Abstract
Perinatal arterial ischemic stroke (AIS) is an important cause of long-term morbidity in children. Thus, there is an urgent need to better understand the mechanisms of stroke in newborns in order to develop effective treatment and prevention strategies. The purpose of this study was to assess brain perfusion within the first month of life in newborns with AIS. In this study, magnetic resonance imaging (MRI) and perfusion imaging by arterial spin labeling (ASL) were used to assess brain perfusion in four term newborns with AIS. One patient had a stroke within the territory of the right middle cerebral artery (MCA); the other three patients had a stroke within the territory of the left MCA. None of them displayed any hemorrhagic component. All four patients demonstrated abnormal brain perfusion in the stroke area. Cerebral blood flow (CBF) within the stroke area was increased in patient # 1. In all other three patients, CBF was decreased within the stroke center and increased in the periphery of the stroke area. These results show the feasibility of the ASL sequence in newborns with AIS and support its addition to the current MRI protocol used in these newborns as it provides useful information on brain hemodynamics. Its value for identifying salvageable tissue in newborns needs to be further assessed, as well as its potential role in stroke follow-up and for tissue-specific treatment screening.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Arterial ischemic stroke has one of its peak incidence around birth, with an incidence of 1/1,600 to 1/5,000 live-births [1–4]. Perinatal stroke may be symptomatic early during the neonatal period (i.e., seizures: usually focal seizures or recurrent apnea/desaturation) or may remain unrecognized until later when long-term impairment becomes evident [5–8]. When symptomatic during the neonatal period without any evident cause (such as, e.g., cardiac surgery or catheterization), clinical manifestations usually occur during the first week of life and mostly within the first 3 days of life [5–9], suggesting that the stroke likely happened during very late pregnancy, during birth, or no more than the first 1 to 2 days of life [2, 8, 10]. Neonatal seizures associated with stroke are most often easily controlled, and there is usually no recurrence of stroke events in the same patient [11]. Unfortunately, however, many children with perinatal stroke develop long-term impairment, such as motor impairment, developmental delay, cognitive or behavioral problems, or post-neonatal seizures [12, 13].
One major concern is that there is currently no other treatment for perinatal arterial strokes than supportive care, including assuring adequate oxygenation, glucose homeostasis, and temperature control (i.e., avoid hyperthermia), prevention of dehydration and anemia/polycythemia, and treatment of seizures or other evident conditions [8]. Especially there is a consensus to avoid treatment with antithrombotic medications in newborns with stroke [14–16]. Otherwise, recommendations for treatment of perinatal arterial stroke only exist for cardioembolic arterial ischemic stroke (i.e., treatment with low molecular weight or unfractioned heparin) or recurrent arterial ischemic stroke (i.e., treatment with antiplatelet or anticoagulant therapy) [14–16].
Thus, as perinatal stroke is an important cause of long-term morbidity in children, there is an urgent need to better understand the mechanisms of stroke in newborns in order to develop effective treatment and prevention strategies. In the adult stroke literature, studies of brain perfusion changes following the obstruction of one of the cerebral arteries have provided additional insight into this disease and the potential approaches to treat it. The aim of this study was to assess brain perfusion in newborns with arterial ischemic stroke to determine the pattern of brain perfusion abnormalities associated with perinatal stroke and thus understand better some of the physiopathology underlying this condition.
Subjects and Methods
Four term newborns with perinatal stroke admitted during their first month of life to the neonatal intensive care unit were studied. Each of them was scanned once for clinical purposes on days 2, 3, 5, or 17 of life. In each case, perfusion imaging by arterial spin labeling (ASL-PI) was added to the conventional sequences to assess brain perfusion. Any ventilatory support, pressor support, or sedation was maintained during the MRI scanning process; additional sedation was avoided. This study was approved by the Institutional Review Board.
