Abstract
Background
Neural injuries such as spinal cord injuries, traumatic brain injuries, or nerve transection injuries pose a major health problem. Neurotrophins such as nerve growth factor (NGF) or brain-derived neurotrophic factor (BDNF) have been shown to improve the outcome of neural injuries in several pre-clinical models, but their use in clinics is limited by the lack of a robust delivery system that enhances their bioavailability and half-life.
Objectives
We describe two fusion proteins comprising NGF or BDNF fused with elastin-like peptides (ELPs). The aim of this study was to investigate the biological activity of neurotrophin-ELP (N-ELP) fusion proteins via in vitro culture models.
Methods
NGF and BDNF were cloned in front of an elastin-like polypeptide sequence V40C2. These proteins were expressed in bacteria as inclusion bodies. These fusion proteins underwent solubilization via 8 M urea and purification via inverse transition cycling (ITC). We measured the particle size and the effect of temperature on precipitated particles using dynamic light scattering (DLS). We used western blot analysis to confirm the specificity of NGF-ELP to tropomyosin receptor kinase A (TrkA) antibody and to confirm the specificity of BDNF-ELP to TrkB antibody. PC12 cells were used to perform a neurite outgrowth assay to determine the biological activity of NGF-ELP. Bioactivity of BDNF-ELP was ascertained via transfecting human epithelial kidney (HEK 293-T) cells to express the TrkB receptor.
Results
The proteins were successfully purified to high homogeneity by exploiting the phase transition property of ELPs and urea, which solubilize inclusion bodies. Using PC12 neurite outgrowth assay, we further demonstrated that the biological activity of NGF was retained in the fusion. Similarly, BDNF-ELP phosphorylated the TrkB receptor, suggesting the biological activity of BDNF was also retained in the fusion. We further show that owing to the phase transition property of ELPs in the fusion, these proteins self-assembled into nanoparticles at their respective transition temperatures.
Conclusion
These fusion proteins are useful for neural regeneration, as they not only retain the biological activity of the neurotrophin but also self-assemble into nanoparticles, thereby simultaneously serving as drug-delivery vehicles. These nanoparticles can serve as drug depots and will increase bioavailability by limiting neurotrophin loss due to diffusion, thereby allowing controlled spatio-temporal delivery of the neurotrophin.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Bioactive fusion proteins demonstrated reversibility after they formed inactive inclusion bodied proteins and were denatured prior to purification. |
Fusion proteins retained the performance characteristics of neurotrophins and the phase transition properties of elastin-like peptides. |
Fusion proteins self-assembled into nanoparticles around physiological temperatures. |
1 Introduction
Neural injuries such as spinal cord injuries, traumatic brain injuries, or nerve transection injuries pose a major health problem, especially among male adolescents and young adults aged 15–24 years and among people of both sexes aged ≥75 years. Approximately 1.4 million people are estimated to experience traumatic brain injury each year in the USA, costing an estimated $US56 billion. Of these people, 50,000 will die from head injury. Every year, around the world, between 250,000 and 500,000 people experience a spinal cord injury (SCI). More than 1 million Americans live day to day with the disabling effects of SCI. The costs of managing the care of patients with SCI approaches $US4 billion each year. Despite several advances in neuroscience, current clinical treatment options for these injuries are severely restricted. As the regenerative capacity of the nervous system is limited, treatment options are unable to restore complete function to these patients. In the peripheral nervous system, direct end-to-end surgical reconnection and nerve autographs are used to repair the injury gaps in nerves [1]. However, these approaches are limited by a shortage of donor grafts, potential loss of function at the donor sites, and the requirement for multiple surgeries. Nerve regeneration in the central nervous system (CNS) is even more challenging as the inhibitory environment formed after injury in the CNS restricting nerve repair [2]. Demand is increasing for a treatment that will be less invasive and more cost efficient that will also increase motor and sensory function and elicit axonal regeneration [3].
Neurotrophins such as nerve growth factor (NGF), neurotrophin (NT)-3, brain-derived neurotrophic factor (BDNF) are a family of growth factors that play crucial roles in the development and maintenance of the nervous system [4]. Consequently, they have been widely investigated for their influence on cell mortality and differentiation and function in the CNS and peripheral nervous system. Neurons not receiving appropriate quantities of neurotrophins undergo apoptosis. For signaling, each neurotrophin binds to its specific high-affinity tropomyosin receptor kinase (Trk) receptor, with NGF, BDNF, and NT-3 signaling through the TrkA, TrkB, and TrkC receptors, respectively [4]. NGF plays critical roles in sympathetic and sensory neuron survival and maintenance [5], NT-3 plays an important role in neurogenesis [6], and BDNF helps direct normal neural development and is involved with synaptic transmission and maintaining plasticity [7]. Additionally, all three possess neuroprotective properties that are crucial for nerve repair after injury. Thus, they have been widely used for treatment of a variety of neural injuries [8]. NGF has been investigated for treatment of peripheral nerve injuries, and NT-3 has been shown to promote survival and outgrowth of motor neurons after SCIs and to improve peripheral nerve regeneration [4]. The potential of BDNF to treat SCIs has also been investigated [9]. The successful application of neurotrophins in neuronal repair depends on a suitable delivery system that ensures the bioavailability of the neurotrophin at the injury site [4, 10]. Due to the short in vivo half-life of neurotrophins, sustained delivery to the injury site results in significantly better recovery than a single injection [10]. Some delivery strategies include the use of scaffolds [4], conjugation of the neurotrophins to fibrin gels [11], mini-pumps [12], hydrogels [13], or gene therapy [14]. However, strategies requiring chemical conjugation or polymer delivery vehicles still require large quantities of growth factor, making these therapies prohibitively expensive. On the other hand, while gene therapy has proven effective in some cases, several extracellular and intracellular barriers must be overcome to obtain successful expression of the transgene [15]. Moreover, once these barriers have been successfully overcome, there is generally little control over the duration of expression or amount of growth factor produced by the transfected cell [16, 17]. Furthermore, in instances where the delivery of multiple growth factors is desired, the recalcitrance of some transfected cells to further transfections may be an issue.
