Abstract
Background
The Pain Anxiety Symptoms Scale (PASS-20) consists of 20 items designed to assess four aspects of pain-related anxiety: cognitive anxiety, escape–avoidance behaviors, fear of pain, and physiological symptoms of anxiety. Although the PASS-20 is a well-established measure of pain-related anxiety in Western samples, different cultures may yield a different factor structure or different associations with pain-related outcome variables.
Purpose
The purposes of this study were (1) to examine the factor structure of a Korean language version of the PASS-20 (KPASS-20); (2) to examine reliability and construct validity of the KPASS-20; and (3) to compare the findings of this study with those of the original psychometric study using a Western sample.
Method
A total of 166 patients seeking treatment in a university pain management center located in Seoul, Korea participated.
Results
Results indicated that the KPASS-20 consists of three factors, “fearful thinking,” “physiological response,” and “avoidance,” and has adequate reliability and construct validity estimates. On the mean total score of the KPASS-20, the Korean sample had a significantly higher score than the original Western sample. In addition, in correlation analyses between the total score of the KPASS-20, physical functioning, and pain severity, the Korean sample had significantly higher coefficients, whereas similar differences were not found in the analyses of psychological functioning and depression.
Conclusion
The findings provide preliminary support for the reliability and validity of the KPASS-20.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has been well established that pain-related anxiety (e.g., [1, 2]) and avoidance (e.g., [3, 4]) contribute significantly to physical and psychological adjustment in individuals with chronic pain. One of the most commonly used questionnaires to measure these constructs is the Pain Anxiety Symptoms Scale (PASS) [2], which consists of 40 items designed to assess four aspects of pain-related anxiety: cognitive anxiety, escape–avoidance behaviors, fear of pain, and physiological symptoms of anxiety. Several studies that have employed the PASS demonstrated that scores are significantly related to pain severity and measures of patient functioning, including depression and physical disability (e.g., [5, 6]). A shorter 20-item version of the PASS has been developed [7]. Subsequent studies have demonstrated that the four-factor structure and adequate psychometric characteristics of the PASS are retained in the PASS-20 across clinical [7–9] and nonclinical samples [10].
Although the PASS-20 has been well validated and widely used in Western samples, it has apparently not yet been validated in Eastern sociocultural contexts. This is important as there are demonstrated differences in responses to and expression of pain among cultures, e.g., [11, 12]. For example, Asians tend to minimize overt expression of their pain compared to Euro-Americans (e.g., [13, 14]), possibly due to their cultural values placing greater emphasis on toleration and suppression of pain and its relevant emotions such as anxiety and depression, especially in the presence of others [13, 15]. Cultural factors may influence the underlying factor structure or other psychometric properties of the PASS-20. In addition, they may influence how separate aspects of pain-related anxiety predict certain outcome variables (e.g., pain severity, depression). Thus, it is necessary to investigate the cross-cultural generality of the PASS-20, particularly to Eastern countries, such as Korea.
The purposes of this study were (1) to examine the factor structure of a Korean language version of the PASS-20 (KPASS-20); (2) to examine reliability (i.e., internal consistency, mean interitem correlation, test–retest stability) and construct validity (i.e., convergent validity, predictive validity) of the KPASS-20; and (3) to compare the findings of this study with those of the original psychometric study using a Western sample [7].
Materials and Methods
Participants
This study used archival data from the larger Korean Pain Study: Phase I. The purpose of the larger study was to develop the infrastructure for pain psychology research in Korea, through cross-cultural validation of three commonly used pain-related measurement devices including the Pain Anxiety Symptoms Scale-20 (PASS-20) [7]. A total of 213 patients seeking treatment at a university pain management center located in Seoul, Korea, were invited to participate in the larger study. The inclusion criterion for the present study was having a history of at least 3 months of persistent pain. A number of patients had pain less than 3 months (n = 20), and others refused to participate (n = 27), resulting in a final sample of 166. The mean age of the sample was 48.70 years (SD = 13.04), and most were women (70.5%), were married (74.1%; never married 18.7%), and had at least a high school education (81.5%; high school 38.8%; college 36.1%; graduate 6.6%). The median duration of pain was 36 months (range 6–480 months), and over half of the sample was taking pain-related medication (57.2%). The primary pain locations were lower back (20.0%), neck (15.8%), head (15.8%), and shoulder(s) (15.2%). The remaining 33.2% reported primary pain in a variety of other locations.
Measures
A demographic form was created to measure background information. Participants were asked to indicate their age, sex, marital status, educational level, employment status, location(s) of most significant pain, duration of pain, current pain medication use, current financial compensation and litigation due to pain, and pain severity. Pain severity was assessed by summing present, usual, lowest, and highest pain, as well as pain-related distress during the past week, on a 0 to 10 numeric rating scale (NRS), resulting in a total score ranging from 0 to 50. The NRS has been commonly used and shown to have adequate psychometric properties in pain research [16]. The internal consistency for the summary NRS in the present study was α = 0.92 and the mean interitem correlation r = 0.71.
