Abstract
Autism spectrum disorders (ASDs) are known to be characterized by restricted and repetitive behaviors and interests and by impairments in social communication and interactions mainly including “theory of mind” (ToM) processes. The cerebellum has emerged as one of the brain regions affected by ASDs. As the cerebellum is known to influence cerebral cortex activity via cerebello-thalamo-cortical (CTC) circuits, it has been proposed that cerebello-cortical “disconnection” could in part underlie autistic symptoms. We used resting-state (RS) functional magnetic resonance imaging (fMRI) to investigate the potential RS connectivity changes between the cerebellar dentate nucleus (DN) and the CTC circuit targets, that may contribute to ASD pathophysiology. When comparing ASD patients to controls, we found decreased connectivity between the left DN and cerebral regions known to be components of the ToM network and the default mode network, implicated in specific aspects of mentalizing, social cognition processing, and higher order emotional processes. Further, a pattern of overconnectivity was also detected between the left DN and the supramodal cerebellar lobules associated with the default mode network. The presented RS-fMRI data provide evidence that functional connectivity (FC) between the dentate nucleus and the cerebral cortex is altered in ASD patients. This suggests that the dysfunction reported within the cerebral cortical network, typically related to social features of ASDs, may be at least partially related to an impaired interaction between cerebellum and key cortical social brain regions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Autism spectrum disorders (ASDs) are neurodevelopmental conditions mainly characterized by core deficits in social communication and interaction, as well as the presence of restricted and repetitive behaviors and interests [1]. It has been proposed that ASDs’ deficits can be explained by individuals’ difficulties with “theory of mind” (ToM) processes, a crucial component of social behavior referring to the ability of attributing mental states to self and other in order to predict and explain behaviors [2, 3]. According to the ToM hypothesis, pragmatic impairments of language and communication typically observed in ASDs may be explained in terms of social behavior deficits. The theory that individuals with ASD are unable to represent mental states shed light on the nature of social communication impairments, assuming that a specific communication deficit lies in the use of language to affect other minds and to give evidence of a speaker’s thoughts and intentions. In this context, more general deficiencies in communication caused by this deficit in the ToM might account for language impairments and the range of deficits found in autism, thus suggesting that they may be the result of one unique deficit in the cognitive function of mentalizing [4]. The interpretation of the underlying neuropathology of the disorder has been evolving in the literature, and it is now believed to affect a complex neural network and specific brain regions clearly related to core behavioral domains, such as ToM, consisting of frontal lobe portions, temporo-parietal areas, and subcortical structures [5]. The heterogeneity and complexity of core symptoms in ASD can be explained as a fundamental involvement of both gray (GM) and white matter (WM) of these structures [6]. The cerebellum has also been suggested to be part of the distributed neural circuits that may be dysfunctional in ASD [7–11]. Voxel-based morphometry (VBM) studies have investigated the structural brain network changes in autism and found decreased bilateral cerebellar cortical volume as one of the biomarkers for classification of ASD brains [12]. Decreased cerebellar GM has been reported in the midline lobule IX, crus I, and lobule VIII in ASD, while increased cortical volume has been found in lobule VI [13–16]. Cerebellar WM has also been proposed to be implicated in the pathophysiology of autism by diffusion tensor MRI tractography studies. Reduced integrity of cerebellar output fibers (i.e., superior cerebellar peduncle) [17, 18] and incoming cerebellar projections from the controlateral hemisphere (middle cerebellar peduncle) [19] have been previously reported. Altogether, considering the breadth and depth of symptoms of ASD, connection abnormalities, as opposed to focal regional abnormalities, may provide valuable insights into explaining the widespread symptomatology related to ASD. In this context, it may be important to consider that while the notion of functional specialization suggests that specific brain areas may play a crucial role in mediating given functions, a collective effort of different areas may be necessary in order to accomplish more complex functions. The cortical underconnectivity theory has been proposed as an explanatory model for ASDs which suggests that an abnormal functional connectivity among brain areas may be responsible for ASD patients’ ability to accomplish cognitive functions and social task successfully [20–24]. Thus, in addition to anatomical connectivity, investigation of functional connectivity may be necessary to further understand ASD cognitive and behavioral profile since it may help characterize the neural basis of higher order integrative processes typically impaired in ASDs [3, 25]. The term “functional connectivity” (FC) refers to synchronous activation of spatially remote brain regions [26–28] and can be investigated both, during a task, or simply measuring the spontaneous fluctuations in resting-state functional magnetic resonance imaging (RS-fMRI) signals [29]. Thus, functional connectivity is the mechanism underpinning the synchronization of regional brain activation and mediating complex cognitive tasks [30]. The cerebellum is known to modulate cerebral cortical activity via cerebello-thalamo-cortical (CTC) circuits [31] and has been reported to selectively contribute to distinct functional networks clearly related to higher level functions beyond motor control [32–34]. The cerebellar outputs converge onto the dentate nucleus (DN), which, in turn, sends neural fibers to the cerebral cortex and the thalamus via the superior cerebellar peduncles, thus completing the CTC circuit [31]. The DN represents one of the major cerebellar output channel participating in CTC circuits, with a more dorsal portion projecting to motor and premotor cortex, while caudal and ventral portions project to prefrontal and parietal cortex [35]. Axonal integrity of the dentate-thalamic pathway has been recently related to the behavioral phenotype of ASDs. Specifically, altered integrity of dorsal portion of dentate-thalamic pathway has been associated with motor features of ASDs, while ventral and caudal portions have been related to communication behavior [36]. In line with these evidences, communication and social scores in ASD population have been found to correlate with GM differences in the cerebellar crus I/II [37] that are anatomically and functionally connected to prefrontal and parietal regions of the cerebral cortex [38–40]. Altogether, this evidence suggests that specific cerebello-cortical circuits are involved in determining certain ASD core symptoms. However, since functional connectivity expresses only partially structural abnormalities associated with a white matter tract [19], in the present study we assessed for the first time potential changes in functional connectivity between the DN and CTC circuit targets using RS-fMRI in order to test the relationship between cerebello-cerebral functional connectivity and ASDs and to assess whether a lack of connectivity within specific cerebellar-cerebral circuits could also characterize ASD pathophysiology.
