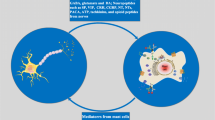
Abstract
Mast cells (MCs) are derived from hemopoietic precursor cells, undergo their maturation in peripheral tissues, and play a significant role in both the innate and adaptive immune response. Cross-linking of the FcεRI on MCs initiates activation of several cytoplasmic protein tyrosine kinases which rapidly lead to phosphorylation and recruitment of adaptor molecules. These effects trigger the release of preformed mediators stored in the cytoplasmic granules, including histamine, serotonin and tryptase, as well as newly synthesized mediators, such as cytokines/chemokines, prostaglandins, leukotrienes, and growth factors. Serotonin (5-HT) is a bioactive monoamine, which has seven specific cell surface membrane bound receptors which are coupled to G-proteins, plays an important role in the central and peripheral nervous system, and is one of the key mediators in signaling between nervous and immune systems. Serotonin is not stored in all MC types but is implicated in MC adhesion, chemotaxis, tumorigenesis, and tissue regeneration through smooth muscle differentiation of stromal cells. Recent evidence indicates that serotonin has immunoregulatory actions that may be important in neuropsychiatric conditions. Chemokines, RANTES/CCL5, MCP-1/CCL2, and related molecules, constitute the C–C class of chemokine supergene family, play a role in regulating T helper-cell cytokine production and MC trafficking, and are involved in histamine and serotonin generation and MC functions. Pro-inflammatory cytokines such as interleukin-1-β and tumor necrosis factor which mediate MC response, are capable of activating p38 MAPK, and might increase serotonin generation through p38 MAPK activation. Here, we review the relationship between MCs and serotonin and its role in inflammatory diseases and neuroimmune interactions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Mast cells (MCs) are multifunctional immune cells derived from hematopoietic precursors implicated in the pathophysiological processes including allergic diseases, inflammation, autoimmunity, cancer, and neurodegenerative diseases (Kritas et al. 2013a, b, c, d; Starkl et al. 2013). MCs are found preferentially in intraepithelial locations, around blood vessels, bronchioles, and mucus-secreting glands, perform important beneficial roles in host defense, and are necessary for the development of allergic reactions, through cross-linking of their surface receptors for IgE (FcεRI), leading to degranulation, and release vasoactive, pro-inflammatory, and nociceptive mediators that include histamine, serotonin, pro-inflammatory, and anti-inflammatory cytokines and proteolytic enzymes (Table 1) (Petra et al. 2014). The relationship between the central nervous system (CNS) and the endocrine system has been known for many years and the neuroendocrine and immune systems are closely linked and are involved in a bidirectional communication. MCs are found in mammalian brains, especially in the hypothalamus. There is much evidence to suggest that MCs are capable of communication with nerves. MCs are located around the ganglion in adjacent leptomeningeal and connective tissues, as well as between the ganglion cells and nerve fibers, and are occasionally found in the posterior root of the ganglion (Panula et al. 1985). In addition, MCs interact with CNS where they secrete an array of potent mediators, including histamine, serotonin, tumor necrosis factor, interleukin (IL)-1, and other cytokines/chemokines (Theoharides et al. 2007). Therefore, the generation and release of neuropeptides activate endothelial cells, mast cells, and platelets to then increase extracellular levels of arachidonate metabolites, peptides, and ions (Theoharides et al. 2010).
For many years, there has been great interest in the mechanisms of release of biogenic amines, and serotonin [5-hydroxytryptamine (5-HT)] is one of the most extensively studied neurotransmitters.
Serotonin (originally from serum plus tonic), a monoamine, is an important compound, which acts in both central and peripheral nervous systems and is one of the key mediators in signaling between the nervous system and the immune system (6). 5-HT is contained in cytoplasmic vesicles in enterochromaffin cells (Ahern 2011), as well as in platelets and MCs, with 5-HT being released when these cells are activated (Meuer et al. 1981; Papaliodis et al. 2008). The generation of 5-HT starts with hydroxylation of l-tryptophan at the fifth position on the indole ring to yield 5-HT, a reaction that requires molecular oxygen and the reducing cofactor 6-tetrahydrobiopterin; this reaction is catalyzed by tryptophan hydroxylase (TPH) an enzyme encoded by TPH1, which is expressed ubiquitously, while TPH2 genes are expressed predominantly in brain (Nordlind et al. 2008). The enzymes required to synthesize 5-HT from tryptophan are also present in the skin of certain animal species such as rodents. 5-HT is known to be produced and stored by murine MCs. However, a few studies have suggested the presence of serotonin in human MCs (Kushnir-Sukhov et al. 2008).
