Abstract
Multidrug resistance (MDR) is the main obstacle in breast cancer chemotherapy, a reversal reagent with high reversal effect but low toxicity is the hotpot issue at present. The antidepressant fluoxetine (FLX) is a new highly effective chemosensitizer; however, the possible mechanism of FLX in reversal of MDR is unclear. In this study, the effect of FLX on MDR mediated by apoptosis was researched in resistant/sensitive breast cancer cells, which treated by FLX/adriamycin (ADM)/paclitaxel (PTX) alone or FLX–ADM, FLX–PTX combination. Apoptosis assay demonstrated that FLX combined with ADM enhanced the proportion of apoptosis remarkably in MCF-7/ADM but not MCF-7 cells; however, increased the apoptosis rates in both cells when FLX–PTX combination. Results of apoptosis proteins assay showed a upgrade of p53 and a downgrade of Bcl-2 level by FLX–ADM or FLX–PTX combinations in both cells. Our findings indicated that by synergism with anticancer drugs, FLX modulation of apoptosis via targeting p53 and Bcl-2 expression, FLX reverse the breast cancer cell’s resistance and enhance the chemosensitivity to ADM and PTX.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multidrug resistance (MDR) includes intrinsic and acquired drug resistance. The mechanism of MDR involves many aspects [1–3]. It has been demonstrated that in addition to the overexpression of ABC transporters, other phenotypes, such as altered apoptotic response due to altered p53 expression and function or altered expression of Bcl-2 protein may lead to MDR [4, 5]. p53 is an anticancer gene; normal p53 protein is activated in response to various cell injuries and its alterations result in cell cycle arrest or apoptosis [6]. p53 mutant frequently in tumor cells refrains cells from apoptosis or arrests in a certain period of cell cycle, which develops MDR [7, 8]. Bcl-2 is an oncogene which contributes to tumor occurrence due to inhibition of apoptosis. Overexpression of Bcl-2 contributes to MDR, while reduced its expression sensitizes the tumor cells to apoptosis [9–11]. Furthermore, Bcl-2 protein is able to inhibit the apoptosis induced by p53 in response to genotoxic stress [12]. MDR is a major barrier for breast cancer chemotherapy [13]. The enhancement of chemotherapy sensitiveness is a key to overcome MDR.
Besides MDR in cancer patients, mental disorder as a serious complication of cancer also merits attention. With the increase incidence of breast cancer these years, more and more breast cancer patients suffer from mental stress [14], which result in serious depression. Fluoxetine (FLX), the selective serotonin reuptake inhibitors (SSRI) was used to treat depression effectively in clinical, could improve cancer patients’ immunity, life quality and extend their live time [15–17]. Furthermore, FLX was reported to be a new highly effective chemosensitizer [18]. A drug not only improves the depression of cancer patients but also acts as a chemosensitizer, which made the research is of great interest for cancer therapy. Considering the regulatory role played by FLX on the apoptosis pathway [19, 20], the aim of this work was to study the possible mechanism involved in apoptosis of FLX modulates MDR and enhancement chemotherapy sensitivity in breast cancer cells.
Materials and methods
Chemicals and reagents
Adriamycin (ADM) was purchased from Shenzhen Main Luck Pharmaceuticals Inc (Shenzhen, China). Paclitaxel (PTX) was from Hainan Chuntch Pharmaceutical Co. Ltd. (Haikou China). FLX was obtained from Sigma (St. Louis, MO, USA). Materials for cell culture were from Gibco (Life Technologies, USA). 3-(4,5-Dimethylthiazol-2-yl)-2, 5-diphenyl-tetrazolium bromide (MTT) was purchased from Sijiqing Biological Co. (Hangzhou, China). Rabbit monoclonal anti-p53, Bcl-2 antibodies were purchased from Cell Signaling Technology Co. The second antibody goat anti-rabbit IgG was obtained from Merck.
