Abstract
Phosphatidylinositol 3-kinase (PI3K) signaling plays a critical role in cholangiocarcinoma (CCA), as well as anti-cancer drug resistance and autophagy, the type II program cell death regulation. In this work, we aimed to: (1) determine the expression levels of several key components of PI3K signaling and (2) evaluate whether NVP-BEZ235, a novel dual PI3K/mTOR inhibitor, could inhibit CCA cell growth. Immunohistochemistry for p85α, p110α, AKT, p-AKT (T308), mTOR, p-mTOR (S2448), GSK-3β, p-GSK-3β (S9), PTEN, and p-PTEN (S380, T382/383) was performed in 30 CCA patients. Western blotting was used to analyze PTEN and p-PTEN expression in the cell lines (KKU-OCA17, KKU-100, KKU-M055, KKU-M139, KKU-M156, KKU-M213, and KKU-M214). The effects of NVP-BEZ235 on CCA cells were evaluated using a growth inhibition assay, flow cytometer and migration assay. Increased activation of PI3K/AKT signaling was reproducibly observed in the CCA tissues. The expression of p85α, mTOR, and GSK-3β was significantly correlated with metastasis. Interestingly, PTEN suppression by loss of expression or inactivation by phosphorylation was observed in the majority of patients. Furthermore, NVP-BEZ235 effectively inhibited CCA cell growth and migration through reduced AKT and mTOR phosphorylation and significantly induced G1 arrest without apoptosis induction, although increase autophagy response was observed. In conclusion, the constitutive activation of PI3K/AKT pathway in CCA is mainly due to PTEN inactivation by either loss of expression or phosphorylation along with an increased expression in its pathway components heralding a poor prognosis for CCA patients. This work also indicates that inhibition of PI3K and mTOR activity by the inhibitor NVP-BEZ235 has anti-cancer activity against CCA cells which might be further tested for CCA treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cholangiocarcinoma (CCA) is an aggressive cancer originating from the bile duct epithelium. CCA is a major public health problem in the northeastern part of Thailand where the highest incidence in the world has been reported [1, 2]. Chronic inflammation caused by liver fluke (Opisthorchis viverrini, Ov) infection is documented as the major etiology of CCA development in this area [1, 3, 4]. CCA is recognized as a highly metastatic cancer [5–7]. CCA patients are mostly clinically silent and difficult to diagnose until the disease is advanced and often in the metastatic stage resulting in a poor prognosis. Surgical treatment of early stage disease is the only curative therapy, but unfortunately, the majority of CCA patients present late with advanced stage disease, which is not surgically curable [8]. The addition of current chemotherapy regimens is helpful but does not appreciably improve the long-term survival rate [9]. In order to develop new molecular therapies for CCA, a better understanding of the molecular pathogenesis of CCA is needed. So far, the majority of molecular strategies target anti-apoptotic or growth-stimulating pathways, in order to interfere with cancer-specific mechanisms and reduce adverse effects on normal cells have been extensively explored [10].
We have previously demonstrated that PRKAR1A, a regulatory subunit 1 alpha of protein kinase A type I, is involved in CCA carcinogenesis [11]. Furthermore, inhibition of PRKAR1A had anti-cancer activity against CCA cells and enhanced apoptosis induction with an associated decrease in several protein kinases pathways including MAPK, PI3K/AKT, JAK/STAT, and Wnt/β-catenin signaling. This indicates that PRKAR1A might be a target for CCA treatment [12]. Therefore, these data lead us to focus more on the roles of other protein kinases in CCA.
We have recently identified that multiple protein kinases are activated in both CCA cell lines and CCA tissues. Among those activated protein kinases in CCA, PI3K/AKT signaling pathway is prominently activated [13]. In addition, a previous study has shown upregulation of a downstream of AKT in CCA tissues, mTOR, which was analyzed by a genomic DNA copy number arrays [14]. These results convince us to pay more attention on the roles of PI3K/AKT signaling pathway in CCA development.
PI3K/AKT signaling pathway plays a role as a regulator of many cellular processes including cell division, growth, and programmed cell death. On the other hand, activation of this particular pathway is central to the growth of many human cancers, including colon cancer [15], glioblastoma [16, 17], and CCA [18–24]. PI3K/AKT activation leads to increased resistance to radiation therapy and chemotherapy, and inhibition of this pathway can sensitize CCA cells to these therapies [23, 25, 26]. In addition, Menakongka and Suthiphongchai reported hepatocyte growth factor (HGF)-induced invasiveness in CCA cell lines was seen via PI3K/AKT signaling [27]. Conversely, inhibition of this pathway markedly suppressed HGF-stimulated CCA cell invasion.
In the present study, we demonstrated that the aberrant activation of the PI3K signaling pathway in human CCA correlated with tumor metastasis. We also evaluated the in vitro anti-tumorigenic effect of NVP-BEZ235, a dual PI3K/mTOR inhibitor which is an imidazo[4,5-c]quinoline derivative that inhibits activity by binding to the kinase ATP-binding cleft. This compound equally targets wild-type, mutated p110 and mTOR [28] in CCA.
Materials and methods
Human CCA specimens
The 30 paraffin-embedded tissues collected from primary tumors of CCA patients were obtained from the specimen bank of the Liver Fluke and Cholangiocarcinoma Research Center, Faculty of Medicine, Khon Kaen University, Thailand. Informed consent was obtained from each patient prior to surgery, and the Ethics Committee for Human Research at Khon Kaen University approved the research protocols (#HE561035).
