Abstract
Although giant cell arteritis (GCA), clinically designated as temporal arteritis, is recognized as a systemic disease, the breast may be the primary organ in which it is manifested. GCA of the breast is a rare disease that mainly occurs in postmenoposal elderly women. It manifests as nodules or pain in the breast, with or without tenderness, and is associated with significant constitutional symptoms that resemble those of polymyalgia rheumatica (PMR). These symptoms can be treated with or without prednisone therapy and can improve without the development of organ dysfunction. The clinical manifestations can often be recognized only by retrospective analysis after excisional biopsy. GCA of the breast occasionally mimics carcinoma, and its initial manifestations may be similar to those of other forms of vasculitis involving the breast, such as polyarteritis nodosa and Wegener granulomatosis. Biopsy is indispensable for establishing a definitive diagnosis. Thus far, the findings of imaging procedures, such as mammography and ultrasonography, for patients with mammary GCA have not been reported in detail, and no distinctive findings associated with this condition have been identified. Considering this and the fact that spontaneous remission may occur in some cases, mammary GCA probably often goes undiagnosed or may be misdiagnosed as an ordinary mammary disease. GCA of the breast should be considered as a potential diagnosis in the case of elderly women presenting with PMR-like symptoms and tenderness, lumps, or pain in the breast. We report a case of GCA affecting the breast and review previous reports on this condition in an attempt to summarize the features that distinguish this disease from other vascular diseases of the breast.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Giant cell arteritis (GCA) of the breast is a rare disease that mainly occurs in postmenoposal elderly women. Although it is a systemic disease, it often primarily involves the breast. Since the first case of mammary arteritis reported by Waugh in 1950 [1], some cases of mammary GCA, as either the primary clinical feature or the dominant feature of a generalized disease, have been reported. The characteristic clinical findings include tender unilateral or bilateral nodules of the breast, significant constitutional symptoms of anorexia, weight loss, myalgia, fever, and arthralgia. These symptoms should be treated rapidly, with or without prednisone therapy, and they can improve without the development of organ dysfunction [1–18]. These typical features suggest that GCA of the breast is a unique syndrome [2].
We present a case of GCA affecting the breast and review previously published reports on this condition in an attempt to summarize the features that distinguish this disease from other vascular diseases of the breast.
Case report
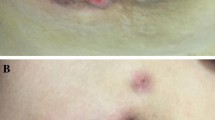
A 74-year-old woman visited our hospital, presenting with tenderness in both breasts, which had persisted for several months, a subjective symptom of swelling, and erythema, which she had recently noticed. She also had mild trismus, but no headaches or visual disturbance. Physical examination confirmed the presence of multiple tender lumps (approximately 1 cm in diameter), diffuse erythema without edema in both breasts, and swollen soft lymph nodes in both axillae. A mammography (MMG) revealed bilateral vascular calcification with dense mammary parenchyma but no evidence of malignancy (Fig. 1). Ultrasonography (US) revealed no mass lesions in the breasts, although the mammary parenchyma appeared slightly hypoechoic (Fig. 2).
Considering inflammatory breast cancer as a potential diagnosis, we performed a needle biopsy and scheduled a follow-up visit. Six days later, she unexpectedly visited the hospital for the second time, presenting with severe pain in both breasts. The physical examination findings had not changed, and loxoprofen sodium, a nonsteroidal antiinflammatory drug (NSAID), was prescribed. The core needle biopsy (CNB) specimen did not exhibit any specific pathological features.
Eight days later, that is, 16 days after the patient’s first visit to the hospital, the erythema in both breasts had disappeared, and the lumps had become slightly softer. However, systemic symptoms, such as general fatigue, low-grade fever, arthralgia, and trismus, were present; this led us to perform a blood examination. The results of the laboratory tests revealed the following values: white blood cell count, 13.3 × 103 cells/μl; hemoglobin level, 10.7 g/dl; platelet count, 44.2 × 104 cells/μl; C-reactive protein level, 10.0 mg/dl. The serum levels of immunoglobulin G (IgG) and complement factor C3 were slightly elevated, but autoantibody screening, such as antinuclear antibody and rheumatoid factor, proved negative. We did not measure the erythrocyte sedimentation rate (ESR). The findings of chest radiography were normal. A rheumatologist at our institution suspected the condition to be temporal arteritis, but an ophthalmologist rejected this possibility. The persistence of pain and lumps in both the patient’s breasts indicated the urgent need for a definitive diagnosis; moreover, the patient herself sought an accurate diagnosis. An excisional biopsy was performed for a representative lump in order to clarify the pathology of the condition.
Continual treatment with loxoprofen sodium for 2 months was prescribed. By the end of the treatment period, the patient’s symptoms had completely resolved, and the lumps in her breasts had disappeared. Currently, that is, about 2 years after the biopsy, the patient is in excellent health.
