Abstract
Intracerebral hemorrhage in combination with intraventricular hemorrhage (IVH) is a severe type of stroke frequently leading to prolonged clinical care, continuous disability, shunt dependency, and high mortality. The molecular mechanisms induced by IVH are complex and not fully understood. Moreover, the treatment options for IVH are limited. Intraventricular recombinant tissue plasminogen activator (rt-PA) dissolves the blood clot in the ventricular system; however, whether the clinical outcome is thereby positively affected is still being debated. The mechanistic cascade induced by intraventricular rt-PA therapy may cure and harm in parallel. Despite the fact that intraventricular blood clots are thereby dissolved, blood derivatives enter the parenchyma and may still adversely affect functional structures of the brain: Smaller blood clots may obstruct the perivascular (Virchow-Robin) space and thereby the glymphatic system with detrimental consequences for cerebrospinal fluid (CSF)/interstitial fluid (ISF) flow. These clots, blood cells but also blood derivatives in the perivascular space, destabilize the blood-brain barrier from the brain parenchyma side, thereby also functionally weakening the neurovascular unit. This may lead to further accommodation of serum proteins in the ISF and particularly in the perivascular space further contributing to the adverse effects on the neuronal microenvironment. Finally, the arterial (Pacchionian) granulations have to cope with ISF containing this “blood, cell, and protein cocktail,” resulting in obstruction and insufficient function of the arterial granulations, followed by a malresorptive hydrocephalus. Particularly in light of currently improved knowledge on the physiologic and pathophysiologic clearance of cerebrospinal fluid and interstitial fluid, a critical discussion and reevaluation of our current therapeutic strategies to treat intraventricular hemorrhages are needed to successfully treat patients suffering from this severe type of stroke. In this review, we therefore summarize and discuss recent clinical trials and future directions for the field of IVH with respect to the currently increased understanding of the glymphatic system and the neurovascular unit pathophysiology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intracerebral and particularly intraventricular hemorrhages (IVH) are severe types of stroke with interrelated etiologies and a complex pathophysiology representing a challenge for neurocritical care [1,2,3,4,5,6,7]. Combined neurosurgical and pharmacological treatment may be one option to treat these severely ill IVH patients (Fig. 1). Hence, clinical trials addressing intraventricular thrombolysis [8,9,10] including the most recent trial [11] and its sequential sub-analyses [12,13,14] were anticipated and discussed with great interest [15]. For example, CLEAR III was a randomized, multicenter, placebo-controlled trial that included 500 patients suffering from IVH, mostly originating from intracerebral hemorrhage (ICH) [11]. Patients were randomized to receive intraventricular alteplase (recombinant tissue plasminogen activator, rt-PA) as treatment or intraventricular saline as placebo. While the primary outcome measurement (moderate disability, modified Rankin scale, mRS ≤ 3) was slightly but not significantly higher in the rt-PA group (48%) compared to placebo (45%), the rt-PA group had a significantly lower mortality rate after 180 days. Nevertheless, some surviving patients had severe disabilities (mRS = 5) in the rt-PA group, which is not unusual for this critical cerebrovascular disease. The ambitious and well-designed trial was expected to improve knowledge on how to treat IVH patients. However, the pathophysiologic sequelae following IVH treatment with intraventricular alteplase raised new questions and may potentially implicate a therapeutic double-edged sword. But the question arises—why?
Cranial CT scans of two patients suffering from massive (a–d) or less severe (e–h) intraventricular hemorrhages (IVH). Both patients received intraventricular rt-PA via external ventricular drainage. a–d Axial images of a cranial CT scan of a male patient (82 years) suffering from a subarachnoid and intraparenchymal hemorrhage with a massive IVH. Most likely, the IVH is a result of an aneurysm rupture of the left distal anterior cerebral artery. The CT-based morphology and distribution of the intracranial hemorrhage and the presentation of the patient’s symptoms suggest the occurrence of an initial bleed and a later re-bleed. Note the edema formation particularly at the semi-oval center of the left hemisphere adjacent to the large blood clot, particularly visible in a and b. c, d The external ventricular drainage in the right lateral ventricle. e–h Axial and coronal CT images of a male patient (61 years). The images show a less severe intraventricular hemorrhage. The external ventricular drainage is seen in f and particularly in the coronal image g. The implantation accidentally caused some amounts of intracranial air (e, f). Blood clot-adjacent regional edema formation can be seen in g and h. Yellow arrows signifies blood or blood clots. Blue arrow heads signifies brain parenchyma with vasogenic edema formation and/or cerebrospinal fluid diapedesis from the ventricles. Red arrows signifies external ventricular drainage
Please find the search criteria for this review online (Supplementary material: Method and Search criteria).
