Abstract
Background
Reversine, a small synthetic purine analogue, has been reported to be effective in tumor suppression. In the present study, we demonstrated an antitumor activity of reversine that could suppress cellular proliferation and induce cell cycle arrest and apoptosis in human breast cancer cell lines.
Methods
To evaluate whether reversine could suppress cell growth of MCF-7 and MDA-MB-231 cells and induce cell death, the cell viability, cell cycle, and apoptosis were determined in this study.
Results
Reversine treatment in human breast cancer cells reduced cell viability in a dose-dependent manner. Cell cycle accumulation at the G2/M phase in reversine-treated cells was also determined. Moreover, polyploidy was also found in reversine-treated cells. Apoptosis in reversine-treated cells was exhibited with PARP cleavage and caspase-3 and caspase-8 activation, but not caspase-9 activation, indicating that caspase-dependent apoptosis mediated by an extrinsic pathway took place in reversine-treated cells. Furthermore, reversine attenuated cell death in cells pretreated with a pan-caspase inhibitor before reversine treatment.
Conclusions
In the present study, we demonstrated that reversine contributes to growth inhibition in human breast cancer cells through cell cycle arrest, polyploidy, and/or apoptosis induction. The apoptosis mediated by reversine was induced by the mitochondria-independent pathway. Therefore, the potential role of reversine as a novel therapeutic agent for the treatment of breast cancer is worthy of further investigation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Breast cancer is the most common malignant tumor among women globally, and approximately 10 % of newly diagnosed breast cancer patients have locally advanced and/or metastatic disease. Among these patients, 20–85 % of those who are diagnosed with early breast cancer will later develop recurrent or metastatic disease [1]. Despite advances in the treatment of breast cancer, metastatic breast cancer remains aggressive and lethal in women, and the 5-year mortality rate is approximately 25 % [2]. This is due to the heterogeneity between human breast cancers and the multiple encompassing subgroups with various molecular signatures, prognoses, and responses to therapies [3]. Three major subtypes of human breast cancer have distinguishing features closely associated with subtypes defined by gene expression profiling, including distinct clinical outcomes, different responses to adjuvant therapy, and different patterns of metastatic recurrence [3–5].
Reversine, a 2,6-disubstituted purine, was identified as being able to induce dedifferentiation of murine myoblasts into multipotent progenitor cells [6]. Moreover, the role of reversine in regenerative medicine has been well recognized [6–10]. Cell differentiation is also speculated to be relevant to cancer therapy. Up to now, three reports have demonstrated the antitumor capabilities of reversine against myeloid leukemia, oral squamous cells, and multiple myeloma cells [11–13]. In a human myeloid leukemia study, reversine was demonstrated to suppress the colony formation of acute myeloid leukemia cells as well as VX-680, a potent inhibitor of Aurora kinases, but was less toxic [11]. Recently, reversine was found to inhibit multiple myeloma cells, using a tumor cell-specific in vitro bioluminescence imaging (CS-BLI) anticancer drug screening assay [12]. In that report, reversine was demonstrated to suppress the kinase activity of Aurora kinase A (Aur-A), Aurora kinase B (Aur-B), JAK2, and SRC [12]. Structurally, reversine is an ATP analogue and is suspected to inhibit multiple cellular enzymatic activities, possibly not limited to Aur. In addition, reversine was also found to suppress the proliferation of human oral squamous cells and human thyroid cancer cells and induce cell cycle arrest, apoptosis, and/or autophagy [13, 14]. Therefore, reversine could be a novel anticancer agent; however, the definite mechanisms of reversine with regard to its antitumor behavior have not yet been clearly elucidated.
MCF-7 and MDA-MB-231 cells were used in the present study. MCF-7 is an estrogen receptor positive and p53 wild-type cell line, and MDA-MB-231 is an estrogen receptor negative and p53 mutant cell line. In the present study, we demonstrated that reversine can be used as an anticancer agent against human breast cancer cells. We also showed that cell cycle arrest occurred and that caspase-dependent apoptosis is induced through activation of a mitochondria-independent pathway. Our data suggest that reversine is a potential chemotherapeutic agent that can be used against human breast cancer cells.
