Abstract
Background
The balance between pro-atherogenic and anti-atherogenic factors is very crucial in the development of atherosclerotic lesions. Although the expression of the six-transmembrane epithelial antigen of the prostate 4 (STEAP4) in myeloid cells is known to be atheroprotective, there is not a single study reporting on the status of STEAP4 expression in circulating monocytes in the early stages of diet-induced obesity or in events of glycemic excursions.
Methods
We induced glycemic spikes twice daily for a 1-week duration to rats fed on regular chow and western diet, and analyzed gene expression changes in the peripheral blood mononuclear cells (PBMCs). We also conducted experiments on RAW 264.7 cells to gain insight into some of our in vivo findings.
Results
Diet-induced obesity and glycemic excursions independently caused a significant increase in STEAP4 mRNA expression in PBMCs. This was also accompanied by an induction of a substantial number of pro-inflammatory cytokines, chemokines, and chemokine receptors. However, the combined effect of western diet and hyperglycemic spikes was subtle and non-additive. In the in vitro setting, either glucose spikes, persistent hyperglycemia, or a combination of palmitic acid and insulin resulted in a parallel increase in expression of STEAP4 and pro-inflammatory genes. This was, however, significantly abrogated with 4-octyl itaconate or attenuated by inhibitors of p38MAPK and NF-kB.
Conclusions
STEAP4 expression in mononuclear cells is induced by increasing inflammation or oxidative stress. The observed increase in STEAP4 expression in circulating monocytes due to visceral obesity or glycemic excursions is a compensatory response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Atherosclerotic cardiovascular disease is increasingly becoming one of the top leading causes of adult mortality all over the world [1]. The disease is reported to occur when there is an imbalance between the pro-atherogenic and anti-atherogenic factors [2, 3]. Epidemiological studies have established that visceral obesity is an independent risk factor for cardiovascular diseases, mainly because it is associated with pro-atherogenic factors, such as dyslipidemia, insulin resistance, hypertension, and type 2 diabetes [4, 5]. Apart from visceral obesity, the role of postprandial hyperglycemic spikes occurring in individuals with subclinical and full-blown type 2 diabetes in the pathogenesis of atherosclerosis is well established [6,7,8,9,10]. Formerly, atherosclerosis was considered to be a consequence of a passive buildup of atherogenic lipids in the vessel wall [11]. However, it is currently known that immune cells, particularly the monocytes, are crucial in developing atherosclerotic lesions [11]. The fact that inflammation is very fundamental in the formation, progression, and even rupture of atherosclerotic plaques underscores the crucial role of monocytes or plaque macrophages as the chief inflammatory cells in the process [12,13,14,15].
Both visceral obesity and glycemic excursions are known for their potential to activate circulating monocytes and stir up inflammation in the vessel wall [10, 16, 17]. In response to this, various cellular protective mechanisms are activated; the transcription factor Nrf2 (nuclear factor erythroid 2–related factor 2) is just one of them [18]. However, the philosophical underpinning that atherosclerosis occurs when there is an imbalance between the pro-atherogenic and anti-atherogenic factors underscores the importance of identifying the status of other novel anti-inflammatory mexpressed as a fold change normalizedediators as well.
Mounting evidence shows that the six transmembrane epithelial antigen of the prostate (STEAP4), also known as Tumor Necrosis Factor-α-induced Adipose-related Protein (TIARP), or the six transmembrane protein of prostate (STAMP2) is another one [19]. STEAP4 was initially discovered while searching for genes and proteins that could potentially mediate the effect of TNFα on adipocyte development and metabolism [20]. It has been shown that a whole-body STEAP4 knockout mouse tends to develop obesity, insulin resistance, glucose intolerance, hyperglycemia, and type 2 diabetes [21]. There are also a good number of studies showing that STEAP4 is protective against stress-induced by nutrient overload or inflammatory mediators. Specifically, the lack of STEAP4 expression in hepatocytes has been shown to correlate with the onset of fatty liver disease [21]. STEAP4 overexpression has been shown to ameliorate high-fat diet-induced hepatic steatosis and insulin resistance [22]. Likewise, there is evidence showing that STEAP4 overexpression in diabetic Apo E-/-LDLR-/- mice helps to protect against adipose tissue dysfunction by indirectly affecting adipose tissue-macrophage polarization shift, and consequently leading to reduced insulin resistance [23]. Studies conducted to discern the expression and role of STEAP4 in monocytes/macrophages are even scantier. In the year 2010, Wang et al. reported for the first time that STEAP4 expression is detectable in circulating mononuclear cells and that its expression was found low in female patients with metabolic syndrome. They further showed that STEAP4 expression in circulating monocytes was negatively correlated with carotid intima–media thickness [24]. According to a study by Hotamisligil et al., the lack of STEAP4 expression in macrophages causes an aberrant response to inflammatory mediators. In their study, they concretely demonstrated that STEAP4 expression in bone marrow-derived cells protects against atherosclerosis [25].
Despite the mentioned protective roles, the relative expression of STEAP4 by monocytes in the early stages of diet-induced obesity or intermittent hyperglycemic state is not known. Therefore, in this study, we aimed to ascertain whether there are any glucose spikes or dietary obesity-induced changes in STEAP4 expression in mononuclear cells, the correlation of such changes with obesity-related factors, and mechanisms responsible for such expressional alterations.
Research design and methods
Note that; details of some of the methods employed in this study can be traced in the supplementary information section.
-
A.