Classic and Hypothetical Routes of Cerebrospinal Fluid
To constructively debate this question, we should briefly recall the routes of the cerebrospinal fluid (CSF, Fig. 2a). The CSF is filtrated and actively transported (“produced”) at a rate of approximately 0.35 mL/min predominantly by the choroid plexuses, specialized endothelium and ependyma-like two-layered structures building the fairly tight blood-CSF barrier (BCSFB). Other parts of the CSF may directly leak from cerebral capillaries. However, the respective amounts are still under debate [16]. From the choroid plexuses, the CSF circulates through the entire ventricular system and reaches various cisterns via physiologic apertures. As a CSF-brain barrier hardly exists, CSF partially penetrates into the brain parenchyma, quasi-communicating with the interstitial fluid (ISF) [17], particularly when severe IVH occurs (compare Fig. 1a–d). Due to arterial pulsation and inspiration, the glymphatic system (see below) participates in driving the CSF/ISF flow (in IVH conditions together with blood-derived solutes) forward to the perivascular Virchow-Robin space, passing through the brain parenchyma and alongside cerebral vessels into the subarachnoid space [17, 18]. In the cortex, CSF is mainly resorbed by arachnoid granulations (pacchionian granulations) allowing the fluid to return into the venous circulation (Fig. 2). Other parts leave the subarachnoid space alongside larger cranial nerves and elsewhere, reaching the peripheral lymphatic system and then the venous circulation [16,17,18].
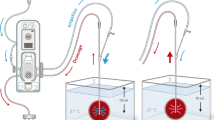
Pathophysiological mechanisms after intraventricular hemorrhages including particular changes after intraventricular rt-PA treatment. a An overview of the brain and the ventricular system including the CSF flow. b A schematic illustration of the most important functional parts of the parenchymal CSF/ISF pathways and the so-called glymphatic system. a Intraventricular blood and rt-PA predominately affect different brain barriers, the glymphatic system, and other brain structures clearing the CSF/ISF. The CSF is produced by the choroid plexus and initially circulates in the ventricular system before inflowing the interstitial space of the brain parenchyma via certain perivascular routes and through more or less tight brain barriers. At this stage, the CSF is called ISF building the distinguished neuronal and glial extracellular microenvironment, which may also contain waste products. ISF leaves the parenchyma via multiple routes such as the perivascular glymphatic system, thereby reappearing as CSF (external CSF). CSF of the subarachnoid space near the sagittal sinus is taken up by the pacchionian granulations that direct the fluid into the venous circulation, guaranteeing a steady state of CSF production and resorption. b After intraparenchymal and/or intraventricular hemorrhage, blood including its solutes and degradation products enters the interstitial space thus disturbing the microenvironment and the neuronal and glial functions. This “blood cocktail” destabilizes brain barriers to a certain extent, therefore entering the interstitial space by various short cuts. This cerebral barrier dysfunction is further enhanced by the use of intraventricular rt-PA application. More importantly, therapeutic rt-PA resolves the (intraventricular) blood clot in a shorter time period compared to the physiologic pathways, thereby increasing the concentration of the “blood cocktail” in the CSF/ISF including all devastating consequences for the microenvironment such as cellular dysfunction and death. Please see further detailed explanation in the main text body. Arrows signify direction of CSF/ISF flow
Cerebrospinal and Interstitial Fluid Flow after Intraventricular Hemorrhage
During and after IVH, blood-derived solutes, e.g., thrombin, potassium, and other vaso-/endothelium-active substances, affect the distinct environment of the brain parenchyma, particularly the neurovascular unit (NVU) [11, 19, 20] and the CSF-generating and CSF-clearing mechanisms [11, 21]. The NVU is the conceptual unity of brain cells (neurons, astrocytes, etc.), immune cells, pericytes, endothelial cells, and other blood vessel cells [21]. Overall, it is now recognized as a core signaling unit within the cerebrovascular network, regulating blood supply to the brain depending on functional demand, thereby guaranteeing brain homeostasis. Similarly, the CSF serves a variety of functions including supplying nutrients and clearing waste products. In this, it works in conjunction with the glymphatic system (Fig. 2b), which appears to be a crucial paravascular clearing mechanism for brain waste products [17, 18, 22]. Indeed, the glymphatic system may help to clear blood derivatives from the CSF/ISF after IVH in general, but particularly after therapeutically boosted plasmin-mediated clot lysis [17, 18]. However, the function of the glymphatic system, as well as of the pacchionian granulations and choroid plexuses, could be impaired in severe IVH by blood derivatives including albumin and fibrin resulting in disturbed CSF flow and various forms of hydrocephalus [2, 4, 5, 18, 20, 22].