The Pain Anxiety Symptoms Scale-20 (PASS-20) [7] is a 20-item self-report measure designed to assess pain-related anxiety. The PASS-20 contains four subscales: cognitive anxiety, escape–avoidance behaviors, fear of pain, and physiological symptoms of anxiety. Each item reflecting pain-related anxiety symptoms is rated on a six-point scale ranging from 0 (never) to five (always). Total scores range from 0 representing no pain anxiety to 100 representing severe pain anxiety. Research on the PASS-20 has shown good internal consistency as well as factorial and construct validity across clinical [7–9] and nonclinical samples [10]. The PASS-20 was translated from English into Korean (KPASS-20) and then back-translated to check for accuracy.
The Beck Anxiety Inventory (BAI) [17] is a 21-item self-report measure designed to assess anxiety symptoms that are distinct from depression. Each item reflecting general anxiety symptoms is rated on a four-point scale anchored from not at all to severely. The scores range between 0 representing no anxiety and 63 representing severe anxiety. The BAI has well-established psychometric properties across a wide range of clinical as well as general population samples (e.g., [17, 18]). In addition, a Korean language version of the BAI (KBAI) has been shown to have adequate psychometric properties in terms of reliability and validity estimates across clinical and general population samples (e.g., [19, 20]). The internal consistency for the KBAI in the present study was α = 0.94 and the mean interitem correlation r = 0.44.
The Beck Depression Inventory (BDI) [21] is a 21-item self-report measure designed to assess severity of depressive symptoms. Each item contains four graded statements that reflect a four-point scale ranging from 0 to 3. The scores range from 0 representing no depression to 63 representing severe depression. Since the BDI is one of the most commonly used self-report measures, its psychometric properties have been widely reported across a variety of populations, demonstrating good reliability and validity estimates (e.g., [22, 23]). Also, a Korean language version of the BDI (KBDI) has been found to have good reliability and validity estimates in both clinical and general population samples (e.g., [24, 25]). The internal consistency for the KBDI in the present study was α = 0.92 and the mean interitem correlation r = 0.36.
The Short Form-36 (SF-36) [26] is a 36-item self-report measure designed to assess health-related functioning. The SF-36 contains eight subscales with four pertaining to physical functioning (i.e., physical functioning, role limitation due to physical health problems, bodily pain, and general health) and four pertaining to psychological functioning (i.e., vitality, social functioning, role limitation due to emotional health problems, and mental health). Scores on each subscale can range from 0 to 100, with a higher score representing better health-related functioning. Also, two composite scores (i.e., physical and psychological/mental component summary scales) are calculated by averaging all of the scores for four subscales pertaining to each of the two general aspects of functioning [27]. In the present study, two composite scores were used instead of eight SF-36 subscales, in order to reduce a number of statistical analyses, given the sample size [28, 29]. Many studies have established the psychometric properties of the SF-36 (e.g., [30, 31]). A Korean version of the SF-36 (KSF-36) also has been shown to have adequate internal consistency as well as factorial and construct validity in a sample of the general population [32]. The internal consistency for the physical component of the KSF-36 in the present study was α = 0.91 and the mean interitem correlation r = 0.34 and for the psychological component α = 0.89 and the mean interitem correlation r = 0.38.
Procedures
After the patients completed an appointment at the pain clinic, volunteers were directed to a private room to complete the questionnaire packet. These volunteers also were provided with the same questionnaire packet and a stamped addressed envelope for a second administration. They were instructed to take the packets to their home, complete the questionnaires after 2 weeks, and mail the packet back to the clinic. This larger study received full approval from appropriate institutional review panels, and study participants provided informed consent.