Material and Methods
Subjects
Ten adults aged 17 to 33 years [mean (SD) age = 23.8 (6.1); M/F = 6/4], with a previous diagnosis of Asperger syndrome or high-functioning autism based on DSM-IV-TR criteria, that had been made by an appropriately qualified professional using established assessment techniques [Autism Diagnostic Observation Schedule (ADOS)] [mean (SD) 9.8 (3.65)] [41], were recruited for the current study. All participants completed Autistic Spectrum Quotient (AQ) [42] (mean/SD 36/7.9) and the Wechler Adult Intelligence Scale-Revised (WAIS-R) [43] for evaluation of total IQ scores (mean/SD 104.6/18.2), and a comprehensive neurological examination was performed by an expert neurologist. According to the inclusion criteria, the absence of any structural brain abnormality or psychiatric comorbidities was also ensured. Additionally, participants with ASDs did not take any medication at the time of testing.
In addition, 36 typically developing adults (TDAs) aged 19 to 35 years [mean (SD) age = 26.5 (3.83); M/F = 18/18] with no history of psychiatric or neurological illness were enrolled as control group. The mean age of ASD patients and TDAs did not significantly differ (p = 0.13).
This research study was approved by the Ethics Committee of Santa Lucia Foundation, according to the principles expressed in the Declaration of Helsinki. Written informed consent was obtained from all subjects (or their responsible guardian if incapable) before study initiation.
MRI Acquisition Protocol
All subjects underwent an MRI examination at 3T (Magnetom Allegra, Siemens, Erlangen, Germany) that included the following acquisitions: (1) dual-echo turbo spin echo [TSE] (TR = 6190 ms, TE = 12/109 ms); (2) fast-FLAIR (TR = 8170 ms, 204TE = 96 ms, TI = 2100 ms); (3) T1-weighted 3D high-resolution scan (3D modified driven equilibrium Fourier transform (MDEFT) [44] (TR = 1338 ms, TE = 2.4 ms, matrix = 256 × 224 × 176, in-plane FOV = 250 × 250 mm2, slice thickness = 1 mm); (4) T2* weighted echo planar imaging (EPI) sensitized to blood oxygenation-level dependent imaging (BOLD) contrast (TR 2080 ms, TE 30 ms, 32 axial slices parallel to AC-PC line, matrix 64 × 64, pixel size 3 × 3 mm2, slice thickness 2.5 mm, flip angle 70°) for resting-state fMRI. BOLD echo planar images were collected during rest for a 7 min and 20 s period, resulting in a total of 220 volumes. During this acquisition, subjects were instructed to keep their eyes closed, not to think of anything in particular, and not to fall asleep. The TSE scans of patients, acquired as part of this research study, were reviewed by an expert neuroradiologist in order to characterize the brain anatomy and determine the presence of macroscopic structural abnormalities. For the TDAs, conventional MRI was inspected in order to exclude any pathological conditions according to the inclusion criteria.
Resting-State fMRI Data Preprocessing
Data were pre-processed using Statistical Parametric Mapping [Wellcome Department of Imaging Neuroscience; SPM8 (http://www.fil.ion.ucl.ac.uk/spm/)], and in-house software implemented in Matlab (The Mathworks Inc., Natick, Massachussetts, USA). For each subject, the first four volumes of the fMRI series were discarded to allow for T1 equilibration effects. The pre-processing steps included correction for head motion, compensation for slice-dependent time shifts, normalization to the EPI template in MNI coordinates provided with SPM8, and smoothing with a 3D Gaussian Kernel with 8 mm3 full width at half maximum. For each data set, motion correction was checked to ensure that the maximum absolute shift did not exceed 2 mm and the maximum absolute rotation did not exceed 1.5°. The global temporal drift was removed using a third-order polynomial fit, and the signal was regressed against the realignment parameters, and the signal averaged over whole brain voxels, to remove other potential sources of bias. Then, all images were filtered by a phase-insensitive band-pass filter (pass band 0.01–0.08 Hz) to reduce the effect of low-frequency drift and high-frequency physiological noise. Every participant’s MDEFT was segmented in SPM in order to estimate the total GM volume. This quantity was compared (using a two-sample t test) between patients and controls to exclude the presence of macroscopic atrophy in patients.
Definition of Regions of Interest
The left and right DN masks were separately extracted according to the spatially unbiased atlas template of the cerebellum and brainstem (SUIT) [45] (Fig. 1) and resliced into EPI standard space.
Seed-Based Analyses
In order to estimate the correlation between each voxel in the brain and the seed regions, we used a first-level SPM model. The mean time course within each seed region of interest (ROI) was extracted for every participant and used as a regressor in a first-level SPM analysis (without conditions). The resulting beta images are thus equivalent to the Fisher z-transformed maps of the correlation coefficient. These images were taken to the second level, for a group analysis. At second level, a two-sample t test model was used to explore differences in connectivity between patients and controls in each ROI.