Pathophysiologic Sequelae After Intraventricular Hemorrhage and rt-PA Treatment
Several clinical trials on IVH with rt-PA treatment have been conducted in the last decade. Table 1 provides an overview of important clinical trials investigating treatment options, occurrence of hydrocephalus, and outcome after IVH. After these trials, particularly after CLEAR III and the recently published related sub-studies [11,12,13,14,15], however, it still remains unclear whether fast clot lysis may decrease the pathophysiologic problem of blood plus its solutes flooding the ventricular system and subsequently the brain parenchyma/ISF, or whether fast clot lysis may augment this problem. One could speculate that intraventricular rt-PA may add to the initial damage after IVH by quickly overwhelming physiological clearing routes and specific structures in the short time frame of iatrogenic intensified clot lysis. Although our hypothesis appears to be fairly straightforward from a physiologic point of view, more basic science and clinical studies are needed to draw final conclusions. On the other hand, the rationale behind the CLEAR III trial was strong and the positive results regarding mortality were promising [7, 11]. Moreover, other authors discussed further benefits and other indications of rt-PA perhaps supporting the glymphatic system [22]. At the same time, the neutral results regarding the primary outcome measure after rt-PA in IVH appear disappointing [11].
The question still remains whether blood of any aggregate status should be therapeutically cleared by using the physiologic parenchymal CSF/ISF routes, such as the glymphatic system [18], thereby potentially inducing secondary brain cell damage and barrier impairment (Fig. 2b). Alternatively, it may be better to remove the blood burden before its components affect the ISF, the glymphatic system, and thereby directly the brain parenchyma cells including the NVU and the blood-brain barrier (BBB).
Fisher considered an organ-specific (including a brain-specific) coagulation and plasmin activity [23]. Particularly in the brain, the endogenous plasmin-mediated clot lysis system is known to function efficiently in extravascular cerebral compartments [23, 24]. In addition, it is a well-recognized clinical observation, and most neurosurgeons know exactly that CSF interferes with the coagulation, which barely reaches its final stage in the brain parenchyma or cerebral fluids: a persistently stable clot [23, 24]. This fact may be due to a lack of cerebral transglutaminase activity in CSF/ISF, such as seen in acquired coagulation factor XIII deficiency in chronic subdural hematoma/hemorrhage patients [24]. Application of intraventricular rt-PA further amplifies the endogenous plasmin system with anti-coagulation characteristics of the CSF, leading not only to timely intraventricular clot lysis but also to an increased cerebral inflammatory response [11, 13]. The question arises of whether fast clot lysis in the CSF beyond the endogenous lytic rate helps or harms IVH patients. Plasmin-/plasminogen-boosted clot lysis using rt-PA treatment subsequently opens and impairs and may thus harm important brain barriers such as the BBB [25] or the BCSFB [26], thereby affecting brain cells as well [27]. It is unknown whether the endogenous, i.e., intrinsic plasmin activity, represents a physiological strategy to moderately open certain brain barriers, thereby increasing fluid turnover and clearance of the CSF/ISF from harmful blood solutes. On the other hand, rt-PA itself is a powerful drug, but it is also known to induce serious side-effects in brain parenchyma and in particular at the NVU; for a review, see [27]. CSF inflammation after IVH is not only dependent on the initial volume of the IVH; intraventricular rt-PA further augments this inflammatory response, even after correcting for initial IVH volume [13]. However, although this augmented inflammatory response may harm the NVU, it was not associated with a noticeably worse modified Rankin scale score 180 days after IVH [13].