Materials and methods
Breast cancer cell lines and cell culture
The human breast cancer cell lines, MCF-7 and MDA-MB-231, were purchased from Bioresource Collection and Research Center (BCRC), Taiwan. The MCF-7 cells were maintained in RPMI medium (Gibco BRL, Grand Island, NY) supplemented with 10 % fetal bovine serum, 100 U/ml penicillin, and 0.1 μg/ml streptomycin in a 5 % CO2 humidified atmosphere at 37 °C. The MDA-MB-231 cells were maintained in DMEM medium (Gibco BRL, Grand Island, NY) supplemented with 10 % fetal bovine serum, 100 U/ml penicillin, and 0.1 μg/ml streptomycin in a humidified atmosphere at 37 °C with 5 % CO2.
Cell proliferation assay (MTT assay)
Reversine was purchased from Cayman Chemical (Ann Arbor, MI, USA). For the assay, 5 × 103 of MCF-7 and MDA-MB-231 cells/100 μl were plated into 96-well tissue culture plates and grown in the mentioned medium individually. After an overnight attachment, the cells were treated with medium only (containing 0.01 % DMSO) or medium containing reversine at 0.5, 1, 5, 10, 25, 50, and 100 μM. After incubation for 24, 48, and 72 h, cellular viability was determined by MTT assay. MTT labeling reagent was added to fresh medium and incubated cells for 4 h at room temperature. Absorbance was examined at 590 nm by use of a microplate reader. The final results were analyzed using statistical methods with three independent studies.
Cell cycle analysis
The MCF-7 and MDA-MB-231 cells were incubated with either DMSO 0.01 % or reversine at 1, 5 and 10 μM for 4, 8, 12, 16, 20, and 24 h. Cells were harvested and fixed in 70 % ethanol overnight. After double washing with PBS, cells were labeled with 500 μl PI staining buffer (Sigma, St. Louis, MO) and incubated at room temperature in the dark for 30 min. DNA content was analyzed using FACS Canto II (Becton–Dickinson, San Diego, CA) with WMDI 2.9 software.
Cell death analysis
After treatment, Annexin-V staining (Sigma, St. Louis, MO) was performed to detect apoptotic cells among the MCF-7 and MDA-MB-231 cells. The cells were washed with PBS twice and centrifuged at 1,500×g for 10 min. The cell pellets were resuspended in 100 μl of staining solution (2 μl Annexin-V-FITC and 2 μl PI in 100 μl binding buffer) and incubated for 15 min at room temperature in darkness. Annexin-V or PI fluorescent intensities were analyzed by FACScan (Becton–Dickinson, San Diego, CA), and 10,000 cells were evaluated in each sample.
Apoptotic mechanisms investigation
Flow cytometry data analysis led to the conclusion that apoptosis had occurred in MCF-7 and MDA-MB-231 cells after reversine treatment. Further apoptotic mechanisms were investigated by detecting activation of caspase-3, caspase-8, caspase-9, etc. using western blotting. Cells were cultured and treated with or without reversine, and the total cell extracts harvested at various time points were subjected to the sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE). The separated proteins in the gel were electrically transferred to a PVDF membrane (Millipore Corporation, Bedford, MA, USA), followed by hybridization with the specific primary antibodies, anti-caspase-3 Ab (Cell signaling, USA), anti-caspase-8 Ab (Cell signaling, USA), anti-caspase-9 Ab (Cell signaling, USA), anti-PARP (poly ADP-ribose polymerase) Ab (GeneTex, USA), anti-Bcl-x Ab (GeneTex, USA), anti-Bid Ab (GeneTex, USA), anti-GAPDH Ab (GeneTex, USA), and the secondary antibodies. After incubation with the enhanced chemiluminescence (ECL) solution (Millipore, Billerica, MA, USA) for 1 min, the membrane was exposed to an X-ray film (Eastman Kodak, NY, USA).
Statistical analysis
Data are presented as mean ± standard deviation for the indicated number of separate experiments. Statistical software (SPSS 16.0) was used, and the Mann–Whitney U test was performed for comparisons. Statistical significance was defined as a P value less than 0.05 in all tests.
