Abstract
Individual monocyte subsets have been associated with atherosclerotic disease, but their distribution has not been evaluated in aortic valve stenosis (AS) so far. In the present study, we have asked whether levels of the circulating intermediate monocyte subset are increased in AS. Classical (CD14++CD16−), intermediate (CD14++CD16+), and non-classical (CD14+CD16++) CD86-positive monocytes and monocyte activation (intensity of CD11b expression) were determined by flow cytometry in peripheral blood of patients with severe AS (n = 100) and matched AS-free controls (n = 75). AS patients exhibited significantly higher levels of circulating intermediate monocytes, while levels of circulating classical and non-classical monocytes or monocyte activation did not differ compared to controls. The difference in levels of intermediate monocytes between groups was independent of age, gender, BMI, LDL-C, NT-proBNP, NYHA functional class, or creatinine levels. The present pilot study provides evidence of an association of severe AS with increased levels of circulating intermediate monocytes. Further studies need to clarify whether this finding is related to the inflammatory status and hemodynamic disturbances associated with severe AS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Severe aortic valve stenosis (AS) represents the most prevalent valvular disease in older adults [1]. While in the past, AS was considered to be a passive degeneration of valve tissue it is nowadays recognized as an active and chronic inflammatory disease. Its pathogenesis shares similarities with atherosclerotic plaque development including systemic inflammation and ectopic calcification processes [2–4]. During the development of AS lipoproteins and immune cells, in particular monocytes, infiltrate the aortic valve tissue, where they become macrophages, take up oxidized lipids, maintain inflammatory processes by secretion of inflammatory mediators, and promote calcification of the valve [5–8]. Despite similarities between AS and atherosclerosis in terms of risk factors and involvement of inflammation, differences exist in particular for later stage pathology, in which fibrotic and calcification processes predominate in AS distinct to atherosclerosis (see [9] for review).
Monocytes originate in the bone marrow, from where they are mobilized and released into the circulation by chemokine stimuli such as monocyte chemoattractant protein-1 (MCP-1) [10, 11]. In humans, the current nomenclature of monocytes [12] differentiates three subsets according to their surface markers CD14 and CD16: classical (CD14++CD16−), intermediate (CD14++CD16+), and non-classical (CD14 + CD16++). Classical monocytes comprise the largest group of the three subsets (80–85%), while CD16-positive monocytes account for approximately 10–20% of all monocytes [12]. Levels of intermediate monocytes are rather low under healthy conditions, but are preferentially mobilized in inflammatory settings [10, 13]. They have been designated as the more inflammatory subtype as they have a higher capacity to produce inflammatory cytokines such as tumor necrosis factor (TNF)-α or interleukin-1β (IL-1β) compared to classical and non-classical monocytes [10, 14]. Particularly circulating CD16-positive monocytes have been associated with atherosclerotic disease and were shown to be predictors for cardiovascular (CV) risk and prognostic markers after acute myocardial infarction [15–17]. For example, in the HOM SWEET HOMe (heterogeneity of monocytes in subjects who undergo elective coronary angiography - the Homburg evaluation) study, comprising of 951 patients undergoing coronary angiography, frequencies of intermediate monocytes (but not of classical and non-classical monocytes) independently predicted future CV events [15].
So far, the distribution of individual circulating monocyte subsets has not been evaluated in aortic valve stenosis. Recently, Shimoni et al. reported that CD14+ positive monocytes are increased in patients with moderate to severe AS compared to AS-free controls, but monocytes subsets have not been further differentiated in that study [18]. However, based on the inflammatory status and the disturbed hemodynamic in the presence of advanced AS, it can be hypothesized that the distribution of individual circulating monocyte subsets is changed in these patients.
In the present pilot study, we have asked whether levels of circulating intermediate monocytes are increased in patients with AS.
