Abstract
Objectives
MUC16 (mucin 16, also known as CA-125, cancer antigen 125, carcinoma antigen 125, or carbohydrate antigen 125) has been predicted as tumor biomarker for therapy. We determined to investigate effects and regulatory mechanism of MUC16 on cervical tumorigenesis.
Methods
Expression levels of MUC16 in cervical cancer cell lines was analyzed via qRT-PCR (quantitative real-time polymerase chain reaction). Knockdown of MUC16 was conducted via shRNA (Short hairpin RNA) transfection. MTT and colony formation assays were used to investigate effect of MUC16 on cell proliferation. Wound healing assay was utilized to detect migration and transwell assay to detect invasion. The underlying mechanism was demonstrated via western blot analysis.
Results
MUC16 was elevated in cervical cancer cell lines. MUC16 knockdown inhibited cell proliferation, invasion and migration. Gain- and loss-of functional assays revealed that over-expression of MUC16 activated Janus Kinase 2 (JAK2)/signal transducer and activator of transcription 3 (STAT3) via phosphorylation, thus facilitating cyclooxygenase-2 (COX-2) expression, while knockdown of MUC16 demonstrated the reverse effect on JAK2/STAT3 activation and COX-2 expression. Moreover, inhibition of JAK2/STAT3 attenuated the regulation of MUC16 on COX-2.
Conclusions
MUC16 enhanced proliferation and invasion of cervical cancer cells via JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression, suggesting the potential therapeutic target ability of MUC16 to treat cervical cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cervical cancer is one of the most common gynecological malignancies (Khalil et al. 2015), which is accounting for 10% of all gynecological cancers and about 5% of all tumors (Hovland et al. 2010). Although the recent therapeutical treatment for cervical cancer, including radiotherapy, chemotherapy, or surgery (Tzafetas et al. 2018), has been progressed tremendously in the last several decades, the 5-year survival for cervical cancer patients has not improved due to distant metastasis (Burki 2018). Therefore, it is of great clinical significance to elucidate the underlying mechanism about cervical tumorigenesis, as well as discover therapeutic target to regulate cervical cancer progression.
MUC16 (mucin 16, also known as CA-125, cancer antigen 125, carcinoma antigen 125, or carbohydrate antigen 125) has been characterized as tumor biomarker of epithelial ovarian cancer (Sturgeon et al. 2010). Additional, MUC16 is found to be up-regulated in pancreatic ductal adenocarcinoma (Shimizu et al. 2012) and ovarian cancer (Clarke et al. 2011). High expression of MUC16 could promote invasion ability of tumor cells (Shimizu et al. 2012) via activation of mTOR and c-MYC (Shukla et al. 2015). Study has shown that MUC16 binds with Janus Kinase 2 (JAK2) to activates JAK2/STAT3 (signal transducer and activator of transcription 3) signaling pathway, promotes cell proliferation and inhibits apoptosis in breast cancer (Lakshmanan et al. 2012). Recently, research has shown that up-regulation of MUC16 in cervical cancer might be useful marker for prognosis of cervical cancer (Porika et al. 2010). However, the molecular mechanism of MUC16 in the progression process of cervical cancer has not been reported.
Cyclooxygenase (COX), with two isoforms (COX-1 and COX-2), is the key enzyme in the conversion of arachidonic acid (Wang et al. 2017). Recent studies have shown that COX-2 is highly expressed in many human malignant tumors, and might have an impact on apoptosis, angiogenesis and immune suppression, as well as cancer progression (Feng and Wang 2006; Kanaoka et al. 2007; Takaoka et al. 2006). Recently, COX-2 was found to be an angiogenic factor in uterine cervical cancer (Fujimoto et al. 2006), and activation of JAK2/STAT3 signaling pathway could promote expression of COX-2 (Gao et al. 2009). Therefore, we evaluated the hypothesis that MUC16, together with the downstream regulators JAK2/STAT3/COX-2, may be involved in regulation of cervical cancer progression.