MRI scans were performed using a 3 Tesla Siemens Magnetom Trio (Siemens HealthCare, Erlangen, Germany), using a 32-channel head coil (Siemens HealthCare, Erlangen, Germany) [17] or a standard 12-channel head coil. A pulsed arterial spin labeling (PASL) sequence (PICORE Q2TIPS) [18] was acquired together with high spatial resolution anatomic T1- and T2-weighted images and diffusion-weighted images. Anatomic sequences included a T1-weighted magnetization prepared rapid gradient echo and a T2-weighted fast spin echo. They were supplemented by single shot spin-echo echo-planar diffusion-weighted isotropic images. Apparent diffusion coefficient (ADC) maps were generated off-line. Regional cerebral blood flow maps were obtained from the Siemens ASL Postprocessing Functor (Siemens, Erlangen, Germany). Quantitative estimates of regional cerebral blood flow (CBF) were made using the formula described by Wang et al. [19]:
M 0 was estimated by measuring the fully relaxed signal intensity and ∆M by the average difference in signal between control and tag acquisitions. The conversion efficiency α was assumed to be 95% and the blood/tissue water partition coefficient λ to be 1.2 mL/g, with inversion times TI1/TI2 = 700/1,400 ms and the longitudinal relaxation time of blood T 1a = 1,500 ms [20]. The imaging slices were positioned axially covering the brain, and the acquisition order was ascending (inferior to superior) to reduce the required TI2. The labeling slab had a thickness of 50 mm and was positioned with a gap of 10 mm below the most proximal slice. The labeling slab thus covered the lower part of the head and the neck, but not the upper part of the chest, and thus not the heart. Quantification of regional CBF was performed using the rCBF images. When possible, manually drawn regions of interest (ROIs) were placed in four types of tissue: cortical gray matter (CGM) (within frontal, parietal, and occipital cortex), white matter (WM) (within frontal and posterior white matter and the centrum semiovale), and basal ganglia (BG) (within the lentiform nucleus, the posterior limb of internal capsule, and the thalamus), and within the stroke area, its edges, and symmetrically on the contralateral side. Stroke center and edges ROIs were defined based on CBF maps and were usually circular. Measurements were obtained in the right and left side of the cerebrum in several places for each of these four tissue regions in order to include variations of perfusion in these areas. Their size depended on the location of the ROIs. ROIs were always drawn by one observer, who was blinded to the knowledge of the patient’s characteristics and outcome. ROIs were manually drawn on the ASL data by simultaneously viewing the ASL data and the corresponding T2-weighted imaging; co-registration was not used. Motion during the MR scan may cause severe artifacts in the acquired images, especially the PASL images. This was minimized by wrapping the newborns in an MRI-compatible vacuum cushion. In addition, a 3D prospective acquisition correction was utilized with the PASL sequence for reducing motion-induced effects on magnetization history.
Conventional sequences obtained during the same MRI studies were used to define the extent of brain injury in these patients and to correlate it with brain perfusion measurements. Neuroradiologists, who were blinded to the clinical condition of the newborns, interpreted the brain MRI images (T1- and T2-weighted images and diffusion-weighted images).
Results
Four term neonates with perinatal stroke were studied (Table 1). One had a stroke within the territory of the right middle cerebral artery (patient # 1) (Fig. 1); the other three patients had a stroke within the territory of the left middle cerebral artery (patients # 2, 3, and 4) (Figs. 2a, 3a, and 4a). None of them displayed any hemorrhagic component. The stroke was demonstrated in each patient in a brain MRI performed after the patients started to develop seizures (i.e., 1, 2, and 3 days after the beginning of the seizures). Patients # 1 and 2 were scanned within the 24 h following the beginning of seizures on days of life 2 and 3; patient #3 was scanned on day of life 5, i.e., 2 days after the beginning of the seizures, and patient # 4 was scanned on day of life 17, i.e., 3 days after the beginning of the seizures. Size of the infarct was more extensive in patients # 3 and 4. In each case, the infarct was clearly visible on the apparent diffusion coefficient maps and on the diffusion-weighted images but was also demonstrated on the conventional T1- and T2-weighted imaging sequences.