Increased doses of l-tryptophan proportionally increase 5-HT (or serotonin) formation. 5-HT is a bioactive mediator also implicated in MC adhesion, as well as chemotaxis, tumorigenesis, and tissue regeneration through induction of smooth muscle differentiation of bone marrow stromal cells (Hirota et al. 2014). Therefore, 5-HT mediates signaling by a wide range of neural and non-neural cells including mast cells. Moreover, the generation of 5-HT by mast cells is an important component for understanding mast cell function in the pathogenesis of inflammatory diseases and neurodegenerative disorders. The cellular sources of 5-HT in peripheral nerves are mostly platelets and mast cells (Sommer 2004). Immune cells express receptors for monoamine and intracellular serotonin transporters, and macrophages and murine mast cells have the ability to synthesize 5-HT. In addition, T cells are also able to produce 5-HT and to up-regulate its synthesis. Th1–Th2 cells, which are generated in human and animal models, are likely involved in resistance or susceptibility to brain diseases. T regulatory cells (Tregs) mediate protective immunity and inflammatory T-cell response to antigens. Tregs can easily differentiate into inflammation-associated Th17 which along with IL-23 are strongly associated with psoriasis a psycho-neuroimmunological and autoimmune-related chronic inflammatory skin disease (Mashayekhi et al. 2014). Moreover, Tregs and CD4+CD25(high)Foxp3+ are strong immunomodulators and are likely to play a major role in cancer development and are typically considered inhibitors of autoimmune responses including CNS disorders. 5-HT participates in T-cell activation via phosphorylation of extracellular signal-related kinase-1 and -2 (ERK1/2) (Bovenschen et al. 2011). Naive T cells, regulated by 5-HT, express the 5-HT receptor (Stefulj et al. 2001), however, the exact role of 5-HT in modulating immune function, particularly T-cell function, remains to be clarified.
In the brain, 5-HT neurons play a part in sleep–wakefulness cycles, mood, emotional and food behaviors, and thermoregulation, and in pathophysiological conditions, such as depression and insomnia (Jha et al. 2005). The strategic position of 5-HT suggests its involvement in the transduction of organ stimuli and reflex responses affecting motor and secretory function. Changes in serotonin concentration may occur in sensory innervation or pathways within the CNS leading to pain and hypersensitivity (Suter et al. 2007), an effect also mediated by MCs. In addition, when injected subcutaneously, 5-HT produces edema and increases capillary permeability, an important effect on peripheral and pulmonary vascular smooth muscle (Maleki-Dizaji et al. 2010). Since MCs tend to be in juxtaposition to blood vessels, 5-HT is expected to be secreted to act on these vessels. Therefore, 5-HT and its receptors are involved in hypersensitivity and inflammation (Enerbäck 1965) (Table 2). The release of serotonin by intracellular granules of MCs in humans is possibly regulated by the influx of Ca2+, an effect also highlighted in mast cell lines and freshly isolated peritoneal mast cells in experimental rodent models (Gordon and Galli 1991).
5-HT is present in murine mucosal MCs in the lamina propria; some authors have reported that human mast cells may also contain serotonin, especially in subjects with mastocytosis. In such patients, abnormal blood levels of 5-HT have been reported (Kushnir-Sukhov et al 2007; Metcalfe 1984). 5-HT is considered to be an inflammatory mediator in the periphery, being released from platelets and mast cells after tissue injury, to exert direct actions on C-fibers (Sommer 2004).
Human MC cultures in vitro contained less than 1 ng/mL of 5-HT, while mouse mast cells contained about tenfold more (22). In addition, some studies revealed the presence of mRNA and protein for tryptophan hydroxylase in human mast cells and concluded that human mast cells contain and release 5-HT (Kushnir-Sukhov et al. 2007; Metcalfe 1984).