In vivo studies
Experimental animals used
We purchased 48, 7 weeks old male Wistar rats from Charles River Laboratories (Japan). These animals were individually housed in standard cages at an ambient temperature of 23 ± 1°C, relative humidity of 50 ± 10%, and a 12-h cycle of alternating light and dark. All the procedures involved in the animal care, interventions, and even euthanasia were carried out at the Kagoshima University, Institute of Laboratory Animal Science according to IACUCs guidelines; protocol approval number MD20022. During the first week at our facility, animals were acclimated to the new environment and were fed ad libitum.
Animal grouping and interventions
All the animal grouping and assigned interventions are summarized in Fig. 1. At the age of 8 weeks, animals were randomly divided into two groups; the standard chow (MF) and western-type diet (WTD) groups, respectively. Whereas the MF group of rats was fed on the 3.6 kcal/g standard chow (Oriental Yeast Co., Ltd.) for a duration of 8 weeks, the WTD group was fed on 4.5 kcal/g western-type diet (Oriental Yeast Co., Ltd., Japan) for a similar duration.
At the age of 16 weeks, each of the two groups was further subdivided into two subgroups such that four groups designated as MFGS (−), MFGS (+), WTDGS (−), and WTDGS (+) were formed. To make glucose spike models, the MFGS (+) and WTDGS (+) groups were subjected to intraperitoneal injection of 1 g/kg sterile glucose solution at 10:00 A.M and 4:00 PM, twice daily for a duration of 1 week. The control MFGS (-) and WTDGS (-) groups were injected with an equivalent volume of intraperitoneal sterile saline following the same protocol. With a blood glucose sensor attached to the back of the animal before the commencement of intraperitoneal injections, we were able to perform a 24-h continuous blood glucose monitoring using a flash glucose monitoring system, Freestyle Libre Pro (Abbott, USA) (Fig. 2). At 17 weeks of age, all animal groups were fasted overnight and euthanized according to the approved protocol. Adequate blood samples for PBMCs isolation and biochemical tests were collected by cardiac puncture.
Isolation of peripheral blood mononuclear cells (PBMCs)
OptiPrep™ Density Gradient Medium was obtained from Sigma Aldrich and handled according to the manufacturer’s instructions. PBMCs were isolated by floatation (iodixanol mixer technique) following almost similar steps stipulated in the Opti Prep ™ Application Sheet C06: 8th edition, January 2018 (Available in the electronic supplementary material).
Biochemical tests
We carried out relevant biochemical tests in the serum samples of our animal groups. The list includes fasting blood glucose, total cholesterol, triglycerides, free-fatty acids, TNF-α, and High Molecular Weight (HMW) adiponectin (details of each test is available in the electronic supplementary information).
-
B.
In vitro studies
A frozen tube of murine monocyte/macrophage cell line (RAW 264.7 (ATCC® TIB-71™) was purchased from American Type Culture Collection (ATCC); Low & High-lucose Dulbecco’s Modified Eagle’s Medium (DMEM), palmitic acid, and low-endotoxin fatty acid-free bovine serum albumin (BSA, FFA-free) from Sigma; antibiotic (penicillin/streptomycin) solution, and qualified Fetal Bovine Serum (FBS) from Gibco; 2-Mercaptoethanol, HEPES, L-Glutamine, Lipopolysaccharide, Superscript™ IV VILO™ master mix, and TaqMan™ Fast Advanced Master mix from Thermo Fisher Scientific; Phorbol Myristate Acetate (PMA), and SB203580 from Invivo Gen ( San Diego, USA); Recombinant mouse TNF & IL6 proteins from R&D systems (Minneapolis, USA); 4-octyl itaconate from Stem Cell Technologies company, PDTC (Ammonium pyrrolidinedithiocarbamate), and NF-kappaB inhibitor antioxidant (ab141406) from abcam.
Preparation of a stock solution of palmitic acid
Using a protocol by Seahorse Bioscience, we prepared 1 mM palmitic acid/0.17 mM BSA stock solution (6:1 molar ratio palmitic acid: BSA). A stock solution of palmitic acid-BSA conjugate and vehicle control (BSA, FFA-free) were aliquoted in small volumes of 4 ml and kept at − 20 °C. On the day of the experiment, the palmitic acid-BSA conjugate stock solution and vehicle control aliquots were thawed at 37 °C for 10 min before mixing with cell culture media to obtain the desired final concentration.
Cell culture
RAW 264.7 cells were primarily cultured in DMEM-high glucose supplemented with 10% of FBS and 1% of an antibiotic solution containing 10,000 units/mL of penicillin and 10,000 µg/mL of streptomycin. At all times cell cultures were maintained in a humidified 5% CO2 incubator set at a temperature of 37 °C. RAW 264.7 cells used in all experiments were between passage numbers 5 and 15. We maintained the required standard cell culture practices, such as regular examination of cell cultures, timely change of cell culture media, and stringent aseptic techniques in all experiments.
Exposure of RAW 264.7 cells to stable or fluctuating glucose concentration
We performed preliminary cultures of RAW 264.7 cells in DMEM-low glucose supplemented with 10% FBS. The concentration of FBS in the cell culture media was subsequently lowered to 0.1% and cells incubated under stable glycemic condition (DMEM-30 mM glucose) for a duration of 72 h or repeated cycles of glucose fluctuation (DMEM-5.5 mM glucose for 16 h followed by DMEM-30 mM glucose for 8 h) for the same duration of 72 h. In a similar set of experiments, cells incubated in high glucose conditions (including those subjected to fluctuating glucose concentration) were concurrently treated with or without 10 µM of SB203580 (p38 MAPK inhibitor), 40 µM of PDTC (NF-kB) inhibitor, or 0.1 mM of a cell permeable Nrf2 activator (4-octyl itaconate), respectively. In all these experiments, a 25 mM low-endotoxin mannitol-added to DMEM-low glucose was used as an osmotic control.