We first detect the impact of MUC16 on tumor proliferation, migration and invasion of cervical cancer, and then explore the underlying mechanism. The meaning results would shed light on development of novel therapeutics to cervical cancer.
Materials and methods
Cell culture and transfection
Cervical cancer cell lines (Caski, HeLa and SiHa) and human cervical mucosa epithelial cell line H8, purchased from CHI Scientific (Maynard, MA, USA), were cultured in Dulbecco modified Eagle medium (DMEM; Lonza, Basel, Switzerland) supplemented with 10% fetal bovine serum (FBS, Gibco, MA, USA) with additional streptomycin (100 μg/mL) and penicillin (100 U/mL). 37 °C constant temperature incubator with 5% CO2 was utilized to incubating cells.
For the over-expression of MUC16, full-length of MUC16 was amplified and cloned into pcDNA3.1 (Invitrogen, Carlsbad, CA, USA). SiHa cells were seeded at 4 × 105 cells per well in 12-well plates and then transfected with pcDNA3.1-MUC16 or the empty control (pcDNA3.1-NC) via Lipofectamine 2000 (Invitrogen). For the knock down of MUC16, shRNAs (1#: 5′-ACAGCAGCATCAAGAGTTATT-3′ and 2#: 5′-GCCATCCACTTCAAAGTATTC-3′) as well as the negative control (5′-GGAATCTCATTCGATGCATAC-3′) were synthesized by GenePharm (Shanghai, China) and transfected to HeLa cells via Lipofectamine 2000. The inhibitors of STAT3, C188-9, was added at a concentration of 5 µM to SiHa cells transfected with pcDNA3.1-MUC16 for 24 h before the subsequently experiments.
Cell proliferation
HeLa cells with different treatment were seeded in 96-well plates at a density of 1 × 103 cells per well, and cultured as before overnight. The cell viabilities were determined via MTT assay and calculated via detection of absorbance at 450 nm. For the colony formation assay, 1 × 103 HeLa cells per well were plated in six-well plate, and cultured as before for 14 days. The colonies were stained by 1% crystal violet-2% ethanol suspended in PBS (Beyotime, Shanghai, China), counted and photographed under light microscope (Olympus, Tokyo, Japan).
Wound healing
HeLa cells at a concentration of 5 × 105/well were seeded in six-well plate. 200 μL sterile pipette tip was used to generate linear scratch wounds. The plate was then washed with PBS to remove debris or suspended cell, and the cells were cultured as before. After 24 h, the wounds were imaged under the microscope and calculated the distance.
Transwell
HeLa cells at a concentration of 2 × 104/well were suspended in 200 μL serum-free DMEM medium, and plated in the upper chamber of well (Corning, Tewksbury, MA, USA) with 0.1 mL 50 μg/mL Matrigel-coated membrane (BD Biosciences, Bedford, MA, USA). 400 μL DMEM with 10% FBS was added to the lower chamber. 24 h later, stained the invasive cells at the bottom of chambers with 1% crystal violet for 30 min. The stained cells were imaged and counted under microscope (Olympus).
qRT-PCR
Total RNAs from cervical cancer cell lines were isolated with Trizol (Invitrogen). RNAs were then reverse-transcribed by PrimeScript RT Reagent (Takara, Shiga, Japan). qRT-PCR was conducted with SYBR Green Master (Roche, Mannheim, Germany) on ViiA 7 (Applied Biosystems, Austin, TX, USA). GAPDH was used as endogenous control for normalizing mRNA level. The primer sequences were showed as follows:
Primers sequence
ID | Sequence (5′–3′) |
|---|---|
GAPDH F | ACCACAGTCCATGCCATCAC |
GAPDH R | TCCACCACCCTGTTGCTGTA |
MUC16 F | GCCTCTACCTTAACGGTTACAATGAA |
MUC16 R | GGTACCCCATGGCTGTTGTG |
Western blot
30 µg proteins extracted from cultured cervical cancer cells were separated by SDS-PAGE, and then electro-transferred onto PVDF membrane. After blocking with 5% BSA, the membrane was incubated overnight with primary antibody: anti-MUC16 antibody (1:1500, Abcam, Cambridge, MA, USA), JAK2 and p-JAK2 (1:2000, Abcam), STAT3 and p-STAT3 (1:2500, Abcam, COX-2 and GAPDH (1:3000, Abcam) at 4 °C. Following incubation with HRP labeled secondary antibody (1:5000; Abcam), the immunoreactivities were detected by enhanced chemiluminescence (KeyGen, Nanjin, China).