Neurotransmitter 5-HT modulates antigen presenting cells, lymphocytes, and macrophages and is implicated in cytokine/chemokine generation and inflammation (Aune et al. 1993). Cytokines/chemokines are present in the hypothalamic–pituitary–adrenal axis, and inflammatory cytokines/chemokines produced within the brain may affect the course of neurodegenerative diseases (Cao et al. 2005). Pituitary gland generates several cytokines including IL-2, IL-1, TNF, and IL-6 (Kielian et al. 2004).
IL-6, a 26,000 molecular weight B-cell differentiation cytokine, is synthesized and released within neuroendocrine structures such as glia and astrocytes of the CNS, and stimulates prolactin, GH, and luteinizing hormone (LH) release from anterior pituitary cells in vitro (Jara et al. 2001). Certain pro-inflammatory cytokines such as IL-1, TNF, IL-6, and IL-33 regulate intracellular communication and are often elevated in a number of psychiatric conditions (Gemma et al. 2000). They are also involved in autoimmune diseases and cancer (Kritas et al. 2013a, b, c, d). In addition IL-1β regulates IL-6 release and induces several chemokines from neuroendocrine cells, demonstrating that products of the immune system, such as cytokines and chemokines may affect neuroendocrine activation and cell proliferation (Spangelo et al. 2000). Cytokines can mediate the release of 5-HT and other pro-inflammatory compounds from CNS mast cells, a process that contributes to inflammation and probably mortality. Therefore, in neuropathological diseases, cytokines have access to the CNS and are expressed in the brain, altering the metabolism and perhaps releasing 5-HT (Spangelo et al. 2000). The two potent pro-inflammatory cytokines, IL-1-β and TNF, are able to activate p38 MAPK in peripheral systems (28) and might increase 5-HT activity through p38 MAPK activation (Baud et al. 1999).
Several neuropeptides induce MC 5-HT release and may mediate neuroendocrine-linked mast cell activation (Hu and Tang 2009). It is proposed that MCs are capable of playing a more general transduction role, instead of acting as an immune cell, and may be capable of responding to a variety of stimuli (Sharkey and Mawe 2002).
5-HT and its receptor 5-HT1AR are expressed in human mastocytosis, and an agonist of the 5-HT1AR could be of value in the treatment of these patients (Ritter et al. 2012). 5-HT has seven specific cell surface membrane bound receptors (R) which are coupled to G-proteins (Sodhi et al. 2001) (Table 3).
5-HT syndrome is caused by hyperstimulation of 5-HT1A receptors in central gray nuclei and the medulla, and perhaps hyperstimulation of 5-HT2 receptors as well (Klimek et al. 1994). Besides its general effects, 5-HT also has an impact on cell proliferation, migration, and apoptosis (Kritas et al. 2014a, b, c, d). 5-HT1A receptor-positive MCs, and 5-HT2A receptor, and 5-HT reuptake transporter-positive T lymphocytes may be targets for drug therapy (Noro et al., 2010). It has been reported that in the apical epidermis of atopic eczematous of human skin melanocytes, MCs express 5-HT1A receptors (Ando et al. 2013; Kim 2012). In addition, we previously reported that chemokines RANTES/CCL5, MCP-1/CCL2, and related molecules constitute the C–C class of chemokine supergene family, playing a role in regulating Th-cell cytokine production and MC trafficking, and are involved in histamine and 5-HT generation and cell function in mast cells (Kritas et al. 2013a, b, c, d). Using immortal tumor-derived cell lines such as rat basophilic leukemia 2H3 (RBL) cells, it has been shown that CXCL10 (CXCR3 ligand) and CCL5 (CCR5 ligand) chemoattract mast cells in the site of inflammation and generate small amounts of serotonin and other granule mediators, increasing vascular dilation (Gruba et al. 2014). Recently, it has been shown that mast cell degranulation also involves CXCL10 and CCL5 which are two important related inflammatory chemokines (Sepiashvili et al. 2013). Therefore, CXCL10 and CCL5 chemokines play an important role on MC activation through a different pathway than IgE-mediated allergen stimulation (Kritas et al. 2014a, b). 5-HT and other mediators alter vascular dilation (46) and CXCL10 and CCL5 function, allowing mast cells to migrate to sites of inflammation, including sites in the CNS (Juremalm et al. 2005; Kritas et al. 2014c).
Smooth muscle constitutively expresses transforming growth factor (TGF)-β1, and its release is mediated by 5-HT. This effect demonstrates that 5-HT promotes smooth muscle differentiation and tissue remodeling, contributing to the pathogenesis of several neurological diseases (Hirota et al. 2014).