Exposure of RAW 264.7 cells to obesity related factors
We conducted three sets of experiments under this category (details of each can be traced in the electronic supplementary information). In summary, serum-starved RAW 264.7 cells cultured in DMEM-low glucose were incubated for 24 h with either vehicle control (BSA), 100 µM palmitic acid, 100 nM insulin, a combination of palmitic acid and insulin, palmitic acid and high glucose, or high glucose and insulin, followed by gene expression studies. We also conducted mechanistic studies in which cells incubated with palmitic acid and high insulin, were also incubated with or without 10 µM of SB203580 (p38 MAPK inhibitor),40 µM of PDTC (NF-kB) inhibitor, or 0.1 mM of 4-octyl itaconate, respectively.
Treatment of RAW 264.7 with inflammatory cytokines
Under conditions of extreme serum starvation (0.1% FBS), RAW 264.7 cells precultured in DMEM-high glucose were exposed to a combination of IL6 (20 ng/ml) and TNF (10 ng/ml) with or without 10 µM SB203580 (p38MAPK inhibitor), and 40 µM PDTC (NF-kB inhibitor), respectively, for a duration of 12 h. The control group of cells was treated with vehicle control for the same duration before being harvested for experiments.
RNA extraction and synthesis of cDNA for quantitative polymerase chain reaction (qPCR)
Total RNA was extracted from the mononuclear cells using a slightly modified version of the Yale University TRIZOL RNA Isolation Protocol (Available in the electronic supplementary material). All total RNA samples that were used for the microarray study underwent further clean-up using a Qiagen column purification kit (Qiagen). Total RNA was quantitated using NanoDrop™ 1000 spectrophotometer and RNA integrity measured using Agilent 2100 Bioanalyzer. All total RNA samples used in the microarray study conformed to the quality requirement of A260/280 ≥ 1.8 and RIN ≥ 2.0, respectively.
Microarray analysis
Microarray analysis was outsourced to Hokkaido System Science Co., Ltd (Japan). A total of sixteen total RNA samples comprised of 4 samples from each of the animal groups, i.e., MFGS (-), MFGS ( +), WTDGS (-), and WTDGS ( +), respectively, were pulled into equal weights in their respective groups and used in the analysis (Details of microarray protocol and data analysis are available in the electronic supplementary information).
Selection and validation of microarray candidate genes
We randomly picked up the traditional and novel inflammation-related genes whose expression changed by ≥ 2folds in response to glucose spikes or diet-induced obesity (Suppl Figs. 1 and 2). Out of these, four representative genes were chosen for quantitative validation. The list includes CCL2, IL1B, TNF, and STEAP4.
Real-time quantitative reverse transcription PCR (RT-qPCR)
Total RNA was reverse-transcribed to synthesize cDNA using Superscript™ IV VILO™ Master Mix. Relative quantification of target genes was carried out using TaqMan gene expression assays and TaqMan™ Fast Advanced Master Mix in a Step One Plus Real-Time PCR system (Applied Biosystems). All PCR reactions for the given samples were carried out in triplicates in a PCR compatible MicroAmp Fast 96-Well Reaction Plate (Applied Biosystem). The relative expression of all the target genes was normalized to housekeeping genes hypoxanthine phosphoribosyl transferase 1 (HPRT1) and Glyceraldehyde 3-phosphate dehydrogenase (GAPDH). Details of TaqMan primers and probes used in RT-qPCR can be traced from supplementary Table 1.
Statistical analysis
Data analysis was carried out using IBM SPSS Statistics 25 (SPSS, Inc., USA). For normally distributed data, the student’s t test or one-way analysis of variance (ANOVA) or two-way ANOVA was applied to determine the statistical significance between different experimental groups. On the other hand, the Mann–Whitney test was used to determine the statistical significance of non-normally distributed data obtained from two independent groups. Specifically, in ascertaining differential gene expression, statistical analysis was performed on 2−delta Ct. The value of p < 0.05 was considered statistically significant.
Results
There was a distinct difference between our two animal models. Whereas western diet resulted in visceral obesity and insulin resistance, glucose spikes produced no metabolic effects. There was also marked dyslipidemia, borderline-high fasting glucose, and an increase in circulating levels of TNF-α in the western-type diet group (Tables 1 and 2).
Our transcriptional profiling results show that western diet-induced obesity and glucose spikes independently caused more than a twofold increase in the expression of STEAP4 and eight pro-inflammatory genes in common. The list includes CCL2, IL1B, TNF, CXCL2, CCR2, CXCR2, S100A8, and IL1R2 (Suppl Fig. 3).
