Abstract
Introduction
Sedating effects of some medications used to treat allergic rhinitis (AR) symptoms can impair an individual’s ability to function optimally. The objective of this study was to characterize the effects of a single dose of loratadine/montelukast (L/M) versus placebo and diphenhydramine on daytime somnolence and psychomotor performance in healthy volunteers.
Methods
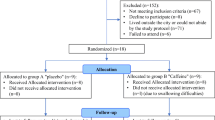
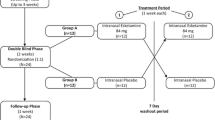
In this single-center, randomized, double-blind, placebo- and activecontrolled,three-way crossover study, healthy volunteers received single doses of placebo, L/M 10 mg/10 mg, and diphenhydramine 50 mg. Subjects (n=23) were evaluated under simulated cabin pressure using the following tools: Vigilance and Tracking Task (VigTrack), measuring vigilance and tracking performance; the Multi-Attribute Task Battery (MAT), measuring ability to perform multiple tasks simultaneously; and the Stanford Sleepiness Scale (SSS), measuring sedative effects of medication, at baseline and each hour from 1 to 6 hours postdose. Safety was monitored via adverse events and vital signs.
Results
Performances on VigTrack and MAT from 1 to 6 hours after dosing were not significantly different between L/M and placebo groups; in contrast, diphenhydramine resulted in significant impairment of tracking for up to 5 hours (P≤0.01) and vigilance performance for up to 3 hours (P≤0.05) on VigTrack versus placebo. Scores of subjective sleepiness as measured by SSS were similar for patients treated with L/M versus placebo, whereas significant increases in sleepiness occurred between 1–5 hours posttreatment in diphenhydraminetreated patients versus placebo-treated patients (P≤0.05).
Conclusions
L/M is similar to placebo in effects on daytime somnolence and psychomotor performance. L/M treatment resulted in significantly less sleepiness and impairment of vigilance and tracking than diphenhydramine.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Salib RJ, Drake-Lee A, Howarth PH. Allergic rhinitis: past, present and the future. Clin Otolaryngol Allied Sci. 2003;28:291–303.
Bousquet J, Neukirch F, Bousquet PJ, et al. Severity and impairment of allergic rhinitis in patients consulting in primary care.J Allergy Clin Immunol. 2006;117:158–162.
Green RJ, Davis G, Price D. Concerns of patients with allergic rhinitis: the Allergic Rhinitis Care Programme in South Africa. Prim Care Respir J. 2007; 16:299–303.
Stull DE, Roberts L, Frank L, Heithoff K. Relationship of nasal congestion with sleep, mood, and productivity. Curr Med Res Opin. 2007;23:811–819.
Shedden A. Impact of nasal congestion on quality of life and work productivity in allergic rhinitis: findings from a large online survey. Treat Respir Med. 2005;4:439–446.
Sundberg R, Toren K, Hoglund D, Aberg N, Brisman J. Nasal symptoms are associated with school performance in adolescents. J Adolesc Health. 2007; 40:581–583.
Szeinbach SL, Seoane-Vazquez EC, Beyer A, Williams PB. The impact of allergic rhinitis on work productivity. Prim Care Respir J. 2007;16:98–105.
Corey JP, Houser SM, Ng BA. Nasal congestion: a review of its etiology, evaluation, and treatment. Ear Nose Throat J. 2000;79:690–702.
Stokes J, Fenstad E, Casale TB. Managing impairment in patients with allergic rhinitis. Allergy Asthma Proc. 2006;27:12–16.
Casale TB, Blaiss MS, Gelfand E, et al. First do no harm: managing antihistamine impairment in patients with allergic rhinitis. J Allergy Clin Immunol. 2003;111:S835–S842.
Sen A, Akin A, Craft KJ, Canfield DV, Chaturvedi AK. First-generation H1 antihistamines found in pilot fatalities of civil aviation accidents, 1990-2005. Aviat Space Environ Med. 2007;78:514–522.
Eriksen CA, Akerstedt T. Aircrew fatigue in trans-Atlantic morning and evening flights. Chronobiol Int. 2006;23:843–858.
Wright N, McGown A. Vigilance on the civil flight deck: incidence of sleepiness and sleep during long-haul flights and associated changes in physiological parameters. Ergonomics. 2001;44:82–106.
Chaturvedi AK, Craft KJ, Canfield DV, Whinnery JE. Toxicological findings from 1587 civil aviation accident pilot fatalities, 1999-2003. Aviat Space Environ Med. 2005;76:1145–1150.
Soper JW, Chaturvedi AK, Canfield DV. Prevalence of chlorpheniramine in aviation accident pilot fatalities, 1991-1996. Aviat Space Environ Med. 2000;71:1206–1209.
Butler GC, Nicholas J, Lackland DT, Friedberg W. Perspectives of those impacted: airline pilot’s perspective. Health Phys. 2000;79:602–607.
Smith A. Hypoxia symptoms reported during helicopter operations below 10,000 ft: a retrospective survey. Aviat Space Environ Med. 2005;76:794–798.
Valk P, Simons M, Struyvenberg P, Kruit H, Van berge Hengouwen M. Effects of a single dose of loratadine on flying ability under conditions of simulated cabin pressure. Am J Rhinology. 1997; 11:27–33.
Kay GG, Berman B, Mockoviak SH, et al. Initial and steady-state effects of diphenhydramine and loratadine on sedation, cognition, mood, and psychomotor performance. Arch Intern Med. 1997;157: 2350–2356.
Simons M, Valk P, de Ree J, Veldhuijzen van Zanten O, D’Huyvetter K. Quantity and quality of onboard and layover sleep; effects on crew performance and alertness. Soesterberg, The Netherlands: Netherlands Aerospace Medical Centre; 1994.
Kay GG, Harris AG. Loratadine: a non-sedating antihistamine. Review of its effects on cognition, psychomotor performance, mood and sedation. Clin Exp Allergy. 1999;29(suppl. 3):147–150.
Weiler JM, Bloomfield JR, Woodworth GG, et al. Effects of fexofenadine, diphenhydramine, and alcohol on driving performance. A randomized, placebo-controlled trial in the Iowa driving simulator. Ann Intern Med. 2000;132:354–363.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Valk, P.J.L., Simons, M. Effects of loratadine/montelukast on vigilance and alertness task Performance in a simulated cabin environment. Adv Therapy 26, 89–98 (2009). https://doi.org/10.1007/s12325-008-0127-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-008-0127-6