Abstract
Depression is a common serious mental disorder with unclear pathogenesis. Currently, specific diagnostic biomarkers are yet to be characterized. The close homolog of L1 (CHL1) is a L1 family cell adhesion molecule involved in the regulation of neuronal survival and growth. Although genome-wide expression profiling of human lymphoblastoid cell lines (LCLs) reported neural cell adhesion molecule (NCAM) L1 as a tentative biomarker for selective serotonin reuptake inhibitor (SSRI) antidepressant response, the involvement of CHL1 in depression is unclear. In this study, using a well-established chronic unpredictable mild stress (CUMS) depression mouse model, we examined the mRNA and protein expression of CHL1 in normal control, CUMS, vehicle (VEH), fluoxetine (FLU), and clozapine (CLO) groups. We found that in the CUMS group, both mRNA and protein expression of CHL1 were downregulated in both the hippocampus and the cortex. Treatment of CUMS mice with FLU and CLO reversed CHL1 mRNA and protein expression. In the human study, we showed that CHL1 expression was significantly downregulated in monocytes of unipolar and bipolar depressive patients compared with healthy donors (HD) at both mRNA and protein levels. Consistently, ELISA showed that CHL1 levels in the serum of patients with depression were reduced and negatively correlated with their HRSD-21 scores. Further flow cytometry studies showed that the reduced number of CHL1 positive CD19+ and CD20+ B cells of patients with depression was subsequently reversed with antidepressant treatment. Our findings suggested that downregulation of CHL1 from both immune cells and the brain may be linked to the immunopathogenesis of depression. In conclusion, CHL1 may be an important predictive marker for both diagnosis and treatment outcome of depression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Depression, a mood disorder, can be classified as unipolar or bipolar. Currently, depression greatly threatens the mental health of patients and accounts for the third largest share of the world’s burden of disease in terms of years lost to disability (GBD 2016 Disease and Injury Incidence and Prevalence Collaborators, 2017). In recent years, immunological mechanisms and inflammation are increasingly implicated in the pathogenesis of depressive symptoms (Bhattacharya and Drevets 2017). Some reports suggest that activation of the peripheral immune system has been consistently associated with depression (Chamberlain et al. 2019). However, the underlying pathobiology behind inflammation in depression is not fully understood, and further investigations are required to identify specific diagnostic biomarkers. As an important step towards immunotherapy for treatment of depression, it is essential to explore the peripheral immune biomarkers which are linked closely to the development of this disease.
The interplay of chronic mild stress, neuroinflammation, and altered immune reactivity has been shown to be important for pathophysiology of depressive disorders (Vasileva et al. 2019). There are an increasing number of studies suggesting that the nervous system is closely related to the immune system (Boorman et al. 2016; Duda et al. 2019). Depression can cause T/B lymphocytes imbalance and functional decline of natural killer T (NKT) cells, subsequently leading to low immune function, infection susceptibility, tumor formation, and other diseases (Boorman et al. 2016). In addition, stress exposure causes the dysfunction of peripheral T lymphocytes, and the lack of CD4+ T cells protects mice with xanthine metabolic disorder from stress-induced anxiety-like behavior, implying that CD4+ T cells trigger anxiety-like behavior (Fan et al. 2019). Regulatory immune cells can be divided into regulatory T cells and regulatory B cells, which play a negative regulatory role in immune regulation and can induce immune tolerance (Pierini et al. 2015; Correale et al. 2014). B lymphocytes also have been reported to play a significant role in suppressing inflammatory immune responses and preventing autoimmunity through the production of interleukin-10 (IL-10) (Mavropoulos et al. 2016).
Cell adhesion molecules (CAMs) are distributed to the extracellular environment for the adhesion of epithelial cells (Tang et al. 2019). CHL1 is a transmembrane CAM with unique functions in neural signal transduction pathway (Schlatter et al. 2008). Recent genome-wide expression profiling of human lymphoblastoid cell lines has identified CHL1 as a putative SSRI antidepressant response biomarker (Morag et al. 2011; Oved et al. 2012). CHL1 belongs to the immunoglobulin (Ig) superfamily cell adhesion molecules at 3p26.3, also known as L1 family cell adhesion molecules (Senchenko et al. 2011). These adhesion molecules consist of six Ig-like domain and five fibronectin type III extracellular domains (Kenwrick et al. 2000). CHL1 is expressed at the cell surface throughout the central and peripheral nervous system, mainly in areas of high plasticity (Probst-Schendzielorz et al. 2015). In the developing nervous system, CHL1 plays a pivotal role in the regulation of neuronal differentiation and survival, neurite outgrowth, and axon guidance (Barao et al. 2015; Schmalbach et al. 2015). In the mature nervous system, CHL1 is involved in the regulation of synaptic activity and plasticity, including learning and memory (Pratte and Jamon 2009; Kolata et al. 2008). Single-nucleotide polymorphisms, deletions, and duplications in the CHL1 gene were associated with a higher risk of developing various neurological disorders including Parkinson’s disease, schizophrenia, autism, epilepsy, and intellectual disability (Shoukier et al. 2013; Palumbo et al. 2015; Li et al. 2016; Guseva et al. 2018; Shaltout et al. 2013). At the present, little is known about the association of CHL1 expressed by lymphocytes with the prognosis of depression.
In the current study, we hypothesize that the level of CHL1 in blood lymphocytes of depressive patients is consistent with CHL1 in the brain using our well-established chronic unpredictable mild stress (CUMS) depression mouse model. We propose that the CHL1 levels in lymphocytes of depressive patients will mirror the CHL1 levels in the brain. In order to test this hypothesis and characterize lymphocyte subtypes which predominately express CHL1 during depression, we first assessed the mRNA and protein expression levels of CHL1 in the brain of mice under chronic stress regime, and then we examined the mRNA and protein expression levels of CHL1 in lymphocytes isolated from depressive patients, as well as their serum CHL1 level. In addition, we explored the CHL1 level in peripheral B cell subsets of depressive patients with and without antidepressant treatment compared with healthy controls.
Material and Methods
CUMS Model
The study was carried out on 2-month-old male C57BL/6 J mice (23–27 g). All the animals were housed in groups of three to five per standard cage with food and water for at least 2 weeks before commencement of experimental tests. The animals were maintained under standard laboratory conditions (12 h light/dark cycle, 22 ± 1 °C, 52 ± 2% humidity). All experiments were performed in accordance with the Animal Management Rules of the Ministry of Health of the People’s Republic of China. All animal experiments were approved by the Animal Research Ethics Committee, Tianjin Medical University. All efforts were made to minimize the number of mice used and their suffering. For each treatment group in these series of experiments, 9–10 mice were used. The detailed CUMS procedures were described in our previous paper (Yang et al. 2017). The experimental schedules are depicted in Fig. 1a.
