Abstract
Previously, we reported the radiosensitizing potential of the combination of 2-deoxy-d-glucose (2DG) and ferulic acid (FA) in NCI-H460 non-small cell lung carcinoma cells in vitro. The present study aims to explore the relevant mechanism of cell death induced by the combination of 2DG and FA along with irradiation in NCI-H460 cells. Incubation of NCI-H460 cells with the combination of 2DG and FA for 24 h before irradiation upregulated the expression of proapoptotic proteins p53 and Bax. Combination of 2DG and FA also increased the levels of p21 and GADD45A in NCI-H460 cells. DNA repair inhibition is expected to be a possible mechanism for the radiosensitization observed, which is evidenced by the downregulation of radiation-induced ataxia-telangiectasia mutated gene expression upon treatment with 2DG and/or FA. Moreover, Western blotting analysis of NF-κB and caspase-3 revealed the involvement of apoptotic signals in the cytotoxicity exhibited by the combination of 2DG and FA. Cell cycle analysis data also showed the increased percentage of Sub-G0 phase cells upon treatment with the combination of 2DG and FA before irradiation. Taken together, the results of our study clearly suggested that the cell death induced by the combination of 2DG and FA along with irradiation would involve alteration in expression of p53, p21, NF-κB, Bax, and caspase-3, indicating oxidative mechanism in NCI-H460 cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer can be categorized into two broadly defined groups: small cell lung carcinoma and non-small cell lung cancer (NSCLC) [1]. NSCLC accounts for 86 % of all lung cancer diagnosed. Radiation and chemotherapy are the primary treatments for non-resectable, locally advanced NSCLC. However, it has been observed that NSCLC often resists both chemotherapy and radiotherapy and that overexpression of glucose transporter 1 and 3 is associated with poor survival of non-small cell lung cancer [2, 3].
Cancer cells depend mainly on glucose metabolism for their energy production and macromolecular synthesis. Even under aerobic conditions, tumor cells continue to rely on glycolysis rather than oxidative phosphorylation (Warburg effect), resulting in high glucose requirements to generate energy and support metabolic function [4, 5]. 2DG, a glycolytic inhibitor, has been shown to inhibit the proliferation of tumor cells and also induce cell death. Indeed, many studies have found that 2DG inhibits the growth of neoplastic cells in vitro [6, 7]. 2DG exhibits a cytotoxic effect in cancer cells, but the same dose spares normal cells [8]. Many mechanisms are postulated to contribute to the antitumor effect of 2DG, including inhibition of glucose transport [9] and hexokinase II activity, depletion of cellular ATP, blockage of cell cycle progression, induction of apoptosis [10], induction of endoplasmic reticulum stress [11], and/or induction of oxidative stress [12]. 2DG sensitizes cancer cells to radiation through mechanisms such as inhibition of DNA repair processes and recovery from potentially lethal damage [13], and induction of oxidative stress [12].
Combining glycolytic inhibition with plant-derived phenolics is a new approach being considered to selectively kill cancer cells. Plant phenolics are usually considered to be antioxidants, but they also exhibit prooxidant properties in cancer cells; this is because of acidic environment that prevails in cancer cells and presence of high levels of peroxidases which act on phenolics and produce phenoxy radicals [14]. The prooxidant action of phenolic phytochemicals has been predicted to be an important mechanism for radiosensitization property in cancer cells [15]. Tumor cells have higher levels of ROS than their normal counterparts and are therefore more sensitive to the additional oxidative stress generated by anticancer agents [16]. Emerging evidence suggests that ROS induce programmed cell death in several cancer cells. Recently, many compounds like phenolic phytochemicals have been shown to induce apoptosis in cancer cells by the generation of ROS [15]. Earlier reports from our laboratory indicated the radiosensitizing effect of FA, a dietary phenolic acid, in NCI-H460 cells through prooxidant mechanism [17].
Approximately 80 % of human lung cancers are NSCLC, and their development involves multiple genetic abnormalities that lead to malignant transformation of the bronchial epithelial cells, followed by invasion and lymph node and distant metastases. Among such genetic abnormalities, the TP53 tumor suppressor gene appears to be the most frequent target, and abnormality of TP53 plays an important role in the tumorigenesis of lung epithelial cells. The transcription factor, TP53 can activate the transcription of numerous downstream genes, such as p21 and MDM2, by binding to specific sequences, which often mediates their biological functions [18]. Ionizing radiation induces a number of DNA and nonDNA lesions [19], causing disturbances in the signal transduction pathways and alterations in gene expression [20], leading to the initiation of repair processes, delayed cell proliferation, and apoptosis [21].
