Abstract
Permanent implants are going to be replaced by the implementation of biodegradable magnesium-based implants in fixation of internal bone fractures because of many concerns associated with conventional implants. However, biodegradable magnesium-based biomaterials exhibit higher biodegradation rate and low mechanical properties which are the main challenges. This work aims to almost overcome both disadvantageous by grain refining of a WE43 magnesium alloy containing 93.04 wt% Mg, 4.12 wt% Y, 2.15 wt% Nd, 0.43 wt% Zr, and 0.26 wt% La. In this study, the consequences of combined severe plastic deformation (SPD) on the mechanical properties, microstructure, and in vivo degradation behavior of WE43 magnesium alloy were investigated. To do so, WE43 magnesium alloy was chosen and processed through multi-pass equal channel angular pressing (ECAP) at 330 °C for up to four passes followed by an extrusion process. The results showed that higher strength and hardness with minimum ductility less was obtained in the sample processed via two-pass ECAP followed by extrusion. In vivo biodegradation experiments showed higher degradation rate for the unprocessed coarse-grained (CG) WE43 sample. The two-pass ECAP and extruded sample with ultrafine-grained (UFG) structure exhibited the lowest in vivo biodegradation rate besides appropriate mechanical properties. It may be concluded that the WE43 magnesium alloy processed via two-pass ECAP and extrusion could be a very promising candidate for biodegradable implants from both mechanical and biocorrosion viewpoints.
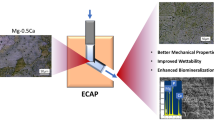
Graphic abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Using metallic implants in order to assist the bone fracture recovery has been developed in the last few decades. Appropriate mechanical properties such as tensile strength, hardness, load-bearing properties, and suitable formability led to a considerable increase in the implementation of these materials [1]. Proper biocompatibility is the key factor in the material selection process [2, 3]. Titanium and stainless steel are commonly used materials in bone implants [4, 5]. However, current biomaterials which are used in the case of plates, pins, and screws are removed after bone recovery due to infection, pain, and discomfort, tissue irritation and interference with radiological imaging [6, 7]. Moreover, the plastic module of former materials does not conform to natural bone tissue that causes stress-shielding effects [8]. Biodegradable biomaterials have been widely investigated to reduce these concerns. Magnesium and its alloys are among the major candidates for this purpose. Moreover, desirable mechanical properties, i.e., density of 1.74 g·cm−3, the elastic modulus of 45 GPa and yield strength of 65–100 MPa which are closer to those of the natural bone in comparison with titanium and stainless steel, make this material more appropriate [9]. However, the low corrosion resistance of magnesium and its alloys is one of the main factors limiting their usage. This disadvantage is alleviated using proper alloy compositions [10, 11]. Elements such as calcium, rare earth, and aluminum are the most commonly used components for alloying [12]. Surface treatment and coatings, as well as alloying, can improve the corrosion behavior of magnesium [13,14,15]. Coatings and protective films are the surface treatment examples which inhibit direct magnesium surface contact with the surrounding fluids [16,17,18]. Subsequence processes such as rolling [19] or extruding [20] are other solutions to enhance corrosion behavior of magnesium and its alloys. Grain refinement in these processes has an effective role in the sample corrosion properties [19, 20]. Grain boundaries perform as physical barriers which affect the corrosion behavior. In other words, finer grains result in the increase in the number of grain boundaries that reduce the corrosion rate [21]. The degradation of magnesium and its alloys in physiological fluids can be explained according to the following reactions [22]:
Anodic reaction:
Cathodic reaction:
Product formation:
According to the former reactions, magnesium corrosion is accompanied by hydrogen gas creation which is dependent on magnesium corrosion rate. The high corrosion rate of magnesium causes hydrogen accumulation as subcutaneous gas bubbles which are not suitable for clinical applications [23, 24].