Cell lines
Human breast cancer cell line resistance MCF-7/ADM was a kind gift from the Cancer Center of Sun Yat-Sen University, Guangzhou, China. Sensitive MCF-7 was passaged in our laboratory. Cells were cultured in DMEM medium, supplemented with 10 % fetal bovine serum (FBS), 100 units/ml penicillin, 100 μg/ml streptomycin at 37 °C in 5 % CO2.
Cytotoxicity assay
The viability of the MCF-7/ADM and MCF-7 cells was quantified by using MTT assay. Cells were seeded into 96-well plates and treated with various doses of FLX (2.5–80 μg/ml in both cell lines)/ADM (2.5–80 μg/ml in MCF-7/ADM cells; 0.125–4 μg/ml in MCF-7 cells)/PTX (0.5–16 μg/ml in both cells) alone or FLX–ADM FLX–PTX (5 μg/ml FLX with various concentrations of ADM or PTX the same as it treated alone) combination for 72 h. Next, 20 μl of 5 mg/ml MTT was stained to each well and incubated at 37 °C for 4 h. Subsequently, the culture medium was removed and 150 μl of dimethyl sulfoxide (DMSO; Sigma) was added and mixed for 10 min. Finally, optical densities (ODs) were measured by the spectrometric absorbance at 570 nm on a microplate reader (Bio-Rad). Results were plotted as percent of survival and concentration–response curves were fitted in order to determine the 50 % effective concentration (IC50).
Flow cytometry (FCM) analysis of apoptotic cells
MCF-7/ADM and MCF-7 cells were seeded into 6-well plates and treated with 5 μg/ml FLX, various concentrations of ADM–PTX alone or FLX–ADM, FLX–PTX combination for 24 h. Cells were collected and washed by PBS twice, stained with Annexin V-FITC and PI (Sigma). Samples were analyzed on an EPICS XL flow cytometry (Beckman Coulter, Bren, CA, USA). Annexin V-FITC positive and PI negative cells were considered as apoptotic cells.
Western blotting assay for p53, Bcl-2 proteins expression
MCF-7/ADM or MCF-7 cells were treated the same as above for 72 h, collected and washed by PBS. The total protein was extracted using cell lysis buffer. The extract (40 μg) was run on SDS-polyacrylamide gel electrophoresis (SDS-PAGE) and electrophoretically blotted onto polyvinylidene difluoride membrane (PVDF; Millipore Corp., Bedford, MA, USA). The blots were blocked with 50 g/l nonfat milk in TBST buffer at room temperature for 2 h, then incubated with antibodies at 4 °C overnight. All antibodies were diluted in TBST according to the manufacturer’s instructions. The blots were washed with TBST buffer five times (5 min each time) at room temperature, then labeled with peroxidase-conjugated secondary antibodies, respectively, at room temperature for 2 h. Protein bands were detected using an enhanced chemiluminescence (ECL) detection kit (Pierce).
Statistical analysis
Data were processed with the SPSS 13.0 for Windows software package. The results were presented as means ± standard deviation (SD). Experiments were done three times with different passages of cells. Statistical differences between the two groups were calculated using unpaired Student’s t-test; and the differences among more than two groups were tested by one-way ANOVA. Results were considered to be statistically significant at P < 0.05.
Results
Proliferation inhibited by drugs
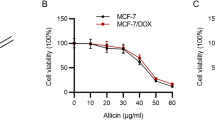
To assess the level of MCF-7/ADM resistance and to evaluate the ability of FLX to modulate its reversal, we studied responses of these cells to treatments by ADM or PTX alone or with FLX. Cells were exposed to FLX alone over the concentration range of 2.5–80 μg/ml. Inhibition rates of FLX in MCF-7 and MCF-7/ADM were less than 10 % (5.43 ± 2.12 % and 7.52 ± 1.24 %, respectively) at a concentration of 5 μg/ml, so we chose 5 μg/ml as the combination concentration. The concentration–survival curves (Fig. 1) showed that FLX enhancement the inhibition rate of ADM and PTX in the two cell lines, especially at the low concentrations. Concretely, with ADM less than 20 μg/ml in MCF-7/ADM cells and 2 μg/ml in MCF-7 cells, PTX under 4 μg/ml in the two cell lines, combination with FLX showed a significantly increase in the proliferation inhibit rates.