Pathological NF-κB-induced gene expression is essential for tumorigenesis and metastasis [22]. In NSCLC cell lines, it has been demonstrated that tobacco components stimulate NF-κB-dependent survival [23]. It has been reported earlier that curcumin induces apoptosis by targeting mitochondria, affecting p53-related signaling or blocking NF-κB activation [24]. Caspases, a group of cysteine proteases, are found to be responsible for most of the morphological and biochemical changes observed in apoptotic cells and are considered to be the central executioners of apoptotic process [25]. In vitro, chemotherapy-resistant NSCLC is associated with reduced expression of apical CASP9 and CASP3 as measured by immunochemistry [26]. CASP3 plays an important role in cytotoxic drug-induced apoptosis in NSCLC [27]. It was reported earlier that the apoptotic markers p53, Bax, and Bcl-2 expression would influence the treatment outcome in NSCLC patients [28]. NSCLC pathologic samples have shown that Bcl-2 and Bax proteins may also impact chemotherapy response in patients [29]. The cytotoxicity of ionizing radiation is mainly mediated through the generation of DNA-double strand break (DSB) as evidenced by the pronounced radiosensitivity of cells and organisms defective in the machinery of DSB repair [30]. The ataxia-telangiectasia mutated (ATM) protein kinase is a critical component in these pathways. Xing and his colleagues have reported the prognostic significance of ATM expression in patients with NSCLC [31]. In the present study, we investigated the modulatory role of 2DG and FA on radiation response signaling in terms of radiosensitization in relatively radioresistant NCI-H460 cells in vitro.
Materials and methods
Chemicals
2DG, FA, RPMI-1640 medium, glutamine–penicillin–streptomycin solution, heat inactivated fetal calf serum (FCS), trypsin-EDTA solution were purchased from Sigma Chemicals Co., St. Louis, USA. CellsDirect™ One-Step qRT-PCR kit was purchased from Invitrogen Company, California, USA. Primers for the genes were purchased from Sigma Chemicals Co. Monoclonal antibodies anti-β actin, anti-TP53, anti-TP21, anti-NF-κB, anti-Bax, anti-caspase-3 antibody, and IgG-HRP polyclonal antibody were purchased from Sigma Chemicals Co.
Cell and culture conditions
Human non-small cell lung carcinoma cell line, NCI-H460, was obtained from National Centre for Cell Science, Pune, India. Cells were maintained in RPMI-1640 medium supplemented with 10 % FCS, 1 mM sodium pyruvate, 10 mM HEPES, 1.5 g/L sodium bicarbonate, 2 mM l-glutamine, 10,000 U/ml penicillin, and 10 mg/ml streptomycin. Cells were grown in 5 % CO2 and air in a humidified 37 °C incubator. Stocks were maintained in 25-cm2 tissue culture flasks at 37 °C in 5 % CO2 incubator.
Drug and radiation treatment
Stock solutions of 1 M 2DG and FA were dissolved in PBS and diluted in culture medium to the indicated final concentration for cell treatment. Radiation doses were given as single fractions. Irradiation (IR) was carried out using Phonex Teletherapy Unit (Cobalt 60), G.V.N. Cancer Hospitals, Trichy, India. Radiation dose was given at a rate of 1.6 Gy/min.
Experimental groups
To evaluate the radiosensitizing potential of 2DG and FA, the NCI-H460 cells were treated with 4 mM 2DG and/or 53.8 μM FA for 24 h and then exposed to 2-Gy irradiation. Upon 24 h postirradiation, different cellular and molecular end points were studied. This has been clearly given under material and methods. Group 1: untreated control cells; Group 2: 2DG (4 mM) treated; Group 3: FA (53.8 μM) treated; Group 4: 2DG (4 mM)+FA (53.8 μM) treated; Group 5: IR (2 Gy) treated; Group 6: 2DG (4 mM)+IR (2 Gy) treated; Group 7: FA (53.8 μM)+IR (2 Gy) treated; Group 8: 2DG (4 mM)+FA (53.8 μM)+IR (2 Gy) treated.
Gene expression analysis: qRT-PCR assay
Total cellular RNA was extracted with the RNeasyTM mini kit in accordance with the manufacturer’s instructions from Qiagen Company. The concentrations of extracted RNA were determined by measuring the absorbance at 260 and 280 nm, and the quality of RNA was determined from the absorbance ratio of A260/A280 (A260/A280 > 1.8) and confirmed by gel electrophoresis. Extracted RNA was preserved at −80 °C until used. cDNA was synthesized using 5 μg total RNA by superscript III reverse transcriptase enzyme (Invitrogen). Primers sequences for 18S rRNA F: 5′ AGGAATTCCCAGTAAGTGCG 3′, R: 5′ GCCTCACTAAACCATCCAA 3′, TP53 F: 5′ CTTCGAGATGTTCCGAGAGC 3′, R: 5′ TTATGGCGGGAGGTAGACTG 3′, Bax F: 5′ CATGGAGCTGCAGAGGATGAT 3′, R: 5′ TTGCCGTCAGAAAACATGTCA 3′, ATM F: 5′ TGGATCCAGCTATTTGGTTTGA 3′, R: 5′ CCAAGTATGTAACCAACAATAGAAGAAGTAG 3′, and GADD45A F: 5′ TCAGCGCACGATCACTGTC 3′, R: 5′ CCAGCAGGCACAACACCAC 3′. Complimentary DNA was amplified in 50 μl total volume containing SYBR green master mix and 600 nM of the specific primers. Real time-PCR was performed on Eppendorf Mastercycler. Cycling conditions were as follows: For cDNA synthesis, 25 °C for 10 min, 42 °C for 50 min, and 75 °C for 15 min; for DNA amplification, 2-min denaturation step at 95 °C followed by 40 cycles with 15 s denaturation at 95 °C, 15 s primer annealing at 55 °C, and 20 s of elongation at 68 °C; for quantitation, differences between treatments were analyzed by comparing mRNA levels to the control after normalization to 18S rRNA mRNA levels. The statistical analysis of the real time-PCR results was calculated by using the ΔCt value (Ct gene of interest − Ct reporter gene). Relative gene expression was obtained by ΔΔCt methods (ΔCt sample − ΔCt calibrator) with the use of the sham-operated group as a calibrator for comparison of all unknown sample gene expression levels. The conversion between ΔΔCt and relative gene expression levels is as follows: fold induction = 2-ΔΔCt, where 2-ΔΔCt is relative gene expression [32].
