Abstract
To understand their role in epilepsy, the nitric oxide synthetase (NOS), argininosuccinate synthetase (AS), argininosuccinate lyase (AL), glutamine synthetase (GS), and arginase activities, along with the concentration of nitrate/nitrite (NOx), thiobarbituric acid reactive substances (TBARS), and total antioxidant status (TAS), were estimated in different regions of brain in rats subjected to experimental epilepsy induced by subcutaneous administration of kainic acid (KA). The short-term (acute) group animals were killed after 2 h and the long term (chronic) group animals were killed after 5 days of single injection of KA (15 mg/kg body weight). After decapitation of rats, the brain regions were separated and in their homogenates, the concentration of NOx, TBARS and TAS and the activities of NOS, AS, AL, arginase and glutamine synthetase were assayed by colorimetric methods. The results of the study demonstrated the increased activity of NOS and formation of NO in acute and chronic groups epilepsy. The activities of AS and AL were increased and indicate the effective recycling of citrulline to arginine. The activity of glutamine synthetase was decreased in acute and chronic groups of epilepsy compared to control group and indicate the modulation of its activity by NO in epilepsy. The activity of arginase was not changed in acute group; however it was decreased in chronic group and may favor increased production of NO in this condition. The concentration TBARS were increased and TAS decreased in acute and chronic groups of epilepsy and supports the oxidative stress in epilepsy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuronal excitation involving the excitatory glutamate receptors is recognized as an important underlying mechanism in neurodegenerative disorders [11]. Glutamate and related excitatory amino acids are considered major neurotransmitters in the central nervous system [10]. In the CNS, the conversion of glutamate to glutamine by glutamine synthetase (GS), that takes place within the astrocytes, represents a key mechanism in the regulation of excitatory neurotransmission under normal conditions as well as in injured brain [41]. Kainic acid (KA) is a potent CNS excitotoxin, producing acute and sub-acute epilepticform activity, ultimately resulting in widespread irreversible neuropathological changes [38]. KA induced status epilepticus was associated with both apoptotic and necrotic cell death and induction of heat sensitive proteins in hippocampus and cortical regions of rodent brain [1, 18, 43]. The exact mechanisms contributing to increased concentration of nitric oxide (NO) in epilepsy are not well established. Earlier studies reported that NOS knockout mice were more severely affected by epileptic activity than controls and the response to NO during epilepsy depends on its concentration [17]. It was also indicated that NO may be regarded as an anticonvulsant and proconvulsant substance in relation to convulsions induced by pentylenetetrazole PTZ [17]. Reactive oxygen species (ROS)/reactive nitrogen species (RNS) have been implicated in the pathogenesis of various neurological disorders including epilepsy [12]. Intracellular ROS are capable of inducing damage and, in severe cases, cell death through mitochondrial alterations leading to the release of cytochrome c [4, 15], through activation of the JNK pathway [42] or by activation of nuclear factor-KB (NF-KB) transcription factors [24]. The ability to control ROS is thus critical in neurodegenerative diseases, because neuronal damage occurs when the “oxidant- anti-oxidant” balances are disturbed in favor of excess oxidative stress [25]. Stimulation of glutamate-KA receptors induces neuronal NO release, which in turn modulates glutamate transmission [2, 28]. NO induces changes in neuronal and signaling-related functions by several ways [29]. Generation of NO, a versatile molecule in signaling processes and unspecific immune defense, is intertwined with synthesis, catabolism and transport of arginine which thus ultimately participates in the regulation of a fine-tuned balance between normal and pathophysiological consequences of NO production [44]. NO is synthesized from arginine by nitric oxide synthase (NOS; EC 1.14.13.39), and the citrulline generated as a by-product can be recycled to arginine by successive actions of argininosuccinate synthetase (AS; EC 6.3.4.5) and argininosuccinate lyase (AL; EC 4.3.2.1) via the citrulline-NO cycle [46]. Arginine in brain is also utilized by arginase (EC 3.5.3.1) for production of ornithine. Co-induction of AS, cationic amino acid transporter-2, and NOS in activated murine microglial cells [19] and co-induction of inducible NOS and arginine recycling enzymes in cytokine-stimulated PC12 cells and high output production of NO were reported by Zhang et al. [44]. It was reported earlier that GS becomes nitrated and inhibited during PTZ induced seizure model at repeated PTZ seizure induction, but there was no decrease in GS protein level [5]. In our earlier study we reported the increased activities of NOS, AS, AL and decreased activity of GS in KA mediated excitotoxicity in rat brain [40]. As the epilepsy is a chronic disease leading to neurodegeneration, the studies comparing acute and chronic group may provide further information to understand the different mechanisms playing a role in this condition. Therefore the present study was conducted to assess the activities of AS, AL, NOS, GS, and estimation of NOx, TBARS, and TAS concentration in cerebral cortex (CC), cerebellum (CB) and brain stem (BS) of rats in acute and chronic groups of kainic acid mediated epilepsy.
