Abstract
Background
Dehydration is the most common fluid and electrolyte problem among elderly patients. It is reported to be widely prevalent and costly to individuals and to the health care system. The purpose of this review is to summarize the literature on the economic burden of dehydration in the elderly.
Method
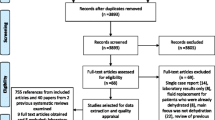
A comprehensive search of several databases from database inception to November 2013, only in English language, was conducted. The databases included Pubmed and ISI Web of Science. The search terms «dehydration» / “hyponaremia” / “hypernatremia” AND «cost» AND «elderly» were used to search for comparative studies of the economic burden of dehydration. A total of 15 papers were identified.
Results
Dehydration in the elderly is an independent factor of higher health care expenditures. It is directly associated with an increase in hospital mortality, as well as with an increase in the utilization of ICU, short and long term care facilities, readmission rates and hospital resources, especially among those with moderate to severe hyponatremia.
Conclusions
Dehydration represents a potential target for intervention to reduce healthcare expenditures and improve patients’ quality of life.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
WHO (World Health Organization) Health and ageing. 2002.
Wakefield BJ, Mentes J, Holman JE, Culp K. Risk factors and outcomes associated with hospital admission for dehydration. Rehabil Nurs [Internet]. 2008;33(6):233–41. Available from: http://www.ncbi.nlm.nih.gov/pubmed/19024237
Begum MN, Johnson CS. A review of the literature on dehydration in the institutionalized elderly. E Spen Eur E J Clin Nutr Metab [Internet]. Elsevier Ltd; 2010 Feb [cited 2014 Jun 4];5(1):e47–e53. Available from: http://linkinghub.elsevier.com/retrieve/pii/S1751499109000936
Kayser-Jones J, Schell ES, Porter C, Barbaccia JC, Shaw H. Factors contributing to dehydration in nursing homes: inadequate staffing and lack of professional supervision. [Internet]. Journal of the American Geriatrics Society. 1999. p. 1187–94. Available from: http://www.ncbi.nlm.nih.gov/pubmed/10522951
Himmelstein DU, Jones AA WS. Hypernatremic dehydration in nursing home patients: An indicator of neglect. J Am Geriatr Soc. 1983;31(8):466–71.
JC M. Oral hydration in older adults: greater awareness is needed in preventing, recognizing, and treating dehydration. Am J Nurs. 106:40-9.
Gross CR, Lindquist RD, Woolley AC, Granieri R, Allard K WB. Clinical indicators of dehydration severity in elderly patients. J Emerg Med. 1992;10(3):267–74.
Mentes JC, Chang BL, Morris J. Keeping nursing home residents hydrated. West J Nurs Res [Internet]. 2006 Jun [cited 2014 Jun 4];28(4):392–406; discussion 407–18. Available from: http://www.ncbi.nlm.nih.gov/pubmed/16672630
Borghi L, Meschi T, Amato F, Briganti A, Novarini A GA. Urinary Volume, water and recurrences in idiopathic calcium nephrolithiasis: a 5-year randomized prospective study. Urology. 1996;155:839–43.
Hughes J NR. Diet and calcium stones. Cab Ned Assoc J. 1992;146:137–43.
Lax D, Eicher M GS. Mild dehydration induces echocardiographic signs of mitral valve prolapse in healthy females with prior normal cardiac findings. Am Hear J. 1992;124(6):1533–40.
Ship JA FD. The relationship between dehydration and parotid salivary gland function in yong and older healthy adults. J Gerontol. 1997;52A:M310–M319.
Bitterman WA, Faarhadian H, Abu S-C, Lerner D, Amoun H, Krapf D MU. Environment and nutritional factors significantly associated with cancer of the urinary tract among different ethnic groups. Urol Clin North Am. 1991;18:501–18.
Wilkens LR, Kadir MM, Kolonel LN, Nomura AM HJ. Risk factors for lower urinary tract cancer: the role of total fluid consumption, nitrites and nitrosamines, and selected foods. Cancer Epidemiol, Biomarkers Prev. 1996;5:161–6.
Asadollahi K, Beeching N G. Hyponatraemia as a risk factor for hospital mortality. Q J Med. 2006;99:877–80.
Centers for Disease Control and Prevention. Heart failure fact sheet. Accessed November 12, 2013 [Internet]. Available from: http://www.cdc.gov /DHDSP/data_statistics/fact_sheets/fs_heart_failure.htm.