Two out of ten patients were excluded from the study due to motion exceeding the set thresholds (2 mm translation and 1.5° rotation) occurring during their MRI scans. Thus, only eight patients [mean (SD) age = 23.7 (6.3); M/F = 4/4] with ASD were included in the sample. None of the controls showed significant motion.
Between-group statistical significance was set at p < 0.05 FWE-corrected at cluster level (clusters formed with uncorrected voxels p < 0.005 at voxel level). Sex was set as covariate of no interest.
Results
Between Groups Differences of DN Functional Connectivity
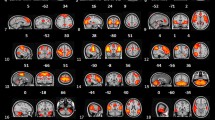
No significant difference between groups was detected in GM volumes (p = 0.87). When comparing the pattern of left DN functional connectivity in ASDs against TDA group, the group level analyses showed decreased FC of the left DN with contralateral regions of the cerebral cortex (Fig. 2). Clusters of significant FC decrease included the right precentral gyrus and the middle frontal gyrus, the right angular gyrus with extension in the superior parietal lobe, and the posterior division of right supramarginal gyrus (rSMG), the right parietal opercular cortex, right planum temporal, and superior temporal gyrus (see Table 1 for details).
Left DN functional connectivity with brain regions. Differences in functional connectivity of the left DN between control and patients groups are shown in sagittal (left column), coronal (central column), and axial slices (right column). Clusters of decreased functional connectivity are labeled in different colors: precentral gyrus (x = 46, y = −4, z = 48) in light blue; angular gyrus (x = 46, y = −46, z = 42) in red; parietal opercular cortex (x = 54, y = −20, z = 14) in yellow. See Table 1 for details. S superior, I inferior, R right, L left, A anterior, P posterior
When looking at the FC between the right DN and the cerebral cortex, no significant reduction was found in ASDs compared to TDAs.
In light of the present results, we additionally investigated whether and which regions of the cerebellar cortex were involved in the impaired FC of the left dentate nucleus.
A two-sample t test model was used to compare the two groups’ contrast images for positive correlation obtained at the first level, as described above, but restricting the analysis to the voxels of the sole cerebellar cortex.
When comparing the ASDs against TDA group, the second-level analyses showed a pattern of overconnectivity between the left DN with bilateral regions of the cerebellar cortex (Fig. 3). Cluster of significant FC increase included the left cerebellar lobule VI with extension to the left crus I (lobule VIIA), contralateral right V and VI, and vermis VI (see Table 2 for details). Conversely, no significant pattern of underconnectivity was detected throughout the cerebellar cortex.
Left DN functional connectivity with regions in the cerebellar cortex. Differences in functional connectivity of the left DN between control and patient groups are shown in coronal (right), axial (middle), and sagittal (left) slices. Cluster of increased functional connectivity (labeled in red) is centered in the left cerebellar lobule VI with extension in the left crus I and cerebellar regions in the contralateral hemisphere
Discussion
The present RS-fMRI study provides the first evidence of specific patterns of reduced functional connectivity between the DN and specific cerebral structures in patients with ASDs.
Underconnectivity theory has characterized autism as a neural system disorder [20]. In this study, an impaired connectivity between cerebellum and medial frontal and posterior temporal and parietal regions is the prominent findings in ASD group. These results are consistent with our hypothesis that dentate-cerebral FC may contribute to ASD pathophysiology. This is also in line with existent literature that evidenced cerebellar structural abnormalities [12, 37] and altered cerebello-cerebral white matter pathways in individuals with ASD [17–19]. More specifically, our results demonstrated that a set of regions consistent with the ToM brain network [46] has reduced connectivity with cerebellar DN.
The impairment in social cognition skills, particularly referring to the ToM, is one of the hallmarks of ASDs. Brain imaging studies have indicated that ToM processing is based on the activity of at least two brain areas, the right posterior temporal sulcus with the nearby temporo-parietal junction, and the medial frontal areas [46].
It is well known that the interactions between cerebellum and cortex play an important role in higher order functions, including emotional regulation and social cognition [47–50]. Temporo-parietal junction, together with medial frontal region are two of the major projections areas of the cerebellar efferent output [51, 52] and have been found to have reduced activation in ASDs during mentalizing tasks [53]. Evidence from a recent fMRI study showed a reliable reduction in the synchronous activation between the frontal ToM areas (medial frontal, orbitofrontal) and posterior ToM areas (right middle and superior temporal gyri, temporoparietal junction) in the group with autism compared to controls during the ToM task [46]. In line with the underconnectivity theory of autism [20], the authors posit that the ToM deficit is due to an impairment in frontal-posterior connectivity and that restrict communication between frontal and posterior areas of ToM cortical network regions may be responsible of ToM deficits [46].
It is worth noting that we found decreased functional connectivity with the cerebellar dentate nucleus in regions belonging to the default mode network (DMN) [54], a network indispensable for functions underpinning the social understanding of others, such as perceiving and interpreting other’s emotion status, showing empathy to other people, inferring other people’s intention and beliefs [55, 56], all features related to social deficits observed in ASDs.
