Abstract
Introduction
Functional impairment associated with mood disorders may be related to a characteristic “profile” of normative personality dimensions.
Methods
Individuals (age ≥ 18 years) with MDD (n = 400) or BD (n = 317), as defined by the Diagnostic and Statistical Manual of Mental Disorders, fourth edition, text revision (DSM-IV-TR), were enrolled in the IMDCP. Personality was evaluated with the Neuroticism–Extraversion–Openness Five-Factor Inventory (NEO-FFI), and functionality with the Sheehan Disability Scale and Endicott Work Productivity Scale. Path analysis using linear multiple regressions was performed to identify direct and indirect effects of personality on functional impairment.
Results
Lower conscientiousness exerted a significant direct effect on global (p = 0.017) and family life dysfunction in individuals with MDD (p = 0.002), as well as lower work productivity in both MDD (p = 0.020) and BD (p = 0.018). Lower extraversion exerted a significant direct effect on social impairment in individuals with BD (p = 0.017). Higher neuroticism and agreeableness as well as lower extraversion exerted indirect effects on global and social dysfunction in individuals with MDD via their effects on depression severity. In BD, higher neuroticism and openness indirectly affected global dysfunction. Family dysfunction was indirectly affected by higher neuroticism and openness as well as lower extraversion in MDD and BD.
Conclusion
The results suggest that discrete personality dimensions may exert direct and indirect effects on functional outcomes in individuals with mood disorders. Personalizing disease management approaches in mood disorders with emphasis on vocational rehabilitation may benefit from measurement and intervention targeting personality.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Personality is one of the primary factors responsible for human adaptation, interaction and behavior in different environments [1]. Personality psychopathology is reflected in the current Diagnostic and Statistical Manual of Mental Disorders, fourth edition, text revision (DSM-IV-TR) Axis II classification of personality disorders, which are characterized by persistent and maladaptive traits [2–4]. However, recent evidence supports the characterization of normative personality traits in other psychiatric disorders including major depressive disorder (MDD) and bipolar disorder (BD) [5–8]. Characteristic personality traits have also been described in other medical conditions (e.g., obesity, metabolic syndrome) [9–11]. Despite the available evidence, assessment of normative personality traits in other non-Axis II disorders is not currently part of routine clinical assessment or diagnostic criteria.
It has been suggested that psychosocial function is influenced by one’s personality characteristics [1, 12, 13]. Classically three domains of psychosocial function have been described: social life, family life and work function. Identifying normative personality traits that may be indicative of long-term functional outcomes may be useful in mood disorders. Mood disorders are highly prevalent conditions [14, 15] associated with a high rate of non-recovery, recurrence, and are a leading cause of disability in developed and developing nations [16–18]. In the United States, the estimated annual economic cost of mental illness was approximately $100 billion of which $51 billion was associated with work impairment [19, 20]. Similarly, the estimated losses due to lost work productivity and healthcare in Canada were $83.1 and $14.1 billion, respectively [21]. The work-related losses included both direct and indirect costs due to absenteeism and presenteeism (low work productivity) [22]. From the economic standpoint, decreasing the human capital costs of mood disorders has been identified as a primary objective; therefore, identifying barriers or facilitators to functional recovery is a research and clinical priority.
The five-factor model (FFM) of personality organizes personality traits along five basic dimensions [1]. The five dimensions include normative personality traits and can be described as follows: neuroticism (anxious, self-conscious, vulnerable), extraversion (assertive, energetic, outgoing), openness (curious, imaginative, wide interests), agreeableness (trusting, compliant, altruistic) and conscientiousness (competent, responsible, achievement striving). The role of maladaptive and impairing personality traits in characterizing function has been evaluated in individuals with personality disorders [23, 24]. The relationship between normative personality traits and functional outcomes in other populations has also been described [24, 25]. Using data from subjects diagnosed with a mood disorder (i.e., MDD and BD), as part of the International Mood Disorders Collaborative Project (IMDCP), this analysis explores the role of personality dimensions in characterizing global and domain-specific function in mood disorders.