Methods
Study Design and Population
From 2013 to 2016, patients with acquired severe AS and control patients without AS were consecutively screened at the Charité-Universitätsmedizin Berlin, Campus Mitte (Berlin, Germany). All patients had been hospitalized for diagnostic and/or therapeutic procedures to a non-intensive care cardiology ward or cardiothoracic surgical ward. Of 711 patients with severe AS screened 436 patients did not meet in/or exclusion criteria and 175 patients declined participation in the study resulting in 100 AS patients, who were included into the study (Online Resource 1). In parallel, 75 age- and gender-matched control patients without AS were selected and recruited to the study. Reasons for admission of control patients to the hospital were: stable coronary artery disease (CAD, n = 26), exclusion of CAD (n = 12), atrial fibrillation (n = 18), stable chronic heart failure (n = 13), pacemaker, and/or implantable cardioverter-defibrillator implantation for intermittent AV-Block III or sick sinus syndrome (n = 4), obstructive sleep apnea (n = 1), moderate tricuspid regurgitation (n = 1).
Inclusion criteria were written informed consent, age >18 years, and (except for controls) severe AS. Exclusion criteria comprised history of congenital bicuspid aortic valve, acute coronary syndrome or stroke within 30 days, signs of acute infection, endocarditis, sepsis or SIRS with fever, leukocytosis (>11*103/μl; reference range: 4.5–11.0*103/μl), C-reactive protein (CRP) levels >15 mg/dL or current antibiotic therapy, infectious disease, rheumatic or non-rheumatic autoimmune diseases that can trigger an inflammatory reaction, current immunosuppressive therapy, severe acute or chronic renal failure (glomerular filtration rate <30 mL/min/1.73 m2), ongoing malignant disease, acute fractures, surgery within 30 days.
Written informed consent was obtained from each study participant. The study protocol was approved by the Ethics Committee of the Charité-Universitätsmedizin Berlin. The study complied with the Declaration of Helsinki. Medical history was assessed in all study participants by clinical interview and medical records. Functional class was assessed according to the New York Heart Association (NYHA) classification. CAD was defined as a history of myocardial infarction or evidence of CAD on coronary angiography or computer tomography. Peripheral artery disease (PAD) was defined as an ankle-brachial pressure index below 0.90 and/or a history of intermittent claudication, evidence of PAD in peripheral angiography or ultrasound, peripheral arterial bypass, angioplasty or amputation.
Echocardiographic analyses were performed according to recommendations of the American Society of Echocardiography (ASE) and European Association of Cardiovascular Imaging (EACVI) [19]. Severe AS was defined as an aortic valve area (AVA) of <1.0 cm2 or indexed for body surface area of <0.6 cm2/m2, mean transaortic pressure gradient of >40 mmHg or peak aortic jet velocity of >4.0 m/s according to the European Society of Cardiology (ESC) guidelines and EAE/ASE recommendations for echocardiographic assessment of valve stenosis [20, 21]. AVA was not available in only five AS patients.
Blood Sampling and Biochemical Studies
Blood samples were collected from cubital veins on the day of admission to the hospital. Standard laboratory parameters including differential blood count, N-terminal pro-B-type natriuretic peptide (NT-proBNP; Elecsys; Roche Diagnostics GmbH, Mannheim, Germany), interleukin-6 (IL-6), TNF-α (both IMMULITE; Siemens, Eschborn, Germany), and CRP (Roche Diagnostics GmbH) were obtained by established assays.