Material and methods
Animals and epilepsy induction
Male Sprague Dawley rats weighing 200–250 g were used for the study. The animals had free access to food and water. Animal ethics committee of Universiti Sains Malaysia, Health campus, Kubang Kerian, Malaysia, approved the experimental design [USM/Animal Ethics Approval/2007/(34) (105)]. The animals were divided into control, acute group and chronic groups (n = 6 rats/group). In the acute group, epilepsy was produced by subcutaneous administration of KA (15 mg/kg body weight, dissolved in normal saline) and control group received normal saline subcutaneously [26]. The animals showed convulsions after 40–45 min of KA injection for 2–3 min and afterwards became drowsy. The animals were killed after 2 h of injection using the guillotine and the brains were quickly removed, placed in ice cold saline and blotted with filter paper to remove blood and the different regions (CC, CB and BS) were separated as described by Sadasivudu and Lajtha [35]. Each of the brain regions was weighed and used for the preparation of homogenates in 0.05 M phosphate buffer pH 7.3. In the chronic group, the animals were given KA injection; a single dose (15 mg/kg body weight, dissolved in normal saline) on day one and the animals were killed after 5 days of KA administration. They were given free access to food and water during the 5 days after KA administration.
Enzyme assays
Nitric oxide synthase
NOS activity was estimated by the method of Yui et al. [45] as described by Swamy et al. [39]. In the assay the tissue homogenate is incubated with substrate mixture and the stable end products, NOx, were estimated using the Nitric Oxide Synthase assay Kit from Calbiochem, USA (Catalogue Number 482702). As high amounts of NADPH interferes with Griess reagents, the kit uses lactate dehydroginase to destroy excess NADPH, to remove its interference with Griess reagents. The reaction mixture 400 μl containing 50 mM Tri-HCl (pH 7.4), 1 mM NADPH, 1 mM l-arginine, 1 mM Ca2+, 10 μM FAD, 0.5 mM DTT and 0.1 mM (6R)-BH4 was incubated with 200 μl of homogenate (5%) for 20 min at 37°C, and the reaction stopped by boiling at 100°C for 30 s. The tubes were centrifuged at 1,500×g for 20 min and 40 μl supernatant used for NOx estimation as per the procedure of kit. The enzyme activity was expressed in nanomoles of NOx formed/gram wet weight of tissue/hour.