5-HT-containing mast cells are also involved in intestinal inflammation and the mobilization of 5-HT attributable to specific pro-inflammatory cytokines, such as IL-1β, IL-6, and TNF (Hajj Hussein et al. 2014; Komiyama et al. 2011). Therefore, neuroimmune interactions and tissue inflammation, which can also be mediated by stress (Papathanasiou et al. 2013), are regulated by a number of factors including MC-derived 5-HT generated under the influence of IL-3 [termed multi-colony-stimulating-factor (multi-CSF) or mast cell growth factor] produced by T-cells, causing severe hypersensitive reactions and playing a pivotal role in exacerbating the inflammatory response in vivo (Conti et al. 1995; Prevete et al. 2013).
5-HT has been reported to be involved in blood–brain barrier permeability. Where blood barrier opening is seen, there is evidence for activation of 5-HT2 receptors and a Ca2+-dependent permeability increase and augmentation of inflammatory mediator effects. Therefore, there is a clear intercommunication between mast cells and CNS, and this crosstalk suggests a functional connection. Inhibition of MC mediators, including 5-HT, may hold promise for therapeutic intervention of neuroinflammatory diseases (Abbott 2000; Kritas et al. 2013a, b, c, d).
Neurotransmitters (such as substance P) in contact with mast cells cause MC degranulation, an effect increased in acute stress in mice. Mast cells increase also in lesional psoriatic skin, and there appears to be an association among sensory nerves, mast cell numbers, and stress. It is interesting that psoriasis is worsened by acute stress, although it is not known whether 5-HT is involved in this disease (Theoharides et al. 2010).
Stimulated mast cells produce also IL-33 or IL-1F11 which is one of the newest inflammatory members of the IL-1 family, synthesized as a 31-kDa peptide precursor cleaved by caspase-1 to generate mature cytokine IL-33 (Dinarello 2005). This interleukin acts by binding its receptor T1/ST2 (Toll-IL-1 receptor), an orphan member of the IL-1 receptor family, activating NF-κB pathway, and MAP kinases. This process induces biological effects in mast cells: increasing in mice the production of IL-4, IL-5, and IL-13 which suppress the differentiation of inflammatory lymphocyte Th1 while increasing Th2 in adaptive immunity (Castellani et al. 2009). In mast cells, IL-33 stimulates production of arachidonic acid products such as PGD2 and inflammatory cytokines including TNF, MCP-1, and time-dependent stimulated IL-6 secretion, while it fails to release IL-2, IL-4, IL-5, or alter tryptase activity (Dinarello 2005). Substance P (SP), an undecapeptide belonging to a group of proteins termed tachykinins, is the key transmitter of pain to the brain and an activator of mast cells in several inflammatory diseases, including stress and neurological dysfunctions (Boyd and Leeman 1987). Whenever fibers come into contact with SP, they react by swelling—an effect that produces headache and sinus symptoms. In MCs, SP strongly induces the release of VEGF, chemoattractants, and promotes secretion of a number of intracellular molecules such as 5-HT and histamine (Shaik-Dasthagirisaheb et al. 2013a, b). IL-33 may play an important role in asthma, allergic-type diseases, and neurological disorders, without direct activation of 5-HT (61). IL-33 is abundantly expressed by endothelial veinules, and when injected into mouse, it causes several pathological effects in the mucosal tissues and brain such as eosinophilia and an increase of mast cell number, without mast cell degranulation (Theoharides et al. 2010). We recently found that IL-33 is a strong activator of human mast cell lines (LAD II cells) able to induce MCP-1, IL-8, TNF, and VGEF release at the transcriptional and translational level, suggesting a possible role of this new cytokine in inflammatory responses and in neurological disorders (Theoharides et al. 2010). However, it is still unknown whether IL-33 is implicated in the generation and release of 5-HT. Collectively, these observations suggest that IL-33 is a central regulator of mast cell responses. These studies may therefore implicate MCs and 5-HT as novel targets for the treatment and control of allergies, as well as autoimmune and neurodegenerative diseases. Nevertheless, the exact biological role of IL-33 and its molecular mechanisms regulating MC remain to be defined.