Elastin-like peptides (ELPs) are a class of stimuli-responsive biopolymers that consist of a peptide repeat VPGXG, where X can be any amino acid except proline. An interesting property of ELPs is their ability to undergo phase transition at physiological temperatures. ELPs are soluble in aqueous solutions at a temperature below their lower critical solution temperature (LCST). However, as the temperature is raised above their LCST, they undergo an entropically driven contraction, rendering them insoluble. This property enables recombinant ELPs to be expressed in bacteria and rapidly purified to high homogeneity using inverse temperature cycling (ITC) [18]. Moreover, our laboratory and several others have shown that biologically active moieties can be fused to ELPs recombinantly [19, 20]. The fusion proteins retain the biological activity of the fused moiety as well as the physical phase transitioning property of ELPs [20]. Consequently, they can be expressed in bacteria and purified to high homogeneity using ITC. Additionally, different ELP sequences can be chosen or designed so that the fusion protein undergoes molecular self-assemblies, resulting in the formation of different nano and micro structures when exposed to an external stimulus such as changes in temperature or pH. Different structures refer to, but are not limited to, injectable hydrogels [21], thermoresponsive extracellular matrix [22], nanofibers [23], and nanoparticles [20]. ELPs that contain the amino acid cysteine are capable of forming disulfide cross-linked hydrogels in situ [21]. These structures are useful not only as scaffolds providing the topographical cues for nerve regeneration but also as drug-delivery vehicles.
Here, we report the expression and purification of two fusion proteins, namely NGF-ELP and BDNF-ELP. The fusion proteins were expressed in bacteria as inclusion bodies. The aim of this study was to evaluate the biological activity of neurotrophin-ELP fusion proteins via in vitro culture models after the N-ELP fusion proteins formed inclusion bodies.
2 Methods
2.1 Synthesis of Genes Encoding Neurotrophin-Elastin-Like Peptide (ELP) Fusion Proteins
We purchased the PUC57 plasmid containing the gene encoding recombinant human NGF (UniProtKB-P01138, Ser122-Ala241) and BDNF (UniProtKB-P23560, His129—Arg247) from GenScript. The PUC19 plasmid containing the elastin cassette V40C2 has been described previously [20]. We used PflMI and BglI enzymes to excise the gene fragment encoding recombinant NGF or BDNF from the PUC57 plasmid. The excised gene fragments were cloned in frame in the plasmid containing the elastin cassette to create a gene encoding either NGF-ELP or BDNF-ELP, as described previously [20, 24]. The gene encoding the fusion proteins was then excised from the PUC19 plasmid and inserted into the expression plasmid pET25b+ for protein expression.
2.2 Expression and Purification of Neurotrophin-ELPs
The expression vector pET25b+ containing NGF-ELP or BDNF-ELP was transformed into Escherichia coli BLR (DE3) cells through heat shock at 42 °C. A starter culture of 75 ml was then inoculated overnight and added to a 1-L culture the next day. The 1-L culture was then propagated overnight. The next day, bacterial cells were harvested via centrifugation (3000g, 20 min) at 4 °C. After two washes with washing buffer [50 mM Tris Base, 10 % glycerol, 1 % Triton X-100, 50 mM DTT, and 1 mM Ethylenediaminetetraacetic acid (EDTA)], the bacterial cells were lysed by sonic disruption on ice (six cycles, 50 % amplitude, and 30 s on/off). The solution was centrifuged (20,000g, 15 min), and the pellet containing the inclusion-bodied protein was collected and the supernatant discarded. The pellet was re-suspended in lysis buffer (50 mM Tris Base, 10 % glycerol, 1 % Triton X-100, 50 mM DTT, 1 mM EDTA, 100 μg/ml lysozyme, and 100 mM NaCl) followed by sonication on ice (three cycles, 50 % amplitude, and 10 s on/off). The sonicated mixture was centrifuged again and the pellet collected. This pellet was re-suspended in solubilization buffer [8 M urea + 10 mM DTT, 1X phosphate buffered saline (PBS), pH 3.0] followed by sonication on ice to assist in the solubilization of the inclusion bodies. After another round of centrifugation, the supernatant containing the ELP fusion proteins was transferred to a clean centrifuge tube. The pellet was re-suspended once more in the solubilization buffer, and another round of centrifugation was performed. The supernatant containing the fusion protein was dialyzed overnight against 2 M urea. The next day, 1 M NaCl was added to the dialyzed supernatant and heated to 40 °C to enable the transition of the fusion protein. A hot spin at 40 °C was performed to pellet the fusion protein. The supernatant was then discarded, and the pellet was re-solubilized in a transition buffer (2 M urea + 10 mM DTT, 1X PBS, pH 9.5) on ice followed by another cold spin at 4 °C. The pellet was discarded, and the supernatant was collected to complete one purification cycle. This cycle was repeated twice for a total of three cycles. For the final re-suspension step, the fusion protein was re-suspended in 2 M urea and then dialyzed overnight against deionized water at 4 °C. The purified NGF-ELP and BDNF-ELP proteins were then lyophilized the next day for storage.