M F. Confusion in hospitalized elderly: Incidence, onset and associated factors. Res Nurs Health. 1989;12:21–9.
Salmon P. Nutrition cognitive performance, and mental fatigue». Nutrition. 1994;10:427–8.
LM B. Fluid balance during team sports. J Sport Sci. 1997;15:287–95.
Suhr JA, Hall J, Patterson SM NR. The relation of hydration status to cognitive performance in healthy older adults. Int J Psychophysiol. 2004;53:121–5.
Wilson MM MJ. Impaired cognitive function and mental performance in mild dehydration. Eur J Clin Nutr. 2003;57(2):24–9.
Weinberg A.D., Pals J.K., McGlinchey-Berroth R. MKL. Indices of dehydration among frail nursing home patients: highly variable but stable over time. J Am Geriatr Soc. 1994;42:1070–3.
Palevsky PM, Bhagrath R GA. Hypernatremia in hospitalized patients. Ann Intern Med,. 1996;124:197–203.
Snyder A, Fiegal DW AA. Hypernatremia in elderly patients: a heterogeneous, morbid, and iatrogenic entity. Ann Intern Med. 1987;107:309–19.
J Am Geriar Soc. Clinical presentation of hypernatremia in elderly patients. A case control study. Chass P, Druesne L, Capet C, Menard JF, Bercoff E. 2006;56:1225–30.
Terzian C, Frye EB PZ. Admission hyponatremia in the elderly: factors influencing prognosis. J Gen Intern Med. 1994;9:89–91.
Wald R, Jaber BL, Price LL, Upadhyay A, Madias NE. Impact of hospital-associated hyponatremia on selected outcomes. Arch Intern Med [Internet]. 2010 Feb 8;170(3):294–302. Available from: http://www.ncbi.nlm.nih.gov/pubmed/20142578
RC H. Age and gender as risk factors for hyponatremia and hypernatremia. Dep Pathol Lab Med. 2003;337(1–2):169–72.
Lynn J AD. Living well at end of life: adapting health care to serious chronic illness in old age. Rand Heal White Pap. 2003;137.
Davies I, O’Neill P MK. Age-associated alterations in thirst and arginine vasopressin in response to a water or sodium load. Age Ageing. 1995;24:151–9.
Lindeman RD, Tobin J SN. Longitudinal studies on the rate of decline in renal function with age. J Am Geriatr Soc. 1985;33:278–85.
Davis KM MK. Disorders of fluid balance. In: Hazard W. Principles of Geriatric Medicine and Gerontology. 1994.
Chumlea WC, Guo SS, Zeller CM, Reo NV SR. Total body water data for white adults 18 to 64 years of age: the FELS Longitudinal study. Kidney Int. 1999;56:244–52.
Sheehy CM, Perry PA CS. Dehydration: Biological Considerations, Age-Related Changes, and Risk Factors in Older Adults. Biol Res Nurs. 1999;1(1):30–7.
A M. Senescence of renal cells: molecular basis and clinical implications. Nephrol Dial Transpl. 2003;18:2474–8.
Phillips PA, Roll BJ, Ledingham JG, Forsling M, Morton J CM. Reduced thirst after water deprivation in helthy elerlymen. N Engl J Med. 1984;311:753–9.
Warren JL., Bacon W.E., Harris T., McBean A.M., Foley D.J. PC. The burden and outcomes associated with dehydration among US elderly. Am J Pub Heal. 1994;84:1265–1269.
Armstrong-Esther C a, Browne KD, Armstrong-Esther DC, Sander L. The institutionalized elderly: dry to the bone! Int J Nurs Stud [Internet]. 1996 Dec;33(6):619–28. Available from: http://www.ncbi.nlm.nih.gov/pubmed/8970859
Hodgkinson. Maintaining oral hydration in older adults: A systematic review. 2003;9(3):19–28.
Feinsod FM, Levenson SA, Rapp K, Rapp MP, Beechinor E LL. Dehydration in frail, older residents in long-term care facilities. J Am Med Dir Assoc. 2004;5(2):35–41.
AC S. Dehydration in the elderly: strategies for prevention and management. Nurse Pract. 1997;22(4):41–72.
Rajasoorya C, Holdaway IM, Wrightson P et al. Determinants of clinical outcome and survival in acromegaly. Clin Endocrinol (Oxf). 1994;41:95–102.
