Abstract
Nevirapine (NVP) and efavirenz (EFV) belong to the class of anti-HIV drugs called non-nucleoside reverse transcriptase inhibitors (NNRTIs), commonly used as part of highly active antiretroviral therapy (HAART). Although the HAART is able to bring down viral load to undetectable levels and restore immune function, their prolonged use causes several adverse effects. It has been demonstrated that both NVP and EFV are able to cross the blood–brain barrier, causing important central nervous system-related side effects. Thus, this study investigated the effects of chronic administration of EFV (10 mg/kg) and NVP (3.3 mg/kg) in mice submitted to two distinct series of experiments, which aimed to evaluate: (1) the emotional behavior (elevated plus-maze, forced swimming, and open-field test) and (2) the cognitive performance (object recognition and inhibitory avoidance test) of mice. Our results demonstrated that EFV, but not NVP, reduced the exploration to open arms in the elevated plus-maze test. Neither NVP nor EFV altered mouse behavior in the forced swimming and open-field tests. Both drugs reduced the recognition index in the object recognition test, but only EFV significantly impaired the aversive memory assessed in the inhibitory avoidance test 24 h after training. In conclusion, our findings point to a genuine anxiogenic-like effect to EFV, since it reduced exploration to open arms of elevated plus-maze test without affecting spontaneous locomotion. Additionally, both drugs impaired recognition memory, while only the treatment with EFV impaired significantly aversive memory.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The highly active antiretroviral therapy (HAART) completely changed the clinical evolution of HIV infection, reducing the morbidity and mortality among HIV-1 infected patients and changing the incidence of neurological complications in acquired immunodeficiency syndrome (AIDS) patients (Sacktor et al. 2001). Nevirapine (NVP) and efavirenz (EFV) are antiretroviral drugs belonging to potent class of non-nucleoside reverse transcriptase inhibitors (NNRTIs), commonly used as part of HAART regimen. They are recommended at initial therapy for asymptomatic HIV patients or in advanced disease (Brazil 2008). Although the HAART is able to bring down viral load to undetectable levels and restore immune function, their prolonged use causes several adverse effects (Roca 2009). The majority of non-therapeutic actions of antiretroviral drugs are linked with induction or inactivation of enzymatic hepatic systems and/or cutaneous adverse effects (Saitoh et al. 2007; Rivero et al. 2007). Besides these side effects, NNRTIs require larger attention, once it was well demonstrated that both NVP and EFV are able to cross the blood–brain barrier and enter the central nervous system (CNS) (Treisman and Kaplin 2002; von Giesen et al. 2002), thus causing important adverse effects related to their presence within this tissue, especially EFV (Bickel et al. 2005; Arendt et al. 2007).
NVP is the oldest NNRTI offering a better treatment compliance due to its once daily initial dosage. Despite this advantage, side effects such as hypersensitivity reaction, gastric complications, and hepatotoxicity can be frequently observed (de Maat et al. 2003; Phillips and Mallal 2007). Furthermore, neuropsychiatric complications have been associated with its use (Wise et al. 2002). It has been demonstrated that NVP in combination with nucleoside reverse transcriptase inhibitors (NRTIs) significantly improves HIV-1 associated psychomotor slowing, compared with NRTIs alone (von Giesen et al. 2002).
EFV, similarly to NVP, is also known by its efficacy and easy treatment compliance. However, the lipophilic profile of EFV impairs its excretion, thus, remains high plasma concentration longer. This chemical characteristic of EFV supports wide range of central side effects observed after acute and chronic treatments. In fact, it was observed that more than 50% of patients receiving EFV reported neurological adverse symptoms, which are very specific of this NNRTI. CNS side effects including insomnia, dizziness, impaired concentration, vertigo, depression, abnormal dreams, and hallucinations are very frequent during the first week of therapy (Treisman and Kaplin 2002; Bickel et al. 2005). Some studies have demonstrated that neuropsychiatric disorders may persist in patients chronically treated with EFV (Fumaz et al. 2005; Gutiérrez et al. 2005; Rihs et al. 2006). The exact mechanism responsible for CNS toxicity associated with EFV remains unknown, but plasma and intracellular drug concentrations as well CYP2B6 genotype have been found to be predictors of early neuropsychological disturbances in patients starting antiretroviral therapy regimens containing EFV (Haas et al. 2004).