Western blot analysis
Cultured cells were washed with PBS solution and detached from the culture dishes using a rapid treatment with trypsin-EDTA solution. Cell suspensions were centrifuged at 1,000 rpm for 10 min, and the pellets were lysed with an ice-cold lysis buffer (50 mM; Tris–HCl pH 7.4; 1 % NP-40; 150 mM NaCl; 2 mM EDTA; 0.1 % SDS; 1 mM EGTA; 1 mM PMSF; 0.15 % bME) containing a protease inhibitor cocktail (Sigma–Aldrich, Saint Louis, Missouri, USA) for 30 min. The lysate was cleared by centrifugation at 4 °C for 10 min at 14,000 rpm, and the supernatant was used to determine the protein concentration of the lysates using the Lowry protein assay [33]. Cell extracts containing 50 μg of proteins were fractionated on 10 and 12 % SDS–PAGE gel and transferred to a nitrocellulose acetate membrane (Amersham Biosciences, Piscataway, NJ, USA) using Bio-Rad semi-dry apparatus. Nitrocellulose membrane were blocked with 5 % (w/v) nonfat milk (blocking solution) in Tris-buffered saline–Tween-20 (TBST) (1.5 M NaCl, 20 mM Tris–HCl, 0.05 % (v/v) Tween-20) for 6 h and then incubated with primary antibodies (Sigma–Aldrich), diluted 1:1,000 in blocking solution, overnight at 37 °C. The membranes were washed with TBST thrice with 10-min intervals and then incubated with horseradish peroxidase conjugated secondary antibody diluted 1:2,000 in blocking solution incubated for 2 h at 37 °C. Then, the membranes were washed with TBST thrice with 10-min intervals, and the bands were detected using a DAB solution. The images were acquired by Image Station 2000R (Kodak, NY, USA). The graph represents the quantification results normalized to β-actin levels.
Cell cycle analysis
The cells at the density of 3.5 × 106 cells were seeded in T-25 culture flasks. The cells (treated/untreated) were then exposed to 2 Gy gamma radiation. After exposure, the cells were washed in PBS, and the viability of the cells was determined by the trypan blue dye exclusion method. For analyzing DNA content, 1 × 106 viable cells were fixed in cold 70 % ethanol in PBS at −20 °C. After 12 h, the fixed cells were pelleted, gently resuspended in ice-cold PBS, and supplemented with 0.5 mg/ml propidium iodide plus 50 μg/ml RNase A. The samples were then incubated at 37 °C for 30 min and stored in dark at 4 °C. The red fluorescence of individual cells was measured at an excitation wavelength of 540 nm and emission wavelength at 610 nm on a FACS caliber flow cytometry (Becton Dickinson, San Jose, CA, USA). A minimum of 10,000 events were analyzed per samples in the flow cytometer.
Statistical analysis
All experiments were performed two times independently, and each experiment included two or three replicates. The data were statistically analyzed using one-way analysis of variance (ANOVA) on statistical package for social sciences, and the group means were compared by Duncan’s multiple range test (DMRT). The results were considered statistically significant if the P value is the less than 0.05 levels.
Results
Figure 1 shows the effect of 2DG, FA, and IR on the expression pattern of p53 and p21 proteins in NCI-H460 cells. p53 and p21 protein expression was increased significantly in 2DG+FA treatment group as compared to the groups treated with 2DG and FA alone. Radiation exposure to NCI-H460 cells has significantly increased the expression of p53 and p21 proteins. Combination treatment of 2DG+FA+IR showed a further increase in the expression of p53 and p21 proteins compared to all other groups.