Methods
Study Design
Individuals (age ≥ 18 years) with MDD and bipolar I/II disorder (BD-I and BD-II) were enrolled in the IMDCP. This is an ongoing, cross-sectional, naturalistic study evaluating individuals who present for an assessment or treatment at the Mood Disorders Psychopharmacology Unit (MDPU) at the University Health Network (UHN) in Toronto, Ontario or at the Cleveland Clinic, Lutheran Hospital, Cleveland, OH, USA. The MDPU is an outpatient program while the Cleveland Clinic offers both outpatient and inpatient services. All patients enrolled between August 2005 and December 2010 with a primary working diagnosis of a mood disorder, who were willing and able to provide informed consent, were included in the current analysis. The IMDCP was approved by the UHN Research Ethics Board and the Institutional Review Board of the Cleveland Clinic Foundation.
Assessments
The Mini-International Neuropsychiatric Interview (MINI Plus 5.0) [26] was used to confirm Axis I diagnoses. Depression severity was assessed using the Montgomery-Asberg Depression Rating Scale (MADRS) [27] and the 17-item Hamilton Depression Rating scale (HAMD-17) [28]. Manic symptom severity was assessed using the Young Mania Rating Scale (YMRS) [29]. Personality was assessed using the Neuroticism–Extraversion–Openness Five-Factor Inventory (NEO-FFI) [30]; a self-report scale that measures personality traits along five basic dimensions (extraversion, agreeableness, conscientiousness, neuroticism, and openness to experiences). The Sheehan Disability Scale (SDS) [31] and the Endicott Work Productivity Scale (EWPS) [32] were used for the assessment of psychosocial function. The SDS evaluates the degree of functional impairment over the past week in work, social, and family life. A total score reflects the degree of global functional impairment. The EWPS evaluates productivity in the workplace during the past week, with higher scores indicating greater dysfunction. All data were collected using paper versions of the scales and either manually entered or scanned using automated capture software (TeleForm, Version 8, Syscom Services, Inc., Silver Spring, MD, USA).
Statistical Analysis
Statistical analyses were conducted using Statistical Product and Service Solutions (SPSS) for Windows, Version 20.0 (SPSS Inc., Chicago, IL, USA). The Chi-square statistic was used for nominal variables and independent t tests were used for continuous dependent variables. All tests were two-tailed, with statistical significance set at p < 0.05. Path analyses using linear multiple regressions were performed to determine which personality dimensions exert a direct effect on function as the primary objective, and which dimensions exert an indirect influence on function via depression severity as the secondary objective of the study. Age, sex, age at onset, MADRS total score, YMRS total score (for BD group only), employment status, education and presence or absence of a medical co-morbidity were included in each step-wise regression model. Separate regression analyses were performed for MDD and BD.
Results
A total of 717 individuals with MDD (n = 400) and BD (BD-I, n = 208; BD-II, n = 109) were included in the analysis. There were no significant differences between individuals with MDD and BD in terms of demographic characteristics except for age (p = 0.027; Table 1). At the time of assessment, individuals with MDD were significantly older than individuals with BD [mean (SD): 40.63 (12.82) and 38.52 (12.22) years, respectively]. Differences between sex (p = 0.079), employment (p = 0.065), marital status (p = 0.405), annual household income (p = 0.079), education (p = 0.660), race (p = 0.587) were all non-significant. Individuals with MDD had significantly greater MADRS (p = 0.002) and HAMD-17 (p = 0.011) total scores, older age at illness (p < 0.001) and depression onset (p < 0.001) as well as older age at first treatment of depression (p = 0.048) compared to individuals with BD. A significantly lower number of lifetime depressive episodes (p < 0.001) as well as shorter illness duration (p < 0.001) was observed in MDD versus BD subjects (Table 2).