2.3 Characterization of the Fusion Proteins
The purity and yields of recombinant proteins were analyzed by electrophoresis on a 15 % sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) under reducing conditions. The protein stain was performed according to the gelcode blue safe protein stain protocol (Thermo Scientific), and Western blotting was performed with NGF antibody (cell signaling, 1:1000) or BDNF antibody (R&D Systems, 1:100).
Lyophilized protein was re-suspended in PBS at a concentration of 1 mg/ml, and particle sizes at different temperatures were measured by dynamic light scattering using a zeta-sizer (Malvern instruments).
2.4 Neurite Outgrowth Assay
PC12 cells were seeded in poly-l-lysine (PLL)-treated 24-well plates at a density of 400,000 cells/ml and maintained under Roswell Park Memorial Institute (RPMI) 1640 (5 % fetal bovine serum, 10 % heat-inactivated horse serum, 1 % AA) at 37 °C for 7 days. Prior to seeding, the wells were coated with PLL for 2 h and then washed with PBS. Every 2 days, the cells were treated with 1 mg/ml NGF-ELP or 50 ng/ml recombinant NGF. PC12 cells containing neurite extensions were counted and averaged over the total number of PC12 cells in a frame.
2.5 TrkB Phosphorylation Assay
Human epithelial kidney (HEK) 293-T cells were seeded in 24-well plates at the density of 200,000 cells/well and maintained under Dulbecco’s modified eagle medium (DMEM). Transfection of the cells was conducted with a DNA solution containing 2 M calcium chloride, nuclease water, 2X Hepes buffered saline (HBS), 25 uM chloroquine, and 0.25 μg pEGFP TrkB plasmid (Addgene) or 0.25 μg of pCDNA TrkB plasmid (Addgene). The plasmid solution was added to the cells and incubated for 2 h. The solution was removed, the cells were washed once with PBS, and fresh DMEM was added. After 2 days, the cells were treated with either 1 mg/ml BDNF-ELP, ELP, no treatment (control), or 50 ng/ml recombinant BDNF for 15 min. After treatment, the cells were lysed in lysis buffer (3X sample buffer from cell signaling technology, nuclease free water, 30X DTT, protease/phosphatase inhibitors). The lysates were subjected to western blots using either Phospho TrkB antibody (Cell Signaling Technology, 1:1000) or TrkB antibody (1:1000, Cell Signaling Technology).
2.6 Molecular Weight of Neurotrophin-ELP
The molecular weight of recombinant NGF and BDNF was 13.5 Kda while that of ELP (V40C2) was 20.5 Kda. Thus the molecular weights of the fusion proteins NGF-ELP and BDNF-ELP were 34 Kda.
2.7 RNA Isolation and Real-Time Polymerase Chain Reaction (RT-PCR) Analysis
PC12 cells (400,000/well) were seeded in PLL-treated 6-well plates and treated every 2 days for 7 days with 1 mg/ml NGF-ELP or 50 ng/ml recombinant NGF. RNA was isolated from PC12 cells using the SV Total RNA Isolation System (Promega cat #Z3100). Complementary DNA (cDNA) synthesis was conducted using a iScript cDNA Synthesis Kit from Bio-Rad (cat # 1708890) following the manufacturer’s protocol. Real-time polymerase chain reaction (RT-PCR) was performed using Bio-Rad C1000 thermal cycler. The following primers were used for PCR β3-tubulin: forward 5′-TCTACGACATCTGCTTCCGC-3′, reverse 5′-GTCGAACATCTGCTGGGTGA-3′ (40 PCR cycles); GAP43: forward 5′-CAGGAAAGATCCCAAGTCCA-3′, reverse 5′-GAACGGAACATTGCACACAC-3′ (40 PCR cycles); GAPDH: forward 5′-CCTGCACCACCAACTGCTTA-3′, reverse 5′-GCCTGCTTCACCACCTTCTT-3′.
2.8 Statistical Analysis
In the case of neurite outgrowth analysis, the differences in various conditions were assessed by means of analysis of variance (ANOVA) single factor. We used the one-tailed test for comparisons between two groups, and a value of p < 0.05 was considered to be statistically significant in all cases.
3 Results
3.1 Neurotrophin-ELP Fusion Proteins are Expressed in Bacteria as Inclusion Bodies
The genes encoding recombinant NGF and BDNF were cloned at the N-terminus of the ELP variant (VPGVG)40(VPGVGVPGVGVPGCGVPGVGVPGVG)2 to create two genes encoding proteins of the form NGF-ELP and BDNF-ELP (Fig. 1). The two genes encoding the fusion proteins were cloned into the modified pET25b+ expression plasmid for protein expression in bacterial cells (BLR strain). Western blots using antibody specific to the neurotrophins demonstrated the successful expression of the proteins in bacterial cells. Interestingly, these fusion proteins were expressed as inclusion bodies (Fig. 2a, b).