Although HAART regimen represents a very important role in the treatment of HIV/AIDS, its side effects can be responsible for patients’ non-adherence to drugs, contributing to the treatment failure and development of resistant HIV strains (Piacenti 2006). In addition, little information is still available about the central effects of EFV and NVP in rodent, and it is quite relevant to manage this question to understand the underlying mechanisms involved in the expression of these effects. In this context, the present study investigated the behavioral effects of chronic administration of two major NNRTIs used in clinic: EFV and NVP. In order to develop this study, mice were treated for, at least, 28 days with EFV and NVP, and mouse behavior was assessed in two distinct series of experiments: (1) elevated plus-maze, open-field test, and forced swimming test, which was aimed to evaluate anxiety- and mood-related behaviors, and (2) object recognition and inhibitory avoidance test that were used for testing cognitive performance of mice.
Materials and Methods
Animals
Male CF-1 mice (age 60 days; weight 30 g) were obtained from the State Foundation for Health Science Research (FEPPS-RS, Porto Alegre, Brazil) and maintained in the animal facility of Universidade do Extremo Sul Catarinense (UNESC) for at least 2 weeks before drug treatment. The animals were housed in plastic cages, eight per cage, under 12 h light/dark cycle (lights on 7:00 a.m.) at constant room temperature of 23 ± 1°C with water and food ad libitum. In order to minimize the possible effect of circadian fluctuations on emotion and activity, experiments were performed between 9.00 and 12.00 h. Animals were acclimated to the room at least 1 h before each behavioral test.
To perform, this study was employed a number of 18–20 mice per group. All experimental procedures were performed in accordance with NIH Guideline for the Care and Use of Laboratory Animals and the Brazilian Society for Neuroscience and Behavior (SBNeC) recommendations for animal care, with the approval of local Ethics Committee.
Drugs and Treatment
Two NNRTIs were employed in this study: efavirenz (EFV; 8-chloro-5-(2-cyclopropylethynyl)-5-(trifluoromethyl)-4-oxa-2-azabicyclo [4.4.0]deca-7,9,11-trien-3-one; Patheon Inc., Mississauga, ON, Canada) and nevirapine (NVP; 1-cyclopropyl-5,11-dihydro-4-methyl-6H-dipyrido [3,2-b:2′,3′-e][1,4] diazepin-6-one; Boehringer Ingelheim Roxane, Inc. Columbus, OH, USA).
Mice were treated orally, once a day for 36 days, with EFV 10 mg/kg, NVP 3.3 mg/kg, or vehicle in a volume of 10 ml/kg. The animals were weighed once a week, and drug volumes were adapted to animal weight. The doses employed in this study were based on the doses used for human therapy and previous studies with animals (Lewis et al. 2005; O’Mahony et al. 2005; Streck et al. 2008). EFV and NVP were dissolved in distillated water slightly warmed with Tween-80 1%. The control group received a solution consisting of distillated water with Tween-80 1%. Drug solutions were prepared daily just before the oral administration.
Behavioral Tests
The present study was divided in two parts to assess the effects of chronic treatment with NNRTIs drugs in: (1) emotional behavior and (2) cognitive performance. Considering that previous experiences can influence animal behavior in the elevated plus-maze test (Andreatini and Bacellar 1999), in the first part of this study, on day 28, 32, and 36 of drug treatment, mice were subjected to the elevated plus-maze test, open-field test, and forced swimming test, respectively. In order to assess the cognitive performance of mice chronically treated with NVP and EFV, on day 31 and 36 of drug treatment, mice were first subjected to the object recognition test and then after to the inhibitory avoidance test.