Natural compounds such as quercetin and capsaicin have a negative effect(s) on intracellular regulator signal events initiated by FcεRI receptor cross-linking and other activating receptors with an inhibitory effect on mast cells (Frydas et al. 2013; Shaik-Dasthagirisaheb et al. 2013a, b). It would be interesting to see the effect(s) of these natural compounds on the generation of 5-HT and other mediators derived from degranulated and non- degranulated activated MCs (Karamitopoulou et al. 2014).
The purpose of this paper was to review and possibly clarify the relationship between MCs and 5-HT in inflammation. The present report indicates that modulation of 5-HT may have a role in MC function and differentiation. However, further studies on the effects of MC-secreted cytokines/chemokines and 5-HT are needed to better understand the complex role that mast cell activation plays in inflammatory and neurodegenerative diseases.
References
Abbott NJ (2000) Inflammatory mediators and modulation of blood-brain barrier permeability. Cell Mol Neurobiol 20(2):131–147
Ahern GP (2011) 5-HT and the immune system. Curr Opin Pharmacol 11(1):29–33
Ando T, Matsumoto K, Namiranian S, Yamashita H, Glatthorn H, Kimura M, Dolan BR, Lee JJ, Galli SJ, Kawakami Y, Jamora C, Kawakami T (2013) Mast cells are required for full expression of allergen/SEB-induced skin inflammation. J Invest Dermatol 133(12):2695–2705
Aune TM, McGrath KM, Sarr T, Bombara MP, Kelley KA (1993) Expression of 5-HT1A receptors on activated human T cells. Regulation of cyclic AMP levels and T cell proliferation by 5-hydroxytryptamine. J Immunol 151(3):1175–1183
Baud V, Liu ZG, Bennett B, Suzuki N, Xia Y, Karin M (1999) Signaling by proinflammatory cytokines: oligomerization of TRAF2 and TRAF6 is sufficient for JNK and IKK activation and target gene induction via an amino-terminal effector domain. Genes Dev 13(10):1297–1308
Bovenschen HJ, van de Kerkhof PC, van Erp PE, Woestenenk R, Joosten I, Koenen HJ (2011) Foxp3+ regulatory T cells of psoriasis patients easily differentiate into IL-17A-producing cells and are found in lesional skin. J Invest Dermatol. 131(9):1853–1860
Boyd ND, Leeman SE (1987) Multiple actions of substance P that regulate the functional properties of acetylcholine receptors of clonal rat PC12 cells. J Physiol 389:69–97
Cao J, Papadopoulou N, Kempuraj D, Boucher WS, Sugimoto K, Cetrulo CL, Theoharides TC (2005) Human mast cells express corticotropin-releasing hormone (CRH) receptors and CRH leads to selective secretion of vascular endothelial growth factor. J Immunol 174(12):7665–7675
Castellani ML, Kempuraj D, Salini V, Vecchiet J, Tete S, Ciampoli C, Conti F, Cerulli G, Caraffa A, Antinolfi P, Theoharides TC, De Amicis D, Perrella A, Cuccurullo C, Boscolo P, Shaik Y (2009) The latest interleukin: IL-33 the novel IL-1-family member is a potent mast cell activator. J Biol Regul Homeost Agents 23(1):11–14
Conti P, Boucher W, Letourneau R, Feliciani C, Reale M, Barbacane RC, Vlagopoulos P, Bruneau G, Thibault J, Theoharides TC (1995) Monocyte chemotactic protein-1 provokes mast cell aggregation and [3H]5-HT release. Immunology 86(3):434–440
Dinarello CA (2005) An IL-1 family member requires caspase-1 processing and signals through the ST2 receptor. Immunity 23(5):461–462
Enerbäck L (1965) Mast cells in carcinoid tumours. Distribution, histochemical properties and 5-hydroxytryptamine content. Acta Pathol Microbiol Scand 64(4):491–505