Statistical Analyses
The SPSS 15.0 and Amos 7.0 for Windows software were used for the analyses. All analyses were based on the first administration of the questionnaire packet to 166 participants with the exception of test–retest stability estimates which were based on 117 participants who completed both the first and second administration. Although the four-factor structure of the PASS-20 has been consistently reported in Western societies, this study considered that Eastern culture may have an impact on the factor structure of the KPASS-20. Thus, we performed an exploratory factor analysis considering both maximum likelihood (ML) with oblique (promax) rotation and principal axis factoring (PAF) with oblique (promax) rotation. The eventual selection of extraction method was based on whether the KPASS-20 data generally had a normal distribution (i.e., ML) or a significantly nonnormal distribution (i.e., PAF) [33]. The number of factors retained was based on eigenvalues, Cattell’s scree test, and parallel analysis using the mean eigenvalues and 95th percentile eigenvalues. Parallel analysis has been considered one of the most accurate factor retention tests [33, 34]. Also, only items with a factor loading of 0.40 or greater instead of 0.30 or greater used by some investigators [35] were retained, due to relatively small sample size of the study [36]. Then, the factor model obtained was compared with the original factor model of the PASS-20, using confirmatory factor analysis with maximum-likelihood estimation. Specifically, the comparison of factor models was made using several goodness-of-fit indices: (a) root-mean-square error of approximation (RMSEA); (b) comparative fit index (CFI); (c) nonnormed fit index (NNFI); (d) expected cross-validation index (ECVI); (e) Akaike information criterion (AIC); and (f) Bayesian information criterion (BIC). For the RMSEA, values below 0.10 are considered a good fit to the data, values below 0.05 a very good fit to the data, and values below 0.01 an outstanding fit to the data [37]. For the CFI and NNFI, values above 0.9 indicate a good fit to the data [38]. The ECVI, AIC, and BIC aimed to compare the competing models and lower values of the ECVI and AIC indicate better fit [39, 40]. For the BIC, it has been suggested that a difference of six points or more between the competing models strongly supports the model with lower BIC value having a better fit [41]. The final derived factor solution was then used for subsequent reliability and validity analyses. Cronbach’s α and mean interitem correlations and Pearson product moment correlations were calculated to examine internal consistency and test–retest stability of the KPASS-20 total and subscale scores.
Correlations were calculated to examine convergent validity among the KBAI total score and the KPASS-20’s subscale and total scores. In order to investigate predictive validity, four hierarchical multiple regressions were performed on physical and psychological functioning, pain severity, and depression. In order to examine the differences in the mean total and/or subscale scores of the PASS-20 between the Korean sample and the original Western sample [7], a t test(s) was performed. Also, in order to compare intercorrelations (i.e., PASS-20 total and/or subscale scores and outcome variables) between the Korean sample and the original Western sample [7], a test was performed using the Fisher’s r-to-z transformation. For comparison, this study selected four outcome variables (i.e., physical functioning, psychological functioning, pain severity, depression), measuring the same or similar construct to those from the study using the original Western sample [7].
Results
Descriptive Statistics and Factor Structure of the KPASS-20
Descriptive data of the KPASS-20 items are presented in Table 1. Given that the KPASS-20 items generally had a significantly nonnormal distribution (Table 1), the PAF with oblique (promax) rotation was selected and performed. Three factors of the KPASS-20 were consistently indicated by eigenvalues, Cattell’s scree test, and parallel analysis. In addition, initial item communalities were moderate, ranging from 0.49 to 0.73 [33] and at least half of the items of each factor had a factor loading of 0.60 or greater, which supported the factor stability of the KPASS-20 [42]. However, it was found that item 16 saliently loaded (loading of 0.32 or greater [34]) on two factors (i.e., 0.51 on factor 1 vs. 0.48 on factor 2). Elimination of item 16 did not improve the internal consistency of factor 1 (α = 0.91 and mean interitem correlation r = 0.55 when including item 16 vs. α = 0.90 and mean interitem correlation r = 0.55 when excluding item 16). Thus, item 16 was retained. The three-factor model accounted for 62.6% of the total variance, and the correlation coefficients among the factors ranged from 0.66 to 0.75 (p < 0.001), indicating a significant relationship among the factors. Considering the characteristics of the items loaded on each factor, factor 1 was labeled as “fearful thinking” (e.g., having pain-related fear or worry), factor 2 as “physiological response” (e.g., feeling dizzy or nauseous), and factor 3 as “avoidance” (e.g., stopping an activity when feeling pain). The factor loadings and item communalities of the three-factor solution are presented in Table 2, together with those of the four-factor solution for comparison purposes, to gain better understanding in the three-factor model retained. However, this study did not yield exactly the same factor structure (i.e., four factors, but different items loaded onto the factors) as the original four-factor model [7].
In order to further determine the factor structure of the KPASS-20, the three-factor model retained from the PAF was compared to the original four-factor model. The goodness-of-fit indices were compared between these two models and are reported in Table 3. The RMSEA, CFI, and NNFI values of the three-factor model were good. The RMSEA, CFI, and NNFI values of the four-factor model were below the values for good fit. Taken together with interpretability and parsimony, the three-factor model was also deemed to have a better fit than the four-factor model based on the lower ECVI, AIC, and BIC values with a difference of 78.71 points (a difference of six points or more between the competing models strongly supports the model with lower BIC value having better fit). Thus, the three-factor model was finally selected and used for subsequent analyses. Descriptive statistics for the three subscale and total scores of the KPASS-20 are shown in Table 4.