Elevated Plus-Maze Test
As previously described by Lister (1987), the plus-maze consisted of two open (30 × 5 cm) and two wall-enclosed arms (30 × 5 × 15 cm) connected by a central platform (5 × 5 cm). The apparatus was elevated 50 cm above the floor. The floor and the walls of the enclosed arms of the maze were constructed of brown wood. Each mouse was placed on the central platform, facing a closed arm, and observed for a 5-min period. The frequencies of entry into either open or enclosed arms, as well as the times spent in each arm type, were recorded (in seconds). An entry was scored as such only when the animal placed all four limbs into any given arm. Drugs with anxiolytic-like activity usually increase the time spent in and/or frequency of entries into open arms, whereas the reverse holds true for anxiogenic-like drugs. Furthermore, the number of entries into closed arms was used as an index of general activity. The elevated plus-maze apparatus was placed in a small closed room lit by a red light with intensity of 100 lx in the open arms. After each mouse, the apparatus was cleaned with ethanol 10%.
Open-Field Test
The open field consisted of a squared arena (40 × 40 cm), made of opaque white polyethylene with the floor divided in 16 sections. These experiments were performed in a calm and low-intensity illuminated (around 100 lx at the center of the arena) room. The parameters measured during the 5 min of observation were number of crossings and frequency of rearings. The open-field arena has been cleaned with ethanol 10% after each animal (Choleris et al. 2001).
Behavioral Despair Test
The mouse forced swimming test, described previously by Porsolt et al. (1977), consisted of placing mice, individually, in polyethylene cylinders (18.5 cm high, 12.5 cm diameter), containing water (25°C, 13.5 cm deep) for 6 min. The duration of immobility was measured during the last 4 of the 6 min test period by observers blind to the treatment conditions. Mice were considered to be immobile when floating motionless or making only those movements necessary to keep its head above water. At the end of each swimming session, the animal was removed from the cylinder, dried with paper towels, placed in an individual cage to rest and recover, and then it was returned to its collective home cage.
Object Recognition Test
The object recognition was performed as previously described by our research group (Réus et al. 2008). The task took place in a 40 × 60 cm open field surrounded by 50 cm high walls made of plywood with a frontal glass wall. The floor of the open field was divided into 12 equal rectangles by black lines. All animals were submitted to a habituation session where they were allowed to freely explore the open field for 5 min. No objects were placed in the box during the habituation trial. Twenty-four hours after habituation, training was conducted by placing individual mouse for 5 min in the open field, in which two identical objects (objects A1 and A2; both being cubes) were positioned in two adjacent corners, 10 cm from the walls. In a long-term recognition memory test given 24 h after training, the mice explored the open field for 5 min in the presence of one familiar (A) and one novel (B, a pyramid with a square-shaped base) object. All objects had similar textures (smooth), colors (blue), and sizes (weight 150–200 g), but distinctive shapes. A recognition index calculated for each animal was calculated in the test session, and it reports the ratio TB/(TA + TB) (TA = time spent exploring the familiar object A; TB = time spent exploring the novel object B). Between trials, the objects were washed with 10% ethanol solution. Exploration was defined as sniffing (exploring the object 3–5 cm away from it) or touching the object with the nose and/or forepaws.
Step-Down Inhibitory Avoidance Test
The step-down inhibitory avoidance apparatus consisted of a 50 × 25 × 25 cm plastic box with a front glass wall, whose floor had parallel 10-mm bronze bars. The left end of the grid was occupied by a 7-cm wide, 2.5-cm high Formica platform. The mice were gently placed on the platform facing the rear wall, and their latency to step down with all four paws on the grid was recorded. In the training session, after stepping down, the animals received a 0.3-mA, 2-s scrambled footshock and were withdrawn immediately from the cage. In the test session, 24 h later, the procedure was repeated, but footshock was not given. Test session step-down latency was used as a measure of retention. A ceiling of 180 s was imposed on this measure, i.e., animals whose test latency was more than 180 s were considered to have a latency of 180 s, as previously described (Roesler et al. 1999).
Statistical Analysis
Results were analyzed by Graphpad INSTAT® version 3.0 software. The data from the elevated plus-maze, forced swimming, and open-field tests are reported as means ± SEM and were analyzed by one-way ANOVA followed by Dunnett’s test or by the non-parametric test Kruskal–Wallis test followed by Dunn test, when data distribution did not assume normality. Data for recognition indexes and latency to step-down from the platform were reported as median ± interquartile ranges (25 and 75). Comparisons among groups were performed using the Kruskal–Wallis test followed by Dunn test when necessary. P values less than 0.05 were considered to be statistically significant.