Recombinant neurotrophin-ELP fusion proteins. NGF-ELP contains the 120 amino acid sequence of the mature NGF fused in frame at the N-terminus of the ELP sequence V40C2, where V VPGVG and C (VPGVG)2VPGCG(VPGVG)2. BDNF-ELP contains the 120 amino acid sequence of the mature BDNF fused in frame at the N-terminus of the ELP sequence V40C2, where V VPGVG and C (VPGVG)2VPGCG(VPGVG)2. BDNF brain-derived neurotrophic factor, ELP elastin-like peptide/polypeptide, NGF nerve growth factor
Expression and purification of the neurotrophin-ELP fusion proteins. a Successful expression of NGF-ELP in bacteria, accumulated in inclusion bodies. The expression of NGF-ELP was confirmed by western blot using an antibody reactive to NGF, where IB inclusion body, 1 8 M urea, 2 after dialysis, 3 1st cycle cold supernatant, 4 lyophilized NGF-ELP, M ladder. b Successful expression of BDNF-ELP in bacteria, accumulated in inclusion bodies. The expression of BDNF-ELP was confirmed by western blot using an antibody reactive to BDNF. IBB inclusion body BDNF-ELP, 5 8 M urea, 6 after dialysis overnight, 7 2nd cold supernatant, 8 lyophilized BDNF-ELP, M ladder. c Successful purification of NGF-ELP from inclusion bodies as shown by a total protein stain. The final lyophilized product just represents one single band that was reactive to NGF antibody as shown in a. d Successful purification of BDNF-ELP from inclusion bodies as shown by a total protein stain. The final lyophilized product just represents one single band that was reactive to BDNF antibody as shown in b. BDNF brain-derived neurotrophic factor, ELP elastin-like peptide/polypeptide, NGF nerve growth factor
3.2 Purification of Neurotrophin-ELP Fusion Proteins Using Inverse Temperature Cycling
ELP fusion proteins have typically been shown to be purified by exploiting their phase transition properties using a series of hot and cold spins [18]. However, for this to be successful, the fusion protein needs to be soluble in aqueous solution. To solubilize the inclusion bodies, we used 8 M urea as a denaturant, which solubilized them (Fig. 2a, b). However, since urea is a denaturant, the fusion proteins will not transition in the presence of 8 M urea, so it was removed using dialysis overnight. The fusion proteins remained soluble after the removal of urea and transitioned when the temperature was increased. Thus, a hot spin was used to spin down the fusion protein. However, for re-suspension of the pellet, a lower concentration of 2 M urea was used to solubilize the fusion proteins successfully (Fig. 2a, b). This completed one full cycle of ITC and was repeated three more times to constitute a total of four cycles of ITC that yielded a highly purified protein (Fig. 2c, d). Western blots using antibodies specific to NGF and BDNF, respectively, demonstrated that the purified protein was indeed the neurotrophin-ELP (Fig. 2a, b). Thus, employing urea to slightly modify ITC resulted in the successful purification of the fusion proteins from inclusion bodies.
3.3 Neurotrophin-ELP Fusion Proteins Self-Assemble into Nanoparticles at the Transition Temperature
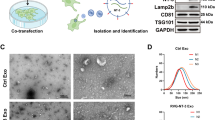
That we were able to successfully purify both NGF-ELP and BDNF-ELP indicates that the physical phase transitioning property of ELPs was still retained in the fusion. The lyophilized proteins formed loose aggregates in the aqueous solutions at lower temperatures (Fig. 3a, b, red line, 4 °C, 1 mg/ml). Interestingly, when the temperature was increased beyond the transition temperature, both fusion proteins self-assembled into nanoparticles. These nanoparticles were fairly mono-dispersed, with NGF-ELP displaying a peak at 199 nm and BDNF-ELP displaying a peak at 124 nm (Fig. 3a, b, green line).
Neurotrophin-ELP fusion proteins self-assemble into monodispersed nanoparticles at physiological temperature. a NGF-ELP and b BDNF-ELP formed loose aggregates at 4 °C (red). When the temperature was raised, at 37 °C (green) a NGF-ELP and b BDNF-ELP self-assembled into nanoparticles with a diameter of 199 and 124 nm, respectively. The lyophilized proteins were dissolved in phosphate buffered saline and particle sizes were measured by dynamic light scattering. BDNF brain-derived neurotrophic factor, ELP elastin-like peptide/polypeptide, NGF nerve growth factor
3.4 Neurotrophin-ELP Fusion Proteins Retain the Biological Activity of the Fused Neurotrophin
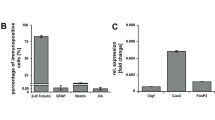
Finally, we evaluated the biological activity of the fused neurotrophin using in vitro cell culture models. NGF has been shown to promote differentiation and neurite outgrowth of PC12 cells, a clonal cell line derived from a rat pheochromocytoma. When NGF is introduced to PC12 cells, the cells cease dividing, and neurite extension follows within a week [25]. Cells treated with NGF-ELP and recombinant NGF remained attached and displayed neurite outgrowth (Fig. 4a, d), while no attachment or neurite outgrowth was observed in cells treated with ELP alone or that underwent no treatment (Fig. 4b, c). We further quantified the number of differentiated cells and found that the NGF-ELP induced neurite outgrowth in PC12 cells, though the number of differentiated cells was less than induced by recombinant NGF (Fig. 5). Negative control (ELP) exhibited no differentiation; *p < 0.05 when compared with the indicated samples.