Cell lines and cell culture
Human CCA cell lines including KKU-OCA17, KKU-100, KKU-M055, KKU-M139, KKU-M156, KKU-M213, and KKU-M214 were obtained from CCA patient, which were established at Khon Kaen University Liver Fluke and Cholangiocarcinoma Research Center. All cell lines were cultured in Ham’s F-12 medium (Gibco/BRL, Grand Island, NY, USA) supplemented with 44 mM NaHCO3, penicillin (100 units/ml), streptomycin (100 mg/ml), and 10 % fetal bovine serum in a humidified atmosphere containing 5 % CO2.
Antibodies and inhibitor
Antibodies used for this study were as follows: anti-PI3K (p85α), PI3K (p110α), AKT, p-AKT(S473), p-AKT (T308), mTOR, p-mTOR (S2448), GSK-3β, p-GSK-3β (S9), PTEN were purchased from Cell Signaling Technology (Cell Signaling Technology, Danvers, MA, USA.), p-PTEN (S380, T382/383) and LC3B were purchased from Abcam (Abcam, Cambridge, UK), and anti-β-actin antibody was purchased from Sigma (Sigma-Aldrich, St. Louis, MO, USA). The dual PI3K/mTOR inhibitor, NVP-BEZ235, was kindly supplied by Novartis Pharma AG (Basel, Switzerland). The inhibitor was dissolved in dimethylsulfoxide (DMSO; Amresco, Solon, OH, USA) at a stock concentration of 10 mM and stored at −20 °C until used.
Immunohistochemistry staining and scoring
Paraffin-embedded tissues were sectioned for immunohistochemistry (IHC) staining according to standard methods. Briefly, the sections of CCA tissues were deparaffinized and rehydrated through a graded series of aqueous ethanol solutions. Next, microwave antigen retrieval was performed with sodium citrate buffer for 10 min. Then, endogenous peroxidase activity was blocked with 0.3 % hydrogen peroxide in phosphate-buffered saline (PBS) for 30 min, and non-specific binding was blocked by 10 % skim milk in PBS for 1 h. The tissue sections were incubated overnight with the primary antibody against designed target proteins at 4 °C. After that, sections were incubated with peroxidase-conjugated Envision™ secondary antibody (DAKO, Denmark) for 1 h. After washing, peroxidase-labeled polymer, 0.1 % diaminobenzidinetetrahydrochloride solution was used for the signal development and then counterstained with Mayer’s hematoxylin. The stained sections were observed under a light microscope by using the high magnification power ×200 and ×400 (Axioscope A1, Carl Zeiss, Jena, Germany).
The IHC scoring system was used for quantitation of results. Grading of staining depended upon the intensity and frequency of staining in tumor area. Intensity of protein expression was classified into four groups: 0, negative; +1, weak expression; +2, moderate expression; +3, strong expression, respectively. The frequency of staining was divided into four groups: 0, negative; +1, 1–25 %; +2, 26–50 %; +3, >50 %, respectively. Staining scores were calculated by multiplying intensities and frequencies in each case which are classified into two groups: low expression levels; scores are <4 and high expression levels; sores are ≥4 [6, 29].
Growth inhibition assay
CCA cells (5 × 103) in 100 μl media were seeded in 96-well plates (Costar, Corning, NY, USA) and incubated overnight. Then, the cells were treated with different concentrations of NVP-BEZ235 ranging from 1 to 105 nM. After 48 h of incubation, cell numbers were estimated using the sulforhodamine B(SRB) assay (Sigma-Aldrich, St. Louis, MO, USA). The optical densities were read using a microtiter plate reader (Sunrise, TECAN Trading, Switzerland) at 540 nm. The experiments were performed in triplicate. The percentage of growth inhibition (%GI) was calculated by using the equation: %GI = (1 − (Nt/Nc) × 100, where Nt and Nc represent the absorbance in treated and control cultures, respectively. IC50, the drug concentration causing cells GI of 50 %, was determined by interpolation from dose–response curves, as previously described [30].
Flow cytometry analysis
CCA cells were seeded at 1.5 × 105 cells in six-well plates, cultured overnight, and then cells were treated with 10, 100, and 1,000 nM of NVP-BEZ235 or control medium for 48 h. After that, the cell cycle distribution was detected by staining DNA with propidium iodide (Invitrogen, Paisley, UK), while apoptosis and necrosis were detected by using Annexin-V-FLUOS staining kit (Roche, Penzberg, Germany), respectively. The cell cycle distribution and apoptosis were determined by flow cytometry (BD FACSCanto™ II, BD Biosciences, CA, USA) and analyzed by BDFACSDiva™ software (BD Biosciences, CA, USA).
Western blot analysis
Cells were treated with NVP-BEZ235 at a concentration as 10, 100, and 1,000 nM or control medium for 48 h, respectively. Cell lysates were electrophoresed and transferred to polyvinylidenedifluoride membranes (Millipore, Bedford, USA). Membranes were blocked with 5 % skim milk in Tris-buffered saline (TBS) at room temperature for 1 h and incubated with primary antibody at 4 °C overnight. After rinsing with TBS containing 0.1 % polyoxyethylenesorbitanmonolaurate (Tween-20; TBST), membranes were incubated with horseradish peroxidase-conjugated secondary antibody (Santa Cruz Biotechnology, CA, USA) at room temperature for 1 h. After rinsing with TBST, membranes were exposed to the ECL Prime Western Blotting Detection System (GE Healthcare Bio-Science, UK). The immunoblot and intensity were analyzed by the ImageQuant™ analysis system (GE Healthcare Bio-Science, UK). Human β-actin was used as a loading control.