Results
Reversine reduced the cellular viability of MCF-7 and MDA-MB-231 cell lines
The human breast cancer cells, MCF-7 and MDA-MB-231, were used to evaluate the growth inhibition effect of reversine treatment. The cellular numbers of MCF-7 and MDA-MB-231 were observed by microscopy after treatment with DMSO or reversine, and both decreased significantly in a time- and dosage-dependent manner during reversine treatment (data not shown). DMSO was used as a negative control. Furthermore, cellular viability was quantified by MTT analysis after reversine treatment, and was shown in a time- and dose-dependent manner after reversine treatment in both breast cancer cell lines (Fig. 1a, b). According to the MTT data, the GI50 of reversine in MCF-7 and MDA-MB-231 cells was 8 and 38 μM after treatment for 48 h, respectively (Fig. 1a, b). The MDA-MB-231 cells, a more aggressive human breast cancer cell line, showed more resistance to treatment with reversine than the MCF-7 cells (Fig. 1). These data demonstrated that reversine could reduce cell viability in human breast cancer cells. In addition, MCF-7 cells were more susceptible than MDA-MB-231 cells to reversine-mediated cell viability reduction (Fig. 1).
Reversine suppressed the growth of human breast cancer cells. The human breast cancer cells, a MCF-7 and b MDA-MB-231, were incubated with reversine with multiple dosages for 12, 24, 48, and 72 h, and the proliferation inhibitions were determined by MTT assay. The results of MTT assay are expressed as mean ± SEM of three independent experiments
Reversine-induced polyploidization and cell cycle arrest at the G2/M phase
The cells, both MCF-7 and MDA-MB-231, were observed to be bigger under microscopy analysis in the reversine-treated groups than in the control group after treatment for 48 and 72 h (Fig. 2a, c). Moreover, the cellular publication of G2/M (4 N; tetraploidization) was significantly elevated in both of the MCF-7 and MDA-MB-231 cells under flow cytometry analysis (Fig. 2b, d). In addition, cells with 8 N population were significantly present in the reversine-treated MCF-7 cells (Fig. 2b), and partially in the MDA-MB-231 cells (Fig. 2d). The polyploidy phenomenon was found in a time-dependent manner after reversine treatment, indicating the propensity for mitotic slippage and/or deficiency in the completion of mitosis as was reported in a previous study [15].
Polyploidy induced after reversine treatment in human breast cancer cells. Human breast cancer cells, (a, b) MCF-7 and (c, d) MDA-MB-231, were treated with reversine. The cellular morphology was determined under microscopy (a, c) and the polyploidy phenomena were analyzed with flow cytometry (b, d). The results were confirmed by three independent experiments and data from one of them are shown
The MCF-7 and MDA-MB-231 cell numbers were reduced after reversine treatment (Fig. 1). The reduction in cell numbers could be mediated by cell cycle arrest and/or cell death. We further examined whether cell cycle arrest was induced after reversine treatment. Flow cytometry was used to evaluate the cell cycle of MCF-7 and MDA-MB-231 cells after reversine treatment, and DMSO was used as the negative control. Figure 3 shows that the ratio of G0/G1 was decreased in reversine-treated MCF-7 and MDA-MB-231 cells, in a time- and dosage-dependent manner, and the ratio of G2/M during reversine treatment was elevated in both the MCF-7 and MDA-MB-231 cells, in a time- and dosage-dependent manner (Fig. 3). In addition, the sub-G1 phase was partially increased in the MCF-7 and MDA-MB-231 cells after reversine treatment for 24 h (Fig. 3). The sub-G1 phase was increased significantly after 48- and 72-h treatment with reversine in MCF-7 and MDA-MB-231 cells (data not shown). Taken together, these data demonstrated that reversine could induce polyploidization and cell cycle arrest at the G2/M phase in human breast cancer cells, especially in MCF-7 cells. Moreover, a sub-G1 group was found in reversine-treated MCF-7 and MDA-MB-231 cells, suggesting that apoptosis may be induced during reversine treatment. Our data demonstrated that reversine could suppress human breast cancer growth by cell cycle arrest induction and/or apoptosis.