A number of resting-state functional connectivity studies have demonstrated that the cerebellum contributes to different higher order cortical networks, including fronto-parietal networks as well as DMN [33, 34, 38, 57, 58]. Crus I/II has been shown to participate in the default mode network by mediating default regions’ activity [59]. The DMN includes a set of brain structures such as the posterior cingulate cortex, the retrosplenial cortex including the precuneus region, the lateral parietal cortex/angular gyrus, the medial prefrontal cortex, the superior frontal gyrus, the temporal lobe, the parahippocampal gyrus, and the temporo-parietal junction (TPJ) [54]. RS-fMRI studies have investigated DMN activation and connectivity in adults and adolescents with ASDs and identified reduced anterior/posterior DMN connectivity using both ROIs based and whole brain methods of image analysis [23, 60–63]. Furthermore, autistic traits related to social cognition processing have been shown to be associated to modified FC between regions within the DMN [64]. The right supramarginal gyrus and the right angular gyrus have been reported to be part of the anatomical parcellation of the rTPJ [65–68]. Previous social neuroscience research has consistently implicated the TPJ, particularly the right TPJ, in ToM self-other distinction tasks [65, 66, 69, 70] and specific mentalizing tasks [71–75]. Structural and functional connectivity measures have supported the anatomical segregation of the TPJ. A more anterior subdivision, encompassing the SMG, has been found to exhibit strongest connectivity with areas (such as medial cingulate cortex and insular cortex) [67] generally associated with affect regulation [76, 77] and affect sharing [78] and more strongly activated during emotion mentalizing (inferring another person’s emotion) [79]. In contrast, a more posterior subdivision centered on the angular gyrus has been reported to show the strongest connectivity with areas generally associated with ToM (such as the precuneus and medial prefrontal cortex) and the suppression of imitative tendencies [65, 66]. The same area is more strongly activated during intention mentalizing (inferring another person’s intention) [79]. The cerebellum has been implicated in setting up distant cortical networks in the brain during development [80]. It follows that specialization of cortical regions involved in language, social interaction, and motor control in ASDs might be impaired due to disruptions of specific cerebro-cerebellar networks and may lead to long-term impairments in these domains. Over the years, evidence for cerebellar involvement in ASDs has been growing in literature. Increased and decreased cerebellar gray matter volume [37, 81], vermal lobular hypoplasia [8], and cerebellar abnormalities in Purkinje cells and in the major input and output structures [82] have been reported in ASDs. Rogers and coll. [83] hypothesized a developmental cerebellar neuropathology to affect the autistic brain and a subsequent “disconnection” due to a loss of the outflow of the cerebellar cortex [11, 82]. This may result not only in disrupted communications between the cerebellum and its efferent target but also activate compensations or adaptation mechanisms of the affiliated neuronal circuitry accounting for behavioral and cognitive symptoms associated with autism [83]. Consistently, cerebro-cerebellar underconnectivity in supramodal cognitive networks has been found in children and adolescents with ASDs compared to controls [84]. In light of this, it is reasonable that a cerebellar dysfunction may affect long distance regions of the brain and that clinical symptoms may be related with changes in such cortical networks.
Connectivity between mentalizing network of the cerebrum and mentalizing areas in the cerebellum has been demonstrated by a recent connectivity analysis [85], supporting that the cerebellum plays a crucial role in social cognition by recruitment of domain-specific mentalizing processes [86]. The general assumption is that the cerebellum makes internal sequencing predictions based on the input of the mentalizing areas of the cerebrum and sends back error signals if mismatches occur between anticipated social events and current behavior [85].
This suggests that the dysfunction reported within the regions typically related to social features of ASDs may be due to a loss or dysregulation of the cerebellar output to certain “social brain areas” impeding the cerebellar modulation necessary to accomplish complex cognitive task and adaptive social behavior successfully. The decreased functional connectivity between the cerebellar DN and regions of the social brain network (i.e., fronto-parietal areas and DMN) evidenced in the present study gives a strong support to this hypothesis.
We only found altered FC to affect the left dentate nucleus. This finding seems to be in contrast with existing literature investigating cerebellar alterations in individuals with ASD and suggesting a vulnerability of the right cerebellar neural pathways [17, 36]. However, these previous studies were both focused on assessing structural connectivity, while the current study is based on FC. For its own nature, FC does not necessarily reflect structural abnormalities within specific white matter tracts [19]. For this reason, structural and functional connectivity findings are likely to reflect complementary aspects rather than being in contrast to each other.
On the other hand, a recent functional connectivity study in ASD subjects reported altered correlations between cortical areas and cerebellar lobuli in the right as well as in the left cerebellar hemisphere. Further, this abnormal cerebro-cerebellar correlation was not in line with the “primarily crossed connectivity between cerebral and cerebellar hemispheres” [84]. In view of these considerations, our data regarding the selective involvement of the left dentate nucleus raise the question about the functional significance of such a lateralization. Further investigations are needed to address this important issue.
Finally, the pattern of increased FC between the left dentate nucleus and regions of the cerebellar cortex needs to be discussed.
Our results are at least partially consistent with Khan et al. [84] showing that overconnectivity in the cerebellar cortex of ASD subjects occurs predominantly in lobule VI, crus I and II, and lobules VIIIA and VIIIB. However, it should be considered that this previous study investigated correlations between cerebellar cortex and cerebral supramodal and sensorimotor regions, but not within the cerebellum itself.
From an anatomical point of view, efferent projections from the cerebellar cortex first synapse in the deep cerebellar nuclei (e.g., dentate nucleus) and then project to a second synapse in the contralateral thalamus. The thalamus, in turn, serves as a relay to the cerebral cortex (the dentate-thalamo-cortical tract) [87, 88]. These anatomical observations provide strong support to our results. The Purkinje cells are the only output neurons from the cerebellar cortex that inhibit the deep cerebellar nuclei. It is therefore conceivable that the overconnectivity we found in the cerebellar cortex exerts increased inhibition on the dentate nucleus, which, in turn, reduces its excitatory outputs to the cerebral cortex. As consequence, this might explain the pattern of reduced dentate-cerebral FC we observed here. Finally, it is worth noting that, according to different functional imaging studies [38, 58], the cerebellar lobules showing overconnectivity with the left dentate are classified as supramodal cerebellar regions and have been reported to be associated with the default mode network [34, 57].