Flow Cytometry
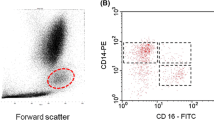
Whole blood samples were collected in EDTA tubes and analyzed directly after collection. 200 μL of whole blood was stained with monoclonal antibodies (CD86 PE [B7–2; Biolegend, San Diego, USA], CD14 PB [M5E2; Biolegend], CD16 APC [3G8; Biolegend], CD11b PECy7 [ICRF44; Biolegend]) at 4 °C for 15 minutes in the dark before incubation with lysing reagent (EasyLyse, Dako, Carpinteria, USA) at room temperature for 15 minutes. Samples were centrifuged at 300×g for 5 minutes, supernatant was removed, cells were resuspended in phosphate-buffered saline, and run on a flow cytometer (CyAn™ ADP Analyzer; Beckman Coulter, Inc., Fullerton, USA). Data was analyzed using Summit™ 4.3 software applying the following gating strategy (in adaption to [22]): first, peripheral blood mononuclear cells (PBMCs) were chosen and plotted on a CD86 histogram, eliminating granulocytes; monocytes were identified as CD86+ cells; secondly, CD86+ leukocytes were depicted in a FSC/SSC dot plot for monocytes specific scatter properties; thirdly, monocytes were divided into three subsets: CD14++CD16− (classical), CD14++CD16+ (intermediate), and CD14 + CD16++ (non-classical) according to the surface expression pattern of CD14 and CD16. To differentiate between intermediate and non-classical monocytes, a straight vertical line was drawn to the left of the CD14 staining of the classical monocyte subset in the CD14 and CD16 dot plot [22, 23]. Monocyte activation was assessed by median fluorescence intensity (MFI) of CD11b staining for total monocytes and each individual monocyte subset (in adaption to [24]). Analyses of flow cytometry data were performed by two blinded observers; results represent averaged values from both analyses. Intraclass correlation coefficient was calculated using SPSS 23.0 (SPSS Inc.) to evaluate interobserver variability of flow cytometry analyses. Interobserver variability was 0.85 (95% confidence interval [CI]: 0.80–0.89), 0.88 (CI: 0.84–0.91), 0.97 (CI: 0.96–0.98), and 0.99 (CI: 0.99–1.00) for classical, intermediate, and non-classical monocyte subsets and total monocyte activation, respectively.
Statistical Analysis
Results are generally expressed as arithmetic mean ± standard deviation (SD) for normally distributed data, as median with interquartile ranges (IQR = 25th–75th percentile) for non-normally distributed data, and categorical data are presented as absolute numbers and respective percentages. Mann-Whitney U test was used for comparison of two independent groups. Correlations were calculated with Spearman’s rank correlation coefficient. Frequencies of various groups were compared by chi-square test. Non-parametric analysis of covariance (with covariates: age, body mass index (BMI), low-density lipoprotein cholesterol (LDL-C), NT-proBNP, NYHA functional class and creatinine) and multifactorial analyses (with factors: gender, diabetes, hypercholesterolemia, and medication with angiotensin-converting enzyme inhibitor, loop diuretics, or statins) were performed for intermediate monocytes based on Brunner [25]. Statistical analyses were performed using SPSS 23.0 (SPSS Inc.) and SAS 9.4 (Statistical Analysis System Institute Inc.) software; p <0.05 was considered statistically significant. A post hoc power analysis was performed based on the observed results of intermediate monocytes with a sample size of 75 and alpha of 0.05 using nQuery Advisor program (version 7.0; Statistical Solutions Ltd.).
Results
Clinical Characteristics
Clinical characteristics of AS patients and controls are shown in Table 1. Both groups were similar in terms of age, gender distribution, renal function, and presence of CAD or CV risk factors. AS patients had significantly higher levels of NT-proBNP and were more symptomatic according to the NYHA functional class (Table 1).
There were no significant differences in white blood cell counts, total monocyte counts, levels of CRP, IL-6 or TNF-α between AS patients and controls (Table 2).
Monocyte Subsets and Activation
Patients with severe AS had significantly higher absolute and relative levels of circulating intermediate monocytes compared to controls (6.5% [5.2–7.9%] versus 5.7% [4.5–6.6%], p = 0.001), while levels of circulating classical (77.9% [74.7–81.7%] versus 80.0% [74.9–83.6%], p = 0.179) and circulating non-classical (8.7% [6.1–11.5%] versus 8.4% [5.6–11.5%], p = 0.488) monocyte subsets did not differ significantly between both groups (Fig. 1, Table 3). Next, we evaluated whether potential confounders (heart failure, age, BMI, or renal function) that are associated with levels of individual monocyte subsets [15, 26, 27], factors that predispose for AS (age, gender, or LDL-C) [28, 29] or differences in baseline characteristics (NYHA functional class, NT-proBNP, BMI, medication with angiotensin-converting enzyme inhibitor or loop diuretics) of our study groups had an impact on the difference in levels of circulating intermediate monocytes between groups. The difference in levels of circulating intermediate monocytes was significant after adjustment for the covariates age, BMI, LDL-C, NT-proBNP, NYHA functional class, and levels of creatinine (p = 0.006 for relative and p = 0.01 for absolute levels of circulating intermediate monocytes). Furthermore, multifactorial analyses showed that the difference was independent of the factors gender, diabetes, hypercholesterolemia, and medication with angiotensin-converting enzyme inhibitor, loop diuretics, or statins (Online Resource 2). A post hoc power analysis of the study showed a power of 86% and 72% to detect the observed differences in relative and absolute levels of circulating intermediate monocytes between groups, respectively.