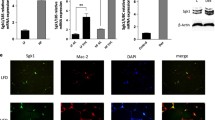
To validate these microarray findings, we chose four representative genes; STEAP4, CCL2, IL1B, and TNF. RT-qPCR confirmed that visceral obesity and glucose spikes independently induced STEAP4 and pro-inflammatory gene (CCL2, TNF, IL1B) expression in PBMCs. However, the combined effect of glucose spikes and western diet in altering the expression of the STEAP4 and aforementioned pro-inflammatory genes was subtle and non-additive (Fig. 3).
mRNA expression of A STEAP4 B CCL2 C TNF and D IL1B in PBMCs in response to glucose spikes or western-type diet (RT-qPCR) Data expressed as a fold change normalized to HPRT1 Values are means ± SEM (n = 8–10–10–10) *p < 0.05 **p < 0.01 versus the MFGS (−) group MF and WTD stand for the control diet and western diet groups, respectively, GS (−/+) denotes without or with glucose spikes
As mentioned above, visceral obesity-induced not only pro-inflammatory genes but also anti-inflammatory genes, such as STEAP4. We also observed a strong positive correlation between STEAP4 and pro-inflammatory gene expression (Fig. 4). Moreover, both pro-inflammatory genes and STEAP4 gene expression were positively correlated with body weight, adiposity index, non-esterified fatty acid (NEFA) concentration, and the homeostasis model assessment of insulin resistance (HOMA-IR) (Suppl Fig. 4a–d).
Similar to our in vivo observation, an intermittent hyperglycemic condition caused a parallel increase in the expression of STEAP4 and pro-inflammatory genes in RAW 264.7 cells. However, the effect of constant hyperglycemic condition was stronger than glucose spikes (Fig. 5).
mRNA expression of A STEAP4 B CCL2 C TNF and D ILIB after 72 h exposure of RAW 264.7 cells to either 30 mM mannitol hyperosmolar condition persistent high glucose (30 mM) or 8/16 h repetitive cycles of glucose fluctuations (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 6–6–6) *p < 0.05 **p < 0.01 ***p < 0.001 versus the mannitol-control group
Since our visceral obesity animal model displayed significant insulin resistance together with an increase in circulating levels of NEFA, we attempted to elucidate the role of these factors in altering the expression of genes of interest. In this case, the mouse monocytes/macrophage cell-line (RAW 264.7 cells) were treated with either palmitic acid, high insulin, or a combination of both. We then found that neither palmitic acid nor high insulin could significantly alter STEAP4 expression. However, the two synergistically increased the expression of STEAP4 in RAW 264.7 cells. To some extent, a similar trend was observed in the pro-inflammatory genes (Fig. 6a).
A The mRNA expression of (a1) STEAP4 (a2) CCL2 (a3) TNF and (a4) ILIB after 24 hours exposure of RAW 264.7 cells to either a vehicle control (BSA) 100μM palmitic acid 100nM Insulin or a combination of 100μM palmitic acid and 100nM Insulin (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 5–5–5–5) *p < 0.05 ***p < 0.001 versus the vehicle-control group. B The mRNA expression of (b1) STEAP4 (b2) CCL2 (b3) TNF and (b4) ILIB after 48 hours exposure of RAW 264.7 cells to either a vehicle control (BSA) 100μM palmitic acid high glucose (30mM) or a combination of 100μM palmitic acid and high glucose (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n=5-5-5-5) * **p<0.001 versus the vehicle-control group. C The mRNA expression of (c1) STEAP4 (c2) CCL2 (c3) TNF and (c4) ILIB after 48 hours exposure of RAW 264.7 cells to either 5.5mM glucose (control group) high glucose (30mM) high insulin (100nM) or a combination of high glucose and high insulin Data expressed as a fold change normalized to GAPDH Values are means ± SEM (n = 7–7–7–7) **p < 0.01 ***p< 0.001 versus the control group. D The effect of (d1) PDTC an inhibitor of NF-κB activation on inflammatory cytokines-induced STEAP4 mRNA expression (d2) SB203580 a p38 MAPK inhibitor on inflammatory cytokines-induced STEAP4 mRNA expression Data expressed as a fold change normalized to GAPDH Values are Means ±SEM (n = 5–5–5–5) ***p < 0.001 *p < 0.05
We further attempted to investigate the combined effect of either high glucose and palmitic acid or high glucose and insulin in which the former but not the latter resulted in a marked increase in STEAP4 and pro-inflammatory gene expression in RAW 264.7 (Fig. 6b, c). Moreover, our attempt to stimulate the RAW 264.7 cells with inflammatory cytokines resulted in an increase in STEAP4 expression at least partly through the p38 MAPK/NF-κB signaling pathways (Fig. 6d). This tends to suggest that inflammatory cytokines secreted in the culture media in response to various treatments, such as high glucose are responsible for the observed effect.
In our supplementary experiments, we also observed a respective dose-dependent LPS, AGE-BSA, and PMA-induced increase in the expression of STEAP4 and pro-inflammatory genes (Suppl Fig. 5a–c).
We eventually tried to clarify the mechanism responsible for STEAP4 induction in which it was observed that a cell-permeable Nrf2 activator, 4-octyl itaconate, respectively, suppressed glucose spikes, palmitic acid + high insulin, and LPS-induced expression of STEAP4 and pro-inflammatory genes in RAW 264.7 cells (Fig. 7a, b and Suppl Fig. 6). Moreover, because STEAP4 expression was coupled to the expression of inflammatory genes, we also attempted to determine if STEAP4 expression is associated with some changes in key inflammatory signaling pathways, in this case, inhibitors of p38 MAPK and NF-KB attenuated STEAP4 expression induced by either glucose spikes, or a consistent hyperglycemic condition, or a combination of palmitic acid and high insulin, respectively (Fig. 7c, d).