Effect of chronic treatment with antidepressants and CUMS on depressive and anxiety-like behavior. a Experimental protocol. b CUMS mice showed less sucrose consumption than the control mice. The treatment of FLU and CLO for 14 days significantly reversed the decrease of sucrose preference in CUMS mice. c, d A 4-week period of CUMS exposure resulted in a typical reduction in the total distance traveled and central square in mice, as compared with the controls in OFT. FLU and CLO treatment increased the total distance traveled and central square in the CUMS group. e, f FLU and CLO exposure significantly induced immobility time in FST and increased the number of climbs compared with VEH. g Treatment of antidepressant of CUMS mice significantly decreased anxiety-like behavior as displayed by increase in percentage of open/closed zone ratio in the EOM. CUMS, chronic unpredictable mild stress; VEH, vehicle; FLU, fluoxetine; CLO, clozapine; OFT, open-field test; FST, forced swim test; EOM, elevated zero maze. *p < 0.05, **p < 0.01, ***p < 0.001; #p < 0.05, ##p < 0.01, ###p < 0.001; all data are presented as mean ± SEM
Experimental Design and Antidepressant Drug Treatment
Fluoxetine hydrochloride (FLU) was purchased from Lilly S. A. Spain. Clozapine (CLO) was made by the Jiangsu Nhwa Pharmaceutical Group. Both FLU and CLO were dissolved separately in sterile saline. The animals were randomly divided: (group I) unstressed mice with free access to standard food and water, used as normal control (n = 10); (group II) mice after CUMS exposure (n = 10) for 28 days; (group III) CUMS-induced depression models treated with daily intraperitoneal (I.P.) injections of sterile saline (0.01 ml/g) for 14 days, used as a vehicle (VEH) group (n = 10); (group IV) CUMS-induced depression models treated with daily I.P. injections of FLU (n = 10) (18 mg/kg; 0.01 ml/g) for 14 days; and (group V) CUMS-induced depression models treated with daily I.P. injections of CLO (n = 10) (20 mg/kg; 0.01 ml/g) for 14 days. Both groups IV and V were used as the positive controls for antidepressant action.
Behavioral Testing (SPT, OFT, FST, O Maze)
Sucrose preference (SPT), open-field (OFT), forced swimming (FST), and O maze tests were performed as previously described (Yang et al. 2017; Yang et al. 2020). Detailed procedures are described in supplementary material. During the behavioral experiments, there were some accidents resulted in data loss from some rodents. Specifically, two bottles were found leaking after SPT, one in VEH group and one in CLO group. During the O maze test, one mouse in FLU group always jumped to the open arm. The data from these animals were excluded. So control (n = 10), CUMS (n = 10), VEH (n = 9), FLU (n = 9), and CLO (n = 9) were used in the analysis of behavioral data. At the end point, animals were humanely killed by an overdose of carbon dioxide via inhalation, and brain tissues were isolated for total RNA and protein extraction and stored at − 80 °C.
Human Subjects
Forty-four patients, 18–60 years old, both male and female, were recruited from Tianjin Mental Health Center in this study. Major depression was diagnosed according to the International Statistical Classification of Diseases and Related Health Problems 10th Revision (ICD-10) criteria. The control population consisted of forty-two healthy age- and gender-matched volunteers at the Second Hospital of Tianjin Medical University. We declare that our study was carried out in accordance with the latest version of the Declaration of Helsinki. The Ethics Committee of Tianjin Mental Hospital approved all procedures (KY2018K015). Patients were enrolled to participate in the study after they had signed the informed consents for participation. The patients were all drug-naive. We have excluded the participants who had history of autoimmune diseases, chronic inflammatory diseases, or other immune-associated disorders in this study. After having obtained the permission, peripheral blood samples were collected from healthy volunteers and patients. The details of the blood collection for these studies were given in the supplementary material.
Enzyme-Linked Immunosorbent Assay of CHL1 (Isolation of Serum)
Serum was assayed for CHL1 in duplicate, using an ELISA assay kit (L1CAM, cat.#SEQ118Hu, China), according to the protocol provided by the manufacturer. Briefly, ELISA plates were coated with protein G-purified mouse anti-CHL1 monoclonal antibody (2 μg/ml in coating buffer), blocked with PBS-BSA, loaded with serum at 1:5 dilution, detected with detection antibodies, and incubated with TMB, and OD values were obtained at 450 nm.
Quantitative Real-Time PCR
Total RNA was extracted from the entire cortex, hippocampus tissues from the rodents, and peripheral blood mononuclear cells (PBMCs) from participant donors, which were extracted by TRIzol® reagent (Sigma), following the manufacturer’s recommendation. The RNA samples were dissolved in 30 μl of DEPC-H2O and subsequently stored at − 80 °C. The cDNA was obtained using the reverse transcription kit (Thermo-Fisher Scientific, CA, USA). Quantitative real-time PCR was performed with SYBR Green (Takara, Japan) on CFX96 Touch™ Deep Well Real-Time PCR Detection system (Bio-Rad Laboratories, Inc., Hercules, CA, USA). Q-PCR was performed as follows: 95 °C for 3 min, and 39 cycles of 95 °C for 10 s and 60 °C for 30 s. The experiment was repeated in triplicate. Gene expression level of CHL1 was detected by running quantitative real-time PCR. The gene expression of β-actin/GAPDH was detected as internal control for total RNA used. Data were processed using the 2-ΔΔCTmethod. The primer sequences used are shown in Table 1.
Western Blotting Analysis (Protein Isolation of Lymphocytes)
Protein was extracted from the entire cortex, hippocampus tissues from the rodents, and PBMCs from participant donors harvested at indicated times using radio immunoprecipitation assay (RIPA) lysis buffer supplemented with proteinase inhibitors. Protein concentrations were measured using the BCA Protein Assay Kit (Thermo Scientific, Waltham, MA). Equal amounts of protein were separated by 10% SDS/PAG, followed by immunoblotting with the primary antibodies (rabbit anti-CHL1 antibody 1:1000, cat.#ab106269, abcam, China; mouse β-actin 1:1000, cat.#CW0097, CoWin Biosciences, China; rabbit anti-GAPDH antibody, 1:5000, cat.#ab 9485, abcam, China). Membranes were then incubated with peroxidase-conjugated secondary antibody, and specific bands were detected with Image J software (NIH, USA).
