oral medications are associated with significant risk for drug-induced liver injury. Hepatology. 2013;58(1):388–96. doi:10.1002/hep.26208.
Grove JI, Aithal GP. Human leukocyte antigen genetic risk factors of drug-induced liver toxicology. Expert Opin Drug Metab Toxicol. 2015;11(3):395–409. doi:10.1517/17425255.2015.992414.
Jiang J, Zhang X, Huo R, Li X, Yang Y, Gai Z, et al. Association study of UGT1A9 promoter polymorphisms with DILI based on systematically regional variation screen in Chinese population. Pharmacogenomics J. 2015;15(4):326–31. doi:10.1038/tpj.2014.75.
Urban TJ, Daly AK, Aithal GP. Genetic basis of drug-induced liver injury: present and future. Semin Liver Dis. 2014;34(2):123–33. doi:10.1055/s-0034-1375954.
Overby CL, Hripcsak G, Shen Y. Estimating heritability of drug-induced liver injury from common variants and implications for future study designs. Sci Rep. 2014;21(4):5762. doi:10.1038/srep05762.
Aithal GP. Pharmacogenetic testing in idiosyncratic drug-induced liver injury: current role in clinical practice. Liver Int. 2015;35(7):1801–8. doi:10.1111/liv.12836.
Rodríguez-Sáinz C, Valor L, Hernández DC, Gil J, Carbone J, Pascual-Bernaldez M, et al. Flow cytometry analysis with a new FITC-conjugated monoclonal antibody-3E12 for HLA-B*57:01 rapid screening in prevention of abacavir hypersensitivity in HIV-1-infected patients. HIV Clin Trials. 2013;14(4):160–4. doi:10.1310/hct1404-160.
Matsumoto T, Ohno M, Azuma J. Future of pharmacogenetics-based therapy fortuberculosis. Pharmacogenomics. 2014;15(5):601–7. doi:10.2217/pgs.14.38.
Hirasawa M, Hagihara K, Okudaira N, Izumi T. The possible mechanism of idiosyncratic lapatinib-induced liver injury in patients carrying human leukocyteantigen-DRB1*07:01. PLoS One. 2015;10(6):e0130928. doi:10.1371/journal.pone.0130928.
Chen R, Zhang Y, Tang S, Lv X, Wu S, Sun F, et al. The association between HLA-DQB1 polymorphism and antituberculosis drug-induced liver injury: a Case-Control Study. J Clin Pharm Ther. 2015;40(1):110–5. doi:10.1111/jcpt.12211.
Stephens C, López-Nevot MÁ, Ruiz-Cabello F, Ulzurrun E, Soriano G, Romero-Gómez M, et al. HLA alleles influence the clinical signature of amoxicillin-clavulanate hepatotoxicity. PLoS One. 2013;8(7):e68111. doi:10.1371/journal.pone.0068111.
Daly AK, Donaldson PT, Bhatnagar P, Shen Y, Pe’er I, Floratos A, DILIGEN Study, et al. International SAE Consortium. HLA-B*5701 genotype is a major determinant of drug-induced liver injury due to flucloxacillin. Nat Genet. 2009;41(7):816–9. doi:10.1038/ng.379.
Watkins PB, Lewis JH, Kaplowitz N, Alpers DH, Blais JD, Smotzer DM, et al. Clinical pattern of tolvaptan-associated liver injury in subjects with autosomal dominant polycystic kidney disease: analysis of clinical trials database. Drug Saf. 2015;38(11):1103–13. doi:10.1007/s40264-015-0327-3.
Russmann S, Niedrig DF, Budmiger M, Schmidt C, Stieger B, Hürlimann S, et al. Rivaroxaban postmarketing risk of liver injury. J Hepatol. 2014;61(2):293–300. doi:10.1016/j.jhep.2014.03.026.
Liakoni E, Rätz Bravo AE, Krähenbühl S. Hepatotoxicity of new oral anticoagulants (NOACs). Drug Saf. 2015;38(8):711–20. doi:10.1007/s40264-015-0317-5.