A The mRNA expression of (a1) STEAP4 (a2) CCL2 (a3) TNF and (a4) IL1B after 72 hours exposure of RAW 264.7 cells to either 8/16 hours repetitive cycles of mannitol osmolar fluctuations (control group) glucose fluctuations or 0.1mM of 4-octyl itaconate at every peak of glucose fluctuation (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 5–5–5) **p < 0.01 ***p < 0.001 against the mannitol osmolarity-control group O.I* stands for 4-octyl itaconate. B The mRNA expression of (b1) STEAP4 (b2) CCL2 (b3) TNF and (b4) IL1B after 24 hours exposure of RAW 264.7 cells to either a vehicle control (BSA) a combination of 100μM palmitic acid and 100nM Insulin or a combination of 100μM palmitic acid and 100nM Insulin and 0.1mM of 4-octyl itaconate (RTqPCR)Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 5–5–5) **p < 0.001 against the vehicle-control group O.I* stands for 4-octyl itaconate. C The effect of (c1) PDTC an inhibitor of NF-κB activation on glucose spikes-induced STEAP4 mRNA expression in RAW 264.7 cells (c2) SB203580 a p38 MAPK inhibitor on glucose spikes-inducedSTEAP4 mRNA expression in RAW 264.7 cells (c3) PDTC an inhibitor of NF-κB activation on persistent high-glucose induced STEAP4 mRNA expression in RAW 264.7 cells (c4) SB203580 a p38 MAPK inhibitor on persistent high-glucose induced STEAP4 mRNA expression in RAW 264.7 cells Dataexpressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 5–5–5) ***p < 0.001 **p < 0.01 *p < 0.05 NS means not statistically significant. D The effect of (d1) PDTC an inhibitor of NF-κB activation on palmitic acid-high insulin-induced STEAP4 mRNA expression in RAW 264.7 cells (d2) SB203580 a p38 MAPK inhibitor on palmitic acid high insulin-induced STEAP4 mRNA expression in RAW 264.7 cells Data expressed as a fold change normalized to GAPDH Values are Means ± SEM (n = 5–5–5) ***p < 0.001 **p < 0.01
Discussion
In this study, to the best of our understanding, we have shown for the first time that hyperglycemic spikes and early stages of diet-induced obesity are associated with a concurrent increase in STEAP4 and pro-inflammatory gene expression in mononuclear cells. We have also shown that the combined effect of western diet and glucose spikes in altering the expression of these genes was subtle and non-additive, suggesting that hyperglycemic spikes and obesity-related factors utilize the same pathway in inducing the expression of these genes. In an attempt to replicate our findings ex vivo, a combination of palmitic acid and high insulin synergistically increased STEAP4 and pro-inflammatory gene (such as IL1B, and IL6) expression in RAW 264.7 cells, suggesting that increased circulating free fatty acids and hyperinsulinemia in obesity or insulin-resistance state are metabolic factors responsible for monocyte activation. Furthermore, findings from our mechanistic studies suggest that increased signaling through the p38MAPK/NF-KB pathway, inflammation, and oxidative stress are associated with increased STEAP4 expression in mononuclear cells.
It is already reported that hyperglycemia can potentially induce the expression of pro-inflammatory genes in mononuclear cells [26, 27]. In addition to that, Wang and his co-workers [28] for the first time reported that a constant hyperglycemic state can induce the expression of STEAP4 in RAW 264.7. Although the effect of repetitive glucose spikes was obviously predictable, to the best of our knowledge this is the first report to provide the concrete effect of repetitive glucose spikes on the expression of inflammatory genes and STEAP4 in mononuclear cells.
In our in vitro experiments with RAW 264.7 cells, we observed that the effect of constant hyperglycemic condition in inducing the expression of STEAP4 and pro-inflammatory genes was stronger than that of intermittent hyperglycemic condition. Although Cariello et al. [29,30,31] never conducted a similar experiment, this finding is opposite to many of their reports highlighting the prominent pathophysiological significance of postprandial hyperglycemia or glucose spikes in the pathogenesis of cardiovascular diseases. This finding is also different from a finding by Liu et al. and Li et al. on the relative effect of intermittent high glucose on the expression of cytokines and inflammatory mediators in human coronary artery endothelial cells and THP-1 cells, respectively [32, 33]. Although our study and theirs didn’t follow the same protocol, this discrepancy of results warrants further investigation.
Our visceral obesity animal model exhibited high fasting insulin and free fatty acids levels which are typical of visceral obesity, insulin resistance state. However, surprisingly, in our in vitro experiments, palmitic acid caused no change in the level of expression of our genes of interest, probably because it was used in minimal concentration (100 µM), but a combination of palmitic acid and high insulin caused a synergistic increase in the expression of STEAP4 and pro-inflammatory genes; CCL2, IL6, and IL1B in RAW 264.7 cells.
Although the pro-inflammatory nature of saturated fatty acids (SFA) on immune cells is well-substantiated in a good number of studies [34,35,36], our results align with the recent report by Kikumi et al. questioning the pro-inflammatory character of saturated fatty acids particularly in cell culture systems [37]. It is more likely that increasing the concentration of palmitic acid beyond the one used in this experiment would lead to a concurrent increase in STEAP4 and pro-inflammatory gene expression. However, we observed the phenomenon reported by Kim et al. of higher concentrations of palmitic acid inducing necrosis in RAW 264.7 cells; that’s why a minimal concentration of palmitic acid was used in our cell culture experiments.
Our finding that palmitic acid and high insulin act synergistically to increase CCL2, IL6, and IL1B expression in RAW 264.7 cells is similar to what has been reported by Bunn and his colleagues [38] on the combined effect of palmitate and insulin in inducing the expression of IL6 in human monocytes. Their report suggested that an increase in the free fatty acid flux through the glycerolipid biosynthesis pathway in the hyper-insulinemic state may be responsible for such an observation. However, most striking is the fact that, similar to our finding, they reported that the MAPK inflammatory signaling pathway (an essential secondary branch of the insulin signaling pathway) was responsible for the observed palmitate-high insulin synergy. In this study we also showed for the first time that palmitic acid and high insulin synergistically increase STEAP4 expression in mouse monocyte cell-line (RAW 264.7 cells).