Flow Cytometry
To measure the CHL1 expression in PBMCs from healthy volunteers and depressive patients, human PBMCs were isolated from peripheral blood samples of healthy donors (HD) and depressive patients by lymphoprep separation liquid (Stemcell Technology, Norway). Freshly isolated PBMCs were then counted manually with a hemocytometer, and cell viability was measured by trypan blue (> 96%). PBMCs were stained with fluorescently conjugated monoclonal antibodies (mAbs) at 4 °C for 30 min as follows, respectively: BV421 anti-human CD3 (cat.#ab562427, BD), ECD anti-human CD4 (cat.#ab6604727, BC), APC-CY7 anti-human CD8 (cat.#ab641400, BD), FITC anti-human CD20 (cat.#ab347673, BD), PC7 anti-human CD19 (cat.#abIM3628, BC), V500 anti-human CD45 (cat.#ab560777, BD), PE anti-human CD171 (CHL1, cat.#ab371604, Biolegend), and APC mouse IgG1(cat.#ab400119, Biolegend). After rinse, cells were read on the flow cytometer (Cystek, Fremont, CA, USA), and data were analyzed with FlowJo vX0.7 software. Single-stained cells or OneComp eBeads (eBioscience, San Diego, CA) were used for compensation calculations. Unstained cells, cells with 7-AAD, and fluorescence minus one (FMO) controls were used for cytometry and gating set up.
Statistical Analyses
Data were presented as mean ± SEM and analyzed by SPSS 19.0 version. All statistical analysis was performed with Prism software from GraphPad (San Diego, CA, USA). For difference comparison within groups, Student’s t test was used for the two groups, one-way analysis of variance (ANOVA) for more than two groups, and two-way ANOVA for two groups with two factors. The p < 0.05 was considered statistically significant.
Results
Effects of Antidepressant Drugs on Depressive and Anxiety-Like Behavior
During the analysis of behavioral data, there were VEH (n = 9), FLU (n = 9), and CLO (n = 9). The effect of antidepressant drugs on depressive and anxiety-like behavior is shown in Fig. 1. After 4 weeks, the percentage of sucrose consumption in the sucrose preference test was significantly decreased in the CUMS mice group (n = 10) compared with the control group (n = 10) (Student’s t test, ***p < 0.001, t = 10.541, Fig. 1b), and antidepressant (FLU) and antipsychotic drugs (CLO) treatment reversed the decrease (###p < 0.001, ###p < 0.001, F(2,24) = 27.968, Fig. 1b). In the OFT, a 4-week period of CUMS exposure resulted in a typical reduction in the total distance traveled (***p < 0.001, t = 4.482, Fig. 1c) and central square (**p = 0.002, t = 3.559, Fig. 1d) in mice, as compared with the controls. We have found that antidepressants significantly reversed these behavioral impairments in CUMS mice compared with the VEH group, respectively (##p = 0.006, ##p = 0.004, F(2,24) = 6.515, Fig. 1c; ###p < 0.001, ###p < 0.001, F(2,24) = 14.435, Fig. 1d). The results showed that antidepressant treatment impacted the locomotor activity and exploratory activity in the OFT. In addition, CUMS exposure caused the increased immobility time (***p < 0.001, t = −10.255, Fig. 1e) in the FST, and treatment with antidepressant drugs (FLU, CLO) significantly decreased the immobility time in these mice (##p = 0.002, ##p = 0.009, F(2,24) = 6.693, Fig. 1e). At the same time, the number of climbings (***p < 0.001, t = 5.18, Fig. 1f) in the FST was declined in CUMS mice vs the control group, and treatment with antidepressant drugs (FLU, CLO) increased the numbers in these mice (#p = 0.01, ##p = 0.004, F(2,24) = 5.894, Fig. 1f). Analogously, in the EOM, the percentage of time spent in the open arms/closed zone was significantly decreased following CUMS compared with the controls (**p = 0.002, t = 3.599, Fig. 1g). The results suggested that antidepressants impacted the anxiety activity behaviors compared with the VEH group (##p = 0.004, #p = 0.02, F(2,24) = 5.636, Fig. 1g).
Effects of Antidepressant and Antipsychotic Drugs on CHL1 in the Brain of CUMS Mice
Expression of CHL1 in the cortex and hippocampus was evaluated by real-time PCR (Fig. 2a, c) and Western blotting (Fig. 2b, d). The mRNA and protein level of CHL1 were lower in the CUMS group than that of the control group both in the cortex (*p = 0.029, t = 2.547, Fig. 2a; ***p < 0.001, t = 8.496, Fig. 2b) and hippocampus (*p = 0.022, t = 2.772, Fig. 2c; ***p < 0.001, t = 10.779, Fig. 2d). In order to assess whether antidepressant and antipsychotic drugs could regulate the expression of CHL1, we examined CHL1 expression in CUMS mice treated with FLU and CLO. The mRNA level of CHL1 in the cortex and hippocampus was significantly increased in the FLU group (###p < 0.001, F(2,24) = 10.965, Fig. 2a; #p = 0.027, F(2,24) = 11.074, Fig. 2c) and CLO group (##p = 0.003, F(2,24) = 10.965, Fig. 2a; ###p < 0.001, F(2,24) = 11.074, Fig. 2c) compared with the VEH group. Consistently, the protein level of CHL1 was also increased in the treatment with FLU (#p = 0.03, F(2,24) = 20.264, Fig. 2b; ##p = 0.009, F(2,24) = 48.982, Fig. 2d) and CLO (###p < 0.001, F(2,24) = 20.264, Fig. 2b; ###p < 0.001, F(2,24) = 48.982, Fig. 2d) compared with the VEH group in the cortex and hippocampus.
Effect of antidepressants on the expression of CHL1 mRNA and protein in the cortex and hippocampus. a, b The mRNA and protein expression of CHL1 are downregulated in the cortex. Treatment of CUMS mice with FLU and CLO reversed CHL1 mRNA and protein expression. c, d CHL1 mRNA and protein expression are downregulated in the hippocampus. Treatment of CUMS mice with FLU and CLO reversed CHL1 mRNA and protein expression. β-actin was detected as loading control. *p < 0.05, **p < 0.01, ***p < 0.001; #p < 0.05, ##p < 0.01, ###p < 0.001; all data are presented as mean ± SEM
CHL1 Is Downregulated in the Serum and PBMCs in the Patients with Major Depressive Disorder
The demographic data of the enrolled depressive patients and normal donors was shown in Table 2. There were no significant differences of the average ages and WBC between normal group and patient group (p = 0.27, t = − 1.113; p = 0.318, t = − 1.136, Student’s t test). To examine whether CHL1 in the PBMCs of the enrolled depressive patients was downregulated, we performed real-time PCR on the cell lysates of PBMCs from patients and controls. The CHL1 mRNA level in PBMCs (***p < 0.001, t = 8.229, Fig. 3a) was reduced in the depressive group (n = 44) compared with the normal group (n = 42). Moreover, the protein expression of CHL1 in PBMCs (***p < 0.001, t = 4.583, Fig. 3b) was significantly lower in the depressive group (n = 44) than in the normal group (n = 42). Finally, antidepressant therapy (n = 18) induced high amount of CHL1 production not only at the mRNA level (###p < 0.001, F(2,101) = 43.208, Fig. 3a) but also at the protein level (###p < 0.001, F(2,101) = 181.581, Fig. 3b) compared with the depressive group (n = 44).
