Abstract
Background
The accurate assessment of myocardial blood flow (MBF) is a potential adjunct to the anatomy of CT coronary angiography.
Purpose
To compare semi-quantitative parameters from first-pass CT (FP CT) imaging with absolute measures of MBF in an animal model of altered MBF.
Methods
A pig model of intracoronary adenosine (n = 8) was used during FP CT. This produces a zone with hyperemic MBF and a control zone within a slice. A subset of these animals also underwent LAD occlusion with imaging. Fluorescent microspheres (Mcsp) were injected into the left atrium to determine absolute MBF concurrent with CT imaging. Pigs were placed in a 64-slice (Philips) CT with acquisition performed during IC adenosine and occlusion. A 40% dilution of Iopamidol 370 (1 mL/kg) was injected IV at 5 mL/second. CT acquisition was ECG gated over 40 cardiac phases with the following parameters: 180° axial mode (pitch = 0), field of view = 250 mmsq, 512 × 512 matrix, slice thickness = 2.5 mm × 10 slices, temporal resolution = 330 ms, 120 kV, 495 ma. Mcsp were injected immediately following CT imaging. The heart was sectioned into 2.5 mm slices to match the CT images and segmented. Time attenuation curves (TAC) were generated from CT in intervention and control zones based on Mcsp values. Mcsp coronary flow reserve (CFR) = hyperemic/control MBF, and CT CFR was derived from intervention/control area under curve from baseline corrected TIC.
Results
MBF control = .65 ± .28, MBF adenosine = 2.6 ± .7 mL/min/g (P < .0001). CFR = 4.1 ± 1.1, CT CFR = 4.3 ± 1.4 (P = NS). There was a significant (r = .94, P < .0001) correlation between CFR and CT CFR.
Conclusions
CT first-pass myocardial perfusion imaging is feasible using a simple semi-quantitative analysis which provides reasonable estimates of MBF.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Computed tomography angiography (CTA) of the coronary arteries using multi-slice acquisition scanners can provide accurate anatomical information regarding the presence of arterial disease.1,2 While invasive angiography and CTA can provide prognostic information in certain subsets of patterns of disease,3-8 it cannot provide functional significance of disease. A number of studies have shown the incremental benefit of a measure of myocardial perfusion over and above that provided by coronary anatomy. Consequently, the use of multi-slice coronary CTA in isolation is, in many respects, a return to a less potent, anatomy-based, imaging strategy.
Myocardial perfusion information is inherently available within the CTA coronary examination as it is centered on a bolus administration of contrast. First-pass MR perfusion imaging has been shown to be clinically accurate when combined with pharmacologic stress,9,10 has prognostic value,11 and can be used to quantify myocardial blood flow (MBF) both semi-quantitatively12,13 and for the measurement of absolute values.13,14 This potential exists for coronary CTA.
Prior studies have shown that absolute MBF can be assessed CTA in the setting of reduced coronary blood flow.15,16 These methods require the measurement of both an arterial input function (AIFN) and a myocardial tissue time attenuation curve (TAC, produced as the bolus transits the myocardium). A method based on hyperemic assessment of coronary flow reserve (CFR) independent of the arterial input function may be simpler to apply to clinical studies and parallel clinical nuclear stress protocols. The purpose of this study was to generate AIFN independent, semi-quantitative measures of CFR using first-pass 64-slice CT imaging and compare these to CFR values obtained from absolute MBF measures in a an animal model of hyperemic MBF.
Methods
Surgical Model
We studied 10 sus scrofa swine. Two were excluded: one for sudden death and one for inability to inject microspheres into the left atrium leaving a total of eight pigs in the study group. Pigs were anesthetized with a combination of IM ketamine and pentobarbital and maintained on a 2-4% isoflurane inhalation anesthetic. The chest was opened midline. Surgical dissection was progressive to expose the left anterior descending artery. A 27-gauge catheter was inserted into a branch vessel and advanced into the main channel of the LAD and secured. An occlusion snare was also placed around the vessel. A flexible catheter was inserted into the left atrium for microsphere injection, and a second was placed in the femoral artery and advanced to the descending aorta for reference sampling. An intravenous catheter was placed in the femoral vein.