Frydas S, Varvara G, Murmura G, Saggini A, Caraffa A, Antinolfi P, Tete’ S, Tripodi D, Conti F, Cianchetti E, Toniato E, Rosati M, Speranza L, Pantalone A, Saggini R, Di Tommaso LM, Theoharides TC, Conti P, Pandolfi F (2013) Impact of capsaicin on mast cell inflammation. Int J Immunopathol Pharmacol 26(3):597–600
Gemma C, Smith EM, Hughes TK Jr, Opp MR (2000) Human immunodeficiency virus glycoprotein 160 induces cytokine mRNA expression in the rat central nervous system. Cell Mol Neurobiol 20(4):419–431
Gordon JR, Galli SJ (1991) Release of both preformed and newly synthesized tumor necrosis factor alpha (TNF-alpha)/cachectin by mouse mast cells stimulated via the Fc epsilon RI. A mechanism for the sustained action of mast cell-derived TNF-alpha during IgE-dependent biological responses. J Exp Med 174(1):103–107
Gruba SM, Meyer AF, Manning BM (2014) Time- and concentration-dependent effects of exogenous serotonin and inflammatory cytokines on mast cell function. ACS Chem Biol 9(2):503–509
Hajj Hussein I, Eid A, Maksoud R, Jambart S, Bou Assi T, Zgheib Z, Oueidat D, Chams N, Chams S, Diab R, Barada K, Jurjus R, Cappello F, Reimund J, Kreiker J, Leone A, Jurjus A (2014) Estrogens control inflammation in experimental colitis. J Biol Regul Homeost Agents 28(2):213–224
Hirota N, McCuaig S, O’Sullivan MJ, Martin JG (2014) Serotonin augments smooth muscle differentiation of bone marrow stromal cells. Stem Cell Res 12(3):599–609
Hu R, Tang F (2009) Effect of Weichang Anwan on NO and 5-HT in blood serum, SP and MC in colon in IBS-D rats. Zhongguo Zhong Yao Za Zhi 34(23):3073–3077
Jara LJ, Vera-Lastra O, Miranda JM, Alcala M, Alvarez-Nemegyei J (2001) Prolactin in human systemic lupus erythematosus. Lupus 10(10):748–756
Jha SK, Ross RJ, Morrison AR (2005) Sleep-related neurons in the central nucleus of the amygdala of rats and their modulation by the dorsal raphe nucleus. Physiol Behav 86(4):415–426
Juremalm M, Olsson N, Nilsson G (2005) CCL17 and CCL22 attenuate CCL5-induced mast cell migration. Clin Exp Allergy 35(6):708–712
Karamitopoulou E, Shoni M, Theoharides TC (2014) Increased number of non-degranulated mast cells in pancreatic ductal adenocarcinoma but not in acute pancreatitis. Int J Immunopathol Pharmacol 27(2):213–220
Kielian T, Bearden ED, Baldwin AC, Esen N (2004) IL-1 and TNF-alpha play a pivotal role in the host immune response in a mouse model of Staphylococcus aureus-induced experimental brain abscess. J Neuropathol Exp Neurol 63(4):381–396
Kim K (2012) Neuroimmunological mechanism of pruritus in atopic dermatitis focused on the role of serotonin. Biomol Ther (Seoul) 2(6):506–512
Klimek V, Zak-Knapik J, Mackowiak M (1994) Effects of repeated treatment with fluoxetine and citalopram, 5-HT uptake inhibitors, on 5-HT1A and 5-HT2 receptors in the rat brain. J Psychiatry Neurosci 19(1):63–67
Komiyama Y, Andoh A, Fujiwara D, Ohmae H, Araki Y, Fujiyama Y, Mitsuyama K, Kanauchi O (2011) New prebiotics from rice bran ameliorate inflammation in murine colitis models through the modulation of intestinal homeostasis and the mucosal immune system. Scand J Gastroenterol 46(1):40–52
Kritas SK, Saggini A, Varvara G, Murmura G, Caraffa A, Antinolfi P, Toniato E, Pantalone A, Neri G, Frydas S, Rosati M, Tei M, Speziali A, Saggini R, Pandolfi F, Cerulli G, Theoharides TC, Conti P (2013a) Impact of mast cells on the skin. Int J Immunopathol Pharmacol 26(4):855–859
Kritas SK, Saggini A, Varvara G, Murmura G, Caraffa A, Antinolfi P, Toniato E, Pantalone A, Neri G, Frydas S, Rosati M, Tei M, Speziali A, Saggini R, Pandolfi F, Theoharides TC, Conti P (2013b) Mast cell involvement in rheumatoid arthritis. J Biol Regul Homeost Agents 27(3):655–660