The CHL1 level in PBMCs and serum is reduced in depression. a The PBMCs level of CHL1 mRNA was significantly decreased in major depressive patients compared with health controls. There was a significant difference between major depressive patients and treatment group. b CHL1 protein was significantly increased in therapy patients when compared with major depressive patients. Antidepressant therapy induced significantly high amount of CHL1 production. c The ELISA result of CHL1 was compared among health controls, major depressive patients, and therapy group. d The correlation between CHL1 and HRSD scores. PBMCs, peripheral blood mononuclear cells; ELISA, enzyme-linked immunosorbent assay; HRSD, Hamilton Rating Scale for Depression. *p < 0.05, **p < 0.01, ***p < 0.001; #p < 0.05, ##p < 0.01, ###p < 0.001; all data are presented as mean ± SEM
ELISA result showed that the CHL1 level in the depressive patients (n = 44) was significantly decreased in comparison with the normal donors (n = 42) (**p = 0.001, F(2,101) = 13.181, Fig. 3c). Before the release from hospital, the serum level of CHL1 in some enrolled depressive patients was significantly increased in the antidepressant treatment group (n = 18) (###p < 0.001, F(2,101) = 13.181, Fig. 3c) when compared with non-treated group (n = 44). The analysis of correlation between the relative CHL1 level in the serum and HRSD scores in patients was shown in Fig. 3d. There was significant negative correlation between CHL1 (n = 44, r = − 0.3879, p = 0.0093, Fig. 3d) and HRSD scores. The results indicated that the trend of CHL1 change in the PBMCs and serum was similar to that in the brain of CUMS mice (Fig. 2).
Downregulation of Blood Lymphocytes CHL1 on B Cells
To explore the potential contribution of the immune cell imbalance in the internal environment and any subpopulation of lymphocytes involved, we examined the distribution of immune cells and the expression of the CHL1 (CD171) on T/B cells from depressive patients. Peripheral blood lymphocytes from 23 normal donors, 26 depressive patients, and 16 treatment patients were phenotypically analyzed by flow cytometry for the expression of CD45, CD19, CD20, CD3, CD4, and CD8 surface markers (Fig. 4a). We next examined the frequency of the expression of CHL1 (CD171) on T/B cells from depressive patients (Fig. 5).
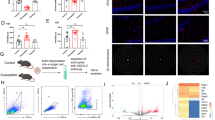
Representative density plots and frequency graphs of in immune subsets. a Representative images of flow cytometry for T and B lymphocytes in normal health control, depressive patients and therapy patients, gating of mononuclear cells isolated from the PBMCs. b Frequency of CD45+ lymphocytes was significantly decreased in the depressive group. These CD45+ lymphocytes from patients after treatment were increased compared with the depressive group. c, d Frequency of CD19+ lymphocytes and CD20+ lymphocytes was not statistically different from those in the depressive group compared with the normal group. They were slightly decreased in the treatment group compared with the depressive group. e No difference among the three groups in frequency of CD3+ lymphocytes. f Frequency of CD4+CD8−--CD3+ lymphocytes was significantly increased between the normal group and the depressive group. g Frequency of CD4−CD8+--CD3+ lymphocytes was decreased between the normal group and the depressive group. h Frequency of CD4+CD8+--CD3+ lymphocytes. i CD4/CD8 ratio was significantly increased in depressive patients compared with the normal group, but no significance was seen between the depressive group and the treatment group. *p < 0.05, **p < 0.01, ***p < 0.001; #p < 0.05, ##p < 0.01, ###p < 0.001; all data are presented as mean ± SEM
Histograms and graphs show CHL1 expression on immune subset. CD19/CD20 B cells exhibit high expression of CHL1. a Frequency of CHL1+ cells in CD45+ lymphocytes was increased in the treatment group. And there was no significance from those in the depressive group compared with the normal group. b Frequency of CHL1+ cells in CD19+ B cells was significantly decreased between the normal group and the depressive group. It was dramatically increased in the treatment group. c Frequency of CHL1+ cells in CD20+ B cells was consistent to the frequency of CHL1+ cells in CD19+ B cells. d Frequency of CHL1+ cells in CD3+ T cells. e Frequency of CHL1+ cells in CD4+CD8− --CD3+ T cells. f Frequency of CHL1+ cells in CD4−CD8+ − -CD3+ T cells. g There was a significant difference between the normal group and the depressive group in the frequency of CHL1+ cells in CD4+CD8+ − -CD3+ T cells. *p < 0.05, **p < 0.01, ***p < 0.001; #p < 0.05, ##p < 0.01, ###p < 0.001; all data are presented as mean ± SEM
As shown in Fig. 4, in contrast to the normal group, the frequency of CD45+ cells was significantly decreased in the depressive group (*p = 0.037, F(2,62) = 3.145, Fig. 4b). Moreover, the percentage of CD45+ leukocytes from patients after treatment was increased compared with the depressive group (#p = 0.045, F(2,62) = 3.145, Fig. 4b). We observed that CD19+ B cells (p = 0.44, F(2,62) = 1.141, Fig.4c) and CD20+ B cells (p = 0.681, F(2,62) = 0.578, Fig. 4d) were not statistically different from those in the depressive group compared with the normal group. Notably, they were slightly decreased in the treatment group compared with the depressive group (p = 0.411, F(2,62) = 1.141, Fig. 4c; p = 0.478, F(2,62) = 0.578, Fig. 4d). We examined the expression of CD3+ T cells and showed no difference among the three group (p = 0.839, F(2,62) = 0.034; p = 0.816, F(2,62) = 0.034, Fig. 4e). Interestingly, CD4+CD8−-CD3+ T cells from the depressive group (**p = 0.005, F(2,62) = 4.848, Fig. 4f) and the treatment group (p = 0.542, F(2,62) = 4.848, Fig. 4f) showed higher frequency than the normal group. On the opposite, CD4−CD8+-CD3+ T cells from the depressive group (*p = 0.013, F(2,62) = 3.663, Fig. 4g) and the treatment group (p = 0.746, F(2,62) = 3.663, Fig. 4g) showed significantly lower frequency than the normal group. However, cells expressing CD4+CD8+-CD3+ T cells seemed to be increased in the depressive group compared with the normal group (p = 0.109, F(2,62) = 1.316, Fig. 4h), but no significant difference was seen compared with the treatment group (p = 0.447, F(2,62) = 1.316, Fig. 4h). As the result, the ratio of CD4+/CD8+ was increased in peripheral blood of depressive patients compared with the normal group (**p = 0.009, F(2,62) = 3.931, Fig. 4i), but no significance was seen between the depressive group and the treatment group (p = 0.659, F(2,62) = 3.931, Fig. 4i). These results reveal that the change of CD45+ leukocytes, CD4+CD8−-CD3+ T cells, and CD4−CD8+-CD3+ T cells perhaps be associated with depression.