Concentration–survival curves, MTT analysis for cells vitality. The cells were treated with varying concentrations of adriamycin (ADM)/paclitaxel (PTX) alone or in the presence of 5 μg/ml fluoxetine (FLX). a Survival rate of MCF-7/ADM cells treated by ADM alone or with FLX (the concentration of ADM range from 2.5 to 80 μg/ml). b Survival rate of MCF-7 cells treated by ADM alone or with FLX (the concentration of ADM in the range of 0.125–4 μg/ml). c Survival rate of MCF-7/ADM and MCF-7 cells treated by PTX alone or with FLX (the concentration of PTX changed from 0.5 to 16 μg/ml in the two cell lines)
The IC50 value and the reversal fold (RF) of ADM/PTX in the two cells are shown in Table 1. The data indicated that MCF-7/ADM cells were 26-fold more resistant to ADM than MCF-7 cells. The ADM combination treatment with FLX (Fig. 1a) generated a statistically significant 5.03-fold reduction in IC50, but had slight effect on MCF-7 (Fig. 1b). The FLX–PTX combination had statistical differences of reversal effect on the two cell lines (Fig. 1c).
Apoptosis enhancement induced by FLX combination
We next investigated whether FLX or FLX–ADM, FLX–PTX decreases cell viability through the induction of apoptosis by flow cytometry.
The results shown in Fig. 2 demonstrated that FLX alone had little effect on cell apoptosis (3.17 ± 0.70 % and 3.84 ± 0.31 %, respectively), while the apoptosis rate significantly increased with FLX–ADM or FLX–PTX combination. In MCF-7/ADM cells, apoptotic proportion increased from 5.63 ± 0.07 % to 19.15 ± 3.35 % when treated by 5 μg/ml ADM with the presence of 5 μg/ml FLX; from 35.53 ± 1.65 % to 49.00 ± 6.05 % when treated by 20 μg/ml ADM and FLX combination; increased 5.73 % and 21.90 %, respectively, by treatment with 1 μg/ml or 4 μg/ml PTX and FLX combination (Fig. 2a). A similar increase was also observed in MCF-7 cells (Fig. 2b).
Results of early apoptosis rate. Cells were treated by ADM or PTX alone at two different concentrations. According to the results of MTT analysis, we chose 1, 4 μg/ml as the low (PTX(l)), high (PTX (h)) combination concentration of PTX in MCF-7/ADM and MCF-7 cells; 5, 20 μg/ml as the low (ADM(l)), high (ADM (h)) concentration of ADM in MCF-7/ADM cells, 0.5, 2 μg/ml as the low (ADM(l)), high (ADM (h)) concentration of ADM in MCF-7. In order to assess the effect of a combination of FLX, cells were exposed to an equivalence concentration of ADM or PTX in addition with 5 μg/ml of FLX. a and c Apoptosis rate of MCF-7/ADM cells resulted from various concentrations of ADM, PTX alone or with FLX. b and d Apoptosis rate of MCF-7 cells resulted from various concentrations of ADM, PTX alone or with FLX. (**P < 0.01,*P < 0.05 versus the control cells with ADM or PTX treatment alone; ##P < 0.01, #P < 0.05 versus untreated control group)
Levels of p53, Bcl-2 proteins expression modulated by FLX
To determine whether FLX causes an alteration in p53, Bcl-2 proteins expression at the translation level, we evaluated the effect of ADM or PTX with the absence or presence of FLX on the level of p53, Bcl-2 proteins expression by Western blot (Fig. 3). Compared with the control group, FLX (5 μg/ml) alone just increased p53 levels in MCF-7 cells, but had no effect on the expression of Bcl-2 protein.