NGF-ELP induces neurite extension in PC12 cells, thereby retaining the biological activity in the fusion. Micrographs of PC12 cells cultured in the presence of a 1 mg/ml NGF- ELP, b 1 mg/ml ELP, c no treatment (control) and d 50 ng/ml of recombinant NGF for 7 days were taken with EVOS™ fl digital inverted fluorescence microscope. PC12 cells were seeded and then treated every 2 days. Red arrows show neurite differentiation and neurite extension. ELP elastin-like peptide/polypeptide, NGF nerve growth factor
Quantification of differentiated cells induced by NGF-ELP and recombinant NGF. A ratio was taken of the amount of cells represented in an image that differentiated (cells with at least one neurite with a length equal to the cell body diameter) vs. the total cells present. Cells were counted on Day 0, Day 4, Day 7. On Day 0, there is no differentiation between the three treatments. Cells begin to differentiate on Day 4. On Day 7, the amount of differentiated cells increased. Negative control (ELP) exhibits no differentiation. *p < 0.05 when compared with the indicated samples. ELP elastin-like peptide/polypeptide, NGF nerve growth factor
We used HEK 293 cells transfected with the TrkB-GFP fusion plasmid to evaluate the biological activity of BDNF. BDNF binds to the human TrkB with high affinity, resulting in its phosphorylation [26]. Indeed, similar to recombinant BDNF, the BDNF-ELP fusion induced phosphorylation of the TrkB receptor (Fig. 6) in the transfected cells, while very little or no phosphorylation was seen in the control or ELP samples. These data clearly indicate that the biological activity of BDNF was retained in the fusion protein.
Biological activity of BDNF in the BDNF-ELP fusion is retained. 293-T cells were transfected with a plasmid containing the TrkB. Cells were then treated with the indicated treatments for 15 min followed by preparation of cell lysates. The cell lysates were subjected to western blots using either an antibody specific to Trk-B (left) or phospho TrkB (right) antibody. BDNF brain-derived neurotrophic factor, ELP elastin-like peptide/polypeptide, NGF nerve growth factor, Trk tropomycin receptor kinase
3.5 Nerve Growth Factor-ELP Expresses Elevated Levels of Genes Related to Neuronal Differentiation
We examined the effect of NGF-ELP at the molecular level and studied the levels of expression of genes related to neuronal differentiation, GAP43 and β3-tubulin. We extracted RNA from cells treated with NGF-ELP and compared them with recombinant NGF and with cells that received no treatment. PCR experiments revealed an elevated level of expression of GAP43 and β3-tubulin genes in cell populations treated with the NGF-ELP, in comparison with no treatment and comparable to recombinant NGF (Fig. 7). As a loading control, we examined the level of expression of GAPDH. Figure 7 shows minimal difference in levels of expression of GAPDH in the samples.
Effect of NGF-ELP on neuronal differentiation genes. PCR for mRNA levels of β3-tubulin [1 no treatment (control) tubulin, 2 no treatment (control) tubulin, 3 recombinant NGF tubulin, 4 recombinant NGF tubulin, 5 NGF-ELP tubulin, 6 NGF-ELP tubulin, 7 recombinant NGF GAP43, 8 NGF-ELP GAP43] and GAP43 [1 no treatment (control) GAPDH, 2 no treatment (control) GAPDH, 3 recombinant NGF GAPDH, 4 recombinant NGF GAPDH, 5 NGF-ELP GAPDH, 6 NGF-ELP GAPDH, 7 recombinant NGF GAPDH, 8 NGF-ELP GAPDH) of differentiated PC12 cells treated with no treatment, recombinant NGF, and NGF-ELP. The panels to the right present a control PCR of GAPDH of the same samples. Data were obtained 1 day after treatment and 7 days after treatment. ELP elastin-like peptide/polypeptide, mRNA messenger RNA, NGF nerve growth factor, PCR polymerase chain reaction
4 Discussion
Neurotrophins are promising agents for the treatment of neural injuries and neurological disorders. Here, we report the creation of two neurotrophin fusion proteins, namely NGF-ELP and BDNF-ELP, that retained the physical phase transition property of ELPs as well as the biological activity of the fused neurotrophins. These proteins were expressed and rapidly purified by exploiting the phase transition property of ELPs. Moreover, these proteins self-assembled into nanoparticles at their respective transition temperatures. These nanoparticles can serve as drug depots and may increase bioavailability by limiting neurotrophin loss due to diffusion, thereby allowing controlled spatio-temporal delivery of the neurotrophin.