Relative distribution of circulating classical (CD14++CD16−), intermediate (CD14++CD16+), and non-classical (CD14+CD16++) monocyte subsets in patients with severe aortic valve stenosis (AS, n = 100) and AS-free controls (n = 75). Data are presented as medians with 25/75 percentiles (boxes) and 10/90 percentiles (bars).
We did not detect significant differences in monocyte activation for all monocytes and each individual monocyte subset (Table 3).
There was no statistically significant association between aortic valve area or mean transaortic pressure gradient and levels of total monocytes, individual monocyte subsets or monocyte activation in AS patients.
Discussion
In the present study, we have evaluated the distribution of circulating monocyte subsets in a large cohort of patients with severe AS and found that levels of intermediate monocytes are increased in the presence of AS compared to AS-free controls. This result was independent of gender or other potential confounders such as age, BMI, or parameters of heart failure. To our knowledge, this is the first report on the distribution of individual monocyte subsets in AS. Recently, Shimoni et al. reported that CD14-positive monocytes are increased in patients with moderate to severe AS compared to AS-free controls and correlate negatively with AVA [18]; however, further differentiation of individual monocyte subsets was not performed in that study. In contrast to Diehl et al. [24], who reported an increased number of activated monocytes in patients with AS, we did not observe differences in monocyte activation neither for total monocytes nor for each individual monocyte subset in our larger cohort of AS patients.
Intermediate monocytes are designated as the more inflammatory monocyte subset as they exhibit a higher capacity to produce inflammatory cytokines compared to classical and non-classical monocytes [10, 14]. As levels of circulating intermediate monocytes have been linked to atherosclerotic cardiovascular diseases and outcome [15, 16], our present findings extend this association to AS. The extent of the difference in levels of circulating intermediate monocytes between AS patients and controls in our study was rather small. However, increased levels of intermediate monocytes to a similar (small) extent were shown to be predictive for future cardiovascular events (in subjects referred for elective coronary angiography) in the HOM SWEET HOMe study [15].
So far, reasons for elevated levels of circulating intermediate monocytes in the presence of severe AS remain speculative: AS patients exhibit an increased inflammatory status including elevated serum levels of inflammatory mediators such as MCP-1 [30–32]; this may derive from the inflamed aortic valve tissue itself, but as well as from the deteriorating hemodynamic as a consequence of the progressing obstruction of the valve. MCP-I is well known for its recruitment of monocytes to inflammatory sites, but it also plays a central role in the mobilization of monocytes from the bone marrow to the peripheral circulation, which is mediated via C-C chemokine receptor type 2 (CCR2) [11, 33]. Besides inflammation, it was reported that changes in hemodynamics (e.g., by exercise) induce expression of MCP-1, but also independently increase levels of circulating intermediate monocytes [34]. Thus, it can be hypothesized that increased levels of circulating intermediate monocytes in AS are a result of the interplay between chronic inflammation and significant hemodynamic disturbances.