Before testing in animals, examination of new magnesium alloy under the standard condition is usually accomplished to determine cytotoxicity and corrosion behavior. Cytotoxicity comparison of magnesium implants between the cell and cancerous origin (human osteosarcoma cell line MG63) is carried out by Fischer et al. [25]. It is reported that higher tolerance toward magnesium extracts for osteoblasts is accomplished as to MG63 [25]. In a similar study, Feyerabend et al. tested rare earth elements on primary mesenchymal stem cells, MG63, and a RAW 264.7 tumor-derived mouse cell line [9, 26]. It was observed that the toleration in REE salts is superior for a primary mesenchymal cell in accordance with other samples [26]. Many studies have investigated the corrosion behavior of magnesium in vitro conditions. In some researches, the weight loss method is accomplished to determine the degradation rate [27, 28]. Another procedure is to measure Mg2+ released from alloy by colorimetric method using inductively coupled plasma atomic emission spectroscopy or xylidyl blue I [9, 29,30,31]. However, in vitro experiments are inadequate to anticipate in vivo corrosion rates trustworthily, but it can be used to compare corrosion behavior of various alloys under standardized circumstances.
One of the first in vivo researches on magnesium implants was investigated by Witte et al. [32]. In his study, implants were prepared from pure magnesium, but the results because of large gas cavities, pain, and local swelling were not acceptable [32]. In another study, Troitskii and Tsitrin [33] used plates and screws which were prepared from magnesium, alloyed with cadmium. Plates and screws were implanted in 39 cases to secure different fractures. The mechanical integrity of the implants after 6–8 weeks and complete degradation after 10–12 months were reported [33]. However, 9 cases of the 34 cases due to infection or difficulties that were occurred while mounting of the plaster cast were unsuccessful [33]. McBRIDE [23] used screws, plates, pegs, and bands which were devised from magnesium–aluminum–manganese alloys in order to secure 20 fractures and bone grafts. By other reports, magnesium alloy usage resulted in no systemic or inflammatory reactions next to the implant [23]. Degradation comparison of magnesium-based alloys is developed by Witte et al. [34]. In their study, the comparison between AZ31 and AZ91 containing only aluminum and zinc, and WE43 and LAE442 containing rare earth alloys is developed [34]. The implants were prepared with 1.5 mm in diameter and 20 mm in length and implanted in the femur of guinea pig, and implant absorption was carried out in 18 weeks [34]. Results showed no harmful effects due to the subcutaneous gas formation. Also, the slowest corrosion rate was observed for LAE442 alloy, while three other implants were degraded with the same rate [34]. Recently, it was shown that grain refinement of WE43 alloy by SPD could enhance the mechanical properties to almost the level of conventional implants such as stainless steel [35,36,37,38]. However, there is almost no investigation on in vivo biodegradability of this important alloy. In this study, the consequences of combined severe plastic deformation (SPD) on the mechanical properties, microstructure, and in vivo degradation behavior of WE43 magnesium alloy were investigated.
2 Experimental
2.1 Experimental details
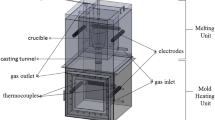
The WE43 magnesium alloy (ELEKTRON WE43 CASTINGS) with chemical composition of 93.04 wt% Mg, 4.12 wt% Y, 2.15 wt% Nd, 0.43 wt% Zr, and 0.26 wt% La in mass fraction was used as the experimental material. Equal channel angular pressing (ECAP) process was performed up to four passes using Bc route at the temperature of 330 °C. Before the process, molybdenum disulfide (MoS2) was applied in order to decrease the friction during process and sample lubrication. The ECAP die consists of two channels with 10 mm in diameter which intersect to each other with a channel angle of φ = 90° and the curvature angle of ψ = 20°, as shown in Fig. 1. Samples used in this study were cut out by electro-discharge machining into 10 mm diameter and 70 mm length. After the ECAP process, the samples were extruded using an extrusion die with a 10-mm entrance and 5-mm exit channel.
Tensile test samples were prepared from the unprocessed sample and strengthened specimens after the extrusion process. Processed and unprocessed samples were machined to tensile test samples with 10 mm in gage length and 3 mm in diameter. Tensile tests were performed at a strain rate of 1 × 10−3 s−1 at room temperature.
2.2 Characterizations
The microstructural observation was investigated using optical microscopy (OM). For this purpose, specimens were prepared from the middle of ECAPed rods perpendicular to the pressing direction, then polished and etched using a solution of 70 ml ethanol, 10 ml acetic acid, 10 ml distilled H2O and 4.2 g picric acid at room temperature. The microstructures of unprocessed and ECAPed + extruded samples were investigated using an Olympus BH-2 OM. X-ray diffraction (XRD) and energy-dispersive X-ray spectroscopy (EDS) were also used to examine various phases and elements existed in the microstructure. The scans were developed over an area of 1 mm × 1 mm with an accelerating voltage of 20 kV and scanning speed of 4 (°)·min−1 using a high-resolution X-ray diffractometer (Rigaku, Japan) with a rotating copper anode (Cu Kα1) radiation. Vickers microhardness test was conducted on the cross section of each sample with a load of 1 N applied for 10 s.