Raschi E, Poluzzi E, Koci A, Salvo F, Pariente A, Biselli M, et al. Liver injury with novel oral anticoagulants: assessing post-marketing reports in the US Food and Drug Administration adverse event reporting system. Br J Clin Pharmacol. 2015;80(2):285–93. doi:10.1111/bcp.12611.
Anastasia EJ, Rosenstein RS, Bergsman JA, Parra D. Use of apixaban after development of suspected rivaroxaban-induced hepatic steatosis; a case report. Blood Coagul Fibrinolysis. 2015;26(6):699–702. doi:10.1097/MBC.0000000000000363.
Hahn KJ, Morales SJ, Lewis JH. Enoxaparin-induced liver injury: case report and review of the literature and FDA Adverse Event Reporting System (FAERS). Drug Saf Case Rep. 2015;2:17.
Soriano V, Barreiro P, de Mendoza C, Peña JM. Hepatic decompensation with sofosbuvir plus simeprevir in a patient with Child-Pugh B compensated cirrhosis. Antivir Ther. 2015;. doi:10.3851/IMP2969.
Okajima A, Yamaguchi K, Taketani H, Hara T, Ishiba H, Seko Y, et al. Drug-induced liver injury in a chronic hepatitis C patient treated by peginterferon, ribavirin and simeprevir. Hepatol Res. 2015;45(10):E156–60. doi:10.1111/hepr.12477.
Igawa T, Fushimi S, Matsuo R, Ikeda F, Nouso K, Yoshino T, et al. Severe liver injury associated with simeprevir plus pegylated interferon/ribavirin therapy in a patient with treatment-naïve genotype 1b hepatitis C virus: a case report. Clin J Gastroenterol. 2014;7(5):465–70. doi:10.1007/s12328-014-0527-x.
Stine JG, Intagliata N, Shah NL, Argo CK, Caldwell SH, Lewis JH, et al. Hepatic decompensation likely attributable to simeprevir in patients with advanced cirrhosis. Dig Dis Sci. 2015;60(4):1031–5. doi:10.1007/s10620-014-3422-x.
Fujii Y, Uchida Y, Mochida S. Drug-induced immunoallergic hepatitis during combination therapy with daclatasvir and asunaprevir. Hepatology. 2015;61(1):400–1. doi:10.1002/hep.27559.
Shibata S, Umemura T, Komatsu M, Tanaka E. Severe hepatotoxicity associated with asunaprevir and daclatasvir in chronic hepatitis C. Hepatology. 2015. doi:10.1002/hep.28113 [Epub ahead of print].
FDA Drug Safety Communication: FDA warns of serious liver injury risk with hepatitis C treatments Viekira Pak and Technivie. 2015. http://www.fda.gov/Drugs/DrugSafety/ucm468634.htm. Accessed on 20 Dec 2015.
Zeuzem S, Ghalib R, Reddy KR, Pockros PJ, Ben Ari Z, Zhao Y, et al. Grazoprevir-elbasvir combination therapy for treatment-naive cirrhotic and noncirrhotic patients with chronic hepatitis C virus genotype 1, 4, or 6 infection: a randomized trial. Ann Intern Med. 2015;163(1):1–13. doi:10.7326/M15-0785.
U.S. Food and Drug Administration. http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm483828.htm. Accessed 27 Feb 2016.
Hayes W, Tschumi S, Ling SC, Feber J, Kirschfink M, Licht C. Eculizumab hepatotoxicity in pediatric aHUS. Pediatr Nephrol. 2015;30(5):775–81. doi:10.1007/s00467-014-2990-5.
Ghabril M, Bonkovsky HL, Kum C, Davern T, Hayashi PH, Kleiner DE, US Drug-Induced Liver Injury Network, et al. Liver injury from tumor necrosis factor-α antagonists: analysis of thirty-four cases. Clin Gastroenterol Hepatol. 2013;11(5):558–564.e3. doi:10.1016/j.cgh.2012.12.025.
Rodrigues S, Lopes S, Magro F, Cardoso H, Horta e Vale AM, Marques M, et al. Autoimmune hepatitis and anti-tumor necrosis factor alpha therapy: a single center report of 8 cases. World J Gastroenterol. 2015;21(24):7584–8. doi:10.3748/wjg.v21.i24.7584.