Wound healing assay
CCA cells were seeded and grown to confluence in the fibronectin-coated 12-well plates (Costar, Corning, NY, USA). The in vitro wound healing assay was made by scraping the middle of the cell monolayer using a sterile micropipette tip. Floating cells were removed by extensive washing with sterile PBS. After that, cells were cultured with control medium (1 % of DMSO) and 10 nM of NVP-BEZ235 in culture medium. The experiments were performed in duplicate well for both conditions. Photographs were taken using a phase-contrast microscope with a digital camera (Axiovert 40, Carl Zeiss, Germany) at 0, 12, and 24 h after wounding. Degrees of cell spreading between groups were observed.
Statistical analysis
Statistical analyses were performed by SPSS software version 17 (IBM Corporation, NY, USA). The correlation between IHC scores of each protein in CCA tissues was calculated using the Pearson’s correlation coefficient. The association of protein expression in CCA tissues and patients’ clinico-pathological factors were assessed by Fisher’s exact test. Results of cell growth inhibition were presented as mean ± SEM of a representative experiment. The cell cycle analysis was represented as mean ± SD, and the significance of differences was addressed by Student’s t test. A P value <0.05 was considered statistically significant.
Results
Altered expression and association of PI3K/AKT signaling pathway molecules with CCA clinicopathological characteristics
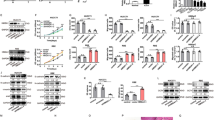
A total of 30 CCA tissues were studied, 70 % were male and 30 % were female. The age of patients ranged from 37 to 71 years old (median = 58 years old). The patients were at an advanced stage with 50 % presenting with metastasis. In this study, the histological types were classified as papillary type CCA (47 %) and non-papillary type CCA (53 %). The results of immunohistochemical staining revealed no or very weak positive staining of all proteins investigated in normal bile duct epithelia, while the increased expression was observed in pre-cancerous and cancer cells, respectively. The percent expression of p85α, p110α, AKT, p-AKT (T308), mTOR, p-mTOR (S2448), GSK-3β, and p-GSK-3β (S9) in CCA tissues is 27, 90, 50, 57, 67, 20, 40, and 27 %, respectively (Fig. 1a, Table 1). Moreover, expression levels of the p110α, catalytic subunit of PI3K, have a significant correlation with its regulatory subunit; p85α and its downstream targets as shown in Table 2. Interestingly, the expression of p85α, mTOR, and GSK-3β was significantly correlated with metastasis (P = 0.035, P = 0.008, and P = 0.025, respectively; Tables 3 and 4). Additionally, elevated expression of AKT, p-AKT, and GSK-3β was significantly correlated with non-papillary type of CCA (P = 0.028, P = 0.030, and P = 0.007, respectively; Tables 3 and 4). Furthermore, there was a trend towards significance between p-AKT expression and metastasis status of patients (P = 0.065). In addition, the expression levels of p110α also showed a trend associated with non-papillary (P = 0.073), with 67 % of these cases are metastatic CCA. Interestingly, we found loss of PTEN expression in the majority of CCA patients (70 %) as shown in Table 1. Furthermore, we observed that within 89 % of the PTEN positive cases, their PTEN were inactivated by phosphorylation. In addition, Western blot analysis revealed the PTEN inactivation by phosphorylation in all CCA cell lines studied (Fig. 1b). Therefore, loss of PTEN expression as well as inactivation by phosphorylation seems to be the major cause of PI3K/AKT overactivation in this series of CCA (Table 5).
Expression of several key components of PI3K/AKT signaling pathway. a The expression of p85α, p110α, AKT, p-AKT (T308), mTOR, p-mTOR (S2448), GSK-3β, p-GSK-3β (S9), PTEN, and p-PTEN (S380, T382/383) in normal adjacent bile duct and tumor area by immunohistochemistry staining. Original magnification is ×400. b Western blot analysis of the expression of PTEN and p-PTEN (S380, T382/383) in a panel of CCA cell lines
NVP-BEZ235 inhibits CCA cell growth through blocking the PI3K/mTOR activity
We examined further if NVP-BEZ235, a dual PI3K/mTOR inhibitor, could inhibit CCA cell proliferation. Seven CCA cell lines (OCA17, KKU100, M055, M139, M156, M213, and M214) were treated with a range of concentration of the small molecule, and cell proliferation was assessed by SRB assay. The results showed that NVP-BEZ235 effectively suppressed CCA cell growth at one nanomolar and in a dose-dependent manner (Fig. 2a). The IC50 values (mean ± SD) of NVP-BEZ235 in seven CCA cell lines, OCA17, KKU100, M055, M139, M156, M213, and M214, were 48 ± 19, 15 ± 4, 5 ± 2, 135 ± 48, 2 ± 1, 30 ± 5, and 45 ± 5, respectively. Additionally, Western blot analysis revealed that NVP-BEZ235 was able to inhibit the phosphorylation of S473 AKT and S2448 mTOR in two representative cell lines in a dose-dependent response (Fig. 2b), suggesting that NVP-BEZ235 blocks the PI3K/AKT pathway resulting in inhibition of CCA cell proliferation. Moreover, flow cytometry analysis demonstrated that NVP-BEZ235 induced significantly G1 arrest as well as reduced S phase progression of CCA cell lines, for M139 at 1,000 nM and M214 at 100 and 1,000 nM (Fig. 2c).