Experimental Protocol
Adenosine was infused at 80 mcg/kg/min intracoronary through the LAD catheter. CT perfusion imaging was performed during the infusion as was left atrial injection of fluorescent microspheres with concurrent arterial reference sampling. The total duration of adenosine infusion was 6-7 min (3 min to reach equilibrium, 1 min for the first-pass study, and 2 min reference sampling following microsphere injection). In four animals, an occlusion scan and microsphere injection were performed during transient coronary occlusion (approximately 6-10 min). Following completion of the scan, the animal was euthanized with an overdose of IV pentobarbital. The heart was later removed and sectioned into 5 mm axial slices using anatomical landmarks (right ventricle, papillary muscles) and sectioned radially into eight segments for MBF analysis. Each segment was weighed and sent for microsphere content (IMT labs, Irvine, CA). MBF was calculated by:
where counts are fluorescent microsphere content, and the arterial sampling rate is 7.5 mL/min. Coronary flow reserve values were generated by dividing peak transmural flow values by control values taken from myocardium radially opposite the hyperemic zone.
CT Acquisition
A Philips 64-slice Brilliance scanner (Philips Healthcare, Andover, MA) was used for all CT imaging. Each animal was placed in the scanner at a mildly oblique angle to approximate a short-axis view of the myocardium. A localization scan was performed in order to acquire CT images with an inferior border just proximal to the apex. Each detector was collimated for ten slices of 2.5 mm thickness. Acquisition was ECG-gated to mid-diastole with one 10-set slice generated per R-R interval. The 360° gantry rotation time was 500 ms and the scan angle was 240° providing a temporal resolution of 333 ms with acquisition timed to mid-diastole. The energy output was 120 kV with a current of 495 mA or 165 mA·s. Field of view was 250 × 250 mm2 using a 512 × 512 matrix. Contrast (1 mL/kg) was injected at 5 mL/second via femoral vein using a 40% mixture of iopamidol with saline in order to minimize beam hardening and remain in the linear range of contrast dose to signal attenuation.17
Perfusion Analysis
CT perfusion serial axial slices were imported into a dicom software program (Cine tool, GEMS, Milwaukee, WI) and Osirix imaging software (open source software). Signal attenuation was measured in Hounsfield units in Osirix with a conversion slope of 1 and an intercept of −1024 for the Cine software. Slices were registered with the absolute MBF values obtained by micropspheres displayed as a circumferential profile. An algorithm was applied to baseline images prior to contrast arrival to correct for signal attenuation and nonuniformity. Three slices were analyzed per animal: apical where the blood pool is first evident, the most proximal slice imaged (approximately just beyond mid-ventricle, and the slice midway between these two slices. Regions of interest were selected within the myocardium in order to generate TACs for these three slices. CT perfusion images were segmented in an identical manner to the pathologic sectioning and a peak hyperemic segment was identified for each of the three slices. A control segment was chosen at each slice, 180° from the hyperemic zone within that slice.
A semi-quantitative method (see Figure 1) was used to obtain flow reserve estimates first described by Klocke et al (slope integral ratio or SIR) using first-pass MR perfusion imaging.12 This method is a ratio of the integral of the areas delineated by two TACs: adenosine zone and control zone curves. Consequently, it is analogous to nuclear SPECT imaging in that perfusion is relative to a predefined control region. The peak of the hyperemic curve upslope defines the cutoff value applied to both curves. A slope/integral ratio was calculated for each hyperemic zone or occlusion zone in three slices per animal. As a check on consistency, the control zones at apical and proximal levels had SIR values generated using the midventricular control area in the denominator. While this method does not provide absolute values of MBF, it has the advantage of being independent of an arterial input function measurement.
Schematic representation of the slope integral method to calculate CFR from first-pass CT images. The summed area under the curve is calculated for both adenosine (A + C) and control (C) TACs from serial CT images from the initial curve upslope to the peak of the adenosine curve). The ratio of these curves (A + C)/C defines the CFR
Imaging characteristics were measured for control segments only. Noise was measured as the standard deviation of the mean attenuation coefficient in an ROI just external to the chest cavity. Contrast to noise (CNR) was defined for this experiment as the change in myocardial signal intensity from baseline (precontrast) to peak enhancement divided by the noise value.
Statistical Analysis
Data are presented as mean ± standard deviation. Unpaired t-tests were used to compare continuous variables by grouping variable. Paired t-tests were used to compare variables with paired measures. Analysis of variance was used when more than two factors were being compared simultaneously with post hoc comparisons performed using the Fischer LSD test. Simple linear regression analysis was used to compare CT perfusion estimates to MBF by microspheres and Bland-Altman plots were constructed from these.