Effect of 2DG, FA, and IR on the expression pattern of p53 and p21 proteins in NCI-H460 cells. (A) Control, (B) 2DG, (C) FA, (D) 2DG+FA, (E) IR, (F) 2DG+IR, (G) FA+IR, and (H) 2DG+FA+IR. The graph represents the quantification results normalized to β-actin levels. Values not sharing a common marking (a, b, and c) differ significantly at P ≤ 0.05 (DMRT)
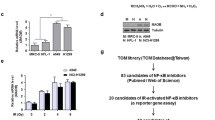
Figure 2 shows the effect of 2DG, FA, and IR on the expression pattern of Bax, caspase-3, and NF-κB proteins in NCI-H460 cells. Bax and caspase-3 protein levels were significantly increased in 2DG+FA treatment group as compared to groups treated with 2DG and FA alone. Radiation exposure to NCI-H460 cells has significantly increased the expression of Bax and caspase-3 proteins. 2DG+FA+IR combined treatment group has showed a further increase in the levels of Bax and caspase-3 proteins. NF-κB protein levels were decreased in 2DG- and FA-treated groups compared to control group. Radiation exposure alone has increased the expression of NF-κB protein in NCI-H460 cells. Combination of 2DG+FA+IR has showed a significant decrease in the expression level of NF-κB protein.
Effect of 2DG, FA, and IR on the expression pattern of Bax, caspase-3, and NF-κB proteins in NCI-H460 cells (A) Control, (B) 2DG, (C) FA, (D) 2DG+FA, (E) IR, (F) 2DG+IR, (G) FA+IR, and (H) 2DG+FA+IR. The graph represents the quantification results normalized to β-actin levels. Values not sharing a common marking (a, b, and c) differ significantly at P ≤ 0.05 (DMRT)
Figure 3 shows the effect of 2DG, FA, and IR on the relative mRNA levels of p53, Bax, ATM, and GADD45A genes in NCI-H460 cells. The mRNA levels of p53, Bax, and GADD45A were overexpressed under 2DG and FA treatments compared to untreated control. Exposing NCI-H460 cells to radiation has resulted in the overexpression of p53, Bax, and GADD45A genes. Combined treatment of 2DG+FA+IR has resulted in the significant overexpression of p53, Bax, and GADD45A genes compared with any treatment group alone. Expression of ATM gene was downregulated upon the treatment with 2DG and FA. Irradiation of NCI-H460 cells resulted in the overexpression of ATM. Combined treatment of 2DG and FA along with irradiation has resulted in the downregulation of radiation-induced expression of ATM.
Figure 4 shows the effect of 2DG, FA, and IR on NCI-H460 cell cycle progression. Table 1 shows the percentage of cells in sub-zero, G0-G1, S, and G2/M phases of cell cycle in NCI-H460 cells. Incubation of cells with 2DG+FA (39.7 %) resulted in the increase of sub-G0 cell population compared with groups treated with 2DG and FA alone. Radiation treatment significantly increased (41.3 %) the population of cells in the sub-G0 phase, indicating the characteristics of apoptosis. Whereas incubation of cells with 2DG and FA before irradiation has further increased (57.2 %) the population of cells in sub-G0 stage when compared to all other treatment modalities.
Discussion
Radiotherapy acts through the induction of double strand breaks to DNA in order to induce elimination of cancerous cells via programmed cell death [34]. The efficiency of radiotherapy for cancer treatment is limited by toxic side effects impeding dose escalation. Moreover, cancer cells often develop radioresistance mechanisms that are related to the DNA repair response. The aim of combining chemotherapy to radiotherapy is to strengthen the efficiency of radiation by inhibition of DNA repair, and overcoming of apoptosis resistance.
It has been shown that 2DG, a glycolytic inhibitor, inhibits growth and induces apoptosis in a number of cancer cell lines [35]. Many reports have well documented the role of p53 in apoptosis. In this study, we have observed that p53 plays an important role in the radiosensitization effect of 2DG in NCI-H460 cells. 2DG sensitizes cancer cells to radiation through mechanisms such as inhibiting DNA repair processes and recovery from potentially lethal damage [13], and inducing oxidative stress [12]. Earlier studies also demonstrated that 2DG induces radiosensitization of p53 wild-type non-small cell lung cancer cells but not of p53-deficient cells [36], and this study also shows that 2DG increases p53 expression in p53 wild-type cells. Ionizing radiation activates p53, causing cell cycle arrest and apoptosis [37]. Consistent with earlier reports, we have also observed an increase of p53 level in NCI-H460 cells upon treatment with 2DG, FA, and/or 2 Gy radiation in the present study. A microarray analysis of H2O2-treated human cells identified one-third of the 48 highly H2O2 responsive genes as targets of p53 [38]. Though it is generally recognized that oxidative stress is associated with p53-dependent cell cycle arrest, DNA repair, and apoptosis, a clear understanding of the mechanisms of the interactions between ROS and p53 is still elusive.