Our study also suffers from some important limitations. First, it is well known that individuals with ASD are more likely to move during their scans than healthy controls, and motion constitutes an important confound in functional connectivity analyses [89]. We have applied a rather simplistic approach to adjust for this confound, whilst more sophisticated approaches, such as using higher order models of motion, or independent component analysis (ICA) to classify motor components on subject by subject basis [90]. We have however excluded from the analysis participants where excessive motion was evident. A second limitation is the small number of subjects who were recruited. Although these data strongly support preliminary evidence of cerebro-cerebellar disconnection to subtend ASD social dysfunction, future studies with larger patient population are needed to reinforce such an interpretation. It is important to reiterate, however, that, despite the relatively small number of individuals with ASD taking part in the study, our results were statistically significant, thus supporting the relevance of our conclusions.
Another issue concerns with the gender distribution within our ASD group, as half of the subjects are female while ASD has typically male prevalence [91]. Although a gender bias is very likely to be genuine, the traditionally accepted 4–5:1 male prevalence has been recently questioned. A recent study highlighted that it may be “partly due to the underrecognition of females (particularly higher functioning), ascertainment bias, and issues of diagnostic instruments” [92]. Furthermore, it should be considered that diagnosis is later in females than in males [93, 94]. In particular, those who are higher functioning and have atypical, compensated, or masked characteristics might be underrecognized or misrecognized until later in adolescence or adulthood. It has to be considered that we only included high-functioning adult subjects and some studies tend to find no sex/gender differences in this kind of ASD population [95–97].
Finally, another drawback that needs to be considered is that, due to the small sample size, we could not perform correlations between social behavioral scores and functional data. This issue should be addressed in future studies in order to clarify the relationship between cerebello-cortical connectivity and ASD pathology as it can provide important additional insight.
Overall, this study provides the first evidence of an impaired resting-state functional connectivity between DN and cortical regions involved in the mediation of social cognitive behavior in individuals with ASD.
Conclusion
We examined for the first time functional connectivity between dentate nucleus and cerebral cortex regions in ASDs thus suggesting that social perception changes typically associated with autism may be also related to altered interaction between cerebellum and key social brain regions.
Specifically, altered functional connectivity was found between cerebellum and cerebral regions known to be components of ToM network and default mode network, strongly implicated in some aspects of social cognition processing.
Altogether, the present results provide a great insight into understanding the potential role the cerebellum may have in core autistic symptoms by mediating key cortical brain networks related to social cognition processing and typically altered in ASDs.
References
American Psychiatry Association Diagnostic and statistical manual of mental disorder (5th ed.). Washington, DC; London, England: American Psychiatric Publishing; 2013.
Baron-Cohen S. Mindblindness: an essay on autism and theory of mind. lgg5. Cambridge: MIT Press; 1995.
Hill EL, Frith U. Understanding autism: insights from mind and brain. Philos Trans R Soc Lond B Biol Sci. 2003;358:281–9.
Frith U, Happé F. Why specific developmental disorders are not specific: online and developmental effects in autism and dislexya. Dev Sci. 1998;1:267–72. Blackwell Publishers Ltd.
Coricelli G. Two-levels of mental states attribution: from automaticity to voluntariness. Neuropsychologia. 2005;43:294–300.
Minshew NJ, Williams DL. The new neurobiology of autism: cortex, connectivity and neuronal organization. Arch Neurol. 2007;6:945–50.
Bauman ML, Kemper TL. Histoanatomic observations of the brain in early infantile autism. Neurology. 1985;35:866–74.
Ritvo ER, Freeman BJ, Scheibel AB, Duong T, Robinson H, Guthrie D, et al. Lower purkinje cell counts in the cerebella of four autistic subjects: Initial findings of the UCLA-NSAC autopsy research report. Am J Psychiatry. 1986;143:862–6.
Courchesne E, Yeung-Courchesne R, Press GA, Hesselink JR, Jernigan TL. Hypoplasia of cerebellar vermal lobules VI and VII in autism. N Engl J Med. 1988;318:1349–54.
Bailey A, Palferman S, Heavey L. Autism: the phenotype in relatives. J Autism Dev Disord. 1998;28:369–91.
Amaral DG, Schumann Mills C, Wu Nordahl C. Neuroanatomy of autism. Trends Neurosci. 2008;31:137–45.
Ecker C, Rocha-Rego V, Johnston P, Mourao-Miranda J, Marquand A, Daly EM, et al. Investigating the predictive value of whole-brain structural MR scans in autism: a pattern classification approach. Neuroimage. 2010;49:44–56.
Cauda F, Geda E, Sacco K, D’Agata F, Duca S, Geminiani G, et al. Grey matter abnormality in autism spectrum disorder: an activation likelihood estimation meta-analysis study. J Neurol Neurosurg Psychiatry. 2011;82:1304–13.
Yu KK, Cheung C, Chua SE, McAlonan GM. Can Asperger syndrome be distinguished from autism? An anatomic likelihood meta-analysis of MRI studies. J Psychiatry Neurosci. 2011;36:412–21.
Duerden EG, Mak-Fan KM, Taylor MJ, Roberts SW. Regional differences in grey and white matter in children and adults with autism spectrum disorders: an activation likelihood estimate (ALE) meta-analysis. Autism Res. 2012;5:49–66.