2.3 Implants
The implants were designed as a cannulated screw with 25 mm in length, 3.7 mm in shaft diameter in the screw head, 3 mm in shaft diameter in the screw tip, and 2 mm in the bore diameter. Furthermore, to gain interfragment compression, different pitches (1.00 and 1.25 mm) were considered in the screw design. At first, samples were machined from raw material and then were undergone ECAP and extrusion processes. The number of ECAP passes varied from one to four, while the extrusion process was only performed once after ECAP pass(es). Finally, implants were obtained by machining of strengthened samples. Raw samples were extruded after one, two, and four passes of ECAP.
2.4 Animal experiment and surgery
All experiments fulfilled the instructions of the Iran Animal Care Committee and were authorized by the faculty of veterinary medicine animal care committee. One young male dog (body weight of 18 kg) was chosen for the experiment. Cefazolin (20 mg·kg−1) was administered intravenously as preoperative antimicrobial prophylaxis. Ketamine (Alfasan, Woerden, The Netherlands) and diazepam (Caspian, Iran) were used to anesthetize the animal. After induction, the animal was intubated, and anesthesia was maintained using inhaled isoflurane (Terrell, Piramal Critical Care, USA). Both femurs were exposed by blunt dissection. Two holes with 3 mm in diameter and 120 mm in distance were drilled on the femur bone. Then each hole was tapped, and the screws were implanted in the former holes. Raw, four-pass ECAPed + extruded, two-pass ECAPed + extruded, and one-pass ECAPed + extruded screws were implanted in the left proximal femur, left distal femur, right proximal, and right distal femur, respectively. After irritation with normal saline 0.9%, muscles were sutured simply interrupted by polyglycolic acid 2.0 suture material. Subcutaneous tissue and skin were sutured by polyglycolic acid 3.0 and stainless-steel stapler. Antibiotic therapy and analgesia were performed using cefazolin (22 mg·kg−1) in the first week after surgery and tramadol (2 mg·kg−1) for three days, respectively.
2.5 Postoperative treatment and radiographic evaluation
Postop radiographic was conducted in order to be sure that the screws were secured appropriately. One week after surgery, the second radiography was accomplished to investigate the screws compatibility with the tissues and to ensure the position of implants. Additional radiographs were performed with three intervals (1, 6, and 12 weeks after surgery) to examine the degradation process and feasible formation of gas cavity detection.
2.6 In vivo degradation
The implants were removed after 85 days of surgery in order to examine degradation and to characterize formed films on the screws surface. Among the samples, unprocessed screw because of the whole degradation of the screw head and two-pass ECAPed + extruded screw due to locking between the screw threads and bone tissue, was broken. SEM and EDS were conducted on one- and four-pass ECAPed + extruded screws for the surface morphology and elemental composition.
2.7 Histopathology
Histopathology studies were performed in the pathological laboratory of the Faculty of Veterinary Medicine, the University of Tehran, for the bone tissues which were collected after 12 weeks of implantation. Samples were cut to 50 mm in length with screw in the center and were retained in formalin solution. Afterward, those were inserted in paraffin and were cut into 5-μm-thin slices.
3 Results and discussion
3.1 Microstructure
The microstructure of as-cast and strengthened WE43 alloy is demonstrated in Fig. 2. Two phases of α-Mg and Mg41Nd5 existed in the microstructure. These phases were accomplished by XRD pattern taken from the unprocessed sample, as shown in Fig. 3. Microstructural examinations were performed on the cross section of the specimens sliced transverse to the pressing direction. Figure 2 shows that the increase in ECAP passes leads to grain refinement. The grain size decreases from ~ 135 μm in the unprocessed sample to ~ 50 μm after the fourth pass of the ECAP process. The content of recrystallized grains increases by the enhancement of deformation passes, and the average grain size decreases. Besides grain refinement, the size of intermetallic phases is reduced significantly and distributed along the grain boundaries and grain interior regions. Also, the dissolution of intermetallic phases takes place because of processing at elevated temperatures [39]. Grain refinement procedure is schematically demonstrated in Fig. 4. An increase in ECAP passes not only enhances the homogeneity of the structure but also develops the amount of grain boundaries.