Reversine induced cell cycle arrest at the G2/M phase and elevated sub-G1 group formation in human breast cancer cells. Cells were incubated with reversine at multiple dosages, and the DNA content of a MCF-7 and b MDA-MB-231 cells was determined by flow cytometry with propidium iodide labeling. The percentage of G0/G1, S, G2/M, and sub-G1 phase distribution of reversine-treated cells was measured by WMDI 2.9 software. Three independent experiments provided confirmation and data from one of them are shown
Reversine-induced apoptosis in human breast cancer cells
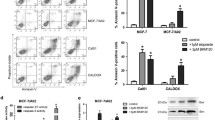
Reversine treatment could induce cell cycle arrest; moreover, sub-G1 was also found in the reversine-treated MCF-7 and MDA-MB-231 cells (Fig. 3). This suggested that apoptosis may occur in human breast cancer cells during reversine treatment. To confirm the apoptosis induction by reversine, MCF-7 and MDA-MB-231 cells were incubated with reversine, and the apoptosis analysis was determined with PI and Annexin-V double staining by flow cytometry. Apoptosis was found significantly in a time-dependent manner in MCF-7 cells, and in a time- and dosage-dependent manner in MDA-MB-231 cells (Fig. 4). The levels of apoptosis were greater in MDA-MB-231 cells than in MCF-7 cells (under 24- and 48-h treatment; Fig. 4). MDA-MB-231 cells were more susceptible to reversine-induced apoptosis. This finding demonstrated that reversine could induce apoptosis in human breast cancer cells.
Reversine elicited apoptosis in human breast cancer cells. Cells were incubated with reversine in multiple dosages, and the apoptotic (a, b) MCF-7 and (c, d) MDA-MB-231 cells were evaluated by flow cytometry with PI/Annexin-V double staining. DMSO was used as the solvent and as a negative control. Three independent experiments provided confirmation; the results were expressed as mean ± SEM, and apoptosis (early + late) is shown in b and d. *P < 0.05; **P < 0.01; ***P < 0.001
Reversine-induced mitochondria-independent apoptosis in human breast cancer cells
Apoptosis was demonstrated by flow cytometry in reversine-treated MCF-7 and MDA-MB-231 cells (Fig. 4). To further investigate the mechanisms involved in reversine-mediated apoptosis in these cells, western blotting was used and caspase-3, -8, and -9 were determined after reversine treatment in MDA-MB-231 cells (Fig. 5). The pro-caspase-8 was significantly decreased at 24 h post-treatment with reversine (5 and 10 μM), and the cleavage form of caspase-8 was found after 72-h treatment (Fig. 5). The pro-caspase-3 was significantly reduced at 48 and 72 h in the reversine-treated groups. However, the active form of caspase-9 was not found after reversine treatment (data not shown), and the expression levels of pro-caspase-9 had no influence in either the reversine-treated or control groups (Fig. 5). This finding was also demonstrated in the reversine-treated MCF-7 cells (data not shown). These data suggested that the mitochondria-independent apoptotic pathway (intrinsic pathway) may not be involved in reversine-mediated cellular apoptosis. To further confirm the hypothesis, the expressions of Bcl-x and Bid were evaluated by western blotting. The expression levels of Bcl-xL and Bid in reversine-incubated groups, as well as the control group, showed no significant difference (Fig. 5). Moreover, the apoptotic isoforms of Bcl-xS and tBid were not detected in reversine-treated MDA-MB-231 cells. These data suggested that reversine could induce apoptosis in human breast cancer cells through an extrinsic pathway. In addition, to determine whether apoptosis had indeed occurred in the reversine-treated groups, PARP was detected by western blotting. The expressions of PARP were decreased significantly after treatment with reversine for 48 and 72 h (Fig. 5). The timing of the PARP decrease was equivalent to the reduction of pro-caspase-3, suggesting that caspase-dependent apoptosis occurred during reversine treatment (Fig. 5).