Results
Absolute MBF in ischemic zones was .24 ± .19 mL/min/g, control zones was .65 ± .25 mL/min/g and was 2.67 ± .66 mL/min/g in adenosine infusion zones (P < .0001 overall and for adenosine vs. control, see Table 1). The mean CFR ratio for hyperemia was 4.1 ± 1.1 as derived from microsphere values. The ratio of ischemic to control MBF was .37 ± .30. Heart rate values at the time of the CT scan were 88 ± 11 bpm for intracoronary adenosine and 87 ± 17 for occlusion studies.
Representative CT perfusion images are shown in Figure 2. Overall, spatial resolution was excellent. Myocardial contrast enhancement was 22 ± 11 HU from baseline. However, noise was high at 5.3 HU. CNR for control zones was 5.7 ± 4. Peak enhancement images demonstrated that CT attenuation values progressively increased from occlusion through control and hyperemic zones but were not linearly related to absolute MBF values in these same zones (Table 1).
CT images at peak enhancement. Top panel: axial images during LAD occlusion from apical to more basal location moving left to right. A perfusion defect is seen (white arrows) in the more apical locations. Bottom panel: images during intracoronary (LAD) adenosine. There is signal enhancement evident (white arrows) but not in proportion to the increase in CFR as measured by microsphere-derived MBF (approximately fourfold in this example)
CFR values by CT were not significantly different from those derived from microsphere MBF measurements: CFR by CT = 4.4 ± 1.4 vs 4.1 ± 1.1 via microspheres. There was a significant correlation between CRF measures by CT and microspheres (Figure 3) that remained linear through a broad range of values. Bland-Altman plots (Figure 4) were generated and produced 95% confidence limits of the agreement between microsphere and CT-derived CFR of 1.08.
Bland-Altman plot from Figure 3 comparing CFR by MBF and that by CT. The 95% confidence limits of the difference between the measures was 1.08 CFR units with virtually no offset of the mean from zero
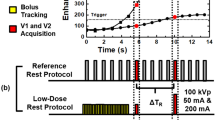
Representative myocardial TACs for control and adenosine zones are shown in Figure 5 as well as a TAC placed in the LV cavity. This latter curve represents the arterial input function that is an essential component for any first-pass perfusion technique targeted at estimating absolute MBF rather than a relative measure of CFR. To capture the slope integral ratio (blue rectangle zone), acquisition time would need to span approximately five heart beats at a heart rate of 80-90 bpm.
Smoothed and extrapolated curves derived from the LV blood pool representing an arterial input function (blue) adenosine myocardial zone (red) and control myocardial zone (orange) as a function of time. The shaded region reflects the necessary acquisition to capture the myocardial curve upslopes (approximately 5 s depending on heart rate)
Discussion
CTA can provide stunning anatomic detail noninvasively. Preliminary studies have suggested that it does serve as a prognosticator for patients being evaluated for the presence or absence of coronary artery disease.4-8 Functional criteria however, whether it be wall motion by stress echocardiography or myocardial perfusion imaging by SPECT techniques, have shown incremental prognostic information when coronary anatomy is known.18-22 To this end, there have been several approaches to combine CTA with an assessment of myocardial perfusion.
One approach is to take advantage of the newer generation PET scanners which have CT acquisition incorporated into the scanner. This provides the ability to acquire a CTA exam followed by a Rubidium-82 perfusion scan, both of which are tightly coregistered.23 The major drawback is the radiation absorbed by the patient from two separate sources. The other approach is to measure the first-pass of the iodinated contrast bolus during hyperemic stress similar to MRI-based stress imaging.15,16 Since the majority of CT scans are helical in nature (different portions of the myocardium are imaged over time), this approach is problematic for first-pass imaging that requires time-resolved serial imaging of a myocardial slice. Consequently, investigators have proposed separate contrast injections for the perfusion (nonhelical) and CTA (helical) portions of the exam. This significantly increases radiation and contrast exposure. The most efficient approach would be to acquire both pieces of information-anatomy and perfusion-simultaneously, but there are complexities to overcome.
This study demonstrates that a reasonable assessment of CFR can be measured from the integral of the upslope TAC. CFR measures were not significantly different between microsphere derived measures of absolute MBF and those by CT slope integral method. The confidence limits of the agreement between these measures were approximately 1 CFR unit which, during full hyperemia, reflects an error width of 20%. This approach has the advantage of not requiring the arterial input function in the calculation. Consequently, the acquisition could be confined to the period between the bolus entry into the myocardium and the peak myocardial enhancement-provided that the timing of such an acquisition was reliable. Such an approach would also require a much larger detector than used in this study in order to visualize the coronary tree without the necessity for helical pitch. Further studies are required to refine the optimal timing and methodology of acquisition.