CHL1 (CD171) expression was examined by flow cytometry. As shown in Fig. 5, the expression of CHL1 (CD171) in CD45+ leukocytes was increased in the treatment group (###p < 0.001, F(2,62) = 16.698, Fig. 5a). And there was no significance from those in the depressive group compared with the normal group (p = 0.573, F(2,62) = 16.698, Fig. 5a). The analysis performed by flow cytometry showed the abundance expression of CHL1 (CD171) in CD19+/CD20+ B cells. There were around 17% CHL1 (CD171)+ in CD19+ B cells in the normal group. Percentage of CHL1 (CD171)+ in CD19+ B cells was decreased to 4% in the depressive group (***p < 0.001, F(2,62) = 44.588, Fig. 5b). In contrast, the percentage of CHL1 (CD171)+ in CD19+ B cells was dramatically increased in the treatment group (###p < 0.001, F(2,62) = 44.588, Fig. 5b). Consistently, the trend of CHL1 (CD171)+ in CD19+ B cells and CD20+ B cells (***p < 0.001, F(2,62) = 33.207; ###p < 0.001, F(2,62) = 33.207, Fig. 5c) was extremely similar. The expression of CHL1 (CD171) in the CD3+ T cells (p = 0.146, F(2,62) = 1.131, Fig. 5d), CD4+ T cells (p = 0.605, F(2,62) = 0.766, Fig. 5e), and CD8+ T cells (p = 0.229, F(2,62) = 0.994, Fig. 5f) was not different between the depressive group and the normal group. The expression of CHL1 (CD171) after treatment administration did not change in the CD3+ T cells (p = 0.737, F(2,62) = 1.131, Fig. 5d), CD4+ T cells (p = 0.221, F(2,62) = 0.766, Fig. 5e), and CD8+ T cells (p = 0.893, F(2,62) = 0.994, Fig. 5f). However, the CHL1 (CD171) expression in the CD4+CD8+ T cells of the depressive group was significantly higher than the normal group (***p < 0.001, F(2,62) = 9.119, Fig. 5g). No significant change of CHL1 in CD4+CD8+ T cells was seen between the depressive group and the treatment group (p = 0.858, F(2,62) = 9.119, Fig. 5g). Taken together, the results showed that CHL1 (CD171) was downregulated in the CD19+ and CD20+ B cell subpopulation, which could be recovered after treatment.
Discussion
The present study demonstrated that the protein and mRNA levels of CHL1 were downregulated in the brain of mice with chronic stress. Consistent with the animal experimental studies, the expression of CHL1 in the serum and PBMCs was also decreased in the depressive patients examined. CHL1 was preferentially expressed in CD19+/CD20+ B cells in the peripheral blood of normal subjects but was decreased in depressive patients. The treatment with antidepressants significantly reversed the biomarker in both rodents and patients. No significant reduction in the CHL1 expression in CD3+, CD4+, and CD8+ T cell subpopulations was found after different treatment. Our study suggests that CHL1 may contribute to pathogenesis of major depression and the dysfunction of immune cells and can be a tentative biomarker for depression.
The Level of CHL1 Is Decreased in the Brain of Mice with Chronic Stress and in PBMCs from Depressive Patients
Over 30% of depressed patients fail to reach sufficient remission after 2–4 weeks of SSRI treatment (Gelenberg 2010). Moreover, it usually takes several weeks to know if antidepressant drug treatment works in a patient. Using genome-wide expression profiling of human LCLs, CHL1 has been reported to be as a leading tentative SSRI sensitivity biomarker (Oved et al. 2012). In our experimental mice models, OFT and EOM tests showed both depressive and anxiety-like behavior, as reflected by a decreased locomotor activity, travel distance in the central square of the OFT, and a decreased time spent in the open arms. However, depressive behavior can be distinguished from anxiety-like behavior through SPT and FST examinations in which mice with depression-like phenotype have less sucrose consumption and a longer immobility time (Zhong et al. 2018). We confirmed that in our CUMS model, there were both depressive and anxiety-like behaviors. In this study, we found that the mRNA and protein level of CHL1 were reduced in the cortex and hippocampus after modeling of mild chronic stress, which is consistent with previous studies (Desarnaud et al. 2008; Laifenfeld et al. 2005a). These results indicate that chronic stress not only elicits depression and anxiety-like phenotypes but also influences expression of CHL1.
Consistent with the animal study, the expression of CHL1 was also decreased in the serum and PBMCs of the depressive patients, suggesting the reduction in CHL1 is a systemic reaction in the depressed patients. In contrast, the expression of CHL1 mRNA and protein was reported to be increased in the prefrontal cortex but decreased in the ventral parieto-occipital cortex, in the depressed patients (Laifenfeld et al. 2005b). In addition, another study reported reciprocal alteration in the expression of NCAM-140, and CHL1 mRNAs could be state dependent and associated with the pathophysiology of bipolar disorder (Wakabayashi et al. 2008). In this study, we collected peripheral blood samples from unipolar and bipolar patients. Our main finding was that the level of CHL1 in the serum was significantly reduced in the depressed patients. In this group, the level of CHL1 had a negative correlation with HRSD-21 scores for major depression severity. These results implicated that a reduction in CHL1 expression is associated with depression severity and may play important roles in mood disorders (Wakabayashi et al. 2008) and multiple neurobiological functions (Sandi 2004; Hochstrasser et al. 2010).
Antidepressant (FLU) and Antipsychotic (CLO) Drugs Restore the Level of CHL1
To further confirm the link between CHL1 and mood regulation, we measured whether antidepressant (FLU) and antipsychotic (CLO) drugs can change the CHL1 level in the brain. Our data showed that the first-line antidepressant drug SSRI (FLU) (Wong et al. 1974) reversed the CUMS-induced depression and anxiety-like behaviors and normalized the CHL1 expression in the cortex and hippocampus of mice brains. These results are consistent with previous studies reporting that chronic antidepressant treatments including FLU increased the MAP-2 (Yang et al. 2015) and BDNF transcriptional levels in rodent brains (Yang et al. 2020). Moreover, CLO reversed depressive and anxiety-like behavior resulted in an increased sucrose preference, total distance traveled, central square, and a decreased immobility time in the FST. CLO is a drug which is used in schizophrenia and other psychotic problems. It mainly blocks receptors in the brain for several neurotransmitter substances including serotonin, D2, D4, and NMDA receptors (Yang et al. 2015). Our study provides the first evidence supporting a novel mechanism underlying the efficacy of FLU and CLO in the treatment of depression, that is, to increase the CHL1 level in the brain of depressive subjects. The result also supports the link between CHL1 and serotoninergic systems in mood regulation.