Statistical analysis
All results are expressed as mean ± SEM. By the means of GraphPad Prism software (GraphPad Prism Software Inc., San Diego, USA) and one-way analysis of variance (ANOVA), we determined the statistical analyses. P < 0.05 was considered as a mark of statistically significant.
Results
MUC16 was up-regulated in cervical cancer cell lines
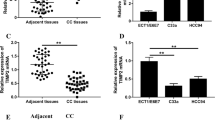
Three available cervical cancer cell lines (Caski, HeLa and SiHa), as well as human cervical mucosa epithelial cell line H8, were used to detect the dysregulation of MUC16 in cervical cancer. qRT-PCR analysis showed that both of mRNA (Fig. 1a) and protein (Fig. 1b) expression of MUC16 were elevated in cervical cancer cell lines compared to H8, indicating that MUC16 may be involved in the regulation of cervical cancer cell progression. Meanwhile, HeLa cells or SiHa with the highest or lowest expression of MUC16 was used for the loss- or gain-of function assays, respectively.
MUC16 was up-regulated in cervical cancer cell lines. a mRNA expression of MUC16 in cervical cancer cell lines (Caski, HeLa and SiHa) and human cervical mucosa epithelial cell line H8 detected by qRT-PCR. Double asterisk represents cervical cancer cell lines vs. H8, P < 0.01. b Protein expression of MUC16 in cervical cancer cell lines (Caski, HeLa and SiHa) and human cervical mucosa epithelial cell line H8 detected by western blot. Double asterisk represents cervical cancer cell lines vs. H8, P < 0.01
MUC16 knockdown inhibited cervical cancer cell proliferation, migration and invasion
To identify the functional role of MUC16 in cervical cancer, loss-of functional assays via transfection of shRNAs target MUC16 (shMUC16#1 and shMUC16#2) in HeLa cells were conducted. qRT-PCR (Fig. 2a) and western blot (Fig. 2b) analysis confirmed the transfection efficiency of shMUC16#1 and shMUC16#2. ShMUC16#2 with the lower expression of MUC16 was used for the subsequent experiments and considered as shMUC16. Moreover, MTT assay showed that MUC16 knockdown via shMUC16 decreased cell viability (Fig. 2c). shMUC16 also inhibited cell proliferation of HeLa cells as demonstrated by colony formation assay in Fig. 2d. Mechanically, proteins involved in DNA replication, PCNA (proliferating cell nuclear antigen) and MCM-2 (Minichromosome Maintenance Complex Component 2) were down-regulated by shMUC16 (Fig. 2e). Proteins involved in cell apoptosis, Bcl-2 (B cell lymphoma 2) was down-regulated while cleaved caspase-3 was up-regulated in HeLa cells transfected with shMUC16. These results revealed that MUC16 knockdown inhibited cervical cancer cell viability and proliferation, while induced cell apoptosis. In addition to the anti-proliferation ability of MUC16 knockdown on cervical cancer cells, MUC16 knockdown also not only suppressed the cell migration (Fig. 3a) but also cell invasion (Fig. 3b) of HeLa cells, indicating the anti-tumorigenicity role of MUC16 knockdown on cervical cancer.
