Abstract
Environmental monitoring is critical in a developing country like Egypt where there is an insufficient framework for recording and tracking outbreaks. In this study, the prevalence of human adenovirus (HAdV), rotavirus group A (RVA) was determined in urban sewage, activated sludge, drainage water, drainage sediment, Nile water, and Nile sediment, using quantitative polymerase chain reaction (qPCR) analysis. HAdV was detected in 50% of urban sewage with viral concentrations ranging from 103 to 107 genome copies/liter (GC/L), 33% of activated sludge with viral concentrations ranging from 103 to 107 GC/kilogram (GC/kg), 95% of drainage water with viral concentrations ranging from 103 to 107 GC/L, 75% of drainage sediment with viral concentrations ranging from 103 to 107 GC/L, 50% of Nile water with viral concentrations ranging from 103 to 107 GC/L, and 45% of Nile sediment with viral concentrations ranging from 103 to 107 GC/kg. RVA was detected in 50% of urban sewage with viral concentrations ranging from 103 to 107 GC/L, 75% of activated sludge with viral concentrations ranging from 103 to 107 GC/L, 58% of drainage water with viral concentrations ranging from 103 to 107 GC/L, 50% of drainage sediment with viral concentrations ranging from 103 to 107 GC/L, and 45% of Nile water with viral concentrations ranging from 103 to 107 GC/kg. In conclusion, Abu-Rawash WWTP acts as a source of HAdV and RVA, releasing them into El-Rahawy drain then to the River Nile Rosetta branch.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The freshwater available on the planet represents about 2.5% of the earth’s water volume (Igor 1993). This resource is becoming scarce due to the acceleration of urbanization, rapid increase in the world population, and global warming. The freshwater scarcity is a major social, environmental, and economic challenge for industry and cities. The wastewater reuse acts as a main solution, which is able to meet this challenge (Barcelo and Kostianoy 2011). Pathogen removal is one outcome of the wastewater treatment facilities to reduce the environmental risks associated with discharging untreated or partially treated effluent into natural water systems. In addition, a tertiary wastewater treatment would be beneficial for this treated water to be used for further non-potable applications (Meneses et al. 2010). Water reuse approaches are designed to address the water scarcity issue without exacerbating other environmental impacts, reflecting the need for their impact assessment (Meneses et al. 2010). Again, these viruses can return back to infect susceptible individuals and continue the cycle of disease through exposure to these contaminated sources (Rzezutka and Cook 2004; Anthony et al. 2010).
Rotavirus group A (RVA) is a member of the family Reoviridae characterized by its double-stranded RNA. Rotavirus genus was classified into eight species according to The International Committee of Taxonomy of Viruses (ICTV) (Attoui et al. 2012). The adenovirus is non-enveloped with size ranging from 70 to 90 nm, and its genome is double-stranded DNA (Harrach et al. 2012). Human adenoviruses (HAdVs) were associated with a wide range of outbreaks of infectious diseases (Lu et al. 2014; Elmahdy et al. 2019). HAdVs consist of approximately 69 known genotypes (Binder et al. 2017), divided into seven species (A to G) based on chemical, physical, and genetic properties. New genotypes of HAdVs are recognized on the basis of complete genome sequencing and phylogenetic analysis (Harrach et al. 2012; Lu et al. 2014).
Globally, HAdV species F and RVA are considered the most important viral agents of gastroenteritis in infants and young children (Zlateva et al. 2005; Mans et al. 2010; Elhag et al. 2013, Shaheen 2017, 2019). Both viruses can survive in wastewater more than other enteric viruses and can remain infectious for a long time in environmental waters (Carducci et al. 2009; Quidort 2013; Xagoraraki et al. 2014). Furthermore, some viral pathogens were not disinfected due to inadequate chlorination or reduced contact time (Fong and Lipp 2005). RV and HAdVs are shed in large concentrations by infected individuals, can contaminate surface water sources through contaminated domestic wastewater, and thus these pathogens may return to various aquatic ecosystems contaminated by human sewage, particularly in communities with low levels of sanitation (Bosch 1998; Kiulia et al. 2010, 2015; Sibanda and Okoh 2012; Eifan 2013).