It has previously been shown that cytotoxic stimuli, such as radiation, activate p53 pathway, which leads to the expression of p21, GADD45, and other downstream targets, resulting cell cycle arrest and apoptosis [39]. The p53 protein is a critical regulator of cellular growth controlling both proliferation and apoptotic response of cells. The induction of the p21WAF1/CIP1 protein after ionizing radiation mediates p53-dependent G1 arrest via its inhibitory effects on cyclin-dependent kinases (CDKs) required for S-phase entry [40]. GADD45 is under transcriptional control by p53; since cellular responses to DNA damage are also under transcriptional control by p53, an understanding of the interaction of p53 with GADD45 is important [41]. In this study, we observed an increase in the GADD45A gene expression upon exposing the NCI-H460 cells to 2-Gy irradiation and a combination of 2DG, FA, and IR greatly enhances the GADD45A expression. Ionizing radiation-induced GADD45 expression has been reported to play a critical role in apoptosis [42]. Curcumin has been reported to increase the GADD45 expression in lung cancer cells [43]. In the present study, radiation-induced GADD45A expression has been upregulated by 2DG and FA treatment.
It has been found earlier that p53 expression precedes Bax expression. It is well recognized that whether a cell becomes committed to apoptosis partly depends upon the balance between proteins that mediate cell death, e.g., Bax, and proteins that promote cell viability, e.g., Bcl-2 or Bcl-xL [44], and the ratio of Bax to Bcl-2 or Bcl-xL appears to be a critical determinant of a cell’s threshold for undergoing apoptosis [44]. Interestingly, wild-type p53 has been shown to be capable of both downregulating the death suppressor Bcl-2 and upregulating the death promoter Bax, thereby changing the Bcl-2/Bax ratio and disposing to programmed cell death [44]. Bax overexpression has recently been shown to enhance radiation-induced apoptosis, but only in the presence of functional p53 [45]. Exposing thymocytes to ionizing radiation has been reported to increase the levels of Bax [46]. Examination of cell death pathway demonstrated proapoptotic protein Bax activation and caspase cleavage in 2DG-treated lymphoma cells [47]. It has been reported earlier that curcumin potentiates p53 DNA binding which in turn induces Bax expression [48]. From the present results, we deduce that the increased expression of p53 by 2DG and FA also triggered the Bax expression.
Irradiated cells have been shown to be able to increase their survival by reducing or repairing IR-induced damage via activation of stress responsive genes [49]. ATM is a nuclear serine kinase that upon sensing DNA damage activates several signaling pathways to regulate cell cycle, stress, and DNA repair [50]. Cells from ataxia-telangiectasia patients lack ATM and suffer from extreme radiosensitivity and cell cycle anomalies [51]. These cells also display a defect in NF-κB activation that could explain in part their enhanced apoptotic responses to DNA damaging agents [52]. Curcumin, a natural compound that interfere with IkappaB kinase (IKK) activation enhanced radiation-induced apoptosis of prostate PC-3 cancer cells [53]. NF-κB-dependent transcription produces proteins that make cells resistant to apoptosis, stimulates oncogene expression and angiogenesis and stimulates cell proliferation. Indeed, high constitutive NF-κB activity prevents cancerous cells from apoptosis and results in a more aggressive potential for prostate [54] or ORL [55] cancer cell lines. Several studies have explored the impact of NF-κB inhibition on radiosensitivity in various models [56]. ATM is essential for activation of the entire NF-κB pathway by DSBs in both cultured human cells and mouse tissues, including IKK activation, IκB degradation, and induction of NF-κB DNA binding activity [57]. In the present study, we observed that the ATM expression was downregulated by 2DG and FA, which ultimately resulted in the decreased expression of NF-κB.
Deregulation of the cell cycle and apoptosis are frequent occurrences in cancer development. In the present study, increased fraction of cells was observed in G0 phase upon treatment with 2DG+FA compared with 2DG and FA alone. During ionizing radiation treatment, a large fraction of cells appeared in the sub-G0 phase which corresponded to cells undergoing apoptosis, and few fraction of cells were distributed in G2/M and S phase of the cell cycle. To enhance radiosensitization of tumor cells, numerous studies have focused on abrogation of G1- and G2-phase arrests [58]. Furthermore, abrogation of DNA damage-induced S and G2/M checkpoints by antisense inhibition of check point protein (CHK2) has been shown to enhance radiation-induced apoptosis in HEK-293 cells [59]. Giammarioli et al. has earlier reported that 2DG induce cell cycle arrest in G0-G1 phase in metastatic melanoma cells [60]. It has been reported earlier that genistein promotes apoptosis and G2/M cell cycle arrest in prostate cancer cells exposed to radiation [61]. Following curcumin treatment of vascular smooth muscle cells, cell cycle analysis revealed a G0-G1 arrest and a reduction in the percentage of cells in S phase [62]. It has been suggested earlier that FA inhibited vascular smooth muscle cell (VSMC) proliferation by regulating the cell progression from G1 to S phase [63]. Concurrent with earlier reports, accumulation of cells in G0 phase during 2DG and FA treatment before irradiation showed that 2DG and FA are involved in bypass of G2/M checkpoint in the present study. Such a bypass of the G2/M phase checkpoint can lead to inappropriate entry into mitosis and subsequent mitotic catastrophe [64].