As can be seen in Fig. 2, new grains nucleated near the initial grain boundaries. During the process, accumulation of dislocations occurs through the grains. Subgrain boundaries consist of low-angle grain boundaries (LAGBs). Performing further ECAP passes increases plastic strain in the specimens. Consequently, subboundaries absorb newly created dislocations in subgrains and it changes the low-angle grain boundaries to high-angle grain boundaries (HAGBs), which makes the structure equiaxed. Therefore, nucleation of new finer grains is taken place along grain boundaries [40, 41]. Furthermore, some rare elements (RE) such as Y are in the composition of the alloy, and they inhibit the movement of grain boundaries known as Zener pinning effect [38]. In addition, dynamic recrystallization postpones due to the presence of Y in WE43 alloy composition, representing lower DRX rate in comparison with other Mg alloys [42]. It also can be concluded that the extrusion process makes equiaxed grains achieved by ECAP process change to elongated grains.
Grain refinement procedure in multi-pass ECAP process is illustrated in Fig. 4. The first pass of the ECAP process is performed on coarse α-Mg grains and dispersed Mg41Nd5 phase of the unprocessed sample. Consequently, nucleation of new grains with some new Mg41Nd5 phase is taken place along the initial grain boundaries (Fig. 4b). Performing the two passes of ECAP makes the structure more homogenous, enhances fraction of new grains, and forms new dynamically recrystallized grains. However, some coarse grains exist in the structure (Fig. 4c). Finally, by operating the fourth pass of the ECAP process, a new structure including fine homogenous grains which contain full crystallized grains with Mg41Nd5 phase is achieved (Fig. 4d). It is also mentioned by Zhang et al. [43] that in Zr-contained Mg alloys, existence of Zr in the composition of Al-free Mg alloys eases the grain refinement.
3.2 Tensile properties
Figure 5 demonstrates comparison of tensile properties between unprocessed and ECAPed + extruded samples with different ECAP passes. It shows that samples strengthened with ECAP and extrusion processes represent excellent mechanical properties. Two significant conclusions can be derived from this plot. At first, both yield strength (YS) and ultimate tensile stress (UTS) are enhanced after the two passes of ECAP and extrusion processes but reduced after the fourth pass of ECAP and extrusion, although the microstructure is refined with an increase in ECAP passes. It can be observed that the UTS of the sample after two-pass ECAP and extrusion processes is 398 MPa which is 150 MPa (about 60%) higher than that of the unprocessed sample. The second conclusion is that the one-pass ECAP strengthened and the extruded sample has the best mechanical properties (sum of tensile strength and ductility) in comparison with other samples. Table 1 summarizes the YS, UTS, and elongation to failure data. It is worthy to mention that sample strengthening in magnesium and its alloys is dependent on both grain size and texture [40, 44].
According to Hall–Petch relation, grain refinement improves mechanical properties like yield strength and ultimate tensile stress. However, after the fourth passes of ECAP and extrusion process, YS and UTS decrease. It is worth to mention that yield stress of Mg alloys depends on both texture and grain size. Different grain sizes in ECAP Mg alloys represent different textures. In fact, yield stress is reduced as the number of ECAP passes increases [40]. This behavior is also observed in other researches. Experimental texture evolution of WE43 was investigated in Agnew et al.’s study [45]. Signatures of prismatic slip mode’s activity were exhibited after the first pass of the ECAP process. Signatures of extensive <c+a> slip and considerable prismatic slip were displayed in further passes of ECAP. Another investigation is accomplished by Akbaripanah et al.’s study [46] on AM60 magnesium alloy; texture modification has an effective role in magnesium and its alloys. It is important to note that dislocation density enhancement because of plastic deformation also improves YS and UTS.
3.3 Microhardness
Microhardness test was performed on the raw and ECAP + extruded samples, and the results are depicted in Fig. 6. Each microhardness value is the average of at least 8 tests with 5% scatter error. The more the ECAP passes are, the more the Vickers hardness is.
