Abstract
Background
Researches on the results of surgical treatment of thoracolumbar spine fractures are infrequent. The aim of this study was to determine midterm outcomes of surgical treatment of these fractures in a prospective survey.
Methods
A case series study on pediatric patients with the diagnosis of thoracic and/or lumbar vertebral fractures was conducted over a ten-year period. Surgically treated patients were evaluated in the follow-up period, based on back pain, independent function, neurological status, and radiographic indices.
Results
There were 102 pediatric individuals, 61 boys and 41 girls, aged 3–17 years (mean 12 years of age) with thoracic and/or lumbar spinal fractures. Motor vehicle accident was the most common mechanism of injury (45.0 %). L1 was the most frequent level of fractured vertebra (24.4 %), and pelvic fracture was the most common associated orthopedic injury (21.5 %). Totally, 20 patients underwent surgery, but only fifteen (14 boys and one girl) participated in follow-up (mean 49 months; range 12–81 months). Posterior spinal fusion and instrumentation was accomplished in 12 cases. Three patients were operated by anterior approach and fusion followed by posterior fusion and instrumentation because of delay in diagnosis. There were no major perioperative complications. Two cauda equina syndromes and two incomplete spinal cord injuries improved back to normal. Five cases (33.3 %) reported occasional back pain, and all patients were functionally independent. Radiographic indices improved significantly.
Conclusions
Spinal fusion and instrumentation in pediatric patients with unstable thoracolumbar vertebral fractures with or without spinal cord injuries have favorable radiographic and functional outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vertebral fractures in children are relatively uncommon and represent 1–3.6 % of all pediatric skeletal injuries [24, 33]. Most of these injuries in children with less than 8 years of age involve cervical spine, while the thoracic and lumbar areas are affected most often in older children and adolescents [1, 9, 16, 28]. Spinal injury in children is a separate entity from adult fractures due to the differences in anatomical and biomechanical features, such as ligamentous laxity, incomplete ossification, the head size relative to the body, and intrinsic elasticity of the spine [24]. These injuries have a substantial potential for recovery in pediatric population [9]. Among all orthopedic injuries in children, the mortality rate is highest in patients with thoracolumbar fractures [19], largely because of high rate of associated brain, thoracic, and abdominal injuries [2, 8, 24] and the usual delay in diagnosis that is reported in up to 50 % of cases [30].
Despite many articles on the frequency and pattern of pediatric vertebral fractures in the literature, limited investigations have focused on surgical results of these injuries. We carried out a prospective study during 10 years with emphasis on midterm outcomes of surgical treatment of thoracolumbar spine fractures in children.
Materials and methods
All patients with thoracolumbar spine fracture aged 17 years and younger who referred to senior authors between April 1999 and April 2009 were included in this study. Complete demographic features of patients, such as age, sex, time of injury, and mechanism of injury, were obtained. Plain anteroposterior and lateral radiographs and CT scan of the spine were taken. Magnetic resonance imaging (MRI) was obtained in patients who were treated by surgery. We evaluated the level and configuration of spinal injury, pattern and frequency of neurological compromise, associated injuries, and radiographic indices, including Denis classification of spinal fractures, kyphosis angle, collapse percentage, and canal compromise of all patients.
Of the 102 patients with thoracolumbar fractures, twenty underwent surgery. Indications for surgery included unstable three-column fractures, fracture dislocations, fractures with more than 20° kyphosis, canal compromise of more than 50 %, or neurological injuries. All patients were operated through posterior approach with posterior instrumentation to reduce the fracture with ligamentotaxis [22] except three cases with a delay in diagnosis that were operated through anterior approach followed by posterior instrumentation and fusion. Operation time, blood loss, perioperative complications, and construct configuration were recorded for these patients. Patients used thoracolumbosacral full-time orthosis for about three months after surgery.
Postoperatively, the patients had follow-up visits at 2, 12 weeks, 6, 12 months, and then annually. The collected data included back pain, level of function, neurologic status, sphincter control, and radiographic features. The pain was recorded using Dennis pain scale shown in Table 1 [10]. Level of function was evaluated using the 7-level functional independence measure (FIM) score designed to evaluate the level of assistance required by a person with the disability to perform basic life activities, with 1 indicating dependence and 7 indicating independence [13]. Neurological deficits and sphincter control were assessed according to the Frankel grade modified by Bradford and McBride as shown in Table 2 [4]. Sphincter evaluations were based on assessments such as voluntary voiding, rectal contraction, any catheterization to drain the bladder, and digital stimulation to trigger a bowel movement.