NVP-BEZ235 inhibits CCA cell proliferation. a Seven CCA cell lines were treated with NVP-BEZ235 with the indicated concentration for 48 h, and cell proliferation was assessed using SRB assay. Data are shown as mean ± SEM of one representative experiment. Each culture was done in three independent experiments. b Effects of NVP-BEZ235 on reducing of AKT and mTOR phosphorylation in CCA cells. Cells were treated with NVP-BEZ235 as indicated concentration for 48 h. Cell extracts were subjected to immunoblotting analysis for AKT, p-AKT (S473), mTOR, and p-mTOR (S2448), respectiviely. c NVP-BEZ235 causes cell cycle arrest at G1 phase. Cells were treated with NVP-BEZ235 for 48 h and subjected to propidium iodide staining analysis. The results were shown as the mean ± SD from three independent experiments.*P < 0.05 compared with control cells
NVP-BEZ235 induces autophagy without a remarkable effect on apoptosis in CCA cells
To test if NVP-BEZ235 inhibited cell growth, at least in part by inducing apoptosis, we performed flow cytometry using Annexin-V-FLUOS staining. The results indicated that NVP-BEZ235 has no remarkable effect on apoptosis induction (Fig. 3a), although NVP-BEZ235 decreased phosphorylation of AKT and mTOR which function as a key negative regulator for autophagy, the type II programmed cell death. We therefore examined the effect of NVP-BEZ235 on autophagy induction. The results revealed that NVP-BEZ235 induces LC3B (LC3-II) protein, a hallmark of cells undergoing autophagy in a dose- and time-dependent manner in treated CCA cell lines (Fig. 3b).
NVP-BEZ235 induces autophagy without remarkable effect on apoptosis in CCA cells. a Cells were treated with NVP-BEZ235 as indicated concentration for 48 h, then apoptosis cells were analyzed by using Annexin-V-FLUOS staining kit and flow cytometry. b NVP-BEZ235 induces autophagy in CCA cell lines. Cells were treated with NVP-BEZ235 for 24 and 48 h, respectively. Protein extracts were analyzed by Western blot with specific antibodies against LC3B (LC3-II), an autophagic marker. The apparent intensity of bands on the membranes was estimated using densitometry
NVP-BEZ235 inhibited migration of CCA cells
The above IHC data indicated the association of several key components of PI3K pathway with the metastasis status of the CCA patients studied. Therefore, we sought to determine if NVP-BEZ235 could inhibit CCA cell migration, an important step in the metastatic process. We performed an in vitro wound healing assay in conditioned culture medium with or without NVP-BEZ235. The results showed that the migration of the M139 and M214 cells was reduced by treating cells with 10 nM of NVP-BEZ235, a concentration which has no effect on cell proliferation (Fig. 4).
Discussion
Although an increased activation of PI3K/AKT pathway along with PTEN loss [20, 22] has been reported in CCA, until now there has been no comprehensive study of PI3K, AKT, p-AKT, mTOR, p-mTOR GSK-3β, p-GSK-3β together with PTEN and its inactive form, p-PTEN, in human CCA tissues. A previous study revealed that altered expression of p110α, the catalytic subunit of class IA PI3K, by amplification, overexpression, or somatic mutation has been found in various human tumors [31]. In this current work, we report the overexpression of p110α in human CCA tissues. Moreover, our results demonstrated the significant positive correlation between expression levels of p110α with its regulatory subunit, p85α, and its downstream targets. However, expression of p85α showed fewer positive cases than p110α, although p110α could be directly activated by RAS proteins [32], which are usually altered in CCA. A high frequency of KRAS proto-oncogene mutation was found in 4–60 % among Japanese and Thai CCA patients [33–36] and 100 % of English patients [37]. Moreover, there are studies that indicate elevated expression of mutated KRAS has been correlated with a more aggressive phenotype of CCA [38–40]. Furthermore, our data revealed that the expression of p85α was significantly associated with metastasis. Phosphorylation at T308 by PDK1 and S473 by mTORC2 is essential for maximal activation of AKT, although phosphorylation of T308 in AKT is essential and necessary for the cell transforming activity and for signaling [41], possibly as a result of changing in conformation that allows substrate binding and phosphorylation [42]. However, several studies focused on S473 rather than T308 phosphorylation, probably caused by relatively effective S473 antibodies, particularly in immunohistochemistry resulting in analyzing p-AKT (T308) in few studies. Thus, this study aimed to reveal the expression of p-AKT (T308) in CCA. Previous studies demonstrated an activation of the PI3K/AKT pathway in human CCA tissues which more than 50 % of cases expressed p-AKT and correlated with poor prognosis [18–23]. These data are consistent with our results as shown by 57 % of the cases positive for p-AKT (T308) and correlated with poor prognosis. Our results showed a few cases, 20 % positive for p-mTOR with no correlation to any clinical data. Chung and coworkers reported that p-mTOR expression was elevated in 83.7 % in extrahepatic CCA tissues [20]. Additionally, there was an altered expression of GSK-3β, which was previously reported to be a tumor suppressor in various types of cancer [43–45]. There is a single study that demonstrated the increased levels of p-GSK-3β (S9), an inactive form in a mouse model of CCA carcinogenesis [22]. In this study, we report the expression of GSK-3β and its inactive form, p-GSK-3β (S9), in human CCA tissues. Our IHC results revealed a strong positive staining intensity in tumors when compared with adjacent normal bile ducts. We found that about 40 % of cases expressed GSK-3β, which correlated with metastasis and histological type of the poor prognosis. Our finding was supported by growing evidence which indicated that GSK-3β can positively regulate cell survival and proliferation [46], as well as promote tumor development and progression. Moreover, inhibition of GSK-3β can sensitize tumor cells to chemotherapeutic drug as shown in pancreatic cancer [47]. In addition, we found that only 8 of 30 cases were positive for p-GSK-3β, an inactive form of GSK-3β. Furthermore, the expression of PTEN, which was defined as a tumor suppressor and a major negative regulator of PI3K/AKT signaling, was investigated. We found loss of PTEN expression in the majority of CCA patients (70 %) and consistent with the study of Chung and coworkers, which showed the absence of PTEN expression in extrahepatic cholangiocarcinoma patients [20]. Moreover, we found that among PTEN positive cases, their PTEN was inactivated through phosphorylation. The results are consistent with the study of Xu and coworkers [22].