Kritas SK, Saggini A, Varvara G, Murmura G, Caraffa A, Antinolfi P, Toniato E, Pantalone A, Neri G, Frydas S, Rosati M, Tei M, Speziali A, Saggini R, Pandolfi F, Cerulli G, Theoharides TC, Conti P (2013c) Luteolin inhibits mast cell-mediated allergic inflammation. J Biol Regul Homeost Agents 27(4):955–959
Kritas SK, Saggini A, Varvara G, Murmura G, Caraffa A, Antinolfi P, Toniato E, Pantalone A, Neri G, Frydas S, Rosati M, Tei M, Speziali A, Saggini R, Pandolfi F, Cerulli G, Theoharides TC, Conti P (2013d) Impact of mast cells in rejection of allografts. Eur J Inflamm 11(3):609–614
Kritas SK, Saggini A, Cerulli G, Caraffa A, Antinolfi P, Pantalone A, Rosati M, Tei M, Speziali A, Saggini R, Conti P (2014a) Relationship between serotonin and mast cells: inhibitory effect of anti-serotonin. J Biol Regul Homeost Agents 28(3):377–380
Kritas SK, Saggini A, Cerulli G, Caraffa A, Antinolfi P, Pantalone A, Saggini R, Frydas S, Rosati M, Tei M, Speziali A, Pandolfi F, Conti P (2014b) Interrelationship between IL-3 and mast cells. J Biol Regul Homeost Agents 28(1):17–21
Kritas SK, Saggini A, Cerulli G, Speziali A, Caraffa A, Antinolfi P, Pantalone A, Rosati M, Tei M, Saggini R, Conti P (2014c) Asthma and mast cell biology. Eur J Inflamm 12(2):261–265
Kritas SK, Saggini A, Cerulli G, Caraffa A, Antinolfi P, Pantalone A, Rosati M, Tei M, Speziali A, Saggini R, Conti P (2014d) Corticotropin-releasing hormone, microglia and mental disorders. Int J Immunopathol Pharmacol 27(2):163–167
Kushnir-Sukhov NM, Brown JM, Wu Y, Kirshenbaum A, Metcalfe DD (2007) Human mast cells are capable of serotonin synthesis and release. J Allergy Clin Immunol 119:498–499
Kushnir-Sukhov NM, Brittain E, Scott L, Metcalfe DD (2008) Clinical correlates of blood serotonin levels in patients with mastocytosis. Eur J Clin Invest 38(12):953–958
Maleki-Dizaji N, Eteraf-Oskouei T, Fakhrjou A, Maljaie SH, Garjani A (2010) The effects of 5-HT3 receptor antagonist granisetron on inflammatory parameters and angiogenesis in the air-pouch model of inflammation. Int Immunopharmacol 10(9):1010–1016
Mashayekhi Goyonlo V, Elnour H, Nordlind K (2014) Serotonin transporter protein overexpression and association to Th17 and T regulatory cells in lupoid leishmaniasis. Arch Dermatol Res 306(2):181–188
Metcalfe DD (1984) Mast cell mediators with emphasis on intestinal mast cells. Ann Allergy 53(6 Pt 2):563–575
Meuer S, Ecker U, Hadding U, Bitter-Suermann D (1981) Platelet-serotonin release by C3a and C5a: two independent pathways of activation. J Immunol 126(4):1506–1509
Nordlind K, Azmitia EC, Slominski A (2008) The skin as a mirror of the soul: exploring the possible roles of serotonin. Exp Dermatol 17(4):301–311
Noro M, Antonijevic I, Forray C, Kasper S, Kocabas NA, Lecrubier Y, Linotte S, Mendlewicz J, Montgomery S, Snyder L, Souery D, Verbanck P, Zohar J, Massat I (2010) 5-HT1A and 5-HT2A receptor genes in treatment response phenotypes in major depressive disorder. Int Clin Psychopharmacol 25(4):228–231
Panula P, Kaartinen M, Mäcklin M, Costa E (1985) Histamine-containing peripheral neuronal and endocrine systems. J Histochem Cytochem 33(9):933–941
Papaliodis D, Boucher W, Kempuraj D, Michaelian M, Wolfberg A, House M, Theoharides TC (2008) Niacin-induced “flush” involves release of prostaglandin D2 from mast cells and serotonin from platelets: evidence from human cells in vitro and an animal model. J Pharmacol Exp Ther 327(3):665–672