Moreover, various additional pathophysiologic mechanisms are relevant for ICH/IVH such as microglia activation, alterations of the interleukin levels, and/or other neuroimmunological responses to blood and its derivatives in the brain and CSF compartments. These specific aspects are out of the scope of this focused review and should be discussed elsewhere.
Future Directions
In general, and for future research, another fact seems to be important: Dissolution of blood (clots) in a fluid (CSF/ISF) does not imply its subsequent removal. In clinical practice, a unique blood removal approach would require a second CSF catheter. This could facilitate volume-neutral addition of artificial CSF, resulting in higher fluid turnover with increased external drainage, thereby leading to clearance of blood from the ventricles before entering the brain parenchyma/ISF. In a recent clinical trial of IVH patients, intraventricular rt-PA treatment plus additional lumbar drainage was shown to reduce permanent shunt dependency after ICH/IVH [28] and thus may be protecting the endogenous “clearance” systems of the brain. Theoretically, even CSF dialysis or apheresis might be feasible with or without intraventricular rt-PA treatment. This technique could be considered as advantageous, because the use of larger CSF catheters alone did not improve the outcome of IVH patients [29]. Other interesting therapeutic options may be (a) the pharmacologic support of the glymphatic system by dexmedetomidine to further increase clearance of blood-derived waste products particularly in the parenchyma [30] or (b) the pharmacologic support of key mechanisms of the NVU e.g. with low-dose lithium to stabilize endothelial cytosolic calcium homeostasis, decrease myosin light chain phosphorylation, thereby improving endothelial barrier, and vascular smooth muscle function [31,32,33]. Using these approaches means potentially mitigating IVH- and rt-PA-induced impairment of the glymphatic system and the NVU dysfunctions. Therefore, further basic research is needed in this field. One should keep in mind, however, that structure and function of the glymphatic system are still not entirely understood and discussed. Most authors believe, but a few doubt the widespread continuum of the glymphatic system or the plausibility of bulk flow therein [34, 35]. Clinical trials may not fully answer important questions regarding the human glymphatic system and the best treatment options after IVH (Table 1). Ultimately, only further translational cerebrovascular research together with subsequent well-designed clinical trials, such as the recent ones [11,12,13,14,15, 28,29,30, 32, 36], may verify that individual IVH patients benefit from therapeutic CSF clearing and removal strategies [37, 38].
References
Jaffe J, Melnychuk E, Muschelli J, Ziai W, Morgan T, Hanley DF, et al. Ventricular catheter location and the clearance of intraventricular hemorrhage. Neurosurgery. 2012;70(5):1258–63; discussion 63-4. https://doi.org/10.1227/NEU.0b013e31823f6571.
Maas MB, Nemeth AJ, Rosenberg NF, Kosteva AR, Prabhakaran S, Naidech AM. Delayed intraventricular hemorrhage is common and worsens outcomes in intracerebral hemorrhage. Neurology. 2013;80(14):1295–9. https://doi.org/10.1212/WNL.0b013e31828ab2a7.
Nowinski WL, Gomolka RS, Qian G, Gupta V, Ullman NL, Hanley DF. Characterization of intraventricular and intracerebral hematomas in non-contrast CT. Neuroradiol J. 2014;27(3):299–315. https://doi.org/10.15274/NRJ-2014-10042.