Results
Patients with thoracic and lumbar spinal injuries
Totally, there were 102 individuals, 61 boys and 41 girls, aged 3–17 years (mean age 12 years) with thoracic and/or lumbar vertebral fractures during the defined period of 10 years. The most common mechanism of injury was motor vehicle accident followed by fall from a height, assault trauma, bicycle accidents, and others including a patient crashed by collapsing wall and a case crashed after entrapment between tractor shank and its wheel (Table 3).
Among 127 fractures in 102 patients, L1 vertebra was the most common fractured level (Table 4). Most patients had only single fractured vertebra (83; 81.5 %). Among 19 cases with multilevel spinal injuries, eighteen had contiguous and one had noncontiguous spinal fracture pattern.
Twenty-eight cases (27.5 %) had associated injuries. Pelvic fracture was the most common associated fractured bone (21.5 %) followed by ankle and calcaneus (Table 5). Two cases had intra-abdominal hemorrhage due to spleen rupture and liver laceration.
Patients with thoracic and lumbar spinal surgeries:
A cohort of 15 (14 boys and one girl—mean age 14 years; range 10–17 years) cases out of 20 accepted to participate in the follow-up examinations (mean 49 months; range 12–81 months) (Table 6). Motor vehicle accident (reported in 10 cases) was the most common mechanism of injury.
Follow-up results
Mean values of radiographic indices of patients undergoing surgery are shown in Table 7. There was a 26.7 % incidence of neurological deficit (4 cases) in these patients. One was a 16-year-old boy with burst fracture of L3 and 80 % canal compromise leading to cauda equina syndrome. He had no sensation, motor function, and sphincter control below the injury level (Frankel grade A). Bladder function recovered 6 weeks after operation. Sensory and motor functions partially improved after 8 months. Another patient was a 12-year-old boy with severe paraplegia without sensory loss following T6–T7 burst fracture with 60 % canal compromise. He recovered 4 months after surgery with normal muscle power. Two other patients were graded as Frankel D1 and Frankel D2. Normal function returned after about 2 and 4 weeks, respectively.
Of 15 cases underwent surgery, ten patients (66.6 %) had no back pain in the follow-up visits as evaluated by Dennis pain scale. Three cases had occasional minimal back pain without any analgesic use (P2). Two patients with moderate back pain (P3) used analgesic occasionally. It was notable that all cases (100 %) were totally independent according to FIM score.
There was no perioperative complication except a wound infection treated by intravenous antibiotics. Also, there were no late complications such as pseudoarthrosis or broken device.
Three patients with delayed diagnosis should be reported separately as follows:
Case 1
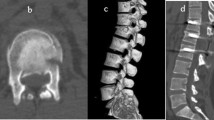
A 15-year-old boy was referred with low back pain about 2 months after bicycle–car accident. On examination, kyphotic deformity was obvious without any neurologic deficit. Spinal injury had been missed on initial evaluation (Fig. 1a). Severe flexion–distraction injury of T10–T11 was obvious on X-rays (Fig. 1b, c) and MRI (Fig. 1d) taken on arrival to our hospital. The patient was treated by anterior spinal release and fusion followed by posterior spinal fusion and instrumentation. Solid fusion without any complication was seen about 3 years after surgery (Fig. 1e, f).
Case 2
A 12-year-old boy, entrapped between tractor wheel and its shank, referred 6 months after injury with nonsurgically treated pelvic fracture and palpable deformity at thoracolumbar junction. Neurological examination was normal. Radiographs showed flexion–distraction injury of T11–T12 (Fig. 2a, b). Surgery was planned in two stages due to rigidity of the deformity. T12 partial corpectomy, T11–T12, T12–L1, L1–L2 discectomy, and rib strut grafting were performed through anterior approach (Fig. 2c) followed by posterior spinal fusion and instrumentation 1 week later. After 5-year follow-up, the patient had normal neurological examination and solid spinal fusion without any complication (Fig. 2d, e).
Case 3
A 10-year-old boy referred 2 months after car pedestrian accident with low back pain. He also had associated femoral shaft fracture. On arrival, his neurological examination was normal. X-rays (Fig. 3a, b) revealed T12–L1 flexion–distraction injury. Anterior release, discectomy, and grafting were performed followed by posterior spinal fusion and instrumentation 1 week later. Follow-up radiographs (Fig. 3c, d) showed acceptable alignment and solid fusion 2 years after operation.