Argininosuccinate synthetase
Argininosuccinate synthetase activity was estimated by the modified method of Levin [23] as described by Swamy et al. [39]. In the ASS assay the argininosuccinate formed can be converted to arginine and fumarate and subsequently arginine is converted to urea and ornithine by successive activities of ASL and arginase present in homogenates. In the ASS assay the ASL present in the homogenate was considered to be sufficient and excessive arginase is added to drag the reaction for the effective formation of urea, because the assay pH kept at 7.3, where the arginase activity is low. In the estimation of ASS, the incubation mixture contained 0.8 ml of 0.01 M each of citrulline, aspartic acid, ATP, magnesium chloride, and 21U of arginase, in 0.05 M phosphate buffer (pH 7.3). Reaction was started with the addition of 0.2 ml of 20% homogenate and incubated at 37°C for 1°h. At the end of incubation period, 0.2 ml of 50% trichloroacetic acid was added to stop the reaction. For controls, trichloroacetic acid was added before the incubation. The mixture was then centrifuged and 0.5 ml of supernatant was used for color development. The supernatant was mixed with 1.5 ml of acid mixture (one part of concentrated sulphuric acid and three parts of concentrated phosphoric acid) and 0.1 ml of isonitrosopropiophenone (5% in absolute alcohol). It was kept in boiling water bath for 30 minutes, and then after cooling the tubes, absorbance was read at 540 nm. Simultaneously, a urea standard was set up by adding to the standard 0.5 ml of substrate mixture and 0.5 ml of water. The color developed was read at 540 nm against the reagent blank. The enzyme activity was expressed as micromoles of urea formed/gram wet weight of tissue/hour
Arginininosuccinate lyase
Argininosuccinate lyase activity was assayed by the method of Levin [23] as described by Swamy et al. [39]. The assay system for ASL consisted of 0.3 ml of 1 M phosphate buffer (pH 7.3), 0.6 ml of argininosuccinate (6.0 mM), 0.2 ml of 20% homogenate, and 0.1 ml of arginase (10.5 U). At the end of 1 h incubation at 37°C, the reaction was stopped by the addition of 0.3 ml of 50% trichloroacetic acid. Controls were identical, except that trichloroacetic acid was added before incubation. After incubation, the mixture was centrifuged at 3,000 rpm for 5 min and 0.5 ml of the supernatant was used for urea estimation. Urea was estimated by the modified diacetylmonoxime (DAM) method. The enzyme activity was then expressed as micromoles of urea formed/gram wet weight of tissue/hour.
Arginase
Arginase activity was assayed according to the method of Herzfeld and Raper [16] as described by Swamy et al., [39]. The enzyme in the homogenate is activated by equal volume of 10% homogenate (in phosphate buffer) with imidazole buffer, containing 56 mM imidazole and 56 mM MnCl2 at pH 7.4, for 10 min at 50°C. The activated preparations were then centrifuged at 3,000 rpm for 5 min, and the supernatants were used for measurement of enzyme activity. Enzyme assay was carried out in a total of 0.8 ml of incubation mixture consisting of 100 μmol of l-arginine and 60 μmol of glycine buffer (both adjusted to pH 9.5 with 1.0 N NaOH), and 0.2 ml of supernatant after activation. After incubation at 37°C for 10 min, the reaction was stopped with the addition of 0.2 ml 50% trichloroacetic acid. For the enzyme controls, the trichloroacetic acid was added first together with the incubation mixture. The mixture was then centrifuged again at 3,000 rpm for 5 min and 0.5 ml of supernatant was taken for estimation of urea. Urea was estimated using the DAM method and the activity was expressed as micromoles of urea formed/gram wet weight of tissue/hour.
Glutamine synthetase
GS activity was assayed by the method Rowe et al. [33] as described by Sadasivudu et al. [36]. Assay mixture consisting of 0.4 ml of imidazole-HCl buffer (pH 7.2), 0.1 ml of 0.2 M magnesium chloride, 0.1 ml of 0.25 M 2-mercaptoethanol, 0.1 ml of 0.1 M ATP, 0.1 ml of 0.5 M glutamate, 0.1 ml of 1 M hydroxyl amine (pH 7.2) and 0.1 ml of 10% homogenates was incubated for 15 min at 37°C. At the end of incubation, 1.5 ml of ferric chloride reagent (0.37 M FeCl3, 0.67 M HCl, and 0.2 M TCA) was added to terminate the reaction and to initiate the color development. Control tubes received homogenate after the addition of ferric chloride reagent. A reagent blank was prepared by omitting homogenate from the assay mixture. After centrifugation, the absorbency in the supernatant was measured at 535 nm. The amount of γ-glutamyl hydroxamate formed was calculated using that 1 μmol of γ-glutamyl hydroxamate gives an OD of 0.34 at 535 nm. Enzyme activity was expressed as micromoles of γ-glutamyl hydroxamate formed/gram wet weight of tissue/hour.
Estimations of NO
NO was estimated as NOx by Griess reaction after conversion of nitrate to nitrite by nitrate reductase, as described by Swamy et al. [39] using the commercially available Nitric Oxide Assay Kit from Cayman Chemical Company (Catalogue number 780001; Ann Arbor, MI, USA). As high amounts of NADPH interferes with Griess reagents, in this kit small amount of NADPH is used in the nitrate reductase reaction in conjunction with a catalytic system for recycling of spent NADPH.
NOx concentration was expressed as nanomoles of NOx/gram wet tissue.