Several reports demonstrated that the CHL1 level might predict responsiveness to SSRIs (Probst-Schendzielorz et al. 2015; Oved et al. 2012). They found that CHL1 was produced at lower levels in the most responsive cell lines and at higher levels in the least responsive cell lines from 58 depressed patients (Probst-Schendzielorz et al. 2015). They thought that paroxetine caused increased production of the ITGB3gene—whose protein product is thought to interact with CHL1 to promote the development of new neurons and synapses (Probst-Schendzielorz et al. 2015). However, a series of studies have shown that chronic stress can markedly affect hippocampal cell adhesion molecules (CAMs) expression (Bisaz et al. 2009). A chronic restraint procedure was found to diminish NCAM but increase expression of another neuronal CAM L1, in the hippocampus (Sandi 2004). According to the theories proposed by Blanpied et al., if the adhesion molecules are not in the correct position at the synapse, the synaptic structure will be destroyed, and the neurotransmitters will not be completed (Tang et al. 2016; Biederer et al. 2017). In the present study, we found that the serum level of CHL1 was significantly increased after antidepressant treatment of depressive patients. Furthermore, we also found that antidepressant therapy induced high amount of CHL1 mRNA and protein production in the PBMCs, raising the possibility of using their levels as biomarkers for major depression.
The Relationship Between Major Depression and the CHL1 Expression in the B/T Cells
Many studies reported that there was a close link between depression and immune disorders of the body and brain (Bullmore 2018; Lynall et al. 2019). Although depression is often associated with a reduction in cellular immune responses, other types of emotional disturbance and psychopathology can activate certain aspects of immunity (Lemieux et al. 2008). In the present study, depressed patients exhibit significantly lower percentage of CD45+ lymphocytes. The change of cells expressing CHL1 on CD45+ lymphocytes was consistent with total blood CD45+ lymphocytes. Reduced blood lymphocyte counts in depression could be reversed after antidepressant treatment, suggesting that CHL1 may influence lymphocytes function via an autocrine/paracrine pathway. Many researchers have reported that activation markers on T cells, in particular, have been found to be elevated in depression and anxiety-like behavior (Laumet et al. 2018; Fan et al. 2019). However, emerging evidence implicates that B cells homeostasis is likely to be involved in the depressive behavior (Ahmetspahic et al. 2018). In our cases, there were no differences in the percentage of CD19+, CD20+, and CD3+ cells among the study samples, whereas a significantly lower percentage of CHL1 expressed in CD19+/CD20+ B cells was found in depressed patients. The treatment with antidepressants obviously reversed the biomarker of CHL1+CD19+/CD20+ B cells in depressed patients. We are the first to have defined the specific changes in CHL1 expression in B cells but not in T cells. Furthermore, we found that a significantly increased CD4+CD8−-CD3+ cells and decreased percentage of CD4−CD8+-CD3+ cells in major depression, and the CD4+/CD8+ ratio was significantly increased. Therefore, we speculate that CHL1 expression could be an important diagnostic biomarker for depression and the response indicator to therapeutic interventions. The function of CHL1 in lymphocyte and immune function is not known, our finding that CHL1 expression in B cells warrants further investigation to elucidate its role in the immune regulation, such as in proliferation and differentiation.
Potential Relationship Between CHL1 and Synaptogenesis
Synapses are the functionally connected parts of neurons, and they are also the structural basis for information transmission in the nervous system (Biederer et al. 2017). Some studies have reported that synapses in the prefrontal cortex and hippocampus are reduced in animal experiments of depression, consistent with evidence of lower number of synapses, and corresponding lower expression of synaptic-function-related genes in the brain of depressed patients in postmortem (Kang et al. 2012; Duric et al. 2013). A recent study also shows that lower synaptic density is associated with depression severity by positron emission tomography (PET) in depressed patients (Holmes et al. 2019) and synaptic regeneration can maintain ketamine’s antidepressant effect in animal trials (Moda-Sava et al. 2019). In the mature nervous system, CHL1 was involved in regulation of synaptic activity and plasticity (Morellini et al. 2007; Andreyeva et al. 2010). Blanpied’s group also concerned about the activity of adhesion molecules, which may be an important part of transcellular nanoalignment of synaptic function (Biederer et al. 2017). These studies all point to the view that the relationship between CHL1 and synaptogenesis is critical for the pathogenesis of depression and likely the drug target of antidepressants. Our current investigation adds additional evidence that reduced CHL1 is associated with depression severity, consistent with the change in synaptic density. Furthermore, antidepressant treatment can increase the expression of CHL1 in the brain of mice with chronic stress and in PBMCs from depressive patients. Certainly, findings from this study provide further incentive to evaluate interventions that restore CHL1 and synaptic connections to treat depression. Further studies are important to elucidate whether CHL1 is directly involved in the pathogenesis of depression and the underlying pathogenic mechanisms by loss of function and/or gain of function experiments.
Conclusion
In summary, the present study modeled the depression in rodents and demonstrated that the downregulation of CHL1 strongly correlated with severity of depression. The downregulation of blood CHL1 in B cells but not T cells may play an important role in pathological immune microenvironments in depressed patient. In the future, CHL1 should be further explored in animal trials in order to confirm whether overexpression of CHL1 could relieve depressive and anxiety-like behaviors or vice versa downregulation/silencing of CHL1 expression could result in development of depression.