We analyzed for the first time in CCA the therapeutic potential of a PI3K/mTOR inhibitor, NVP-BEZ235, an imidazo[4,5-c]quinoline derivative that inhibits activity by binding to the kinase ATP-binding cleft. This compound equally targets wild-type, mutated p110 and mTOR [28] as well as in cells with loss of PTEN expression [48]. We tested the growth inhibition effect of NVP-BEZ235 on a panel of CCA cell lines, which showed PTEN inactivated by phosphorylation. We found that NVP-BEZ235 could suppress CCA cell growth in the one nanomolar range of IC50 values in a dose-dependent manner. Moreover, the agent exerted its anti-cancer activity by reducing AKT and mTOR phosphorylation. Furthermore, flow cytometric analysis demonstrated that NVP-BEZ235 was capable of inducing G1 cell cycle arrest while lacking significant apoptosis induction. On the other hand, NVP-BEZ235 activates the CCA cells undergoing autophagy, a type II cell death which was indicated by increased LC3-II, an autophagic marker level, in a dose-and time-dependent manner. In many cancers, NVP-BEZ235 had no apparent apoptosis induction [48–52]. Liu and coworker demonstrated previously the cell growth inhibition as well as autophagy induction of NVP-BEZ235 in human glioma cells [50]. This is not surprising because NVP-BEZ235 target is mTORC1, an autophagic blocker resulting in autophagy induction. Although many studies demonstrate the proapoptotic properties of NVP-BEZ235 in breast cancer [28], waldenstrom macroglobulinemia [53], and hepatocellular carcinoma [54]. Additionally, it is known that autophagy is a cellular response to stress conditions, which is implicated in both pro-survival and pro-death processes in normal cells, as well as in cancer. It is also defined as a mechanism that may enable tumor cells to survive antineoplastic therapy. In addition, there are several lines of evidence demonstrating that many anti-cancer agents can also induce autophagy [55–58]. There are studies suggesting that NVP-BEZ235 alone was not sufficient to induce apoptosis; hence, this compound should be combined with other therapeutic approaches, such as MEK inhibitor [59] or radiotherapy [49, 52]. Furthermore, some studies mentioned that combined NVP-BEZ235 with autophagy inhibition can enhance its anti-cancer efficacy by driving the cancer cells to undergo apoptosis [60, 61]. Since our IHC analysis demonstrated the expression of several key components in PI3K/AKT pathway is correlated with metastasis in CCA patients, we tested if NVP-BEZ235 could inhibit CCA cell migration. As shown in Fig. 4, treated CCA cells with 10 nM of NVP-BEZ235 resulted in reduced CCA cell migration. This result suggests that this pathway plays a role in metastasis of CCA. This is supported by the study of Menakongka and colleagues who reported that hepatocyte growth factor promotes CCA cell invasiveness through PI3K pathway [27]. Furthermore, there are several reports that are consistent with our finding that NVP-BEZ235 can inhibit cancer cell migration [51, 52]. Moreover, Manara and co-workers also reported that NVP-BEZ235 suppressed cell metastasis of Ewing sarcoma xenografts in vivo mouse models [51]. Therefore, the PI3K pathway may be used as a potential target for treatment or prevention of metastasis in CCA.
Taken together, we demonstrated the constitutive activation of PI3K/AKT pathway in CCA patients as well as CCA cell lines. The possible mechanisms are PI3K overexpression as well as PTEN inactivation by both loss of expression and phosphorylation resulting in poor prognosis in human CCA studied. Therefore, this particular pathway represents a possible useful target for CCA treatment. This work also indicates that inhibition of PI3K and mTOR activity by a novel inhibitor, NVP-BEZ235, has anti-proliferation as well as migration inhibition effects on CCA cells. However, this small inhibitor failed to induce apoptosis of CCA cells while autophagy induction could be observed. Based on these findings, NVP-BEZ235 might be applied in a therapeutic strategy for CCA; however, using this particular drug in combination with other therapies should be considered.
Abbreviations
- CCA:
-
Cholangiocarcinoma
- PI3K:
-
Phosphoinositide 3-kinase
- mTOR:
-
Mammalian target of rapamycin
- MAPK:
-
Mitogen-activated protein kinase
- JAK/STAT:
-
Janus kinase/signal transducer and activator of transcription
References
Yongvanit P, Pinlaor S, Bartsch H. Oxidative and nitrative DNA damage: key events in opisthorchiasis-induced carcinogenesis. Parasitol Int. 2012;61(1):130–5.
