Abstract
Surgical management of parathyroid gland disease may sometimes be difficult, due mainly to the surgeon’s failure to successfully detect parathyroids in unusual locations. The records of 942 cadavers (574 men and 368 women) who underwent autopsy in the Department of Forensic Medicine in Athens during the period 1988–2009 were reviewed. In total, 3,796 parathyroid glands were resected and histologically verified. Parathyroid glands varied in number. In 47 cases (5 %), one supernumerary (fifth) parathyroid was found, while in 19 cases (2 %) three parathyroid glands found. Superior glands were larger than inferior ones. However, there was no significant difference between the genders with respect to gland size. In 324 (8.5 %) out of 3,796, the glands were detected in an ectopic location: 7 (0.2 %) in the thyroid parenchyma, 79 (2 %) in different sites in the neck and 238 (6.3 %) in the mediastinum, 152 (4.1 %) of which were found in the upper and 86 (2.2 %) in the lower mediastinum. Significant anatomical variations of normal parathyroid glands may exist regarding number and location—knowledge that is essential for their successful identification and surgical management.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parathyroid glands were first described by Sandstrom (1880), who discovered them located in or near the thyroid gland in man and several other mammalian species, and defined them as ‘glandulae parathyroideae’. In 1891, von Recklinghausen described the “osteitis fibrosa cystica” disease, whereas Mandl (1947) performed the first surgical excision of a parathyroid adenoma in a patient, who showed dramatic improvement post-operatively. The second patient to be operated on for hyperparathyroidism was Chartell, who overall underwent seven operations, from May 1926 onwards, in order to detect and remove a parathyroid adenoma located in the mediastinum (Cope 1966).
Since these early surgical interventions, it has become clear that a precise knowledge of the anatomical locations of parathyroid glands is of utmost importance for surgeons (Thompson et al. 1982). Moreover, the development of imaging modalities for parathyroid glands makes a knowledge of their normal morphology and location essential.
The purpose of the present study was to report variations in location, number and morphology of normal parathyroid glands in the Greek population.
Materials and methods
Anatomical protocol
This anatomical retrospective study included 942 cadavers, 574 males (mean age 61.3 years, mean height 169.4 cm) and 368 females (mean age 67.4 years, mean height 160.2 cm), who underwent autopsy during the years 1988–2009.
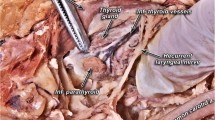
The dissection method followed included: (1) a wide section from the genion to the manubrium of the sternum, (2) search for the parathyroid glands at their usual location, (3) resection of the anterior thoracic wall, (4) removal of the interior organs, and (5) search for ectopic parathyroid tissue in the neck and mediastinum. Lastly, we searched for parathyroids in thyroid gland sections. Thyroid dissection was performed for the purposes of a different ongoing study protocol (Fig. 1).
Each gland was measured and weighed immediately. Macroscopic identification of the parathyroid glands was made judging by their color, soft structure and vascular stalk, as well as by sinking them in salty water for discrimination from fatty tissue (Vail and Coller 1967; Wang 1976). For each gland, the exact dimensions, weight (with Mettler H 45, AR) and location were noted. In addition, all data regarding the subject’s cause of death, morbid conditions and autopsy outcome report were entered into a specific form (Ludwing 1979).
The following cases were excluded: known history or autopsy findings of parathyroid, renal or bone disease. Cases where parathyroid gland pathology (such as adenoma, hyperplasia or carcinoma) was identified, were excluded from the analysis.
Histopathological protocol
All tissues consistent with parathyroid glands were fixed in 10 % formol solution and embedded in paraffin. Sections (8–10 μm) were obtained, stained with hematoxylin and eosin and examined microscopically. All 3,796 glands were examined histopathologically by a single pathologist. Due to the large number of collected glands, it was not possible to obtain frozen sections for designation of fat and weight, as proposed previously (Preisman and Mehnert 1971).
Statistical analysis
Statistical analyses were performed with the Statistical Package for the Social sciences (SPSS, Chicago, IL) for Windows (version 17.0). All statistical tests were two-tailed; P values <0.05 were considered statistically significant.
Results
Four parathyroid glands were detected in 876 (93 %) cadavers, whereas 47 (5 %) harbored five glands. In 19 cases (2 %) only three glands were found (Table 1). The mean gland dimensions, volume and weight in association with location and gender are presented in Tables 2 and 3.
Statistical analysis showed that the upper parathyroids were larger than the lower ones (P = 0.033). However, there were no differences between the two superior or between the two inferior glands as well as between the two genders with respect to parathyroid size. There was a significant positive correlation between gland size and age to age 20–24 years, followed by a plateau to age 60–64, and a decline thereafter (Fig. 2).