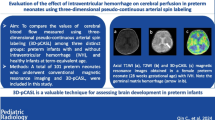
a Brain MRI on day of life 2 in patient # 1, comparison between perfusion map and images obtained from conventional sequences. A–D Area of infarction is noted within a portion of the right middle cerebral artery territory involving the right parietal lobe and, to a lesser extent, the right temporal lobe. The infarct is very well visible (thick arrows) on the apparent diffusion coefficient map (C) and diffusion-weighted images (D) but is also demonstrated on the conventional T1 (A)- and T2 (B)-weighted imaging sequences. E Cerebral blood flow map obtained by perfusion imaging by arterial spin labeling shows increased brain perfusion (thin arrows) in the area of infarction. b Ratio of cerebral blood flow in stroke side versus contralateral side in different regions of interest in patient # 1. Column bar graph (mean with SEM) representation. The different regions of interest consist of the stroke area versus the symmetric contralateral area, as well as the remaining cortical gray matter, white matter and basal ganglia. CBF in the stroke area is clearly increased compared to remaining of the brain
a Brain MRI on day of life 3 in patient # 2, comparison between perfusion map and images obtained from conventional sequences. A–D Area of infarction is noted within a portion of the left MCA territory involving the left postcentral gyrus and likely the inferior aspect of the left precentral gyrus. The infarct is very well visible (thick arrows) on the apparent diffusion coefficient map (C) and diffusion-weighted images (D) but is also demonstrated on the conventional T1 (A)- and T2 (B)-weighted imaging sequences. E CBF map obtained by ASL-PI shows decreased brain perfusion (curved arrows) in the center of the infarct but increased perfusion (thin arrows) on the periphery. b Ratio of CBF in stroke side versus contralateral side in different ROIs in patient # 2. Column bar graph (mean with SEM) representation. The ROIs consist of the stroke area versus the symmetric contralateral area, as well as the remaining CGM, WM, and BG. CBF in the stroke area is clearly decreased in the center and increased in the periphery compared to remaining of the brain
a Brain MRI on day of life 2 in patient # 3, comparison between perfusion map and images obtained from conventional sequences. A–D Extensive area of infarction is noted within the left MCA territory involving the left frontal lobe, the left parietal lobe, the left occipital lobe, the left temporal lobe, and left basal ganglia. The infarct is very well visible (thick arrows) on the apparent diffusion coefficient map (C) and diffusion-weighted images (D) but is also very well demonstrated on the conventional T1 (A)- and T2 (B)-weighted imaging sequences. E CBF map obtained by ASL-PI shows decreased brain perfusion (curved arrows) in the center of the infarct but increased perfusion (thin arrows) on the periphery. b Ratio of CBF in stroke side versus contralateral side in different ROIs in patient # 3. Column bar graph (mean with SEM) representation. The ROIs consist of the stroke area versus the symmetric contralateral area. CBF in the stroke area is clearly decreased in the center and increased in the periphery compared to remaining of the brain
a Brain MRI on day of life 17 in patient # 4, comparison between perfusion map and images obtained from conventional sequences. A–D Area of infarction is noted within the left MCA territory with extensive cortical and subcortical involvement, which is more pronounced in the posterior half of the territory, and also extending to the posterior lateral aspect of the left thalamus. The infarct is very well visible (thick arrows) on the apparent diffusion coefficient map (C) and diffusion-weighted images (D) but is also very well demonstrated on the conventional T1 (A)- and T2 (B)-weighted imaging sequences. E CBF map obtained by ASL-PI shows decreased brain perfusion (curved arrows) in the center of the infarct but increased perfusion (thin arrows) on the periphery. b Ratio of CBF in stroke side versus contralateral side in different ROIs in patient # 4. Column bar graph (mean with SEM) representation. The ROIs consist of the stroke area versus the symmetric contralateral area, as well as the remaining CGM, WM, and BG. CBF in the stroke area is clearly decreased in the center and increased in the periphery compared to remaining of the brain
All four patients demonstrated abnormal brain perfusion in the stroke area. CBF within the stroke area and adjacent regions was approximately quadruple in patient # 1 compared to the contralateral side (the ratio of CBF in stroke side versus contralateral brain side was 4.10 ± 0.91 within the stroke area) (Fig. 1b). In all of the other three patients, CBF was decreased within the stroke center and increased in the periphery of the stroke area compared to the contralateral side. The ratio of CBF in stroke side versus contralateral brain side was decreased within the stroke center to 0.02 ± 0.01 in patient # 2, 0.07 ± 0.02 in patient # 3 and 0.03 ± 0.01 in patient # 4 (Figs. 2b, 3b, and 4b). The ratio of CBF in stroke side versus contralateral brain side was increased in the periphery of the stroke area to 1.96 ± 0.30 in patient # 2, 2.92 ± 0.30 in patient # 3, and 1.71 ± 0.14 in patient # 4 (Fig. 2b, 3b, and 4b). In the remaining morphologically normal parts of the brain, CBF was comparable from one side to the other (the ratio of stroke side versus contralateral brain side was 1.02 ± 0.02 in the remaining brain).