Pathological findings: The biopsy sample obtained from the breast consisted of rubbery fibrous tissue (2 × 1 cm). Serial sections of this tissue showed a white area with no obvious nodular lesions, and the tissue appeared identical or very similar to normal breast tissue. Microscopic evaluation revealed that the breast tissue mainly comprised fat tissue and was atrophic. Some of the small and medium-sized arteries in the fat tissue showed granulomatous inflammation. Intimal thickening and luminal narrowing were noted in the vessels. The transmural inflammatory infiltrate contained lymphocytes, histiocytes, and several multinucleated giant cells (Figs. 3, 4). Further, the internal elastic lamina was found to be fragmented (Fig. 5). Intimal hyperplasia was present in varying degrees and resulted in obliteration of the vessels due to thrombus formation. No fibrinoid necrosis was detected (Figs. 3, 4).
Discussion
Arteritis that manifests itself in the mammary glands, with symptoms such as pain and/or lumps in the breast as the chief complaint, as noted in our case, has been rarely reported [1–23]. Arteritis of the breast is pathologically classified as conditions such as GCA, Wegener granulomatosis (WG), and polyarteritis nodosa (PAN).
The pathology of GCA typically involves fragmentation of the elastica, in association with giant cell infiltration, intimal proliferation, and narrowing of the vascular lumina. Because of these clinical features, GCA is usually recognized as temporal arteritis, polymyalgia rheumatica (PMR), large-vessel arteritis, and Takayasu’s arteritis [24, 25]. PAN clinically presents multisystemic panarteritis involving medium-sized and small arteries; it is accompanied by fibrinoid deposition in the vessel wall, dense inflammatory infiltration, and occasionally luminal occlusion due to narrowing and/or thrombosis. Localized forms of PAN can affect various organs, such as the skin [26], gallbladder [27], and cervix [28]. PAN of the breast is a rare disease that usually does not involve other organs [19, 20]. WG is characterized by distinct clinical and pathological features that include necrotizing granulomatous vasculitis of the arteries and veins in the upper and lower respiratory tracts, accompanied by glomerulonephritis. WG may affect the skin, joints, and eyes, and it rarely affects only the breasts [21]. It has been reported that in eight of ten patients, WG acquires breast involvement during its clinical course [22]. This condition can usually be distinguished from granulomatous mastitis or sarcoidosis on the basis of the organs involved and the clinical course. Such discrimination can typically be achieved by performing an excisional biopsy.
In our review of English medical literature, we encountered only 20 cases [1–18] of GCA, including the present case (Table 1). In all of the cases, the patients were elderly women (median age, 65 years; range, 52–79 years). The mammary involvement was bilateral in 50% of the cases [1, 3, 6–9, 13–15, 18], and the onset of the condition was heterochronic in two of these cases [1, 13].
With regard to symptoms indicative of breast involvement, lumps due to arteritis were present in 80% of the cases (16 of 20 patients) [1–9, 13–16, 18], and redness and tenderness, in the absence of lumps, were noted in 10% (2 of 20 patients) [12, 17]. Further, in 10% (2) of the cases [10, 11], breast carcinoma and arteritis were unexpectedly identified in contiguous segments of the same specimens. These patients had lumps, but no redness or pain in their breasts. It was difficult to determine whether the lumps were due to breast carcinoma or arteritis, and none of the reviewed reports have described the relationship between these two conditions. Many of the patients had multiple lumps in both breasts; however, of 16 patients who had palpable arteritis-related lumps, 4 had only a single lump in one breast [2, 4, 8, 14]. Spontaneous breast pain and tenderness were the chief complaints in 85% (17) of the cases [1–5, 7–9, 13–18]. The condition was suspected to be inflammatory carcinoma in four [12–14] of seven cases, including the present case in which redness was noted on the skin of the breasts. Further, breast cancer was strongly suspected in three cases [1, 6, 15] because the nipples had retracted and/or were fixed to the skin and the adjacent tissue; in one case [1], mastectomy was required because of these symptoms.
Of the reviewed cases of mammary GCA, MMG, US, and/or computed tomography (CT) were performed in eight cases [3, 12–15, 17, 18], including our case; however, no mass lesions or any other specific findings were noted in any of these cases. Moreover, no specific findings were noted for two breast carcinoma patients [10, 11], for whom imaging procedures should have been performed. All these patients had either multiple lumps in both breasts or no lumps; none of them had only one lump. In our case, MMG did not reveal any mass lesions, but indicated that the breast tissue was rather dense for the patient’s age; hence, we considered that small nodules may have been hidden within the tissue. However, US revealed that the breast tissue was homogeneous; this finding suggested that the pathogenesis of the condition was characterized by features such as multiple small nodules and diffuse erythema in both breasts. It is possible that localized breast lesions present specific findings in MMG and US.