Several delivery systems that enhance neurotrophin bioavailability have been described [27]. Typically, the neurotrophins to be delivered are either physically or chemically conjugated to either hydrogels [13], nanoparticles [28], or scaffolds [29]. These include the use of neurotrophin-binding heparin containing fibrin hydrogel [30], engineering of neurotrophin fusion proteins for covalent attachment to fibrin gels [31], or development of a neurotrophin fused with a collagen-binding domain [32] or PEGylated lipid nanoparticles loaded with neurotrophins [33]. However, most of these require large amounts of the recombinant neurotrophin as well as an extra step to conjugate or sequester the neurotrophin within the scaffold or polymeric backbone. The use of neurotrophin fusion proteins eliminates these steps, as the fusion protein itself serves as the neurotrophin as well as the delivery vehicle, thus streamlining the production process. Moreover, since it is produced genetically, it provides better stoichiometric control over chemical conjugation where reproducibility can be an issue. Interestingly, several works have described the successful production and application of ELP-based fusion proteins as delivery systems. These include keratinocyte growth factor (KGF)-ELP fusion for treatment of chronic wounds [20] and vascular endothelial growth factor (VEGF)-ELP fusion for the treatment of vascular disorders [19]. Thus, similar to these studies, we believe the neurotrophin-ELP fusion proteins will enable treatment of neurological disorders and injuries. Further studies are underway in our laboratory to assess the efficacy and performance of these proteins in animal models of neurological injuries.
Recombinantly expressed BDNF and NGF typically form inclusion bodies when expressed in bacterial systems [34, 35]. Thus, it was no surprise that the fusion proteins also formed inclusion bodies when expressed in bacteria. The use of 8 M urea enabled the dissolution of the inclusion bodies for purification. However, the denaturing effect of urea also results in the loss of the ELP phase transition property. This is because urea acts as a bridge between the water molecules and ELP chains, thereby preventing the ELP chains from coming together at the transition temperature. The phase transition property of the ELPs is necessary for successful purification of the property using ITC [18]. Our studies indicate that it is possible to regain the phase transition property of ELPs at lower urea concentrations and higher salt concentrations. This indicates that the two opposing forces of urea and salt can be balanced out, enabling the purification of the fusion proteins from inclusion bodies using ITC. While ITC has been shown to purify ELP fusion proteins, to our knowledge this is the first study reporting the production of the ELP fusion proteins from inclusion bodies.
In vitro cell cultures confirmed the biological activity of NGF-ELP and BDNF-ELP. Using PC12 cells, we show that the NGF-ELP enhanced cell survival as well as axonal sprouting similar to recombinant NGF. However, our data suggest that recombinant NGF was more potent than the fusion protein. This could be attributed to the fusion of ELPs with the NGF. Nonetheless, since the biological activity was retained in the fusion, the NGF-ELP folded correctly without any additives or additional folding steps. Similarly, BDNF-ELP induced phosphorylation of the Trk-B receptor in 293-T cells expressing the TrkB receptor, suggesting the successful yield of biological functional BDNF-ELP. Thus, these data show the feasibility of producing biologically active recombinant neurotrophin fusion proteins from bacteria. This is a major advantage, since recombinant neurotrophins are either produced in mammalian [36] or insect systems [37] to ensure proper folding or in bacteria where several folding steps or pro-sequences enabling proper folding are required to attain biological functionality of neurotrophin [35, 38]. Thus, the fusion proteins eliminate not only the requirement for expensive chromatography columns for purification but also the use of significantly expensive mammalian expression systems.
Additionally, compared with recombinant NGF and recombinant BDNF, high concentrations of N-ELP were used in this study to offset a possible decrease in activity. Despite the possible decrease of activity when a neurotrophin is fused with an ELP, ELPs are capable of providing the neurotrophin a secure place to interact with the cell without being quickly diffused throughout the system. Another possibility of the loss of activity in the fusion protein may be due to a solubility issue in which the proper pH/buffer system is needed to increase protein stability. Studies are underway in our laboratory to investigate the protein stability of these fusion proteins and elucidate the appropriate pH/buffer system needed to re-suspend lyophilized protein to avoid the possible solubility issue. This future work, along with investigating the pathway along which these neurotrophin-ELP fusion proteins are internalized, will make them strong contenders in therapeutic translational studies.
ELPs and ELP fusion proteins have been discovered to enter cells via caveolae-independent endocytic mechanisms [39] and macropinocytosis [40]. It has been shown that internalization of ELP fusion proteins can depend upon cell-surface heparan sulfate proteoglycans (HSPGs) [40]. HSPGs are found on the surface of axons of dorsal root ganglion neurons [41], and early accumulation of HSPGs has been found in Alzheimer’s disease and other amyloid-related disorders [42]. HSPGs stimulate Schwann cell proliferation, which provides myelin for the transport of neurotrophins along the axon [41]. NGF/TrkA promotes retrograde transport up the axon to the cell body [43, 44], whereas BDNF/TrkB promotes anterograde transport down the axon to the synapse [45]. Neurotrophins can promote transport when internalized via pincher-mediated endocytosis [46], receptor-mediated endocytosis [47], or clathrin-mediated endocytosis [48]. The phosphorylation of the TrkB receptor when BDNF-ELP is introduced into the cellular environment suggests that BDNF-ELP binds to the TrkB receptor and may enter the cell via receptor-mediated endocytosis. Therapeutic transport of these ELP fusions and neurotrophins suggest that N-ELP fusion proteins may have various ways of entering the cell. Further work is needed to investigate the pathway of internalization of these neurotrophin-ELP fusion proteins.