Nickl-Jockschat T, Habel U, Michel TM, Manning J, Laird AR, Fox PT, et al. Brain structure anomalies in autism spectrum disorder—a meta-analysis of VBM studies using anatomic likelihood estimation. Hum Brain Mapp. 2012;33:1470–89.
Catani M, Jones D, Daly E, Embiricos N, Deeley Q, Pugliese L, et al. Altered cerebellar feedback projections in Asperger syndrome. Neuroimage. 2008;41:1184–91.
Sivaswamy L, Kumar A, Rajan D, Behen M, Muzik O, Chugani D, et al. A diffusion tensor imaging study of the cerebellar pathways in children with autism spectrum disorder. J Child Neurol. 2010;25:1223–31.
Groen WB, Buitelaar JK, van der Gaag RJ, Zwiers MP. Pervasive microstructural abnormalities in autism: a DTI study. J Psychiatry Neurosci. 2011;36:32–40.
Just MA, Cherkassky VL, Keller TA, Minshew NJ. Cortical activation and synchronization during sentence comprehension in high-functioning autism: evidence of underconnectivity. Brain. 2004;127:1811–21.
Courchesne E. Mapping early brain development in autism. Neuron. 2007;56:399–413.
Kleinhans NM, Richards T, Sterling L, Stegbauer KC, Mahurin R, Johnson LC, et al. Abnormal functional connectivity in autism spectrum disorders during face processing. Brain. 2008;131:1000–12.
Weng SJ, Wiggins JL, Peltier SJ, Carrasco M, Risi S, Lord C, et al. Alterations of resting state functional connectivity in the default network in adolescents with autism spectrum disorders. Brain Res. 2010;1313:202–14.
Kana RK, Libero LE, Moore MS. Disrupted cortical connectivity theory as an explanatory model for autism spectrum disorders. Phys Life Rev. 2011;8:410–37.
Minshew NJ, Goldstein G, Siegel DJ. Neuropsychologic functioning in autism: profile of a complex information processing disorders. J Int Neuropsychol Soc. 1997;3:303–16.
Friston KJ, Frith CD, Liddle PF, Frackowiak RS. Functional connectivity: the principal-component analysis of large (PET) data sets. J Cereb Blood Flow Metab. 1993;13:5–14.
van de Ven VG, Formisano E, Prvulovic D, Roeder CH, Linden DE. Functional connectivity as revealed by spatial independent component analysis of fMRI measurements during rest. Hum Brain Mapp. 2004;22:165–78.
Broyd SJ, Demanuele C, Debener S, Helps SK, James CJ, Sonuga Barke EJ. Default-mode brain dysfunction in mental disorders: a systematic review. Neurosci Biobehav Rev. 2009;33:279–96.
Biswal BB, Van Kylen J, Hyde JS. Simultaneous assessment of flow and BOLD signals in resting-state functional connectivity maps. NMR Biomed. 1997;10:165–70.
Damoiseaux JS, Rombouts SA, Barkhof F, Scheltens P, Stam CJ, Smith SM, et al. Consistent resting-state networks across healthy subjects. Proc Natl Acad Sci U S A. 2006;103:13848–53.
Middleton FA, Strick PL. Basal ganglia and cerebellar loops: motor and cognitive circuits. Brain Res Brain Res Rev. 2000;31:236–50.
Allen G, McColl R, Bernard H, Ringe WK, Fleckenstein J, Cullum CM. Magnetic Resonance Imaging of cerebellar-prefrontal and cerebellar parietal functional connectivity. Neuroimage. 2005;28:39–48.
Habas C, Kamdar N, Nguyen D, Prater K, Beckmann CF, Menon V, et al. Distinct cerebellar contributions to intrinsic connectivity networks. J Neurosci. 2009;29:8586–94.
Bernard JA, Seidler RD, Hassevoort KM, Benson BL, Welsh RC, Wiggins JL, et al. Resting state functional connectivity networks: a comparison of anatomical and self-organizing map approaches. Front Neuroanat. 2012;10:6–31.
Dum RP, Strick PL. An unfolded map of the cerebellar dentate nucleus and its projections to cerebral cortex. J Neurophysiol. 2003;89:634–9.
Jeong JW, Chugani DC, Behen ME, Tiwari VN, Chugani HT. Altered white matter structure of the dentantorubrothalamic pathway in children with Autistic Spectrum Disorders. Cerebellum. 2012;11:957–71.
D’Mello AM, Crocetti D, Mostofsky SH, Stoodley CJ. Cerebellar gray matter and lobular volumes correlate with core autism symptoms. Neuroimage: Clin. 2015;7:631–9.
Buckner RL, Krienen FM, Castellanos A, Diaz JC, Yeo BT. The organization of the human cerebellum estimated by intrinsic functional connectivity. J Neurophysiol. 2011;106:2322–45.
Strick PL, Dum RP, Fiez JA. Cerebellum and nonmotor function. Annu Rev Neurosci. 2009;32:413–34.
Kelly RM, Strick PL. Cerebellar loops with motor cortex and prefrontal cortex of a nonhuman primate. J Neurosci. 2003;23:8432–44.
Lord C, Rutter M, Goode S, Heemsbergen J, Jordan H, Mawhood L, et al. Autism Diagnostic Observation Schedule: a standardized observation of communicative and social behavior. J Autism Dev Disord. 1989;19:185–212.
Baron-Cohen S, Wheelwright S, Skinner R, Martin J, Clubley E. The Autism Spectrum Quotient (AQ). Evidence from Asperger syndrome/high functioning autism, males and females, scientists and mathematicians. J Autism Dev Disord. 2001;31:5–17.