Reversine induced caspase-dependent apoptosis, and apoptosis occurred through an extrinsic pathway in MDA-MB-231 cells. Cells were incubated with reversine at multiple dosages, and caspase-3, -8, and -9 were detected by western blotting. PARP, used as a marker of apoptosis, was also determined. In addition, the Bid and Bcl-xL were further detected to demonstrate the existence of the extrinsic apoptosis pathway
In addition, to further evaluate whether the caspase-dependent apoptosis induced by reversine could suppress the growth of human breast cancer cells, a pan-caspase inhibitor, Z-VAD-FMK, was used to block the activation of caspase. The cell number of the MDA-MB-231 cells was significantly reduced after reversine treatment (comparing with the non-treated group; Fig. 6b, panel C), and could be restored partially after Z-VAD-FMK treatment (Fig. 6b, panel D). However, cells treated with Z-VAD-FMK only showed no significant difference in cell numbers (Fig. 6b, panel B). Altogether, we demonstrated that reversine could induce cellular apoptosis through an extrinsic pathway and further reduce human breast cancer growth.
Reversine-mediated apoptosis reduced the cell number of human breast cancer cells. To evaluate whether growth inhibition was mediated by reversine-induced apoptosis, a pan-caspase inhibitor (Z-VAD-FMK) was used to block the activation of the caspases, and caspase-8 and -3 were determined after treatment for 24 h. After 2 h pretreatment with or without Z-VAD-FMK, MDA-MB-231 cells were incubated with or without reversine (10 μM) for 24 h, a caspase inhibition was determined by western blotting. The GAPDH in the western blot was used as the internal control. b The cellular phenomena were determined by microscopy. A mock treated cells. B Z-VAD-FMK (20 μM) treated cells. C reversine (10 μM) treated cells. D cells treated with reversine (10 μM) and Z-VAD-FMK (20 μM)
Discussion
In the present study, we demonstrated an antitumor activity of reversine in human breast cancer cells (Fig. 1). Of the two cell types, MCF-7 cells were more susceptible to growth inhibition by reversine (Fig. 1). Moreover, the cell cycle arrest at the G2/M phase was found in both MCF-7 and MDA-MB-231 cells (Fig. 3). However, MCF-7 showed polyploidy induction significantly more than MDA-MB-231 cells during reversine treatment (Fig. 2). These findings were consistent with the observations in HeLa, CWR22Rv1, DU-145, and PC-3 cells after reversine treatment [15, 16]. In addition, apoptosis was induced significantly in both MDA-MB-231 and MCF-7 cells (Fig. 4), and the apoptosis levels in reversine-treated MDA-MB-231 cells were elevated 10 to 20 % compared to MCE-7 cells (Fig. 4b, d). Altogether, the growth inhibition in reversine-treated MCF-7 was mediated by cell cycle arrest, polyploidy, and apoptosis, and cell cycle arrest and apoptosis occurred in MDA-MB-231 cells.
The Aurora kinases, a family of serine/threonine kinase, are composed of Aurora-A (Aur-A), Aurora-B (Aur-B), and Aurora-C (Aur-C) in mammalian cells, and are the key regulators of mitosis [17]. Amplification and overexpression of Aur-A and/or Aur-B have been reported in different tumors, including breast, colon, pancreatic, ovarian, gastric, prostate, thyroid, glioblastoma, and non-small cell lung cancer, and are associated with tumor grade and prognosis [18–29]. Owing to the strong association of Aur-A and/or Aur-B with human malignancies, identifying and developing Aurora kinase inhibitors for the treatment of human cancers have been the subject of investigation in many reports [30–32]. Reversine has reported to be an Aurora kinase inhibitor [11]. In the present study, we demonstrated that reversine mediated cell cycle arrest at the G2/M phase and polyploid formation in human breast cancer cells (Figs. 2, 3). Therefore, whether reversine can suppress human breast cancer cell growth through inhibition of Aur kinases and/or other factors should be further investigated.