MUC16 knockdown inhibited cervical cancer cell proliferation. a Transfection efficiency of shRNAs target MUC16 (shMUC16#1 and shMUC16#2) in HeLa cells detected by qRT-PCR. Double asterisk represents shMUC16#1 or shMUC16#2 vs. shNC, P < 0.01. b Transfection efficiency of shRNAs target MUC16 (shMUC16#1 and shMUC16#2) in HeLa cells detected by western blot. Double asterisk represents shMUC16#1 or shMUC16#2 vs. shNC, P < 0.01. c MUC16 knockdown via shMUC16 decreased cell viability detected by MTT assay. Double asterisk represents shMUC16 vs. shNC, P < 0.01. d MUC16 knockdown via shMUC16 decreased cell proliferation detected by colony formation assay. Double asterisk represents shMUC16 vs. shNC, P < 0.01. e MUC16 knockdown via shMUC16 decreased PCNA, MCM-2 and Bcl-2, while increased cleaved caspase-3 detected by western blot. Double asterisk represents shMUC16 vs. shNC, P < 0.01
MUC16 knockdown inhibited cervical cancer cell migration and invasion. a MUC16 knockdown via shMUC16 inhibited cell migration detected by wound healing assay. Double asterisk represents shMUC16 vs. shNC, P < 0.01. b MUC16 knockdown via shMUC16 inhibited cell invasion detected by transwell assay. Double asterisk represents shMUC16 vs. shNC, P < 0.01
MUC16 down-regulated JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression
In order to uncover the underlying mechanism involved in the regulation of MUC16 on cervical cancer, gain-of functional assay was conducted via transfection of pcDNA 3.1-MUC16 in SiHa cells for ectopically over-expression of MUC16. qRT-PCR (Fig. 4a) and western blot (Fig. 4b) analysis also confirmed the transfection efficiency of pcDNA 3.1-MUC16, as demonstrated by up-regulation of MUC16 compared to pcDNA3.1-NC. Moreover, although MUC16 knockdown did not affect the expression of JAK2 and STAT3, it significantly decreased p-JAK2/JAK2 and p-STAT3/STAT3 ratio (Fig. 4c), indicating the inactivation of JAK2/STAT3 signaling pathway by MUC16 knockdown. However, ectopically over-expression of MUC16 reversed the effect of shMUC16 on JAK2/STAT3 signaling pathway, as demonstrated by increase of p-JAK2/JAK2 and p-STAT3/STAT3 ratio (Fig. 4d). Moreover, the downstream of JAK2/STAT3 signaling pathway, COX-2, was up-regulated by over-expression of MUC16 (Fig. 4d) while down-regulated by sh-MUC16 (Fig. 4c), revealing that MUC16 down-regulated JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression in cervical cancer cells.
MUC16 down-regulated JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression. a Transfection efficiency of pcDNA 3.1-MUC16 in SiHa cells detected by qRT-PCR. Double asterisk represents pcDNA 3.1-MUC16 vs. pcDNA 3.1-NC, P < 0.01. b Transfection efficiency of pcDNA 3.1-MUC16 in SiHa cells detected by western blot. Double asterisk represents pcDNA 3.1-MUC16 vs. pcDNA 3.1-NC, P < 0.01. c MUC16 knockdown via shMUC16 decreased the expression of p-JAK2, p-STAT3 and COX-2. Asterisk, Double asterisk represents shMUC16 vs. shNC, P < 0.05, P < 0.01. d Over-expression of MUC16 via pcDNA 3.1-MUC16 increased the expression of p-JAK2, p-STAT3 and COX-2. Asterisk, double asterisk represents pcDNA 3.1-MUC16 vs. pcDNA 3.1-NC, P < 0.05, P < 0.01
Suppression of JAK2/STAT3 pathway attenuated the promotion ability of MUC16 on COX-2
SiHa cells were treated with inhibitors of STAT3 (C188-9) and transfected with pcDNA3.1-MUC16 to detect whether the regulation ability of MUC16 on COX-2 was mediated by JAK2/STAT3 signaling pathway. Western blot analysis revealed that treatment with C188-9 alone decreased expression of p-STAT3 while did not affect STAT3, thus decreasing p-STAT3/STAT3 ratio (Fig. 5). Moreover, treatment with C188-9 alone also decreased expression of COX-2 (Fig. 5). Treatment with C188-9 increased expression of p-STAT3 in SiHa cells transfected with pcDNA3.1-MUC16 compared to cells treated with C188-9 alone (Fig. 5), thus increasing p-STAT3/STAT3 ratio (Fig. 5). The decrease of COX-2 by C188-9 treatment was also reversed by additional transfection of pcDNA3.1-MUC16 (Fig. 5). These results indicated that suppression of JAK2/STAT3 pathway attenuated the promotion ability of MUC16 on COX-2.