Using the NEO-FFI, individuals with MDD scored significantly lower on extraversion (p < 0.001), but higher on agreeableness (p = 0.004) than individuals with BD. No significant differences between the two groups were found for any other personality factor. Greater global function (p = 0.031) and SDS-social disability (p = 0.024) were observed in MDD as compared to BD individuals. No significant differences between the two disorders were evident for the SDS-family and SDS-work domains or EWPS (Table 2).
Direct Effects of Personality on Functional Measures in Mood Disorders
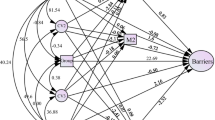
After adjusting for potential confounders, lower conscientiousness was significantly predictive of a greater SDS total score in individuals with MDD (p = 0.017), but not BD (Table 3; Fig. 1). No other personality factors exerted significant direct effects on global function. Family impairment was also predicted by lower conscientiousness in MDD (p = 0.020) but not BD, while social impairment was significantly predicted by lower extraversion in BD (p = 0.017), but not MDD (Table 3; Fig. 1). No personality factors significantly predicted work impairment on the SDS. Lower work productivity, measured with the EWPS, was predicted by lower conscientiousness in both mood disorder groups (MDD, p = 0.002; BD, p = 0.018) (Table 3; Fig. 1).
Indirect Effects of Personality on Function through Depression Severity
Path analysis revealed that the effect of personality on global functional impairment is largely indirect, occurring via effects on depression severity (Table 4; Figs. 2, 3). Global functional impairment was indirectly influenced by higher neuroticism and agreeableness as well as lower extraversion in individuals with MDD, and by higher neuroticism and openness in BD (Figs. 2, 3, respectively). No significant indirect effects on work productivity on the EWPS through depression severity were identified. Social and work dysfunctions on the SDS were indirectly affected by higher neuroticism and agreeableness, and lower extraversion in individuals with MDD (Table 4). Higher neuroticism and openness indirectly influenced greater work and social dysfunction in BD (Table 4). In MDD, higher neuroticism and agreeableness with lower extraversion indirectly influenced greater work and social dysfunction (Table 4). Family dysfunction in MDD was indirectly influenced by higher neuroticism, agreeableness, and lower extraversion, whereas in BD family dysfunction was indirectly influenced by higher neuroticism and openness (Table 4).
Discussion
This study identified that conscientiousness and extraversion exert direct effects on function while different combinations of personality features including neuroticism, extraversion, agreeableness and openness indirectly influence function by affecting depression severity. Lower conscientiousness directly contributes to lower work productivity in MDD and BD, and global and family impairment in MDD. Lower extraversion had a direct impact on social dysfunction in individuals with BD but not MDD. Higher neuroticism and agreeableness and lower extraversion exerted indirect effects on global and social dysfunction in MDD. In BD, higher neuroticism and openness indirectly affected global dysfunction. In MDD, family life impairment was indirectly affected by higher neuroticism and openness and lower extraversion while, in BD, family life impairment was indirectly affected by higher neuroticism and openness.
Taken together, distinct personality features may either directly or indirectly influence the severity of global and domain-specific functional impairment as well as the degree of workplace dysfunction in individuals with MDD and BD. Conscientiousness is the most consistent direct contributor to global and domain-specific (i.e. family) functioning, as well as work productivity. Conscientiousness is the personality dimension that organizes and directs behavior according to one’s conscience and is characterized by motivation, self-discipline, achievement striving, responsibility and thoroughness [33]. As such, conscientiousness would be expected to contribute to functioning, and lower levels can be expected to negatively relate to both function and work productivity [34, 35]. Conscientiousness and extraversion have been documented to have the greatest influence of the personality factors on adaptation in interpersonal relationships [36]. Extraversion was found to exert a direct effect on social function in individuals with BD but not MDD. Those with lower levels of these traits have the tendency to withdraw and not seek interaction, contributing to social impairment with decreased levels of social activity and satisfaction in social relationships [36, 37]. This is thought to lead to functional impairment in the areas of social and family life because of decreased tendencies to maintain responsibilities, be reliable, committed and dutiful. Moreover, conscientiousness is described as the strongest predictor of workplace performance [38]. This stems from the facets used to describe conscientious traits and behaviors which relate strongly to work performance and motivational tendencies [39]. It is possible that these behaviors and tendencies may perpetuate greater dysfunction that can affect other domains [40]. For example, impairing facets that result in poor work performance may include the inability to handle responsibilities, which may extend to family and social commitments.