Estimatin of TBARS
Lipid peroxidation was determined by the method of Chatterjee et al., [9] by estimating Thiobarbituric acid reactive substances (TBARS). A 100 μl aliquot of homogenate will be added to a reaction mixture containing 200 μl 8.1% (w/v) lauryl sulphate, 1.5 ml 20% (v/v) acetic acid, 1.5 ml 0.8 (w.v) thiobarbituric acid and 700 μl distilled water. Samples will than boiled for 1 h at 95°C and centrifuged at 3,000×g for 10 min. The absorbance of the supernatant will be measured spectrophotometrically at 650 nm.1,1,3,3-tetraethoxy propane, a form of MDA will be used as standard in this assay. Lipid peroxidation was expressed as nanomoles of MDA equivalent/gram wet tissue.
Estimation of TAS
TAS was estimated according to the method of Koracevic et al., [20]. A standard solution of Fe-EDTA complex reacts with hydrogen peroxide by a Fenton-type reaction, leading to formation of hydroxyl radicals (.OH). These reactive oxygen species degrade benzoate, resulting in the release of TBARS. Antioxidants from the added sample cause suppression of the production of TBARS. This reaction was measured spectrophotometrically at 532 nm and the inhibition of color development defined as antioxidant activity. TAS was expressed as nanomol of uric acid equivalent/g wet tissue.
Statistical analysis
Results were reported as mean ± standard deviation (SD) from 6 animals for each parameter calculated. Statistical analysis of results was done by one-way analysis of variance (ANOVA) followed by post hoc analysis using Bonferroni's test, using the SPSS software (version 12.0.1) to determine the statistical significance of difference in values between the control, acute and chronic groups. p value of <0.05 was taken as statistically significant at 95% confidence interval.
Results
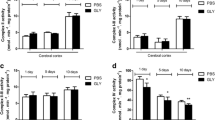
The activity of NOS (Fig. 1) increased in all the brain regions tested in acute group and showed further increase in chronic group in CC and CB compared to control group. AS and AL activities (Fig. 2) were significantly increased in all the three brain regions in acute and chronic groups of KA mediated epilepsy compared to control group. No significant change observed in arginase activity (Fig. 2) in the brain regions tested in acute group compared to control, however the activity of arginase was decreased in chronic group. The results of GS activity are shown in Fig. 3. In the acute group GS activity was decreased and in chronic group the activity remained decreased in all the brain regions studied in epilepsy compared to control group. Figure 4 shows the concentration of NOx, TAS and TBARS in this study. The concentration of NOx increased significantly in all the brain regions tested in acute and chronic group compared to control. The pattern observed for the increase in concentration of NOx in the three different brain regions was nearly similar to that of the NOS activity increase in both acute and chronic groups of epilepsy. The concentration of TAS (Fig. 4) was decreased significantly and the concentration of TBARS (Fig. 4) increased significantly in all the brain regions tested in acute and chronic groups compared to control group.
Activity of NOS in different regions of rat brain in acute and chronic groups of epilepsy. Statistical analysis was done by one-way ANOVA followed by post hoc analysis using Bonferroni's test. Values are mean ± SD for six animals in each group; a p < 0.001 versus control group; b p < 0.001 versus acute group
Activities of AS, AL, and arginase in different regions of rat brain in acute and chronic groups of epilepsy. Statistical analysis was done by one-way ANOVA followed by post hoc analysis using Bonferroni’s test. Values are mean ± SD for six animals in each group; a p < 0.001, a1 p < 0.01, and a2 p < 0.05 versus control group; b p < 0.001 vs acute group
Activity of glutamine synthetase in different regions of rat brain in acute and chronic groups of epilepsy. Statistical analysis was done by one-way ANOVA followed by post hoc analysis using Bonferroni's test. Values are mean ± SD for six animals in each group; a p < 0.001 vs control group; b p < 0.001 vs acute group
Concentration of NOxx, TASy, and TBARSz in different regions of rat brain in acute and chronic groups of epilepsy. xConcentration expressed as nanomol of NOx/g wet weight of tissue. yConcentration expressed as nanomol of uric acid equivalent/gram wet weight of tissue. zConcentration expressed as nanomoles of MDA equivalent/gram wet weight of tissue Statistical analysis was done by one-way ANOVA followed by post hoc analysis using Bonferroni's test. Values are mean ± SD for six animals in each group; a p < 0.001, a1 p < 0.01, and a2 p < 0.05 vs control group; b p < 0.001, b1 p < 0.01, and b2 p < 0.05 vs acute group
Discussion