Shelton E, Chaudrey K, Sauk J, Khalili H, Masia R, Nguyen DD, et al. New onset idiosyncratic liver enzyme elevations with biological therapy in inflammatory bowel disease. Aliment Pharmacol Ther. 2015;41(10):972–9. doi:10.1111/apt.13159.
French JB, Bonacini M, Ghabril M, Foureau D, Bonkovsky HL. Hepatotoxicity associated with the use of anti-TNF-α agents. Drug Saf. 2016;39(3):199–208. doi:10.1007/s40264-015-0366-9.
Bertrand A, Kostine M, Barnetche T, Truchetet ME, Schaeverbeke T. Immune related adverse events associated with anti-CTLA-4 antibodies: systematic review and meta-analysis. BMC Med. 2015;4(13):211. doi:10.1186/s12916-015-0455-8.
Cheng R, Cooper A, Kench J, Watson G, Bye W, McNeil C, et al. Ipilimumab-induced toxicities and the gastroenterologist. J Gastroenterol Hepatol. 2015;30(4):657–66. doi:10.1111/jgh.12888.
Serper M, Wolf MS, Parikh NA, Tillman H, Lee WM, Ganger DR. Risk factors, clinical presentation, and outcomes in overdose with acetaminophen alone or with combination products: results from the acute liver failure study group. J Clin Gastroenterol. 2016;50(1):85–91. doi:10.1097/MCG.0000000000000378.
King JP, McCarthy DM, Serper M, Jacobson KL, Mullen RJ, Parker RM, et al. Variability in acetaminophen labeling practices: a missed opportunity to enhance patient safety. J Med Toxicol. 2015;11(4):410–4. doi:10.1007/s13181-015-0464-1.
Chan ST, Chan CK, Tse ML. Paracetamol overdose in Hong Kong: is the 150-treatment line good enough to cover patients with paracetamol-induced liver injury? Hong Kong Med J. 2015;21(5):389–93. doi:10.12809/hkmj144481.
McGovern AJ, Vitkovitsky IV, Jones DL, Mullins ME. Can AST/ALT ratio indicate recovery after acute paracetamol poisoning? Clin Toxicol (Phila). 2015;53(3):164–7. doi:10.3109/15563650.2015.1006399.
Hawton K, Bergen H, Simkin S, Dodd S, Pocock P, Bernal W, et al. Long term effect of reduced pack sizes of paracetamol on poisoning deaths and liver transplant activity in England and Wales: interrupted time series analyses. BMJ. 2013;7(346):f403. doi:10.1136/bmj.f403.
Gulmez SE, Larrey D, Pageaux GP, Bernuau J, Bissoli F, Horsmans Y, et al. Liver transplant associated with paracetamol overdose: results from the seven-country SALT study. Br J Clin Pharmacol. 2015;80(3):599–606. doi:10.1111/bcp.12635.
McGill MR, Jaeschke H. MicroRNAs as signaling mediators and biomarkers of drug- and chemical-induced liver injury. J Clin Med. 2015;4(5):1063–78. doi:10.3390/jcm4051063.
McGill MR, Jaeschke H. Mechanistic biomarkers in acetaminophen-induced hepatotoxicity and acute liver failure: from preclinical models to patients. Expert Opin Drug Metab Toxicol. 2014;10(7):1005–17. doi:10.1517/17425255.2014.920823.
Dear JW, Antoine DJ. Stratification of paracetamol overdose patients using new toxicity biomarkers: current candidates and future challenges. Expert Rev Clin Pharmacol. 2014;7(2):181–9. doi:10.1586/17512433.2014.880650.
Wang Y, Chen T, Tong W. miRNAs and their application in drug-induced liver injury. Biomark Med. 2014;8(2):161–72. doi:10.2217/bmm.13.147.
Antoine DJ, Dear JW, Lewis PS, Platt V, Coyle J, Masson M, et al. Mechanistic biomarkers provide early and sensitive detection of acetaminophen-induced liver injury at first presentation to hospital. Hepatology. 2013;58(2):777–87. doi:10.1002/hep.26294.