References
Ahmetspahic D, Schwarte K, Ambree O, Burger C, Falcone V, Seiler K, Kooybaran MR, Grosse L, Roos F, Scheffer J, Jorgens S, Koelkebeck K, Dannlowski U, Arolt V, Scheu S, Alferink J (2018) Altered B cell homeostasis in patients with major depressive disorder and normalization of CD5 surface expression on regulatory B cells in treatment responders. J NeuroImmune Pharmacol 13(1):90–99
Andreyeva A, Leshchyns'ka I, Knepper M, Betzel C, Redecke L, Sytnyk V, Schachner M (2010) CHL1 is a selective organizer of the presynaptic machinery chaperoning the SNARE complex. PLoS One 5(8):e12018
Barao S, Gartner A, Leyva-Diaz E, Demyanenko G, Munck S, Vanhoutvin T, Zhou L, Schachner M, Lopez-Bendito G, Maness PF, De Strooper B (2015) Antagonistic effects of BACE1 and APH1B-gamma-secretase control axonal guidance by regulating growth cone collapse. Cell Rep 12(9):1367–1376
Bhattacharya A, Drevets WC (2017) Role of neuro-immunological factors in the pathophysiology of mood disorders: implications for novel therapeutics for treatment resistant depression. Curr Top Behav Neurosci 31:339–356
Biederer T, Kaeser PS, Blanpied TA (2017) Transcellular Nanoalignment of synaptic function. Neuron 96(3):680–696
Bisaz R, Conboy L, Sandi C (2009) Learning under stress: a role for the neural cell adhesion molecule NCAM. Neurobiol Learn Mem 91(4):333–342
Boorman E, Zajkowska Z, Ahmed R, Pariante CM, Zunszain PA (2016) Crosstalk between endocannabinoid and immune systems: a potential dysregulation in depression? Psychopharmacology 233(9):1591–1604
Bullmore E (2018) The art of medicine: inflamed depression. Lancet 392(10154):1189–1190
Chamberlain SR, Cavanagh J, de Boer P, Mondelli V, Jones DNC, Drevets WC, Cowen PJ, Harrison NA, Pointon L, Pariante CM, Bullmore ET (2019) Treatment-resistant depression and peripheral C-reactive protein. Br J Psychiatry 214(1):11–19
Correale J, Farez MF, Ysrraelit MC (2014) Role of prolactin in B cell regulation in multiple sclerosis. J Neuroimmunol 269(1–2):76–86
Desarnaud F, Jakovcevski M, Morellini F, Schachner M (2008) Stress downregulates hippocampal expression of the adhesion molecules NCAM and CHL1 in mice by mechanisms independent of DNA methylation of their promoters. Cell Adhes Migr 2(1):38–44
Duda W, Curzytek K, Kubera M, Connor TJ, Fagan EM, Basta-Kaim A, Trojan E, Papp M, Gruca P, Budziszewska B, Leskiewicz M, Maes M, Lason W (2019) Interaction of the immune-inflammatory and the kynurenine pathways in rats resistant to antidepressant treatment in model of depression. Int Immunopharmacol 73:527–538
Duric V, Banasr M, Stockmeier CA, Simen AA, Newton SS, Overholser JC, Jurjus GJ, Dieter L, Duman RS (2013) Altered expression of synapse and glutamate related genes in post-mortem hippocampus of depressed subjects. Int J Neuropsychopharmacol 16(1):69–82
Fan KQ, Li YY, Wang HL, Mao XT, Guo JX, Wang F, Huang LJ, Li YN, Ma XY, Gao ZJ, Chen W, Qian DD, Xue WJ, Cao Q, Zhang L, Shen L, Tong C, Zhong JY, Lu W, Lu L, Ren KM, Zhong G, Wang Y, Tang M, Feng XH, Chai RJ, Jin J (2019) Stress-induced metabolic disorder in peripheral CD4(+) T cells leads to anxiety-like behavior. Cell 179(4):864–879 e819
GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. (2017). Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 390(10100):1211–1259
Gelenberg AJ (2010) A review of the current guidelines for depression treatment. J Clin Psychiatry 71(7):e15
Guseva D, Jakovcevski I, Irintchev A, Leshchyns'ka I, Sytnyk V, Ponimaskin E, Schachner M (2018) Cell adhesion molecule close homolog of L1 (CHL1) guides the regrowth of regenerating motor axons and regulates synaptic coverage of motor neurons. Front Mol Neurosci 11:174
Hochstrasser T, Weiss E, Marksteiner J, Humpel C (2010) Soluble cell adhesion molecules in monocytes of Alzheimer’s disease and mild cognitive impairment. Exp Gerontol 45(1):70–74
Holmes SE, Scheinost D, Finnema SJ, Naganawa M, Davis MT, DellaGioia N, Nabulsi N, Matuskey D, Angarita GA, Pietrzak RH, Duman RS, Sanacora G, Krystal JH, Carson RE, Esterlis I (2019) Lower synaptic density is associated with depression severity and network alterations. Nat Commun 10(1):1529
Kang HJ, Voleti B, Hajszan T, Rajkowska G, Stockmeier CA, Licznerski P, Lepack A, Majik MS, Jeong LS, Banasr M, Son H, Duman RS (2012) Decreased expression of synapse-related genes and loss of synapses in major depressive disorder. Nat Med 18(9):1413–1417
Kenwrick S, Watkins A, De Angelis E (2000) Neural cell recognition molecule L1: relating biological complexity to human disease mutations. Hum Mol Genet 9(6):879–886
Kolata S, Wu J, Light K, Schachner M, Matzel LD (2008) Impaired working memory duration but normal learning abilities found in mice that are conditionally deficient in the close homolog of L1. J Neurosci 28(50):13505–13510
Laifenfeld D, Karry R, Grauer E, Klein E, Ben-Shachar D (2005a) Antidepressants and prolonged stress in rats modulate CAM-L1, laminin, and pCREB, implicated in neuronal plasticity. Neurobiol Dis 20(2):432–441
Laifenfeld D, Karry R, Klein E, Ben-Shachar D (2005b) Alterations in cell adhesion molecule L1 and functionally related genes in major depression: a postmortem study. Biol Psychiatry 57(7):716–725
Laumet G, Edralin JD, Chiang AC, Dantzer R, Heijnen CJ, Kavelaars A (2018) Resolution of inflammation-induced depression requires T lymphocytes and endogenous brain interleukin-10 signaling. Neuropsychopharmacology 43(13):2597–2605
Lemieux A, Coe CL, Carnes M (2008) Symptom severity predicts degree of T cell activation in adult women following childhood maltreatment. Brain Behav Immun 22(6):994–1003
Li C, Liu C, Zhou B, Hu C, Xu X (2016) Novel microduplication of CHL1 gene in a patient with autism spectrum disorder: a case report and a brief literature review. Mol Cytogenet 9:51
Lynall ME, Turner L, Bhatti J, Cavanagh J, de Boer P, Mondelli V, Jones D, Drevets WC, Cowen P, Harrison NA, Pariante CM, Pointon L, Clatworthy MR, Bullmore E (2019) Peripheral blood cell-stratified subgroups of inflamed depression. Biol Psychiatry
Mavropoulos A, Simopoulou T, Varna A, Liaskos C, Katsiari CG, Bogdanos DP, Sakkas LI (2016) Breg cells are numerically decreased and functionally impaired in patients with systemic sclerosis. Arthritis Rheum 68(2):494–504
Moda-Sava RN, Murdock MH, Parekh PK, Fetcho RN, Huang BS, Huynh TN, Witztum J, Shaver DC, Rosenthal DL, Alway EJ, Lopez K, Meng Y, Nellissen L, Grosenick L, Milner TA, Deisseroth K, Bito H, Kasai H, Liston C(2019) Sustained rescue of prefrontal circuit dysfunction by antidepressant-induced spine formation. Science 364(6436)