Globally, waterborne outbreaks remain a considerable risk to human health (Pons et al. 2015; Wang et al. 2018), despite advances in wastewater treatment technologies (Amenu 2014). Environmental monitoring is critical in a developing country like Egypt where there is an insufficient framework for recording and tracking outbreaks. Interestingly, epidemiological studies for enteric viruses become highly imperative because of their low infectious doses (Nadan et al. 2003; La Rosa et al. 2012; Murray et al. 2013). Water reuse approaches are designed to address the water scarcity issue without exacerbating other environmental impacts, reflecting the need for their impact assessment (Meneses et al. 2010). Quantitative PCR (qPCR) is a sensitive and accurate method for the identification and quantification of viral nucleic acid and has been a very effective and useful technique for microbial risk assessment in food and water (Dunn et al. 2014). This study was therefore designed to use qPCR technique to evaluate the prevalence of HAdV and RVA in surface water, and EL-Rahawy drainage, and wastewater treatment plant (WWTP), and their sediment.
Materials and Methods
Study Area
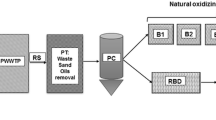
The study was performed in Abou-Rawash WWTP and El-Rahawy drainage canal. Abu-Rawash WWTP is located in the western sector of Giza, Egypt (El-Fakharany 2013). Abu-Rawash WWTP is one of the largest in Egypt with a capacity of treatment about 1.20 million m3/day and their primary treated wastewater disposes directly to many drains then finally into El-Rahawy drain. El-Rahawy drain is one of the main sources for Rosetta branch of River Nile (with an average daily discharge of about 2 million m3/day). El-Rahawy drainage, during this pathway the treated wastewater receives a significant pollution by many sources from municipalities' effluents, agriculture wastewater, and domestic industries and ultimately makes its way to the Rosetta River Nile Branch.
Sample Collection
Thirty-six raw sewage, treated effluent, and activated sludge samples were collected from Abu-Rawash WWTP during the period from October 2017 to September 2018. In addition, 96 surface water samples were collected from six points along El-Rahawy drainage canal (from sites 1 to 6) and two points at Rosetta Branch (site 7 at El-Rahawey with the Rosetta branch meeting point, and the site 8 at Rosetta Branch before mixing) during the period from April 2017 to March 2018. Over the same period, 48 sediment samples were collected from four sites as shown in Fig. 1.
Viral Concentration in Samples of Surface Water and Sewage
The protocol described by Katayama et al. (2002) was used to determine viral concentrations in drainage water and wastewater samples (the recovery rate was approximately 10%), with a minor modification. Briefly, water samples were processed in a vacuum system (negatively charged membrane, Nihon Millipore®, Tokyo, Japan) with a pore size of 0.45 μm and a diameter of 142 mm and a flow rate of 200 mL/min. The membrane was once again washed after filtration with 200 mL solution [0.5 mM H2SO4] pH 3.0 to ensure viral particle retention and eliminate all biosolids present. Then, the membrane was removed from the filter holder and applied 11 mL of NaOH [1 mM] pH 10.5 to elute the viruses in sterile glassware. Then the membrane was kept in contact with NaOH and stirred for 10 min. The obtained eluate was neutralized by adding 50 μL of H2SO4 solution [50 mM] and 50 μL Tris–EDTA buffer solution [100X] 1 mM pH 8.0.
Viral Concentration from Sediment and Sludge Samples
Viruses were concentrated from samples based on methods described by Schlindwein et al. (2010a, b) with a recovery rate by 46%. Briefly, with the addition of an equal volume of phosphate buffer (PBS), 0.05 M AlCl3 solution was applied to 20 g of wet sediment or sludge, and the pH was changed to 3.5 using 5 M HCl. Samples were then subjected to ice sonication three times to dislodge viruses, each 30 s followed by a centrifugation phase at 2.422×g at 4 °C for 15 min. The resulting pellet was suspended in a 10 mL 0.25 M glycine buffer, pH 9.5, and stirred for 1 h, accompanied by a further centrifugation stage at 7.656×g at 4 °C for 30 min. PEG 6000 precipitation was used for viral concentration as defined by Lewis and Metcalf (1988).The supernatant was transferred to another tube containing 8% PEG 6000 as a final concentration, pH 7.2, and stirred for about 2 h at 4 °C. A final centrifugation step was done at 7.656×g for 90 min at 4 °C. The pellet was suspended in 10 mL of 0.1 M PBS (pH 7.2). The decontamination stage was achieved by adding chloroform (1:3), followed by centrifugation for 15 min at 7.656×g. The upper (aqueous) phase was recovered, aliquoted, and stored at − 80 °C until further analysis.