Yang X, Salminen WF, Shi Q, Greenhaw J, Gill PS, Bhattacharyya S, et al. Potential of extracellular microRNAs as biomarkers of acetaminophen toxicity in children. Toxicol Appl Pharmacol. 2015;284(2):180–7. doi:10.1016/j.taap.2015.02.013.
Vliegenthart AD, Shaffer JM, Clarke JI, Peeters LE, Caproali A, Bateman DN, et al. Comprehensive microRNA profiliing acetaminophen toxicity identifies novel ciruclating biomarkers for human liver and kidney injury. Sci Rep. 2015;5:15501. doi:10.1038/srep15501.
Thulin P, Nordahl G, Gry M, Yimer G, Aklillu E, Makonnen E, et al. Keratin-18 and microRNA-122 comlement alanine aminotransferase as novel safety biomarkers for drug-induced liver injury in two human cohorts. Liver Int. 2014;34(3):367–8. doi:10.1111/liv.12322.
Senior JR. New biomarkers for drug-induced liver injury: are they really better? What do they diagnose? Liver Int. 2014;34(3):325–7.
Stutchfield BM, Antoine DJ, Mackinnon AC, Gow DJ, Bain CC, Hawley CA, et al. CSF1 restores innate immunity after liver injury in mice and serum levels indicate outcomes of patients with acute liver failure. Gastroenterology. 2015;149(7):1896–1909.e14. doi:10.1053/j.gastro.2015.08.053.
Devarbhavi H, Singh R, Patil M, Sheth K, Adarsh CK, Balaraju G. Outcome and determinants of mortality in 269 patients with combination anti-tuberculosis drug-induced liver injury. J Gastroenterol Hepatol. 2013;28(1):161–7. doi:10.1111/j.1440-1746.2012.07279.x.
Hayashi PH, Fontana RJ, Chalasani NP, Stolz AA, Talwalkar JA, Navarro VJ US Drug-Induced Liver Injury Network Investigators, et al. Under-reporting and poor adherence to monitoring guidelines for severe cases of isoniazid hepatotoxicity. Clin Gastroenterol Hepatol. 2015;13(9):1676–82.e1. doi:10.1016/j.cgh.2015.02.024.
Martinez MA, Vuppalanchi R, Fontana RJ, Stolz A, Kleiner DE, Hayashi PH, et al. Clinical and histologic features of azithromycin-induced liver injury. Clin Gastroenterol Hepatol. 2015;13(2):369–376.e3. doi:10.1016/j.cgh.2014.07.054.
Alqahtani SA, Kleiner DE, Ghabril M, Gu J, Hoofnagle JH, Rockey DC, Drug-Induced Liver Injury Network (DILIN) Study Investigators. Identification and characterization of cefazolin-induced liver injury. Clin Gastroenterol Hepatol. 2015;13(7):1328–1336.e2. doi:10.1016/j.cgh.2014.11.036.
Dandakis D, Petrogiannopoulos C, Hartzoulakis G, Flevaris C, Lagoutari D, Drakogiogos G, et al. Cholestatic hepatitis associated with amoxicillin-clavulanic acid combination. A case report. Ann Gastroenterol. 2002;15(1):85–7.
Orman ES, Conjeevaram HS, Vuppalanchi R, Freston JW, Rochon J, Kleiner DE, DILIN Research Group, et al. Clinical and histopathologic features of fluoroquinolone-induced liver injury. Clin Gastroenterol Hepatol. 2011;9(6):517–523.e3. doi:10.1016/j.cgh.2011.02.019.
Yeong TT, Lim KH, Goubet S, Parnell N, Verma S. Natural history and outcomes in drug-induced autoimmune hepatitis. Hepatol Res. 2015. doi:10.1111/hepr.12532.
Björnsson E, Talwalkar J, Treeprasertsuk S, Kamath PS, Takahashi N, Sanderson S, et al. Drug-induced autoimmune hepatitis: clinical characteristics and prognosis. Hepatology. 2010;51(6):2040–8. doi:10.1002/hep.23588.