Papathanasiou E, Palaska I, Theoharides TC (2013) Stress hormones regulate periodontal inflammation. J Biol Regul Homeost Agents 27(3):621–626
Petra AI, Panagiotidou S, Stewart JM, Conti P, Theoharides TC (2014) Spectrum of mast cell activation disorders. Expert Rev Clin Immunol 10(6):729–739
Prevete N, Staiano RI, Granata F, Detoraki A, Necchi V, Ricci V, Triggiani M, De Paulis A, Marone G, Genovese A (2013) Expression and function of Angiopoietins and their tie receptors in human basophils and mast cells. J Biol Regul Homeost Agents 27(3):827–839
Ritter M, El-Nour H, Hedblad MA, Butterfield JH, Beck O, Stephanson N, Holst M, Giscombe R, Azmitia EC, Nordlind K (2012) Serotonin and its 5-HT1 receptor in human mastocytosis. Immunopharmacol Immunotoxicol 34(4):679–685
Sepiashvili RI, Balmasova IP, Staurina LN (2013) Serotonin and its immune and physiological effects. Ross Fiziol Zh Im I M Sechenova 99(1):17–32
Shaik-Dasthagirisaheb YB, Varvara G, Murmura G, Saggini A, Caraffa A, Antinolfi P, Tetè S, Rosati M, Cianchetti E, Toniato E, Speranza L, Pantalone A, Saggini R, Di Tommaso LM, Conti P, Theoharides TC, Pandolfi F (2013a) Inhibitor effect of antioxidant flavonoids quercitin, and capsaicin in mast cell inflammation. Eur J Inflamm 11(2):353–357
Shaik-Dasthagirisaheb YB, Varvara G, Murmura G, Saggini A, Potalivo G, Caraffa A, Antinolfi P, Tete’ S, Tripodi D, Conti F, Cianchetti E, Toniato E, Rosati M, Conti P, Speranza L, Pantalone A, Saggini R, Theoharides TC, Pandolfi F (2013b) Vascular endothelial growth factor (VEGF), mast cells and inflammation. Int J Immunopathol Pharmacol. 26(2):327–335 (Review)
Sharkey KA, Mawe GM (2002) Neuroimmune and epithelial interactions in intestinal inflammation. Curr Opin Pharmacol 2(6):669–677
Sodhi MS, Burnet PW, Makoff AJ, Kerwin RW, Harrison PJ (2001) RNA editing of the 5-HT2C receptor is reduced in schizophrenia. Mol Psychiatry 6(4):373–379
Sommer C (2004) Serotonin in pain and analgesia: actions in the periphery. Mol Neurobiol 30(2):117–125
Spangelo BL, Farrimond DD, Pompilius M, Bowman KL (2000) Interleukin-1 beta and thymic peptide regulation of pituitary and glial cell cytokine expression and cellular proliferation. Ann NY Acad Sci 917:597–607
Starkl P, Marichal T, Galli SJ (2013) PLA2G3 promotes mast cell maturation and function. Nat Immunol 14(6):527–529
Stefulj J, Cicin-Sain L, Schauenstein K, Jernej B (2001) Serotonin and immune response: effect of the amine on in vitro proliferation of rat lymphocytes. NeuroImmunoModulation 9(2):103–108
Suter MR, Wen YR, Decosterd I, Ji RR (2007) Do glial cells control pain? Neuron Glia Biol 3(3):255–268
Theoharides TC, Kempuraj D, Iliopoulou BP (2007) Mast cells, T cells, and inhibition by luteolin: implications for the pathogenesis and treatment of multiple sclerosis. Adv Exp Med Biol 601:423–430 (Review)
Theoharides TC, Zhang B, Kempuraj D, Tagen M, Vasiadi M, Angelidou A, Alysandratos KD, Kalogeromitros D, Asadi S, Stavrianeas N, Peterson E, Leeman S, Conti P (2010) IL-33 augments substance P-induced VEGF secretion from human mast cells and is increased in psoriatic skin. Proc Natl Acad Sci USA 107(9):4448–4453
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Conti, P., Shaik-Dasthagirisaheb, Y.B. Mast Cell Serotonin Immunoregulatory Effects Impacting on Neuronal Function: Implications for Neurodegenerative and Psychiatric Disorders. Neurotox Res 28, 147–153 (2015). https://doi.org/10.1007/s12640-015-9533-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-015-9533-0