Neuronal excitation involving the excitatory glutamate receptors is recognized as an important underlying mechanism in neurodegenerative disorders [11]. NO is postulated to be involved in the pathophysiology of many epilepsy models resulting from increased action of excitatory neurotransmitter namely glutamate [22, 34]. In neurons, NO synthesis is stimulated by Ca2+-influx, which is induced by activation of glutamate receptors, preferentially NMDA receptor [30]. The literature findings implicate neuronal NO generation in the pathogenesis of both direct and secondary excitotoxic neuronal injuries in vivo. Although NMDA receptors likely contribute critically to neuronal injury in various acute conditions, several observations support the hypothesis that AMPA/KA receptors may be of greater importance to the neurodegenerative process [7]. Though there are most kainate receptors in the hippocampus, earlier studies showed a high production of NO in cortex than amygdala and hippocampus [26]. The increased concentration of NO in brain in epilepsy as observed by increase in NOx concentration in this study support the earlier findings of NO involvement in pathophysiology of excitotoxicity [14, 17, 26, 40]. The sustained increase of NOx in chronic group indicates the continuous increased production of NO and its deleterious effects in CNS in chronic conditions of epilepsy. Increased formation of NO by stimulated activity of NOS depends upon a continuous supply of arginine at the site of synthesis. Activities of AS and AL were elevated in all the brain regions of rats subjected to epilepsy. The mechanism of increased activities of these enzymes is not clear. However the possibility of induction cannot be ruled out along with the modification of enzyme with unknown mechanism. Further, our observation of higher activities of NOS, AS, and AL in cerebellum suggests a higher flux of the citrulline-NO cycle in cerebellum. The functional significance of such a high flux of citrulline-NO cycle in cerebellum needs further clarification. Our results on the activities of AS and AL suggest that the citrulline-NO cycle plays a significant role in ensuring adequate supply of arginine for the increased production of NO observed in epilepsy. A similar increase of NOS, AS and AL activities along with increased production of NO in KA mediated excitotoxicity was earlier reported [5]. The sustained high activities of these enzymes observed in chronic group may be responsible for continuous high production of NO and provide an important functional role for these enzymes in chronic condition of epilepsy
Apart from NO synthesis l-arginine may also serve as a substrate for glutamate formation and may also provide increased substrate for arginase [6]. No significant changes in the activity of arginase in the acute group indicate that there is no enhanced utilization of arginine by this enzyme in anoxia. However the observed decrease of arginase in chronic group may favor increased production of NO in this condition. Both NOS and arginase use arginine as a common substrate, and arginase may down-regulate NO production by competing with NOS for arginine [27]. The decreased arginase activity and increased activities of citrulline-NO cycle enzymes in chronic group provide more favorable condition for the high production of NO in this group of epilepsy.
In the brain the conversion of glutamate to glutamine by GS, that takes place within the astrocytes, represents a key mechanism in the regulation of excitatory neurotransmission [41]. The glutamine synthetase activity is present in all parts of brain and it is equally high in cerebral cortex, cerebellum and hippocampus [13, 32]. The modulation of GS activity in brain, therefore, is important and its impairment or saturation may have pathological consequences [31]. The decreased activity of GS observed in this study indicates the probable inhibition of GS by NO. The exact mechanism of inhibition of GS by NO is not known, but it is thought to be as a covalent modification as a result of nitrosylation or nitration of tyrosin in GS [21, 32]. It is proposed that the inhibition of GS by NO may provide prolonged availability of glutamate, which is causing excitotoxicity. In view of these observations the pharmacological agents who can increase GS may prove beneficial in the treatment of neurological disorders involving excitotoxicity including epilepsy. Activity of the GS could be involved in the regulation of concentration of glutamate in the extra-cellular space of neurons with other systems, astroglial glutamate transporter-I (GLT-1), and also microglial antiporter for cystine and glutamate which may release glutamate when the demand of glutathione synthesis was increased by oxidative stress [3]. Excitotoxicity and disrupted energy metabolism were considered to be acting in a synergistic manner leading to nerve cell death in neurodegenerative disorders [11]. These cooperative pathways trigger oxidative stress by free radical formation [37] and ROS/RNS are believed to cause lipid peroxidation with high levels of MDA resulting in damage to biological membranes [8]. Epileptic form activity was shown to cause excessive production of ROS/RNS, a factor believed to be involved in the mechanisms leading to neurodegeneration and cell death [17]. The increased levels of TBARS and reduced concentration of TAS observed in this study indicate the presence of oxidative stress in epilepsy. The sustained increase in concentration of TBARS and decreased TAS level in chronic group compared to control suggest the continuation of adverse effects in epilepsy in long term and may be leading to neurodegeneration.