Discussion
Despite widespread of cervical screening dramatically reducing the incidence of cervical cancer, it remains third leading cause of cancer-related death among females in the developing countries (Bray et al. 2018). Moreover, the highly recurrence and metastasis limited the usage of traditional drug therapy for cervical cancer (Li et al. 2017). Therefore, new therapeutical drugs with anti-proliferation, anti-migration and anti-invasion abilities are needed to improve the therapeutic efficacy for cervical cancer. Considering the promotion ability of MUC16 on various tumors, we prospectively suggested that MUC16 may participate in cervical cancer pathogenesis.
One of the major findings of the present study is that high expression of MUC16 was occurred in cervical cell lines, in line with previous report that MUC16 was up-regulated in southern Indian cervical cancer patients (Porika et al. 2010). However, devoid of directly analysis between MUC16 expression and clinical parameters of cervical cancer patients, the clinical significance of MUC16 in cervical cancer patients needs to further investigated. Moreover, in vitro loss- of function assays for the first time showed that MUC16 knockdown inhibited cell proliferation, suppressed cell invasion and migration of cervical cancer cells, indicating that MUC16 is a potential therapeutic target in cervical cancer.
Since the “oncogene” function of MUC16 on cervical cancer has been uncovered, the underlying mechanism was then clarified. The present study found that MUC16 knockdown could decrease PCNA and MCM-2 to suppress cervical cancer cell proliferation. Moreover, we also confirmed that MUC16 knockdown could decrease Bcl-2 and increase Cleaved caspase-3 to activate apoptosis signaling, thus suppressing cervical cancer growth and progression. In addition, Bcl-2 can also regulate cell migration and invasion during tumor progression (Bonneau et al. 2013), the functional targets of MUC16 involved in regulation of cervical cancer migration and invasion are the hotspot of further research.
In molecular level, we then found that MUC16 could facilitate cervical cancer progression via JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression, and suppression of JAK2/STAT3 pathway attenuated the regulation ability of MUC16 on COX-2. As well known, activation of STAT3 via JAK2-mediated phosphorylation plays an important role in cell proliferation, apoptosis, migration and invasion (Behera et al. 2010; Kundu et al. 2014). Propofol demonstrated anti-tumor activity in cervical cancer via inactivation of JAK2/STAT3 signaling pathway (Li et al. 2017). Inactivation of STAT3 was also involved in the suppression of cervical cancer growth, invasion and metastasis (Fan et al. 2015). Moreover, up-regulation of COX-2 via JAK2/STAT3 signaling pathway is correlated with proliferative effect on gastric cancer cells (Xu et al. 2013). The present study indicated that MUC16 knockdown could inactivate JAK2/STAT3 signaling pathway and down-regulated COX-2 to suppress cervical cancer progression. Additionally, research has shown that administration of COX-2 inhibitors could suppression of uterine cervical cancer regrowth or recurrence (Fujimoto et al. 2006). Therefore, MUC16 might be a therapeutical target for cervical cancer progression via regulation of JAK2/STAT3 phosphorylation-mediated COX-2. However, JAK2/STAT3 signaling pathway also participates in the epithelial-mesenchymal transition of cancer cells (Teng et al. 2014) to facilitate for cervical cancer stemness (Qureshi et al. 2015). JAK2/STAT3-mediated COX-2 also modulate inflammatory/immune responses in cervical cancer (Zhu et al. 2018). The functional roles of MUC16 on cervical cancer stemness or inflammatory response are needed to be further studied.