Statistical analysis revealed the differences in ratio of CBF to be significantly increased in the stroke area and adjacent regions compared to the remaining parts of the brain (p < 0.0001). Although we recognize the caveat of running a statistical analysis on values obtained in only four patients, we nonetheless decided to present these results due to highly different values yielded by the analysis.
Discussion
This study is one of only a few studies measuring brain perfusion with ASL-PI in newborns [21, 22]. It is the only such study of brain perfusion in newborns with arterial stroke.
All four patients demonstrated abnormal brain perfusion in the stroke area. One patient displayed only hyperperfusion within the stroke area; the other three patients displayed hypoperfusion within the center of the stroke area and hyperperfusion in the periphery of the stroke. This pattern of brain perfusion abnormalities has been previously described in the adult stroke literature [23], but not in newborns. As typically described in adult stroke, irreversible damage progresses over time in an ischemic territory from the centre of the most severe blood flow reduction to the periphery with less disturbed perfusion [24]. This centrifugal progression of irreversible tissue damage is characterized by a complex cascade of interconnected perfusion, metabolic, molecular, and electrophysiological disturbances [24, 25]. Perfusion abnormalities are related to neurovascular coupling [25]. The hyperperfusion is related to “luxury perfusion,” which is thought to represent physiologic transient reperfusion (flow restoration by recanalization and/or collateral flow) that is a marker of favorable tissue outcome and may be protective of hemorrhagic transformation [26–28]. It is thought that functionally impaired tissue can survive and recover if sufficient reperfusion is re-established within a limited time period, which depends on the level of residual flow [24]. The hypoperfusion profile is more poorly understood than that of hyperperfusion. It has been implicated in three potential mechanisms in cases of stroke: oligemia, misery perfusion, and spreading ischemia [27–29]. Benign oligemia is defined by a physiologic mild decrease of regional CBF after the recovery from tissue depolarization in tissue that is not actually at risk of infarction [25]. Misery perfusion is the condition describing when CBF is progressively or chronically marginal due to severe obstruction of an artery and no longer sufficient to meet the oxygen requirement of the brain tissue [28, 29]. Finally, hypoperfusion associated with spreading ischemia has also been described as a pathological inverse hemodynamic response in response to neuronal injury, with a severe arteriolar constriction coupled to spreading depolarization, thus causing further lesion progression [25]. From a technical point of view, it is also possible that ASL underestimates CBF in regions of perfusion delay, giving this picture of hypoperfusion [30]. In the adult stroke literature, the debate over these different causes of hypoperfusion is still ongoing [29]. In newborns with perinatal stroke, the exact significance of these perfusion abnormalities is currently unclear. Further studies are required to determine if similar mechanisms as those described in adults are involved in the immature brain of a newborn. From the data in newborns presented here, the exact duration of the hyperperfusion and the hypoperfusion phases cannot be assessed. Follow-up brain MRIs would be useful in these patients to assess evolution of brain perfusion over time and to better understand these brain perfusion abnormalities. It would also be interesting to find better ways to identify early on these newborns, in order to be able to obtain a hyperacute imaging in these patients and understand, for example, if the hyperperfusion (luxury perfusion) in newborns with AIS might be caused by reperfusion following an initially reduced CBF.