Neuroticism, openness and agreeableness did not demonstrate significant direct effects on global functional impairment but did influence function through depression severity. Specifically, in BD and MDD, respectively, higher openness in conjunction with higher neuroticism, and agreeableness in conjunction with lower extraversion were found to indirectly influence function. This indirect effect may explain the conflicting results pertaining to openness and its moderational role on function as reported by others [24, 25, 41, 42].
Higher conscientiousness has also been shown to be predictive in positive health-promoting behaviors [43, 44]. Thus, enhancing conscientiousness may positively affect functioning not only in the affected functional domain but also health in general. Moreover, lower conscientiousness has a significant impact on mood and may be a vulnerability factor for depressed individuals that persists into remission [45]. Taken together there is a bidirectional association between conscientiousness and work performance; poor performance as caused by low conscientiousness helps to form negative beliefs about one’s self and abilities, which in turn further hinders performance [46].
The major limitations of our analysis were its cross-sectional assessment, retrospective post hoc design, and small number of subjects per group. Observations regarding the longitudinal stability of personality features and their predictive ability over time could not be explored. Measures of function relied on self-report, and are vulnerable to recollection bias and potential under-reporting or over-reporting of dysfunction. There was a discrepancy between the predictive personality dimensions identified by the two work function measures (SDS-work and EWPS) likely due to the related but not identical outcome measures and the sensitivity of the two self-reported scales; SDS-work assessed general functional work impairment with one item compared to the EWPS which assessed work productivity with 25-items. It is possible that the personality traits identified as predictive of dysfunction may not be unique to the mood disorder population but may extend to other conditions and the general population.
Conclusion
Identification of factors that predict functionality may facilitate long-term management strategies aimed at full functional recovery. This study suggests that personality measurement tools in combination with other factors (e.g., depression severity) may facilitate clinical care planning and management. Personality measures may also be used to monitor treatment efficacy; recent evidence supports the use of personality assessments for monitoring personality changes resulting from treatment with selective serotonin reuptake inhibitors in individuals with depression [47, 48].
Personality screening tools may also guide personalized treatment strategies targeting the dysfunctional personality facets, mitigating their effects on function. For example, occupational health services or related programs may offer counseling to employees identified as having poor work productivity and/or depression [49–51]. The potential use of interventions to target-specific individual personality traits has previously been described. Subjective belief of performance inadequacies in depressed patients has been shown to be an accurate representation of true performance; therefore, skill(s) training that target(s) these inadequacies may improve both performance and affect [45]. Therapeutic treatments (e.g., cognitive-behavioral therapy) aimed at enhancing extraversion and reducing neuroticism have also been described [52]. As a result, by targeting personality traits the clinician may improve a patient’s function across the affected domains directly, and indirectly by mitigating depressive symptoms. A “general mental illness” personality “profile” (high neuroticism, low extraversion, agreeableness and conscientiousness) [7] and a “depression profile” (high neuroticism, low extraversion) [5] have been reported. Hopwood et al. [24] explored the relation between FFM personality dimensions and function in a sample of individuals with personality disorders and MDD. They found that functional impairment in MDD was related to high neuroticism, low extraversion, openness and conscientiousness, which is similar to the general mental illness profile [24]. In our study, conscientiousness accounted for most of the direct contribution to function, while for the other personality factors, the effect on function was mediated by depression severity.
The goal of personalized medicine is to identify more effective and better tolerated treatments which consequentially improve functional outcomes and reduce costs. Mood disorders are the most disabling and costly chronic medical disorders in the working population. The importance of the role of psychological factors, particularly personality, and the integration of this knowledge into clinical practice are emerging. Our results are some of the first to characterize the contribution of personality to function, and document the pertinence of conscientiousness to functional impairment in mood disorders.