Effect of FLX on apoptotic proteins activation. a, b Expression of p53, bcl-2 proteins in MCF-7/ADM and MCF-7 cells. (i), (ii) Relative p53, bcl-2 expression in MCF-7/ADM and MCF-7 cells, respectively. Drugs treatment manner were the same as apoptosis assay. Western blot for β-actin was used as an internal control. Relative proteins levels normalized against β-actin expression in MCF-7/ADM cells and MCF-7 cells. The ratios of p53, bcl-2 to β-actin are shown on the y-axis, respectively. (**P < 0.01, *P < 0.05 versus the control cells with ADM or PTX treatment alone; ##P < 0.01, #P < 0.05 versus untreated control group)
As shown in Fig. 3a, in MCF-7/ADM cells, treatment with ADM alone up-regulated the expression of p53 in a concentration-dependent manner, regretfully that FLX-ADM just showed a tendency of inducing p53 but did not reach statistical significance. Much better results were obtained by treatment with PTX alone or FLX–PTX combination (Fig. 3a(i)). Bcl-2 level induced no change by treatment with ADM alone but decreased by FLX–ADM combination. Interestingly, Bcl-2 level rose to more than 2-fold when treated by PTX alone, but decreased sharply to less than 50 % compared with the control group when treated by FLX–PTX combination (Fig. 3a(ii)).
Next, we examined whether FLX regulates the expression of p53, Bcl-2 in MCF-7 cells. Similar results were obtained by treatment using ADM–PTX with the absence or presence of FLX, but the result not so pronounced as it was in MCF-7/ADM cells (Fig. 3b).
Discussion
MDR reversal agents come to the third generation at present, from first generation such as calcium ion channels blocker Verapamil, PKC inhibitor, Tamoxifen to second generation (Dexverapamil, Dexniguldipine, PSC833) and to third generation such as Tetrandrine [3, 21]. Although so many reversal agents have been certified to reverse MDR, clinical application is limited due to serious adverse drug reactions and toxicity. Therefore, research and development on new MDR reversal agents is a hotspot in cancer pharmacology [22]. In this study, we evaluated the efficacy of FLX as a potent chemosensitizer to overcome the MDR of MCF-7/ADM cells, and the possible molecular mechanism involved in FLX–ADM, FLX–PTX-induced apoptosis in MCF-7 and MCF-7/ADM cells.
There is dispute on the relationship between FLX and cancer [23, 24]. On one hand, a clinical dose of FLX was reported to accelerate the growth of mammary tumors in rodents, whereas recent studies revealed that FLX inhibits proliferation of several cancer cell lines, including MCF-7 cells. Our data tended to support the latter (Table 1, tier 2). In 2004, FLX was first reported to be a new highly effective chemosensitizer by slowing-down drug efflux, increasing drug accumulation in both inherent and acquired MDR cells. The combination treatment (FLX–ADM) restrained tumor progression in vivo. Therefore, FLX was considered as the fourth-generation chemosensitizer because it reversed MDR at a low safe dose [18, 25, 26]. In our research, FLX when used alone had little effect on cytotoxicity, but had remarkable effects when combined with other drugs — FLX–ADM and FLX–PTX combinations — especially in resistance cells (Fig. 1). In a previous study, stealth liposome coencapsulating ADM and FLX (ADM–FLX-SL) was reported to circumvent MDR. Synergism was demonstrated at specific ADM/FLX ratios of between 0.09 and 0.5 (molar ratio) in MCF-7 cells, but across all drug ratios in MCF-7/ADM cells. Pharmacokinetic studies also revealed that ADM–FLX-SL effectively prolonged drug-circulation time and reduced tissue biodistribution [27]. Synergism with chemotherapy drugs revealed a reversal and sensitization effect on resistance and sensitive cell lines, respectively (Table 1). However, sensitization to PTX was less than that to ADM in MCF-7/ADM cells, thereby showing a cross-resistance to PTX.