Discussion
Not only pediatric thoracolumbar spinal injuries are generally considered to be rare, but also they may be missed or diagnosis may be delayed. Thoracic and lumbar spine injuries become more common with age in children [3, 9, 23]. Likewise, about 96 % of cases in the current study had an age of more than 10 years. Motor vehicle accident was the leading cause of thoracolumbar spine fractures (45.0 %). It is similar to other studies [21, 25, 29]; however, some researchers have reported sports-related injuries [18] or falls from a height [20, 34] as the most frequent mechanism of injury.
Thoracolumbar junction is the most common injured site in pediatric population [12]. The most common fractured vertebra in our series was L1 (31 cases) with more than 50 % of fractures occurred between T12 and L2. We found that fractures of lumbar spine were more common than thoracic spine (82 vs. 45). Similar finding was reported by other authors such as Rumball and Jarvis [30], Turgut et al. [34], Cirak et al. [8], and Dogan et al. [9]. Nonetheless, some authors reported the opposite. Reddy et al. [29] described the thoracic region (T2–T10) as the most commonly injured area, accounting for 28.7 % of fractures, followed by the lumbar region (L2–L5). According to the study of Parente et al. [25], T4–T8 (38.5 %) and T11–L2 (31.5 %) are the most frequent sites. Moreover, vertebral fractures in children most often appeared in the midthoracic region (47 %) in the study done by Kraus et al. [18].
Thoracolumbar injuries in children often present with multiple levels of fractures [1], particularly in smaller children [33]. Incidence of multilevel spinal injury ranges from 6 to 52 % [21, 24, 26, 33]. The result of our study was also in this range (18.5 %). Only one case in nineteen (5.26 %) had noncontiguous spinal injury. Noncontiguous injury is defined as spine injuries at more than one level separated by a region of normal spine [5]. Patients with noncontiguous multilevel spinal injuries are more likely to experience neurological injuries and are usually missed on initial examination [11]. Neurological injuries have been reported in 11.8–37.5 % of multilevel thoracolumbar fractures [11, 24].
Associated injures have been reported in over 65 % of children with spinal fractures [19] with traumatic brain injury being the most common associated injury [8, 24]. While we excluded major multiply injured patients from the survey, pelvic and acetabular fractures were the most frequent fractured bone associated with thoracolumbar spinal injuries in children. Two patients had intra-abdominal hemorrhage from liver and spleen lacerations.
About 7.5–30 % of patients with thoracolumbar fractures need operative treatment [9, 18, 21, 24, 28]. About 20 % of patients in the current study underwent surgery, whereas 82 cases received nonsurgical treatment. Although early surgical treatment is mandatory for unstable spinal injuries or fractures with myelopathy [26], we have treated three cases of delayed diagnosis with satisfactory follow-up results. Late diagnosis has been reported in up to 50 % of patients [30]. High index of suspicion is required for early diagnosis of spinal injuries in children. Furthermore, screening radiographs and MRI may be necessary in these patients because clinical examination alone identifies these injuries with a sensitively of 81–87 % and specificity of 68 % [17, 27, 31].
We also described some unusual cases of flexion–distraction injuries (type B in AO classification). The injury was posterior ligamentous disruption associated with transverse disruption through the disk. Flexion–distraction spinal injuries are among the most challenging topics to spine surgeons. Although these fractures have been linked to seat-belt injuries, it may occur in any deceleration injuries involving flexion force with the fulcrum anterior to middle column of the spine [32]. Bicycle crashes are the mechanism of injury in about 2 % of cases with these fractures [2]. The mechanism of injury in all three reported cases in our series was severe flexion of the spine after different types of accidents. MRI findings are the most relevant modality to differentiate between spinal pathologies not only in adults [7] but also in children with flexion–distraction injuries [12]. We recommend this modality for early diagnosis of flexion–distraction injuries particularly in patients with unusual mechanisms of injury.
Outcome of thoracolumbar spinal injuries in children depends predominantly on the severity of spinal cord injury and associated neurological deficits [14, 34]. Spinal cord injury has been reported in 15–45 % of cases [9, 14, 28, 33, 35]. Neurological deficit is related to the level of injury and the degree of canal compromise. Although patients with complete spinal cord injury have a poor prognosis for functional recovery, the children with cauda equine injury in our series had near-complete improvement after several months.
The safety and efficacy of spinal surgery in pediatric patients has been well established [15, 26]. There was no complication in 13 and 23 cases that underwent surgery by Santiago et al. [31] and Dogan et al. [9], respectively. We also had no major complication except a wound infection treated by intravenous antibiotics.