References
McCrae RR, Costa PT Jr. The five factor theory of personality. In: Pervin LA, John OP, editors. Handbook of personality. 2nd ed. New York: The Guilford Press; 1999. p. 139–53.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: 4th Editon Text Revision (DSM-IV-TR). Washington: American Psychiatric Association; 2000.
Krueger RF, Skodol AE, Livesley WJ, Shrout PE, Huang Y. Synthesizing categorical and dimensional approaches to personality disorders: refining the research agenda for DSM-V Axis II. Int J Methods Psychiatr Res. 2007;16:65–73.
Widiger TA, Trull TJ. Plate tectonics in the classification of personality disorder: shifting to a dimensional model. Am Psychol. 2007;62:71–83.
Clark LA, Watson D, Mineka S. Temperament, personality, and the mood and anxiety disorders. J Abnorm Psychol. 1994;103:103–16.
Kotov R, Gamez W, Schmidt F, Watson D. Linking “big” personality traits to anxiety, depressive and substance use disorders: a meta-analysis. Psychol Bull. 2010;136:768–821.
Malouff JM, Thorsteinsson EB, Schutte NS. The relationship between the five-factor model of personality and symptoms of clinical disorders: a meta-analysis. J Psychopathol Behav Assess. 2005;27:101–14.
Bagby RM, Young LT, Schuller DR, Bindseil KD, Cooke RG, Dickens SE, et al. Bipolar disorder, unipolar depression and the five-factor model of personality. J Affect Disord. 1996;41:25–32.
Sutin AR, Terracciano A, Deiana B, Uda M, Schlessinger D, Lakatta EG, et al. Cholesterol, triglycerides, and the five-factor model of personality. Biol Psychol. 2010;84:186–91.
Sutin AR, Costa PT Jr, Uda M, Ferrunni L, Schlessinger D, Terracciano A. Personality and metabolic syndrome. Age. 2010;32:513–9.
Terracciano A, Sutin AR, McCrae RR, Deiana B, Ferrucci L, Schlessinger D, et al. Facets of personality linked to underweight and overweight. Psychosom Med. 2009;71:682–9.
McCrae RR, Costa PT Jr. Toward a new generation of personality theories: theoretical contexts for the five-factor model. In: Wiggins J, editor. The five factor model of personality: theoretical perspectives. New York: The Guilford Press; 1996. p. 51–87.
Bromberger JT, di Scalea TL. Longitudinal associations between depression and functioning in midlife women. Maturitas. 2009;64:145–59.
Kessler RC, Akiskal HS, Ames M, Birnbaum H, Greenberg P, Hirschfeld RM, et al. Prevalence and effects of mood disorders on work performance in a nationally representative sample of U.S. workers. Am J Psychiatry. 2006;163:1561–8.
Vasiliadis HM, Lesage A, Adair C, Wang PS, Kessler RC. Do Canada and the United States differ in prevalence of depression and utilization of services? Psychiatr Serv. 2007;58:63–71.
Murray CJ, Lopez AD. Global mortality, disability, and the contribution of risk factors: global burden of disease study. Lancet. 1997;349:1436–42.
Simon GE. Social and economic burden of mood disorders. Biol Psychiatry. 2003;54:208–15.
Keck PE Jr, Kessler RC, Ross R. Clinical and economic effects of unrecognized or inadequately treated bipolar disorder. J Psychiatr Pract. 2008;14:31–8.
Greenberg PE, Kessler RC, Nells TL, Finkelstein SN, Berndt ER. Depression in the workplace: an economic perspective. In: Feighner JP, Boyer WF, editors. Selective serotonin reuptake inhibitors: Advances in basic research and clinical practice. 2nd ed. New York: Wiley; 1996. p. 327–63.
Wyatt RJ, Henter I. An economic evaluation of manic-depressive illness—1991. Soc Psychiatry Psychiatr Epidemiol. 1995;30:213–9.