FLX alone can inhibit the growth of many cancer cell lines by inducing apoptosis such as rat glioma cell lines, human neuroblastoma cell lines and Burkitt lymphoma cells [28–30]. Our data indicated that 24 h after FLX treatment alone (at 5 μg/ml concentration) had slight effect on apoptosis, while treatment with FLX–ADM or FLX–PTX combination induced apoptosis in a concentration-dependent manner in both cells (Fig. 2). Interestingly, a considerable intensity apoptosis effect was obtained in MCF-7 cells treated by the same concentration of PTX alone or with FLX. It thus appears that MCF-7 cells had more sensitivity than MCF-7/ADM to PTX at the same concentrations. However, the sensitization effect was much notable in MCF-7/ADM cells by treatment with FLX–ADM compared with MCF-7 cells, exerting a reversal effect of FLX on resistance cells.
Apoptosis is triggered via the intrinsic pathway inasmuch as caspases are activated: Bax was oligomerized and cytochrome c released. FLX induced cell apoptosis through inhibition of ERK1/2 kinases, followed by changes of gene expression of cell cycle regulating genes, anti-apoptosis Bcl-2 proteins family [19, 20, 31–33]. According to Western blot, FLX alone hardly affected the protein expression except for inducing p53 expression in MCF-7 cells. We speculated that it might be associated with the concentrations we used. At the concentration of 5 μg/ml, FLX just improved the influence of anticancer drugs. In the protein level, FLX activated the p53 protein and suppressed Bcl-2 protein expression, leading to the sensitization of cells to anticancer agents.
Interestingly, although p53 and Bcl-2 expression trended to unification, a difference existed yet. Protein assay results revealed that FLX–PTX was more sensitized than FLX–ADM in inducing p53 expression (Fig. 3a(i), b(i)), but had the opposite effect in reducing Bcl-2 (Fig. 3a(ii), b(ii)). We conjectured that it is related to survivin, that is, survivin’s expression negative correlation with PTX chemotherapy sensitivity, as well as p53 [34]. However, it is unclear whether FLX inhibits the expression of survivin through an unknown pathway. The expression of p53 and Bcl-2 is a positive correlation [35], which led Bcl-2 to decrease retardation in FLX–PTX groups.
A chemosensitizer is expected to improve the effect of anti-cancer drugs on drug-resistant or drug-sensitive cells, while at the same time have no effect on cell viability. In our research, we also validated that FLX acts as a chemosensitizer and that FLX–ADM or FLX–PTX combination increased cytotoxicity; in addition, we revealed synergism with chemotherapy drugs in MCF-7/ADM cells, in agreement with the studies mentioned above. However, the sensitization mechanism is a little different. In the previous studies, FLX increased drug accumulation as well as prevented its excretion to increase the intracellular concentration so as to improve the effect of anticancer drugs [18, 25–27]. The reason was that FLX is a substrate and a partial inhibitor of ABCB1 (P-gp) [36]. In this study, we conjectured that by inhibiting P-gp to stop drug effusing from intracellular, to increase the intracellular concentration of anticancer drugs, FLX increased apoptotic cell death associated with changes in levels of apoptosis-related proteins p53 and Bcl-2 after 72 h incubation of MCF-7/ADM and MCF-7 cells. We thus confirmed that by synergism with anticancer drugs ADM and PTX, FLX modulated MDR and enhanced chemotherapy sensitivity in breast cancer cells.
In addition, FLX has a very wide safety range; serious adverse events in humans may occur only when FLX is administered at doses 75 times of the therapeutic doses [37]. In this work, FLX was used at a low concentration, thus evoking less cytotoxicity. Based on the results above, we suggest that FLX can be used in combination treatment for resistant cancer patients with depression and for sensitive cancer patients; however, the dose of anticancer drugs need to be modulated.
References
Baguley BC. Multiple drug resistance mechanisms in cancer. Mol Biotechnol. 2010;46:308–16.