Conclusion
This study clearly demonstrated the increased concentration of NO and supports the involvement of NO in the pathophysiology of excitotoxicity in epilepsy. The increased activities of AS and AL indicate the effective recycling of citrulline to arginine and suggest a functional role to citrulline–NO cycle enzymes in epilepsy. The activity of arginase was not changed in acute group; however it was decreased in chronic group and may favor increased production of NO in this condition. The decreased activity of GS in the brain regions tested indicate the modulation of its activity by NO and favors the prolonged availability of glutamic acid causing excitotoxicity leading to neuronal damage in epilepsy. The increased concentration of TBARS and decreased concentration of TAS supports the oxidative stress in KA mediated epilepsy. The sustained increase in concentration of TBARS and decreased TAS level in chronic group compared to control suggest the continuation of adverse effects in epilepsy in long term leading to neurodegeneration and suggests a possible role for anti oxidants in preventing neurodegeneration in epilepsy.
References
Akbar MT, Wells DJ, Latchman DS, de Belleroche J (2001) Heat shock protein 27 shows a distinctive widespread spatial and temporal pattern of induction in CNS glail and neuronal cells compared to heat shock protein 70 and caspase 3 following kainate administration. Brain Res Mol Brain Res 93:148–163
Alabadi J, Thibault JL, Pinard E, Seylaz J, Lasbennes F (1999) 7-Nitroindazole a selective inhibitor of nNOS increases hippocampal extracellular glutamate concentration in status epilepticus induced by kainic acid in rats. Brain Res 839:305–312
Barger SW, Goodwin ME, Porter MM, Beggs ML (2007) Glutamate release from activated microglia requires the oxidative burst and lipid peroxidation. J Neurochem 101:1205–1213
Berman SB, Hastings TG (1999) Dopamine oxidation alters mitochondrial respiration and induces permeability transition in brain mitochondria, implications for Parkinson’s disease. J Neurochem 73:1127–1137
Bidmon HJ, Gorg B, Palomero-Gallagher N, Schleicher A, Haussinger D, Speckmann EJ, Zilles K (2008) Glutamine synthetase becomes nitrated and its activity is reduced during repetitive seizure activity in the pentylenterazole model of epilepsy. Epilepsia 49:1733–1748
Bommarius AS, Makryaleas K, Drauz K (1991) An enzymatic route to l-ornithine from l-arginine–activation and stabilization studies on l-arginase. Biomed Biochim Acta 50:S249–S255
Carriedo SG, Sensi SL, Yin HZ, Weiss JH (1998) Rapid Ca2+entry through Ca2+ permeable AMPa/kainite channels triggers marked intracellular Ca2+ rises and consequent oxygen radical production. J Neurosci 18:7727–7738
Chan PH (2001) Reactive oxygen radicals in signaling and damage in the ischemic brain. J Cereb Blood Flow Metab 21:2–14
Chatterjee PK, Cuzzocrea S, Brown PA, Zacharowiski K, Stewart KN, Motafilipe H, Thiemermann C (2000) Tempol, a membrane-permeable radical scavenger, reduces oxidant stress-mediated renal dysfunction and injury in the rat. Kidney Int 58:658–673
Coyle JT, Puttfarcken P (1993) Oxidative stress, glutamate and neurodenerative disorders. Science 262:689–695
Dong XX, Wang Y, Qin ZH (2009) Molecular mechanisms of excitotoxicity and their relevance to pathogenisis of neurodegenerative diseases. Acta Pharmacol Sin 30:379–387
Frantseva MV, Perez Velzquez JL, Tsoraklidis G, Mendonca AJ, Adamchik Y, Mills LR, Carlen PL, Burnham MW (2000) Oxidative stress is involved in seizure-induced neurodegeneration in the kindling model of epilepsy. Neuroscience 97:431–435