Figure 6 shows that grain refinement due to the applied strain results in the increase in Vickers hardness, which is in conformance with Hall–Petch relation for severely deformed ultrafine materials [47]. Additionally, plastic deformation causes the increase in microhardness due to a reduction in sample cross section during the extrusion process. Plastic strain accumulation increases dislocation density, leading to microhardness enhancement [38].
3.4 In vivo studies
Figure 7 illustrates the photographs of the implants before and after 12 weeks postsurgery. After this period, the unprocessed implant was considerably degraded and cannot be exited from the bone tissue. The contact between implant after two passes of ECAP and extrusion process and the bone tissue is so great that it was broken during exiting. Two other implants (screws after one and four passes of ECAP and extrusion process) were completely removed and prepared for SEM and EDX analysis.
3.4.1 Radiographs
Figure 8 indicates the region of implanting in the femur of a dog. The implant is shown via arrow marks. Figure 9 demonstrates the femoral bone of the dog after diverse periods of time. It can be seen that implants were degraded with various corrosion rates, and after 12 weeks of implantation, the samples were not degraded completely.
It can visually figure out from the radiographs in Fig. 9 that the implant degradation rate is diverse. As illustrated in radiography images, two-pass ECAPed sample has been degraded lower than other strengthened samples and one-pass ECAPed sample has the most degradation rate. This result can be described as follows: due to new grain nucleation, the energy of grain boundary increases after the first pass of ECAP; on the other hand, the existence of new seeds of Mg41Nd5 phase near α-Mg matrix leads to galvanic corrosion. Indeed, synergies of galvanic corrosion and grain boundary corrosion make one-pass ECAPed sample to be the most corroded sample. Since two-pass ECAP sample contains less grain boundary density, because of more coarse grains in comparison with four-pass ECAP sample, the corrosion rate of two-pass ECAP sample is lower than that of the four-pass ECAP sample. In addition, the lack of Mg41Nd5 phase in grain boundaries of four-pass ECAP sample results in fewer galvanic corrosion in comparison with one-pass ECAP sample. Furthermore, among all the samples, the most corrosion rate belongs to the unprocessed specimen which contains superior Mg41Nd5 phase. As can be seen in Fig. 2, unprocessed sample consists of the most Mg41Nd5 phases, leading to higher galvanic corrosion in the raw sample in comparison with other samples. According to Cao et al.’s studies on Mg-RE alloys, many alloys containing Zr, Nd, La, Y, Gd, and Al do not have strong passivity ability and form some films on the surface of Mg alloys that are not protective [48]. This behavior results in the exhibition of passivity in the aforementioned Mg alloys. Moreover, magnesium decay implies that the amount of emerged hydrogen near the bone is low and hydrogen has escaped across the cell membrane which makes no sign of hydrogen accumulation in this region. It is obvious that implant degradation causes no health abnormality to the dog.
3.4.2 Surface analysis
Figure 10 shows SEM image implant surface. SEM images of the one-pass ECAPed + extruded and four-pass ECAPed + extruded samples after 12 weeks of implantation are demonstrated in Figs. 11 and 12. The comparative elemental composition of the deposited mineral phase on the samples can be investigated by evaluating area EDS analysis on the tip, middle, and end of the specimens. Rapid mineralization of the sample is worked out by comparing the two samples. According to EDS analysis, the major components of phases above are figured out to be Mg, Ca, P, O, C, and Y. Attendance of Ca and P on the surface of two sample evidences that some Ca/P mineral phases are formed after the implantation test. Irregular cracks can be detected on the surface of the specimens.
3.4.3 Histopathology
Figure 13 illustrates the histology photographs of the dog’s bone tissue after 12 weeks of implantation. New chondrocytes in matrices (depicted by the black arrow) were presented in the ECAP sample implanted tissue, evidencing the new bone fabrication. Histological results of the samples were investigated to measure the vitality of the bone tissues, bone to implant contact, and level of inflammation.
Level of inflammation in the unprocessed sample was in grade 4 which represents severe inflammation in this sample (existence of more than 50 inflammation cells in a tissue). It was in grade 3 for one-pass ECAPed and two-pass ECAPed samples (existence of 10–50 inflammation cells in a tissue) and in grade 2 for four-pass ECAPed sample (existence of 10–50 inflammation cells in a tissue). It can be concluded that a mild inflammatory response in the four-pass ECAPed sample in comparison with the unprocessed sample suggests more biocompatibility in that sample.