Stavrovskaya AA. Cellular mechanisms of multidrug resistance of tumor cells. Biochemistry (Mosc). 2000;65:95–106.
O'Connor R. A review of mechanisms of circumvention and modulation of chemotherapeutic drug resistance. Curr Cancer Drug Targets. 2009;9:273–80.
Borst P, Jonkers J, Rottenberg S. What makes tumors multidrug resistant? Cell Cycle. 2007;6(22):2782–7.
Shi X, Liu S, Kleeff J, Friess H, Buchler MW. Acquired resistance of pancreatic cancer cells towards 5-fluorouracil and gemcitabine is associated with altered expression of apoptosis-regulating genes. Oncology. 2002;62:354–62.
Rathinasamy K, Jindal B, Asthana J, Singh P, Balaji PV, Panda D. Griseofulvin stabilizes microtubule dynamics, activates p53 and inhibits the proliferation of MCF-7 cells synergistically with vinblastine. BMC Cancer. 2010;10:213.
Saha MN, Micallef J, Qiu L, Chang H. Pharmacological activation of the p53 pathway in haematological malignancies. J Clin Pathol. 2010;63(3):204–9.
Takeba Y, Sekine S, Kumai T, Matsumoto N, Nakaya S, Tsuzuki Y, et al. Irinotecan-induced apoptosis is inhibited by increased P-glycoprotein expression and decreased p53 in human hepatocellular carcinoma cells. Biol Pharm Bull. 2007;30(8):1400–6.
Desoise B. Anticancer drug resistance and inhibition of apoptosis. Anticancer Res. 1994;14:2291–4.
Bush JA, Li G. Cancer chemoresistance: the relationship between P53 and multidrug transporters. Int J Cancer. 2002;98:323–30.
Pommier Y, Sordet O, Antony S, Hayward RL, Kohn KW. Apoptosis defects and chemotherapy resistance: molecular interaction maps and networks. Oncogene. 2004;23(16):2934–49.
Leonard GD, Fojo T, Bates SE. The role of ABC transporters in clinical practice. Oncologist. 2003;8:411–24.
Kuo MT. Roles of multidrug resistance genes in breast cancer chemoresistance. Adv Exp Med Biol. 2007;608:23–30.
Massie MJ, Holland JC. Depression and the cancer patient. J Clin Psychiatry. 1990;51:12–7.
Cheer SM, Goa KL. Fluoxetine. A review of its therapeutic potential in the treatment of depression with physical illness. Drugs. 2001;61:81–110.
Razavi D, Allilaire JF, Smith M, Salimpour A, Verra M, Desclaux B, et al. The effect of fluoxetine on anxiety and depression symptoms in cancer patients. Acta Psychiatr Scand. 1996;94(3):205–10.
Navari RM, Brenner MC, Wilson MN. Treatment of depressive symptoms in patients with early stage breast cancer undergoing adjuvant therapy. Breast Cancer Res Treat. 2008;112:197–201.
Peer D, Dekel Y, Melikhov D, Margalit R. Fluoxetine inhibits multidrug resistance extrusion pumps and enhances responses to chemotherapy in syngeneic and in human xenograft mouse tumor models. Cancer Res. 2004;64:7562–9.
Choi MR, Oh DH, Kim SH, Yang BH, Lee JS, Choi J, et al. Fluoxetine up-regulates bcl-xL expression in rat c6 glioma cells. Psychiatry Investig. 2011;8:161–8.
Fumagalli F, Molteni R, Calabrese F, Frasca A, Racagni G, Riva MA. Chronic fluoxetine administration inhibits extracellular signal-regulated kinase 1/2 phosphorylation in rat brain. J Neurochem. 2005;93:1551–60.
Leonard GD, Polgar O, Bates SE. ABC transporters and inhibitors: new targets, new agents. Curr Opin Invest Drugs. 2002;3:1652–9.