Bessone F, Lucena MI, Roma MG, Stephens C, Medina-Cáliz I, Frider B, et al. Cyproterone acetate induces a wide spectrum of acute liver damage including corticosteroid-responsive hepatitis: report of 22 cases. Liver Int. 2015. doi:10.1111/liv.12899.
Friedrich ME, Akimova E, Huf W, Konstantinidis A, Papageorgiou K, Winkler D, et al. Drug-induced liver injury during antidepressant treatment: results of AMSP, a drug surveillance program. Int J Neuropsychopharmacol. 2015. doi:10.1093/ijnp/pyv126.
Gahr M, Zeiss R, Lang D, Connemann BJ, Schönfeldt-Lecuona C. Hepatotoxicity associated with agomelatine and other antidepressants: Disproportionality analysis using pooled pharmacovigilance data from the Uppsala Monitoring Centre. J Clin Pharmacol. 2015;55(7):768–73. doi:10.1002/jcph.475.
Davidov Y, Har-Noy O, Pappo O, Achiron A, Dolev M, Ben-Ari Z. Methylprednisolone-induced liver injury: case report and literature review. J Dig Dis. 2016;17(1):55–62. doi:10.1111/1751-2980.12306.
Caster O, Conforti A, Viola E, Edwards IR. Methylprednisolone-induced hepatotoxicity: experiences from global adverse drug reaction surveillance. Eur J Clin Pharmacol. 2014;70(4):501–3. doi:10.1007/s00228-013-1632-3.
Navarro VJ, Lucena MI. Hepatotoxicity induced by herbal and dietary supplements. Semin Liver Dis. 2014;34(2):172–93. doi:10.1055/s-0034-1375958.
Stickel F, Shouval D. Hepatotoxicity of herbal and dietary supplements: an update. Arch Toxicol. 2015;89(6):851–65. doi:10.1007/s00204-015-1471-3.
Raschi E, De Ponti F. Drug- and herb-induced liver injury: progress, current challenges and emerging signals of post-marketing risk. World J Hepatol. 2015;7(13):1761–71. doi:10.4254/wjh.v7.i13.1761.
Stournaras E, Tziomalos K. Herbal medicine-related hepatotoxicity. World J Hepatol. 2015;7(19):2189–93. doi:10.4254/wjh.v7.i19.2189.
Teschke R, Wolff A, Frenze C, Schulze J. Review article: herbal hepatotoxicity—an update on traditional Chinese medicine preparations. Aliment Pharmacol Ther. 2014:40 (1);32–50. doi:10.1111/apt.12798.
Navarro VJ, Barnhart H, Bonkovsky HL, Davern T, Fontana RJ, Grant L, et al. Liver injury from herbals and dietary supplements in the U.S. Drug-Induced Liver Injury Network. Hepatology. 2014;60(4):1399–408. doi:10.1002/hep.27317.
Lee WJ, Kim HW, Lee HY, Son CG. Systematic review on herb-induced liver injury in Korea. Food Chem Toxicol. 2015;84:47–54. doi:10.1016/j.fct.2015.06.004.
Hayashi PH, Barnhart HX, Fontana RJ, Chalasani N, Davern TJ, Talwalkar JA, et al. Reliability of causality assessment for drug, herbal and dietary supplement hepatotoxicity in the Drug-Induced Liver Injury Network (DILIN). Liver Int. 2015;35(5):1623–32. doi:10.1111/liv.12540.
Teschke R, Frenzel C, Schulze J, Eickhoff A. Herbal hepatotoxicity: challenges and pitfalls of causality assessment methods. World J Gastroenterol. 2013;19(19):2864–82. doi:10.3748/wjg.v19.i19.2864.
Roytman MM, Porzgen P, Lee CL, Huddleston L, Kuo TT, Bryant-Greenwood P, et al. Outbreak of severe hepatitis linked to weight-loss supplement OxyELITE Pro. Am J Gastroenterol. 2014;190:1296–8. doi:10.1038/ajg.2014.159.
Foley S, Butlin E, Shields W, Lacey B. Experience with OxyELITE pro and acute liver injury in active duty service members. Dig Dis Sci. 2014;59(12):3117–21. doi:10.1007/s10620-014-3221-4.