Reliability of the KPASS-20
Reliability was evaluated using estimates of internal consistency and test–retest stability over a 2-week interval of the KPASS-20 subscale and total scores. The internal consistency for fearful thinking was α = 0.91 and the mean interitem correlation r = 0.55; physiological response, α = 0.85 and mean interitem correlation r = 0.54; avoidance, α = 0.90 and mean interitem correlation r = 0.52; and total score, α = 0.95 and mean interitem correlation r = 0.50, indicating high interrelatedness of items. Test–retest correlations over a 2-week interval were as follows: fearful thinking, 0.91; physiological response, 0.85; avoidance, 0.89; and total score 0.91, all ps < 0.001, indicating high stability.
Convergent Validity of the KPASS-20
Descriptive statistics of the NRS, KBAI, KBDI, and KSF-36 are presented in Table 5. Convergent construct validity was examined using intercorrelations among the KBAI (i.e., general anxiety) and the KPASS-20 subscale and total scores. The correlations ranged from r = 0.52 to r = 0.70 (average r = 0.62), all ps <0.001, indicating convergent validity evidence that the KPASS-20 measures an aspect of anxiety.
Predictive Validity of the KPASS-20
Table 6 presents Pearson product moment correlations between the KPASS-20 subscale and total scores and the four outcome variables of physical and psychological functioning, pain severity, and depression. All correlations were significant at the p < 0.001 level, indicating that greater pain-related anxiety was related to lower physical functioning, lower psychological functioning, greater pain severity, and greater depression. Therefore, the predictive validity evaluation of the KPASS-20’s three subscales included these four outcome variables.
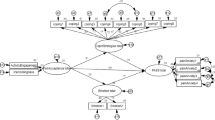
Predictive construct validity of the KPASS-20 was further evaluated using four hierarchical multiple regressions on hypothesized relationships among three subscales of the KPASS-20 and the four outcome variables. In each equation, participants’ sex, age, education, and pain duration were controlled first, and pain severity (not controlled when used as an outcome variable) was controlled next, followed by the three subscales of the KPASS-20 entered in the final step (the regression table is available upon request to the first author).
In general, the results indicated a significant overall effect (p < 0.001) in all of the equations with the smallest, F(7, 157) = 8.69 for pain severity and the largest, F(8, 156) = 22.59 for physical functioning. The block of patient background variables did not significantly contribute variance in any of the regression analyses. The pain severity score, on the other hand, added a significant contribution to explained variance in all of the equations (all ps <0.001) with, the smallest, ΔR 2 = 0.14, for depression and the largest, ΔR 2 = 0.37, for physical functioning. Three subscales of the KPASS-20 added a significant increment in explained variance in all of the equations, ranging from ΔR 2 = 0.15 to 0.26 (all ps <0.001). Specifically, the regression coefficients for fearful thinking were significant in the equation for pain severity, β = 0.34, t(157) = 2.95, p < 0.01. For physiological response, the regression coefficients were significant in two of four equations (i.e., physical functioning, β = −0.55, t(156) = −2.03, p < 0.05; depression, β = 0.66, t(156) = 4.18, p < 0.001). For avoidance, the regression coefficients were significant in two of four equations (i.e., physical functioning, β = −0.69, t(156) = −3.30, p < 0.01; psychological functioning, β = −0.73, t(156) = −3.23, p < 0.01).
Comparison of the PASS-20 and the KPASS-20
Since the three-factor model was retained for the KPASS-20, only total scores rather than also subscale scores could be compared to the original PASS-20. Results indicated that the mean KPASS-20 total score (M = 49.40, SD = 24.24, n = 166) was significantly higher than the mean PASS-20 total score (M = 38.62, SD = 20.38, n = 282), t(446) = 5.03, p < 0.001, r 2 = 0.05. In addition, 5% of all the variation among values is explained by differences between the two group means.
Predictive validity estimates between the KPASS-20 and PASS-20 were also compared. The KPASS-20 yielded significantly higher coefficients than the PASS-20 on the correlation coefficients between the total score and physical functioning (z = 2.73, p > 0.01) and pain severity (z = 1.98, p > 0.05). On the other hand, no significant difference in coefficients was found in analyses of psychological functioning and depression (Table 6).
Discussion
The present study primarily examined the factor structure and other psychometric properties of a Korean language version of the PASS-20. The PASS-20 has been shown to have a four-factor structure with Western clinical [7–9] and nonclinical samples [10]. In contrast, results from the present study indicated that the KPASS-20 consists of three factors instead of four in a clinical sample. This three-factor structure is congruent with the three basic aspects of anxiety (i.e., cognitive, physiological, overt behavioral) proposed by Borkovec [43].