Extraction of RNA/DNA and Quantification of Viruses
The final processed samples were applied to the extraction of nucleic acid (viral RNA and DNA) using a QIAamp MiniElute Virus Spin Kit (Qiagen, Germany) as instructed by the manufacturer. To examine PCR inhibition, a representative sample was taken from each type of samples collected during this study and inoculated with 7 × 108 GC/ml human adenovirus type 2 and 7 × 105 GC/ml of Simian rotavirus SA-11 as sample process control virus (SPCV) (previously tested negative for HAdV-2 and simian rotavirus SA-11 by qPCR) and no inhibitory effects could be observed. For molecular detection of HAdV, the qPCR was performed in accordance with Hernroth et al. (2002) using Rotor-Gene Probe PCR Kit (Qiagen, Germany) using the following thermal profile 50 °C for 2 min, 95 °C for 10 min and 45 cycles of 95 °C for 15 s and 60 °C for 1 min., while RVA were quantified in accordance with Zeng et al. (2008) using one-step Rotor-Gene Probe RT-PCR Kit using the following thermal profile 48 °C for 30 min, followed by 95 °C at 10 min then 40 cycles of 95 °C for 15 s and 1 min at 60 °C. All amplifications were performed in duplicate. Standard HAdV and RVA curves were prepared with a tenfold serial dilution of the DNA standard ranging from 5 × 101 to 5 × 109 GC/reaction. A serial tenfold dilution of nucleic acids was used to dilute the inhibitor and increase PCR efficiency. Real-time PCR mixture (25 μL) contained 5 μL of DNA or RNA extract, 12.5 μL 2 × RG PCR MM and RG RT-PCR MM reagents (Qiagen, Germany), respectively, 400 nM of each primer, 250 nM of TaqMan probe, and nuclease-free water up to 25 μL. PBS was used as the negative nucleic acid extraction control. This qPCR mixture was transferred into the Rotor-Gene Q system. At the end of each stage of the annealing, fluorescence data are measured by the provided Rotor-Gene software.
Statistical Analysis
Using GraphPad Prism version 5.0 (USA), statistical analysis was carried out. The test's crucial P-value was set at < 0.05. To evaluate the correlations between viral distributions and water samples, the Pearson correlation was applied. The mean viral loads between samples were compared with a one-way variance analysis. Student t tests and ANOVA tests are conducted to determine discrepancies at the measured points between the variables.
Results
Quantification of HAdV and RVA in Abu-Rawash WWTP
The incidence of HAdV in wastewater samples ranged from 1.8 × 103 to 5.3 × 107 GC/L with a median of 3.06 × 105 GC/L, while in sludge samples the incidence of HAdV ranged from 1.1 × 103 to 6.7 × 104 GC/L with a median of 4.52 × 104 GC/L. The incidence of RVA in wastewater samples ranged from 1.8 × 102 to 5.3 × 105 GC/L with a median of 7.03 × 103 GC/L, while in sludge samples, no RVA RNA was detected in collected samples as shown in Fig. 2.
Quantification of HADV and RVA in El-Rahawy Drain, Rosetta Branch, and Sediment
The incidence of HAdV in surface water samples of El-Rahawy drain ranged from 1.8 × 103 to 5.3 × 108 GC/L with a median of 1.5 × 107 GC/L, while in sediment samples, the incidence of HAdV ranged from 1.1 × 104 to 6.7 × 108 GC/Kg with a median of 3.7 × 107 GC/L. The incidence of RVA in drainage water samples at El-Rahawi drain canal ranged from 1.8 × 103 to 5.3 × 105 GC/L with a median of 1.1 × 105 GC/L. While in sediment samples, the incidence of RVA ranged from 1.1 × 104 to 6.7 × 105 GC/Kg with a median of 1.5 × 105 GC/L as shown in Fig. 3. Our study detected that HAdV had more prevalence in drainage water and sediment as shown in Figs. 2, 3, respectively.
Discussion
The diseases of waterborne viruses are a major concern in both developing and developed countries, and wastewater treatment plants play a crucial role in reducing aquatic environment viral contamination. In the current study, HAdVs were found with different loads in wastewater, drainage, River Nile, and sediment samples because this virus has a DNA genome that gives greater resistance to environmental stressors such as UV radiation, temperature, chlorine concentration, and variability in pH, including wastewater treatment processes (Lechevallier and Au 2004; Fong and Lipp 2005). In addition, it was found that HAdV is more prevalent than other enteric viruses (Garcia et al. 2012; Moresco et al. 2012; Elmahdy et al. 2016). HAdV has therefore been suggested as an effective indicator for the emerging viral pathogens of human origin, as they have been identified throughout the year in various types of water worldwide, being much more resistant to wastewater treatment processes (Bofill-Mas et al. 2010; Wyn-Jones et al. 2011; Wyer et al. 2012; Elmahdy et al. 2016). In several studies of surface waters around the world, adenoviruses have been found indicating a high prevalence of human viral pathogens for surface water. The concentrations of enteric viruses in five different countries are varied from 1 to about 100,000 genome copies per liter of surface water (Chapron et al. 2000; Kishida et al. 2012; Kern et al. 2013; Lin and Singh 2015; Huang et al. 2015). The incidence of RVA in drainage water samples at El-Rahawy drain canal ranged from 1.8 × 103 to 5.3 × 105 GC/L. In several countries, RVA was found with almost equal loads for surface waters, primarily from rivers and water samples from lakes (Vieira et al. 2012, 2016; Assis et al. 2015), while in other countries, the virus was fluctuated in a high concentration (Fongaro et al. 2012), and a low concentration (Chigor and Okor 2012).