Teschke R, Schulze J, Eickhoff A, Wolff A, Frenzel C. Mysterious Hawaii liver disease case—naproxen overdose as cause rather than OxyElitePro. J Liver Clin Res. 2015;2(2):1013.
Teschke R, Schwarzenboeck A, Frenzel C, Schulze J, Eickhoff A, Wolff A. The mystery of the Hawaii liver disease cluster in summer 2013: A pragmatic and clinical approach to solve the problem. Ann Hepatol. 2015;15(1):91–109.
Klontz KC, DeBeck HJ, LeBlanc P, Mogen KM, Wolpert BJ, Sabo JL, et al. The role of adverse event reporting in the FDA response to multistate outbreak of liver disease associated with a dietary supplement. Public Health Rep. 2015;130(5):526–32.
Johnston DI, Chang A, Viray M, Chatham-Stephens K, He H, Taylor E. Hepatotoxicity associated with the dietary supplement OxyELITE Pro—Hawaii, 2013. Drug Test Anal. 2015. doi:10.1002/dta.1894.
Navarro VJ, Bonkovsky HL, Hwang SI, Vega M, Barnhart H, Serrano J. Catechins in dietary supplements and hepatotoxicity. Dig Dis Sci. 2013;58(9):2682–90. doi:10.1007/s10620-013-2687-9.
Fontana RJ, Ellerbe C, Durkalski VE, Rangnekar A, Reddy RK, Stravitz T, US Acute Liver Failure Study Group, et al. Two-year outcomes in initial survivors with acute liver failure: results from a prospective, multicentre study. Liver Int. 2015;35(2):370–80. doi:10.1111/liv.12632.
Fontana RJ, Hayashi PH, Barnhart PH, Kleiner DE, Reddy KR, Chalasan N, et al. Persistent liver biochemistry abnormalities are more common in older patients and those with cholestatic drug induced liver injury. Am J Gastroenterol. 2015;110(10):1450–9. doi:10.1038/ajg.2015.283.
Aithal PG, Day CP. The natural history of histologically proved drug induced liver disease. Gut. 1999;44(5):731–5.
Andrade RJ, Lucena MI, Kaplowitz N, García-Muņoz B, Borraz Y, Pachkoria K, et al. Outcome of acute idiosyncratic drug-induced liver injury: long-term follow-up in a hepatotoxicity registry. Hepatology. 2006;44(6):1581–8.
Björnsson E, Davidsdottir L. The long-term follow-up after idiosyncratic drug-induced liver injury with jaundice. J Hepatol. 2009;50(3):511–7. doi:10.1016/j.jhep.2008.
Robles-Diaz M, Lucena MI, Kaplowitz N, Stephens C, Medina-Cáliz I, González-Jimenez A, SLatinDILI Network; Safer and Faster Evidence-based Translation Consortium, et al. Use of Hy’s law and a new composite algorithm to predict acute liver failure in patients with drug-induced liver injury. Gastroenterology. 2014;147(1):109–118.e5. doi:10.1053/j.gastro.2014.03.050.
Lo Re V 3rd, Haynes K, Forde KA, Goldberg DS, Lewis JD, Carbonari DM, et al. Risk of acute liver failure in patients with drug-induced liver injury: evaluation of Hy’s law and a new prognostic model. Clin Gastroenterol Hepatol. 2015;13(13):2360–8. doi:10.1016/j.cgh.2015.06.020.
Jeong R, Lee YS, Sohn C, Jeon J, Ahn S, Lim KS. Model for end-stage liver disease score as a predictor of short-term outcome in patients with drug-induced liver injury. Scand J Gastroenterol. 2015;50(4):439–46. doi:10.3109/00365521.2014.958094.
Possamai LA, McPhail MJ, Khamri W, Wu B, Concas D, Harrison M, et al. The role of intestinal microbiota in murine models of acetaminophen-induced hepatotoxicity. Liver Int. 2015;35(3):764–73. doi:10.1111/liv.12689.