However, our observational study cannot answer the question whether elevated levels of circulating intermediate monocytes in the presence of AS represent a causal factor for AS progression, or rather reflect a consequence of the disease [3, 35]. Proving causality of individual monocyte subsets in AS progression in humans would require large prospective, long-term studies with longitudinal assessments of monocyte subsets. However, an answer to this question is of utmost importance: 1.) while sclerosis of the aortic valve is widely present in an older population, only a minority (10–15%) progresses to hemodynamically relevant obstructive aortic valve stenosis; stimuli triggering this transformation are unknown and biomarkers identifying patients at risk are lacking so far [28, 35, 36]; 2.) as medical therapies including statins failed to prevent AS progression once aortic sclerosis is present (in contrast to atherosclerosis) [37], surgical aortic valve replacement or transcatheter aortic valve implantation (TAVI) remain the only therapeutic options once AS becomes severe and/or symptomatic. Thus, novel, causal treatment targets to prevent, delay or halt progression of AS are urgently needed. Our finding of increased levels of circulating intermediate monocytes in severe AS may serve as a departure for further studies to evaluate the particular roles of individual circulating monocyte subsets in the pathogenesis of AS.
There are some limitations in the present study. Although we found a robust association of circulating intermediate monocytes with severe AS, the clinical significance of this finding deriving from one time point measurements remains to be determined. In this regard, it would be important for future studies to prove whether circulating monocyte subsets reflect the inflammatory status within the aortic valve itself for example by association with inflammatory activity in the valve as assessed by positron emission tomography using the tracer 18F-fluorodeoxyglucose [38, 39] or by determining inflammatory M1 versus anti-inflammatory M2 macrophage content within aortic valve specimen [40]. In contrast to the study from Shimoni et al. on CD14-positive monocytes, we did not observe an association of AVA with individual monocyte subsets, which may be explained by the fact that we only recruited patients with severe AS, while Shimoni et al. included patients with moderate to severe AS [18]. Levels of CRP, IL-6, and TNF-α did not differ significantly between AS patients and AS-free controls; this may to some extent be explained by the stringent patient selection criteria, excluding patients with markedly elevated CRP levels in order to minimize confounding factors for the evaluation of monocyte subsets [28].
In conclusion, our data provide evidence of an association of severe AS with increased levels of circulating intermediate monocytes. Our pilot study underlines the importance to further evaluate dynamics and functional characteristics of circulating monocyte subsets, in particular of intermediate monocytes, in AS.
Abbreviations
- AS:
-
Aortic valve stenosis
- AVA:
-
Aortic valve area
- CAD:
-
Coronary artery disease
- CV:
-
Cardiovascular
- IL-1β:
-
Interleukin-1β
- IL-6:
-
Interleukin-6
- MCP-1:
-
Monocyte chemoattractant protein-1
- NT-proBNP:
-
N-terminal pro-B-type natriuretic peptide
- NYHA:
-
New York Heart Association
- PAD:
-
Peripheral artery disease
- TNF-α:
-
Tumor necrosis factor-α
- WBC:
-
White blood cells
References
Iung, B., Baron, G., Butchart, E. G., Delahaye, F., Gohlke-Barwolf, C., Levang, O. W., et al. (2003). A prospective survey of patients with valvular heart disease in Europe: the euro heart survey on valvular heart disease. European Heart Journal, 24(13), 1231–1243 http://www.ncbi.nlm.nih.gov/pubmed/12831818.
Stangl, V., Baldenhofer, G., Knebel, F., Zhang, K., Sanad, W., Spethmann, S., et al. (2012). Impact of gender on three-month outcome and left ventricular remodeling after transfemoral transcatheter aortic valve implantation. The American Journal of Cardiology, 110(6), 884–890. doi:10.1016/j.amjcard.2012.04.063.
Galante, A., Pietroiusti, A., Vellini, M., Piccolo, P., Possati, G., De Bonis, M., et al. (2001). C-reactive protein is increased in patients with degenerative aortic valvular stenosis. Journal of the American College of Cardiology, 38(4), 1078–1082 http://www.ncbi.nlm.nih.gov/pubmed/11583885.
Gerber, I. L., Stewart, R. A., Hammett, C. J., Legget, M. E., Oxenham, H., West, T. M., et al. (2003). Effect of aortic valve replacement on c-reactive protein in nonrheumatic aortic stenosis. The American Journal of Cardiology, 92(9), 1129–1132 http://www.ncbi.nlm.nih.gov/pubmed/14583374.