The average concentration of HAdV genes was 5.3 × 107 GC/L in the inlet of Abu-Rawash WWTP. Other environmental studies detected high loads of HAdV (La Rosa et al. 2010; Carducci and Verani 2013), lower loads (He and Jiang 2005; Hewitt et al. 2013), and nearly similar loads (Bofill-Mas et al. 2010; Schlindwein et al. 2010a, b) in wastewater samples. In wastewater of Abu-Rawash WWTP, the concentration of RVA ranged from 1.8 × 102 to 5.3 × 105 GC/L. Previous environmental studies recorded closely the concentrations of RVA in sewage (Kitajima et al. 2014; Barril et al. 2015), but higher concentrations (5.9 × 103 to 2.9 × 108) were detected in other studies (Prado et al. 2011). The differences in the given results might be attributed to the differences in viral infection loads in the communities. To minimize concentrations of infectious viral particles in the aquatic environment, the removal of viruses in wastewater treatment is necessary. The main drivers of spatial differences in viral emissions in the environment are population size, type of sanitation, and the technologies used for wastewater treatment (da Silva et al. 2016).
In the present study, HAdV and RVA were detected in the outlet of the WWTP and in El-Rahawy drain with relatively high loads. In the previous studies from Egypt, other enteric viruses such as astrovirus, norovirus, human bocavirus, Aichi virus, and group C rotavirus were detected by traditional PCR in samples collected from Abu-Rawash WWTP, El-Rahawy drain, and Rosetta branch of River Nile (Shaheen et al. 2018, 2020; Shaheen and Elmahdy 2019a, b). The role of WWTPs as possible sources of pathogenic microbes is highly critical, particularly in water scarcity in various parts of the world due to the increasing need for water reuse (Okoh et al. 2010). In fact, the removal efficiency is variable depending on the design and operation of the wastewater treatment facility. Abu-Rawash WWTP was designed to treat an average flow of 400,000 m3/day; the last expansion allows the plant to accommodate 1.20 million m3/day average flows. This plant receives approximately 1,450,000 m3 of raw sewage daily (383,049,475 gallons). Because the amount of wastewater that arrives at the plant exceeds the plant's capacity, which provides only primary treatment, more than 250,000 m3 of excess wastewater is discharged directly into the Barakat drain every day without even primary treatment, as a result, water pollution in the El-Rahawy drain increased (Mostafa and Peters 2015). Moreover, total viral removal cannot be achieved through primary or secondary treatment. So, we recommend providing a tertiary treatment in Abu-Rawash WWTP to protect river Nile from viral contamination, the consequences of which cause risks to public health.
The detection and quantification of enteric viruses in matrices reported in this study supports the idea of solid-associated DNA viruses and their importance of taking into account the risk of disease from enteric viruses during routine monitoring of the aquatic environment. Many authors in the literature have found that viral sediment abundance exceeds that in the water column by magnitude order (Danovaro et al. 2002; Danovaro and Middelboe 2010; Elmahdy et al. 2016). The current study is limited due to the absence of infectivity assay for the positive samples because the presence of DNA or RNA of viruses does not necessarily mean they are infectious particles. However, the highly quantified DNA or RNA genome copies in wastewater and River Nile water may refer to the widespread circulation of both viruses among the Egyptian community. In conclusion, the existence of HAdV and RVA in the final-treated effluent, El-Rahawy drain, and the Nile River is a major concern for public health. Regulatory and local authorities must consider the levels of viral contamination in the treated effluent of Abu-Rawash WWTP in order to improve the efficiency of the pathogens removal facility. It is imperative to increase the design capacity of Abu-Rawash WWTP to avoid the bypass of the wastewater to El-Rahawy drain without any treatment. Also, Abu-Rawash WWTP should be improved by providing secondary treatment to reduce viral loads before reaching El-Rahawy drain then the river Nile.
References
Amenu, D. (2014). Wastewater treatment plants as a source of microbial pathogens in receiving watersheds. Research Journal of Chemical and Environmental Sciences, 2(6), 11–19.