According to the results illustrated in Table 2, vitality in all of the samples is positive, proving the existence of osteocyte in Lacuna. Collagen sequences were regular, suggesting that the bone is in good order. Bone to implant contact in all samples was connected. In total, 3–9 cellular layers containing collagen and fibrosis were observed in all connected tissues. Comparison between one-pass ECAPed and four-pass ECAPed with unprocessed and two-pass ECAPed samples could not be established due to that tissue gets out when removing the implants.
To put everything in a nutshell, it can be noticed that the degradation behavior of WE43 magnesium alloy is affected by the grain size of the samples. Finer grain size leads to fast mineralization and greater implant–tissue interaction that promotes lowering the degradation rate. Severe plastic deformation which modifies microstructure of the samples can be used to implement advantages of ultrafine grain structuring in new developing degradable magnesium-based implants. Different types of degradable orthopedic implants including rods, plates, fixtures, nails, and screws can be manufactured using ECAP process by producing bulk ultrafine-grained metals to stabilize fractured bones.
4 Conclusion
This work aims to almost overcome both disadvantageous by grain refining of WE43 magnesium alloy. In this study, the consequences of combined severe plastic deformation (SPD) on the mechanical properties, microstructure, and in vivo degradation behavior of WE43 magnesium alloy were investigated. To do so, WE43 magnesium alloy was chosen and processed through ECAP at 330 °C for up to four passes followed by an extrusion process. The results showed that higher strength and hardness with minimum ductility less was obtained in the sample processed via two-pass ECAP followed by extrusion. In vivo biodegradation experiments showed higher degradation rate for the unprocessed coarse-grained (CG) WE43 sample. The two-pass ECAP and extruded sample with ultrafine-grained (UFG) structure exhibit the lowest in vivo biodegradation rate besides appropriate mechanical properties. Furthermore, the degradation of magnesium alloy resulted in no harmful health effects on the animal body. It may be concluded that the WE43 magnesium alloy processed via two-pass ECAP and extrusion could be a very promising candidate for biodegradable implants from both mechanical and biocorrosion viewpoints.
References
Staiger MP, Pietak AM, Huadmai J, Dias G. Magnesium and its alloys as orthopedic biomaterials: a review. Biomaterials. 2006;27(9):1728.
Waizy H, Diekmann J, Weizbauer A, Reifenrath J, Bartsch I, Neubert V, Schavan R, Windhagen H. In vivo study of a biodegradable orthopedic screw (MgYREZr-alloy) in a rabbit model for up to 12 months. J Biomater Appl. 2014;28(5):667.
Mahmoodian R, Annuar NSM, Faraji G, Bahar ND, Razak BA, Sparham M. Severe plastic deformation of commercial pure titanium (CP-Ti) for biomedical applications: a brief review. JOM. 2019;71(1):256.
Castellani C, Lindtner RA, Hausbrandt P, Tschegg E, Stanzl-Tschegg SE, Zanoni G, Beck S, Weinberg AM. Bone–implant interface strength and osseointegration: biodegradable magnesium alloy versus standard titanium control. Acta Biomater. 2011;7(1):432.
Reshadi F, Faraji G, Baniassadi M, Tajeddini M. Surface modification of severe plastically deformed ultrafine grained pure titanium by plasma electrolytic oxidation. Surf Coat Technol. 2017;316:113.
Meslemani D, Kellman RM. Recent advances in fixation of the craniomaxillofacial skeleton. Curr Opin Otolaryngol Head Neck Surg. 2012;20(4):304.
Chaya A, Yoshizawa S, Verdelis K, Myers N, Costello BJ, Chou DT, Pal S, Maiti S, Kumta PN, Sfeir C. In vivo study of magnesium plate and screw degradation and bone fracture healing. Acta Biomater. 2015;18:262.
Nagels J, Stokdijk M, Rozing PM. Stress shielding and bone resorption in shoulder arthroplasty. J Shoulder Elbow Surg. 2003;12(1):35.
Waizy H, Seitz JM, Reifenrath J, Weizbauer A, Bach F-W, Meyer-Lindenberg A, Denkena B, Windhagen H. Biodegradable magnesium implants for orthopedic applications. J Mater Sci. 2013;48(1):39–50.