Mazzone, A., Epistolato, M. C., Gianetti, J., Castagnini, M., Sassi, C., Ceravolo, R., et al. (2006). Biological features (inflammation and neoangiogenesis) and atherosclerotic risk factors in carotid plaques and calcified aortic valve stenosis: two different sites of the same disease? American Journal of Clinical Pathology, 126(4), 494–502. doi:10.1309/W75NTE5QBC9DXE03.
Freeman, R. V., & Otto, C. M. (2005). Spectrum of calcific aortic valve disease: pathogenesis, disease progression, and treatment strategies. Circulation, 111(24), 3316–3326. doi:10.1161/CIRCULATIONAHA.104.486738.
Skowasch, D., Schrempf, S., Wernert, N., Steinmetz, M., Jabs, A., Tuleta, I., et al. (2005). Cells of primarily extra-valvular origin in degenerative aortic valves and bioprostheses. European Heart Journal, 26(23), 2576–2580. doi:10.1093/eurheartj/ehi458.
Wypasek, E., Natorska, J., Grudzien, G., Filip, G., Sadowski, J., & Undas, A. (2013). Mast cells in human stenotic aortic valves are associated with the severity of stenosis. Inflammation, 36(2), 449–456. doi:10.1007/s10753-012-9565-z.
Dweck, M. R., Boon, N. A., & Newby, D. E. (2012). Calcific aortic stenosis: a disease of the valve and the myocardium. Journal of the American College of Cardiology, 60(19), 1854–1863. doi:10.1016/j.jacc.2012.02.093.
Stansfield, B. K., & Ingram, D. A. (2015). Clinical significance of monocyte heterogeneity. Clinical and Translational Medicine, 4, 5. doi:10.1186/s40169-014-0040-3.
Tsou, C. L., Peters, W., Si, Y., Slaymaker, S., Aslanian, A. M., Weisberg, S. P., et al. (2007). Critical roles for CCR2 and MCP-3 in monocyte mobilization from bone marrow and recruitment to inflammatory sites. The Journal of Clinical Investigation, 117(4), 902–909. doi:10.1172/JCI29919.
Ziegler-Heitbrock, L., Ancuta, P., Crowe, S., Dalod, M., Grau, V., Hart, D. N., et al. (2010). Nomenclature of monocytes and dendritic cells in blood. Blood, 116(16), e74–e80. doi:10.1182/blood-2010-02-258558.
Mukherjee, R., Kanti Barman, P., Kumar Thatoi, P., Tripathy, R., Kumar Das, B., & Ravindran, B. (2015). Non-classical monocytes display inflammatory features: validation in sepsis and systemic lupus erythematous. Scientific Reports, 5, 13886. doi:10.1038/srep13886.
Yang, J., Zhang, L., Yu, C., Yang, X. F., & Wang, H. (2014). Monocyte and macrophage differentiation: circulation inflammatory monocyte as biomarker for inflammatory diseases. Biomark Res, 2(1), 1. doi:10.1186/2050-7771-2-1.
Rogacev, K. S., Cremers, B., Zawada, A. M., Seiler, S., Binder, N., Ege, P., et al. (2012). CD14++CD16+ monocytes independently predict cardiovascular events: a cohort study of 951 patients referred for elective coronary angiography. Journal of the American College of Cardiology, 60(16), 1512–1520. doi:10.1016/j.jacc.2012.07.019.
Hristov, M., & Weber, C. (2011). Differential role of monocyte subsets in atherosclerosis. Thrombosis and Haemostasis, 106(5), 757–762. doi:10.1160/TH11-07-0500.
Tsujioka, H., Imanishi, T., Ikejima, H., Kuroi, A., Takarada, S., Tanimoto, T., et al. (2009). Impact of heterogeneity of human peripheral blood monocyte subsets on myocardial salvage in patients with primary acute myocardial infarction. Journal of the American College of Cardiology, 54(2), 130–138. doi:10.1016/j.jacc.2009.04.021.