In total, 324 (8.5 %) parathyroid glands were ectopic. In particular, 7 (0.2 %) were intrathyroidal, 79 (2 %) were located in various sites of the neck, 152 (4.1 %) in the upper and 86 (2.2 %) in the lower mediastinum. The vast majority (91.5 %) of parathyroid glands were orthotopic, with the cricothyroid junction and the upper pole of the thyroid being the most common sites for the upper glands. The most common sites for the lower parathyroids were the lower thyroid pole and the thymic tongue, which is a distinct structure at the thoracic inlet, extending from the lower thyroid pole to the mediastinal thymus.
Discussion
Primary hyperparathyroidism (PHPT) is a relatively common entity, with an estimated prevalence from 20 to 250 cases per 100,000 adults in various studies, and is associated with increased morbidity and mortality due mainly to bone disease (Preisman and Mehnert 1971; Friedman et al. 1973; Dauphine et al. 1975; Anagnostis et al. 2010). Minimally invasive parathyroidectomy is the established therapy for PHPT (Quiros et al. 2004). However, the surgical management of PHPT may prove difficult and the main reason for this is the surgeon’s failure to successfully detect parathyroid glands in unusual locations (ectopic parathyroids) (Thompson et al. 1982; Mohebati and Shaha 2012).
The failure rate of cervical exploration is estimated at 4 % (Thompson et al. 1982). Most common anatomical abnormalities include: (1) ectopic parathyroids embedded in the thyroid, (2) ectopic parathyroids located in the neck and upper mediastinum, and (3) supernumerary parathyroids (Vail and Coller 1967; Alveryd 1968; Friedman et al. 1973; Wang et al. 1979; Russell and Edis 1982). Intrathyroidal parathyroid glands often present as hyperfunctioning adenomas, constituting a complex surgical problem (Vellar et al. 1973; Russell and Edis 1982). They may be located in a fissure of a thyroid lobe (being mainly extracapsular), in an agger of thyroid capsule or they may be truly intracapsular (Cathelineau and Siegrist 1977). Ectopic parathyroid glands can be detected anywhere from the hyoid bone to the lower mediastinum (Herbst et al. 1976).
The lower parathyroid glands are ectopic more frequently than the upper parathyroid glands and with wider distribution. The lower parathyroids develop on either side from the third branchial cleft in close proximity to the primordium of the thymus gland, as the parathyroid tissue follows the descending pathway of thymus from the pharynx to its final position in the anterior mediastinum (Cope 1941; Hunt et al. 1968; Thompson et al. 1982). The occurrence of parathyroids in the anterior mediastinum necessitates extension of the surgical section from the neck to the mediastinum and, thus, the division of the operation into two stages. The neck must first be explored as heretofore and, if all of the offending glands are not disclosed, at a second stage the anterior mediastinum must be opened through the sternum (Cope 1941).
The prevalence of normal ectopic parathyroid glands was quite high in our study. Similar (Mendoza et al. 2010), higher (42.8 %) (Hojaij et al. 2011) or lower (1.4 %) (Zerizer et al. 2011) rates also have been reported. In a small study of patients with end stage renal disease submitted to parathyroidectomy, the prevalence of ectopic parathyroids was 45.7 % (Gomes et al. 2007). In cases of a suspected ectopic parathyroid adenoma, sestamibi (MIBI) scan and ultrasound of the neck are useful, although their sensitivity is quite low (Gomes et al. 2007; Zerizer et al. 2011). Nevertheless, the combination of MIBI with computed tomography (CT) or magnetic resonance imaging (MRI), may raise the sensitivity and specificity to 100 % (Gomes et al. 2007; Zerizer et al. 2011). Common sites for surgical investigation of ectopic parathyroids are, for the upper pair of parathyroids: the upper pole of the thyroid lobe (usually very close to the recurrent laryngeal nerve) and the upper vascular thyroid stalk behind the hypopharynx and the cervical part of the esophagus (Wang 1976; Wang et al. 1979; Russell and Edis 1982). The lower parathyroids must be investigated along the common carotid artery to its bifurcation and at the thymic tongue, from the thyroid to the pericardium. Other more uncommon sites have also been reported (Wang 1976; Wang et al. 1979). The larger a parathyroid adenoma, the more likely it is to be ectopic (Thompson et al. 1982).
With regard to supernumerary parathyroids, their prevalence is about 2–6 % (Wang et al. 1979) as in the present series, although lower (1 %) (Palmer and Sutton 1978) or higher (13–14 %) rates have been reported (Akerström et al. 1984; Gomes et al. 2007). The possibility of an abnormal fifth gland as the cause of PHPT should be considered when four parathyroids of normal size and histology have been found in the neck, mainly in patients with diffuse parathyroid hyperplasia of secondary hyperparathyroidism. The fifth gland is usually in the lower neck or upper mediastinum, frequently within the thymus (Palmer and Sutton 1978). On the contrary, some cases of three parathyroids may be attributed rather to surgical failure of identification of the fourth gland (Friedman et al. 1973; Wang 1976; Wang et al. 1979; Russell and Edis 1982). Similar rates (3 %) of occurrence of three parathyroids have also been reported previously (Akerström et al. 1984). The common sites for superior orthotopic parathyroids are just above the intersection between the recurrent laryngeal nerve and the inferior thyroid artery. The inferior parathyroids most often lie close to the lower thyroid pole or in the upper thymus or thyrothymic ligament (Akerström et al. 1984), in accordance with our findings.