In conclusion, it has been observed in the present study that incubation of NCI-H460 cells with 2DG and FA before irradiation triggered many apoptosis-related signaling cascades including p53, Bax, caspase-3, and GADD45. The decreased expression of ATM by 2DG and FA also caused the negative impact on the NF-κB activation. 2DG and FA also decreased the percentage of cells that lies in the G2/M check point there by forcing the cells to undergo apoptosis.
References
Molina JR, Yang P, Cassivi SD, Schild SE, Adjei AA. Non-small cell lung cancer: epidemiology, risk factors, treatment, and survivorship. Mayo Clin Proc. 2008;83(5):584–94.
Spira A, Ettinger DS. Multidisciplinary management of lung cancer. N Engl J Med. 2004;350(4):379–92.
Younes M, Brown RW, Stephenson M, Gondo M, Cagle PT. Over expression of Glut1 and Glut3 in stage I non small cell lung carcinoma is associated with poor survival. Cancer. 1997;80(6):1046–51.
Warburg O. On the origin of cancer cells. Science. 1956;123(3191):309–14.
Weber G. Enzymology of cancer cells. N Engl J Med. 1997;296(9):541–51.
Aft RL, Zhang FW, Gius D. Evaluation of 2-deoxy-d-glucose as a chemotherapeutic agent: mechanism of cell death. Br J Cancer. 2002;87(7):805–12.
Dwarakanath BS, Adhikari JS, Khaitan D, Chandna S, Mathur R, Ravindranath T. Growth inhibition and induction of apoptosis by 2-deoxy-d-glucose in human squamous carcinoma cell lines. Biomedicine. 2005;24:36–47.
Swamy RK, Manickam J, Adhikari JS, Dwarakanath BS. Glycolytic inhibitor, 2-deoxy-d-glucose, does not enhance radiation-induced apoptosis in mouse thymocytes and splenocytes in vitro. Indian J Exp Biol. 2005;43(8):686–92.
Nelson CA, Wang JQ, Leav I, Crane PD. The interaction among glucose transport, hexokinase, and glucose-6-phosphatase with respect to 3 H-2-deoxyglucose retention in murine tumor models. Nucl Med Biol. 1996;23(4):533–41.
Maher JC, Krishan A, Lampidis TJ. Greater cell cycle inhibition and cytotoxicity induced by 2-deoxy-d-glucose in tumor cells treated under hypoxic vs aerobic conditions. Cancer Chemother Pharmacol. 2004;53(2):116–22.
Heminger K, Jain V, Kadakia M, Dwarakanath B, Berberich SJ. Altered gene expression induced by ionizing radiation and glycolytic inhibitor 2-deoxy-glucose in a human glioma cell line: implications for radio sensitization. Cancer Biol Ther. 2006;5(7):815–23.
Coleman MC, Asbury CR, Daniels D, Du J, Aykin-Burns N, Smith BJ, et al. 2-deoxy-d-glucose causes cytotoxicity, oxidative stress, and radiosensitization in pancreatic cancer. Free Radic Biol Med. 2008;44(3):322–31.
Dwarkanath BS, Zolzer F, Chandana S, Bauch T, Adhikari JS, Muller WU, et al. Heterogeneity in 2-deoxy-d-glucose-induced modifications in energetics and radiation responses of human tumor cell lines. Int J Radiat Oncol Biol Phys. 2001;50(4):1051–61.
Lee KW, Lee HJ. The roles of polyphenols in cancer chemoprevention. Biofactors. 2006;26(2):105–21.
Garg AK, Buchholz TA, Aggarwal BB. Chemosensitization and radiosensitization of tumors by plant polyphenols. Antioxid Redox Signal. 2005;7(11–12):1630–47.
Trachootham D, Alexandre J, Huang P. Targeting cancer cells by ROS-mediated mechanisms: a radical therapeutic approach? Nat Rev Drug Discov. 2009;8(7):579–91.
Reddy BV, Prasad NR. 2-deoxy-d-glucose combined with ferulic acid enhances radiation response in non-small cell lung carcinoma cells. Cent Eur J Biol. 2011;6(5):743–55.
Levine AJ. p53, the cellular gatekeeper for growth and division. Cell. 1997;88(3):323–31.
Schmidt-Ullrich RK. Molecular targets in radiation oncology. Oncogene. 2003;22(37):5730–3.
Dent P, Yacoub A, Contessa J, Caron R, Amorino G, Valerie K, et al. Stress and radiation-induced activation of multiple intracellular signaling pathways. Radiat Res. 2003;159(3):283–300.
Iliakis G, Wang Y, Guan J, Wang H. DNA damage checkpoint control in cells exposed to ionizing radiation. Oncogene. 2003;22(37):5834–47.
Karin M, Cao Y, Greten F, Li Z. NF-kB in cancer: from innocent bystander to major culprit. Nat Rev Cancer. 2002;2(4):301–10.
Tsurutani J, Castillo SS, Brognard J, Granville CA, Zhang C, Gills JJ, et al. Tobacco components stimulate Akt-dependent proliferation and NFkappaB-dependent survival in lung cancer cells. Carcinogenesis. 2005;26(7):1182–95.