Orsini A, Laicardi C, WAIS-R. Contributo alla taratura italiana. Firenze: Organizzazioni Speciali; 1997.
Norris DG. Reduced power multislice MDEFT imaging. J Magn Reson Imaging. 2000;11:445–51.
Diedrichsen J, Balsters JH, Flavell J, Cussans E, Ramnani N. A probabilistic atlas of the human cerebellum. Neuroimage. 2009;46:39–46.
Just MA, Keller TA, Malave VL, Kana RK, Varma S. Autism as a neural system disorder: a theory of frontal-posterior underconnectivity. Neurosci Biobehav Rev. 2012;36:1292–313.
Andreasen NC, Pierson R. The role of the cerebellum in schizophrenia. Biol Psychiatry. 2008;64:81–8.
Baillieux H, De Smet HJ, Paquier PF, De Deyn PP, Mariën P. Cerebellar neurocognition: insights into the bottom of the brain. Clin Neurol Neurosurg. 2008;110:763–73.
Stoodley CJ, Schmahmann JD. Evidence for topographic organization in the cerebellum of motor control versus cognitive and affective processing. Cortex. 2010;46:831–44.
Van Overwalle F, Baetens K, Mariën P, Vandekerckhove M. Social cognition and the cerebellum: a meta-analysis of over 350 fMRI studies. Neuroimage. 2014;86:554–72.
Clower DM, West RA, Lynch J, Strick PL. The inferior parietal lobule is the target of output from the superior colliculus, hippocampus and cerebellum. J Neurosci. 2001;21:6283–91.
Middleton FA, Strick PL. Cerebellar projections to the prefrontal cortex of the primate. J Neurosci. 2001;21:700–12.
Castelli F, Frith C, Happe F, Frith U. Autism, Asperger syndrome and brain mechanisms for the attribution of mental states to animated shapes. Brain. 2002;125:1839–49.
Raichle EM, MacLeod AM, Snyder AZ, Powers WJ, Gusnard DA, Shulman GL. A default mode of brain function. Proc Natl Acad Sci U S A. 2001;98:676–82.
Schilbach L, Eickhoff SB, Rotarska-Jagiela A, Fink GR, Vogeley K. Minds at rest? Social cognition as the default mode of cognizing and its putative relationship to the default system of the brain. Conscious Cogn. 2008;17:457–67.
Laird AR, Fox PM, Eickhoff SB, Turner JA, Ray KL, McKay DR, et al. Behavioral interpretations of intrinsic connectivity networks. J Cogn Neurosci. 2011;23:4022–37.
Krienen FM, Buckner RL. Segregated fronto-cerebellar circuits revealed by intrinsic functional connectivity. Cereb Cortex. 2009;19:2485–97.
O’Reilly JX, Beckmann CF, Tomassini V, Ramnani N, Johansen-Berg H. Distinct and overlapping functional zones in the cerebellum defined by resting state functional connectivity. Cereb Cortex. 2010;20:953–65.
Halko MA, Farzan F, Eldaief MC, Schmahmann JD, Pascual-Leone A. Intermittent theta-burst stimulation of the lateral cerebellum increases functional connectivity of the default mode network. J Neurosci. 2014;34:12049–56.
Cherkassky VL, Kana RK, Keller TA, Just MA. Functional connectivity in a baseline resting-state network in autism. Neuroreport. 2006;17:1687–90.
Kennedy DP, Redcay E, Courchesne E. Failing to deactivate: resting functional abnormalities in autism. Proc Natl Acad Sci U S A. 2006;103:8275–80.
Assaf M, Jagannathan K, Calhoun VD, Miller L, Stevens MC, Sahl R, et al. Abnormal functional connectivity of default mode sub-networks in autism spectrum disorder patients. Neuroimage. 2010;53:247–56.
Monk CS, Weng SJ, Wiggins JL, Kurapati N, Louro HM, Carrasco M, et al. Neural circuitry of emotional face processing in autism spectrum disorders. J Psychiatry Neurosci. 2010;35:105–14.
Jung M, Kosaka H, Saito DN, Ishitobi M, Morita Y, Inohara K, et al. Default mode network in young male adults with autism spectrum disorder: relationship with autism spectrum traits. Mol Autism. 2014;5:35.
Brass M, Ruby P, Spengler S. Inhibition of imitative behaviour and social cognition. Philos Trans R Soc Lond B Biol Sci. 2009;364:2359–67.
Mar RA. The neural bases of social cognition and story comprehension. Annu Rev Psychol. 2011;62:103–34.
Mars RB, Sallet J, Schüffelgen U, Jbabdi S, Toni I, Rushworth MF. Connectivity-based subdivisions of the human right “temporoparietal junction area”: evidence for different areas participating in different cortical networks. Cereb Cortex. 2012;22:1894–903.
Bzdok D, Langner R, Schilbach L, Jakobs O, Roski C, Caspers S, et al. Characterization of the temporo-parietal junction by combining data-driven parcellation, complementary connectivity analyses, and functional decoding. Neuroimage. 2013;81:381–92.
Decety J, Lamm C. The role of the right temporoparietal junction in social interaction: how low-level computational processes contribute to meta-cognition. Neuroscientist. 2007;13:580–93.
Corbetta M, Patel G, Shulman GL. The reorienting system of the human brain: from environment to theory of mind. Neuron. 2008;58:306–24.
Perner J, Aichhorn M, Kronbichler M, Staffen W, Ladurner G. Thinking of mental and other representations: the roles of left and right temporo-parietal junction. Soc Neurosci. 2006;1:245–58.