Results
Elevated Plus-Maze Test
In the elevated plus maze test, the average time spent in and frequency of entries into open arms of control mice were 30.1 ± 9.2 s (corresponding to 16.4 ± 4.3% of the total time spent in open and closed arms) and 3.4 ± 0.9 (corresponding to 20.6 ± 3.8% of the total entries into open and closed arms), respectively. As shown in Fig. 1a, mice chronically treated with EFV exhibited a significant reduction of time spent in the open arms compared to control mice (U′ = 249.5; P = 0.017). In addition, EFV-treated mice entered the open arms of the apparatus less frequently than vehicle-treated mice (Fig. 1b; U′ = 250.0; P = 0.016). No statistical alterations were observed in the behavior of mice chronically treated with NVP in the elevated plus-maze test compared to control. Additionally, as illustrated in Fig. 1c, neither the treatment with EFV nor NVP modified the frequency of entries into closed arms of elevated plus-maze test compared to control mice (P > 0.05).
Effects of chronic administration of the non-nucleoside reverse transcriptase inhibitors nevirapine (NVP; 3.3 mg/kg/day) and efavirenz (EFV; 10 mg/kg/day) on the time spent in open arms (a), and frequency of entries into open (b) and closed (c) arms in mice subjected to the elevated plus-maze test. Data are mean ± SEM of 18–20 animals, and are analyzed by ANOVA (Dunnett’s test) or by Kruskal–Wallis test (followed by Dunn test), if necessary. * P < 0.05 versus control group
Open-Field and Forced Swimming Tests
In the open-field test, mice treated with EFV and NVP did not display any significant alteration in the number of crossing (Control: 79.1 ± 7.4; NVP = 68.1 ± 9.1; EFV = 90.7 ± 9.9; P > 0.05), and in the frequency of rearings compared to vehicle (Control: 6.3 ± 2.1; NVP = 8.0 ± 3.0; EFV = 12.7 ± 3.2; P > 0.05).
In the forced swimming test, vehicle-treated mice spent 46 ± 8 s of immobility time. The present study demonstrated that CF-1 mice chronically treated with EFV and NVP displayed an immobility time similar to that displayed by control mice (P > 0.05; Fig. 2).
Cognitive Assessment
As illustrated in Fig. 3, in the object recognition test, control mice displayed a statistical significant increase in the recognition index in the test session compared to the training session (Fig. 3; P = 0.04; t = 2.13), thus suggesting that, for control mice, recognition memory was acquired during this task. However, the chronic treatment with EFV and NVP impaired recognition memory formation. In fact, in the test session the recognition index of mice treated with both NNRTIs drugs, NVP and EFV, did not statistically differ from those values achieved during the training session (Fig. 3; P > 0.05 for both drugs).
Effects of chronic administration of the non-nucleoside reverse transcriptase inhibitors nevirapine (NVP; 3.3 mg/kg/day) and efavirenz (EFV; 10 mg/kg/day) on the recognition index in mice subjected to the object recognition test. Data are median ± interquartile ranges (25 and 75) of 18–20 animals, and are analyzed by Kruskal–Wallis test (followed by Dunn test). * P < 0.05 versus control group
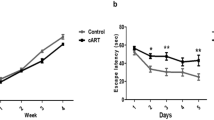
In the inhibitory avoidance test, an increase in the time spent to step-down the platform in the test sessions (1.5 and 24 h) compared to the training session was observed for all groups, thus indicating that, for all groups, aversive memory was acquired (Fig. 4). Importantly, there are no statistical significant differences among groups (vehicle- and drug-treated mice) neither in the training session nor in the test session at 1.5 h of the inhibitory avoidance task (Fig. 4; P > 0.05). However, the chronic treatment with EFV reduced the latency to step-down from the platform in the test session at 24 h compared to control, while the administration of NVP did not reach the statistical significance (Fig. 4; P = 0.04, KW = 6.46).