Gu X, Zheng Y, Cheng Y, Zhong S, Xi T. In vitro corrosion and biocompatibility of binary magnesium alloys. Biomaterials. 2009;30(4):484.
Zhang S, Zhang X, Zhao C, Li J, Song Y, Xie C, Tao H, Zhang Y, He Y, Jiang Y, Bian Y. Research on an Mg–Zn alloy as a degradable biomaterial. Acta Biomater. 2010;6(2):626.
Witte F, Hort N, Vogt C, Cohen S, Kainer KU, Willumeit R, Fererabend F. Degradable biomaterials based on magnesium corrosion. Curr Opin Solid State Mater Sci. 2008;12(5):63.
Zhang Y, Zhang G, Wei M. Controlling the biodegradation rate of magnesium using biomimetic apatite coating. J Biomed Mater Res B Appl Biomater. 2009;89(2):408.
Gu X, Zheng W, Cheng Y, Zheng Y. A study on alkaline heat treated Mg–Ca alloy for the control of the biocorrosion rate. Acta Biomater. 2009;5(7):2790.
Hänzi AC, Gunde P, Schinhammer M, Uggowitzer PJ. On the biodegradation performance of an Mg–Y–RE alloy with various surface conditions in simulated body fluid. Acta Biomater. 2009;5(1):162.
Gray J, Luan B. Protective coatings on magnesium and its alloys—a critical review. J Alloy Compd. 2002;336(1):88.
Song G. Recent progress in corrosion and protection of magnesium alloys. Adv Eng Mater. 2005;7(7):563.
Chiu K, Wong M, Cheng F, Man H. Characterization and corrosion studies of fluoride conversion coating on degradable Mg implants. Surf Coat Technol. 2007;202(3):590.
Wang H, Estrin Y, Fu H, Song G, Zuberova Z. The effect of pre-processing and grain structure on the bio-corrosion and fatigue resistance of magnesium alloy AZ31. Adv Eng Mater. 2007;9(11):967.
Hamu GB, Eliezer D, Wagner L. The relation between severe plastic deformation microstructure and corrosion behavior of AZ31 magnesium alloy. J Alloy Compd. 2009;468(1):222.
Aung NN, Zhou W. Effect of grain size and twins on corrosion behaviour of AZ31B magnesium alloy. Corros Sci. 2010;52(2):589.
Yang L, Zhang E. Biocorrosion behavior of magnesium alloy in different simulated fluids for biomedical application. Mater Sci Eng C. 2009;29(5):1691.
McBRIDE ED. Absorbable metal in bone surgery: a further report on the use of magnesium alloys. J Am Med Assoc. 1938;111(27):2464.
McCord C, Prendergast J, Meek S, Harrold G. Chemical gas gangrene from metallic magnesium. Ind Med. 1942;11(2):71.
Fischer J, Pröfrock D, Hort N, Willumeit R, Feyerabend F. Reprint of: improved cytotoxicity testing of magnesium materials. Mater Sci Eng B. 2011;176(20):1773.
Feyerabend F, Fischer J, Holtz J, Witte F, Willumeit R, Drücker H, Vogt C, Hort N. Evaluation of short-term effects of rare earth and other elements used in magnesium alloys on primary cells and cell lines. Acta Biomater. 2010;6(5):1834.
Li Y, Hodgson PD, Ce Wen. The effects of calcium and yttrium additions on the microstructure, mechanical properties and biocompatibility of biodegradable magnesium alloys. J Mater Sci. 2011;46(2):365.
Harandi SE, Idris MH, Jafari H. Effect of forging process on microstructure, mechanical and corrosion properties of biodegradable Mg–1Ca alloy. Mater Des. 2011;32(5):2596.
Gu X, Li N, Zheng Y, Ruan L. In vitro degradation performance and biological response of a Mg–Zn–Zr alloy. Mater Sci Eng B. 2011;176(20):1778.
Yamamoto A, Hiromoto S. Effect of inorganic salts, amino acids and proteins on the degradation of pure magnesium in vitro. Mater Sci Eng C. 2009;29(5):1559.
Zhang E, Yang L. Microstructure, mechanical properties and bio-corrosion properties of Mg–Zn–Mn–Ca alloy for biomedical application. Mater Sci Eng A. 2008;497(1):111.