To our knowledge, the present series is the second largest anatomical study in the literature regarding the location, number and morphology of parathyroid glands. We must stress the high prevalence of detection of parathyroids in the lower mediastinum, which may be explained by the lack of clinical constraints provided by autopsy conditions. A high prevalence of mediastinal parathyroids was also been reported previously [28 % of the inferior parathyroids were located within the thymus in one study of cases with PHPT (Nanka et al. 2006) and 31 % of the ectopic parathyroids in another study (Mendoza et al. 2010)]. Notably, we found a low prevalence of intrathyroidal parathyroids (0.2 % of all parathyroids and 2 % of ectopic parathyroids), since 17.5–33 % of ectopic parathyroids have been reported in the thyroid parenchyma in previous studies (Gomes et al. 2007; Mendoza et al. 2010). However, in older studies no ectopic parathyroid adenomas were located in the thyroid parenchyma (Thompson et al. 1982). A small recent anatomical study reported lower rates for ectopic parathyroids located in the thyroid parenchyma (5.4 %) and higher in the thyroid subcapsular space (12.5 %) (Hojaij et al. 2011). The difference in prevalence among series is attributed to various factors, such as the number of slices examined or the criteria of successful diagnosis (Feliciano 1992).
In another study, the ectopic upper parathyroids were found mostly at the retroesophageal sites, while the anterior mediastinum (thymus gland) was the common site for lower ectopic parathyroids (Summers 1996).
With respect to age and sex distribution, there were no differences between the genders with respect to the size of the parathyroids; the glands were larger in persons between 20–24 years of age and smaller in those older than 60–64. Similar results regarding age were demonstrated by a large anatomical study (Wang 1976), although the parathyroids were heavier in men. There are conflicting data regarding the difference in size or weight between the genders, since a recent study showed no difference at all (Hojaij et al. 2011). In general, the combined weight of the normal parathyroids in men varies from 106 to 166 mg and from 130 to 168 mg in women, with a mean weight of each gland about 30–40 mg (Mohebati and Shaha 2012).
Extending our discussion on size and weight, as presented in Table 2, the mean dimensions of parathyroids in our study were 6.8 × 4 × 1.3 mm, with the largest being 7.6 × 4.3 × 1.4 mm and the smallest 5.5 × 3 × 1 mm. The smallest parathyroid weighed 30 mg and the largest 57 mg (mean weight 40 mg). The mean weight was similar to that reported in old and recent studies (30–40 mg), with the smallest parathyroid weighing 10 mg and the largest 78 mg (Wang 1976; Hojaij et al. 2011). The mean measurements were similar to those reported recently (6.7 × 3.9 × 2.0 mm) (Hojaij et al. 2011), although smaller dimensions (5 × 3 × 1 mm) have also been reported (Wang 1976). We also found that the upper parathyroids were larger than the lower ones. We cannot provide any feasible explanation for this finding, since others have found no difference at all (Hojaij et al. 2011). This finding remains to be verified in large anatomical studies in the future.
A limitation of our study is that the sample was relatively selective and representative mainly of older ages. However, it constituted a large number of cases and it lacked any limitation regarding the time provided for investigation (Ludwing 1979).
In conclusion, we provided the results of a large anatomical series of parathyroid glands, highly representative of the Greek population. Despite its retrospective nature, we hope that our results will contribute to a greater understanding of anatomical variations of normal parathyroid glands, in terms of their location and morphology, a knowledge that appears to be essential for the successful identification of the glands. This may further lead to safer thyroidectomies and more successful management of PHPT.