Leu TH, Maa MC. The molecular mechanisms for the antitumorigenic effect of curcumin. Curr Med Chem Anticancer Agents. 2002;2(3):357–70.
Rupinder SK, Gurpreet AK, Manjeet S. Cell suicide and caspases. Vasc Pharmacol. 2007;46(6):383–93.
Okouoyo S, Herzer K, Ucur E, Mattern J, Krammer PH, Debatin KM, et al. Rescue of death receptor and mitochondrial apoptosis signaling in resistant human NSCLC in vivo. Int J Cancer. 2004;108(4):580–7.
Weigel TL, Lotze MT, Kim PK, Amoscato AA, Luketich JD, Odoux C. Paclitaxel-induced apoptosis in non-small cell lung cancer cell lines is associated with increased caspase-3 activity. J Thorac Cardiovasc Surg. 2000;119(4 pt 1):795–803.
Krug LM, Miller VA, Filippa DA, Venkatraman E, Ng KK, Kris MG. Bcl-2 and bax expression in advanced non-small cell lung cancer: lack of correlation with chemotherapy response or survival in patients treated with docetaxel plus vinorelbine. Lung Cancer. 2003;39(2):139–43.
Porebska I, Wyrodek E, Kosacka M, Adamiak J, Jankowska R, Harłozińska-Szmyrka A. Apoptotic markers p53, Bcl-2 and Bax in primary lung cancer. In Vivo. 2006;20(5):599–604.
Sakata K, Someya M, Matsumoto Y, Hareyama M. Ability to repair DNA double-strand breaks related to cancer susceptibility and radiosensitivity. Radiat Med. 2007;25(9):433–8.
Xing J, Wu X, Vaporciyan AA, Spitz MR, Gu J. Prognostic significance of ataxia-telangiectasia mutated, DNA-dependent protein kinase catalytic subunit, and Ku heterodimeric regulatory complex 86-kD subunit expression in patients with non small cell lung cancer. Cancer. 2008;112(12):2756–64.
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2-ΔΔCt method. Methods. 2001;25(4):402–8.
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ. Protein measurement with the Folin phenol reagent. J Biol Chem. 1951;193(1):265–75.
Li L, Story M, Legerski R. Cellular responses to ionizing radiation damage. Int J Radiat Oncol Biol Phys. 2001;49(4):1157–62.
Zhang XD, Deslandes E, Villedieu M, Poulain L, Duval M, Gauduchon P, et al. Effect of 2-deoxy-d-glucose on various malignant cell lines in vitro. Anticancer Res. 2006;26(5A):3561–6.
Sinthupibulyakit C, Grimes KR, Domann FE, Xu Y, Fang F, Ittarat W, et al. p53 is an important factor for the radiosensitization effect of 2-deoxy-d-glucose. Int J Oncol. 2009;35(3):609–15.
Cao C, Shinohara ET, Subhawong TK, Geng L, Woon Kim K, Albert JM, et al. Radiosensitization of lung cancer by nutlin, an inhibitor of murine double minute 2. Mol Cancer Ther. 2006;5(2):411–7.
Desaint S, Luriau S, Aude JC, Rousselet G, Toledano MB. Mammalian antioxidant defenses are not inducible by H2O2. J Biol Chem. 2004;279(30):31157–63.
El-Deiry WS, Tokino T, Velculescu VE, Levy DB, Parsons R, Trent JM, et al. WAF1, a potential mediator of p53 tumor suppression. Cell. 1993;75(4):817–25.
Brugarolas J, Chandrasekaran C, Gordon JI, Beach D, Jacks T, Hannon GJ. Radiation-induced cell cycle arrest compromised by p21 deficiency. Nature. 1995;377(6549):552–7.
Zou C, Guan Y, Zou C, Wang J, Wang LE, Liebert M, Grossman HB, Wei Q. N-(4-hydroxyphenyl)retinamide (4-HPR) modulates GADD45 expression in radiosensitive bladder cancer cell lines. Cancer Lett. 2002;180(2):131–7.
Sheikh MS, Hollander MC, Fornace Jr AJ. Role of GADD45 in apoptosis. Biochem Pharmacol. 2000;59(1):43–5.
Saha A, Kuzuhara T, Echigo N, Fujii A, Suganuma M, Fujiki H. Apoptosis of human lung cancer cells by curcumin mediated through up-regulation of growth arrest and DNA damage inducible genes 45 and 153. Biol Pharm Bull. 2010;33(8):1291–9.
Haupt S, Berger M, Goldberg Z, Haupt Y. Apoptosis—the p53 network. J Cell Sci. 2003;116(20):4077–85.
Brady HJ, Salomons GS, Bobeldijk RC, Berns AJ. T cells from baxalpha transgenic mice show accelerated apoptosis in response to stimuli but do not show restored DNA damage-induced cell death in the absence of p53. EMBO J. 1996;15(6):1221–30.