Anthony, I. O., Sibanda, T., & Gusha, S. S. (2010). Inadequately treated wastewater as a source of human enteric viruses in the environment. International Journal of Environmental Research and Public Health, 7, 2620–2637.
Assis, A., Cruz, L., Ferreira, A., Bessa, M., Pinto, M., Vieira, C., et al. (2015). Relationship between viral detection and turbidity in a watershed contaminated with group A rotavirus. Environmental Science and Pollution Research, 22(9), 6886–6897.
Attoui, H., Mertens, P. P. C., Becnel, J., Belaganahalli, S., Bergoin, M., Brussaard, C. P., et al. (2012). Family reoviridae. In A. M. Q. King, M. J. Adams, E. B. Carstens, & E. J. Lefkowitz (Eds.), Virus taxonomy: Classification and nomenclature: Ninth report of the international committee on taxonomy of viruses (pp. 541–637). San Diego, California: Elsevier Academic Press.
Barcelo, D., & Kostianoy, A.G. (2011). The handbook of environmental chemistry, founded by Otto Hutzinger Editors-in-Chief: Volume 14.
Barril, P. A., Fumian, T. M., Prez, V. E., Gil, P. I., Martínez, L. C., Giordano, M. O., et al. (2015). Rotavirus seasonality in urban sewage from Argentina: Effect of meteorological variables on the viral load and the genetic diversity. Environmental Research, 138, 409–415. https://doi.org/10.1016/j.envres.2015.03.004.
Binder, A. M., Biggs, H. M., Haynes, A. K., Chommanard, C., Lu, X., Erdman, D. D., et al. (2017). Human adenovirus surveillance—United States, 2003–2016. MMWR Morbidity and Mortality Weekly Report, 66, 1039–1042.
Bofill-Mas, S., Calgua, B., Clemente-Casares, P., La Rosa, G., Iaconelli, M., Michele, M., et al. (2010). Quantification of human adenovirus in European recreational Waters. Food and Environmental Virology, 2, 101–109.
Bosch, A. (1998). Human enteric viruses in the water environment: A minireview. International Microbiology, 1(3), 191–196.
Carducci, A., Battistini, R., Rovini, E., & Verani, M. (2009). Viral removal by wastewater treatment: Monitoring of indicators and pathogens. Food and Environmental Virology, 1, 85–91.
Carducci, A., & Verani, M. (2013). Effects of bacterial, chemical, physical and meteorological variables on virus removal by a wastewater treatment plant. Food and Environmental Virology, 5, 69–76.
Chapron, C. D., Ballester, N. A., Fontaine, J. H., Frades, C. N., & Margolin, A. B. (2000). Detection of astroviruses, enteroviruses, and adenovirus types 40 and 41 in surface waters collected and evaluated by the information collection rule and an integrated cell culture-nested PCR procedure. Applied and Environmental Microbiology, 66, 2520–2525.
Chigor, V. N., & Okoh, A. I. (2012). Quantitative RT-PCR detection of hepatitis A virus, rotaviruses and enteroviruses in the Buffalo River and source water dams in the Eastern Cape Province of South Africa. International Journal of Environmental Research and Public Health, 9(11), 4017–4032.
Da Silva, M., Victoria, M., & Miagostovich, M. (2016). Rotavirus and Astroviruses. In: J.B. Rose and B. JiménezCisneros, (eds) Global Water Pathogen Project. https://www.waterpathogens.org (J.S Meschke, and R. Girones (eds) Part 3 Viruses) https://www.waterpathogens.org/book/rotavirus Michigan State University, E. Lansing, MI, UNESCO.
Danovaro, R., Manini, E., & Dellanno, A. (2002). Higher abundance of bacteria than viruses in deep Mediterranean sediments. Applied and Environmental Microbiology, 68, 1468–1472.
Danovaro, R., & Middelboe, M. (2010). Separation of free virus particles from sediments in aquatic systems. In S. W. Wilhelm, M. G. Weinbauer, & C. A. Suttle (Eds.), Chapter 8. Manual of aquatic viral ecology, (pp. 74–81). Waco: American Society of Limnology and Oceanograph.
Dunn, G., Harris, L., Cook, C., & Prystajecky, N. A. (2014). A comparative analysis of current microbial water quality risk assessment and management practices in British Columbia and Ontario, Canada. Science of the Total Environment, 468–469, 544–552.
Eifan, S. A. (2013). Enteric viruses and aquatic environment. The Internet Journal of Microbiology, 12.
El-Fakharany, Z. (2013). Environmental impact assessment of artificial recharge of treated wastewater on groundwater aquifer system. Case study: Abu Rawash, Egypt. Journal of American Science, 9(2), 494–502.