Rabinstein AA, Anderson CD. Time is brain also counts for ICH. Neurology. 2015;84(10):970–1. https://doi.org/10.1212/WNL.0000000000001349.
Witsch J, Bruce E, Meyers E, Velazquez A, Schmidt JM, Suwatcharangkoon S, et al. Intraventricular hemorrhage expansion in patients with spontaneous intracerebral hemorrhage. Neurology. 2015;84(10):989–94. https://doi.org/10.1212/WNL.0000000000001344.
Ziai WC, Nyquist PA, Hanley DF. Ventriculostomy and lytic therapy for intracerebral hemorrhage. Front Neurol Neurosci. 2015;37:130–47. https://doi.org/10.1159/000437118.
Ziai WC, Tuhrim S, Lane K, McBee N, Lees K, Dawson J, et al. A multicenter, randomized, double-blinded, placebo-controlled phase III study of Clot Lysis Evaluation of Accelerated Resolution of Intraventricular Hemorrhage (CLEAR III). Int J Stroke. 2014;9(4):536–42. https://doi.org/10.1111/ijs.12097.
Herrick DB, Ziai WC, Thompson CB, Lane K, McBee NA, Hanley DF. Systemic hematologic status following intraventricular recombinant tissue-type plasminogen activator for intraventricular hemorrhage: the CLEAR IVH Study Group. Stroke. 2011;42(12):3631–3. https://doi.org/10.1161/STROKEAHA.111.625749.
Naff N, Williams MA, Keyl PM, Tuhrim S, Bullock MR, Mayer SA, et al. Low-dose recombinant tissue-type plasminogen activator enhances clot resolution in brain hemorrhage: the intraventricular hemorrhage thrombolysis trial. Stroke. 2011;42(11):3009–16. https://doi.org/10.1161/STROKEAHA.110.610949.
Webb AJ, Ullman NL, Mann S, Muschelli J, Awad IA, Hanley DF. Resolution of intraventricular hemorrhage varies by ventricular region and dose of intraventricular thrombolytic: the Clot Lysis: Evaluating Accelerated Resolution of IVH (CLEAR IVH) program. Stroke. 2012;43(6):1666–8. https://doi.org/10.1161/STROKEAHA.112.650523.
Hanley DF, Lane K, McBee N, Ziai W, Tuhrim S, Lees KR, et al. Thrombolytic removal of intraventricular haemorrhage in treatment of severe stroke: results of the randomised, multicentre, multiregion, placebo-controlled CLEAR III trial. Lancet. 2017;389(10069):603–11. https://doi.org/10.1016/S0140-6736(16)32410-2.
Fam MD, Pang A, Zeineddine HA, Mayo S, Stadnik A, Jesselson M, et al. Demographic risk factors for vascular lesions as etiology of intraventricular hemorrhage in prospectively screened cases. Cerebrovasc Dis. 2017;43(5–6):223–30. https://doi.org/10.1159/000458452.
Fam MD, Zeineddine HA, Eliyas JK, Stadnik A, Jesselson M, McBee N, et al. CSF inflammatory response after intraventricular hemorrhage. Neurology. 2017;89(15):1553–60. https://doi.org/10.1212/WNL.0000000000004493.
Murthy SB, Awad I, Harnof S, Aldrich F, Harrigan M, Jallo J, et al. Permanent CSF shunting after intraventricular hemorrhage in the CLEAR III trial. Neurology. 2017;89(4):355–62. https://doi.org/10.1212/WNL.0000000000004155.
Fam MD, Hanley D, Stadnik A, Zeineddine HA, Girard R, Jesselson M, et al. Surgical performance in minimally invasive surgery plus recombinant tissue plasminogen activator for intracerebral hemorrhage evacuation phase III clinical trial. Neurosurgery. 2017;81(5):860–6. https://doi.org/10.1093/neuros/nyx123.
Oreskovic D, Rados M, Klarica M. Role of choroid plexus in cerebrospinal fluid hydrodynamics. Neuroscience. 2017;354:69–87. https://doi.org/10.1016/j.neuroscience.2017.04.025.