Lin IC, Yang HC, Strong C, Yang CW, Cho YT, Chen KL, et al. Liver injury in patients with DRESS: a clinical study of 72 cases. J Am Acad Dermatol. 2015;72(6):984–91. doi:10.1016/j.jaad.2015.02.1130.
Avancini J, Maragno L, Santi CG, Criado PR. Drug reaction with eosinophilia and systemic symptoms/drug-induced hypersensitivity syndrome: clinical features of 27 patients. Clin Exp Dermatol. 2015;40(8):851–9. doi:10.1111/ced.12682.
Devarbhavi H, Raj S, Aradya VH, Rangegowda VT, Veeranna GP, Singh R, et al. Drug-induced liver injury associated with Stevens-Johnson syndrome/toxic epidermal necrolysis: patient characteristics, causes and outcome in 36 cases. Hepatology. 2015. doi:10.1002/hep.28270.
Lee T, Lee YS, Yoon SY, Kim S, Bae YJ, Kwon HS, et al. Characteristics of liver injury in drug-induced systemic hypersensitivity reactions. J Am Acad Dermatol. 2013;69(3):407–15. doi:10.1016/j.jaad.2013.03.024.
Foureau DM, Walling TL, Maddukuri V, Anderson W, Culbreath K, Kleiner DE, et al. Comparative analysis of portal hepatic infiltrating leucocytes in acute drug-induced liver injury, idiopathic autoimmune and viral hepatitis. Clin Exp Immunol. 2015;180(1):40–51. doi:10.1111/cei.12558.
Nooredinvand HA, Connell DW, Asgheddi M, Abdullah M, O’Donoghue M, Campbell L, et al. Viral hepatitis prevalence in patients with active and latent tuberculosis. World J Gastroenterol. 2015;21(29):8920–6. doi:10.3748/wjg.v21.i29.8920.
Lewis JH. Clinical perspective: statins and the liver–harmful or helpful? Dig Dis Sci. 2012;57(7):1754–63. doi:10.1007/s10620-012-2207-3.
Cuchel M, Meagher EA, du Toit Theron H, Blom DJ, Marais AD, Hegele RA, Phase 3 HoFH Lomitapide Study investigators, et al. Efficacy and safety of a microsomal triglyceride transfer protein inhibitor in patients with homozygous familial hypercholesterolaemia: a single-arm, open-label, phase 3 study. Lancet. 2013;381(9860):40–6. doi:10.1016/S0140-6736(12)61731-0.
Lambert G, Sjouke B, Choque B, Kastelein JJ, Hovingh GK. The PCSK9 decade. J Lipid Res. 2012;53(12):2515–24. doi:10.1194/jlr.R026658 (Epub 2012 Jul 17. Review).
Bergeron N, Phan BA, Ding Y, Fong A, Krauss RM. Proprotein convertase subtilisin/kexin type 9 inhibition: a new therapeutic mechanism for reducing cardiovascular disease risk. Circulation. 2015;132(17):1648–66. doi:10.1161/CIRCULATIONAHA.115.016080.
Raal FJ, Stein EA, Dufour R, Turner T, Civeira F, Burgess L, et al. RUTHERFORD-2 Investigators. PCSK9 inhibition with evolocumab (AMG 145) in heterozygous familial hypercholesterolaemia (RUTHERFORD-2): a randomised, double-blind, placebo-controlled trial. Lancet. 2015;385(9965):331–40. doi:10.1016/S0140-6736(14)61399-4.
Raal FJ, Honarpour N, Blom DJ, Hovingh GK, Xu F, Scott R, et al. TESLA Investigators. Inhibition of PCSK9 with evolocumab in homozygous familial hypercholesterolaemia (TESLA Part B): a randomised, double-blind, placebo-controlled trial. Lancet. 2015;385(9965):341–50. doi:10.1016/S0140-6736(14)61374-X.
Sabatine MS, Wasserman SM, Stein EA. PCSK9 Inhibitors and Cardiovascular Events. N Engl J Med. 2015;373(8):774–5.
Gupta S. LDL cholesterol, statins and PCSK 9 inhibitors. Indian Heart J. 2015;67(5):419–24. doi:10.1016/j.ihj.2015.05.020 (Epub 2015 Aug 5. Review).