Elhag, W. I., Saeed, H. A., Omer, E. E., & Ali, A. S. (2013). Prevalence of rotavirus and adenovirus associated with diarrhoea among displaced communities in Khartoum Sudan. BMC Infectious Diseases, 13(209), 1–6.
Elmahdy, E. M., Ahmed, N. I., Shaheen, M. N. F., Mohamed, E. B., & Loutfy, S. A. (2019). Molecular detection of human adenovirus in urban wastewater in Egypt and among children suffering from acute gastroenteritis. Journal of Water and Health, 17, 287–294.
Elmahdy, M. E. I., Fongaro, G., Magri, M. E., Petruccio, M. M., & Barardi, C. R. (2016). Spatial distribution of enteric viruses and somatic coliphages in a lagoon used as drinking water source and recreation in Southern Brazil. International Journal of Hygiene and Environmental Health, 219, 617–625.
Fong, T. T., & Lipp, E. K. (2005). Enteric viruses of humans and animals in aquatic environments: Health risks, detection, and potential water quality assessment tools. Microbiology and Molecular Biology Reviews, 69(2), 357–371.
Fongaro, G., Nascimento, M. A., & Viancelli, A. (2012). Surveillance of human viral contamination and physicochemical profiles in a surface water lagoon. Water Science and Technology, 66(12), 2682–2687.
Garcia, L. A. T., Viancelli, A., Rigotto, C., Pilotto, M. R., Esteves, P. A., Kunz, A., et al. (2012). Surveillance of human and swine adenovirus, human norovirus and swine circovirus in water samples in Santa Catarina, Brazil. Journal of Water and Health, 10, 445–452.
Harrach, B., Benko, M., Both, G. W., Brown, M., Davison, A. J., Echavarria, M., et al. (2012). Adenoviridae. In A. M. Q. King, M. J. Adams, E. B. Carstens & E. J. Lefkowitz (Eds.), Virus taxonomy. Classification and nomenclature of viruses ninth report of the international committee on taxonomy of viruses (pp. 125–141). San Diego: Academic Press.
He, J. W., & Jiang, S. (2005). Quantification of enterococci and human adenoviruses in environmental samples by real-time PCR. Applied and Environmental Microbiology, 71, 2250–2255.
Hernroth, B. E., Conden-Hansson, A. C., Rehnstan-Holm, A. S., et al. (2002). Environmental factors influencing human viral pathogens and their potential indicator organisms in the blue mussel, Mytilus edulis: The first Scandinavian report. Applied and Environmental Microbiology, 68, 4523–4533.
Hewitt, J., Greening, G. E., Leonard, M., & Lewis, G. D. (2013). Evaluation of human adenovirus and human polyomavirus as indicators of human sewage contamination in the aquatic environment. Water Research, 47, 6750–6761.
Huang, Z. M., Hsu, B. M., Kao, P. M., Chang, T. Y., Hsu, T. K., Ho, Y. N., et al. (2015). Prevalence, quantification, and typing of human adenoviruses detected in river water in Taiwan. Environmental Science and Pollution Research International, 22, 8359–8366.
Igor Shiklomanov, A. (1993). Igor Shiklomanov's chapter "World fresh water resources". In P. H. Gleick (Ed.), Water in crisis: A guide to the world's fresh water resources. New York: Oxford University Press.
Katayama, H., Shimasaki, A., & Ohgaki, S. (2002). Development of a virus concentration method and its application to detection of enterovirus and norwalk virus from coastal seawater. Applied and Environmental Microbiology, 68, 1033–1039.
Kern, A., Kadar, M., Szomor, K., Berencsi, G., Kapusinszky, B., & Vargha, M. (2013). Detection of enteric viruses in Hungarian surface waters: First steps towards environmental surveillance. Journal of Water and Health, 11, 772–782.
Kishida, N., Morita, H., Haramoto, E., Asami, M., & Akiba, M. (2012). One-year weekly survey of noroviruses and enteric adenoviruses in the Tone River water in Tokyo metropolitan area, Japan. Water Research, 46, 2905–2910.
Kitajima, M., Iker, B. C., Pepper, I. L., & Gerba, C. P. (2014). Relative abundance and treatment reduction of viruses during wastewater treatment processes–identification of potential viral indicators. Science of the Total Environment, 488, 290–296.
Kiulia, N. M., Hofstra, N., Vermeulen, L. C., Obara, M. A., Medema, G., & Rose, J. B. (2015). Global occurrence and emission of rotaviruses to surface waters. Pathogens, 4, 229–255.