Dynamic light scattering data showed that the fusion proteins formed big aggregates below their transition temperature. This could be attributed to the partial solubility of the fusion proteins. However, as the temperature was raised, the big aggregates self-assembled into nanoparticles. These nanoparticles were highly monodispersed and were biologically active, as demonstrated by our in vitro experiments. Thus, ELP may assist in the proper folding of the fusion protein into functional nanoparticles. Further studies are underway to investigate this intriguing hypothesis.
5 Conclusion
We created novel neurotrophin-ELP-based fusion proteins that maintain the biological activity of the neurotrophin and can self-assemble into nanoparticles at the transition temperature. These nanoparticles may increase bioavailability by limiting neurotrophin loss due to diffusion and allow controlled spatio-temporal delivery of the neurotrophin. Additionally, a mixture of two or more fusion proteins containing different neurotrophins can be used to create multi-functional nanoparticles. These nanoparticles will allow controlled spatio-temporal co-delivery of multiple neurotrophins, thereby allowing combination therapy. The ease of production and usage of the neurotrophin fusion proteins will have a broader impact in the field of neuronal regeneration and treatment of neurodegenerative diseases.
References
Trumble TE, Shon FG. The physiology of nerve transplantation. Hand Clin. 2000;16(1):105–22.
Fawcett JW, Asher RA. The glial scar and central nervous system repair. Brain Res Bull. 1999;49(6):377–91.
Blesch A, Tuszynski MH. Spinal cord injury: plasticity, regeneration and the challenge of translational drug development. Trends Neurosci. 2009;32(1):41–7.
Willerth SM, Sakiyama-Elbert SE. Approaches to neural tissue engineering using scaffolds for drug delivery. Adv Drug Deliv Rev. 2007;59(4–5):325–38.
Huang EJ, Reichardt LF. Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci. 2001;24:677–736.
Grill R, et al. Cellular delivery of neurotrophin-3 promotes corticospinal axonal growth and partial functional recovery after spinal cord injury. J Neurosci. 1997;17(14):5560–72.
Bramham CR, Messaoudi E. BDNF function in adult synaptic plasticity: the synaptic consolidation hypothesis. Prog Neurobiol. 2005;76(2):99–125.
Mortazavi MM, et al. Chemical priming for spinal cord injury: a review of the literature part II-potential therapeutics. Childs Nerv Syst. 2011;27(8):1307–16.
Wang YC, et al. Sustained intraspinal delivery of neurotrophic factor encapsulated in biodegradable nanoparticles following contusive spinal cord injury. Biomaterials. 2008;29(34):4546–53.
Katz JS, Burdick JA. Hydrogel mediated delivery of trophic factors for neural repair. Wiley Interdiscip Rev Nanomed Nanobiotechnol. 2009;1(1):128–39.
Willerth SM, et al. Rationally designed peptides for controlled release of nerve growth factor from fibrin matrices. J Biomed Mater Res A. 2007;80(1):13–23.
Sly DJ, et al. Brain-derived neurotrophic factor modulates auditory function in the hearing cochlea. J Assoc Res Otolaryngol. 2012;13(1):1–16.
Lindsey S, et al. Beta hairpin peptide hydrogels as an injectable solid vehicle for neurotrophic growth factor delivery. Biomacromolecules. 2015:16(9):2672–83.
Wolfe D, Mata M, Fink DJ. Targeted drug delivery to the peripheral nervous system using gene therapy. Neurosci Lett. 2012;527(2):85–9.
Hirsch T, et al. Gene therapy in cutaneous wound healing. Front Biosci. 2007;12:2507–18.
Byrnes CK, et al. Success and limitations of a naked plasmid transfection protocol for keratinocyte growth factor-1 to enhance cutaneous wound healing. Wound Repair Regen. 2001;9(5):341–6.
Yao F, Eriksson E. Gene therapy in wound repair and regeneration. Wound Repair Regen. 2000;8(6):443–51.
Meyer DE, Chilkoti A. Purification of recombinant proteins by fusion with thermally-responsive polypeptides. Nat Biotechnol. 1999;17(11):1112–5.
George EM, et al. Growth factor purification and delivery systems (PADS) for therapeutic angiogenesis. Vasc Cell. 2015;7(1):1.
Koria P, et al. Self-assembling elastin-like peptides growth factor chimeric nanoparticles for the treatment of chronic wounds. Proc Natl Acad Sci USA. 2011;108(3):1034–9.
Asai D, et al. Protein polymer hydrogels by in situ, rapid and reversible self-gelation. Biomaterials. 2012;33(21):5451–8.
Mie M, Mizushima Y, Kobatake E. Novel extracellular matrix for cell sheet recovery using genetically engineered elastin-like protein. J Biomed Mater Res Part B: Appl Biomater. 2008;86B(1):283–90.
Le DHT, Okubo T, Sugawara-Narutaki A. Beaded nanofibers assembled from double-hydrophobic elastin-like block polypeptides: effects of trifluoroethanol. Biopolymers. 2015;103(3):175–85.