Effects of chronic administration of the non-nucleoside reverse transcriptase inhibitors nevirapine (NVP; 3.3 mg/kg/day) and efavirenz (EFV; 10 mg/kg/day) on the latency to step-down from the platform in mice subjected to the inhibitory avoidance test. Data are median ± interquartile ranges (25 and 75) of 18–20 animals, and are analyzed by Kruskal–Wallis test (followed by Dunn test). * P < 0.05 versus control group
Discussion
Our results demonstrated for the first time that the chronic treatment with EFV, but not NVP, induced a potent anxiogenic-like effect, without affecting the spontaneous locomotion. In contrast, the treatment with both EFV and NVP did not alter mice behavior in the forced swimming test. Additionally, EFV and NVP impaired significantly recognition memory, but only EFV caused a substantial impairment of aversive memory assessed in the inhibitory avoidance test. It is worth mentioning that NVP caused a non-statistical significant impairment of aversive memory in the inhibitory avoidance. Taken together, the repeated administration of EFV evoked anxiogenic-like effects and cognitive impairment, whereas NVP mainly affected recognition memory in mice.
The most common adverse effects of EFV are related to sleep disorders, such as insomnia, nightmares, and vivid dreams, and also dizziness, headaches, confusion, stupor, attention deficit (Treisman and Kaplin 2002). There are some reports suggesting that neuropsychiatric features like anxiety, hostility, and depression found in patients with long-term EFV use were associated with high serum drug concentration (Gutiérrez et al. 2005; Rihs et al. 2006). Regarding NVP, central side effects such as neuropsychiatric complications and headaches have been sometimes associated with its use (Wise et al. 2002). These effects are induced by the action of NVP into the CNS; in fact, NVP has been found in the CSF in a concentration ranging from 15 to 40% of plasma levels (van Praag et al. 2002; von Giesen et al. 2002). Further studies demonstrated that the degree of NVP brain uptake was higher compared to other antiviral HIV drug, such as abacavir, amprenavir, and ritonavir (Anthonypillai et al. 2004). It is worth mentioning that in the present study, we did not investigate the plasma or cerebrospinal fluid concentrations of NNRTIs, but as commented above, both drugs seem to have good CNS penetration (Tashima et al. 1999; Wynn et al. 2002; Gibbs et al. 2006), which could support the central side effects observed in our study.
Despite the growing body of evidence for CNS side effects of EFV and NVP in HIV patients, little information is available about behavioral effects of NNRTIs in the rodent CNS. In fact, O’Mahony et al. (2005) demonstrated that EFV-treated rats displayed spatial memory deficits in the Morris water maze. Rats treated with EFV also appeared to be more susceptible to stress than controls. These authors showed that the production of interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α) by rat blood cells stimulated in vitro with concanavalin A or lipopolysaccharide were significantly higher in the EFV-treated group. Additionally, the treatment with the antidepressant paroxetine reduced the susceptibility to stress and prevented such increase in pro-inflammatory cytokines. Based on these findings, the authors concluded that EFV could induce depressive-like behavior in rats, which could be due to in part the increase of pro-inflammatory cytokines into the brain (for a review, see Anisman and Merali 2002).
The elevated plus-maze test is the most widely used, well-documented and validated animal model for studying anxiety in rodents. This animal model of anxiety is based on the conflict between the tendency of mice to explore a novel environment and their natural aversion to unprotected areas (Rodgers and Dalvi 1997). In this context, anxiolytic drugs (i.e. benzodiazepines) increase the exploration to open arms. In contrast, anxiogenic agents reduce the time spent in open areas without altering spontaneous activity (Rodgers and Dalvi 1997). In the present study, we demonstrated that EFV, but not NVP, reduced the time spent in and the frequency of entries into open arms in the elevated plus-maze test. Thus, suggesting anxiogenic-like effects in mice chronically treated with EFV. Additionally, no alterations in the spontaneous locomotion have been found in mice treated with EFV and NVP in the open-field test. Altogether, these findings point to a genuine anxiogenic-like effect for EFV.
The forced swimming test is a behavioral assay widely used for assessing the effects of antidepressant drugs in rodents. Generally, antidepressants of distinct classes are able to reduce immobility time in mice and rats (Cryan et al. 2002). In this study, no alterations have been observed in the behavior of mice treated with NVP and EFV. It should be mentioned that the forced swimming is not considered an animal model of depression, since this assay did not reach the required face and construct validity (McArthur and Borsini 2006). Thus, studies employing a well-validated animal model of depression could provide additional information in this regard.