Shimoni, S., Meledin, V., Bar, I., Fabricant, J., Gandelman, G., & George, J. (2016). Circulating CD14(+) monocytes in patients with aortic stenosis. Journal of Geriatric Cardiology, 13(1), 81–87. doi:10.11909/j.issn.1671-5411.2016.01.015.
Lang, R. M., Badano, L. P., Mor-Avi, V., Afilalo, J., Armstrong, A., Ernande, L., et al. (2015). Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. European Heart Journal. Cardiovascular Imaging, 16(3), 233–270. doi:10.1093/ehjci/jev014.
Vahanian, A., Alfieri, O., Andreotti, F., Antunes, M. J., Baron-Esquivias, G., Baumgartner, H., et al. (2012). Guidelines on the management of valvular heart disease (version 2012). European Heart Journal, 33(19), 2451–2496. doi:10.1093/eurheartj/ehs109.
Baumgartner, H., Hung, J., Bermejo, J., Chambers, J. B., Evangelista, A., Griffin, B. P., et al. (2009). Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. European Journal of Echocardiography, 10(1), 1–25. doi:10.1093/ejechocard/jen303.
Zawada, A. M., Rogacev, K. S., Schirmer, S. H., Sester, M., Bohm, M., Fliser, D., et al. (2012). Monocyte heterogeneity in human cardiovascular disease. Immunobiology, 217(12), 1273–1284. doi:10.1016/j.imbio.2012.07.001.
Ziegler-Heitbrock, L., & Hofer, T. P. (2013). Toward a refined definition of monocyte subsets. Frontiers in Immunology, 4, 23. doi:10.3389/fimmu.2013.00023.
Diehl, P., Nagy, F., Sossong, V., Helbing, T., Beyersdorf, F., Olschewski, M., et al. (2008). Increased levels of circulating microparticles in patients with severe aortic valve stenosis. Thrombosis and Haemostasis, 99(4), 711–719. doi:10.1160/TH07-05-0334.
Brunner, E., Domhof, S., & Langer, F. (2002). Nonparametric analysis of longitudinal data in factorial experiments (1st ed.pp. 187–210). New York: Wiley.
Heine, G. H., Ortiz, A., Massy, Z. A., Lindholm, B., Wiecek, A., Martinez-Castelao, A., et al. (2012). Monocyte subpopulations and cardiovascular risk in chronic kidney disease. Nature Reviews. Nephrology, 8(6), 362–369. doi:10.1038/nrneph.2012.41.
Goonewardena, S. N., Stein, A. B., Tsuchida, R. E., Rattan, R., Shah, D., & Hummel, S. L. (2016). Monocyte subsets and inflammatory cytokines in acute decompensated heart failure. Journal of Cardiac Failure, 22(5), 358–365. doi:10.1016/j.cardfail.2015.12.014.
Otto, C. M., & Prendergast, B. (2014). Aortic-valve stenosis--from patients at risk to severe valve obstruction. The New England Journal of Medicine, 371(8), 744–756. doi:10.1056/NEJMra1313875.
Smith, J. G., Luk, K., Schulz, C. A., Engert, J. C., Do, R., Hindy, G., et al. (2014). Association of low-density lipoprotein cholesterol-related genetic variants with aortic valve calcium and incident aortic stenosis. JAMA, 312(17), 1764–1771. doi:10.1001/jama.2014.13959.
Kapelouzou, A., Tsourelis, L., Kaklamanis, L., Degiannis, D., Kogerakis, N., & Cokkinos, D. V. (2015). Serum and tissue biomarkers in aortic stenosis. Glob Cardiol Sci Pract, 2015(4), 49. doi:10.5339/gcsp.2015.49.
Kastellanos, S. S., Toumpoulis, I. K., Aggeli, C., Zezas, S., Chlapoutakis, E., Kastellanos, S., et al. (2007). Time course of C-reactive protein, tumour necrosis factor-alpha and monocyte chemoattractant protein-1 following the surgical treatment of patients with aortic valve stenosis. Hellenic Journal of Cardiology, 48(1), 5–14 http://www.ncbi.nlm.nih.gov/pubmed/17388104.