In all the reviewed cases except one [1], analysis of the excisional biopsy specimens or the resected tissues provided crucial information that led to a definitive diagnosis. In the one exceptional case, a diagnosis of GCA was established before the biopsy, on the basis of the systemic symptoms, and the lumps in the breast were considered to be associated with systemic GCA. A diagnosis could not be achieved using a small amount of tissue, for example, the amount obtained by fine-needle aspiration (FNA) [12, 15, 16] or core-needle biopsy (CNB) [16] in any of the cases. Similarly, in our case, the CNB-derived sample did not contain the vessels required for the evaluation. This suggests that a considerable amount of tissue is required to achieve a diagnosis of GCA of the breast.
Symptoms not related to the mammary glands, such as low-grade fever, arthralgia, myalgia, anorexia, and those suggestive of PMR, were present in 65% (13) of the cases [2–4, 6, 7, 9–11, 13, 14, 16, 18]. Biochemical tests revealed an increase in the ESR, a mild increase in the white blood cell count, slight anemia, and the absence of autoantibodies, such as antinuclear antibodies and rheumatoid factors in almost all cases in which these parameters were examined. In our case, biochemical test and PMR-like manifestations led our rheumatologist to suspect the condition to be temporal arteritis, but unfortunately, our ophthalmologist rejected this possibility because of the absence of visual disturbance. Visceral organ involvement was not observed in any of the cases, and the prognosis was good in all cases. However, one patient [10] developed reversible visual disturbance as a possible complication of temporal arteritis, which is a typical clinical feature of GCA. With regard to the clinical course of the condition, spontaneous remission occurred in 30% (6) of the cases [1, 5, 6, 8, 15, 17] after removal of the lumps or even without any treatment. In 60% (12) of the cases [2–4, 7, 9–14, 16, 18], the condition improved with prednisone treatment and in 10% (2) of the cases [14], including our case, with NSAID treatment. A previous report has described the case of one patient with PAN [23] where the painful mass of mammary tissue developed central necrosis after surgical debridement, and this eventually led to ulceration of the breast skin; however, no such case has been reported for patients with GCA.
A temporal artery biopsy was performed in 20% (4) [2, 4, 10, 11] of the reviewed cases; analysis of the biopsy specimen indicated the condition to be GCA in only one of these cases, but revealed the artery to be normal in the other cases. In another case [9], the condition was definitively diagnosed as GCA of the thyroid artery after a thyroid lobectomy had been performed for adenomatous goiter. GCA generally occurs in branches of the cranial arteries such as the temporal artery; therefore, it is reasonable to assume that it can also develop in branches of the carotid artery, such as the thyroid artery, or in branches of the subclavian artery, such as the internal mammary artery and the external thoracic artery (i.e., in the breasts). Furthermore, considering that spontaneous remission may occur in some cases, mammary GCA probably often goes undiagnosed. Moreover, GCA of the breast can be mistaken for an ordinary mammary disease if no distinctive features are noted in imaging studies.
Prednisone treatment has proven effective for mammary GCA, and it improves both the general and breast-specific manifestations of the disease. Therefore, this treatment is considered essential for patients with severe symptoms. However, because of the adverse side effects associated with long-term steroid therapy [2–4, 12, 18], a definitive diagnosis should be established by performing a biopsy before the initiation of prednisone treatment. In cases of mammary GCA mimicking breast cancer (e.g., [6]), a biopsy could eliminate the need for mastectomy. A definitive diagnosis of GCA is a welcome relief for both patients and their physicians because of the associated expectation that the symptoms will gradually improve with NSAID or prednisone treatment. Interestingly, some cases of WG [22, 23] have been reported, wherein the breast seemed to be the first organ involved and the manifestations resembled those of mammary GCA. In such cases, where subclinical manifestations are present in organs other than the breasts, delayed diagnosis and inadequate initial treatment may give rise to lethal conditions, including organ failure; therefore, it is important to establish an accurate early differential diagnosis by performing a biopsy.
Conclusion
GCA of the breast may be misdiagnosed as an ordinary mammary disease. Physicians should consider the possibility of vasculitis or even GCA of the breasts among patients with pain or lumps in the breasts. Further, the importance of biopsy for ensuring adequate treatment should be recognized.
Abbreviations
- GCA:
-
Giant cell arteritis
- NSAIDs:
-
Nonsteroidal anti-inflammatory drugs
- ESR:
-
Erythrocyte sedimentation rate
- WG:
-
Wegener granuromatosis
- PAN:
-
Polyarteritis nodosa
- MMG:
-
Mammography
- US:
-
Ultrasound
- CT:
-
Computed tomography
- FNA:
-
Fine-needle aspiration
- CNB:
-
Core needle biopsy
- PMR:
-
Polymyalgia rheumatica
References
Waugh TR. Bilateral mammary arteritis; report of a case. Am J Pathol. 1950;26:851–61.