In our experiments increased STEAP4 expression by RAW 264.7 cells in different conditions, such as glucose spikes, persistent high glucose, and a combination of palmitic acid, and insulin was attenuated by either a cell-permeable Nrf2 activator or inhibitors of p38MAPK and NF-kB. In addition, inflammatory cytokines (TNF and IL6) additively increased STEAP4 expression in these cells. This corroborate the findings of previous all studies showing that STEAP4 expression is induced by increasing oxidative stress or inflammation [20,21,22,23,24,25].
As mentioned earlier, the balance between pro-atherogenic and anti-atherogenic factors (inflammatory status being one of such factors) is very crucial in the development of atherosclerotic lesions. To the best of our knowledge, this is the first study showing that repetitive hyperglycemic spikes and visceral obesity can induce the expression of not only pro-inflammatory genes but also the anti-inflammatory gene (STEAP4) in mononuclear cells.
Conclusion
In conclusion, diet-induced obesity and glucose spikes independently induced the expression of STEAP4 and pro-inflammatory genes in mononuclear cells, but, their combined effect was not additive. An increase in STEAP4 expression is a compensatory response.
Change history
17 October 2021
A Correction to this paper has been published: https://doi.org/10.1007/s13340-021-00549-8
References
Barquera S, Tobias AP, Medina C, Hernandez-Barrera L, Bibbins-Domingo K, Lozano R, Moran AE. Global overview of atherosclerotic cardiovascular disease. Arch Med Res. 2015. https://doi.org/10.1016/j.arcmed.2015.06.006.
Okajima F, Sato K, Kimura T. Anti-atherogenic actions of high-density lipoprotein through sphingosine 1-phosphate receptors and scavenger receptor class B type I. Endocr J. 2009. https://doi.org/10.1507/endocrj.K08E-228.
Harvey EJ, Ramji DP. Interferon-γ and atherosclerosis: Pro- or anti-atherogenic? Cardiovasc Res. 2005. https://doi.org/10.1016/j.cardiores.2005.04.019.
Cercato C, Fonseca FA. Cardiovascular risk and obesity. Diabetol Metab Syndr. 2019. https://doi.org/10.1186/s13098-019-0468-0.
Alexopoulos N, Katritsis D, Raggi P. Visceral adipose tissue as a source of inflammation and promoter of atherosclerosis. Atherosclerosis. 2014. https://doi.org/10.1016/j.atherosclerosis.2013.12.023.
Shuto Y, Asai A, Nagao M, Sugihara H, Oikawa S. Repetitive glucose spikes accelerate atherosclerotic lesion formation in C57BL/6 mice. PLoS ONE. 2015. https://doi.org/10.1371/journal.pone.0136840.
Hanssen NMJ, Kraakman MJ, Flynn MC, Nagareddy PR, Schalkwijk CG, Murphy AJ. Postprandial glucose spikes, an important contributor to cardiovascular disease in diabetes. Front Cardiovasc Med. 2020. https://doi.org/10.3389/fcvm.2020.570553.
Ceriello A, Esposito K, Piconi L, Ihnat M, Thorpe J, Testa R, Bonfigli AR, Giugliano D. Glucose ‘peak’ and glucose ‘spike’: Impact on endothelial function and oxidative stress. Diabetes Res Clin Pract. 2008;82:262–7.
Mita T, Otsuka A, Azuma K, Uchida T, Ogihara T, Fujitani Y, Hirose T, Mitsumata M, Kawamori R, Watada H. Swings in blood glucose levels accelerate atherogenesis in apolipoprotein E-deficient mice. Biochem Biophys Res Commun. 2007;358:679–85.
Azuma K, Kawamori R, Toyofuku Y, Kitahara Y, Sato F, Shimizu T, Miura K, Mine T, Tanaka Y, Mitsumata M, Watada H. Repetitive fluctuations in blood glucose enhance monocyte adhesion to the endothelium of rat thoracic aorta. Arterioscler Thromb Vasc Biol. 2006;26:2275–80.
Schaftenaar E, Frodermann F, Kuiper V, Lutgens J. Atherosclerosis: the interplay between lipids and immune cells. Curr Opin Lipidol. 2016. https://doi.org/10.1097/MOL.0000000000000302.
Gerrity RG. The role of the monocyte in atherogenesis. I. Transition of blood-borne monocytes into foam cells in fatty lesions. Am J Pathol. 1981;103:181–90.
Flynn MC, Pernes G, Lee MKS, Nagareddy PR, Murphy AJ. Monocytes, macrophages, and metabolic disease in atherosclerosis. Front Pharmacol. 2019. https://doi.org/10.3389/fphar.2019.00666.
Wolf D, Ley K. Immunity and inflammation in atherosclerosis. Circ Res. 2019. https://doi.org/10.1161/CIRCRESAHA.118.313591.
Wu MY, Li CJ, Hou MF, Chu PY. New insights into the role of inflammation in the pathogenesis of atherosclerosis. Int J Mol Sci. 2017. https://doi.org/10.3390/ijms18102034.
Ghanim H, Aljada A, Hofmeyer D, Syed T, Mohanty P, Dandona P. Circulating mononuclear cells in the obese are in a proinflammatory state. Circulation. 2004. https://doi.org/10.1161/01.CIR.0000142055.53122.FA.