There are limitations to this study that need to be considered. The current animal model was designed to produce regional differences in MBF through selective hyperemia or occlusion, producing two levels of flow within a tomographic slice. During a clinical SPECT study, the entire myocardium is subjected to hyperemia and CFR is determined using both a hyperemic scan and a rest scan as baseline. However, the methodology of semi-quantitation in this study could be used to detect differences in regional MBF without a rest scan, similar to the relative methods employed by SPECT imaging (i.e., the highest slope integral value can be set as the normalization standard with all other regions being a percentage of this value). Balanced ischemia in all three territories may be less of a problem than with SPECT as the reduction and delay in TAC upslope would be evident. Such an approach requires validation.
The study did not acquire a coronary angiogram simultaneous with a perfusion scan. The focus of the study was to validate a short, zero-pitch perfusion acquisition. With larger multidetectors (320 slice), the entire myocardium and vasculature might be covered without table movement. This may allow for a concurrent assessment of perfusion and anatomy, but there are a number of issues regarding adequate signal from the vasculature to reconstruct the angiogram and radiation exposure that need to be addressed. Additionally, systemic vasodilation will increase heart rate (approximately 10 bpm increase at 140 mcg/kg/min IV adenosine23,24) and reduce effective temporal resolution. This may degrade the image quality of the angiogram.
The change in contrast in these studies is small and difficult to discern visually despite significant differences in MBF in the same axial slice, as apparent from the data in Table 1. In contrast to first-pass MR perfusion studies with Gd-DTPA, the signal emanating from the myocardium at baseline is quite high for CT. Consequently, the transit of the bolus, while producing a similar change in absolute signal to MRI, provides a smaller percentage of signal change from baseline. This suggests that a form of quantitation may be necessary for any assessment of CT perfusion in the absence of methodology that nulls the baseline signal. These initial results do suggest that a short perfusion acquisition can adequately reflect CFR in normal vasculature.
References
Mollet NR, Cademartin F, Van Meigham CAG, Runza G, McFadden EP, Baks T, et al. High-resolution spiral computed tomography coronary angiography in patients referred for diagnostic conventional coronary angiography. Circulation 2005;112:2318-23
Miller JM, Rochitte CE, Dewey M, Arbab-Zadeh A, Niinuma H, Gottlieb I, et al. Diagnostic performance of coronary angiography by 64-row CT. N Engl J Med 2008;359:2324-36
Califf RM, Phillips HR III, Hindman MC, Mark DB, Lee KL, Behar VS, et al. Prognostic value of a coronary artery jeopardy score. J Am Coll Cardiol 1985;5(5):1055-63
Min JK, Shaw LJ, Devereux RB, Okin PM, Weinsaft JW, Russo DJ, et al. Prognostic value of multidetector coronary computed tomographic angiography for prediction of all-cause mortality. J Am Coll Cardiol 2007;50:1161-70
Gaemperil O, Valenta I, Schepis T, Husmann L, Scheffel H, Desbiolles L, et al. Coronary 64-slice CT angiography predicts outcome in patients with known or suspected coronary artery disease. Eur Radiol 2008;18:1162-73
Van Lingen R, Kakani N, Veitch A, Manghat NE, Roobottom CA, Morgan-Hughes JG. Prognostic and accuracy data of multidetector CT coronary angiography in an established clinical service. Clin Radiol 2009;64:601-7
Gopal A, Nasir K, Ahmadi N, Gul K, Tiano J, Flores M, et al. Cardiac computed tomographic angiography in an outpatient setting: An analysis of clinical outcomes over a 40-month period. J Cardiovasc Comput Tomogr 2009;3:90-5
Shaw LJ, Berman DS, Hendel RC, Borges-Neto S, Min JK, Callister TQ. Prognosis by coronary computed tomographic angiography: Matched comparison with myocardial perfusion single-photon emission computed tomography. J Cardiovasc Comput Tomogr 2008;2:102-4