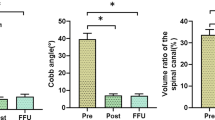
Kyphosis angle improved from 26.5° at presentation to 12.5° at final follow-up. This amount of correction is more than what explained by Vander Have et al. [35]. Even though all radiographic indices deteriorated during the follow-up period, it was small and generally insignificant.
While Moller et al. [23] reported occasional back pain in five out of 23 cases (21.7 %) during a long-term follow-up, we only had five cases (33.3 %) with some degrees of occasional back pain without any interruption of daily activities. Further investigation is necessary to clarify the incidence of chronic axial back pain in pediatric patients with spine fractures.
All patients were functionally independent with FIM score of 7, which is better than the report by Carreon et al. [6]. It seems that spinal fusion and instrumentation in pediatric spine fracture is highly successful in terms of functional outcome even in patients with spinal cord injury.
Conclusion
Although relatively rare, pediatric thoracolumbar spine fracture is an important diagnosis not to miss. Early diagnosis and treatment is critical, and a high index of clinical suspicion is essential in these patients. Spinal fusion and instrumentation of children with unstable thoracolumbar fractures with or without spinal cord injury has favorable radiographic and functional outcomes.
References
Basu S (2012) Spinal injuries in children. Front Neurol 3:96
Bernstein MP, Mirvis SE, Shanmuganathan K (2006) Chance-type fractures of the thoracolumbar spine: imaging analysis in 53 patients. AJR Am J Roentgenol 187:859–868
Bilston LE, Brown J (2007) Pediatric spinal injury type and severity are age and mechanism dependent. Spine (Phila Pa 1976) 32:2339–2347
Bradford DS, McBride GG (1987) Surgical management of thoracolumbar spine fractures with incomplete neurologic deficits. Clin Orthop Relat Res 218:201–216
Calenoff L, Chessare JW, Rogers LF, Toerge J, Rosen JS (1978) Multiple level spinal injuries: importance of early recognition. AJR Am J Roentgenol 130:665–669
Carreon LY, Glassman SD, Campbell MJ (2004) Pediatric spine fractures: a review of 137 hospital admissions. J Spinal Disord Tech 17:477–482
Cicala D, Briganti F, Casale L, Rossi C, Cagini L, Cesarano E, Brunese L, Giganti M (2013) Atraumatic vertebral compression fractures: differential diagnosis between benign osteoporotic and malignant fractures by MRI. Musculoskelet Surg 97(Suppl 2):S169–S179
Cirak B, Ziegfeld S, Knight VM, Chang D, Avellino AM, Paidas CN (2004) Spinal injuries in children. J Pediatr Surg 39:607–612
Dogan S, Safavi-Abbasi S, Theodore N, Chang SW, Horn EM, Mariwalla NR, Rekate HL, Sonntag VK (2007) Thoracolumbar and sacral spinal injuries in children and adolescents: a review of 89 cases. J Neurosurg 106:426–433
Farcy JP, Weidenbaum M, Glassman SD (1990) Sagittal index in management of thoracolumbar burst fractures. Spine (Phila Pa 1976) 15:958–965
Firth GB, Kingwell SP, Moroz PJ (2012) Pediatric noncontiguous spinal injuries: the 15-year experience at 1 pediatric trauma center. Spine (Phila Pa 1976) 37:E599–E608
Groves CJ, Cassar-Pullicino VN, Tins BJ, Tyrrell PN, McCall IW (2005) Chance-type flexion-distraction injuries in the thoracolumbar spine: MR imaging characteristics. Radiology 236:601–608
Hamilton BB, Laughlin JA, Fiedler RC, Granger CV (1994) Interrater reliability of the 7-level functional independence measure (FIM). Scand J Rehabil Med 26:115–119
Hamilton MG, Myles ST (1992) Pediatric spinal injury: review of 174 hospital admissions. J Neurosurg 77:700–704
Hedequist DJ, Hall JE, Emans JB (2004) The safety and efficacy of spinal instrumentation in children with congenital spine deformities. Spine (Phila Pa 1976) 29:2081–2086
Hofbauer M, Jaindl M, Höchtl LL, Ostermann RC, Kdolsky R, Aldrian S (2012) Spine injuries in polytraumatized pediatric patients: characteristics and experience from a Level I trauma center over two decades. J Trauma Acute Care Surg 73:156–161
Junkins EP Jr, Stotts A, Santiago R, Guenther E (2008) The clinical presentation of pediatric thoracolumbar fractures: a prospective study. J Trauma 65:1066–1071