PM, Gaspar GN. What determines how much patients drink., Geriatr Nurs. 1988;9:221–4.
Garcia, M. Esperanza GD. Dehydration in the elderly, Nutrition Noteworthy. Nutr Noteworthy, Dep Biol Chem UCLA, David Geffen Sch Med. 2001
RJ L-M. Dehydration in the elderly: A short review! J Natl Med Assoc. 1987;79:1033–8.
Lavizzo-Mourey RJ, Johnson J SP. Risk factors for dehydration among elderly nursing home residents. JAmGeriatr Soc. 1988;36:213–8.
Carlsson M, Gustafson Y, Eriksson S HL. Body composition in Swedish old people aged 65–69 years, living in residential care facilities. Arch Gerontol Geriatr. 2009;49:98–107.
Farrell MJ, Zamarripa F, Shade R et al. Effect of aging on regional cerebral blood flow responses associated with osmotic thirst and its satiation by water drinking: a PET study. PNAS. 2008;105:382–7.
Hong X., Janet B. ES. Economical, Burden of Dehydration among elderly hospitalized patients. Am J Heal Pharm. 2004;61.
Warren JL, Bacon WE, Haris T, Mcbean AM, Foley DJ, Phillips C.. * ¢- j } ! _ ]. 1991;1265–9.
Haveman-Nies A, de Groot LC VSW. Fluid intake of elderly Europeans. J Nutr Heal Aging. 1997;1(3):151–5.
Shea AM, Hammill BG, Curtis LH, Szczech L a, Schulman K a. Medical costs of abnormal serum sodium levels. J Am Soc Nephrol [Internet]. 2008 Apr [cited 2014 Jun 4];19(4):764–70. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2390974&tool=pmcentrez&rendertype=abstract
Glaser R, Naidu SS, Selzer F, Jacobs AK, Laskey WK, Srinivas VS, et al. Factors associated with poorer prognosis for patients undergoing primary percutaneous coronary intervention during off-hours: biology or systems failure? JACC Cardiovasc Interv [Internet]. American College of Cardiology Foundation; 2008 Dec [cited 2014 Apr 29];1(6):681–8. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2774122&tool=pmcentrez&rendertype=abstract
Curtze S, Meretoja A, Mustanoja S, Putaala J, Lindberg T, Leppä M, et al. Does time of day or physician experience affect outcome of acute ischemic stroke patients treated with thrombolysis? A study from Finland. Int J Stroke [Internet]. 2012 Aug [cited 2014 May 16];7(6):511–6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/22494345
P S. The risk of hyponatremia in the elderly compared with younger in the hospital inpatient and outpatient. JIndonesian ournal Intern Med. 2011;13(3):158–61.
Sunderam SG M. Hyponatraemia in the elderl,. Review. Age Ageing. 1983;12(1):77–80.
JC M. A typology of oral hydration problems exhibited by frail nursing home residents. J Gerontol Nurs. 2006;32(1):13–9.
Amin A, Deitelzweig S, Christian R, Friend K, Lin J, Belk K, et al. Evaluation of incremental healthcare resource burden and readmission rates associated with hospitalized hyponatremic patients in the US. J Hosp Med [Internet]. 2012 Oct [cited 2014 Jun 4];7(8):634–9. Available from: http://www.ncbi.nlm.nih.gov/pubmed/22961813
Turgutalp K, Ozhan O, Gok Oguz E, Horoz M, Camsari A, Yilmaz A, et al. Clinical features, outcome and cost of hyponatremia-associated admission and hospitalization in elderly and very elderly patients: a single-center experience in Turkey. Int Urol Nephrol [Internet]. 2013 Feb [cited 2014 Jun 4];45(1):265–73. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23065433
Amin A, Deitelzweig S, Christian R, Friend K, Lin J, Lowe TJ. Healthcare resource burden associated with hyponatremia among patients hospitalized for heart failure in the US. J Med Econ [Internet]. 2013 Jan [cited 2014 Jun 4];16(3):415–20. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23336297
Mukand J A, Cai C, Zielinski A, Danish M, Berman J. The effects of dehydration on rehabilitation outcomes of elderly orthopedic patients. Arch Phys Med Rehabil [Internet]. 2003 Jan [cited 2014 Jun 8];84(1):58–61. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12589621
Zilberberg MD, Exuzides A, Spalding J, Foreman A, Jones AG, Colby C, et al. Hyponatremia and hospital outcomes among patients with pneumonia: a retrospective cohort study. BMC Pulm Med [Internet]. 2008 Jan [cited 2014 Jun 4];8:16. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2531075&tool=pmcentrez&rendertype=abstract
Zilberberg MD, Exuzides A, Spalding J, Foreman A, Jones AG, Colby C, et al. Epidemiology, clinical and economic outcomes of admission hyponatremia among hospitalized patients. Curr Med Res Opin [Internet]. 2008 Jun [cited 2014 Jun 4];24(6):1601–8. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18426691
Elixhauser A, Yu K SC et al. Hospitalizations in the United States., 2000; AHRQ,1997. Rockville, MD Agency Healthc Res Qual AHRQ,1997. 2000;00-0031.