Saxe R. Uniquely human social cognition. Curr Opin Neurobiol. 2006;16:235–9.
Saxe R, Powell JT. It’s the thought that counts: specific brain regions for one component of theory of mind. Psychol Sci. 2006;17:692–9.
Sommer M, Dohnel K, Sodian B, Meinhardt J, Thoermer C, Hajak G. Neural correlates of true and false belief reasoning. Neuroimage. 2007;35:1378–84.
Aichhorn M, Perner J, Weiss B, Kronbichler M, Staffen W, Ladurner G. Temporo-parietal junction activity in theory of mind tasks: falseness, beliefs, or attention. J Cogn Neurosci. 2009;21:1179–92.
Vogt BA. Pain and emotion interactions in subregions of the cingulate gyrus. Nat Rev Neurosci. 2005;6:533–44.
Craig AD. How do you feel--now? The anterior insula and human awareness. Nat Rev Neurosci. 2009;10:59–70.
Lamm C, Decety J, Singer T. Meta-analytic evidence for common and distinct neural networks associated with directly experienced pain and empathy for pain. Neuroimage. 2011;54:2492–502.
Atique B, Erb M, Gharabaghi A, Grodd W, Anders S. Task-specific activity and connectivity within the mentalizing network during emotion and intention mentalizing. Neuroimage. 2011;55:1899–911.
Wang SS, Ad K, Badura A. The cerebellum, sensitive period and autism. Neuron. 2014;83:518–32.
Stoodley CJ. Distinct regions of the cerebellum show gray matter decreases in autism, ADHD, and developmental dyslexia. Front Syst Neurosci. 2014;8:1–17.
Palmen SJ, van Engeland H, Hof PR, Schmitz C. Neuropathological findings in autism. Brain. 2004;127:2572–83.
Rogers TD, McKimm E, Dickson PE, Goldowitz D, Blaha DA, Mittleman G. Is autism a disease of the cerebellum? An integration of clinical and pre-clinical research. Front Syst Neurosci. 2013;7:15.
Khan AJ, Nair A, Keown CL, Dakto MC, Lincoln AJ, Muller RA. Cerebro-cerebellar Resting state Functional Connectivity in Children and adolescents with Autism Spectrum Disorder. Biol Psychiatry. 2015;78:625–34.
Van Overwalle F, Mariën P. Functional connectivity between the cerebellum and cerebrum in social cognition: a multi-study analysis. Neuroimage. 2016;124:248–55.
Van Overwalle F, Baetens K, Mariën P, Vandekerckhove M. Cerebellar areas dedicated to social cognition? A comparison of meta-analytic and connectivity results. Soc Neurosci. 2015;10:337–44.
Schmahmann JD, Pandya DN. The cerebrocerebellar system. Int Rev Neurobiol. 1997;41:31–60.
Strick PL. How do the basal ganglia and cerebellum gain access to the cortical motor areas? Behav Brain Res. 1985;18:107–23.
Satterhwaite TD, Wolf DH, Ruparel K, Erus G, Elliott MA, Eickhoff SB, et al. Heterogeneous impact of motion on fundamental patterns of developmental changes in functional connectivity during youth. Neuroimage. 2013;83:45–57.
Griffanti L, Salimi-Khorshidi G, Beckman CF, Auerbach EJ, Douaud G, Sexton CE, et al. ICA-based artifact removal and accelerated fMRI acquisition for improved resting state network imaging. Neuroimage. 2014;95:232–47.
Fombonne E. Epidemiology of autistic disorder and other pervasive developmental disorders. J Clin Psychiatry. 2005;10:3–8.
Lai MC, Lombardo MV, Auyeung B, Chakrabarti B, Baron-Cohen S. Sex/gender differences and autism: setting the scene for future research. J Am Acad Child Adolesc Psychiatry. 2015;54:11–24.
Begeer S, Mandell D, Wijnker-Holmes B. Sex differences in the timing of identification among children and adults with autism spectrum disorders. J Autism Dev Disord. 2013;43:1151–6.
Giarelli E, Wiggins LD, Rice CE. Sex differences in the evaluation and diagnosis of autism spectrum disorders among children. Disabil Health J. 2010;3:107–16.
Lai MC, Lombardo MV, Pasco G, Ruigrok AN, Wheelwright SJ, Sadek SA, et al. A behavioral comparison of male and female adults with high functioning autism spectrum conditions. PLoS One. 2011;6(6):e20835. doi:10.1371/journal.pone.0020835.
Hofvander B, Delorme R, Chaste P. Psychiatric and psychosocial problems in adults with normal-intelligence autism spectrum disorders. BMC Psychiatry. 2009;9:35.
Lugnegård T, Hallerback MU, Gillberg C. Psychiatric comorbidity in young adults with a clinical diagnosis of Asperger syndrome. Res Dev Disabil. 2011;32:1910–7.
Acknowledgments
Special thanks to the subjects who were involved in this study. The authors also thank Gruppo Asperger onlus, Spazio Asperger onlus, CulturAutismo onlus, and Cooperativa Giuseppe Garibaldi for invaluable assistance, providing supports for subjects’ recruitment.
Funding
This work was supported by the Ministry of Education, Universities, and Research (MIUR) (Grant Number C26A1329AR).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Olivito, G., Clausi, S., Laghi, F. et al. Resting-State Functional Connectivity Changes Between Dentate Nucleus and Cortical Social Brain Regions in Autism Spectrum Disorders. Cerebellum 16, 283–292 (2017). https://doi.org/10.1007/s12311-016-0795-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-016-0795-8