The first factor emerging from the present analyses was labeled fearful thinking, embracing the two subscales of the PASS-20 entitled “fear of pain” and “cognitive anxiety.” In fact, both subscales of the PASS-20 are designed to measure some cognitive aspects of pain-related anxiety. The second factor was labeled physiological response, and the third factor was labeled avoidance, which closely correspond to “physiological symptoms of anxiety” and “escape–avoidance behavior,” respectively, of the PASS-20. Given the above, in a broad sense, the KPASS-20 appears to be conceptually congruent to the PASS-20 except that the KPASS-20 failed to differentiate types of fearful thinking. The results suggest that the KPASS-20 can be scored with three subscales rather than the four subscales of the PASS-20. Separate fearful thinking content on the PASS-20, as measured by the fear subscale, and anxious disruption in clear thinking, as measured by the cognitive anxiety subscale, were not differentiated in the Korean sample on the KPASS-20. This fact may point to a more generic cognitive anxiety among Korean pain patients than among Western pain patients. Sohn [44] noted that cultural values in Korea that discourage public display of emotions and leads to suppression of anxiety and other emotions may also contribute to a relatively less discriminated awareness of various anxious experiences.
Results of this study also showed that the KPASS-20 has sound internal consistency and test–retest stability, as well as support for convergent and predictive validity. In terms of convergent validity, the subscale and total scores of the KPASS-20 had significant relationships with the total scores of the KBAI, indicating that the KPASS-20 is conceptually related with general anxiety. In terms of predictive validity, first correlation analyses indicated that all of the subscale and total scores of the KPASS-20 were significantly associated with all of the four health functioning indices measured on the KSF-36, NRS, and BDI (Table 6). Previously reported correlation coefficients between total scores of the PASS-20 and four indicators of health functioning (i.e., pain severity, depression, physical and psychological functioning) were comparable to those reported in this study of the KPASS-20 [7].
Given all of the KPASS-20 subscales were correlated significantly with all the health functioning indices, there was some overlap in the predictive validity of the three KPASS-20 subscales. However, considering these three subscales and other variables (i.e., patient background variables and/or pain severity) taken together, each of the four health functioning indices was significantly predicted by either one or two of the three subscales of the KPASS-20. These findings suggest that there may be specific relations among specific types of functioning for separate aspects of pain-related anxiety. Use of the subscales therefore could be useful for individual assessment and for tailoring treatment. Treatment approaches can be targeted to a certain extent at particular processes of pain-related anxiety and avoidance [45, 46].
The fearful thinking subscale significantly predicted pain severity. This type of thinking (also called catastrophic thinking) [47] involves a tendency to narrowly attend to and exaggerate the pain experience (e.g., pain, emotional reactivity to pain), leading to a decrease in pain threshold, thereby maintaining or exacerbating pain severity. This possible causal relationship has been documented (e.g., [47, 48]). Also, this same causal relationship has been replicated with a Korean sample [49].
The physiological response subscale significantly predicted physical functioning and depression. Physiological symptoms of anxiety (e.g., trembling, dizziness, nausea) induced or accompanied by pain may yield fear and the belief of having a serious illness or facing adverse consequences (also called health anxiety) [50]. It has been shown that pain patients exhibit a higher level of health anxiety than do nonpain patients [51]. This type of anxiety may result in amplified attention to the physiological symptoms [52, 53] and misinterpretation of those symptoms as being indicative of a serious illness process [54], followed by increases in emotional distress and suffering [55, 56]. To our knowledge, there have not been any studies published on the effects of somatic/physiological symptoms on either physical functioning or depression in a population with pain and/or comorbid health conditions in Korea. However, given that cultural values in Korea discourage display of emotion (particularly emotional distress) in public [44, 57], which may contribute to the development of somatic/physiological symptoms [58], Koreans with chronic pain may be relatively more likely to present physiological symptoms and consequent health anxiety than their Western counterparts.
Finally, the avoidance subscale significantly predicted both physical and psychological functioning. As a strategy of controlling pain, avoidance of physical activities may have immediate effects in the short term [59], which can be beneficial to patients with acute pain in the early stage of treatment. However, persistent avoidance over a long period of time may produce negative effects upon physical conditions and feelings, consequently deteriorating physical, social, and/or emotional well-being (e.g., [2, 60, 61]). A study of pain patients in Korea [62] also indicated that avoidance strategies involve poorer physical and psychological functioning, and this can be influenced or maintained by stable external health locus of control beliefs. For example, pain patients who believe their pain is controlled by external causes such as luck or health professionals may be less likely to engage in activities causing pain, thus contributing to the preservation of their sense of powerlessness over situations [63]. Accordingly, health professionals oftentimes aim to decrease pain patients’ attribution of pain control to external causes and increase their sense of pain control, thus encouraging them to engage in more activities despite the presence of pain [64]. Considering that people in the East (e.g., Korea, Japan, China) may tend to present more external locus of control beliefs than those in a Western society [65], Koreans with chronic pain may be more likely to utilize avoidance strategies than those in Western societies.