Susmano A, Roseman D, Haber MH. Giant cell arteritis of the breast. A unique syndrome. Arch Intern Med. 1990;150:900–4.
McCarty DJ, Imbrigia J, Hung JK. Vasculitis of the breasts. Arthritis Rheum. 1968;11:796–803.
Dega FJ, Hunder GG. Vasculitis of the breast: an unusual manifestation of polyarteritis. Arthritis Rheum. 1974;17:973–6.
Chaitin B, Kohout ND, Goldman RL. Focal arteries of the breast. Angiology. 1981;32:334–7.
Potter BT, Housley E, Thomson D. Giant-cell arteritis mimicking carcinoma of the breast. Br Med J (Clin Res Ed). 1981;282:1665–6.
Thaell JF, Saue GL. Giant cell arteritis involving the breasts. J Rheumatol. 1983;10:329–31.
Nirodi NS, Stirling WJ, White MF. Giant cell arteritis presenting as a breast lump. Br J Clin Pract. 1985;39:84–6.
Stephenson TJ, Underwood JC. Giant cell arteritis: an unusual cause of palpable masses in the breast. Br J Surg. 1986;73:105.
Clement PB, Senges H, How AR. Giant cell arteritis of the breast: case report and literature review. Hum Pathol. 1987;18:1186–9.
Horne D, Crabtree TS, Lewkonia RM. Breast arteritis in polymyalgia rheumatica. J Rheumatol. 1987;14:613–5.
Cook DJ, Bensen WG, Carroll JJ, Joshi S. Giant cell arteritis of the breast. CMAJ. 1988;139:513–5.
Kim KH, Yang WI, Choi IJ. Giant cell arteritis of the breast: a case report. Yonsei Med J. 1990;31:80–4.
McKendry RJ, Guindi M, Hill DP. Giant cell arteritis (temporal arteritis) affecting the breast: report of two cases and review of published reports. Ann Rheum Dis. 1990;49:1001–4.
Pappo I, Beglaibter N, Amir G. Mammary arteritis mimicking cancer. Case report. Eur J Surg. 1992;158:191–3.
Lau Y, Mak YF, Hui PK, Ahchong AK. Giant cell arteritis of the breast. Aust N Z J Surg. 1996;66:259–61.
Anim JT, van Herk EJ. Giant cell arteritis of the breast. Med Princ Pract. 2004;13:234–6.
Marie I, Audeguy P, Francois A, Kergal F, Richard C. Giant cell arteritis presenting as a breast lesion: report of a case and review of the literature. Am J Med Sci. 2008;335:489–91.
Ng WF, Chow LT, Lam PW. Localized polyarteritis nodosa of breast–report of two cases and a review of the literature. Histopathology. 1993;23:535–9.
Trueb RM, Scheidegger EP, Pericin M, Singh A, Hoffmann U, Sauvant G, et al. Periarteritis nodosa presenting as a breast lesion: report of a case and review of the literature. Br J Dermatol. 1999;141:1117–21.
Jordan JM, Manning M, Allen NB. Multiple unusual manifestations of Wegener’s granulomatosis: breast mass, microangiopathic hemolytic anemia, consumptive coagulopathy, and low erythrocyte sedimentation rate. Arthritis Rheum. 1986;29:1527–31.
Jordan JM, Rowe WT, Allen NB. Wegener’s granulomatosis involving the breast. Report of three cases and review of the literature. Am J Med. 1987;83:159–64.
Veerysami M, Freeth M, Carmichael AR, Carmichael P. Wegener’s granulomatosis of the breast. Breast J. 2006;12:268–70.
Alarcon-Segovia D. The necrotizing vasculitides. A new pathogenetic classification. Med Clin North Am. 1977;61:241–60.
Healey LA, Wilske KR. Manifestations of giant cell arteritis. Med Clin North Am. 1977;61:261–70.
Thomas RH, Black MM. The wide clinical spectrum of polyarteritis nodosa with cutaneous involvement. Clin Exp Dermatol. 1983;8:47–59.
Bohrod MG, Bodon GR. Isolated polyarteritis nodosa of the gallbladder. Am Surg. 1970;36:681–5.
Ansell ID, Evans DJ, Wight DG. Asymptomatic arteritis of the uterine cervix. J Clin Pathol. 1974;27:664–8.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kadotani, Y., Enoki, Y., Itoi, N. et al. Giant cell arteritis of the breast: a case report with a review of literatures. Breast Cancer 17, 225–232 (2010). https://doi.org/10.1007/s12282-009-0120-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-009-0120-1