Li CR, Zhou Z, Zhu D, Sun YN, Dai JM, Wang SQ. Protective effect of paeoniflorin on irradiation-induced cell damage involved in modulation of reactive oxygen species and the mitogen-activated protein kinases. Int J Biochem Cell Biol. 2007;39(2):426–38.
Zagorodna O, Martin SM, Rutkowski DT, Kuwana T, Spitz DR, Knudson CM. 2-Deoxyglucose-induced toxicity is regulated by Bcl-2 family members and is enhanced by antagonizing Bcl-2 in lymphoma cell lines. Oncogene 2011: Epub 2011 Oct 10.
Choudhuri T, Pal S, Agwarwal ML, Das T, Sa G. Curcumin induces apoptosis in human breast cancer cells through p53-dependent Bax induction. FEBS Lett. 2002;512(1–3):334–40.
Stecca C, Gerber GB. Adaptive response to DNA-damaging agents: a review of potential mechanisms. Biochem Pharmacol. 1998;55(7):941–51.
Rotman G, Shiloh Y. ATM: a mediator of multiple responses to genotoxic stress. Oncogene. 1999;18(45):6135–44.
Lavin M, Shiloh Y. Ataxia-telangiectasia: a multifaceted genetic disorder associated with defective signal transduction. Curr Opin Immunol. 1996;8(4):459–64.
Piret B, Schoonbroodt S, Piette J. The ATM protein is required for sustained activation of NF-kB following DNA damage. Oncogene. 1999;18(13):2261–71.
Chendil D, Ranga RS, Meigooni D, Sathishkumar S, Ahmed MM. Curcumin confers radiosensitizing effect in prostate cancer cell line PC-3. Oncogene. 2004;23(8):1599–607.
Lindholm PF, Bub J, Kaul S, Shidman VB, Kajdacsy-Balla A. The role of constitutive NF-kB activity in PC-3 human prostate cancer cell invasive behavior. Clin Exp Metastasis. 2000;18(6):471–9.
Nakayama H, Ikebe T, Beppu M, Shirasuna K. High expression levels of nuclear factor kappaB, IkappaB kinase alpha and Akt kinase in squamous cell carcinoma of the oral cavity. Cancer. 2001;92(12):3037–44.
Pajonk F, Pajonk K, McBride WH. Apoptosis and radiosensitization of Hodgkin cells by proteasome inhibition. Int J Radiat Oncol Biol Phys. 2000;47(4):1025–32.
Li N, Banin S, Ouyang H, Li GC, Courtois G, Shiloh Y, et al. ATM is required for IkappaB kinase (IKKk) activation in response to DNA double strand breaks. J Biol Chem. 2001;276(12):8898–903.
Higuchi K, Mitsuhashi N, Saitoh J, Maebayashi K, Sakurai H, Akimoto T, et al. Caffeine enhanced radiosensitivity of rat tumor cells with a mutant-type p53 by inducing apoptosis in a p53-independent manner. Cancer Lett. 2000;152(2):157–62.
Yu Q, La Rose JH, Zhang HL, Pommier Y. Antisense inhibition of Chk2/hCds1 expression attenuates DNA damage-induced S and G2 checkpoints and enhances apoptotic activity in HEK-293 cells. FEBS Lett. 2001;505(1):7–12.
Giammarioli AM, Gambardella L, Barbati C, Pietraforte D, Tinari A, Alberton M, et al. Differential effects of the glycolysis inhibitor 2-deoxy-d-glucose on the activity of pro-apoptotic agents in metastatic melanoma cells, and induction of a cytoprotective autophagic response. Int J Cancer 2011: Epub 2011 Sep 12.
Raffoul JJ, Wang Y, Kucuk O, Forman JD, Sarkar FH, Hillman GG. Genistein inhibits radiation-induced activation of NF-kB in prostate cancer cells promoting apoptosis and G2/M cell cycle arrest. BMC Cancer. 2006;6:107.
Chen HW, Huang HC. Effect of curcumin on cell cycle progression and apoptosis in vascular smooth muscle cells. Br J Pharmacol. 1998;124(6):1029–40.
Hou YZ, Yang J, Zhao GR, Yuan YJ. Ferulic acid inhibits vascular smooth muscle cell proliferation induced by angiotensin II. Eur J Pharmacol. 2004;499(1–2):85–90.
Mackey MA, Ianzini F. Enhancement of radiation-induced mitotic catastrophe by moderate hyperthermia. Int J Radiat Biol. 2000;76(2):273–80.
Acknowledgments
The financial assistance in the form of senior research fellowship to Mr. Bandugula Venkata Reddy, by the Indian Council of Medical Research, Government of India, New Delhi, is gratefully acknowledged. We greatly acknowledge Dr G. Prabavathi, radiation safety officer, GVN cancer hospital, Tiruchirapalli, India, for giving us technical assistance in handling irradiation facility.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bandugula, V.R., N., R.P. 2-Deoxy-d-glucose and ferulic acid modulates radiation response signaling in non-small cell lung cancer cells. Tumor Biol. 34, 251–259 (2013). https://doi.org/10.1007/s13277-012-0545-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-012-0545-6