References
Akerström G, Malmaeus J, Bergström R (1984) Surgical anatomy of human parathyroid glands. Surgery 95:14–21
Alveryd A (1968) Parathyroid glands in thyroid surgery. I. Anatomy of parathyroid glands. II. Postoperative hypoparathyroidism—identification and autotransplantation of parathyroid glands. Acta Chir Scand 389:1–120
Anagnostis P, Karagiannis A, Tziomalos K, Athyros VG, Kita M, Mikhailidis DP (2010) Endocrine hypertension: diagnosis and management of a complex clinical entity. Curr Vasc Pharmacol 8:646–660
Cathelineau G, Siegrist JL (1977) Intrathyroidal parathyroidal adenoma associated to a cold thyroidal nodule (author’s translation). Nouv Presse Med 6:3089–3091
Cope O (1941) Surgery of hyperparathyroidism: the occurrence of parathyroids in the anterior mediastinum and the division of the operation into two stages. Ann Surg 114:706–733
Cope O (1966) The study of hyperparathyroidism at the Massachusetts General Hospital. N Engl J Med 274:1174–1182
Dauphine RT, Riggs BL, Scholz DA (1975) Back pain and vertebral crush fractures: an unemphasized mode of presentation for primary hyperparathyroidism. Ann Intern Med 83:365–367
Feliciano DV (1992) Parathyroid pathology in an intrathyroidal position. Am J Surg 164:496–500
Friedman EW, Schwartz AE, Spiro RH (1973) Changing patterns in hyperparathyroidism. Surg Gynecol Obstet 137:941–944
Gomes EM, Nunes RC, Lacativa PG, Almeida MH, Franco FM, Leal CT, Patrício Filho PJ, Farias ML, Gonçalves MD (2007) Ectopic and extranumerary parathyroid glands location in patients with hyperparathyroidism secondary to end stage renal disease. Acta Cir Bras 22:105–109
Herbst JW, Neff WR, Freeman JB (1976) Hyperparathyroidism: ectopic parathyroid glands. Am J Surg 131:380–381
Hojaij F, Vanderlei F, Plopper C, Rodrigues CJ, Jácomo A, Cernea C, Oliveira L, Marchi L, Brandão L (2011) Parathyroid gland anatomical distribution and relation to anthropometric and demographic parameters: a cadaveric study. Anat Sci Int 86:204–212
Hunt PS, Poole M, Reeve TS (1968) A reappraisal of the surgical anatomy of the thyroid and parathyroid glands. Br J Surg 55:63–66
Ludwing J (ed) (1979) Autopsy protocols, death certificates and interviews. In: Current methods of autopsy practice. Saunders, Orlando, pp 190–197
Mandl F (1947) Hyperparathyroidism: a review of historical developments and the present state of knowledge on the subject. Surgery 21:394–440
Mendoza V, Ramírez C, Espinoza AE, González GA, Peña JF, Ramírez ME, Hernández I, Mercado M (2010) Characteristics of ectopic parathyroid glands in 145 cases of primary hyperparathyroidism. Endocr Pract 16:977–981
Mohebati A, Shaha AR (2012) Anatomy of thyroid and parathyroid glands and neurovascular relations. Clin Anat 25:19–31
Nanka O, Libánsky P, Sedý J, Pozniak J, Adámek S (2006) Surgical–anatomical study as a part of operative treatment of primary hyperparathyroidism. Rozhl Chir 85:618–623
Palmer JA, Sutton FR (1978) Importance of a fifth parathyroid gland in the surgical treatment of hyperparathyroidism. Can J Surg 21:350–351
Preisman RA, Mehnert JH (1971) A plethora of primary hyperparathyroidism. Arch Surg 103:12–13
Quiros RM, Alioto J, Wilhelm SM, Ali A, Prinz RA (2004) An algorithm to maximize use of minimally invasive parathyroidectomy. Arch Surg 139:501–506
Russell CF, Edis AJ (1982) Surgery for primary hyperparathyroidism: experience with 500 consecutive cases and evaluation of the role of surgery in the asymptomatic patient. Br J Surg 69:244–247
Sandstrom I (1880) Om en ny Kortl has menniskan och atskilliga daggdjur. Upsala lakarforening Forh 15:441
Summers GW (1996) Parathyroid update: a review of 220 cases. Ear Nose Throat J 75:434–439
Thompson NW, Eckhauser FE, Harness JK (1982) The anatomy of primary hyperparathyroidism. Surgery 92:814–821
Vail AD, Coller FC (1967) The parathyroid glands: clinicopathologic correlation of parathyroid disease as found in 200 unselected autopsies. Mol Med 64:234–238
Vellar ID, Shaw J, Brosnan G (1973) Glandula in glandula: the intrathyroid parathyroid. Aust N Z J Surg 42:257–259
Wang C (1976) The anatomic basis of parathyroid surgery. Ann Surg 183:271–275
Wang CA, Mahaffey JE, Axelrod L, Perlman JA (1979) Hyperfunctioning supernumerary parathyroid glands. Surg Gynecol Obstet 148:711–714
Zerizer I, Parsaï A, Win Z, Al-Nahhas A (2011) Anatomical and functional localization of ectopic parathyroid adenomas: 6-year institutional experience. Nucl Med Commun 32:496–502
Conflict of interest
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lappas, D., Noussios, G., Anagnostis, P. et al. Location, number and morphology of parathyroid glands: results from a large anatomical series. Anat Sci Int 87, 160–164 (2012). https://doi.org/10.1007/s12565-012-0142-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12565-012-0142-1