Nandy D, Janardhanan R, Mukhopadhyay D, Basu A. Effect of hyperglycemia on human monocyte activation. J Investig Med. 2011. https://doi.org/10.2310/JIM.0b013e31820ee432.
Costa RM, Rodrigues D, Pereira CA, Silva JF, Alves JV, Lobato NS, Tostes RC. Nrf2 as a potential mediator of cardiovascular risk in metabolic diseases. Front Pharmacol. 2019. https://doi.org/10.3389/fphar.2019.00382.
Scarl RT, Lawrence CM, Gordon HM, Nunemaker CS. STEAP4: its emerging role in metabolism and homeostasis of cellular iron and copper. J Endocrinol. 2017. https://doi.org/10.1530/JOE-16-0594.
Moldens M, Lasnier F, Gauthereau X, Klein C, Pairault J, Feve B, Marie A, Guerin C. Tumor necrosis factor-α-induced adipose-related protein (TIARP), a cell-surface protein that is highly induced by tumor necrosis factor-α and adipose conversion. J Biol Chem. 2001. https://doi.org/10.1074/jbc.M105726200.
Wellen KE, Fucho R, Gregor MF, Furuhashi M, Morgan C, Lindstad T, Vaillacourt E, Gorgun CZ, Saatcioglu F, Hotamisligil GS. Coordinated regulation of nutrient andinflammatory responses by STAMP2Is essential for metabolic homeostasis. Cell. 2007. https://doi.org/10.1016/j.cell.2007.02.049.
Kim HY, Park SY, Lee MH, Oh YJ, Jung HU, Yoo SH, Jeong NY, Lee HJ, Suh SH, Seo SY, Cheong JH, Jeong JS, Yoo YH. Hepatic STAMP2 alleviates high fat diet-induced hepatic steatosis and insulin resistance. J Hepatol. 2015;63:477–85.
Han L, Tang MX, Ti Y, Wang ZH, Wang J, Ding WY, Wang H, Zhang Y, Zhang W, Zhong M. Overexpressing STAMP2 improves insulin resistance in diabetic ApoE2/2/LDLR2/2 mice via macrophage polarization shift in adipose tissues. PLoS ONE. 2013. https://doi.org/10.1371/journal.pone.0078903.g005.
Wang ZH, Zhang W, Gong HP, Guo ZX, Zhao J, Shang YY, Feng JB, Zhang Y, Zhong Y. Expression of STAMP2 in monocytes associates with cardiovascular alterations. Eur J Clin Investig. 2017. https://doi.org/10.1111/j.1365-2362.2010.02288.x.
Freyhaus HT, Calay ES, Yalcin A, Vallerie SN, Yang L, Calay ZZ, Saatcioglu F, Hotamisligil GS. Stamp2 controls macrophage inflammation through nicotinamide adenine dinucleotide phosphate homeostasis and protects against atherosclerosis. Cell Metab. 2012. https://doi.org/10.1016/j.cmet.2012.05.009.
Tanaka M, Masuda S, Matsuo Y, Sasaki Y, Muranaka K, Wada H, Hasegawa K, Tsukahara T, Shimatsu A, Asahara NS. Hyperglycemia and inflammatory property of circulating monocytes are associated with inflammatory property of carotid plaques in patients undergoing carotid endarterectomy. J Atheroscler Thromb. 2016. https://doi.org/10.5551/jat.32680.
Shanmugam N, Reddy MA, Guha M, Natarajan R. High glucose-induced expression of proinflammatory cytokine and chemokine genes in monocytic cells. Diabetes. 2003. https://doi.org/10.2337/diabetes.52.5.1256.
Wang J, Han L, Wang Z, Ding W, Shang Y, Tang M, Li W, Zhang Y, Zhang W, Zhong M. Overexpression of STAMP2 suppresses atherosclerosis and stabilizes plaques in diabetic mice. J Cell Mol Med. 2014. https://doi.org/10.1111/jcmm.12222.
Esposito K, Nappo F, Marfella R, Giugliano G, Giugliano F, Ciotola M, Quagliaro L, Ceriello A, Giugliano D. Inflammatory cytokine concentrations are acutely increased by hyperglycemia in humans role of oxidative stress. Circulation. 2002. https://doi.org/10.1161/01.CIR.0000034509.14906.AE.
Ceriello A. Does postprandial blood glucose matter and why? Endocrinol Nutr. 2009;56(Suppl 4):8–11.
Ceriello A, Genovese S. Atherogenicity of postprandial hyperglycemia and lipotoxicity. Rev Endocr Metab Disord. 2016. https://doi.org/10.1007/s11154-016-9341-8.
Liu T, Gong J, Chen Y, Jiang S. Periodic vs constant high glucose in inducing pro-inflammatory cytokine expression in human coronary artery endothelial cells. Inflamm Res. 2013. https://doi.org/10.1007/s00011-013-0623-2.
Li H, Luo H-Y, Liu Q, Xiao Y, Tang L, Zhong F, Huang G, Xu G-M, Xu A-M, Zhou ZG, Dai R-P. Intermittent high glucose exacerbates A-FABP activation and inflammatory response through TLR4-JNK signaling in THP-1 cells. J Immunol Res. 2018. https://doi.org/10.1155/2018/1319272.
Huang S, Rutkowsky JM, Snodgrass RG, Ono-Moore KD, Schneider DA, Newman JW, Adams SH, Hwang DH. Saturated fatty acids activate TLR-mediated proinflammatory signaling pathways. J Lipid Res. 2012. https://doi.org/10.1194/jlr.D029546.