Witte F. The history of biodegradable magnesium implants: a review. Acta Biomater. 2010;6(5):1680.
Troitskii V, Tsitrin D. The resorbing metallic alloy ‘Osteosinthezit’ as material for fastening broken bone. Khirurgiia. 1944;8(1):41.
Witte F, Kaese V, Haferkamp H, Switzer E, Meyer-Lindenberg A, Wirth C, Windhagen H. In vivo corrosion of four magnesium alloys and the associated bone response. Biomaterials. 2005;26(17):3557.
Amani S, Faraji G, Kazemi Mehrabadi H, Abrinia K, Ghanbari H. A combined method for producing high strength and ductility magnesium microtubes for biodegradable vascular stents application. J Alloy Compd. 2017;723:467.
Amani S, Faraji G. Recrystallization and mechanical properties of WE43 magnesium alloy processed via cyclic expansion extrusion. Int J Miner Metall Mater. 2018;25(6):672.
Amani S, Faraji G, Mehrabadi HK, Baghani M. Manufacturing and mechanical characterization of Mg–4Y–2Nd–0.4Zr–0.25La magnesium microtubes by combined severe plastic deformation process for biodegradable vascular stents. Proc Inst Mech Eng Part B J Eng Manuf. 2019;233(4):1196.
Torkian A, Faraji G, Karimpour M. Mechanical properties and microstructure of WE43 Mg alloy processed by warm ECAP followed by extrusion. Arch Metall Mater. 2018;63(3):1093.
Ensafi M, Faraji G, Abdolvand H. Cyclic extrusion compression angular pressing (CECAP) as a novel severe plastic deformation method for producing bulk ultrafine grained metals. Mater Lett. 2017;197:12.
Galiyev A, Kaibyshev R, Gottstein G. Correlation of plastic deformation and dynamic recrystallization in magnesium alloy ZK60. Acta Mater. 2001;49(7):1199.
Bin C, Chen L, Dongliang L, Xiaoqin Z. Characterization of microstructure in high strength Mg96Y3Zn1 alloy processed by extrusion and equal channel angular pressing. J Rare Earths. 2011;29(9):902.
Farzadfar S, Sanjari M, Jung I-H, Essadiqi E, Yue S. Role of yttrium in the microstructure and texture evolution of Mg. Mater Sci Eng A. 2011;528(22–23):6742.
Zhang X, Yuan G, Wang Z. Effects of extrusion ratio on microstructure, mechanical and corrosion properties of biodegradable Mg–Nd–Zn–Zr alloy. Mater Sci Technol. 2013;29(1):111.
Kim W, Hong S, Kim Y, Min S, Jeong H, Lee J. Texture development and its effect on mechanical properties of an AZ61Mg alloy fabricated by equal channel angular pressing. Acta Mater. 2003;51(11):3293.
Agnew S, Mehrotra P, Lillo T, Stoica G, Liaw P. Texture evolution of five wrought magnesium alloys during route A equal channel angular extrusion: experiments and simulations. Acta Mater. 2005;53(11):3135.
Akbaripanah F, Fereshteh-Saniee F, Mahmudi R, Kim H. The influences of extrusion and equal channel angular pressing (ECAP) processes on the fatigue behavior of AM60 magnesium alloy. Mater Sci Eng A. 2013;565:308.
Stráská J, Janeček M, Čížek J, Stráský J, Hadzima B. Microstructure stability of ultra-fine grained magnesium alloy AZ31 processed by extrusion and equal-channel angular pressing (EX–ECAP). Mater Charact. 2014;94:69.
Shi Z, Cao F, Song G-L, Liu M, Atrens A. Corrosion behaviour in salt spray and in 3.5% NaCl solution saturated with Mg(OH)2 of as-cast and solution heat-treated binary Mg–RE alloys: RE = Ce, La, Nd, Y, Gd. Corros Sci. 2013;76:98.
Acknowledgements
This work was financially supported by the Iran National Science Foundation (No. 96000854).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Torkian, A., Faraji, G. & Pedram, M.S. Mechanical properties and in vivo biodegradability of Mg–Zr–Y–Nd–La magnesium alloy produced by a combined severe plastic deformation. Rare Met. 40, 651–662 (2021). https://doi.org/10.1007/s12598-019-01353-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12598-019-01353-9