The Korean sample reported a significantly higher total mean score of the KPASS-20 than did the Western sample on the PASS-20 [7]. As discussed above, Koreans with chronic pain may be relatively more likely to present physiological symptoms than their Western counterparts, possibly reflecting a cultural tendency to suppress emotional distress [44, 57, 58]. Also, they may be relatively more likely to avoid activities causing pain than their Western counterparts, possibly due to a cultural tendency to attribute their pain control to external things [62]. Taken together, these cultural tendencies may lead the Korean sample to more endorsing of pain-related anxiety symptoms than the Western sample. However, since this study selected the three-factor model, comparison of the mean subscales scores of the PASS-20 was not made between these two samples. Thus, this result needs to be interpreted with caution.
In addition, correlations for the total score of the PASS-20 with physical functioning and pain severity in the Korean sample were significantly higher than the Western sample, whereas no significant difference was found with psychological functioning and depression. These findings suggest that Koreans with chronic pain may be more likely to report complaints on physical aspects than do their Western counterparts. Again, the aforementioned cultural tendencies in Korea may be able to provide explanation on these findings to some extent.
Despite the psychometric support found for the KPASS-20, this present study must be viewed within the following limitations. First, although both translation and back-translation of the PASS-20 was conducted to minimize potential differences in semantic equivalence, the KPASS-20 still may have yielded differences in meaning. Second, taken together with interpretability and parsimony, this present study selected the three-factor model over the four-factor model based on the lower ECVI, AIC, and BIC values. However, differences in the RMSEA, CFI, and NNFI values between two models were comparable, and thus the results of the study may not be sufficient to warrant suggesting against the previously well-established four-factor model. Accordingly, the three-factor model must be viewed with care and investigated further. Third, this study used a cross-sectional design. Thus, no causal relationships among variables can be inferred and must be interpreted with care. Fourth, since this study involved a heterogeneous sample attending a tertiary care pain clinic, the results may not generalize to a specific pain population (e.g., lower back pain, headache, arthritis) or other settings (e.g., primary care pain clinic, community).
The findings of the study indicate that the KPASS-20 has adequate reliability and validity support. Given that pain management clinics in Korea do not currently employ psychological interventions, the KPASS-20 may facilitate the investigation of the effectiveness of adding this component to treatment programming. The KPASS-20 could be useful for identifying three aspects of pain-related anxiety (i.e., fearful thinking, physiological response, and avoidance) and thus aid the selection of interventions and the evaluation of their outcome in pain management clinics in Korea. However, given that this study was the first attempt to examine the psychometric properties of the PASS-20 in Korea, such application of the KPASS-20 to clinical settings should be preceded by further studies, including its utility for supporting treatment decisions and as an aid in further treatment development.
References
Burns JW, Mullen JT, Higdon LJ, Wei JM, Lansky D. Validity of the Pain Anxiety Symptoms Scale (PASS): prediction of physical capacity variables. Pain. 2000;84:247–52.
McCracken LM, Zayfert C, Gross RT. The pain anxiety symptoms scale: development and validation a scale to measure fear of pain. Pain. 1992;50:67–73.
Fordyce WE, Shelton JL, Dundore DE. The modification of avoidance learning pain behaviors. J Behav Med. 1982;5:405–14.
Phillips HC. Avoidance behavior and its role in sustaining chronic pain. Behav Res Ther. 1987;25:273–9.
McCracken LM, Faber SD, Janeck AS. Pain-related anxiety predicts non-specific physical complaints in persons with chronic pain. Behav Res Ther. 1998;36:621–30.
Strahl C, Kleinknecht RA, Dinnel DL. The role of pain anxiety, coping, and pain self- efficacy in rheumatoid arthritis patient functioning. Behav Res Ther. 2000;38:863–73.
McCracken LM, Dhingra L. A short version of the Pain Anxiety Symptoms Scale (PASS- 20): preliminary development and validity. Pain Res Manag. 2002;7:45–50.
Coons MJ, Hadjistavropoulos HD, Asmundson GJG. Factor structure and psychometric properties of the Pain Anxiety Symptoms Scale-20 in a community physiotherapy clinic sample. Eur J Pain. 2004;8:511–6.
Roelofs J, McCracken LM, Peters ML, Crombez G, van Breukelen G, Vlaeyen JWS. Psychometric evaluation of the Pain Anxiety Symptoms Scale (PASS) in chronic pain patients. J Behav Med. 2003;27:167–83.
Abrams MP, Carleton RN, Asmundson GJG. An exploration of the psychometric properties of the PASS-20 with a nonclinical sample. J Pain. 2007;8:879–86.
Chapman C, Toru S, Martin R, Tanaka A, Okazaki N, Colpitts Y, et al. Comparative effects of acupuncture in Japan and the United States on dental pain perception. Pain. 1982;12:319–28.
Morse JM, Morse RM. Cultural variation in the inference of pain. J Cross Cult Psychol. 1988;19:232–42.