In conclusion, our results demonstrated that MUC16 knockdown inhibited cell proliferation, migration and invasion of cervical cancer cells, via JAK2/STAT3 phosphorylation-mediated COX-2. This finding illuminated the relation between MUC16/JAK2/STAT3/COX-2 regulatory axis and cervical cancer progression, suggesting potential application of MUC16 in treatment for the disease.
Availability of data and materials
All data generated or analyzed during this study are included in this published article.
References
Behera R, Kumar V, Lohite K, Karnik S, Kundu GC (2010) Activation of JAK2/STAT3 signaling by osteopontin promotes tumor growth in human breast cancer cells. Carcinogenesis 31:192–200
Bonneau B, Prudent J, Popgeorgiev N, Gillet G (2013) Non-apoptotic roles of Bcl-2 family: the calcium connection. Biochim Biophys Acta 1833:1755–1765
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Burki TK (2018) Outcomes after minimally invasive surgery in cervical cancer. Lancet Oncol 19:e674
Clarke CH, Yip C, Badgwell D, Fung ET, Coombes KR, Zhang Z, Lu KH, Bast RC Jr (2011) Proteomic biomarkers apolipoprotein A1, truncated transthyretin and connective tissue activating protein III enhance the sensitivity of CA125 for detecting early stage epithelial ovarian cancer. Gynecol Oncol 122:548–553
Fan Z, Cui H, Xu X, Lin Z, Zhang X, Kang L, Han B, Meng J, Yan Z, Yan X et al (2015) MiR-125a suppresses tumor growth, invasion and metastasis in cervical cancer by targeting STAT3. Oncotarget 6:25266–25280
Feng L, Wang Z (2006) Chemopreventive effect of celecoxib in oral precancers and cancers. Laryngoscope 116:1842–1845
Fujimoto J, Toyoki H, Sato E, Sakaguchi H, Jahan I, Alam SM, Tamaya T (2006) Expression of cyclooxygenase-2 related to angiogenesis in uterine cervical cancers. J Biomed Sci 13:825–832
Gao J, Tian J, Lv Y, Shi F, Kong F, Shi H, Zhao L (2009) Leptin induces functional activation of cyclooxygenase-2 through JAK2/STAT3, MAPK/ERK, and PI3K/AKT pathways in human endometrial cancer cells. Cancer Sci 100:389–395
Hovland S, Muller S, Skomedal H, Mints M, Bergstrom J, Wallin KL, Karlsen F, Johansson B, Andersson S (2010) E6/E7 mRNA expression analysis: a test for the objective assessment of cervical adenocarcinoma in clinical prognostic procedure. Int J Oncol 36:1533–1539
Kanaoka S, Takai T, Yoshida K (2007) Cyclooxygenase-2 and tumor biology. Adv Clin Chem 43:59–78
Khalil J, Bellefqih S, Sahli N, Afif M, Elkacemi H, Elmajjaoui S, Kebdani T, Benjaafar N (2015) Impact of cervical cancer on quality of life: beyond the short term (results from a single institution): quality of life in long-term cervical cancer survivors: results from a single institution. Gynecol Oncol Res Pract 2:7
Kundu J, Choi BY, Jeong CH, Kundu JK, Chun KS (2014) Thymoquinone induces apoptosis in human colon cancer HCT116 cells through inactivation of STAT3 by blocking JAK2- and Srcmediated phosphorylation of EGF receptor tyrosine kinase. Oncol Rep 32:821–828
Lakshmanan I, Ponnusamy MP, Das S, Chakraborty S, Haridas D, Mukhopadhyay P, Lele SM, Batra SK (2012) MUC16 induced rapid G2/M transition via interactions with JAK2 for increased proliferation and anti-apoptosis in breast cancer cells. Oncogene 31:805–817
Li H, Lu Y, Pang Y, Li M, Cheng X, Chen J (2017) Propofol enhances the cisplatin-induced apoptosis on cervical cancer cells via EGFR/JAK2/STAT3 pathway. Biomed Pharmacother 86:324–333