In order to assess the cognitive performance of those mice, in this study two behavioral tests were used: the inhibitory avoidance and the object recognition test. The inhibitory avoidance task is a behavioral test widely used for studying the effects of drugs on aversive memory. It is easy to use and displays quite good pharmacological prediction to amnesic and enhancer memory drugs (Gold 1986; Izquierdo and Medina 1997). Our findings indicated that mainly EFV, but in some extention NVP also, caused aversive memory impairment compared to control. In contrast to classic anxiogenic drugs, such as carbolines (Izquierdo et al. 1990), EFV did not improved aversive memory in rodents. Thus, these observations point to a genuine impairment of cognitive performance induced by EFV and NVP in mice.
The object recognition task is a behavioral assay broadly used to assess the recognition memory performance of rodents. It is important to note that the object recognition task taxes memory after only one trial (of 5 min), which makes this assay more sensitive to amnesic experimental interventions, compared to other tasks, in which incremental learning across multiple trials is induced, such as in the radial maze and water maze tasks (Dere et al. 2007). In the present study, both drugs EFV and NVP impaired object recognition memory in mice.
The underlying mechanisms of NNRTIs side effects are still poorly understood. In fact, no information is still available about the effects of EFV and NVP on central neurotransmission. However, O’Mahony et al. (2005) demonstrated that EFV could effectively increase the production of pro-inflammatory cytokines in rats, which could be, at least, relevant for depressive symptoms. Recently, our group has demonstrated that brain creatine kinase activity was significantly inhibited in cerebellum, hippocampus, striatum, and cortex of mice chronically treated with EFV and NVP (Streck et al. 2008). These observations suggest that EFV and NVP could reduce the distribution of cellular energy in the mouse CNS, thus being, at least in part, responsible for the cognitive impairment observed in EFV- and NVP-treated mice. These conclusions could be supported by the fact that knockout mice for the brain type of creatine kinase enzyme displayed cognitive impairments (Jost et al. 2002).
In conclusion, the present study demonstrated that the chronic treatment with EFV and NVP did not change explorative behavior and immobility time in the forced swimming test. However, EFV-treated mice, but not NVP, displayed increased anxiety-related behavior in the elevated plus-maze test. Additionally, EFV impaired recognition and aversive memory, while NVP-treatment specifically affected the mouse performance in the object recognition test and in the inhibitory avoidance test. These findings confirm the induction of central side effects for EFV and NVP in mice, which is vastly reported for humans. Additionally, these observations are necessary for understanding the mechanisms by which NNRTIs induce CNS side effects and contribute to the development of novel strategies to attenuate these adverse effects in patients under chronic regimens.
References
Andreatini R, Bacellar LF (1999) The relationship between anxiety and depression in animal models: a study using the forced swimming test and elevated plus-maze. Braz J Med Biol Res 32:1121–1126
Anisman H, Merali Z (2002) Cytokines, stress, and depressive illness. Brain Behav Immun 16:513–524
Anthonypillai C, Sanderson RN, Gibbs JE, Thomas SA (2004) The distribution of the HIV protease inhibitor, ritonavir, to the brain, cerebrospinal fluid, and choroid plexuses of the guinea pig. J Pharmacol Exp Ther 308:912–920
Arendt G, Nocker D, von Giesen HJ, Nolting T (2007) Neuropsychiatric side effects of efavirenz therapy. Expert Opin Drug Saf 6:147–154