Dreha-Kulaczewski S, Joseph AA, Merboldt KD, Ludwig HC, Gartner J, Frahm J. Identification of the upward movement of human CSF in vivo and its relation to the brain venous system. J Neurosci. 2017;37(9):2395–402. https://doi.org/10.1523/JNEUROSCI.2754-16.2017.
Iliff JJ, Wang M, Liao Y, Plogg BA, Peng W, Gundersen GA, et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid beta. Sci Transl Med. 2012;4(147):147ra11. https://doi.org/10.1126/scitranslmed.3003748.
Bosche B, Graf R, Ernestus RI, Dohmen C, Reithmeier T, Brinker G, et al. Recurrent spreading depolarizations after subarachnoid hemorrhage decreases oxygen availability in human cerebral cortex. Ann Neurol. 2010;67(5):607–17. https://doi.org/10.1002/ana.21943.
Macdonald RL. Delayed neurological deterioration after subarachnoid haemorrhage. Nat Rev Neurol. 2014;10(1):44–58. https://doi.org/10.1038/nrneurol.2013.246.
Iadecola C. The neurovascular unit coming of age: a journey through neurovascular coupling in health and disease. Neuron. 2017;96(1):17–42. https://doi.org/10.1016/j.neuron.2017.07.030.
Gaberel T, Gakuba C, Goulay R, Martinez De Lizarrondo S, Hanouz JL, Emery E, et al. Impaired glymphatic perfusion after strokes revealed by contrast-enhanced MRI: a new target for fibrinolysis? Stroke. 2014;45(10):3092–6. https://doi.org/10.1161/STROKEAHA.114.006617.
Fisher MJ. Brain regulation of thrombosis and hemostasis: from theory to practice. Stroke. 2013;44(11):3275–85. https://doi.org/10.1161/STROKEAHA.113.000736.
Bosche B, Molcanyi M, Noll T, Kochanek M, Kraus B, Rieger B, et al. Occurrence and recurrence of spontaneous chronic subdural haematoma is associated with a factor XIII deficiency. Clin Neurol Neurosurg. 2013;115(1):13–8. https://doi.org/10.1016/j.clineuro.2012.03.045.
Burggraf D, Martens HK, Dichgans M, Hamann GF. rt-PA causes a dose-dependent increase in the extravasation of cellular and non-cellular blood elements after focal cerebral ischemia. Brain Res. 2007;1164:55–62. https://doi.org/10.1016/j.brainres.2007.05.066.
Renu A, Laredo C, Lopez-Rueda A, Llull L, Tudela R, San-Roman L, et al. Vessel wall enhancement and blood-cerebrospinal fluid barrier disruption after mechanical Thrombectomy in acute ischemic stroke. Stroke. 2017;48(3):651–7. https://doi.org/10.1161/STROKEAHA.116.015648.
Vivien D. Can the benefits of rtPA treatment for stroke be improved? Rev Neurol (Paris). 2017;173(9):566–71. https://doi.org/10.1016/j.neurol.2017.07.003.
Staykov D, Kuramatsu JB, Bardutzky J, Volbers B, Gerner ST, Kloska SP, et al. Efficacy and safety of combined intraventricular fibrinolysis with lumbar drainage for prevention of permanent shunt dependency after intracerebral hemorrhage with severe ventricular involvement: a randomized trial and individual patient data meta-analysis. Ann Neurol. 2017;81(1):93–103. https://doi.org/10.1002/ana.24834.
Gilard V, Djoubairou BO, Lepetit A, Metayer T, Gakuba C, Gourio C, et al. Small versus large catheters for ventriculostomy in the management of intraventricular hemorrhage. World Neurosurg. 2017;97:117–22. https://doi.org/10.1016/j.wneu.2016.09.105.
Benveniste H, Lee H, Ding F, Sun Q, Al-Bizri E, Makaryus R, et al. Anesthesia with dexmedetomidine and low-dose isoflurane increases solute transport via the glymphatic pathway in rat brain when compared with high-dose isoflurane. Anesthesiology. 2017;127(6):976–88. https://doi.org/10.1097/ALN.0000000000001888.