Kars MD, Işeri OD, Gunduz U, Molnar J. Reversal of multidrug resistance by synthetic and natural compounds in drug-resistant MCF-7 cell lines. Chemotherapy. 2008;54:194–200.
Steingart AB, Cotterchio M. Do antidepressants cause, promote, or inhibit cancers? J Clin Epidemiol. 1995;48:1407–12.
Freire-Garabal M, Núñez MJ, Pereiro D, Riveiro P, Losada C, Fernández-Rial JC, et al. Effects of fluoxetine on the development of lung metastases induced by operative stress in rats. Life Sci. 1998;63:31–8.
Peer D, Margalit R. Fluoxetine and reversal of multidrug resistance. Cancer Lett. 2006;237:180–7.
Argov M, Kashi R, Peer D, Margalit R. Treatment of resistant human colon cancer xenograftsby a fluoxetine–doxorubicin combination enhances therapeutic responses comparable to an aggressive bevacizumab regimen. Cancer Lett. 2009;274:118–25.
Ong JC, Sun F, Chan E. Development of stealth liposome coencapsulating doxorubicin and fluoxetine. J Liposome Res. 2011;21(4):261–71.
Serafeim A, Holder MJ, Grafton G, Chamba A, Drayson MT, Luong QT, et al. Selective serotonin reuptake inhibitors directly signal for apoptosis in biopsy-like Burkitt lymphoma cells. Blood. 2003;101(8):3212–9.
Cloonan SM, Williams DC. The antidepressants maprotiline and fluoxetine induce Type II autophagic cell death in drug-resistant Burkitt’s lymphoma. Int J Cancer. 2011;128:1712–23.
Hait WN. JM Yang. The individualization of cancer therapy: the unexpected role of p53. Trans Am Clin Climatol Assoc. 2006;117:85–101.
Lee CS, Kim YJ, Jang ER, Kim W, Myung SC. Fluoxetine induces apoptosis in ovarian carcinoma cell line OVCAR-3 through reactive oxygen species-dependent activation of nuclearfactor-kappaB. Basic Clin Pharmacol Toxicol. 2010;106:446–53.
Djordjevic J, Djordjevic A, Adzic M, Elaković I, Matić G, Radojcic MB. Fluoxetine affects antioxidant system and promotes apoptotic signaling in Wistar rat liver. Eur J Pharmacol. 2011;659:61–6.
Frick LR, Rapanelli M, Arcos ML, Cremaschi GA, Genaro AM. Oral administration of fluoxetine alters the proliferation/apoptosis balance of lymphoma cells and up-regulates T cell immunity in tumor-bearing mice. Eur J Pharmacol. 2011;659:265–72.
Liu F, Xie ZH, Cai GP, Jiang YY. The effect of survivin on multidrug resistance mediated by P-glycoprotein in MCF-7 and its adriamycin resistant cells. Biol Pharm Bull. 2007;30(12):2279–83.
Cen J, Qi Y, Tao YF, Deng Y, Fang WR, Li YM, et al. HZ08, A great regulator to reverse multidrug resistance via cycle arrest and apoptosis sensitization in MCF-7/ADM. Eur J Pharmacol. 2010;647:21–30.
Hegedus T, Orfi L, Seprodi A, Varadi A, Sarkadi B, Keri G. Interaction of tyrosine kinase inhibitors with the human multidrug transporter proteins, MDR1 and MRP1. Biochim Biophys Acta. 2002;1587:318–25.
Barbey JT, Roose SP. SSRI safety in over dose. J Clin Psychiatry. 1998;59:42–8.
Acknowledgement
This project sponsored by the Scientific Research Foundation for the Returned Overseas Chinese Scholars, State Education Ministry (No. [2010] 609).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhou, T., Duan, J., Wang, Y. et al. Fluoxetine synergys with anticancer drugs to overcome multidrug resistance in breast cancer cells. Tumor Biol. 33, 1299–1306 (2012). https://doi.org/10.1007/s13277-012-0377-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-012-0377-4