Schwitter J, Nanz D, Kneifel S, et al. Assessment of myocardial perfusion in coronary artery disease by magnetic resonance: A comparison with positron emission tomography and coronary angiography. Circulation 2001;103:2230-5
Al-Saadi N, Nagel E, Gross M, et al. Noninvasive detection of myocardial ischemia from perfusion reserve based on cardiovascular magnetic resonance. Circulation 2000;101:1379-83
Jahnke C, Nagel E, Gebker R, Kokocinski T, Kelle S, Manka R, et al. Prognostic value of cardiac magnetic resonance stress tests: Adenosine stress perfusion and dobutamine stress wall motion imaging. Circulation 2007;115:1769-76
Klocke FJ, Simonetti OP, Judd RM, et al. Limits of detection of regional differences in vasodilated flow in viable myocardium by first-pass magnetic resonance perfusion imaging. Circulation 2001;104:2412-6
Christian TF, Rettmann D, Aletetras AH, Liao S, Taylor JL, Balaban RS, et al. Absolute myocardial perfusion in canines measured by using dual-bolus first-pass MR imaging. Radiology 2004;232:677-84
Jerosch-Herold M, Wilke N, Wang Y, et al. Direct comparison of an intravascular and an extracellular contrast agent for quantification of myocardial perfusion: Cardiac MRI Group. Int J Card Imaging 1999;15:453-64
George RT, Jerosch-Herold M, Silva C, Kitagawa K, Bluemke DA, Lima JA, et al. Quantification of myocardial perfusion using dynamic 64-detector computed tomography. Invest Radiol 2007;42:815-22
Groves AM, Goh V, Rajasekharan S, Kayani I, Endozo R, Dickson JC, et al. CT coronary angiography: Quantitative assessment of myocardial perfusion using test bolus data-initial experience. Eur Radiol 2008;18:2155-63
Rumberger JA, Bell MR. Measurement of myocardial perfusion and cardiac output using intravenous injection methods by ultrafast (cine) computed tomography. Invest Radiol 1992;27:S40-6
Borges-Neto S, Shaw LK, Tuttle RH, Alexander JH, Smith IV WT, Chambless M, et al. Incremental prognostic power of single-photon emission computed tomographic myocardial perfusion imaging in patients with known or suspected coronary artery disease. Am J Cardiol 2005;95:182-8
Marie PY, Danchin N, Durand JF, Feldmann L, Grentzinger A, Olivier P, et al. Long-term prediction of major ischemic events by exercise thallium-201 single-photon emission computed tomography. Incremental prognostic value compared with clinical, exercise testing, catheterization and radionuclide angiographic data. J Am Coll Cardiol 1995;26:879-86
Pollock SG, Abbott RD, Boucher CA, Beller GA, Kaul S. Independent and incremental prognostic value of tests performed in hierarchical order to evaluate patients with suspected coronary artery disease. Validation of models based on these tests. Circulation 1992;85:237-48
Ciaroni S, Bloch A, Hoffman JL, Bettoni M, Fournet D. Prognostic value of dobutamine echocardiography in patients with intermediate coronary lesions at angiography. Echocardiography 2002;19:549-53
Rizzello V, Poldermans D, Schinkel AF, Biagini E, Boersma E, Elhendy A, Sozzi FB, Maat A, Crea F, Roelandt JR, Bax JJ. Long-term prognostic value of myocardial viability and ischemia during dobutamine stress echocardiography in patients with ischemic cardiomyopathy undergoing coronary revascularization. Heart 2006;92:239-44
Javadi M, Mahesh M, McBride G, Voicu C, Epley W, Merrill J, et al. Lowering radiation dose for integrated assessment of coronary morphology and physiology: First experience with step-and-shoot CT angiography in a rubidium 82 PET-CT protocol. J Nucl Cardiol 2008;15:783-90
Verani MS, Mahmarian JJ, Hixson JB, Boyce TM, Staudacher RA. Diagnosis of coronary artery disease by controlled coronary vasodilation with adenosine and thallium-201 scintigraphy in patients unable to exercise. Circulation 1990;82:80-7
Author information
Authors and Affiliations
Corresponding author
Additional information
See related editorial on doi:10.1007/s12350-010-9250-2.
Rights and permissions
About this article
Cite this article
Christian, T.F., Frankish, M.L., Sisemoore, J.H. et al. Myocardial perfusion imaging with first-pass computed tomographic imaging: Measurement of coronary flow reserve in an animal model of regional hyperemia. J. Nucl. Cardiol. 17, 625–630 (2010). https://doi.org/10.1007/s12350-010-9206-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-010-9206-6