In addition, reversine has also been shown to suppress enzymes, such as JAK2, SRC, and Akt, involved in cell growth or metastasis signaling pathways [6, 12]. The overexpression and/or activation of the JAK2, SRC, and Akt pathways may contribute to tumor growth, metastasis, and/or invasion in human breast cancers [33, 34]. Inhibition of src by siRNA has been reported to suppress the tumor growth and metastasis of human breast cancer cells [35]. Clinical trials have reported that dasatinib, an inhibitor of multiple oncogenic tyrosine kinases, including src, has limited single-agent activity in unselected patients with triple-negative breast cancer [36]. In addition, the aberrant activation of the JAK2/STAT pathway has been reported to be associated with breast cancer formation [37–39]. Inhibition of the JAK2/STAT pathway demonstrated antitumor activity through growth inhibition and/or apoptosis [40]. Therefore, whether reversine can suppress human breast tumor growth and induce cancer death through the inhibition of these pathways should be further investigated.
The GI50 of the MCF-7 and MDA-MB-231 cells was 8 and 38 μM after 48-h treatment with reversine, showing that MCF-7 cells were more susceptible than MDA-MB-231 cells (Fig. 1). This finding may cast light on the cell cycle arrest, polyploidy formation, and apoptosis induction in MCF-7 cells during reversine treatment. However, only cell cycle arrest and apoptosis were found in reversine-treated MDA-MB-231 cells. Nevertheless, we cannot eliminate the possibility that this was mediated by the genetic alterations and/or novel signaling pathways in these cells.
Altogether, we demonstrated that reversine plays an anticancer role in human breast cancer cells and could induce cell cycle arrest, cellular polyploidy, and apoptosis. Moreover, the apoptosis induction during reversine treatment in human breast cancer cells was through a caspase-dependent extrinsic pathway. This study suggests that reversine alone or in combination with other chemotherapeutic agents may be a novel therapeutic regimen for breast cancer patients.
References
Bernard-Marty C, Cardoso F, Piccart MJ. Facts and controversies in systemic treatment of metastatic breast cancer. Oncologist. 2004;9:617–32.
DeSantis C, Siegel R, Bandi P, Jemal A. Breast cancer statistics, 2011. CA Cancer J Clin. 2011;61:409–18.
Sorlie T, Perou CM, Tibshirani R, Aas T, Geisler S, Johnsen H, et al. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc Natl Acad Sci U S A. 2001;98:10869–74.
Carey LA, Perou CM, Livasy CA, Dressler LG, Cowan D, Conway K, et al. Race, breast cancer subtypes, and survival in the Carolina Breast Cancer Study. JAMA. 2006;295:2492–502.
Perou CM, Sorlie T, Eisen MB, van de Rijn M, Jeffrey SS, Rees CA, et al. Molecular portraits of human breast tumours. Nature. 2000;406:747–52.
Kim YK, Choi HY, Kim NH, Lee W, Seo DW, Kang DW, et al. Reversine stimulates adipocyte differentiation and downregulates Akt and p70(s6k) signaling pathways in 3T3-L1 cells. Biochem Biophys Res Commun. 2007;358:553–8.
Anastasia L, Sampaolesi M, Papini N, Oleari D, Lamorte G, Tringali C, et al. Reversine-treated fibroblasts acquire myogenic competence in vitro and in regenerating skeletal muscle. Cell Death Differ. 2006;13:2042–51.
Saraiya M, Nasser R, Zeng Y, Addya S, Ponnappan RK, Fortina P, et al. Reversine enhances generation of progenitor-like cells by dedifferentiation of annulus fibrosus cells. Tissue Eng Part A. 2010;16:1443–55.
Jung DW, Williams DR. Novel chemically defined approach to produce multipotent cells from terminally differentiated tissue syncytia. ACS Chem Biol. 2011;6:553–62.
Anastasia L, Pelissero G, Venerando B, Tettamanti G. Cell reprogramming: expectations and challenges for chemistry in stem cell biology and regenerative medicine. Cell Death Differ. 2010;17:1230–7.
D’Alise AM, Amabile G, Iovino M, Di Giorgio FP, Bartiromo M, Sessa F, et al. Reversine, a novel Aurora kinases inhibitor, inhibits colony formation of human acute myeloid leukemia cells. Mol Cancer Ther. 2008;7:1140–9.
McMillin DW, Delmore J, Weisberg E, Negri JM, Geer DC, Klippel S, et al. Tumor cell-specific bioluminescence platform to identify stroma-induced changes to anticancer drug activity. Nat Med. 2010;16:483–9.