Lee JY, Sohn KH, Rhee SH, Hwang D. Saturated fatty acids, but not unsaturated fatty acids, induce the expression of cyclooxygenase-2 mediated through toll-like receptor 4. J Biol Chem. 2001. https://doi.org/10.1074/jbc.M011695200.
Snodgrass RG, Huang S, Choi I-W, Rutledge JC, Hwang DH. Inflammasome-Mediated secretion of IL-1β in human monocytes through TLR2 activation; modulation by dietary fatty acids. J Immunol. 2013. https://doi.org/10.4049/jimmunol.1300298.
Ono-Moore KD, Blackburn ML, Adams SH. Is palmitate truly proinflammatory? Experimental confounders and context-specificity. Am J Physiol Endocrinol Metab. 2018. https://doi.org/10.1152/ajpendo.00187.2018.
Bunn RC, Cockrell GE, Ou Y, Thrailkill KM, Lumpkin CK, Fowlkes JL. Palmitate and insulin synergistically induce IL-6 expression in human monocytes. Cardiovasc Diabetol. 2010. https://doi.org/10.1186/1475-2840-9-73.
Acknowledgements
I am indebted to the enormous contribution played by individuals and the Government of Japan in general. First and foremost, special gratitude goes to Dr. Mihoko Kurano (Kagoshima University) and Dr. Katsutaro Morino (Shiga University) for their coaching in experimental techniques. Second, I would like to express my sincere thanks to the non-academic members of staff, particularly Ms. Miki Mihara, for her support in the entire period of the study. I am also indebted to my wife, Restituta, for her kind understanding and moral support during the entire period of execution of this study. Last but not least, I would like to acknowledge the Government of Japan through the Ministry of Education for supporting my study in Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Human and animal rights
In this study, all institutional and national guidelines for the care and use of laboratory animals were followed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised due to Figure 7D1, D2 was missing and included in this version.
Supplementary Information
Below is the link to the electronic supplementary material.
13340_2021_542_MOESM4_ESM.pdf
Supplementary file4 Suppl fig.1 The MRNA expression of STEAP4 and pro-inflammatory genes in PBMCs in response to western diet feeding (DNA-microarray) Data expressed as fold change versus the MFGS (-) group. Suppl fig.2 The MRNA expression of STEAP4 and pro-inflammatory genes in PBMCs in response repetitive glucose spikes (DNA-microarray) Data expressed as fold change versus the MFGS (-) group. Suppl fig.3 The MRNA expression of inflammation-related genes altered by glucose spikes and western diet in-common (DNA microarray) Data expressed as fold change versus the MFGS (-) group. Suppl fig.4a The correlation between STEAP4 expression in rat PBMCs and (a1) body weight (a2) adiposity index (a3) HOMA-IR and (a4) NEFA concentration r stands for Pearson’s correlation coefficient and p stands. for p-value. Suppl fig.4b The correlation between CCL2 expression in rat PBMCs and (b1) body weight (b2) adiposity index (b3) HOMA-IR and (b4) NEFA concentration r stands for Pearson’s correlation coefficient and p stands for p-value. Suppl fig.4c The correlation between TNF expression in rat PBMCs and (c1) body weight (c2) adiposity index (c3) HOMA-IR and (c4) NEFA concentration r stands for Pearson’s correlation coefficient and p stands for p-value. Suppl fig.4d The correlation between IL1B expression in rat PBMCs and (d1) body weight (d2) adiposity index (d3) HOMA-IR and (d4) NEFA concentration r stands for Pearson’s correlation coefficient and p stands for p-value. Suppl fig.5a The MRNA expression of (a1) STEAP4 (a2) TNF, NOS2, CCL2, IL1B, and IL6 in RAW 264.7 cells after 6 hours of no specific treatment (control) treatment with 0.5ng/mL or 1ng/mL of LPS (RT-qPCR). Data expressed as a fold change normalized to GAPDH Values are means ± SEM (n=5-4-4) *p<0.05 **p<0.01 ***p<0.001 versus the control group. Suppl fig.5b The MRNA expression of (b1) STEAP4 (b2) CCL2, IL6 and IL1B in RAW 264.7 cells after 6 hours treatment with either 600 μg/mL BSA (control) 200 μg/mL 400 μg/mL or 600 μg/mL AGE-BSA (RTqPCR). Data expressed as a fold change normalized to GAPDH Values are means ± SEM (n=5-5-5) **p<0.01 ***p<0.001 versus the control group. Suppl fig. 5c The MRNA expression of (c1) STEAP4 (c2) NOS2, TNF, CCL2, and IL6 in RAW 264.7 cells after 24 hours of no specific treatment (control) treatment with 100ng/mL or 500ng/mL of PMA (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are means ± SEM (n=5-5-5) *p<0.05 **p<0.01 versus the control group. Suppl fig.6 The mRNA expression of (a) STEAP4 (b) CCL2 (c) TNF (d) IL1B after 6 hours of no specific treatment (control) treatment with 10ng/mL LPS or a combination of 10ng/mL LPS and 0.1mM of 4-octyl itaconate (RT-qPCR) Data expressed as a fold change normalized to GAPDH Values are means ± SEM (n=5-5-5) ***p<0.001 versus the control group (PDF 482 KB)
About this article
Cite this article
Shayo, S.C., Ogiso, K., Kawade, S. et al. Dietary obesity and glycemic excursions cause a parallel increase in STEAP4 and pro-inflammatory gene expression in murine PBMCs. Diabetol Int 13, 358–371 (2022). https://doi.org/10.1007/s13340-021-00542-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-021-00542-1