Bosche B, Molcanyi M, Noll T, Rej S, Zatschler B, Doeppner TR, et al. A differential impact of lithium on endothelium-dependent but not on endothelium-independent vessel relaxation. Prog Neuro-Psychopharmacol Biol Psychiatry. 2016;67:98–106. https://doi.org/10.1016/j.pnpbp.2016.02.004.
Bosche B, Molcanyi M, Rej S, Doeppner TR, Obermann M, Muller DJ, et al. Low-dose lithium stabilizes human endothelial barrier by decreasing MLC phosphorylation and universally augments cholinergic vasorelaxation capacity in a direct manner. Front Physiol. 2016;7:593. https://doi.org/10.3389/fphys.2016.00593.
Bosche B, Schafer M, Graf R, Hartel FV, Schafer U, Noll T. Lithium prevents early cytosolic calcium increase and secondary injurious calcium overload in glycolytically inhibited endothelial cells. Biochem Biophys Res Commun. 2013;434(2):268–72. https://doi.org/10.1016/j.bbrc.2013.03.047.
Bedussi B, van der Wel NN, de Vos J, van Veen H, Siebes M, VanBavel E, et al. Paravascular channels, cisterns, and the subarachnoid space in the rat brain: a single compartment with preferential pathways. J Cereb Blood Flow Metab. 2017;37(4):1374–85. https://doi.org/10.1177/0271678X16655550.
Faghih MM, Sharp MK. Is bulk flow plausible in perivascular, paravascular and paravenous channels? Fluids Barriers CNS. 2018;15(1):17. https://doi.org/10.1186/s12987-018-0103-8.
Staykov D, Huttner HB, Struffert T, Ganslandt O, Doerfler A, Schwab S, et al. Intraventricular fibrinolysis and lumbar drainage for ventricular hemorrhage. Stroke. 2009 Oct;40(10):3275–80. https://doi.org/10.1161/STROKEAHA.109.551945.
Garton T, Hua Y, Xiang J, Xi G, Keep RF. Challenges for intraventricular hemorrhage research and emerging therapeutic targets. Expert Opin Ther Targets. 2017;21(12):1111–22. https://doi.org/10.1080/14728222.2017.1397628.
Abdelmalik PA, Ziai WC. Spontaneous intraventricular hemorrhage: when should intraventricular tPA be considered? Semin Respir Crit Care Med. 2017;38(6):745–59. https://doi.org/10.1055/s-0037-1607991.
Acknowledgments
The authors acknowledge Sebastian Zachar, M.F.A. for creating the illustrations of Fig. 2 based on the drafts by BB and MM.
Funding
BB was supported by grants of the Deutsche Forschungsgemeinschaft (BO 4229/1-1, BO 4229/2-1, novel strategies to protect the neurovascular unit in cerebrovascular diseases) and PM by the European Union’s Seventh Framework Program (FP7/2008–2013) under grant agreement 627951 (Marie Curie IOF), the German Academic Exchange Service DAAD PPP Canada program with funds of the German Federal Ministry of Education and Research (BMBF, grant no. 57212163), and the German Federal Ministry of Education and Research (BMBF, grant no. 16GW0191). PM is a fellow of the BIH Charité Clinician Scientist Program funded by the Charité – Universitätsmedizin Berlin and the Berlin Institute of Health.
Author information
Authors and Affiliations
Contributions
BB wrote the initial draft of the manuscript, which was intellectually extended by PM and MM, and finally re-edited by BB, PM, TD, JH, and MM. BB, TD, and MM created the drafts of the figures. All authors substantially contributed to the manuscript and approved the final version.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 16 kb)
Rights and permissions
About this article
Cite this article
Bosche, B., Mergenthaler, P., Doeppner, T.R. et al. Complex Clearance Mechanisms After Intraventricular Hemorrhage and rt-PA Treatment—a Review on Clinical Trials. Transl. Stroke Res. 11, 337–344 (2020). https://doi.org/10.1007/s12975-019-00735-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-019-00735-6