Kiulia, N. M., Netshikweta, R., Page, N. A., Van Zyl, W. B., Kiraithe, M. M., Nyachieo, A., et al. (2010). The detection of enteric viruses in selected urban and rural river water and sewage in Kenya, with special reference to rotaviruses. Journal of Applied Microbiology, 109(3), 818–828.
La Rosa, G., Fratini, M., della Libera, S., Iaconelli, M., & Muscillo, M. (2012). Emerging and potentially emerging viruses in water environments. Annali dell’Istituto Superiore di Sanità, 48(4), 397–406.
La Rosa, G., Pourshaban, M., Iaconelli, M., & Muscillo, M. (2010). Quantitative real-time PCR of enteric viruses in influent and effluent samples from wastewater treatment plants in Italy. Annali dell'Istituto Superiore di Sanita, 46, 266–273.
Lechevallier, M. W., & Au, K. (2004). Water treatment and pathogen control process—Efficiency in achieving safe drinking water. World Health Organization (WHO) (1st ed., Vol. 1). Cornwall: TJ International.
Lewis, G. D., & Metcalf, T. G. (1988). Polyethylene glycol precipitation for recovery of pathogenic virus including hepatitis A and human rotaviruses from oysters water and sediments. Applied and Environmental Microbiology, 54, 1983–1988.
Lin, J., & Singh, A. (2015). Detection of human enteric viruses in Umgeni River, Durban, South Africa. Journal of Water and Health, 13, 1098–1112.
Lu, Q. B., Tong, Y. G., Wo, Y., Wang, H. Y., Liu, E. M., Gray, G. C., et al. (2014). Epidemiology of human adenovirus and molecular characterization of human adenovirus 55 in China, 2009–2012. Influenza and Other Respiratory Viruses, 8(3), 302–308.
Mans, J., Corrie de Villiers, J., du Plessis, N. M., Avenant, T., & Taylor, M. B. (2010). Emerging norovirus GII.4 2008 variant detected in hospitalised pediatric patients in South Africa. Journal of Clinical Virology, 49(4), 258–264.
Meneses, M., Pasqualino, J., & Castells, F. (2010). Environmental assessment of urban wastewater reuse: Treatment alternatives and applications. Chemosphere, 81, 266–272.
Moresco, V., Viancelli, A., Nascimento, M. A., et al. (2012). Microbiological and physical-chemical analysis of the coastal waters of southern Brazil. Marine Pollution Bulletin, 64, 40–48.
Mostafa, M., & Peters, R. W. (2015). Manage water quality at Abu-Rawash WWTP, Egypt. Environmental Division 2015—Core programming area at the 2015 AIChE Annual Meeting (November), 335–40.
Murray, T. Y., Mans, J., & Taylor, M. B. (2013). Human calicivirus diversity in wastewater in South Africa. Journal of Applied Microbiology, 114, 1843–1853.
Nadan, S., Walter, J. E., Grabow, W. O. K., Mitchell, D. K., & Taylor, M. B. (2003). Molecular characterisation of astroviruses by reverse transcriptase PCR and sequence analysis: Comparison of clinical and environmental isolates from South Africa. Applied and Environmental Microbiology, 69(2), 747–753.
Okoh A. I., Sibanda T., & Gusha S. S. (2010). Inadequately treated wastewater as a source of human enteric viruses in the environment. International Journal of Environmental Research and Public Health, 7, 2620-2637.
Pons, W., Young, I., Truong, J., Jones-Bitton, A., McEwen, S., Pintar, K., et al. (2015). A systematic review of waterborne disease outbreaks associated with small non-community drinking water systems in Canada and the United States. PLoS ONE, 10(10), e0141646.
Prado, T., Silva, D. M., Guilayn, W. C., Rose, T. L., Gaspar, A. M., & Miagostovich, M. P. (2011). Quantification and molecular characterization of enteric viruses detected in effluents from two hospital wastewater treatment plants. Water Research, 45, 1287–1297.
Quidort, W. L. (2013). Detection and infectivity of human adenovirus in wastewater effluent, biosolids, and shellfish, and its persistence in estuarine water. PhD Dissertation. The College of William and Mary.
Rzezutka, A., & Cook, N. (2004). Survival of human enteric viruses in the environment and food. FEMS Microbiology Reviews, 28(4), 441–453.
Schlindwein, A. D., Rigotto, C., Simões, C. M., & Barardi, C. R. (2010a). Detection of enteric viruses in sewage sludge and treated wastewater effluent. Water Science and Technology, 61, 537–544.