Meyer DE, Chilkoti A. Genetically encoded synthesis of protein-based polymers with precisely specified molecular weight and sequence by recursive directional ligation: examples from the elastin-like polypeptide system. Biomacromolecules. 2002;3(2):357–67.
Greene LA, Tischler AS. Establishment of a noradrenergic clonal line of rat adrenal pheochromocytoma cells which respond to nerve growth factor. Proc Natl Acad Sci USA. 1976;73(7):2424–8.
Soppet D, et al. The neurotrophic factors brain-derived neurotrophic factor and neurotrophin-3 are ligands for the trkB tyrosine kinase receptor. Cell. 1991;65(5):895–903.
Mohtaram NK, Montgomery A, Willerth SM. Biomaterial-based drug delivery systems for the controlled release of neurotrophic factors. Biomed Mater. 2013;8(2):022001.
Angelova A, et al. Neurotrophin delivery using nanotechnology. Drug Discov Today. 2013;18(23–24):1263–71.
Wang TY, et al. Biofunctionalisation of polymeric scaffolds for neural tissue engineering. J Biomater Appl. 2012;27(4):369–90.
Sakiyama-Elbert SE, Hubbell JA. Controlled release of nerve growth factor from a heparin-containing fibrin-based cell ingrowth matrix. J Control Release. 2000;69(1):149–58.
Sakiyama-Elbert SE, Panitch A, Hubbell JA. Development of growth factor fusion proteins for cell-triggered drug delivery. FASEB J. 2001;15(7):1300–2.
Sun W, et al. The effect of collagen-binding NGF-beta on the promotion of sciatic nerve regeneration in a rat sciatic nerve crush injury model. Biomaterials. 2009;30(27):4649–56.
Angelova A, et al. Protein entrapment in PEGylated lipid nanoparticles. Int J Pharm. 2013;454(2):625–32.
Dicou E. Expression of recombinant human nerve growth factor in Escherichia coli. Neurochem Int. 1992;20(1):129–34.
Negro A, et al. Synthesis and purification of biologically active rat brain-derived neurotrophic factor from Escherichia coli. Biochem Biophys Res Commun. 1992;186(3):1553–9.
Park E, et al. Production and characterization of fusion proteins containing transferrin and nerve growth factor. J Drug Target. 1998;6(1):53–64.
Meyer SL, et al. Production and characterization of recombinant mouse brain-derived neurotrophic factor and rat neurotrophin-3 expressed in insect cells. J Neurochem. 1994;62(3):825–33.
Rattenholl A, et al. The pro-sequence facilitates folding of human nerve growth factor from Escherichia coli inclusion bodies. Eur J Biochem. 2001;268(11):3296–303.
Bidwell GL, Raucher D. Cell penetrating elastin-like polypeptides for therapeutic peptide delivery. Adv Drug Deliv Rev. 2010;62(15):1486–96.
Iglesias R, Koria P. Leveraging growth factor induced macropinocytosis for targeted treatment of lung cancer. Med Oncol. 2015;32(12):259.
Ratner N, Bunge RP, Glaser L. A neuronal cell surface heparan sulfate proteoglycan is required for dorsal root ganglion neuron stimulation of Schwann cell proliferation. J Cell Biol. 1985;101(3):744–54.
Snow AD, et al. Early accumulation of heparan sulfate in neurons and in the beta-amyloid protein-containing lesions of Alzheimer’s disease and Down’s syndrome. Am J Pathol. 1990;137(5):1253–70.
Sandow SL, et al. Signalling organelle for retrograde axonal transport of internalized neurotrophins from the nerve terminal. Immunol Cell Biol. 2000;78(4):430–5.
Delcroix J-D, et al. NGF signaling in sensory neurons. Neuron. 2003;39(1):69–84.
Cheng PL, et al. Self-amplifying autocrine actions of BDNF in axon development. Proc Natl Acad Sci. 2011;108(45):18430–5.
Shao Y. Pincher, a pinocytic chaperone for nerve growth factor/TrkA signaling endosomes. J Cell Biol. 2002;157(4):679–91.
Valdez G. Pincher-mediated macroendocytosis underlies retrograde signaling by neurotrophin receptors. J Neurosci. 2005;25(21):5236–47.
Howe CL, et al. NGF signaling from clathrin-coated vesicles. Neuron. 2001;32(5):801–14.
Acknowledgments
The authors acknowledge Yuan Yuan, Raul Iglesias, and Bernard Batson.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Tamina Johnson and Piyush Koria have no conflicts of interest that are directly relevant to the content of this study.
Funding
This work was funded by startup funds from the University of South Florida (PK) and the new researcher grant (PK) from University of South Florida, and in part by Institutional Research Grant number 93-032-16 from the American Cancer Society (PK). Tamina Johnson was supported by NSF Florida Georgia Louis Stokes Alliance for Minority Participation Bridge to the Doctorate Award HRD #1139850, the USF Graduate Student Success Diversity Fellowship, and The Alfred P. Sloan Minority Ph.D. Program.
Rights and permissions
About this article
Cite this article
Johnson, T., Koria, P. Expression and Purification of Neurotrophin-Elastin-Like Peptide Fusion Proteins for Neural Regeneration. BioDrugs 30, 117–127 (2016). https://doi.org/10.1007/s40259-016-0159-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40259-016-0159-4