Canada Health. A report on mental illness in Canada. Ottawa: Canadian Cataloguing in Publication Data; 2002.
McIntyre RS, Wilkins K, Gilmour H, Soczynska JK, Konarksi JZ, Miranda A, et al. The effect of bipolar I disorder and major depressive disorder on workforce function. Chronic Dis Can. 2008;28:84–91.
Skodol AE, Gunderson JG, McGlashan TH, Dyck IR, Stout RL, Bender DS, et al. Functional impairment in patients with schizotypal, borderline, avoidant, or obsessive-compulsive personality disorder. Am J Psychiatry. 2002;159:276–83.
Hopwood CJ, Morey LC, Ansell EB, Grilo CM, Sanislow CA, McGlashan TH, et al. The convergent and discriminant validity of five-factor traits: current and prospective social, work, and recreational dysfunction. J Pers Disord. 2009;23:466–76.
Hopwood CJ, Morey LC, Shea MT, McGlashan TH, Sanislow CA, Grilo CM, et al. Personality traits predict current and future functioning comparably for individuals with major depressive and personality disorders. J Nerv Ment Dis. 2007;195:266–9.
Sheehan D, Lecrubier Y, Sheehan K, Amorim P, Janavs J, Weiller E, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(Suppl 20):22–33.
Montgomery SA, Asberg M. A new depression scale designed to be sensitive to change. Br J Psychiatry. 1979;134:382–9.
Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23:56–62.
Young RC, Biggs JT, Ziegler VE, Meyer DA. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133:429–35.
McCrae RR, Costa PT Jr. A contemplated revision of the NEO Five-Factor Inventory. Pers Individ Dif. 2004;36:587–96.
Leon AC, Olfson M, Portera L, Farber L, Sheehan DV. Assessing psychiatric impairment in primary care with the Sheehan Disability Scale. Int J Psychiatry Med. 1997;27:93–105.
Endicott J, Nee J. Endicott Work Productivity Scale (EWPS): a new measure to assess treatment effects. Psychopharmacol Bull. 1997;33:13–6.
McCrae RR, John OP. An introduction to the five factor theory and its applications. J Pers. 1992;60:175–215.
Ross SR, Canada KE, Rausch MK. Self-handicapping and the five factor model of personality: mediation between neuroticism and conscientiousness. Pers Individ Dif. 2002;32:1173–84.
Minibashian A, Backmann N, Wood RE. Task-contingent conscientiousness as a unit of personality at work. J Appl Psychol. 2010;95:793–806.
Cukrowicz KC, Franzese AT, Thorp SR, Cheavens JS, Lynch TR. Personality traits and perceived social support among depressed older adults. Aging Ment Health. 2008;12:669.
Kitamura T, Watanabe K, Takara N, Hiyama K, Yasumiya R, Fujihara S. Precedents of perceived social support: personality, early life experiences, and gender. Psychiatry Clin Neurosci. 2002;56:169–76.
Hurtz GM, Donovan JJ. Personality and job performance: the big five revisited. J Appl Psychol. 2000;85:869–79.
Major DA, Turner JE, Fletcher TD. Linking proactive personality and the big five to motivation to learn and development activity. J Appl Psychol. 2006;91:927–35.
Barrick MR, Mount MK. The big five personality dimensions and job performance: a meta-analysis. Pers Psychol. 1991;44:1–26.
Peabody D, Goldberg LR. Some determinants of factor structures from personality-trait descriptors. J Pers Soc Psychol. 1989;57:552–67.
McCrae RR, Costa PT Jr. Openness to experience. In: Hogan R, Jones W, editors. Perspectives in personality: theory, measurement, and interpersonal dynamics. Connecticut: JAI Press; 1985. p. 145–72.
Tucker JS, Elliot MN, Klein DJ. Social control of health behaviour: associations with conscientiousness and neuroticism. Pers Soc Psychol Bull. 2006;32:1143–52.
Chapman BP, Franks P, Duberstein PR, Jerant A. Differences between individual and societal health state valuations. Med Care. 2009;47:902–7.