Schlindwein, A. D., Simões, C. M. O., & Barardi, C. R. M. (2010b). Comparative study of two extraction methods for enteric virus recovery from sewage sludge by molecular methods. Memoria’s of Institute Oswaldo Cruz, Rio de Janeiro, 104(4), 576–579.
Shaheen, M. N. F. (2017). Rotavirus gastroenteritis among hospitalized children under 5 years of age in the Middle Eastern and North African Region: A review. Eastern Mediterranean Health Journal, 25(6), 422–430.
Shaheen, M. N. F., Abd El-Daim, S. A., Ahmed, N. I., & Elmahdy, M. E. (2018). Molecular detection of three gastroenteritis viruses in in urban sewage treatment plant and river water in Egypt. Egyptian Journal of Aquatic Biology and Fisheries, 22(5), 615–627.
Shaheen, M. N. F., Abd El-Daim, S. A., Ahmed, N. I., & Elmahdy, M. E. (2020). Environmental monitoring of Aichivirus and human Bocavirus in samples from wastewater treatment plant, drain, and River Nile in Egypt. Journal of Water and Health. https://doi.org/10.2166/wh.2019.075.
Shaheen, M. N. F., & Elmahdy, M. E. (2019a). Molecular detection of group C Rotavirus in environmental samples in Giza, Egypt. Asian Journal of Water, Environment and Pollution, 16(4), 17–22.
Shaheen, M. N. F., & Elmahdy, M. E. (2019b). Environmental monitoring of astrovirus and norovirus in Rosetta River Nile and El-Rahawy drain, Egypt. Water Supply Journal, 19(5), 1381–1387.
Shaheen, M. N. F., Elmahdy, E. M., & Chawla-Sarkar, M. (2019). Quantitative PCR-based identification of enteric viruses contaminating fresh produce and surface water used for irrigation in Egypt. Environmental Science and Pollution Research, 26(21), 21619–21628.
Sibanda, T., & Okoh, A. I. (2012). Assessment of the incidence of enteric adenovirus species and serotypes in surface water in the Eastern Cape Province of South Africa: Tyume River as a study case. The Scientific World Journal. https://doi.org/10.1100/2012/949216.
Vieira, C. B., de Abreu Corrêa, A., de Jesus, M. S., Luz, S. L., Wyn-Jones, P., Kay, D., et al. (2016). Viruses surveillance under different season scenarios of the Negro River basin, Amazonia, Brazil. Food and Environmental Virology, 8, 57–69.
Vieira, C. B., Mendes, A. C., Guimarães, F. R., Fumian, T. M., Leite, J. P., Gaspar, A. M., et al. (2012). Detection of enteric viruses in recreational waters of an urban lagoon in the city of Rio de Janeiro, Brazil. Memórias do Instituto Oswaldo Cruz, 107, 778–784.
Wang, Y., Edward, A., McBean, E. A., & Gharabaghi, B. (2018). Increased risks of waterborne disease outbreaks in northern Ontario due to climate change. Journal of Water Management Modeling, 26, C436.
Wyer, M. D., Wyn-Jones, A. P., Kay, D., et al. (2012). Relationships between human adenoviruses and faecal indicator organisms in European recreational waters. Water Research, 46, 4130–4141.
Wyn-Jones, A. P., Carducci, A., Cook, N., et al. (2011). Surveillance of adenoviruses and noroviruses in European recreational waters. Water Research, 45, 1025–1038.
Xagoraraki, I., Yin, Z., & Svambayev, Z. (2014). Fate of viruses in water systems. Journal of Environmental Engineering, 140(7), 04014020.
Zeng, S. Q., Halkosalo, A., Salminen, M., Szakal, E. D., Puustinen, L., & Vesikari, T. (2008). One-step quantitative RT-PCR for the detection of rotavirus in acute gastroenteritis. Virological Methods, 153, 238–240.
Zlateva, K. T., Maes, P., Rahman, M., & Ranst, M. V. (2005). Chromatography paper strip sampling of enteric adenoviruses 40 and 41 positive stool specimens. Virology Journal, 2, 6.
Acknowledgements
This work was fully funded by Academy of Scientific Research and Technology (ASRT) (2017–2019) title of the project: Improving environmental and health conditions for workers in Abu-Rawash wastewater treatment plant and remediation of pollution resources at El-Rahawy Drain.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Elmahdy, E.M., Shaheen, M.N.F., Rizk, N.M. et al. Quantitative Detection of Human Adenovirus and Human Rotavirus Group A in Wastewater and El-Rahawy Drainage Canal Influencing River Nile in the North of Giza, Egypt. Food Environ Virol 12, 218–225 (2020). https://doi.org/10.1007/s12560-020-09429-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12560-020-09429-x