Lee YR, Wu WC, Ji WT, Chen JY, Cheng YP, Chiang MK, et al. Reversine suppresses oral squamous cell carcinoma via cell cycle arrest and concomitantly apoptosis and autophagy. J Biomed Sci. 2012;19:9.
Hua SC, Chang TC, Chen HR, Lu CH, Liu YW, Chen SH, et al. Reversine, a 2,6-disubstituted purine, as an anti-cancer agent in differentiated and undifferentiated thyroid cancer cells. Pharm Res. 2012;29:1990–2005.
Hsieh TC, Traganos F, Darzynkiewicz Z, Wu JM. The 2,6-disubstituted purine reversine induces growth arrest and polyploidy in human cancer cells. Int J Oncol. 2007;31:1293–300.
Perreira M, Jiang JK, Klutz AM, Gao ZG, Shainberg A, Lu C, et al. “Reversine” and its 2-substituted adenine derivatives as potent and selective A3 adenosine receptor antagonists. J Med Chem. 2005;48:4910–8.
Nigg EA. Mitotic kinases as regulators of cell division and its checkpoints. Nat Rev Mol Cell Biol. 2001;2:21–32.
Bischoff JR, Anderson L, Zhu Y, Mossie K, Ng L, Souza B, et al. A homologue of Drosophila aurora kinase is oncogenic and amplified in human colorectal cancers. EMBO J. 1998;17:3052–65.
Sen S, Zhou H, Zhang RD, Yoon DS, Vakar-Lopez F, Ito S, et al. Amplification/overexpression of a mitotic kinase gene in human bladder cancer. J Natl Cancer Inst. 2002;94:1320–9.
Zhu J, Abbruzzese JL, Izzo J, Hittelman WN, Li D. AURKA amplification, chromosome instability, and centrosome abnormality in human pancreatic carcinoma cells. Cancer Genet Cytogenet. 2005;159:10–7.
Gritsko TM, Coppola D, Paciga JE, Yang L, Sun M, Shelley SA, et al. Activation and overexpression of centrosome kinase BTAK/Aurora-A in human ovarian cancer. Clin Cancer Res. 2003;9:1420–6.
Pihan GA, Purohit A, Wallace J, Malhotra R, Liotta L, Doxsey SJ. Centrosome defects can account for cellular and genetic changes that characterize prostate cancer progression. Cancer Res. 2001;61:2212–9.
Jeng YM, Peng SY, Lin CY, Hsu HC. Overexpression and amplification of Aurora-A in hepatocellular carcinoma. Clin Cancer Res. 2004;10:2065–71.
Zhou H, Kuang J, Zhong L, Kuo WL, Gray JW, Sahin A, et al. Tumour amplified kinase STK15/BTAK induces centrosome amplification, aneuploidy and transformation. Nat Genet. 1998;20:189–93.
Tatsuka M, Katayama H, Ota T, Tanaka T, Odashima S, Suzuki F, et al. Multinuclearity and increased ploidy caused by overexpression of the aurora- and Ipl1-like midbody-associated protein mitotic kinase in human cancer cells. Cancer Res. 1998;58:4811–6.
Chieffi P, Cozzolino L, Kisslinger A, Libertini S, Staibano S, Mansueto G, et al. Aurora B expression directly correlates with prostate cancer malignancy and influence prostate cell proliferation. Prostate. 2006;66:326–33.
Sorrentino R, Libertini S, Pallante PL, Troncone G, Palombini L, Bavetsias V, et al. Aurora B overexpression associates with the thyroid carcinoma undifferentiated phenotype and is required for thyroid carcinoma cell proliferation. J Clin Endocrinol Metab. 2005;90:928–35.
Vischioni B, Oudejans JJ, Vos W, Rodriguez JA, Giaccone G. Frequent overexpression of aurora B kinase, a novel drug target, in non-small cell lung carcinoma patients. Mol Cancer Ther. 2006;5:2905–13.
Zeng WF, Navaratne K, Prayson RA, Weil RJ. Aurora B expression correlates with aggressive behaviour in glioblastoma multiforme. J Clin Pathol. 2007;60:218–21.