Morag A, Pasmanik-Chor M, Oron-Karni V, Rehavi M, Stingl JC, Gurwitz D (2011) Genome-wide expression profiling of human lymphoblastoid cell lines identifies CHL1 as a putative SSRI antidepressant response biomarker. Pharmacogenomics 12(2):171–184
Morellini F, Lepsveridze E, Kahler B, Dityatev A, Schachner M (2007) Reduced reactivity to novelty, impaired social behavior, and enhanced basal synaptic excitatory activity in perforant path projections to the dentate gyrus in young adult mice deficient in the neural cell adhesion molecule CHL1. Mol Cell Neurosci 34(2):121–136
Oved K, Morag A, Pasmanik-Chor M, Oron-Karni V, Shomron N, Rehavi M, Stingl JC, Gurwitz D (2012) Genome-wide miRNA expression profiling of human lymphoblastoid cell lines identifies tentative SSRI antidepressant response biomarkers. Pharmacogenomics 13(10):1129–1139
Palumbo O, Fischetto R, Palumbo P, Nicastro F, Papadia F, Zelante L, Carella M (2015) De novo microduplication of CHL1 in a patient with non-syndromic developmental phenotypes. Mol Cytogenet 8:66
Pierini A, Schneidawind D, Nishikii H, Negrin RS (2015) Regulatory T cell immunotherapy in immune-mediated diseases. Curr Stem Cell Rep 1(4):177–186
Pratte M, Jamon M (2009) Impairment of novelty detection in mice targeted for the Chl1 gene. Physiol Behav 97(3–4):394–400
Probst-Schendzielorz K, Scholl C, Efimkina O, Ersfeld E, Viviani R, Serretti A, Fabbri C, Gurwitz D, Lucae S, Ising M, Paul AM, Lehmann ML, Steffens M, Crisafulli C, Calabro M, Holsboer F, Stingl J (2015) CHL1, ITGB3 and SLC6A4 gene expression and antidepressant drug response: results from the Munich antidepressant response signature (MARS) study. Pharmacogenomics 16(7):689–701
Sandi C (2004) Stress, cognitive impairment and cell adhesion molecules. Nat Rev Neurosci 5(12):917–930
Schlatter MC, Buhusi M, Wright AG, Maness PF (2008) CHL1 promotes Sema3A-induced growth cone collapse and neurite elaboration through a motif required for recruitment of ERM proteins to the plasma membrane. J Neurochem 104(3):731–744
Schmalbach B, Lepsveridze E, Djogo N, Papashvili G, Kuang F, Leshchyns'ka I, Sytnyk V, Nikonenko AG, Dityatev A, Jakovcevski I, Schachner M (2015) Age-dependent loss of parvalbumin-expressing hippocampal interneurons in mice deficient in CHL1, a mental retardation and schizophrenia susceptibility gene. J Neurochem 135(4):830–844
Senchenko VN, Krasnov GS, Dmitriev AA, Kudryavtseva AV, Anedchenko EA, Braga EA, Pronina IV, Kondratieva TT, Ivanov SV, Zabarovsky ER, Lerman MI (2011) Differential expression of CHL1 gene during development of major human cancers. PLoS One 6(3):e15612
Shaltout TE, Alali KA, Bushra S, Alkaseri AM, Jose ED, Al-Khainji M, Saleh R, Salama DA, Shaltout H, Al-Abdullah M, Rizk NM (2013) Significant association of close homologue of L1 gene polymorphism rs2272522 with schizophrenia in Qatar. Asia Pac Psychiatry 5(1):17–23
Shoukier M, Fuchs S, Schwaibold E, Lingen M, Gartner J, Brockmann K, Zirn B (2013) Microduplication of 3p26.3 in nonsyndromic intellectual disability indicates an important role of CHL1 for normal cognitive function. Neuropediatrics 44(5):268–271
Tang AH, Chen H, Li TP, Metzbower SR, MacGillavry HD, Blanpied TA (2016) A trans-synaptic nanocolumn aligns neurotransmitter release to receptors. Nature 536(7615):210–214
Tang H, Jiang L, Zhu C, Liu R, Wu Y, Yan Q, Liu M, Jia Y, Chen J, Qin Y, Lee VH, Luo S, Wang Q, Guan XY (2019) Loss of cell adhesion molecule L1 like promotes tumor growth and metastasis in esophageal squamous cell carcinoma. Oncogene 38(17):3119–3133
Vasileva LV, Ivanovska MV, Murdjeva MA, Saracheva KE, Georgiev MI (2019) Immunoregulatory natural compounds in stress-induced depression: an alternative or an adjunct to conventional antidepressant therapy? Food Chem Toxicol 127:81–88
Wakabayashi Y, Uchida S, Funato H, Matsubara T, Watanuki T, Otsuki K, Fujimoto M, Nishida A, Watanabe Y (2008) State-dependent changes in the expression levels of NCAM-140 and L1 in the peripheral blood cells of bipolar disorders, but not in the major depressive disorders. Prog Neuro-Psychopharmacol Biol Psychiatry 32(5):1199–1205
Wong DT, Horng JS, Bymaster FP, Hauser KL, Molloy BB (1974) A selective inhibitor of serotonin uptake: Lilly 110140, 3-(p-trifluoromethylphenoxy)-N-methyl-3-phenylpropylamine. Life Sci 15(3):471–479
Yang CR, Bai YY, Ruan CS, Zhou HF, Liu D, Wang XF, Shen LJ, Zheng HY, Zhou XF (2015) Enhanced aggressive behaviour in a mouse model of depression. Neurotox Res 27(2):129–142
Yang CR, Bai YY, Ruan CS, Zhou FH, Li F, Li CQ, Zhou XF (2017) Injection of anti-proBDNF in anterior cingulate cortex (ACC) reverses chronic stress-induced adverse mood behaviors in mice. Neurotox Res 31(2):298–308
Yang CR, Zhang XY, Liu Y, Du JY, Liang R, Yu M, Zhang FQ, Mu XF, Li F, Zhou L, Zhou FH, Meng FJ, Wang S, Ming D, Zhou XF (2020) Antidepressant drugs correct the imbalance between proBDNF/p75NTR/sortilin and mature BDNF/TrkB in the brain of mice with chronic stress. Neurotox Res 37(1):171–182
Zhong F, Liu L, Wei JL, Hu ZL, Li L, Wang S, Xu JM, Zhou XF, Li CQ, Yang ZY, Dai RP (2018) Brain-derived neurotrophic factor precursor in the hippocampus regulates both depressive and anxiety-like behaviors in rats. Front Psychiatry 9:776
Funding
This research was supported by grant from the Science & Technology Development Fund of Tianjin Education Commission for Higher Education (2018KJ086), by the Youth Fund of the Second Hospital of Tianjin Medical University (2018ydey01) and by the MST grant (2011CB944200) to XFZ.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All experiments were performed in accordance with the Animal Management Rules of the Ministry of Health of the People’s Republic of China. We declare that our study was carried out in accordance with the latest version of the Declaration of Helsinki. The Ethics Committee of Tianjin Mental Hospital approved all procedures (KY2018K015).
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Yang, C.R., Ning, L., Zhou, F.H. et al. Downregulation of Adhesion Molecule CHL1 in B Cells but Not T Cells of Patients with Major Depression and in the Brain of Mice with Chronic Stress. Neurotox Res 38, 914–928 (2020). https://doi.org/10.1007/s12640-020-00234-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-020-00234-9