Dimitrow, P. P., & Jawien, M. (2010). Anti-inflammatory effect of atorvastatin in patients with aortic sclerosis or mild aortic stenosis independent of hypercholesterolemia. Pharmacological Reports, 62(6), 1250–1254 http://www.ncbi.nlm.nih.gov/pubmed/21273686.
Mandl, M., Schmitz, S., Weber, C., & Hristov, M. (2014). Characterization of the CD14++CD16+ monocyte population in human bone marrow. PloS One, 9(11), e112140. doi:10.1371/journal.pone.0112140.
Van Craenenbroeck, A. H., Van Ackeren, K., Hoymans, V. Y., Roeykens, J., Verpooten, G. A., Vrints, C. J., et al. (2014). Acute exercise-induced response of monocyte subtypes in chronic heart and renal failure. Mediators of Inflammation, 2014, 216534. doi:10.1155/2014/216534.
Beckmann, E., Grau, J. B., Sainger, R., Poggio, P., & Ferrari, G. (2010). Insights into the use of biomarkers in calcific aortic valve disease. The Journal of Heart Valve Disease, 19(4), 441–452 http://www.ncbi.nlm.nih.gov/pubmed/20845891.
Novaro, G. M., Katz, R., Aviles, R. J., Gottdiener, J. S., Cushman, M., Psaty, B. M., et al. (2007). Clinical factors, but not C-reactive protein, predict progression of calcific aortic-valve disease: the cardiovascular health study. Journal of the American College of Cardiology, 50(20), 1992–1998. doi:10.1016/j.jacc.2007.07.064.
Rossebo, A. B., Pedersen, T. R., Boman, K., Brudi, P., Chambers, J. B., Egstrup, K., et al. (2008). Intensive lipid lowering with simvastatin and ezetimibe in aortic stenosis. The New England Journal of Medicine, 359(13), 1343–1356. doi:10.1056/NEJMoa0804602.
Dweck, M. R., Khaw, H. J., Sng, G. K., Luo, E. L., Baird, A., Williams, M. C., et al. (2013). Aortic stenosis, atherosclerosis, and skeletal bone: is there a common link with calcification and inflammation? European Heart Journal, 34(21), 1567–1574. doi:10.1093/eurheartj/eht034.
Dweck, M. R., Jones, C., Joshi, N. V., Fletcher, A. M., Richardson, H., White, A., et al. (2012). Assessment of valvular calcification and inflammation by positron emission tomography in patients with aortic stenosis. Circulation, 125(1), 76–86. doi:10.1161/CIRCULATIONAHA.111.051052.
Wang, R., Chen, W., Ma, Z., Li, L., & Chen, X. (2014). M1/M2 macrophages and associated mechanisms in congenital bicuspid aortic valve stenosis. Experimental and Therapeutic Medicine, 7(4), 935–940. doi:10.3892/etm.2014.1529.
Acknowledgements
We thank all the participants of the study. Our appreciation also goes to the following for their valuable support: Prof. Dr. Manfred Dietel and Dr. Iris Klempert, Ms. Nicole Rösener and Ms. Andrea Weller for technical assistance, Ms. Urte Lemma, Ms. Christine Scholz, and Ms. Annette Falkenthal for organizational support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study. No animal studies were carried out by the authors for this article.
Funding
This work was supported by the Friede-Springer-Herz-Stiftung (Germany) and clinical internal financing. BH and LH are participants in the BIH Charité Clinician Scientist Program funded by the Charité-Universitätsmedizin Berlin and the Berlin Institute of Health. BH received funding from the DZHK (German Center for Cardiovascular Research). PvD received funding from the German Society of Cardiology (DGK).
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Associate Editor Lorrie Kirshenbaum oversaw the review of this article
Rights and permissions
About this article
Cite this article
Hewing, B., Au, S.CD., Ludwig, A. et al. Severe Aortic Valve Stenosis in Adults is Associated with Increased Levels of Circulating Intermediate Monocytes. J. of Cardiovasc. Trans. Res. 10, 27–34 (2017). https://doi.org/10.1007/s12265-016-9726-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-016-9726-9