Kraus R, Stahl JP, Heiss C, Horas U, Dongowski N, Schnettler R (2013) Fractures of the thoracic and lumbar spine in children and adolescents. Unfallchirurg 116:435–441
Leonard M, Sproule J, McCormack D (2007) Paediatric spinal trauma and associated injuries. Injury 38:188–193
Leucht P, Fischer K, Muhr G, Mueller EJ (2009) Epidemiology of traumatic spine fractures. Injury 40:166–172
Mahan ST, Mooney DP, Karlin LI, Hresko MT (2009) Multiple level injuries in pediatric spinal trauma. J Trauma 67:537–542
Mohanty SP, Bhat SN, Ishwara-Keerthi C (2011) The effect of posterior instrumentation of the spine on canal dimensions and neurological recovery in thoracolumbar and lumbar burst fractures. Musculoskelet Surg 95:101–106
Moller A, Hasserius R, Besjakov J, Ohlin A, Karlsson M (2006) Vertebral fractures in late adolescence: a 27 to 47-year follow-up. Eur Spine J 15:1247–1254
Mortazavi MM, Dogan S, Civelek E, Tubbs RS, Theodore N, Rekate HL, Sonntag VK (2011) Pediatric multilevel spine injuries: an institutional experience. Childs Nerv Syst 27:1095–1100
Parente A, Navascués JA, Hernández E, Sánchez-París O, Cañizo A, Cerdá J, Molina E, De Tomás E, De Agustín JC, Matute JA, Vázquez J (2005) Spinal cord and vertebral column injuries in children. Cir Pediatr 18:132–135
Parisini P, Di Silvestre M, Greggi T (2002) Treatment of spinal fractures in children and adolescents: long-term results in 44 patients. Spine (Phila Pa 1976) 27:1989–1994
Papavasiliou A, Stanton J, Sinha P, Forder J, Skyrme A (2007) The complexity of seat belt injuries including spinal injury in the pediatric population: a case report of a 6-year-old boy and the literature review. Eur J Emerg Med 14:180–183
Puisto V, Kääriäinen S, Impinen A, Parkkila T, Vartiainen E, Jalanko T, Pakarinen MP, Helenius I (2010) Incidence of spinal and spinal cord injuries and their surgical treatment in children and adolescents: a population-based study. Spine (Phila Pa 1976) 35:104–107
Reddy SP, Junewick JJ, Backstrom JW (2003) Distribution of spinal fractures in children: does age, mechanism of injury, or gender play a significant role? Pediatr Radiol 33:776–781
Rumball K, Jarvis J (1992) Seat-belt injuries of the spine in young children. J Bone Joint Surg Br 74:571–574
Santiago R, Guenther E, Carroll K, Junkins EP Jr (2006) The clinical presentation of pediatric thoracolumbar fractures. J Trauma 60:187–192
Strømsøe K, Magnaes B, Nakstad P (2000) Open reduction and internal fixation in flexion-distraction injuries to the lower spine in children and adolescents involved in traffic accidents as car occupants. A report and literature review. Arch Orthop Trauma Surg 120:96–99
Stulík J, Pesl T, Kryl J, Vyskocil T, Sebesta P, Havránek P (2006) Spinal injuries in children and adolescents. Acta Chir Orthop Traumatol Cech 73:313–320
Turgut M, Akpinar G, Akalan N, Ozcan OE (1996) Spinal injuries in the pediatric age group: a review of 82 cases of spinal cord and vertebral column injuries. Eur Spine J 5:148–152
Vander Have KL, Caird MS, Gross S, Farley FA, Graziano GA, Stauff M, Segal LS (2009) Burst fractures of the thoracic and lumbar spine in children and adolescents. J Pediatr Orthop 29:713–719
Acknowledgments
This article has been extracted from a thesis submitted to Shiraz University of Medical Sciences in partial fulfillment of the requirement for the degree of specialty in orthopedic surgery. Source of funding is Bone and Joint Disease Research Center of Shiraz University of Medical Sciences.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was carried out in Bone and Joint Disease Research Center, Department of Orthopedic Surgery, Chamran Hospital, Shiraz University of Medical Sciences, Shiraz, Iran.
Rights and permissions
About this article
Cite this article
Erfani, M.A., Pourabbas, B., Nouraie, H. et al. Results of fusion and instrumentation of thoracic and lumbar vertebral fractures in children: a prospective ten-year study. Musculoskelet Surg 98, 107–114 (2014). https://doi.org/10.1007/s12306-014-0313-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-014-0313-4