Girard G, Giguere J-F, Butterworth RF (1993) Region selective reductions in activities of glutamine synthetase in rat brain following portacaval anastomosis. Metab Brain Dis 8:207–215
Guix FX, Uribesalgo M, Coma M, Munoz FJ (2005) The physiology and patophysiology of nitric oxide in the brain. Prog Neurobiol 76:126–152
Halestrap AP, Doran E, Gillespie JP, O’Toolee A (2000) Mitochondria and cell death. Biochem Soc Trans 28:170–177
Herzfeld A, Raper SM (1976) The heterogeneity of arginase in rat tissues. Biochem J 153:469–478
Itoh K, Watanabe M (2009) paradoxical facilitation of pentylenetetrazole-induced convulsion susceptibility in mice lacking neuronal nitric oxide synthase. Neuroscience 159:735–743
Kato K, Katoh-Semba R, Takeuchi IK, Ito H, Kamei K (1999) Responses of heat shock proteins hsp27, alphaB-crystalline, and hsp70 in rat brain after kainic acid-induced seizure activity. J Neurochem 73:229–236
Kawahara K, Gotoh T, Oyadomari S, Kajizono M, Kuniyasu A, Ohsawa K, Imai Y, Kohsaka S, Nakayama H, Mori M (2001) Co-induction of argininosuccinate synthetase, cationic amino acid transporter-2, and nitric oxide synthase in activated murine microglial cells. Mol Brain Res 90:165–173
Koracevic D, Koracevic G, Djordjevic V, Andrejevic S, Cosic V (2000) Method for the measurement of antioxidant activity in human fluids. J Clin Pathol 54:356–361
Kosenko E, Llansola M, Montoliu C, Monfort P, Rodrigo R, Hernandez-Viadel M, Erceg S, Sanchez-Perez AM, Felipo V (2003) Glutamine synthetase activity and glutamine content in brain: modulation by NMDA receptors and nitric oxide. Neurochem Int 43:493–499
Lapouble E, Montecot C, Sevestre A, Pichon J (2002) Phosphinothricin induces epileptic activity via nitric oxide production through NMDA receptor activation in adult mice. Brain Res 957:46–52
Levin B (1971) Hereditary metabolic disorders of urea cycle. In: Bodensky O, Latner AL (eds) Advances in clinical chemistry, vol 14. Academic, New York, p 66
Luo Y, Hattori A, Munoz J, Qin ZH, Roth GS (1999) Intrastriatal dopamine injection induces apoptosis through oxidation-involved activation of transcription factors AP-1 and NK-kappaB in rats. Mol Pharmacol 56:254–264
Maalouf M, Sullivan PG, Davis L, Kim DY, Rho JM (2007) Ketones inhibit mitochondrial production of reactive oxygen species production following glutamate excitotoxicity by ncreasing NADH oxidation. Neuroscience 145:256–264
Milatovic D, Gupta RC, Dettbarn WD (2002) Involvement of nitric oxide in Kainic acid-induced excitotoxicity in rat brain. Brain Res 957:330–337
Mori M (2007) Regulation of Nitric oxide synthesis and apoptosis by arginase and arginine recycling. J Nutr 137:1616S–1620S
Nakaki T, Mishima A, Suzuki E, Shintani F, Fujii T (2000) Glufosinate ammonium stimulates nitric oxide production through N-methyl-D-aspartate receptors in rat cerebellum. Neurosci Lett 290:209–212
Prast H, Philippu A (2001) Nitric oxide as modulator of neuronal function. Prog Neurobiol 64:51–68
Radenovic L, Selakovic V (2005) Differential effects of NMDA and AMPA/Kainate receptor antagonists on nitric oxide production in rat brain following intrahippocampal injection. Brain Res Bull 67:133–141
Rodrigo R, Felipo V (2007) Control of brain glutamine synthesis by NMDA receptors. Front Biosci 12:883–890
Rose C, Felipo V (2005) Limited capacity for ammonia removal by brain in chronic liver failure: potential role of nitric oxide. Metab Brain Dis 20:275–283