Hardwicke MA, Oleykowski CA, Plant R, Wang J, Liao Q, Moss K, et al. GSK1070916, a potent Aurora B/C kinase inhibitor with broad antitumor activity in tissue culture cells and human tumor xenograft models. Mol Cancer Ther. 2009;8:1808–17.
Jani JP, Arcari J, Bernardo V, Bhattacharya SK, Briere D, Cohen BD, et al. PF-03814735, an orally bioavailable small molecule aurora kinase inhibitor for cancer therapy. Mol Cancer Ther. 2010;9:883–94.
Agnese V, Bazan V, Fiorentino FP, Fanale D, Badalamenti G, Colucci G, et al. The role of Aurora-A inhibitors in cancer therapy. Ann Oncol. 2007; 18 Suppl 6:vi47–52.
Acosta JJ, Munoz RM, Gonzalez L, Subtil-Rodriguez A, Dominguez-Caceres MA, Garcia-Martinez JM, et al. Src mediates prolactin-dependent proliferation of T47D and MCF7 cells via the activation of focal adhesion kinase/Erk1/2 and phosphatidylinositol 3-kinase pathways. Mol Endocrinol. 2003;17:2268–82.
Furth PA, Nakles RE, Millman S, Diaz-Cruz ES, Cabrera MC. Signal transducer and activator of transcription 5 as a key signaling pathway in normal mammary gland developmental biology and breast cancer. Breast Cancer Res. 2011;13:220.
Bjorge JD, Pang AS, Funnell M, Chen KY, Diaz R, Magliocco AM, et al. Simultaneous siRNA targeting of Src and downstream signaling molecules inhibit tumor formation and metastasis of a human model breast cancer cell line. PLoS ONE. 2011;6:e19309.
Finn RS, Bengala C, Ibrahim N, Roche H, Sparano J, Strauss LC, et al. Dasatinib as a single agent in triple-negative breast cancer: results of an open-label phase 2 study. Clin Cancer Res. 2011;17:6905–13.
Marotta LL, Almendro V, Marusyk A, Shipitsin M, Schemme J, Walker SR, et al. The JAK2/STAT3 signaling pathway is required for growth of CD44CD24 stem cell-like breast cancer cells in human tumors. J Clin Invest. 2011;121:2723–35.
Gupta N, Grebhardt S, Mayer D. Janus kinase 2—a novel negative regulator of estrogen receptor alpha function. Cell Signal. 2012;24:151–61.
Vaclavicek A, Bermejo JL, Schmutzler RK, Sutter C, Wappenschmidt B, Meindl A, et al. Polymorphisms in the Janus kinase 2 (JAK)/signal transducer and activator of transcription (STAT) genes: putative association of the STAT gene region with familial breast cancer. Endocr Relat Cancer. 2007;14:267–77.
Lin KL, Su JC, Chien CM, Tseng CH, Chen YL, Chang LS, et al. Naphtho[1,2-b]furan-4,5-dione disrupts Janus kinase-2 and induces apoptosis in breast cancer MDA-MB-231 cells. Toxicol In Vitro. 2010;24:1158–67.
Acknowledgments
This work was supported by grants from the National Science Council (NSC 99-2314-B-705-002-MY2) and Chiayi Christian Hospital (R98-11).
Conflict of interest
The authors confirm that there are no conflicts of interest.
Ethical approval
All the authors declare that this manuscript is original, has not been published before, and is not currently being considered for publication elsewhere. We confirm that the manuscript has been read and approved by all named authors and that there are no other persons who satisfied the criteria for authorship but are not listed. We further confirm that the order of authors listed in the manuscript has been approved by all of us.
Author information
Authors and Affiliations
Corresponding author
Additional information
C.-H. Kuo and Y.-C. Lu contributed equally to this work.
About this article
Cite this article
Kuo, CH., Lu, YC., Tseng, YS. et al. Reversine induces cell cycle arrest, polyploidy, and apoptosis in human breast cancer cells. Breast Cancer 21, 358–369 (2014). https://doi.org/10.1007/s12282-012-0400-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-012-0400-z