Anderson KW, McLean PD. Conscientiousness in depression: tendencies, predictive utility, and longitudinal stability. Cognitive Ther Res. 1997;21:223–38.
Pekrun R. The impact of emotions on learning and achievement: towards a theory of cognitive/motivational mediators. J Appl Psychol. 1992;41:359–76.
Tang TZ, DeRubeis RJ, Hollon SD, Amsterdam J, Shelton R, Schalet B. A placebo-controlled test of the effects of paroxetine and cognitive therapy on personality risk factors in depression. Arch Gen Psychiatry. 2009;66:1322–30.
Simmons JG, Allen NB. Mood and personality effects in healthy participants after administration of sertraline. J Affect Disord. 2011;134:377–85.
Tu HT, Boukus ER, Cohen GR. Workplace clinics: a sign of growing employer interest in wellness. Res Briefs. 2010;17:1–16.
Kristen W. Making the link between health and productivity at the workplace. Ind Health. 2010;48:251–5.
Mills PR, Kessler RC, Cooper J, Sullivan S. Impact of a health promotion program on employee health risks and work productivity. Am J Health Promot. 2007;22:45–53.
Sanderson C, Clarkin JF. Use of the NEO-PI personality dimensions in differential treatment planning. In: Widiger TA, Costa PT, editors. Personality disorders and the five-factor model of personality. Washington: American Psychological Association; 1994. p. 219–35.
Acknowledgments
The authors acknowledge the unrestricted grant provided by Pfizer, Canada Inc. Dr McIntyre is the guarantor for this article, and takes responsibility for the integrity of the work as a whole.
Conflict of interest
Roger McIntyre has received grants from Stanley Medical Research Institute, the National Alliance for Research on Schizophrenia and Depression (NARSAD), Eli Lilly, Janssen-Ortho, Shire, Astra-Zeneca, Pfizer and travel funds from Bristol-Myers Squibb. He has been an advisory board member for Astra Zeneca, Bristol-Myers Squibb, the France Foundation, GlaxoSmithKline, Janssen-Ortho, Solvay/Wyeth, Eli Lilly, Organon, Lundbeck, Biovail, Pfizer, Shire, Schering-Plough, and Merck. Dr McIntyre has also served on speaker bureaus for Janssen-Ortho, Astra-Zeneca, Eli Lilly, Lundbeck, Biovail, and Merck and has performed continuing CME activities for Astra-Zeneca, Bristol-Myers Squibb, the France Foundation, I3CME, Solvay/Wyeth, the Physicians’ Postgraduate Press, CME Outfitters, Optum Health, Schering-Plough, Merck and Eli Lilly. Joanna Soczynska has received travel funds from Janssen and is a recipient of the Eli Lilly Canada Fellowship Award. Mohammad Alsuwaidan has equity ownership in Sanofi-Aventis. David Muzina has received grant/research support from Repligen and has received honoraria from AstraZeneca, Pfizer, and Wyeth. Sideny Kennedy has been a consultant for St. Jude Medical, Bioavail, Eli Lilly, GlaxoSmithKline, Janssen-Ortho, Lundbeck and Merck Frost and has received honoraria from and served on speaker and advisory boards for medical education committees for Astra Zeneca, Bristol-Myers Squibb, the France Foundation, AstraZeneca, Bioavail, Eli Lilly, GlaxoSmithKline, Janssen-Ortho, Lundbeck, Servier, and Wyeth. Jessica Leen, Laura Ashley Gallaugher and Hanna Woldeyohannes declare no conflict of interest.
Compliance with ethics guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 and 2008. Informed consent was obtained from all patients for being included in the study. The IMDCP is approved by the UHN Research Ethics Board and the Institutional Review Board of the Cleveland Clinic Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leen, J., Soczynska, J.K., Gallaugher, L.A. et al. The Effect of Personality Dimensions on Functional Outcomes in Mood Disorders. Adv Ther 30, 671–683 (2013). https://doi.org/10.1007/s12325-013-0042-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-013-0042-3