Rowe WB, Ronzio RA, Wellner VP, Meister A (1970) Glutamine synthetase (Sheep brain). In: Tabor H, Tabor CW (eds) Methods in Enzymol, vol XVII Part A. Academic, New York, pp 900–910
Rundfeldt C, Koch R, Richter A, Mevissen M, Gerecke U, Loscher W (1995) Dose-dependent anticonvulsant and proconvulsant effects of nitric oxide synthase inhibitors on seizure threshold in a cortical stimulation model in rats. Eur J Pharmacol 274:73–81
Sadasivudu B, Lajtha A (1970) Metabolism of amino acids in incubated slices of mouse brain. J Neurochem 17:1299–1311
Sadasivudu B, Nasreen Z, Swamy M (1985) Functional significance of the activities of gutaminase and ornithine-ω- aminotransferase in rat brain. Neurochem Int 7:449–454
Silva-Adaya D, Perez-De La Cruz V, Herrera-Mundo MN, Mendoza-Maccedo K, Villeda-Hernandez J, Bininda Z, Ali SF, Santamria A (2008) Excitotoxic damage, disrupted energy metabolism, and oxidative stress in the rat brain: antioxidant and neuroprotective effects of L-carnitine. J Neurochem 105:677–689
Sperk G (1994) Kainic acid seizures in the rat. Prog Neurobiol 42:1–32
Swamy M, Adlin ZZ, Chandran G, Sirajudeen KNS, Nadiger HA (2005) Effect of acute ammonia toxicity on nitric oxide (NO), citrulline-NO cycle enzymes, arginase and related metabolites in different regions of rat brain. Neurosci Res 53:116–122
Swamy M, Sirajudeen KNS, Chandran G (2009) Nitric oxide [NO] citrulline-NO cycle enzymes, glutamins synthetase and oxidative status in kainic acid-mediated excitotoxicity in rat brain. Drug Chem Toxicol 32:326–331
Szatkowski M, Attwell D (1994) Triggering and execution of neuronal death in brain ischaemia: two phases of glutamate release by different mechanisms. Trends Neurosci 17:359–365
Tournier C, Hes P, Yang DD, Xu J, Turner TK, Nimnual A, Bar-Sagi D, Jones SN, Flavella RA, Davis RJ (2000) Requirement of JNK for stress-induced activation of the cytochrome c-mediated death pathway. Science 288:870–874
White HS (2002) Animal models of epileptogenesis. Neurology 59:S7–S12
Wiesinger H (2001) Arginine metabolism and the synthesis of nitric oxide in the nervous system. Prog Neurobiol 64:365–391
Yui Y, Hattori R, Kosuga K, Eizawa H, Hiki K, Ohkawa S, Ohnishi K, Terao S, Kawai C (1991) Calmodulin-independent nitric oxide synthase from rat polymorphonuclear neutrophils. J Biol Chem 266:3369–3371
Zhang WY, Gotoh T, Oyadomari S, Mori M (2000) Coinduction of inducible nitric oxide synthase and arginine recycling enzymes in cytokine-stimulated PC 12 cells and high output production of nitric oxide. Mol Brain Res 83:1–8
Acknowledgements
This study project received financial support from Universiti Sains Malaysia–Research University grant (A/C No: 1001/PSKBP/8120196). WRWY received NSF from MOSTI. The programme leader of the research cluster, Prof. Jafri Malin Abdullah is duly acknowledged. The findings of the study were presented in seventh COSTAM/SFRR (Asia/Malaysia) International Workshop 2009, 9th–12th July 2009, Meritus Pelangi Beach Resort, Langkawi, Malaysia and 14th National Conference on Medical and Health Sciences, 21–22 May 2009, Health Campus, Kubang Kerian, Kota Bharu, Kelantan, Malaysia
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Swamy, M., Yusof, W.R.W., Sirajudeen, K.N.S. et al. Decreased glutamine synthetase, increased citrulline–nitric oxide cycle activities, and oxidative stress in different regions of brain in epilepsy rat model. J Physiol Biochem 67, 105–113 (2011). https://doi.org/10.1007/s13105-010-0054-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-010-0054-2