Vatanasapt V, Sriamporn S, Vatanasapt P. Cancer control in Thailand. Jpn J Clin Oncol. 2002;32(Suppl):S82–91.
Thamavit W, Bhamarapravati N, Sahaphong S, Vajrasthira S, Angsubhakorn S. Effects of dimethylnitrosamine on induction of cholangiocarcinoma in Opisthorchis viverrini-infected Syrian golden hamsters. Cancer Res. 1978;38(12):4634–9.
Ohshima H, Bartsch H. Chronic infections and inflammatory processes as cancer risk factors: possible role of nitric oxide in carcinogenesis. Mutat Res. 1994;305(2):253–64.
Loilome W, Wechagama P, Namwat N, Jusakul A, Sripa B, Miwa M, et al. Expression of oxysterol binding protein isoforms in opisthorchiasis-associated cholangiocarcinoma: a potential molecular marker for tumor metastasis. Parasitol Int. 2012;61(1):136–9.
Namwat N, Puetkasichonpasutha J, Loilome W, Yongvanit P, Techasen A, Puapairoj A, et al. Downregulation of reversion-inducing-cysteine-rich protein with Kazal motifs (RECK) is associated with enhanced expression of matrix metalloproteinases and cholangiocarcinoma metastases. J Gastroenterol. 2011;46(5):664–75.
Techasen A, Loilome W, Namwat N, Takahashi E, Sugihara E, Puapairoj A, et al. Myristoylated alanine-rich C kinase substrate phosphorylation promotes cholangiocarcinoma cell migration and metastasis via the protein kinase C-dependent pathway. Cancer Sci. 2010;101(3):658–65.
Blechacz B, Gores GJ. Cholangiocarcinoma: advances in pathogenesis, diagnosis, and treatment. Hepatology. 2008;48(1):308–21.
Khan SA, Thomas HC, Davidson BR, Taylor-Robinson SD. Cholangiocarcinoma. Lancet. 2005;366(9493):1303–14.
Faivre S, Djelloul S, Raymond E. New paradigms in anticancer therapy: targeting multiple signaling pathways with kinase inhibitors. Semin Oncol. 2006;33(4):407–20.
Loilome W, Yongvanit P, Wongkham C, Tepsiri N, Sripa B, Sithithaworn P, et al. Altered gene expression in Opisthorchis viverrini-associated cholangiocarcinoma in hamster model. Mol Carcinog. 2006;45(5):279–87.
Loilome W, Juntana S, Namwat N, Bhudhisawasdi V, Puapairoj A, Sripa B, et al. PRKAR1A is overexpressed and represents a possible therapeutic target in human cholangiocarcinoma. Int J Cancer. 2011;129:34–44.
Dokduang H, Juntana S, Techasen A, Namwat N, Yongvanit P, Khuntikeo N et al. Survey of activated kinase proteins reveals potential targets for cholangiocarcinoma treatment. Tumor Biol. 2013. doi:10.1007/s13277-013-0930-9
McKay SC, Unger K, Pericleous S, Stamp G, Thomas G, Hutchins RR, et al. Array comparative genomic hybridization identifies novel potential therapeutic targets in cholangiocarcinoma. HPB (Oxford). 2011;13(5):309–19.
Johnson SM, Gulhati P, Rampy BA, Han Y, Rychahou PG, Doan HQ, et al. Novel expression patterns of PI3K/Akt/mTOR signaling pathway components in colorectal cancer. J Am Coll Surg. 2010;210(5):767–76. 76–8.
McDowell KA, Riggins GJ, Gallia GL. Targeting the AKT pathway in glioblastoma. Curr Pharm Des. 2011;17(23):2411–20.
Gallia GL, Tyler BM, Hann CL, Siu IM, Giranda VL, Vescovi AL, et al. Inhibition of Akt inhibits growth of glioblastoma and glioblastoma stem-like cells. Mol Cancer Ther. 2009;8(2):386–93.
Chen Y, Xu J, Jhala N, Pawar P, Zhu ZB, Ma L, et al. Fas-mediated apoptosis in cholangiocarcinoma cells is enhanced by 3,3'-diindolylmethane through inhibition of AKT signaling and FLICE-like inhibitory protein. Am J Pathol. 2006;169(5):1833–42.
Javle MM, Yu J, Khoury T, Chadha KS, Iyer RV, Foster J, et al. Akt expression may predict favorable prognosis in cholangiocarcinoma. J Gastroenterol Hepatol. 2006;21(11):1744–51.
Chung JY, Hong SM, Choi BY, Cho H, Yu E, Hewitt SM. The expression of phospho-AKT, phospho-mTOR, and PTEN in extrahepatic cholangiocarcinoma. Clin Cancer Res. 2009;15(2):660–7.
Schmitz KJ, Lang H, Wohlschlaeger J, Sotiropoulos GC, Reis H, Schmid KW, et al. AKT and ERK1/2 signaling in intrahepatic cholangiocarcinoma. World J Gastroenterol. 2007;13(48):6470–7.
Xu X, Kobayashi S, Qiao W, Li C, Xiao C, Radaeva S, et al. Induction of intrahepatic cholangiocellular carcinoma by liver-specific disruption of Smad4 and Pten in mice. J Clin Invest. 2006;116(7):1843–52.
Tanno S, Yanagawa N, Habiro A, Koizumi K, Nakano Y, Osanai M, et al. Serine/threonine kinase AKT is frequently activated in human bile duct cancer and is associated with increased radioresistance. Cancer Res. 2004;64(10):3486–90.