Bickel M, Stephan C, Rottmann C, Carlebach A, Haberl A, Kurowsk IM, Staszewski S (2005) Severe CNS side-effect and persistent high efavirenz plasma levels in a patient with HIV/HCV coinfection and liver cirrhosis. Scand J Infect Dis 37:520–522
Brazil, Brazilian Ministry of Health, Division of Health Surveillance, National Program on STD/AIDS (2008) Recommendations on antiretroviral therapy in HIV-infected adults – 2008. Brazilian Ministry of Health, Brasília, 244 pp. Available: http://www.aids.gov.br/data/documents/storedDocuments/%7BB8EF5DAF-23AE-4891-AD36-1903553A3174%7D/%7B762E0EBF-A859-4779-8A92-704EB1F3B290%7D/consensoAdulto005c_2008montado.pdf. Accessed 12 May 2009
Choleris E, Thomas AW, Kavaliers M, Prato FS (2001) A detailed ethological analysis of the mouse open field test: effects of diazepam, chlordiazepoxide and an extremely low frequency pulsed magnetic field. Neurosci Biobehav Rev 25:235–260
Cryan JF, Markou A, Lucki I (2002) Assessing antidepressant activity in rodents: recent developments and future needs. Trends Pharmacol Sci 23:238–245
de Maat MM, ter Heine R, van Gorp EC, Mulder JW, Mairuhu AT, Beijnen JH (2003) Case series of acute hepatitis in a non-selected group of HIV-infected patients on nevirapine-containing antiretroviral treatment. AIDS 17:2209–2214
Dere E, Huston JP, De Souza Silva MA (2007) The pharmacology neuroanatomy and neurogenetics of one-trial object recognition in rodents. Neurosci Biobehav Rev 31:673–704
Fumaz CR, Munõz-Moreno JA, Moltó J, Negredo E, Ferrer MJ, Sirera G, Pérez-Alvarez N, Gómez G, Burger D, Clotet B (2005) Long-term neuropsychiatric disorders on efavirenz-based approaches: quality of life, psychologic issues, and adherence. J Acquir Immune Defic Syndr 38:560–565
Gibbs JE, Gaffen Z, Thomas SA (2006) Nevirapine uptake into the central nervous system of the Guinea pig: an in situ brain perfusion study. J Pharmacol Exp Ther 317:746–751
Gold PE (1986) The use of avoidance training in studies of modulation of memory storage. Behav Neural Biol 46:87–98
Gutiérrez F, Navarro A, Padilla S, Antón R, Masiá M, Borrás J, Martín-Hidalgo A (2005) Prediction of neuropsychiatric adverse events associated with long-term efavirenz therapy, using plasma drug level monitoring. Clin Infect Dis 41:1648–1653
Haas DW, Ribaudo HJ, Kim RB, Tierney C, Wilkinson GR, Gulick RM, Clifford DB, Hulgan T, Marzolini C, Acosta EP (2004) Pharmacogenetics of efavirenz and central nervous system side effects: an Adult AIDS Clinical Trials Group study. AIDS 18:2391–2400
Izquierdo I, Medina JH (1997) Memory Formation: the sequence of biochemical events in the hippocampus and its connection to activity in other brain structures. Neurobiol Learn Mem 68:285–316
Izquierdo I, Pereira ME, Medina JH (1990) Benzodiazepine receptor ligand influences on acquisition: suggestion of an endogenous modulatory mechanism mediated by benzodiazepine receptors. Behav Neural Biol 54:27–41
Jost CR, Van Der Zee CE, In’t Zandt HJ, Oerlemans F, Verheij M, Streijger F, Fransen J, Heerschap A, Cools AR, Wieringa B (2002) Creatine kinase B-driven energy transfer in the brain is important for habituation and spatial learning behaviour, mossy fibre field size and determination of seizure susceptibility. Eur J Neurosci 15:1692–1706
Lewis W, Haase CP, Miller YK, Ferguson B, Stuart T, Ludaway T, McNaught J, Russ R, Steltzer J, Santoianni R, Long R, Fiermonte G, Palmieri F (2005) Transgenic expression of the deoxynucleotide carrier causes mitochondrial damage that is enhanced by NRTIs for AIDS. Lab Invest 85:972–981
Lister RG (1987) The use of a plus-maze to measure anxiety in the mouse. Psychopharmacology 92:180–185
McArthur R, Borsini F (2006) Animal models of depression in drug discovery: a historical perspective. Pharmacol Biochem Behav 84:436–452
O’Mahony SM, Myint AM, Steinbusch H, Leonard BE (2005) Efavirenz induces depressive-like behaviour, increased stress response and changes in the immune response in rats. Neuroimmunomodulation 12:293–298