As mentioned previously, stroke onset is difficult to identify in newborns compared to adults. In our four cases, the patients developed seizures, which prompted brain MRI for diagnosis purposes within 72 h after the onset of seizures. In each of these four cases, the stroke was very well visible on the diffusion sequences but also somewhat already visible on the conventional sequences, suggesting acute to subacute phase of the stroke [31]. By that time, in these four cases, areas of abnormal brain perfusion were mostly matching abnormalities on diffusion sequences; only the peri-infarct hyperperfusion in patient # 3 seemed larger than the infarct size evaluated on the other sequences. In future research in such newborns, co-registration will be developed between perfusion and diffusion maps, in order to compare more exactly ADC values in regions with decreased versus increased CBF. In the adult stroke literature, mismatch between diffusion and perfusion imaging has been used to determine tissue viability and differentiate between areas of irreversible infarct (“ischemic core”) and areas of salvageable but at-risk tissue (“ischemic penumbra”) [30, 32], in order to target more efficient treatments. However, even in adults, questions are now arising about whether treatments may be of benefit even if there is no more mismatch between diffusion and perfusion imaging, especially in patients with enough collaterals to expand the time-to-treatment window [27, 30]. If this last hypothesis is confirmed to also be true in newborns, it would likely mean that some ischemic tissue is salvageable from definitive infarct when early clinical symptoms permit diagnosis of the stroke when diffusion and perfusion abnormalities are still present, and thus, the long-term outcome of these newborns might be improved if appropriate treatment is offered. These patients may be candidates for therapeutic options such as for example endovascular recanalization (in patients with peri-infarct hyperperfusion) or treatments aimed at increasing blood flow (in patients with a hypoperfusion profile) [29, 32].
Further research is needed to investigate treatment options in newborns with perinatal stroke and to guide the selection patients who would be the best candidates for these therapies. Recognition of the perfusion abnormalities associated with perinatal stroke is an important step in the care and management of these patients and should facilitate research aimed at improving the flow state of the brain to improve their outcome. Understanding whether patterns of perfusion abnormalities are useful in predicting outcome of these patients [27] is another important step. Long-term follow-up was unfortunately not available in our patients but will be included in future research. Although the immature brain of a newborn is not simply a “small adult brain” and the mechanisms underlying perinatal stroke is certainly very unique compared to those underlying adult stroke [33], it is time to develop similar strategies for newborns as those described in adult stroke literature. These strategies may include imaging several times to localize occlusion, to exclude hemorrhage, to differentiate ischemia versus oligemia, to determine if there is tissue at risk (“penumbra”), to assess for recanalization and reperfusion, to study functional collateral circulation, and to evaluate the ultimate infarct size [26, 27]. Such strategies may help guide both acute and long-term therapy for perinatal stroke [26, 30].
Compared with other methods of measuring brain perfusion in newborns, including Doppler ultrasound, near-infrared spectroscopy, positron emission tomography, or xenon, only ASL-PI permits the direct assessment of CBF values in different areas of the brain without injecting contrast. Absolute measurements, despite their known limitations [20, 34], permit the noninvasive assessment of perfusion in different ROIs of newborns’ brains, as well as comparisons between newborns. However, some persistence of labeling in the major arteries presents a possible limitation to the accuracy of quantification by this method, since the entire label may not have reached the imaging plane. Regardless, the data presented here from newborns with perinatal stroke show the feasibility of the ASL method and support the addition of ASL-PI to current imaging protocol in newborns with perinatal stroke. As demonstrated, it can provide useful information on brain hemodynamics and, by combination with diffusion imaging, on the viability of the brain tissue [32]. Some data also suggest that ASL can provide good assessment of collateral flow to the ischemic zone [35].
Conclusion
ASL-PI performed during the first month of life in term newborns with perinatal arterial stroke demonstrates clear brain perfusion abnormalities associated with the infarcted area in the acute to subacute phase. The exact significance of these perfusion disturbances remains unclear, and these results warrant further study. In particular, future work should assess the value of ASL-PI in identifying salvageable tissue in newborns with perinatal stroke, as well as its potential role in stroke follow-up and for tissue-specific treatment screening.