Lee D, Do IG, Choi K, Sung CO, Jang KT, Choi D, et al. The expression of phospho-AKT1 and phospho-MTOR is associated with a favorable prognosis independent of PTEN expression in intrahepatic cholangiocarcinomas. Mod Pathol. 2012;25(1):131–9.
Leelawat K, Narong S, Udomchaiprasertkul W, Leelawat S, Tungpradubkul S. Inhibition of PI3K increases oxaliplatin sensitivity in cholangiocarcinoma cells. Cancer Cell Int. 2009;9:3.
Yoon H, Min JK, Lee JW, Kim DG, Hong HJ. Acquisition of chemoresistance in intrahepatic cholangiocarcinoma cells by activation of AKT and extracellular signal-regulated kinase (ERK)1/2. Biochem Biophys Res Commun. 2010;405(3):333–7.
Menakongka A, Suthiphongchai T. Involvement of PI3K and ERK1/2 pathways in hepatocyte growth factor-induced cholangiocarcinoma cell invasion. World J Gastroenterol. 2010;16(6):713–22.
Serra V, Markman B, Scaltriti M, Eichhorn PJ, Valero V, Guzman M, et al. NVP-BEZ235, a dual PI3K/mTOR inhibitor, prevents PI3K signaling and inhibits the growth of cancer cells with activating PI3K mutations. Cancer Res. 2008;68(19):8022–30.
Jamnongkan W, Techasen A, Thanan R, Duenngai K, Sithithaworn P, Mairiang E, et al. Oxidized alpha-1 antitrypsin as a predictive risk marker of opisthorchiasis-associated cholangiocarcinoma. Tumour Biol. 2013;34(2):695–704.
Sun SY, Yue P, Dawson MI, Shroot B, Michel S, Lamph WW, et al. Differential effects of synthetic nuclear retinoid receptor-selective retinoids on the growth of human non-small cell lung carcinoma cells. Cancer Res. 1997;57(21):4931–9.
Bader AG, Kang S, Zhao L, Vogt PK. Oncogenic PI3K deregulates transcription and translation. Nat Rev Cancer. 2005;5(12):921–9.
Ong SH, Hadari YR, Gotoh N, Guy GR, Schlessinger J, Lax I. Stimulation of phosphatidylinositol 3-kinase by fibroblast growth factor receptors is mediated by coordinated recruitment of multiple docking proteins. Proc Natl Acad Sci U S A. 2001;98(11):6074–9.
Furubo S, Harada K, Shimonishi T, Katayanagi K, Tsui W, Nakanuma Y. Protein expression and genetic alterations of p53 and ras in intrahepatic cholangiocarcinoma. Histopathology. 1999;35(3):230–40.
Tada M, Omata M, Ohto M. High incidence of ras gene mutation in intrahepatic cholangiocarcinoma. Cancer. 1992;69(5):1115–8.
Petmitr S. Cancer genes and cholangiocarcinoma. Southeast Asian J Trop Med Public Health. 1997;28 Suppl 1:80–4.
Wattanasirichaigoon S, Tasanakhajorn U, Jesadapatarakul S. The incidence of K-ras codon 12 mutations in cholangiocarcinoma detected by polymerase chain reaction technique. J Med Assoc Thai. 1998;81(5):316–23.
Levi S, Urbano-Ispizua A, Gill R, Thomas DM, Gilbertson J, Foster C, et al. Multiple K-ras codon 12 mutations in cholangiocarcinomas demonstrated with a sensitive polymerase chain reaction technique. Cancer Res. 1991;51(13):3497–502.
Ohashi K, Nakajima Y, Kanehiro H, Tsutsumi M, Taki J, Aomatsu Y, et al. Ki-ras mutations and p53 protein expressions in intrahepatic cholangiocarcinomas: relation to gross tumor morphology. Gastroenterology. 1995;109(5):1612–7.
Isa T, Tomita S, Nakachi A, Miyazato H, Shimoji H, Kusano T, et al. Analysis of microsatellite instability, K-ras gene mutation and p53 protein overexpression in intrahepatic cholangiocarcinoma. Hepatogastroenterology. 2002;49(45):604–8.
Ahrendt SA, Rashid A, Chow JT, Eisenberger CF, Pitt HA, Sidransky D. p53 overexpression and K-ras gene mutations in primary sclerosing cholangitis-associated biliary tract cancer. J Hepatobiliary Pancreat Surg. 2000;7(4):426–31.
Hart JR, Vogt PK. Phosphorylation of AKT: a mutational analysis. Oncotarget. 2011;2(6):467–76.
Pearce LR, Komander D, Alessi DR. The nuts and bolts of AGC protein kinases. Nat Rev Mol Cell Biol. 2010;11(1):9–22.
Thiel A, Heinonen M, Rintahaka J, Hallikainen T, Hemmes A, Dixon DA, et al. Expression of cyclooxygenase-2 is regulated by glycogen synthase kinase-3beta in gastric cancer cells. J Biol Chem. 2006;281(8):4564–9.
Wang Y, Lam JB, Lam KS, Liu J, Lam MC, Hoo RL, et al. Adiponectin modulates the glycogen synthase kinase-3beta/beta-catenin signaling pathway and attenuates mammary tumorigenesis of MDA-MB-231 cells in nude mice. Cancer Res. 2006;66(23):11462–70.