Safe-T Consortium. http://www.imi-safe-t.eu. Accessed 27 Feb 2016.
International SAE Consortium. http://www.saeconsortium.org. Accessed 27 Feb 2016.
DILIsym. http://www.dilisym.com. Accessed 27 Feb 2016.
Stine JG, Lewis JH. Current and future directions in the treatment and prevention of drug-induced liver injury: a systematic review. Expert Rev Gastroenterol Hepatol. 2015;25:1–20.
Lee WM, Hynan LS, Rossaro L, Fontana RJ, Stravitz RT, Larson AM, Acute Liver Failure Study Group, et al. Intravenous N-acetylcysteine improves transplant-free survival in early stage non-acetaminophen acute liver failure. Gastroenterology. 2009;137(3):856–64, 864.e1. doi:10.1053/j.gastro.2009.06.006.
Squires RH, Dhawan A, Alonso E, Narkewicz MR, Shneider BL, Rodriguez-Baez N, Pediatric Acute Liver Failure Study Group, et al. Intravenous N-acetylcysteine in pediatric patients with nonacetaminophen acute liver failure: a placebo-controlled clinical trial. Hepatology. 2013;57(4):1542–9. doi:10.1002/hep.26001.
Chughlay MF, Kramer N, Spearman CW, Werfalli M, Cohen K. N-Acetylcysteine for non-paracetamol drug-induced liver injury: a systematic review. Br J Clin Pharmacol. 2016. doi:10.1111/bcp.12880.
Gu J, Tang SJ, Tan SY, Wu Q, Zhang X, Liu CX, et al. An open-label, randomized and multi-center clinical trial to evaluate the efficacy of silibinin in preventing drug-induced liver injury. Int J Clin Exp Med. 2015;8(3):4320–7.
Luangchosiri C, Thakkinstian A, Chitphuk S, Stitchantrakul W, Petraksa S, Sobhonslidsuk A. A double-blinded randomized controlled trial of silymarin for the prevention of antituberculosis drug-induced liver injury. BMC Complement Altern Med. 2015;15(1):334. doi:10.1186/s12906-015-0861-7.
Tsipotis E, Shuja A, Jaber BL. albumin dialysis for liver failure: a systematic review. Adv Chronic Kidney Dis. 2015;22(5):382–90. doi:10.1053/j.ackd.2015.05.004.
Olin P, Hausken J, Foss A, Karlsen TH, Melum E, Haugaa H. Continuous molecular adsorbent recirculating system treatment in 69 patients listed for liver transplantation. Scand J Gastroenterol. 2015;50(9):1127–34. doi:10.3109/00365521.2015.1027262.
Maiwall R, Maras JS, Nayak SL, Sarin SK. Liver dialysis in acute-on-chronic liver failure: current and future perspectives. Hepatol Int. 2014;8(Suppl 2):505–13. doi:10.1007/s12072-014-9534-8.
Lee KC, Baker LA, Stanzani G, Alibhai H, Chang YM, Jimenez Palacios C, et al. Extracorporeal liver assist device to exchange albumin and remove endotoxin in acute liver failure: Results of a pivotal pre-clinical study. J Hepatol. 2015;63(3):634–42. doi:10.1016/j.jhep.2015.04.020.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
No sources of funding were used to assist in the preparation of this study.
Conflict of interest
Dr. Philip Sarges and Dr. Joshua Steinberg have no conflicts of interest that are directly relevant to the content of this study. Dr. James H. Lewis is a consultant to Otsuka America Pharmaceutical, Inc., Astra Zeneca, Sanofi, Lundbeck Pharmaceuticals, GlaxoSmithKline, and Takeda Pharmaceuticals; and is a member of speaker bureaus for Gilead Sciences and Bristol Myers Squibb.
Rights and permissions
About this article
Cite this article
Sarges, P., Steinberg, J.M. & Lewis, J.H. Drug-Induced Liver Injury: Highlights from a Review of the 2015 Literature. Drug Saf 39, 801–821 (2016). https://doi.org/10.1007/s40264-016-0427-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-016-0427-8