Abbreviations
- AIS:
-
Arterial ischemic stroke
- ASL-PI:
-
Perfusion imaging by arterial spin labeling
- BG:
-
Basal ganglia
- CBF:
-
Cerebral blood flow
- CGM:
-
Cortical gray matter
- DWI:
-
Diffusion-weighted imaging
- MCA:
-
Middle cerebral artery
- MRI:
-
Magnetic resonance imaging
- ROIs:
-
Regions of interest
- WM:
-
White matter
References
Estan J, Hope P. Unilateral neonatal cerebral infarction in full term infants. Arch Dis Child Fetal Neonatal Ed. 1997;76:F88–93.
Lee J, Croen LA, Backstrand KH, Yoshida CK, Henning LH, Lindan C, et al. Maternal and infant characteristics associated with perinatal arterial stroke in the infant. JAMA. 2005;293:723–9.
Schulzke S, Weber P, Luetschg J, Fahnenstich H. Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants. J Perinat Med. 2005;33:170–5.
Laugesaar R, Kolk A, Tomberg T, Metsvaht T, Lintrop M, Varendi H, et al. Acutely and retrospectively diagnosed perinatal stroke: a population-based study. Stroke. 2007;38:2234–40.
Wu YW, Lynch JK, Nelson KB. Perinatal arterial stroke: understanding mechanisms and outcomes. Semin Neurol. 2005;25:424–34.
Govaert P, Ramenghi L, Taal R, de Vries L, Deveber G. Diagnosis of perinatal stroke I: definitions, differential diagnosis and registration. Acta Paediatr. 2009;98:1556–67.
Kirton A, deVeber G. Advances in perinatal ischemic stroke. Pediatr Neurol. 2009;40:205–14.
Chabrier S, Husson B, Dinomais M, Landrieu P, Nguyen The Tich S. New insights (and new interrogations) in perinatal arterial ischemic stroke. Thromb Res. 2011;127:13–22.
Govaert P, Ramenghi L, Taal R, Dudink J, Lequin M. Diagnosis of perinatal stroke II: mechanisms and clinical phenotypes. Acta Paediatr. 2009;98:1720–6.
Curry CJ, Bhullar S, Holmes J, Delozier CD, Roeder ER, Hutchison HT. Risk factors for perinatal arterial stroke: a study of 60 mother–child pairs. Pediatr Neurol. 2007;37:99–107.
Kurnik K, Kosch A, Sträter R, Schobess R, Heller C, Nowak-Göttl U. Childhood stroke study group recurrent thromboembolism in infants and children suffering from symptomatic neonatal arterial stroke: a prospective follow-up study. Stroke. 2003;34:2887–92.
Lee J, Croen LA, Lindan C, Nash KB, Yoshida CK, Ferriero DM, et al. Predictors of outcome in perinatal arterial stroke: a population-based study. Ann Neurol. 2005;58:303–8.
Sehgal A. Perinatal stroke: a case-based review. Eur J Pediatr. 2011. doi:10.1007/s00431-011-1509-3.
Monagle P, Chalmers E, Chan A, DeVeber G, Kirkham F, Massicotte P, et al. American College of Chest Physicians. Antithrombotic therapy in neonates and children: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133:887S–968S.
Roach ES, Golomb MR, Adams R, Biller J, Daniels S, Deveber G, et al. American Heart Association Stroke Council; Council on Cardiovascular Disease in the Young. Management of stroke in infants and children: a scientific statement from a Special Writing Group of the American Heart Association Stroke Council and the Council on Cardiovascular Disease in the Young. Stroke. 2008;39:2644–91.
Cnossen MH, van Ommen CH, Appel IM. Etiology and treatment of perinatal stroke; a role for prothrombotic coagulation factors? Semin Fetal Neonatal Med. 2009;14:311–7.
Wiggins GC, Triantafyllou C, Potthast A, Reykowski A, Nittka M, Wald LL. 32-channel 3 Tesla receive-only phased-array head coil with soccer-ball element geometry. Magn Reson Med. 2006;56:216–23.
Luh WM, Wong EC, Bandettini PA, Hyde JS. QUIPSS II with thin-slice TI1 periodic saturation: a method for improving accuracy of quantitative perfusion imaging using pulsed arterial spin labeling. Magn Reson Med. 1999;41:1246–54.