Hobara M. Beliefs about appropriate pain behavior: cross-cultural and sex differences between Japanese and Euro-Americans. Eur J Pain. 2005;9:389–93.
Nayak S, Shiflett SC, Eshun S, Levine FM. Culture and gender effects in pain beliefs and the prediction of pain tolerance. Cross Cult Res. 2000;34:135–51.
Brena SF, Sanders SH, Motoyama H. American and Japanese chronic low back pain patients: cross-cultural similarities and differences. Clin J Pain. 1990;6:118–24.
Jensen MP, Karoly P. Self-report scales and procedures for assessing pain in adults. In: Turk DC, Melzack R, editors. Handbook of pain assessment. New York: Guilford; 2001. p. 15–34.
Beck AT, Epstein N, Brown G, Steer RA. An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol. 1988;56:893–7.
Borden JW, Peterson DR, Jackson EA. The Beck Anxiety Inventory in nonclinical samples: initial psychometric properties. J Psychopathol Behav Assess. 1991;13:345–56.
Han EK, Cho YR, Park SH, Kim HR, Kim SH. Factor structure of the Korean version of the Beck Anxiety Inventory: an application of confirmatory factor analysis in psychiatric patients. Kor J Clin Psychol. 2003;22:261–70.
Yook SP, Kim JS. A clinical study on the Korean version of Beck Anxiety Inventory: comparative study of patient and non-patient. Kor J Clin Psychol. 1997;16:185–97.
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–71.
Beck AT, Steer RA, Garbin MG. Psychometric properties of the Beck Depression Inventory: twenty five years of evaluation. Clin Psycho Rev. 1988;8:77–100.
Gallagher D, Nies G, Thompson LW. Reliability of the Beck Depression Inventory with older adults. J Consult Clin Psychol. 1982;50:152–3.
Han HM, Yum TH, Shin YW, Kim KH, Yoon DJ, Jung KJ. A standardization study of Beck Depression Inventory in Korea. Kor J Neuropsy Assoc. 1986;25:487–500.
Lee YH, Song JY. A study of the reliability and the validity of the BDI, SDS, and MMPI-D scales. Kor J Clin Psychol. 1991;10:98–113.
Ware JE, Sherbourne CD. 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care. 1992;30:473–83.
Hays RD, Sherbourne CD, Mazel RM. 36-item health survey 1.0. Health Econ. 1993;2:217–27.
Fanuele JC, Birkmeyer J, William A, Tosteson T, Weinstein J. The impact of spinal problems on the health status of patients. Spine. 2000;25:1509–14.
Ware J, Kosinski M, Keller S. SF-36 physical and mental health summary scales: v User’s Manual. Boston: The Health Institute; 1994.
Brazier JE, Harper R, Jones NM, O’Cathain A, Tomas KJ, Usherwood T, et al. Validation of the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ. 1992;305:160–4.
Garratt AM, Ruta DA, Abdalla MI, Buckingham JK, Russell IT. The SF-36 health survey questionnaire: an outcome measure suitable for routine use within the NHS? BMJ. 1993;306:1440–4.
Koh SB, Chang SJ, Kang MG, Cha BS, Park JK. Reliability and validity on measurement instrument for health status assessment in occupational workers. Kor J Prev Med. 1997;30:251–66.
Costello AB, Osborne JW. Best practices in exploratory factor analysis: four recommendations for getting the most from your analysis. Pract Assessment Res Eval 2005; 10. Available online: http://pareonline.net/getvn.asp?v=10&n=7.
Tabachnick BG, Fidell LS. Using multivariate statistics. 4th ed. New York: Harper Collins; 2001.
Bordens KS, Abbott BB. Research design and methods. Mountain View: Mayfield; 1988.
Gorsuch RL. Factor analysis. Philadelphia: Saunders; 1974.
Steiger JH. Structural model evaluation and modification. Multivar Behav Res. 1990;25:173–80.
Bentler PM. Comparative fit indices in structural models. Psychol Bull. 1990;107:238–46.
Akaike H. Information theory and an extension of the maximum likelihood principle. In: Petrov BN, CSAKI F, editors. Second international symposium on information theory. Budapest: Akademiai Kiado; 1973. p. 267–81.
Browne MW, Cudeck R. Alternative ways of assessing model fit. In: Bollen K, Long S, editors. Testing structural equation models. Newbury Park: Sage; 1993. p. 136–62.
Raftery AE. Bayesian model selection in social research. In: Marsden PV, editor. Sociological methodology. Cambridge: Basil Blackwell; 1995. p. 111–63.
Guadagnoli E, Velicer WF. Relation of sample size to the stability of component patterns. Psychol Bull. 1988;103:265–75.
Borkovec TD. Physiological and cognitive process in the regulation of anxiety. In: Schwartz GE, Shapiro D, editors. Consciousness and self-regulation. Advances in research, vol. 1. New York: Plenum; 1976. p. 239–52.