1997 HCUP Nationwide Inpatient Sample (NIS) Design Report [Internet]. Available from: http://www.hcup-us.ahrq.gov/db/nation/nis/reports/NIS_1997_Design_ Report.jsp
Chin MH GL. Correlates of major complications or death in patients admitted to the hospital with congestive heart failure. Arch Intern Med [Internet]. 1996;156:1814–20. Available from: http://www.ncbi.nlm.nih.gov/pubmed/8790075.
Shorr AF, Tabak YP, Johannes RS, Gupta V, Saltzberg MT, Costanzo MR. Burden of sodium abnormalities in patients hospitalized for heart failure. Congest Heart Fail [Internet]. 2011 [cited 2014 Jun 4];17(1):1–7. Available from: http://www.ncbi.nlm.nih.gov/pubmed/21272220
Gheorghiade M, Abraham WT, Albert NM, Gattis Stough W, Greenberg BH, O’Connor CM, et al. Relationship between admission serum sodium concentration and clinical outcomes in patients hospitalized for heart failure: an analysis from the OPTIMIZE-HF registry. Eur Heart J [Internet]. 2007 Apr [cited 2014 Jun 8];28(8):980–8. Available from: http://www.ncbi.nlm.nih.gov/pubmed/17309900
Rabinovitz A, Raiszadeh F, Zolty R. Association of hyponatremia and outcomes in pulmonary hypertension. J Card Fail [Internet]. Elsevier Inc; 2013 Aug [cited 2014 Jun 8];19(8):550–6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23910584
Doshi SM, Shah P, Lei X, Lahoti A SA. Hyponatremia in hospitalized cancer patients and its impact on clinical outcomes,. Am J Kidney Dis. 2012;59(2):222–8.
Callahan MA1, Do HT, Caplan DW Y-FK. Economic impact of hyponatremia in hospitalized patients: a retrospective cohort study. Postgr Med. 2009;12(2):186–91.
Wakefield BJ, Mentes J, Holman JE, Culp K. Risk factors and outcomes associated with hospital admission for dehydration. Rehabil Nurs [Internet]. 2008;33(6):233–41. Available from: http://www.ncbi.nlm.nih.gov/pubmed/19024237
Movig KL, Leufkens HG, Lenderink AW EA. Validity of hospital discharge International Classification of Diseases (ICD) codes for identifying patients with hyponatremia,. J Clin Epidemiol. 2003;56:530–5.
Waikar SS, Mount DB, Curhan GC. Mortality after hospitalization with mild, moderate, and severe hyponatremia. Am J Med [Internet]. Elsevier Inc.; 2009 Sep [cited 2014 Jun 8];122(9):857–65. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3033702&tool=pmcentrez&rendertype=abstract
Hoorn EJ LJ& ZR. Acute and concomitant deterioration of hyponatremia and renal dysfunction associated with heart and liver failure. Clin Nephrol. 2006;65:248–55.
Licata G, Di Pasquale P, Parrinello G, Cardinale A, Scandurra A, Follone G, Argano C, Tuttolomondo A PS. Effects of high dose furosemide and small-volume hypertonic saline solution infusion in comparison with a high dose of furosemide as bolus in refractory congestive heart failure: Long-term effects. Am Hear J. 2003;145:456–66.
Leadbetter RA, Shutty MS Jr, Higgins PB PD. Multidisciplinary approach to psychosis, intermittent hyponatremia, and polydipsia. Schizophr Bull. 1994;20:375–385.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Frangeskou, M., Lopez-Valcarcel, B. & Serra-Majem, L. Dehydration in the elderly: A review focused on economic burden. J Nutr Health Aging 19, 619–627 (2015). https://doi.org/10.1007/s12603-015-0491-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0491-2