Porika M, Vemunoori AK, Tippani R, Mohammad A, Bollam SR, Abbagani S (2010) Squamous cell carcinoma antigen and cancer antigen 125 in southern Indian cervical cancer patients. Asian Pac J Cancer Prev 11:1745–1747
Qureshi R, Arora H, Rizvi MA (2015) EMT in cervical cancer: its role in tumour progression and response to therapy. Cancer Lett 356:321–331
Shimizu A, Hirono S, Tani M, Kawai M, Okada K, Miyazawa M, Kitahata Y, Nakamura Y, Noda T, Yokoyama S et al (2012) Coexpression of MUC16 and mesothelin is related to the invasion process in pancreatic ductal adenocarcinoma. Cancer Sci 103:739–746
Shukla SK, Gunda V, Abrego J, Haridas D, Mishra A, Souchek J, Chaika NV, Yu F, Sasson AR, Lazenby AJ et al (2015) MUC16-mediated activation of mTOR and c-Myc reprograms pancreatic cancer metabolism. Oncotarget 6:19118–19131
Sturgeon CM, Duffy MJ, Hofmann BR, Lamerz R, Fritsche HA, Gaarenstroom K, Bonfrer J, Ecke TH, Grossman HB, Hayes P et al (2010) National Academy of Clinical Biochemistry Laboratory Medicine Practice Guidelines for use of tumor markers in liver, bladder, cervical, and gastric cancers. Clin Chem 56:e1–48
Takaoka K, Kishimoto H, Segawa E, Hashitani S, Zushi Y, Noguchi K, Sakurai K, Urade M (2006) Elevated cell migration, invasion and tumorigenicity in human KB carcinoma cells transfected with COX-2 cDNA. Int J Oncol 29:1095–1101
Teng Y, Ross JL, Cowell JK (2014) The involvement of JAK-STAT3 in cell motility, invasion, and metastasis. JAKSTAT 3:e28086
Tzafetas M, Mitra A, Kalliala I, Lever S, Fotopoulou C, Farthing A, Smith JR, Martin-Hirsch P, Paraskevaidis E, Kyrgiou M (2018) Fertility-sparing surgery for presumed early-stage invasive cervical cancer: a survey of practice in the United Kingdom. Anticancer Res 38:3641–3646
Wang Q, Shi G, Teng Y, Li X, Xie J, Shen Q, Zhang C, Ni S, Tang Z (2017) Successful reduction of inflammatory responses and arachidonic acid-cyclooxygenase 2 pathway in human pulmonary artery endothelial cells by silencing adipocyte fatty acid-binding protein. J Inflamm (Lond) 14:8
Xu W, Chen GS, Shao Y, Li XL, Xu HC, Zhang H, Zhu GQ, Zhou YC, He XP, Sun WH (2013) Gastrin acting on the cholecystokinin2 receptor induces cyclooxygenase-2 expression through JAK2/STAT3/PI3K/Akt pathway in human gastric cancer cells. Cancer Lett 332:11–18
Zhu L, Tu H, Liang Y, Tang D (2018) MiR-218 produces anti-tumor effects on cervical cancer cells in vitro. World J Surg Oncol 16:204
Funding
This work is partly supported by Science and Technology Development Fund of Nanjing Medical University-Key Project (Grant No. 2017NJMUZD133).
Author information
Authors and Affiliations
Contributions
HS conceived and designed the experiments, MG and LW analyzed and interpreted the results of the experiments, XYC performed the experiments
Corresponding author
Ethics declarations
Conflict of interest
The authors state that there are no conflicts of interest to disclose.
Ethical approval and consent to participate
The animal use peotocol listed below has been reviewed and approved by the Animal Ethical and Welfaer Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shen, H., Guo, M., Wang, L. et al. MUC16 facilitates cervical cancer progression via JAK2/STAT3 phosphorylation-mediated cyclooxygenase-2 expression. Genes Genom 42, 127–133 (2020). https://doi.org/10.1007/s13258-019-00885-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13258-019-00885-9