Sohn CN. The construing of chronic pain: the constructive alternativism of the chronic patients? Kor J Health Psychol. 2006;11:437–55.
Vlaeyen JWS, De Jong JR, Geilen M, Heut PHTG, Van Breukelen G. Graded exposure in vivo in the treatment of pain-related fear. A replicated single-case experimental design in four patients with chronic low back pain. Behav Res Ther. 2001;39:151–66.
Vlaeyen JWS, De Jong JR, Geilen M, Heut PHTG, Van Breukelen G. The treatment of fear of movement/(re)injury in chronic low back pain: further evidence on the effectiveness of exposure in vivo. Clin J Pain. 2002;18:251–61.
Sullivan MJL, Thorn B, Haythornthwaite JA, Keefe F, Martin M, Bradley LA. Theoretical perspectives on the relation between catastrophizing and pain. Clin J Pain. 2001;17:52–64.
France CR, France JL, Al’Absi M, Ring C, McIntyre D. Catastrophizing is related to pain ratings, but not nociceptive flexion reflex threshold. Pain. 2002;99:459–63.
Kim CS, Hyun MH. Effects of catastrophizing and neuroticism on experimental pressure pain threshold. Kor J Health Psychol. 1998;3:169–78.
Lucock MP, Morley S. The health anxiety questionnaire. Brit J Health Psychol. 1996;1:137–50.
Hadjistavropoulos H, Snider B, Hadjistavropoulos T. Anxiety in older persons waiting for cataract surgery: investigating the contributing factors. Can J Aging. 2001;80:97–111.
Barsky AJ, Wyshak G, Klerman GL. The somatosensory amplification scale and its relationship to hypochondriasis. J Psychiatr Res. 1990;24:323–34.
Park SY, Lee YJ, Hwang SH, Eom SY, Jeon WT. The difference in psychological characteristics of patients with somatic symptom according to the presence of physical illness. Kor J Clin Psychol. 2006;25:147–67.
Hadjistavropoulos HD, Owens KMB, Hadjistavropoulos T, Asmundson GJG. Hypochondriasis and health anxiety among pain patients. In: Asmundson GJG, Taylor S, Cox BJ, editors. Health anxiety: clinical and research perspectives on hypochondriasis and related conditions. Chichester: Wiley; 2001. p. 298–323.
Barsky AJ, Fama JM, Bailey ED, Ahern DK. A prospective 4- to 5-year study of DSM-III-R hypochondriasis. Arch Gen Psychiatry. 1998;55:737–44.
Gramling SE, Clawson EP, McDonald MK. Perceptual and cognitive abnormality model of hypochondriasis: amplification and physiological reactivity in women. Psychosom Med. 1996;58:423–31.
Kim KI. Consideration of proneness to somatization among Koreans. New Med J. 1972;15:1440–3.
Min SK, Park CS, Han JO. Defense mechanisms and coping strategies in Hwabyung. Kor J Neuropsy Assoc. 1993;32:506–16.
McCracken LM. Contextual cognitive-behavioral therapy for chronic pain. Seattle: IASP; 2005.
Asmundson GJG, Norton PJ, Norton GR. Beyond pain: the role of fear and avoidance in chronicity. Clin Psychol Rev. 1999;19:97–119.
McCracken LM, Gross RT, Aikens J, Carnrike CLM. The assessment of anxiety and fear in persons with chronic pain: a comparison of instruments. Behav Res Ther. 1996;34:927–33.
Chung YS, Lee YH. The effects of health locus of control, pain acceptance, and pain coping on adaptation of pain patients. Kor J Clin Psychol. 2005;24:615–29.
Geist CR, Borecki S. Social avoidance and distress as a predictor of perceived locus of control and level of self-esteem. J Clin Psychol. 1982;38:612–4.
Thorn BE. Cognitive therapy for chronic pain. New York: Guilford; 2004.
Berry JW, Poortinga YH, Segall MH, Dasen PR. Cross-cultural psychology: research and applications. Cambridge: Cambridge University Press; 1992.
Morgan GA, Leech NL, Gloeckner GW, Barrett KC. SPSS for introductory statistics: use and interpretation. Mahwah: Lawrence Erlbaum Associates; 2004.
Bergner M, Bobbitt RA, Carter WB, Gilson BS. The Sickness Impact Profile: development and final revision of a health status measure. Med Care. 1981;19:787–805.
Acknowledgments
This study was supported by the Center for Korean Studies at the University of Hawaii at Manoa.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cho, S., Lee, SM., McCracken, L.M. et al. Psychometric Properties of a Korean Version of the Pain Anxiety Symptoms Scale-20 in Chronic Pain Patients. Int.J. Behav. Med. 17, 108–117 (2010). https://doi.org/10.1007/s12529-010-9080-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-010-9080-2