Luo J. Glycogen synthase kinase 3beta (GSK3beta) in tumorigenesis and cancer chemotherapy. Cancer Lett. 2009;273(2):194–200.
Shin S, Wolgamott L, Yu Y, Blenis J, Yoon SO. Glycogen synthase kinase (GSK)-3 promotes p70 ribosomal protein S6 kinase (p70S6K) activity and cell proliferation. Proc Natl Acad Sci U S A. 2011;108(47):E1204–13.
Shimasaki T, Ishigaki Y, Nakamura Y, Takata T, Nakaya N, Nakajima H, et al. Glycogen synthase kinase 3beta inhibition sensitizes pancreatic cancer cells to gemcitabine. J Gastroenterol. 2012;47(3):321–33.
Maira SM, Stauffer F, Brueggen J, Furet P, Schnell C, Fritsch C, et al. Identification and characterization of NVP-BEZ235, a new orally available dual phosphatidylinositol 3-kinase/mammalian target of rapamycin inhibitor with potent in vivo antitumor activity. Mol Cancer Ther. 2008;7(7):1851–63.
Konstantinidou G, Bey EA, Rabellino A, Schuster K, Maira MS, Gazdar AF, et al. Dual phosphoinositide 3-kinase/mammalian target of rapamycin blockade is an effective radiosensitizing strategy for the treatment of non-small cell lung cancer harboring K-RAS mutations. Cancer Res. 2009;69(19):7644–52.
Liu TJ, Koul D, LaFortune T, Tiao N, Shen RJ, Maira SM, et al. NVP-BEZ235, a novel dual phosphatidylinositol 3-kinase/mammalian target of rapamycin inhibitor, elicits multifaceted antitumor activities in human gliomas. Mol Cancer Ther. 2009;8(8):2204–10.
Manara MC, Nicoletti G, Zambelli D, Ventura S, Guerzoni C, Landuzzi L, et al. NVP-BEZ235 as a new therapeutic option for sarcomas. Clin Cancer Res. 2010;16(2):530–40.
Fokas E, Yoshimura M, Prevo R, Higgins G, Hackl W, Maira SM, et al. NVP-BEZ235 and NVP-BGT226, dual phosphatidylinositol 3-kinase/mammalian target of rapamycin inhibitors, enhance tumor and endothelial cell radiosensitivity. Radiat Oncol. 2012;7:48.
Roccaro AM, Sacco A, Husu EN, Pitsillides C, Vesole S, Azab AK, et al. Dual targeting of the PI3K/Akt/mTOR pathway as an antitumor strategy in Waldenstrom macroglobulinemia. Blood. 2010;115(3):559–69.
Masuda M, Shimomura M, Kobayashi K, Kojima S, Nakatsura T. Growth inhibition by NVP-BEZ235, a dual PI3K/mTOR inhibitor, in hepatocellular carcinoma cell lines. Oncol Rep. 2011;26(5):1273–9.
Ertmer A, Huber V, Gilch S, Yoshimori T, Erfle V, Duyster J, et al. The anticancer drug imatinib induces cellular autophagy. Leukemia. 2007;21(5):936–42.
Shinojima N, Yokoyama T, Kondo Y, Kondo S. Roles of the Akt/mTOR/p70S6K and ERK1/2 signaling pathways in curcumin-induced autophagy. Autophagy. 2007;3(6):635–7.
Kanzawa T, Germano IM, Komata T, Ito H, Kondo Y, Kondo S. Role of autophagy in temozolomide-induced cytotoxicity for malignant glioma cells. Cell Death Differ. 2004;11(4):448–57.
Saiki S, Sasazawa Y, Imamichi Y, Kawajiri S, Fujimaki T, Tanida I, et al. Caffeine induces apoptosis by enhancement of autophagy via PI3K/Akt/mTOR/p70S6K inhibition. Autophagy. 2011;7(2):176–87.
Faber AC, Li D, Song Y, Liang MC, Yeap BY, Bronson RT, et al. Differential induction of apoptosis in HER2 and EGFR addicted cancers following PI3K inhibition. Proc Natl Acad Sci U S A. 2009;106(46):19503–8.
Fan QW, Cheng C, Hackett C, Feldman M, Houseman BT, Nicolaides T, et al. Akt and autophagy cooperate to promote survival of drug-resistant glioma. Sci Signal. 2010;3(147):ra81.
Xu CX, Zhao L, Yue P, Fang G, Tao H, Owonikoko TK, et al. Augmentation of NVP-BEZ235's anticancer activity against human lung cancer cells by blockage of autophagy. Cancer Biol Ther. 2011;12(6):549–55.
Acknowledgments
This study is supported the Higher Education Research Promotion and National Research University Project of Thailand, Office of the Higher Education Commission, through the Center of Excellence in Specific Health Problems in Greater Mekong Sub-region cluster (SHeP-GMS), Khon Kaen University to SY and WL. WL thanks the Thailand Research Fund (grant no. MRG5400834) for the grant. We are also grateful to Novartis for providing us with NVP-BEZ235 to complete this work. GJR is supported in part by the Irving J. Sherman Research Professorship in Neurosurgery Research and the Virginia and D.K. Ludwig Fund for Cancer Research.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yothaisong, S., Dokduang, H., Techasen, A. et al. Increased activation of PI3K/AKT signaling pathway is associated with cholangiocarcinoma metastasis and PI3K/mTOR inhibition presents a possible therapeutic strategy. Tumor Biol. 34, 3637–3648 (2013). https://doi.org/10.1007/s13277-013-0945-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-013-0945-2