Wang J, Licht DJ, Jahng GH, Liu CS, Rubin JT, Haselgrove J, et al. Pediatric perfusion imaging using pulsed arterial spin labeling. J Magn Reson Imaging. 2003;18:404–13.
Cavuşoğlu M, Pfeuffer J, Uğurbil K, Uludağ K. Comparison of pulsed arterial spin labeling encoding schemes and absolute perfusion quantification. Magn Reson Imaging. 2009;27:1039–45.
Miranda MJ, Olofsson K, Sidaros K. Noninvasive measurements of regional cerebral perfusion in preterm and term neonates by magnetic resonance arterial spin labeling. Pediatr Res. 2006;60:359–63.
Wintermark P, Hansen A, Gregas MC, Soul J, Labrecque M, Robertson RL, Warfield SK. Brain perfusion in asphyxiated newborns treated with therapeutic hypothermia. AJNR Am J Neuroradiol 2011. doi:10.3174/ajnr.A2708.
Chalela JA, Alsop DC, Gonzalez-Atavales JB, Maldjian JA, Kasner SE, Detre JA. Magnetic resonance perfusion imaging in acute ischemic stroke using continuous arterial spin labeling. Stroke. 2000;31:680–7.
Heiss WD. The concept of the penumbra: can it be translated to stroke management? Int J Stroke. 2010;5:290–5.
Dreier JP. The role of spreading depression, spreading depolarization and spreading ischemia in neurological disease. Nat Med. 2011;17:439–47.
Lim CC, Petersen ET, Ng I, Hwang PY, Hui F, Golay X. MR regional perfusion imaging: visualizing functional collateral circulation. AJNR Am J Neuroradiol. 2007;28:447–8.
Viallon M, Altrichter S, Pereira VM, Nguyen D, Sekoranja L, Federspiel A, et al. Combined use of pulsed arterial spin-labeling and susceptibility-weighted imaging in stroke at 3T. Eur Neurol. 2010;64:286–96.
Yamashita E, Kanasaki Y, Fujii S, Tanaka T, Hirata Y, Ogawa T. Comparison of increased venous contrast in ischemic stroke using phase-sensitive MR imaging with perfusion changes on flow-sensitive alternating inversion recovery at 3 Tesla. Acta Radiol. 2011;52:905–10.
Klijn CJ, Kappelle LJ. Haemodynamic stroke: clinical features, prognosis, and management. Lancet Neurol. 2010;9:1008–17.
Burgess RE, Kidwell CS. Use of MRI in the assessment of patients with stroke. Curr Neurol Neurosci Rep. 2011;11:28–34.
Barkovich AJ. MR imaging of the neonatal brain. Neuroimaging Clin N Am. 2006;16:117–35.
Lövblad KO, Altrichter S, Viallon M, Sztajzel R, Delavelle J, Vargas MI, et al. Neuro-imaging of cerebral ischemic stroke. J Neuroradiol. 2008;35:197–209.
Jensen FE. Developmental factors regulating susceptibility to perinatal brain injury and seizures. Curr Opin Pediatr. 2006;18:628–33.
Zappe AC, Reichold J, Burger C, Weber B, Buck A, Pfeuffer J, et al. Quantification of cerebral blood flow in nonhuman primates using arterial spin labeling and a two-compartment model. Magn Reson Imaging. 2007;25:775–83.
van Laar PJ, van der Grond J, Hendrikse J. Brain perfusion territory imaging: methods and clinical applications of selective arterial spin-labeling MR imaging. Radiology. 2008;246:354–64.
Acknowledgments
Pia Wintermark receives research grant funding from the William Randolph Hearst Fund Award and the Thrasher Research Fund Early Career Award Program. The work of Simon K. Warfield is supported by NIH grants R01 RR021885, R01 GM074068, R03 EB008680, and P30 HD018655. The authors thank Aaron Johnstone for his thorough review of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wintermark, P., Warfield, S.K. New Insights in Perinatal Arterial Ischemic Stroke by Assessing Brain Perfusion. Transl. Stroke Res. 3, 255–262 (2012). https://doi.org/10.1007/s12975-011-0122-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-011-0122-0