Phillips E, Mallal S (2007) Drug hypersensitivity in HIV. Curr Opin Allergy Clin Immunol 7:324–330
Piacenti FJ (2006) An update and review of antiretroviral therapy. Pharmacotherapy 26:1111–1133
Porsolt RD, Le Pichon M, Jalfre M (1977) Depression: a new animal model sensitive to antidepressant treatments. Nature 266:730–732
Réus GZ, Valvassori SS, Machado RA, Martins MR, Gavioli EC, Quevedo J (2008) Acute treatment with low doses of memantine does not impair aversive, non-associative and recognition memory in rats. Naunyn Schmiedebergs Arch Pharmacol 376:295–300
Rihs TA, Begley K, Smith DE, Sarangapany J, Callaghan A, Kelly M, Post JJ, Gold J (2006) Efavirenz and chronic neuropsychiatric symptoms: a cross-sectional case control study. HIV Med 7:544–548
Rivero A, Mira JA, Pineda JA (2007) Liver toxicity induced by non-nucleoside reverse transcriptase inhibitors. J Antimicrob Chemother 59:342–346
Roca B (2009) Adverse drug reactions to antiretroviral medication. Front Biosci 14:1785–1792
Rodgers RJ, Dalvi A (1997) Anxiety, defense and the elevated plus-maze. Neurosci Biobehav Rev 21:801–810
Roesler R, Walz R, Quevedo J, de-Paris F, Zanata SM, Graner E, Izquierdo I, Martins VR, Brentani RR (1999) Normal inhibitory avoidance learning and anxiety, but increased locomotor activity in mice devoid of PrP(C). Brain Res Mol Brain Res 71:349–353
Sacktor N, Lyles RH, Skolasky R, Kleeberger C, Selnes OA, Miller EN, Becker JT, Cohen B, McArthur JC (2001) HIV-associated neurologic disease incidence changes: Multicenter AIDS Cohort Study, 1990–1998. Neurology 56:257–260
Saitoh A, Sarles E, Capparelli E, Aweeka F, Kovacs A, Burchett SK, Wiznia A, Nachman S, Fenton T, Spector SA (2007) CYP2B6 genetic variants are associated with nevirapine pharmacokinetics and clinical response in HIV-1-infected children. AIDS 21:2191–2199
Streck EL, Scaini G, Rezin GT, Moreira J, Fochesato CM, Romão PRT (2008) Effects of the HIV treatment drugs nevirapine and efavirenz on brain creatine kinase activity. Metab Brain Dis 23:485–492
Tashima KT, Caliendo AM, Ahmad M, Gormley JM, Fiske WD, Brennan JM, Flanigan TP (1999) Cerebrospinal fluid human immunodeficiency virus type 1 (HIV-1) suppression and efavirenz drug concentrations in HIV-1-infected patients receiving combination therapy. J Infect Dis 180:862–864
Treisman GJ, Kaplin AI (2002) Neurologic and psychiatric complications of antiretroviral agents. AIDS 16:1201–1215
van Praag RM, van Weert EC, van Heeswijk RP, Zhou XJ, Sommadossi JP, Jurriaans S, Lange JM, Hoetelmans RM, Prins JM (2002) Stable concentrations of zidovudine, stavudine, lamivudine, abacavir, and nevirapine in serum and cerebrospinal fluid during 2 years of therapy. Antimicrob Agents Chemother 46:896–899
von Giesen HJ, Köller H, Theisen A, Arendt G (2002) Therapeutic effects of nonnucleoside reverse transcriptase inhibitors on the central nervous system in HIV-1-infected patients. J Acquir Immune Defic Syndr 29:363–367
Wise ME, Mistry K, Reid S (2002) Drug points: neuropsychiatric complications of nevirapine treatment. BMJ 324:879
Wynn HE, Brundage RC, Fletcher CV (2002) Clinical implications of CNS penetration of antiretroviral drugs. CNS Drugs 16:595–609
Acknowledgments
This research was supported by the Brazilian funding agencies: Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Fundação de Apoio à Pesquisa Científica e Tecnológica do Estado de Santa Catarina (FAPESC), and Universidade do Extremo Sul Catarinense (UNESC).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Romão, P.R.T., Lemos, J.C., Moreira, J. et al. Anti-HIV Drugs Nevirapine and Efavirenz Affect Anxiety-Related Behavior and Cognitive Performance in Mice. Neurotox Res 19, 73–80 (2011). https://doi.org/10.1007/s12640-009-9141-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-009-9141-y